Abstract
Background:
Hypothermic machine perfusion (HMP) parameters are influenced by donor variables which further affect recipient outcome. Interplay between these parameters can help to predict kidney performance on pump and the long term outcome.
Methods:
All the kidneys transplanted at our center between May 2013 through November 2017 were included in the study. Donor and recipient data was obtained from internal database. Multiple logistic regression models with backward selection were used to determine significant donor and pump variables.
Results:
Donor BMI, KDPI, age and donor sex had a significant association with pump flow. Donor sex, donor type, KDPI and age had significant effect on RI. Diastolic pressure and KDPI were significantly associated with DGF. Duration on pump, KDPI, flow, donor creatinine and type of donor were significantly associated with day 5 creatinine. KDPI was significantly associated with Day 365 creatinine.
Conclusion:
HMP effects early graft function while the long term function depends on donor parameters.
Keywords: Hypothermic machine perfusion, Pump variables, Donor variables
Introduction
Due to the limited number of kidneys available for transplantation, there is a need to utilize this valuable resource in the most efficient manner. There are nearly 100,000 patients awaiting kidney transplant at any time and only 20,931 transplants were performed till December 2,020.1 Hence, every effort should be made to ensure that the maximum number of kidneys are successfully transplanted. Renal preservation has become important as the use of kidneys from donors after circulatory death (DCD) and expanded criteria donors (ECD) have increased over the years. These kidneys are particularly susceptible to ischemic injury which presents clinically as delayed graft function (DGF), primary nonfunction (PNF) and poor long term function.2,3 The first report of hypothermic pulsatile perfusion was presented by Belzer in 1968.4 Soon after, hypothermic pulsatile perfusion was replaced by static cold storage as it was shown to be an easy and cheap method providing kidney preservation up to 30 h without the need for any special equipment.5
As the donor profile changed over the years, interest in pulsatile perfusion re-emerged. Subsequent studies showed lower rates of DGF and PNF in pumped kidneys.6–10 Various studies have used pump flow and resistance (RI) on the pump to predict the probability of DGF and PNF of the kidneys.11–17 It would be of vital clinical interest if a predictive correlation can be established between various donor and pump parameters, with the clinical outcome. Hence, this study was planned to delineate the dynamic correlation between individual donor, pump and recipient parameters and, to apply this correlation in clinical decision making in transplantation. As our center pumps the majority of deceased donor renal allografts, this becomes the largest single center contemporary series evaluating the co-relation of donor/pump variables and their relation to early and late renal allograft function.
Material and methods
After approval by The Ohio State University Institutional Review Board (study ID 2019H0191), all the deceased donor kidneys transplanted at our center from May 2013 through November 2017 were included in the study. The data regarding kidney pump parameters, donor characteristics and clinical outcomes were obtained from an internal prospective database. All the kidneys at our center are pumped on the RM3 pulsatile hypothermic kidney perfusion system (Waters Medical systems). Once the kidneys are on the pump, peak pressure (systolic) is set at 40 mm Hg and remains static. Lower pressure (diastolic) is dynamic and is monitored along with perfusate flow (ml/hour), RI, and temperature (Celsius) of the perfusate. Verapamil is infused into the perfusate to induce vascular dilatation. The acceptable pump parameters at our center are RI < 0.4 and flow greater than 70 ml/min. For this analysis, we included the last pump perfusion characteristics prior to the kidneys being taken off the pump for transplantation. Recipient creatinine measured on post-transplant days used in this study were approximate, using days as close to days 5 and 365 as possible. DGF was defined as the need for dialysis within the first 7 post-operative days. The decision to pump or not to pump the kidneys at our center depends on donor characteristics, especially age and any expected delay in implantation.
Additionally, kidney transplant UNOS STAR data as of June 10, 2019 was used to calculate KDPI and DGF rates of deceased donor kidneys transplanted in the US during the study period.
