Abstract
Justice-involved youth (JIY) have high rates of behavioral health disorders, but few can access, much less complete, treatment in the community. Behavioral health treatment completion among JIY is poorly understood, even within treatment studies. Measurement, reporting, and rates of treatment completion vary across studies. This systematic review and meta-analysis synthesizes the literature on rates of treatment completion among JIY enrolled in research studies and identifies potential moderators. After systematically searching 6 electronic databases, data from 13 studies of 20 individual treatment groups were abstracted and coded. A meta-analysis examined individual prevalence estimates of treatment completion in research studies as well as moderator analyses. Prevalence effect sizes revealed high rates of treatment completion (pr = 82.6). However, analysis suggests a high likelihood that publication bias affected the results. Treatment groups that utilized family- or group-based treatment (pr = 87.8) were associated with higher rates of treatment completion compared to treatment groups utilizing individual treatment (pr = 61.1). Findings suggest that it is possible to achieve high rates of treatment completion for JIY, particularly within the context of family- and group-based interventions. However, these findings are limited by concerns about reporting of treatment completion and publication bias.
Keywords: Adolescent, juvenile delinquency, behavioral medicine, patient participation, meta-analysis
Introduction
Approximately 50% of youth who have been arrested, are on probation post-adjudication, or are otherwise involved with the justice system (justice-involved youth; JIY) have a mental health disorder [1,2]. More than a third meet diagnostic criteria for a substance use disorder (SUD) [2]. Behavioral health disorders (i.e., both mental illness and SUD) are associated with an increased likelihood of recidivism and additional involvement with the justice system [3,4]; further justice system involvement, in turn, is associated with higher rates of behavioral health disorders [2]. While treatment completion has been associated with positive health and life outcomes (i.e., employment, housing) in substance use treatment [5] and with reduced recidivism among JIY youth specifically [6], JIY often do not complete available treatment for behavioral health disorders [7,8], even in the context of well-resourced treatment studies [9–11]. It is critical to understand factors involved in treatment completion among JIY.
Data suggest that JIY and their families experience challenges in completing treatment for behavioral health disorders [12]. For example, 2017 data from the Substance Abuse and Mental Health Services Administration indicate that only 45% of youth aged 12–20 years who were referred to publicly funded substance abuse treatment by a criminal justice organization successfully completed treatment [13] – most dropped out of treatment early or were discharged by the service provider due to lack of compliance with treatment. A recent cross-sectional analysis of administrative data from the Florida Department of Juvenile Justice suggests that, although 32% of the sample met criteria for SUD treatment, only 11.5% completed a SUD treatment program [14].
While administrative data may show the extent of the problem, they provide little understanding of how to address the problem. However, treatment studies for JIY may provide more insight. These studies often provide high-quality, evidence-based care, or are testing new interventions. In these contexts, researchers often make considerable efforts to help participants and their families maintain participation [15], and may therefore represent the best-case scenario for measuring treatment completion among JIY. A better understanding of the factors that contribute to successful completion in these contexts may help inform future research and practice.
Influences on treatment completion among JIY
Existing research suggests a number of possible moderators of behavioral health treatment completion among JIY. A recent systematic review examined empirical evidence on the effects of three types of interventions designed to improve engagement in behavioral health treatment among adolescents (not exclusively focused on JIY): systems-level (e.g., offering treatment services in-home), family-level (e.g., informing family members about treatment topics), or individual-level (e.g., utilizing contingency management interventions) [16]. Findings suggested that any type of intervention designed to increase behavioral health treatment engagement has positive influences on attendance at varying stages of treatment. Type of treatment (i.e., group, individual, family) may also have an influence on the extent to which youth are able to engage in and complete treatment; existing research suggests that family-based treatments are associated with greater engagement in substance use treatment among adolescents [17]. JIY who are members of ethnic and/or racial minority groups may be less likely to have access to or utilize mental health treatment [8]; research also finds that JIY of color have lower rates of treatment completion [14]. Some have argued that these disparities might reflect a difference in needs – for example, Black JIY are at an increased risk of experiencing poly-victimization, defined as having experienced many different types of traumatic victimization in their lifetime including assault, family/community violence, physical or sexual abuse, and trauma from racially driven encounters [18,19]. JIY of color are also more likely to experience a wide array of comorbid mental disorders [20], further demonstrating their need for high quality treatment. Researchers have argued that current treatment options may not be properly poised to address the complex stressors that JIY of color experience [19,21], thus discouraging engagement with treatment. Despite this, many youth of color do not have access to quality treatment options due to the fact that these youth tend to live in poorer communities with fewer resources, a systematic barrier [20]. Other barriers unique to engaging JIY youth of color include cultural mistrust of healthcare services rooted in historical oppression [22], greater logistical challenges (e.g., transportation, insurance issues) [20], and difficulties engaging family members in treatment (e.g., language barriers, competing demands) [20].
Low rates of treatment completion among JIY may be surprising, since JIY often enter treatment because of legal mandates (e.g., as a condition of probation). However, the effect of juvenile drug courts – one of the most common examples of mandated treatment – has been highly variable, especially in comparison to more commonly successful adult drug courts [23]. Current evidence suggests that most juvenile drug courts minimally engage parents and youth; a meta-analytic review found that slightly more than half of all youth who initially enroll in a juvenile drug court program end up graduating and that youth who enroll but do not graduate (i.e., are terminated unsuccessfully) do not appear to benefit from participating in the program based on later measures of substance use and recidivism [24]. Given these findings, researchers conclude that it is necessary to implement additional efforts to engage youth in treatment, beyond or instead of court mandates [24]. Especially given the increase in diversion of youth away from the justice system, it is critically important to understand how to constructively engage youth without the force of court mandates [25]; the first step in this process is understanding complexities in current rates of treatment completion among JIY and identifying potential moderators.
Purpose of Study
Longitudinal studies of behavioral health treatment among JIY report inconsistent findings, with wide ranges in rates of treatment completion [26–28] even in the context of additional resources available to researchers to help engage participants. The current study aims to conduct a meta-analysis to quantify treatment completion among JIY enrolled in behavioral health treatment studies. In addition, the current study aims to determine whether demographic variables (i.e., gender, race/ethnicity) and methodological variables (i.e., intervention focus, type of treatment, the presence or absence of interventions to increase treatment engagement) moderate the prevalence of treatment completion among JIY.
Methods
Procedures and results are reported in accordance with the Preferred Reporting Items for Systematic Reviews and Meta Analyses (PRISMA) Statement [29,30], which is available in Table 1.
Table 1.
