Abstract
More than 70% of breast cancers contain lymphocytic infiltration in the stroma and preclinical studies suggest that immune-editing and partial control of cancer progression by the local immune microenvironment operates in most breast cancers. Consistent with this hypothesis, a large number of studies demonstrated a favorable prognostic and chemotherapy response predictive role for immune infiltration in breast cancer. The evidence is particularly strong for triple negative and HER2 positive cancers. The development of clinically effective immune checkpoint inhibitors now provides an opportunity to test the therapeutic potential of augmenting the local anti-tumor immune response. Several Phase I clinical trials using single agent anti-PD1 and anti-PDL1 antibodies demonstrated objective tumor response rates, with remarkably durable responses, in heavily pretreated, metastatic, triple negative cancers and somewhat lower responses in estrogen-receptor positive cancers. Currently, close to 50 ongoing, or soon to open, clinical trials evaluate the role of this new treatment modality in breast cancer.
Background
The prognostic and predictive roles of the immune microenvironment in breast cancer
The presence of immune cells in the breast cancer microenvironment has long been recognized as a good prognostic indicator (1). More recently, it also became clear that the prevalence of lymphocytic infiltration and its prognostic role varies by molecular subtype. Immune infiltration is most prevalent in triple negative breast cancers (TNBC) followed by HER2 positive and highly proliferative estrogen receptor (ER) positive cancers. Immune infiltration is least prominent in low grade, luminal A type, ER positive cancers.
In TNBC, high levels of immune infiltration, measured either as tumor infiltrating lymphocyte (TIL) count or captured by various immune gene signatures, predicts for good survival even in patients not receiving systemic adjuvant therapy, indicating a pure prognostic function (2,3). Additionally, several neoadjuvant (preoperative) chemotherapy studies demonstrated significantly higher pathologic complete response (pCR) rates among immune-rich compared to immune-poor TNBC, indicating a chemotherapy response predictive role (4–7). Not surprisingly, among TNBC patients who received adjuvant chemotherapy, TIL counts are strongly predictive of cancer-free survival; each 10% increase in TIL count is associated with an 18% reduction of risk of distant recurrence (8,9). At diagnosis, approximately 5–15% of TNBCs are classified as lymphocyte predominant (LPBC), variably defined as either ≥ 50% or ≥ 60% lymphocytes in the stroma, another 15–20% has no lymphocytic infiltration, while the majority (65–80%) harbor low to moderate level of immune cells (9,10). Both stromal lymphocytes (residing in the stroma without direct contact with neoplastic cells) and intratumoral lymphocytes (intermingled with and in direct contact with cancer cells) provide prognostic and predictive information but stromal TILs are more abundant and therefore, can be quantified more reliably (11). Lymphocyte predominance in residual cancer (≥ 60% of stromal cells) after neoadjuvant chemotherapy is seen in about 10% of TNBC treated with neoadjuvant chemotherapy, and is also associated with excellent survival even in patients who have high risk pathologic features such as positive nodes or > 2 cm residual tumor size (12).
In HER2 positive breast cancer, TIL and immune signatures are also associated with better prognosis with or without systemic adjuvant therapy (13). Similar to TNBC, each 10% increase in TILs is associated with a significantly decreasing risk of distant recurrence in patients receiving adjuvant chemotherapy concomitant with trastuzumab (14). This association with outcome was confirmed in the NeoALTTO, but not in the N9831 trial (15). The expression of CD40 (a co-stimulatory protein on antigen presenting cells) related genes was associated with higher probability of achieving pCR to neoadjuvant trastuzumab containing chemotherapy in HER2 positive cancers (16), however, TILs did not show a linear association with pCR in the NeoALTTO and NeoSphere trials, while it was shown that patients with intermediate TIL infiltration significantly benefited from HER2-targeted therapies (15,17). NeoSphere also demonstrated a more complex interplay between the immune system and clinical response in the presence of monoclonal antibodies. This trial included a combined treatment arm of trastuzumab and pertuzumab without chemotherapy. Higher expression of several immune genes and metagenes were associated with a higher pCR rate, while PDL1 mRNA expression and MHC1 metagenes were associated with resistance. (17).
The prognostic and predictive value of immune cells in estrogen receptor (ER) positive cancers is less extensively studied. However, the available literature suggests that in low risk ER positive patients no such prognostic role is apparent while in highly proliferative ER-positive cancers immune cells do predict for better prognosis (18).
Overall, a highly consistent body of literature indicates an association between survival and immune cells in the breast cancer microenvironment. These associations are particularly strong in TNBC and HER2 positive cancers, but can also be seen in high risk ER positive cancers and raise the possibility that immune cells mediate the observed favorable clinical outcome.