Statistical analyses
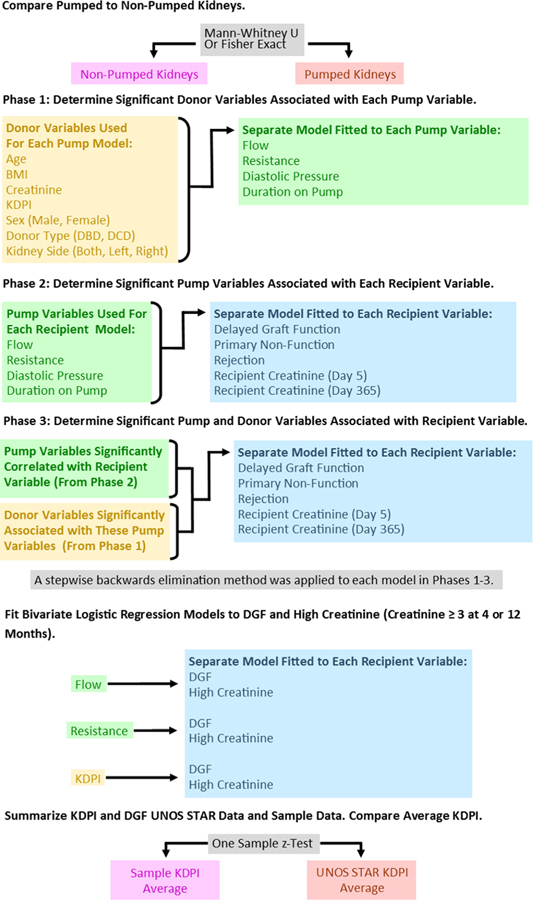
Summary statistics were reported for each continuous variable (median, interquartile range or IQR, range, and sample size) and categorical variable (counts and percentages). Pumped and non-pumped kidneys were compared using Mann-Whitney U tests and Fisher Exact tests. Propensity score inverse probability of treatment weighting (IPTW) was considered to adjust for selection bias between pumped and non-pumped kidneys. However, a larger sample size and additional variables not available for the study would be needed to optimally balance the data. For the model selection process using pumped kidneys, kidney results were excluded if any variable included in the model had a missing value for that kidney. This is to ensure the data stays consistent while the model selection is taking place. The statistical analysis plan included three phases for model variable selection, as shown in Diagram 1. Phases 1 and 2 determined which donor variables were significantly related to each pump variable, and which pump variables were significantly related to each recipient variable. A stepwise backwards elimination method using a p-value threshold of 0.05 was applied to each model to determine variable selection. Each recipient variable was fitted separately with either a multiple logistic regression model for binary recipient variables (DGF, PNF, rejection) or a multiple regression model for continuous recipient variables (recipient creatinine at days 5 and 365). Phase 3 provided evidence as to whether the significant donor variables or significant pump variables were more strongly associated with each recipient variable. After backwards elimination, R2 for the Phase 3 models are provided to measure how strongly model predictions agree with observed values. For logistic regression models, the likelihood-based pseudo R2 is reported.
Diagram 1.
Statistical Analysis Plan.
To show the impact of variables on creatinine a cutoff of 3 mg/dl was used 4–12 months after transplant.
With KDPI being calculated using other donor variables, a multicollinearity analysis was performed to determine whether correlation among the donor variables would affect modeling. A multiple regression model was fitted to day 365 recipient creatinine, treating categorical variables as binary, to determine the variance inflation factor (VIF) of donor variables. A VIF of 10 or greater indicates severe multicollinearity issues. Additionally, the correlation between KDPI and each donor variable was calculated.
Kidney function, based on DGF and high recipient creatinine, was characterized using flow, resistance, and KDPI. KDPI and DGF were summarized using UNOS STAR data and our sample data, comparing the UNOS STAR KDPI to the sample mean KDPI.
Statistical results were interpreted at a 0.05 significance level. SAS (9.4 TS1M3, 64-bit, Cary, NC) was used for statistical analysis.
Results
There were 39 non-pumped kidney recipients and 581 pumped kidneys. Overall, 100 of the 581 pump observations (17%) were missing at least one variable result.
Though not significantly different (Table 1), the non-pumped kidneys had younger donors (36 yr vs 31 yr, p-value = 0.1601), lower donor terminal creatinine (0.9 vs 0.7, p-value = 0.1912), lower donor KDPI (34 vs 30, p-value = 0.0854), more DBD donors (80.9% vs 89.7%, p-value = 0.2050). There was no significant differences in DGF, PNF, rejection (Table 2), and day 5 recipient creatinine. The non-pumped kidneys had lower day 365 creatinine (1.59 vs 1.34, p-value = 0.0049). Excluding 100 observations due to missing values, 481 observations were used for model selection.
Table 1.
Summary of Donor, Pump, and Recipient Results with Mann-Whitney U Tests Comparing Pumped vs Non-Pumped.
| Donor | |||||||
| Pumped | Not Pumped | ||||||
|
|
|
|
|
||||
| Variable | Median (IQR) | Range | N | Median (IQR) | Range | N | P-value |
|
| |||||||
| Age (yrs) | 36 (25–48) | 2–72 | 581 | 31 (22–42) | 9–64 | 39 | 0.1601 |
| BMI (kg/m2) | 27.3 (23.1–31.4) | 14.5–67.5 | 580 | 27.1 (23.6–31.3) | 15.1–49.4 | 39 | 0.9701 |
| Creatinine (mg/dl) | 0.9 (0.7–1.3) | 0.3–6.6 | 581 | 0.7 (0.6–1.2) | 0.4–2.7 | 39 | 0.1912 |
| KDPI | 34 (19–62) | 1–99 | 581 | 30 (17–44) | 1–95 | 39 | 0.0854 |
| Pump Variable | Median (IQR) | Range | N | ||||
| Flow (ml/hr) | 120 (100–133) | 0–240 | 527 | ||||
| Resistance | 0.21 (0.17–0.26) | 0.00–0.57 | 527 | ||||
| Diastolic Pressure | 18 (15–21) | 0–41 | 505 | ||||
| Duration on Pump (hrs) | 8.7 (5.5–12.1) | 0.6–39.8 | 501 | ||||
| Recipient Creatinine (mg/dl) | |||||||
| Day Post Operation | Pumped Median (IQR) | Range | N | Not Pumped Median (IQR) | Range | N | P-value |
| 5 | 2.22 (1.48–4.58) | 0.62–13.39 | 581 | 1.91 (1.16–3.68) | 0.48–8.38 | 39 | 0.1003 |
| 365 | 1.59 (1.25–2.04) | 0.54–15.19 | 568 | 1.34 (0.95–1.63) | 0.65–3.08 | 39 | 0.0049 |
Table 2.
