Abstract
Background and Objective
Protozoa of the genus Leishmania are obligate intracellular parasites, and Leishmania species cause a spectrum of species-specific clinical symptoms known as cutaneous, mucocutaneous, and visceral leishmaniasis. For example, Leishmania major and Leishmania tropica cause cutaneous leishmaniasis, while Leishmania infantum and Leishmania donovani cause visceral leishmaniasis (VL). However, molecular studies in recent years have shown that Leishmania species cause different clinical symptoms.
Objectives
Our aim was to evaluate the relationship between the clinical and molecular characterization of leishmania isolates in children with VL defined in Turkey, an intercontinental transitional region.
Methods
The clinical diagnosis of VL was confirmed by detecting amastigotes in the bone marrow aspirate and/or the rK39 test and/or molecular methods (genus-specific PCR, Real-Time PCR, ITS1 PCR-RFLP, DNA sequencing).
Results
Most of the VL patients were referred from the districts of Adana (53.3%) and others from neighboring provinces; Hatay (16.6%), Osmaniye (3%), Gaziantep (3%), Adıyaman (3%), and 20% case were Syrian immigrants A clinical diagnosis of VL was confirmed in 30 patients with different diagnostic methods. 93% was found positive with microscopic examination, 79.1% with rK39 dipstick test, and 60% with genus-specific PCR assay in clinical samples. The Leishmania isolates were identified as L. infantum (40%), L. donovani (26.7%), and L. tropica (23.3%) using Real-Time PCR, ITS1 PCR-RFLP, and DNA sequencing. There was no cutaneous finding in any case in clinical examination.
The most common clinical findings were fever (93.3%) and splenomegaly (90%), followed by hepatomegaly (76.6%). The most common laboratory finding was thrombocytopenia (86.6%), followed by anemia (70%). In addition, hemophagocytic lymphohistiocytosis was detected in bone marrow aspiration in two of our patients. Since pentavalent antimony salts treatment initially failed in four patients, it was necessary to switch to Liposomal-Amphotericin B with treatment success.
Conclusions
The presence of L. tropica in VL patients, despite the absence of cutaneous findings in any of the cases, shows that this strain can cause VL, contrary to conventional knowledge. In the Adana province, where this study was carried out, L. infantum from CL cases in previous studies should be taken into account, and visceral spread in CL cases and accompanying cutaneous lesions in VL cases should be investigated in detail.
Keywords: Visceral leishmaniasis, DNA Sequencing, Leishmania infantum, Leishmania donovani, Leishmania tropica
Introduction
Leishmaniasis, a chronic and persistent intracellular protozoal infection caused by many different species in the genus Leishmania, according to the World Health Organization (WHO), is one of the most neglected tropical diseases in the world.1 It is a poverty-associated parasitic disease that is endemic in over 90 countries and transmitted by sandflies and is associated with malnutrition, displacement, inadequate housing, illiteracy, weakened immune systems, and lack of resources. Leishmaniasis is also related to geographic changes, and the geographic distribution of leishmaniasis cases reflects the mobility of the population in displacement.2
There are three main forms of the disease: Cutaneous leishmaniasis (CL), Visceral leishmaniasis (VL), also known as kala-azar (KA), and Mucocutaneous leishmaniasis (MCL).3,4 It is known that approximately twenty Leishmania species are the causative agents of leishmaniasis, of which Leishmania tropica (L. tropica) is the causative agent of CL, while Leishmania donovani (L. donovani) and Leishmania infantum (L. infantum) are the causative agents of VL in the literature to date. However, in molecular studies on Leishmania species in recent years, it has been reported that L. donovani and L. infantum can also cause CL in some cases.5,6,7 Global warming and changes in climatic conditions may affect the distribution of the causative species of this disease. In addition, the molecular epidemiology of leishmaniasis may change with the increase in migration due to war in regions where leishmaniasis is endemic and the rise in business and touristic travels with the developing technology. Therefore, up-to-date information on this disease’s molecular epidemiology is needed in regions where leishmaniasis is endemic. The aim of this study was to identify the causative Leishmania species in children with a clinical diagnosis of VL and to investigate the effects of these species on the disease.
Materials and Methods
Study Area and Clinical Analysis
Turkey is located at 36° to 42° North latitude and is described as one of the endemic countries for leishmaniasis. Turkey is divided into seven regions covering a surface area of 783.562 km2. Adana province, where the study was conducted, is located at 37° north latitude and 35.32° east longitude in the eastern Mediterranean region. Adana province borders Osmaniye, Kahramanmaras, Gaziantep in the east, Icel in the west, Nigde in the northwest, Hatay in the southeast, the Mediterranean Sea in the south, and Syria in the southeast. Due to its location, Adana province receives a lot of immigration, especially from Syria. In addition, the Adana has the characteristics of the Mediterranean climate, the median relative humidity is approximately 90%, and the median temperature is 28°C. The geographical and climatic conditions of Adana province are suitable for the development of Phlebotomus species, which are the causative agents of leishmaniasis.
This study characterizes pediatric patients admitted for investigation and confirmed diagnosis of VL by Çukurova University Hospital, Pediatric Infectious Diseases Department, Adana, in the south of Turkey. It serves as a research hospital and is an important center where patients come for treatment from the south/southeast regions of Turkey and Syrian immigrants. In addition, other family members of the case were questioned and examined in terms of clinical findings, and simple hematological tests were performed.
In the clinical examination of the patients included in this study, permanent systemic infections such as fever, fatigue, anorexia, weight loss, and sizes of liver and spleen were investigated. In addition, demographic characteristics of the patients, such as age and gender, were examined in this study. Body mass index (BMI) was determined by dividing weight (kg) by height (m) squared. On WHO charts, the normal range is generally defined as between −2 SD and +2 SD (i.e., Z-scores between −2.0 and +2.0), corresponding to approximately the 2nd and 98th percentiles. In addition, non-specific laboratory data such as full blood count, gamma-globulin concentration, and erythrocyte sedimentation rate (ESR) were reported.
Laboratory Methods
Clinical examination of VL was confirmed by detection of amastigotes in bone-marrow aspirate, and/or rK39, and/or molecular tests (genus-specific PCR, Real-Time PCR, ITS1 PCR-RFLP, DNA sequencing, and Phylogenetic analysis).
