Abstract
Systemic sclerosis (SSc) is an autoimmune rheumatic disease with high mortality, which is featured by inflammation, vascular damage, and aggressive fibrosis. To date, the pathogenesis of SSc remains unclear and effective treatments are still under research. Active NLRP3 recruits downstream proteins such as ASC and caspase-1 and assembles into inflammasome, resulting in excretion of inflammatory cytokines including IL-1β and IL-18, as well as in pyroptosis mediated by gasdermin D. Various studies demonstrated that NLRP3 inflammasome might be involved in the mechanism of tenosynovitis, arthritis, fibrosis, and vascular damage. The pathophysiological changes might be due to the activation of proinflammatory Th2 cells, profibrotic M2 macrophages, B cells, fibroblasts, and endothelial cells. Here, we review the studies focused on NLRP3 inflammasome activation, its association with innate and adaptive immune cells, endothelium injury, and differentiation of fibroblasts in SSc. Furthermore, we summarize the prospect of therapy targeting NLRP3 pathway.
Keywords: Systemic sclerosis, NLRP3, Inflammasome, Caspase-1, IL-1β
Background
Systemic sclerosis (SSc) is an autoimmune disease characterized with inflammation, vascular damage, and fibrosis, in which the progressive fibrosis of skin and lungs is the most characteristic [1]. Epigenetics might play an important role in initiating the disease as many events were reported to trigger SSc onset [2]. However, the pathogenic mechanism of SSc still remains clarified. To date, there is lack of effective therapy for SSc. Pattern recognition receptors (PRRs) are cellular receptors which recognize various pathogen-associated molecular patterns (PAMPs) or damage-associated molecular patterns (DAMPs). NLRP3, a PRR which is classified as nucleotide-binding oligomerization domain (NOD)-like receptors (NLRs), is associated with numerous inflammation-related diseases [3]. Once activated, NLRP3 recruits downstream proteins and assembles into NLRP3 inflammasome, which leads to maturation and excretion of proinflammatory cytokines including interleukin(IL)-1β and IL-18, and exacerbates subsequent inflammatory cascades [4]. Recent studies suggest a remarkable link between NLRP3 and the pathological process in SSc, which might provide a potential therapeutic target for SSc treatment. In this paper, we summarize the key roles of NLRP3 in SSc pathogenesis, as well as the potential prospect of NLRP3 as a therapeutic target in SSc treatment.
Overview of NLRP3
As the first line against invading microbes and cellular damage, innate immune cells could be activated by pathogens or defective cells through various PRRs expressed on membranes or in cytoplasm. PRRs expressed on membranes are transmembrane proteins, including Toll-like receptors (TLRs) and C-type lectin receptors (CLRs). The cytoplasmic PRRs consist of retinoic acid-inducible gene-I (RIG-I)-like receptors (RLRs), absent in melanoma 2 (AIM2)-like receptors (ALRs), and NLRs [5]. The heterotrimer NLRP3 is the most characterized protein in NLRs, formed by three domains: a C-terminal leucine-rich repeat (LRR) domain with self-regulating function, a nucleotide-binding NACHT domain with ATPase activity, because of which ATP binding is regarded necessary for NLRP3 activation [6], and a N-terminal pyrin domain (PYD) which recruits downstream proteins for assembling to functional form [6, 7]. Besides its remarkable ability in inflammatory regulation, NLRP3 exerts an indispensable role in embryonic development, antigen presentation, and cell death [8]. Once activated, NLRP3 proteins assemble into NLRP3 inflammasome consisted of a sensor (NLRP3), an adaptor (ASC, an apoptosis-associated speck-like protein containing a caspase recruitment domain), and an effector (caspase-1). Activated caspase-1 cleaves precursor of IL-1β and IL-18 into mature form to exert their biological effects. Abnormal activation of NLRP3 is considered as a key in several autoimmune diseases such as rheumatoid arthritis (RA), systemic lupus erythematosus (SLE), as well as SSc [3].
SSc, as an autoimmune disease featured by inflammation, vascular damage, and fibrosis, involves immune cells, endothelial cells (ECs), and fibroblasts [2]. Studies suggested that overactivation of NLRP3 might lead to inflammation and dysimmunity, acting as a sensor of danger signals [9, 10]. However, adverse evidence argues that NLRP3 appears to contribute to immune homeostasis [11, 12]. As a key role in vascular pathology, ECs could be activated by NLRP3, conducing to excretion of cytokines and further immune response [13]. NLRP3-mediated damage and necrosis of ECs were also found in diseases which are relevant to vasculopathy [14, 15]. NLRP3 also shows ability to activate fibroblasts, the most important cellular component of fibrosis, in chronic inflammatory diseases, inducing cell activation and differentiation [16, 17].
Activation and regulation of NLRP3
The activation of NLRP3 requires two signals. The first one is the priming signal initiated by TLRs, regulating gene expression and posttranslational modification [7]. Once activated, TLRs recruits myeloid differentiation primary response gene-88 (MyD88) through homotypic interaction of its intracellular domain Toll-IL-1 receptor (TIR) domain and induces nuclear translocation of nuclear factor (NF)κB, which upregulates the expression of NLRP3 and its downstream proinflammatory proteins including pro-caspase-1, pro-IL-1β, and pro-IL-18 [7]. The second signal is also called the activation signal which initiates the assembly of NLRP3 inflammasome after activated by stimuli, including virus infections, extracellular ATP, pore-forming bacterial toxins, crystals, particulate matters, and other inflammation-concerned signals [18, 19]. NLRP3 oligomerizes via NACHT domain interaction and then recruits its downstream proteins. Because of containing one PYD domain and one CARD domain, ASC could be recruited by NLRP3 through PYD-PYD homotypic interaction and aggregated into a macromolecular focus which is identified as ASC speck formation [20, 21]. ASC speck then gathers pro-caspase-1 via CARD-CARD homotypic interaction [20]. Polymerized pro-caspase-1 releases active caspase-1, which cleaves pro-IL-1β and pro-IL-18 into bioactive formation, further modulating inflammation [4, 22]. IL-1β is widely known as an efficient proinflammatory cytokine, which could mediate differentiation and infiltration of inflammatory cells and induce synthesis of more proinflammatory cytokines and the inflammatory change of microenvironment, contributing to enlargement of inflammation [23]. IL-18 was initially discovered to induce interferon (IFN)-gamma production. To date, previous studies have revealed pleiotropy of IL-18 in metabolism, allergic diseases, and autoimmune respond [24].
Pyroptosis is a recently discovered type of programmed cell death which could be conducted by activated NLRP3 inflammasome [25]. Different from apoptosis, pyroptosis leads to cell lysis and release of intracellular substances. Pore-forming protein gasdermin D (GSDMD) plays a crucial role in pyroptosis after being cleaved by caspase-1 [25]. GSDMD consists of N-terminal cell death domain (GSDMDNterm), central linker region, and C-terminal self-inhibition domain [26, 27]. Once its C-terminal inhibitory region is cutoff by caspase-1, it embeds into cell membranes, forming a 10–14-nm channel which induces release of cytokines and pyroptosis [28].
Besides the canonical NLRP3 activation which promotes caspase-1 activation, the non-canonical NLRP3 activation contributes to activation of caspase-4 (or caspase-11 in mice) and caspase-5 [29]. Caspase-4 and -5 were reported to recognize LPS and then activate GSDMD [30, 31]. Evidence suggests that non-canonical activation might be an upstream event of canonical activation, as activated caspase-11 in non-canonical activation leads to caspase-1 activation and secretion of IL-1β and IL-18, which also requires NLRP3 inflammasome assembly [32, 33]. Although non-canonical activation of inflammasome is widely concerned as defense of Gram-negative bacteria, increased caspase-4 and caspase-11 in allergic airways present potential involvements in over-activated immune response [34, 35].
Different from typical PRRs, NLRP3 appears not to directly sense DAMP or PAMP. Although the mechanism remains to be fully elucidated, there are some studies trying to illuminate how NLRP3 inflammasome gets activated. Transmembrane pore proteins are supposed to play a crucial part in initiating inflammasome assembly. Stimuli like nigericin, mostly bacterial toxins, are pore-forming compounds, which might permeabilize cell membrane for ion flows while ion redistribution seems to be the key to inflammasome activation [36]. K+ efflux appears to be necessary for never in mitosis A-related kinase 7 (NEK7) activation and is confirmed to be an upstream event of NLRP3 activation [37, 38]. The mitotic kinase NEK7 is a newly found essential molecule for NLRP3 activation by directly combining to NLRP3 and mediating NLRP3 oligomerization [37, 39, 40]. A number of activation signals such as nigericin, crystals, and ATP induce K+ efflux before inflammasome activation, and the activation could be induced by low potassium independent of other triggers [41–43]. However, K+ concentration remains unchanged while NLRP3 activating in some research [44]. Other ion flows including Ca2+ influx and Cl− efflux may also play a role in NLRP3 activation [45, 46]. But in contrary, evidence also shows that NLRP3 can be activated without Ca2+ influx or Cl− efflux [41, 47]. It requires more evidence to clarify the role of ion flows in NLRP3 activation.