Summary of Donor and Recipient Categorical Results with Fisher Exact Tests Comparing Pumped vs Non-Pumped and Propensity IPTW Chi-Square Tests.
| Donor | |||||||
| Pumped | Not Pumped | ||||||
|
|
|
|
|
||||
| Variable | Value | Count | Percent | Value | Count | Percent | P-value |
|
| |||||||
| Donor Sex | Female | 225 | 38.7% | Female | 15 | 38.5% | 1.0000 |
| Male | 356 | 61.3% | Male | 24 | 61.5% | ||
| Donor Type | DBD | 470 | 80.9% | DBD | 35 | 89.7% | 0.2050 |
| DCD | 111 | 19.1% | DCD | 4 | 10.3% | ||
| Kidney Side | Both | 4 | 0.7% | Both | 0 | 0.0% | 0.9004 |
| Left | 285 | 49.1% | Left | 19 | 48.7% | ||
| Right | 283 | 48.7% | Right | 20 | 51.3% | ||
|
| |||||||
| Recipient | |||||||
| Pumped | Not Pumped | ||||||
| Variable | Count | Percent | Count | Percent | P-value | ||
| Delayed Graft Function | 93 | 16.0% | 2 | 5.1% | 0.1033 | ||
| Primary Non-Function | 2 | 0.3% | 0 | 0.0% | 1.0000 | ||
| Rejection | 61 | 10.5% | 1 | 2.6% | 0.1634 | ||
Association between donor variables and pump variables
Donor BMI, KDPI, age and sex had a significant association with pump flow (Table 3). Donor BMI and age had a positive association with flow (kidneys from older donors and those with high BMI had greater flow on the pump). KDPI had a negative association with flow (kidneys from donors with higher KDPI had lower flow on the pump). Female donor kidneys had lower average flow on the pump than male donor kidneys. Donor sex, type (DCD or DBD), KDPI, and age had significant association with RI on the pump. Kidneys from brain dead donors and female donor kidneys had higher RI on pump. Kidneys with higher KDPI were also associated with higher RI when pumped. Older donor kidneys were associated with lower RI when pumped. Donor BMI and KDPI had positive association with diastolic pressure (donors with high BMI and high KDPI pumped with high pressure on the pump). Kidneys from brain dead donors were associated with less duration on pump than cardiac death donors, while donor creatinine was positively associated with duration on pump (kidneys with higher donor creatinine had longer duration on pump).
Table 3.
Multiple regression fitted separately to each pump variable with significant donor variables (phase 1, N = 481).
| Pump Model* | Donor Parameter | Parameter Level | Parameter Estimate | Final P-value |
|---|---|---|---|---|
|
| ||||
| Flow (ml/hr) | Donor BMI | 0.601 | 0.0018 | |
| KDPI | −0.511 | <0.0001 | ||
| Donor Age (yrs) | 0.316 | 0.0468 | ||
| Donor Sex | Female | −12.5 | <0.0001 | |
| Resistance | Donor Sex | Female | 0.0288 | <0.0001 |
| Donor Type (DCD vs DBD) | DBD | 0.0230 | 0.0056 | |
| KDPI | 0.00141 | <0.0001 | ||
| Donor Age | −0.000927 | 0.0113 | ||
| Diastolic Pressure | Donor BMI | 0.0714 | 0.0033 | |
| KDPI | 0.0356 | <0.0001 | ||
| Duration On Pump | Donor Type (DCD vs DBD) | DBD | −1.25 | 0.0252 |
| Donor Creatinine | 0.613 | 0.0170 | ||
Association between pump variables and post-operative outcome
Table 4 presents the pump variables significantly associated with DGF, day 5 creatinine and day 365 creatinine separately. Diastolic pressure was significantly associated with DGF (higher diastolic pressure being associated with greater odds of a DGF). No pump variables had any significant effect on post-operative rejection. As only two recipients (one in the 481 observations) experienced PNF, a logistic regression model could not be fitted. Flow on the pump, duration on the pump, and diastolic pressure significantly correlated with day 5 creatinine whereas only diastolic correlated with day 365 creatinine.
Table 4.
