Abstract
Background
Mounting evidence supports the effective acquisition of skills through simulation-based training including intubation skills of neonates. Our aim is to compare the effect of using high- versus low-fidelity mannequin simulation-based training on the acquisition and retention of neonatal intubation skills by junior pediatric residents.
Methods
Randomized controlled trial involving first- and second-year pediatric residents from two centers in Jeddah, Saudi Arabia.
Results
Twenty-eight junior pediatric residents (12 low- and 16 high-fidelity mannequins) completed the study. A significantly greater number of residents achieved and retained the required skills after completing the training course in both arms. There was no significant difference in the achieved skills between residents trained on high- versus low-fidelity mannequins at the baseline, immediately after training, and at 6–9 months after training.
Conclusion
Simulation-based training resulted in improving pediatric residents’ intubation skills regardless of the level of fidelity.
Keywords: Simulation, Fidelity, Intubation, Neonate
Background
Approximately 10% of newborns require some assistance to begin breathing at birth, and approximately 1% need extensive resuscitative measures to survive [1]. Optimal care provided during the first few minutes of life plays a significant role in reducing neonatal morbidity and mortality [2, 3]. Therefore, the Accreditation Council for Graduate Medical Education (ACGME) currently mandates the completion of formal training via the neonatal resuscitation program (NRP) by all pediatric residents [4]. Neonatal resuscitation is defined as the set of interventions at the time of birth to support the establishment of breathing and circulation [5].
Neonatal endotracheal intubation is an essential skill that every pediatrician must be trained to perform. Neonates are often exposed to more than one intubation attempt before the endotracheal tube is successfully placed and that is not without adverse effects [6]. Moreover, residents’ opportunities to intubate a neonate have been shown to decline and therefore simulation-based training was suggested [7–9].
Fidelity in simulation-based training is classified into low-, medium-, and high-fidelity simulators [10–12]. The term ‘fidelity’ is used to refer to the degree of realism of a simulation. Low-fidelity simulator (LFS) mannequins allow practitioners to demonstrate basic knowledge and technical and behavioral skills with verbal prompts from instructors. A LFS mannequin may or may not include the ability for intubation, chest rise, or electrocardiographic tracings. Medium-fidelity simulators (MFSs) produce physiological responses on a computer screen but lack various cues essential for participants to engage in the simulated scenario. For example, a medium-fidelity mannequin can produce breath sounds but no corresponding chest rise. High-fidelity simulators (HFSs) provide the trainee with the cues necessary to interact with the patient as they would in a real clinical environment. High-fidelity simulators can demonstrate physiologic signals (e.g., heart sounds, breath sounds, pulses, oxygen saturation and blood pressure) for the trainee to act upon. In response to the changing physiologic feedback received from the mannequin, the trainee is challenged to apply the correct interventions such as the administration of oxygen, endotracheal intubation or chest drain insertion to improve the condition of the simulated mannequin.
High-fidelity simulation is a rapidly developing technology that has been in use for years in a variety of medical fields. A growing body of evidence supports the effective acquisition and retention of technical skills through HFS [13–15]. However, there are few studies describing the use of HFS in teaching neonatal resuscitation.
Our research question was the following: Among junior (first year) pediatric residents, would HFS training result in better neonatal intubation technical skills compared to LFS training? Answering this question can inform the supporting and financing bodies to whether selecting a training method that is more costly (HFS) is justified by a better outcome of improving pediatric trainees’ neonatal intubation skills and the retention of these skills towards enhanced patient care.
Methods
This is a randomized controlled trial that was approved by the King Abdulaziz University Hospital (KAUH) Hospital’s Ethical Review Board (Reference No 471-lE) and registered in the ISCRTN registry (ISRCTN16251230) 21/03/2018. The study was carried out in accordance with the CONSORT 2010 statement guidelines for reporting parallel group randomized trials [16]. Our primary objective was to determine the effectiveness of using HFSs compared to LFSs in improving the technical skills to successfully intubate a neonate, defined as the passage of the endotracheal tube (ET) beyond the vocal cords. The secondary objectives included determining whether using HFSs will result in a shorter time taken to intubate a neonate and better retention of technical neonatal intubation skills compared to LFSs.