PRISMA reporting checklist for systematic reviews and meta-analysis
| Section/topic | # | Checklist item | Reported on page # |
|---|---|---|---|
| Title | |||
| Title | 1 | Identify the report as a systematic review, meta-analysis, or both. | 1 |
| Abstract | |||
| Structured summary | 2 | Provide a structured summary including, as applicable: background; objectives; data sources; study eligibility criteria, participants, and interventions; study appraisal and synthesis methods; results; limitations; conclusions and implications of key findings; systematic review registration number. | 2 |
| Introduction | |||
| Rationale | 3 | Describe the rationale for the review in the context of what is already known. | 3 - 6 |
| Objectives | 4 | Provide an explicit statement of questions being addressed with reference to participants, interventions, comparisons, outcomes, and study design (PICOS). | 5 - 6 |
| Methods | |||
| Protocol and registration | 5 | Indicate if a review protocol exists, if and where it can be accessed (e.g., Web address), and, if available, provide registration information including registration number. | NA |
| Eligibility criteria | 6 | Specify study characteristics (e.g., PICOS, length of follow-up) and report characteristics (e.g., years considered, language, publication status) used as criteria for eligibility, giving rationale. | 6 |
| Information sources | 7 | Describe all information sources (e.g., databases with dates of coverage, contact with study authors to identify additional studies) in the search and date last searched. | 7 |
| Search | 8 | Present full electronic search strategy for at least one database, including any limits used, such that it could be repeated. | 7, Table 2 |
| Study selection | 9 | State the process for selecting studies (i.e., screening, eligibility, included in systematic review, and, if applicable, included in the meta-analysis). | 6–7 |
| Data collection process | 10 | Describe method of data extraction from reports (e.g., piloted forms, independently, in duplicate) and any processes for obtaining and confirming data from investigators. | 7 |
| Data items | 11 | List and define all variables for which data were sought (e.g., PICOS, funding sources) and any assumptions and simplifications made. | 7 - 9 |
| Risk of bias in individual studies | 12 | Describe methods used for assessing risk of bias of individual studies (including specification of whether this was done at the study or outcome level), and how this information is to be used in any data synthesis. | 9 |
| Summary measures | 13 | State the principal summary measures (e.g., risk ratio, difference in means). | 9 |
| Synthesis of results | 14 | Describe the methods of handling data and combining results of studies, if done, including measures of consistency (e.g., I [2]) for each meta-analysis. | 9–11 |
| Risk of bias across studies | 15 | Specify any assessment of risk of bias that may affect the cumulative evidence (e.g., publication bias, selective reporting within studies). | 11 |
| Additional analyses | 16 | Describe methods of additional analyses (e.g., sensitivity or subgroup analyses, meta-regression), if done, indicating which were pre-specified. | 10 - 11 |
| Results | |||
| Study selection | 17 | Give numbers of studies screened, assessed for eligibility, and included in the review, with reasons for exclusions at each stage, ideally with a flow diagram. | 7, 11, Fig. 1 |
| Study characteristics | 18 | For each study, present characteristics for which data were extracted (e.g., study size, PICOS, follow-up period) and provide the citations. | 11–13, Table 3 and 4 |
| Risk of bias within studies | 19 | Present data on risk of bias of each study and, if available, any outcome-level assessment (see item 12). | 13 |
| Results of individual studies | 20 | For all outcomes considered (benefits or harms), present, for each study: (a) simple summary data for each intervention group and (b) effect estimates and confidence intervals, ideally with a forest plot. | 13, Fig. 2 |
| Synthesis of results | 21 | Present results of each meta-analysis done, including confidence intervals and measures of consistency. | 13, Table 5 |
| Risk of bias across studies | 22 | Present results of any assessment of risk of bias across studies (see Item 15). | 14 |
| Additional analysis | 23 | Give results of additional analyses, if done (e.g., sensitivity or subgroup analyses, meta-regression [see Item 16]). | 13 |
| Discussion | |||
| Summary of evidence | 24 | Summarize the main findings including the strength of evidence for each main outcome; consider their relevance to key groups (e.g., healthcare providers, users, and policy makers). | 14- 15, 18 |
| Limitations | 25 | Discuss limitations at study and outcome level (e.g., risk of bias), and at review-level (e.g., incomplete retrieval of identified research, reporting bias). | 16 |
| Conclusions | 26 | Provide a general interpretation of the results in the context of other evidence and implications for future research. | 15–18 |
| Funding | |||
| Funding | 27 | Describe sources of funding for the systematic review and other support (e.g., supply of data); role of funders for the systematic review. | NA |
Inclusion and Exclusion Criteria
Studies were included if: 1) they were available in English, 2) the sample included youth who are involved in the juvenile justice system and who resided in the community at the time of the study (e.g., youth on probation, youth who have been arrested and then diverted from the justice system through a diversion program), 3) the study included an assessment to determine eligibility for treatment and the provision of a behavioral health treatment, and 4) the authors reported criteria for treatment completion. Studies in which all JIY were eligible (i.e., the primary goal of services was to prevent recidivism) were excluded; however, studies targeting behavioral problems (i.e., youth adjudicated through drug court, youth who sexually offend) indicative of a specific behavioral health disorder being treated were included. Book chapters and dissertations were included in literature searches. Studies were excluded if they were cross-sectional, were primarily studies of behavioral health service utilization (i.e., assessing whether youth access treatment not provided as part of the study), or represented evaluations of treatment services in which only participants who completed treatment were included in analyses. Studies that combined youth who were and were not JIY or included both adult and juvenile participants were excluded unless information for only the JIY participants could be obtained.
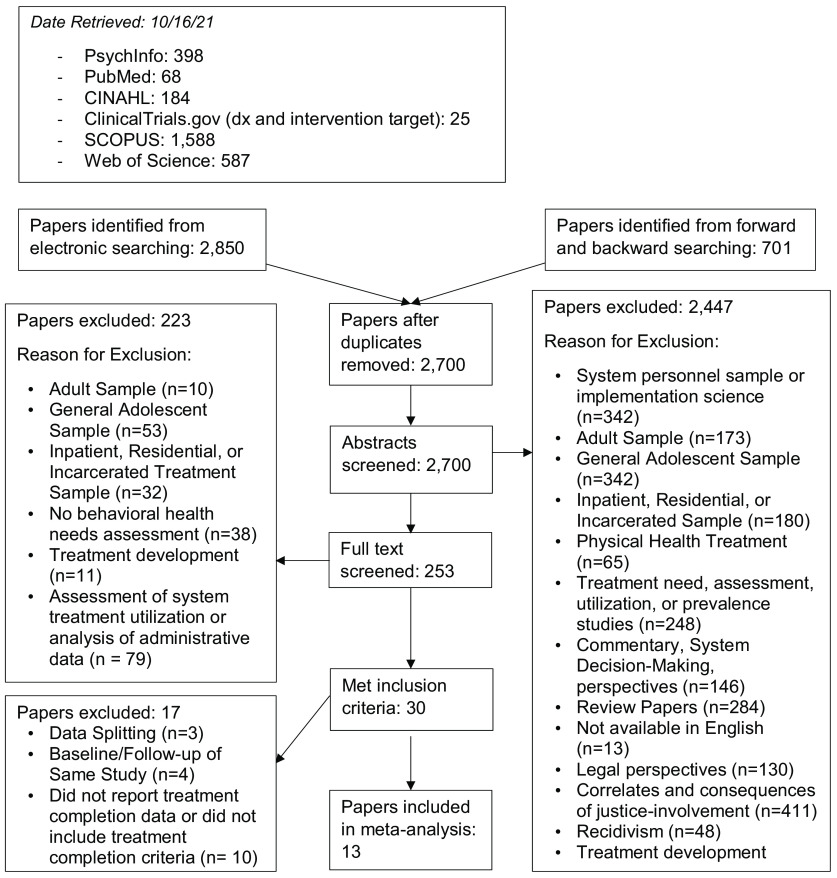
Literature Search
We identified studies meeting criteria for inclusion using four concurrent methods. First, we identified 2,850 studies through database literature searches (see Table 2 for databases and search terms). Second, because the terminology to identify JIY is quite heterogeneous (e.g., justice-involved, juvenile offender, probationers, delinquent, justice-referred), we identified 701 articles through extensive forward- and backward-literature searching of reviews on behavioral health treatments for adolescents and reviews of interventions for JIY [31–47]; this is an established method of conducting literature searches in areas where the terminology is not standardized [48]. Third, subject matter experts were contacted (i.e., authors of published articles on studies funded by JJTrials) to inquire about data from unpublished studies, but no additional studies were obtained from these contacts. Finally, we created email alerts in Google Scholar for the above search; no newly eligible studies were identified prior to manuscript submission. After duplicates were removed, we reviewed the title and abstract of 2,700 articles with the full text of 253 articles being reviewed (see Fig. 1 for PRISMA flow chart and article exclusions). Thirteen studies were coded for inclusion in the data analysis.
Table 2.
Database search terms
| Database | Search Terms |
|---|---|
| PSYCHInfo | ((MM “Substance Use Treatment” OR MM “Alcohol Treatment” OR MM “Mental Health Services” OR MM “Community Mental Health Services”) AND (MM “Juvenile Delinquency” OR MM “Juvenile Justice”) using PSYCHInfo subject headings thesaurus |
| CINAHL | ((MM “Substance Use Rehabilitation Programs+” OR MM “Mental Health Services+”) AND (MM “Juvenile Offenders+” OR MM “Juvenile Delinquency”)) using CINAHL subject headings |
| PubMed | ((“juvenile delinquency” [MeSH Terms]) AND ((“substance-related disorders“[MeSH Terms]) OR (“mental processes/psychology“[MeSH Terms])) AND (“treatment outcome“[MeSH Terms])) using MeSH terms |
| ClinicalTrials.gov | (“juvenile justice” OR “juvenile delinquent”) AND (“treatment” OR “intervention” OR “therapy”) | (“Mental health disorder” OR “substance use disorder”) |
| SCOPUS | ((“juvenile justice” OR “juvenile delinquent”) AND (“mental health treatment” OR “substance use treatment” OR “behavioral health treatment” OR “mental health intervention” OR “substance use intervention” OR “behavioral health intervention”)) |
| Web of Science | (ALL = (adolescent OR youth OR juvenile) AND ALL = (“juvenile justice” OR “juvenile delinquent” OR probation OR diversion OR diverted) AND ALL = (“mental health treatment” OR “substance use treatment” OR “behavioral health treatment” OR “mental health intervention” OR “substance use intervention” OR “behavioral health intervention” OR therapy)) AND LANGUAGE: (English) |
Fig. 1.
PRISMA flow chart.
Coding
We coded studies according to a fixed coding protocol, following guidelines from Lipsey, Wilson [49], and Card [50]; variables included study characteristics, primary outcomes of interest, moderators, and study quality. Each study was coded independently by the first, second, and third authors; after coding, the authors met to identify and resolve discrepancies in coding.
Prevalence Estimates
We coded the number of JIY who began treatment and the number who completed treatment according to the study’s stated treatment completion criteria. This prevalence rate was coded as treatment completion. If studies reported sufficient data on multiple treatment conditions, separate effect sizes were estimated for each treatment condition. For RCTs where “treatment completion” criteria were not specified for the control condition (usually “services as usual”), the treatment completion prevalence rate was only coded for the experimental condition(s).
