Abstract
Background
In 1971, the National Cancer Act created a process to recognize the leadership, facilities, and research efforts at cancer centers throughout the United States. Toward this goal, each National Cancer Institute (NCI)-designated Cancer Center defines and describes a catchment area to which they tailor specific scientific and community engagement activities.
Methods
The geographically defined catchment areas of 63 NCI-designated comprehensive and clinical Cancer Centers are collated and presented visually. Additionally, the NCI-designated Cancer Centers catchment areas are geographically linked with publicly available data sources to aggregate sociodemographic and epidemiologic characteristics across the NCI Cancer Centers Program.
Results
The national map portrays the size, shape, and locations for 63 catchment areas of the 71 NCI-designated Cancer Centers. The findings illustrate the geographic extent of the NCI Cancer Centers Program during the 50th anniversary of the National Cancer Act.
Conclusions
NCI-designated Cancer Centers occupy a prominent role in the cancer control ecosystem and continue to perform research to address the burden of cancer among their local communities. The strength of the NCI Cancer Centers Program is partly defined by the scope, quality, and impact of community outreach and engagement activities in the catchment areas.
Impact
The collation and geographic presentation of the distinct, but complementary, NCI-designated Cancer Center catchment areas are intended to support future research and community outreach activities among NCI-designated Cancer Centers.
Keywords: National Cancer Institute, Cancer Centers, catchment area, geography, GIS
1. Introduction
Fifty years ago, the National Cancer Act (NCA) established a flagship program for “cancer research and demonstration centers” to be administered by the National Cancer Institute (NCI) (1). Through a competitive application process, the NCI Cancer Centers Program – now representing 71 basic, clinical, and comprehensive Cancer Centers – remains a central part of the cancer research, education, and oncology care enterprise in the United States (U.S.).
In 2012, NCI published a revised funding opportunity announcement for the P30 Cancer Center Support Grant (CCSG) that contained guidance for defining the Cancer Center’s geographic catchment area (2), which has been sustained through subsequent reissuances of the P30 CCSG funding opportunity (3). Initially, the concept of understanding the geographic footprint of areas served by the NCI-designated Cancer Centers stemmed from conversations among state and national partners, including NCI and the Centers for Disease Control and Prevention, about how to best coordinate cancer prevention and control efforts across the U.S. Holistically, the catchment area definition provides a geographic scope for monitoring cancer trends, identifying pronounced socioeconomic- and health-related disparities, informing high impact translational science, and guiding the implementation of evidence-based interventions in clinical and community settings (2,4). Understanding local sociodemographic and epidemiologic characteristics allows NCI Cancer Center administrative leaders, researchers and clinicians, and community outreach and engagement staff to focus on issues that are most relevant to their communities (5–7).
The place-based research strategy was supported by additional activities pertaining to the NCI-designated Cancer Centers. In 2016, the NCI Office of Cancer Centers, in collaboration with the Division of Cancer Control and Population Sciences (DCCPS), announced a P30 grant administrative supplement opportunity to support population health assessments among the catchment populations (8). DCCPS funded 29 NCI-designated Cancer Centers to conduct local-area surveys to characterize cancer-relevant knowledge, attitudes, beliefs, and behaviors across the breadth of the catchment area (9). Following this initiative, NCI incorporated the sustainment of local-area assessments into the core CCSG funding mechanism (10). In 2017, the CCSG was revised to include a new Community Outreach and Engagement component, which extended NCI Cancer Centers’ involvement in their respective catchment areas and promoted community input into Center activities (11). In 2019, a stakeholder listening session and community impact forum helped galvanize the paradigm of “research driven by the catchment area of a cancer center” (4,12,13).
Coinciding with the celebration of the 50th anniversary of the NCA, herein, this effort presents a national map of NCI-designated Cancer Center catchment areas, representing 63 actively funded comprehensive and clinical cancer centers. Standardized geographic codes were used to link each catchment area with population-based datasets to visualize social, behavioral, or environmental factors in communities served by NCI-designated Cancer Centers. The purpose of this presentation and data linkage is not to advocate for specific policies or NCI Cancer Centers Program coverage goals, but rather to inform the broader context of cancer research and community engagement efforts across the U.S. The geographic dataset strengthens the ability to communicate clear, consistent evidence on issues that affect catchment area residents. The map can be used, in part, to support cancer control research, program planning for community outreach and engagement, and communication and dissemination activities related to the NCI Cancer Centers Program.
2. Materials and Methods
NCI-designated Cancer Center Catchment Area Definitions
The P30 CCSG asks each applicant to describe their catchment area. With permission from the NCI-designated Cancer Center directors (i.e., principal investigators of the P30 CCSG awards), the catchment area definitions were collected from grants that were funded during the most recent application cycle in fiscal years 2016–2021. In May 2021, NCI staff asked NCI-designated Cancer Center directors to report any catchment area updates or changes that occurred after the most recent competitive resubmission.
NCI-designated Cancer Centers are typically affiliated with academic medical centers and research institutions located in large cities, with catchment areas extending to surrounding communities. NCI-designated Cancer Centers define their catchment area boundaries by U.S. state, county, zip code tabulation areas (ZCTAs), public use microdata areas (PUMAs), or other geographic landmarks (e.g., U.S.-affiliated Pacific Islands [U.S.-API]) (Supplemental Table 1). The corresponding shapefiles for the state, county, ZCTA, or PUMA boundaries were retrieved from the 2018 U.S. Census Bureau Topologically Integrated Geographic Encoding and Referencing (TIGER)/Line database (14). Each catchment area was then assembled into a separate, unique shapefile. The total surface area (square miles) of each catchment area was calculated by summing the geographic area within the included boundaries.