Population
The study participants were all pediatric residents in their first year of postgraduate training in pediatrics recruited from two hospitals in Jeddah, Kingdom of Saudi Arabia (KSA), and agreed to participate in the study. A total of 28 pediatric residents from KAUH and Maternity and Children Hospital (MCH) were included in the study after signing an informed consent form. The pediatric residency program in Saudi Arabia is a 4-year National Training Program during which pediatric residents rotate through the Neonatal Intensive Care Unit (NICU) for 2 months in the first year and one month in the second, third and fourth years of their program. NRP training is not a requirement for pediatric residency programs in the two participating hospitals. Junior residents acquire skills to intubate a neonate through rotating in NICU in which a neonatal specialist or fellow will be present for all neonatal intubation attempts. There was no didactic intubation training or structured intubation apprenticeship in NICU in either hospital.
Intervention
After recruitment, residents were randomly assigned to training on either a high-fidelity or low-fidelity mannequin. The assignment was achieved using a computer-generated random number that was placed in sequentially numbered concealed opaque envelopes by one of the simulation center organizers. The participating residents were first assessed at the baseline on their allocated mannequin, where they were asked to manage a standardized simulated scenario of a neonate requiring intubation. A training course was designed to improve the intubation skills of pediatric residents using the assigned mannequins and delivered by two NRP providers with more than ten-year experience in neonatology. The high-fidelity mannequin (SimBaby, Laerdal Medical Corporation, USA) is an advanced infant patient simulator with realistic airway anatomy and clinical functionality. It features airway opening by appropriate maneuvers, suctioning motion, anatomical landmarks of oropharyngeal and nasopharyngeal airways, and chest rise and oxygen saturation changes in response to intervention. The mannequin utilizes software-based medical model that was programmed to display changes in physical findings in response to progressing medical circumstances. The resident will have to continually evaluate the mannequin’s condition rather than relying on cues provided by an instructor [17, 18]. The low-fidelity mannequin is a standard plastic mannequin (ALS Baby, Laerdal Medical Corporation, USA) that allows passing ET tube and demonstrates chest rises in response to successful intubation. It does not, however, feature anatomical landmarks of the neonatal airway or give physiological cues such as oxygen saturation, heart rate and changes in CO2 detector color [17]. A one-hour introductory lecture outlining the indications for intubations, anatomical landmarks and steps taken to prepare for, perform and confirm successful intubation was given to both groups by one of the physicians assigned for training. The residents then had the chance to practice the steps of successful intubation on the assigned mannequin 2–3 times in the presence of the other residents in the group. Constructive feedback was provided to trainees in both groups after a successful intubation attempt. Each participant was re-evaluated using a standardized simulated scenario of intubating a neonate after training using a high-fidelity mannequin.
Outcome
Two trained assessors who were certified NRP instructors independently evaluated the technical neonatal intubation skills of pediatric residents using a checklist of appropriate and inappropriate actions derived from the published literature at the baseline and both at the end of the training course and 6–9 months after completion of the course. The evaluators were blinded to the training intervention and different from the physicians who trained the residents. The technical skills were evaluated using a 13-item binary intubation checklist that was used in a previous study evaluating the skills needed to intubate a neonate, including preparing for the intubation, technical skills for positioning and inserting the endotracheal tube and confirming successful intubation [19]. The checklist scores in the study had an interrater reliability of 0.88 and correlated positively with the global rating scores (Spearman’s coefficient 0.68). The authors of the study gave permission to use their checklist. The time taken to intubate and ensure correct placement was documented (using a stopwatch) from the start of the intubation attempt until the trainee presented evidence of correct placement. A 5-point Likert global rating score (1 being the lowest and 5 being the highest score) was utilized by the evaluators to provide an overall assessment of resident’s capability to perform a neonatal intubation.