The local immune system in breast cancer
Several outstanding reviews have been published recently on the tumor promoting and suppressing roles role of immune and inflammatory cells (19–21). Cancer tissues are host to multiple different types of immune cells mediating innate and adoptive immunity. However, there are large cancer to cancer differences in the extent and composition of immune cells. In the majority of the literature, T-lymphocytes represent the largest proportion of immune cells in breast cancer (70–80%), followed by B-cells (10–20%), macrophages (5–10%), natural killer (NK) cells (<5%) and antigen presenting dendritic cells (4,10, 22). Each of these main cell types can be subdivided into further functional subtypes (e.g. CD8+ effector T cells, CD4+ T helper cells and CD4+ regulatory T cells [Th1, Th2, Treg]) and cells can be found in different activity states (e.g. naïve, activated and memory). The cells form a complex system with dynamic transitions between immune activating and suppressing functions. The obligatory, simultaneous presence of multiple different immune cell types in the microenvironment accounts for the highly correlated nature of immune gene expression patterns (5,17). The strong co-expression of various immune genes explains several seemingly paradoxical associations. For example, high PD1 (programmed death 1) and PD-L1 (programmed death ligand 1) expression, both negative regulators of the local immune response, are associated with better overall survival and higher pCR rate in TNBC (23, 24). Also, high expression of CTLA4 (cytotoxic T lymphocyte associated protein 4), a complimentary immune checkpoint mechanism to PD1/PD-L1, was associated with benefit from anti-PD-L1 antibody therapy to the same extent as PD-L1 expression in lung cancer (25). The strong correlation between immune marker expression and lymphocyte counts could also limit the independent predictive and prognostic value that immune marker expression adds to TIL counts (5,7). It is also important to recognize that there are several methodological concerns regarding detection of PD-L1 (and other immune marker) expression; these include lack of standardized detection methods by immunohistochemistry (IHC), variable cutoffs to determine positivity, and often substantial discordance between mRNA and IHC based measurements (7,24). Furthermore, multiple different cell types (neoplastic as well as stromal) can express these markers and expression levels can be up- or down-regulated in response to an ongoing antitumor immune response, hypoxia, and oncogenic pathway activation (26). These sources of variation contribute to the conflicting results reported in the literature. A central question also remains unanswered; what biological mechanism underlies the variable levels of immune infiltration and different levels of immune control in different breast cancers.
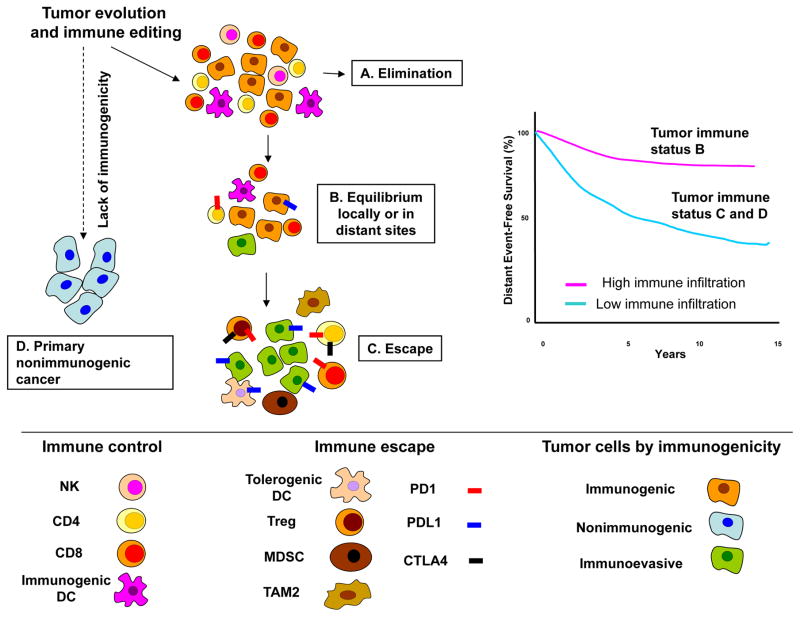
Results from pre-clinical experiments and correlative observations in patients suggest that most breast cancers trigger some immune response (22). According the immune-editing hypothesis, the local immune response plays a dual role in cancer progression. On one hand, it suppresses tumor growth through immune-mediated cell death, which may result in complete elimination of some cancers (before they become detectable) and slow growth or stagnation in others. On the other hand, it also promotes tumor progression by establishing inflammatory conditions that facilitate tumor growth and selecting for tumor cells that survive immunosurveillance (27). An important corollary of this hypothesis is that even during the escape phase, when cancers are clinically apparent, some degree of immune-mediated control is retained, which may account for the better prognosis observed in the immune-rich cancers (Figure 1).
Figure 1.
Immunoediting during tumor evolution. All clinically apparent early breast cancers are already partially edited or not immunogenic enough since the elimination phase (A) has failed. Tumors in the equilibrium phase (B) are likely represented in the high immune infiltration group. Recurrences in this group are at least in part due to subsequent immune escape. Tumors with low immune infiltration may include cancers with intrinsicly low immunogenicity and cancers that have effectively escaped from immune surveillance (C, D). Abbreviations: DC, dendritic cells; MDSC, myeloid-derived suppressor cells; TAM1, tumor-associated macrophages M1 or classically activated; TAM2, tumor-associated macrophages M2 or alternatively activated.