Moderators
Racial and ethnic minority participants
The prevalence of racial and ethnic minority participants was coded as a percentage for each study or treatment group and included in analysis of moderators.
Intervention Focus
We assessed intervention focus as a moderator; this variable was coded as 1 = substance use disorders and 2 = other behavioral health for analyses.
Type of Treatment
Type of treatment was coded as 1 = individual, 2 = group, and 3 = family for analyses. When treatments included multiple components (e.g., individual sessions with the youth as well as sessions with youth and parent(s), individual therapy with group skills training classes), it was coded according to the study’s identified type of treatment (e.g., a family-based treatment) and the highest level of clinical intensity in the treatment. Thus, if a treatment included both individual and family components and was described as family-based treatment, it was coded as 3 = family. If a treatment included individual therapy sessions and less-frequent group skill-building classes, it was coded as 1 = individual.
Interventions to Increase Treatment Engagement
The presence or absence of reported interventions to increase treatment engagement was coded as a moderator (1 = present, 2 = not present). Interventions to increase engagement commonly included contingency management programs, engaging family in the treatment planning process, providing treatment in the youth’s home or other convenient locations, providing transportation to treatment, or a comprehensive assessment of barriers to engagement and subsequent problem solving that focuses on the whole ecology of youths and families, as is standard in multisystemic therapy (MST). Basic phone or text-message reminders of treatment appointments, as are commonly provided in behavioral healthcare, were not coded as interventions to increase engagement.
Treatment Mandates
Whether or not youth were mandated by a court to participate in outpatient treatment was coded as the percentage of youth in the study who were required to participate in outpatient treatment.
Primary Study Quality
Standardized measures for assessing primary study quality in systematic reviews and meta-analyses typically focus on specific study designs (e.g., quasi-experimental studies, noncontrolled longitudinal studies) and are geared toward assessing risk of bias in the study’s main outcome variable. Because we were primarily interested in judging the quality of measures of attendance and attrition (rather than bias in outcome) across studies with varied designs, we developed a checklist after reviewing existing measures of study quality [51–53] as well as review articles on the measurement of treatment engagement [16,17,54,55]. The checklist was composed of 5 yes/no questions for all primary studies and 2 additional questions for studies with randomized designs; the checklist is available as a Supplementary file.
Data Analysis
Effect Size Calculations
All analyses were performed in R (Version 4.1.3) with packages Metafor and Meta [56–58]. To assess proportional data, an analysis of binary outcomes was pooled in the form of proportions with a generalized linear mixed model (GLMM) using the logit link function with Clopper-Pearson intervals to stabilize the variance [59,60]. Simulation studies indicate that the GLMM model provides the most accurate estimate in proportional meta-analysis because GLMM models do not require data transformations within studies [61,62], fully account for uncertainties, and produce confidence intervals with satisfactory coverage probabilities [63]. We implemented all parameters via the maximum likelihood approach. Random effects models were selected to calculate effect sizes because they represent a more conservative estimate of mean prevalence and to account for heterogeneity between studies.
We examined forest plots to identify potential outliers, i.e., studies whose individual 95% CI did not overlap with the 95% CI for the mean effect [64,65]. Potential outliers were removed from calculation of effect size if overall prevalence rates were affected [65]. Heterogeneity of the studies was assessed using Cochran’s Q-Test, which tests for the presence of heterogeneity across studies [66], and Higgins I2, which describes the percent of variation in prevalence across studies due to heterogeneity rather than chance [67]. Low heterogeneity was defined as Q scores < critical chi square values and I2 < 25%; moderate if Q > critical chi square values and I2 around 50%; and high if Q > critical chi square values and I2 > 50%. Statistical significance was defined as P < 0.05 [67].
Moderator Analyses
If significant heterogeneity of individual prevalence estimates was found via the two criteria, mixed-effect meta regression was used to attempt to explain the between-study heterogeneity based on study-level fixed-effect covariates (i.e., subgroups defined by categorical covariates or continuous covariates). Specifically, candidate variables were tested to identify significant moderators (i.e., candidate variables that account for a significant proportion of variability in individual prevalence across studies) in nonlinear mixed-effects models, such that random-effect terms were used to combine studies within each subgroup, and fixed-effect terms were used to combine subgroups and yield the overall effect [68]. Study-to-study variance (T 2) was not assumed to be the same for all subgroups; the value was computed within subgroups [69]. The Q between statistic (analogous to analysis of variance) tested categorical variables to report between-study variance explained by moderators. We calculated mean effect sizes within all variable levels [70]. Variables were considered moderators if the mixed(random)-effects model indicated statistical significance (P < 0.05) on the Q between statistic [71]. Interactions among moderator variables were not tested due to insufficient power.
Publication Bias
Publication bias was assessed with funnel plot symmetry both visually and statistically by using Egger’s linear regression method to assess any relationship between sample size and prevalence [72]. If significant funnel plot asymmetry was present, the trim and fill method was used to determine the number of missing studies that would be needed to correct the asymmetry [73]. An additional quantitative assessment of bias used the Begg’s rank method [74] to identify relationships between effect sizes and sample sizes. Low publication bias was deemed present if funnel plots were visually symmetrical and were not statistically significant. Finally, given the gaps in the ability to assess publication bias in proportional meta-analyses using established statistical methods, we offer qualitative assessments of the role of publication bias in these analyses.
Results
Description of Included Studies
Altogether, 13 studies [9–11,26,28,75–82] representing 20 treatments (e.g., services as usual, Multisystemic Therapy) met inclusion criteria (see Table 3). Three of the 13 studies included services as usual treatment conditions in which they did not specify treatment completion criteria (see Table 4 for details); adolescents in these groups were not included in the tables or in the descriptions below. All studies were peer-reviewed published articles and were located in the United States. Complete descriptions of all 13 studies are included in Tables 3 and 4.
Table 3.
Effect size variables and demographics
| Effect Size Variables | Demographics | |||||||
|---|---|---|---|---|---|---|---|---|
| Eligible N | Initiation N | Treatment Group | Treatment Group N |
Completion N | Age (SD) | % Minority | % Female | |
| Borduin et al., 2009 | 51 | 48 | MST (T) | 24 | 24 | 14 (1.9) | 29.2 | 4.2 |
| SAU (C) | 24 | 22 | ||||||
| Burrow-Sanchez et al., 2015 | 71 | 70 | Standard CBT (T1) | 36 | 24 | 15.3 (1.3) | 100.0 | 11.1 |
| Accommodated CBT (T2) | 34 | 27 | 15.1 (1.2) | 100.0 | 8.8 | |||
| Dakof et al., 2015 | 119 | 112 | MDFT (T1) | 55 | 53 | 16.0 (1.1) | 100.0 | 10.9 |
| AGT (T2) | 57 | 49 | 16.1 (0.9) | 100.0 | 10.5 | |||
| Henderson et al., 2016 | 145 | 126 | ACRA (T) | 63 | 40 | 15.1 (1.1) | 25.2 | 20.6 |
| SAU * | 63 | not reported | 15.3 (1.0) | 22.0 | 26.9 | |||
| Henggeler et al., 1999 | 141 | 118 | MST (T) | 58 | 57 | 15.7 (1.0) | 53.0 | 21.1 |
| SAU (C) | 60 | 3 | ||||||
| Henggeler et al., 2015 | 115 | 104 | CM (T) | 73 | 63 | 15.4 (0.9) | 43.5 | 17.6 |
| SAU (C) | 42 | 41 | ||||||
| Kaminer et al., 2019 | 142 | 113 | MET-CBT (T) | NA | 102 | 16.1 (1.0) | 62.3 | 12.1 |
| Letourneau et al., 2009 | 178 | 131 | MST (T) | 68 | 62 | 14.6 (1.7) | 85.0 | 2.4 |
| SAU (C) | 66 | 58 | ||||||
| Schaeffer et al., 2014 | 104 | 97 | Community Restitution (T) | 50 | 33 | 15.8 (0.9) | 82.0 | 17.0 |
| SAU * | 47 | not reported | 15.9 (0.9) | 85.0 | 18.0 | |||
| Sharkey et al., 2010 | not reported | 150 | Neighborhood enrichment (T) | NA | 150 | 16.02 (1.2) | 80.9 | 38.0 |
| Silovsky et al., 2019 | 418 | 320 | CBT (T) | NA | 188 | 12.8 (1.6) | not reported | 9.1 |
| Tolou-Shams et al., 2017 | 233 | 60 | Family Affect Management(T1) | 30 | 25 | 15.6 (1.3) | 50.7 | 30.0 |
| Health Promotion (T2) | 30 | 22 | ||||||
| Walker et al., 2019 | 136 | 101 | Girls Active Learning | 66 | 57 | 15.2 (1.7) | 41.0 | 100.0 |
| SAU * | 35 | not reported | ||||||
Note: In some cases, authors reported demographics for all participants (rather than by treatment group) after finding that there were no significant demographic differences between treatment groups.
