Abstract
The omicron variant of severe acute respiratory syndrome coronavirus 2 causes much less olfactory dysfunction than the previous variants. There are several potential mechanisms for how omicron may change tissue tropism and spare olfactory function. The new mutations make omicron more hydrophobic and alkaline than previous variants, which may reduce penetration of the mucus layer. Overall, the new mutations minimally change receptor binding affinity, but entry efficiency into host cells is reduced in cells expressing transmembrane serine protease 2 (TMPRSS2). Because the support cells in the olfactory epithelium abundantly express TMPRSS2, these main target cells in the olfactory epithelium may become infected less by the new omicron variant.
Keywords: omicron, SARS-CoV-2, COVID-19, anosmia, prevalence, D614G mutation, loss of smell, mucus, ACE2, TMPRSS2
The omicron variant of severe acute respiratory syndrome coronavirus 2 causes 3–4-fold less anosmia prevalence than previous variants. The molecular mechanisms responsible for reduced infection of olfactory cells may explain the sparing of olfactory function with the omicron variant.
When the coronavirus virus 2019 (COVID-19) pandemic developed in East Asia early in 2020, loss of smell or taste was a rare symptom [1]. Within a few months of the pandemic, new severe acute respiratory syndrome (SARS) coronavirus 2 (SARS-CoV-2) variants emerged. Most of these variants caused a much more frequent loss of smell, presumably due to the D614G spike mutation [2]. Curiously, the omicron variant retains the D614G mutation, yet it largely spares chemosensory function when compared with the previous variants.
In this perspective piece, we focus on the sense of smell, because much of subjective taste dysfunction is thought to be caused by loss of smell [3], and olfactory dysfunction in COVID-19 is better understood than taste dysfunction. We examine the epidemiological evidence and the emerging insights into the net effect of omicron’s numerous spike mutations on properties of the virus that may modify its impact on the olfactory epithelium, including mucus penetration, angiotension-converting enzyme 2 (ACE2) binding, host cell entry, and immune responses. Relevant properties of omicron can be tested in animal models and will provide new insights into the mechanism of anosmia in COVID-19.
EPIDEMIOLOGY OF VARIANTS AND OLFACTORY DYSFUNCTION
Loss of smell became a cardinal symptom of COVID-19 infection with the predominance of variants containing the D614G mutation [4] (Figure 1A). This difference between variants was surprising, given the fact that all SARS-CoV-2 variants identified to date use the same virus entry receptor, ACE2, to enter host cells [2, 5, 19]. Variants with the D614G mutation appeared to be more successful at infecting the support cells in the olfactory epithelium [2, 20]. This observation established the concept that certain spike mutations may affect the prevalence of this COVID-19 symptom, although minor spike mutations present in alpha, beta, and delta variants minimally altered the virus’s ability to induce chemosensory deficits according to epidemiological reports [6, 7] (Figure 1A).
Figure 1.