Microscopic Examination
The bone marrow sample was smeared onto a glass slide. The prepared bone marrow samples were fixed with absolute methanol, stained with 10% Giemsa, and examined under the light microscope with magnification oil 100X objective. The preparations with amastigote were considered positive, and those without amastigote were considered negative.
The Recombinant Antigen Dipstick Test (rK39)
The rapid immune-chromatographic test is based on a recombinant 39-amino acid repeat antigen. The dipstick test was performed according to the manufacturers’ instructions (InBios International, Inc. Seattle, WA). Twenty microliters of serum taken from the patients were mixed with two drops of buffer in the rK39 dipstick test. After 10 minutes of incubation, serum samples with two bands on the cellulose strip were considered positive, and serum samples without were considered negative only if the control band appeared.
Molecular tests.8–10
Genus-Specific PCR Assay
DNA was extracted from bone marrow samples with an Agencourt DNA kit (Beckman Coulter, Beverly, USA), according to the manufacturer’s protocol. The kDNA using the primers 13A (5′-GTG GGG GAG GGG CGT TCT-3′) and 13B (5′-ATT TTC CAC CAA CCC CCA GTT-3′) was investigated for the presence of Leishmania in clinical samples.8 A reaction mix with a final volume of 25 μL consisted of 0.2 mM of dNTP, 1.5 mM MgCl2, 1 unit of Taq polymerase, 1 μM of each primer, and 5 μL DNA samples for use PCR analyses. The DNA was amplified for 35 cycles in a thermocycler, set to run at 94 °C for 1 min, 54 °C for 1 min, and 72°C for 1 min for each one.
The amplification reactions were analyzed by bromide staining and visualization under UV light. The PCR products with a fragment image of approximately 120 bp under UV light were considered positive.
Real-Time PCR Assay
The kDNA minicircle gene region was targeted to identify Leishmania species, and Leishmania isolates were amplified by melting real-time curve PCR (Real-Time PCR) using primers JW13 and JW14.9 The Real-Time PCR was performed by hot-start PCR using the LightCycler FastStart DNA Master SYBR Green I Kit in a LightCycler™ (Roche Diagnostics). The 20 μL reaction mixture contained 1 X LightCycler FastStart DNA Master SYBR Green I (Roche Diagnostics, Meylan, France), 2 mM MgCl2, 10 μM of each primer and 5 μL of DNA of the parasite.
The Real-Time PCR Reaction and DNA samples were amplified using a 35 cycles thermal cycler program consisting of 10 s at 95°C, 10 s at 53°C, and 10 s at 72°C. The melting program consisted of one cycle of 95°C for 10 s, 67°C for 10 s, and heating at 0.1°C per 1 second to 98°C. The transition rates were 20°C/s except for the extension step and the final step, which had a temperature transition rate of 1°C/s and 0.1°C, respectively. Fluorescence was measured through the slow heating phase. For improved visualization of the melting temperatures (Tm), melting peaks were derived from the initial melting curves (fluorescence [F] versus temperature [T] by plotting the negative derivative of fluorescence over-temperature –dF/dT versus dT). The melting temperatures were 88.5±0.4°C for L. donovani, 89.3±0.2°C for L. tropica, and 90.5±0.2°C for L. infantum, respectively.
ITS1 PCR-RFLP Assay
In this study, to identify Leishmania species according to the study of Schönian et al., the ITS1 gene region was targeted, and LITSR-L5.8S primers were designed.10 The 40 μL PCR reaction mixture consisted of PCR buffer 1 X (75 mM KCl, pH 8.3 and 20 mM Tris-HCl, 1.5 mM MgCl2, 1U Taq polymerase), 0.2 mM dNTPs, 0.5 pmol of each primer and 5 μL of DNA sample. After the initial denaturation (5 min at 94 °C), 35 cycles of denaturation for 1 min at 94 °C, annealing for 1 min at 54°C, and elongation for 1 min at 72°C were carried out, and a final extension terminated the PCR at 72°C for 10 min. The PCR products were analyzed in 1% agarose gel by electrophoresis at 100 V in 1 X Tris-boric-EDTA buffer (0.04 mM Tris-boric and 1mM EDTA, pH 8) and visualized by UV light after being stained with ethidium bromide.
All PCR samples with approximately 350 bp fragment length bands were considered positive according to the agarose gel electrophoresis. ITS1 PCR products (10 μL) were digested with the Hae III restriction enzyme (Promega, Wisconsin, USA) according to the manufacturer’s instructions, and the restriction fragments were analyzed by 2% agarose gel electrophoresis. The restriction products were identified as L. donovani, L. infantum, and L. tropica, according to Schönian et al.10
DNA Sequencing
ITS1 PCR products were purified for DNA sequencing using a SentroPure DNA purification kit (Sentromer DNA, Istanbul, Turkey). Purified PCR products were sequenced with LITSR-L5.8S primers using BigDye Terminator V 3.1 cycle sequencing kit (Applied Biosystems). This reaction was analyzed according to the instructions for the 3730 DNA analyzer (Applied Biosystems). The ITS1 PCR products of Leishmania isolate sequences were approximately 320 bp in length. The reference strains of Leishmania species (L. donovani ATC 50212, WHOM/IN/80/DD8; L. infantum ATCC 501340, WHOM/TN/80/IPT-1; L. tropica ATCC 50129, WHOM/SU/74/K27) were used in this analysis. The obtained sequences were processed with the available GenBank and checked using basic local alignment search tool (BLAST) analysis software (www.ncbi.nlm.nih.gov/BLAST.
Treatment
The conventional treatment of VL/kala-azar consists of pentavalent antimony salts (PAS-Sbv) - sodium stibogluconate (SSG (Pentostam)) and meglumine antimoniate (MA, (Glucantime®)). In addition, liposomal amphotericin B (L-AMB (AmBisome®)) was used intravenously at a dosage of 3 mg/kg on days 1–5, 10, and 21 (for a cumulative dose of 21 mg/kg). The therapy used in our department was one of the following in Table 1 (choice made according to a supplied drug that day, and/or the patient’s suitability, and/or the physician’s preference).