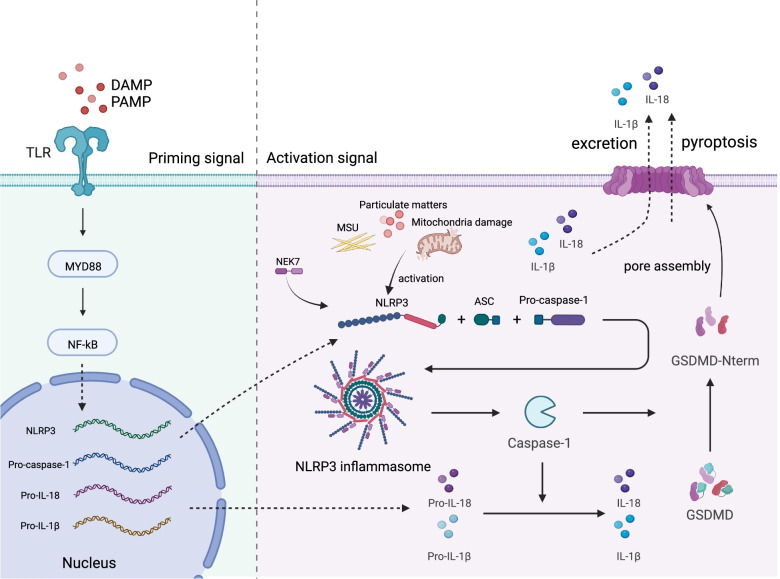
Research indicates mitochondria damage may initiate NLRP3 activation by mitochondrial DNA (mtDNA) release and cardiolipin externalization [48]. Mitophagy may be a self-regulating mechanism to reduce NLRP3 inflammasome activation by mitochondrial dysfunction, and in which mitochondrial reactive oxygen species (mtROS) appears to be necessary [44, 49, 50]. Metabolism of glucose and fatty acid is suggested to show potential role on the inflammatory procedure. Hexokinase relocalization from mitochondrial membrane to cytoplasm is reported involving in NLRP3 activation [51]. Fatty acid might activate NLRP3 inflammasome through elevated mtROS via AMP-activated protein kinase signaling [52]. The contribution to inflammasome activation of extracellular ATP, hexokinase, and fatty acid indicate a possible association between energy reserve and NLRP3 activation. A summary of activation of NLRP3 could be found in Fig. 1.
Fig. 1.
Activation of NLRP3 inflammasome. The activation of NLRP3 inflammasome requires two signals. Priming signal: TLRs are activated by extracellular DAMPs or PAMPs and mediate translocation of NF-κB, finally resulting in increased expression of NLRP3, pro-caspase-1, pro-IL-1β, and pro-IL-18. Activation signal: NLRP3 activated by stimuli like MSU and particulate matters activate, recruiting ASC and pro-caspase-1, then forming into inflammasome and releasing mature caspase-1. Caspase-1 cleaves pro-IL-1β, pro-IL-18, and GSDMD into mature form, contributing to further inflammation. TLR, Toll-like receptor; DAMP, Damage-associated molecular pattern; PAMP, Damage-associated molecular pattern; MSU, monosodium urate; GSDMD, Gasdermin D
NLRP3 and SSc
Although what ignites the onset of disease remains an issue, immunology dysfunction and vascular damage seem to be early pathological changes in SSc, as perivascular edema and infiltration of immune cells are seen ahead of fibrotic involvement [53, 54]. Consistent inflammatory activation and autoimmune reaction might be responsible for differentiation of fibroblasts into myofibroblasts, the functional phenotype, which synthesize and excrete extracellular matrix (ECM) [55]. However, the exact pathogenesis of SSc is currently unknown. Except for genetics, environmental risk factors such as certain chemicals, viral infections, frequent thermal, and mechanical injury show great importance in the immune system dysregulation of SSc [56–58]. Abnormal activation and recruitment of immune cells, and consequent production of cytokines and autoantibodies are prominent in SSc pathological development. The consequent inflammation and over-deposition of ECM results in irreversible damage of tissue structure and ultimate organ failure, which is regarded as the tough nut in SSc treatments [55]. Previous research revealed that the expression of NLRP3 and its downstream proteins including caspase-1, IL-1β, and IL-18 increase in serum and skin biopsies from SSc patients and show positive relevance with lung and skin involvement [59, 60]. In bleomycin (BLM)-induced SSc mice, upregulation of IL-1β and IL-18 could be detected in serum and lung tissue, and alleviated disease performance could be found when NLRP3, ASC, or caspase-1 genes were knocked out [61, 62].
Circulating monocytes could differentiate into fibroblasts and macrophages [63], and both of them mediate disease progression of SSc [63–65]. As classical innate immune cells, macrophages are classified or polarized into two phenotypes, classical activated macrophages (M1) and alternative activated macrophages (M2). Traditional views regard M2 as the key role in fibrosis due to it producing profibrotic cytokines including IL-4, IL-13, and transforming growth factor β (TGF-β), leading to overexpression of ECM and scleroderma [63, 66]. Indeed, M1 also shows relevance to lung and skin involvement in SSc [67, 68]. NLRP3 inflammasome is usually regarded as an inhibitor in M2 activation; however, an increased number of M2 and the activation of NLRP3 inflammasome appear simultaneously in asthma patients [69]. What is more, research discovered that IL-1β-treated vascular endothelial cells mediated M2 activation in highly fibrotic skin [70].
Th1 and Th2 are two classical subtypes of T helper (Th) cell. Th1 secretes IFN-γ and tumor necrosis factor (TNF)-α, showing proinflammatory function [71], while Th2 secretes IL-4 and IL-13, presenting profibrotic properties [72]. It is comprehensible that NLRP3/IL-1 signaling activation regulating Th1/Th2 balance is involved in the immune mechanism in SSc [66, 73]. B cells participate in SSc pathogenesis through producing autoantibody, secretion of pro-fibrosis cytokines, and direct regulation of other effective cells like fibroblasts [74]. Dephosphorylase protein tyrosine phosphatase N22 (PTPN22) contributing to NLRP3 activation was reported as a crucial molecule in B cell signaling and autoantibody titer [75–77]. A recent study verified that BAFF, a B cell activating factor, activated NLRP3 in primary B cells and B lymphocyte lines through increasing NF-κB expression and upregulating ROS as well as K+ efflux [78]. NLRP3 displays capabilities in regulating antibody expression and cytokine secretion of B cells in infection model and plays potential role in inducing lymphocyte infiltration [79, 80]. These studies suggested that NLRP3/IL-1 signaling regulating T and B cells are related to the immune imbalance in SSc pathogenesis.
NLRP3 and vascular damage in SSc
Microvascular dysfunction appears to play a prominent role at the early stage in SSc [81]. An increasing number of molecules inducing endothelial injury were proved NLRP3-dependent [82–85]. The high expression of NLRP3 in SSc skin biopsies is positively correlated with endothelin (ET)-1 expression [59]. Reduction of nitric oxide (NO), an efficient vasodilator, and increasing ET-1 expression appear to be responsible for vascular abnormalities like vasospasm, which is responsible for Raynaud’s phenomenon, a common symptom in SSc patients [54, 86]. NO also acts as an inhibitor of NLRP3 inflammasome assembly through removal of dysfunctional mitochondria while decreased NO might partly contribute to the activation of NLRP3 [87, 88].
ECs or endothelium injury gives rise to increased permeability as well as persistent vascular leakage and triggers the vascular microenvironment ischemia along with activating inflammation [58, 89]. ECs could be activated by IL-1β and exert its proinflammation action through secreting IL-1β in SSc vascular damage [81]. IL-1β participates in upregulating vascular endothelial growth factor (VEGF) and its receptor, resulting in hypoangiogenesis and vessel sparse in SSc patients [90]. Pulmonary hypertension (PAH) is related to severe outcomes in SSc patients. The expression of caspase-1 and IL-1β increases in peripheral blood mononuclear cells (PBMCs) of SSc patients with PAH compared to that in non-PAH SSc patients [91]. It suggests a potential function of IL-1β and its activator, NLRP3 inflammasome, in vasculopathy of SSc.
NLRP3 and fibrosis in SSc
Excessive fibrosis is the most characteristic pathological feature in SSc, which results from excessive synthesis and deposition of ECM. The fibroblast-to-myofibroblast transition (FMT) after activation by inflammatory factors and mechanical damage is a crucial procedure in fibrosis. Myofibroblasts feature increased excretion of inflammatory factors and ECM [92]. ECM consists of collagen, elastin, glycosaminoglycans, tenascin, and fibronectin [58]. TGF-β is an important profibrotic mediator which could be secreted by several immune cells as well as myofibroblasts.
