ABSTRACT
Objective:
To correlate vertical (VFO) and horizontal (HFO) femoral offset with hip range of motion (ROM), peak muscle torque (PT), functional, capacity, and lower limb length in patients with total hip arthroplasty (THA).
Methods:
A cross-sectional case control study, in which 22 individuals (10 men and 12 women) - aged 61 (41-72), and within 23 (10-40) postoperative days - were evaluated for active hip ROM (fleximetry); Isometric PT (portable dynamometer); functional capacity (Timed up and Go test (TUG) and Harris Hip Score questionnaire); lower limb length (measuring tape); and VFO and HFO (radiographs).
Results:
The operated limb showed a reduction in length (p = 0.006), ROM for abduction (p = 0.001), flexion (p = 0.003), and external rotation (p = 0.003), as well as in all PT (p < 0.05) when compared with the contralateral limb. Moderate correlations were observed between VFO and external rotators (r = 0.487; p = 0.021); HFO and external rotators PT (r = −0.508; p = 0.016); and the difference between the VFO (operated and non-operated limb) and the TUG (r = −0.570; p = 0.006).
Conclusion:
Changes to the femoral offset seem to influence functional capacity, as well as the movement and external rotators PT of the hips in patients with THA, considering the postoperative period evaluated. Level of Evidence III, Case Control Study.
Keywords: Arthroplasty, Replacement, Hip; Muscle Strength; Hip Injuries
RESUMO
Objetivo:
Correlacionar achados do offset femoral vertical (OFV) e horizontal (OFH) aos da amplitude de movimento do quadril (ADM), pico de torque muscular (PT), capacidade funcional (CF) e comprimento dos membros inferiores (CM) em pacientes com artroplastia total de quadril (ATQ).
Métodos:
Estudo transversal, caso controle (nível de evidência III), foram avaliados 22 indivíduos (10 homens e 12 mulheres) com idade de 61 (41-72) anos e 23 (10-40) dias de pós-operatório, quanto à: ADM ativa do quadril (fleximetria); PT isométrico (dinamômetro portátil); CF - teste Timed up and Go (TUG) e questionário Harris Hip Score (HHS); CM (fita métrica); e OFV e OFH a partir de radiografias.
Resultados:
O membro operado apresentou redução no CM (p = 0,006), ADM de abdução (p = 0,001), flexão (p = 0,003) e RE (p = 0,003), e em todos os PT (p < 0,05) em comparação ao membro contralateral. Correlações moderadas encontradas entre: OFV e RE (r = 0,487; p = 0,021); OFH e PT dos RE (r = −0,508; p = 0,016);
e a diferença do OFV (membro operado e não operado) e o TUG (r = −0,570; p = 0,006).
Conclusão:
Alterações no OF parecem influenciar a CF, bem como o movimento e o PT dos RE do quadril em pacientes com ATQ para o período pós-operatório avaliado. Nível de Evidência III, Estudo de Caso-Controle.
Descritores: Artroplastia de Quadril, Força Muscular, Lesões do Quadril
INTRODUCTION
Total hip arthroplasty (THA) consists in the surgical replacement of the femur (femoral head) and pelvic (acetabulum) components of the hip joint. 1 The number of THA performed in the world has been growing annually. It is estimated that, by the year 2046, the number of THA performed worldwide will have increased 219%, representing a higher cost to the health system. 2 Preoperative planning is essential for the proper choice of prosthetic components to restore the biomechanics of the hip to normal conditions. 3
The measurements of the vertical (VFO) and horizontal (HFO) femoral offset can be considered both in surgical planning and in the verification of postoperative results. Previous studies have shown positive associations between femoral offset (FO) and hip abductors muscle strength. 4 )-( 10 A more lateral position of the femur followed by a greater offset could provide a biomechanical advantage, associated with greater stability of prosthetic components. It is believed that this positioning would allow a better range of motion (ROM) and strength production by the hip abductors, as well as an improvement in the tension of soft tissues. 11 However, more studies are needed to verify the possible relationships between the radiographic variables and the clinical outcomes.
