Abstract
The discovery and the development of safe and efficient therapeutics against arthritogenic alphaviruses (e.g., chikungunya virus) remain a continuous challenge. Alkaloids are structurally diverse and naturally occurring compounds in plants, with a wide range of biological activities including beneficial effects against prominent pathogenic viruses and inflammation. In this short review, we discuss the effects of some alkaloids of three biologically relevant structural classes (isoquinolines, indoles and quinolizidines). Based on various experimental models (viral infections and chronic diseases), we highlight the immunomodulatory effects of these alkaloids. The data established the capacity of these alkaloids to interfere in host antiviral and inflammatory responses through key components (antiviral interferon response, ROS production, inflammatory signaling pathways and pro- and anti-inflammatory cytokines production) also involved in alphavirus infection and resulting inflammation. Thus, these data may provide a convincing perspective of research for the use of alkaloids as immunomodulators against arthritogenic alphavirus infection and induced inflammation.
Keywords: alkaloids, arthritogenic alphaviruses, immunomodulators, biological activity
1. Introduction
Alphaviruses (family: Togaviridae) are positive-sensed, single-stranded RNA and are related to arthropod-borne viruses (arboviruses) [1]. Arthritogenic alphaviruses are a group related to re-emergent “Old World” alphaviruses, globally distributed and genetically closed (Semliki Forest complex), including chikungunya virus (CHIKV), O’nyong-nyong virus (ONNV), Ross River virus (RRV), Barmah Forest virus (BFV), Mayaro virus (MAYV), Sindbis virus (SINV) and Semliki Forest virus (SFV), which have had recent outbreaks [2,3]. Arthritogenic alphavirus infection usually causes dengue-like symptoms (debilitating fever, rash and/or myalgia), but also severe chronic rheumatic disorders (polyarthralgia and polyarthritis) resulting from musculoskeletal inflammation [2,4].
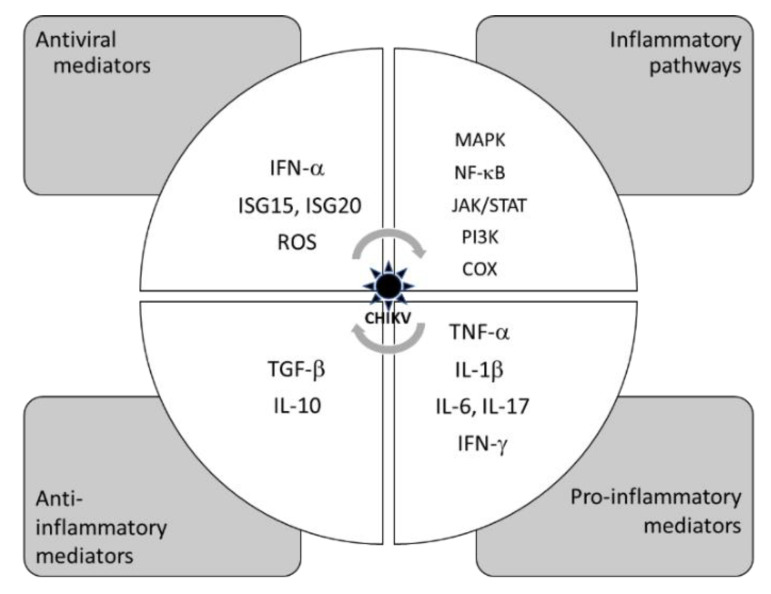
Recent knowledge on arthritogenic alphavirus infection highlighted the pivotal role of host immunity in protective antiviral and inflammatory responses but also an exuberant inflammatory response which can lead to the aforementioned severe complications [5]. As summarized in Figure 1 for the most investigated CHIKV, after viral detection and recognition, the complex immune response mainly involves the production of antiviral effectors (interferons (IFNs), interferon-stimulated genes (ISGs) and reactive oxygen species (ROS)), the release of pro-inflammatory cytokines through the activation of kinase signaling pathways (mitogen-activated protein kinase (MAPK), nuclear factor kappa B (NF-κB), Janus kinase/signal transducer and activator of transcription (JAK/STAT) or phosphoinositide 3-kinase (PI3K)) or the cyclooxygenase (COX)-dependent arachidonic cascade, and the subsequent attenuation of the inflammatory process via anti-inflammatory cytokines. The development of arthritic diseases was assumed on the viral infection of skeletal muscles and synovial tissues which upregulate pro-inflammatory cytokines (interleukin (IL)-6, tumor necrosis alpha (TNF-α) and IFN-β), as seen in patients infected with CHIKV [6], RRV [7] and MAYV [8]. Clinical data from CHIKV patients established that a robust cytokine profile is preventive to chronic joint pain during acute infection, while a low cytokine profile is predictive of chronic arthritis pathogenesis [9]. Thus, the regulation of the immune response is a key therapeutic strategy against arthritogenic alphavirus infection and induced inflammation.
Figure 1.
Simplified representation of antiviral and inflammatory components of the host immune system illustrated from cumulative experimental data for CHIKV infection and inflammation [5].
To date, there are no specific therapeutics for arthritogenic alphavirus infection and the related inflammatory diseases. For the recent investigations on CHIKV, viral inhibitors were mostly assessed using old drugs such as the broad-spectrum antiviral arbidol [10], the anti-IAV amantadine [11], the anti-trypanosomal suramin [12], the naturally occurring anti-cancer lobaric acid from the antarctic lichen Stereocaulon alpinum [13] and the antibiotic ribostamycin isolated from Streptomyces ribosidificus [14], or by designing novel synthetic series from triazolopyrimidinone [15] or thiazolidinone [16] scaffolds. Similarly, inhibitors of the essential host cell functions for the virus life cycle were evaluated with approved synthetic drugs, including the anti-malarial chloroquine (quinoline) [17], the antiparasitic atovaquone (naphthoquinone) [18] or the anti-depressant imipramine (dibenzoazepine) [19]. For the resulting inflammatory disorders, the available medications include non-steroidal anti-inflammatory drugs (NSAIDs) such as aspirin, ibuprofen or diclofenac used for the symptomatic relief of mild-to-moderate inflammation to decrease prostaglandin (PG) (e.g., PGE2) production via the inhibition of COX activity. Disease-modifying antirheumatic drugs (DMARDs), such as the well-investigated methotrexate (MTX) [20], are employed to alleviate chronic inflammation and decrease joint damage through the suppression of exuberant immune and/or inflammatory responses over the time, but without the relief of symptoms, as experienced in those with chronic CHIKV infection [21].
