Abstract
Vaccination is a major tool for mitigating the coronavirus disease 2019 (COVID-19) pandemic, and mRNA vaccines are central to the ongoing vaccination campaign that is undoubtedly saving thousands of lives. However, adverse effects (AEs) following vaccination have been noted which may relate to a proinflammatory action of the lipid nanoparticles used or the delivered mRNA (i.e., the vaccine formulation), as well as to the unique nature, expression pattern, binding profile, and proinflammatory effects of the produced antigens – spike (S) protein and/or its subunits/peptide fragments – in human tissues or organs. Current knowledge on this topic originates mostly from cell-based assays or from model organisms; further research on the cellular/molecular basis of the mRNA vaccine-induced AEs will therefore promise safety, maintain trust, and direct health policies.
Keywords: adverse effects, COVID-19, lipid nanoparticle, mRNA vaccine, SARS-CoV-2, spike protein
Fighting the COVID-19 pandemic with SARS-CoV-2 S protein-encoding mRNA vaccines
COVID-19 is caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) (Box 1 ) and has resulted in millions of deaths worldwide. Nevertheless, for the majority of SARS-CoV-2-infected individuals, COVID-19 will remain asymptomatic or only mildly symptomatic [1,2]. Although SARS-CoV-2 may also circulate in the gastrointestinal tract [3], being a respiratory virus, the virus itself or its related antigens will not, in most cases, impact tissues and organs other than the respiratory system (RS) (Box 1) [4., 5., 6.]. In patients with severe disease, infection of airway and lung tissues may cause pneumonia and excessive inflammation which can lead to acute respiratory distress syndrome (ARDS) (see Glossary) (Box 1) [7., 8., 9., 10.]. ARDS may then lead to organ damage beyond the RS because of micro-/macro-thromboembolism, hyperinflammation, aberrant complement activation, or extended viremia [7., 8., 9., 10., 11., 12., 13.]. This may be due to the broad expression of its receptor angiotensin-converting enzyme 2 (ACE2) in several cell types and tissues [14., 15., 16.] which results in an expanding tropism of SARS-CoV-2 for various critical organs (heart, pancreas, kidneys, etc.). If systemic collapse and death are avoided, the postulated direct virus ‘attack’ – or indirect effects due to cytokine storm [10,13] or imbalance of the renin–angiotensin system (RAS) [13] – causing multiorgan damage, possibly foster systemic defects which cause a chronic condition (referred to as long COVID-19) which is independently associated with the severity of the initial illness [17].
Box 1. SARS-CoV-2 infection of human cells.
SARS-CoV-2 infection of human cells proceeds via its binding to the cell surface protein ACE2 through the RBD of its protruding S glycoprotein [127] which remains in a metastable prefusion state through the association of subunits 1 (S1) and 2 (S2) via noncovalent interactions [18,19]; the infection process is also facilitated by host proteases [127,128]. In most of SARS-CoV-2-infected carriers the virus is contained in the upper RS, resulting in either no symptoms or mild symptoms [1,2]. A minority will require hospitalization; this is due to severe symptoms which develop due to extensive inflammation, a process often referred to as a ‘cytokine storm’, causing ARDS which may be accompanied by viremia and can lead to systemic multiorgan collapse [7., 8., 9., 10.]. The risk for severe COVID-19 increases significantly with age or pre-existing comorbidities [1,2,129], and younger individuals have a substantially lower risk – even compared to influenza infection [129] – for developing severe COVID-19 [130,131]. It has been postulated that higher pediatric innate interferon responses restrict viral replication and disease progression [132]. In a recent trial, in which young people were intentionally exposed to a low dose of SARS-CoV-2, nearly half of the participants did not become infected, some were asymptomatic, and those who developed COVID-19 reported mild to moderate symptoms, including sore throats, runny noses, sneezing, and loss of sense of smell and taste; fever was less common, and no one developed a persistent cough [133].
SARS-CoV-2 infection in healthy individuals triggers innate as well as adaptive immune system responses, that is, CD4+ and CD8+ T cells and antibodies, including neutralizing antibodies (NAbs) produced by terminally differentiated B cells, which altogether suppress the extent of infection [132,134,135]. As SARS-CoV-2 initially infects the upper RS, defensive immune responses start to develop at respiratory mucosal surfaces, and this is followed by systemic immunity [136,137]. These immune responses are age- and gender-dependent and may either mount poorly in a background of genetic causes and pre-existing morbidities, or become very intense and essentially uncontrolled in severe disease leading to ARDS and systemic failure [11., 12., 13.].
Alt-text: Box 1
Following an unprecedented effort of biomedical research and mobilization of resources, two mRNA vaccines – namely BNT162b2 (ComirnatyTM) from Pfizer-BioNTech and the mRNA-1273 of Moderna (encoded antigen: SARS-CoV-2 S protein of the Wuhan-Hu-1 strain) [18., 19., 20.] – were the first to receive FDA emergency use authorization. In mRNA vaccines, which are characterized by relatively rapid prototyping and manufacturing on a large scale, the S protein-encoding mRNA is delivered via lipid nanoparticles (LNPs) to human cells that produce the mature viral protein or related antigens (Figure 1 , Key figure), which can exhibit a rather wide tissue/organ distribution (discussed later) [20., 21., 22.]. In addition to the plausible proinflammatory role of LNPs (evidenced also from reported immediate allergic reactions) [23,24] and of packaged mRNA – which has nonetheless been engineered by a replacement of uridine with pseudouridine [20,25,26] so as not to trigger innate immunity through pathogen-associated molecular patterns (PAMPs) or damage-associated molecular patterns (DAMPs) receptors – we surmise that vaccination-mediated adverse effects (AEs) can be attributed to the unique characteristics of the S protein itself (antigen) either due to molecular mimicry with human proteins or as an ACE2 ligand.
Figure 1.
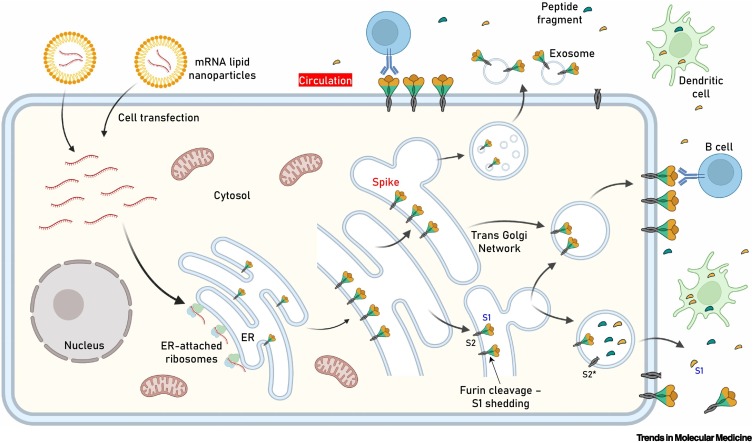
Key figure. Antigen expression–localization following cell transfection with spike (S) protein mRNA-containing lipid nanoparticles (LNPs) used in anti-severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) mRNA vaccines.
Following LNP internalization and mRNA release, the authentic viral signal peptide (as in the Pfizer–BioNTech and Moderna vaccines) drives antigen production in the lumen of the endoplasmic reticulum (ER) where it adopts its natural transmembrane localization via subunit 2 (S2) anchoring. After sorting in the trans Golgi network (TGN), S protein acquires its final position in the transfected human cell membrane, where S1 is exposed to the extracellular space (i.e., may face circulation). Although the extent of antigen expression per cell remains unknown, it is reasonable to assume that this process results in rather extended decoration of transfected cells with S protein. Furin-mediated proteolytic cleavage (as in SARS-CoV-2-infected cells) in the absence of a mutated S1/S2 furin cleavage site at the TGN may result in shedding of cleaved S1 and conversion of S2 into its postfusion structure (S2*). Antigen sorting and trafficking may also induce the release of S protein-containing exosomes. The events shown will occur in the apical and/or basolateral surfaces of polarized (e.g., epithelial) cells. The Pfizer–BioNTech and Moderna constructs do not contain a mutated S1/S2 furin cleavage site. Further research will clarify the impact of the S1/S2 subunits stabilizing D614G (or other) mutation or of a mutated furin cleavage site in antigen distribution, the immunogenicity of the vaccine, and induced adverse events (AEs). Also shown are dendritic cells (professional antigen-presenting cells, APCs) engulfing circulating antigens, and antibody-mediated binding of B cells to cell-anchored antigens.
As delivered mRNAs can theoretically trigger the production of distinct antigens that can distribute systemically [20], they are radically different from conventional platforms (i.e., inactivated whole-virus vaccines or even protein-subunit nanoparticle vaccines) (Box 2 ) where the produced antigen and its distribution are more predictable. As all COVID-19 vaccines rely on the S protein of the original Wuhan-Hu-1 strain [19,20], the differences across different vaccination platforms thus far reported (Box 2) may relate to the various vectors and formulations and/or the S protein constructs employed.
Box 2. Other types of COVID-19 vaccine.
