Abstract
Objective:
To assess characteristics and perceptions associated with vaccine hesitancy among healthcare workers to increase coronavirus disease 2019 (COVID-19) vaccine uptake in this population.
Design:
Cross-sectional quantitative survey.
Setting:
A not-for-profit healthcare system in southwestern Virginia.
Participants:
A convenience sample of 2,720 employees of a not-for-profit healthcare system.
Methods:
Between March 15 and 29, 2021, we conducted an Internet-based survey. Our questionnaire assessed sociodemographic and work-related characteristics, vaccine experience and intentions, agreement with vaccine-related perceptions, the most important reasons for getting or not getting vaccinated, and trusted sources of information about COVID-19. We used χ2 analyses to assess the relationship between vaccine hesitancy and both HCW characteristics and vaccine-related perceptions.
Results:
Overall, 18% of respondents were classified as vaccine hesitant. Characteristics significantly associated with hesitancy included Black race, younger age, not having a high-risk household member, and prior personal experience with COVID-19 illness. Vaccine hesitancy was also significantly associated with many vaccine-related perceptions, including concerns about short-term and long-term side effects and a belief that the vaccines are not effective. Among vaccine-acceptant participants, wanting to protect others and wanting to help end the pandemic were the most common reasons for getting vaccinated. Personal physicians were cited most frequently as trusted sources of information about COVID-19 among both vaccine-hesitant and vaccine-acceptant respondents.
Conclusions:
Educational interventions to decrease vaccine hesitancy among healthcare workers should focus on alleviating safety concerns, emphasizing vaccine efficacy, and appealing to a sense of duty. Such interventions should target younger adult audiences. Personal physicians may also be an effective avenue for reducing hesitancy among their patients through patient-centered discussions.
Keywords: Vaccine hesitancy, healthcare workers, COVID-19 vaccines
The US Food and Drug Administration (FDA) granted emergency use authorization of coronavirus disease 2019 (COVID-19) vaccines developed by Pfizer and Moderna in December 2020, and the Johnson & Johnson vaccine received the same authorization in February 2021. Given the high risk of exposure 1 and the importance of keeping healthcare workers (HCWs) well, the Centers for Disease Control and Prevention (CDC) guidelines prioritized HCWs to receive these vaccines starting in December 2020. 2 However, continued reports suggest that many HCWs in the United States are reluctant to receive the COVID-19 vaccine. 3
Although vaccine hesitancy in other contexts has been studied extensively, reasons for HCW reluctance to receive COVID-19 vaccines are not well understood. Studies performed prior to or in the earliest stages of vaccine roll-out identified common HCW barriers to vaccination including concerns about safety, efficacy, and evolving science, as well as perceptions that COVID-19 is mild. 4–8 In some studies, HCWs who were more likely to accept vaccination included those directly involved in COVID-19 patient care or who consider themselves at risk for severe disease, 5 those who believe in vaccine safety, 8 those who believe vaccination will support herd immunity, 8,9 and those who trust public health experts. 4 Being a physician, 5,6 male sex, 3,5 and younger age 9 were also associated with vaccine acceptance among HCWs.
Although these studies provide useful insights, most focused on frontline HCW characteristics and broad vaccine-related perceptions. Additionally, we are not aware of any studies that have examined trusted sources of COVID-19 information among HCWs to inform message dissemination channels.
In the present study, we assessed specific barriers to vaccine uptake among different types of HCWs, including characteristics and vaccine-related perceptions, that can be used to improve outreach and educational messaging to reduce COVID-19 vaccine hesitancy among HCWs.
Methods
Between March 15 and 29, 2021, we conducted a cross-sectional survey targeting all 13,690 employees of a not-for-profit healthcare system in southwestern Virginia comprised of a network of hospitals and ambulatory care facilities. Our survey was developed based on existing vaccine hesitancy literature and consisted of multiple-choice questions about personal experiences with COVID-19, COVID-19 vaccine experience and intentions, COVID-19 vaccine-related perceptions, trusted sources of COVID-19 information, and sociodemographic characteristics. Professional role was captured in broad categories: providers (ie, physicians, physician assistants, or nurse practitioners), nursing staff (ie, nurses, nursing assistants, clinical associates, or nursing management), other responsibilities in patient care areas, other responsibilities in nonpatient care areas, and managers without patient care responsibilities. We used 5-point Likert scales were used to assess positive and negative vaccine-related perceptions; response options ranged from “strongly disagree” to “strongly agree.” Those who had already received at least 1 dose of vaccine were asked their most important reason for deciding to be vaccinated; all others were asked their most important reason for not being vaccinated.
A small pilot test was conducted with infection control staff and frontline HCWs to support comprehensiveness and clarity. The survey was administered through Research Electronic Data Capture (REDCap), a secure, web-based data collection platform for research. An article with a link to the survey was placed prominently on the healthcare system intranet, and a COVID-19 update from the organization’s leadership included a link to the survey. The study team and infection preventionists distributed flyers with a quick response (QR) code to employee break rooms throughout clinical sites. Confidentiality was assured throughout all promotion efforts. Participants who completed the survey could enter a raffle to win one of ten $20 gift cards. Employees self-administered the survey electronically on a computer, laptop, tablet, or smartphone. Responses were deidentified before being shared with the study team. we received a determination from our organization’s institutional review board that this study was not human-subjects research.
