Abstract
Objective
This study aimed at exploring the perspectives and experiences of individuals with neck pain by synthesizing all available qualitative studies.
Methods
A systematic, qualitative meta-summary and meta-synthesis was conducted following the 5-step methodology proposed by Sandelowski and Barroso. A systematic search of 9 electronic databases was conducted in May 2021. Methodological quality was assessed using the Critical Appraisal Skills Programme tool.
Results
Nine studies were included in the meta-synthesis for a total of 103 participants (73 women). Eleven categories were identified as belonging to 3 main themes: physical (“My neck has gone wrong”); psychological (“I am worried about my recovery”); and social (“Pain limits my life”). In the physical theme, the categories with the highest frequency were symptoms (67%) followed by body perception (44%). The psychological theme frequencies from highest to lowest were psychological consequences (100%), coping strategies (100%), mindset (67%), expectations from health care professionals (44%), and gender influence (22%). In the social theme, frequencies from highest to lowest were social relationships (56%), work, and activities of daily living and physical activity (44%, respectively).
Conclusion
An individual’s experience with neck pain is a multidimensional phenomenon in which physical, psychological, and social dimensions influence each other. These findings suggested that health care professionals should be aware of recognizing and evaluating all of the individual’s experiences to offer a truly patient-centered care pathway.
Impact
This qualitative meta-synthesis responded to a call to action to explore perspectives and experiences of individuals with neck pain. These findings can provide crucial guidance for clinicians as they plan and implement evidence-based recommendations for neck pain.
Keywords: Neck Pain, Qualitative, Rehabilitation
Introduction
Neck pain is defined as “pain located in the anatomic region of the neck, with or without radiation to the head, trunk, and upper limbs.”1 It represents a widespread and disabling condition with high prevalence and incidence worldwide.2 The impact of neck pain on individuals is high in terms of pain, disability, and socioeconomic and health management implications, in addition to important psychological implications due to its multifactorial nature.3,4 Thus, there is the need to go beyond the impact of neck pain on the impairments of body and function,5 and to consider the individual’s lived experience (eg, beliefs, expectations, needs) as a fundamental element of the care process.1,6–8
This transition represents an opportunity to reduce the distance between patients and health care professionals and to shift toward a more patient-centered approach.9 Within this context, the narrative synthesis of qualitative data allows for a deeper understanding of the individual’s lived experiences, providing the necessary information to foster this shift in perspective.1,10 Despite this, some scholars have reservations about the value of many of the available methodological approaches (eg, aggregated, interpretative).11,12 These reservations arise from the difficulty of combining and generalizing findings derived from heavily context-dependent studies, and the subjective nature of the interpretation process exposed to the researcher’s epistemological assumptions.13 The systematic review of qualitative studies with meta-summary and meta-synthesis offers a possible solution to these problems by implementing a more rigorous and systematic approach to collect, analyze, interpret, and organize qualitative data, thus allowing for informing practices and guiding decision-making.14
In recent years, several systematic reviews of qualitative studies have analyzed the participant’s experience in different musculoskeletal disorders such as shoulder pain,15 chronic low back pain,16,17 hip and/or knee osteoarthritis,18–20 and chronic pelvic pain,21 and across different conditions.22 However, to the best of our knowledge, a similar investigation focusing on neck pain has not been published to date. Therefore, we aim to identify the individual’s perspective and experience by performing a systematic review with meta-summary and meta-synthesis of all available qualitative studies involving individuals with neck pain.
Methods
Design
We conducted a systematic, qualitative meta-summary (quantitative summation of qualitative research findings) and meta-synthesis (integration of the qualitative findings through a new interpretation of findings) using Sandelowski and Barroso’s methodology.14
The study process has 5 basic steps: (1) develop the research question, (2) search and systematically extract studies to be analyzed, (3) appraise the quality of the included studies, (4) classify the studies, and (5) synthesize data through meta-summary and meta-synthesis.14
The research protocol was registered in the Open Science Framework Registries Database (doi.org/10.17605/OSF.IO/XTF7P) on November 20, 2020. The reporting of this systematic review was developed according to Enhance Transparency in Reporting The Synthesis of Qualitative Research,23 Preferred Reporting Items for Systematic reviews and Meta-Analyses statements,24–26 and the Qualitative Meta-Analysis Article Reporting Standards Information Recommended for Inclusion in Manuscripts Reporting Qualitative Meta-Analyses.27
Data Sources and Searches
Two authors (Z.L., G.R.) independently conducted a systematic search in the following 9 databases: Cumulative Index to Nursing and Allied Health Literature, Cochrane Library, Embase, PEDro, PsycINFO, MEDLINE, Scopus, Sportdiscus, and Web of Science. The last search was performed on May 16, 2021.
All the entry terms have been identified and organized according to the Sample, Phenomenon of Interest, Design, Evaluation, Research type approach28 for qualitative research:
S (sample): adult participants;
PI (phenomenon of interest): neck pain, cervicodynia, cervical pain, neck ache;
D (design): interview, discussion, observational, focus groups, narration, semistructured, structured, informal, in-depth, face-to-face, narrative accounts;
E (evaluation): viewpoint, experience, opinion, attitude, perception, beliefs, feelings, knowledge, behavior, understanding, perspective, involvement, engagement, first-person perspectives, feedback, quality of life, health-related quality-of-life, psychosocial, psychological, emotions, mental outlook, needs, living with, coping with, self-understanding, well-being, health status, patient-reported outcomes, patient-centered care, health care, barriers and enablers;
R (research type): qualitative, mixed-method, methodology, research, synthesis, approaches.
In addition, we used a “berry-picking” method14 to ensure a comprehensive search of studies that met our inclusion criteria, including footnote chasing, citation searching, hand searching, journal run, author searching, and fugitive literature (eg, masters theses and doctoral dissertations). The detailed search strategies for each database are reported in Supplementary Table 1.
Study Selection
The inclusion criteria adopted were qualitative primary studies published in English that involved adults (18–75 years of age) and considered the participant’s experience with a diagnosis of neck pain irrespective of phase (eg, acute, sub-acute, chronic), intervention (eg, manual therapy, therapeutic exercise, modalities) and time of publication. The exclusion criteria were (1) quantitative studies (eg, prospective studies, case studies, case reports), (2) mixed-methods studies with no clear identification of participants and findings from the qualitative methods, (3) studies conducted on participants with specific pathologies (eg, tumors, spondylolysis; fractures, cervical myelopathy) or traumatic origin (eg, whiplash, concussion), and (4) studies including young (<18 years of age) or elderly (>75 years of age) participants.
Three authors (Z.L., G.R., L.F.M.) independently reviewed the studies. All duplicates were removed after identifying the records in the databases. Titles and abstracts of the selected records were screened, and the full text of the eligible records was assessed according to the inclusion criteria. Any disagreement was resolved by consensus with the research group.
Data Extraction and Quality Assessment
Data from included studies were independently extracted by 2 authors (Z.L., G.R.) and organized in an ad-hoc synoptic table, including year of publication, country (setting), diagnosis, aim, participants, data collection, data analysis, and the qualitative findings summarizing the participant’s experience (see Tab. 1).
