Abstract
Background:
The number of lumbar spine surgery increased in recent years. Spinal instrumentation surgery was an integral component in the treatment of spinal pathologies, which can cause surgical site infection (SSI). Surgical site infections (SSIs) are the leading cause of mortality and morbidity after spinal instrumentation surgery. The management of SSI was implant retention and removal is still unclear.
Objective:
The objective of this literature is to systematically review the implant removal and retention method for SSI management after spinal instrumentation surgery.
Methods:
We searched in PubMed and ScienceDirect for cohort and randomized control trial studies in English, published between 2002 and 2022, which had data on patients with spinal instrumentation surgery. The underlying disease, comorbidities, common bacteria, type of infection, the onset of infection, implant removal, and retention percentage and recommendation were analyzed. Bias analysis using Newcastle-Ottawa Quality Assessment.
Results:
We included 15 studies with a total sample were 2.584 with an average of age 15 to 66 years old. The most common organism detected were S. Aureus, MRSA, and S. Epidermis. The most common surgical procedure indications were degenerative followed by scoliosis. Implant removal and retention rate were 0-100% and 0-90,32% respectively. Implant removal is more frequently used in patients after spinal instrumentation surgery than the implant retention method.
Conclusion:
Implant retention can be performed in case of SSI is < 3 months after surgery. Implant removal is recommended if the incidence of SSI is > 3 months. Empirical antibiotics therapy is necessary to reduce the possibility of implant removal after debridement. Further studies on the effect of implant removal and retention in patients on infection recurrence, pain, and quality of life of patients are needed.
Keywords: implant, removal, retention, SSI, spinal instrumentation surgery.
1. BACKGROUND
The rate of spine surgery increased by 54%, from 78 to 120 per 100.000, from 1999 to 2013. Among elderly people over 75 years, lumbar surgery increased by a factor of five during the 15-year period. The rates of complications were low, but increased from 0.7% in 1999 to 2.4% in 2013 (1). Instrumentation, now an integral component in the treatment of numerous spinal pathologies, is correlated with a 2-20% infection rate (2)implants must be removed following instrumented PSF. Indications for removal include infection and late operative site pain. Previously, it has been thought that there was little morbidity associated with implant removal in the presence of a solid fusion. However, recent studies have reported loss of coronal correction after implant removal in patients who had a PSF for adolescent idiopathic scoliosis. Few long-term studies have assessed the clinical or radiographic results of complete implant removal after PSF. METHODS: We identified 56 patients who had undergone PSF for idiopathic scoliosis and subsequently had complete removal of all instrumentation. None of these patients had a pseudarthrosis at the time of implant removal. After IRB approval, 43 of 56 (77%. The ability to manage postoperative wound infections has become more critical and challenging, as they are positively associated with extended hospitalizations, increased morbidity and healthcare costs, poorer long-term outcomes, and greater dissatisfaction with the initial operative procedure (3). Other research showed that the incidence of wound infection after spinal surgery without instrumentation is relatively low (4)and 65 were treated percutaneously. A standardized MRI protocol using axial T1-weighted sequences was performed at a minimum 1-year follow-up after implant removal. Two independent observers measured cross-sectional areas (CSAs, in cm(2. However, using spinal instrumentation clearly increases the risk for postoperative soft tissue infections, and recent estimates from retrospective reviews range from 2.1% to 8.5% (5)arthrodesis, use of spinal instrumentation, age, obesity, diabetes, tobacco use, operating-room environment and estimated blood loss are well established in the literature to affect the risk of infection. Infection after spine surgery with instrumentation is becoming a common pathology. The reported infection rates range from 0.7% to 11.9%, depending on the diagnosis and complexity of the procedure. Besides operative factors, patient characteristics could also account for increased infection rates. These infections after instrumented spinal fusion are particularly difficult to manage due to the implanted, and possibly infected, instrumentation. Because the medical, economic and social costs of SSI after spinal instrumentation are enormous, any significant reduction in risks will pay dividends. The goal of this literature review was to analyse risk factors, causative organisms, diagnostic elements (both clinical and biological. Whereas the incidence of surgical site infection (SSI) after adult spine surgery knows a wide variety from 0.7% to 12.0% cause health care costs, patient morbidity and mortality will increase (6)retrospective cohort analysis. OBJECTIVE: To evaluate the presentation, etiology, and treatment of surgical site infections (SSI.