Recently, the role of NLRP3 inflammasome in SSc fibrosis has attached great concern. High expression of NLRP3, caspase-1, IL-1β, and IL-18 and over-activated NLRP3 inflammasome were found in skin biopsy specimen from SSc patients and showed a positive correlation with modified Rodnan skin thickness score (mRSS), a measure of skin involvement, in which higher scores represent severe skin fibrosis [59]. NLRP3 seems crucial in fibrosis as the involvement of skin and lung is alleviated when NLRP3 or ASC is knocked out in BLM-induced mice [62]. Similar results could be seen in caspase-1 or IL-18 knocked out mice [61]. Caspase-1 takes part in α-SMA expression of myofibroblasts from SSc dermis [62]. Reduction in collagen expression level and myofibroblast thickness in SSc derma could be induced by selectively blocking caspase-1 [62]. However, Bozena et al. found a decrease of serum caspase-1 in SSc patients comparing to healthy control and the caspase-1 levels demonstrate negative correlation with involvement in skin and visceral organ [93]. IL-18 was reported to upregulate IFN-γ and IL-13 production in T cells and induce lung fibrosis [94]. Zhang et al. also found increased αiSMA expression in myofibroblasts and enhanced fibrosis in liver, which could be inhibited by anti-IL-18 treatment [95]. It suggested that the function of NLRP3 inflammasome and its downstream products in SSc might be more than a proinflammatory role, which requires further investigation. Table 1 shows the role of NLRP3 inflammasome in fibrosis of SSc.
Table 1.
Mechanism of NLRP3 inflammasome in SSc fibrosis
| Samples | Method | Blockage target | Treatment | Results | Reference |
|---|---|---|---|---|---|
| SSc dermal and lung fibroblasts | Z-YVAD (OMe)-FMK | Caspase-1 | - | Reduced expression of collagen, α-SMA, and contractile fibers | [62] |
| SSc dermal and lung fibroblasts | SiRNA of caspase-1 | Caspase-1 | - | Reduced secretion of hydroxyproline | [62] |
| C57BL/6 mice-derived fibroblasts | NLRP3−/− | NLRP3 | BLM | Undetected hydroxyproline secretion | [62] |
| C57BL/6 mice-derived fibroblasts | ASC−/− | ASC | BLM | Undetected hydroxyproline secretion | [62] |
| C57BL/6 mice-derived fibroblasts | Z-YVAD (OMe)-FMK | Caspase-1 | BLM | Reduced secretion of hydroxyproline | [62] |
| C57BL/6 mice | ASC−/− | ASC | BLM injection | Removed increased skin thickness and pulmonary fibrosis induced by BLM | [62] |
| C57BL/6 mice | NLRP3−/− | NLRP3 | BLM injection | Removed increased skin thickness and pulmonary fibrosis induced by BLM | [62] |
| C57BL/6 mice | Caspase-1−/− | Caspase-1 | BLM injection | Decreased neutrophils in BALF | [61] |
| C57BL/6 mice | IL-18−/− | IL-18 | BLM injection | Decreased lung injury and pulmonary fibrosis | [61] |
| B6×129 hybrid mice | Caspase-1−/− | Caspase-1 | BLM injection | Alleviated pulmonary fibrosis and lower lung hydroxyproline content | [61] |
Abbreviations: BLM bleomycin, BALF bronchoalveolar lavage fluid, SSc systemic sclerosis
Recently, studies showed more interesting mechanisms of SSc onset. Fibroblasts from SSc patients exhibited higher Ca2+ permeability responding to P2X7R activating, which might give rise to NLRP3 activation in SSc [96]. MiR-155 was marked as the most expressed miRNA in fibroblasts from SSc patients and a necessary role in collagen synthesis [97, 98], and the function of miR-155 signaling in fibrosis is dependent on activation of NLRP3 [99].
NLRP3 and musculoskeleton involvement in SSc
Musculoskeletal symptoms, involving joints, tendon, and muscle are quite common in SSc patients and contribute greatly in reducing quality of life [100, 101]. Articular involvement such as arthralgia and synovitis exists during course of SSc in nearly half of the patients and some of them are diagnosed as arthritis at first [102]. Myalgia and weakness resulted from myositis, while tendon friction rubs and tenosynovitis with a prevalence of about 11% are most featured tendon involvement in SSc [103]. Relations between NLRP3 and musculoskeletal involvement was reported as over-activated NLRP3 leads to chronic arthritis in mice [104]. Moreover, it was found that NLRP3 might contribute to ECM disorganization and inflammation in tendon injury [105]. What is more, upregulated expression of IL-1β and caspase-1 could be found in muscle biopsies from SSc patients with myositis [106]. Thus, the role of NLRP3 in musculoskeleton involvement deserves further investigation.
Therapeutic target on NLRP3 in SSc
Recently, research of treatments aiming at NLRP3 inflammasome signaling cascade shows a promising target for inflammatory diseases including SSc. MCC950, also known as CP-456,773, is a highly specific NLRP3 inhibitor which declines maturation and excretion of IL-1β through suppressing assembly of NLRP3 inflammasome [107, 108]. Van et al. demonstrated NEK7 as a potential target of MCC950 whereas Perera et al. argued that MCC950 could not prevent NEK7-NLRP3 interaction [109, 110]. MCC950 has shown its protective property through inhibition of NLRP3 activation in silicon dioxide-induced pulmonary fibrosis through preventing macrophage-derived IL-1β excretion and then impeding myofibroblasts transition [111]. The anti-fibrosis function of MCC950 is also reported in liver, myocardium, and kidney [112–114]. However, MCC950 presented hepatotoxicity in clinical trials for RA, which might limit its further development [115]. CY-09 is a newly found selective NLRP3 inhibitor which inhibits ATPase activity through directly binding to NACHT domain [116]. Gao et al. suggested that CY-09 could reduce myocardial fibrosis induced by ischemia [117].
Addition to small-molecule inhibitors, several endogenous molecules targeting NLRP3 are also of note. A20, an anti-inflammatory protein which is also known as TNF-α-induced protein 3 (TNFAIP3), shows a protective role in pulmonary fibrosis and it was reported to reduce NLRP3-mediated cytokine secretion and pyroptosis in RA [104, 118]. What is more, β-hydroxybutyrate (BHB), an oxidative metabolite of fat, was demonstrated to suppress NLRP3 inflammasome activation through inhibiting K+ efflux and ASC speck formation [119]. Intriguingly, ketogenic diet, which could elevate BHB levels in serum, also reduces caspase-1 maturation and IL-1β secretion, indicating a supplementary means of dietary therapy to treatment in NLRP3-relevant diseases [119].
Caspase-1 as the executor in NLRP3 inflammasome is also a remarkable target for NLRP3 block. YVAD-CHO is a reversible caspase-1 inhibitor, which reduces IL-1β excretion in SSc monocytes [120]. Treatment of another caspase-1 inhibitor Z-YVAD-FMK eliminates oversecretion of IL-1β in fibroblasts from skin and lung of SSc patients [62]. IL-1 signaling blockers targeting IL-1R have attracted much attention as several of them have been used in clinic. Anakinra, an IL-1R antagonist, manifests capacity in improving BLM-induced pulmonary fibrosis in mice [121]. Evidence in clinical trial conducted in RA patients suggests that anakinra improves vascular function [122]. However, no clear conclusion could be drawn in SSc management due to the lack of data. A summary of NLRP3 inflammasome inhibitors is shown in Table 2.
Table 2.
Inhibitors of NLRP3 inflammasome in SSc therapy
| Inhibitor | Target | Evidence | Reference |
|---|---|---|---|
| MCC950(CP-456,773) | NLRP3 | Prevents IL-1β excretion, impeding myofibroblast transition and pulmonary fibrosis | [111] |
| Reduces inflammation and liver fibrosis | [112] | ||
| Reduces immune cell infiltration and myocardial fibrosis | [113] | ||
| Reduces immune cell infiltration and collagen production in kidney | [114] | ||
| CY-09 | NLRP3 | Reduces ischemia-induced myocardial fibrosis | [117] |
| A20 (TNFAIP3) | NLRP3 | Prevents pulmonary fibrosis | [118] |
| Reduces NLRP3-mediated cytokine secretion and pyroptosis in RA | [104] | ||
| BHB | NLRP3 | Reduces caspase-1 maturation and IL-1β secretion | [119] |
| YVAD-CHO | Caspase-1 | Reduces IL-1β excretion in SSc monocytes | [120] |
| Z-YVAD-FMK | Caspase-1 | Eliminates oversecretion of IL-1β in fibroblasts from skin and lung of SSc patients | [62] |
| Anakinra | IL-1R | Alleviates BLM-induced inflammation and pulmonary fibrosis | [121] |
| Improves vascular function in RA patients | [122] |
Abbreviations: SSc systemic sclerosis, IL interleukin, RA rheumatoid arthritis, BHB β-hydroxybutyrate
Possible side effects should be of note as NLRP3 plays an important role in immune defense system. Treatment with MCC950 weakens early protective immune response towards influenza A virus [123]. Infections like pneumonia and gastroenteritis turns out to be the most common serious adverse events in anakinra treatments [124]. Thus, it requires cautious consideration when taking NLRP3 and its products as the therapeutic target.