The COVID-19 vaccine was widely available to staff in numerous easily accessed locations throughout the healthcare system beginning in December 2020. Because data collection occurred 3 months into vaccine availability for this population, we classified respondents as hesitant if they had not received at least 1 dose of the vaccine at the time of survey completion. 10 All other respondents were considered acceptant. We condensed the 5-point Likert responses into 3 categories (ie, “disagree,” “neither agree nor disagree,” and “agree”) by combining the 2 disagreement categories and the 2 agreement categories. For analyses involving personal experience with COVID-19, “unsure” responses were excluded. We calculated frequencies and proportions associated with each survey item by vaccine hesitancy status. We used χ2 analyses to identify respondent characteristics and vaccine-related perceptions that were associated with vaccine hesitancy. For questions with multiple-response options, pairwise comparisons for each response option were performed using the Fisher exact test.
Missing responses were excluded from all analyses. We used the Benjamini–Hochberg false discovery rate control procedure to adjust for multiple comparisons. 11 All analyses were conducted using SAS version 9.4 software (SAS Institute, Cary, NC). 12
Results
In total, 2,720 HCWs completed the survey, accounting for just fewer than 20% of all targeted participants. The details of respondents’ sociodemographic and professional characteristics and personal experiences with COVID-19 are presented in Table 1. Female sex (83%) and White race (89%) were slightly overrepresented in our sample compared to the overall employee population. Although nursing staff comprised the largest proportion of survey respondents (34%), response rates were highest among those who identified themselves as managers (60% of managers responded to the survey). For all other role categories, response rates ranged between 14% and 20%.
Table 1.
Respondent Characteristics
| Characteristic | No. | % |
|---|---|---|
| Age, y (n = 2,712) | ||
| 18–24 | 118 | 4.4 |
| 25–34 | 600 | 22.1 |
| 35–44 | 588 | 21.7 |
| 45–54 | 682 | 25.1 |
| 55–64 | 629 | 23.2 |
| 65+ | 95 | 3.5 |
| Sex (n = 2,708) | ||
| Female | 2,223 | 82.1 |
| Male | 473 | 17.5 |
| Other | 12 | 0.4 |
| Race/Ethnicity (n = 2,720)a | ||
| African American/Black | 151 | 5.6 |
| American Indian/Alaska Native | 26 | 1.0 |
| Asian/Pacific Islander | 70 | 2.6 |
| Caucasian/White | 2,444 | 89.9 |
| Hispanic/Latino(a) | 41 | 1.5 |
| Other | 27 | 1.0 |
| Role at Carilion (n = 2,715) | ||
| Provider | 211 | 7.8 |
| Nursing staff | 924 | 34.0 |
| Management | 310 | 11.4 |
| Other (patient care) | 663 | 24.4 |
| Other (nonpatient care) | 607 | 22.4 |
| Work setting (n = 2,656) | ||
| Outpatient | 865 | 32.6 |
| Both | 512 | 19.3 |
| Other | 521 | 19.6 |
| Have you had COVID-19 before? (n = 2,716) | ||
| Yes | 410 | 15.1 |
| No | 2,124 | 78.2 |
| Unsure | 182 | 6.7 |
| Have you had a family member or loved one become ill due to COVID-19? (n = 2,701) | ||
| Yes | 1,191 | 44.1 |
| No | 1,468 | 54.4 |
| Unsure | 42 | 1.6 |
| Have you had a family member or loved one die as a result of COVID-19? (n = 2,688) | ||
| Yes | 212 | 7.9 |
| No | 2,465 | 91.7 |
| Unsure | 11 | 0.4 |
| Is there anyone living in your household that may be considered high-risk for a bad outcome? (n = 2,694) | ||
| Yes | 859 | 31.9 |
| No | 1,742 | 64.7 |
| Unsure | 93 | 3.5 |
Respondents were able to select multiple racial/ethnic categories.
Participant characteristics and vaccine hesitancy
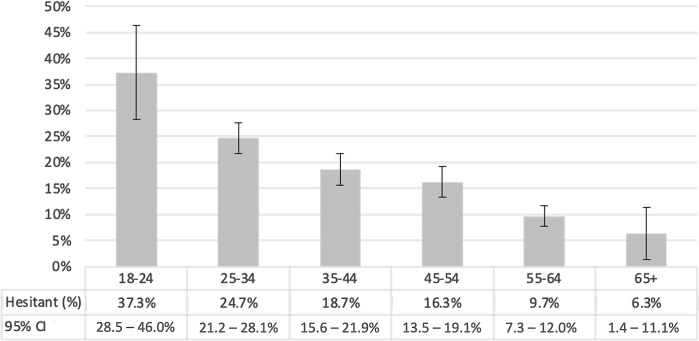
Overall, 82% of respondents were considered vaccine acceptant and the remaining 18% were considered vaccine hesitant. Among vaccine-hesitant individuals, 20% indicated an intention to get the vaccine in the future. For each characteristic measured in the survey, Table 2 shows the proportions who were vaccine hesitant and vaccine acceptant. Age was significantly associated with vaccine hesitancy (P < .0001). Among participants under the age of 25, 37% were vaccine hesitant compared to only 6% among those aged ≥65 years (Fig. 1). A higher proportion of women (19%) were vaccine hesitant than men (13%) (P < .005).