Table 1.
Used antileishmanial drugs in this study and their prescribed dosage.
| Drug | Dose | Admistration site | Action Mechanism | Side effects |
|---|---|---|---|---|
Pentavalent antimony salts (PAS)
|
20 mg/kg daily for 28–30 d | IV or IM | Inhibits glycolysin and other metabolic pathways | Musculoskeletal pain, gastrointestinal disturbances, headache, and increase in liver and pancreatic enzymes |
| Liposomal amphotericin B (L-AMB) | 3 mg/kg on 1–5, 14, and 21 d | IV | Inhibits cell membrane synthesis | Elevation of LFT, cytopenia, nephrotoxicity, pancreatitis |
Follow-up
Post-treatment follow-up (at least 1 year, every month for the first 3 months, then every 2 months, and every 3 months after 6 months) included clinical examination, blood cell count, and ESR.
Statistical analysis
The medications used and/or management modalities were collected on a spreadsheet. The Statistical Package for the Social Sciences (SPSS) version 23.0 (IBM, Somers, NY, USA) was used for statistical analysis. Categorical measurements were summarized as numbers and percentages, while continuous measurements were summarized as mean, deviation, and minimum-maximum.
Ethics Statement
Confidentiality and patient privacy were maintained throughout the process. Ethical approval was obtained from Çukurova University Scientific Research Ethics Committee (decision no: 03.04.2022/120) and was performed in accordance with the ethical standards of the Declaration of Helsinki.
Results
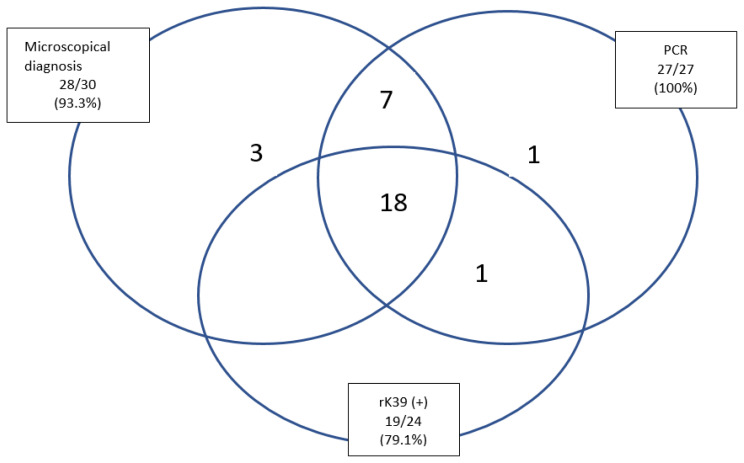
In this study, the VL clinical diagnosis of 30 patients was confirmed by different diagnostic methods. According to the results of microscopic examination, 28 (93%) of 30 patients who were clinically diagnosed with VL were found to be positive, while 2 patients (7%) were negative. Of the patients with VL, 19 (79.1%) were positive, and 5 (20.9%) were negative using the rK39 dipstick test. However, the rK39 dipstick test could not be studied in 6 (20%) patients for technical reasons. The leishmania parasite was detected by genus-specific PCR assay in 27 (90%) VL patients. Still, genus-specific PCR assay could not be studied in 3 (10%) of the VL patients due to technical reasons in the laboratory. The Real-Time PCR method was used to identify Leishmania species in VL patients, and 12 (40%) L. infantum, 8 (26.7%) L. donovani, and 7 (23.3%) L. tropica were identified in the study; according to this method. ITS1 PCR-RFLP assay and DNA sequencing were analyzed to confirm the Leishmania species in this study. The results of the ITS1 PCR-RFLP assay confirmed the Real-Time PCR results in this study. In addition, each of the samples and reference strains of Leishmania species (L. donovani ATC 50212, WHOM/IN/80/DD8; L. infantum ATCC 501340, WHOM/TN/80/IPT-1; L. tropica ATCC 50129, WHOM/SU/74/K27) was identical to the sequence of Leishmania species reported in GenBank. Compared with the previous records in GenBank, we determined 100% similarity between sequences of leishmania isolates from VL patients and Leishmania strains in GenBank. All of the diagnostic results used in this study have been shown in Table 2 and Figure 1. The Leishmania species and the patients’ clinical symptoms were compared, and no significant relationship was found between them.
Table 2.
Demographic findings of the patients diagnosed VL.
