Abstract
Background and objectives
Bilateral quadratus lumborum block has been described for major abdominal procedures when sepsis is present, because risks associated to epidural are considered elevated. In an open aortic surgery, a single-shot bilateral quadratus lumborum block type 1 may be an alternative to thoracic epidural block for post-operative analgesia in a patient having an increased cumulative risk for thoracic epidural hematoma.
Case report
A 56-year-old female patient presenting controlled hypertension, chronic renal disease stage 3b, dyslipidemia and a platelet count of 102,000/μl, and taking aspirin, was scheduled for bilateral aortoiliac endarterectomy. She was submitted to a sole general anesthesia plus, at end of the surgery, a bilateral quadratus lumborum block type 1 for post-operative analgesia with 20 mL of ropivacaine 0.5%, per side, before extubation. Immediately after post anesthesia care unit admission, patient developed moderate hypotension (dopamine infusion was needed during 18 h), concomitantly with a rapid reduction in the pain scores. Low numeric rating scale and opioid consumption were noted, particularly in the first 24 h post-operatively.
Conclusions
Quadratus lumborum block was an effective analgesic technique for open aortic surgery in this case, although hypotension associated to bilateral quadratus lumborum block type 1 may occur. Associated sympathetic block probably related to the bilateral paravertebral extension of the block, may contribute for post-operative hypotension associated to reperfusion-ischemia syndrome in a patient that had long-lasting intraoperative aortic cross-clamping. The use of high concentration of local anesthetic to obtain longer duration of action of a single-shot quadratus lumborum block to avoid thoracic epidural or bilateral quadratus lumborum block catheterization should be used judiciously.
Keywords: Quadratus lumborum block, Open aortic surgery, Hypotension
Resumo
Justificativa e objetivos
O bloqueio bilateral do quadrado lombar foi descrito para procedimentos abdominais de grande porte quando há presença de sepse, uma vez que os riscos associados à peridural são considerados altos. Em uma cirurgia aórtica aberta, um único bloqueio bilateral do quadrado lombar tipo 1 (QL tipo 1) pode ser uma opção ao bloqueio peridural torácico para analgesia pós-operatória em paciente com risco cumulativo aumentado de hematoma epidural torácico.
Relato de caso
Paciente feminina de 56 anos, portadora de hipertensão arterial controlada, doença renal crônica (estágio 3b), dislipidemia, plaquetopenia de 102.000/μl e tomava aspirina, estava programada para endarterectomia aortoilíaca bilateral. A paciente foi submetida à anestesia geral e, no fim da cirurgia, a bloqueio do quadrado lombar tipo 1 bilateralmente para analgesia pós-operatória com 20 mL de ropivacaína a 0,5%, para cada lado, antes da extubação. Imediatamente após a internação na sala de recuperação pós-anestésica, a paciente evoluiu com hipotensão moderada (necessidade de infusão de dopamina durante 18 horas), concomitante à rápida redução dos escores de dor. Escore numérico para dor baixo e consumo de opioides foram observados, especialmente nas primeiras 24 horas de pós-operatório.
Conclusões
O bloqueio do quadrado lombar foi uma técnica analgésica eficaz nesse caso de cirurgia aórtica aberta, embora a hipotensão associada ao bloqueio bilateral do quadrado lombar possa ocorrer. O bloqueio simpático associado, causado pelo bloqueio do QL tipo 1, provavelmente relacionado à extensão paravertebral bilateral do bloqueio, pode contribuir para a hipotensão pós-operatória associada à síndrome de isquemia-reperfusão em paciente submetido a pinçamento aórtico intraoperatório de longa duração. Alta concentração de anestésico local para prolongar a ação de uma injeção única no bloqueio do quadrado lombar, com o objetivo de evitar cateterização de ambas anestesias peridural e do quadrado lombar bilateral, deve ser usada de modo criterioso.
Palavras chave: Bloqueio do quadrado lombar, Cirurgia aórtica aberta, Hipotensão
Introduction
We describe a bilateral Quadratus Lumborum Block Type 1 (QLB1) for post-operative analgesia in an open aortic surgery case, as an alternative to thoracic epidural block in a patient presenting an increased cumulative risk for epidural hematoma. QLB1 blocks T6 to L1 dermatomes, at least, thus having the potential to cover the entire sensitive innervation of the abdominal wall and, differently from other TAP blocks; they also block visceral afferent pathways to the spinal cord, through the paravertebral extension of the blockade. These techniques may be very important in major abdominal vascular surgery in selected patients, but the risks associated to bilateral extension of the paravertebral blockade may exist.