Since implantable devices are highly susceptible to bacterial colonization even low virulent bacteria can cause infection and recurrent infections due to biofilms, making them difficult to detect and eradicate (7). One way to reduce infection is to remove the spinal instruments. But, the incidence of complete removal after surgery for remains unclear (8). In instrumented spine surgery especially implant retention is discussed ambiguously due to potential loss of correction even in infused patients (7).
2. OBJECTIVE
The purpose of this study was to determine the incidence of implant removal and retention following spinal instrumental surgery as well as to characterize patients undergoing these procedures based on diagnosis and reason for removal.
3. MATERIAL AND METHODS
Protocol and registration
A protocol for this review was registered in Saiful Anwar General Hospital. The focus of the review was narrowed to retention or removal of spine instrumentation post-surgery
Eligibility criteria
Inclusion of publications that were observational studies, such as cohort, cross-sectional and case-control research, and randomized control trial. Additionally, we excluded letters, viewpoints, and review studies that provide further advice about spine surgery. The editorials or review studies that just summarize other studies were excluded. Studies didn’t consider focused on those that removal and retention spine instrumentation surgery were excluded.
Search strategy
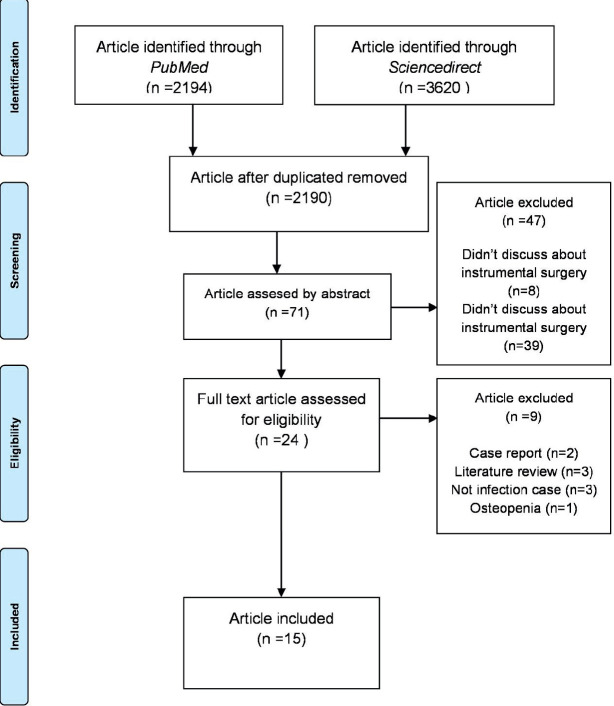
An unrestricted search to 31 April 2022 in PubMed and ScienceDirect was executed. We developed search strategies using keywords and Mesh terms of instrumentation surgery, retention, removal, and infection. In addition, reference lists of eligible articles were screened for further relevant studies and systematic reviews were scanned for appropriate references. (Figure 1)
Figure 1. Literature Search Process.
Search validation and data selection
All articles were discovered by using the search terms and those that were available on the indicated databases during the period of this review were included. All articles not meeting the inclusion criteria as stated above were later discarded. Citations were downloaded into Mendeley. Two authors independently reviewed all titles and abstracts for irrelevant studies. Potentially eligible manuscripts were exported. At this stage, the selected papers were screened again to identify articles relevant to retention or removal and instrumentation surgery and eliminated those duplicated. We obtained the full text of the remaining articles and examined them independently. Results were compared and any controversies surrounding any particular included or excluded paper were resolved by discussion. Data extraction was performed independently using a standard extraction form.