NCI-designated Cancer Center Catchment Area Linkages
Geographic Information System tools and R software were used to link geographic locations with publicly available datasets. Federal Information Processing Standard (FIPS) codes for each catchment area and the tidycensus package were used to retrieve sociodemographic data from the 2015–2019 American Community Survey (15,16). If the NCI-designated Cancer Center used PUMA or ZCTA boundaries, the corresponding FIPS codes for all counties within the defined catchment area, including all partial counties, were selected. This study reports total population estimates and four demographic characteristics (sex, age, race, and ethnicity) because they correspond with federal reporting guidelines (17,18). Specifically, descriptive statistics of the catchment populations, such as percent female, percent greater than 65 years old, and percent per race and ethnicity are presented herein. In addition, SEER*Stat software (version 8.3.9) was used to link cancer mortality data from the National Center for Health Statistics, available through the NCI Surveillance, Epidemiology, and End Results (SEER) program (19,20). Variables were selected that align with Healthy People 2030 objectives – a federal public health initiative to improve health and well-being over the next decade (21). Specifically, the 2015–2019 age-adjusted overall cancer mortality rates and site-specific mortality rates for lung, breast (female), prostate, and colorectal cancers are presented herein.
The seven NCI-designated basic laboratory centers were excluded for this mapping exercise because they are not required to identify a catchment area. St. Jude Children’s Research Hospital was also excluded because its unique mission is solely devoted to pediatric cancers. The NCI-designated University of Hawaii Cancer Center catchment area includes the U.S.-API; however, the U.S.-API was not included in the descriptive analysis due to data reporting limitations of the U.S. Census demographic characteristics and National Vital Statistics System cancer mortality data. Instead, statistics for the NCI-designated University of Hawaii Cancer Center catchment population were reported using the state of Hawaii only.
NCI-designated Cancer Center Catchment Area Visualization
For each of the included NCI-designated Cancer Centers, the point-location was geocoded based on textual name matching of the center’s address in Google Earth Pro (version 7.3.3.7699). The statistical software R (version 4.1.0) was used to visualize the NCI-designated Cancer Centers and their catchment areas (22). The tigris package (15) was used to obtain the U.S. Census TIGER/Line files, the sf package to collate the geographic information (23), and the ggplot2 package to render the map (24). R code used to generate the geographic visualizations has been deposited in a repository on GitHub (https://github.com/idblr/NCI_Cancer_Center_Catchment_Areas).
Data Availability Statement
The data generated in this study are available within the article and its supplementary data files. Demographic data analyzed in this study were obtained from the 2015–2019 American Community Survey 5-Year Estimates, available from the U.S. Census Bureau (16). Epidemiologic data analyzed in this study were obtained from National Center for Health Statistics 5-year data (2015–2019), available through the NCI SEER program (19).
3. Results
The 63 NCI-designated Cancer Center catchment areas touch 43 states, the District of Columbia, and the U.S.-API (Figure 1). Catchment areas are bound by state borders (n=24), county borders (n=38), ZCTA boundaries (n=1), PUMA boundaries (n=1), or other geographic landmarks (n=1). Multiple NCI-designated Cancer Centers are located in areas with large populaces such as New York, New York (Supplemental Figure 1), the Delaware Valley (Supplemental Figure 2), and southern California (Supplemental Figure 3), which are presented as exemplars in the Supplementary Materials.
Figure 1.
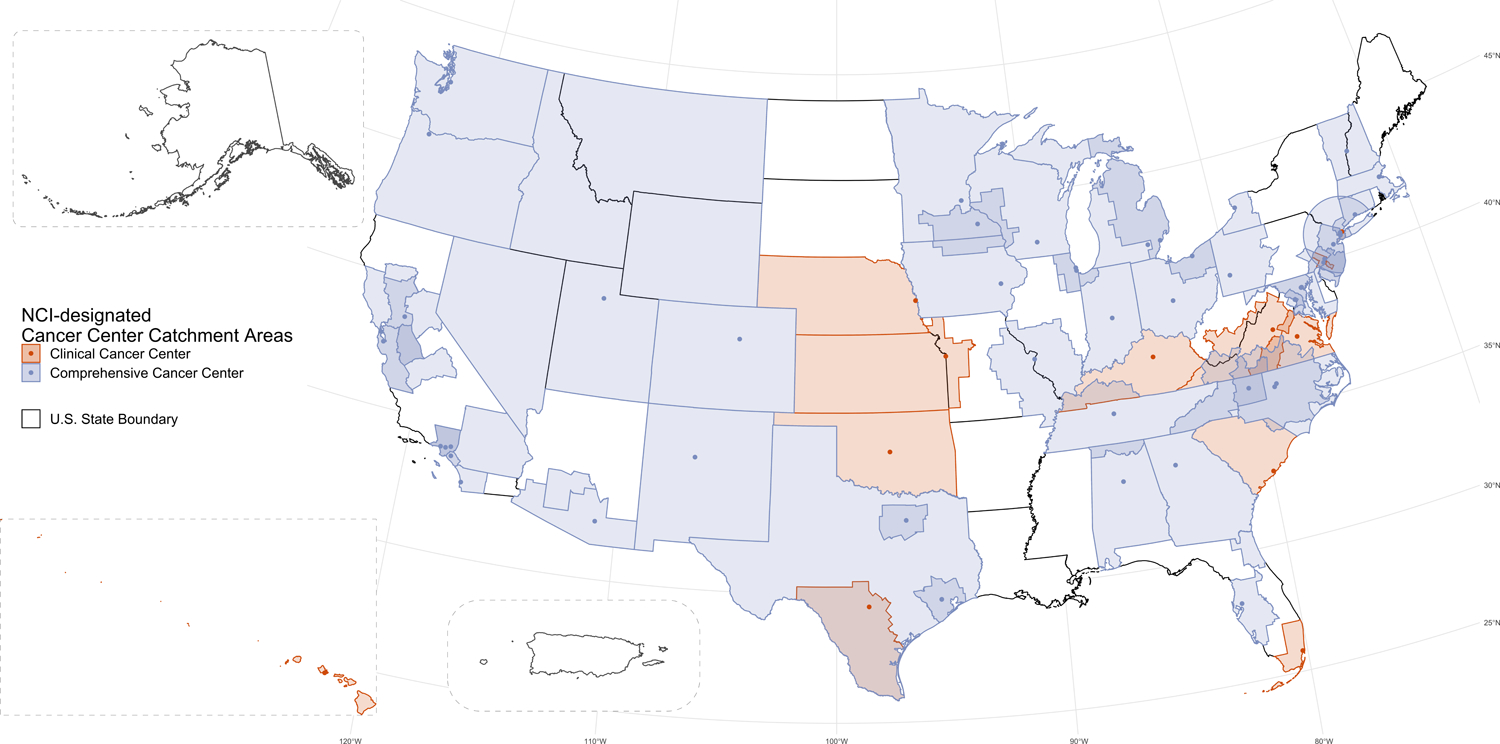
Visualization of the catchment areas for clinical (orange) and comprehensive (blue) NCI-designated Cancer Centers. Points represent NCI-designated Cancer Center locations. NCI-designated Basic and Pediatric Cancer Centers are not shown. Alaska, Hawaii, and Puerto Rico are not to scale.