In viral vector vaccines, the S protein coding information is delivered via a replication-deficient adenoviral vector system that contains an encoding dsDNA. In this case, transcripts from adenoviral vectors are generated in the cell nucleus. Here, a major reported AE is immune thromboembolism (including cerebral venous sinus thrombosis) in various organs, probably through excessive innate immune system and endothelial activation [138]. Apart from the S protein itself, AEs can be also attributed to background expression of remaining adenoviral genes or to persisting adenovirus-vector DNA in a transcriptionally active form. Further concerns are the presence of other contaminant proteins, remnants of the vaccine production line, and to pre-existing antivector immunity [20]; this last issue does not apply to the recombinant ChAdOx1-S (Oxford–AstraZeneca) vaccine which employs a nonhuman adenovirus vector. More importantly, the infectious cycle of SARS-CoV-2 takes place exclusively in the cytoplasm, and thus there has been no evolutionary pressure against the presence of splice donor and acceptor sites in its genes. This is a major difference from mRNA vaccines that function in the cytoplasm, since various spliced transcripts from adenoviral vectors can be generated in the cell nucleus [56].
In protein subunit nanoparticle vaccines (e.g., NVX-CoV2373), the S protein is harvested in a cell culture system, purified, and delivered as a trimer via a nanoparticle assembly in an adjuvant. Although preliminary trials indicate that these vaccines can trigger robust immunity [139], reports on AEs are still scarce due to the limited amount of vaccination data.
Finally, in conventional vaccines, the whole virus is inactivated and inoculated using an appropriate adjuvant [26]. A significant benefit is that whereas in the previously discussed technologies the S protein is the sole source of immunogenic epitopes, in this case a wide repertoire of epitopes in other viral proteins is presented. Possible disadvantages include lower immunogenicity, production issues, AEs due to used adjuvant(s) (e.g., aluminum hydroxide), as well as issues that relate to incomplete inactivation of the virus. Given that these vaccines have not reached mass production, reports on possible AEs do not exist.
Alt-text: Box 2
Anti-SARS-CoV-2 mRNA vaccines and their reported adverse effects
Both the BNT162b2 and mRNA-1273 vaccines are administered intramuscularly and mobilize robust and likely durable innate, humoral, and cellular adaptive immune responses [27., 28., 29., 30.]. Existing data on the available mRNA vaccines are mostly limited to serological analyses. Nonetheless, beyond the assessment of immune responses, the understanding of the safety profile of these vaccines is critical to ensure safety, maintain trust, and inform policy. Reportedly, mRNA vaccines are in general well tolerated, with very low frequencies of associated severe postimmunization AEs. Although rare, AEs include serious clinical manifestations such as acute myocardial infarction, Bell’s palsy, cerebral venous sinus thrombosis, Guillain–Barré syndrome, myocarditis/pericarditis (mostly in younger ages), pulmonary embolism, stroke, thrombosis with thrombocytopenia syndrome, lymphadenopathy, appendicitis, herpes zoster reactivation, neurological complications, and autoimmunity (e.g., autoimmune hepatitis and autoimmune peripheral neuropathies [31., 32., 33., 34.]) (see Clinician’s corner). Apart from AEs documented in clinical trials, most of the syndromes or isolated manifestations have been reported in multicenter or even nationwide retrospective observational studies and case series. Although correlation does not necessarily mean causation, active monitoring and awareness regarding reported postvaccination AEs are essential. Importantly, these associated AEs are significantly less frequent than analogous or additional serious AEs induced after severe COVID-19 [31,32,34]. Some vaccine-induced AEs (e.g., myocardial infarction, Guillain–Barré syndrome) were found to increase with age, while others (e.g., myocarditis, anaphylaxis, appendicitis) were more common in younger people [35,36]. Although myocarditis cases are rather rare, in a study of US military personnel the number was higher than expected among males after a second vaccine dose [37]; similarly, the rate of postvaccination cardiac AEs was higher in young boys following the second dose [38,39]. Finally, a recent study showed an increased risk of neurological complications in COVID-19 vaccine recipients (which was nevertheless lower than the risk in COVID-19 patients) [34]. The molecular basis of these AEs remains largely unknown. We postulate that, since most (if not all) of them are also apparent in severe COVID-19 [31], they may be related to acute inflammation caused by both the virus and the vaccine, as well as in the common denominator between the virus and the vaccine, namely, the SARS-CoV-2 S protein (Box 1). The vaccine-encoded antigen (S protein) is stabilized in its prefusion form in the BNT162b2 and mRNA-1273 vaccines [19,20]; it is therefore plausible that, if entering the circulation and distributing systemically throughout the human body (Figure 2 ), it can contribute to these AEs in susceptible individuals.
Clinician’s corner.
Given the plethora of existing data on the available mRNA vaccines, a major ‘known’ is that in the short-term mRNA vaccines are well tolerated by the recipient, and that they can induce a robust immune response and therefore provide prolonged protection against severe COVID-19 (including emerging variants of concern); thus, vaccination remains a major tool for mitigating the COVID-19 pandemic and saving thousands of lives.
It is well established that the risk for severe COVID-19 increases with age or pre-existing comorbidities. Given the ‘unknowns’ discussed herein, boosting doses in healthy children and even adolescents should be delivered only if the benefit–risk profile is clearly established.
Multidisciplinary clinical and basic research aiming at understanding the cellular–molecular basis of the COVID-19 mRNA vaccine-induced AEs – along with active pharmacovigilance and long-term recording in the clinical setting of reported AEs in vaccinated recipients – are critical components for improving vaccines, guaranteeing safety, maintaining trust, and directing health policies.
The technology of the mRNA vaccines will continue to evolve as it opens up a whole new era of novel applications for large-scale development of new vaccines against various infectious and other diseases, including cancer.
Alt-text: Clinician’s corner
Figure 2.
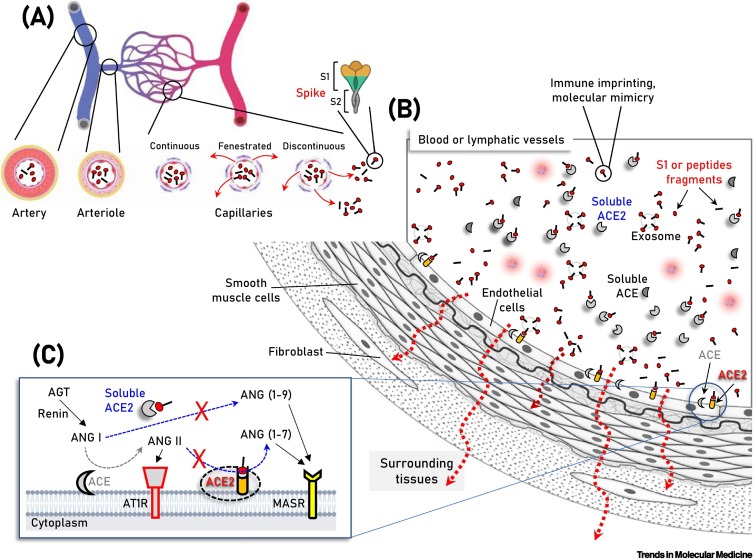
Schematic of the vasculature components showing vaccination-produced S protein/subunits/peptide fragments in the circulation, as well as soluble or endothelial cell membrane-attached angiotensin-converting enzyme 2 (ACE2).
(A,B) Parallel to immune system activation, circulating S protein/subunits/peptide fragments (B) binding to ACE2 may occur not only to ACE2-expressing endothelial cells, but also in multiple cell types of the vasculature and surrounding tissues due to antigen diffusion (e.g., in fenestrated or discontinuous capillary beds) (A, red arrows). These series of molecular events are unlikely for any severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2)-related antigen in the absence of severe coronavirus disease 2019 (COVID-19), where SARS-CoV-2 is contained in the respiratory system. In (C) the two counteracting pathways of the renin–angiotensin system (RAS), namely the ‘conventional’ arm, that involves ACE which generates angiotensin II (ANG II) from angiotensin I (ANG I), and the ACE2 arm which hydrolyzes ANG II to generate angiotensin (1–7) [ANG (1–7)] or ANG I to generate angiotensin (1–9) [ANG (1–9)] are depicted. ANG II binding and activation of the ANG II type 1 receptor (AT1R) promotes inflammation, fibrotic remodeling, and vasoconstriction, whereas the ANG (1–7) and ANG (1–9) peptides binding to MAS receptor (MASR) activate antifibrotic, anti-inflammatory pathways and vasodilation. Additional modules of the RAS (i.e., renin and angiotensinogen, AGT) are also shown. Abbreviation: AT1R, angiotensin II type 1 receptor.
There is also evidence that ionizable lipids within LNPs can trigger proinflammatory responses by activating Toll-like receptors (TLRs) [40]. A recent report showed that LNPs used in preclinical nucleoside-modified mRNA vaccine studies are (independently of the delivery route) highly inflammatory in mice, as evidenced by excessive neutrophil infiltration, activation of diverse inflammatory pathways, and production of various inflammatory cytokines and chemokines [41]. This finding could explain the LNPs’ potent adjuvant activity, supporting the induction of robust adaptive immune responses [24]. Interestingly, inflammatory responses can be exacerbated on a background of pre-existing inflammatory conditions, as was recently shown in a mouse model after administration of mRNA–LNPs [42]; this effect was proven to be specific to the LNP, acting independently of the mRNA cargo.