A written consent from the patient for publication was obtained.
Case report
A woman, aging 56-year-old, ASA III, weighting 60 kg, was a massive smoker. She suffered from chronic progressive ischemia of lower limbs, caused by left common iliac artery occlusion, and pre-occlusive stenosis of right common iliac artery.
Other comorbidities were controlled hypertension, chronic renal disease stage 3b, dyslipidemia and mild chronic thrombocytopenia.
She was scheduled for bilateral aortoiliac endarterectomy. Patient suspended clopidogrel 75 mg 2 weeks before surgery and kept aspirin 100 mg until surgery's day. Relevant pre-operative evaluation: platelet count: 102,000/μl, creatinine clearance 37.1 mL.min−1.
Despite absence of absolute contraindication, considering the risk for thoracic epidural in this context, it was planned to perform a sole general anesthesia plus, at end of surgery, a bilateral single-shot QLB1 for post-operative analgesia.
Intraoperative management
Antibiotic prophylaxis was administered before induction (Cefazolin 2000 mg). Induction of anesthesia and intubation were performed with Fentanyl 0.15 mg, Propofol 120 mg, and Rocuronium 50 mg. A standard ASA (American Society of Anesthesiologists) monitoring was used, including esophageal temperature measurement. After induction, an arterial line was placed in the right radial arteria – initial Arterial Pressure (AP): 130/70 mmHg. A right subclavian central line was also placed and central venous pressure was monitored (4–6 mmHg throughout surgery). Anesthesia was maintained with a Propofol 1% infusion (5–7.5 mg.kg−1.h−1), and a remifentanil infusion (0.35–0.6 μg.kg−1.min−1).
A surgical sagittal incision from T6 to T12 incision was done. Two hours after induction 5000 UI of unfractioned heparin was administered. Before infrarenal aortic cross-clamping, a restrictive fluid strategy and a moderate permissive hypotension were kept. During cross-clamping (duration: 1.5 h) a labetalol infusion (20 mg.h−1) was started after a bolus of 10 mg. Unclamping was anticipated: 2000 cc of crystalloids were given. After unclamping, no vasopressor infusion was needed, despite patient has received 0.3 mg of phenylephrine to normalize AP. Intraoperative total blood loss was 500 cc. Urinary output during surgery was about 2 mL.kg−1.h−1. Remifentanil was stopped 30 min before extubation and morphine 4 mg IV, metamizol 2000 mg IV, paracetamol 1000 mg IV, ondansetron 4 mg IV were administered. No additional analgesia was given, and propofol infusion was maintained up to the beginning of emergence from anesthesia. At the end of surgery patient was hemodynamically stable. After assessing again the risks of a thoracic epidural catheter (4 h have passed since last administration of unfractioned heparin), we performed a QLB1 as the primary analgesic technique at the end of surgery (15 min before extubation).
The patient was kept in dorsal decubitus. Alternately, both sides were lifted by a small pillow, and abdominal wall was pushed to the opposite side by an assistant to facilitate puncture and progression of the needle.
The bilateral US-guided QLB1 was performed with 20 mL of Ropivacaine 0.5%, per side, using a 21G 85 mm needle (echoplex, Vigon®), with a linear probe (frequency: 12 MHz) and the Acuson® P300 ultrasound system, under aseptic technique.
The 3 muscle layers of the anterior abdominal wall were identified (Supplementary material Video 1). The fascia surrounding the transversus abdominis muscle was tracked posteriorly to its origin (probe positioned in anteroposterior direction), where the transversus abdominis muscle merges with the Thoracolumbar Fascia (TLF), which surrounds the Quadratus Lumborum muscle (QL) through its anterior and middle layers (Fig. 1 and Supplementary material Video 1).