There are various catchment area sizes; some catchment areas are smaller than a single county while others exceed 200 counties. In total, the analyzed NCI-designated Cancer Center catchment area encompasses approximately 2.4 million square miles. As illustrated in Figure 2, over 77% of U.S. counties have at least one NCI-designated Cancer Center catchment area assignation (n=2,069), and 13% of U.S. counties appear in two or more NCI-designated Cancer Center catchment areas (n=409). Together, the combined catchment areas account for 285 million residents, which represents nearly 88% of the U.S. population (Figure 3). As presented in Figure 4, the catchment areas have a median population of 6.0 million residents (range: 1.4 million to 32.6 million residents) and a median area of 26,500 square miles (range: 48 to 524,000 square miles).
Figure 2.
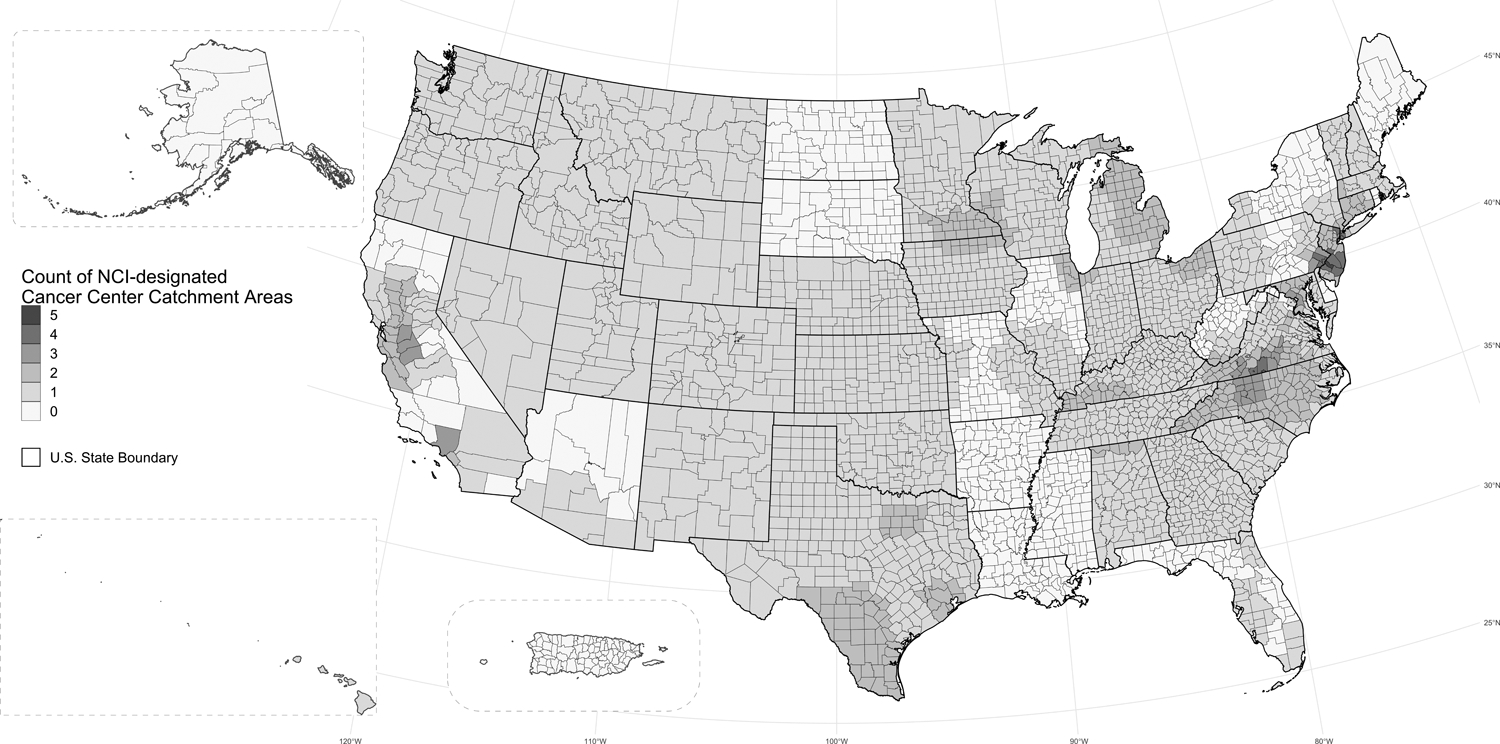
Visualization of the number of NCI-designated Cancer Center catchment areas ascribed to each U.S. county. Darker shades of color signify a higher count of NCI-designated Cancer Centers that consider a county within their catchment area. NCI-designated Basic and Pediatric Cancer Centers are excluded. Alaska, Hawaii, and Puerto Rico are not to scale.
Figure 3.