Although chemical modifications in the RNA molecules used in vaccines (detailed earlier) are intended to decrease TLR sensing of external single-stranded RNAs (and thus proinflammatory signals), there is some evidence that modified uracil residues do not completely abrogate TLR detection of the mRNA; also, while efforts are made to reduce double-stranded (ds) RNA production, there may be small amounts of dsRNA that can occasionally get packaged within mRNA vaccines [26].
In this context, frequent booster immunizations may increase the frequency and/or the severity of the reported AEs.
Vaccine-encoded antigen distribution in the human body and possible interactions with human proteins
Following vaccination, a cell may present the produced S protein (or its subunits/peptide fragments) to mobilize immune responses or be abolished by the immune system (e.g., cytotoxic T cells) [25]. Consequently, the debris produced, or even the direct secretion (including shedding) of the antigen by the transfected cells, may release large amounts of the S protein or its subunits/peptide fragments to the circulation (Figure 1) [19,20]. The anti-SARS-CoV-2 vaccine mRNA-containing LNPs are injected into the deltoid muscle and exert an effect in the muscle tissue itself, the lymphatic system, and the spleen, but can also localize in the liver and other tissues [21,22,43,44] from where the S protein or its subunits/peptide fragments may enter the circulation and distribute throughout the body. It is worth mentioning that liver localization of LNPs is not a universal property of carrier nanoparticles, as specific modifications in their chemistry can retain immunogenicity with minimal liver involvement [43,45]. In line with a plausible systemic distribution of the antigen, it was found that the S protein circulates in the plasma of the BNT162b2 or mRNA-1273 vaccine recipients as early as day 1 after the first vaccine injection [46]. Reportedly, antigen clearance is correlated with the production of antigen-specific immunoglobulins or may remain in the circulation (e.g., in exosomes) for longer periods [47,48], providing one reasonable explanation (among others) for the robust and durable systemic immune responses found in vaccinated recipients [49,50]. Therefore, there is likely to be an extensive range of expected interactions between free-floating S protein/subunits/peptide fragments and ACE2 circulating in the blood (or lymph), or ACE2 expressed in cells from various tissues/organs (Figure 2) [14., 15., 16.]. This notion is further supported by the finding that in adenovirus-vectored vaccines (Box 2), the S protein produced upon vaccination has the native-like mimicry of SARS-CoV-2 S protein’s receptor binding functionality and prefusion structure [51].
Additional interactions with human proteins in the circulation, or even the presentation to the immune system of S protein antigenic epitopes [52] mimicking human proteins (molecular mimicry) may occur [53., 54., 55., 56.]. Reportedly, some of the near-germline SARS-CoV-2-NAbs against S receptor-binding domain (RBD) reacted with mammalian self-antigens [57], and SARS-CoV-2 S antagonizes innate antiviral immunity by targeting multiple pathways controlling interferon (IFN) production [58]. Also, a sustained elevation in T cell responses to SARS-CoV-2 mRNA vaccines has been found (data not yet peer-reviewed) in patients who suffer from chronic neurologic symptoms after acute SARS-CoV-2 infection as compared with healthy COVID-19 convalescents [59]. Given the reported (rare) neurological AEs following vaccination, it was suggested that further studies are needed to assess whether antibodies against the vaccine-produced antigens can cross-react with components of the peripheral nerves [34]. Further concerns include the possible development of anti-idiotype antibodies against vaccination-induced antibodies as a means of downregulation; anti-idiotype antibodies – apart from binding to the protective neutralizing SARS-CoV-2 antibodies – can also mirror the S protein itself and bind ACE2, possibly triggering a wide array of AEs [60]. Worth mentioning is a systems vaccinology approach (31 individuals) of the BNT162b2 vaccine (two doses) effects, where anticytokine antibodies were largely absent or were found at low levels (contrary to findings in acute COVID-19 [61,62]), while two individuals had anti-interleukin-21 (IL-21) autoantibodies, and two other individuals had anti-IL-1 antibodies [63]. In this context, anti-idiotypic antibodies can be particularly enhanced after frequent boosting doses that trigger very high titers of immunoglobulins [64]. Frequent boosting doses may also become a suboptimal approach as they can imprint serological responses toward the ancestral Wuhan-Hu-1 S protein, minimizing protection against novel viral S variants [65,66].
The potential interaction at a whole-organism level of the native-like S protein and/or subunits/peptide fragments with soluble or cell-membrane-attached ACE2 (Figure 2) can promote ACE2 internalization and degradation [67,68]. In support of this, soluble ACE2 induces receptor-mediated endocytosis of SARS-CoV-2 via interaction with proteins related to the RAS [69]. Prolonged loss or reduced ACE2 activity may result in extensive destabilization of the RAS which may then trigger vasoconstriction, enhanced inflammation, and/or thrombosis due to unopposed ACE and angiotensin-2 (ANG II)-mediated effects (Figure 2) [13]. Indeed, decreased ACE2 expression and/or activity contributes, among other things, to the development of ANG II-mediated hypertension in mice, indicating vasculature dysfunction [67]. The baseline expression levels of ACE2 in endothelial cells, or its induced expression levels upon stimulation from other tissue-resident cells, along with the potential of endothelial cells to shed ACE2 to the circulation, or their sensitivity to SARS-CoV-2 infection is debatable [70., 71., 72., 73.]. Nonetheless, even relatively low ACE2 expression levels in endothelial cells (e.g., compared to levels in epithelial cells) [15,16,70,71], along with the high expression levels of ACE2 in other cell types of the vasculature (e.g., heart fibroblasts/pericytes) [15,74], indicate that the vasculature can be sensitive to free-floating S protein or its subunits/peptide fragments (Figure 2). These effect(s), especially in capillary beds, and the prolonged antigen presence in the circulation [46., 47., 48.], along with the systemic excessive immune response to the antigen, can then trigger sustained inflammation (discussed later) which can injure the endothelium, disrupting its antithrombogenic properties in multiple vascular beds.
The SARS-CoV-2 S protein-induced effects in mammalian cells or model organisms
Reportedly, intravenous (i.v.) injection of the S1 subunit in mice results in its localization in endothelia of mice brain microvessels showing colocalization with ACE2, caspase-3, IL-6, tumor necrosis factor α (TNF-α), and C5b-9; it was thus suggested that endothelial damage is a central part of SARS-CoV-2 pathology which may be induced by the S protein alone [75]. Also, the S1 subunit (or recombinant S1 RBD) impaired endothelial function via downregulation of ACE2 [76] and induced degradation of junctional proteins that maintain endothelial barrier integrity in a mouse model of brain microvascular endothelial cells or cerebral arteries; this latter effect was more enhanced in endothelial cells from diabetic versus normal mice [77]. Similarly, the S1 subunit decreased microvascular transendothelial resistance and barrier function in cultured human pulmonary cells [78]. Further, S protein disrupted human cardiac pericytes function and triggered increased production of proapoptotic factors in pericytes, causing endothelial cells death [79]. In support of this, administration of the S protein promoted dysfunction of human endothelial cells as evidenced by, for example, increased expression of the von Willebrand factor [80]. Other reports indicate that S1 can directly induce coagulation by competitive binding to both soluble and cellular heparan sulfate/heparin (an anticoagulant) [81., 82., 83., 84.], while cell-free hemoglobin, as a hypoxia counterbalance, cannot attenuate disruption of endothelial barrier function, oxidative stress, or inflammatory responses in human pulmonary arterial endothelial cells exposed to S1 [85]. Consistently, S protein binds fibrinogen (a blood coagulation factor), and S protein virions have been found to enhance fibrin-mediated microglia activation (data not yet peer-reviewed) and induce fibrinogen-dependent lung pathology in mice [86], while S1 binding to platelets' ACE2 triggers their aggregation [84]. Interestingly, both the ChAdOx1 (AstraZeneca) and BNT162b2 vaccines can elicit antiplatelet factor 4 (anti-PF4) antibody production even in recipients without clinical manifestation of thrombosis [87].
Intriguingly, the S protein increases human cell syncytium formation [88,89], triggering pyroptosis of syncytia formed by fusion of S and ACE2-expressing cells [90]. Also, in cells or mouse experimental models, it was shown that S removes lipids from model membranes and interferes with the capacity of high-density lipoprotein to exchange lipids [91], inhibits DNA damage repair processes [92], and induces Snail-mediated epithelial–mesenchymal transition marker changes and lung metastasis in a breast cancer mouse model [93].