Table 2.
Vaccine Hesitancy by Respondent Characteristics
| Characteristic | Vaccine Hesitancy Status | ||||
|---|---|---|---|---|---|
| Hesitant | Acceptant | χ2
P
Value |
|||
| No. | % | No. | % | ||
| Total | 482 | 17.7% | 2,238 | 82.3% | |
| Age, y | <.0001 | ||||
| 18–24 | 44 | 37.3 | 74 | 62.7 | |
| 25–34 | 148 | 24.7 | 452 | 75.3 | |
| 35–44 | 110 | 18.7 | 478 | 81.3 | |
| 45–54 | 111 | 16.3 | 571 | 83.7 | |
| 55–64 | 61 | 9.7 | 568 | 90.3 | |
| 65+ | 6 | 6.3 | 89 | 93.7 | |
| Sexa | .0037 | ||||
| Female | 411 | 18.5 | 1,812 | 81.5 | |
| Male | 61 | 12.9 | 412 | 87.1 | |
| Race/Ethnicityb | |||||
| African American/Black | 38 | 25.2 | 113 | 74.8 | .0206 |
| American Indian/Alaska native | 7 | 26.9 | 19 | 73.1 | .2035 |
| Asian/Pacific Islander | 8 | 13.3 | 52 | 86.7 | .5106 |
| Caucasian/White | 415 | 17.0 | 2,029 | 83.0 | .0035 |
| Hispanic/Latino(a) | 11 | 26.8 | 30 | 73.2 | .1461 |
| Other | 13 | 48.1 | 14 | 51.9 | .0003 |
| Role at Carilion | <.0001 | ||||
| Provider | 15 | 7.1 | 196 | 92.9 | |
| Nursing staff | 182 | 19.7 | 742 | 80.3 | |
| Management | 34 | 11.0 | 276 | 89.0 | |
| Other (patient care) | 116 | 17.5 | 547 | 82.5 | |
| Other (nonpatient care) | 134 | 22.1 | 473 | 77.9 | |
| Work setting | .0775 | ||||
| Inpatient | 121 | 16.0 | 637 | 84.0 | |
| Outpatient | 162 | 18.7 | 703 | 81.3 | |
| Both | 77 | 15.0 | 435 | 85.0 | |
| Other | 105 | 20.2 | 416 | 79.8 | |
| I believe I am at risk of getting COVID-19 while at work | .0001 | ||||
| Agree | 145 | 13.8 | 902 | 86.2 | |
| Unsure | 140 | 20.9 | 530 | 79.1 | |
| Disagree | 195 | 19.5 | 804 | 80.5 | |
| I believe I am at risk of getting COVID-19 outside of work | <.0001 | ||||
| Agree | 109 | 12.3 | 778 | 87.7 | |
| Unsure | 178 | 20.5 | 692 | 79.5 | |
| Disagree | 194 | 20.3 | 760 | 79.7 | |
| Have you had COVID-19 before? | <.0001 | ||||
| Yes | 101 | 24.6 | 309 | 75.4 | |
| No | 321 | 15.1 | 1,803 | 84.9 | |
| Have you had a family member or loved one become ill due to COVID-19? | .0004 | ||||
| Yes | 244 | 20.5 | 947 | 79.5 | |
| No | 223 | 15.2 | 1,245 | 84.8 | |
| Have you had a family member or loved one die as a result of COVID-19? | .9623 | ||||
| Yes | 37 | 17.5 | 175 | 82.5 | |
| No | 203 | 21.3 | 752 | 78.7 | |
| Is there anyone living in your household who might be considered high-risk for a bad outcome? | <.0001 | ||||
| Yes | 111 | 12.9 | 748 | 87.1 | |
| No | 336 | 19.3 | 1,406 | 80.7 | |
Due to small sample size, respondents who selected “Other” were excluded from the present analysis.
Respondents were able to select more than one racial/ethnic category which precluded the use of χ2 testing. As a result, the Fisher exact tests was used to perform pairwise comparisons for each racial/ethnic category.
Fig. 1.
Vaccine hesitancy by age (proportion hesitant and 95% confidence interval).
Participants who self-identified as Black race were more likely to be hesitant than non-Black respondents (25% vs 17%; P < .05). Professional role was also associated with hesitancy status (P < .0001); HCWs with other responsibilities in non–patient-care areas (22%) and nursing staff (20%) were most likely to be hesitant, whereas providers (7%) were least likely to be hesitant.
