Abstract
Introduction. The world health organization (WHO) has declared the outbreak of novel coronavirus (2019-nCoV), which is now known as Coronavirus Disease 2019 (COVID-19). Whereas, its quick global spread has resulted in a worldwide pandemic. The present review article was intended to evaluate intrauterine vertical transmission of SARS-CoV-2 infection among confirmed cases of pregnant women. Methods. Web of Science, EMBASE, PubMed, African Journals OnLine, Scopus, PsycINFO, HINARI, Cochrane Library, Wiley Online Library, and Google scholar were used for search. Result. A total of 43 articles were included in to this systematic review. A total of 1,300 neonates born from pregnant women confirmed for COVI-19 were tested for SARS-CoV-2 infection by real-time reverse transcriptase–polymerase chain reaction (RT-PCR). From the 1,300 neonates tested for SARS-CoV-2 infection, 93 neonates were found positive for this infection by RT-PCR. From this systematic review finding, the vertical transmission rate of SARS-CoV-2 infection was 7.15%. This pandemic has stressed the entire public, particularly pregnant women and healthcare providers, while it challenged antenatal care and postnatal care by far. Thus, even being under lockdown in the middle of a global pandemic is stressful enough. Therefore, imagine the added burden of being pregnant, which could be a double burden for these women. Conclusion. There is no concrete evidence of vertical transmission of SARS-CoV-2. Therefore, due to the limited number of clinical evidences, obstetricians, pediatricians, and other healthcare providers should continuously update their knowledge and be conscious about the transmission of SARS-CoV-2 vertically during pregnancy.
Keywords: COVID-19, SARS-CoV-2, novel coronavirus, pregnancy, vertical transmission
Introductions
The COVID-19 pandemic was initially reported from Wuhan, China.1-4 The outbreak of infection with SARS-CoV-2 has developed in China and has spread across different countries since December 2019. 5 Emergency action have been taken by Chinese government to control this outbreak. 6 It has been brought to worldwide attention and stated as a pandemic by the WHO. 7 Since this pandemic is an extremely contagious disease, 8 it is spreading swiftly. 9 It is spreading globally,10,11 and remains a worldwide challenge. 12 This pandemic has a substantial mortality and morbidity rates,1,9,13 while it also causes an extensive economic crisis. 14
This burden has required drastic measures across all continents. 15 The COVID-19 has the potential to devastatingly influence young children’s development globally. 16 Due to this, mental health is a key community problem. 17 It has an enormous influence on the mental health of youth. 18 Moreover, fears are growing regarding the impact of the virus on the sexual and reproductive health of women and girls. This is due to that the virus has an devastating effect on them. 19 This pandemic has also put massive stress on healthcare workers, patients, and healthcare systems. The pregnancy care and fetal diagnosis should be continued. 20 It has an extreme effect on pregnant mothers and women in the early postpartum period emotional wellbeing. 21 There is the potential for pregnant women to be susceptible to mental problems during this pandemic. 22
The governments have applied lockdowns to limit the movements of people as methods to control the spread this pandemic. 23 Several countries have employed physical distancing, lockdowns, and stay-at-home actions to control it. 24 Its spread has formed several of the problems for the society because of the absence of a vaccine and effective treatment. 25 The extent of the COVID-19 crisis represents an extraordinary global challenge. 26 This has resulted in problems such as isolation, mental health problems and economic instability. 25 This pandemic has brought major deviations to social behavior. 27
There has been a hasty increase in the study in reply to the outbreak of this pandemic. Despite the researches are pertinent to control this pandemic, further quality study is required to offer reliable strategies to manage this health crisis in a short term and long term. 28 Therefore, this systematic review was intended to evaluate the potential intrauterine vertical transmission of a novel SARS-CoV-2 among confirmed cases of pregnant women.
Methods
Research Question
“Is the Intrauterine Vertical Transmission of SARS-CoV-2 Infection being possible among confirmed cases of pregnant women?”
“Is there a controversy on the possibility of the Intrauterine Vertical Transmission of SARS-CoV-2 Infection among confirmed cases of pregnant women?”
Study Period, Setting, and Type
In this systematic review, studies published up to December 15, 2021 were comprised. During this, several studies from different countries were considered. Moreover, any reports in any setting in any country were considered for this study. Regarding to the included study types, different study types were included in to this systematic review. For instance; cross-sectionals, letters to the editor, case report, short communications, case-control, case series, and cohort studies were included in to this study.
Study Subjects
The study subject for this systematic review was newborns delivered by COVID-19 infected women. Pregnant women infected by COVID-19 confirmed by RT-PCR laboratory were considered for this study.
Search Strategy
Web of Science, EMBASE, PubMed, African Journals OnLine, Scopus, PsycINFO, HINARI, Cochrane Library, Wiley Online Library, and Google scholar were used for search. All electronic sources of information were searched for the articles. “COVID-19,” “SARS-CoV-2,” “pregnancy,” “neonates,” and “Newborn” were the search terms used to find the related articles. To integrate these search terms; “AND” and “OR” Boolean operators were used.
Study Selection Criteria
The inclusion criteria for this study were; (1) articles which reported findings from newborn/s born by pregnant women infected by COVID-19 (confirmed by RT-PCR laboratory) and for which the laboratory test was done and reported with in the article; and (2) articles published in English language. Whereas, the articles which didn’t reported the test results for newborn/s and pregnant women, articles with poor quality and articles which were not fully accessible were excluded from this study.
Outcome Interest
The primary outcome of this study was the potential vertical transmission of a novel SARS-CoV-2 infection in pregnant women. Thus, the outcome variable was the positive/negative vertical transmission of a novel SARS-CoV-2infection in pregnant women as per the report of the included studies.
Data Extraction
Data were exported to Thomson Reuters EndNote version 8 after retrieval of the articles from the databases used. The articles were checked for the relevance of the title and abstracts to be included in to this study according to a pre-setted study selection criterion. A Microsoft Excel worksheet was used to extract the data from the selected articles. The prepared format has incorporated first author name, year of publication, sample size, study country, participants, study design, possible vertical transmission, and sample type and results.
