Introduction
Infections that at times affect intracranial structures are a prominent cause of secondary headaches in children.1 Petrous apicitis (PA) is an extremely rare complication of otitis media (OM), a very common childhood infection. PA is an infection that spreads from the middle ear to the apex of the temporal bone and is known as Gradenigo’s syndrome when it presents as the triad of deep facial pain, otorrhea, and abducens nerve palsy.2 However, usually only 1 of these signs is present, and the 3 signs rarely occur concurrently.3 Before the routine use of antibiotics, this syndrome was much more common and often had a lethal outcome. In this case report, we describe a case of PA in a 5-year-old child who was misdiagnosed for a time because of its presentation mainly as a headache, and the late onset of characteristic symptoms.
CASE PRESENTATION
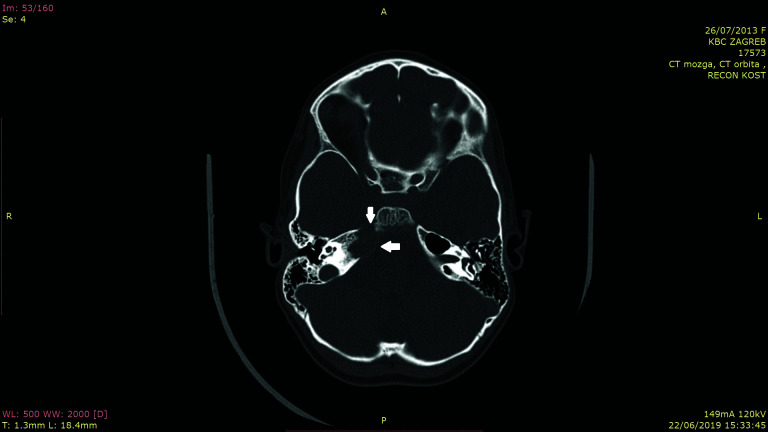
A 5-year-old girl presented to the emergency department with a unilateral headache on the right side, concentrated around her right ear. No ear secretion or fever was noted. She was diagnosed with non-suppurative OM, and amoxicillin and clavulanic acid were prescribed for 10 days. Tympanometry suggested middle ear effusion (type B tympanogram), and audiometry revealed ipsilateral moderate conductive hearing loss. Although the intensity of pain decreased after therapy, her headache persisted. A follow-up ENT examination 7 days later revealed that there were no signs of a tympanic membrane infection, and her leukocyte count was normal. However, her unilateral headache persisted, especially during the night, and she experienced some disturbances in her sense of balance during the day. Over the following 2 months, she was examined numerous times by neurologists as well as ENT and pediatric specialists, but no organic cause of the headache was detected. Computed tomography (CT) did not show any brain abnormalities. Chronic OM with effusion, a reaction to emotional stress, or neuropathic pain, were some of the diagnoses suggested at that time. The patient then presented to the ENT emergency department of our tertiary care center with the same symptoms. Her parents stated that in the past few days, the girl had been covering her right eye with her hand. There were no signs of eardrum infection and no pain in the right mastoid on percussion, but eye movement tests revealed right-sided abducens nerve palsy. A second CT scan along with magnetic resonance imaging (MRI) showed extensive destruction of the petrous part of the temporal bone below the carotid canal on the right, with expansion toward the inner auditory canal and Dorello’s canal (Figures 1 and 2). PA was diagnosed, and parenteral vancomycin, ceftriaxone and metronidazole were prescribed. The headache disappeared several days after the start of antibiotic therapy. The triple therapy was continued for 6 weeks, when the patient was discharged from the hospital with a complete resolution of the inflammation on MRI.
Figure 1.
CT scan
Figure 2.
MRI T2 sequence
DISCUSSION
Although PA or Gradenigo’s syndrome is associated with a characteristic triad of symptoms, the presence of all 3 symptoms is not very likely, even according to its author.2 According to later studies, the presence of all 3 symptoms occurs in approximately 25%4 or 13.6% of cases.3 Most studies and case reports agree that the most prominent signs are the combination of OM and deep facial or retro-orbital pain in the area of the first or second trigeminal nerve branches.5,6 Abducens nerve palsy seems to be the least frequent symptom and very rarely presents alone or prior to the other 2 signs.7 Our case, in which OM was the preceding event and abducens nerve palsy was a late symptom of the unrecognized severe intracranial inflammatory process, is thus in concordance with these statements. In the past, the entire triad could be observed more often because of the lack of antibiotic treatment and advanced imaging modalities. In addition, a change in the approach to this disorder can be seen from the literature: surgical treatment is becoming less common, with >50% cases in the 1970s compared with only 12% undergoing surgery in recent years.3,8 Currently, approximately 11% of all PA cases affect children,3 which can be attributed to effective medical and surgical treatment of OM. Nevertheless, the high grade of attentiveness required for diagnosing this condition must be emphasized. In our case, the initial symptoms were non-specific—apart from the OM treated in the beginning—the main complaint was a headache that lasted for weeks. Although our patient underwent examinations by numerous physicians, the condition was repeatedly misdiagnosed because of her non-specific symptoms. The patient experienced sleeping difficulties, decreased appetite, and personality changes. The problem with suspecting such a rare and dangerous condition in small children is its mimicking symptoms that could be classified as tension headache or migraine, associated with a common infection such as OM, or that it could even be psychogenic. Moreover, children are unable to precisely describe their symptoms and can often be noncompliant. In our case, this led to considering pregabalin to manage possible neuropathic pain and melatonin for a sleeping disorder. Another confounding fact was the sheer scarceness of this syndrome (<2 in 100 000 OM cases)9 and therefore, the lack of experience in recognizing its potential signs. In this case, the patient underwent a CT scan too early to detect the signs of intracranial propagation of the infection, resulting in an unwillingness to perform another imaging soon and thus postponing the necessary diagnostic procedure.