Conclusion
As its function on mediating proinflammatory cytokines such as IL-1β and IL-18, NLRP3 is involved in many inflammatory immune-relevant diseases, including SSc. This review elaborate NLRP3 and its potential association with the autoimmune dysfunction, vascular damage, fibrosis of skin, and visceral organ in SSc. Despite contradictory conclusions, NLRP3 might play a potential role in SSc pathogenesis and offers promising insight into SSc treatment.
Acknowledgements
The authors acknowledge the support from the National Natural Science Foundation of China (No. 82161138022) and Shanghai Pujiang Young Rheumatologists Training Program (No. SPROG2106).
Abbreviations
- SSc
Systemic sclerosis
- PRR
Pattern recognition receptors
- PAMP
Pathogen-associated molecular pattern
- DAMP
Damage-associated molecular pattern
- NLR
Nucleotide-binding oligomerization domain-like receptor
- IL
Interleukin
- TLR
Toll-like receptor
- CLR
C-type lectin receptor
- RLR
Retinoic acid-inducible gene-I-like receptor
- ALR
Absent in melanoma 2-like receptor
- LRR
Leucine-rich repeat
- PYD
Pyrin domain
- IFN
Interferon
- RA
Rheumatoid arthritis
- SLE
Systemic lupus erythematosus
- MyD88
Myeloid differentiation primary response gene-88
- TIR
Toll-IL-1 receptor
- GSDMD
Gasdermin D
- Nterm
N-terminal cell death domain
- mtDNA
Mitochondrial DNA
- mtROS
Mitochondrial reactive oxygen species
- NEK7
Never in mitosis A-related kinase 7
- ECM
Excrete extracellular matrix
- BLM
Bleomycin
- M1
Classical activated macrophages
- M2
Alternative activated macrophage
- TGF-β
Transforming growth factor β
- Th
T helper
- TNF
Tumor necrosis factor
- PTPN22
Protein tyrosine phosphatase N22
- EC
Endothelial cell
- VEGF
Vascular endothelial growth factor
- PAH
Pulmonary hypertension
- PBMC
Peripheral blood mononuclear cell
- ET
Endothelin
- NO
Nitric oxide
- FMT
Fibroblast-to-myofibroblast transition
- mRSS
Modified Rodnan skin thickness score
- TNFAIP3
TNF-α-induced protein 3
- BHB
β-hydroxybutyrate
Authors’ contributions
CL contributed to material collecting and manuscript drafting. ZJ and LC contributed to the literature retrieval and selection. XZ and HZ contributed to revise the manuscript with significant input. All authors reviewed the manuscript. All authors read and approved the final manuscript.
Funding
This work was supported by the National Natural Science Foundation of China under Grant (No. 82161138022) and Shanghai Pujiang Young Rheumatologists Training Program (No. SPROG2106).
Availability of data and materials
All data are available from the corresponding author.
Declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
All of the authors approved the manuscript for publication.
Competing interests
The authors declare that they have no competing interests.
Footnotes
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Allanore Y, Simms R, Distler O, Trojanowska M, Pope J, Denton CP, Varga J. Systemic sclerosis. Nat Rev Dis Primers. 2015;1:15002. doi: 10.1038/nrdp.2015.2. [DOI] [PubMed] [Google Scholar]
- 2.Tsou P-S, Varga J, O'Reilly S. Advances in epigenetics in systemic sclerosis: molecular mechanisms and therapeutic potential. Nat Rev Rheumatol. 2021;17(10):596–607. doi: 10.1038/s41584-021-00683-2. [DOI] [PubMed] [Google Scholar]
- 3.Li Z, Guo J, Bi L. Role of the NLRP3 inflammasome in autoimmune diseases. Biomed Pharmacother. 2020;130:110542. doi: 10.1016/j.biopha.2020.110542. [DOI] [PubMed] [Google Scholar]
- 4.Fusco R, Siracusa R, Genovese T, Cuzzocrea S, Di Paola R. Focus on the role of NLRP3 inflammasome in diseases. Int J Mol Sci. 2020;21(12):4223. doi: 10.3390/ijms21124223. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Gong T, Liu L, Jiang W, Zhou R. DAMP-sensing receptors in sterile inflammation and inflammatory diseases. Nat Rev Immunol. 2020;20(2):95–112. doi: 10.1038/s41577-019-0215-7. [DOI] [PubMed] [Google Scholar]
- 6.Duncan JA, Bergstralh DT, Wang Y, Willingham SB, Ye Z, Zimmermann AG. Ting JP-Y: Cryopyrin/NALP3 binds ATP/dATP, is an ATPase, and requires ATP binding to mediate inflammatory signaling. Proc Natl Acad Sci U S A. 2007;104(19):8041–8046. doi: 10.1073/pnas.0611496104. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Swanson KV, Deng M, Ting JPY. The NLRP3 inflammasome: molecular activation and regulation to therapeutics. Nat Rev Immunol. 2019;19(8):477–489. doi: 10.1038/s41577-019-0165-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Chen L, Cao S-Q, Lin Z-M, He S-J, Zuo J-P. NOD-like receptors in autoimmune diseases. Acta Pharmacol Sin. 2021;42(11):1742–1756. doi: 10.1038/s41401-020-00603-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Milner MT, Maddugoda M, Götz J, Burgener SS, Schroder K. The NLRP3 inflammasome triggers sterile neuroinflammation and Alzheimer's disease. Curr Opin Immunol. 2021;68:116–124. doi: 10.1016/j.coi.2020.10.011. [DOI] [PubMed] [Google Scholar]
- 10.Vandanmagsar B, Youm Y-H, Ravussin A, Galgani JE, Stadler K, Mynatt RL, Ravussin E, Stephens JM, Dixit VD. The NLRP3 inflammasome instigates obesity-induced inflammation and insulin resistance. Nat Med. 2011;17(2):179–188. doi: 10.1038/nm.2279. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Hirota SA, Ng J, Lueng A, Khajah M, Parhar K, Li Y, Lam V, Potentier MS, Ng K, Bawa M, et al. NLRP3 inflammasome plays a key role in the regulation of intestinal homeostasis. Inflamm Bowel Dis. 2011;17(6):1359–1372. doi: 10.1002/ibd.21478. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Daley D, Mani VR, Mohan N, Akkad N, Pandian GSDB, Savadkar S, Lee KB, Torres-Hernandez A, Aykut B, Diskin B, et al. NLRP3 signaling drives macrophage-induced adaptive immune suppression in pancreatic carcinoma. J Exp Med. 2017;214(6):1711–1724. doi: 10.1084/jem.20161707. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Xie CB, Qin L, Li G, Fang C, Kirkiles-Smith NC, Tellides G, Pober JS, Jane-Wit D. Complement membrane attack complexes assemble NLRP3 inflammasomes triggering IL-1 activation of IFN-γ-primed human endothelium. Circ Res. 2019;124(12):1747–1759. doi: 10.1161/CIRCRESAHA.119.314845. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Wang X, Li X, Wu Y, Song Y. Upregulation of miR-223 abrogates NLRP3 inflammasome-mediated pyroptosis to attenuate oxidized low-density lipoprotein (ox-LDL)-induced cell death in human vascular endothelial cells (ECs) In Vitro Cell Dev Biol Anim. 2020;56(8):670–679. doi: 10.1007/s11626-020-00496-9. [DOI] [PubMed] [Google Scholar]
- 15.Ma P, Zha S, Shen X, Zhao Y, Li L, Yang L, Lei M, Liu W. NFAT5 mediates hypertonic stress-induced atherosclerosis via activating NLRP3 inflammasome in endothelium. Cell Commun Signal. 2019;17(1):102. doi: 10.1186/s12964-019-0406-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Lee S, Kim SK, Park H, Lee YJ, Park SH, Lee KJ, et al. Contribution of autophagy-Notch1-mediated NLRP3 inflammasome activation to chronic inflammation and fibrosis in keloid fibroblasts. Int J Mol Sci. 2020;21(21):8050. doi: 10.3390/ijms21218050. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Kapetanaki S, Kumawat AK, Persson K, Demirel I. The fibrotic effects of TMAO on human renal fibroblasts is mediated by NLRP3, caspase-1 and the PERK/Akt/mTOR pathway. Int J Mol Sci. 2021;22(21):11864. doi: 10.3390/ijms222111864. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Zhao C, Zhao W. NLRP3 Inflammasome-a key player in antiviral responses. Front Immunol. 2020;11:211. doi: 10.3389/fimmu.2020.00211. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Sayan M, Mossman BT. The NLRP3 inflammasome in pathogenic particle and fibre-associated lung inflammation and diseases. Particle Fibre Toxicol. 2016;13(1):51. doi: 10.1186/s12989-016-0162-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Lu A, Magupalli VG, Ruan J, Yin Q, Atianand MK, Vos MR, Schröder GF, Fitzgerald KA, Wu H, Egelman EH. Unified polymerization mechanism for the assembly of ASC-dependent inflammasomes. Cell. 2014;156(6):1193–1206. doi: 10.1016/j.cell.2014.02.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Schmidt FI, Lu A, Chen JW, Ruan J, Tang C, Wu H, Ploegh HL. A single domain antibody fragment that recognizes the adaptor ASC defines the role of ASC domains in inflammasome assembly. J Exp Med. 2016;213(5):771–790. doi: 10.1084/jem.20151790. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Yang X, Chang HY, Baltimore D. Autoproteolytic activation of pro-caspases by oligomerization. Mol Cell. 1998;1(2):319–325. doi: 10.1016/S1097-2765(00)80032-5. [DOI] [PubMed] [Google Scholar]