Data extraction and report
Data extraction was performed in this systematic review. The studies were subsequently screened for reporting factors that could influence removal or retention on spine instrumentation surgery. The characteristics of each study and the method are described and presented in the table, in which, patients, the prevalence of implant retention and removal, and also related factors are reported. The descriptions of the extracted data are guided by the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA)statement.
4. RESULTS
The identification of the journals in this systematic review is shown in Table 1. In this study show that the most of the journals have a retrospective cohort research design. The largest number of samples was 2.584. The average age of the study subjects varied from 15 to 66 years old. In addition, there were 2 studies that did not analyze the mean age of the patients. Table 2 shows that from 15 journals there are 12 journals with good quality and 3 journals with poor quality. Table 3 shows that most of the causes of infection are S. aureus. The other bacteria that can cause infection were S. epidermidis and P.acnes. While most journals use implant removal rather than retention in cases of spinal infection.
Table 1. Journals Identification.
| No | Author | Year | Country | Design | Disease | Sample Size | Mean age |
|---|---|---|---|---|---|---|---|
| 1 | Khanna | 2018 | US | Cohort retrospective | N/A | 67 | 61,9 |
| 2 | Manet | 2018 | France | Cohort retrospective | Degenerative | 1694 | 55 |
| 3 | Wille | 2017 | France | Cohort retrospective | Degenerative | 129 | 57 |
| 4 | Tsubouchi | 2018 | Japan | Cohort retrospective | Degenerative | 55 | 66 |
| 5 | Kim | 2010 | Korea | Cohort retrospective | N/A | 20 | 55.8 |
| 6 | Jentzsch | 2016 | Switzerland | Cohort retrospective | Fracture | 137 | 39 |
| 7 | Stavridis | 2010 | Greece | Cohort retrospective | Degenerative spinal disease or spinal fracture | 57 | 46,5 |
| 8 | Rathjen | 2007 | USA | Cohort retrospective | Scoliosis | 43 | ? |
| 9 | Muschik | 2004 | Germany | Cohort retrospective | Scoliosis | 45 | 15 |
| 10 | Ntilikina | 2017 | France | cross-sectional | Fracture | 27 | 43,2 |
| 11 | Farshad | 2013 | Switzerland | case-control | Scoliosis | 50 | ? |
| 12 | Ameri | 2021 | USA | Cohort retrospective | Scoliosis | 31 | 14,4 |
| 13 | Alanay | 2007 | USA | Cohort retrospective | Degenerative | 25 | 45,56 |
| 14 | Smits | 2017 | Netherlands | Cohort retrospective | Fracture | 102 | 38 |
| 15 | Cho | 2018 | Korea | Cohort retrospective | Degenerative | 102 | 63 |
Table 2. Bias Analysis by Newcastle-Ottawa Scale.
| No | Author | Year | Design | Selection | Comparability | Outcome | Quality | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| I | II | III | IV | I | II | III | ||||||
| 1 | Khanna | 2018 | Cohort retrospective | * | * | * | * | ** | * | * | * | Good |
| 2 | Manet | 2018 | Cohort retrospective | * | * | * | * | * | * | * | * | Good |
| 3 | Wille | 2017 | Cohort retrospective | * | * | - | * | ** | - | * | * | Good |
| 4 | Tsubouchi | 2018 | Cohort retrospective | * | - | * | * | ** | - | * | * | Good |
| 5 | Kim | 2010 | Cohort retrospective | * | * | * | - | * | - | - | * | Poor |
| 6 | Jentzsch | 2016 | Cohort retrospective | * | * | * | - | - | * | * | * | Good |
| 7 | Stavridis | 2010 | Cohort retrospective | * | * | * | * | - | * | - | - | Poor |
| 8 | Rathjen | 2007 | Cohort retrospective | * | * | * | * | * | - | - | * | Poor |
| 9 | Muschik | 2004 | Cohort retrospective | * | * | * | - | * | - | * | * | Good |
| 10 | Ntilikina | 2017 | cross-sectional | * | * | * | * | * | * | * | * | Good |
| 11 | Farshad | 2013 | case-control | * | * | * | * | * | - | * | * | Good |
| 12 | Ameri | 2021 | Cohort retrospective | * | * | * | * | - | - | * | * | Poor |
| 13 | Alanay | 2007 | Cohort retrospective | * | * | * | * | - | - | * | * | Poor |
| 14 | Smits | 2017 | Cohort retrospective | * | * | * | * | * | * | * | * | Good |
| 15 | Cho | 2018 | Cohort retrospective | * | * | * | * | ** | - | * | * | Good |
Table 3. Study of Implant Retention and Removal in Spinal Instrumentation Surgery.