Immunomodulators are becoming an attractive therapeutic strategy for immune suppression and to decrease inflammation (immunosuppressants) or immune potentiation (immunostimulants) in cancer, cardiovascular, metabolic and immune-mediated inflammatory disorders or viral infections [22,23,24,25]. Immunomodulatory effects have been characterized for some antiviral compounds with prophylactic and/or therapeutic action against arthritogenic-alphavirus-induced damage, including (semi)-synthetic glycosaminoglycans mimetics such as the approved pentosane polysulfate used for the treatment of osteoarthritis [26] or the promising anticancer pixatimod previously investigated against RRV-induced cell damage [27,28], as well as tilorone (fluorenone) assessed for CHIKV [29] and earlier reported for SINV [30].
Plant-derived immunomodulators have attracted increasing interest, with a large variety of chemical classes of natural compounds [31,32,33]. Alkaloids are a large and diverse group of nitrogen-containing compounds and are specialized or ‘secondary’ metabolites [34], mainly from plants of various botanical families, and exhibit a wide range of biological activities including antiviral and/or anti-inflammatory properties [35,36,37,38,39,40,41,42]. Nowadays, more than 27,000 alkaloids have been identified, but despite their drug-like features [43,44,45,46] and their traditional medicinal use, they are currently under-represented in marketed or licensed medicines (‘drugs’) [47]. Recently, we demonstrated the immunomodulatory effects in vitro of the quinoline-derived alkaloid camptothecin [48] against ONNV. Isoquinolines, indoles and quinolizidines are major chemical classes of biologically relevant alkaloids with potent antiviral activities [44,49,50] and anti-inflammatory effects [35]. The great potential of plant-containing alkaloids to modulate viral infections and related inflammation has been recently reviewed for prominent human pathogenic viruses, e.g., human immunodeficiency virus 1 (HIV-1), Influenza A virus (IAV) and hepatitis B or C viruses (HBV or HCV) [51]. Growing interest is being paid to the immunomodulatory activity of alkaloids [42], but their beneficial effects against arthritogenic alphaviruses have been poorly investigated. We discuss here the immunomodulatory effects of some alkaloids belonging to the isoquinoline, indole or quinolizidine classes from various botanical sources (Figure 2). These compounds were selected for their activities in vitro, ex vivo and/or in vivo established against various pathogenic viruses and chronic diseases. We highlighted the recent interest in alkaloids against arthritogenic alphavirus infection, as well as their immunomodulatory effects through the foremost mechanisms involved in arthritogenic alphavirus pathogenesis.
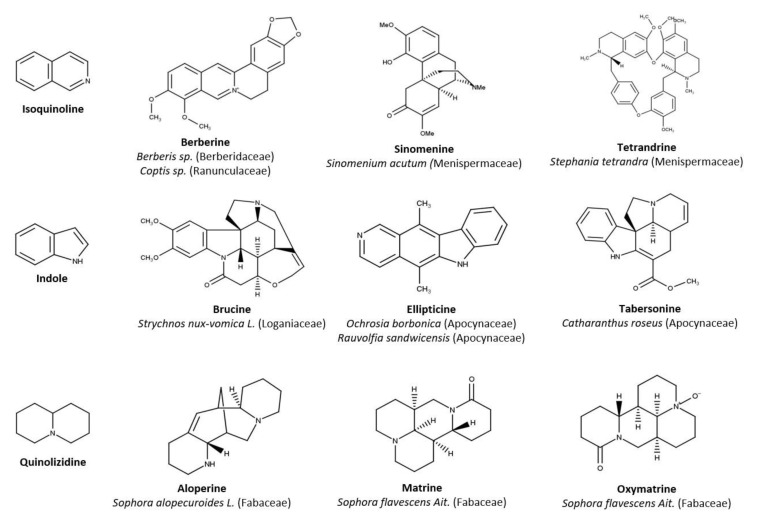
Figure 2.
Chemical structures of the selected isoquinoline-, indole- and quinolizidine-derived alkaloids with their common botanical sources. Molecules were drawn using MarvinSketch.
2. Results and Discussion
In the recent challenge of drug discovery against alphaviruses, safe and efficient immunomodulators are expected to promote both a profitable antiviral immune response and a well-balanced inflammatory response. To date, there is little evidence of natural alkaloids that may serve as such a dual and attractive therapeutic strategy. Tomatidine, a natural steroidal alkaloid, has been recently reported as a valuable antiviral compound in vitro (EC50 = 1.3 µM; CC50 = 156 µM; SI 120) against CHIKV through the inhibition of the viral production, but additional immunomodulatory effects have not been established yet [52,53,54].
From the wide structural variety of alkaloids, we focused on three major classes based on their biological importance and their pharmaceutical relevance. Isoquinolines are the most structurally diverse and widely distributed group of alkaloids and are divided into 13 major subclasses derived from the benzylisoquinoline sub-unit represented here by berberine and sinomenine, or by a dimeric form (bisbenzylisoquinoline) with tetrandrine. The great value of isoquinoline alkaloids has been recently established for their multitarget potential in multifactorial chronic health conditions including immunological, metabolic and neurologic disorders [55]. Indole alkaloids are characterized by fused benzopyrrole ring systems which create large structural variety [56]. Brucine, ellipticine and tabersonine refer to the predominant monoterpene indole alkaloids which display various biological activities including anti-infectious and cytotoxic effects [57,58]. Quinolizidines include matrine- and aloperine-type alkaloids with multieffects evidenced by their anti-inflammatory, anti-tumoral, anti-microbial, cardioprotective or anti-atherosclerosis activity [59,60].