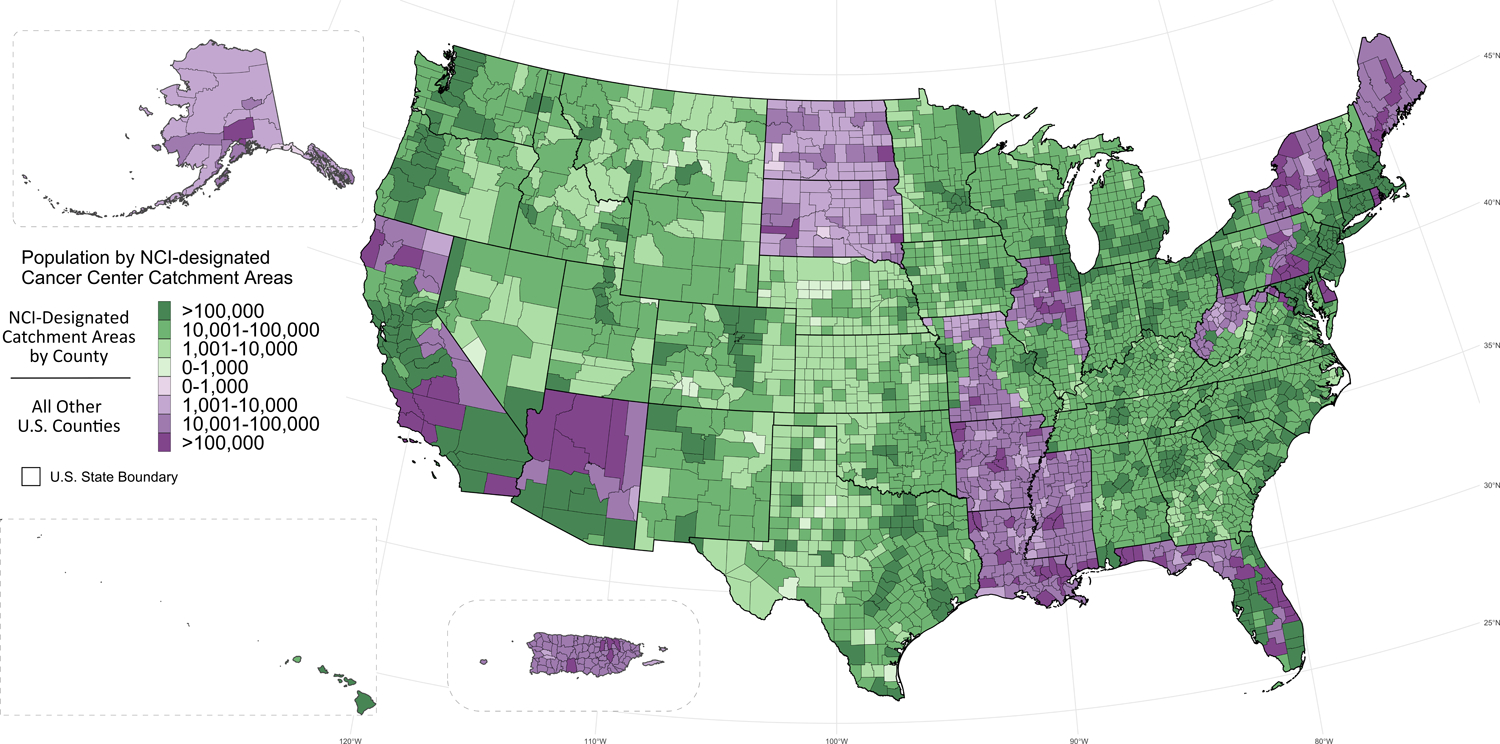
Visualization of the combined NCI-designated Cancer Center catchment areas relative to the U.S. population by county. Underlying data are from the American Community Survey (2015–2019). Green colors signify a county is considered in one or more NCI-designated Cancer Center catchment area definition. Purple colors signify a county that is not considered in at least one NCI-designated Cancer Center catchment area definition. Darker shades of color signify larger populations within a county. NCI-designated Basic and Pediatric Cancer Centers are excluded. Alaska, Hawaii, and Puerto Rico are not to scale.
Figure 4.
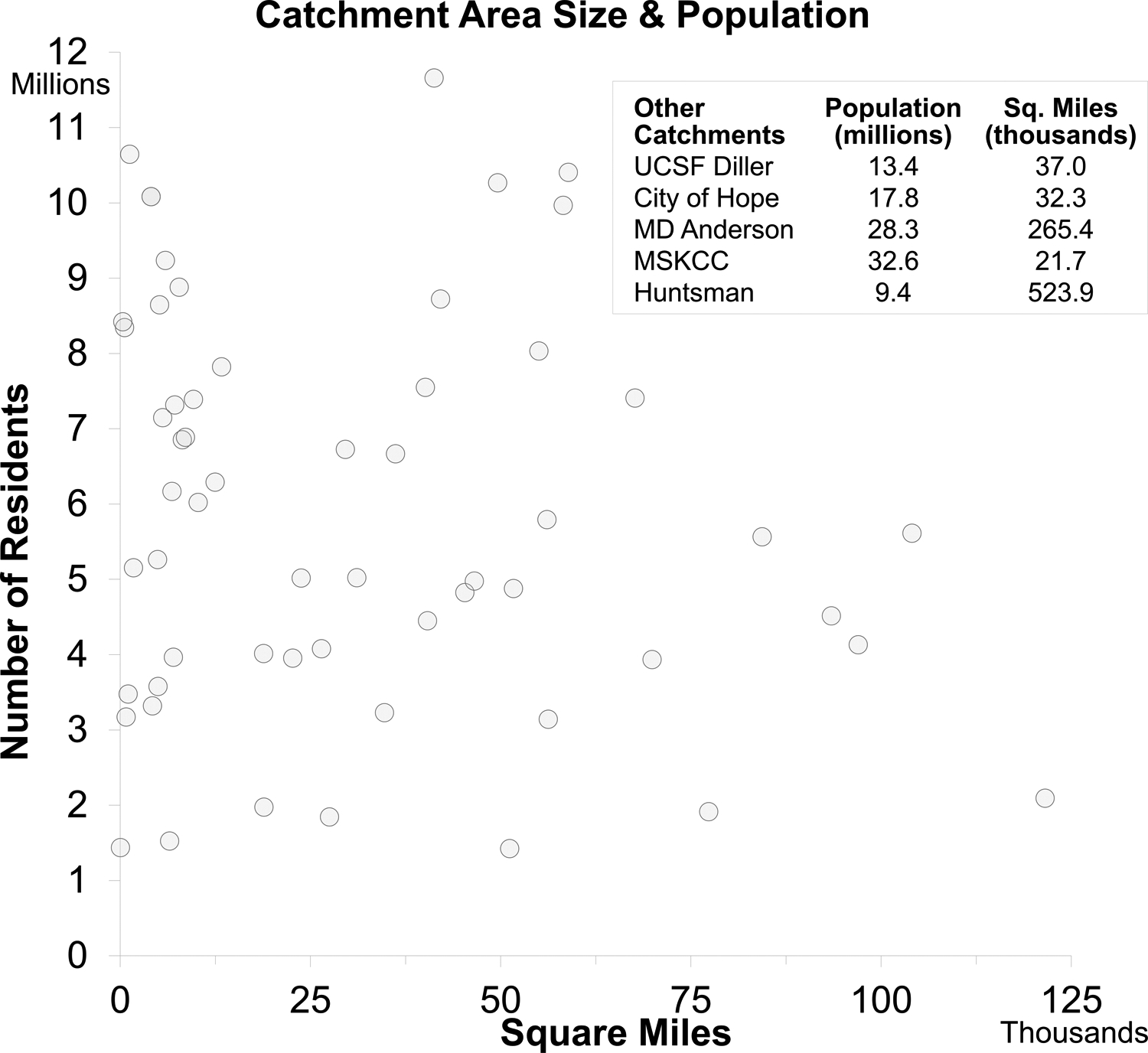
Scatterplot of U.S. population and land area within each NCI-designated Cancer Center catchment area. Underlying data are from the American Community Survey (2015–2019). UCSF Diller: UCSF Helen Diller Family Comprehensive Cancer Center; City of Hope: City of Hope Comprehensive Cancer Center; MD Anderson: The University of Texas MD Anderson Cancer Center; MSKCC: Memorial Sloan-Kettering Cancer Center; Huntsman: Huntsman Cancer Institute at the University of Utah.