Quality Assessment, Data Synthesis, and Reporting
The quality of each article was checked to include in to this study. The quality of articles which were case report and case series were assessed by the “Methodological quality and synthesis of case series and case reports” prepared by Murad et al 29 The Newcastle-Ottawa Scale (NOS) quality assessment criteria was used for other studies.30,31 For this study, a modified NOS was used and ≥5 from 10 scores was used to classify the article as a high quality score and to include the articles in this study. 32 This systematic review was conducted on the vertical transmission of a novel COVID-19 infection among pregnant women. For study screening, selection, and inclusion in to this systematic review, a PRISMA flowchart diagram,33,34 and PRISMA checklist 34 were used.
Ethics Approval and Consent to Participate
This study is a systematic review which was done by reviewing different articles published on different journals worldwide. There was no data collected from human. Therefore, Ethics approval and consent to participate were not applicable for this study.
Result
Search Results
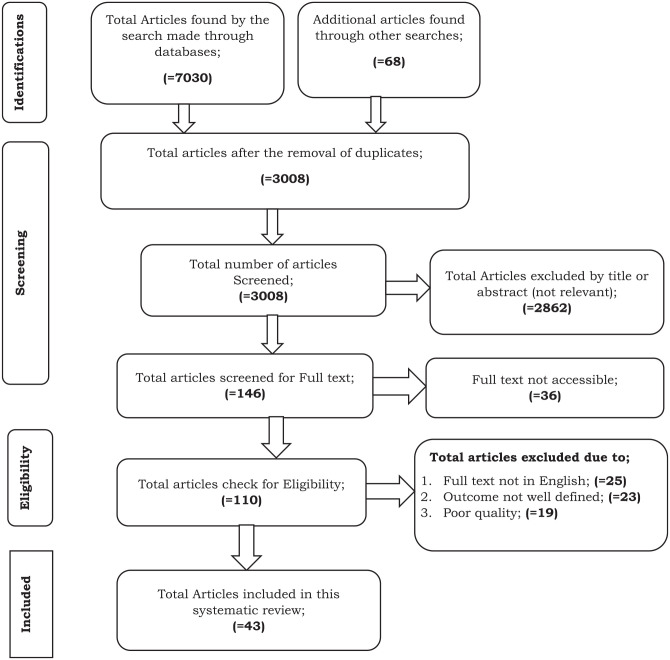
A total of 7098 articles were identified through a search made by all the above listed databases. From these, 4090 articles were excluded because of the duplications found. From the remaining 3008 articles, 2862 were excluded by title and abstract due to irrelevance. From the total 146 articles screened for full text, 36 articles were omitted because of full text were not accessible. From the remaining 110 articles screened for eligibility, 25 articles excluded due to full text not in English, 23 articles excluded due to the outcome variable not well defined, and 19 articles excluded because of poor quality. Finally, 43 articles were included in to this systematic review (Figure 1).
Figure 1.
PRISMA flowchart of a study selection for systematic review on the Vertical Transmission of a Novel COVID-19 Infection Among Pregnant Women. It was adapted from “Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. Journal of Clinical Epidemiology. 2009;62:1006–12.” 34
Study Characteristics
A total of 43 articles were included in to this systematic review. This systematic review has included various articles from different countries such as China, Spain, United states, Central America, India, Iran, Italy, Timisoara, Rome, French Guiana, United states, and Brazil (Table 1).
Table 1.
Characteristics of the Studies Included in the Systematic Review on the Vertical Transmission of a Novel SARS-CoV-2 Infection in Pregnant Women and Who Then Gave Birth.
| S. N | Author | Year | SS | Study design | Country | Mode of delivery | VT | Type of test and result | |
|---|---|---|---|---|---|---|---|---|---|
| (+ve) | (−ve) | ||||||||
| 1 | Dong et al 37 | 2020 | 1 | Case report | China | CS | 0 | 1 | • Sample used for RT-PCR tests: nasopharyngeal
swabs.
• RT-PCR result: negative. • Chest CT: normal. |
| 2 | Zeng et al 51 | 2020 | 6 | Case series | China | CS | 0 | 6 | • Sample used for RT-PCR tests: neonatal throat
swabs and blood.
• RT-PCR result: negative. |
| 3 | Fan et al 38 | 2020 | 2 | Case series | China | CS | 0 | 2 | • Sample used for Serial qRT-PCR assays: newborn’s
nasopharyngeal swab, placenta tissues, umbilical cord
blood, and amniotic fluid.
• qRT-PCR result: negative. |
| 4 | Liu et al 39 | 2020 | 19 | Case series | China | CS, VR | 0 | 19 | • Sample used for RT-PCR tests: throat swab, urine,
andfeces of neonate.
• RT-PCR result: negative. |
| 5 | Lu et al 40 | 2020 | 1 | Case report | China | CS | 0 | 1 | • Sample used for RT-PCR tests: throat swab
• RT-PCR result: negative. • Chest CT scanning: normal. |
| 6 | Pereira et al 41 | 2020 | 60 | Case series | Spain | CS, VR | 0 | 60 | • Sample used for qRT-PCR tests: nasopharyngeal swab
and placentas.
• qRT-PCR result: negative. |
| 7 | Pierce-Williams et al 42 | 2020 | 64 | cohort study | United States | CS | 0 | 64 | • Sample used for RT-PCR tests: nasopharyngeal
swab.
• RT-PCR result: negative. |
| 8 | Schwartz 43 | 2020 | 38 | Case series | China | CS, VR | 0 | 38 | • Sample used for RT-PCR tests: all neonatal
specimens tested.
• RT-PCR result: negative. |
| 9 | Chen et al 36 | 2020 | 9 | Case series | China | CS | 0 | 9 | • Sample used for RT-PCR tests: throat swab,
amniotic fluid, and cord blood.
• RT-PCR result: negative. |
| 10 | Khan et al 44 | 2020 | 3 | Case series | China | VR | 0 | 3 | • Sample used for qRT-PCR tests: Cord blood and
neonatal throat swab.
• qRT-PCR result: negative. |
| 11 | Li et al 45 | 2020 | 1 | Case report | China | CS | 0 | 1 | • Sample used for RT-PCR tests: oropharyngeal swab,
blood, feces, and urine.
• RT-PCR result: negative. |
| 12 | Peng et al 46 | 2020 | 1 | Case report | China | CS | 0 | 1 | • Sample used for RT-PCR tests: urine, anal swab,
throat swab, and serum.
• RT-PCR result: negative. |
| 13 | Xiong et al 47 | 2020 | 1 | Case report | China | VR | 0 | 1 | • Sample used for RT-PCR tests: rectal swab,
amniotic fluid, and throat swab.