Data analysis
IPM SPSS 22.0 (SPSS Inc, Chicago, IL) was used for the data analyses. Normally distributed data are presented as the mean ± SD and were compared between two groups using Student’s t-test. Repeated measures analysis of variance (ANOVA) was applied when the three periods of assessment were compared. Categorical parameters are presented as frequencies and percentages and were compared by applying the chi-squared test. The level of significance was specified at p < 0.05.
Results
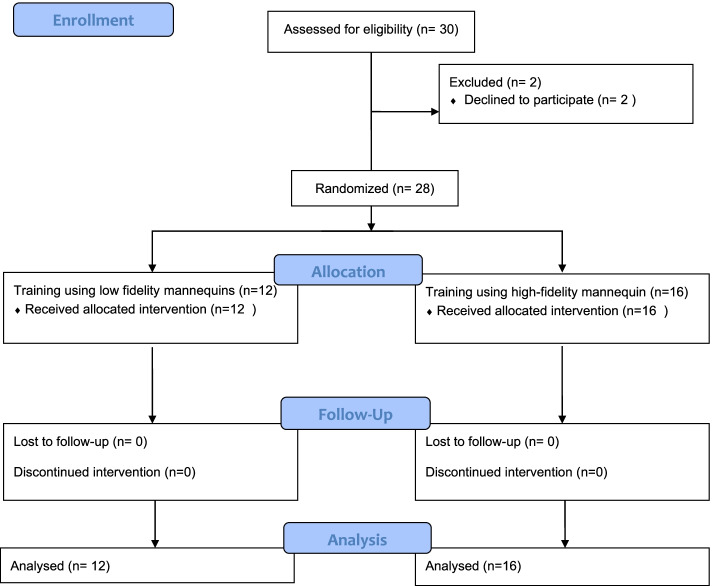
Thirty residents were invited to participate in the study (Fig. 1). Twenty-eight residents participated and completed the study. Twelve residents were allocated to the low-fidelity arm and sixteen to the high-fidelity arm (Fig. 2). There was no difference between participants in either arm regarding age, sex, training center, NRP certification and whether they intubated a neonate before the training course (Table 1). A significantly greater number of residents achieved the required skills immediately after the training course in both arms (Table 2). In addition, the achieved skills were retained when the residents were tested at 6–9 months after training (Table 2). There was no significant difference between the achieved skills between residents trained on high-fidelity mannequins compared to those trained on low-fidelity mannequins at the baseline, immediately after training, and at 6–9 months after training (Table 3).
Fig. 1.
CONSORT Diagram for the Randomized Controlled Trial (RCT)
Fig. 2.
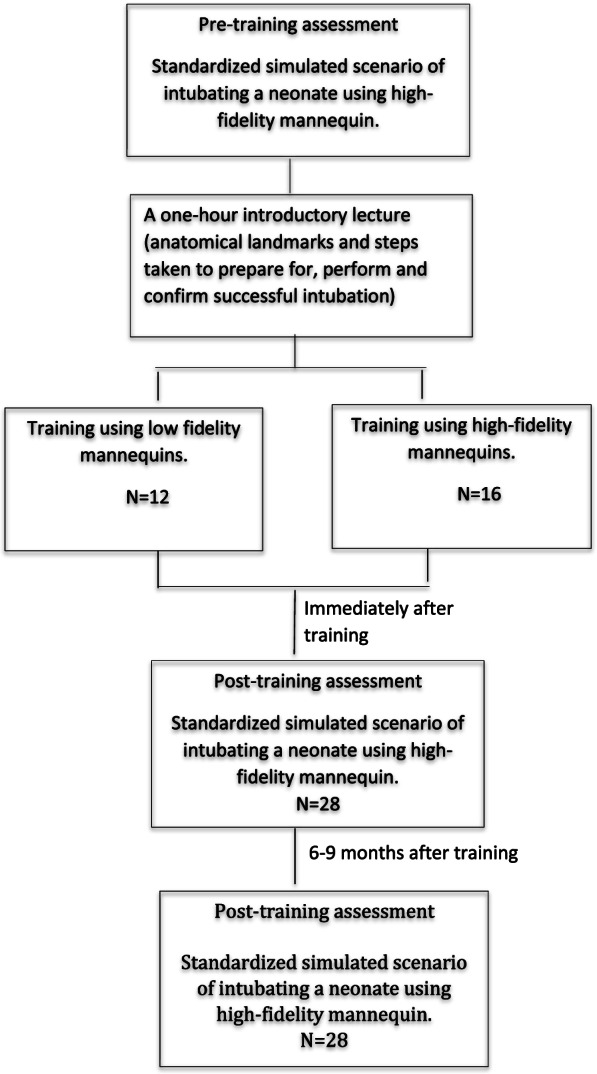
Flow diagram of participated residents
Table 1.