Another important concept emerging from preclinical models is that tumor response to chemotherapy and trastuzumab is influenced by the host immune system (28). Chemotherapy-induced cellular injury, particularly caused by doxorubicin and cyclophosphamide, can elicit a cytotoxic immune response that partially mediates the clinical response. It has also been suggested that chemotherapy may induce somatic mutations, leading to new antigens which, in turn, elicit immune responses. Chemotherapy, in a drug and dose dependent manner, can also stimulate anticancer immune effectors indirectly by inhibiting immunosuppressive regulatory cells (e.g. myeloid-derived suppressor cells and FOXP3+ regulatory T cells) (29, 30). Consistent with these pre-clinical observations, analysis of TILs in pre- and post-neoadjuvant chemotherapy specimens showed that development of lymphocytic infiltration during treatment correlates with clinical response (31). The development of clinically effective immune checkpoint inhibitors now provides an opportunity to test the therapeutic potential of augmenting the local anti-tumor immune response.
On the Horizon
Immune biomarkers
In most analyses, the prognostic and predictive values of TILs and immune gene signatures are independent of histologic grade, tumor size or nodal status and therefore, immune markers hold a potential for increasing the predictive accuracy of existing prognostic models (2–6). Furthermore, the reproducibility of stromal TIL counts among pathologists is high; for LPBC category, inter-pathologist agreement ranged from good to moderate (Cohen’s kappa, κ = 0.60 to 0.90) and consistency for semi-quantitative TIL scoring was excellent (correlation coefficient, 0.97) (4). These results are similar to other broadly accepted measures such histologic grading or hormone receptor scoring and better than inter-observer agreement for Ki-67. An international guideline was recently published to standardize TIL assessment and reporting which sets the stage for introducing this prognostic variable into routine pathology reporting (11). However, no studies have been performed to date that included immune signatures, or TIL counts, in existing multivariate prognostic models such as Adjuvant Online, Nottingham Prognostic Index, 21-gene Recurrence Score, Risk of Recurrence (ROR) score, or others to demonstrate improved prognostic accuracy and therefore lymphocyte markers are not yet recommended for routine clinical use.
Immune parameters are also attractive candidates to be predictors of response to immunotherapy. In the simplest form, one could hypothesize that immunotherapy will be most useful for cancers with intermediate TIL counts because LPBCs already have an excellent prognosis and cancers with no lymphocytes have no local immune surveillance to boost. The validity of this hypothesis is being tested in ongoing immunotherapy trials in breast cancer. The therapeutic anti-PD1/PDL1 antibodies represent one of the most exciting novel class of therapies due to the remarkably durable responses in melanoma, lung, head and neck and bladder cancers (32). PD1 is broadly expressed on several different cells types including CD4 and CD8 positive T-cells, B lymphocytes, NK cells and T regulatory cells, and therefore it is considered of limited biomarker value. Most studies focused on PD-L1 expression as a potential response marker for PD1/PD-L1 targeted therapies. In breast cancer, PD-L1 protein expression (i.e. ≥ 1% of IHC+ cells) is detected in 20–30% of cases, primarily seen in TNBC (7, 33–35) while PD-L1 mRNA expression is identified in substantially larger subsets of breast tumors (16, 23, 24, 34, 35). The correlation between PD-L1 protein and mRNA levels is modest (Spearman Rank Correlation Coefficient 0.15–0.17) (35). In other cancer types, there is a statistically significant association between PD-L1 expression and the amount of clinical benefit from immune checkpoint therapy; but in each of these studies response and clinical benefit is also consistently seen in PD-L1 negative cancers (25). Pembrolizumab, an anti-PD1 antibody, is currently approved by the US Food and Drug Administration (FDA) for the treatment of metastatic non-small cell lung cancer (NSCLC) that expresses PD-L1 protein detected by a companion diagnostic IHC assay (IHC 22C3 pharmDx test made by Dako North America). Interestingly, another anti-PD1 antibody, nivolumab, is also approved by the FDA for the treatment of metastatic squamous cell lung cancer, but without the requirement of a companion diagnostic test. However, a recent FDA indication extension of nivolumab to patients with NSCLC (including non-squamous cell) endorses the use of a complementary diagnostic assay (IHC 28-8 pharmDx, also made by Dako North America but distinct from IHC 22C3 and applying a different threshold to define positivity) to help guide patient selection for treatment. The test is considered “complementary,” not “companion,” diagnostic because its use is not mandated prior to administering nivolumab. It is important to note that most PD-L1 expression is detected on stromal cells and not on cancer cells, hence the often cited explanation that PD-L1 expression by tumor cells is a main mechanism of immune escape appears simplistic.
Currently, no published data exists on the predictive value of PD-L1 expression for immune checkpoint inhibitor therapy in breast cancer. However, all Phase I trials in breast cancer that reported clinical outcome required PD-L1 expression for eligibility.