In support of the possibility that there is a wide range of S protein binders, Aβ1 – 42 (the 42 amino acid form of amyloid β in cerebrospinal fluid) was found to bind with high affinity to the S1 subunit and ACE2 [94]. Aβ1 – 42 strengthened the binding of S1 to ACE2 and increased viral entry and production of IL-6 in a SARS-CoV-2 pseudovirus infection mouse model. Data from this surrogate mouse model with IV inoculation of Aβ1 – 42 showed that the clearance of Aβ1 – 42 in the blood was dampened in the presence of the extracellular domain of the S protein trimers [94]. Given the wide ACE2 expression in human brain [95], a study of particular interest showed that IV-injected radioiodinated S1 (I-S1) readily crossed by adsorptive transcytosis the blood–brain barrier in male mice, was taken up by brain regions, and entered the parenchymal brain space. I-S1 was also taken up by the lung, spleen, kidney, and liver; intranasally administered I-S1 also entered the brain, although at lower levels than after i.v. administration [96]. Similarly, S1 was found to disrupt the blood–brain barrier integrity at a 3D blood–brain barrier microfluidic model [97]. In support of this, biodistribution studies of the mRNA–LNP platform by Moderna in Sprague Dawley rats revealed the presence of low levels of mRNA in the brain, indicating that the mRNA–LNPs can cross the blood–brain barrier [22].
Finally, it was recently reported that human T cells express ACE2 at levels sufficient to interact with the S protein [98], while it had been shown previously that SARS-CoV-2 uses CD4 to infect T helper lymphocytes, and that S promotes a proinflammatory activation profile on the most potent antigen-presenting cells (APCs) (i.e., human dendritic cells) [99]. If these observations are confirmed, they may explain a SARS-CoV-2 vaccination-mediated AE, namely, reactivation of varicella zoster virus [100,101].
S protein-induced proinflammatory responses and unique gene expression signatures following vaccination
Reportedly, S protein (apart from the LNP–mRNA platform discussed earlier) mediates proinflammatory and/or injury (of different etiology) responses in various human cell types [102., 103., 104.], and ACE2-mediated infection of human bronchial epithelial cells with S protein pseudovirions induced inflammation and apoptosis [105]. Also, S protein promoted an inflammatory cytokine IL-6/IL-6R-induced trans signaling response and alarmin secretion in human endothelial cells, along with increased oxidative stress, induction of inflammatory paracrine senescence, and higher levels of leucocyte adhesion [106]. Other reports indicate that S protein triggers an inflammatory response signature in human corneal epithelial cells [107], increases oxidative stress and DNA ds breaks in human peripheral-blood mononuclear cells (PBMCs) postvaccination [108], and binds to lipopolysaccharide, boosting its proinflammatory activity [109,110]. Furthermore, S protein induces neuroinflammation and caspase-1 activation in BV-2 microglia cells [111] and blocks neuronal firing in sensory neurons [112]. The S protein-induced systemic inflammation may proceed via TLR2-dependent activation of the nuclear factor κB (NF-κB) pathway [113], while structure-based computational models showed that S protein exhibits a high-affinity motif for binding T cell receptors (TCRs), and may form a ternary complex with histocompatibility complex class II molecules; indeed, analysis of the TCR repertoire in COVID-19 patients showed that those with severe hyperinflammatory disease exhibit TCR skewing consistent with superantigen (S protein) activation [114]. In in vivo mouse models, S protein activated macrophages and contributed to induction of acute lung inflammation [115], while intratracheal instillation of the S1 subunit in transgenic mice overexpressing human ACE2 induced severe COVID-19-like acute lung injury and inflammation. These effects were milder in wild-type mice, indicating the phenotype dependence on human ACE2 expression [78]. Consistently, the S1 subunit has been found to act as a PAMP that, via pattern recognition receptor engagement, induces viral infection-independent neuroinflammation in adult rats [116].
These observations correlate with the finding of a systemic inflammatory signature after the first BNT162b2 vaccination which was accompanied by TNF-α and IL-6 upregulation after the second dose [117]; these effects may also relate to a proinflammatory action of the mRNA–LNP platform (see earlier). In a thorough systems vaccinology study of the BNT162b2 mRNA vaccine effects, younger participants tended to have greater changes in monocyte and inflammatory modules 1 day after the second dose, whereas older individuals had increased expression of B and T cell modules. Moreover, single-cell transcriptomics analysis at the same time point revealed the emergence of a unique myeloid cell cluster out of 18 cell clusters identified in total. This cell cluster does not represent myeloid-derived suppressor cells, it expressed IFN-stimulated genes and was not found in COVID-19 infection; also, it was similar to an epigenetically reprogrammed monocyte population found in the blood of donors being vaccinated with two doses of an influenza vaccine [63]. Whether epigenetic reprogramming underlies the enhanced IFN-induced gene response in C8 cells after secondary BNT162b2 vaccination remains to be clarified. Finally, a comparison between the BNT162b2 vaccine-induced gene expression signatures at day 7 post-prime (d7PP) and post-boost (d7PB) doses and that of other vaccine types (e.g., inactivated or live-attenuated vaccines) exhibited weak correlation both between d7PP and d7PB as well as with other vaccines [63]. These findings suggest the evolution of novel genomic responses after the second dose and, more importantly, the unique biology of mRNA vaccines versus other more conventional platforms. Of particular interest is also the report of a cytokine release syndrome (CRS) – an extremely rare immune-related AE of immune checkpoint inhibitors – post-BTN162b2 vaccination in a patient with colorectal cancer on longstanding anti-programmed death 1 (PD-1) monotherapy; the anti-PD1 blockade-mediated CRS was evidenced by increased inflammatory markers, thrombocytopenia, elevated cytokine levels, and steroid responsiveness [118]. These proinflammatory effects could be particularly pronounced in the elderly, since recent data revealed that senescent cells become hyperinflammatory in response to the S1 subunit, followed by increased expression of viral entry proteins and reduced antiviral gene expression in nonsenescent cells through a paracrine mechanism [119].
The need to investigate the molecular basis of vaccination-induced AEs
Anti-SARS-CoV-2 mRNA vaccines induce durable and robust systemic immunity, and thus their contribution in mitigating the COVID-19 pandemic and saving thousands of lives is beyond doubt. This technology has several advantages over conventional vaccines [120] and opens a whole new era for the development of novel vaccines against various infectious and other diseases, including cancer. Based on currently available molecular insights (mostly in cell-based assays and model organisms), we hypothesize that the rare AEs reported following vaccination with S protein-encoding mRNA vaccines may relate to the nature and binding profile of the systemically circulating antigen(s) (Figure 1, Figure 2), although the contribution of the LNPs and/or the delivered mRNA is likely also significant [24,26,41]. Therefore, the possibility of subclinical organ dysfunction in vaccinated recipients which could increase the risk, for example, of future (cardio)vascular or inflammatory diseases should be thoroughly investigated. Given that severe COVID-19 correlates with older age, hypertension, diabetes, and/or cardiovascular disease, which all share a variable degree of ACE2 signaling deregulation, additional ACE2 downregulation induced by vaccination may further amplify an unbalanced RAS. Regarding localization of LNPs in the liver and consequent antigen expression, it is worth mentioning that the liver is continuously exposed to a multitude of self and foreign antigens and can mount efficient immune responses against pathogens as it hosts convectional APCs (e.g., dendritic cells, B cells, and Kupfer cells). Additional liver cell types – such as liver sinusoidal endothelial cells, hepatic stellate cells, and hepatocytes – also have the capacity to act as APCs [121]. It is plausible, though as yet unproven, that as the S protein is produced in liver cells, both conventional and unconventional APCs may prime adaptive but also innate immune responses in the liver’s immunological niche. Despite the liver’s major tolerogenic role [122], the sustained expression of S protein-related antigens (Figure 1) can potentially skew the immune response towards autoimmune-like tissue damage, as in the observed cases of autoimmune hepatitis following vaccination [123,124]. It therefore merits further investigation whether LNPs can transfect any other nonimmunological body tissues bearing cells that can act as unconventional APCs, thus inducing a sustained immune response but also a self-response, as in cases of chronic viral infections [125].
Concluding remarks
Although the benefit–risk profile remains strongly in favor of COVID-19 vaccination for the elderly and patients with age-related or other underlying diseases, an understanding of the molecular–cellular basis of the anti-SARS-CoV-2 mRNA vaccine-induced AEs is critical for the ongoing and future vaccination and booster campaigns. In parallel, the prospective pharmacovigilance and long-term monitoring (clinical/biochemical) of vaccinated recipients versus matched controls should evolve in well-designed clinical trials. Moreover, the use of alternative chemistries for LNPs, and of S protein in its closed form (not prone to ACE2 binding) [126], along with the use of SARS-CoV-2 nucleocapsid protein or solely the S RDB, may be valuable alternatives for refined, next-generation mRNA vaccines. Finally, as we essentially do not know for how long and at what concentration the LNPs and the antigen(s) remain in human tissues or the circulation of poor vaccine responders, the elderly, or children (see Outstanding questions), and given the fact that cellular immunity likely persists despite reduced in vitro neutralizing titers [28], boosting doses should be delivered only where the benefit–risk profile is clearly established.
Outstanding questions.
What are the localization pattern, transfection efficacy, and clearance rates of the mRNA vaccine LNPs in the human body?
Can we refine LNP chemistry towards retaining transfection efficacy and at the same time assuring on-demand tissue distribution?
Do the adverse inflammatory reactions noted postvaccination also relate – and if yes, to what extent – to LNPs and/or the mRNA used in mRNA vaccines?
What are the mechanistic details of antigen expression, processing, and cellular localization following cell transfection with the LNPs?
What would the impact be of excessive ‘decoration’ of nonprofessional antigen-presenting transfected human (e.g., liver) cells with transmembrane S protein?