For the nine representative compounds, experimental data were selected for their dual antiviral and/or immunomodulatory effects in various health conditions (Table 1 and Table 2).
Table 1.
Antiviral and immunomodulatory effects of alkaloids during viral infection.
| Virus | Alkaloid | Model/Tested Doses | Efficacy and/or Safety In Vitro (a) | Effect | Ref. |
|---|---|---|---|---|---|
| Viral RNA | |||||
| Influenza A virus (IAV) | Berberine | In vitro, murine macrophage-like cell (RAW 264.7)/25 μM | IC50 = 0.01 μM | Inhibits virus growth Decreases pro-inflammatory TNF-α and PGE2 |
[70] |
| Respiratory syncytial virus (RSV) | In vitro, human adenocarcinoma alveolar basal epithelial cell (A549)/25 or 100 µM | CC50 > 100 μM | Inhibits pro-inflammatory IL-6 | [71] | |
| Chikungunya virus (CHIKV) | In vitro, human osteosarcoma cell (HOS)/0.1–800 μM In vivo, mouse/10 mg/kg |
EC50 = 12.2 μM CC50 = 429.5 μM SI = 35 |
Inhibits MAPK/PI3K-AKt signaling pathways Reduces viral load and joint swelling in mice |
[72] | |
| Chikungunya virus (CHIKV), Semliki Forest virus (SFV) and Sindbis virus (SINV) | In vitro, baby hamster kidney cell (BHK)/3 µM | For CHIKV: EC50 = 1.8 μM CC50 > 100 μM SI > 27 |
Inhibits viral replication | [64] | |
| Severe acute respiratory syndrome related to Coronavirus-2 (SARS-CoV-2) | In vitro, primary human nasal epithelial cell/10 μM | EC50 = 9.1 μM CC50 > 150 μM SI > 16 |
Inhibits viral replication | [65] | |
| Severe acute respiratory syndrome related to Coronavirus-2 (SARS-CoV-2) | Matrine | In vivo, human | - | Decreases sera levels of lymphocytes and CRP | [73] |
| Hepatitis B virus (HBV) |
Oxymatrine | In vivo, mouse/200 mg/kg/day | - | Increases pro-inflammatory TH1-cytokines (IFN-γ and IL-2) Decreases anti-inflammatory TH2-cytokines (IL-4 and IL-10) |
[74] |
| Influenza A virus (IAV) | In vitro, human adenocarcinoma alveolar basal epithelial cell (A549)/190 μM In vivo, mouse/60 or 120 mg/kg |
EC50 = 64.47 μM AI = 3868.1359 |
Decreases pro-inflammatory IL-1β, IL-6, IL-8 and TNF-α Inhibits MAPK and NF-κB pathways |
[75] | |
| Hepatitis C virus (HCV) | Aloperine | In vitro, human-derived hepatoma cell (Huh 7.5)/20 μM | EC50 = 7.06 μM CC50 > 200 μM |
Inhibits virus attachment and replication Blocks viral cell-to-cell transmission |
[67] |
| Viral DNA | |||||
| Herpes virus simplex 1 and 2 (HSV-1 and HSV-2) | Berberine | In vitro, Vero cells/2400 μM | HSV-1: IC50 = 24.4 μM CC50 = 39.2 μM SI = 161 HSV-2: IC50 = 26.7 μM CC50 = 39.2 μM SI = 141 |
Inhibits viral replication and DNA synthesis | [76] |
| Human immunodeficiency virus 1 (HIV-1) | In vitro, T cells containing a plasmid encoding the green fluorescent protein (CEM-GFP)/0.29 μM | IC50 = 0.33 μM CC50 = 2.09 μM SI = 16.07 |
Inhibits reverse transcriptase (RTase) activity | [66] | |
| Human cytomegalovirus (HCMV) | In vitro, human foreskin fibroblasts (HFF)/2.65 ± 0.35 µM | EC50 = 2.65 μM CC50 = 390 μM SI = 147 |
Inhibits viral E protein gene expression | [77] | |
| Hepatitis B virus (HBV) |
Oxymatrine | In vivo, mouse/200 mg/kg | - | Decreases antigen expression | [78] |
| Hepatitis B virus (HBV) |
In vivo, mouse/20.0 mg/kg | - | Inhibits viral replication Decreases antigen levels Promotes IFN-γ |
[69] | |
| Human immunodeficiency virus 1 (HIV-1) | Aloperine | In vitro, fibroblast-like COS cells and TZM-bl cells—0.01–10 μM | EC50 = 1.75 μM CC50 > 86.2 μM |
Inhibits virus fusion and entry | [68] |
(a) IC50: 50% inhibitory effect; EC50: 50% cytotoxic concentration; CC50 = 50% cytotoxic concentration; SI: selectivity index; AI: antiviral index.
Table 2.
Immunomodulatory effects of alkaloids in non-viral related models.