Table 1.
Characteristics of the Included Studiesa
| Study | Country (Setting) | Diagnosis | Aim | Participants | Data Collection | Data Analysis | Declared Themes of Patients’ Experience |
|---|---|---|---|---|---|---|---|
| Ahlsen et al43 (2012a) | Norway | Chronic NP | To examine how men present themselves as patients with chronic pain and how men’s subjective experience of pain interplays with dominant norms of masculinity | n = 10 M/F = 10/0 Age = 28–47 y | Qualitative interview | Narrative method, combined with a gender-sensitive perspective | Physical damage Working difficulties Troubled private affairs Personal suffering |
| Ahlsen et al44 (2012b) | Norway | Chronic NP | To find out more about men’s experiences living with chronic NP and being in treatment | n = 10 M/F = 10/0 Age = 28–47 y | Qualitative interview | Narrative method combined with gender-sensitive perspective | Rebuilding a self Being comforted Being connected |
| Cramer et al41 (2013) | Germany | Chronic nonspecific NP | To investigate the perceived influence of yoga on body awareness and the psychosocial aspects of life for people with chronic NP | n = 18 M/F = 3/15 Age = 19–59 y | Body drawings Semistandardized interviews | Content analysis techniques | Physical dimension Cognitive dimension Emotional dimension Behavioral dimension Social dimension |
| Holmberg et al45 (2016) | Germany | Unspecific chronic NP | To understand how mind–body therapies and exercise therapy may influence the experience of pain among people with chronic NP | n = 20 M/F = 4/16 Age = 29–59 y | Semistructured interviews | Grounded theory | Experiencing NP Intervention experiences in Qigong study arm Intervention experiences in exercise therapy study arm |
| Langenfeld et al40 (2018) | Switzerland | NP | To evaluate the association between objective and subjective cervical range of motion among people with NP and assess awareness of impairments | n = 10 (9 chronic, 1 acute) M/F = 4/6 Age = 23–77 y | Semistructured interviews | Content analysis techniques | Reason for seeing physical therapist ADL restrictions due to NP General description of problem Perception on head movement Subjective impression of movement restriction ADL limitations due to movement restrictions |
| Lauche et al42 (2012) | Germany | Chronic nonspecific NP | To explore body image and its influence on everyday life in people with chronic NP, influence of cupping therapy on people with chronic NP, and to better understand the relationship between chronic pain and body image | n = 6 M/F = 2/4 Age = 52–62 y | Body image drawings and semistructured interviews | Content analysis techniques | Perception of body and pain Handling pain Changes after cupping therapy |
| MacDermid et al46 (2013) | Canada Australia | Chronic or recurrent NP with or without associated arm/shoulder pain | To describe the experience of receiving health care for NP and to determine the meaning of that experience for people living with NP | n = 19 M/F = 1/18 Age = 20–69 y | Semistructured interview | Coding of text (modified Stevick-Colaizzi-Keen) | Complexity in finding effective health care Need for informative, personalized, respectful communication |
| MacDermid et al47 (2016) | Canada | Chronic or recurrent NP with or without associated arm/shoulder pain | To describe quality, distribution, and behavior of NP; to describe pain experiences of people with nonspecific NP using qualitative descriptive approach | n = 16 M/F = 1/15 Age = 20–69 y | Semistructured interview Electronic descriptive pain tool | Descriptive content analysis | Anatomic distribution of pain Quality and intensity of pain Behavior of pain Mediators of pain Impact on activity |
| Schrer et al39 (2010) | Germany | NP | To investigate perspectives and expectations of people presenting with NP in clinical practice | n = 20 M/F = 6/14 Age = 20–78 y | Semistructured telephone interviews | Grounded theory using thematic framework approach | Communication of individual and clinician about reason for encounter People’s competencies Clinician–patient situation from patients’ perspective Experiences with therapeutic options |
ADL = activities of daily living; CNP = chronic neck pain; F = female; GPE = global perceived effect; M = male; NP = neck pain; RTW = return to work.
The qualitative findings of the participants’ experience were classified as thematic surveys, conceptual/thematic descriptions, and interpretative explanations, considering the different degree of data transformation of findings.29 Any disagreement was resolved by consensus within the research group.
We used the Critical Appraisal Skills Programme (CASP) tool,30 commonly applied in qualitative health reviews31 as suggested by the Cochrane Collaboration,32,33 to assess the rigor, credibility, and relevance of the evidence produced14 and discuss any methodological issues that arose.34 According to Sandelowski and Barroso’s advice, low quality was not an exclusion criterion but a step to improve the rigor of our systematic review.14,35,36 CASP is composed of 10 items30 that address (1) study aim(s), (2) appropriateness of qualitative methodology, (3) research design, (4) recruitment strategy, (5) data collection, (6) researcher and participant relationship (researcher reflexivity), (7) research ethics, (8) data analysis, (9) findings, and (10) contribution to knowledge. For items 1 to 9, the scoring system considers 3 values based on whether the topic is: well described in the article (Y: yes), completely not described (N: no), or unclear lacking details (CT: cannot tell); the item number 10 is based on an open-ended question about the importance of the study (eg, valuable or not valuable).30 Two authors (L.F.M, G.R.) independently assessed each study; any disagreements were resolved by consensus with the research group.14
Data Synthesis and Analysis
All of the following steps planned for the synthesis process were performed simultaneously rather than sequentially14 by 3 independent authors (Z.L., G.R., L.M.): (1) identify the topic through multiple readings and line-by-line review of studies; (2) extract the target findings of each study and eliminate irrelevant data; (3) edit the findings to ensure the original wording is captured to preserve the authors’ intention(s); (4) group similar findings by topic to establish, when compared, if findings across studies are related to each other; (5) abstract the grouped findings by eliminating redundancies, refining statements, and preserving contradictions and ambiguities; (6) generate categories and themes from the final findings by means of a 2-method cycle coding: first an inductive analysis procedure and then by axial coding37; and (7) evaluate the findings for similarities and differences within and between studies and synthetize using a constant target comparison.
We then proceeded with the estimation of (1) the manifest interstudy frequency effect size, for example, prevalence rate of findings; calculated as ([number of studies containing a finding/total number of studies] × 100); and (2) the intrastudy intensity effect size, for example, concentration of findings in each report; calculated as ([number of findings in the study/total number of findings] × 100).38
Any disagreements were resolved by consensus and consultation with the overall research group. The detailed meta-synthesis process is reported in Supplementary Table 2.
We ensured the trustworthiness and rigor of this meta-synthesis and meta-summary combining multiple strategies14 by (1) adopting a multidisciplinary research group of clinicians (physical therapists, nurses) and scholars (researchers, methodologists) from different backgrounds, (2) using a systematic search approach for literature, (3) involving multiple researchers in each of the stages of the review, (4) holding regular meetings to plan and discuss emergent themes and challenges, and (5) keeping an audit trail to extensively document the research team’s process and outputs. Furthermore, the active participation of each member of the group allowed each decision to be discussed and negotiated using a “think-aloud” strategy and discrepancies were resolved through consensus.14 All the implemented strategies are summarized in Supplementary Table 3.