Abbreviations: Multisystemic Therapy (MST), Services as Usual (SAU), Cognitive Behavioral Therapy (CBT), Multidimensional Family Therapy (MDFT), Motivational Enhancement Therapy (MET), Adolescent Group Treatment (AGT), Adolescent Community Reinforcement Approach (ACRA), Contingency Management (CM).
SAU treatment groups that did not define or report treatment completion data were not included in analyses.
Table 4.
Methodological variables
| Methodological Variables | ||||||||
|---|---|---|---|---|---|---|---|---|
| Study Design | Intervention Focus | Justice-Involvement Type | Treatment Mandates | Type of Treatment | Engagement Interventions | Treatment Length | Completion Criteria | |
| Borduin et al., 2009 | RCT | Problematic Sexual Behavior | arrested; could be pre- or post- adjudication | Court-ordered outpatient sexual offender counseling | MST; family (T) | Services provided in convenient location; therapists available 24/7 | Averaged 30 weeks | Collaboratively identified by MST therapist and patient |
| SAU; individual (C) | None reported | Averaged 30 weeks | Collaboratively identified by MST therapist & patient | |||||
| Burrow-Sanchez et al., 2015 | RCT | Any SUD | heterogeneous; all participants referred by juvenile probation department | 74% court-ordered to treatment | Standard-CBT; group (T1) | None reported | 12 weeks | Attended 9 of 12 treatment sessions |
| accommodated CBT; family (T2) | Treatment manual modified to increase relevancy for Latino adolescents and include family treatment; promoted regular phone/mail contact between therapist and patients/families | 12 weeks | Attended 9 of 12 treatment sessions | |||||
| Dakof et al., 2015 | RCT | Any SUD | All participants enrolled in drug court | Court-ordered to treatment | MDFT; family (T1) | Financial assistance with transportation; services provided in convenient location; included family in treatment planning | Averaged 20 weeks | Graduation from drug court |
| Adolescent Group Treatment; group (T2) | Financial assistance with transportation; therapists reached out to DC and family if youth failed to attend | Averaged 20 weeks | Graduation from drug court | |||||
| Henderson et al., 2016 | RCT | Any SUD | On probation | Not reported | Adolescent-Community Reinforcement Approach; individual (T) | Financial assistance with transportation; services provided in convenient location | Averaged 36 weeks | Attended 3 or more sessions |
| SAU; individual * | None reported | Averaged 36 weeks | Not specified | |||||
| Henggeler et al., 1999 | RCT | Any SUD | Formal or informal probation | Not reported | MST; family (T) | Services provided in convenient location; therapists available 24/7 | Averaged 18 weeks | Collaboratively identified by MST therapist & patient |
| SAU; individual (C) | None reported | Not Described | Collaboratively identified by MST therapist & patient | |||||
| Henggeler et al., 2015 | RCT | Problematic drug use | All participants enrolled in drug court | Court-ordered to treatment | Contingency management – family engagement; family (T) | Contingency management intervention; included family in treatment planning | Averaged 20 weeks | Graduation from drug court |
| SAU; group (C) | None reported | Averaged 12 weeks | Graduation from drug court | |||||
| Kaminer et al., 2019 | Non-controlled | Cannabis use disorder | All participants referred by juvenile probation department | Not reported | MET-CBT; individual (T) | None reported | 7 weeks + additional 10 weeks for non-responders | Attending at least the first and last session of each phase |
| Letourneau et al., 2009 | RCT | Problematic sexual behavior | On probation or in a diversion program | Court-ordered outpatient sexual offender counseling | MST; family (T) | Services provided in convenient location; therapists available 24/7 | Averaged 28.4 weeks | Collaboratively identified by MST therapist & patient |
| SAU; group (C) | None reported | Averaged 50 weeks | Collaboratively identified by MST therapist & patient | |||||
| Schaeffer et al., 2014 | RCT | Any SUD | All participants referred by juvenile probation department | Not reported | Community restitution apprentice-focused training; individual (T) | Financial assistance with transportation; individualized program attendance schedules coordinated with schools | 6 months | Attendance for a minimum of 100 hrs of instruction & proficiency in all core skill areas |
| SAU; individual * | None reported | Not described | Not specified | |||||
| Sharkey et al., 2010 | Non-controlled | Any SUD | Identified for services through juvenile probation or truancy | Not reported | Neighborhood enrichment with vision involving services, treatment, and services; family | Services centrally located for easier transportation; culturally modified treatment by recruiting providers from community | Not described | Completion of curriculum |
| Silovsky et al., 2019 | Non-controlled | Problematic sexual behavior | Juvenile probation actively involved in all treatment teams; participants on probation or diverted | 42% court-ordered to treatment | CBT with concurrent groups for youth and caregivers; family (T) | None reported | Not described | Completion of curriculum |
| Tolou-Shams et al., 2017 | RCT | Problematic drug use | All participants enrolled in drug court | Not reported; notes that court was unaware of youth participation in study | Family-based Affect Management Intervention; family (T1) | None reported | 7 weeks | Completed core intervention (4 weeks) |
| Adolescent-only Health Promotion Intervention; individual (T2) | None reported | 7 weeks | Completed core intervention (4 weeks) | |||||
| Walker et al., 2019 | Quasi-experimental | Problematic drug use | On probation | Not reported | Girls Only Active Learning; group (T) | Weekly text messages to parents about attendance and the weekly program topic | 10 weeks | Completed if youth did not miss more than 3 sessions |
| SAU; individual * | None reported | Not described | Not specified | |||||
Abbreviations: Multisystemic Therapy (MST), Services as Usual (SAU), Cognitive Behavioral Therapy (CBT), Multidimensional Family Therapy (MDFT), Motivational Enhancement Therapy (MET).
In some studies, Services as Usual (SAU) conditions did not report treatment completion criteria or data. These conditions were not included in analyses.
The 20 eligible treatment conditions included a total sample size of 1,269 adolescents, with a mean sample size of 74.7 (SD = 70.7, range = 24–320). Samples averaged 15.2 years of age, were predominantly male (80.2%), and were predominantly from minority ethnic or racial populations (68.1%). Studies were primarily focused on substance use disorders (n = 10, 76.9%). Individual treatment conditions utilized different types of treatment, categorized as family (n = 9, 52.9%), individual (n = 4, 23.5%), or group (n = 4, 23.5%). When treatment length and completion criteria were reported, treatments were designed to last an average of 18.4 weeks (SD = 8.6).
Studies employed a wide range of strategies to increase treatment completion; of 20 individual treatment groups (including services as usual and experimental treatment conditions, which often used different treatment engagement strategies between groups), 11 (65%) reported employing interventions to increase treatment engagement; see Table 4. Six treatment groups provided services in locations convenient to the youth or family (e.g., home, school, community spaces). Four treatment groups offered financial assistance with transportation to treatment, three made on-call therapists available to families at all times, and 4 included family in-treatment planning (e.g., contacting family each week to describe the group session topic, encouraging regular contact between therapists and families). Two treatment groups modified services to be culturally adapted, e.g., by recruiting providers from the local community. Finally, only one treatment group utilized a contingency management intervention to increase youth attendance in treatment. Nine treatment groups did not specify any treatment engagement strategies. See Table 4 for descriptions of engagement strategies used in each study.
Supervision or JIY court involvement varied widely both between and within studies; youth were on probation, arrested and entering treatment pre-adjudication, in formal diversion programs, or enrolled in drug court. In three studies (23.1%), participants were recruited entirely from juvenile drug courts. Whether or not youth had been mandated to participate in treatment also varied widely both within and between studies; 7 studies (53.8%) did not report information on treatment mandates; see Table 4.