Thus, this study aims to correlate the findings of FO with those of hip ROM, hip muscle peak torque, lower limb length, and functional capacity in patients subjected to primary THA surgery.
MATERIALS AND METHODS
A cross-sectional study was conducted with patients subjected to primary THA surgery in hospitals in Porto Alegre, south of Brazil. Prior to data collection, a written informed consent was obtained from all participants. This study was approved by the Federal University of Health Science Research Ethics Committee (protocol 3.049.371) and a registered in Clinical Trials (NCT3208829) as part of a larger study. Individuals with postoperative complications (infections, deep vein thrombosis, prosthesis dislocation, periprosthetic fractures, and neural injuries), THA surgery on the contralateral limb less than a year prior to this study, and other orthopedic surgeries on the lower limbs were excluded from the study. All surgeries were performed using the posterior hip approach.
Participants attended a single evaluation session with the same experienced and trained assessor, between 10 to 40 days after surgery. In this evaluation, data regarding age, body mass index (BMI), lower limb length (LLL), hip ROM, hip muscle peak torque (PT), and functional capacity were obtained. The LLL was measured using a tape measure, considering the anterior superior iliac spine and the medial malleolus as anatomical points, with the patients in the supine position with the lower limbs extended.
Active ROM was assessed bilaterally using a fleximeter (model FL6010, Sanny, Brazil). Participants were instructed to perform each movement twice and were interrupted if compensatory movements (pelvis or trunk) were observed. Figure 1 shows the positions used. 12
Figure 1. Range of motion assessment positions.
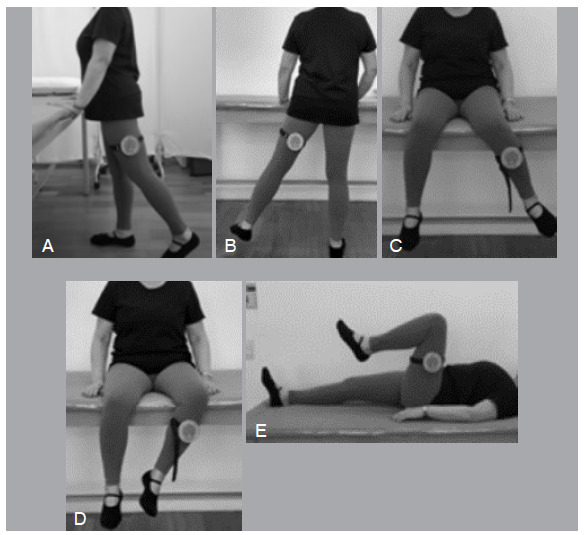
A: assessment of left hip extension; B: assessment of left hip abduction; C: assessment of left hip internal rotation; D: assessment of left hip external rotation; E: assessment of left hip flexion.
Hip muscle PT was measured bilaterally, using a portable dynamometer (Micro-Fet II model, Hoggan Health Industries). Three measurements of maximum voluntary isometric contraction were performed for each movement and the average of the values was used for analysis. Each measurement lasted 5 seconds with an interval of 30 seconds for resting. Figure 2 shows the positioning protocol of the evaluation, and the placing of the dynamometer according to the evaluated muscle group: abductors, dynamometer positioned approximately 10 cm above the knee joint; extensors, approximately 10 cm above the popliteal foramen; flexors, 10 cm above the patella; internal and external rotators, 5 cm above the lateral and edial malleolus (Figure 2). 13 All PT measurements were normalized by body mass according to the equation PT = peak of torque (Nm)/body mass (Kg) × 100.
Figure 2. Muscle torque assessment positions.