Difference Between Protocol and Review
We included 2 studies39,40 in which the participant age range exceeded the definition of adult established in our Open Science Framework Registries Database protocol (18–77 years of age and 18–78 years instead of 18–75 years). We agreed there was no clinical reason to exclude these studies; therefore, we expanded the inclusion criterion to age 80 years to be more comprehensive.
Results
Studies Included
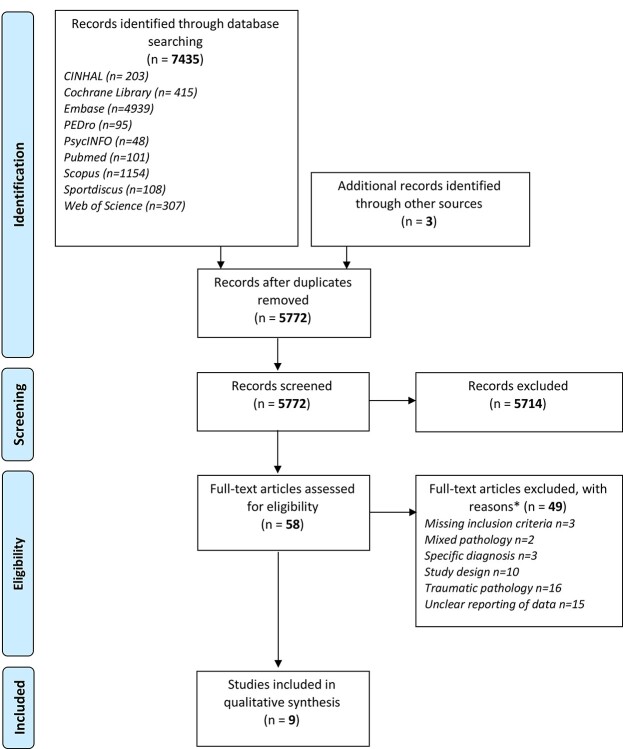
The initial search produced a total of 7438 records (5772 after duplicate removal). After title and abstract reading, 5714 records were excluded and 58 underwent the eligibility process.
After reading the full textsw, 49 studies were excluded for different reasons (see Suppl. Tab. 4), and a total of 9 studies were included39–47 (see Fig. 1). Of these, 4 originated from 2 cohorts of participants: that of McDermid et al46,47 and that of Ahlsen et al.43,44
Figure 1.
Study selection flow diagram. (see Suppl. Tab. 2 for details and rationale for the excluded studies).
Characteristics of the Studies
A total of 103 participants (73 females) with a nonspecific neck pain diagnosis were included in the studies. In 2 studies,46,47 35 participants presented chronic or recurrent neck pain as a principal symptom with or without associated arm/shoulder pain. The participants’ ages ranged from 18 to 78 years; the median number of participants included in the studies was 16, ranging from 642 to 20.39,45 Two studies included only male participants,43,44 whereas in the others the majority were female.39–42,45–47
Seven studies were conducted in Europe: 4 in Germany,39,41,42,45 1 in Switzerland,40 and 2 in Norway.43,44 Two studies were conducted in Canada and Australia.46,47 The included studies were categorized as thematic surveys,40 conceptual/thematic description,39,41,42,45–47 and interpretive explanations.43,44 The characteristics of the 9 included studies are summarized in Table 1.
Quality Appraisal of the Included Studies
Items 1, 2, and 3 were evaluated as “yes” in all studies.39–47 Items 4 and 5 were reported, respectively, as “cannot tell” in 1 study42 and 6 studies.40–44,47 Item 6 was rated as “no” in 6 studies.39–42,46,47 Item 7 obtained a score as “cannot tell” in 4 studies39,40,43,45 and “no” in 2 studies.44,47 Items 8 and 9 were judged as “cannot tell” in 3 studies.40,43,44 Finally, the research group rated item 10 as valuable in all studies.39–47 The detailed quality appraisal and the CASP score are reported in Table 2.
Table 2.
Quality Appraisal of the Included Studies Using the CASPa
| Ahlsen et al 43 (2012a) | Ahlsen et al 44 (2012b) | Cramer et al 41 (2016) | Holmberg et al 45 (2016) | Langenfeld et al 40 (2018) | Lauche et al 42 (2012) | MacDermid et al 47 (2016) | MacDermid et al 46 (2013) | Schrer et al 39 (2010) | |
|---|---|---|---|---|---|---|---|---|---|
| Item 1. Was there a clear statement of the aims of the research? | Y | Y | Y | Y | Y | Y | Y | Y | Y |
| Item 2. Is a qualitative methodology appropriate? | Y | Y | Y | Y | Y | Y | Y | Y | Y |
| Item 3. Was the research design appropriate to address the aims of the research? | Y | Y | Y | Y | Y | Y | Y | Y | Y |
| Item 4. Was the recruitment strategy appropriate to the aims of the research? | Y | Y | Y | Y | Y | CT | Y | Y | Y |
| Item 5. Were the data collected in a way that addressed the research issue? | CT | CT | CT | Y | CT | CT | CT | Y | Y |
| Item 6. Has the relationship between researcher and participants been adequately considered? | Y | Y | N | Y | N | N | N | N | N |
| Item 7. Have ethical issues been taken into consideration? | CT | N | Y | CT | CT | Y | Y | N | CT |
| Item 8. Was the data analysis sufficiently rigorous? | CT | CT | Y | Y | CT | Y | Y | Y | Y |
| Item 9. Is there a clear statement of findings? | CT | CT | Y | Y | CT | Y | Y | Y | Y |
| Item 10. How valuable is the research? | Val | Val | Val | Val | Val | Val | Val | Val | Val |
Data evaluated using the Critical Appraisal Skills Programme (CASP).30 CT = cannot tell; N = no; Val = valuable; Y = yes.
Meta-Summary and Meta-Synthesis Outcomes
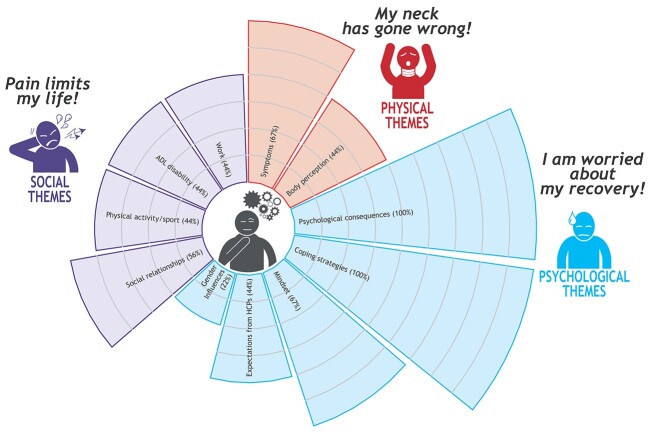
A total of 252 target findings were extracted, modified, grouped, abstracted, and summarized in 196 final declarations. The first cycle of the encoding method outlined 209 codes. After the second cycle, the codes were reduced to 157 and condensed into 11 categories that were summarized into 3 main themes: (1) “My neck has gone wrong” (physical dimension), (2) “I am worried about my recovery” (psychological dimension), and (3) “Pain limits my life” (social dimension) (see Fig. 2). The categories with the highest-frequency effect size among studies were: psychological consequences (100%), coping strategies (100%), mindset (67%), and symptoms (67%), whereas the lowest frequency was documented by gender influence (22%). The greatest intrastudy intensity was reported by Holmberg et al and Ahlsen et al (73%)43,45 followed by Langenfeld et al and by Ahlsen et al (64%)40,44 (see Tab. 3).