Logistic regression fitted to DGF and multiple regression fitted separately to day 5 and Day 365 recipient creatinine with significant pump variables (phase 2), and with both significant donor and pump variables (phase 3, N = 481).
| Pump to DGF (Phase 2) | ||||
|
|
|
|||
| Recipient Model | Pump Parameter | Odds Ratio | Final P-value | |
|
| ||||
| DGF | Diastolic Pressure | 1.10 | 0.0006 | |
|
| ||||
| Pump to Recipient Creatinine Models (Phase 2) | ||||
|
|
|
|||
| Recipient Model | Pump Parameter | Parameter Estimate | Final P-value | |
|
| ||||
| Day 5 Recipient Creatinine (mg/dl) | Flow (ml/hr) | −0.0155 | 0.0002 | |
| Duration on Pump (hrs) | 0.125 | <0.0001 | ||
| Diastolic Pressure | 0.0727 | 0.0254 | ||
| Day 365 Recipient Creatinine (mg/dl) | Diastolic pressure | 0.0403 | 0.0073 | |
|
| ||||
| Donor and Pump to DGF (Phase 3) | ||||
|
|
|
|||
| Recipient Model | Donor or Pump Parameter | Parameter Level | Odds Ratio | Final P-value |
|
| ||||
| DGF | Diastolic Pressure | 1.07 | 0.0159 | |
| KDPI | 1.02 | <0.0001 | ||
|
| ||||
| Donor and Pump to Recipient Creatinine Models (Phase 3) | ||||
|
|
|
|||
| Recipient Model | Donor or Pump Parameter | Parameter Estimate | Final P-value | |
|
| ||||
| Day 5 Recipient Creatinine (mg/dl) | Duration on Pump (hrs) | 0.0889 | 0.0003 | |
| KDPI | 0.0149 | 0.0018 | ||
| Flow (ml/hr) | −0.0125 | 0.0007 | ||
| Donor Creatinine | 1.05 | <0.0001 | ||
| Donor Type (DCD vs DBD) | DBD | −1.94 | <0.0001 | |
| Day 365 Recipient Creatinine (mg/dl) | KDPI | 0.0105 | <0.0001 | |
Association between donor/pump variables to post-operative outcome
As diastolic pressure was significantly associated with DGF, diastolic pressure along with its associated donor variables were included in the DGF model. The final model concluded that diastolic pressure and KDPI were significantly associated with DGF. The odds of a DGF increases with higher KDPI and diastolic pressure. The DGF model had an R2 of 0.06.
As diastolic pressure, flow and duration on pump were significantly associated with day 5 recipient creatinine, diastolic pressure, flow and duration, along with their associated donor variables were included in the model. After the backward selection process the models concluded that duration on pump, KDPI, flow, donor creatinine, and donor type (DBD and DCD) were significantly associated with day 5 creatinine. Higher KDPI, longer duration on pump, higher donor creatinine, DCD, and lower flow were associated with higher day 5 recipient creatinine. The final day 5 creatinine model had an R2 of 0.25.
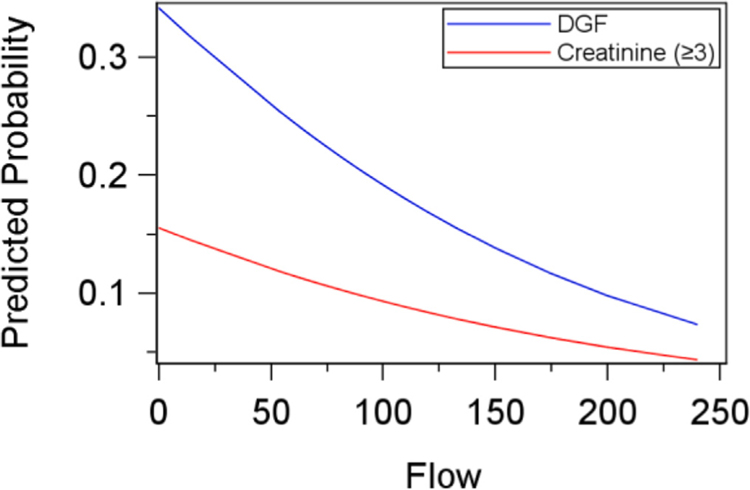
Similarly as diastolic pressure was significantly associated with day 365 recipient creatinine, diastolic pressure, along with the associated donor variables (Donor BMI and KDPI), were included in the model. The final model for day 365 recipient creatinine included concluded only a significant positive association with KDPI with an R2 of 0.04. (Table 4). Figs. 1–3 show the probability of DGF and high creatinine with each of the pump parameters (Resistance, KDPI and Flow). It can be clearly seen that all the pump parameters more strongly predict DGF than creatinine.
Fig. 1.
Predicted Probability Based on Logistic Regression for DGF and elevated Creatinine By Flow.
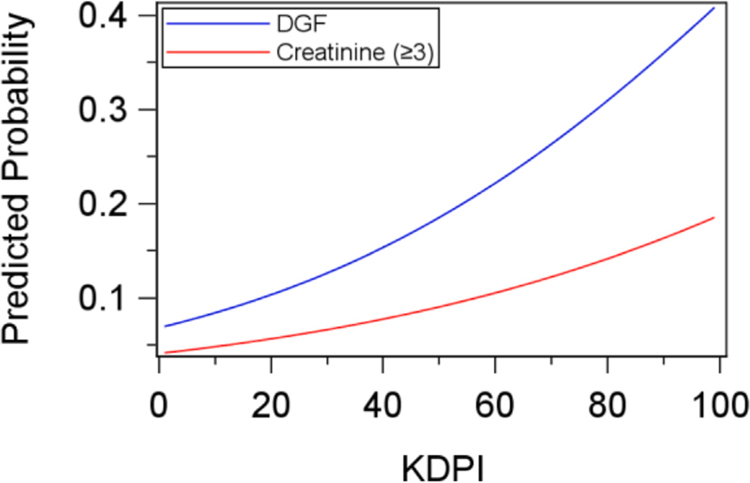
Fig. 3.