• RT-PCR result: negative. |
| 14 | Yan et al 64 | 2020 | 100 | Case series | China | CS, VR | 14 | 86 | • Sample used for qRT-PCR tests: amniotic fluid,
cord blood, and pharyngeal swab.
• qRT-PCR result: 86 of the 100 had negative results. |
| 15 | Yang et al 48 | 2020 | 55 | Case control | China | CS, VR | 0 | 55 | • Sample used for RT-PCR tests: throat
swab.
• RT-PCR result: negative. |
| 16 | Zambrano et al 49 | 2020 | 1 | Case report | Central America | VR | 0 | 1 | • Sample used for RT-PCR tests: nasopharyngeal swab
and blood.
• RT-PCR result: negative. |
| 17 | Zhu et al 50 | 2020 | 9 | Case series | China | CS, VR | 0 | 9 | • Sample used for RT-PCR tests: Pharyngeal
swab.
• RT-PCR result: negative. |
| 18 | Chen et al 35 | 2020 | 4 | Case series | China | CS, VR | 0 | 4 | • Sample used for RT-PCR tests: Throat
swab.
• RT-PCR result: negative. |
| 19 | Bandyopadhyay et al 63 | 2020 | 1 | Case report | India | VR | 1 | 0 | • Sample used for RT-PCR tests: pharyngeal
swab.
• RT-PCR result: positive. |
| 20 | Parsa et al 65 | 2020 | 25 | Case series | Iran | CS | 9 | 16 | • Sample used for RT-PCR tests: nasopharyngeal
swab.
• RT-PCR result: 9 out of 25 were tested positive. |
| 21 | Rabiei et al 66 | 2021 | 3 | Case series | Iran | CS | 1 | 2 | • Sample used for RT-PCR tests: nasopharyngeal
swab.
• RT-PCR result: 1 out of 3 were tested positive. |
| 22 | Hu et al 67 | 2020 | 7 | Case series | China | CS, VR | 1 | 6 | • Sample used for RT-PCR tests: amniotic
fluid.
• RT-PCR result: 1 out of 7 were tested positive. • Chest radiograph: normal |
| 23 | Nie et al 68 | 2020 | 26 | Case series | China | CS, VR | 1 | 25 | • Sample used for RT-PCR tests: throat
swab.
• RT-PCR result: 1 out of 26 were tested positive. |
| 24 | Wang et al 52 | 2020 | 1 | Case report | China | CS | 0 | 1 | • Sample used for RT-PCR tests: pharyngeal and anal
swabs.
• RT-PCR result: negative. • Chest CT: a few small pieces of patchy shadow in the upper lobe of the right lung. |
| 25 | Yu et al 69 | 2020 | 3 | Cross sectional | China | CS | 1 | 2 | • Sample used for RT-PCR tests: Throat
swabs.
• RT-PCR result: 1 out of 3 were tested positive. |
| 26 | Zamaniyan et al 70 | 2020 | 1 | Case report | Iran | CS | 1 | 0 | • Sample used for RT-PCR tests: nasal and throat
swabs.
• RT-PCR result: positive. |
| 27 | Zeng et al 71 | 2020 | 33 | Cohort study | China | CS, VR | 3 | 30 | • Sample used for RT-PCR tests: throat and anal
swab.
• RT-PCR result: 3 out of 33 were positive. |
| 28 | Li et al 53 | 2020 | 34 | Case control | China | CS, VR | 0 | 34 | • Sample used for RT-PCR tests: throat
swab.
• RT-PCR result: negative. |
| 29 | Zhang et al 54 | 2020 | 10 | Case control | China | CS | 0 | 10 | • Sample used for RT-PCR tests: throat
swab.
• RT-PCR result: negative. |
| 30 | Liao et al 55 | 2020 | 7 | Case control | China | VR | 0 | 7 | • Sample used for RT-PCR tests: throat
swab.
• RT-PCR result: negative. |
| 31 | Yin et al 56 | 2020 | 17 | Cohort | China | CS, VR | 0 | 17 | • Sample used for RT-PCR tests: throat, amniotic
fluid, placenta, and anal swab.
• RT-PCR result: negative. |
| 32 | Yang et al 57 | 2020 | 7 | Cross sectional | China | CS | 0 | 7 | • Sample used for qRT-PCR tests: amniotic fluid,
pharyngeal swab, and umbilical blood.
• qRT-PCR result: negative. |
| 33 | Qiancheng et al 58 | 2020 | 23 | Cross sectional | China | CS, VR | 0 | 23 | • Sample used for RT-PCR tests: throat
swab.
• RT-PCR result: negative. |
| 34 | Ferrazzi et al 62 | 2020 | 42 | Cross sectional | Italy | CS, VR | 2 | 40 | • Sample used for RT-PCR tests: throat
swab.
• RT-PCR result: 2 out of 42 were positive. |
| 35 | Citu et al 59 | 2021 | 74 | Cohort | Timisoara | CS | 0 | 74 | • Sample used for RT-PCR tests: amniotic
fluid.
• RT-PCR result: negative. |
| 36 | Conti et al 72 | 2021 | 37 | Cross sectional | Rome | CS | 1 | 36 | • Sample used for RT-PCR tests: nasopharyngeal
swab.
• RT-PCR result: 1 out of 37 was positive. |
| 37 | Hcini et al 73 | 2021 | 29 | Cohort | French Guiana | CS, VR | 4 | 25 | • Sample used for RT-PCR tests: nasopharyngeal
swab.
• RT-PCR result: 4 out of 29 were positive. |
| 38 | Jacob et al 74 | 2021 | 342 | Cohort | India | CS, VR | 49 | 293 | • Sample used for RT-PCR tests: nasopharyngeal
swab.
• RT-PCR result: 49 were positive. |
| 39 | Kulkarni et al 75 | 2021 | 1 | Case report | India | VR | 1 | 0 | • Sample used for RT-PCR tests: nasopharyngeal
swab.
• RT-PCR result: positive. |
| 40 | Kumari et al 60 | 2021 | 41 | Cross sectional | India | CS, VR | 0 | 41 | • Sample used for RT-PCR tests: nasopharyngeal
swab.
• RT-PCR result: negative. |
| 41 | Lamba et al 76 | 2021 | 70 | Cohort | United states | CS, VR | 2 | 68 | • Sample used for RT-PCR tests: nasopharyngeal
swab.