| Case/gender/age | Time to diagnosis | Symptoms | Physican findings | Hematologic findings | Parasitological findings | Treatment | Outcome | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
|
|
|
|
||||||||||||
| Fever | BMI (Z-score) | Others | Liver (cm) | Spleen (cm) | HCT | WBC | Trombocit | Response time | BM mic | IC | Species | ||||
|
| |||||||||||||||
| 1/EK/m/3 y | 90 d | + | 15.7 (−3.11) | Abd pain | 9 | 11 | 21 | 5100 | 138.000 | 25 d | + | Nd | L. tropica | MA | Cure |
| 2/TG/f/5 y 3 m | 7 d | + | 12.1 (−3.11) | Fatigue | 3 | 0 | 28 | 4800 | 112.000 | 10 d | + | Neg | L. tropica | MA | Cure |
| 3/YAA/m/2 y | 20 d | + | 14.8 (−1.17) | Fatigue, vomiting | 3 | 6 | 23 | 4000 | 92.000 | 5 d | + | + | L. infantum | MA | Cure |
| 4/YK/m/5 y 9 m | 30 d | + | 15.5 (0.11) | Jaundice | 0 | 10 | 22 | 3200 | 113.000 | 10 d | + | + | L. infantum | MA | Cure |
| 5/OK/m/3 y 3 m | 10 d | + | 16.3 (0.56) | - | 2 | 0 | 32 | 5200 | 210.000 | 1 d | + | + | L. tropica | MA | Cure |
| 6/AK/m/2 y 8 m | 15 d | + | 19.8 (2.18) | - | 7 | 12 | 19 | 2000 | 44.000 | 15 d | + | Nd | L. donovani | SSG | Cure |
| 7/EK/m/2 y | 10 d | + | 16.5 (−1.06) | Fatigue, anorexia | 2 | 4 | 28 | 5000 | 100.000 | 5 d | + | + | L. infantum | MA | Reccurens (3 m later) Cure with AmB |
| 8/KS/f/1 y | 30 d | + | 14.07 (−2.15) | Pallor | 5 | 6 | 27 | 4900 | 32.000 | 10 d | + | + | L. donovani | AmB | Cure |
| 9/R Ç /m/7 y | 60 d | Neg | 21.15 (−0.01) | Abd distantion, pallor | 8 | 12 | 23 | 2500 | 99.000 | Uk | + | + | L. tropica | SSG | Unresponsiveness Cure with AmB |
| 10/AS/f/5 y Father death of VL | 90 d | + | 12.58 (−2.56) | Weigh loss | 2 | 5 | 19 | 3700 | 190.000 | 15 d | + | + | L. donovani | SSG | Cure |
| 11/ İÖ /m/11 y | 20 d | + | 15.20 (−0.99) | Abd pain, weight loss | 5 | 4 | 28 | 3500 | 160.000 | 10 d | + | + | L. tropica | SSG | Cure |
| 12/YET/f/1 y 6 m | 30 d | + | 16.8 (0.9) | Abd pain | 7 | 8 | 24 | 8300 | 117.000 | 10 d | Neg | + | L. donovani | SSG | Cure |
| 13/AA/m/2 y 2 m | 30 d | + | 17.58 (0.87) | Abd pain | 10 | 9 | 21 | 2600 | 77.000 | 25 d | + | + | L. infantum | SSG | Unresponsiveness Cure with AmB |
| 14/SA/f/6 y | 180 d | + | 13.65 (−1.35) | Fatigue, abd distantion | 4 | 10 | 28 | 5500 | 97.000 | 25 d | + | + | L. infantum | SSG | Unresponsiveness Cure with AmB+MA |
| 15/SK/f/2 y | 10 d | + | 13.2 (−2.26) | Weigh loss | 5 | 5 | 27 | 3400 | 123.000 | 30 d | + | + | L. donovani | L-AmB | Unresponsiveness Cure with MA |
| 16/CY/m/4 y | 10 d | + | 14.6 (−0.84) | - | 5 | 5 | 23 | 5900 | 97.000 | 5 d | + | + | L. infantum | MA | Cure |
| 17/FD/m/4 y 6 m | 10 d | + | 14.79 (−0.64) | - | 3 | 4 | 18 | 2700 | 63.000 | 15 d | + | + | L. donovani | MA | Cure |
| 18/ZK/f/2 y 9 m | 30 d | + | 16.19 (0.51) | Abd pain, HLH | 2 | 2 | 15 | 1130 | 11.000 | 40 d | + | Nd | Nd | L-AmB | Cure |
| 19/SG/f/1 y | 15 d | + | 14.9 (−1.29) | - | 4 | 6 | 23 | 1270 | 43.000 | 15 d | + | Neg | L. tropica | L-AmB | Cure |
| 20/ İ S/m/2 y 8 m | 30 d | + | 16.19 (0.51) | Abd pain | 5 | 7 | 15 | 2970 | 32.000 | 15 d | + | + | L. donovani | L-AmB | Cure |
| 21/MA/f/1 y | 3 d | + | 19.39 (1.65) | Pallor | 2 | 4 | 19 | 3370 | 60.000 | 15 d | + | + | L. infantum | MA | Cure |
| 22/SA/f/7 y | 15 d | + | Uk | Fatigue | 2 | 4 | 22 | 1500 | 94.000 | 10 d | + | Nd | L. infantum | L-AmB | Cure |
| 23 a/HC/m/5 y | 3 years | Neg | 15.33(−0.12) | Abd distantion, pallor | 5 | 10 | 33 | 4100 | 110.000 | Uk | + | + | L. infantum | L-AmB | Cure |
| 24 a/MŞ/m/3 y 4 m | 180 d | + | 13.74 (−2.09) | Fatigue, abddistantion | 8 | 5 | 24 | 2600 | 47.000 | 5 d | + | Nd | L. tropica | L-AmB | Cure |
| 25 a/MH/m/3 y 2 m | 60 d | + | 14.58 (0.53) | Abd distantion | 4 | 6 | 27 | 2200 | 14.000 | 10 d | + | + | L. infantum | L-AmB | Cure |
| 26 a/AR/m/7 y | 7 d | + | 13.38(−2.77) | Fatigue | 5 | 8 | 24 | 1240 | 13.000 | 10 d | + | + | L. infantum | L-AmB | Cure |
| 27 a/DA/m/7 y | 15 d | + | 14.35 (−2.59) | Fatigue, abd pain, pallor | 10 | 10 | 16 | 41900 | 43.000 | Out of follow | + | Neg | Nd | L-AmB | Out of follow b |
| 28 a/AH/m/3 y 6 Chronic Granulomatous Disease | Uk | + | 17.0 (1.24) | Fatigue, abd distantion, vomiting | 10 | 12 | 24 | 2700 | 222.000 | 5 d | + | Neg | L. infantum | L-AmB | Cure |
| 29/FY/m/12 y | Uk | + | 14.2 (−2.16) | Abd distantion, HLH | 4 | 6 | 18 | 2700 | 62.000 | 20 d | Neg | Neg | L. donovani | L-AmB | Cure |
| 30/G Ç /f/1 y 4 m Glycogen Store Disease | 7 d | + | 14.0 (−3) | Fatigue, edema | 3 | 0 | 20 | 2400 | 44.000 | 15 d | + | Nd | Nd | L-AmB | Cure |
Syrian patient; Uk: Unknown, Nd: not done HLH: hemophagositosis; BM: bone marrow; IC: rk39-based immunochromatographic test; −: negative; +: positive. SSG (Sodium stilgluconate-Pentostam), MA-Meglumine antimonite (Glucantime®) L-AmB: Lipozomal amphoterisin B
Figure 1.
Venn diagram with data about PCR, r K39 and microscopic examination positivity regarding VL patients (N: 30 VL pediatric case).