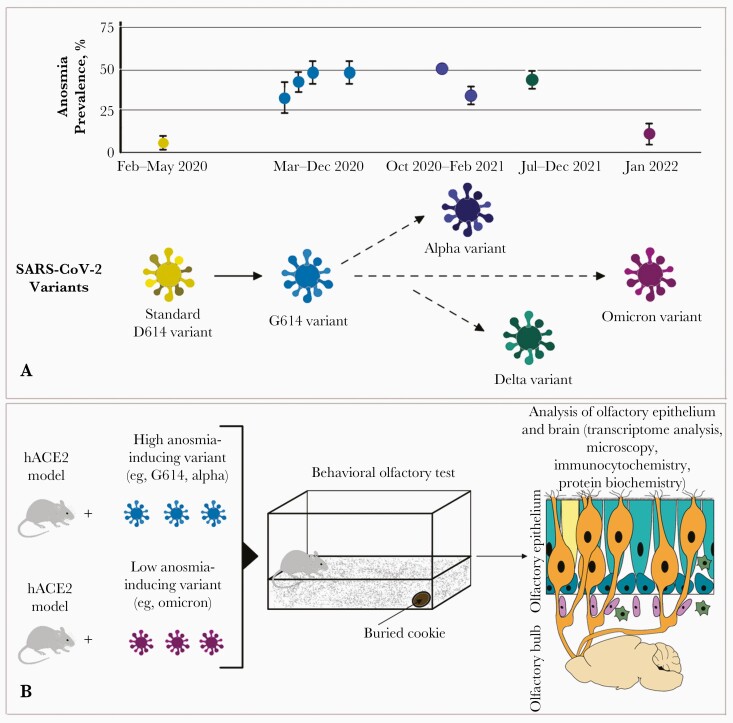
Anosmia prevalences associated with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) variants (A) and proposed experimental strategy to elucidate the mechanism underlying varying anosmia prevalences in an animal model (B). A, Graph shows pooled anosmia prevalence for the original D614 strain [2], the G614 variant according to multiple meta-analyses [2, 5], and the alpha [6, 7] and delta [7] variants and our pooled estimate for the omicron variant according to the first 12 studies from 4 continents (Table 1). The approximate time periods of variant predominance are indicated on the x-axis. These periods overlap somewhat, because variants were dominant in different regions of the world at different times. For data compiled from multiple studies, error bars indicate the 95% confidence interval. Note that the D614G mutation generally leads to higher anosmia prevalence but not for omicron. B, As a strategy to elucidate mechanisms, a suitable mouse model expressing the viral entry receptor (human angiotension-converting enzyme [hACE2]) is infected with either a virus variant inducing a high prevalence of anosmia (eg, alpha or G614) or a virus variant inducing low anosmia prevalence (eg, omicron). The animals undergo standard behavioral testing to measure and verify the time needed to find a hidden cookie. The olfactory epithelium and brains (olfactory bulbs) of the same animals are then processed for various morphological, histochemical, and biochemical analyses to quantify the amount of virus that infected the olfactory epithelium, to identify infected cell types, and to measure the extent and timing of damage and other parameters in the olfactory system.
The emergence of the omicron variant recently identified in South Africa presents a new twist. This new variant has a much higher transmissibility and therefore spreads rapidly. The omicron variant contains the largest number of unique mutations in the spike protein, compared with earlier variants [21]. Even though the omicron variant retains the D614G mutation [21], the prevalence of chemosensory dysfunction with this variant is low (Table 1 and Figure 1A). Based on the first 12 reports, including 190 778 patients, we calculated a pooled weighted estimate of olfactory dysfunction for the omicron variant of 13%, which is 3–4-fold lower than the prevalence in regions and times when the alpha and delta variants prevailed [2, 5–7]. Why does omicron largely spare olfaction?
Table 1.
Studies Reporting the Prevalence of Loss of Smell for the Omicron Variant
| Date of 1st Publication | Reference | Author(s)/Source | Country | Cohort Size, No. of Patients | Patients With Loss of Smell, No. (%) |
|---|---|---|---|---|---|
| 27 Nov 2021 | [8] | Telegraph | South Africa | 70 | 0 (0) |
| 16 Dec 2021 | [9] | Brandal et al | Norway | 81 | 12 (14.8) |
| 17 Dec 2021 | [10] | CDC | US | 43 | 3 (8) |
| 17 Dec 2021 | [11] | Times of India | India | 32 | 0 (0) |
| 14 Jan 2022 | [12] | UKHSA | UK | 182 133 | 23 677 (13) |
| 17 Jan 2022 | [13] | Kim et al | Korea | 40 | 1 (2.5) |
| 18 Jan 2022 | [7] | Vihta et al | UK | 7000a | 910 (13) |
| 25 Jan 2022 | [14] | Hajjo et al | Jordan | 500 | 6 (1.2) |
| 27 Jan 2022 | [15] | Søraas et al | Norway | 52 | 8 (15) |
| 03 Feb 2022 | [16] | Helmsdal et al | UK | 21 | 4 (19) |
| 12 Feb 2022 | [17] | Maisa et al | France | 468 | 39 (8.3) |
| 18 Feb 2022 | [18] | Boscolo-Rizzo et al | Italy | 338 | 83 (24.6) |
| Total | … | … | … | 190 778 | 24 743 (12.97b) |
Abbreviations: CDC, Center for Disease Control and Prevention; UK, United Kingdom; UKHSA, UK Health Security Agency; US, United States.