Predicted Probability Based on Logistic Regression for DGF and elevated Creatinine By KDPI.
Multicollinearity can be an issue in an analysis if variables are strongly correlated, potentially causing inflated variability, unstable models, and misleading results. Table 5 presents the multicollinearity analysis results. The Variance inflation factor (VIF) of the multiple regression fitted to day 365 recipient creatinine was calculated using donor variables as covariates. Though there were correlations between donor variables, most notably KDPI and age (R = 0.76), the VIF for each donor variable was well below 10, indicating only very mild multicollinearity among the donor variables. The correlation among the variables is not large enough to undermine model fitting, and the variables can all be safely included as covariates.
Table 5.
Variance inflation factor based on multiple regression fitted to day 365 recipient creatinine and correlation between KDPI and other donor variables.
| Variable | Variance Inflation Factor | Correlation With KDPI |
|---|---|---|
|
| ||
| KDPI | 2.77358 | |
| Age | 2.71180 | 0.75675 |
| BMI | 1.10170 | 0.09642 |
| Creatinine | 1.20208 | 0.15626 |
| Gender (Male) | 1.07985 | −0.13352 |
| Donor Type (DBD) | 1.11127 | −0.07144 |
| Kidney Side (Left) | 1.00903 | 0.08298 |
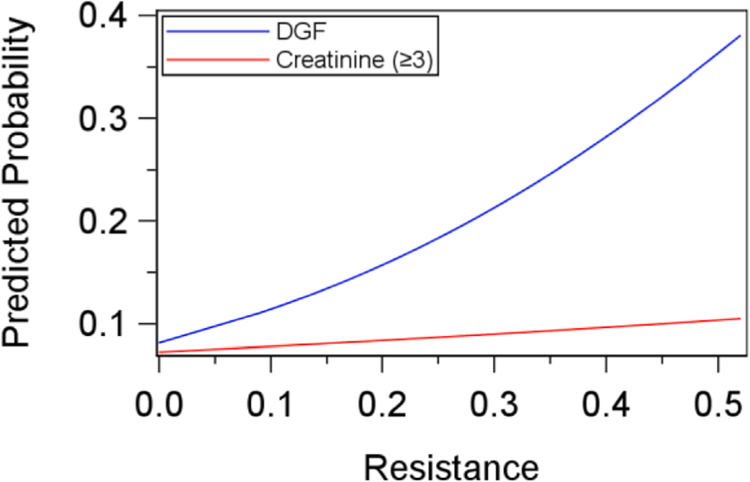
Based on the summary statistics presented in Table 6, the kidneys that had DGF in our study had low median flow, high median KDPI, and high median resistance on the pump compared to the kidneys without DGF. Kidneys with high creatinine (≥3 mg/dl) had a noticeably high median KDPI but median flow and resistance were similar to kidneys with creatinine below 3. The logistic regression models showed that KDPI was a significant effect for both the odds of DGF and the odds of high creatinine at 4 or 12 months (Table 7, Fig. 3), with flow and resistance also being a significant effect on the odds of DGF (Figs. 1 and 2). Decreased flow, increased KDPI and increased resistance each had greater odds for DGF, while only increased KDPI had greater odds for high creatinine at 4 or 12 months.
Table 6.
Median and IQR flow, KDPI, and resistance by DGF and creatinine results.
| Variable | DGF |
4–12 mo. Creatinine≥3 |
||
|---|---|---|---|---|
| No (N = 398) |
Yes (N = 83) |
No (N = 440) |
Yes (N = 41) |
|
| Median (IQR) | Median (IQR) | Median (IQR) | Median (IQR) | |
|
| ||||
| Flow (ml/hr) | 120(100–133) | 109 (92–133) | 120(100–133) | 120(92–133) |
| KDPI | 32 (19–61) | 53 (37–69) | 36 (20–63) | 55 (30–72) |
| Resistance | 0.20 (0.16–0.26) | 0.23 (0.19–0.29) | 0.21 (0.17–0.26) | 0.20 (0.17–0.28) |
Table 7.
Odds ratios for DGF and creatinine based on logistic regression fitted separately to flow, KDPI, and resistance.
| Model | DGF |
4–12 mo. Creatinine≥3 |
||
|---|---|---|---|---|
| Odds Ratio (95% CI) | P-value | Odds Ratio (95% CI) | P-value | |
|
| ||||
| Flow (ml/hr) | 0.99 (0.99, 1.00) | 0.0345 | 0.99 (0.98, 1.00) | 0.2328 |
| KDPI | 1.02 (1.01, 1.03) | <0.0001 | 1.02 (1.00, 1.03) | 0.0078 |
| Resistance | 41.36 (2.46, 696.22) | 0.0098 | 2.37 (0.05, 116.28) | 0.6638 |
Fig. 2.