In addition, the epidemiological findings, clinical features, treatment, and outcome of the patients with VL have been shown in Table 2. Most of the VL patients were referred from the districts of Adana (53.3%) and others from neighboring provinces; Hatay (16.6%), Osmaniye (3%), Gaziantep (3%), Adıyaman (3%), and 20% case were Syrian immigrants (Table 3). Therefore, it was determined that 76.6% of the patients in this study lived in rural areas, and 23.4% lived in urban areas.
Table 3.
Distribution of Leishmania strains by age and provinces.
| L. infantum 12 case (40%) | L. tropica 7 case (23.3%) | L. donovani 8 case (26.7%) | ND 3 case (10%) | Unresponsive/reccurens 5 case (16.6%) | |
|---|---|---|---|---|---|
| 0–12 month (3 case, 10%) | 1 | 1 | 1 | ||
| 13 month–2 years (5 case, 16.6%) | 2* | - | 2* | - | 2 |
| 2 years–6 years (17 case, 56.6%) | 7** | 5 | 4 | 2 | |
| 7 years–12 years (5 case, 16.6%) | 2 | 1* | 1 | 1 | |
| Province | |||||
| Adana (16) | 6 | 4 | 5 | 1 | 3 |
| Hatay (5) | - | 1 | - | - | - |
| Gaziantep (1) | 2 | 1 | 2 | - | 2 |
| Osmaniye (1) | - | - | 1 | - | - |
| Ad ı yaman (1) | - | - | - | 1 | - |
| Syrian refugees (6) | 4 | 1 | 1 | 1 | - |
for each case that was non-responsive to first treatment.
According to family history, a sibling of Case 3 was previously diagnosed with VL, while the father of Case 11 had just died due to VL before the boy applied. The median age of the 30 patients [20 male (66.7%)] was 37 months (range 12 months – 12 years, mean ± SD, 47.96 ± 32.87 months).
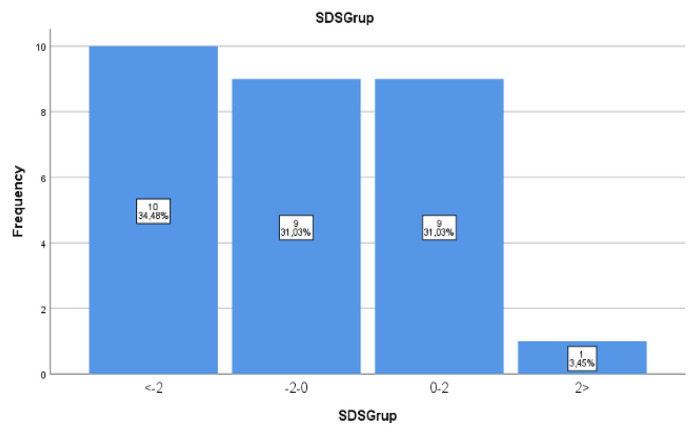
Duration of symptoms before admission ranged from 3 days to 6 months (mean 37.5 ± 46.3, median 20 days), while a Syrian boy (Case 23) complained for 3 years of abdominal distention and pallor. In the study, the body mass index values of the patients were 14,9 (12,1–21,15) on average, and malnutrition was detected in 34.48 % of our patients (Figure 2); 10 cases were below the BMI-2 score. No association was found between BMI and parasite type. Fever was present in all patients except 2 (93.3%) (Table 3). The duration of fever persists between 3 and 21 days (mean 10.9± 5.3, median 10 days) after beginning treatment. In the study, splenomegaly (90%) and hepatomegaly (76.6%) were found to be the most common clinical findings after fever (93.3%). No relationship was found between symptoms and parasite types. The most common laboratory finding was thrombocytopenia (86.6%), followed by anemia (70%) (Table 4). In two of our patients, we detected hemophagocytic lymphohistiocytosis (HLH) in bone marrow aspiration (Case 18 and Case 2). HIV was not detected in any patient. In this study, although the PAS regimens were effective in the treatment, some disadvantages were experienced like prolonged hospitalizations and side effects, such as malaise, arthralgia, abdominal pain, increased levels of liver transaminases, amylase, and lipase, vomiting, renal effects, and T-wave changes in the electrocardiogram.
Figure 2.
Distribution of patients according to body mass index. SDS = standard deviation scores.
Table 4.
Clinical findings of the VL diagnosed pediatric patients.
| Symptoms/findings | Number of cases (%)(Total 30 case) |
|---|---|
| Fever | 28 (93.3) |
| Fatigue | 10 (33.3) |
| Abdominal distention | 7 (23.3) |
| Abdominal pain | 7 (23.3) |
| Pallor | 5 (16.6) |
| Weight loss | 3 (10) |
| Vomiting | 2 (6) |
| HLH | 2 (6) |
| Jaundice | 1 (3) |
| Edema | 1 (3) |
| Trombocytopenia | 26 (86.6) |
| Anemia | 21 (70) |
| Neutropenia | 19 (63.3) |
| Splenomegaly | 27 (90) |
| Hepatomegaly | 23 (76.6) |
The treatment outcome of only one of our patients remained unknown. This patient was the child of a Syrian immigrant family, and they had returned to their hometown; the patient’s family discharged the patient before the treatment was finished. Therefore, the patient’s treatment outcome could not be followed up. In this study, it was observed that 5 (17%) of VL patients did not respond to the initial PAS treatment. One of these had anorexia, and the VL infection recurred. While four unresponsive patients were shifted to L-AMB treatment, and a full cure was achieved. Finally, a single patient who did not respond while receiving L-AMB treatment was moved to PAS treatment, which was concluded successfully (Table 2). No patient died.
Discussion
According to WHO data, more than 1 billion people live in leishmaniasis endemic areas and are at risk for this disease. More than 90% of new cases reported to WHO occurred in 10 countries: Brazil, China, Ethiopia, Eritrea, India, Kenya, Somalia, South Sudan, Sudan, and Yemen.2 Leishmania is also widespread in most countries in the Mediterranean basin, including Turkey and our neighbor countries, Syria, Iran, and Iraq.11 Turkey is an endemic area for CL, according to the data of WHO. New outbreaks of CL cases in the southeast of Turkey are concurrent with the start of the war in Syria (now a day, one of the top countries in the world for CL) and large migration to Turkey;12 in addition, Turkey is a geographical transition region that receives immigrants from many other countries (e.g., Afghanistan, Pakistan). Besides this, many people go to endemic areas outside of Turkey for work and military duty (e.g., Iraq, Syria, Afghanistan). Leishmaniasis is an important public health problem for Turkey due to its geographical location, climatic conditions, and internal and external migration prevalence.