| Disease Model | Alkaloid | Model/Tested Doses | Effect | Ref. |
|---|---|---|---|---|
| Cancer | Berberine | In vitro, carcinoma cell (KB) and oral squamous carcinoma cell (OC2)/1, 10 or 100 μM In vivo, Wistar rats/1, 5 or 10 mg/kg |
Inhibits PGE2 synthesis and COX-2 expression | [84] |
| In vitro, human gastric cancer cell (SNU-5)/75 μM | Increases ROS production Inhibits NF-κB pathway |
[85] | ||
| In vitro, human thyroid carcinoma cell (C643, OCUT1, TPC1 and Htori3)/20 or 80 µM | Inhibits MAPK pathway | [86] | ||
| In vitro, breast cancer cell (MDA-MB231 and MCF-7)/3.125–100 µM | Inhibits MAPK pathway | [87] | ||
| Tetrandrine | In vitro, colon cancer cell (CT-26)/0.1–250 μM In vivo, tumor model mouse/50 and 150 mg/kg |
Activates MAPK pathway for cell apoptosis | [88] | |
| Ellipticine | In vitro, human endometrial cancer cell (RL95-2)/ 0.1–10 μM |
Increases ROS production and activates MAPK pathways for cell apoptosis | [89] | |
| Cardiovascular disease | Matrine | In vivo, ischemia/reperfusion in rats/50 or 100 mg/kg Ex vivo, cardiomyocytes from rats/200 or 400 µM |
Activates JAK/STAT pathway for a protective protein (HSP70) | [90] |
| Atherosclerosis | Aloperine | In vitro, ox-LDL induced inflammation in human umbilical vein endothelial cell (HUVEC)/50 and 100 µM | Decreases ROS production Inhibits pro-inflammatory IL-6 and MCP-1 |
[91] |
| Arthritis diseases | Berberine | In vivo, collagen-induced arthritis (CIA) in rats/200 mg/kg | Decreases pro-inflammatory TNF-α, IL-1β, IL-6 and IL-17 Inhibits MAPK pathway |
[92] |
| In vivo, Freund’s complete adjuvant (FCA) induced arthritis rats/75 and 150 mg/kg | Decreases pro-inflammatory IL-6 and IL-17 Increases the levels of regulatory IL-10 and TGF-β |
[93] | ||
| Ex vivo, Freund’s complete adjuvant (FCA) induced arthritic fibroblast-like synoviocytes (AA-FLS) from rats/15, 30 and 45 µM In vitro, bone-marrow-derived monocytes (BMMs)/15, 30 and 45 µM |
Decreases pro-inflammatory TNF-α, IL-1β, IL-6 and IL-23 Inhibits PI3K pathway |
[94] | ||
| Oxymatrine | In vivo, collagen-induced arthritis (CIA) in rats—25, 50 and 100 mg/kg | Decreases pro-inflammatory TNF-α and IL-17A | [95] | |
| In vitro, rheumatoid arthritis fibroblast-like synoviocytes (RA-FLS)/10–100 μM | Decreases pro-inflammatory IL-6 and IL-8 Inhibits NF-κB and MAPK signaling pathways |
[96] | ||
| Osteoarthritis | Berberine | In vitro, osteoarthritis synovial fibroblasts (OASFs)/5–100 µM | Inhibits pro-inflammatory IL-1β Inhibits NF-κB pathway |
[97] |
| Arthritis diseases | Sinomenine | In vitro, rheumatoid arthritis fibroblast-like synoviocytes (RA-FLS)/0.1 and 1 μM | Decreases expression of proinflammatory TNF-α and IL-6 Inhibits COX and NF-κB pathways |
[98] |
| Ex vivo, fibroblast-like synoviocytes (FLS) of adjuvant-induced arthritis (AIA) rat/50–400 µM | Inhibits kinase (ERK/Egr-1) pathway | [99] | ||
| Chronic arthritis | Tetrandrine | In vivo, adjuvant-induced arthritis (AIA) rat/25 mg/kg/day or 80 mg/kg/day | Inhibits pro-inflammatory TNF-α and IL-1 | [100] |
| Inflammation (other pathological conditions) | Brucine | In vivo, carrageenan-induced rat paw edema/15 and 30 mg/kg | Inhibits pro-inflammatory PGE2 | [101] |
| Ellipticine | In vitro, bone-marrow-derived macrophages (BMDMs)/5 μM In vivo, mouse with LPS-induced septic shock/20 mg/kg |
Decrease pro-inflammatory TNF-α and IL-6 Inhibits NF-κB pathway |
[102] | |
| Tabersonine |
In vivo, LPS-induced inflammation in acute lung injury (ALI) mouse model/10, 20 or 40 mg/kg Ex vivo, bone-marrow-derived macrophages (BMDMs)/10 μM In vitro, human embryonic kidney cell (HEK293T)/10 μM |
Inhibits pro-inflammatory TNF-α, IL-6 and IL-1β Inhibits NF-κB and MAPK pathways |
[103] | |
| Oxymatrine | In vivo, Wistar rats after intracerebral hemorrhage (ICH)/120 mg/kg/day | Inhibits pro-inflammatory TNF-α, IL-1β and IL-6 Inhibits NF-κB pathway |
[104] |
The antiviral activities of the reported alkaloids (Table 1) were characterized on both prominent RNA and DNA viruses, and their broad-spectrum activity is of interest to identify novel applications, as illustrated by the traditionally used and clinically promising isoquinoline berberine [61,62]; the latter proved to be efficient in disrupting the replication process of various DNA viruses [63] and has been also assessed against RNA viruses including CHIKV, SINV and SFV [64] or the novel severe acute respiratory syndrome related to Coronavirus-2 (SARS-CoV-2) [65]. These data support the broad-spectrum potential of berberine against genetically different viruses and at low micromolar range and low toxicity in vitro (EC50 = 1.8 µM; CC50 > 100 µM; SI > 127) for CHIKV [64] compared to its potency against the other reported RNA or DNA viruses. Of note, berberine demonstrated substantial inhibitory effects in vitro on the essential host component reverse transcriptase for HIV-1 (IC50 = 0.33 µM; CC50 = 2.09 µM; SI = 16.07) [66]. The inhibitory potential of the quinolizidines was not evidenced against arthritogenic alphaviruses but was supported with multiple targets on the virus life cycle for HCV attachment, replication and cell-to-cell transmission [67] or HIV-1 (fusion and entry) [68] using aloperine with satisfactory potency in vitro (EC50 = 7.06 µM; CC50 > 200 µM and EC50 = 1.75 µM; CC50 > 86.2 µM, respectively) and HBV replication in vivo using oxymatrine [69].
The above data established typical antiviral mechanisms related to viral clearance by interference on the virus life cycle (entry, replication, assembly and release) and/or the specific virus–host interactions (viral cell-to-cell transmission and enzyme activity such as reverse transcriptase for HIV-1) [79]. Interestingly, additional immunomodulatory effects of interest during viral infection were also evidenced. Such effects have been previously exploited for anti-HIV therapy [80] and more recently for the treatment of infection with SARS-CoV-2 viruses [81] or arthritogenic alphaviruses [2] to prevent the excessive release of cytokines that may cause inflammation or pathogenesis [25]. The selected experimental data in vitro and in vivo established the multifocal immunomodulatory effects of alkaloids during viral infection.