Figure 2.
Themes of participants’ experiences with neck pain. Each sector represents a participant experience theme. The color of the sector indicates the category to which it belongs: physical (red), psychological (blue), or social (dark blue). In addition, the sector arches indicate the number of studies dealing with the theme (eg, in the theme “gender influences,” the 2-sector arches indicate that 2 of the 9 included studies dealt with that theme, for a total of 22%). ADL = activities of daily living; HCPs = health care professionals.
Table 3.
Meta-Summarya
| Themes/Dimension | Categories | Authors | Interstudy Frequency Effect Sizes | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Ahlsen et al43 (2012a) | Ahlsen et al44 (2012b) | Cramer et al41 (2016) | Holmberg et al45 (2016) | Langenfeld et al40 (2018) | Lauche et al42 (2012) | MacDermid et al47 (2016) | MacDermid et al46 (2013) | Schrer et al39 (2010) | |||
| My neck has gone wrong | Symptoms | √ | – | – | √ | √ | √ | – | √ | √ | 67 |
| Physical dimension | Body perception | √ | – | – | √ | √ | √ | – | – | – | 44 |
| I am worried about my recovery | Psychological consequences | √ | √ | √ | √ | √ | √ | √ | √ | √ | 100 |
| Psychological dimension | Coping strategies | √ | √ | √ | √ | √ | √ | √ | √ | √ | 100 |
| Mindset | √ | √ | – | √ | – | √ | √ | √ | – | 67 | |
| Gender influence | √ | √ | – | – | – | – | – | – | – | 22 | |
| Expectations from health care professionals | – | √ | – | – | – | √ | √ | – | √ | 44 | |
| Pain limits my life | Work | √ | √ | – | √ | √ | – | – | – | – | 44 |
| Social dimension | ADL disability | – | – | √ | √ | √ | – | – | √ | – | 44 |
| Physical activity/ sport | – | – | √ | – | √ | – | √ | – | √ | 44 | |
| Social relationships | √ | √ | √ | √ | – | – | – | – | √ | 56 | |
| Intrastudy intensity effect sizes | 73 | 64 | 45 | 73 | 64 | 55 | 45 | 45 | 55 | ||
Interstudy frequency effect size = ([number of studies containing a finding/total number of studies] × 100); intrastudy intensity effect size = ([number of findings in the study/total number of findings] × 100). ADL = activities of daily living.
Theme 1: “My Neck Has Gone Wrong”
Symptoms
The most commonly experienced symptom was persistent neck pain,40,42,43,45,47 varying in terms of intensity and quality and often described as a mixed type.47
Participants never complained of neck pain as their isolated symptom; rather, they considered neck pain to be the cause of many other symptoms and diseases. For example, the pain was also referred to the shoulders, arms,40,43,47 and, more rarely, to the upper back.47 Other frequently experienced symptoms were stiffness, tightness, and blockage in the neck, which caused difficulty moving39,40,45 and increased pain, presenting an obstacle to normal function.42 The participants also experienced different headaches in terms of duration and location43,45,47 as well as intensity.43 Headaches could become very intense, mimicking a migraine attack, which was the most annoying symptom.45 Pain was also associated with dizziness, visual disturbances, tinnitus,40,45 nausea, jaw pain,40 joint “click” and “popping” sounds during neck movement,40,47 as well as sleep disturbances.45
Body Perception
Pain sometimes changed the body perception of participants.42,43 Both the neck and shoulders were perceived to be altered in their shape, function,43 and position.42 The execution of neck movements was sometimes reported as unnatural, limited, or distorted in proportion40; participants struggled to focus attention on non-painful areas.42
Theme 2: “I’m Worried About My Recovery”
Psychological Consequences
Neck pain negatively influenced some psychological aspects of participants’ experience, resulting in frailty and emotional suffering. Participants reported feelings of discouragement, hopelessness, helplessness, distress, frustration, and anger caused by pain-induced disability42–46 and difficulty in accessing appropriate care services or treatments.46 Participants were afraid of movement because they thought it could potentially worsen their neck pain41,42; nevertheless, participating in various activities seemed to reinforce the hope of finding a solution to one’s problem.44 Some cognitive functions, such as concentration, memory, and thinking, were impaired by lack of sleep and the negative effects of medication.40,46 Mood was also affected, with feelings of irritability, strangeness, and betrayal.45 Participants often felt “controlled” by the pain that became a burden.42,45 Overall, participants avoided talking openly about pain in order not to reinforce it and avoid being stigmatized as neurotic.39
Coping Strategies
Participants adopted several coping strategies aimed at improving their efficiency to fully complete their daily duties.42,44 Many participants changed their lifestyle, behavior (postural adaptations or relaxation techniques), or external environment, modifying, for example, their work context or their job. In general, they preferred to self-manage their health39,40,45–47 and turned to external professional help only when their strategies failed.39,45 In contrast, some ignored the pain, using endurance strategies to fulfill daily tasks even when their symptoms worsened.41,42 Some also sought distractions42 or resorted to excessive use of painkiller medications44 to avoid feeling overwhelmed by the pain.
Mindset
Participants expressed a common need to receive specific and concrete health care explanations44 that described the origin of neck pain. They needed information about how to relieve pain and what the best available treatments were; they also wanted to know what behaviors should be adopted and avoided.46
During their care process, participants needed to feel understood, respected, and closely followed, with constant monitoring and feedback.44,46
Participants believed that the pain was caused by increased tension in the neck45 due to heavy daily or work activities, poor posture, or mental stressful conditions.43,47 For some participants, the pain seemed something “alien,” not coming from their own body, which consequently made it difficult to control.42
Participants believed that their symptoms could be worsened by ineffective treatments; even if they did not know if this worsening was caused by the interventions offered by the health service or some other factors, this condition led participants to believe that the health care provider was responsible.46 Participants also preferred “challenging” treatments (eg, exercises that are more difficult to perform) that were perceived as more effective in the long term.46 Although these exercises were positively perceived, it was more difficult for participants to remain compliant.