Demographic characteristics of groups at baseline
| Low fidelity Mannequin (N = 12) |
High fidelity Mannequin (N = 16) |
|
|---|---|---|
| Age (years) | 25.6 (0.67) | 26 (1.9) |
| Male | 4 (33.3) | 2 (12.5) |
| Female | 8 (66.7) | 14 (87.5) |
| NRP | 2 (16.7) | 5 (31.3) |
| Intubation before training | 1 (8.3) | 2 (12.5) |
| Centre 1 | 5 (41.7) | 8 (50.0) |
| Centre 2 | 7 (58.3) | 8 (50.0) |
Data are presented as n (%) or mean (SD)
Table 2.
Comparison between intubation skills at baseline, immediately and 6–9 months after training for each training method
| Low fidelity (N = 12) |
High fidelity (N = 16) |
|||||||
|---|---|---|---|---|---|---|---|---|
| Baseline | Immediately after training | 6–9 months after training |
P-value | Baseline | Immediately after training | 6–9 months after training |
P-value | |
| Select appropriate size tube | 1 (8.3) | 11 (91.7) | 12 (100) | 0.000 | 3 (18.8) | 16 (100) | 12 (75.0) | 0.000 |
| Ensures availability of all needed equipment | 0 | 12 (100) | 9 (75.0) | 0.000 | 0 | 16 (100) | 9 (56.3) | 0.000 |
| Pre-oxygenate | 1 (8.3) | 8 (6.7) | 5(41.7) | 0.013 | 1 (6.3) | 7 (43.8) | 10 (62.5) | 0.004 |
| Position the head | 1 (8.3) | 6 (50) | 6 (50.0) | 0.049 | 0 | 10 (62.5) | 10 (62.5) | 0.000 |
| Insertion of blade correctly using left hand | 5 (41.1) | 7 (58.3) | 9 (75.0) | 0.254 | 5 (31.3) | 14 (87.5) | 12 (75.0) | 0.002 |
| Lifts handle forward | 3 (25) | 4 (33.3) | 8 (66.7) | 0.091 | 1 (6.3) | 8 (50.0) | 5 (31.3) | 0.024 |
| Visualization of vocal cords | 2 (16.7) | 7 (58.3) | 10 (35.7) | 0.004 | 2 (12.5) | 8 (50.0) | 7(43.8) | 0.059 |
| Suction appropriately | 12 (100) | 8 (66.7) | 5 (41.7) | 0.003 | 16(100) | 4 (25.0) | 7 (43.8) | 0.013 |
| Pass tube smoothly | 1 (8.3) | 8 (66.7) | 4 (33.3) | 0.012 | 1 (6.3) | 8 (50.0) | 5 (31.3) | 0.024 |
| Check position of tube | 0 | 7 (58.3) | 3 (25.0) | 0.006 | 3 (18.3) | 7 (43.8) | 7 (43.8) | 0.233 |
| Check placement by auscultation | 4 (33.3) | 9 (75.0) | 5 (41.7) | 0.097 | 5 (31.3) | 13 (81.3) | 10 (62.5) | 0.015 |
| Successful intubation | 2 (16.7) | 6 (50) | 4 (33.3) | 0.223 | 2 (12.5) | 7 (43.8) | 9 (56.3) | 0.083 |
| Overall Score | 1.25 (0.45) | 3.08 (1.24) | 3.33 (1.55) | 0.000 | 1.19 (0.54) | 2.75 (0.86) | 3.25 (1.0) | 0.000 |
| Duration of intubation (seconds) | 51.1 (22.9) | 51.8 (48.55) | 36.2 (13.14) | 0.344 | 46.38 (19.9) | 34.6 (19.27) | 42.8 (14.8) | 0.126 |
Data are presented as n (%) or mean (SD)
Table 3.