First of all, the management of host antiviral signaling occurs via the downregulation of the pro-inflammatory inducer TNF-α, as shown in vitro for berberine [70] or oxymatrine [75] during IAV infection. Such an effect is of interest for the prominent role of TNF-α established during arthritogenic alphavirus infection. In contrast, alkaloids can increase the regulatory type II interferon IFN-γ as established with oxymatrine during HBV infection [69].
Secondly, the regulation of viral-related inflammation was demonstrated by the inhibition of inflammatory mediators or signaling pathways. The inhibition of PGE2 in vitro via berberine during IAV infection ascertained the sensitivity of the arachidonic cascade to alkaloids [70]. The downregulation of other inflammatory signaling pathways was supported in vitro via the inhibition of MAPK using berberine against RSV [71]. In vivo experiments demonstrated the multikinase effects (MAPK, NF-κB and PI3-AKt) of berberine against CHIKV [64] or oxymatrine against IAV [75]. Of note, the clinical value of matrine to resolve inflammation was recently supported by the reduction in C- reactive protein (CRP) levels against SARS-CoV-2 infection [73].
Finally, alkaloids could trigger an immune response during viral infection. As shown in vivo during HCV infection, oxymatrine increases the pro-inflammatory TH1-cytokines (IFN-γ and IL-2) for viral neutralization and decreases the regulatory TH2-cytokines (IL-4 and IL-10) [74]. Oxymatrine also increases IFN-γ against HBV in vivo (Sang et al. 2017). Remarkable immunosuppressive effects were shown in vitro using berberine against RSV [71] by the decreases in the crucial IL-6 in persistent arthralgia related to arthritogenic alphavirus infection [82], or in vitro and in vivo using oxymatrine against IAV [75] for the inhibition of IL-1β involved in the severity of arthritogenic alphavirus infection [83].
The immunomodulatory effects of the representative alkaloids were also demonstrated in various chronic health conditions not related to viral infection (Table 2). These effects are typically assessed at non-toxic doses of the tested compound.
Alkaloids proved to be efficient in resolving inflammation established as a risk factor and promoter of cancer, and they act through common pathways and biochemicals with inflammation induced by infection [105]. Defensive ROS production was promoted in several models of cancer with berberine [86] or ellipticine [89]. The downregulation of the arachidonic cascade was demonstrated by the decrease in PGE2 production and the inhibition of COX-2 at the transcriptional level using berberine [84]. Interference with the pivotal kinase inflammatory signaling pathways (MAPK, NF-κB and PI3-AKt) occurred with berberine [86,87], tetrandrine [88] and ellipticine [89]. Of note, the isoquinoline berberine demonstrated substantial immunomodulatory effects at low micromolar inhibitory concentrations in human thyroid carcinoma cell (IC50 = 0.891 μM) [86], to moderate concentrations in breast cancer cell (IC50 = 15 μM) [87], and at higher doses in human gastric cancer cell (IC50 = 48 μM) [85]. Apoptosis in colon cancer (SNU-5) cells using the isoquinoline tetrandrine [88] and in human endometrial cancer (RL 95-2) cells treated with the indole ellipticine [89] underlined an essential antiproliferative effect of these alkaloids [106].
The representative matrine and aloperine quinolizidines showed multiple and valuable immunomodulatory effects in complex pathologies. In a cardiovascular model, matrine demonstrated the in vivo and ex vivo activation of the JAK2/STAT3 signaling pathway [90] with the upregulation of the HSP70 protein which had a cardioprotective effect [107]. In atherosclerosis, aloperine demonstrated a protective effect in vitro via the downregulation of the key immune effectors including excessive ROS, the pro-inflammatory cytokine IL-6, the signaling chemokine MCP-1 and the inducible endothelial cell adhesion molecules, vascular cell adhesion molecule 1 (VCAM-1) and E-selectin.
Rheumatoid arthritis is a chronic, systemic autoimmune and inflammatory disease which causes damage to joint tissues, and alphavirus infection results in rheumatoid-arthritis-like symptoms and complications. The immunomodulatory effects of alkaloids in the reported arthritic disorders were supported by robust experimental models: in vitro using bone-marrow-derived monocyte macrophages (BMMs) [108] or osteoarthritis synovial fibroblasts (OASF) [109]; ex vivo using key effectors rheumatoid arthritis fibroblast-like synoviocytes (RA-FLS) [110]; and in vivo using inflammatory stimulators in preclinical test models via adjuvant-induced arthritis (AIA) in rats including collagen-induced arthritis (CIA) [111] or Freund’s complete adjuvant (FCA)-induced arthritis [112]. As illustrated for the overall arthritic diseases with the isoquinolines berberine [92,93,94], sinomenine [98,99] and tetrandrine [100] and the quinolizidine oxymatrine [95,96], the suppression of inflammatory signaling pathways decreases the common pro-inflammatory cytokines (e.g., TNF-α, IL-1β and IL-6), as well as the critical IL-17 involved in inflammation and bone loss in rheumatoid arthritis and also evidenced in CHIKV chronically affected patients [82].
The immunomodulatory effects of alkaloids were assessed on other inflammation test models in vitro, ex vivo or in vivo, as illustrated with the isoquinoline tabersonine [103], the indole alkaloid brucine [101] and ellipticine [102] and the quinolizidine oxymatrine [104]. The data highlighted similar effects to those previously discussed, and noticeably, the suppression of kinase signaling pathways (MAPK and NF-κB) and the downregulation of pro-inflammatory mediators (TNF-α, IL-6, IL-1β and PGE2) which are critical during arthritogenic alphavirus infection and related inflammation.