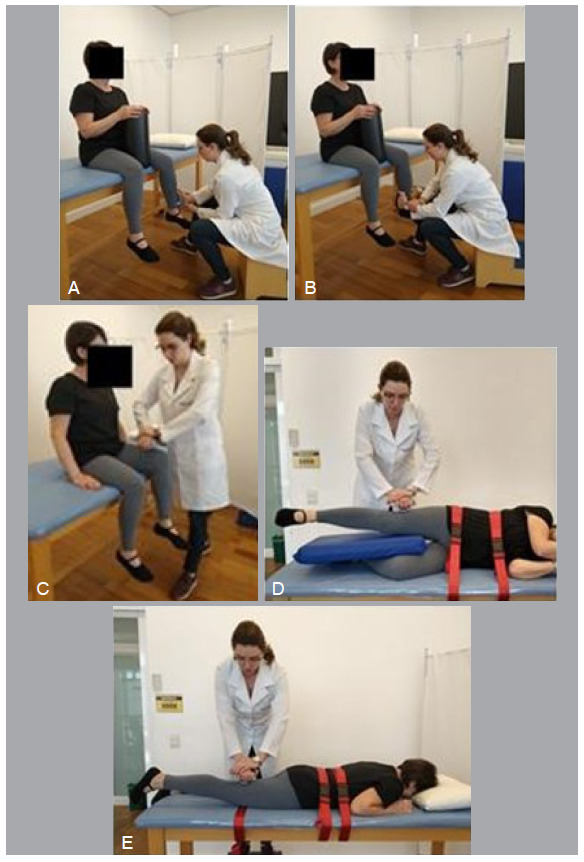
A: hip internal rotator isometric muscle torque assessment; B: hip external rotator isometric muscle torque assessment; C: hip flexors isometric muscle torque assessment; D: hip abductor isometric muscle torque assessment; E: hip extensors isometric muscle torque assessment.
Functional capacity was assessed using Timed Up and Go Test (TUG) and Harris Hip Score (HHS) questionnaire, both of which have excellent validity and reliability. 14 ),( 15 To perform the TUG test, participants had to rise from a chair, without the support of their arms, walk 3 meters at their usual speed, using their auxiliary devices if necessary, until they reach a mark on the floor; then they had to turn around, walk back to the chair, and sit down. 16 ),( 17 The HHS has a score ranging from 0 to 100, distributed across the domains: pain, function-gait, function-activity, deformity, and ROM. According to the obtained scores, the results were classified: poor, below 70 points; normal, 70-79 points; good, 80-89 points; and excellent, 90-100 points. 9
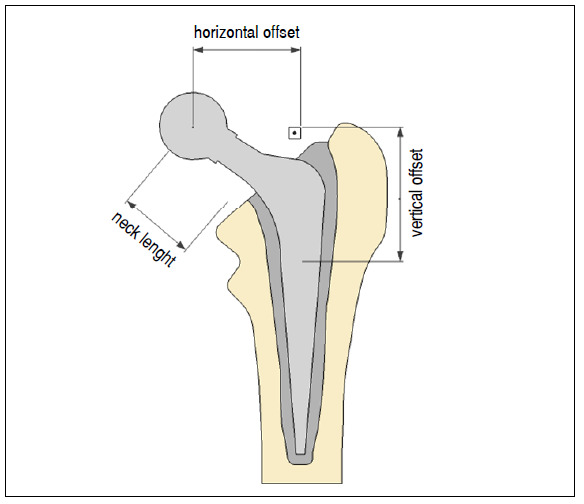
VFO and HFO measurements were performed from radiographs of the pelvis (anteroposterior view), with the patient in the supine position and lower limbs neutrally positioned, obtained in the hospitals computerized systems. The VFO was determined by the distante from the center of the femoral head to the starting point for lesser trochanter (Figure 3). HFO was defined as the distance comprised by a line passing perpendicularly from the center of rotation of the femoral head to the meeting point with another line that passes through the long axis of the femur (Figure 3). According to the literature, from the difference between the HFO of the operated limb and the non-operated limb, the HFO can be classified as: increased, difference of 5 mm or more with the operated limb being bigger; reconstructed, difference of up to 5 mm between the limbs; and reduced, difference of less than 5 mm, with the operated limb being smaller. 9 ),( 18 ),( 19
Figure 3. Femoral offset.