• RT-PCR result: 2 were positive. |
| 42 | Maeda et al 77 | 2021 | 54 | Cohort | Brazil | CS, VR | 2 | 52 | • Sample used for RT-PCR tests: oropharyngeal
swab.
• RT-PCR result: 2 were positive. |
| 43 | Peter et al 61 | 2021 | 27 | Cohort | United states | CS, VR | 0 | 27 | • Sample used for RT-PCR tests: throat
swab.
• RT-PCR result: negative. |
Sample size is explained in number of newborn/s included in the articles.
Abbreviations: SS, sample size; CS, cesarean section; VR, vaginal route; SARS-CoV-2, severe acute respiratory syndrome coronavirus; RT-PCR, real-time reverse transcriptase–polymerase chain reaction; SARS, severe acute respiratory syndrome; CT, computed tomography; VT, Vertical transmission, qRT-PCR, quantitative real-time polymerase chain reaction;
Intrauterine Vertical Transmission of SARS-CoV-2 Infection
A total of 1300 neonates born from pregnant women confirmed for COVI-19 were tested for SARS-CoV-2 infection by RT-PCR. From the 1300 neonates tested for SARS-CoV-2 infection, 93 neonates were found positive for this infection by RT-PCR. From this systematic review findings, the vertical transmission rate of SARS-CoV-2 infection was 7.15% (Table 1).
Controversy on intrauterine vertical transmission of SARS-CoV-2 infection
Below is a brief summary of studies conducted among COVID-19 positive pregnant mothers who gave birth. According to these studies, there are controversies upon the outcome of neonates born from confirmed cases of COVID-19 women. Discrepancies were seen between the currently existing literatures. Some of the studies are reported that there were no positive infants born from COVID-19 positive pregnant women.35-61 This because of that the findings from some studies showed that there were SARS-CoV-2 positive infants born to SARS-CoV-2 positive women62-77 (Table 1).
Discussion
A total of 43 articles were included in to this study. This systematic review has included various articles from different countries such as China, Spain, United States, Central America, India, Iran, Italy, Timisoara, Rome, French Guiana, United states, and Brazil. A total of 1300 neonates born from confirmed COVI-19 pregnant women who were tested for SARS-CoV-2 infection by RT-PCR.
From the 1300 neonates tested for SARS-CoV-2 infection, 93 neonates were found positive for this infection by RT-PCR. From this systematic review finding, the vertical transmission rate of SARS-CoV-2 infection was 7.15%. According to the studies, there are controversies upon the outcome of neonates born from confirmed cases of COVID-19. Discrepancies were seen between the currently existing literatures. Some of the studies are reported that there were no positive infants born from COVID-19 positive pregnant women.35-61 This because of that the findings from some studies showed that there were SARS-CoV-2 positive infants born to SARS-CoV-2 positive women.62-77
The vertical transmission of several microorganisms to the fetus from an infected mother can lead to shocking consequences. This can be happened during antenatal or per-partum, but perinatal or postnatal transmission can have severe results. 78 The evidence revealed that COVD-19 causes some histopathological changes. Even though the vertical transmission of the virus is clear not yet, however, the available data indicated that there was an indirect effect of the virus on the fetus. 79
The earliest data have reported as there is no concrete evidence for vertical transmission of SARS-CoV-2 virus because of intrauterine infections.52,80-88 It will probably be a rare that fetuses will be uninfected at the time of their birth, if intrauterine transmission of SARS-CoV-2 occur. 83 There is no information found for vertical transmission of this virus from confirmed pregnant mothers to fetuses. However, the women could be at augmented risk for more severe respiratory complications. 84 The available data revealed that the vertical transmission of this virus from infected mothers in a third trimester maybe doesn’t happen. 85 The vertically transmission, short-term, and long-term harm of SARS-CoV-2 to offspring is still uncertain. 52
Currently, there is no strong evidence of intrauterine transmission of SARS-CoV-2. 86 The earliest data showed that COVID-19 may not lead to the augmented risk in the pregnant population. Besides, they were not confirmed the vertical transmission. 87 The earliest study showed that the clinical features of infected pregnant women with this virus in late pregnancy were found to be similar to those of nonpregnant patients. 80 However, since the impact of this virus on pregnant women is still limited, they should be given a consideration including their newborns, about COVID-19 management and prevention means. 89 The pregnant mother must be focused as high-risk for COVID-19 and need to lessen the contact. 90 They may be more prone to this virus which is because of the immunological and physiological changes. So that, they must apply routine preventive actions. 91
COVID-19 in pregnancy were found to be related to maternal morbidity and preterm birth. The associated risk factors were age of women beyond 35 years, being overweight, and obesity. 92 Besides, miscarriage, fetal distress, respiratory distress, and preterm delivery can be caused by COVID-19. 81 Contrary, most of the experts have accepted approach the approach of isolating the infants from women suspected or confirmed with COVID-19 as a means of decreasing the risk of transmission to baby. 93 Those infected pregnant women should obtain better consideration. This pandemic virus could asymptotically arise at gestation time. However, they get diagnosed after delivery. 94
The study done among asymptomatic and symptomatic pregnant women in New York showed that the severity of this disease in pregnant women was mild, severe, and critical; appears similar to that in nonpregnant in 86%, 9.3%, and 4.7% of them respectively. 95 According to the research conducted on 9 pregnant women with confirmed cases; 7 out of 9 were died, 1 out of 9 was remains critically ill, and 1 out of 9 was recovered after long hospitalization at the time of reporting. 96 In pregnancy, the management of this pandemic comprises such as; infection control procedures, oxygen therapy, early isolation, avoidance of fluid overload, consideration of empiric antibiotics, laboratory testing, fetal monitoring, uterine contraction monitoring, separated delivery planning, early mechanical ventilation, and multidisciplinary consultation. 97
Recommendations
If the pregnant mothers are confirmed for infection of COVID-19, the choice of delivery judgment would be better if individualized depending on factors like maternal, fetal, gestational age, and delivery circumstances. Vaginal delivery via induction of labor, with eventual instrumental delivery to prevent maternal fatigue, should be selected to prevent needless surgical consequences. 98 Besides, a study suggested that COVID-19 management for positive pregnant mothers must be adopted and performed by a multi-disciplinary team method.98-100
A multidisciplinary team which includes obstetricians, intensivists, maternal–fetal medicine subspecialists, virologists, obstetric anesthetists, neonatologists, internal medicine, midwives, and infectious disease specialists are better to be undertaken during managing these patients. 100 Furthermore, recognizing the extent to which COVID-19 affects women and men differently will be the essential to understand the bigger influence of this disease both during the crisis and during individual and societal recovery. 101
Overall, Since the SARS-CoV-2 vertical transmission has no evidence till now, it is important to keep all the specimens of SARS-CoV-2 infected and suspected pregnant women and their newborns for in-depth study and continuous follow-up observation of future generations. 52 The study described that if the exposure arose at a delivery time, the virus may need a longer incubation period prior to test swabs show positive outcomes. As a result, nasopharyngeal testing instantly after delivery may not be the ideal method to assess vertical transmission. Particularly, the existence of viral RNA in placental and membranes samples by RT-PCR during the delivery shows the requirement for more research for likelihood of vertical transmission. 102
Conclusions
The quick global spread of COVID-19 has resulted in a worldwide pandemic. This pandemic remains a global challenge. Currently, it is a major and critical global health emergency. From this systematic review findings, out of 1300 neonates tested for SARS-CoV-2 infection, 93 neonates were found positive for this infection by RT-PCR. The rate of vertical transmission of SARS-CoV-2 infection was 7.15%. The present review found that the possibility of a vertical transmission of COVID-19 is recently a highly controversial issues across the worldwide. This is because there is a discrepancy of literatures were found. Some studies stated as the were no vertical transmission of SARS-CoV-2 in neonates born of COVID-19 confirmed women, whereas the other studies reported that as there was a vertical transmission of this virus.
