Abstract
Introduction
Herbal medicine plays a significant role in modern medicine. The difficulty in integrating the two, lies in the unknown quantities of active ingredients in herbal remedies. This proved true in this clinical scenario. The quantity of coumarin, in the form of cinnamon ingested by this patient over ten months is unknown. The only quantifiable measure was the derangement in his extrinsic coagulation pathway.
Presentation of case
A 49-year-old male with a history of celiac disease presented with haematochezia secondary to a malignant adenocarcinoma of the transverse colon. The patient underwent a laparoscopic subtotal colectomy and on the second post-operative day, he was noted to have peritonitis and a positive Fox sign. Diagnostic laparoscopy confirmed intraabdominal bleeding. Over the next four days, the patient's haemoglobin plummeted from 17.4 g/dL to 8.0 g/dL. Investigations revealed an INR of 1.59, which led to further questioning into dietary practices. The patient admitted he had been taking Ceylon cinnamon one tablespoon daily for ten months in the period leading up to surgery.
Discussion
Coumarin is a chemical compound readily available in food items such as cinnamon. Coumarin possesses the ability to inhibit vitamin K epoxide reductase complex 1 which is responsible for the recycling of vitamin K. This impedes the gamma-carboxylation of coagulation factors II, VII, IX, X. Vitamin K antagonism can manifest as a prolonged INR and normal activated partial thromboplastin time.
Conclusion
Bleeding diathesis secondary to dietary coumarin is a rare but dangerous phenomenon that emphasizes the need for a thorough interrogation into a patient's dietary history.
Keywords: Case report, Postoperative haemorrhage, Alternative medicine, Coumarin, colon cancer, Cinnamon
Highlights
-
•
Cinnamon is a coumarin that can cause coagulopathy when used in excess.
-
•
Dietary coumarin is a recognized cause of postoperative haemorrhage.
-
•
Reactive haemorrhage can cause significant morbidity.
-
•
Coagulopathy due to dietary coumarin can be rectified with fresh frozen plasma.
-
•
A thorough dietary history is imperative in safe patient care.
1. Introduction
Herbal medicine plays a significant role in modern medicine. The difficulty in integrating the two lies in the unknown quantities of active ingredients in herbal remedies. We present the case of a 49-year-old male diagnosed with transverse colon adenocarcinoma who underwent a laparoscopic subtotal colectomy in a private surgical centre. The surgery was complicated by significant post-operative haemorrhage secondary to the overzealous use of cinnamon. The quantity of coumarin, in the form of cinnamon ingested by this patient over the last ten months is unknown. The only quantifiable measure was the derangement in his extrinsic coagulation pathway. This work has been reported in line with the SCARE criteria [1].
2. Case presentation
A 49-year-old black male with a history of celiac disease noted two episodes of bright red blood mixed with his stools in December 2020. He had no other changes in bowel habit and denied constitutional symptoms. He reported no personal history of prolonged bleeding with minor trauma. Our patient's family history was only significant for prostate cancer and he had no prior surgery or invasive procedures done which would have tested his clotting capability. In addition, he was not on any pharmaceutical antiplatelet or anticoagulation therapy and denied alcohol or tobacco use.
The patient's history of haematochezia prompted a visit to a private gastroenterologist. Colonoscopy showed a 5 cm friable fungating mass 45 cm from the anal verge, along with mild right-sided diverticulosis. Histology confirmed a moderately differentiated adenocarcinoma. Staging with computed tomography (CT) scan of the abdomen and chest showed an irregular soft tissue lesion to the left side of the transverse colon (Fig. 1). There were no enlarged mesenteric lymph nodes or metastases. The patient was seen by a fellowship-trained minimally invasive surgeon and the plan was to proceed with a laparoscopic left hemicolectomy. Preoperative blood investigations showed his haemoglobin to be 17.4 g/dL. His urea, electrolytes and liver function tests were normal. Blood was taken for a carcinoembryonic antigen level but no reagent was available at the local public hospital.