In general, medications were thought to be useful on occasion, but participants generally preferred to avoid them.46 Diagnostic examinations (x-rays or magnetic resonance imaging) were often counterproductive, causing frustration when, in the face of neck pain, the images showed no physical structural problems.46
Gender Influence
Two studies reported the experience of neck pain as different between males and females.43 Men tended to minimize the problem so as not to appear weak or lacking masculinity in their social role. Consequently, rehabilitation assumed great importance as it enabled, through the recovery of strength, an opportunity to “rebuild” oneself.44
Expectations From Health Care Professionals
Participants wanted to be closely followed by the professional and not abandoned and isolated within a treatment session (eg, when the practitioner, after assigning an exercise, leaves to assist another participant). The information provided by the professional had to be comprehensive, and treatments had to lead to long-term benefits.44,46 Participants expected their problems to be solved42 by competent health care professionals with whom a good therapeutic relationship was established.46
Professionals were judged positively when they were able to establish a positive therapeutic relationship by dedicating enough time to treatment, showing interest in the participant’s condition, and demonstrating knowledge and expertise.46 The practitioner also had to have good communication skills and empathy in addition to implementing effective therapeutic strategies that respected participants’ expectations and preferences, even when they were experimental or alternative treatments.39,46 In the absence of these conditions, many participants decided to change health care professionals.46
Other obstacles in the treatment process included long waiting lists, disagreements between the physical therapist and other clinicians, and “health system regulations” that imposed treatment prescriptions different from what the participants expected.39
Receiving a specific diagnosis was not always essential. In some cases, participants preferred to focus more on strategies for symptom resolution rather than on the etiology of their problem.39
Theme 3: “Pain Limits My Daily Life”
Work
Work was one of the activities most limited by neck pain. Due to physical impairment, many participants claimed that they were no longer able to work at full capacity40,43–45 and were forced into long periods of absence.44 Work was deemed harmful, and high levels of responsibility and stress were considered to be the cause of neck pain.43
Activity of Daily Living Disability
Many participants felt pain-disabled for both physical and emotional reasons.41 Instrumental daily activities commonly limited due to movement restrictions and concentration challenges were housework, driving, and some hobbies such as reading and using the computer.40,45 Participants also avoided activities that involved the use of neck and shoulder muscles, such as lifting and carrying weights, as they aggravated neck pain.47
Physical Activity and Sport
A complex relationship emerged between physical activity and neck pain.47 On the one hand, participants tended to avoid exercise for fear of triggering or worsening the pain39–41,47; on the other hand, they reported that without physical activity, the pain worsened. Participants also reported concern about reduced physical activity and the negative long-term health consequences.47 Ultimately, physical exercise was generally considered very challenging but effective in the long term.39,46
Social Relationships
Participants generally felt their social relationships were limited due to the unpredictable nature of the pain and fear of making it worse.41,43–45 Some participants experienced a real “social fall” with the loss of their role in society.44 The family assumed a dual role: in some cases, it was perceived as an additional burden to manage, whereas in others it represented a supportive context favoring well-being and relaxation.39 Sometimes participants reported they preferred not talking about their problem with family39 to avoid feeling stigmatized or humiliated44; however, there was also a strong need to feel socially connected.44
Discussion
Our systematic review of 9 qualitative studies offered a unique insight into the experience of participants with neck pain. We found that the experience of participants with neck pain could best be described as a multidimensional construct that permeates all dimensions of life among which the psychosocial aspects were the most represented as documented by the interstudy frequency effect size. Indeed, the most described categories were those in the psychological (n = 5) and social dimension (n = 4), whereas the physical dimension was less represented (n = 2).
As emerged in the first theme, participants reported negative experiences of neck pain that was perceived as intense, unpredictable, and disabling. Pain represented the overarching complaint capable of disrupting the participants’ bodies, as also emerged in other musculoskeletal15–21 and nonmusculoskeletal conditions.22 In addition, participants often reported other impairments (eg, stiffness, altered body perceptions) and associated disorders (eg, dizziness, visual disturbances), thus highlighting the complexity of living with neck pain. The variety of physical impairments associated with neck pain48 offers precious insights into the participants’ unique somatoperceptual experiences. Moreover, it stimulates clinicians to adopt physical therapy to promote discrimination between safe and threatening stimuli, thus helping participants at regaining a perceived sense of ownership over their bodies (eg, “This is my neck and I am in control of it”).49,50
As revealed in the second theme, participants reported that living with neck pain triggers a psychological burden, with nuances ranging from cognitive and emotional difficulties to loss of self-control. This thread echoes the subjective experience observed in other painful conditions,15–22 emphasizing the impact of suffering on the whole person. Participants also showed different levels of awareness of their neck pain: whereas some openly revealed expectations on their conditions and needs, others did not share their experience for fear of being stigmatized or considered socially inappropriate (eg, men as “weak and frail”). Moreover, participants with neck pain mentioned living suspended between their desire for autonomy in the management and their desire to be followed by health care providers. Overall, these findings inform clinicians of the need to guarantee a safe therapeutic encounter where participants can feel safe talking about their illness.51 This would help the participants to validate and legitimate their suffering and to shift their mindset toward a proactive approach,52,53 thus making sense of their condition.
In the third theme, we highlighted how neck pain worsens the participants’ lives, impacting their daily, sporting, and working activities. Dysfunctional beliefs (eg, “movement exacerbates neck pain”) and unhelpful behaviors (eg, excess vs avoidance of activities) often supported these difficulties, representing critical issues that clinicians should address with tailored educational interventions to improve treatment outcomes.54 Furthermore, the deprivation of social relationships for participants living with neck pain further worsened their disability, especially those experiencing a paucity of human connections and support from family relatives and friends. In this context of suffering, clinicians should help participants to increase their self-efficacy and develop appropriate coping strategies.55
However, despite their values, our findings should be critically analyzed in light of the methodological limitations of the included studies, considering that (1) two-thirds of the studies reported an unclear role of researchers that could potentially have biased the research question and unclear data collection, (2) one-third of the studies presented unclear data presentation, and (3) one-half of the included studies documented unclear ethical issues (Tab. 2). These limitations may have influenced the results of the included studies, ultimately influencing the quality of our metasynthesis.