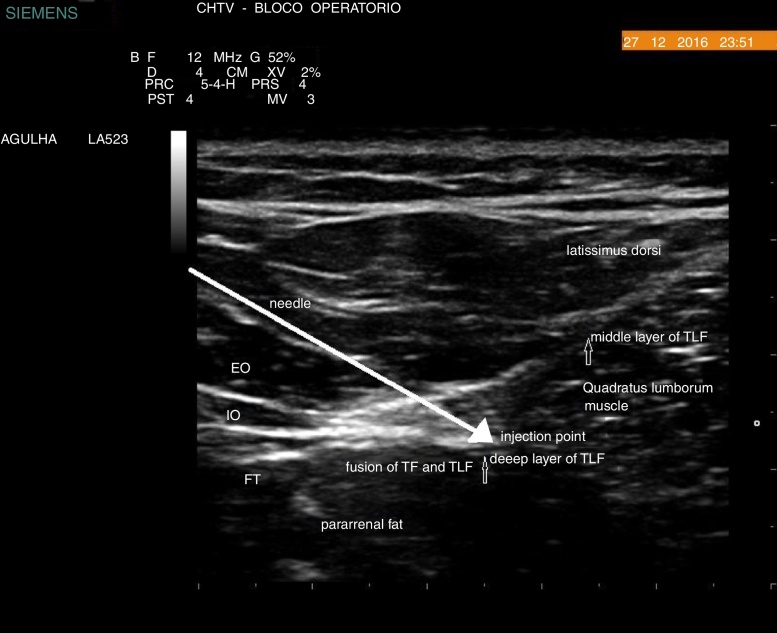
Figure 1.
Sonoanatomy of quadratus lumborum block Type 1. TFL, thoracolumbar fascia; FT, fascia transversalis; IO, internal oblique muscle; EO, external oblique muscle.
We visualized the injection spreading in the anterior surface of Quadratus Lumborum (QL) posteriorly to the anterior layer of TLF (QLB1), placing the needle in-plane (skin puncture at the level of L3, at the medium axillar line, directed medially and posteriorly, in an angle of 30° to the anterior skin). In this patient injection site depth was 3.5 cm.
After 200 mg of sugammadex was given (total rocuronium: 80 mg) patient was extubated and transferred to PACU. At admission to PACU, 20 min before bilateral QLB, patient developed moderate hypotension (minimum 90/50 mmHg). Fluids were administered and dopamine infusion (200 mg.50 cc−1) was started, at 4 μg.kg.−1min−1, after a bolus of phenylephrine (0.2 mg). Urine output was stable.
This event occurred concomitantly with a progressive reduction of pain (NRS 7/10 at extubation, and NRS 0/10 ten minutes after PACU admission). No surgical complications were noted. Dopamine infusion was progressively withdrawn during 18 h.
After QLB1, the patient had a reduction in the ability to feel cold bilaterally during 4–6 h. Patient examination revealed sensory level T3–L1, from right side, and T4–L1, in the opposite side.
She remained in PACU for 24 h (pain was evaluated hourly). During this period pain NRS was always 0–1. During the first 18 h patient received paracetamol 1000 mg IV twice, and only a total of 4 (2 + 2) mg of morphine IV were given to obtain optimal analgesia (NRS 0). In PACU morphine IV was given as patient was under continuous monitoring. In the next 6 h patient required 2 mg of morphine to obtain a NRS 0.
In the ward it was prescribed paracetamol IV 3id, tramadol 100 mg IV 3id, and metamizol 2000 mg IV bid, and meperidine 50 mg IM (rescue). Pain was assessed every 8 h. Patient presented only mild pain (NRS 2–3/10) between 24 h and 48 h post-operatively at rest (meperidine was administered once).
Between 48 h and 72 h a pain NRS was 2/10, at rest and movement. After this period, patient presented NRS 0–1 until discharge, at rest and movement.
Patient tolerated liquid and solid ingestion during the hospital stay and started ambulation 72 h after procedure. No ileus was reported. No significant aggravation of renal failure has occurred. Patient was discharged 10 days after intervention.
Discussion
Thoracic epidural catheters may bring some major complications such as hypotension, post-dural puncture headache, direct neural injury, epidural hematoma, meningitis and epidural abcess.1
Previously studies have documented a higher rate of epidural hematoma associated to thoracic epidural when compared to lumbar epidural.1
In open aortic surgery it is planned to administer intraoperative unfractioned heparin before aortic cross-clamping. Major bleeding and coagulation disorders are frequent, particularly if prolonged cross-clamping is necessary. Additionally, this patient was under aspirin, and had an initial platelet count of 102,000/μl. A post-operative decompensation of renal function may occur in a pre-existing renal disease, after aortic cross-clamp. Cumulatively, all these factors may increase the risk of epidural hematoma.