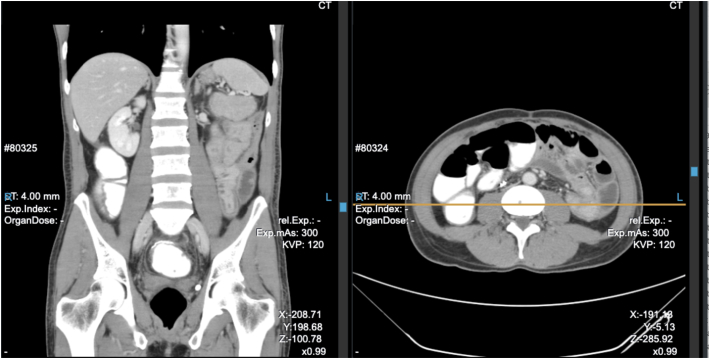
Fig. 1.
CT scan of the abdomen showing tumour to the left side of the transverse colon.
A laparoscopic left hemicolectomy was performed but an abnormally short mesentery of the remnant colon did not facilitate a tension-free colo-sigmoid anastomosis even after attempts at lengthening the mesentery. The decision was made to perform a near subtotal colectomy with an ileo-sigmoid anastomosis. The middle colic and inferior mesenteric vessels were isolated and ligated with an echelon flex stapler with vascular reloads. A leak test was performed with satisfactory results. The surgery lasted 369 min with an estimated blood loss of 100mls. The specimen was removed via a Pfannenstiel incision.
Day one post-operation the patient was dizzy with postural tachycardia. Blood investigations showed the patient's haemoglobin decreased from 17.4 g/dL to 16 g/dL and he had mild leukocytosis (12.97 K/uL). Within 6 h he developed generalized peritonitis with features of Fox sign (ecchymosis along the inguinal ligament). A diagnosis of postoperative haemorrhage was made and a diagnostic laparoscopy performed. This revealed blood within the peritoneal cavity and clot in the region of the middle colic vessels which extended into the retroperitoneal space, and inferiorly into the space of Retzius. There was no active bleeding. The bowel appeared dilated but there were no signs of intraperitoneal sepsis. Endoscopy was performed to ensure the anastomosis was intact along with a leak test which was negative. In the postoperative period, deep venous thrombosis prophylaxis was held. At this point, the patient was transferred to the local tertiary care centre. Postoperatively his haemoglobin was 9.3 g/dL.
Day one post-re-laparotomy he had flank ecchymosis and scrotal swelling. A bleeding diathesis was considered and prothrombin time (PT), international normalized ratio (INR), partial thromboplastin time (PTT) and liver function test (LFT) were performed. Unfortunately, thrombin time and fibrinogen levels were not available at our institution. The deranged results were PT 22.5 s and INR 1.59. His PTT (35.9 s) and LFT were normal. Upon further dietary interrogation, the patient admitted he had been consuming one tablespoon of Ceylon cinnamon daily for the past ten months for its purported health benefits.
Six hourly haemoglobin levels were ordered which showed his haemoglobin decreased from 9.3 g/dL to 8.0 g/dL. The decision was made to transfuse two units of packed red blood cells. The patient was also transfused 795 ml of fresh frozen plasma under advisement from the on-service haematologist. The patient also had three episodes of bilious vomiting and a nasogastric tube was passed. Day two post relaparotomy investigations showed a stable haemoglobin of 11.6 g/dL (post-transfusion) and PT 19.2 s/INR 1.32. There was no more fresh frozen plasma available. Serial blood tests were discontinued. Total parental nutrition was commenced on day four post-operation. Over the following seven days nasogastric output was greater than 1 l per day. A CT scan of the abdomen and pelvis was performed and the scan showed that no contrast was able to get past the anastomosis and the patient was diagnosed with anastomotic stenosis (Clavien-Dindo 3). Relaparotomy was performed and the abdomen was entered by opening the Pfannenstiel incision. The stenosed segment was resected and the anastomosis was refashioned between the distal ileum and the rectum.