Treatment Completion
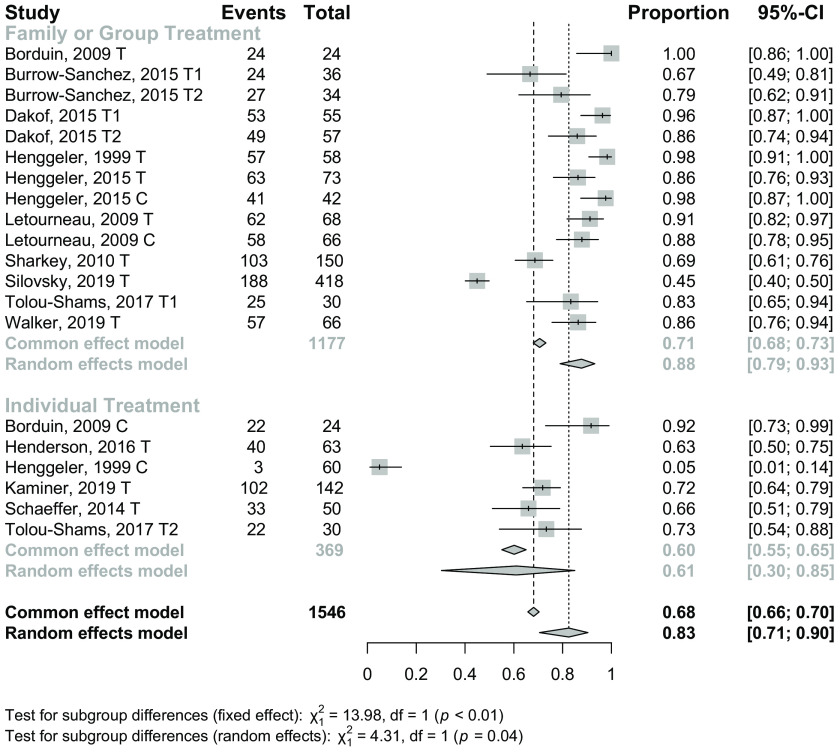
A total of 13 studies yielded 20 individual prevalence estimates; see Fig. 2 for the forest plot of effect sizes and Table 5 for associated model statistics. Although there were two significant outliers from the mean prevalence estimate [9,77], neither of these individual estimates had a significant effect on the overall estimate when removed from analyses, so individual estimates from all studies were retained. The main effect size for treatment completion was pr = 82.6 (CI = 70.6, 90.3), indicating that approximately 82.6% of JIY completed treatment, as defined by each study’s individual treatment completion criteria. The heterogeneity in individual prevalence estimates across studies was high (Q = 221.3, I2 = 91.4), meeting criteria for moderation analyses.
Fig. 2.
Treatment completion by treatment type. Note: Treatment groups are marked as T (treatment group), C (control group), or T1 and T2 for multiple treatments in comparative effectiveness studies.
Table 5.
Effect sizes and associated statistics
| Full model results for meta-analysis | ||||||||
|---|---|---|---|---|---|---|---|---|
| Number of effects |
Effect Size |
95% CI | Range |
Q
Statistic |
I2
Index |
Begg’s rank correlation | Egger’s weighted regression |
|
| Treatment Completion |
20 | 82.6 | 70.6, 90.3 | 5.0–98.0 | 221.3 | 91.4 | 0.08 | < 0.01 |
| Mixed effects models for analysis of categorical moderators | ||||||||
| k | Effect Size |
95 % CI | Range |
Q
between
Statistic |
df | P | ||
| Intervention Focus | ||||||||
| SUD | 15 | 80.0 | 66.7, 96.9 | 1.6–99.7 | 0.63 | 1 | 0.39 | |
| Other | 5 | 88.7 | 66.7, 96.9 | 40.3–99.9 | ||||
| Treatment Type | ||||||||
| Family or Group | 14 | 87.8 | 78.9, 93.2 | 38.0–99.9 | 4.31 | 1 | 0.04 | |
| Individual | 6 | 61.1 | 30.4, 84.9 | 1.6–97.9 | ||||
| Interventions to Increase Treatment Engagement | ||||||||
| Absent | 9 | 75.9 | 49.7, 90.1 | 1.6–99.7 | 0.9 | 1 | 0.33 | |
| Present | 11 | 86.0 | 75.4, 92.5 | 50.0–99.9 | ||||
| Meta-regression models for analysis of continuous moderators | ||||||||
| Coefficient | Standard Error |
95% CI | P | |||||
| % Minority | 0.17 | 0.13 | –0.09, 0.42 | 0.21 | ||||
Moderator Analyses
Subgroup analyses revealed that treatment completion was higher in studies that provided family- or group-based treatment (pr = 87.8, CI = 78.9, 93.2, k = 14) compared to studies providing individual treatment (pr = 61.1, CI = 30.4, 84.9, k = 6); see Fig. 2 for a forest plot of effect sizes by type of treatment and Table 5 for full results from moderator analyses. No other significant moderators were identified.
Primary Study Quality
Studies included a range of designs: 9 studies (52.9%) were RCTs (some of these employed a cluster-randomized design), one (7.7%) was a quasi-experimental trial with a control group, and three (23.1%) were noncontrolled longitudinal trials of treatment effectiveness (see Supplemental Table). All but one study conducted intent-to-treat analyses, in which all participants who entered treatment were included in outcome analyses. Only three studies (23.1%) provided a detailed description of youth who did not complete treatment, including reasons for attrition and demographic characteristics of those who did not complete treatment.
Publication bias
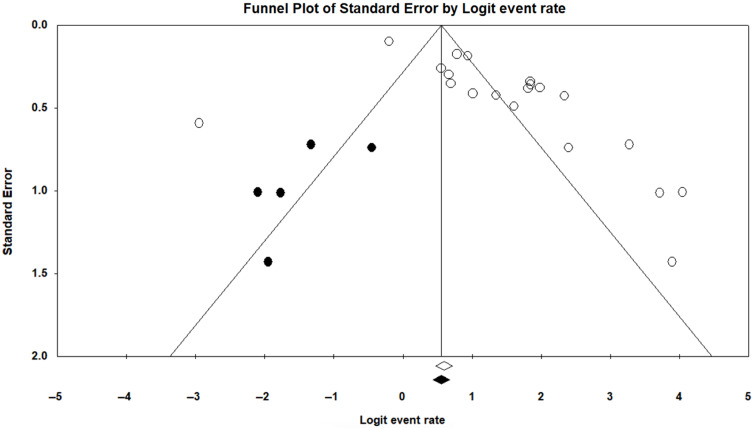
Visual assessment of the funnel plot for treatment completion suggests moderate publication bias (see Fig. 3 for the funnel plot with unpublished studies imputed). Quantitative assessments using Begg’s rank correlation analysis trended toward significance (p = 0.08), while assessment of Egger’s test of the intercept was statistically significant (p < 0.01), suggesting some publication bias. We used the trim-and-fill method to determine the number of missing studies that would be needed to correct the asymmetry (see Fig. 3); this method suggests 5 imputed studies; however, current literature indicates that substantial heterogeneity in effect sizes (as is present in this analysis) seriously impairs the power of the trim-and-fill method, since the plot’s asymmetry may be confounded by heterogeneity [83–85]. Therefore, these results should be interpreted with caution. Although established statistical methods for assessing publication bias in meta-analysis are traditionally used to examine bias in treatment effects, these results may also have implications for examining bias in study completion rates. In particular, studies with low completion rates may be likely to have fewer positive treatment effects, increasing the probability that results will not be published.
Fig. 3.
Funnel plot of treatment completion with imputed studies. Note: Imputed studies are shown in black.
Discussion
This systematic review and meta-analysis represent the first attempt to quantitatively review and synthesize behavioral health treatment completion data among JIY enrolled in treatment studies. This meta-analysis aimed to derive a more accurate estimate of treatment completion among JIY and better understand issues related to treatment engagement strategies and barriers to treatment completion. Findings indicated relatively high rates of treatment completion, with 82.6% of youth who initiated treatment completing treatment according to the treatment’s specified completion criteria. Our findings suggest when some systemic barriers to treatment (i.e., low treatment availability, difficulty identifying appropriate treatment, treatment cost) are removed by the presence of providing treatment within a study, JIY may not be any more difficult to engage in treatment than the general adolescent population.
One aim of this investigation was to begin to disentangle the influence of barriers to behavioral health treatment from the challenge of helping JIY complete treatment. That is, when behavioral health treatment is available and accessible (i.e., where treatment is provided through the study and JIY have been determined to be in-need of treatment), is it still difficult for JIY to complete treatment? This does not seem to be true in these studies, as the majority did complete treatment. Another aim of this investigation was to identify moderators of treatment completion. Type of treatment (i.e., family, group, individual) was a significant moderator, with treatments that provided family- or group-based treatment having higher rates of treatment completion compared to treatment groups that provided individual treatment. This is consistent with prior research findings that family-based treatments are associated with greater engagement in care [17,86]. Some have argued that the greater engagement associated with family and group-based interventions for adolescents may relate to the social components inherent to these types of interventions [87]. Adolescence, marked by many important socio-developmental milestones, typically includes dynamic changes to the role and identification of supportive others in their lives [16,88,89], and this may be particularly true for JIY [90]. For adolescents who may not have a strong, existing support network, group- and family-based interventions may be one desirable method of facilitating or improving these social connections, making them more engaging and desirable. These types of interventions may align more with helping adolescents meet important developmental milestones than individual modalities might. Even further, qualitative literature examining perspectives from youth, caregivers, treatment providers, and juvenile justice personnel consistently suggests that caregiver involvement is essential to achieve youth uptake in treatment and maintain engagement [91,92]. Thus, family-focused treatments may increase rates of treatment completion by increasing caregiver involvement and support.