| No | Author | Disease | Comorbidities | Common Bacteria | Removed | Retention | ||
|---|---|---|---|---|---|---|---|---|
| N | % | N | % | |||||
| 1 | Khanna | N/A | N/A | S. epidermidis | 19 | 28,00 | 42 | 62 |
| 2 | Manet | Degenerative | N/A | S.aureus | 28 | 1,65 | 9 | 0,53 |
| 3 | Wille | Degenerative | N/A | S.aureus | 0 | 0 | 1006 | 23,45 |
| 4 | Tsubouchi | Degenerative | N/A | N/A | 12 | 21,82 | 33 | 60 |
| 5 | Kim | N/A | Diabetes Melitus, Hipertension, Chronic Renal Failure | methicillin-resistant S.aureus | 0 | 0 | 20 | 100 |
| 6 | Jentzsch | Fracture | N/A | N/A | 137 | 100 | 0 | 0 |
| 7 | Stavridis | degenerative spinal disease or spinal fracture | N/A | N/A | 36 | 63,16 | 0 | 0 |
| 8 | Rathjen | Scoliosis | N/A | N/A | 22 | 51,16 | 0 | 0 |
| 9 | Muschik | Scoliosis | N/A | N/A | 35 | 77,78 | 0 | 0 |
| 10 | Ntilikina | Fracture | N/A | N/A | 27 | 100 | 0 | 0 |
| 11 | Farshad | Scoliosis | N/A | P.acnes | 50 | 100 | 0 | 0 |
| 12 | Ameri | Scoliosis | N/A | S.aureus | 3 | 9,68 | 28 | 90,32 |
| 13 | Alanay | Degenerative | N/A | N/A | 25 | 100 | 0 | 0 |
| 14 | Smits | Fracture | N/A | N/A | 102 | 100 | 0 | 0 |
| 15 | Cho | Degenerative | N/A | methicillin-resistant S.aureus | 19 | 18,63 | 83 | 81,37 |
Table 4. The Recommendation of Implant Retention and Removal in Spinal Instrumentation Surgery.
| NO | Author | Disease | Removal n(%) | Retention n(%) | Type Infection | Onset | Common Bacteria | Recommendation | Other Recommendation |
|---|---|---|---|---|---|---|---|---|---|
| 1 | Khanna | N/A | 19 (28,00) | 42 (62) | N/A | N/A | S.epidermidis | Implant retention correlated with the sum of debidement surgery. | IV antibiotic higher in implant removal but oral antibiotic higher in implant retention. |
| 2 | Manet | Degenerative | 28 (1,65) | 9 (0,53) | Deep SSI 46 patients | 41 patients (89%) early SSI (< 1 month) 3 patient (7%) delayed SSI (from 1 to 3 months) 2 patient (4%) late SSI (>3 months) | S.aureus | Debridement, antibiotic, implant retention is effective in 3 month after surgery. | N/A |
| 3 | Wille | Degenerative | 0 | 129 (100) | Deep SSI 129 patients | N/A | S.aureus | Debridement, antibiotic, implant retention is effective in first 3 month. | Polymicrobial infection increases the risk of implant removal. |
| 4 | Tsubouchi | Degenerative | 12 (21,82) | 33 (60) | N/A | N/A | N/A | Retention rate increase in <3 month and posterior cervical surgery. Delay administration of antibiotic cause increase risk implant removal | N/A |
| 5 | Kim | N/A | 0 | 20 (100) | N/A | N/A | methicillin-resistant S.aureus | Spinal fusion has higher the index dissability and lower patient satisfaction than non fusion. | N/A |
| 6 | Jentzsch | Fracture | 137 (100) | 0 | N/A | N/A | N/A | Implant removal reduce the pain and fingertip floor distance. | Implant removal complication was persistent pain (1%) and dystesia (3%) |
| 7 | Stavridis | Degenerative spinal disease or spinal fracture | 36 (63,16) | 0 | N/A | N/A | N/A | Implant removal can decrease the pain | N/A |
| 8 | Rathjen | Scoliosis | 22 (51,16) | 0 | N/A | N/A | N/A | Implant removal cause larger main thoracic and lumbar coronal curve | N/A |
| 9 | Muschik | Scoliosis | 35 (77,78) | 0 | Late infection | N/A | Implant removal in late infection cause increase the wound healing | N/A | |
| 10 | Ntilikina | Fracture | 27 (100) | 0 | N/A | N/A | N/A | Implant removal has benefit in thoracolumbar fracture | Percutaneus surgery decrease the fat infiltration after implant removal better than open surgery |