Immunotherapy of breast cancer
Preliminary results from 5 Phase I clinical trials testing the activity of immune checkpoint inhibitors in metastatic breast cancer are currently available in abstract form. There is also one published phase I trial (n=26) that reported results for tremelimumab (anti-CTLA4 antibody) in combination with exemestane in ER positive metastatic breast cancer and demonstrated stable disease for ≥12 weeks in 11 patients (42%) as the best overall response (36). The KEYNOTE-012 trial assessed the safety and efficacy of single pembrolizumab (10 mg/kg every 2 weeks) in metastatic TNBC that showed ≥ 1% PD-L1 positivity by IHC. One hundred and eleven patients were screened for PD-L1 expression using the 22C3 antibody and 59% were positive. In the 27 patients who were evaluable for efficacy assessment, the overall response rate was 18.5% and the median duration of response was not reached at the time of the presentation at the 2014 San Antonio Breast Cancer Symposium (37). The KEYNOTE-028 trial assessed the same drug in metastatic ER-positive breast cancer and also required ≥ 1% PD-L1 positivity by IHC; PD-L1 positivity rate was 19%. In the 25 patients who were evaluable for efficacy, the overall response rate was 12% and all 3 responders remained on study treatment for ≥26 weeks at the time of presentation at the 2015 San Antonio Breast Cancer Symposium (38). Adverse events were mostly grade 1–2 and included arthralgia, fatigue, myalgia, and nausea in both studies. Another Phase I trial tested the efficacy and safety of the anti-PD-L1 antibody atezolizumab (15 mg/kg, 20 mg/kg, and 1200 mg fixed dose) in metastatic TNBC and also required ≥5% PD-L1 positivity by IHC using the SP142 antibody (39). Sixty-nine percent of patients tested positive for PD-L1 expression, 21 were evaluable for efficacy, and 19% objective response rate was observed, the 24-week progression-free survival rate was 27%. Adverse events were mostly ≤ grade 2 but 11% of pastients had treatment-related ≥ grade 3 adverse events. The JAVELIN study tested the anti-PD-L1 antibody avelumab (10 mg/kg every 2 weeks) and included all breast cancer subtypes regardless PDL1 status (40). In the TNBC cohort (n=58), the response rate was 8.6%. In the ER-positive/HER2-negative (n=72) and HER2-positive (n=26) cohorts the response rate was 2.8% and 3.8%, respectively. The preliminary results suggested higher response rate in tumors with PD-L1 positive immune cells (33.3% [4/12] vs 2.4% [3/124]). Preliminary results were also reported from a study that combined atezolizumab (anti-PDL1 antibody) with Nab-Paclitaxel in metastatic TNBC (n=24) (41). The combination was well tolerated and 42% of patients had objective response. Due to these promising early results, there are currently around 50 clinical trials that evaluate this class of drugs in breast cancer in the metastatic, neoadjuvant and adjuvant treatment settings (Table 1).
Table 1.
Ongoing clinical trials with immunotherapies that accrue breast cancer patients. Data extracted from https://clinicaltrials.gov/ and accessed on January 24, 2016.
| Phase | Clinical Trial Gov | Disease setting | Type of disease | Breast cancer subtype | Immunotherapies | Combined treatments |
|---|---|---|---|---|---|---|
| I | NCT02303366 | Metastatic | Only BC | All | Pembrolizumab | Stereotactic Ablative Body Radiosurgery |
| I | NCT02605915 | Metastatic and neoadjuvant | Only BC | HER2-pos | Atezolizumab | Trastuzumab/pertuzumab or T-DM1 or Trastuzumab/Pertuzumab/Carbopla tin/Docetaxel |
| I | NCT02649686 | Metastatic | Only BC | HER2-pos | Durvalumab | Trstuzumab |
| I/II | NCT02129556 | Metastatic | Only BC | HER2-pos | Pembrolizumab | Trastuzumab |
| I/II | NCT02513472 | Metastatic | Only BC | TNBC | Pembrolizumab | Eribulin mesylate |
| I/II | NCT02628132 | Metastatic | Only BC | TNBC | Durvalumab | Paclitaxel |
| II | NCT02411656 | Metastatic* | Only BC | TNBC or ER+/HER2− | Pembrolizumab | |
| II | NCT02447003 | Metastatic | Only BC | TNBC | Pembrolizumab | |
| II | NCT02499367 | Metastatic | Only BC | TNBC | Nivolumab | Doxorubicin low dose, Cyclophosphamide metronomic, Radiation therapy, Cisplatin |
| II | NCT02411656 | Metastatic | Only BC | HER2-neg | Pembrolizumab | |
| II | NCT02447003 | Metastatic | Only BC | TNBC | Pembrolizumab | |
| II | NCT02395627 | Metastatic | Only BC | HR+ (endocrine resistant BC) | Pembrolizumab | Vorinostat and Tamoxifen |
| II | NCT02536794 | Metastatic | Only BC | TNBC ER+/HER2-neg |
Durvalumab Tremelimumab |
|
| II | NCT02563925 | Metastatic (brain) | Only BC | All | Tremelimumab | Brain radiotherapy or Stereotactic |