The Shapiro-Wilk test was used to verify data distribution. In the descriptive analysis, measures of central tendency (median, minimum, and maximum) were applied. In order to analyze the reliability of the ROM and PT measurements, the Intraclass Correlation Coefficient (ICC) was used, which can be classified as excellent (ICC > 0.75), satisfactory (ICC = 0.40-0.75), and weak (ICC < 0.40), of which only those classified as at least satisfactory (α < 0.05) are considered relevant. 20 For the intra-group comparative analysis (operated lower limb and non-operated lower limb) the Wilcoxon test was applied for nonparametric data. For correlational analyses, Spearman’s Linear Correlation was used. A significance level (α) of 5% and a confidence interval of 95% were adopted. All statistical analyses were performed using the Statistical Package for Social Sciences (SPSS) for Windows (version 22.0).
RESULTS
The data found in this study had a non-normal distribution. In total, 22 individuals (10 men and 12 women) were included; they had a median age of 61 (41-72) years, a BMI of 29.48 (21.59-37.01) kg/m², and were evaluated 23 (10-40) days after surgery. Table 1 has further information on the characterization of the sample.
Table 1. Total hip arthroplasty patients’ characterization.
| THA patients (n = 22) | |
|---|---|
| Age (years) | 61.00 (41.00 - 72.00) |
| Sex (M/F) | 10/12 |
| Height (m) | 1.67 (1.39 - 1.78) |
| Weight (kg) | 77.00 (57.00 - 100.50) |
| BMI (kg/m2) | 29.58 (21.59 - 37.010) |
| P.O. Period (days) | 23.00 (10.00 - 40.00) |
| Fixation Type (H/C) | 14/8 |
| Contralateral hip prosthesis (Y/N) | 5/17 |
| Auxiliary Device (1C/2C/W) | 2/8/12 |
| TUG(s) | 26.41 (12.30 - 60.38) |
| HHS | 57.45 (37.20 - 73.50) |
1C: one crutch; 2C: two crutches; BMI: body mass index; C: cemented; F: female; H: hybrid; M: male; N: no; P.O.: postoperative; THA: total hip arthroplasty; TUG: Timed Up and Go Test; Y: yes; W: walker. Values expressed as median (minimum-maximum).
All participants received routine care during the hospitalization period, with daily physiotherapy sessions and guidelines related to postoperative care. Regarding functional capacity, the individuals presented a time of 26.41 (12.30-60.38) seconds in performing the TUG test and a score of 57.45 (37.20-73.50) on the HHS (Table 1). The internal reliability of the measurements obtained in this study was considered excellent for both hip PT (ICC = 0.95-0.98; p > 0.05) and ROM (ICC = 0.93-0.99; p < 0.05).
Table 2 shows the data regarding FO, LLL, ROM, and PT. No statistically significant differences were found between the lower limbs (operated and non-operated) according to the VFO (p = 0.152) and HFO (p = 0.162). However, from the values of the difference between members for the HFO, 2 individuals were classified as increased HFO, 2 as reduced, and 8 as reconstructed. Statistically significant differences, with lower values in the operated limb, were found in the comparisons between the lower limbs, in relation to the LLL (p = 0.006); hip abduction (p = 0.001), flexion (p = 0.003) and external rotation (p = 0.003) ROM and peak torque for hip flexion (p = 0.002), abduction (p = 0.001), extension (p = 0.001), external rotation (p = 0.002) and internal rotation (p = 0.001)(Table 2).
Table 2. Comparison between operated and non-operated lower limbs for joint range of motion (degrees), normalized muscle torque peaks (Nm/kg), femoral offset (mm), and lower limb length (cm).