Estimate based on graph provided by Vihta et al [7], fig 1A].
This percentage—12.97%—was the weighted pooled estimate of the prevalence of loss of smell. The mean percentage in these studies was 10%.
SOLUBILITY OF OMICRON IN OLFACTORY MUCUS
To access the olfactory epithelium, viruses and other pathogens have to dissolve in and penetrate the mucus layer that allows odorants to reach the olfactory receptors but also protects the olfactory epithelium from toxins and pathogens [22]. Hydrophilic and acidic proteins are more soluble in the mucus and penetrate the mucus barrier without the need of specific carrier proteins [22]. Many of the omicron variant’s mutations introduce new hydrophobic stretches in the spike protein [23]. In addition, owing to its new mutations, omicron’s spike protein is more alkaline than the Wuhan and delta strains [23]. Omicron thus may have a lower solubility in mucus and therefore may generate a reduced infection of the olfactory epithelium. Since the composition of the olfactory mucus differs significantly from that of other mucus layers—in the respiratory tract [24], for example—reduced access of omicron to the olfactory epithelium may be relatively specific and could contribute to the sparing of olfaction in patients infected with the omicron variant.
MOLECULAR MECHANISMS OF HOST CELL ENTRY
Mechanisms underlying anosmia in COVID-19 involve high binding affinity of the virus to ACE2 and efficient viral-host membrane fusion, which collectively lead to high efficiency of cell entry of the virus to nonneuronal cells of the olfactory epithelium within the nasal cavity [19, 20, 25, 26]. This conclusion is further supported by protein structural data on the D614G mutation, which predicts increased virus entry into the host cell because of reduced target cell–independent premature spike shedding (thus making more spike trimers accessible for ACE2 binding) and also by enhancing the membrane fusion step [25].
Does the omicron variant spare olfaction because it has a lower binding affinity to ACE2? There is an emerging consensus that the net effect of all 15 mutations present in the receptor binding domain of omicron’s spike does not significantly alter its affinity to the ACE2 receptor [21, 27, 28]. Therefore, omicron’s sparing of olfaction cannot be due to lower ACE2 binding. But what are the effects of omicron’s mutations on other steps of the cell entry process? Importantly, viruses can use 2 distinct cell entry routes: one by surface membrane fusion involving the protease expressing transmembrane serine protease 2 (TMPRSS2) and the other by endosomal membrane fusion through cathepsins [28–30].
Omicron can use both entry routes but prefers the endosomal route to TMPRSS2-mediated membrane fusion. This suggests that it has a lower cell entry efficiency because of lower membrane fusion in cell types that robustly express TMPRSS2 [21, 28–31]. Because support cells in the olfactory epithelium express the highest level of TMPRSS2, omicron may be less efficient in infecting these cells, resulting in a lower frequency of anosmia [32]. Replication of omicron is markedly attenuated in both the upper and the lower respiratory tract [29, 31]. Such a tissue-specific difference of omicron infectivity also seems to apply to the olfactory epithelium [28, 33]. Indeed, a recent study shows that omicron produces only mild infection of the olfactory mucosa but causes significant disease in the respiratory mucosa in hamsters [33], although the specific cell types that become infected in the olfactory epithelium after omicron inoculation remain to be identified (Figure 1B).
Taking into account the properties of the new omicron variant, it is possible to design experiments in animal models, ideally in human ACE2 knock-in mice, that compare the disease caused by infection with omicron with that caused by other variants known to induce high prevalence of anosmia. If the omicron variant infects fewer olfactory epithelial cells, especially support cells, this will suggest that the lower incidence of anosmia is caused by less efficient cell entry into this cell type. However, if the cell type–specific and temporal extent of infection in the olfactory epithelium is similar for both variants, it would argue against a central role of the support cell and would rather suggest that virus-induced host immune responses [34] may trigger the sudden anosmia experienced by patients with COVID-19 (Figure 1B). Accordingly, the omicron variant and its effects on chemosensory epithelia may help elucidate the biological mechanisms underlying olfactory dysfunction in COVID-19.