To counteract and control this aggressive pandemic virus, the global healthcare system should update and modify their tools and practices accordingly with time manner. There is an increasing requirement for information concerning to the mother and neonate outcomes during COVID-19 pandemic. This study has addressed the significant issues for healthcare providers giving care for COVID-19 confirmed cases of pregnant, for stakeholders, for health policy makers and implementers, and for the pregnant populations as the whole.
The available data regarding to the pregnant mothers with COVID-19 provides a favorable outcome. However, the risks for maternal, and fetal should not be underrated. The available information is limited to the mothers who developed the COVID-19 in late gestation and mothers who delivered shortly after the diagnosis of COVID-19. But, the baby outcome from a long-standing of COVID-19 disease diagnosed mother, which occurred in early gestation are unknown. Because of the inadequate figure of clinical evidences, pediatricians, obstetricians, and other healthcare providers should continually update their knowledge and be conscious regarding the transmissions of SARS-CoV-2 vertically during pregnancy. Furthermore, it is expected that the future researches would offer more evidence on maternal and baby circumstances for obstetrical interventions. Lastly, the present review recommends that a further high-quality study is needed to conclude this critical issue of confusion concerning to the vertical transmission surely.
Footnotes
Author’s Contributions: The author made a substantial contribution to this study on the entire aspects.
Declaration of Conflicting Interests: The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding: The author(s) received no financial support for the research, authorship, and/or publication of this article.
ORCID iD: Addisu Dabi Wake  https://orcid.org/0000-0003-1219-0836
https://orcid.org/0000-0003-1219-0836
References
- 1. Dariya B, Nagaraju GP. Understanding novel COVID-19: its impact on organ failure and risk assessment for diabetic and cancer patients. Cytokine Growth Factor Rev. 2020;53:43-52. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Lake MA. What we know so far: COVID-19 current clinical knowledge and research. Clin Med. 2020;20:124-127. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Sohrabi C, Alsafi Z, O’Neill N, et al. World Health Organization declares global emergency: a review of the 2019 novel coronavirus (COVID-19). Int J Surg. 2020;77:217-226. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Dey SK, Rahman MM, Siddiqi UR, Howlader A. Analyzing the epidemiological outbreak of COVID-19: a visual exploratory data analysis approach. J Med Virol. 2020;92:632-638. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Wen R, Sun Y, Xing Q-S. A patient with SARS-CoV-2 infection during pregnancy in Qingdao, China. J Microbiol Immunol Infect. 2020;53:499-500. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. Han Y, Yang H. The transmission and diagnosis of 2019 novel coronavirus infection disease (COVID-19): a Chinese perspective. J Med Virol. 2020;92(6):639-644. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Jin Y, Yang H, Ji W, et al. Virology, Epidemiology, Pathogenesis, and control of COVID-19. Viruses. 2020;12:372. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8. Wang L, Wang Y, Ye D, Liu Q. Review of the 2019 novel coronavirus (SARS-CoV-2) based on current evidence. Int J Antimicrob Agents. 2020;55:105948. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Cao W, Li T. COVID-19: towards understanding of pathogenesis. Cell Res. 2020;30:367-369. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10. Sun P, Lu X, Xu C, Sun W, Pan B. Understanding of COVID-19 based on current evidence. J Med Virol. 2020;92:548-551. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Shanafelt T, Ripp J, Trockel M. Understanding and addressing sources of anxiety among health care professionals during the COVID-19 Pandemic. JAMA. 2020;323(21):2133-2134. [DOI] [PubMed] [Google Scholar]
- 12. Lotfi M, Hamblin MR, Rezaei N. COVID-19: transmission, prevention, and potential therapeutic opportunities. Clin Chim Acta. 2020;508:254-266. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13. Lu Q, Shi Y. Coronavirus disease (COVID-19) and neonate: what neonatologist need to know. J Med Virol. 2020;92:564-567. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14. Ataguba JE. COVID-19 pandemic, a war to be won: understanding its economic implications for Africa. Appl Health Econ Health Policy. 2020;18:325-328. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. Dashraath P, Wong JLJ, Lim MXK, et al. Coronavirus disease 2019 (COVID-19) pandemic and pregnancy. Am J Obstet Gynecol. 2020;222:521-531. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16. Yoshikawa H, Wuermli AJ, Britto PR, et al. Effects of the global coronavirus disease-2019 pandemic on early childhood development: short- and long-term risks and mitigating program and policy actions. J Pediatr. 2020;223:188-193. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Kajdy A, Feduniw S, Ajdacka U, et al. Risk factors for anxiety and depression among pregnant women during the COVID-19 pandemic: a web-based cross-sectional survey. Medicine. 2020;99:e21279. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18. Liang L, Ren H, Cao R, et al. The effect of COVID-19 on Youth Mental Health. Psychiatr Q. 2020;91:841-852. doi: 10.1007/s11126-020-09744-3 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19. Cousins S. COVID-19 has “devastating” effect on women and girls. Lancet. 2020;396:301-302. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Deprest J, Choolani M, Chervenak F, et al. Fetal diagnosis and therapy during the COVID-19 pandemic: guidance on behalf of the International Fetal Medicine and Surgery Society. Fetal Diagn Ther. 2020;47:689-698. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Ceulemans M, Hompes T, Foulon V. Mental health status of pregnant and breastfeeding women during the COVID-19 pandemic: a call for action. Int J Gynecol Obstet. 2020;151:146-147. [DOI] [PubMed] [Google Scholar]
