Influenza virus is associated with considerable morbidity and mortality worldwide. These epidemics occur annually and can be prevented through prophylactic vaccination and mitigated with interventions such as social control measures and specific antiviral use.1, 2 Since the recognition of the widespread community transmission of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), surveillance indicators for influenza have reduced worldwide.3 The measures implemented for coronavirus disease 2019 (COVID-19), including physical distancing, wearing masks, quarantining, and restricting virus spread/circulation, are also essential to reduce infections caused by influenza and respiratory syncytial viruses; thus, the detection levels of these respiratory viruses became historically low and reduced numbers of influenza viruses were available for WHO characterization than in previous years.4, 5
Although >65% of the Brazilian population had been fully vaccinated against covid-19 with two doses by the end of 2021, Brazil started the year 2022 with an increase in the number of cases and hospitalizations due to Omicron variant of SARS-CoV-2 and influenza A H3N2 Darwin-like virus also spread of the summer. This study sought to report the outbreak of H3N2 in this context.
This is retrospective, observational study evaluated patients with flu-like symptoms who were admitted to the emergency department of Hospital São Paulo, São Paulo, Brazil, between November 2021 and January 2022. Nasal and nasopharyngeal swabs were collected from the patients and placed in 2 mL of sterile Ringer's lactate solution according to the instructions of the Brazilian Ministry of Health protocol for the management of the influenza A (H1N1) 2009 pandemic. Total RNA was extracted from the samples using the QIAamp Viral RNA Mini Kit (Qiagen, Hilden, Germany) according to the manufacturer's instructions. Subsequently, a one-step quantitative reverse transcription-polymerase chain reaction was performed against the viral M gene, with the human RNase P target as the internal control of the sample quality and normalization factor of the cycle threshold values.
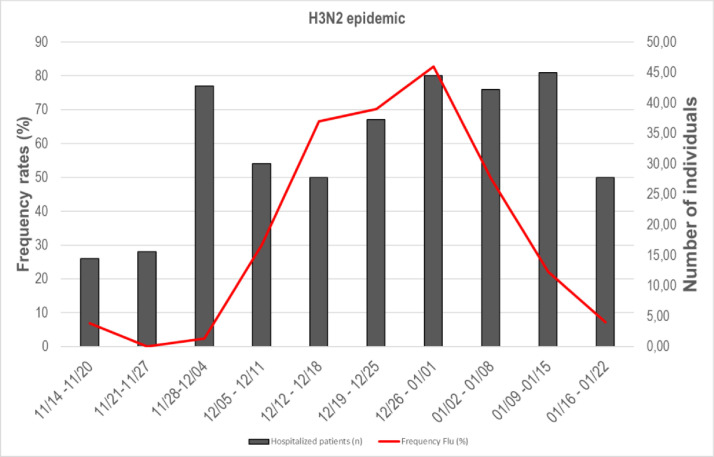
A total of 134 patients with a confirmed diagnosis of influenza A H3N2 were evaluated. The median age was 58.5 years; 24 (17.9%) patients had lung disease, 21 (15.6%) had heart disease, 21 (15.6%) had hematological disease, 9 (6.7%) were pregnant, 9 (6.7%) were aged <5 years, 7 (5.2%) had diabetes, and 6 (4.4%) had nephropathy. Among the patients, 18 (13.4%) required advanced support in the intensive care unit, 8 (5.9%) died, 5 (3.7%) were coinfected with SARS-CoV-2 and one of them died at ICU. A report of previous influenza vaccination was uncommon except for those over 65 years. Fig. 1 shows the relative frequency of the confirmed cases of influenza (H3N2) in the epidemiological weeks starting in November 2021.
Fig. 1.
Relative frequency of the confirmed cases of H3N2 influenza over the epidemiological weeks.
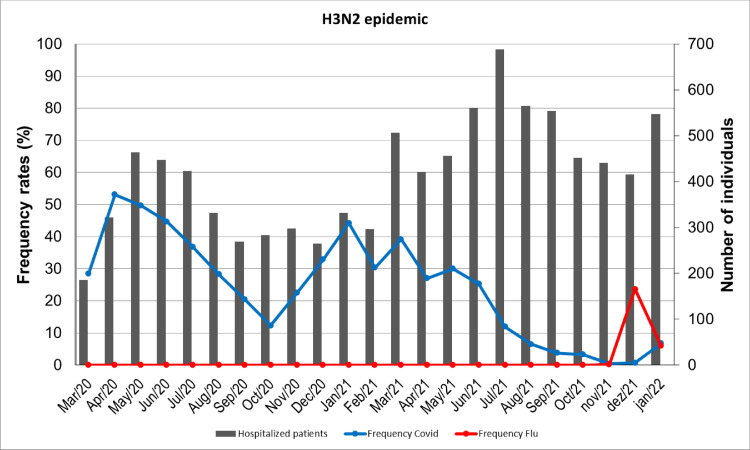
Fig. 2 illustrates influenza surveillance performed since the beginning of the pandemic as well as the relative frequency of the cases of COVID-19 and influenza in patients hospitalized with severe acute respiratory syndrome. The graph reflects the ecological niche occupied competitively by the two viruses—a significant decrease in SARS-CoV-2 cases was necessary for the H3N2 outbreak to occur.
Fig. 2.
Relative frequency of COVID-19 and H3N2 influenza during the pandemic in patients hospitalized with severe acute respiratory syndrome.