| 11 | Farshad | Scoliosis | 50 (100) | 0 | N/A | N/A | P.acnes | Late implant removal can loss Cobbs angle in scoliosis patient | N/A |
| 12 | Ameri | Scoliosis | 3 (9,68) | 28 (90,32) | Late infection (1 year) | S.aureus | Late infection case should use impant removal. | Implant replacement with titanium implant so it can increase the curve correction and reduce the recurrence infection | |
| 13 | Alanay | Degenerative | 25 (100) | 0 | N/A | N/A | N/A | Impant removal can reduce VAS and increase the free pain | N/A |
| 14 | Smits | Fracture | 102 (100) | N/A | N/A | N/A | Impant removal is safe and increase the quality of life | N/A | |
| 15 | Cho | Degenerative | 19 (18,63) | 83 (81,37) | • Deep SSI | 3 patients superficial wound infection (3%) 2 patients deep wound infection (2%) | methicillin-resistant S.aureus | Implant retention were independent risk factors for treatment failure | Rifampicin is an potential antibiotic against MSSA and MRSA in surgical site infection |
5. DISCUSSION
Surgical site infections (SSIs) represent the second most common type of healthcare-associated infections and remain a relatively common postoperative complication and the most common reason for readmission after surgery. SSIs have dire implications for the surgeon, patient, and institution which often require prolonged treatment, impose an economic burden and double the risk of patient mortality. Staphylococcus aureus is currently the most common cause of SSIs causing as many as 37% of cases of SSIs in community hospitals with methicillin-resistant S. aureus (MRSA) of particular concern (9)patient, and institution which often require prolonged treatment, impose an economic burden and double the risk of patient mortality. Staphylococcus aureus is currently the most common cause of SSIs causing as many as 37% of cases of SSIs in community hospitals with methicillin-resistant S. aureus (MRSA. This research showed that the most of bacteria species were Staphylococcus aureus.
The total subject in this systematic review was 2.584. The most common spinal instrumentation surgery with SSIs was degenerative spinal disease followed by scoliosis. Spine surgery has seen a rapid advancement in recent years due to novel technological innovations, safety improvements, and increased understanding of the pathophysiology of spinal conditions (10). With the rising number of annual spinal procedures performed worldwide, the associated growing costs are becoming a major health economic burden (11).
In SSI after spinal instrumentation surgery, implant removal or retention can be performed. In the case of infection, implant retention can be performed if the infection is < 3 months from the onset of surgery (12,13). However, other studies have shown that implant retention can be used if >3 months with modified debridement-irrigation, antibiotic therapy, and implant retention (14). Treatment based on debridement, implant retention, graft replacement and lengthy courses of antimicrobial therapy seems a very effective strategy in the treatment of patients with deep surgical site infection in spine surgery (15)between January 2010 and December 2014 in the traumatology and orthopaedic surgery department of our institution. All patients with SSIs were treated by debridement, graft replacement, retention of the instrumentation and lengthy courses of antimicrobial therapy. The patients were followed up for a period of 12 months. RESULTS: Of all the patients with arthrodesis, 32 (4%.