COMPARISON OF OMICRON, PREVIOUS SARS-CoV-2 VARIANTS, AND SARS CORONAVIRUS 1
The omicron variant shares some features with SARS coronavirus 1 (SARS-CoV-1), mainly a higher dependence on the endosomal route for cell entry and lower viral-host membrane fusigenic activity [26, 28]. The ability of SARS-CoV-2 variants alpha and delta to induce rapid anosmia may require the TMPRSS2 route of cell entry and high membrane fusion capacity combined with effective furin cleavage, and only this route may enable the enhanced infectivity needed for rapid induction of anosmia in COVID-19. SARS-CoV-1 and the omicron variant appear to fail to induce frequent anosmia because they use the less efficient endosomal route. Why is the endosomal route to enter support cells not an effective way to infect this cell type? Cells have evolved strategies to prevent entry of viruses at the endocytosis step by expressing endosomal restriction factors such as interferon-induced transmembrane proteins [35]. Olfactory support cells may express such factors and are therefore better protected from endosomal virus entry but are more susceptible to cell surface entry mediated by TMPRSS2.
OLFACTION THRESHOLDS FOR FUNCTIONAL LOSS
Only 5%–10% of functional olfactory neurons are required for a relatively normal sense of smell [36]. Therefore, minor changes in mucus penetration or cell entry efficiencies can have significant (magnified) effects on reaching this threshold. To cause anosmia, it can be estimated that the virus needs to eliminate, within a 3–4-day period (before their regeneration), at least 90% of all support cells. Because of the above-mentioned mechanisms, omicron and the D614 strain may struggle to eliminate 90% of cells, and then the infected patients will not experience anosmia (but possibly hyposmia, when appropriately tested; Supplementary Figure 1).
CONCLUSIONS
The emerging data on the omicron variant show that such an important and characteristic symptom of COVID-19 as chemosensory dysfunction is not fixed at a certain level but changes during virus evolution as a result of new mutations. This is important information not only for researchers but also for patients and clinicians. In the second phase of the pandemic, when the alpha and delta variants dominated, chemosensory dysfunction helped quickly identify new infection outbreaks and patients at risk. With the appearance of the omicron variant, this will no longer be possible. However, the good news is that now a much smaller fraction of patients with COVID-19 will suffer from chemosensory dysfunction, including those who maintain such dysfunction for a prolonged duration (“long COVID”), which significantly diminishes quality of life.
Supplementary Data
Supplementary materials are available at The Journal of Infectious Diseases online. Supplementary materials consist of data provided by the author that are published to benefit the reader. The posted materials are not copyedited. The contents of all supplementary data are the sole responsibility of the authors. Questions or messages regarding errors should be addressed to the author.
Notes
Acknowledgments. We thank Stanley Perlman, MD, PhD (University of Iowa) and Bing Chen, PhD (Harvard University) for helpful comments and discussions.
Financial support. This work was supported by the National Institute of General Medical Sciences at the National Institutes of Health (grant GM103554 to C. v. B.).
Contributor Information
Rafal Butowt, L. Rydygier Collegium Medicum, Nicolaus Copernicus University, Bydgoszcz, Poland.
Katarzyna Bilińska, L. Rydygier Collegium Medicum, Nicolaus Copernicus University, Bydgoszcz, Poland.
Christopher von Bartheld, Department of Physiology and Cell Biology, University of Nevada, Reno School of Medicine, Reno, Nevada, USA.