Not having a household member at high risk for severe disease was associated with vaccine hesitancy (19% vs 13%; P < .0001). Vaccine hesitancy was also more common among respondents with a history of COVID-19 (25%) compared to those without (15%; P < .0001). Likewise, 21% respondents who had had a family member or loved one get sick from COVID-19 were vaccine hesitant, a significantly higher proportion than the those without that experience (15%) (P < .001). Perceptions of risk both at work (P < .0001) and outside of work (P < .0001) were significantly associated with vaccine hesitancy.
Perceptions of safety and vaccine hesitancy
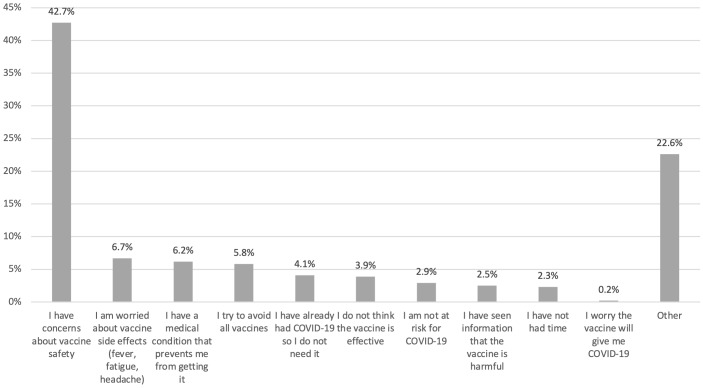
Among vaccine-hesitant participants, 43% cited safety concerns as the most important reason they had not gotten vaccinated (Fig. 2). Unease about safety remained the most common primary reason for not getting vaccinated (23%) among the subset of vaccine-hesitant respondents who intended to get the vaccine in the future. Examining vaccine-related perceptions by hesitancy status, safety concerns were strongly associated with vaccine hesitancy. Table 3 presents responses to Likert-type statements about vaccine-related perceptions dichotomized by hesitancy status.
Fig. 2.
Most important reasons for not getting vaccinated.
Table 3.
Vaccine Perceptions by Hesitancy Status
| Survey Item | Agree | Unsure | Disagree | χ2
P
Value |
|||
|---|---|---|---|---|---|---|---|
| No. | % | No. | % | No. | % | ||
| I believe the COVID-19 vaccine is safe | <.0001 | ||||||
| Hesitant | 81 | 16.9 | 155 | 32.4 | 242 | 50.6 | |
| Acceptant | 1,703 | 76.7 | 396 | 17.8 | 122 | 5.5 | |
| I feel there is enough information/data about the COVID-19 vaccine to make an informed decision | <.0001 | ||||||
| Hesitant | 96 | 19.9 | 109 | 22.6 | 277 | 57.5 | |
| Acceptant | 1,468 | 65.7 | 511 | 22.9 | 255 | 11.4 | |
| I believe the COVID-19 vaccine is effective in preventing COVID-19 | <.0001 | ||||||
| Hesitant | 22.8 | 215 | 45.0 | 154 | 32.2 | ||
| Acceptant | 74.8 | 457 | 20.6 | 101 | 4.6 | ||
| I believe the COVID-19 vaccine will help stop the pandemic | <.0001 | ||||||
| Hesitant | 29.7 | 176 | 36.5 | 163 | 33.8 | ||
| Acceptant | 79.5 | 332 | 15.0 | 122 | 5.5 | ||
| I feel that COVID-19 vaccine development was rushed without sufficient quality control | <.0001 | ||||||
| Hesitant | 78.5 | 11 | 2.9 | 71 | 18.6 | ||
| Acceptant | 11.4 | 592 | 26.5 | 1,388 | 62.1 | ||
| I am worried about the known/reported short-term side effects from the COVID-19 vaccine (eg, fever, fatigue, headache) | <.0001 | ||||||
| Hesitant | 46.0 | 127 | 26.5 | 132 | 27.5 | ||
| Acceptant | 11.7 | 380 | 17.1 | 1,582 | 71.2 | ||
| I am worried about potential (unknown) long-term side effects of the COVID-19 vaccine | <.0001 | ||||||
| Hesitant | 83.1 | 59 | 12.3 | 22 | 4.6 | ||
| Acceptant | 32.0 | 589 | 26.5 | 920 | 41.4 | ||
| I am concerned about information I have seen that the vaccine is very harmful | <.0001 | ||||||
| Hesitant | 24.3 | 185 | 38.5 | 179 | 37.2 | ||
| Acceptant | 6.9 | 369 | 16.6 | 1,699 | 76.5 | ||
| I am worried the vaccine will negatively affect a current pregnancy or my future ability to have children | <.0001 | ||||||
| Hesitant | 31.7 | 134 | 28.1 | 192 | 40.3 | ||