In characterizing the demographic attributes of each catchment area population (Figure 5A), the 63 reported NCI-designated Cancer Center catchment areas reflect the U.S. population on the basis of sex, age, race, and ethnicity. The 2015–2019 total U.S. population estimate falls within the range of the catchment area values for each attribute. Also, geographic variations in these characteristics reflect the spatial differences within the total U.S. population. For example, the proportion of adults over 65 years old varies similarly between catchment areas as it does between states.
Figure 5.
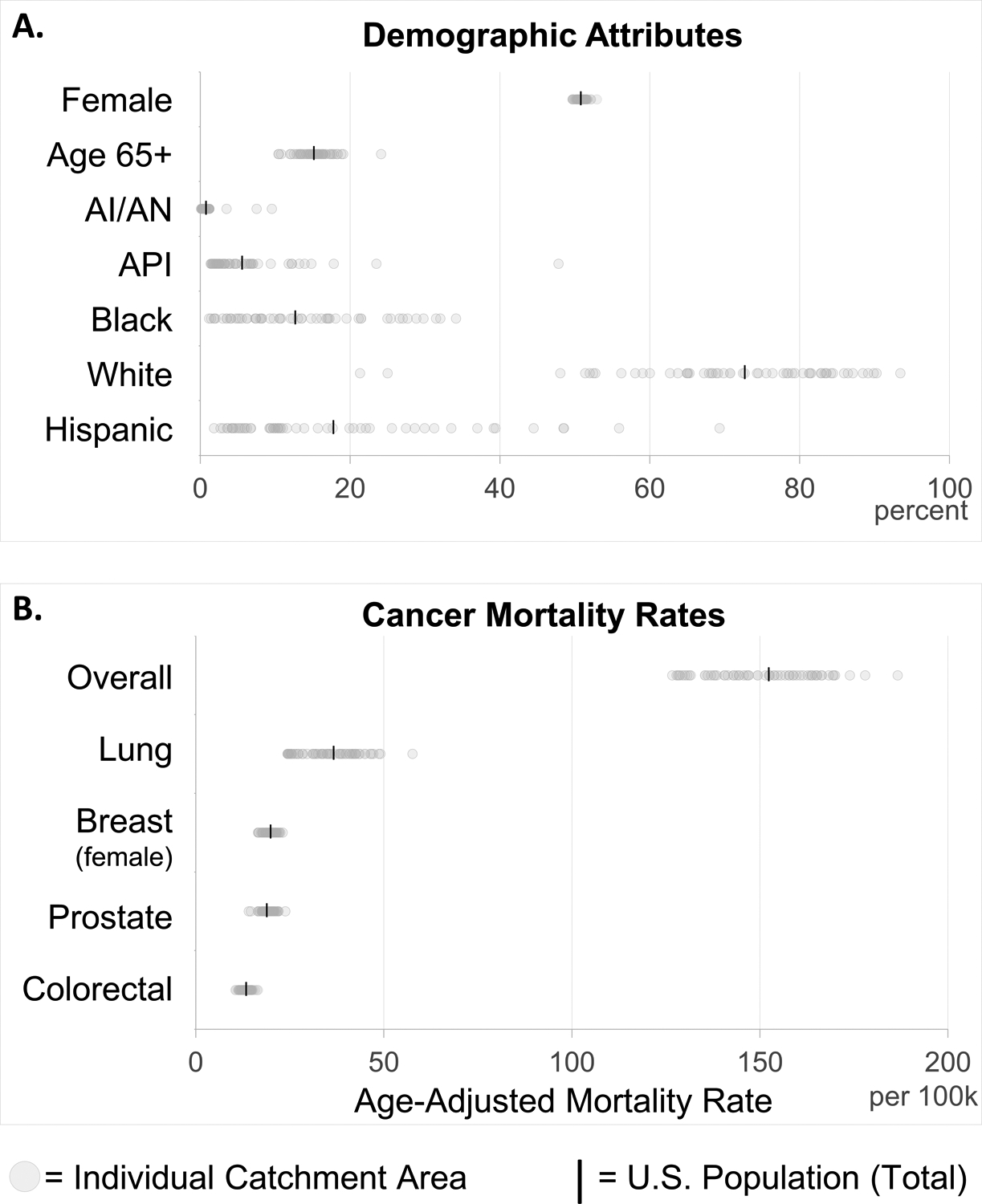
Demographic (A) and epidemiologic (B) characteristics by catchment area (grey circles), compared to the total U.S. estimate (black bar). Underlying data are from the American Community Survey and National Vital Statistics System (2015–2019). AI/AN: American Indian or Alaskan Native; API: Asian or Pacific Islander.