It is emphasized that the development of infection with Leishmania is a complex structure under the influence of different factors. Individual factors (age group, nutritional status) and infecting parasite species/virulence factors, as well as the host’s immune status, play a major role in the disease formation of this agent. Macrophages and neutrophils are the primary cells interacting with Leishmania parasites after host infection. Macrophages and neutrophils are considered the primary cells that react to Leishmania infection. Still, several other immune cells, such as monocytes, dendritic cells (DCs), natural killer (NK) cells, and CD4+ and CD8+ T cells, as well as effector molecules, such as cytokines like interferon (IFN)-γ and interleukin (IL)-12 and nitric oxide (NO) produced by inducible NO synthase (iNOS), play distinct roles in the host response. The development of an immune response against Leishmania is associated with the parasite’s activation of CD4+ T cells and the differentiation of these cells into T-helper (Th) 1 or Th2 effector cells. In addition, interleukin 10 (IL-10) and transforming growth factor-beta (TGF-β), which are defined as immune response regulators, play a key role in VL formation by inducing parasite proliferation.13,14
The prevalence of leishmaniasis is increasing rapidly in the pediatric population in many parts of the world. The mechanisms underlying its higher incidence in children still contain many speculations, and the exact mechanism that causes VL sensitivity is unknown. Still, it is thought to be associated with immunodeficiency in particular. In addition, studies in South America and Africa have reported malnutrition may increase the risk of VL infection in children.14 Kumar et al. have examined the effect of malnutrition on the profile of innate immune functions of polymorphonuclear neutrophil granulocytes (PMNs) and monocytes by comparing well-nourished and malnourished Indian patients with VL. They have reported that malnourished VL patients were observed with severely dysfunctional PMNs and monocytes in terms of ROS activity that could not be recovered by stimulation with Leishmania parasites.15 Other studies have been conducted on the relationship between malnutrition and VL infection and have suggested that in many cases, malnutrition plays a critical role in the progression of VL to its severe form.16,17 In our study, malnutrition was detected in 34.48% of patients, and VL infection recurred in a patient during anorexia.
The clinical presentation, combined with the epidemiological context and non-specific biological parameters,18 raises suspicion of VL, but laboratory confirmation of the diagnosis before deciding on treatment is required. The gold standard for VL diagnosis is direct Leishmania amastigotes visualization by microscopic examination in the Giemsa-stained slides of tissue aspirate samples (spleen, bone marrow, or lymph node).19 Although our success in the direct microscopic evaluation of the bone marrow in the diagnosis was high (93.3%), two children were diagnosed only by molecular testing, and these results made us think that many cases may have been missed. The rK39 dipstick test positivity in the current study was 79.1% in all VL patients. The PCR assays are a rapid tool with high sensitivity (99%), allowing species-specific diagnosis, therapeutic approach, and clinical progress.20
The literature shows that L. tropica is the causative agent of CL, while L. donovani and L. infantum are the causative agents of VL. However, it has been reported with the development of molecular methods that leishmaniasis causative species vary. Recent studies have reported the presence of L. infantum in CL cases without a VL history and that of L. tropica in VL cases without a CL history.21,22 The L. infantum, L. major, L. tropica, and L. donovani from leishmaniasis agents have been reported in the southern/southeast Anatolia region of Turkey.23,24 In the present study, as causative agents of VL in pediatric cases, L. infantum, L. donovani, and L. tropica were as follows; 40%, 26.7%, and 23.3%, respectively. In the Persian Gulf War (1990–1991), L. tropica was the causative agent for leishmaniasis in American soldiers and veterans at bases in Bahrain and Northern Saudi Arabia,6,25 and several other reports from various parts of the world suggest that L. tropica can cause VL.26–28 Southern and southeast Anatolia has a geography similar to the settlements where these notifications are made. In our study, L. tropica was isolated in VL patients without CL symptoms. Therefore, L. tropica may be the causative agent for VL more than expected in the area of Turkey. L. donovani and L. infantum species have also been detected in VL patients. When the relationship between Leishmania species and clinical symptoms was compared, no significant association was found between them.
The VL is the most severe form of leishmaniasis and represents a spectrum of chronic infections. The incubation period ranges from weeks to months (even years); thus, due to slow progression, most patients remain subclinical and are correctly diagnosed only very late in the course of the disease. While WHO estimates that the illness in Syria is 2–5 times higher than the actual reported figures, this is frightening considering the risk posed by asymptomatic Leishmania carriers to the Turkish population, especially due to the massive influx of immigrants from Syria in recent years.2 Due to the prolonged presence of asymptomatic and subclinical people in the community, the VL infection can be transmitted to many people. In addition, the asymptomatic VL patients may serve as a silent reservoir of parasites, presenting a risk to public health through infection of the phlebotomine vector.29 Although most of our patients in our study had a history of being in rural areas and having contact with sandflies, some lived in the city and whose risks were not defined.
WHO has established a useful and suspicious clinical case definition for a diagnostic algorithm: being in an endemic area, prolonged fever (more than two weeks), splenomegaly (mostly), and weight loss, also with pancytopenia, VL is suspected in any case.30 Including VL in the differential diagnosis of leukemia-like syndromes in infants living in/traveling (even in the past) to endemic areas such as the Mediterranean basin31. VL is an infection not commonly managed by Turkish practitioners and even more by the European physicians of Mediterranean and non-Mediterranean countries, where immigrants can bring the disease. This situation can lead to delayed recognition of undiagnosed reactivated VL, inappropriate treatment in VL, and poor clinical outcomes.
Turkey is an endemic country for CL, with the main causative agent as L. tropica.32 Although about a quarter of our VL cases, the cause was L. tropica, cutaneous lesions were not found in any of them. Concomitant cutaneous lesions should be investigated, and each patient with cutaneous lesions should be examined in detail regarding visceral spread. In southeast Anatolia, where CL is known to be endemic, the possibility of VL in a patient diagnosed with leukemia should not be forgotten.