| II | NCT00083278 | Metastatic | Only BC | All | Ipilimumab | |
| II | NCT02648477 | Metastatic | Only BC | TNBC and ER+/HER2− | Pembrolizumab | Doxorubicin or Letrozole or Anastrozole or Exemestane |
| III | NCT02555657 | Metastatic | Only BC | TNBC | Pembrolizumab‡ | |
| III | NCT02425891 | Metastatic | Only BC | TNBC | Atezolizumab¶ | Nab-paclitaxel |
| I | NCT02622074 | Neoadjuvant | Only BC | TNBC (LABC) | Pembrolizumab | Nab-paclitaxel → AC or Nab-paclitaxel/Carboplatin → AC |
| I/II | NCT02489448 | Neoadjuvant | Only BC | TNBC | Durvalumab | Nab-paclitaxel → ddAC |
| II | NCT01042379 | Neoadjuvant | Only BC | All | Pembrolizumab | Paclitaxel |
| II | NCT02530489 | Neoadjuvant | Only BC | TNBC | Atezolizumab | Nab-paclitaxel |
| III | NCT02620280 | Neoadjuvant | Only BC | TNBC | Atezolizumab§ | Nab-paclitaxel/Carboplatin |
| II | NCT01502592 | Pre-surgical | Only BC | All | Ipilimumab | Cryoablation |
| I | NCT02453620 | Metastatic or LABC | Multiple | TNBC ER+/HER2-neg |
Nivolumab +/− Ipilimumab |
Etinostat |
| I | NCT01375842 | Metastatic | Multiple | TNBC | Atezolizumab | |
| I | NCT02309177 | Metastatic | Multiple | TNBC ER+/HER2-neg |
Nivolumab | Nab-paclitaxel |
| I | NCT00836888 | Metastatic | Multiple | All | Nivolumab | |
| I | NCT02655822 | Metastatic | Multiple | TNBC | Atezolizumab CPI-444 |
|
| I | NCT01848834 | Metastatic | Multiple | TNBC | Pembrolizumab | |
| I | NCT02054806 | Metastatic | Multiple | All | Pembrolizumab | |
| I | NCT01772004 | Metastatic | Multiple | All | Avelumab | |
| I | NCT01975831 | Metastatic | Multiple | ER+/HER2− and HER2-pos | Durvalumab Tremelimumab |
|
| I | NCT02658214 | Metastatic | Multiple | TNBC | Durvalumab Tremelimumab |
Gemcitabine/carboplatin or nab-paclitaxel/carboplatin |
| I/II | NCT02318901 | Metastatic | Multiple | HER2-pos | Pembrolizumab | Trastuzumab or TDM1 |
| I/II | NCT02543645 | Metastatic | Multiple | TNBC | Atezolizumab Varlilumab |
|
| I/II | NCT02657889 | Metastatic | Multiple | TNBC | Pembrolizumab | Niriparib |
| I/II | NCT02178722 | Metastatic | Multiple | TNBC | Pembrolizumab INCB024360 (IDO inhibitor) |
|
| I/II | NCT02331251 | Metastatic | Multiple | TNBC and ER+/HER2− | Pembrolizumab | Vinorelbine (ER+/HER2−) Gemcitabine (TNBC) |
| I/II | NCT01928394 | Metastatic | Multiple | TNBC | Nivolumab +/− Ipilimumab |
|
| I/II | NCT02452424 | Metastatic | Multiple | TNBC | Pembrolizumab PLX3397 (anti-CSF1R) |
|
| I/II | NCT02331251 | Metastatic | Multiple | All | Pembrolizumab | Various CT |
| I/II | NCT02318901 | Metastatic | Multiple | HER2-pos | Pembrolizumab | Trastuzumab or TDM1 |
| I/II | NCT02543645 | Metastatic | Multiple | TNBC | Atezolizumab Varlilumab (CD27 agonist) |
|
| I/II | NCT02403271 | Metastatic | Multiple | TNBC and HER2-pos | Durvalumab | Ibrutinib |
| I/II | NCT02404441 | Metastatic | Multiple | TNBC | PDR001 | |
| I/II | NCT02643303 | Metastatic | Multiple | All | Durvalumab and Poly-ICLC +/− Tremelimumab |
|
| II | NCT02661100 | Metastatic | Multiple | TNBC | Pembrolizumab CDX-1401 and Poly-ICLC |
|
| II | NCT02644369 | Metastatic | Multiple | TNBC | Pembrolizumab | |
| II | NCT02527434 | Metastatic | Multiple | TNBC | Tremelimumab Durvalumab |
|
| II | NCT02478099 | Metastatic | Multiple | TNBC | Atezolizumab |
Note: Ipilimumab, Tremelimumab (anti-CTLA4); Nivolumab, Pembrolizumab, PDR001 (anti-PD1); Durvalumab, Atezolizumab, Avelumab (anti-PDL1)
Abbreviations: BC, Breast Cancer; TNBC, triple negative breast cancer; ddAC, dose dense doxorubicin and cyclophosphamide; IBC, inflammatory breast cancer;
Including only metastatic inflammatory breast cancer, with clinical response after receiving chemotherapy
Usage of investigational imaging (89Zr-MPDL3280A-PET and 18F-FB-IL2-PET) as complementary tools for selection of patients to be treated with Atezolizumab
Randomized trial versus chemotherapy single agent (capecitabine, eribulin, gemcitabine, or vinorelbine)
Randomized versus nab-paclitaxel (first line metastatic disease)
Randomized versus nab-paclitaxel/carboplatin in locally advanced TNBC
Summary
Immune checkpoint inhibitors emerged as a new and effective treatment modality for melanoma, NSCLC and RCC where these drugs are now approved by the US FDA. Clinical trials also show activity in a broad range of solid tumors including TNBC and to a lesser extent ER-positive breast cancer. A large number of clinical trials in the neoadjuvant and metastatic setting are now underway to determine the clinical role of immunotherapies and their combinations in breast cancer.