- 22. Thapa SB, Mainali A, Schwank SE, Acharya G. Maternal mental health in the time of the COVID-19 pandemic. Acta Obstet Gynecol Scand. 2020;99:817-818. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23. Babvey P, Capela F, Cappa C, Lipizzi C, Petrowski N, Ramirez-Marquez J. Using social media data for assessing children’s exposure to violence during the COVID-19 pandemic. Child Abuse Negl. 2021;116:104747. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24. World Health Organization. (2020). Addressing violence against children, women and older people during the COVID-19 pandemic: key actions, 17 June 2020. World Health Organization. https://apps.who.int/iris/handle/10665/332458 [Google Scholar]
- 25. Mittal S, Singh T. Gender-based violence during COVID-19 pandemic: a mini-review. Front Glob Womens Health. 2020;1:4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26. Singh JA, Bandewar SV, Bukusi EA. The impact of the COVID-19 pandemic response on other health research. Bull World Health Organ. 2020;98:625-631. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. Arora T, Grey I. Health behaviour changes during COVID-19 and the potential consequences: a mini-review. J Health Psychol. 2020;25:1155-1163. [DOI] [PubMed] [Google Scholar]
- 28. Adhikari SP, Meng S, Wu YJ, et al. Epidemiology, causes, clinical manifestation and diagnosis, prevention and control of coronavirus disease (COVID-19) during the early outbreak period: a scoping review. Infect Dis Poverty. 2020;9:29. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29. Murad MH, Sultan S, Haffar S, Bazerbachi F. Methodological quality and synthesis of case series and case reports. Evid Based Med. 2018;23:60-63. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30. Modesti PA, Reboldi G, Cappuccio FP, et al. Panethnic differences in blood pressure in Europe: a systematic review and meta-analysis. PLoS One. 2016;11:e0147601. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31. Wells GA, Shea B, O’Connell D, Peterson J, Welch V, Losos M, et al. The Newcastle-Ottawa Scale (NOS) for Assessing the Quality of Nonrandomized Studies in Meta-Analyses. Ottawa Hospital Research Institute, Ottawa, Canada. Accessed May 21, 2021. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. [Google Scholar]
- 32. Yazew KG, Walle TA, Azagew AW. Prevalence of anti-diabetic medication adherence and determinant factors in Ethiopia: a systemic review and meta-analysis, 2019. Int J Afr Nurs Sci. 2019;11:100167. [Google Scholar]
- 33. Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ. 2009;339:b2700-b2700. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34. Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred Reporting Items for systematic reviews and Meta-Analyses: the PRISMA Statement. J Clin Epidemiol. 2009;62:1006-1012. [DOI] [PubMed] [Google Scholar]
- 35. Chen Y, Peng H, Wang L, et al. Infants born to mothers with a new Coronavirus (COVID-19). Front Pediatr. 2020;8:104. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36. Chen H, Guo J, Wang C, et al. Clinical characteristics and intrauterine vertical transmission potential of COVID-19 infection in nine pregnant women: a retrospective review of medical records. Lancet. 2020;395:809-815. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37. Dong L, Tian J, He S, et al. Possible vertical transmission of SARS-CoV-2 from an infected mother to her newborn. JAMA. 2020;323:1846-1848. doi: 10.1001/jama.2020.4621 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38. Fan C, Lei D, Fang C, et al. Perinatal transmission of 2019 Coronavirus disease–Associated Severe Acute Respiratory Syndrome Coronavirus 2: should We Worry? Clin Infect Dis. 2021;72:862-864. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39. Liu W, Wang J, Li W, Zhou Z, Liu S, Rong Z. Clinical characteristics of 19 neonates born to mothers with COVID-19. Front Med. 2020;14:193-198. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40. Lu D, Sang L, Du S, Li T, Chang Y, Yang XA. Asymptomatic COVID-19 infection in late pregnancy indicated no vertical transmission. J Med Virol. 2020;92:1660-1664. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41. Pereira A, Cruz-Melguizo S, Adrien M, Fuentes L, Marin E, Perez-Medina T. Clinical course of coronavirus disease-2019 in pregnancy. Acta Obstet Gynecol Scand. 2020;99:839-847. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42. Pierce-Williams RA, Burd J, Felder L, et al. Clinical course of severe and critical coronavirus disease 2019 in hospitalized pregnancies: a United States cohort study. Am J Obst Gynecol. 2020;2:100134. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43. Schwartz DA. An analysis of 38 pregnant women with COVID-19, their newborn infants, and maternal-fetal transmission of SARS-CoV-2: maternal Coronavirus infections and Pregnancy Outcomes. Arch Pathol Lab Med. 2020;144:799-805. [DOI] [PubMed] [Google Scholar]
- 44. Khan S, Peng L, Siddique R, et al. Impact of COVID-19 infection on pregnancy outcomes and the risk of maternal-to-neonatal intrapartum transmission of COVID-19 during natural birth. Infect Control Hosp Epidemiol. 2020;41:748-750. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45. Li Y, Zhao R, Zheng S, et al. Lack of vertical transmission of severe Acute Respiratory Syndrome Coronavirus 2, China. Emerg Infect Dis. 2020;26(6):1335-1336. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46. Peng Z, Wang J, Mo Y, et al. Unlikely SARS-CoV-2 vertical transmission from mother to child: a case report. J Infect Public Health. 2020;13:818-820. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47. Xiong X, Wei H, Zhang Z, et al. Vaginal delivery report of a healthy neonate born to a convalescent mother with COVID-19. J Med Virol. 2020;92:1657-1659. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48. Yang H, Sun G, Tang F, et al. Clinical features and outcomes of pregnant women suspected of coronavirus disease 2019. Infect J. 2020;81:e40-e44. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49. Zambrano LI, Fuentes-Barahona IC, Bejarano-Torres DA, et al. A pregnant woman with COVID-19 in Central America. Travel Med Infect Dis. 2020;36:101639. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50. Zhu H, Wang L, Fang C, et al. Clinical analysis of 10 neonates born to mothers with 2019-nCoV pneumonia. Transl Pediatr. 2020;9:51-60. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51. Zeng H, Xu C, Fan J, et al. Antibodies in infants born to mothers with COVID-19 pneumonia. JAMA. 2020;323:1848-1849. doi: 10.1001/jama.2020.4861 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52. Wang S, Guo L, Chen L, et al. A case report of Neonatal 2019 Coronavirus disease in China. Clin Infect Dis. 2020;71:853-857. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53. Li N, Han L, Peng M, et al. Maternal and neonatal outcomes of pregnant women with Coronavirus Disease 2019 (COVID-19) pneumonia: a case-control study. Clin Infect Dis. 2020;71:2035-2041. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54. Zhang L, Jiang Y, Wei M, et al. [Analysis of the pregnancy outcomes in pregnant women with COVID-19 in Hubei Province]. Zhonghua Fu Chan Ke Za Zhi. 2020;55:166-171. [DOI] [PubMed] [Google Scholar]
- 55. Liao J, He X, Gong Q, Yang L, Zhou C, Li J. Analysis of vaginal delivery outcomes among pregnant women in Wuhan, China during the COVID-19 pandemic. Int J Gynecol Obstet. 2020;150:53-57. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56. Yin M-Z, Zhang L, Deng G-T, Han C-F, Shen M-X, Sun H-Y, et al. Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) Infection During Pregnancy In China: A Retrospective Cohort Study. 2020. medRxiv;Preprint. [Google Scholar]
- 57. Yang P, Wang X, Liu P, et al. Clinical characteristics and risk assessment of newborns born to mothers with COVID-19. J Clin Virol. 2020;127:104356. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58. Qiancheng X, Jian S, Lingling P, et al. Coronavirus disease 2019 in pregnancy. Internet J Infect Dis. 2020;95:376-383. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59. Citu C, Neamtu R, Sorop V-B, et al. Assessing SARS-CoV-2 vertical transmission and neonatal complications. J Clin Med. 2021;10:5253. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60. Kumari K, Yadav R, Mittra S, et al. Pregnancy outcomes and vertical transmission capability of SARS-CoV-2 infection among asymptomatic females: a cross-sectional study in a tertiary care rural hospital. J Fam Med Prim Care. 2021;10:3247-3251. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61. Peter B, Ree N, Ferrer K, et al. Risk factors associated with COVID-19 symptoms and potential vertical transmission during pregnancy: a retrospective cohort study. Cureus. 2022; 14(3): e22900. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62. Ferrazzi E, Frigerio L, Savasi V, et al. Vaginal delivery in SARS-CoV-2-infected pregnant women in Northern Italy: a retrospective analysis. BJOG: Int J Obstet Gy. 2020;127:1116-1121. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63. Bandyopadhyay T, Sharma A, Kumari P, Maria A, Choudhary R. Possible early vertical transmission of COVID-19 from an infected pregnant female to her neonate: a Case Report. J Trop Pediatr. 2021;67:1-4. doi: 10.1093/tropej/fmaa094 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64. Yan J, Guo J, Fan C, et al. Coronavirus disease 2019 in pregnant women: a report based on 116 cases. Am J Obstet Gynecol. 2020;223:111.e1-111.e14. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65. Parsa Y, Shokri N, Jahedbozorgan T, Naeiji Z, Zadehmodares S, Moridi A. Possible vertical transmission of COVID-19 to the newborn; a case report. Arch Acad Emerg Med. 2020;9(1):1-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66. Rabiei M, Soori T, Abiri A, Farsi Z, Shizarpour A, Pirjani R. Maternal and fetal effects of COVID-19 virus on a complicated triplet pregnancy: a case report. J Med Case Rep. 2021;15:87. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67. Hu X, Gao J, Luo X, et al. Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) vertical transmission in neonates born to mothers with Coronavirus Disease 2019 (COVID-19) pneumonia. Obstet Gynecol. 2020;136:65-67. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68. Nie R, Wang S, Yang Q, Fan C, Liu Y, He W, et al. Clinical Features and the Maternal and Neonatal Outcomes of Pregnant Women With Coronavirus Disease 2019. 2020. medRxiv; Preprint. [Google Scholar]
- 69. Yu N, Li W, Kang Q, et al. Clinical features and obstetric and neonatal outcomes of pregnant patients with COVID-19 in Wuhan, China: a retrospective, single-centre, descriptive study. Lancet Infect Dis. 2020;20:559-564. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70. Zamaniyan M, Ebadi A, Aghajanpoor S, Rahmani Z, Haghshenas M, Azizi S. Preterm delivery, maternal death, and vertical transmission in a pregnant woman with COVID-19 infection. Prenat Diagn. 2020;40:1759-1761. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71. Zeng L, Xia S, Yuan W, et al. Neonatal early-onset infection with SARS-CoV-2 in 33 neonates born to mothers with COVID-19 in Wuhan, China. JAMA Pediatr. 2020;174(7):722-725. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72. Conti MG, Natale F, Stolfi I, et al. Consequences of early separation of maternal-newborn dyad in neonates born to SARS-CoV-2 positive mothers: an Observational Study. Int J Environ Res Public Health. 2021;18:5899. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73. Hcini N, Maamri F, Picone O, et al. Maternal, fetal and neonatal outcomes of large series of SARS-CoV-2 positive pregnancies in peripartum period: a single-center prospective comparative study. Eur J Obstet Gynecol Reprod Biol. 2021;257:11-18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74. Jacob AS, Mtp M, Gopinath R, Divakaran B, Harris T. Clinical profiles of neonates born to mothers with COVID-19. Paediatr Indones. 2021;61:277-282. [Google Scholar]