| Acceptant | 5.1 | 542 | 24.7 | 1,543 | 70.2 | ||
| I am worried that the vaccine will give me COVID-19 | <.0001 | ||||||
| Hesitant | 5.5 | 74 | 15.5 | 376 | 79.0 | ||
| Acceptant | 1.9 | 75 | 3.4 | 2,097 | 94.8 | ||
| I believe natural immunity from getting COVID-19 is more protective than a vaccine | <.0001 | ||||||
| Hesitant | 35.4 | 200 | 41.7 | 110 | 22.9 | ||
| Acceptant | 7.3 | 635 | 28.6 | 1,426 | 64.1 | ||
| COVID-19 is not that dangerous so I do not need a vaccine | <.0001 | ||||||
| Hesitant | 11.0 | 143 | 29.7 | 285 | 59.3 | ||
| Acceptant | 2.2 | 109 | 4.9 | 2,071 | 93.0 | ||
| In general, I try to avoid vaccinations | <.0001 | ||||||
| Hesitant | 22.9 | 96 | 20.0 | 274 | 57.1 | ||
| Acceptant | 5.7 | 140 | 6.3 | 1,945 | 88.0 | ||
Responses to the statement “I believe the COVID-19 vaccine is safe” were significantly associated with hesitancy status (P < .0001). Only 17% of vaccine-hesitant individuals agreed with this statement compared with 77% of vaccine-acceptant individuals. Perceptions about fast-tracked vaccine development were also associated with hesitancy status (P < .0001). Among those who were vaccine hesitant, 79% felt that vaccine development was rushed without sufficient quality control, whereas only 11% of vaccine acceptant participants shared this view. Similarly, views about the sufficiency of information to make an informed decision about getting vaccinated were associated with hesitancy status (P < .0001). Even though only 20% of vaccine-hesitant participants felt that adequate data were available, 66% of vaccine-acceptant individuals did. On specific safety concerns, worry over unknown, long-term side effects of the vaccine and concerns about the vaccine affecting a current pregnancy or future ability to have children were both significantly (P < .0001) associated with hesitancy status.
Perceptions of efficacy and vaccine hesitancy
Responses to the statement “I believe the COVID-19 vaccine is effective in preventing COVID-19” were significantly associated with hesitancy status (P < .0001), and only 23% of vaccine-hesitant individuals agreed with this statement. However, agreement jumped to 75% among vaccine-acceptant individuals. Also, 30% of hesitant participants agreed that the vaccine would help end the pandemic compared to 80% of vaccine-acceptant participants (P < .0001). In addition, 35% of vaccine-hesitant participants believed that natural immunity would be more protective than a vaccine, whereas only 7% of acceptant individuals agreed with this statement (P < .001).
Drivers of vaccine acceptance
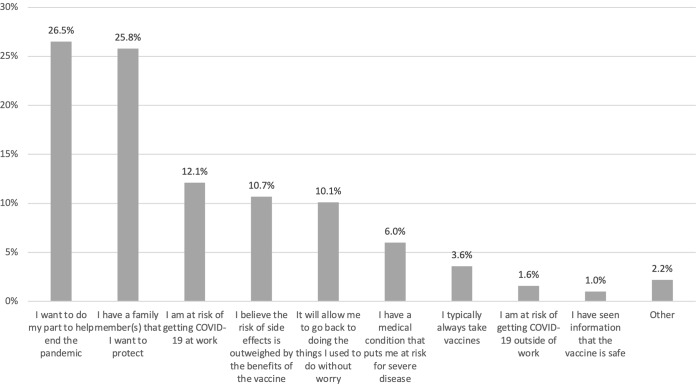
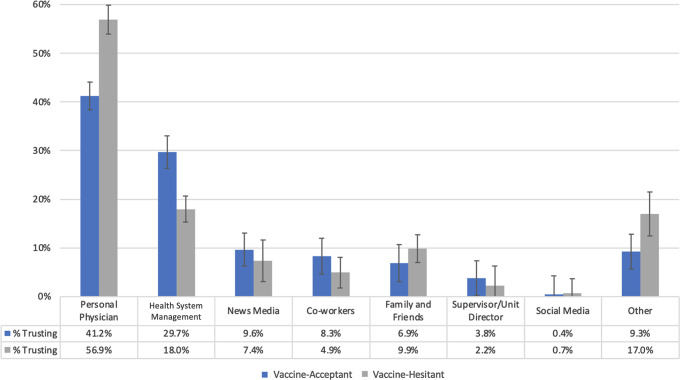
For vaccine-acceptant individuals, wanting to do their part to end the pandemic (27%) and wanting to protect family members (26%) were the most important reasons for getting vaccinated (Fig. 3). When asked about trusted sources of COVID-19 information, personal physicians were cited more frequently than other sources by both vaccine-hesitant (48%) and vaccine-acceptant (38%) participants (Fig. 4).
Fig. 3.
Most important reasons for getting vaccinated.
Fig. 4.
Trusted sources of information by vaccine hesitancy status (percent and 95% confidence interval).