| OLL | NOLL | ||
|---|---|---|---|
| LLL | 86.25 (72.00 - 99.00)* | 87.00 (73.00 - 97.00) | |
| Offset | VOF | 30.00 (21.00 - 44.00) | 28.00 (20.00 - 45.00) |
| HOF | 17.50 (10.00 - 22.00) | 17.50 (13.00 - 33.00) | |
| ROM | Flexion | 41.50 (11.00 - 56.00)* | 60.00 (15.00 - 90.00) |
| Extension | 19.50 (10.00 - 26.00) | 19.00 (7.00 - 40.00) | |
| Abduction | 15.00 (8.00 - 32.00)* | 21.50 (14.00 - 40.00) | |
| IR | 15.00 (6.00 - 30.00) | 17.50 (4.00 - 35.00) | |
| ER | 10.00 (3.00 - 26.00)* | 18.00 (1.00 - 37.00) | |
| PT | Flexion | 114.00 (54.00 - 247.00)* | 186.00 (52.00 - 257.00) |
| Extension | 67.00 (30.00 - 173.00)* | 117.00 (37.00 - 323.00) | |
| Abduction | 68.00 (36.00 - 184.00)* | 114.00 (16.00 - 314.00) | |
| IR | 43.00 (29.00 - 137.00)* | 92.00 (36.00 - 202.00) | |
| ER | 73.00 (30.00 - 137.00)* | 109.00 (38.00 - 167.00) | |
HFO: horizontal femoral offset; IR: internal rotation; ER: external rotation; LLL: lower limb length; OLL: operated lower limb; NOLL: non-operated lower limb; PT: peak muscle torque; ROM: range of motion; VFO: vertical femoral offset. Values expressed as median (minimum-maximum). *p > 0.05.
Regarding the correlation between the FO (VFO and HFO) and other variables, some relationships were found, but only the following were statistically significant: VFO and external rotation ROM (r = 0.487; p = 0.021); HFO and external rotators PT (r = −0.508; p = 0.016); and moderate correlations with the TUG test (r = −0.570; p = 0.006) was found when using the difference between the operated and non-operated VFO.
DISCUSSION
Our study correlated the findings of FO with those of hip ROM, hip PT, LLL, and functional capacity, as well as compared the operated and non-operated lower limbs in patients undergoing primary THA surgery. The main findings of this study refer to the scores of functional capacity, the differences between the operated and non-operated limbs, and the correlations between the measurements of the FO and the individuals’ ROM, PT, and functional capacity.
Based on the score of the HHS questionnaire, classified as bad, and the time of 26.41 (12.30-60.38) seconds taken to perform the TUG test, we observed that the individuals in this study showed a reduction in their functional capacity considering the post-operative period evaluated. According to Bohannon, 21 the time taken to perform the TUG test increases with age. In a population aged 60-69 years an 8.1 (7.1-9.0) seconds time should be considered a reference value, and in a population aged 70-79 year, a 9.2 (8.2-10.2) seconds time should be considered normal. Values higher than those of reference suggest disturbances. 21 These alterations may be related to balance, muscle strength, and/or mobility disorders, and are frequently found in individuals in the post-operative period of THA, as is the case of the patients in this study (about 23 days post-operatively). 22 )-( 25
Our findings are in line with those of other studies, which also found positive correlations between the FO and THA patients’ functional capacity. 26 ),( 27 In this study, statistically significant correlations were found between FO and the TUG test, but not with HHS questionnaire. These findings suggest that the greater the difference between the operated and the non-operated lower limb, that is, when there is an increase in VFO in the operated in relation to the non-operated limb, there is a decrease in the time to perform the TUG test and an increase in the score obtained. The association found with the TUG test, but not with HHS, may be related to the fact that the TUG is a dynamic test that comprises movements used in daily life, being more directly involved and dependent on biomechanical issues, since it allows assessing sitting balance, transferring from sitting to standing position, stability in ambulation, and change of direction. 26
Contrary to our findings, Buecking et al. 27 found correlations between the FO and the HHS questionnaire, but not with the TUG test; whereas Hartel et al. 28 found no correlations between FO and functional capacity. It is worth mentioning, however, that those studies differ from ours regarding patients profile; their patients had a higher age average, 27 ),( 28 underwent THA due to femoral neck fracture, 27 ),( 28 and, in some cases, had associated pathologies (dementia, sarcopenia and/or neurological disorders), 28 which makes comparing studies difficult.