References
- 1. Mao L, Jin H, Wang M, et al. Neurologic manifestations of hospitalized patients with coronavirus disease 2019 in Wuhan, China. JAMA Neurol 2020; 77:683–90. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. von Bartheld CS, Hagen MM, Butowt R.. The D614G virus mutation enhances anosmia in COVID-19 patients: evidence from a systematic review and meta-analysis of studies from South Asia. ACS Chem Neurosci 2021; 12:3535–49. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Hintschich CA, Niv MY, Hummel T.. The taste of the pandemic-contemporary review on the current state of research on gustation in coronavirus disease 2019 (COVID-19). Int Forum Allergy Rhinol 2022; 12:210–6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Korber B, Fischer WM, Gnanakaran S, et al. Tracking changes in SARS-CoV-2 spike: evidence that D614G increases infectivity of the COVID-19 virus. Cell 2020; 182:812–27.e19. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. von Bartheld CS, Hagen MM, Butowt R.. Prevalence of chemosensory dysfunction in COVID-19 patients: a systematic review and meta-analysis reveals significant ethnic differences. ACS Chem Neurosci 2020; 11:2944–61. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. Graham MS, Sudre CH, May A, et al. Changes in symptomatology, reinfection, and transmissibility associated with the SARS-CoV-2 variant B.1.1.7: an ecological study. Lancet Public Health 2021; 6:e335–45. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Vihta KD, Pouwels KB, Peto TEA, et al. Omicron-associated changes in SARS-CoV-2 symptoms in the United Kingdom. medRxiv [Preprint: not peer reviewed]. 4 February 2022. Available from: https://www.medrxiv.org/content/10.1101/2022.01.18.22269082v2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8. South African doctor who raised alarm about omicron variant says symptoms are “unusual but mild.” https://www.telegraph.co.uk/global-health/science-and-disease/south-african-doctor-raised-alarm-omicron-variant-says-symptoms/. Accessed 13 March 2022.
- 9. Brandal LT, MacDonald E, Veneti L, et al. Outbreak caused by the SARS-CoV-2 omicron variant in Norway, November to December 2021. Euro Surveill 2021; 26:1–5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10. CDC COVID-19 Response Team. SARS-CoV-2 B.1.1.529 (omicron) variant—United States, December 1-8, 2021. MMWR Morb Mortal Wkly Rep 2021; 70:1731–4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Omicron-hit had sore throat, body ache, didn’t lose smell. https://timesofindia.indiatimes.com/city/mumbai/mumbai-omicron-hit-had-sore-throat-body-ache-didnt-lose-smell/articleshow/88327372.cms. Accessed 13 March 2022.
- 12. UK Health Security Agency. SARS-CoV-2 variants of concern and variants under investigation in England. Technical briefing 34. 2022. https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/1046853/technical-briefing-34-14-january-2022.pdf. Accessed 28 January 2022.
- 13. Kim MK, Lee B, Choi YY, et al. Clinical characteristics of 40 patients infected with the SARS-CoV-2 omicron variant in Korea. J Korean Med Sci 2022; 37:e31. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14. Hajjo R, AbuAlSamen MM, Alzoubi HM, Alqutob R.. The epidemiology of hundreds of individuals infected with omicron BA.1 in Middle Eastern Jordan. medRxiv [Preprint: not peer reviewed]. 14 February 2022. Available from: https://www.medrxiv.org/content/10.1101/2022.01.23.22269442v2. [Google Scholar]
- 15. Søraas A, Grødeland G, Granerud BK, et al. Breakthrough infections with the omicron and delta variants of SARS-CoV-2 result in similar re-activation of vaccine-induced immunity. medRxiv [Preprint: not peer reviewed]. 27 January 2022. Available from: https://www.medrxiv.org/content/10.1101/2022.01.27.22269895v1.full. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16. Helmsdal G, Hansen OK, Møller LF, et al. Omicron outbreak at a private gathering in the Faroe Islands, infecting 21 of 33 triple-vaccinated healthcare workers. Clin Infect Dis 2022; 75:893–6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Maisa A, Spaccaferri G, Fournier L, et al. First cases of omicron in France are exhibiting mild symptoms, November 2021-January 2022. Infect Dis Now 2022:S2666-9919(22)00036-7. [in press]. doi: 10.1016/j.idnow.2022.02.