Influence of Publication Bias and Study Quality
Analyses indicated some likelihood that publication bias has influenced the results; funnel plots show imputed studies with lower effect sizes than those reported by published studies, which suggests rates of treatment completion may be lower. While funnel plots should be interpreted with caution given the high level of heterogeneity present in the data [93,94], 6 studies that otherwise met eligibility criteria for inclusion in these analyses did not report full data on treatment completion and therefore could not be included in these analyses. Further, the majority of studies did not sufficiently describe withdrawals and dropouts, making it difficult to identify reasons or demographic characteristics predictive of treatment noncompletion.
Moderators not Supported by the Current Investigation
Hypotheses regarding the intervention focus (i.e., substance use disorders, conduct disorders, etc.) and racial or ethnic minority participants were not supported as moderators. In the case of intervention focus, the majority of studies (n = 15, 71.4%) were focused on addressing substance use disorders or problematic substance use, so it is possible that our analyses were underpowered to detect differences between studies with different intervention foci. It is less likely that moderator analyses of the prevalence of racial or ethnic minority participants were underpowered, given that there was a wide range of study participants who identified as racial or ethnic minorities. Previous research suggests that minority youth face significant barriers to accessing behavioral health treatment but fewer barriers when that treatment is available and accessible [20]. For example, a systematic review of literature on referrals to behavioral health services from the juvenile justice system [95] finds that a majority of the 26 articles reviewed reveal at least some evidence of racial disparities in decisions to refer youth. Thus, disparities in “utilization” may be more appropriately named disparities in access.
The inclusion of interventions to increase treatment engagement was not a significant moderator of treatment completion. Given the broad heterogeneity in treatment engagement interventions provided by studies included in this analysis, it may be important to conduct additional research assessing the success of such interventions.
Another potentially important moderator that should be examined in future studies is mandated treatment (i.e., when youth are required by the court to seek outpatient behavioral health treatment). We did not examine this as a moderator in the current study since only 6 studies reported information about whether or not youth were court-mandated to engage in behavioral health treatment. Of the 6 that reported on treatment mandates, results were highly heterogeneous (i.e., 42–100%). Literature on the effectiveness of court mandates for outpatient treatment is mixed and may depend in particular on the variability of court mandates by jurisdiction [24,96]. However, recent research [97] found that youth who attended treatment at court-direction (compared to voluntarily) demonstrated higher rates of SUD treatment completion; this variable should be further examined as a possible moderator in future research. One limitation of this analysis is that, due to the small number of control groups providing services as usual that reported data on treatment completion (k = 2), we were unable to consider experimental treatment group as a moderator of treatment completion. It is important for studies examining treatment completion in JIY to report this data for all treatment groups. Future systematic reviews should consider this factor in their analyses.
Implications and Recommendations for the Future
Overall, our findings suggest that existing high-quality studies of behavioral health treatment among JIY have generally achieved high rates of treatment completion. While included studies were not limited by presenting problem, all the studies included in this meta-analysis examine treatment of either substance use or problematic sexual behavior. Notably, the majority of treatments provided in these studies (Multisystemic Therapy, MET-CBT, Multidimensional Family Therapy) are not specific to inappropriate sexual behavior or substance use and are frequently provided to youth and families with a broad range of diagnoses. Thus, we expect that these results are generalizable to many JIY and families receiving behavioral healthcare. However, it is likely helpful for the field to consider what the effectiveness of other evidence-based practices (e.g., behavioral activation) may look like for JIY. Expanding access to evidence-based treatment and helping youth and their families remain engaged in services will both be critical challenges for researchers, policymakers, juvenile justice professionals, and community mental health administrators. Based on the results of our systematic review and meta-analysis, we make three recommendations for future research, implementation, and practice of behavioral health interventions for JIY:
1. Researchers should place a greater focus on measuring and reporting treatment completion. This includes thoroughly describing dropouts and withdrawals and reporting treatment completion or “dose” criteria, to ensure that estimates of treatment efficacy are not confounded by youth engaging in different amounts of treatment.
2. Given the potentially important role that treatment mandates play in the referral of JIY to behavioral health treatment, researchers should attempt to document the nature of youth’s justice involvement and whether they have been mandated to participate in outpatient treatment (even if study participation is not mandatory).
3. Researchers should consider utilizing interventions that include family- or group-based services to improve rates of treatment completion.
Acknowledgements
This project was made possible in part by a pre-doctoral fellowship awarded to AJK by the National Institute on Drug Abuse (F31DA054721). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Supplementary material
For supplementary material accompanying this paper visit https://doi.org/10.1017/cts.2022.418.
click here to view supplementary material
Disclosures
All authors have no conflict of interest to declare.
References
- 1. Wasserman GA, McReynolds LS, Ko SJ, Katz LM, Carpenter JR. Gender differences in psychiatric disorders at juvenile probation intake. American Journal of Public Health 2005; 95(1): 131–137. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Wasserman GA, McReynolds LS, Schwalbe CS, Keating JM, Jones SA. Psychiatric disorder, comorbidity, and suicidal behavior in juvenile justice youth. Criminal Justice and Behavior 2010; 37(12): 1361–1376. [Google Scholar]
- 3. Henggeler SW, Clingempeel WG, Brondino MJ, Pickrel SG. Four-Year follow-up of multisystemic therapy with substance-abusing and substance-dependent juvenile offenders. Journal of the American Academy of Child & Adolescent Psychiatry 2002; 41(7): 868–874. [DOI] [PubMed] [Google Scholar]
- 4. Kandel DB. Stages and Pathways of Drug Involvement: Examining the Gateway Hypothesis. Cambridge: Cambridge University Press, 2002. [Google Scholar]
- 5. Mutter R, Ali MM, Smith K, Strashny A. Factors associated with substance use treatment completion in residential facilities. Drug and Alcohol Dependence 2015; 154: 291–295. [DOI] [PubMed] [Google Scholar]
- 6. Kretschmar JM, Butcher F, Flannery DJ, Singer MI. Diverting juvenile justice-involved youth with behavioral health issues from detention: preliminary findings from Ohio’s Behavioral Health Juvenile Justice (BHJJ) initiative. Criminal Justice Policy Review 2016; 27(3): 302–325. [Google Scholar]
- 7. Aarons GA, Brown SA, Garland AF, Hough RL. Race/ethnic disparity and correlates of substance abuse service utilization and juvenile justice involvement among adolescents with substance use disorders. Journal of Ethnicity in Substance Abuse 2004; 3(1): 47–64. [Google Scholar]
- 8. Yonek JC, Dauria EF, Kemp K, Koinis-Mitchell D, Marshall BDL, Tolou-Shams M. Factors associated with use of mental health and substance use treatment services by justice-involved youths. Psychiatric Services 2019; 70(7): 586–595. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Silovsky JF, Hunter MD, Taylor EK. Impact of early intervention for youth with problematic sexual behaviors and their caregivers. Journal of Sexual Aggression 2019; 25(1): 4–15. [Google Scholar]
- 10. Henderson CE, Wevodau AL, Henderson SE, et al. An independent replication of the Adolescent-Community Reinforcement Approach with justice-involved youth. The American Journal on Addiction 2016; 25(3): 233–240. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Burrow-Sanchez JJ, Minami T, Hops H. Cultural Accommodation of group substance abuse treatment for latino adolescents: results of an RCT. Cult Divers Ethn Minor Psychol 2015; 21(4): 571–583. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. Yeterian JD, Greene MC, Bergman BG, Kelly JF. Does mandated treatment benefit youth? A prospective investigation of adolescent justice system involvement, treatment motivation, and substance use outcomes. Alcoholism Treatment Quarterly 2013; 31(4): 431–449. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13. SAMHSA. Treatment Episode Data Set (TEDS): 2017 Admissions to and Discharges from Publicly-Funded Substance Use Treatment. Rockville, MD: Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration, 2019. [Google Scholar]