Discussion
Our findings align with previous studies reports that providers were more vaccine acceptant than other HCWs like nursing staff. 5,6 Our survey also included nonclinical staff and thus provides a more nuanced picture revealing high levels of vaccine hesitancy among workers in both clinical and nonclinical settings. This finding indicates that perception of work-related risk is not the sole driver of this association, suggesting that vaccine-related outreach may be needed in both contexts with a focus on nursing and nonmanagement staff.
Even though HCWs in our system had similar and easy access to the vaccine, Black respondents to our survey demonstrated higher levels of hesitancy than non-Blacks. This finding mirrored hesitancy rates for the general population early in the vaccine rollout. 13 Although the proportion of Blacks in the United States who are vaccinated is still lower than other races and ethnicities, more recent data indicate that racial disparities in vaccine uptake have diminished over time. 14 This difference may be in part due to more equitable vaccine access. Strategies that address structural barriers and mistrust of the scientific community may further reduce vaccine hesitancy among Blacks. 15–17,18 Like Dror et al, 18 we found that vaccine hesitancy was more common among female HCWs, running counter to the higher COVID-19 vaccination rates among women in the general population. 18 In our study, concerns about the vaccine affecting fertility or future child-bearing ability were cited by a substantial proportion of both vaccine-hesitant men (22%) and vaccine-hesitant women (34%). This concern in HCWs can be alleviated by highlighting more recent research that addresses the safety of the vaccine in the context of both pregnancy and fertility, 19,20 but this perception may continue to drive vaccine hesitancy for some. 21
Our data suggest that vaccine outreach should target younger HCWs. Older individuals have been more susceptible to severe disease throughout the COVID-19 pandemic; thus, it is unsurprising that they are more accepting of the vaccine even in a healthcare context in which vaccines were not prioritized by age. With virus variants taking hold throughout the United States and with many older adults already vaccinated, younger adults are now experiencing a more substantial burden of disease and comprise most recent COVID-19 hospitalizations. 18 In addition, one study found that adults aged 20–49 years are currently driving transmission in the United States, making this age group an important population for epidemic control. 22
The observed association between low risk perception and vaccine hesitancy is consistent with existing research. 5 Unexpectedly, in our study, experience with COVID-19—either a personal history of infection or a loved one having the disease—was associated with greater vaccine hesitancy. This difference may be because individuals with a personal history feel they already have sufficient natural immunity, or perhaps because those with a personal and/or family history of COVID-19 may have a lower perception of risk, having survived the disease. Alternatively, it is possible that the association is attributable to broader attitudes about the pandemic. One study reported that participants who did not engage in protective behaviors such as social distancing and masking were less likely to report an intention to vaccinate. 23 Because these behaviors are known to reduce the incidence of COVID-19, these findings might help explain the observed relationship.
Consistent with prior studies, we found that overcoming vaccine hesitancy among HCWs will require addressing common safety concerns, especially fears around possible long-term side effects. Alleviating vaccine safety fears in a context of fast-tracked development and evolving science will be paramount, and public health messaging should focus on the decades-long development of mRNA vaccine technology. 24 Addressing other common fears, such as concerns about effects on fertility and serious side effects such as blood clots, while debunking pervasive myths like the vaccine having a tracking microchip or altering DNA, 25 will likely be needed to encourage vaccination among some vaccine-hesitant HCWs. Studies of vaccine hesitancy in other contexts suggest that approachable scientific messaging may be beneficial. 26
At this stage of vaccine roll-out, it may be a challenge to overcome the sentiment that there is insufficient information available to make an informed vaccination decision. Interestingly, 34% acceptant individuals did not feel that there was enough information, and a similar proportion of acceptant individuals (32%) had concerns about potential long-term side effects. Future research should examine how such individuals overcame these barriers, which could have implications for encouraging hesitant individuals to get vaccinated.
The finding that vaccine hesitancy was associated with perceptions of low efficacy indicate a need for clearer, more approachable public health messaging about the well-documented protective benefits of the vaccine for the individual and the community. Wanting to protect others was the most important reason for getting vaccinated for most acceptant participants in our study. This finding indicates that messaging emphasizing protecting loved ones and contributing to a collective effort may be effective at increasing uptake, particularly among those less concerned about their personal risk.
In our study, personal physicians were a trusted source of information on COVID-19, particularly for hesitant individuals (Fig. 4). Recent publications describe different categories of COVID-19 vaccine hesitancy based on influences, fears, barriers, and motivations, each requiring different strategies to address. 27–29 This situation implies that transitioning vaccine delivery to more personalized channels such as doctors’ offices could reduce hesitancy. Through patient-centered conversations, trusted medical professionals can address these individual influences on hesitancy through active listening and tailored messaging. Our findings suggest that these conversations will be most effective if they address safety concerns while reinforcing efficacy and community benefits.
This study has several important limitations. We relied on a convenience sample of participants, so our findings may not be generalizable to the entire population of HCWs in this healthcare system or to healthcare systems in different settings given the narrow geographic scope of the study. Additionally, our reliance on e-mail and computers or smartphones for survey administration likely reduced participation among individuals and departments that do not use these technologies in their day-to-day work. However, the similar response rates we observed across nonmanagement positions suggests that our sample likely represents the diverse roles in this healthcare system.