Many factors influence cancer health outcomes, and different parts of the country experience different cancer mortality rates. Figure 5B shows examples of the distribution of age-adjusted cancer mortality (2015–2019) when aggregated by catchment area. In the U.S., the Healthy People 2030 guidelines specify five objectives to address the overall cancer death rate and site-specific mortality rates for lung, breast (female), prostate, and colorectal cancers. In the preceding decade (2010–2019), all the catchment areas exceeded the benchmark for at least one of these objectives, and 56% of the catchment areas met all five objectives. Among the selected cancer sites, lung cancer mortality exhibits the highest variation between catchment area populations, with a range of 24.4 to 57.6 deaths per 100,000 residents (2015–2019).
4. Discussion
NCI-designated Cancer Centers are an important element of the U.S. cancer control ecosystem. They are expected to collaborate with local, state, and regional partners to identify and address cancer disparities, work with researchers and clinicians on high-impact science and delivery of cancer care, and deploy evidence-based strategies for cancer control. For the first time, the present effort compiled a national map that offers a convenient, precise, and easily accessible portrait of the size, shape, and locations for 63 catchment areas of the 71 NCI-designated Cancer Centers.
This effort also demonstrated how to geographically link publicly available datasets to the catchment map, which enables the exploration of sociodemographic attributes, epidemiologic trends, and other systemic factors, such as the distribution healthcare services or exposure to environmental risk factors, to document the burden of cancer in NCI-designated Cancer Center communities and across the NCI Cancer Centers Program. The guidelines for NCI-designation emphasize the importance of research pertaining to the catchment area, which stems from a recognition that community engagement enhances all aspects of the translational research process and ultimately strengthens the benefit to the public. The catchment map may help communicate the priorities and commitments that guide clinical care and community outreach activities of each NCI-designated Cancer Center. For example, catchment area information can help ensure that accrual to cancer clinical trials reflects the local populations, thus allowing researchers to detect and respond to clinical preferences or molecular variations that affect different patient groups (25–27).
Timely and actionable information gleaned from catchment areas analyses can inform efforts to ensure that all segments of the population benefit from scientific advances in cancer prevention, early detection, treatment, and survivorship care. These advantages were demonstrated in outcomes from 29 population health assessments conducted as part of the P30 CCSG administrative supplement opportunity described earlier (8,9,28,29). In these studies, researchers used catchment area information to inform and improve programs for tobacco control (30,31), cancer screening (32–35), sun safety (36,37), risk assessment (38,39), and other health behaviors (40–42).
The description of the NCI-designated Cancer Center catchment areas raises several important considerations. First, this paper and related visualization efforts are not policy statements and should not be interpreted as such. Future reviewers of CCSG applications should note that the NCI does not prescribe catchment area boundaries, beyond that it is a geographic determination that includes the immediate area of the NCI-designated Cancer Center and the area from which the NCI-designated Cancer Center draws the majority of its patients (3). NCI-designated Cancer Centers define for themselves the most appropriate way to situate their unique organizational, research, and community outreach capabilities. There are myriad ways that an NCI-designated Cancer Center can be positioned in the catchment area, and one size does not fit all. Second, this study focuses on 63 NCI-designated comprehensive and clinical Cancer Centers and does not include the valuable contributions of other academic medical centers or community oncology programs. For example, a recent study from the Association of American Cancer Institutes (AACI) reported the catchment areas for 103 AACI-affiliated Cancer Centers (43). Regardless of pursuit or attainment of NCI designation, the collectivity of cancer research and care delivery programs across the U.S. advances the mission of cancer prevention and control, including the promotion of cancer health equity among vulnerable and underrepresented populations. The images presented here are not intended to represent the full extent of all NCI-funded activities, but only one element of the larger cancer research enterprise.
The catchment map has several limitations. First, the map is a snapshot of boundaries that are not permanent. In response to the changing healthcare market, growing cancer patient volume, and community needs, NCI-designated Cancer Centers may shift their catchment area boundaries over time. Second, NCI-designated Cancer Center catchment areas often overlap, especially in the densely populated regions near New York City, Philadelphia, and Los Angeles. Overlapping areas are challenging to visualize in a static image; therefore, NCI is preparing an interactive web application that will allow users to navigate between catchment areas. Lastly, catchment areas do not define the presence or absence of medical or scientific infrastructure, nor do they determine the accessibility or quality of healthcare services. For example, the NCI Community Oncology Research Program (https://ncorp.cancer.gov) expands access to cancer clinical trials to diverse communities within and beyond the NCI-designated catchment areas. It is also important to note that cancer care is not limited to individuals within NCI-designated Cancer Centers’ catchment areas as patients often come from outside these geographic boundaries. Similarly, NCI-designated Cancer Centers are also actively engaged in global health research.
The present study also contains technical limitations that influence the results. First, state- and county-level sources were used for demographic and epidemiologic linkages. Therefore, the population estimates do not perfectly represent the geographic catchment areas that utilize PUMA or ZCTA boundaries. The sources for the presented data linkages do not include attributes for the U.S.-API, and therefore, the entire NCI-designated University of Hawaii Cancer Center catchment population is not presented herein. It is important to document the full extent of each catchment area, and individual NCI-designated Cancer Centers can provide more precise characterizations of their communities than those presented in this study.
As one of the original cornerstones in the NCA of 1971, the NCI-designated Cancer Centers Program continues to contribute to the evolution of more rigorous and ambitious research to improve cancer control in the U.S. Key to this mission, NCI requires designated comprehensive and clinical Cancer Centers to document and address the health issues and priorities that affect residents of their catchment area. Among their many functions, this is one example of how NCI-designated Cancer Centers mobilize their scientific and organizational capabilities in service to their local communities and the Nation.
Supplementary Material
Acknowledgements
The authors thank the NCI Office of Cancer Centers as well as the NCI-designated Cancer Center community for their support of this project. They also thank James Cucinelli and Jeremy Lyman of Information Management Services, Inc. for their technical assistance. I.D. Buller and R.R. Jones are supported by the Intramural Research Program of the National Cancer Institute.