- 23.Galozzi P, Bindoli S, Doria A, Sfriso P. The revisited role of interleukin-1 alpha and beta in autoimmune and inflammatory disorders and in comorbidities. Autoimmun Rev. 2021;20(4):102785. doi: 10.1016/j.autrev.2021.102785. [DOI] [PubMed] [Google Scholar]
- 24.Yasuda K, Nakanishi K, Tsutsui H. Interleukin-18 in Health and Disease. Int J Mol Sci. 2019;20(3):649. doi: 10.3390/ijms20030649. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Shi J, Gao W, Shao F. Pyroptosis: gasdermin-mediated programmed necrotic cell death. Trends Biochem Sci. 2017;42(4):245–254. doi: 10.1016/j.tibs.2016.10.004. [DOI] [PubMed] [Google Scholar]
- 26.He W-t, Wan H, Hu L, Chen P, Wang X, Huang Z, Yang Z-H, Zhong C-Q, Han J. Gasdermin D is an executor of pyroptosis and required for interleukin-1β secretion. Cell Res. 2015;25(12):1285–1298. doi: 10.1038/cr.2015.139. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Shi J, Zhao Y, Wang K, Shi X, Wang Y, Huang H, Zhuang Y, Cai T, Wang F, Shao F. Cleavage of GSDMD by inflammatory caspases determines pyroptotic cell death. Nature. 2015;526(7575):660–665. doi: 10.1038/nature15514. [DOI] [PubMed] [Google Scholar]
- 28.Ding J, Wang K, Liu W, She Y, Sun Q, Shi J, Sun H, Wang D-C, Shao F. Pore-forming activity and structural autoinhibition of the gasdermin family. Nature. 2016;535(7610):111–116. doi: 10.1038/nature18590. [DOI] [PubMed] [Google Scholar]
- 29.Downs KP, Nguyen H, Dorfleutner A, Stehlik C. An overview of the non-canonical inflammasome. Mol Asp Med. 2020;76:100924. doi: 10.1016/j.mam.2020.100924. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Platnich JM, Chung H, Lau A, Sandall CF, Bondzi-Simpson A, Chen H-M, et al. Shiga toxin/lipopolysaccharide activates caspase-4 and gasdermin D to trigger mitochondrial reactive oxygen species upstream of the NLRP3 inflammasome. Cell Rep. 2018;25(6):1525–1536. doi: 10.1016/j.celrep.2018.09.071. [DOI] [PubMed] [Google Scholar]
- 31.Viganò E, Diamond CE, Spreafico R, Balachander A, Sobota RM, Mortellaro A. Human caspase-4 and caspase-5 regulate the one-step non-canonical inflammasome activation in monocytes. Nat Commun. 2015;6:8761. doi: 10.1038/ncomms9761. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Kayagaki N, Warming S, Lamkanfi M, Vande Walle L, Louie S, Dong J, Newton K, Qu Y, Liu J, Heldens S, et al. Non-canonical inflammasome activation targets caspase-11. Nature. 2011;479(7371):117–121. doi: 10.1038/nature10558. [DOI] [PubMed] [Google Scholar]
- 33.Rathinam VAK, Vanaja SK, Waggoner L, Sokolovska A, Becker C, Stuart LM, Leong JM, Fitzgerald KA. TRIF licenses caspase-11-dependent NLRP3 inflammasome activation by gram-negative bacteria. Cell. 2012;150(3):606–619. doi: 10.1016/j.cell.2012.07.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Cheng KT, Xiong S, Ye Z, Hong Z, Di A, Tsang KM, Gao X, An S, Mittal M, Vogel SM, et al. Caspase-11-mediated endothelial pyroptosis underlies endotoxemia-induced lung injury. J Clin Invest. 2017;127(11):4124–4135. doi: 10.1172/JCI94495. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Zasłona Z, Flis E, Wilk MM, Carroll RG, Palsson-McDermott EM, Hughes MM, Diskin C, Banahan K, Ryan DG, Hooftman A, et al. Caspase-11 promotes allergic airway inflammation. Nat Commun. 2020;11(1):1055. doi: 10.1038/s41467-020-14945-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Armstrong H, Bording-Jorgensen M, Chan R, Wine E. Nigericin promotes NLRP3-independent bacterial killing in macrophages. Front Immunol. 2019;10:2296. doi: 10.3389/fimmu.2019.02296. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.He Y, Zeng MY, Yang D, Motro B, Núñez G. NEK7 is an essential mediator of NLRP3 activation downstream of potassium efflux. Nature. 2016;530(7590):354–357. doi: 10.1038/nature16959. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Pétrilli V, Papin S, Dostert C, Mayor A, Martinon F, Tschopp J. Activation of the NALP3 inflammasome is triggered by low intracellular potassium concentration. Cell Death Differ. 2007;14(9):1583–1589. doi: 10.1038/sj.cdd.4402195. [DOI] [PubMed] [Google Scholar]
- 39.Schmid-Burgk JL, Chauhan D, Schmidt T, Ebert TS, Reinhardt J, Endl E, Hornung V. A genome-wide CRISPR (clustered regularly interspaced short palindromic repeats) screen identifies NEK7 as an essential component of NLRP3 inflammasome activation. J Biol Chem. 2016;291(1):103–109. doi: 10.1074/jbc.C115.700492. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Sharif H, Wang L, Wang WL, Magupalli VG, Andreeva L, Qiao Q, Hauenstein AV, Wu Z, Núñez G, Mao Y, et al. Structural mechanism for NEK7-licensed activation of NLRP3 inflammasome. Nature. 2019;570(7761):338–343. doi: 10.1038/s41586-019-1295-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Muñoz-Planillo R, Kuffa P, Martínez-Colón G, Smith BL, Rajendiran TM, Núñez G. K+ efflux is the common trigger of NLRP3 inflammasome activation by bacterial toxins and particulate matter. Immunity. 2013;38(6):1142–1153. doi: 10.1016/j.immuni.2013.05.016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Di A, Xiong S, Ye Z, Malireddi RKS, Kometani S, Zhong M, et al. The TWIK2 potassium efflux channel in macrophages mediates NLRP3 inflammasome-induced inflammation. Immunity. 2018;49(1):56–65. doi: 10.1016/j.immuni.2018.04.032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Tapia-Abellán A, Angosto-Bazarra D, Alarcón-Vila C, Baños MC, Hafner-Bratkovič I, Oliva B, Pelegrín P. Sensing low intracellular potassium by NLRP3 results in a stable open structure that promotes inflammasome activation. Sci Adv. 2021;7(38):eabf4468. doi: 10.1126/sciadv.abf4468. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Groß CJ, Mishra R, Schneider KS, Médard G, Wettmarshausen J, Dittlein DC, Shi H, Gorka O, Koenig P-A, Fromm S, et al. K efflux-independent NLRP3 inflammasome activation by small molecules targeting mitochondria. Immunity. 2016;45(4):761–773. doi: 10.1016/j.immuni.2016.08.010. [DOI] [PubMed] [Google Scholar]