This outbreak presents some peculiar features. First, it occurred during the Brazilian summer, an atypical situation when it comes to the seasonal flu virus.2 Flu circulation during summer is usually minimal because weather conditions are less favorable for the transmission of respiratory droplets and aerosols.6 Second feature is the low immunity of the population, a few numbers of Influenza B was detected among our hospitalized patients during the beginning of first wave but influenza A/H3N2 infection was not detected among our patients since the pandemic has started.7, 8. Besides, AH3N2 /Darwin strain was not included in any flu vaccine administered worldwide. Current flu vaccines are updated annually to include strains expected to spread in the upcoming influenza season. Previous H3N2 vaccine strain recommended to the southern hemisphere formulation was the A H3N2/Hong Kong strain but ferret and human antisera react poorly against the Darwin virus in the reference hemagglutination assay.9 This mismatch between Hong Kong vaccine strain and the circulating AH3N2/Darwin like virus also contribute to increase the susceptibility to infection among population. Finally, previous studies have also reported the occurrence of other respiratory viruses when there is a decline in the number of COVID-19 cases in various parts of the world,10 further confirming the hypothesis of ecological niche competition among respiratory viruses. Nonetheless influenza outbreaks can be unpredictable and possible co-circulation during future waves of SARS-CoV-2 can occur. Increase immunization and surveillance for respiratory virus infections should be considered part of an essential public health strategy to combat epidemics that are frequent worldwide.
References
- 1.Iuliano A.D., Roguski K.M., Chang H.H., Muscatello D.J., Palekar R., Tempia S., et al. Estimates of global seasonal influenza-associated respiratory mortality: a modelling study. Lancet. 2018 Mar 31;391(10127):1285–1300. doi: 10.1016/S0140-6736(17)33293-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Siegers J.Y., Dhanasekaran V., Xie R., Deng Y.-.M., Patel S., Ieng V., et al. Genetic and Antigenic Characterization of an Influenza A(H3N2) Outbreak in Cambodia and the Greater Mekong Subregion during the COVID-19 Pandemic, 2020. J Virol [Internet] 2021;95(24) doi: 10.1128/JVI.01267-21. https://journals.asm.org/doi/abs/10.1128/JVI.01267-21 Nov 23 [cited 2022 Mar 21]Available from. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Olsen S.J., Azziz-Baumgartner E., Budd A.P., Brammer L., Sullivan S., Pineda R.F., et al. Decreased influenza activity during the COVID-19 pandemic—United States, Australia, Chile, and South Africa, 2020. Am J Transplant. 2020;20(12):3681–3685. doi: 10.1111/ajt.16381. https://onlinelibrary.wiley.com/doi/full/10.1111/ajt.16381 [Internet]Dec 1 [cited 2022 Mar 21]Available from. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Sullivan S.G., Carlson S., Cheng A.C., Chilver M.B.N., Dwyer D.E., Irwin M., et al. Vol. 25. Eurosurveillance; Australia: 2020. https://www.eurosurveillance.org/content/10.2807/1560-7917.ES.2020.25.47.2001847 (Where Has All the Influenza gone? The impact of COVID-19 On the Circulation of Influenza and Other Respiratory Viruses). March to September[Internet]. 2020 Nov 1 [cited 2022 Mar 21]Available from. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Yeoh D.K., Foley D.A., Minney-Smith C.A., Martin A.C., MacE A.O., Sikazwe C.T., et al. Impact of Coronavirus Disease 2019 Public Health Measures on Detections of Influenza and Respiratory Syncytial Virus in Children During the 2020 Australian Winter. Clin Infect Dis. 2021;72(12):2199–2202. doi: 10.1093/cid/ciaa1475. https://academic.oup.com/cid/article/72/12/2199/5912591 [Internet]Jun 15 [cited 2022 Mar 21]Available from. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Tamerius J.D., Shaman J., Alonso W.J., Bloom-Feshbach K., Uejio C.K., Comrie A., et al. Environmental Predictors of Seasonal Influenza Epidemics across Temperate and Tropical Climates. PLOS Pathog. 2013;9(3) doi: 10.1371/journal.ppat.1003194. https://journals.plos.org/plospathogens/article?id=10.1371/journal.ppat.1003194 [Internet][cited 2022 Mar 21]Available from. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Bullard B.L., Weaver E.A. Strategies Targeting Hemagglutinin as a Universal Influenza Vaccine. Vaccines. 2021;9(3):257. doi: 10.3390/vaccines9030257. https://www.mdpi.com/2076-393X/9/3/257/htm Page 257 [Internet]. 2021 Mar 13 [cited 2022 Mar 21];9Available from. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.de Souza Luna L.K., Perosa D.A.H., Conte D.D., Carvalho J.M.A., Alves V.R.G., Cruz J.S., et al. Different patterns of Influenza A and B detected during early stages of COVID-19 in a university hospital in São Paulo, Brazil. J Infect. 2020 Aug 1;81(2):e104–e105. doi: 10.1016/j.jinf.2020.05.036. http://www.journalofinfection.com/article/S0163445320303133/fulltext [Internet][cited 2022 Mar 28]Available from. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.WHO. Recommended composition of influenza virus vaccines for use in the 2022 southern hemisphere influenza season [Internet]. 2021 Sep [cited 2022 Mar 28]. Available from: https://cdn.who.int/media/docs/default-source/influenza/who-influenza-recommendations/vcm-southern-hemisphere-recommendation-2022/202109_recommendation.pdf.
- 10.Kivit C., Groen K., Jongbloed M., Linssen C., van Loo A., van Gorp E., et al. An off-season outbreak of human metapneumovirus infections after ending of a COVID-19 lockdown. J Infect. 2022 doi: 10.1016/j.jinf.2022.01.042. Feb 3. [DOI] [PMC free article] [PubMed] [Google Scholar]