As summarized in Figure 3 from the reported data (Table 1 and Table 2), the selected alkaloids have substantial effects on various host-based targets involved in viral infection and inflammation. Antiviral immune response is mediated by cell-surface (receptor) or cytosolic viral sensors (e.g., RIG-I and MDA-5 for alphaviruses) involved in viral entry or detection (1). The inhibition of these host cell components, as evidenced with the isoquinoline berberine and the quinolizidines oxymatrine and aloperine, prevents viral invasion. Alternatively, the quinolizidine oxymatrine proved to be able to mount an antiviral response mediated by IFN production (2A) and signaling via the IFN cell-surface receptor (2B). As shown, the selected alkaloids, especially the isoquinoline berberine, can interfere with different inflammatory signaling pathways, including the JAK/STAT pathway (2C), the kinase pathways (3A), the COX-2-related pathways (4A) and (4B), as well as the oxidative pathways (5A) and (5B). The inhibitory and/or inductive effects may be of interest to achieve a well-balanced inflammatory response and consequently, to prevent complications resulting from the dysregulation of the immune system. The potential of the selected alkaloids was also established in the upregulation and/or downregulation of the major inflammatory mediators.
Figure 3.
Effects of the selected alkaloids on virus detection (1), antiviral and/or inflammatory signaling pathways (2A), (2C), (3A), (4A) or (5A) and mediators (2A), (2B), (2D), (3B), (4B) and (5B). The figure was created using biorender.com.
The combined data support the immunomodulatory effects of the selected alkaloids against arthritogenic alphaviruses as the latter mobilizes the same host key functions.
Plant-derived alkaloids are major sources for drug discovery, with highly potent naturally occurring compounds, including isoquinolines (e.g., the anticancer noscapine and the analgesics morphine and codeine), indoles (e.g., the anticancer vinblastine and vincristine) and quinolizidines (e.g., the anti-Influenza A oseltamivir and zanamivir) [43,113], and they are gaining increasing consideration in managing viral infection and inflammation [51]. However, the pharmaceutical development of natural alkaloids is often faced with the problem of their low activity and/or their toxic effects [114]. Therefore, many efforts are devoted to the structural optimization of an original alkaloid and to identifying ‘druggable’ derivatives. As exemplified in some of the reported studies, structure-activity relationship (SAR) studies have been successfully applied to improve potent viral inhibitory effects. In vitro anti-HIV assays on a set of O-esters derivatives of the berberine allowed two compounds with better therapeutic indexes for antiviral activity to be identified [66], in line with intensive efforts to promote benzylisoquinoline alkaloids [44]. The valuable quinolizidine aloperine and N-substituted derivatives have been established as a new class of HIV entry inhibitors [68]. The most potent molecules against alphaviruses are so far limited [115], and there is no evidence for structural optimization directed to the discovery of efficient immunomodulators of both antiviral and inflammatory responses.
3. Conclusions
From robust experimental models of viral infection and/or inflammation, the selected isoquinoline-, indole- and quinolizidine-derived alkaloids demonstrated substantial immunomodulatory effects. As evidenced, they can interfere with the canonical signaling pathways and biochemicals of the immune system. The effects of these alkaloids on arthritogenic alphavirus infection and related inflammation have been poorly studied, and the collective data ascertain the great potential of natural alkaloids or more toxicologically acceptable derivatives from structure–activity relationship studies. The most convincing evidence arises from the isoquinoline berberine, which can disrupt not only CHIKV replication but also the resulting immunological disorders. Other compounds investigated concerning other viruses or diseases shed light on the diverse mechanisms of action of interest for their application as immunomodulators against arthritogenic alphavirus infection and related inflammation.
Author Contributions
Conceptualization, A.-L.S.S., E.G.-V. and J.S.; methodology, A.-L.S.S. and J.S.; software, A.-L.S.S.; validation, E.G.-V., J.S. and P.G. (Philippe Gasque); investigation, A.-L.S.S., E.G.-V. and J.S.; original draft preparation, A.-L.S.S. and J.S.; writing—review and editing, A.-L.S.S., A.S.-M., E.G.-V., J.S., P.G (Pascale Guiraud) and P.G (Philippe Gasque); supervision, E.G.-V. and J.S. All authors have read and agreed to the published version of the manuscript.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
On demand–EPI research unit.
Conflicts of Interest
The authors declare no conflict of interest.
Funding Statement
A.-L.S.S. was supported by a PhD fellowship from the Regional Council of La Réunion and this work was supported by Regional Council of La Réunion, French State, and Europe (CPER-FEDER, GURDTI 2017-1198-0002583 VIROPAM).
Footnotes
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Strauss J.H., Strauss E.G. The Alphaviruses: Gene Expression, Replication, and Evolution. Microbiol. Rev. 1994;58:491–562. doi: 10.1128/mr.58.3.491-562.1994. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Suhrbier A., Jaffar-Bandjee M.-C., Gasque P. Arthritogenic Alphaviruses—An Overview. Nat. Rev. Rheumatol. 2012;8:420–429. doi: 10.1038/nrrheum.2012.64. [DOI] [PubMed] [Google Scholar]