Does the antigen or related subunits‐peptide fragments leak into the circulation, and if so, in which form, at what concentration, and for how long? Is there any association with the vaccine-mediated immune responses?
Is the probable binding of the antigen to ACE2 in the vasculature accountable for the cardiovascular, metabolic, or other (e.g., inflammation-related) reported AEs?
Does the antigen cross the blood–brain barrier?
Is there any noteworthy molecular mimicry (especially of the major antigenic sites) between the S protein and the human proteome?
What is the profile of mucosal immunity induced by the mRNA COVID-19 vaccines?
It is the case that vaccination-mediated immunity (two doses) against the used ancestral antigen (Wuhan-Hu-1 S protein) wanes over time, or do we simply partially lose protection due to evolutionary leaps of the S protein (e.g., at the Omicron variant)? In that case, do we really need boosting doses with the same antigen?
Does boosting, apart from raising antibody titers, also promote antibody diversification?
What would be the profile of immune responses and AEs following mRNA-guided expression of the S protein in its closed form (a form not prone to ACE2 binding)?
Alt-text: Outstanding questions
Overall, parallel to the ongoing research on the most challenging topics of SARS-CoV-2 biology, evolving dynamics and adaptation capacity to human species (i.e., transmission–infection rate and disease severity), the basic and clinical research (see Outstanding questions) aiming to understand the molecular–cellular basis of the rare AEs of the existing first-generation mRNA vaccines should be accelerated as an urgent and vital public health priority.
Acknowledgments
Acknowledgments
The authors received no funding for the preparation of this opinion article.
Author contributions
I.P.T.: conceptualization, writing, and preparation of the figures. E.T., D.P., H.A., M.P., A.S., E.A., E.K. and M.A.D.: review, comments, and further additions. All authors contributed to discussions of the scope of this opinion article and approved the final revised version of the manuscript.
Declarations of interests
The authors declare no competing interests related to this opinion article.
Glossary
- Acute respiratory distress syndrome (ARDS)
a life-threatening condition in which fluid builds up in the lungs, interfering with the gas exchange function and preventing oxygenation of the blood and organs.
- Adverse effect (AE)
an undesired effect of a medication or clinical intervention with potentially harmful consequences.
- Angiotensin-converting enzyme 2 (ACE2)
an enzyme involved in the homeostatic regulation of circulating angiotensin I and angiotensin II levels by converting them to angiotensin (1–9) and angiotensin (1–7) peptides respectively.
- Bell’s palsy
an idiopathic episode of facial muscle weakness or paralysis on one side of the face. This condition results from dysfunction of the seventh cranial nerve (the facial nerve).
- Cerebral venous sinus thrombosis
a rare blood-clotting event that occurs in the venous sinuses of the brain and prevents blood from draining out of the brain. As a result, pressure builds up and can lead to swelling and hemorrhage.
- Cytokine storm
a characteristic of COVID-19 (or other disease) where abnormally high levels of circulating cytokines are produced and contribute to disease severity.
- Guillain–Barré syndrome
a rare, autoimmune neurological disorder in which the body's immune system erroneously attacks the peripheral nerves, causing muscle weakness and, if left untreated, paralysis.
- Long COVID-19
a term that refers to a range of new, returning, or ongoing symptoms that persist beyond the initial phase of a SARS-CoV-2 infection.
- Molecular mimicry
the process in which an immune response against a foreign antigen is inadvertently also directed against a self-antigen that closely resembles the triggering foreign antigen.
- Receptor-binding domain (RBD)
the part of a binding protein (e.g., in SARS-CoV-2 S protein) used to anchor the protein to its receptor.
- Renin–angiotensin system (RAS)
a system that is critical in the physiological regulation of (among others) neural, gut, cardiovascular, blood pressure, and kidney functions, as well as fluid and salt balance. It involves the enzyme renin which catalyzes the production of angiotensin I.
- Serological analysis
any analysis performed with blood serum, usually focusing on measuring antibody levels.
- Syncytium
a cell with multiple nuclei resulting from multiple fusions of uninuclear cells.
- Viremia
the detection of replication-competent viral particles in the bloodstream.
References
- 1.Jin J., et al. Individual and community-level risk for COVID-19 mortality in the United States. Nat. Med. 2021;27:264–269. doi: 10.1038/s41591-020-01191-8. [DOI] [PubMed] [Google Scholar]
- 2.O’Driscoll M., et al. Age-specific mortality and immunity patterns of SARS-CoV-2. Nature. 2021;590:140–145. doi: 10.1038/s41586-020-2918-0. [DOI] [PubMed] [Google Scholar]
- 3.Gaebler C., et al. Evolution of antibody immunity to SARS-CoV-2. Nature. 2021;591:639–644. doi: 10.1038/s41586-021-03207-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Andersson M.I., et al. SARS-CoV-2 RNA detected in blood products from patients with COVID-19 is not associated with infectious virus. Wellcome Open Res. 2020;5:181. doi: 10.12688/wellcomeopenres.16002.1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Wang W., et al. Detection of SARS-CoV-2 in different types of clinical specimens. JAMA. 2020;323:1843–1844. doi: 10.1001/jama.2020.3786. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Wölfel R., et al. Virological assessment of hospitalized patients with COVID-2019. Nature. 2020;581:465–469. doi: 10.1038/s41586-020-2196-x. [DOI] [PubMed] [Google Scholar]
- 7.Chen G., et al. Clinical and immunological features of severe and moderate coronavirus disease 2019. J. Clin. Invest. 2020;130:2620–2629. doi: 10.1172/JCI137244. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Deinhardt-Emmer S., et al. Early postmortem mapping of SARS-CoV-2 RNA in patients with COVID-19 and the correlation with tissue damage. eLife. 2021;10 doi: 10.7554/eLife.60361. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Fajnzylber J., et al. SARS-CoV-2 viral load is associated with increased disease severity and mortality. Nat. Commun. 2020;11:5493. doi: 10.1038/s41467-020-19057-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Gupta A., et al. Extrapulmonary manifestations of COVID-19. Nat. Med. 2020;26:1017–1032. doi: 10.1038/s41591-020-0968-3. [DOI] [PubMed] [Google Scholar]
- 11.Andreakos E., et al. A global effort to dissect the human genetic basis of resistance to SARS-CoV-2 infection. Nat. Immunol. 2022;23:159–164. doi: 10.1038/s41590-021-01030-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Galani I.-E., et al. Untuned antiviral immunity in COVID-19 revealed by temporal type I/III interferon patterns and flu comparison. Nat. Immunol. 2021;22:32–40. doi: 10.1038/s41590-020-00840-x. [DOI] [PubMed] [Google Scholar]
- 13.Trougakos I.P., et al. Insights to SARS-CoV-2 life cycle, pathophysiology, and rationalized treatments that target COVID-19 clinical complications. J. Biomed. Sci. 2021;28:9. doi: 10.1186/s12929-020-00703-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Gkogkou E., et al. Expression profiling meta-analysis of ACE2 and TMPRSS2, the putative anti-inflammatory receptor and priming protease of SARS-CoV-2 in human cells, and identification of putative modulators. Redox Biol. 2020;36 doi: 10.1016/j.redox.2020.101615. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Muus C., et al. Single-cell meta-analysis of SARS-CoV-2 entry genes across tissues and demographics. Nat. Med. 2021;27:546–559. doi: 10.1038/s41591-020-01227-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Ziegler C.G.K., et al. SARS-CoV-2 Receptor ACE2 is an interferon-stimulated gene in human airway epithelial cells and is detected in specific cell subsets across tissues. Cell. 2020;181:1016–1035. doi: 10.1016/j.cell.2020.04.035. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Blomberg B., et al. Long COVID in a prospective cohort of home-isolated patients. Nat. Med. 2021;27:1607–1613. doi: 10.1038/s41591-021-01433-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Martínez-Flores D., et al. SARS-CoV-2 vaccines based on the spike glycoprotein and implications of new viral variants. Front. Immunol. 2021;12 doi: 10.3389/fimmu.2021.701501. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Jackson C.B., et al. Mechanisms of SARS-CoV-2 entry into cells. Nat. Rev. Mol. Cell Biol. 2022;23:3–20. doi: 10.1038/s41580-021-00418-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Heinz F.X., Stiasny K. Distinguishing features of current COVID-19 vaccines: knowns and unknowns of antigen presentation and modes of action. NPJ Vaccines. 2021;6:104. doi: 10.1038/s41541-021-00369-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.European Medicines Agency . European Medicines Agency; 2021. Comirnaty Assessment Report COVID-19 Vaccine Comirnaty. EMA/707383/2020 Corr.1*1. [Google Scholar]
- 22.European Medicines Agency . European Medicines Agency; 2021. Moderna Assessment Report COVID-19 Vaccine Moderna. EMA/15689/2021 Corr.1*1. [Google Scholar]