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18. Boscolo-Rizzo P, Tirelli G, Meloni P, et al. COVID-19-related smell and taste impairment with widespread diffusion of SARS-CoV-2 omicron variant. Int Forum Allergy Rhinol 2022:1–9. doi: 10.1002/alr.22995. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19. Butowt R, Bilinska K, von Bartheld CS.. Chemosensory dysfunction in COVID-19: integration of genetic and epidemiological data points to D614G spike protein variant as a contributing factor. ACS Chem Neurosci 2020; 11:3180–4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Khan M, Yoo SJ, Clijsters M, et al. Visualizing in deceased COVID-19 patients how SARS-CoV-2 attacks the respiratory and olfactory mucosae but spares the olfactory bulb. Cell 2021; 184:5932–49.e15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Hoffmann M, Krüger N, Schulz S, et al. The omicron variant is highly resistant against antibody-mediated neutralization: implications for control of the COVID-19 pandemic. Cell 2022; 185:447–456.e11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22. Kurtz DB, Zhao K, Hornung DE, Scherer P.. Experimental and numerical determination of odorant solubility in nasal and olfactory mucosa. Chem Senses 2004; 29:763–73. [DOI] [PubMed] [Google Scholar]
- 23. Kumar S, Thambiraja TS, Karuppanan K, Subramaniam G.. Omicron and delta variant of SARS-CoV-2: a comparative computational study of spike protein. J Med Virol 2022; 94:1641–9. [DOI] [PubMed] [Google Scholar]
- 24. Yoshikawa K, Wang H, Jaen C, et al. The human olfactory cleft mucus proteome and its age-related changes. Sci Rep 2018; 8:17170. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25. Zhang J, Cai Y, Xiao T, et al. Structural impact on SARS-CoV-2 spike protein by D614G substitution. Science 2021; 372:525–30. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26. Jackson CB, Farzan M, Chen B, Choe H.. Mechanisms of SARS-CoV-2 entry into cells. Nat Rev Mol Cell Biol 2022; 23:3–20. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. Mannar D, Saville JW, Zhu X, et al. SARS-CoV-2 omicron variant: antibody evasion and cryo-EM structure of spike protein-ACE2 complex. Science 2022; 375:760–4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28. Meng B, Abdullahi A, Ferreira IATM, et al. Altered TMPRSS2 usage by SARS-CoV-2 omicron impacts tropism and fusogenicity. Nature 2022; 603:706–14. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29. Shuai H, Chan JF, Hu B, et al. Attenuated replication and pathogenicity of SARS-CoV-2 B.1.1.529 omicron. Nature 2022; 603:693–9. [DOI] [PubMed] [Google Scholar]
- 30. Zhao H, Lu L, Peng Z, et al. SARS-CoV-2 omicron variant shows less efficient replication and fusion activity when compared with delta variant in TMPRSS2-expressed cells. Emerg Microbes Infect 2021; 11:277–83. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31. Suzuki R, Yamasoba D, Kimura I, et al. Attenuated fusogenicity and pathogenicity of SARS-CoV-2 omicron variant. Nature 2022; 603:700–5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32. Cooper KW, Brann DH, Farruggia MC, et al. COVID-19 and the chemical senses: supporting players take center stage. Neuron 2020; 107:219–33. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33. Armando F, Beythien G, Kaiser F, et al. SARS-CoV-2 omicron variant causes mild pathology in the upper and lower respiratory tract of Syrian golden hamsters (Mesocricetus auratus). Res Square [Preprint: not peer reviewed]. 1 February 2022. Available from: https://www.researchsquare.com/article/rs-1315280/v1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34. Zazhytska M, Kodra A, Hoagland DA, et al. Non-cell-autonomous disruption of nuclear architecture as a potential cause of COVID-19-induced anosmia. Cell 2022; 185:1052–64.e12. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35. Peacock TP, Goldhill DH, Zhou J, et al. The furin cleavage site in the SARS-CoV-2 spike protein is required for transmission in ferrets. Nat Microbiol 2021; 6:899–909. [DOI] [PubMed] [Google Scholar]
- 36. Harding JW, Getchell TV, Margolis FL.. Denervation of the primary olfactory pathway in mice. V. Long-term effect of intranasal ZnSO4 irrigation on behavior, biochemistry and morphology. Brain Res 1978; 140:271–85. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.