Few anti-leishmanial formulas have been proven worthy; PAS, L-AMB, pentamidine, miltefosine, and paromomycin. Socio-economic and pharmaceutical conditions (production, distribution) have a tremendous impact on the choice of therapeutic option.33 Although only PAS is given free of charge by the government in Turkey, L-AMB has recently become the first choice drug instead of PAS due to its faster effect (7 days’ hospitalization versus 28–30 days. Approximately 17% of the patients were reported to fail to respond to the current study’s initial therapy; four failed to respond to PAS therapy, resulting in a complete cure with L-AMB. Considering the cost advantage of shortening the hospital stay, despite the high cost of L-AMB treatment, it seems to be a cost-effective regimen compared to antimonial agents with its high success rate and being the most effective treatment.34,35 In addition, the less toxic effect of L-AMB confirms its preference.
Conclusions
The present study reveals that all three isolate L. infantum, L. donovani and L. tropica are causative agents of pediatric VL in Turkey’s south/southeast Mediterranean region. However, this study must be supported by studies with more examples. Furthermore, determining possible animal reservoir hosts for effective control should be explored using molecular methods. While it is obvious that the cost spent for the diagnosis and treatment of leishmaniasis, an important public health problem, is higher than the measures to prevent this disease, it is very sad that not enough attention is paid to this issue in the world.
Footnotes
Competing interests: The authors declare no conflict of Interest.
References
- 1.Mehand MS, Al-Shorbaji F, Millett P, Murgue B. The WHO R&D Blueprint: 2018 review of emerging infectious diseases requiring urgent research and development efforts. Antiviral Res. 2018;159:63–67. doi: 10.1016/j.antiviral.2018.09.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Leishmaniasis. Jan 8, 2022. https://www.who.int/news-room/fact-sheets/detail/leishmaniasis .
- 3.Burza S, Croft SL, Boelaert M. Leishmaniasis. Lancet. 2018;392:951–70. doi: 10.1016/S0140-6736(18)31204-2. [DOI] [PubMed] [Google Scholar]
- 4.Curtin JM, Aronson NE. Leishmaniasis in the United States: Emerging Issues in a Region of Low Endemicity. Microorganisms. 2021;9(3):578. doi: 10.3390/microorganisms9030578. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Tabbabi A. Review of Leishmaniasis in the Middle East and North Africa. Afr Health Sci. 2019;19(1):1329–1337. doi: 10.4314/ahs.v19i1.4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Stratton CW. Visceral leishmaniasis Caused by Leishmania tropica in American military personnel deployed to Southwest Asia during Operation Desert Storm. Infect Dis Newsletter IDN. 1992;11:9–12. doi: 10.1016/0278-2316(92)90037-E. [DOI] [Google Scholar]
- 7.Ok UZ, Balcioğlu IC, Taylan Ozkan A, Ozensoy S, Ozbel Y. Leishmaniasis in Turkey. Acta Trop. 2002;84(1):43–8. doi: 10.1016/S0001-706X(02)00134-1. [DOI] [PubMed] [Google Scholar]
- 8.Motazedian H, Karamian M, Noyes HA, Ardehali S. DNA extraction and amplification of Leishmania from archived, Giemsa-stained slides, for the diagnosis of cutaneous Leishmaniasis by PCR. Ann Trop Med Parasitol. 2002;96(1):31–4. doi: 10.1179/000349802125000484. [DOI] [PubMed] [Google Scholar]
- 9.Nicolas L, Milon G, Prina E. Rapid differentiation of Old World Leishmania species by LightCycler polymerase chain reaction and melting curve analysis. J Microbiol Methods. 2002;51(3):295–9. doi: 10.1016/S0167-7012(02)00099-4. [DOI] [PubMed] [Google Scholar]
- 10.Schönian G, Nasereddin A, Dinse N, Schweynoch C, Schallig HD, Presber W, Jaffe CL. PCR diagnosis and characterization of Leishmania in local and imported clinical samples. Diagn Microbiol Infect Dis. 2003;47(1):349–58. doi: 10.1016/S0732-8893(03)00093-2. [DOI] [PubMed] [Google Scholar]
- 11.Tabbabi A. Review of Leishmaniasis in the Middle East and North Africa. Afr Health Sci. 2019;19(1):1329–1337. doi: 10.4314/ahs.v19i1.4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Ergönül Ö, Tülek N, Kayı I, Irmak H, Erdem O, Dara M. Profiling infectious diseases in Turkey after the influx of 3.5 million Syrian refugees. Clin Microbiol Infect. 2020;26(3):307–312. doi: 10.1016/j.cmi.2019.06.022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Pagliano P, Esposito S. Visceral leishmaniosis in immunocompromised host: an update and literature review. J Chemother. 2017;29(5):261–266. doi: 10.1080/1120009X.2017.1323150. [DOI] [PubMed] [Google Scholar]
- 14.Elmahallawy EH, Alkhaldi AAM, Saleh AA. Host immune response against leishmaniasis and parasite persistence strategies: A review and assessment of recent research. Biomedicine & Pharmacotherapy. 2021;139:111671. doi: 10.1016/j.biopha.2021.111671. [DOI] [PubMed] [Google Scholar]
- 15.Kumar V, Bimal S, Singh SK, Rajesh C, Das S, Chadrashekher Lal, Pandey K, Das V, Das P. Leishmania donovani: dynamics of L. donovani evasion of innate immune cell attack due to malnutrition in visceral leishmaniasis. Nutrition. 2014;30(4):449–58. doi: 10.1016/j.nut.2013.10.003. [DOI] [PubMed] [Google Scholar]