- 23.Moghimi S.M. Allergic reactions and anaphylaxis to LNP-based COVID-19 vaccines. Mol. Ther. 2021;29:898–900. doi: 10.1016/j.ymthe.2021.01.030. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Igyártó B.Z., et al. Future considerations for the mRNA–lipid nanoparticle vaccine platform. Curr. Opin. Virol. 2021;48:65–72. doi: 10.1016/j.coviro.2021.03.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Chaudhary N., et al. mRNA vaccines for infectious diseases: principles, delivery and clinical translation. Nat. Rev. Drug Discov. 2021;20:817–838. doi: 10.1038/s41573-021-00283-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Chung Y.H., et al. COVID-19 vaccine frontrunners and their nanotechnology design. ACS Nano. 2020;14:12522–12537. doi: 10.1021/acsnano.0c07197. [DOI] [PubMed] [Google Scholar]
- 27.Pegu A., et al. Durability of mRNA-1273 vaccine-induced antibodies against SARS-CoV-2 variants. Science. 2021;373:1372–1377. doi: 10.1126/science.abj4176. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Sahin U., et al. BNT162b2 vaccine induces neutralizing antibodies and poly-specific T cells in humans. Nature. 2021;595:572–577. doi: 10.1038/s41586-021-03653-6. [DOI] [PubMed] [Google Scholar]
- 29.Trougakos I.P., et al. Comparative kinetics of SARS-CoV-2 anti-spike protein RBD IgGs and neutralizing antibodies in convalescent and naïve recipients of the BNT162b2 mRNA vaccine versus COVID-19 patients. BMC Med. 2021;19:208. doi: 10.1186/s12916-021-02090-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Gagne M., et al. Protection from SARS-CoV-2 Delta one year after mRNA-1273 vaccination in rhesus macaques coincides with anamnestic antibody response in the lung. Cell. 2022;185:113–130. doi: 10.1016/j.cell.2021.12.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Barda N., et al. Safety of the BNT162b2 mRNA Covid-19 vaccine in a nationwide setting. N. Engl. J. Med. 2021;385:1078–1090. doi: 10.1056/NEJMoa2110475. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.García-Grimshaw M., et al. Neurologic adverse events among 704,003 first-dose recipients of the BNT162b2 mRNA COVID-19 vaccine in Mexico: a nationwide descriptive study. Clin. Immunol. 2021;229 doi: 10.1016/j.clim.2021.108786. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Klein N.P., et al. Surveillance for adverse events after COVID-19 mRNA vaccination. JAMA. 2021;326:1390–1399. doi: 10.1001/jama.2021.15072. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Patone M., et al. Neurological complications after first dose of COVID-19 vaccines and SARS-CoV-2 infection. Nat. Med. 2021;27:2144–2153. doi: 10.1038/s41591-021-01556-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Li X., et al. Characterizing the incidence of adverse events of special interest for COVID-19 vaccines across eight countries: a multinational network cohort study. BMJ. 2021;373 doi: 10.1136/bmj.n1435. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Oster M.E., et al. Myocarditis cases reported after mRNA-based COVID-19 vaccination in the US From December 2020 to August 2021. JAMA. 2022;327:331–340. doi: 10.1001/jama.2021.24110. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Montgomery J., et al. Myocarditis following immunization with mRNA COVID-19 vaccines in members of the US military. JAMA Cardiol. 2021;6:1202–1206. doi: 10.1001/jamacardio.2021.2833. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Hoeg T., et al. SARS-CoV-2 mRNA vaccination-associated myocarditis in children ages 12–17: a stratified national database analysis. medRxiv. 2021 doi: 10.1101/2021.08.30.21262866. Published online September 8, 2021. [DOI] [Google Scholar]
- 39.Li X., et al. Myocarditis following COVID-19 BNT162b2 vaccination among adolescents in Hong Kong. JAMA Pediatr. 2022 doi: 10.1001/jamapediatrics.2022.0101. Published online February 25, 2022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Verbeke R., et al. Three decades of messenger RNA vaccine development. Nanotoday. 2019;28 [Google Scholar]
- 41.Ndeupen S., et al. The mRNA–LNP platform’s lipid nanoparticle component used in preclinical vaccine studies is highly inflammatory. iScience. 2021;24 doi: 10.1016/j.isci.2021.103479. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Parhiz H., et al. Added to pre-existing inflammation, mRNA–lipid nanoparticles induce inflammation exacerbation (IE) J. Control. Release. 2021;344:50–61. doi: 10.1016/j.jconrel.2021.12.027. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Yang R., et al. A core–shell structured COVID-19 mRNA vaccine with favorable biodistribution pattern and promising immunity. Signal Transduct. Target Ther. 2021;6:213. doi: 10.1038/s41392-021-00634-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Pardi N., et al. Expression kinetics of nucleoside-modified mRNA delivered in lipid nanoparticles to mice by various routes. J. Control. Release. 2015;217:345–351. doi: 10.1016/j.jconrel.2015.08.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Hassett K.J., et al. Optimization of lipid nanoparticles for intramuscular administration of mRNA vaccines. Mol. Ther. Nucleic Acids. 2019;15:1–11. doi: 10.1016/j.omtn.2019.01.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Ogata A.F., et al. Circulating SARS-CoV-2 vaccine antigen detected in the plasma of mRNA-1273 vaccine recipients. Clin. Infect. Dis. 2021;74:715–718. doi: 10.1093/cid/ciab465. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Bansal S., et al. Cutting edge: circulating exosomes with COVID spike protein are induced by BNT162b2 (Pfizer-BioNTech) vaccination prior to development of antibodies: a novel mechanism for immune activation by mRNA vaccines. J. Immunol. 2021;207:2405–2410. doi: 10.4049/jimmunol.2100637. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Cognetti J.S., Miller B.L. Monitoring serum spike protein with disposable photonic biosensors following SARS-CoV-2 vaccination. Sensors (Basel) 2021;21:5827. doi: 10.3390/s21175857. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Goel R.R., et al. mRNA vaccines induce durable immune memory to SARS-CoV-2 and variants of concern. Science. 2021;374 doi: 10.1126/science.abm0829. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Terpos E., et al. Sustained but declining humoral immunity against SARS-CoV-2 at 9 months postvaccination with BNT162b2: a prospective evaluation in 309 healthy individuals. Hemasphere. 2022;6 doi: 10.1097/HS9.0000000000000677. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Watanabe Y., et al. Native-like SARS-CoV-2 spike glycoprotein expressed by ChAdOx1 nCoV-19/AZD1222 vaccine. ACS Cent. Sci. 2021;7:594–602. doi: 10.1021/acscentsci.1c00080. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Li Y., et al. Linear epitope landscape of the SARS-CoV-2 spike protein constructed from 1,051 COVID-19 patients. Cell Rep. 2021;34 doi: 10.1016/j.celrep.2021.108915. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Hwa K.-Y., et al. Peptide mimicrying between SARS coronavirus spike protein and human proteins reacts with SARS patient serum. J. Biomed. Biotechnol. 2008;2008 doi: 10.1155/2008/326464. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Kanduc D., Shoenfeld Y. Molecular mimicry between SARS-CoV-2 spike glycoprotein and mammalian proteomes: implications for the vaccine. Immunol. Res. 2020;68:310–313. doi: 10.1007/s12026-020-09152-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.O’Donoghue S.I., et al. SARS-CoV-2 structural coverage map reveals viral protein assembly, mimicry, and hijacking mechanisms. Mol. Syst. Biol. 2021;17 doi: 10.15252/msb.202010079. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Kowarz E., et al. Vaccine-induced COVID-19 mimicry syndrome. eLife. 2022;11 doi: 10.7554/eLife.74974. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Kreye J., et al. A therapeutic non-self-reactive SARS-CoV-2 antibody protects from lung pathology in a COVID-19 hamster model. Cell. 2020;183:1058–1069. doi: 10.1016/j.cell.2020.09.049. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Freitas R.S., et al. SARS-CoV-2 spike antagonizes innate antiviral immunity by targeting interferon regulatory factor 3. Front. Cell. Infect. Microbiol. 2021;11 doi: 10.3389/fcimb.2021.789462. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Visvabharathy L., et al. Neuro-COVID long-haulers exhibit broad dysfunction in T cell memory generation and responses to vaccination. medRxiv. 2021 doi: 10.1101/2021.08.08.21261763. Published online October 29, 2021. [DOI] [Google Scholar]
- 60.Murphy W.J., Longo D.L. A possible role for anti-idiotype antibodies in SARS-CoV-2 infection and vaccination. N. Engl. J. Med. 2022;386:394–396. doi: 10.1056/NEJMcibr2113694. [DOI] [PubMed] [Google Scholar]
- 61.Zuo Y., et al. Prothrombotic autoantibodies in serum from patients hospitalized with COVID-19. Sci. Transl. Med. 2020;12 doi: 10.1126/scitranslmed.abd3876. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Wang E.Y., et al. Diverse functional autoantibodies in patients with COVID-19. Nature. 2021;595:283–288. doi: 10.1038/s41586-021-03631-y. [DOI] [PubMed] [Google Scholar]