Because our survey was administered through work channels, responses may have been subject to social desirability bias. However, self-administration has been shown to reduce this bias. 30 In addition, participants were assured that their data would be private and deidentified in survey-related communications and within the questionnaire. Administrative data indicated that ∼63% of staff were vaccinated at the time of the survey; therefore, vaccine-acceptant staff are overrepresented in our study. However, the high number of responses even among those who were unvaccinated indicates that some employees were comfortable responding openly about vaccine hesitancy.
All data were collected during a 2-week span, prior to the emergence of key variants including the δ (delta) variant. In the context of a pandemic, in which information about COVID-19, data on vaccine safety and efficacy against different variants, and reports of adverse events are continually evolving, our survey may not reflect newer perceptions about the vaccine. This study was also conducted prior to vaccine mandate discussions or requirements in healthcare settings. However, an understanding of the drivers of hesitancy can inform complementary strategies that support the implementation of mandates while maintaining HCW job satisfaction and patient care standards.
Future plans for these data include analyses that will deepen our understanding of the drivers of vaccine hesitancy by controlling for potential confounders. An analysis of the subset of hesitant individuals who indicated receptivity to receiving the COVID-19 vaccine in the future is also forthcoming. Additionally, many respondents provided free-text responses when asked about their most important reasons for not getting vaccinated. A qualitative analysis of these responses may provide a more nuanced understanding of vaccine hesitancy. Nevertheless, this study fills a gap in the literature, providing empirical evidence about characteristics and perceptions associated with COVID-19 vaccine hesitancy among HCWs. As vaccine demand continues to wane, additional strategies are needed to achieve herd immunity. The characteristics and perceptions associated with vaccine hesitancy, along with the trusted sources of information identified in this study, provide a roadmap to encourage greater vaccine acceptance among HCWs, including improved educational messaging. Personalized efforts by physicians and approachable public health messaging that center on alleviating safety concerns, emphasizing vaccine effectiveness, and promoting a culture of “doing your part” to protect others may be most effective.
Acknowledgments
We thank Mattie Tenzer and Hunter Sharp from Carilion Clinic Health Analytics and Ruth Ndolo, Research Nurse for this study. Finally, we thank all the respondents who shared their information with us.
Financial support
The REDCap platform is supported by the National Center for Advancing Translational Sciences of the National Institutes of Health (grant nos. UL1TR003015 and KL2TR003016). The content is solely the responsibility of the authors and does not represent the views of the National Institutes of Health. We received no other financial support.
Conflicts of interest
All authors report no conflicts of interest relevant to this article.
References
- 1. Abelson R. COVID overload: US hospitals are running out of beds for patients. New York Times website. https://www.nytimes.com/2020/11/27/health/covid-hospitals-overload.html. Published November 28, 2020. Accessed February 10, 2022.
- 2. Dooling K, McClung N, Chamberland M, et al. The Advisory Committee on Immunization Practices’ interim recommendation for allocating initial supplies of COVID-19 vaccine—United States. Morb Mortal Wkly Rep 2020;69:1857–1859. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Lazer D, Perlis RH, Ognyanova K et al. The COVID states project #40: COVID-19 vaccine attitudes among healthcare workers. OSFPreprints 2021. doi: 10.31219/osf.io/p4q9h. [DOI]
- 4. Lucia VC, Kelekar A, Afonso NM. COVID-19 vaccine hesitancy among medical students. J Public Health 2021;43:445–449. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Dror AA, Eisenbach N, Taiber S, et al. Vaccine hesitancy: the next challenge in the fight against COVID-19. Eur J Epidemiol 2020;35:775–779. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. Gadoth A, Halbrook M, Martin-Blais R, et al. Assessment of COVID-19 vaccine acceptance among healthcare workers in Los Angeles. medRxiv 2020. doi: 10.1101/2020.11.18.20234468. [DOI] [PMC free article] [PubMed]
- 7. Grech V, Gauci C, Agius S. Vaccine hesitancy among Maltese healthcare workers toward influenza and novel COVID-19 vaccination. Early Hum Dev 2020. doi: 10.1016/j.earlhumdev.2020.105213. [DOI] [PMC free article] [PubMed]
- 8. Barry M, Temsah MH, Alhuzaimi A, et al. COVID-19 vaccine confidence and hesitancy among healthcare workers: a cross-sectional survey from a MERS-CoV experienced nation. medRxiv 2020. doi: 10.1101/2020.12.09.20246447. [DOI] [PMC free article] [PubMed]
- 9. Kwok KO, Li KK, WEI WI, Tang A, Wong SYS, Lee SS. Influenza vaccine uptake, COVID-19 vaccination intention and vaccine hesitancy among nurses: a survey. Int J Nurs Stud 2021;114:103854. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10. MacDonald NE. Vaccine hesitancy: definition, scope and determinants. Vaccine 2015;33:4161–4164. [DOI] [PubMed] [Google Scholar]
- 11. Benjamini Y, Hochberg Y. Controlling the false discovery rate: a practical and powerful approach to multiple testing. J R Stat Soc Ser B 1995;57:289–300. [Google Scholar]
- 12.The SAS system for Windows. SAS Institute website. http://www.sas.com. Published 2013. Accessed February 10, 2022.