The reductions found in the operated limb, compared to the non-operated limb, in relation to hip ROM and PT, can be expected due to the trauma of the surgical procedure, especially in the postoperative period, such as that of our study. According to our knowledge, this study was one of the few to search for correlations between FO and hip ROM in patients with THA. Positive correlations were found, suggesting that an increased VFO could be related to the greater hip external rotation range of motion. In a study by McGrory et al., 7 positive correlations between FO and ROM were also found, but in relation to hip abduction.
Several studies point to a positive correlation between the FO and the muscular strength of the hip abductors, suggesting that a restored or slightly increased FO would bring mechanical advantage to the hip abductor muscles, greater stability and functionality, and smaller reaction force in the hip joint. 5 ),( 8 ),( 9 ),( 23 Our study did not find such correlations, but it was the first to find a correlation between FO and hip external rotators PT. The results suggest that the higher the HFO, the lower the external rotators PT, that is, an increased HFO in the operated limb would result in a lower muscle force generation of external rotors, represented by a lower PT.
It is difficult to compare the results from our study with those found in other studies, as they differ methodologically from ours in some points: exclusively assessing hip abductors muscle strength; 5 ),( 8 ),( 9 ),( 19 longer postoperative period (6 months to 29 years); 5 ),( 9 ),( 19 measuring muscle strength in an isokinetic dynamometer; 5 ),( 9 ),( 19 measuring FO through computed tomography; and using either HFO alone or global FO (sum of HFO and VFO). 5 ),( 8 ),( 9 ),( 19
The main limitations of this study refer to the impossibility of grouping individuals for comparison according to the increase and decrease in FO, due to the sample size; and the use of simple radiographs instead of computed tomography to measure the FO, which may have underestimated the real differences. According to Sariali et al., 29 measurement on radiographs leads to an underestimation of the FO between 3.5-13 mm. We believe, however, that this underestimation does not seem to be relevant in this case, as we used the comparison between the operated and non-operated sides. Furthermore, simple radiography is a low-cost and accessible test that does not expose the patient to greater risks, being widely used to measure FO in the clinical setting.
CONCLUSIONS
Our findings allow us to conclude that changes in the femoral offset measurements (horizontal and vertical), resulting from the surgical procedure of total hip arthroplasty, can influence the patient’s functional capacity, as well as their range of motion and muscle strength of the external rotators of the hip. These results reinforce that biomechanical factors resulting from surgery must be considered in future works.
AKNOWLEDGEMENTS
The authors would like to thank the professionals of the orthopedics and traumatology services at Hospital de Clínicas de Porto Alegre, Hospital Santa Clara at Santa Casa de Misericórdia de Porto Alegre, Hospital Cristo Redentor at Grupo Hospitalar Nossa Senhora da Conceição and Universidade Federal de Ciências da Saúde de Porto Alegre. The authors would also like to thank the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior - Brazil (CAPES) for financing a part of this study (Finance Code 001).
Footnotes
The study was conducted at Universidade Federal de Ciências da Saúde de Porto Alegre.