Strength and Limitations
To our knowledge, this is the first qualitative systematic review to synthesize participants’ experience of neck pain in response to the “call to action” for research focused on individuals’ experience in physical therapy.8 We conducted an extensive literature search across 9 databases, including the berry-picking method and the quality assessment of the included studies. We limited the search to include only studies published in English. Thus, data not published in English as well as from grey literature may have been missed. Furthermore, the absence of studies reporting findings from other continents (eg, Africa, Asia) limits the generalizability of our results in contexts influenced by different cultures, socioeconomic conditions, and health care systems.56 As emerged, the intrastudy intensity effect sizes ranged from 45%41,46,47 to 73%,43,45 suggesting a substantial homogeneity across studies regarding the themes and categories. However, our study focused on the experiences of participants with neck pain,39–47 limiting the generalizability of our results to individuals with other cervical painful conditions (eg, radiculopathy, whiplash, myelopathy). Given the interpretive nature of the meta-synthesis process, the researchers’ experiences and background might have influenced the findings.31 However, we applied a methodological approach used by a multidisciplinary team of experts to address this potential bias, thereby improving the trustworthiness and rigor of the findings.14
Implications
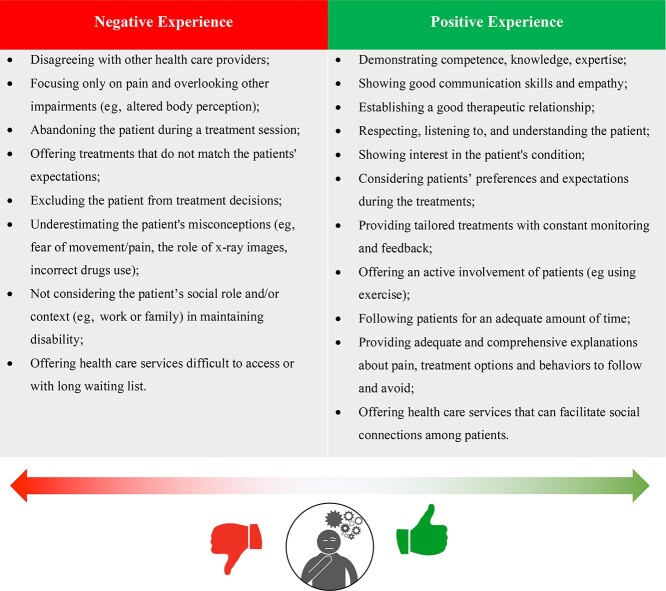
This systematic review offers implications at several levels. From a clinical perspective, our findings highlight the importance of implementing all dimensions of the individual’s experience within the neck pain care process (Fig. 3), in line with international guidelines on neck pain.48,57 Despite the uncertainty about how best to integrate the biopsychosocial model into clinical practice, psychologically informed physical therapy represents a promising strategy.58 Instead of focusing only on biomechanical and pathology-based perspectives, psychologically informed physical therapy merges physical impairment–based treatments (eg, manual therapy, therapeutic exercise) with cognitive-behavioral approaches (eg, motivational interview, reinforcement strategies), offering the opportunity to identify and address both biological and psychological impairments.59,60
Figure 3.
Elements of the neck pain care process and their influence on the participants’ experience.
From an educational perspective, our findings inform the need for tailored training on biopsychosocial dimensions at both undergraduate and postgraduate levels. Several systematic reviews highlighted how physical therapists feel inadequately trained and insecure in managing psychosocial impairments.61,62 This lack of training together with other barriers (eg, time constraints and concerns about professional boundaries) induces a nonstandardized use of psychosocial skills,63 which may lead to inadequate management of these impairments. Although different training methods exist (eg, didactic and experiential learning), there is no consensus on which is the most effective to train a learner’s psychosocial skills.64 Thus, we suggest continuing research on the training of psychosocial skills by enhancing attention to address the individual’s experience in musculoskeletal pain.
From a research perspective, our findings suggest the need for more thorough integration of the individual’s experience into future research on neck pain. Currently, the involvement of participants in health research is encouraged worldwide.65 Accordingly, individuals’ experience could inform future quantitative research on neck pain (eg, randomized-controlled trials)66 by identifying research priorities and individuals’ relevant outcomes67 and helping researchers to improve the poor content validity of commonly used outcome measures for neck pain.68 In this perspective, the validation and transcultural adaptation of patient-reported experience measures, with adequate psychometric properties (eg, Picker Musculoskeletal Disorders Questionnaire), represent a research priority for measuring and capturing the whole concept of individuals’ expectations in various musculoskeletal conditions.6 Future research should invest efforts in qualitative studies on this topic to transparently report their research methods, including the researchers’ roles and how these may influence the conduct and results of the study.
In conclusion, because an individual’s experience is essential to improve clinical outcomes and deliver patient-centered care,6,8 clinicians should be encouraged to integrate it into their decision-making process when designing neck pain care plans.
Supplementary Material
Author Contributions
Concept/idea/research design: L.F. Maistrello, A. Palese, A. Turolla, A. Dell’Isola, G. Rossettini
Writing: L.F. Maistrello, L. Zanconato, A. Palese, T. Geri, A. Turolla, S. Gianola, A. Dell’Isola, G. Rossettini
Data collection: L. Zanconato, G. Rossettini
Data analysis: L.F. Maistrello, L. Zanconato, A. Palese, T. Geri, S. Gianola, G. Rossettini
Project management: L.F. Maistrello, G. Rossettini
Providing institutional liaisons: A. Dell’Isola
Consultation (including review of manuscript before submitting): L.F. Maistrello, L. Zanconato, A. Palese, T. Geri, A. Turolla, S. Gianola, G. Rossettini
Acknowledgments
The authors thank Dr Maxi Miciak for her valuable advice during the advancement of this manuscript.
Funding
There are no funders to report for this study.
Systematic Review Registration
The research protocol was registered in the Open Science Framework Registries Database (doi.org/10.17605/OSF.IO/XTF7P).
Disclosures
The authors completed the ICMJE Form for Disclosure of Potential Conflicts of Interest and reported no conflicts of interest.
References
- 1. Guzman J, Hurwitz EL, Carroll LJ, et al. A new conceptual model of neck pain: linking onset, course, and care: the bone and joint decade 2000-2010 task force on neck pain and its associated disorders. Spine (Phila Pa 1976). 2008;33:14–23. [DOI] [PubMed] [Google Scholar]
- 2. Safiri S, Kolahi AA, Hoy D, et al. Global, regional, and national burden of neck pain in the general population, 1990–2017: systematic analysis of the global burden of disease study 2017. BMJ. 2020;368:m791. 10.1136/bmj.m791. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Henschke N, Kamper SJ, Maher CG.. The epidemiology and economic consequences of pain. Mayo Clin Proc. 2015;90:139–147. [DOI] [PubMed] [Google Scholar]
- 4. Haldeman S, Carroll L, Cassidy JD.. Findings from the bone and joint decade 2000 to 2010 task force on neck pain and its associated disorders. J Occup Environ Med. 2010;52:424–427. [DOI] [PubMed] [Google Scholar]
- 5. Rondoni A, Rossettini G, Ristori D, et al. Intrarater and inter-rater reliability of active cervical range of motion in patients with nonspecific neck pain measured with technological and common use devices: a systematic review with meta-regression. J Manip Physiol Ther. 2017;40:597–608. [DOI] [PubMed] [Google Scholar]