- 63.Arunachalam P.S., et al. Systems vaccinology of the BNT162b2 mRNA vaccine in humans. Nature. 2021;596:410–416. doi: 10.1038/s41586-021-03791-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Terpos E., et al. Third dose of the BNT162b2 vaccine results in very high levels of neutralizing antibodies against SARS-CoV-2: results of a prospective study in 150 health professionals in Greece. Am. J. Hematol. 2022;97:E147–E150. doi: 10.1002/ajh.26468. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Wheatley A.K., et al. Immune imprinting and SARS-CoV-2 vaccine design. Trends Immunol. 2021;42:956–959. doi: 10.1016/j.it.2021.09.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Röltgen K. Immune imprinting, breadth of variant recognition and germinal center response in human SARS-CoV-2 infection and vaccination. Cell. 2022;185:1025–1040. doi: 10.1016/j.cell.2022.01.018. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Deshotels M.R., et al. Angiotensin II mediates angiotensin converting enzyme type 2 internalization and degradation through an angiotensin II type I receptor-dependent mechanism. Hypertension. 2014;64:1368–1375. doi: 10.1161/HYPERTENSIONAHA.114.03743. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Ramos S.G., et al. ACE2 Down-regulation may act as a transient molecular disease causing RAAS dysregulation and tissue damage in the microcirculatory environment among COVID-19 patients. Am. J. Pathol. 2021;191:1154–1164. doi: 10.1016/j.ajpath.2021.04.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Yeung M.L., et al. Soluble ACE2-mediated cell entry of SARS-CoV-2 via interaction with proteins related to the renin–angiotensin system. Cell. 2021;184:2212–2228. doi: 10.1016/j.cell.2021.02.053. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Ferrario C.M., et al. Effect of angiotensin-converting enzyme inhibition and angiotensin II receptor blockers on cardiac angiotensin-converting enzyme 2. Circulation. 2005;111:2605–2610. doi: 10.1161/CIRCULATIONAHA.104.510461. [DOI] [PubMed] [Google Scholar]
- 71.Yang J., et al. Pathological Ace2-to-Ace enzyme switch in the stressed heart is transcriptionally controlled by the endothelial Brg1-FoxM1 complex. Proc. Natl. Acad. Sci. U. S. A. 2016;113:E5628–E5635. doi: 10.1073/pnas.1525078113. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.McCracken I.R., et al. Lack of evidence of angiotensin-converting enzyme 2 expression and replicative infection by SARS-CoV-2 in human endothelial cells. Circulation. 2021;143:865–868. doi: 10.1161/CIRCULATIONAHA.120.052824. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Nicosia R.F., et al. COVID-19 vasculopathy: mounting evidence for an indirect mechanism of endothelial injury. Am. J. Pathol. 2021;191:1374–1384. doi: 10.1016/j.ajpath.2021.05.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74.Coate K.C., et al. SARS-CoV-2 cell entry factors ACE2 and TMPRSS2 are expressed in the microvasculature and ducts of human pancreas but are not enriched in β cells. Cell Metab. 2020;32:1028–1040. doi: 10.1016/j.cmet.2020.11.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Nuovo G.J., et al. Endothelial cell damage is the central part of COVID-19 and a mouse model induced by injection of the S1 subunit of the spike protein. Ann. Diagn. Pathol. 2021;51 doi: 10.1016/j.anndiagpath.2020.151682. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Lei Y., et al. SARS-CoV-2 spike protein impairs endothelial function via downregulation of ACE 2. Circ. Res. 2021;128:1323–1326. doi: 10.1161/CIRCRESAHA.121.318902. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Raghavan S., et al. SARS-CoV-2 spike protein induces degradation of junctional proteins that maintain endothelial barrier integrity. Front Cardiovasc. Med. 2021;8 doi: 10.3389/fcvm.2021.687783. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Colunga Biancatelli R.M.L., et al. The SARS-CoV-2 spike protein subunit S1 induces COVID-19-like acute lung injury in Κ18-hACE2 transgenic mice and barrier dysfunction in human endothelial cells. Am. J. Physiol. Lung Cell Mol. Physiol. 2021;321:L477–L484. doi: 10.1152/ajplung.00223.2021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Avolio E., et al. The SARS-CoV-2 spike protein disrupts human cardiac pericytes function through CD147 receptor-mediated signalling: a potential non-infective mechanism of COVID-19 microvascular disease. Clin. Sci. (Lond.) 2021;135:2667–2689. doi: 10.1042/CS20210735. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Panigrahi S., et al. SARS-CoV-2 spike protein destabilizes microvascular homeostasis. Microbiol. Spectr. 2021;9 doi: 10.1128/Spectrum.00735-21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Clausen T.M., et al. SARS-CoV-2 infection depends on cellular heparan sulfate and ACE2. Cell. 2020;183:1043–1057. doi: 10.1016/j.cell.2020.09.033. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 82.Partridge L.J., et al. ACE2-independent interaction of SARS-CoV-2 spike protein with human epithelial cells is inhibited by unfractionated heparin. Cells. 2021;10:1419. doi: 10.3390/cells10061419. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Zheng Y., et al. SARS-CoV-2 spike protein causes blood coagulation and thrombosis by competitive binding to heparan sulfate. Int. J. Biol. Macromol. 2021;193:1124–1129. doi: 10.1016/j.ijbiomac.2021.10.112. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84.Zhang S., et al. SARS-CoV-2 binds platelet ACE2 to enhance thrombosis in COVID-19. J. Hematol. Oncol. 2020;13:120. doi: 10.1186/s13045-020-00954-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85.Jana S., et al. Cell-free hemoglobin does not attenuate the effects of SARS-CoV-2 spike protein S1 subunit in pulmonary endothelial cells. Int. J. Mol. Sci. 2021;22:9041. doi: 10.3390/ijms22169041. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 86.Ryu J.K., et al. SARS-CoV-2 spike protein induces abnormal inflammatory blood clots neutralized by fibrin immunotherapy. bioRxiv. 2021 doi: 10.1101/2021.10.12.464152. Published online October 13, 2021. [DOI] [Google Scholar]
- 87.Terpos E., et al. High prevalence of anti-PF4 antibodies following ChAdOx1 nCov-19 (AZD1222) vaccination even in the absence of thrombotic events. Vaccines. 2021;9:712. doi: 10.3390/vaccines9070712. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 88.Cattin-Ortolá J., et al. Sequences in the cytoplasmic tail of SARS-CoV-2 spike facilitate expression at the cell surface and syncytia formation. Nat. Commun. 2021;12:5333. doi: 10.1038/s41467-021-25589-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 89.Rajah M.M., et al. SARS-CoV-2 Alpha, Beta, and Delta variants display enhanced spike-mediated syncytia formation. EMBO J. 2021;40 doi: 10.15252/embj.2021108944. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Cheng Y.-W., et al. D614G substitution of SARS-CoV-2 spike protein increases syncytium formation and virus titer via enhanced furin-mediated spike cleavage. mBio. 2021;12 doi: 10.1128/mBio.00587-21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 91.Correa Y., et al. SARS-CoV-2 spike protein removes lipids from model membranes and interferes with the capacity of high-density lipoprotein to exchange lipids. J. Colloid Interface Sci. 2021;602:732–739. doi: 10.1016/j.jcis.2021.06.056. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 92.Jiang H., Mei Y.-F. SARS-CoV-2 spike impairs DNA damage repair and inhibits V(D)J recombination in vitro. Viruses. 2021;13:2056. doi: 10.3390/v13102056. [DOI] [PMC free article] [PubMed] [Google Scholar] [Retracted]
- 93.Lai Y.-J., et al. Epithelial–mesenchymal transition induced by SARS-CoV-2 required transcriptional upregulation of Snail. Am. J. Cancer Res. 2021;11:2278–2290. [PMC free article] [PubMed] [Google Scholar]
- 94.Hsu J.T.-A., et al. The effects of Aβ(1–42) binding to the SARS-CoV-2 spike protein S1 subunit and angiotensin-converting enzyme 2. Int. J. Mol. Sci. 2021;22:8226. doi: 10.3390/ijms22158226. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 95.Chen R., et al. The spatial and cell-type distribution of SARS-CoV-2 receptor ACE2 in the human and mouse brains. Front. Neurol. 2020;11 doi: 10.3389/fneur.2020.573095. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 96.Rhea E.M., et al. The S1 protein of SARS-CoV-2 crosses the blood–brain barrier in mice. Nat. Neurosci. 2021;24:368–378. doi: 10.1038/s41593-020-00771-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 97.DeOre B.J., et al. SARS-CoV-2 spike protein disrupts blood–brain barrier integrity via RhoA activation. J. NeuroImmune Pharmacol. 2021;16:722–728. doi: 10.1007/s11481-021-10029-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 98.Welch J.L., et al. T-cell expression of angiotensin-converting enzyme 2 and binding of severe acute respiratory coronavirus 2. J. Infect. Dis. 2022;225:810–819. doi: 10.1093/infdis/jiab595. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 99.Barreda D., et al. SARS-CoV-2 spike protein and its receptor binding domain promote a proinflammatory activation profile on human dendritic cells. Cells. 2021;10:3279. doi: 10.3390/cells10123279. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 100.Maldonado M.D., Romero-Aibar J. The Pfizer-BNT162b2 mRNA-based vaccine against SARS-CoV-2 may be responsible for awakening the latency of herpes varicella-zoster virus. Brain Behav. Immun. Health. 