Comparison between the two training methods in the achieved skills for intubating a neonate at baseline, immediately after training and 6–9 months after
| Baseline | Immediately after training | 6–9 months after training | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Low fidelity (N = 12) |
High fidelity (N = 16) |
P-value | Low fidelity (N = 12) |
High fidelity (N = 16) |
P-value | Low fidelity (N = 12) |
High fidelity (N = 16) |
P-value | |
| Select appropriate size tube | 1 (8.3) | 3 (18.8) | 0.436 | 11 (91.7) | 16 (100) | 0.240 | 12 (100) | 12 (75) | 0.061 |
| Ensures availability of all needed equipment | 0 | 0 | 12 (100) | 16(100) | 0.595 | 9 (75.0) | 9 (56) | 0.306 | |
| Pre-oxygenate | 1 (8.3) | 1 (6.3) | 0.832 | 8 (6.7) | 7 (43.8) | 0.229 | 5 (41.7) | 10 (62.5) | 0.274 |
| Position the head | 1 (8.3) | 0 | 0.240 | 6 (50.0) | 10 (62.5) | 0.508 | 6 (50.0) | 10 (62.5) | 0.508 |
| Insertion of blade correctly using left hand | 5 (41) | 5 (31.3) | 0.569 | 7 (58.3) | 14 (87.5) | 0.078 | 9 (75.0) | 12 (75) | 1.000 |
| Lifts handle forward | 3 (25) | 1 (6.3) | 0.161 | 4 (33.3) | 8 (50.0) | 0.378 | 8 (66.7) | 5 (31.3) | 0.063 |
| Visualization of vocal cords | 2 (16.7) | 2 (12.5) | 0.755 | 7 (58.3) | 8 (50.0) | 0.662 | 10 (35.7) | 7 (43.8) | 0.034 |
| Suction appropriately | 12 (100) | 16 (100) | NA | 8 (66.7) | 4 (25.0) | 0.027 | 5 (41.7) | 7 (43.8) | 0.912 |
| Pass tube smoothly | 1 (8.3) | 1 (6.3) | 0.832 | 8 (66.7) | 8 (50.0) | 0.378 | 4 (33.3) | 5 (31.3) | 0.907 |
| Check position of tube | 0 | 3 (18.3) | 0.112 | 7 (58.3) | 7 (43.8) | 0.445 | 3 (25.0) | 7 (43.8) | 0.306 |
| Check placement by auscultation | 4 (33.3) | 5 (31.3) | 0.907 | 9 (75.0) | 13(81.3) | 0.690 | 5 (41.7) | 10(62.5) | 0.274 |
| Successful intubation | 2 (16.7) | 2 (12.5) | 0.755 | 6 (50.0) | 7 (43.8) | 0.743 | 4 (33.3) | 9 (56.3) | 0.393 |
| Overall score | 1.25 (0.5) | 1.2 (0.5) | 0.749 | 3.1 (1.2) | 2.8(0.9) | 0.407 | 3.3 (1.6) | 3.3(1.0) | 0.840 |
| Duration of intubation (seconds) | 51.1(22.9) | 46.4(19.9) | 0.567 | 51.8 (48.6) | 34.6(19.3) | 0.205 | 36.2(13.1) | 42.8(14.8) | 0.229 |
Data are presented as n (%) or mean (SD)
Discussion
We found no difference in the effect of high- versus low-fidelity mannequins on the acquisition and retention of technical skills necessary to intubate a neonate by junior pediatric residents from the two academic centers. However, we concluded that training junior pediatric residents using either simulator mannequins resulted in improved intubation skills both immediately and 6–9 months after training.