- 6. Chi-Lun-Chiao A, Chehata M, Broeker K, et al. Patients’ perceptions with musculoskeletal disorders regarding their experience with healthcare providers and health services: an overview of reviews. Arch Phys Ther. 2020;10:17. 10.1186/s40945-020-00088-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Brouwer B, Waardenburg S, Jacobs C, et al. Biopsychosocial baseline values of 15 000 patients suffering from chronic pain: Dutch Data Pain Study. Reg Anesth Pain Med. 2020;45:774–782. [DOI] [PubMed] [Google Scholar]
- 8. Eversole J, Grimm A, Patel N, John K, Garcia AN. Why measure patient experience in physical therapy? Arch Phys Ther. 2021;11:11. 10.1186/s40945-021-00105-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Hutting N, Caneiro JP, Ong’wen OM, Miciak M, Roberts L. Patient-centered care in musculoskeletal practice: key elements to support clinicians to focus on the person. Musculoskelet Sci Pract. 2021;2021:102434. 10.1016/j.msksp.2021.102434. [DOI] [PubMed] [Google Scholar]
- 10. Evans R, Bronfort G, Maiers M, Schulz C, Hartvigsen J. “I know it’s changed”: a mixed-methods study of the meaning of global perceived effect in chronic neck pain patients. Eur Spine J. 2014;23:888–897. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Seers K. Qualitative systematic reviews: their importance for our understanding of research relevant to pain. Br J Pain. 2015;9:36–40. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. Dixon-Woods M, Agarwal S, Jones D, Young B, Sutton A. Synthesising qualitative and quantitative evidence: a review of possible methods. J Health Serv Res Policy. 2005;10:45–53. [DOI] [PubMed] [Google Scholar]
- 13. Barnett-Page E, Thomas J. Methods for the synthesis of qualitative research: a critical review. BMC Med Res Methodol. 2009;9:59. 10.1186/1471-2288-9-59. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14. Sandelowski M, Barroso J. Handbook for Synthesizing Qualitative Research. New York: Springer Publishing Company Inc; 2007. [Google Scholar]
- 15. Maxwell C, Robinson K, McCreesh K. Understanding shoulder pain: a qualitative evidence synthesis exploring the patient experience. Phys Ther. 2021;101:1–15. 10.1093/ptj/pzaa229. [DOI] [PubMed] [Google Scholar]
- 16. Bunzli S, Watkins R, Smith A, Schütze R, O’Sullivan P. Lives on hold: a qualitative synthesis exploring the experience of chronic low-back pain. Clin J Pain. 2013;29:907–916. [DOI] [PubMed] [Google Scholar]
- 17. MacNeela P, Doyle C, O’Gorman D, Ruane N, McGuire BE. Experiences of chronic low back pain: a meta-ethnography of qualitative research. Health Psychol Rev. 2015;9:63–82. [DOI] [PubMed] [Google Scholar]
- 18. Smith TO, Purdy R, Lister S, Salter C, Fleetcroft R, Conaghan P. Living with osteoarthritis: a systematic review and meta-ethnography. Scand J Rheumatol. 2014;43:441–452. [DOI] [PubMed] [Google Scholar]
- 19. Wallis JA, Taylor NF, Bunzli S, Shields N. Experience of living with knee osteoarthritis: a systematic review of qualitative studies. BMJ Open. 2019;9:1–11. 10.1136/bmjopen-2019-030060. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Wride JM, Bannigan K. ‘If you can’t help me, so help me god I will cut it off myself…’ the experience of living with knee pain: a qualitative meta-synthesis. Physiother (United Kingdom). 2018;104:299–310. [DOI] [PubMed] [Google Scholar]
- 21. Toye F, Seers K, Barker K. A meta-ethnography of patients’ experiences of chronic pelvic pain: struggling to construct chronic pelvic pain as “real.”. J Adv Nurs. 2014;70:2713–2727. [DOI] [PubMed] [Google Scholar]
- 22. Crowe M, Whitehead L, Seaton P, et al. Qualitative meta-synthesis: the experience of chronic pain across conditions. J Adv Nurs. 2017;73:1004–1016. [DOI] [PubMed] [Google Scholar]
- 23. Tong A, Flemming K, McInnes E, Oliver S, Craig J. Enhancing transparency in reporting the synthesis of qualitative research: ENTREQ. BMC Med Res Methodol. 2012;12:181. 10.1186/1471-2288-12-181. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24. Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med. 2009;6:e1000100. 10.1371/journal.pmed.1000100. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25. Page MJ, Moher D, Bossuyt PM, et al. PRISMA 2020 explanation and elaboration: updated guidance and exemplars for reporting systematic reviews. BMJ. 2021;372:n160. 10.1136/bmj.n160. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26. Page MJ, McKenzie JE, Bossuyt PM, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71. 10.1136/bmj.n71. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. Levitt HM, Bamberg M, Creswell JW, Frost DM, Josselson R, Suárez-Orozco C. Journal article reporting standards for qualitative primary, qualitative meta-analytic, and mixed methods research in psychology: the APA publications and communications board task force report. Am Psychol. 2018;73:26–46. [DOI] [PubMed] [Google Scholar]
- 28. Cooke A, Smith D, Booth A. Beyond PICO: the SPIDER tool for qualitative evidence synthesis. Qual Health Res. 2012;22:1435–1443. [DOI] [PubMed] [Google Scholar]
- 29. Sandelowski M, Barroso J. Classifying the findings in qualitative studies. Qual Health Res. 2003;13:905–923. [DOI] [PubMed] [Google Scholar]
- 30. Critical Appraisal Skills Programme . CASP (qualitative research) checklist. 2018. Accessed May 20, 2020. https://casp-uk.net/casp-tools-checklists/.
- 31. Rossettini G, Latini TM, Palese A, et al. Determinants of patient satisfaction in outpatient musculoskeletal physiotherapy: a systematic, qualitative meta-summary, and meta-synthesis. Disabil Rehabil. 2020;42:460–472. [DOI] [PubMed] [Google Scholar]
- 32. Noyes J, Popay J, Pearson A, Hannes K, Booth A. Chapter 20: qualitative research and Cochrane reviews. In: Higgins J, Green S, eds., Cochrane Handbook for Systematic Reviews of Interventions. Cochrane: John Wiley & Sons; 2015: 571–592. [Google Scholar]
- 33. Hannes K, Macaitis K. A move to more systematic and transparent approaches in qualitative evidence synthesis: update on a review of published papers. Qual Res. 2012;12:402–442. [Google Scholar]
- 34. Ludvigsen MS, Hall EOC, Meyer G, Fegran L, Aagaard H, Uhrenfeldt L. Using Sandelowski and Barroso’s meta-synthesis method in advancing qualitative evidence. Qual Health Res. 2016;26:320–329. [DOI] [PubMed] [Google Scholar]
- 35. Sandelowski M. A matter of taste: evaluating the quality of qualitative research. Nurs Inq. 2015;22:86–94. [DOI] [PubMed] [Google Scholar]
- 36. Sandelowski M, Docherty S, Emden C. Focus on qualitative methods. Qualitative metasynthesis: issues and techniques. Res Nurs Health. 1997;20:365–371. [DOI] [PubMed] [Google Scholar]
- 37. Saldana J. The Coding Manual for Qualitative Researchers. 3rd ed. Los Angeles, CA: Sage Pubns Ltd; 2015. [Google Scholar]
- 38. Onwuegbuzie AJ. Effect sizes in qualitative research: a prolegomenon. Qual Quant. 2003;37:393–409. [Google Scholar]