Predicted Probability Based on Logistic Regression for DGF and elevated Creatinine By Resistance.
Our sample median KDPI was 37.50%, the population and median KDPI of kidneys pumped overall in the US was 49.00%, and the overall population median KDPI for both non-pumped and pumped kidneys was 45.00% (Table 8). Our sample average KDPI (41.29%) was significantly less than both the pumped population average KDPI (49.17%) and the average KDPI of the overall population (45.82%). The rate of DGF in our study population is 17.3%, the overall DGF rate in the kidneys transplanted was 27.72%.
Table 8.
KDPI percentage mean, standard deviation, median and IQR and percent DGF at the population and sample level.
| Mean KDPI (SD) | Median KDPI (IQR) | % DGF | N | |
|---|---|---|---|---|
|
| ||||
| Population Overalla | 45.82 (26.24) | 45.00 (24.00–67.00) | 27.72 | 44,570 |
| Not Pumped | 42.63 (26.20) | 41.00 (20.00–63.00) | 26.92 | 22,817 |
| Pumpedb | 49.17 (25.85) | 49.00 (28.00–71.00) | 28.57 | 21,753 |
| Sample (Pumped)ab | 41.29 (25.81) | 37.50 (22.00–65.00) | 17.3 | 481 |
One sample z-test comparing the overall population mean KDPI to the pumped sample mean provides a p-value 0.0002.
One sample z-test comparing the pumped population mean KDPI to the pumped sample mean provides a p-value <0.0001.
Discussion
Many centers utilize machine perfusion as a diagnostic and therapeutic intervention for DCD and DBD donor kidneys before transplantation. In previous studies, the use of HMP was described as a dichotomous variable without inference to pump parameters of the kidney being pumped. In this study we were particularly interested to find out the correlation between donor parameters, pump parameters and recipient outcome and to identify the most significant variables.
Overall our analysis summarizes trends between (1) the individual donor parameters and the individual pump parameters, (2) individual pump parameters and post-operative outcomes, (3) combined donor + pump parameters and post-operative outcomes. Multiple models, gave us (1) Donor variables significantly associated with each individual pump variables and their positive or negative effect on pump parameters (2) Pump variables significantly associated with post-operative outcomes and their positive or negative effect on post-operative outcomes, (3) Donor/pump variables (when all donor and pump variables were considered together for analysis) significantly associated with post-operative outcomes and their positive or negative effect on post-operative outcome.
Our analysis has shown that the donor variables effect the flow and resistance on the pump in unique way. Therefore, knowing the positive or negative effect of various donor variables can help to pre-determine the expected performance of kidneys on the pump and whenever there is apparent mismatch between expected and observed performance, other factors should be looked into, to make final decision about the utilization of the kidneys.
KDPI is an important calculation18 considered in kidney allocation and our analysis has shown that KDPI has significant effect on pump variables and post-operative creatinine. Female donor kidneys had low flow and high RI on the pump. Kidneys from brain dead donors had high RI on the pump, which can be attributed to the kidney damage sustained during evolution of brain death19
It has been earlier shown that the kidney flow improves and RI decreases on the pump with time and that average flow is reached after 2 hours on the pump,14 hence a period of time for equilibration of perfusion characteristics is appropriate to properly interpret the flow and resistance values.
RI and pump flow are the primary variables of interest to transplant surgeons. These are used to access the quality of kidneys, hence it's important to understand factors influencing these parameters and factors influenced by these parameters (Tables 3 and 4). As shown in our analysis multiple donor parameters are both positively or negatively impacting flow and resistance on the pump. It is thus important to interpret the RI and flow values keeping in mind the donor parameters as there are no standardized cut off values for pump numbers and each case has to be individualized.
Our analysis provides evidence that early outcomes (day 5 creatinine) are more strongly associated with pump variables and later outcomes (day 365 creatinine) are strongly associated with donor variables. Our cohort of kidneys had low incidence of DGF (18.2%), compared to the national average of 27.72% during the study period, which was likely because of the selection bias as kidneys with high RI and low flow were discarded. Likewise, the median KDPI of kidneys used in our cohort was lower than that of the national cohort of pumped kidneys (Table 8) which likely contributed to the lower DGF we observed.
In our cohort, high KDPI and high RI showed greater odds of DGF (Figs. 2 and 3) which are consistent with published literature. Last RI on pump was reported to be an independent risk factor for DGF by Tai et al.20 and by Jochman et al.11 Matsuno et al.12 found higher rate of PNF and severe ATN in kidneys with low machine perfusion flow. Patel et al.14 have found that the kidneys whose flow improved on continuous perfusion on the pump had high DGF rates (64% vs 39%, p < 0.05) and that flow at 2, 4, 6 h was predictive of DGF. Its particularly important to predict and if possible prevent DGF as it has been shown that DGF decreases the probability of having a functioning graft from 52% to 32%, increases the probability of being on dialysis from 10% to 19%, and increases the probability of death from 38% to 50% relative to transplant recipients who do not experience DGF.21 KDPI had been shown earlier to effect the rates of DGF in the DCD and DBD kidney22 but no study has analyzed multiple variables in a step wise pattern to single out the parameters that have most significant effect on pump and kidney function. Our analysis show donor parameters had most significant effect on DGF.