REFERENCES
- 1.Sizínio H, Xavier R, Pardini AG, Jr, Barros TEP., Filho . Ortopedia e traumatologia: princípios e prática. 4. Porto Alegre: Artmed; 2009. [Google Scholar]
- 2.Onggo JR, Onggo JD, Steiger R, Hau R. The efficacy and safety of inpatient rehabilitation compared with home discharge after hip or knee arthroplasty: a meta-analysis and systematic review. J Arthroplasty. 2019;34(8):1823–1830. doi: 10.1016/j.arth.2019.04.001. [DOI] [PubMed] [Google Scholar]
- 3.Lecerf G, Fessy MH, Philippot R, Massin P, Giraud F, Flecher X. Femoral offset anatomical concept, definition, assessment, implications for preoperative templating and hip arthroplasty. Orthop Traumatol Surg Res. 2009;95(3):210–219. doi: 10.1016/j.otsr.2009.03.010. [DOI] [PubMed] [Google Scholar]
- 4.Asayama I, Naito M, Fujisawa M, Kambe T. Relationship between radiographic measurements of reconstructed hip joint position and the Trendelenburg sign. J Arthroplasty. 2002;17(6):747–751. doi: 10.1054/arth.2002.33552. [DOI] [PubMed] [Google Scholar]
- 5.Asayama I, Chamnongkich S, Simpson KJ, Kinsey TL, Mahoney OM. Reconstructed hip joint position and abductor muscle strength after total hip arthroplasty. J Arthroplasty. 2005;20(4):414–420. doi: 10.1016/j.arth.2004.01.016. [DOI] [PubMed] [Google Scholar]
- 6.Yamaguchi T, Naito M, Asayama I, Ishiko T. Total hip arthroplasty the relationship between posterolateral reconstruction, abductor muscle strength, and femoral offset. J Orthop Surg (Hong Kong) 2004;12(2):164–167. doi: 10.1177/230949900401200205. [DOI] [PubMed] [Google Scholar]
- 7.McGrory BJ, Morrey BF, Cahalan TD, An KN, Cabanela ME. Effect of femoral offset on range of motion and abductor muscle strength after total hip arthroplasty. J Bone Joint Surg Br. 1995;77B(6):865–869. [PubMed] [Google Scholar]
- 8.Mahmood SS, Mukka SS, Crnalic S, Wretenberg P, Sayed-Noord AS. Association between changes in global femoral offset after total hip arthroplasty and function, quality of life, and abductor muscle strength: a prospective cohort study of 222 patients. Acta Orthop. 2016;87(1):36–41. doi: 10.3109/17453674.2015.1091955. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Chamnongkich S, Asayama I, Kinsey TL, Mahoney OM, Simpson KJ. Difference in hip prosthesis femoral offset affects hip abductor strength and gait characteristics during obstacle crossing. Orthop Clin North Am. 2012;43(5):e48–e58. doi: 10.1016/j.ocl.2012.07.008. [DOI] [PubMed] [Google Scholar]
- 10.Tezuka T, Inaba Y, Kobayashi N, Ike H, Kubota S, Kawamura M, Saito T. Effects of hip joint center location and femoral offset on abductor muscle strength after total hip arthroplasty. Mod Rheumatol. 2015;25(4):630–636. doi: 10.3109/14397595.2014.988863. [DOI] [PubMed] [Google Scholar]
- 11.Miashiro EH, Fujiki EN, Yamaguchi EN, Chikude T, Rodrigues LHS, Fontes GM, Rosa FB. Planejamento pré-operatório de artroplastias totais primárias de quadril com o uso de radiografias convencionais. Rev Bras Ortop. 2014;49(2):140–148. doi: 10.1016/j.rboe.2014.03.019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Monteiro GA. Avaliação de flexibilidade: manual de utilização do flexímetro Sanny. São Bernardo do Campo: American Medical do Brasil; 2000. [Google Scholar]
- 13.Poulsen E, Christensen HW, Penny JØ, Overgaard S, Vach W, Hartvigsen J. Reproducibility of range of motion and muscle strength measurements in patients with hip osteoarthritis - a inter-rater study. BMC Musculoskelet Dirsord. 2012;13:242–242. doi: 10.1186/1471-2474-13-242. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Bijur PE, Silver W, Gallagher EJ. Reliability of the visual analog scale for measurement of acute pain. Acad Emerg Med. 2001;8(12):1153–1157. doi: 10.1111/j.1553-2712.2001.tb01132.x. [DOI] [PubMed] [Google Scholar]