- 39. Scherer M, Schaefer H, Blozik E, Chenot J-F, Himmel W. The experience and management of neck pain in general practice: the patients’ perspective. Eur Spine J. 2010;19:963–971. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40. Langenfeld A, Bastiaenen C, Sieben J, Humphreys BK, Swanenburg J. Patient’s subjective impression of cervical range of motion: a mixed-methods approach. Spine (Phila Pa 1976). 2018;43:E1082–E1088. [DOI] [PubMed] [Google Scholar]
- 41. Cramer H, Lauche R, Haller H, Langhorst J, Dobos G, Berger B. “I’m more in balance”: a qualitative study of yoga for patients with chronic neck pain. J Altern Complement Med. 2013;19:536–542. [DOI] [PubMed] [Google Scholar]
- 42. Lauche R, Cramer H, Haller H, et al. My back has shrunk: the influence of traditional cupping on body image in patients with chronic non-specific neck pain. Forsch Komplementmed. 2012;19:68–74. [DOI] [PubMed] [Google Scholar]
- 43. Ahlsen B, Mengshoel AM, Solbrække KN. Troubled bodies--troubled men: a narrative analysis of men’s stories of chronic muscle pain. Disabil Rehabil. 2012;34:1765–1773. [DOI] [PubMed] [Google Scholar]
- 44. Ahlsen B, Mengshoel AM, Solbrække KN. Shelter from the storm; men with chronic pain and narratives from the rehabilitation clinic. Patient Educ Couns. 2012;89:316–320. [DOI] [PubMed] [Google Scholar]
- 45. Holmberg C, Farahani Z, Witt CM. How do patients with chronic neck pain experience the effects of qigong and exercise therapy? A qualitative interview study. Evid Based Complement Alternat Med. 2016;2016:8010891. 10.1155/2016/8010891. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46. Macdermid JC, Walton DM, Miller J, ICON. What is the experience of receiving health care for neck pain? Open Orthop J. 2013;7:428–439. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47. MacDermid JC, Walton DM, Bobos P, Lomotan M, Carlesso L. A qualitative description of chronic neck pain has implications for outcome assessment and classification. Open Orthop J. 2016;10:746–756. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48. Blanpied PR, Gross AR, Elliott JM, et al. Neck pain: revision 2017. J Orthop Sport Phys Ther. 2017;47:A1–A83. [DOI] [PubMed] [Google Scholar]
- 49. Viceconti A, Camerone EM, Luzzi D, et al. Explicit and implicit own’s body and space perception in painful musculoskeletal disorders and rheumatic diseases: a systematic scoping review. Front Hum Neurosci. 2020;14:83. 10.3389/fnhum.2020.00083. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50. Geri T, Viceconti A, Minacci M, Testa M, Rossettini G. Manual therapy: exploiting the role of human touch. Musculoskelet Sci Pract. 2019;44:102044. 10.1016/j.msksp.2019.07.008. [DOI] [PubMed] [Google Scholar]
- 51. McCabe E, Miciak M, Roduta Roberts M, Sun HL, Gross DP. Measuring therapeutic relationship in physiotherapy: conceptual foundations. Physiother Theory Pract. 2021;1–13. 10.1080/09593985.2021.1987604. [DOI] [PubMed] [Google Scholar]
- 52. Caneiro JP, Smith A, Bunzli S, Linton S, Moseley GL, O’Sullivan P. From fear to safety: a roadmap to recovery from musculoskeletal pain. Phys Ther. 2022;102:pzab271. 10.1093/ptj/pzab271. [DOI] [PubMed] [Google Scholar]
- 53. Silva Guerrero AV, Setchell J, Maujean A, Sterling M. A qualitative comparison of reassurance approaches used by physical therapists to address fears and concerns of patients with nonspecific neck pain and whiplash-associated disorders: an online survey. Phys Ther. 2020;100:1132–1141. [DOI] [PubMed] [Google Scholar]
- 54. Caneiro JP, Bunzli S, O’Sullivan P. Beliefs about the body and pain: the critical role in musculoskeletal pain management. Brazilian J Phys Ther. 2021;25:17–29. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55. Calner T, Isaksson G, Michaelson P. Physiotherapy treatment experiences of persons with persistent musculoskeletal pain: a qualitative study. Physiother Theory Pract. 2021;37:28–37. [DOI] [PubMed] [Google Scholar]
- 56. Orhan C, Van Looveren E, Cagnie B, Mukhtar NB, Lenoir D, Meeus M. Are pain beliefs, cognitions, and behaviors influenced by race, ethnicity, and culture in patients with chronic musculoskeletal pain: a systematic review. Pain Physician. 2018;21:541–558. [PubMed] [Google Scholar]
- 57. Bier JD, Scholten-Peeters WGM, Staal JB, et al. Clinical practice guideline for physical therapy assessment and treatment in patients with nonspecific neck pain. Phys Ther. 2018;98:162–171. [DOI] [PubMed] [Google Scholar]
- 58. Foster NE, Delitto A. Embedding psychosocial perspectives within clinical management of low back pain: integration of psychosocially informed management principles into physical therapist practice--challenges and opportunities. Phys Ther. 2011;91:790–803. [DOI] [PubMed] [Google Scholar]
- 59. Keefe FJ, Main CJ, George SZ. Advancing psychologically informed practice for patients with persistent musculoskeletal pain: promise, pitfalls, and solutions. Phys Ther. 2018;98:398–407. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60. Main CJ, George SZ. Psychologically informed practice for management of low back pain: future directions in practice and research. Phys Ther. 2011;91:820–824. [DOI] [PubMed] [Google Scholar]
- 61. Alexanders J, Anderson A, Henderson S. Musculoskeletal physiotherapists’ use of psychological interventions: a systematic review of therapists’ perceptions and practice. Physiotherapy. 2015;101:95–102. [DOI] [PubMed] [Google Scholar]
- 62. Driver C, Kean B, Oprescu F, Lovell GP. Knowledge, behaviors, attitudes and beliefs of physiotherapists towards the use of psychological interventions in physiotherapy practice: a systematic review. Disabil Rehabil. 2017;39:2237–2249. [DOI] [PubMed] [Google Scholar]
- 63. Holopainen R, Simpson P, Piirainen A, et al. Physiotherapists’ perceptions of learning and implementing a biopsychosocial intervention to treat musculoskeletal pain conditions: a systematic review and metasynthesis of qualitative studies. Pain. 2020;161:1150–1168. [DOI] [PubMed] [Google Scholar]
- 64. Simpson P, Holopainen R, Schütze R, et al. Training of physical therapists to deliver individualized biopsychosocial interventions to treat musculoskeletal pain conditions: a scoping review. Phys Ther. 2021;101:pzab188. 10.1093/ptj/pzab188. [DOI] [PubMed] [Google Scholar]
- 65. Buchbinder R, Maher C, Harris IA. Setting the research agenda for improving health care in musculoskeletal disorders. Nat Rev Rheumatol. 2015;11:597–605. [DOI] [PubMed] [Google Scholar]
- 66. Rossettini G, Testa M. Manual therapy RCTs: should we control placebo in placebo control? Eur J Phys Rehabil Med. 2017;;54:500–501. [DOI] [PubMed] [Google Scholar]
- 67. Beneciuk JM, Verstandig D, Taylor C, et al. Musculoskeletal pain stakeholder engagement and partnership development: determining patient-centered research priorities. Res Involv Engagem. 2020;6:28. 10.1186/s40900-020-00192-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68. Randeraad-van der Zee CH, AJHM B, RAHM S, et al. The burden of neck pain: its meaning for persons with neck pain and healthcare providers, explored by concept mapping. Qual Life Res. 2016;25:1219–1225. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.