- 13.Intent to get a COVID-19 vaccine rises to 60% as confidence in research and development process increases. Pew Research Center website. https://www.pewresearch.org/science/2020/12/03/intent-to-get-a-covid-19-vaccine-rises-to-60-as-confidence-in-research-and-development-process-increases/. Published 2020. Accessed February 10, 2022.
- 14. Ndugga N, Hill L, Artiga S, Haldar S. Latest data on COVID-19 vaccinations by race/ethnicity. Kaiser Family Foundation website. https://www.kff.org/coronavirus-covid-19/issue-brief/latest-data-on-covid-19-vaccinations-by-race-ethnicity/. Published 2022. Accessed February 10, 2022.
- 15. Dada D, Djiometio JN, McFadden SM, et al. Strategies that promote equity in COVID-19 vaccine uptake for black communities: a review. J Urban Health 2022. doi: 10.1007/s11524-021-00594-3. [DOI] [PMC free article] [PubMed]
- 16. Boulware LE, Cooper LA, Ratner LE, LaVeist TA, Powe NR. Race and trust in the healthcare system. Public Health Rep 2003;118:358–365. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Njoku A, Joseph M, Felix R. Changing the narrative: structural barriers and racial and ethnic inequities in COVID-19 vaccination. Int J Environ Res Public Health 2021;18:9904. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.COVID data tracker. Centers for Disease Control and Prevention website. https://covid.cdc.gov/covid-data-tracker/#vaccination-demographics-trends. Published 2021. Accessed May 14, 2021.
- 19. Wesselink AK, Hatch EE, Rothman KJ, et al. A prospective cohort study of COVID-19 vaccination, SARS-CoV-2 infection, and fertility. Am J Epidemiol 2022. doi: 10.1093/aje/kwac011. [DOI] [PMC free article] [PubMed]
- 20. Hillson K, Clemens SC, Madhi SA, Voysey M, Pollard AJ, Minassian AM. Fertility rates and birth outcomes after ChAdOx1 nCoV-19 (AZD1222) vaccination. Lancet 2021;398:1683–1684. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Hamel L, Lopes L, Sparks G, et al. KFF COVID-19 vaccine monitor: October 2021. Kaiser Family Foundation website. https://www.kff.org/coronavirus-covid-19/poll-finding/kff-covid-19-vaccine-monitor-october-2021/. Published October 2021. Accessed February 10, 2022.
- 22. Monod M, Blenkinsop A, Xi X, et al. Age groups that sustain resurging COVID-19 epidemics in the United States. Science 2021;371(6536):eabe8372. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23. Latkin CA, Dayton L, Yi G, Colon B, Kong X. Mask usage, social distancing, racial, and gender correlates of COVID-19 vaccine intentions among adults in the US. PLoS One 2021;16(2):e0246970. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24. Thompson D. How mRNA technology could change the world. The Atlantic website. https://www.theatlantic.com/ideas/archive/2021/03/how-mrna-technology-could-change-world/618431/. Published 2021. Accessed February 10, 2022.
- 25.Frequently asked questions about COVID-19 vaccination. Centers for Disease Control and Prevention website. https://www.cdc.gov/coronavirus/2019-ncov/vaccines/faq.html?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fcoronavirus%2F2019-ncov%2Fvaccines%2Fkeythingstoknow.html. Updated February 2, 2022. Accessed February 10, 2022.
- 26. Kuru O, Stecula D, Lu H, et al. The effects of scientific messages and narratives about vaccination. PLoS One 2021;16(3):e0248328. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. Elwy AR, Clayman ML, LoBrutto L, et al. Vaccine hesitancy as an opportunity for engagement: a rapid qualitative study of patients and employees in the US Veterans’ Affairs healthcare system. Vaccine X 2021. doi: 10.1016/j.jvacx.2021.100116. [DOI] [PMC free article] [PubMed]
- 28. Wiysonge CS, Ndwandwe D, Ryan J, et al. Vaccine hesitancy in the era of COVID-19: could lessons from the past help in divining the future? Hum Vaccin Immunother 2021. doi: 10.1080/21645515.2021.1893062. [DOI] [PMC free article] [PubMed]
- 29. Thompson D. The surprising key to combatting vaccine refusal. The Atlantic website. https://www.theatlantic.com/ideas/archive/2021/02/vaccine-hesitancy-isnt-just-one-thing/618164/. Published online February 2021. Accessed February 10, 2022.
- 30. Krumpal I. Determinants of social desirability bias in sensitive surveys: a literature review. Qual Quant 2013;47:2025–2047. [Google Scholar]