Correlation of pump flow and duration on the pump to the post-operative creatinine (Fig. 1) has been observed in our study as well as in our clinical practice. This was also reported by Matsuno et al.,12 who showed a lower creatinine in the early post-operative period in the group of patients with better flow on pump. Others have found correlation of flow with long term function.23
The non-pumped kidneys at our center were from donors with minimal co-morbidities and these kidneys were transplanted with short cold ischemia times. This reflects in the comparison of donor parameters in Table 1, although there is no statistically significant difference, the not pumped group have better parameters.
Kidney perfusion pump may provide numerical values to access the quality and predict the function of the kidney but the pump numbers sometime can be deceiving as has been shown by Guarrera et al.15 who transplanted eleven kidneys with poor perfusion parameters but acceptable donor variables, and all these kidneys attained acceptable function after transplant. Similar observations were also made by Sonnenday et al.16 who re-initiated HMP on imported kidneys which had poor pump parameters (low flow and high resistance) at the time of machine perfusion by host OPO but had acceptable donor parameters. Hence, many authors have cautioned against discarding kidneys solely based on poor pump numbers.13,17,24 So, it can be beneficial to assess the poor pump numbers in accordance with correlation between various parameters provided by our analysis so that kidneys with acceptable donor parameters are not deemed unsuitable based on poor pump parameters.
When both pump and donor variables were included in the models, KDPI and not the pump parameters, had a significant effect on the long term function of the kidneys. During the study period the national overall average KDPI was 45.82% and national pumped average KDPI was 49.17%. Our study sample had an average KDPI of 42.27%, which was significantly less than both the overall national average and the national pumped average. The lower KDPI at our center might be due to the data set not including the discarded kidneys. This also reflects the conservative approach at our center with acceptance of kidneys and pumping them.
Our analysis indicates that kidneys with favorable parameters will continue to improve in renal function after transplant, but in clinical practice this finding might be confounded with other factors that affect post-operative creatinine like immunosuppressive drug levels. The final multiple regression models in our study show that the quality of the donor kidney largely drives the function of the kidney, with flow more influential in the earlier post-operative days. This is an important observation stating that hypothermic pulsatile perfusion has significant correlations with initial function of the kidney and the long term function has significant correlations with donor parameters.
As there is an increase in the utilization of the ECD and DCD kidneys, and the kidneys are sometimes shipped from long distances, HMP has proven to be useful and has secured its place in this continuum of care. Hence, knowing the patterns and correlations between the donor and pump variables with post-transplant outcomes, provides the surgeon additional information to judiciously select the donor recipient combination.
Conclusion
Donor quality and HMP parameters are important factors influencing the post-operative outcomes. Our study provides evidence that mainly pump parameters influences early function of the kidney and that long term function depends on donor organ quality especially KDPI.
Acknowledgements
The authors thank Daria Faulkner for her assistance in manuscript pre preparation. Population data reported were based on data supplied by the United Network for Organ Sharing as the contractor for the Organ Procurement and Transplantation Network. The interpretation and reporting of these data are the responsibility of the author(s) and in no way should be seen as an official policy of or interpretation by the OPTN or the U.S. Government.
Abbreviations:
- ATN
Acute tubular necrosis
- BMI
body mass index
- CIT
cold ischemia time
- DBD
donation after brain death
- DCD
donation after circulatory death
- DGF
delayed graft function
- ECD
expanded criteria donor
- GFR
glomerular filtration rate
- HMP
hypothermic machine perfusion
- IQR
interquartile range
- KDPI
Kidney donor profile index
- OPTN
Organ Procurement and Transplant Network
- PNF
primary non function
- RI
Resistance
- SCD
standard criteria donor
- SD
standard deviation
- STAR
standard transplant analysis and research
- UNOS
United Network for Organ Sharing
- VIF
Variance inflation factor.
Footnotes
Declaration of competing interest
The Authors declare no conflict of interest.
Financial disclosure
The authors gratefully acknowledge funding from The Ohio State University Center for Clinical and Translational Science Grant UL1TR00273.
References
- 1.Network Opat. Candidates by organ. Published, Updated https://optn.transplant.hrsa.gov/data/view-data-reports/national-data/#; 2020. Accessed December 15, 2020.