Acknowledgments
Grant Support
This work was supported in part by grants from the Breast Cancer Research Foundation and Yale Cancer Center Core Grant NIH/NCI P30CA16359 (to L. Pusztai), the H.W. & J. Hector-Stiftung, Mannheim (M67; to T. Karn), and the Associazione Italiana per la Ricerca sul Cancro (AIRC) (MFGA 13428; to G. Bianchini).
Footnotes
Disclosure of Potential Conflicts of Interest
L. Pusztai reports receiving research support from AstraZeneca, Genentech, and Merck and speakers bureau honoraria from Merck. G. Bianchini reports receiving speakers bureau honoraria from Roche. No potential conflicts of interest were disclosed by the other authors.
References
- 1.Hamlin IM. Possible host resistance in carcinoma of the breast: a histological study. British J Cancer. 1968;22:383–401. doi: 10.1038/bjc.1968.47. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Iwamoto T, Bianchini G, Booser D, Qi Y, Coutant C, Shiang C, et al. Gene pathways associated with prognosis and chemotherapy sensitivity in molecular subtypes of breast cancer. J Natl Cancer Inst. 2011;103:264–72. doi: 10.1093/jnci/djq524. [DOI] [PubMed] [Google Scholar]
- 3.Rody A, Karn T, Liedtke C, Pusztai L, Ruckhaeberle E, Hanker L, et al. A clinically relevant gene signature in triple negative and basal-like breast cancer. Breast Cancer Res. 2011;13:R97. doi: 10.1186/bcr3035. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Denkert C, Loibl S, Noske A, Roller M, Muller BM, Komor M, et al. Tumor-associated lymphocytes as an independent predictor of response to neoadjuvant chemotherapy in breast cancer. J Clin Oncol. 2010;28:105–13. doi: 10.1200/JCO.2009.23.7370. [DOI] [PubMed] [Google Scholar]
- 5.Denkert C, Von Minckwitz G, Brase JC, Sinn BV, Gade S, Kronenwett R, et al. Tumor-infiltrating lymphocytes and response to neoadjuvant chemotherapy with or without carboplatin in human epidermal growth factor receptor 2–positive and triple-negative primary breast cancers. J Clin Oncol. 2015;33:983–91. doi: 10.1200/JCO.2014.58.1967. [DOI] [PubMed] [Google Scholar]
- 6.Ono M, Tsuda H, Shimizu C, Yamamoto S, Shibata T, Yamamoto H, et al. Tumor-infiltrating lymphocytes are correlated with response to neoadjuvant chemotherapy in triple-negative breast cancer. Breast Cancer Res Treat. 2012;132:793–805. doi: 10.1007/s10549-011-1554-7. [DOI] [PubMed] [Google Scholar]
- 7.Wimberly H, Brown J, Schalper K, Haack H, Silver M, Nixon C, et al. PD-L1 expession correlates with tumor-infiltrating lumphocytes and response to meoadjuvant chemotherapy in breast cancer. Cancer Immunol Res. 2015;3:326–32. doi: 10.1158/2326-6066.CIR-14-0133. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Loi S, Sirtaine N, Piette F, Salgado R, Viale G, Van Eenoo F, et al. Prognostic and predictive value of tumor-infiltrating lymphocytes in a phase III randomized adjuvant breast cancer trial in node-positive breast cancer comparing the addition of docetaxel to doxorubicin with doxorubicin-based chemotherapy: BIG 02-98. J Clin Oncol. 2013;31:860–7. doi: 10.1200/JCO.2011.41.0902. [DOI] [PubMed] [Google Scholar]
- 9.Adams S, Gray RJ, Demaria S, Goldstein L, Perez EA, Shulman LN, et al. Prognostic value of tumor-infiltrating lymphocytes in triple-negative breast cancers from two phase III randomized adjuvant breast cancer trials: ECOG 2197 and ECOG 1199. J Clin Oncol. 2014;32:2959–66. doi: 10.1200/JCO.2013.55.0491. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Ruffell B, Au A, Rugo HS, Esserman LJ, Hwang ES, et al. Leukocyte composition of human breast cancer. Proc Natl Acad Sci. 2012;109:2796–801. doi: 10.1073/pnas.1104303108. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Salgado R, Denkert C, Demaria S, Sirtaine N, Klauschen F, Pruneri G, et al. The evaluation of tumor-infiltrating lymphocytes (TILs) in breast cancer: recommendations by an International TILs Working Group 2014. Ann Oncol. 2015;26:259–71. doi: 10.1093/annonc/mdu450. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Dieci MV, Criscitiello C, Goubar A, Viale G, Conte P, Guarneri V, et al. Prognostic value of tumor-infiltrating lymphocytes on residual disease after primary chemotherapy for triple-negative breast cancer: a retrospective multicenter study. Ann Oncol. 2014;25:611–8. doi: 10.1093/annonc/mdt556. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Perez EA, Thompson EA, Ballman KV, Anderson SK, Asmann YW, Kalari KR, et al. Genomic analysis reveals that immune function genes are strongly linked to clinical outcome in the north central cancer treatment group n9831 adjuvant trastuzumab trial. J Clin Oncol. 2015;33:701–8. doi: 10.1200/JCO.2014.57.6298. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Loi S, Michiels S, Salgado R, Sirtaine N, Jose V, Fumagalli D, et al. Tumor infiltrating lymphocytes are prognostic in triple negative breast cancer and predictive for trastuzumab benefit in early breast cancer: results from the FinHER trial. Ann Oncol. 2014;25:1544–50. doi: 10.1093/annonc/mdu112. [DOI] [PubMed] [Google Scholar]