- 14. Johnson ME, Tran DX. Factors associated with substance use disorder treatment completion: a cross-sectional analysis of justice-involved adolescents. Substance Abuse Treatment, Prevention, and Policy 2020; 15(92): 1–11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. Cohen DJ, Crabtree BF, Etz RS, et al. Fidelity versus flexibility: translating evidence-based research into practice. American Journal of Preventive Medicine 2008; 35(5): S381–S389. [DOI] [PubMed] [Google Scholar]
- 16. Kim H, Munson MR, McKay MM. Engagement in mental health treatment among adolescents and young adults: a systematic review. Child and Adolescent Social Work Journal 2012; 29(3): 241–266. [Google Scholar]
- 17. Dakof GA, Tejeda M, Liddle HA. Predictors of engagement in adolescent drug abuse treatment. Journal of the American Academy of Child and Adolescent Psychiatry 2001; 40(3): 274–281. [DOI] [PubMed] [Google Scholar]
- 18. Ford J, Blaustein M. Systemic self-regulation: a framework for trauma-informed services in residential juvenile justice programs. Journal of Family Violence 2013; 28(7): 665–677. [Google Scholar]
- 19. Loyd AB, Hotton AL, Walden AL, Kendall AD, Emerson E, Donenberg GR. Associations of ethnic/racial discrimination with internalizing symptoms and externalizing behaviors among juvenile justice-involved youth of color. Journal of Adolescence 2019; 75: 138–150. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Alegria M, Carson NJ, Goncalves M, Keefe K. Disparities in treatment for substance use disorders and co-occurring disorders for ethnic/racial minority youth. Journal of the American Academy of Child & adolescent Psychiatry 2011; 50(1): 22–31. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Rawal P, Romansky J, Jenuwine M, Lyons JS. Racial differences in the mental health needs and service utilization of youth in the juvenile justice system. The Journal of Behavioral Health Services & Research 2004; 31(3): 242–254. [DOI] [PubMed] [Google Scholar]
- 22. Whaley AL. Cultural mistrust and mental health services for African Americans: a review and meta-analysis. The Counseling Psychologist 2001; 29(4): 513–531. [Google Scholar]
- 23. Marlowe DB. Adult and Juvenile Drug Courts. Handbook of Evidence-Based Substance Abuse Treatment in Criminal Justice Settings. New York: Springer, 2011. pp. 123–142. [Google Scholar]
- 24. Stein DM, Deberard S, Homan K. Predicting success and failure in juvenile drug treatment court: a meta-analytic review. Journal of Substance Abuse Treatment 2013; 44(2): 159–168. [DOI] [PubMed] [Google Scholar]
- 25. Abrams LS. Juvenile justice at a crossroads: science, evidence, and twenty-first century reform. Social Service Review 2013; 87(4): 725–752. [Google Scholar]
- 26. Tolou-Shams M, Dauria E, Conrad SM, Kemp K, Johnson S, Brown LK. Outcomes of a family-based HIV prevention intervention for substance using juvenile offenders. Journal of Substance Abuse Treatment 2017; 77: 115–125. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. Henggeler SW, Halliday-Boykins CA, Cunningham PB, Randall J, Shapiro SB, Chapman JE. Juvenile drug court: Enhancing outcomes by integrating evidence-based treatments. Journal of Consulting and Clinical Psychology 2006; 74(1): 42–54. [DOI] [PubMed] [Google Scholar]
- 28. Henggeler SW, McCart MR, Cunningham PB, Chapman JE. Enhancing the effectiveness of juvenile drug courts by integrating evidence-based practices. Journal of Consulting and Clinical Psychology 2012; 80(2): 264–275. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29. Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Medicine 2009; 6(7): e1000100. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30. Moher D, Liberati A, Tetzlaff J, Altman DG, Group TP. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Medicine 2009; 6(7): e1000097. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31. Belenko S, Knight D, Wasserman GA, et al. The Juvenile Justice Behavioral Health Services Cascade: a new framework for measuring unmet substance use treatment services needs among adolescent offenders. Journal of Substance Abuse Treatment 2017; 74: 80–91. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32. Belenko S, Dembo R. Treating adolescent substance abuse problems in the juvenile drug court. International Journal of Law and Psychiatry 2003; 26(1): 87–110. [DOI] [PubMed] [Google Scholar]
- 33. Caldwell MF, Van Rybroek G. Effective treatment programs for violent adolescents: Programmatic challenges and promising features. Aggression & Violent Behavior 2013; 18(5): 571–578. [Google Scholar]
- 34. Carney T, Myers B. Effectiveness of early interventions for substance-using adolescents: Findings from a systematic review and meta-analysis. Substance Abuse Treatment, Prevention, and Policy 2012; 7: 1–15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35. Chassin L. Juvenile justice and substance use. Future Child 2008; 18(2): 165–183. [DOI] [PubMed] [Google Scholar]
- 36. Dauria EF, McWilliams MA, Tolou-Shams M. Substance use prevention and treatment interventions for court-involved, non-incarcerated youth. In: Monti PM, Colby SM, Tevyaw TOL, eds. Brief Interventions for Adolescent Alcohol and Substance Abuse. New York, NY: The Guilford Press, 2018, pp. 213–241. [Google Scholar]
- 37. Dembo R, Livingston S, Schmeidler J. Treatment for drug-involved youth in the juvenile justice system. In: Leukefeld CG, Tims F, Farabee D, eds. Treatment of Drug Offenders: Policies and Issues. New York, NY: Springer Publishing Company, 2002, pp. 226–239. [Google Scholar]
- 38. Evans-Chase M, Zhou HQ. A systematic review of the juvenile justice intervention literature what it can (and cannot) tell us about what works with delinquent youth. Crime & Delinquency 2014; 60(3): 451–470. [Google Scholar]
- 39. Hogue A, Liddle HA. Family-based treatment for adolescent substance abuse: controlled trials and new horizons in services research. Journal of Family Therapy 2009; 31(2): 126–154. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40. Horigian VE, Anderson AR, Szapocznik J. Family-Based treatments for adolescent substance use. Child and Adolescent Psychiatric Clinics of North America 2016; 25(4): 603–628. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41. Latimer J. A meta-analytic examination of youth delinquency, family treatment, and recidivism. Canadian Journal of Criminology 2001; 43(2): 237–253. [Google Scholar]
- 42. Schwalbe CS, Gearing RE, MacKenzie MJ, Brewer KB, Ibrahim R. A meta-analysis of experimental studies of diversion programs for juvenile offenders. Clinical Psychology Review 2012; 32(1): 26–33. [DOI] [PubMed] [Google Scholar]
- 43. Thompson SJ, Pomeroy EC, Gober K. Family-Based treatment models targeting substance use and high-risk behaviors among adolescents: a review. In: Hilarski C, ed. Addiction, Assessment, and Treatment with Adolescents, Adults, and Families. Binghamton, NY: Haworth Social Work Practice Press, 2005, pp. 207–233. [Google Scholar]
- 44. Tripodi SJ, Bender K. Substance abuse treatment for juvenile offenders: a review of quasi-experimental and experimental research. Journal of Criminal Justice 2011; 39(3): 246–252. [Google Scholar]
- 45. Bender K, Tripodi SJ, Sarteschi C, Vaughn MG. A meta-analysis of interventions to reduce adolescent cannabis use. Research on Social Work Practice 2011; 21: 153–164. [Google Scholar]
- 46. Trupin E. Evidence-based treatment for justice-involved youth. In: CL Kessler, LJ Kraus, eds. The Mental Health Needs of Young Offenders: Forging Paths Toward Reintegration and Rehabilitation. New York, NY: Cambridge University Press, 2007, pp. 340–367. [Google Scholar]
- 47. Woolfenden SR, Williams K, Peat JK. Family and parenting interventions for conduct disorder and delinquency: a meta-analysis of randomised controlled trials. Archives of Disease in Childhood 2002; 86(4): 251–256. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48. Briscoe S, Bethel A, Rogers M. Conduct and reporting of citation searching in Cochrane systematic reviews: a cross-sectional study. Research Synthesis Methods 2020; 11(2): 169–180. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49. Lipsey MW, Wilson D. Practical Meta-Analysis. 1st ed. Thousand Oaks, CA: SAGE Publications, Inc. 2000. [Google Scholar]
- 50. Card NA. Applied Meta-Analysis for Social Science Research. New York; London: The Guilford Press, 2015. [Google Scholar]
- 51. Ma L-L, Wang Y-Y, Yang Z-H, Huang D, Weng H, Zeng X-T. Methodological quality (risk of bias) assessment tools for primary and secondary medical studies: what are they and which is better? Military Medical Research 2020; 7: 1–11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52. Zeng X, Zhang Y, Kwong JSW, et al. The methodological quality assessment tools for preclinical and clinical studies, systematic review and meta-analysis, and clinical practice guideline: a systematic review. Journal of Evidence-Based Medicine 2015; 8(1): 2–10. [DOI] [PubMed] [Google Scholar]
- 53. Moja LP, Telaro E, D’Amico R, Moschetti I, Coe L, Liberati A. Assessment of methodological quality of primary studies by systematic reviews: results of the metaquality cross sectional study. BMJ 2005; 330(7499): 1053. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54. McMurran M, Ward T. Treatment readiness, treatment engagement and behaviour change. Criminal Behaviour and Mental Health 2010; 20(2): 75–85. [DOI] [PubMed] [Google Scholar]