In this scenario, some anesthesiologists may not feel comfortable to place a thoracic epidural, and opt for a sole GA, despite the benefits of a combined technique.2
Lumbar epidural has not shown to be sufficiently effective in open aortic surgery to reduce cardiac risk as thoracic epidural, probably because a sympathetic activation above the level of blockade may occur.2
LA action lasts long perineurally than epidurally. We used high concentrations of LA that we cannot use in a thoracic epidural, for post-operative analgesia.
With this option we intended to avoid the placement of catheters, and we could obtain long-lasting analgesia with a single bolus per side, with some degree of thoracic paravertebral blockade. There is not an absolute contraindication for this block or thoracic epidural block, but the consequences of a hematoma will be less severe in the QLB1.
We used QLB1,3 because it is feasible in supine position, which is certainly a major advantage when bilateral techniques are necessary.
The QL is covered by the Transversalis Fascia (TF) and the Thoracolumbar Fascia (TLF), which shares the same embryologic origin. Cadaveric anatomical studies have demonstrated the continuity of the deepest layer of TLF up to cervical level.4
QLB1 blocks, at least, T6 to L1 dermatomes.5 It was demonstrated that QLB1 may produce blockade up to T4, but, at maximum, until L2, caudally.5 In 2011, Carney et al. observed posterior spread of contrast, using a QLB, to the paravertebral space from the fifth thoracic to the first lumbar vertebral level using magnetic resonance imaging, which can produce visceral analgesia but carries the risk of sympathetic blockade and hypotension.5
In our practice we have notice that loss of temperature sensation in some cases up to T2 using 20 mL of ropivacaine 0.5%, particularly if the block is done at end of surgery, probably because patient mobilization or muscle contraction can squeeze the LA between QL and TLF, contributing to a higher block.
Theoretically, rostral spread of LA may be important to produce sympathetic ganglia block, reducing the risk for cardiovascular events, particularly in open aortic surgery.
In this case, prolonged hypotension observed was probably associated to a reperfusion syndrome after long-lasting aortic cross-clamping, potentiated by the abolishment of sympathetic response provoked by QLB1.
We decided to use a non-diluted dose of LA, after surgical closure, for longer duration of action, but concentrated LA may contribute for a more intense sympathetic blockade. Continuous bilateral QLB1 is hard to perform in supine position, and increase risks should be considered, including retroperitoneal hematoma in this context.
We believe that a single-shot bilateral QLB1 may constitute an alternative to thoracic epidural catheters in open aortic surgeries, only when the risks associated to catheter placement are elevated, but the use of non-diluted anesthetics in bilateral QLB, to obtain a longer duration of action may be used judiciously.
Conflicts of interest
The authors declare no conflicts of interest.
Footnotes
Supplementary data associated with this article can be found, in the online version, at doi:10.1016/j.bjane.2018.05.002.
Appendix A. Supplementary data
The following are the supplementary data to this article:
Sonoanatomy of quadratus lumborum block Type 1.
References
- 1.Freise H., Van Aken H.K. Risks and benefits of thoracic epidural anaesthesia. Br J Anaesth. 2011;107:859–868. doi: 10.1093/bja/aer339. [DOI] [PubMed] [Google Scholar]
- 2.McLeod G.A., Cumming C. Thoracic epidural anaesthesia and analgesia. Contin Educ Anaesth Crit Care Pain. 2004;4:16–19. [Google Scholar]
- 3.Børglum J., Gögenur I., Bendtsen T.F. Abdominal wall blocks in adults. Curr Opin Anaesthesiol. 2016;29:638–643. doi: 10.1097/ACO.0000000000000378. [DOI] [PubMed] [Google Scholar]
- 4.Willard F.H., Vleeming A., Schuenke M.D., et al. The thoracolumbar fascia: anatomy, function and clinical considerations. J Anat. 2012;221:507–536. doi: 10.1111/j.1469-7580.2012.01511.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Carney J., Finnerty O., Rauf J., et al. Studies on the spread of local anaesthetic solution in transverses abdominis plane blocks. Anaesthesia. 2011;66:1023–1030. doi: 10.1111/j.1365-2044.2011.06855.x. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Sonoanatomy of quadratus lumborum block Type 1.