Implant retention is also known to correlate with an increase in the number of debridement in SSIs (16)reinstrumentation, retention of instrumentation with continued antibiotic suppression, and retention of instrumentation with no antibiotic suppression. Patient factors, infection factors, debridement, and antibiosis were compared. RESULTS: Of the 67 patients with SSI after spine surgery and instrumentation, 19 (28%. The use of antibiotics is necessary to reduce infection and reduce the types of microbes in SSIs. Polymicrobial correlates with implant removal (13). An antibiotic that is known to be effective in reducing infection is rifampicin (17). Rifampicin is a group of macrocyclic antibiotics mainly used for the treatment of various bacterial infections including tuberculosis (18)”ISSN”:”2373-8227 (Electronic.
Implant removal is one of the methods used when implant retention cannot be fully eradicating the SSI. Implant removal is safe and increases the quality-of-life patients (19). Implant removal also reduces the pain and has low complications such as persistent pain (1%) and dystesia (3%) (20). Implant removal can decrease the pain (21), increase wound healing (22). Late implant removal can cause loss of Cobb’s angle in scoliosis patients (23)who had pedicle screw instrumentation for posterior correction, for at least 10 years. Seven of these patients needed IR after 3.4 years (range, 1.1-7.9 years. The other research showed that implant replacement with titanium implant so it can increase the curve correction and reduce the recurrence of infection (24)who were surgically treated with PSF was collected. Patients were included for the study if they developed late arising infection (> 1 year after index posterior fusion for the deformity, Research by Kim et al, showed that spinal fusion has higher the index disability and lower patient satisfaction than non-fusion (25).
Further research needs to be done to compare implant removal and retention on the infection recurrence, pain, and quality of life of patients. The meta-analysis also needed to conclude the use of implant removal or retention in surgical site infection.
6. CONCLUSION
Implant retention can be performed in case of SSI < 3 months after surgery. Implant removal is recommended if the incidence of SSI is more than 3 months. Empirical antibiotics therapy is necessary to reduce possibility of implant removal after debridement.
Authors contribution:
Andhika Yudistira: conceptualization, writing original draft preparation, supervision. Syaifullah Asmiragani: supervision, conceptualization. Abdul Waris Imran: writing the paper and editing, data interpretation, data collecting. Muhammad Alwy Sugiarto: writing the paper and editing, data interpretation
Conflict of interest statement must be:
There are no conflicts of interest.
Financial support and sponsorship:
None.