- 45.Lee G-S, Subramanian N, Kim AI, Aksentijevich I, Goldbach-Mansky R, Sacks DB, Germain RN, Kastner DL, Chae JJ. The calcium-sensing receptor regulates the NLRP3 inflammasome through Ca2+ and cAMP. Nature. 2012;492(7427):123–127. doi: 10.1038/nature11588. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Swanton T, Beswick JA, Hammadi H, Morris L, Williams D, de Cesco S, El-Sharkawy L, Yu S, Green J, Davis JB, et al. Selective inhibition of the K efflux sensitive NLRP3 pathway by Cl channel modulation. Chem Sci. 2020;11(43):11720–11728. doi: 10.1039/D0SC03828H. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Katsnelson MA, Rucker LG, Russo HM, Dubyak GR. K+ efflux agonists induce NLRP3 inflammasome activation independently of Ca2+ signaling. J Immunol. 2015;194(8):3937–3952. doi: 10.4049/jimmunol.1402658. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Pellegrini C, Antonioli L, Lopez-Castejon G, Blandizzi C, Fornai M. Canonical and non-canonical activation of NLRP3 inflammasome at the crossroad between immune tolerance and intestinal inflammation. Front Immunol. 2017;8:36. doi: 10.3389/fimmu.2017.00036. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Zhou R, Yazdi AS, Menu P, Tschopp J. A role for mitochondria in NLRP3 inflammasome activation. Nature. 2011;469(7329):221–225. doi: 10.1038/nature09663. [DOI] [PubMed] [Google Scholar]
- 50.Yu J, Nagasu H, Murakami T, Hoang H, Broderick L, Hoffman HM, Horng T. Inflammasome activation leads to Caspase-1-dependent mitochondrial damage and block of mitophagy. Proc Natl Acad Sci U S A. 2014;111(43):15514–15519. doi: 10.1073/pnas.1414859111. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Wolf AJ, Reyes CN, Liang W, Becker C, Shimada K, Wheeler ML, Cho HC, Popescu NI, Coggeshall KM, Arditi M, et al. Hexokinase is an innate immune receptor for the detection of bacterial peptidoglycan. Cell. 2016;166(3):624–636. doi: 10.1016/j.cell.2016.05.076. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Wen H, Gris D, Lei Y, Jha S, Zhang L. Huang MT-H, Brickey WJ, Ting JPY: Fatty acid-induced NLRP3-ASC inflammasome activation interferes with insulin signaling. Nat Immunol. 2011;12(5):408–415. doi: 10.1038/ni.2022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Prescott RJ, Freemont AJ, Jones CJ, Hoyland J, Fielding P. Sequential dermal microvascular and perivascular changes in the development of scleroderma. J Pathol. 1992;166(3):255–263. doi: 10.1002/path.1711660307. [DOI] [PubMed] [Google Scholar]
- 54.Asano Y, Sato S. Vasculopathy in scleroderma. Semin Immunopathol. 2015;37(5):489–500. doi: 10.1007/s00281-015-0505-5. [DOI] [PubMed] [Google Scholar]
- 55.Wynn TA. Cellular and molecular mechanisms of fibrosis. J Pathol. 2008;214(2):199–210. doi: 10.1002/path.2277. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Bossini-Castillo L, López-Isac E, Mayes MD, Martín J. Genetics of systemic sclerosis. Semin Immunopathol. 2015;37(5):443–451. doi: 10.1007/s00281-015-0499-z. [DOI] [PubMed] [Google Scholar]
- 57.De Martinis M, Ciccarelli F, Sirufo MM, Ginaldi L. An overview of environmental risk factors in systemic sclerosis. Expert Rev Clin Immunol. 2016;12(4):465–478. doi: 10.1586/1744666X.2016.1125782. [DOI] [PubMed] [Google Scholar]
- 58.Cutolo M, Soldano S, Smith V. Pathophysiology of systemic sclerosis: current understanding and new insights. Expert Rev Clin Immunol. 2019;15(7):753–764. doi: 10.1080/1744666X.2019.1614915. [DOI] [PubMed] [Google Scholar]
- 59.Martínez-Godínez MA, Cruz-Domínguez MP, Jara LJ, Domínguez-López A, Jarillo-Luna RA, Vera-Lastra O, et al. Expression of NLRP3 inflammasome, cytokines and vascular mediators in the skin of systemic sclerosis patients. Isr Med Assoc J. 2015;17(1):5–10. [PubMed] [Google Scholar]
- 60.Lin E, Vincent FB, Sahhar J, Ngian G-S, Kandane-Rathnayake R, Mende R, Morand EF, Lang T, Harris J. Analysis of serum interleukin(IL)-1α, IL-1β and IL-18 in patients with systemic sclerosis. Clin Transl Immunol. 2019;8(4):e1045. doi: 10.1002/cti2.1045. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Hoshino T, Okamoto M, Sakazaki Y, Kato S, Young HA, Aizawa H. Role of proinflammatory cytokines IL-18 and IL-1 beta in bleomycin-induced lung injury in humans and mice. Am J Respir Cell Mol Biol. 2009;41(6):661–670. doi: 10.1165/rcmb.2008-0182OC. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Artlett CM, Sassi-Gaha S, Rieger JL, Boesteanu AC, Feghali-Bostwick CA, Katsikis PD. The inflammasome activating caspase 1 mediates fibrosis and myofibroblast differentiation in systemic sclerosis. Arthritis Rheum. 2011;63(11):3563–3574. doi: 10.1002/art.30568. [DOI] [PubMed] [Google Scholar]
- 63.Dai B, Ding L, Zhao L, Zhu H, Luo H. Contributions of immune cells and stromal cells to the pathogenesis of systemic sclerosis: recent insights. Front Pharmacol. 2022;13:826839. doi: 10.3389/fphar.2022.826839. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Gilbane AJ, Denton CP, Holmes AM. Scleroderma pathogenesis: a pivotal role for fibroblasts as effector cells. Arthritis Res Ther. 2013;15(3):215. doi: 10.1186/ar4230. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Bhandari R, Ball MS, Martyanov V, Popovich D, Schaafsma E, Han S, ElTanbouly M, Orzechowski NM, Carns M, Arroyo E, et al. Profibrotic activation of human macrophages in systemic sclerosis. Arthritis Rheumatol. 2020;72(7):1160–1169. doi: 10.1002/art.41243. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Worrell JC, O'Reilly S. Bi-directional communication: conversations between fibroblasts and immune cells in systemic sclerosis. J Autoimmun. 2020;113:102526. doi: 10.1016/j.jaut.2020.102526. [DOI] [PubMed] [Google Scholar]
- 67.Trombetta AC, Soldano S, Contini P, Tomatis V, Ruaro B, Paolino S, Brizzolara R, Montagna P, Sulli A, Pizzorni C, et al. A circulating cell population showing both M1 and M2 monocyte/macrophage surface markers characterizes systemic sclerosis patients with lung involvement. Respir Res. 2018;19(1):186. doi: 10.1186/s12931-018-0891-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Mohamed ME, Gamal RM, El-Mokhtar MA, Hassan AT, Abozaid HSM, Ghandour AM, Ismail SAA, Yousef HA, El-Hakeim EH, Makarem YS, et al. Peripheral cells from patients with systemic sclerosis disease co-expressing M1 and M2 monocyte/macrophage surface markers: Relation to the degree of skin involvement. Hum Immunol. 2021;82(9):634–639. doi: 10.1016/j.humimm.2021.03.009. [DOI] [PubMed] [Google Scholar]
- 69.Liu T, Wang L, Liang P, Wang X, Liu Y, Cai J, She Y, Wang D, Wang Z, Guo Z, et al. USP19 suppresses inflammation and promotes M2-like macrophage polarization by manipulating NLRP3 function via autophagy. Cell Mol Immunol. 2021;18(10):2431–2442. doi: 10.1038/s41423-020-00567-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Laurent P, Lapoirie J, Leleu D, Levionnois E, Grenier C, Jurado-Mestre B, et al. Interleukin-1β-Activated microvascular endothelial cells promote DC-SIGN-positive alternatively activated macrophages as a mechanism of skin fibrosis in systemic sclerosis. Arthritis Rheumatol. 2021;74(6):1013–1026. doi: 10.1002/art.42061. [DOI] [PubMed] [Google Scholar]
- 71.Wu H, Xu X, Zheng A, Wang W, Mei L, Chen Y, Sun S, Jiang L, Wu Y, Zhou Y, et al. TNF-α-induce protein 8-like 1 inhibits hepatic steatosis, inflammation, and fibrosis by suppressing polyubiquitination of apoptosis signal-regulating kinase 1. Hepatology. 2021;74(3):1251–1270. doi: 10.1002/hep.31801. [DOI] [PubMed] [Google Scholar]
- 72.Boin F, De Fanis U, Bartlett SJ, Wigley FM, Rosen A, Casolaro V. T cell polarization identifies distinct clinical phenotypes in scleroderma lung disease. Arthritis Rheum. 2008;58(4):1165–1174. doi: 10.1002/art.23406. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Birnhuber A, Crnkovic S, Biasin V, Marsh LM, Odler B, Sahu-Osen A, et al. IL-1 receptor blockade skews inflammation towards Th2 in a mouse model of systemic sclerosis. Eur Respir J. 2019;54(3):1900154. doi: 10.1183/13993003.00154-2019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74.Sanges S, Guerrier T, Launay D, Lefèvre G, Labalette M, Forestier A, Sobanski V, Corli J, Hauspie C, Jendoubi M, et al. Role of B cells in the pathogenesis of systemic sclerosis. Rev Med Interne. 2017;38(2):113–124. doi: 10.1016/j.revmed.2016.02.016. [DOI] [PubMed] [Google Scholar]