Abbreviations:
- AACI
Association of American Cancer Institutes
- CCSG
cancer center support grant
- FIPS
Federal Information Processing Standard
- NCA
National Cancer Act
- NCI
National Cancer Institute
- PUMA
public use microdata area
- TIGER
Topologically Integrated Geographic Encoding and Referencing
- U.S.
United States
- U.S.-API
United States-affiliated Pacific Islands
- ZCTA
zip code tabulation area
Footnotes
Conflict of Interest Disclosure Statement: The authors declare no potential conflicts of interest.
Publisher's Disclaimer: Disclaimer: The opinions expressed by the authors are their own and this material should not be interpreted as representing the official viewpoint of the U.S. Department of Health and Human Services, the National Institutes of Health, or the National Cancer Institute.
References
- 1.The national cancer act of 1971. J Natl Cancer Inst 1972;48(3):577–84. [PubMed] [Google Scholar]
- 2.Paskett ED, Hiatt RA. Catchment Areas and Community Outreach and Engagement: The New Mandate for NCI-Designated Cancer Centers. Cancer Epidemiology Biomarkers & Prevention 2018;27(5):517–9. [DOI] [PubMed] [Google Scholar]
- 3.NIH Guide for Grants and Contracts [Internet]. Bethesda (MD): U.S. National Institutes of Health; [cited 2021 Dec 16]. Available from: https://grants.nih.gov/grants/guide/pa-files/PAR-21-321.html. FOA Number: PAR-21-321 [Google Scholar]
- 4.Tai CG, Hiatt RA. The Population Burden of Cancer: Research Driven by the Catchment Area of a Cancer Center. Epidemiol Rev 2017;39(1):108–22. [DOI] [PubMed] [Google Scholar]
- 5.Mudaranthakam DP, Harlan-Williams LM, Jensen RA, Kuo H, Garimella V, Chen RC, et al. OPTIK: a database for understanding catchment areas to guide mobilization of cancer center assets. Database (Oxford) 2020;2020:baaa054. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Cunningham SA, Yu R, Shih T, Giordano S, McNeill LH, Rechis R, et al. Cancer-Related Risk Perceptions and Beliefs in Texas: Findings from a 2018 Population-Level Survey. Cancer Epidemiology Biomarkers & Prevention 2019;28(3):486–94. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.2019 Community Health Needs Assessment: A Report to the Community. Fred Hutch & University of Washington Cancer Consortium; 2019. [Google Scholar]
- 8.Blake KD, Ciolino HP, Croyle RT. Population Health Assessment in NCI-Designated Cancer Center Catchment Areas. Cancer Epidemiology Biomarkers & Prevention 2019;28(3):428–30. [DOI] [PubMed] [Google Scholar]
- 9.Gage-Bouchard EA, Rawl SM. Standardizing Measurement of Social and Behavioral Dimensions of Cancer Prevention and Control to Enhance Outreach and Engagement in NCI-Designated Cancer Centers. Cancer Epidemiology Biomarkers & Prevention 2019;28(3):431–4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.NIH Guide for Grants and Contracts [Internet]. Bethesda (MD): U.S. National Institutes of Health; [cited 2021 Aug 16]. Available from: https://grants.nih.gov/grants/guide/pa-files/PAR-20-043.html. FOA Number: PAR-20-043 [Google Scholar]
- 11.NIH Guide for Grants and Contracts [Internet]. Bethesda (MD): U.S. National Institutes of Health; [cited 2021 Aug 16]. Available from: https://grants.nih.gov/grants/guide/pa-files/PAR-17-095.html. FOA Number: PAR-17-095 [Google Scholar]
- 12.Doykos PM, Chen MS Jr., Watson K, Henderson V, Baskin ML, Downer S, et al. Special Convening and Listening Session on Health Equity and Community Outreach and Engagement at National Cancer Institute-Designated Comprehensive Cancer Centers. Health Equity 2021;5(1):84–90. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Doykos PM, Chen MS Jr., Watson K, Henderson V, Baskin ML, Downer S, et al. Recommendations from a Dialogue on Evolving National Cancer Institute-Designated Comprehensive Cancer Center Community Outreach and Engagement Requirements: A Path Forward. Health Equity 2021;5(1):76–83. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Walker K Load Census TIGER/Line Shapefiles. Version 1.5 [software]. 2021 Sept 23 [cited 2021 Aug 16]. Available from: https://CRAN.R-project.org/package=tigris
- 15.Walker K Tidycensus: Load US Census Boundary and Attribute Data as “tidyverse” and ‘Sf’-Ready Data Frames. Version 1.1 [software]. 2021 Sept 23 [cited 2021 Aug 16]. Available from: https://CRAN.R-project.org/package=tidycensus
- 16.2015–2019 American Community Survey 5-Year Estimates [dataset on the Internet]. Release December 2020. U.S. Census Bureau; 2021 Dec 10 [cited 2021 Sept 22]. Available from: https://www.census.gov/data/developers/data-sets/acs-5year.html [Google Scholar]
- 17.Bernard MA, Clayton JA, Lauer MS. Inclusion Across the Lifespan: NIH Policy for Clinical Research. JAMA 2018;320(15):1535–6. [DOI] [PubMed] [Google Scholar]
- 18.National Institutes of Health (U.S.), Office of Extramural Research. NIH policy and guidelines on the inclusion of women and minorities as subjects in clinical research. Bethesda, Md.: NIH; 2001. [Google Scholar]
- 19.SEER*Stat Database: Mortality - All COD, Aggregated with State, Total U.S. (1969–2019) <Katrina/Rita Population Adjustment> [dataset on the Internet]. Release 2021. National Center for Helath Statistics via the Surveillance, Epidemiology, and End Results Program, Surveillance Research Program, Division of Cancer Control and Population Sciences, National Cancer Institute; 2021. [cited 2021 Sept 22]. Available from: https://seer.cancer.gov/mortality [Google Scholar]
- 20.SEER*Stat Software. Version 8.3.9 [software]. Surveillance Research Program, Division of Cancer Control and Population Sciences, National Cancer Institute; 2021. Aug 20 [cited 2022 Sept 22]. Available from: https://seer.cancer.gov/seerstat [Google Scholar]
- 21.Office of Disease Prevention and Health Promotion [Internet]. Cancer. Healthy People 2030. Rockville (MD): U.S. Department of Health and Human Services; Release 2020 Aug 18 [cited 2021 Sept 4]. Available from: https://health.gov/healthypeople/objectives-and-data/browse-objectives/cancer. [Google Scholar]