REFERENCES
- 1.Grotle M, Småstuen MC, Fjeld O, Grøvle L, Helgeland J, Storheim K, et al. Lumbar spine surgery across 15 years: trends, complications and reoperations in a longitudinal observational study from Norway. BMJ Open. 2019 Aug;9(8):e028743. doi: 10.1136/bmjopen-2018-028743. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Rathjen K, Wood M, McClung A, Vest Z. Clinical and radiographic results after implant removal in idiopathic scoliosis. Spine (Phila Pa 1976) 2007 Sep;32(20):2184–8. doi: 10.1097/BRS.0b013e31814b88a5. [DOI] [PubMed] [Google Scholar]
- 3.Kasliwal MK, Tan LA, Traynelis VC. Infection with spinal instrumentation: Review of pathogenesis, diagnosis, prevention, and management. Surg Neurol Int. 2013;4(Suppl 5):S392–403. doi: 10.4103/2152-7806.120783. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Ntilikina Y, Bahlau D, Garnon J, Schuller S, Walter A, Schaeffer M, et al. Open versus percutaneous instrumentation in thoracolumbar fractures: magnetic resonance imaging comparison of paravertebral muscles after implant removal. J Neurosurg Spine. 2017 Aug;27(2):235–41. doi: 10.3171/2017.1.SPINE16886. [DOI] [PubMed] [Google Scholar]
- 5.Gerometta A, Rodriguez Olaverri JC, Bitan F. Infections in spinal instrumentation. Int Orthop. 2012 Feb;36(2):457–64. doi: 10.1007/s00264-011-1426-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Pull ter Gunne AF, Mohamed AS, Skolasky RL, van Laarhoven CJHM, Cohen DB. The presentation, incidence, etiology, and treatment of surgical site infections after spinal surgery. Spine (Phila Pa 1976) 2010 Jun;35(13):1323–8. doi: 10.1097/BRS.0b013e3181bcde61. [DOI] [PubMed] [Google Scholar]
- 7.Prinz V, Vajkoczy P. Surgical revision strategies for postoperative spinal implant infections (PSII) J spine Surg (Hong Kong) 2020 Dec;6(4):777–84. doi: 10.21037/jss-20-514. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Abola M V, Hardesty CK, Knapik DM, Poe-Kochert C, Son-Hing JP, Thompson GH. Incidence of complete spinal instrumentation removal following surgery for spinal deformity: a 22-year single institution study. J Pediatr Orthop B. 2019 Jul;28(4):380–4. doi: 10.1097/BPB.0000000000000605. [DOI] [PubMed] [Google Scholar]
- 9.Pal S, Sayana A, Joshi A, Juyal D. Staphylococcus aureus: A predominant cause of surgical site infections in a rural healthcare setup of Uttarakhand. J Fam Med Prim care. 2019 Nov;8(11):3600–6. doi: 10.4103/jfmpc.jfmpc_521_19. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Alanay A, Vyas R, Shamie AN, Sciocia T, Randolph G, Wang JC. Safety and efficacy of implant removal for patients with recurrent back pain after a failed degenerative lumbar spine surgery. J Spinal Disord Tech. 2007 Jun;20(4):271–7. doi: 10.1097/01.bsd.0000211283.14143.ad. [DOI] [PubMed] [Google Scholar]
- 11.Jiang F, Wilson JRF, Badhiwala JH, Santaguida C, Weber MH, Wilson JR, et al. Quality and Safety Improvement in Spine Surgery. Glob spine J. 2020 Jan;10(1 Suppl):17S–28S. doi: 10.1177/2192568219839699. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Tsubouchi N, Fujibayashi S, Otsuki B, Izeki M, Kimura H, Ota M, et al. Risk factors for implant removal after spinal surgical site infection. Eur spine J Off Publ Eur Spine Soc Eur Spinal Deform Soc Eur Sect Cerv Spine Res Soc. 2018 Oct;27(10):2481–90. doi: 10.1007/s00586-017-5294-1. [DOI] [PubMed] [Google Scholar]
- 13.Wille H, Dauchy F-A, Desclaux A, Dutronc H, Vareil M-O, Dubois V, et al. Efficacy of debridement, antibiotic therapy and implant retention within three months during postoperative instrumented spine infections. Infect Dis (London, England) 2017 Apr;49(4):261–7. doi: 10.1080/23744235.2016.1255351. [DOI] [PubMed] [Google Scholar]