Day one post-procedure the patient's nasogastric tube was removed and he tolerated sips of clear fluids. A hematoma developed at the Pfannenstiel incision on the first-day. Bowel function returned day two post-procedure but he was now having large volume frequent watery stools. He was allowed home with home nursing and supplemental intravenous fluids. At outpatient review three days post-discharge, he was commenced on antidiarrheal medication. One-week post-discharge his INR was 1.2 and a bleeding time was done which was normal. A blood film showed no morphological abnormalities to the blood cells or platelets.
3. Discussion
Postoperative haemorrhage can be classified as primary, reactive or secondary. Primary bleeding is usually evident during the surgery, whereas secondary haemorrhage can occur up to a week postoperatively. Reactive haemorrhage tends to occur within 24 h and takes place when a ligature or suture has slipped. It may also occur due to a missed vessel that slowly oozed given intraoperative hypotension and vasoconstriction but bled more vigorously once normal blood pressure was restored. We suspect our patient experienced reactive haemorrhage which was compounded by impaired extrinsic coagulation.
Coumarins are biological compounds believed to have anti-inflammatory, anticoagulant and antimicrobial properties [2]. They belong to the chemical class “benzopyrone” and can be found in many accessible food items such as cinnamon, green tea, and peppermint [2]. Coumarins are touted to have anti-cancer properties, and one of its derivatives esculetin has been described as an inhibitor of the beta-catenin pathway which has a correlation with APC gene mutation [3]. This genetic mutation plays a significant role in the adenoma-carcinoma sequence in the progression to colon cancer.
The coumarin content of cinnamon has been shown to vary by the type of cinnamon used. Ceylon cinnamon derived from the bark of Cinnamomum verum is true cinnamon and has the lowest coumarin content [4]. Whereas most of the cinnamon marketed is Cassia, derived from Cinnamomum burmannii with a higher coumarin content [4]. Interestingly our patient specifically purchased Ceylon. Despite this, he had derangement in his extrinsic clotting pathway with an INR of 1.59. This value measures the functionality of the extrinsic clotting cascade, primarily factors II, V, VII, X and fibrinogen [5]. Coumarins enact their anticoagulant properties by antagonizing vitamin K epoxide reductase complex 1 which is responsible for the recycling of vitamin K [6]. Vitamin K plays a key role in the coagulation cascade by facilitating carboxylation of clotting factors II, VII, IX, X. This process allows the clotting factors to bind to calcium and activate the clotting cascade [7]. The fibrinolytic proteins C and S are also depleted in vitamin K deficiency however this would have been exemplified by a hypercoagulable state. Another concern was coumarins can have hepatotoxic effects. Fortuitously our patient had normal liver function test.
It is well recognized in the literature the implications of herbal medicines both on platelet function as well as coagulation, especially in the perioperative period [8]. Given the delayed assessment of bleeding time we cannot rule out platelet dysfunction as the impetus. Numerous publications report postoperative haemorrhage secondary to natural remedies and dietary supplements such as gingko biloba and ginseng [9], [10], [11]. Surprisingly, none have reported cinnamon as an offending agent, making this case report unique. Given the popularity of alternative medicine, governing bodies such as the American Society of Anesthesiologists have recommended the discontinuation of herbal remedies two weeks prior to elective surgery [12].
Ideally, we would have liked to perform thrombin time and fibrinogen levels given the consumption of coagulation factors occurring in this patient, which could have precipitated disseminated intravascular coagulation.
4. Conclusion
This case exemplifies the impact dietary practices can have on surgical care and it is our recommendation that clinicians take a thorough dietary history for all patients and encourage patients to discontinue herbal remedies two weeks prior to elective surgery.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Ethical approval
Exempt from ethical approval.
Queen Elizabeth Hospital.
Consent
Written informed consent was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal on request.
Author contribution
Courtenay Chase: Writing- Original Draft, Review and editing.