- 15.Salgado R, Denkert C, Campbell C, Savas P, Nucifero P, Aura C, et al. Tumor-infiltrating lymphocytes and associations with pathological complete response and event-free survival in HER2-positive early-stage breast cancer treated with lapatinib and trastuzumab: a secondary analysis of the NeoALTTO Trial. JAMA Oncol. 2015;1:448–54. doi: 10.1001/jamaoncol.2015.0830. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Esteva FJ, Wang J, Lin F, Mejia JA, Yan K, Altundag K, et al. CD40 signaling predicts response to preoperative trastuzumab and concomitant paclitaxel followed by 5-fluorouracil, epiribucin, and cyclophosphamide in HER-2-overexpressing breast cancer. Breast Cancer Res. 2007;9:R87. doi: 10.1186/bcr1836. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Bianchini G, Pusztai L, Pienkowski T, Im YH, Bianchi GV, Tseng LM, et al. Immune modulation of pathologic complete response after neoadjuvant HER2-directed therapies in the NeoSphere trial. Ann Oncol. 2015;26:2429–36. doi: 10.1093/annonc/mdv395. [DOI] [PubMed] [Google Scholar]
- 18.Bianchini G, Qi Y, Hugo AR, Iwamoto T, Coutant C, Ibrahim N, et al. Molecular anatomy of breast cancer stroma and its prognostic value in ER-positive and -negative cancers. J Clin Oncol. 2010;28:4316–23. doi: 10.1200/JCO.2009.27.2419. [DOI] [PubMed] [Google Scholar]
- 19.Andre F, Dieci MV, Dubsky P, Sotiriou C, Curigliano G, Denkert C, et al. Molecular pathways: involvement of immune pathways in the therapeutic response and outcome in breast cancer. Clin Cancer Res. 2013;19:28–33. doi: 10.1158/1078-0432.CCR-11-2701. [DOI] [PubMed] [Google Scholar]
- 20.Gingras I, Azim HA, Ignatiadis M, Sotiriou C. Immunology and breast cancer: toward a new way of understanding breast cancer and developing novel therapeutic strategies. Clin Adv Hem Oncol. 2015;13:372–82. [PubMed] [Google Scholar]
- 21.Karn T, Pusztai L, Rody A, Holtrich U, Becker S. The influence of host factors on the prognosis of breast cancer: stroma and immune cell components as cancer biomarkers. Curr Cancer Drug Targets. 2015;15:652–64. doi: 10.2174/156800961508151001101209. [DOI] [PubMed] [Google Scholar]
- 22.Coventry BJ, Weightman MJ, Bradley J, Skinner JM. Immune profiling in human breast cancer using high-sensitivity detection and analysis techniques. J Roy Soc Medicine. 2015;6:1–12. doi: 10.1177/2054270415603909. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Sabatier R, Finetti P, Mamessier E, Adelaide J, Chaffanet M, Ali HR, et al. Prognostic and predictive value of PDL1 expression in breast cancer. Oncotarget. 2015;6:5449–64. doi: 10.18632/oncotarget.3216. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Schalper K, Velcheti V, Carvajal D, et al. In situ tumor PD-L1 mRNA expression is associated with increased TILs and better outcome in breast carcinomas. Clin Cancer Res. 2014;20:2773–82. doi: 10.1158/1078-0432.CCR-13-2702. [DOI] [PubMed] [Google Scholar]
- 25.Herbst RS, Soria JC, Kowanetz M, Fine GD, Hamid O, Gordon MS, et al. Predictive correlates of response to the anti-PD-L1 antibody MPDL3280A in cancer patients. Nature. 2014;515:563–67. doi: 10.1038/nature14011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Mittendorf EA, Philips AV, Meric-Bernstam F, Qiao N, Wu Y, et al. PD-L1 Expression in triple-negative breast cancer. Cancer Immunol Res. 2014;2:361–70. doi: 10.1158/2326-6066.CIR-13-0127. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Schreiber RD, Old LJ, Smyth MJ. Cancer immunoediting: integrating immunity’s roles in cancer suppression and promotion. Science. 2011;331:1565–70. doi: 10.1126/science.1203486. [DOI] [PubMed] [Google Scholar]
- 28.Zitvogel L, Kepp O, Kroemer G. Immune parameters affecting the efficacy of chemotherapeutic regimens. Nat Rev Clin Oncol. 2011;8:151–60. doi: 10.1038/nrclinonc.2010.223. [DOI] [PubMed] [Google Scholar]