- 75.Spalinger MR, Kasper S, Gottier C, Lang S, Atrott K, Vavricka SR, Scharl S, Raselli T, Frey-Wagner I, Gutte PM, et al. NLRP3 tyrosine phosphorylation is controlled by protein tyrosine phosphatase PTPN22. J Clin Invest. 2016;126(5):1783–1800. doi: 10.1172/JCI83669. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Wu M, Mohan C. B-cells in systemic sclerosis: emerging evidence from genetics to phenotypes. Curr Opin Rheumatol. 2015;27(6):537–541. doi: 10.1097/BOR.0000000000000215. [DOI] [PubMed] [Google Scholar]
- 77.Gourh P, Tan FK, Assassi S, Ahn CW, McNearney TA, Fischbach M, Arnett FC, Mayes MD. Association of the PTPN22 R620W polymorphism with anti-topoisomerase I- and anticentromere antibody-positive systemic sclerosis. Arthritis Rheum. 2006;54(12):3945–3953. doi: 10.1002/art.22196. [DOI] [PubMed] [Google Scholar]
- 78.Lim K-H, Chen L-C, Hsu K, Chang C-C, Chang C-Y, Kao C-W, Chang Y-F, Chang M-C, Chen CG. BAFF-driven NLRP3 inflammasome activation in B cells. Cell Death Dis. 2020;11(9):820. doi: 10.1038/s41419-020-03035-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Ali MF, Dasari H, Van Keulen VP, Carmona EM. Canonical stimulation of the NLRP3 inflammasome by fungal antigens links innate and adaptive B-lymphocyte responses by modulating IL-1β and IgM production. Front Immunol. 2017;8:1504. doi: 10.3389/fimmu.2017.01504. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Ding Y, Yan Y, Dong Y, Xu J, Su W, Shi W, Zou Q, Yang X. NLRP3 promotes immune escape by regulating immune checkpoints: a pan-cancer analysis. Int Immunopharmacol. 2022;104:108512. doi: 10.1016/j.intimp.2021.108512. [DOI] [PubMed] [Google Scholar]
- 81.Mostmans Y, Cutolo M, Giddelo C, Decuman S, Melsens K, Declercq H, Vandecasteele E, De Keyser F, Distler O, Gutermuth J, et al. The role of endothelial cells in the vasculopathy of systemic sclerosis: a systematic review. Autoimmun Rev. 2017;16(8):774–786. doi: 10.1016/j.autrev.2017.05.024. [DOI] [PubMed] [Google Scholar]
- 82.Xia M, Boini KM, Abais JM, Xu M, Zhang Y, Li P-L. Endothelial NLRP3 inflammasome activation and enhanced neointima formation in mice by adipokine visfatin. Am J Pathol. 2014;184(5):1617–1628. doi: 10.1016/j.ajpath.2014.01.032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Xia X, Shi Q, Song X, Fu J, Liu Z, Wang Y, Wang Y, Su C, Song E, Song Y. Tetrachlorobenzoquinone stimulates NLRP3 inflammasome-mediated post-translational activation and secretion of IL-1β in the HUVEC endothelial cell line. Chem Res Toxicol. 2016;29(3):421–429. doi: 10.1021/acs.chemrestox.6b00021. [DOI] [PubMed] [Google Scholar]
- 84.Jiang C, Jiang L, Li Q, Liu X, Zhang T, Dong L, Liu T, Liu L, Hu G, Sun X, et al. Acrolein induces NLRP3 inflammasome-mediated pyroptosis and suppresses migration via ROS-dependent autophagy in vascular endothelial cells. Toxicology. 2018;410:26–40. doi: 10.1016/j.tox.2018.09.002. [DOI] [PubMed] [Google Scholar]
- 85.Wu X, Zhang H, Qi W, Zhang Y, Li J, Li Z, Lin Y, Bai X, Liu X, Chen X, et al. Nicotine promotes atherosclerosis via ROS-NLRP3-mediated endothelial cell pyroptosis. Cell Death Dis. 2018;9(2):171. doi: 10.1038/s41419-017-0257-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 86.Block JA, Sequeira W. Raynaud's phenomenon. Lancet. 2001;357(9273):2042–2048. doi: 10.1016/S0140-6736(00)05118-7. [DOI] [PubMed] [Google Scholar]
- 87.Mao K, Chen S, Chen M, Ma Y, Wang Y, Huang B, He Z, Zeng Y, Hu Y, Sun S, et al. Nitric oxide suppresses NLRP3 inflammasome activation and protects against LPS-induced septic shock. Cell Res. 2013;23(2):201–212. doi: 10.1038/cr.2013.6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 88.Mishra BB, Rathinam VAK, Martens GW, Martinot AJ, Kornfeld H, Fitzgerald KA, Sassetti CM. Nitric oxide controls the immunopathology of tuberculosis by inhibiting NLRP3 inflammasome-dependent processing of IL-1β. Nat Immunol. 2013;14(1):52–60. doi: 10.1038/ni.2474. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 89.Frech TM, Revelo MP, Drakos SG, Murtaugh MA, Markewitz BA, Sawitzke AD, Li DY. Vascular leak is a central feature in the pathogenesis of systemic sclerosis. J Rheumatol. 2012;39(7):1385–1391. doi: 10.3899/jrheum.111380. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Saketkoo LA, Distler O. Is there evidence for vasculitis in systemic sclerosis? Curr Rheumatol Rep. 2012;14(6):516–525. doi: 10.1007/s11926-012-0296-9. [DOI] [PubMed] [Google Scholar]
- 91.Pendergrass SA, Hayes E, Farina G, Lemaire R, Farber HW, Whitfield ML, Lafyatis R. Limited systemic sclerosis patients with pulmonary arterial hypertension show biomarkers of inflammation and vascular injury. PLoS One. 2010;5(8):e12106. doi: 10.1371/journal.pone.0012106. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 92.Hinz B, Lagares D. Evasion of apoptosis by myofibroblasts: a hallmark of fibrotic diseases. Nat Rev Rheumatol. 2020;16(1):11–31. doi: 10.1038/s41584-019-0324-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 93.Dziankowska-Bartkowiak B, Waszczykowska E, Zalewska A, Sysa-Jedrzejowska A. Evaluation of caspase 1 and sFas serum levels in patients with systemic sclerosis: correlation with lung dysfunction, joint and bone involvement. Mediat Inflamm. 2003;12(6):339–343. doi: 10.1080/09629350310001633379. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 94.Hayashi N, Yoshimoto T, Izuhara K, Matsui K, Tanaka T, Nakanishi K. T helper 1 cells stimulated with ovalbumin and IL-18 induce airway hyperresponsiveness and lung fibrosis by IFN-gamma and IL-13 production. Proc Natl Acad Sci U S A. 2007;104(37):14765–14770. doi: 10.1073/pnas.0706378104. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 95.Zhang Y, Li P, Li G, Huang X, Meng Q, Lau WY, Wang X. The mechanism of how anti-IL-18 prevents concanavalin-A-induced hepatic fibrosis on a mouse model. J Surg Res. 2007;142(1):175–183. doi: 10.1016/j.jss.2007.01.024. [DOI] [PubMed] [Google Scholar]
- 96.Gentile D, Lazzerini PE, Gamberucci A, Natale M, Selvi E, Vanni F, Alì A, Taddeucci P, Del-Ry S, Cabiati M, et al. Searching novel therapeutic targets for scleroderma: P2X7-receptor is up-regulated and promotes a fibrogenic phenotype in systemic sclerosis fibroblasts. Front Pharmacol. 2017;8:638. doi: 10.3389/fphar.2017.00638. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 97.Henry TW, Mendoza FA, Jimenez SA. Role of microRNA in the pathogenesis of systemic sclerosis tissue fibrosis and vasculopathy. Autoimmun Rev. 2019;18(11):102396. doi: 10.1016/j.autrev.2019.102396. [DOI] [PubMed] [Google Scholar]
- 98.Christmann RB, Wooten A, Sampaio-Barros P, Borges CL, Carvalho CRR, Kairalla RA, Feghali-Bostwick C, Ziemek J, Mei Y, Goummih S, et al. miR-155 in the progression of lung fibrosis in systemic sclerosis. Arthritis Res Ther. 2016;18(1):155. doi: 10.1186/s13075-016-1054-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 99.Artlett CM, Sassi-Gaha S, Hope JL, Feghali-Bostwick CA, Katsikis PD. Mir-155 is overexpressed in systemic sclerosis fibroblasts and is required for NLRP3 inflammasome-mediated collagen synthesis during fibrosis. Arthritis Res Ther. 2017;19(1):144. doi: 10.1186/s13075-017-1331-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 100.Lóránd V, Czirják L, Minier T. Musculoskeletal involvement in systemic sclerosis. Presse Med. 2014;43(10 Pt 2):e315–e328. doi: 10.1016/j.lpm.2014.03.027. [DOI] [PubMed] [Google Scholar]