Experiential learning methods, as the case in simulation-based training, were shown to result in deeper learning and better retention [13, 14]. Experiential learning theory proposes that knowledge is generated through the transformation of experience [20]. In his work on experiential learning, Kolbe described how the learner moves through four stages of adaptive learning modes: more concrete experience, reflective observation, abstract conceptualization, and active experimentation. Dewey was the first to introduce the concept of experience plus reflection equals learning that was considered to be the foundation of simulation-based learning [15]. The quality and amount of active experimentation is judged by the degree to which it reproduces reality. Experiential learning helps individuals understand their strengths and weaknesses; gives the opportunity to apply skills for assessment, examination and evaluation and encourages critical thinking and the development of proficiency in an environment where errors do not have dire consequences. In theory, through experiential learning, trainees retain not only knowledge but also its practical application and how to use it when needed. As a result, novice trainees will move towards becoming experts.
Evidence supporting the use of HFS in neonatal resuscitation and the associated acquisition of technical skills does not agree with the evidence from other medical fields. Similar to our results, Campbell et al. reported that although pediatric residents randomly assigned to the HFS gave better satisfaction scores than those assigned to the LFS, they did not have improved written scores or intubation times [13]. In a small randomized controlled trial of ten second- and third-year pediatric residents, HFS training did not result in a better intubation technique or actual procedural success [20]. More recently, Finan et al. compared the effects of HFS versus LFS in a randomized trial of sixteen neonatal fellows and found no difference in stress measures between the two modalities [21]. Regarding the retention of the learned skills in simulation-based training, studies have shown degradation of the technical skills acquired in certification courses by health professionals over time, which can have significant effects on patient outcomes [19, 22–25].
We would like to acknowledge some of the limitations of this study. The small sample size limits the significance and generalizability of our study as it was a convenience sample of all junior pediatric residents from the two centers which agreed to participate. The high-fidelity mannequin was used both to train and to assess; therefore, additional training exposure might have introduced additional benefits, but that was not statistically evident. Moreover, the residents were allowed to practice 2–3 times on the simulator which might not be enough for robust skill acquisition. We did not record the number of practice repetitions residents did before their evaluation session which may have impacted the results of this study. Furthermore, residents’ experience during the lag time between the training course and assessment of the retention of learned intubation skills might differ as they do not all rotate through the NICU at a fixed time, which might expose some of them to more intubation trials than others. We recorded the intubation trials before the training course but not before the assessment of the retention of skills. We minimized the bias by structuring the training course in a way that only the type of mannequin was the changing variable and blinded the assessors to the intervention applied to strengthen the internal validity of the study. Additionally, the effect on improving noncognitive skills such as attentiveness, perseverance, and teamwork was not part of the current study. Although simulation teaching has been demonstrated to lead to improved educational outcomes, transfer of these skills from simulation to the real clinical world, and to the benefits of clinical patient outcomes will need to be studied.
In conclusion, simulation-based training resulted in improving pediatric residents’ intubation skills regardless of the level of fidelity. The benefit of training on a high-fidelity mannequin will need to be further assessed in real-life intubations to determine its effect on the management and clinical outcome of neonatal intubation.
Acknowledgements
The authors would like to thank the residents who participated and completed the study and the Clinical Skills and Simulation Centre staff at King Abdulaziz University (KAU-CSSC) who helped conduct the study.