- 16.Mengesha B, Endris M, Takele Y, Mekonnen K, Tadesse T, Feleke A, Diro E. Prevalence of malnutrition and associated risk factors among adult visceral leishmaniasis patients in Northwest Ethiopia: a cross sectional study. BMC Res Notes. 2014;4(7):75. doi: 10.1186/1756-0500-7-75. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Cerf BJ, Jones TC, Badaro R, Sampaio D, Teixeira R, Johnson WD. Malnutrition as a risk factor for severe visceral leishmaniasis. J Infec Dis. 1987;156(6):1030–3. doi: 10.1093/infdis/156.6.1030. [DOI] [PubMed] [Google Scholar]
- 18.Al-Ghazaly J, Al-Dubai W, Abdullah M, Al-Gharasi L. Hematological characteristics of Yemeni adults and children with visceral leishmaniasis. Could eosinopenia be a suspicion index? Mediterr J Hematol Infect Dis. 2017;9(1):e2017056. doi: 10.4084/mjhid.2017.056. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Kumar A, Pandey SC, Samant M. A spotlight on the diagnostic methods of a fatal disease Visceral Leishmaniasis. Parasite İmmunol. 2020;42(10):e12727. doi: 10.1111/pim.12727. [DOI] [PubMed] [Google Scholar]
- 20.Sundar S, Singh OP. Molecular Diagnosis of Visceral Leishmaniasis. Mol Diagn Ther. 2018;22(4):443–457. doi: 10.1007/s40291-018-0343-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Özbilgin A, Harman M, Karakuş M, Bart A, Töz S, Kurt Ö, Çavuş İ, Polat E, Gündüz C, Van Gool T, Özbel Y. Leishmaniasis in Turkey: Visceral and cutaneous leishmaniasis caused by Leishmania donovani in Turkey. Acta Trop. 2017;173:90–96. doi: 10.1016/j.actatropica.2017.05.032. [DOI] [PubMed] [Google Scholar]
- 22.Eroglu F, Koltas IS, Alabaz D, Uzun S, Karakas M. Clinical manifestations and genetic variation of Leishmania infantum and Leishmania tropica in Southern Turkey. Exp Parasitol. 2015;154:67–74. doi: 10.1016/j.exppara.2015.04.014. [DOI] [PubMed] [Google Scholar]
- 23.Koltas IS1, Eroglu F, Alabaz D, Uzun S. The emergence of Leishmania major and Leishmania donovani in southern Turkey. Trans R Soc Trop Med Hyg. 2014;108(3):154–8. doi: 10.1093/trstmh/trt119. doi: 10.1093/trstmh/trt119. Epub 2014 Jan 20. [DOI] [PubMed] [Google Scholar]
- 24.Magill AJ, Grogl M, Johnson SC, Gasser RA., Jr Visceral infection due to Leishmania tropica in a veteran of Operation Desert Storm who presented 2 years after leaving Saudi Arabia. Clin Infect Dis. 1994;19(4):805–6. doi: 10.1093/clinids/19.4.805. [DOI] [PubMed] [Google Scholar]
- 25.Alborzi A, Pouladfar GR, Fakhar M. Case report: Isolation of Leishmania tropica from a patient with visceral leishmaniasis and disseminated cutaneous leishmaniasis, Southern Iran. Am J Trop Med Hyg. 2008;79(3):435–7. doi: 10.4269/ajtmh.2008.79.435. [DOI] [PubMed] [Google Scholar]
- 26.Sarkari B, Ahmadpour NB, Moshfe A, Hajjaran H. Molecular evaluation of a case of visceral leishmaniasis due to Leishmania tropica in Southwestern Iran. Iran J Parasitol. 2016;1:126–30. [PMC free article] [PubMed] [Google Scholar]
- 27.Thakur L, Singh KK, Shanker V, Negi A, Jain A, Matlashewski G, Jain M. Atypical leishmaniasis: A global perspective with emphasis on the Indian subcontient. Plos Negl Trop Dis. 2018;12(9):e0006659. doi: 10.1371/journal.pntd.0006659. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Khanra S, Datta S, Mondal D, Saha P, Bandopadhyay SK. RFLPs of ITS, ITS1 and hsp70 amplicons and sequencing of ITS1 of recent clinical isolates of Kala-azar from India and Bangladesh confims the association of L. tropica with the disease. Acta Trop. 2012;124:229–34. doi: 10.1016/j.actatropica.2012.08.017. [DOI] [PubMed] [Google Scholar]
- 29.Ibarra-Meneses AV, Corbeil A, Wagner V, Onwuchekwa C, Fernandez-Prada C. Identification of asymptomatic Leishmania infections: a scoping review. Parasit Vector. 2022;15(1):5. doi: 10.1186/s13071-021-05129-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Gupta AKSingh A, Srivastava S, Mishra PS, Singh S. Visceral Leishmaniasis in children: Diagnosis, treatment, and prevention. J Pediatr Infect Dis. 2017 June;12:214–221. doi: 10.1055/s-0037-1603500. [DOI] [Google Scholar]
- 31.Dursun O, Erişir S, Yeşilipek A. Visceral childhood leishmaniasis in southern Turkey: experience of twenty years. Turk J Pediatr. 2009;51(1):1–5. [PubMed] [Google Scholar]
- 32.Özavcı H, Kaplan M. Cloning and molecular characterization of thiolspecific antioxidant gene of Leishmania tropica Turkey isolate. Turk J Med Sci. 2019;49(1):392–402. doi: 10.3906/sag-1808-98. doi: 10.3906/sag-1808-98. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Alves F, Bilbe G, Blesson S, Goyal V, Monnerat S, Mowbray C, Muthoni Ouattara G, Pécoul B, Rijal S, Rode J, Solomos A, Strub-Wourgaft N, Wasunna M, Wells S, Zijlstra EE, Arana B, Alvar J. Recent Development of Visceral Leishmaniasis Treatments: Successes, Pitfalls, and Perspectives. Clin Microbiol Rev. 2018;31(4):e00048–18. doi: 10.1128/CMR.00048-18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Hadighi R, Mohebali M, Boucher P, Hajjaran H, Khamesipour A, Ouellette M. Unrespon-siveness to glucantime treatment in Iranian cutaneous leishmaniasis due to drug¬resistant Leishmania tropica parasites. PLoS Med. 2006;3:e162. doi: 10.1371/journal.pmed.0030162. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Apa H, Devrim İ, Bayram N, Deveci R, Demir-Özek G, Cartı ÖU. Liposomal amphotericin B versus pentavalent antimony salts for visceral Leishmania in children. Turk J Pediatr. 2013;55(4):378–83. [PubMed] [Google Scholar]