- 2.Weber M, Dindo D, Demartines N, Ambühl PM, Clavien P-A. Kidney transplantation from donors without a heartbeat. N Engl J Med. 2002;347(4): 248–255. [DOI] [PubMed] [Google Scholar]
- 3.Cho YW, Terasaki PI, Cecka JM, Gjertson DW. Transplantation of kidneys from donors whose hearts have stopped beating. N Engl J Med. 1998;338(4): 221–225. [DOI] [PubMed] [Google Scholar]
- 4.Belzer FO, Ashby BS, Gulyassy PF, Powell M. Successful seventeen-hour preservation and transplantation of human-cadaver kidney. N Engl J Med. 1968;278(11):608–610. [DOI] [PubMed] [Google Scholar]
- 5.Collins GM, Bravo-Shugarman M, Terasaki PI. Kidney preservation for transportation: initial perfusion and 30 hours' ice storage. Lancet. 1969;294(7632): 1219–1222. [DOI] [PubMed] [Google Scholar]
- 6.Sandal S, Luo X, Massie AB, Paraskevas S, Cantarovich M, Segev DL. Machine perfusion and long-term kidney transplant recipient outcomes across allograft risk strata. Nephrol Dial Transplant. 2018;33(7):1251–1259. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Hameed AM, Pleass HC, Wong G, Hawthorne WJ. Maximizing kidneys for transplantation using machine perfusion: from the past to the future. Medicine. 2016;95(40), e5083. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Guy A, McGrogan D, Inston N, Ready A. Hypothermic machine perfusion permits extended cold ischemia times with improved early graft function. Exp Clin Transplant. 2015;13(2):130–137. [PubMed] [Google Scholar]
- 9.Treckmann J, Moers C, Smits JM, et al. Machine perfusion versus cold storage for preservation of kidneys from expanded criteria donors after brain death: machine perfusion for ECD kidneys. Transpl Int. 2011;24(6):548–554. [DOI] [PubMed] [Google Scholar]
- 10.Moers C, van Gelder F, Napieralski BP, et al. Machine perfusion or cold storage in deceased-donor kidney transplantation. N Engl J Med. 2009;13. [DOI] [PubMed] [Google Scholar]
- 11.Jochmans I, Moers C, Smits JM, et al. The prognostic value of renal resistance during hypothermic machine perfusion of deceased donor kidneys: renal resistance of machine-perfused kidney grafts. Am J Transplant. 2011;11(10): 2214–2220. [DOI] [PubMed] [Google Scholar]
- 12.Matsuno N, Konno O, Mejit A, et al. Application of machine perfusion preservation as a viability test for marginal kidney graft. Transplantation. 2006;82(11):1425–1428. [DOI] [PubMed] [Google Scholar]
- 13.Mozes MF, Skolek RB, Korf BC. Use of perfusion parameters in predicting outcomes of machine-preserved kidneys. Transplant Proc. 2005;37(1): 350–351. [DOI] [PubMed] [Google Scholar]
- 14.Patel SK, Pankewycz OG, Nader ND, Zachariah M, Kohli R, Laftavi MR. Prognostic utility of hypothermic machine perfusion in deceased donor renal transplantation. Transplant Proc. 2012;44(7):2207–2212. [DOI] [PubMed] [Google Scholar]
- 15.Guarrera JV, Goldstein MJ, Samstein B, et al. ‘When good kidneys pump badly’: outcomes of deceased donor renal allografts with poor pulsatile perfusion characteristics. Transpl Int. 2010;23(4):444–446. [DOI] [PubMed] [Google Scholar]
- 16.Sonnenday CJ, Cooper M, Kraus E, Gage F, Handley C, Montgomery RA. The hazards of basing acceptance of cadaveric renal allografts on pulsatile perfusion parameters alone. Transplantation. 2003;75(12):2029–2033. [DOI] [PubMed] [Google Scholar]
- 17.Sampson D, Kauffman HM, Walczak P. Flow and function in machine-preserved kidneys. Br J Surg. 1978;65(1):37–40. [DOI] [PubMed] [Google Scholar]
- 18.services Udohah. KDPI calculator. https://optn.transplant.hrsa.gov/resources/allocation-calculators/kdpi-calculator/; 2020. Accessed December 16, 2020.
- 19.Westendorp WH, Leuvenink HG, Ploeg RJ. Brain death induced renal injury. Curr Opin Organ Transplant. 2011;16(2):151–156. [DOI] [PubMed] [Google Scholar]
- 20.Tai Q, Xue W, Ding X, et al. Perfusion parameters of donation after cardiac death kidneys predict early transplant outcomes based on expanded criteria donor designation. Transplant Proc. 2018;50(1):79–84. [DOI] [PubMed] [Google Scholar]
- 21.Incerti D, Summers N, Ton TGN, Boscoe A, Chandraker A, Stevens W. The lifetime health burden of delayed graft function in kidney transplant recipients in the United States. MDM Policy Pract. 2018;3(1). [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Zens TJ, Danobeitia JS, Leverson G, et al. The impact of kidney donor profile index on delayed graft function and transplant outcomes: a single-center analysis. Clin Transplant. 2018;32(3), e13190. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Sevinc M, Stamp S, Ling J, Carter N, Talbot D, Sheerin N. Ex vivo perfusion characteristics of donation after cardiac death kidneys predict long-term graft survival. Transplant Proc. 2016;48(10):3251–3260. [DOI] [PubMed] [Google Scholar]
- 24.Doshi MD, Reese PP, Hall IE, et al. Utility of applying quality assessment tools for kidneys with KDPI 80. Transplantation. 2017;101(6):1125–1133. [DOI] [PMC free article] [PubMed] [Google Scholar]