- 101.Bassel M, Hudson M, Taillefer SS, Schieir O, Baron M, Thombs BD. Frequency and impact of symptoms experienced by patients with systemic sclerosis: results from a Canadian National Survey. Rheumatology (Oxford) 2011;50(4):762–767. doi: 10.1093/rheumatology/keq310. [DOI] [PubMed] [Google Scholar]
- 102.Tuffanelli DL, Winkelmann RK. Systemic scleroderma, a clinical study of 727 cases. Arch Dermatol. 1961;84:359–371. doi: 10.1001/archderm.1961.01580150005001. [DOI] [PubMed] [Google Scholar]
- 103.Avouac J, Walker U, Tyndall A, Kahan A, Matucci-Cerinic M, Allanore Y, Miniati I, Muller A, Iannone F, Distler O, et al. Characteristics of joint involvement and relationships with systemic inflammation in systemic sclerosis: results from the EULAR Scleroderma Trial and Research Group (EUSTAR) database. J Rheumatol. 2010;37(7):1488–1501. doi: 10.3899/jrheum.091165. [DOI] [PubMed] [Google Scholar]
- 104.Vande Walle L, Van Opdenbosch N, Jacques P, Fossoul A, Verheugen E, Vogel P, Beyaert R, Elewaut D, Kanneganti T-D, van Loo G, et al. Negative regulation of the NLRP3 inflammasome by A20 protects against arthritis. Nature. 2014;512(7512):69–73. doi: 10.1038/nature13322. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 105.Thankam FG, Roesch ZK, Dilisio MF, Radwan MM, Kovilam A, Gross RM, Agrawal DK. Association of inflammatory responses and ECM disorganization with HMGB1 upregulation and NLRP3 inflammasome activation in the injured rotator cuff tendon. Sci Rep. 2018;8(1):8918. doi: 10.1038/s41598-018-27250-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 106.Mackiewicz Z, Hukkanen M, Povilenaite D, Sukura A, Fonseca JE, Virtanen I, Konttinen YT. Dual effects of caspase-1, interleukin-1 beta, tumour necrosis factor-alpha and nerve growth factor receptor in inflammatory myopathies. Clin Exp Rheumatol. 2003;21(1):41–48. [PubMed] [Google Scholar]
- 107.Coll RC, Robertson AAB, Chae JJ, Higgins SC, Muñoz-Planillo R, Inserra MC, Vetter I, Dungan LS, Monks BG, Stutz A, et al. A small-molecule inhibitor of the NLRP3 inflammasome for the treatment of inflammatory diseases. Nat Med. 2015;21(3):248–255. doi: 10.1038/nm.3806. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 108.Primiano MJ, Lefker BA, Bowman MR, Bree AG, Hubeau C, Bonin PD, Mangan M, Dower K, Monks BG, Cushing L, et al. Efficacy and pharmacology of the NLRP3 inflammasome inhibitor CP-456,773 (CRID3) in murine models of dermal and pulmonary inflammation. J Immunol. 2016;197(6):2421–2433. doi: 10.4049/jimmunol.1600035. [DOI] [PubMed] [Google Scholar]
- 109.Van Hauwermeiren F, Lamkanfi M. The NEK-sus of the NLRP3 inflammasome. Nat Immunol. 2016;17(3):223–224. doi: 10.1038/ni.3391. [DOI] [PubMed] [Google Scholar]
- 110.Perera AP, Fernando R, Shinde T, Gundamaraju R, Southam B, Sohal SS, Robertson AAB, Schroder K, Kunde D, Eri R. MCC950, a specific small molecule inhibitor of NLRP3 inflammasome attenuates colonic inflammation in spontaneous colitis mice. Sci Rep. 2018;8(1):8618. doi: 10.1038/s41598-018-26775-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 111.Hindman B, Ma Q. Carbon nanotubes and crystalline silica stimulate robust ROS production, inflammasome activation, and IL-1β secretion in macrophages to induce myofibroblast transformation. Arch Toxicol. 2019;93(4):887–907. doi: 10.1007/s00204-019-02411-y. [DOI] [PubMed] [Google Scholar]
- 112.Mridha AR, Wree A, Robertson AAB, Yeh MM, Johnson CD, Van Rooyen DM, Haczeyni F, Teoh NCH, Savard C, Ioannou GN, et al. NLRP3 inflammasome blockade reduces liver inflammation and fibrosis in experimental NASH in mice. J Hepatol. 2017;66(5):1037–1046. doi: 10.1016/j.jhep.2017.01.022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 113.Gao R, Shi H, Chang S, Gao Y, Li X, Lv C, Yang H, Xiang H, Yang J, Xu L, et al. The selective NLRP3-inflammasome inhibitor MCC950 reduces myocardial fibrosis and improves cardiac remodeling in a mouse model of myocardial infarction. Int Immunopharmacol. 2019;74:105575. doi: 10.1016/j.intimp.2019.04.022. [DOI] [PubMed] [Google Scholar]
- 114.Krishnan SM, Ling YH, Huuskes BM, Ferens DM, Saini N, Chan CT, Diep H, Kett MM, Samuel CS, Kemp-Harper BK, et al. Pharmacological inhibition of the NLRP3 inflammasome reduces blood pressure, renal damage, and dysfunction in salt-sensitive hypertension. Cardiovasc Res. 2019;115(4):776–787. doi: 10.1093/cvr/cvy252. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 115.Mangan MSJ, Olhava EJ, Roush WR, Seidel HM, Glick GD, Latz E. Targeting the NLRP3 inflammasome in inflammatory diseases. Nat Rev Drug Discov. 2018;17(8):588–606. doi: 10.1038/nrd.2018.97. [DOI] [PubMed] [Google Scholar]
- 116.Jiang H, He H, Chen Y, Huang W, Cheng J, Ye J, Wang A, Tao J, Wang C, Liu Q, et al. Identification of a selective and direct NLRP3 inhibitor to treat inflammatory disorders. J Exp Med. 2017;214(11):3219–3238. doi: 10.1084/jem.20171419. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 117.Gao R-F, Li X, Xiang H-Y, Yang H, Lv C-Y, Sun X-L, Chen H-Z, Gao Y, Yang J-S, Luo W, et al. The covalent NLRP3-inflammasome inhibitor Oridonin relieves myocardial infarction induced myocardial fibrosis and cardiac remodeling in mice. Int Immunopharmacol. 2021;90:107133. doi: 10.1016/j.intimp.2020.107133. [DOI] [PubMed] [Google Scholar]
- 118.Liu S-S, Lv X-X, Liu C, Qi J, Li Y-X, Wei X-P, et al. Targeting degradation of the transcription factor C/EBPβ reduces lung fibrosis by restoring activity of the ubiquitin-editing enzyme A20 in macrophages. Immunity. 2019;51(3):522–534. doi: 10.1016/j.immuni.2019.06.014. [DOI] [PubMed] [Google Scholar]
- 119.Youm Y-H, Nguyen KY, Grant RW, Goldberg EL, Bodogai M, Kim D, D'Agostino D, Planavsky N, Lupfer C, Kanneganti TD, et al. The ketone metabolite β-hydroxybutyrate blocks NLRP3 inflammasome-mediated inflammatory disease. Nat Med. 2015;21(3):263–269. doi: 10.1038/nm.3804. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 120.Zakrzewska K, Arvia R, Torcia MG, Clemente AM, Tanturli M, Castronovo G, et al. Effects of parvovirus B19 in vitro infection on monocytes from patients with systemic sclerosis: enhanced inflammatory pathways by caspase-1 activation and cytokine production. J Investigative Dermatol. 2019;139(10):2125–2133. doi: 10.1016/j.jid.2019.03.1144. [DOI] [PubMed] [Google Scholar]
- 121.Gasse P, Mary C, Guenon I, Noulin N, Charron S, Schnyder-Candrian S, Schnyder B, Akira S, Quesniaux VFJ, Lagente V, et al. IL-1R1/MyD88 signaling and the inflammasome are essential in pulmonary inflammation and fibrosis in mice. J Clin Invest. 2007;117(12):3786–3799. doi: 10.1172/JCI32285. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 122.Ikonomidis I, Lekakis JP, Nikolaou M, Paraskevaidis I, Andreadou I, Kaplanoglou T, Katsimbri P, Skarantavos G, Soucacos PN, Kremastinos DT. Inhibition of interleukin-1 by anakinra improves vascular and left ventricular function in patients with rheumatoid arthritis. Circulation. 2008;117(20):2662–2669. doi: 10.1161/CIRCULATIONAHA.107.731877. [DOI] [PubMed] [Google Scholar]
- 123.Tate MD, Ong JDH, Dowling JK, McAuley JL, Robertson AB, Latz E, Drummond GR, Cooper MA, Hertzog PJ, Mansell A. Reassessing the role of the NLRP3 inflammasome during pathogenic influenza A virus infection via temporal inhibition. Sci Rep. 2016;6:27912. doi: 10.1038/srep27912. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 124.Kullenberg T, Löfqvist M, Leinonen M, Goldbach-Mansky R, Olivecrona H. Long-term safety profile of anakinra in patients with severe cryopyrin-associated periodic syndromes. Rheumatology (Oxford) 2016;55(8):1499–1506. doi: 10.1093/rheumatology/kew208. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
All data are available from the corresponding author.