Abbreviations
- ACGME
Accreditation Council for Graduate Medical Education
- ANOVA
Analysis of variance
- ET
Endotracheal tube
- HFS
High-fidelity simulator
- KAUH
King Abdulaziz University Hospital
- KSA
Kingdom of Saudi Arabia
- LFS
Low-fidelity simulator
- NCH
Maternity and Children Hospital
- MFS
Medium fidelity simulator
- NICU
Neonatal Intensive Care Unit
- NRP
Neonatal Resuscitation Program
Authors’ contributions
HA, AA, AB, and MB contributed to the conception and design of the work; HS and GA the acquisition, analysis, interpretation of data; HA, AA, AB, and MB have drafted the work substantively revised it. All authors have approved the submitted version and have agreed both to be personally accountable for the author's own contributions and to ensure that questions related to the accuracy or integrity of any part of the work are appropriately investigated.
Funding
No funding was received for this study.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Declarations
Ethics approval and consent to participate
The study was approved by the King Abdulaziz University Hospital (KAUH) Hospital’s Ethical Review Board (Reference No 471-lE) and registered in the ISCRTN registry (ISRCTN16251230). Informed written consent was obtained from all residents that confirmed their participation and ensured that confidential information will not be shared. The study was carried out in accordance with the Declaration of Helsinki.
Consent for publication
Not applicable.
Competing interests
The authors have no conflicts of interest relevant to this article.
Footnotes
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.J WGZ. Textbook of Neonatal Resucitation (NRP). 7th Ed. ed2016.
- 2.Duran R, Aladag N, Vatansever U, Sut N, Acunas B. The impact of Neonatal Resuscitation Program courses on mortality and morbidity of newborn infants with perinatal asphyxia. Brain Dev. 2008;30(1):43–46. doi: 10.1016/j.braindev.2007.05.009. [DOI] [PubMed] [Google Scholar]
- 3.Patel D, Piotrowski ZH, Nelson MR, Sabich R. Effect of a statewide neonatal resuscitation training program on Apgar scores among high-risk neonates in Illinois. Pediatrics. 2001;107(4):648–655. doi: 10.1542/peds.107.4.648. [DOI] [PubMed] [Google Scholar]
- 4.Education ACfGM. 2021 [Available from: https://www.acgme.org/specialties/pediatrics/overview/.
- 5.Black RE, Cousens S, Johnson HL, Lawn JE, Rudan I, Bassani DG, et al. Global, regional, and national causes of child mortality in 2008: a systematic analysis. Lancet. 2010;375(9730):1969–1987. doi: 10.1016/S0140-6736(10)60549-1. [DOI] [PubMed] [Google Scholar]
- 6.Foglia EE, Ades A, Sawyer T, et al. Neonatal Intubation Practice and Outcomes: An International Registry Study. Pediatrics. 2019;143(1):e20180902. [DOI] [PMC free article] [PubMed]
- 7.Gozzo YF, Cummings CL, Chapman RL, Bizzarro MJ, Mercurio MR. Who is performing medical procedures in the neonatal intensive care unit? J Perinatol. 2011;31(3):206–211. doi: 10.1038/jp.2010.121. [DOI] [PubMed] [Google Scholar]
- 8.Downes KJ, Narendran V, Meinzen-Derr J, McClanahan S, Akinbi HT. The lost art of intubation: assessing opportunities for residents to perform neonatal intubation. J Perinatol. 2012;32(12):927–932. doi: 10.1038/jp.2012.17. [DOI] [PubMed] [Google Scholar]
- 9.Lopreiato JO, Sawyer T. Simulation-based medical education in pediatrics. Acad Pediatr. 2015;15(2):134–142. doi: 10.1016/j.acap.2014.10.010. [DOI] [PubMed] [Google Scholar]
- 10.Maran NJ, Glavin RJ. Low- to high-fidelity simulation - a continuum of medical education? Med Educ. 2003;37(Suppl 1):22–28. doi: 10.1046/j.1365-2923.37.s1.9.x. [DOI] [PubMed] [Google Scholar]