2021;18 doi: 10.1016/j.bbih.2021.100381. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 101.Psichogiou M., et al. Reactivation of varicella zoster virus after vaccination for SARS-CoV-2. Vaccines. 2021;9:572. doi: 10.3390/vaccines9060572. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 102.Kim E.S., et al. Spike proteins of SARS-CoV-2 induce pathological changes in molecular delivery and metabolic function in the brain endothelial cells. Viruses. 2021;13:2021. doi: 10.3390/v13102021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 103.Kumar N., et al. SARS-CoV-2 spike protein S1-mediated endothelial injury and pro-inflammatory state is amplified by dihydrotestosterone and prevented by mineralocorticoid antagonism. Viruses. 2021;13:2209. doi: 10.3390/v13112209. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 104.Rahman M., et al. Differential effect of SARS-CoV-2 spike glycoprotein 1 on human bronchial and alveolar lung mucosa models: implications for pathogenicity. Viruses. 2021;13:2537. doi: 10.3390/v13122537. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 105.Li F., et al. SARS-CoV-2 spike promotes inflammation and apoptosis through autophagy by ROS-suppressed PI3K/AKT/mTOR signaling. Biochim. Biophys. Acta Mol. basis Dis. 2021;1867 doi: 10.1016/j.bbadis.2021.166260. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 106.Meyer K., et al. SARS-CoV-2 spike protein induces paracrine senescence and leukocyte adhesion in endothelial cells. J. Virol. 2021;95 doi: 10.1128/JVI.00794-21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 107.Zhu G., et al. SARS-CoV-2 spike protein-induced host inflammatory response signature in human corneal epithelial cells. Mol. Med. Rep. 2021;24:584. doi: 10.3892/mmr.2021.12223. [DOI] [PubMed] [Google Scholar]
- 108.Ntouros P.A., et al. Effective DNA damage response after acute but not chronic immune challenge: SARS-CoV-2 vaccine versus systemic lupus erythematosus. Clin. Immunol. 2021;229 doi: 10.1016/j.clim.2021.108765. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 109.Petruk G., et al. SARS-CoV-2 spike protein binds to bacterial lipopolysaccharide and boosts proinflammatory activity. J. Mol. Cell Biol. 2020;12:916–932. doi: 10.1093/jmcb/mjaa067. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 110.Tumpara S., et al. Boosted pro-inflammatory activity in human PBMCs by LIPOPOLYSACCHARIDE and SARS-CoV-2 spike protein is regulated by α-1 antitrypsin. Int. J. Mol. Sci. 2021;22:7941. doi: 10.3390/ijms22157941. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 111.Olajide O.A., et al. SARS-CoV-2 spike glycoprotein S1 induces neuroinflammation in BV-2 microglia. Mol. Neurobiol. 2022;59:445–458. doi: 10.1007/s12035-021-02593-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 112.Moutal A., et al. SARS-CoV-2 spike protein co-opts VEGF-A/neuropilin-1 receptor signaling to induce analgesia. Pain. 2021;162:243–252. doi: 10.1097/j.pain.0000000000002097. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 113.Khan S., et al. SARS-CoV-2 spike protein induces inflammation via TLR2-dependent activation of the NF-κB pathway. eLife. 2021;10 doi: 10.7554/eLife.68563. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 114.Cheng M.H., et al. Superantigenic character of an insert unique to SARS-CoV-2 spike supported by skewed TCR repertoire in patients with hyperinflammation. Proc. Natl. Acad. Sci. U. S. A. 2020;117:25254–25262. doi: 10.1073/pnas.2010722117. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 115.Cao X., et al. Spike protein of SARS-CoV-2 activates macrophages and contributes to induction of acute lung inflammation in male mice. FASEB J. 2021;35 doi: 10.1096/fj.202002742RR. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 116.Frank M.G., et al. SARS-CoV-2 spike S1 subunit induces neuroinflammatory, microglial and behavioral sickness responses: evidence of PAMP-like properties. Brain Behav. Immun. 2022;100:267–277. doi: 10.1016/j.bbi.2021.12.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 117.Bergamaschi C., et al. Systemic IL-15, IFN-γ, and IP-10/CXCL10 signature associated with effective immune response to SARS-CoV-2 in BNT162b2 mRNA vaccine recipients. Cell Rep. 2021;36 doi: 10.1016/j.celrep.2021.109504. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 118.Au L., et al. Cytokine release syndrome in a patient with colorectal cancer after vaccination with BNT162b2. Nat. Med. 2021;27:1362–1366. doi: 10.1038/s41591-021-01387-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 119.Camell C.D., et al. Senolytics reduce coronavirus-related mortality in old mice. Science. 2021;373 doi: 10.1126/science.abe4832. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 120.Kowalzik F., et al. mRNA-based vaccines. Vaccines. 2021;9:390. doi: 10.3390/vaccines9040390. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 121.Racanelli V., Rehermann B. The liver as an immunological organ. Hepatology. 2006;43:S54–S62. doi: 10.1002/hep.21060. [DOI] [PubMed] [Google Scholar]
- 122.Horst A.K., et al. Modulation of liver tolerance by conventional and nonconventional antigen-presenting cells and regulatory immune cells. Cell. Mol. Immunol. 2016;13:277–292. doi: 10.1038/cmi.2015.112. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 123.Avci E., Abasiyanik F. Autoimmune hepatitis after SARS-CoV-2 vaccine: new-onset or flare-up? J. Autoimmun. 2021;125 doi: 10.1016/j.jaut.2021.102745. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 124.Zin Tun G.S., et al. Immune-mediated hepatitis with the Moderna vaccine, no longer a coincidence but confirmed. J. Hepatol. 2021;76:747–749. doi: 10.1016/j.jhep.2021.09.031. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 125.Harryvan T.J., et al. The ABCs of antigen presentation by stromal non-professional antigen-presenting cells. Int. J. Mol. Sci. 2021;23:137. doi: 10.3390/ijms23010137. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 126.Carnell G.W., et al. SARS-CoV-2 spike protein stabilized in the closed state induces potent neutralizing responses. J. Virol. 2021;95 doi: 10.1128/JVI.00203-21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 127.Hoffmann M., et al. SARS-CoV-2 cell entry depends on ACE2 and TMPRSS2 and is blocked by a clinically proven protease inhibitor. Cell. 2020;181:271–280. doi: 10.1016/j.cell.2020.02.052. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 128.Lan J., et al. Structure of the SARS-CoV-2 spike receptor-binding domain bound to the ACE2 receptor. Nature. 2020;581:215–220. doi: 10.1038/s41586-020-2180-5. [DOI] [PubMed] [Google Scholar]
- 129.Piroth L., et al. Comparison of the characteristics, morbidity, and mortality of COVID-19 and seasonal influenza: a nationwide, population-based retrospective cohort study. Lancet Respir. Med. 2021;9:251–259. doi: 10.1016/S2213-2600(20)30527-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 130.Castagnoli R., et al. Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection in children and adolescents: a systematic review. JAMA Pediatr. 2020;174:882–889. doi: 10.1001/jamapediatrics.2020.1467. [DOI] [PubMed] [Google Scholar]
- 131.Goldstein E., et al. On the effect of age on the transmission of SARS-CoV-2 in households, schools, and the community. J. Infect. Dis. 2021;223:362–369. doi: 10.1093/infdis/jiaa691. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 132.Yoshida M., et al. Local and systemic responses to SARS-CoV-2 infection in children and adults. Nature. 2022;602:321–327. doi: 10.1038/s41586-021-04345-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 133.Killingley B., et al. Safety, tolerability and viral kinetics during SARS-CoV-2 human challenge in young adults. Nat Med. 2022 doi: 10.1038/s41591-022-01780-9. Published online March 31, 2022. [DOI] [PubMed] [Google Scholar]
- 134.Zhang J.-Y., et al. Single-cell landscape of immunological responses in patients with COVID-19. Nat. Immunol. 2020;21:1107–1118. doi: 10.1038/s41590-020-0762-x. [DOI] [PubMed] [Google Scholar]
- 135.Low J.S., et al. Clonal analysis of immunodominance and cross-reactivity of the CD4 T cell response to SARS-CoV-2. Science. 2021;372:1336–1341. doi: 10.1126/science.abg8985. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 136.Cagigi A., et al. Airway antibodies emerge according to COVID-19 severity and wane rapidly but reappear after SARS-CoV-2 vaccination. JCI Insight. 2021;6 doi: 10.1172/jci.insight.151463. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 137.Loske J., et al. Pre-activated antiviral innate immunity in the upper airways controls early SARS-CoV-2 infection in children. Nat. Biotechnol. 2021;40:319–324. doi: 10.1038/s41587-021-01037-9. [DOI] [PubMed] [Google Scholar]
- 138.See I., et al. US case reports of cerebral venous sinus thrombosis with thrombocytopenia after Ad26.COV2.S vaccination, March 2 to April 21, 2021. JAMA. 2021;325:2448–2456. doi: 10.1001/jama.2021.7517. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 139.Reimer J.M., et al. Matrix-MTM adjuvant induces local recruitment, activation and maturation of central immune cells in absence of antigen. PLoS One. 2012;7 doi: 10.1371/journal.pone.0041451. [DOI] [PMC free article] [PubMed] [Google Scholar]