Alex Doyle: Writing- Original Draft, Review and editing.
Sahle Griffith: Conceptualization and Supervision.
Shabier St. John – Review and editing.
Theresa Laurent - Review and editing.
Registration of research studies
N/A.
Guarantor
Courtenay Chase.
Alex Doyle.
Sahle Griffith.
Declaration of competing interest
The authors declare that they have no conflict of interest.
Acknowledgments
None.
References
- 1.Agha R.A., Franchi T., Sohrabi C., Mathew G., for the SCARE Group The SCARE 2020 Guideline: Updating Consensus Surgical CAse REport (SCARE) Guidelines. International Journal of Surgery. 2020;84:226–230. doi: 10.1016/j.ijsu.2020.10.034. [DOI] [PubMed] [Google Scholar]
- 2.Garg S.S., Gupta J., Sharma S., Sahu D. An insight into the therapeutic applications of coumarin compounds and their mechanisms of action. Eur. J. Pharm. Sci. 2020;152 doi: 10.1016/j.ejps.2020.105424. [DOI] [PubMed] [Google Scholar]
- 3.Lee S.Y., Lim T.G., Chen H., Jung S.K., Lee H.J., Lee M.H., Kim D.J., Shin A., Lee K.W., Bode A.M., Surh Y.J., Dong Z. Esculetin suppresses proliferation of human colon cancer cells by directly targeting β-catenin. Cancer Prev. Res. 2013;6(12) doi: 10.1158/1940-6207.CAPR-13-0241. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Wang Y.-H., Avula B., Nanayakkara N.P.D., Zhao J., Khan I.A. Cassia cinnamon as a source of coumarin in cinnamon-flavored food and food supplements in the United States. J. Agric. Food Chem. 2013;61(18):4470–4476. doi: 10.1021/jf4005862. [DOI] [PubMed] [Google Scholar]
- 5.Levy J.H., Szlam F., Wolberg A.S., Winkler A. Clinical use of the activated partial thromboplastin time and prothrombin time for screening: A review of the literature and current guidelines for testing. Clinics in Laboratory Medicine. 2014;34(3) doi: 10.1016/j.cll.2014.06.005. [DOI] [PubMed] [Google Scholar]
- 6.Greaves M. Pharmacogenetics in the management of coumarin anticoagulant therapy: The way forward or an expensive diversion? PLoS Medicine. 2005;2(10) doi: 10.1371/journal.pmed.0020342. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Higdon J., Drake V.J., Delage B., Booth S.L. Linus Pauling Institute; 2021, January 1. Vitamin K.https://lpi.oregonstate.edu/mic/vitamins/vitamin-K#authors-reviewers Retrieved December 17, 2021, from. [Google Scholar]
- 8.Ang-Lee M.K., Moss J., Yuan C.S. Herbal medicines and perioperative care. Journal of the American Medical Association. 2001;286(2) doi: 10.1001/jama.286.2.208. [DOI] [PubMed] [Google Scholar]
- 9.Jayasekera N., Moghal A., Kashif F., Karalliedde L. Herbal medicines and postoperative haemorrhage [15] Anaesthesia. 2005;60(7) doi: 10.1111/j.1365-2044.2005.04276.x. [DOI] [PubMed] [Google Scholar]
- 10.Wang L., Lanka L., Chen D., Pruthi R.K. Severe postoperative hemorrhage in a patient on dietary and herbal supplements. Journal of Perioperative Practice. 2018;28(10) doi: 10.1177/1750458918780112. [DOI] [PubMed] [Google Scholar]
- 11.Norred C.L., Finlayson C.A. Hemorrhage after the preoperative use of complementary and alternative medicines. J. Am. Assoc. Nurse Anesth. 2000;68(3) [PubMed] [Google Scholar]
- 12.Weintraub P. New and old media used to distribute ASA’s patient safety meddage about herbal medications. ASA Newsletter. July 1999;23:35. [Google Scholar]