- 11.Epps C, White M, Tofil N. Mannequin Based Simulators. In A. I. Levine, S., DeMaria, A. Schwartz, & A. Sim (Eds) New York, NY: Springer; 2013. [Google Scholar]
- 12.Palaganas J, Ulrich B, Mancini B. Mastering simulation: A handbook for success. : Sigma. 2 2020. [Google Scholar]
- 13.Campbell DM, Barozzino T, Farrugia M, Sgro M. High-fidelity simulation in neonatal resuscitation. Paediatr Child Health. 2009;14(1):19–23. doi: 10.1093/pch/14.1.19. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Thomas EJ, Williams AL, Reichman EF, Lasky RE, Crandell S, Taggart WR. Team training in the neonatal resuscitation program for interns: teamwork and quality of resuscitations. Pediatrics. 2010;125(3):539–546. doi: 10.1542/peds.2009-1635. [DOI] [PubMed] [Google Scholar]
- 15.Yaeger KA, Halamek LP, Coyle M, Murphy A, Anderson J, Boyle K, et al. High-fidelity simulation-based training in neonatal nursing. Adv Neonatal Care. 2004;4(6):326–331. doi: 10.1016/j.adnc.2004.09.009. [DOI] [PubMed] [Google Scholar]
- 16.Schulz KF, Altman DG, Moher D, Group C CONSORT 2010 statement: updated guidelines for reporting parallel group randomized trials. Ann Intern Med. 2010;152(11):726–732. doi: 10.7326/0003-4819-152-11-201006010-00232. [DOI] [PubMed] [Google Scholar]
- 17.Lopreiato JOE, Downing, D., Gammon, W., Lioce, L., Sittner, B., Slot, V., Spain, A. E. (Associate Eds.), and the Terminology & Concepts Working Group. Healthcare simulation dictionary 2016 [Available from: Retrieved from http://www.ssih.org/dictionary. .
- 18.Deutsch ES. High-fidelity patient simulation mannequins to facilitate aerodigestive endoscopy training. Arch Otolaryngol Head Neck Surg. 2008;134(6):625–629. doi: 10.1001/archotol.134.6.625. [DOI] [PubMed] [Google Scholar]
- 19.Bismilla Z, Finan E, McNamara PJ, LeBlanc V, Jefferies A, Whyte H. Failure of pediatric and neonatal trainees to meet Canadian Neonatal Resuscitation Program standards for neonatal intubation. J Perinatol. 2010;30(3):182–187. doi: 10.1038/jp.2009.152. [DOI] [PubMed] [Google Scholar]
- 20.Sharara-Chami R, Taher S, Kaddoum R, Tamim H, Charafeddine L. Simulation training in endotracheal intubation in a pediatric residency. Middle East J Anaesthesiol. 2014;22(5):477–485. [PubMed] [Google Scholar]
- 21.Finan E, Bismilla Z, Whyte HE, Leblanc V, McNamara PJ. High-fidelity simulator technology may not be superior to traditional low-fidelity equipment for neonatal resuscitation training. J Perinatol. 2012;32(4):287–292. doi: 10.1038/jp.2011.96. [DOI] [PubMed] [Google Scholar]
- 22.Smith KK, Gilcreast D, Pierce K. Evaluation of staff's retention of ACLS and BLS skills. Resuscitation. 2008;78(1):59–65. doi: 10.1016/j.resuscitation.2008.02.007. [DOI] [PubMed] [Google Scholar]
- 23.Kaczorowski J, Levitt C, Hammond M, Outerbridge E, Grad R, Rothman A, et al. Retention of neonatal resuscitation skills and knowledge: a randomized controlled trial. Fam Med. 1998;30(10):705–711. [PubMed] [Google Scholar]
- 24.Grant EC, Marczinski CA, Menon K. Using pediatric advanced life support in pediatric residency training: does the curriculum need resuscitation? Pediatr Crit Care Med. 2007;8(5):433–439. doi: 10.1097/01.PCC.0000282044.78432.0B. [DOI] [PubMed] [Google Scholar]
- 25.Hunt EA, Fiedor-Hamilton M, Eppich WJ. Resuscitation education: narrowing the gap between evidence-based resuscitation guidelines and performance using best educational practices. Pediatr Clin North Am. 2008;55(4):1025–50, xii. doi: 10.1016/j.pcl.2008.04.007. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.