- 14.Manet R, Ferry T, Castelain J-E, Pardey Bracho G, Freitas-Olim E, Grando J, et al. Relevance of Modified Debridement-Irrigation, Antibiotic Therapy and Implant Retention Protocol for the Management of Surgical Site Infections: A Series of 1694 Instrumented Spinal Surgery. J bone Jt Infect. 2018;3(5):266–72. doi: 10.7150/jbji.28765. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Gómez Cáceres A, Lucena Jiménez JS, Reyes Martín ÁL, Moriel Durán J, Sobrino Diaz B, García de Quevedo Puerta D. Prognosis of deep infection in spinal surgery using implants, treated by retention, removal of bone graft and lengthy antibiotherapy. Rev Esp Cir Ortop y Traumatol (English ed) 2019;63(1):7–11. doi: 10.1016/j.recot.2018.10.001. [DOI] [PubMed] [Google Scholar]
- 16.Khanna K, Janghala A, Sing D, Vail B, Arutyunyan G, Tay B, et al. An Analysis of Implant Retention and Antibiotic Suppression in Instrumented Spine Infections: A Preliminary Data Set of 67 Patients. Int J spine Surg. 2018 Aug;12(4):490–7. doi: 10.14444/5060. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Cho O-H, Bae I-G, Moon SM, Park SY, Kwak YG, Kim B-N, et al. Therapeutic outcome of spinal implant infections caused by Staphylococcus aureus: A retrospective observational study. Medicine (Baltimore) 2018 Oct;97(40):e12629. doi: 10.1097/MD.0000000000012629. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Pyta K, Janas A, Skrzypczak N, Schilf W, Wicher B, Gdaniec M, et al. Specific Interactions between Rifamycin Antibiotics and Water Influencing Ability To Overcome Natural Cell Barriers and the Range of Antibacterial Potency. ACS Infect Dis. 2019 Oct;5(10):1754–63. doi: 10.1021/acsinfecdis.9b00176. [DOI] [PubMed] [Google Scholar]
- 19.Smits AJ, den Ouden L, Jonkergouw A, Deunk J, Bloemers FW. Posterior implant removal in patients with thoracolumbar spine fractures: long-term results. Eur spine J Off Publ Eur Spine Soc Eur Spinal Deform Soc Eur Sect Cerv Spine Res Soc. 2017 May;26(5):1525–34. doi: 10.1007/s00586-016-4883-8. [DOI] [PubMed] [Google Scholar]
- 20.Jentzsch T, Gomes de Lima V, Seifert B, Sprengel K, Werner CML. The benefits of elective spinal implant removal: a retrospective study of 137 patients. Eur spine J Off Publ Eur Spine Soc Eur Spinal Deform Soc Eur Sect Cerv Spine Res Soc. 2016 Mar;25(3):856–64. doi: 10.1007/s00586-015-4211-8. [DOI] [PubMed] [Google Scholar]
- 21.Stavridis SI, Bücking P, Schaeren S, Jeanneret B, Schnake KJ. Implant removal after posterior stabilization of the thoraco-lumbar spine. Arch Orthop Trauma Surg. 2010 Jan;130(1):119–23. doi: 10.1007/s00402-009-0962-1. [DOI] [PubMed] [Google Scholar]
- 22.Muschik M, Lück W, Schlenzka D. Implant removal for late-developing infection after instrumented posterior spinal fusion for scoliosis: reinstrumentation reduces loss of correction. A retrospective analysis of 45 cases. Eur spine J Off Publ Eur Spine Soc Eur Spinal Deform Soc Eur Sect Cerv Spine Res Soc. 2004 Nov;13(7):645–51. doi: 10.1007/s00586-004-0694-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Farshad M, Sdzuy C, Min K. Late Implant Removal After Posterior Correction of AIS With Pedicle Screw Instrumentation-A Matched Case Control Study With 10-Year Follow-up. Spine Deform. 2013 Jan;1(1):68–71. doi: 10.1016/j.jspd.2012.10.001. [DOI] [PubMed] [Google Scholar]
- 24.Ameri B, Shufflebarger HL, Emerson B, Asghar J, George SG, Ramchandran S. Late spinal infections following posterior spinal fusion in pediatric deformities: treatment using single-stage titanium implant exchange. Spine Deform. 2021 May;9(3):751–5. doi: 10.1007/s43390-020-00266-3. [DOI] [PubMed] [Google Scholar]
- 25.Kim J Il, Suh KT, Kim S-J, Lee JS. Implant removal for the management of infection after instrumented spinal fusion. J Spinal Disord Tech. 2010 Jun;23(4):258–65. doi: 10.1097/BSD.0b013e3181a9452c. [DOI] [PubMed] [Google Scholar]