- 3.Wesula Olivia L., Obanda V., Bucht G., Mosomtai G., Otieno V., Ahlm C., Evander M. Global Emergence of Alphaviruses That Cause Arthritis in Humans. Infect. Ecol. Epidemiol. 2015;5:29853. doi: 10.3402/iee.v5.29853. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Chen W., Foo S.-S., Sims N.A., Herrero L.J., Walsh N.C., Mahalingam S. Arthritogenic Alphaviruses: New Insights into Arthritis and Bone Pathology. Trends Microbiol. 2015;23:35–43. doi: 10.1016/j.tim.2014.09.005. [DOI] [PubMed] [Google Scholar]
- 5.Mostafavi H., Abeyratne E., Zaid A., Taylor A. Arthritogenic Alphavirus-Induced Immunopathology and Targeting Host Inflammation as A Therapeutic Strategy for Alphaviral Disease. Viruses. 2019;11:290. doi: 10.3390/v11030290. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Ng L.F.P., Chow A., Sun Y.-J., Kwek D.J.C., Lim P.-L., Dimatatac F., Ng L.-C., Ooi E.-E., Choo K.-H., Her Z., et al. IL-1β, IL-6, and RANTES as Biomarkers of Chikungunya Severity. PLoS ONE. 2009;4:e4261. doi: 10.1371/journal.pone.0004261. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Lidbury B.A., Rulli N.E., Suhrbier A., Smith P.N., McColl S.R., Cunningham A.L., Tarkowski A., van Rooijen N., Fraser R.J., Mahalingam S. Macrophage-Derived Proinflammatory Factors Contribute to the Development of Arthritis and Myositis after Infection with an Arthrogenic Alphavirus. J. Infect. Dis. 2008;197:1585–1593. doi: 10.1086/587841. [DOI] [PubMed] [Google Scholar]
- 8.Tappe D., Pérez-Girón J.V., Just-Nübling G., Schuster G., Gómez-Medina S., Günther S., Muñoz-Fontela C., Schmidt-Chanasit J. Sustained Elevated Cytokine Levels during Recovery Phase of Mayaro Virus Infection. Emerg. Infect. Dis. 2016;22:750–752. doi: 10.3201/eid2204.151502. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Chang A., Tritsch S., Reid S., Martins K., Encinales L., Pacheco N., Amdur R., Porras-Ramirez A., Rico-Mendoza A., Li G., et al. The Cytokine Profile in Acute Chikungunya Infection Is Predictive of Chronic Arthritis 20 Months Post Infection. Diseases. 2018;6:95. doi: 10.3390/diseases6040095. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Delogu I., Pastorino B., Baronti C., Nougairède A., Bonnet E., de Lamballerie X. In Vitro Antiviral Activity of Arbidol against Chikungunya Virus and Characteristics of a Selected Resistant Mutant. Antivir. Res. 2011;90:99–107. doi: 10.1016/j.antiviral.2011.03.182. [DOI] [PubMed] [Google Scholar]
- 11.Dey D., Siddiqui S.I., Mamidi P., Ghosh S., Kumar C.S., Chattopadhyay S., Ghosh S., Banerjee M. The Effect of Amantadine on an Ion Channel Protein from Chikungunya Virus. PLoS Negl. Trop. Dis. 2019;13:e0007548. doi: 10.1371/journal.pntd.0007548. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Ho Y.-J., Wang Y.-M., Lu J., Wu T.-Y., Lin L.-I., Kuo S.-C., Lin C.-C. Suramin Inhibits Chikungunya Virus Entry and Transmission. PLoS ONE. 2015;10:e0133511. doi: 10.1371/journal.pone.0133511. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Feibelman K.M., Fuller B.P., Li L., LaBarbera D.V., Geiss B.J. Identification of Small Molecule Inhibitors of the Chikungunya Virus NsP1 RNA Capping Enzyme. Antivir. Res. 2018;154:124–131. doi: 10.1016/j.antiviral.2018.03.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Kumar P., Kumar D., Giri R. Targeting the Nsp2 Cysteine Protease of Chikungunya Virus Using FDA Approved Library and Selected Cysteine Protease Inhibitors. Pathogens. 2019;8:128. doi: 10.3390/pathogens8030128. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Gigante A., Gómez-SanJuan A., Delang L., Li C., Bueno O., Gamo A.-M., Priego E.-M., Camarasa M.-J., Jochmans D., Leyssen P., et al. Antiviral Activity of [1,2,3]Triazolo[4,5- d ]Pyrimidin-7(6 H )-Ones against Chikungunya Virus Targeting the Viral Capping NsP1. Antivir. Res. 2017;144:216–222. doi: 10.1016/j.antiviral.2017.06.003. [DOI] [PubMed] [Google Scholar]
- 16.Jadav S.S., Sinha B.N., Hilgenfeld R., Pastorino B., de Lamballerie X., Jayaprakash V. Thiazolidone Derivatives as Inhibitors of Chikungunya Virus. Eur. J. Med. Chem. 2015;89:172–178. doi: 10.1016/j.ejmech.2014.10.042. [DOI] [PubMed] [Google Scholar]
- 17.Khan M., Santhosh S.R., Tiwari M., Lakshmana Rao P.V., Parida M. Assessment of In Vitro Prophylactic and Therapeutic Efficacy of Chloroquine against Chikungunya Virus in Vero Cells. J. Med. Virol. 2010;82:817–824. doi: 10.1002/jmv.21663. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Cifuentes Kottkamp A., De Jesus E., Grande R., Brown J.A., Jacobs A.R., Lim J.K., Stapleford K.A. Atovaquone Inhibits Arbovirus Replication through the Depletion of Intracellular Nucleotides. J. Virol. 2019;93:e00389-19. doi: 10.1128/JVI.00389-19. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Wichit S., Hamel R., Bernard E., Talignani L., Diop F., Ferraris P., Liegeois F., Ekchariyawat P., Luplertlop N., Surasombatpattana P., et al. Imipramine Inhibits Chikungunya Virus Replication in Human Skin Fibroblasts through Interference with Intracellular Cholesterol Trafficking. Sci. Rep. 2017;7:3145. doi: 10.1038/s41598-017-03316-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Bedoui Y., Giry C., Jaffar-Bandjee M.-C., Selambarom J., Guiraud P., Gasque P. Immunomodulatory Drug Methotrexate Used to Treat Patients with Chronic Inflammatory Rheumatisms Post-Chikungunya Does Not Impair the Synovial Antiviral and Bone Repair Responses. PLoS Negl. Trop. Dis. 2018;12:e0006634. doi: 10.1371/journal.pntd.0006634. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Œwierkot J., Szechiñski J. Methotrexate in Rheumatoid Arthritis. Pharmacol. Rep. 2006;58:473–492. [PubMed] [Google Scholar]