An intracranial inflammatory process such as the one reported here could have been an indication for mastoidectomy and petrosectomy with insertion of pressure equalizer (PE) tubes; however, in our case, the patient did not have radiologic evidence of mastoid involvement. Moreover, soon after the therapy initiation, the patient’s condition clinically and subjectively significantly improved. Because the control MRI scan showed regression of the process after triple antibiotic therapy, and also considering the age of the patient, we opted against such a radical surgical procedure. Finally, there were no signs of eardrum or tympanic cavity inflammation upon admission; therefore, we did not consider PE tube insertion to be necessary.
CONCLUSION
In summary, our case report shows the importance of a thorough approach to headache in children. The co-operation of ophthalmologists, neurologists, and ENT specialists is crucial in its diagnosis and management. Additional attention must be applied when examining a child with prolonged symptoms of headache that do not subside on standard therapy, especially in patients presenting with a recent medical history of OM.
Funding Statement
The authors declared that this study has received no financial support.
Footnotes
Informed Consent: Full written informed consent was obtained from the patient in using images of tissue samples and radiologic imaging after discussing the details of the case report contents.
Peer-review: Externally peer-reviewed.
Author Contributions: Concept – M.M., M.G.; Design – M.M.; Supervision – M.G.; Resource – B.M., M.M.; Materials – M.M., B.M.; Data Collection and/or Processing – B.M.; Analysis and/or Interpretation – M.M., B.M.; Literature Search – B.M.; Writing – B.M., M.M.; Critical Reviews – M.G.
Conflict of Interest: The authors have no conflict of interest to declare.
References
- 1. Langdon R, DiSabella MT. Pediatric headache: an overview. Curr Probl Pediatr Adolesc Health Care. 2017;47(3):44–65.. 10.1016/j.cppeds.2017.01.002) [DOI] [PubMed] [Google Scholar]
- 2. Gradenigo G. Über die Paralyse des nervus abducens bei otitis. Arch Ohrenheilkd. 1907;74(1):149–187.. 10.1007/BF01930369) [DOI] [Google Scholar]
- 3. Gadre AK, Chole RA. The changing face of petrous apicitis—a 40-year experience. Laryngoscope. 2018;128(1):195–201.. 10.1002/lary.26571) [DOI] [PubMed] [Google Scholar]
- 4. Chole RA, Donald PJ. Petrous apicitis. Clinical considerations. Ann Otol Rhinol Laryngol. 1983;92(6 Pt 1):544–551.. 10.1177/000348948309200603) [DOI] [PubMed] [Google Scholar]
- 5. Gillanders DA. Gradenigo’s syndrome revisited. J Otolaryngol. 1983;12(3):169–174.. [PubMed] [Google Scholar]
- 6. Jensen PVF, Hansen MS, Møller MN, Saunte JP. The forgotten syndrome? Four cases of Gradenigo’s syndrome and a review of the literature. Strabismus. 2016;24(1):21–27.. 10.3109/09273972.2015.1130067) [DOI] [PubMed] [Google Scholar]
- 7. Price T, Fayad G. Abducens nerve palsy as the sole presenting symptom of petrous apicitis. J Laryngol Otol. 2002;116(9):726-729. 10.1258/002221502760238055) [DOI] [PubMed] [Google Scholar]
- 8. Rossi N, Swonke ML, Reichert L, Young D. Gradenigo’s syndrome in a four-year-old patient: a rare diagnosis in the modern antibiotic era. J Laryngol Otol. 2019;133(6):535–537.. 10.1017/S0022215119001026) [DOI] [PubMed] [Google Scholar]
- 9. Goldstein NA, Casselbrant ML, Bluestone CD, Kurs-Lasky M. Intratemporal complications of acute otitis media in infants and children. Otolaryngol Head Neck Surg. 1998;119(5):444–454.. 10.1016/S0194-5998(98)70100-7) [DOI] [PubMed] [Google Scholar]



 Content of this journal is licensed under a
Content of this journal is licensed under a