- 29.Vincent J, Mignot G, Chalmin F, et al. 5-Fluorouracil selectively kills tumor-associated myeloid-derived suppressor cells resulting in enhanced T cell-dependent antitumor immunity. Cancer Res. 2010;70:3052–61. doi: 10.1158/0008-5472.CAN-09-3690. [DOI] [PubMed] [Google Scholar]
- 30.Roselli M, Cereda V, di Bari MG, Formica V, Spila A, Jochems C, et al. Effects of conventional therapeutic interventions on the number and function of regulatory T cells. Oncoimmunology. 2013;2:e27025. doi: 10.4161/onci.27025. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Demaria S, Volm MD, Shapiro RL, Yee HT, Oratz R, Formenti SC, et al. Development of tumor-infiltrating lymphocytes in breast cancer after neoadjuvant paclitaxel chemotherapy. Clin Cancer Res. 2001;7:3025–30. [PubMed] [Google Scholar]
- 32.Topalian SL, Drake CG, Pardoll DM. Immune checkpoint blockade: a common denominator approach to cancer therapy. Cancer Cell. 2015;27:450–61. doi: 10.1016/j.ccell.2015.03.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Mittendorf EA, Philips AV, Meric-Bernstam F, Qiao N, Wu Y, Harrington S, et al. PD-L1 expression in triple-negative breast cancer. Cancer Immunol Res. 2014;2:361–70. doi: 10.1158/2326-6066.CIR-13-0127. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Soliman H, Khalil F, Antonia S. PD-L1 expression is increased in a subset of basal type breast cancer cells. PloS One. 2014;9:e88557. doi: 10.1371/journal.pone.0088557. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Ali HR, Glont SE, Blows FM, Provenzano E, Dawson SJ, Liu B, et al. PD-L1 protein expression in breast cancer is rare, enriched in basal-like tumours and associated with infiltrating lymphocytes. Ann Oncol. 2015;26:1488–93. doi: 10.1093/annonc/mdv192. [DOI] [PubMed] [Google Scholar]
- 36.Vonderheide RH, LoRusso PM, Khalil M, Gartner EM, Khaira D, Soulieres D, et al. Tremelimumab in combination with exemestane in patients with advanced breast cancer and treatment-associated modulation of inducible costimulator expression on patient T cells. Clin Cancer Res. 2010;16:3485–94. doi: 10.1158/1078-0432.CCR-10-0505. [DOI] [PubMed] [Google Scholar]
- 37.Nanda R, Chow LQ, Dees EC, Berger R, Gupta S, Geva R, et al. A phase Ib study of pembrolizumab (MK-3475) in patients with advanced triple-negative breast cancer [abstract]. Cancer Res; Proceedings of the Thirty-Seventh Annual CTRC-AACR San Antonio Breast Cancer Symposium; 2014 Dec 9–13; San Antonio, TX. Philadelphia (PA): American Association for Cancer Research; 2015. Abstract nr S1–09. [Google Scholar]
- 38.Rugo HS, Delord J-P, Im S-A, Ott PA, Piha-Paul SA, Bedard PL, et al. Preliminary efficacy and safety of pembrolizumab (MK-3475) in patients with PD-L1-positive, estrogen receptor-positive (ER+)/HER2-negative advanced breast cancer enrolled in KEYNOTE-028 [abstract]. Proceedings of the Thirty-Eighth Annual CTRC-AACR San Antonio Breast Cancer Symposium; 2015 Dec 6–10; San Antonio, TX. Philadelphia (PA): American Association for Cancer Research; 2015. Abstract nr S5–07. [Google Scholar]
- 39.Emens LA, Braiteh FS, Cassier P, Delord J-P, Eder JP, Fasso M, et al. Inhibition of PD-L1 by MPDL3280A leads to clinical activity in patients with metastatic triple-negative breast cancer (TNBC) [abstract]. Cancer Res; Proceedings of the 106th Annual Meeting of the American Association for Cancer Research; 2015 Apr 18–22; Philadelphia, PA. Philadelphia (PA): AACR; 2015. Abstract nr 2859. [Google Scholar]
- 40.Dirix LY, Takacs I, Nikolinakos P, Jerusalem G, Arkenau H-T, Hamilton EP, et al. Avelumab (MSB0010718C), an anti-PD-L1 antibody, in patients with locally advanced or metastatic breast cancer: a phase Ib JAVELIN solid tumor trial [abstract]. Proceedings of the Thirty-Eighth Annual CTRC-AACR San Antonio Breast Cancer Symposium; 2015 Dec 6–10; San Antonio, TX. Philadelphia (PA): American Association for Cancer Research; 2015. Abstract nr S1–04. [Google Scholar]
- 41.Adams S, Diamond J, Hamilton E, Pohlmann P, Tolaney S, Molinero L, et al. Safety and clinical activity of atezolizumab (anti-PDL1) in combination with nab-paclitaxel in patients with metastatic triple-negative breast cancer [abstract]. Proceedings of the Thirty-Eighth Annual CTRC-AACR San Antonio Breast Cancer Symposium; 2015 Dec 6–10; San Antonio, TX. Philadelphia (PA): American Association for Cancer Research; 2015. Abstract nr P2-11-06. [Google Scholar]