- 55. Garnick DW, Lee MT, O’Brien PL, et al. The Washington circle engagement performance measures’ association with adolescent treatment outcomes. Drug and Alcohol Dependence 2012; 124(3): 250–258. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56. Balduzzi S, Rücker G, Schwarzer G. How to perform a meta-analysis with R: a practical tutorial. Evidence-Based Mental Health 2019; 22(4): 153–160. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57. Viechtbauer W. Conducting meta-analyses in R with the metafor package. Journal of Statistical Software 2010; 36(3): 1–48. [Google Scholar]
- 58. Team RC. R: A Language and Environment for Statistical Computing. Vienna, R Foundation for Statistical Computing. 2013. [Google Scholar]
- 59. Schwarzer G, Chemaitelly H, Abu-Raddad LJ, Rücker G. Seriously misleading results using inverse of Freeman-Tukey double arcsine transformation in meta-analysis of single proportions. Research Synthesis Methods 2019; 10(3): 476–483. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60. Clopper CJ, Pearson ES. The use of confidence or fiducial limits illustrated in the case of the binomial. Biometrika 1934; 26(4): 404–413. [Google Scholar]
- 61. Trikalinos TA, Trow P, Schmid CH. Simulation-Based Comparison of Methods for Meta-Analysis of Proportions and Rates. Rockville, MD: Agency for Healthcare Research and Quality (US), 2013. [PubMed] [Google Scholar]
- 62. Lin L, Chu H. Meta-analysis of proportions using generalized linear mixed models. Epidemiology 2020; 31(5): 713–717. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63. Hamza TH, van Houwelingen HC, Stijnen T. The binomial distribution of meta-analysis was preferred to model within-study variability. Journal of Clinical Epidemiology 2008; 61(1): 41–51. [DOI] [PubMed] [Google Scholar]
- 64. Baker R, Jackson D. A new approach to outliers in meta-analysis. Health Care Management Science 2008; 11(2): 121–131. [DOI] [PubMed] [Google Scholar]
- 65. Viechtbauer W, Cheung MW-L. Outlier and influence diagnostics for meta-analysis. Research Synthesis Methods 2010; 1(2): 112–125. [DOI] [PubMed] [Google Scholar]
- 66. Huedo-Medina TB, Sánchez-Meca J, Marín-Martínez F, Botella J. Assessing heterogeneity in meta-analysis: Q statistic or I2 index? Psychological Methods 2006; 11(2): 193–206. [DOI] [PubMed] [Google Scholar]
- 67. Fazel S, Doll H, Långström N. Mental disorders among adolescents in juvenile detention and correctional facilities: a systematic review and metaregression analysis of 25 surveys. Journal of the American Academy of Child & Adolescent Psychiatry 2008; 47(9): 1010–1019. [DOI] [PubMed] [Google Scholar]
- 68. Borenstein M, Higgins J. Meta-analysis and subgroups. Prevention Science 2013; 14: 134–143. [DOI] [PubMed] [Google Scholar]
- 69. CMA. Comprehensive Meta-Analysis Version 3 [Computer Program]. Englewood, NJ: Biostat, 2013. [Google Scholar]
- 70. Sagie A, Koslowsky M. Detecting moderators with meta-analysis: an evaluation and comparison of techniques. Personnel Psychology 1993; 46(3): 629–640. [Google Scholar]
- 71. Borenstein M, Hedges L, Higgins J, Rothstein H. Introduction to Meta-Analysis. Chichester, UK: John Wiley & Sons, 2009. [Google Scholar]
- 72. Egger M, Davey Smith G, Altman D. Systematic Reviews in Health Care: Meta-Analysis in Context. London: BMJ Publishing Group, 2001. [Google Scholar]
- 73. Duval S, Tweedie R. A nonparametric “trim and fill” method of accounting for publication bias in meta-analysis. Journal of the American Statistical Association 2000; 95(449): 89–98. [Google Scholar]
- 74. Begg CB, Mazumdar M. Operating characteristics of a rank correlation test for publication bias. Biometrics 1994; 50(4): 1088–1101. [PubMed] [Google Scholar]
- 75. Borduin CM, Schaeffer CM, Heiblum N. A randomized clinical trial of multisystemic therapy with juvenile sexual offenders: effects on youth social ecology and criminal activity. Journal of Consulting and Clinical Psychology 2009; 77: 26–37. [DOI] [PubMed] [Google Scholar]
- 76. Dakof GA, Henderson CE, Rowe CL, et al. A randomized clinical trial of family therapy in juvenile drug court. Journal of Family Psychology 2015; 29(2): 232–241. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77. Henggeler SW, Pickrel SG, Brondino MJ. Multisystemic treatment of substanceabusing and dependent delinquents: outcomes, treatment fidelity, and transportability. Mental Health Services Research 1999; 1: 171–184. [DOI] [PubMed] [Google Scholar]
- 78. Kaminer Y, Ohannessian C, Burke R. Retention and treatment outcome of youth with cannabis use disorder referred by the legal system. Adolescent Psychiatry 2019; 9(1): 4–10. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79. Letourneau EJ, Henggeler SW, Borduin CM, et al. Multisystemic therapy for juvenile sexual offenders: 1-year results from a randomized effectiveness trial. Journal of Family Psychology 2009; 23: 89–102. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80. Schaeffer CM, Henggeler SW, Ford JD, Mann M, Chang R, Chapman JE. RCT of a promising vocational/employment program for high-risk juvenile offenders. Journal of Substance Abuse Treatment 2014; 46(2): 134–143. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81. Sharkey JD, Sander JB, Jimerson SR. Acculturation and mental health: Response to a culturally-centered delinquency intervention. Journal of Criminal Justice 2010; 38(4): 827–834. [Google Scholar]
- 82. Walker SC, Duong M, Hayes C, et al. A tailored cognitive behavioral program for juvenile justice-referred females at risk of substance use and delinquency: a pilot quasi-experimental trial. PLoS One 2019; 14(11): e0225150. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83. Peters JL, Sutton AJ, Jones DR, Abrams KR, Rushton L. Performance of the trim and fill method in the presence of publication bias and between-study heterogeneity. Statistics in Medicine 2007; 26(25): 4544–4562. [DOI] [PubMed] [Google Scholar]
- 84. Jackson D. The implications of publication bias for meta-analysis’ other parameter. Statistics in Medicine 2006; 25(17): 2911–2921. [DOI] [PubMed] [Google Scholar]
- 85. Ioannidis JP, Trikalinos TA. The appropriateness of asymmetry tests for publication bias in meta-analyses: a large survey. Cmaj 2007; 176(8): 1091–1096. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 86. Coatsworth JD, Santisteban DA, McBride CK, Szapocznik J. Brief strategic family therapy versus community control: engagement, retention, and an exploration of the moderating role of adolescent symptom severity. Family Process 2001; 40(3): 313–332. [DOI] [PubMed] [Google Scholar]
- 87. Bolton Oetzel K, Scherer DG. Therapeutic engagement with adolescents in psychotherapy. Psychotherapy: Theory, Research, Practice, Training 2003; 40(3): 215. [Google Scholar]
- 88. Noam GG. The psychology of belonging: reformulating adolescent development. In: Esman AH, Flaherty LT, Horowitz HA, eds. Adolescent Psychiatry: Development and Clinical Studies. Mahwah, NJ: Analytic Press, 1999, vol. 24, pp. 49–68. [Google Scholar]
- 89. Remschmidt H. Psychosocial milestones in normal puberty and adolescence. Hormone Research in Paediatrics 1994; 41(2): 19–29. [DOI] [PubMed] [Google Scholar]
- 90. Zwecker NA, Harrison AJ, Welty LJ, Teplin LA, Abram KM. Social support networks among delinquent youth: an 8-year follow-up study. Journal of Offender Rehabilitation 2018; 57(7): 459–480. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 91. Elkington KS, Lee J, Brooks C, Watkins J, Wasserman GA. Falling between two systems of care: Engaging families, behavioral health and the justice systems to increase uptake of substance use treatment in youth on probation. Journal of Substance Abuse Treatment 2020; 112: 49–59. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 92. Mauro PM, McCart MR, Sheidow AJ, Naeger SE, Letourneau EJ. Parent and youth engagement in court-mandated substance use disorder treatment. Journal of Child & Adolescent Substance Abuse 2017; 26(4): 324–331. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 93. van Assen MA, van Aert RC, Wicherts JM. Meta-analysis using effect size distributions of only statistically significant studies. Psychological Methods 2015; 20(3): 293–209. [DOI] [PubMed] [Google Scholar]
- 94. Terrin N, Schmid CH, Lau J, Olkin I. Adjusting for publication bias in the presence of heterogeneity. Statistics in Medicine 2003; 22(13): 2113–2126. [DOI] [PubMed] [Google Scholar]
- 95. Spinney E, Yeide M, Feyerherm W, Cohen M, Stephenson R, Thomas C. Racial disparities in referrals to mental health and substance abuse services from the juvenile justice system: a review of the literature. Journal of Crime and Justice 2016; 39(1): 153–173. [Google Scholar]
- 96. Stein DM, Homan KJ, Berard S. The effectiveness of juvenile treatment drug courts: a meta-analytic review of literature. Journal of Child & Adolescent Substance Abuse 2015; 24(2): 80–93. [Google Scholar]
- 97. Johnson ME, Tran DX. Factors associated with substance use disorder treatment completion: a cross-sectional analysis of justice-involved adolescents. Substance Abuse Treatment, Prevention, and Policy 2020; 15(1): 1–11. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
For supplementary material accompanying this paper visit https://doi.org/10.1017/cts.2022.418.
click here to view supplementary material