- 22.R Core Team. R: A Language and Environment for Statistical Computing. Version 4.1.0 [software]. 2021 May 19 [cited 2021 Aug 16]. Available from: https://www.R-project.org
- 23.Pebesma E. Simple Features for R: Standardized Support for Spatial Vector Data. The R Journal 2018;10(1):439–46. [Google Scholar]
- 24.Wickham H. ggplot2: Elegant Graphics for Data Analysis. Version 3.3.5 [software]. 2021 June 25 [cited 2021 Aug 16]. Available from: https://ggplot2.tidyverse.org
- 25.Hawk ET, Habermann EB, Ford JG, Wenzel JA, Brahmer JR, Chen MS, et al. Five National Cancer Institute-designated cancer centers’ data collection on racial/ethnic minority participation in therapeutic trials. Cancer 2014;120:1113–21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Vickers SM, Fouad MN. An overview of EMPaCT and fundamental issues affecting minority participation in cancer clinical trials: Enhancing minority participation in clinical trials (EMPaCT): Laying the groundwork for improving minority clinical trial accrual. Cancer 2014;120:1087–90. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Ibraheem A, Polite B. Improving the accrual of racial and ethnic minority patients in clinical trials: Time to raise the stakes. Cancer 2017;123(24):4752–6. [DOI] [PubMed] [Google Scholar]
- 28.Iachan R, Berman L, Kyle TM, Martin KJ, Deng Y, Moyse DN, et al. Weighting Nonprobability and Probability Sample Surveys in Describing Cancer Catchment Areas. Cancer Epidemiology Biomarkers & Prevention 2019;28(3):471–7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Blake K, Croyle R. Rurality, Rural Identity, and Cancer Control: Evidence From NCI’s Population Health Assessment in Cancer Center Catchment Areas Initiative. The Journal of Rural Health 2019;35(2). [DOI] [PubMed] [Google Scholar]
- 30.Chido-Amajuoyi OG, Mantey D, Cunningham S, Yu R, Kelder S, Hawk E, et al. Characteristics of US adults attempting tobacco use cessation using e-cigarettes. Addictive Behaviors 2020;100:106123. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Schnoll R, Kelly S, Miele A, Glanz K. Characterizing tobacco use in an American cancer center’s catchment area can help direct future research priorities. Journal of Cancer Research & Therapy 2018;6(5):36–40. [Google Scholar]
- 32.Camacho-Rivera M, Rice SL, Oh S, Paris M, Akpara E, Molina J, et al. Cancer Health Impact Program (CHIP): Identifying Social and Demographic Associations of mHealth Access and Cancer Screening Behaviors Among Brooklyn, New York, Residents. Cancer Epidemiology Biomarkers & Prevention 2019;28(3):478–85. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Mayhand KN, Handorf EA, Ortiz AG, Gonzalez ET, Devlin A, Sorice KA, et al. Effect of Neighborhood and Individual-Level Socioeconomic Factors on Colorectal Cancer Screening Adherence. Int J Environ Res Public Health 2021;18(9). [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Daniel C, Aly S, Bae S, Scarinci I, Hardy C, Fouad M, et al. Differences Related to Cancer Screening by Minority and Rural/Urban Status in the Deep South: Population-based Survey Results. J Cancer 2021;12(2):474–81. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Rivadeneira NA, Hoskote M, Le GM, Nguyen TT, Nápoles AM, Pasick RJ, et al. Advancing Cancer Control in San Francisco: Cancer Screening in Under-Represented Populations. American Journal of Preventive Medicine 2020;58(1):e1–e9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Cunningham SA, Yu R, Shete S. Differences in Sun Protection Behaviors Between Rural and Urban Communities in Texas. The Journal of Rural Health 2019;35(2):155–66. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Jensen JD, Pokharel M, Carcioppolo N, Upshaw S, John KK, Katz RA. Cancer information overload: Discriminant validity and relationship to sun safe behaviors. Patient Education and Counseling 2020;103(2):309–14. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.McKeon TP, Hwang WT, Ding Z, Tam V, Wileyto P, Glanz K, et al. Environmental exposomics and lung cancer risk assessment in the Philadelphia metropolitan area using ZIP code-level hazard indices. Environ Sci Pollut Res Int 2021;28(24):31758–69. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Patel MR, Green M, Tariq M, Alhawli A, Syed N, Fleming PJ, et al. A Snapshot of Social Risk Factors and Associations with Health Outcomes in a Community Sample of Middle Eastern and North African (MENA) People in the U.S. J Immigr Minor Health 2021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Haggstrom DA, Lee JL, Dickinson SL, Kianersi S, Roberts JL, Teal E, et al. Rural and Urban Differences in the Adoption of New Health Information and Medical Technologies. The Journal of Rural Health 2019;35(2):144–54. [DOI] [PubMed] [Google Scholar]
- 41.Cassel K, Willingham M, Lee HR, Somera LP, Badowski G, Pagano I. Acculturation and Cancer Risk Behaviors among Pacific Islanders in Hawaii. Ethn Dis 2020;30(4):593–602. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Barrett NJ, Hawkins TV, Wilder J, Ingraham KL, Worthy V, Boyce X, et al. Implementation of a Health Disparities & Equity Program at the Duke Cancer Institute. Oncology Issues 2016;31(5):48–57. [Google Scholar]
- 43.Leader AE, McNair C, Yurick C, Huesser M, Schade E, Stimmel EE, et al. Assessing the Coverage of U.S. Cancer Center Primary Catchment Areas. Cancer Epidemiology Biomarkers & Prevention 2022; [in press]. doi: 10.1158/1055-9965.EPI-21-1097. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
The data generated in this study are available within the article and its supplementary data files. Demographic data analyzed in this study were obtained from the 2015–2019 American Community Survey 5-Year Estimates, available from the U.S. Census Bureau (16). Epidemiologic data analyzed in this study were obtained from National Center for Health Statistics 5-year data (2015–2019), available through the NCI SEER program (19).