- 75. Kulkarni R, Rajput U, Dawre R, et al. Early-onset symptomatic neonatal COVID-19 infection with high probability of vertical transmission. Infection. 2021;49:339-343. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76. Lamba V, Lien J, Desai J, Talati AJ. Management and short-term outcomes of neonates born to mothers with active perinatal SARS-CoV-2 infection. BMC Pediatr. 2021;21:400. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77. Maeda MFY, Brizot ML, Gibelli MABC, et al. Vertical transmission of SARS-CoV2 during pregnancy: a high-risk cohort. Prenat Diagn. 2021;41:998-1008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78. Lamouroux A, Attie-Bitach T, Martinovic J, Leruez-Ville M, Ville Y. Evidence for and against vertical transmission for severe acute respiratory syndrome coronavirus 2. Am J Obstet Gynecol. 2020;223:91.e1-91.e4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79. Seymen CM. Being pregnant in the COVID-19 pandemic: effects on the placenta in all aspects. J Med Virol. 2021;93:2769-2773. doi: 10.1002/jmv.26857 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80. Chen S, Huang B, Luo DJ, et al. [Pregnancy with new coronavirus infection: clinical characteristics and placental pathological analysis of three cases]. Zhonghua Bing Li Xue Za Zhi. 2020;49(5):418-423. doi: 10.3760/cma.j.cn112151-20200225-00138 [DOI] [PubMed] [Google Scholar]
- 81. Panahi L, Amiri M, Pouy S. Risks of novel Coronavirus disease (COVID-19) in pregnancy; a narrative review. Arch Acad Emerg Med. 2020;8:e34. [PMC free article] [PubMed] [Google Scholar]
- 82. Yang H, Wang C, Poon LC. Novel coronavirus infection and pregnancy. Ultrasound Obstet Gynecol. 2020;55:435-437. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83. Schwartz DA, Dhaliwal A. Infections in pregnancy with COVID-19 and other respiratory RNA virus diseases are rarely, if ever, transmitted to the fetus: experiences with coronaviruses, Parainfluenza, Metapneumovirus respiratory syncytial virus, and Influenza. Arch Pathol Lab Med. 2020;144(8):920-928. [DOI] [PubMed] [Google Scholar]
- 84. Karimi-Zarchi M, Neamatzadeh H, Dastgheib SA, et al. Vertical transmission of Coronavirus disease 19 (COVID-19) from infected pregnant mothers to neonates: a Review. Fetal Pediatr Pathol. 2020;39:246-250. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85. Mimouni F, Lakshminrusimha S, Pearlman SA, Raju T, Gallagher PG, Mendlovic J. Perinatal aspects on the covid-19 pandemic: a practical resource for perinatal-neonatal specialists. J Perinatol. 2020;40:820-826. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 86. Wang C, Zhou YH, Yang HX, Poon LC. Intrauterine vertical transmission of SARS-CoV-2: what we know so far. Ultrasound Obstet Gynecol. 2020;55:724-725. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87. Dotters-Katz SK, Hughes BL. Considerations for obstetric care during the COVID-19 Pandemic. Am J Perinatol. 2020;37:773-779. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 88. Boyadzhieva VV, Stoilov NR, Stoilov RM. Coronavirus disease 2019 (COVID-19) during pregnancy in patients with rheumatic diseases. Rheumatol Int. 2020;40:1753-1762. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 89. Rodrigues C, Baia I, Domingues R, Barros H. Pregnancy and breastfeeding during covid-19 pandemic: a systematic review of published pregnancy cases. Front Public Health. 2020;8:558144. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90. Alzamora MC, Paredes T, Caceres D, Webb CM, Valdez LM, La Rosa M. Severe COVID-19 during pregnancy and possible vertical transmission. Am J Perinatol. 2020;37:861-865. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 91. Mask M, Irani M, Pakfetrat A. Novel coronavirus disease 2019 and perinatal outcomes. J Educ Health Promot. 2020;9:78. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 92. Sentilhes L, De Marcillac F, Jouffrieau C, et al. Coronavirus disease 2019 in pregnancy was associated with maternal morbidity and preterm birth. Am J Obstet Gynecol. 2020;223:914.e1-914.e15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 93. Stuebe A. Should infants be separated from mothers with COVID-19? First, Do No harm. Breastfeed Med. 2020;15:351-352. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 94. Chen S, Liao E, Cao D, Gao Y, Sun G, Shao Y. Clinical analysis of pregnant women with 2019 novel coronavirus pneumonia. J Med Virol. 2020;92:1556-1561. doi: 10.1002/jmv.25789 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 95. Breslin N, Baptiste C, Gyamfi-Bannerman C, et al. Coronavirus disease 2019 infection among asymptomatic and symptomatic pregnant women: two weeks of confirmed presentations to an affiliated pair of New York City hospitals. Am Journal of Obstetrics & Gynecology MFM. 2020;2:100118. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 96. Hantoushzadeh S, Shamshirsaz AA, Aleyasin A, et al. Maternal death due to COVID-19. Am J Obstet Gynecol. 2020;223:109.e1-109.e16. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 97. Rasmussen SA, Smulian JC, Lednicky JA, Wen TS, Jamieson DJ. Coronavirus Disease 2019 (COVID-19) and pregnancy: what obstetricians need to know. Am J Obstet Gynecol. 2020;222:415-426. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 98. Favre G, Pomar L, Qi X, Nielsen-Saines K, Musso D, Baud D. Guidelines for pregnant women with suspected SARS-CoV-2 infection. Lancet Infect Dis. 2020;20:652-653. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 99. Liang H, Acharya G. Novel corona virus disease (COVID-19) in pregnancy: what clinical recommendations to follow? Acta Obstet Gynecol Scand. 2020;99:439-442. [DOI] [PubMed] [Google Scholar]
- 100. Poon LC, Yang H, Kapur A, et al. Global interim guidance on coronavirus disease 2019 (COVID-19) during pregnancy and puerperium from FIGO and allied partners: information for Health Care Professionals. Obstet Anesth Dig. 2021;41:39-40. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 101. McLaren HJ, Wong KR, Nguyen KN, Mahamadachchi KND. Covid-19 and women’s triple burden: vignettes from Sri Lanka, Malaysia, Vietnam and Australia. Soc Sci. 2020;9:87. [Google Scholar]
- 102. Penfield CA, Brubaker SG, Limaye MA, et al. Detection of severe acute respiratory syndrome coronavirus 2 in placental and fetal membrane samples. Am J Obst Gynecol. 2020;2:100133. [DOI] [PMC free article] [PubMed] [Google Scholar]