- 15.Bookwala J, Harralson TL, Parmelee PA. Effects of pain on functioning and well-being in older adults with osteoarthritis of the knee. Psychol Aging. 2003;18(4):844–850. doi: 10.1037/0882-7974.18.4.844. [DOI] [PubMed] [Google Scholar]
- 16.Blyth FM, March LM, Brnabic AJ, Cousins MJ. Chronic pain and frequent use of health care. Pain. 2004;111(1-2):51–58. doi: 10.1016/j.pain.2004.05.020. [DOI] [PubMed] [Google Scholar]
- 17.Patrizzi LJ, Vilaça KHC, Takata ET, Trigueiro G. Análise pré e pós-operatória da capacidade funcional e qualidade de vida de pacientes portadores de osteoartrose de quadril submetidos à artroplastia total. Rev Bras Reumatol. 2004;44(3):185–191. [Google Scholar]
- 18.Clement ND, Patrick-Patel RS, MacDonald D, Breusch SJ. Total hip replacement: increasing femoral offset improves functional outcome. Arch Orthop Trauma Surg. 2016;136(9):1317–1323. doi: 10.1007/s00402-016-2527-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Sato H, Maezawa K, Gomi M, Kajihara H, Hayashi A, Maruyama Y. Effect of femoral offset and limb length discrepancy on hip joint muscle strength and gait trajectory after total hip arthroplasty. Gait Posture. 2020;77:276–282. doi: 10.1016/j.gaitpost.2020.02.008. [DOI] [PubMed] [Google Scholar]
- 20.Fleiss JL, Levin B, Paik MC. Statistical methods for rates and proportions. 3. Hoboken: Wiley; 2003. [Google Scholar]
- 21.Bohannon RW. Reference values for the timed up and go test: a descriptive meta-analysis. J Geriatr Phys Ther. 2006;29(2):64–68. doi: 10.1519/00139143-200608000-00004. [DOI] [PubMed] [Google Scholar]
- 22.Frost KL, Bertocci GE, Wassinger CA, Munin MC, Burdett RG, Fitzgerald SG. Isometric performance following total hip arthroplasty and rehabilitation. J Rehabil Res Dev. 2006;43(4):435–444. doi: 10.1682/jrrd.2005.06.0100. [DOI] [PubMed] [Google Scholar]
- 23.Skoffer B, Dalgas U, Mechlenburg I. Progressive resistance training before and after total hip and knee arthroplasty: a systematic review. Clin Rehabil. 2015;29(1):14–29. doi: 10.1177/0269215514537093. [DOI] [PubMed] [Google Scholar]
- 24.Shih CH, Du YK, Lin YH, Wu CC. Muscular recovery around the hip joint after total hip arthroplasty. Clin Orthop Relat Res. 1994;(302):115–120. [PubMed] [Google Scholar]
- 25.Sicard-Rosenbaum L, Light KE, Behrman AL. Gait, lower extremity strength, and self-assessed mobility after hip arthroplasty. J Gerontol A Biol Sci Med Sci. 2002;57(1):47–51. doi: 10.1093/gerona/57.1.m47. [DOI] [PubMed] [Google Scholar]
- 26.Cassidy KA, Noticewala MS, Macaulay W, Lee JH, Geller JA. Effect of femoral offset on pain and function after total hip arthroplasty. J Arthroplasty. 2012;27(10):1863–1869. doi: 10.1016/j.arth.2012.05.001. [DOI] [PubMed] [Google Scholar]
- 27.Buecking B, Boese CK, Bergmeister VA, Frink M, Ruchholtz S, Lechler P. Functional implications of femoral offset following hemiarthroplasty for displaced femoral neck fracture. Int Orthop. 2016;40(7):1515–1521. doi: 10.1007/s00264-015-2828-1. [DOI] [PubMed] [Google Scholar]
- 28.Hartel M, Arndt M, Eulenburg CZ, Petersen JP, Rueger JM, Hoffmann M. Restoration of hip architecture with bipolar hemiarthroplasty in the elderly does it affect early functional outcome? Arch Othop Trauma Surg. 2014;134(1):31–38. doi: 10.1007/s00402-013-1878-3. [DOI] [PubMed] [Google Scholar]
- 29.Sariali E, Mouttet A, Pasquier G, Durante E. Three-dimensional hip anatomy in osteoarthritis: analysis of the femoral offset. J Arthroplasty. 2009;24(6):990–997. doi: 10.1016/j.arth.2008.04.031. [DOI] [PubMed] [Google Scholar]