- 22.Robert C. A Decade of Immune-Checkpoint Inhibitors in Cancer Therapy. Nat. Commun. 2020;11:3801. doi: 10.1038/s41467-020-17670-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.McInnes I.B., Gravallese E.M. Immune-Mediated Inflammatory Disease Therapeutics: Past, Present and Future. Nat. Rev. Immunol. 2021;21:680–686. doi: 10.1038/s41577-021-00603-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Murphy A.J., Febbraio M.A. Immune-Based Therapies in Cardiovascular and Metabolic Diseases: Past, Present and Future. Nat. Rev. Immunol. 2021;21:669–679. doi: 10.1038/s41577-021-00580-5. [DOI] [PubMed] [Google Scholar]
- 25.Malemud C.J. Immunomodulators in Autoimmunity and Viral Infections. J. Clin. Cell Immunol. 2018;9 doi: 10.4172/2155-9899.1000537. [DOI] [Google Scholar]
- 26.Herrero L.J., Foo S.-S., Sheng K.-C., Chen W., Forwood M.R., Bucala R., Mahalingam S. Pentosan Polysulfate: A Novel Glycosaminoglycan-Like Molecule for Effective Treatment of Alphavirus-Induced Cartilage Destruction and Inflammatory Disease. J. Virol. 2015;89:8063–8076. doi: 10.1128/JVI.00224-15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Supramaniam A., Liu X., Ferro V., Herrero L.J. Prophylactic Antiheparanase Activity by PG545 Is Antiviral In Vitro and Protects against Ross River Virus Disease in Mice. Antimicrob. Agents Chemother. 2018;62:e01959-17. doi: 10.1128/AAC.01959-17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Dredge K., Brennan T.V., Hammond E., Lickliter J.D., Lin L., Bampton D., Handley P., Lankesheer F., Morrish G., Yang Y., et al. A Phase I Study of the Novel Immunomodulatory Agent PG545 (Pixatimod) in Subjects with Advanced Solid Tumours. Br. J. Cancer. 2018;118:1035–1041. doi: 10.1038/s41416-018-0006-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Ekins S., Madrid P.B. Tilorone, a Broad-Spectrum Antiviral for Emerging Viruses. Antimicrob. Agents Chemother. 2020;64:e00440-20. doi: 10.1128/AAC.00440-20. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Krueger R.F., Mayer G.D. Tilorone Hydrochloride: An Orally Active Antiviral Agent. Science. 1970;169:1213–1214. doi: 10.1126/science.169.3951.1213. [DOI] [PubMed] [Google Scholar]
- 31.Shukla S., Bajpai V.K., Kim M. Plants as Potential Sources of Natural Immunomodulators. Rev. Environ. Sci. Bio Technol. 2014;13:17–33. doi: 10.1007/s11157-012-9303-x. [DOI] [Google Scholar]
- 32.Jantan I., Ahmad W., Bukhari S.N.A. Plant-Derived Immunomodulators: An Insight on Their Preclinical Evaluation and Clinical Trials. Front. Plant Sci. 2015;6:655. doi: 10.3389/fpls.2015.00655. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Ortuño-Sahagún D., Zänker K., Rawat A.K.S., Kaveri S.V., Hegde P. Natural Immunomodulators. J. Immunol. Res. 2017;2017:7529408. doi: 10.1155/2017/7529408. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Twaij B.M., Hasan M.N. Bioactive Secondary Metabolites from Plant Sources: Types, Synthesis, and Their Therapeutic Uses. Int. J. Plant Biol. 2022;13:4–14. doi: 10.3390/ijpb13010003. [DOI] [Google Scholar]
- 35.Barbosa-Filho J.M., Piuvezam M.R., Moura M.D., Silva M.S., Lima K.V.B., da-Cunha E.V.L., Fechine I.M., Takemura O.S. Anti-Inflammatory Activity of Alkaloids: A Twenty-Century Review. Rev. Bras. De Farmacogn. 2006;16:109–139. doi: 10.1590/S0102-695X2006000100020. [DOI] [Google Scholar]
- 36.Evans W.C., Evans D., Trease G.E. Trease and Evans Pharmacognosy. 16th ed. Saunders/Elsevier; Edinburgh, UK: 2009. [Google Scholar]
- 37.Souto A.L., Tavares J.F., da Silva M.S., Diniz M.d.F.F.M., de Athayde-Filho P.F., Filho J.M.B. Anti-Inflammatory Activity of Alkaloids: An Update from 2000 to 2010. Molecules. 2011;16:8515–8534. doi: 10.3390/molecules16108515. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Qiu S., Sun H., Zhang A.-H., Xu H.-Y., Yan G.-L., Han Y., Wang X.-J. Natural Alkaloids: Basic Aspects, Biological Roles, and Future Perspectives. Chin. J. Nat. Med. 2014;12:401–406. doi: 10.1016/S1875-5364(14)60063-7. [DOI] [PubMed] [Google Scholar]
- 39.Li Q., Yang K.-X., Zhao Y.-L., Qin X.-J., Yang X.-W., Liu L., Liu Y.-P., Luo X.-D. Potent Anti-Inflammatory and Analgesic Steroidal Alkaloids from Veratrum Taliense. J. Ethnopharmacol. 2016;179:274–279. doi: 10.1016/j.jep.2015.12.059. [DOI] [PubMed] [Google Scholar]
- 40.Alves de Almeida A.C., de-Faria F.M., Dunder R.J., Manzo L.P.B., Souza-Brito A.R.M., Luiz-Ferreira A. Recent Trends in Pharmacological Activity of Alkaloids in Animal Colitis: Potential Use for Inflammatory Bowel Disease. Evid. Based Complementary Alternat. Med. 2017;2017:8528210. doi: 10.1155/2017/8528210. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Thawabteh A., Juma S., Bader M., Karaman D., Scrano L., Bufo S., Karaman R. The Biological Activity of Natural Alkaloids against Herbivores, Cancerous Cells and Pathogens. Toxins. 2019;11:656. doi: 10.3390/toxins11110656. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Behl T., Kumar K., Brisc C., Rus M., Nistor-Cseppento D.C., Bustea C., Aron R.A.C., Pantis C., Zengin G., Sehgal A., et al. Exploring the Multifocal Role of Phytochemicals as Immunomodulators. Biomed. Pharmacother. 2021;133:110959. doi: 10.1016/j.biopha.2020.110959. [DOI] [PubMed] [Google Scholar]
- 43.Cordell G.A., Quinn-Beattie M.L., Farnsworth N.R. The Potential of Alkaloids in Drug Discovery. Phytother. Res. 2001;15:183–205. doi: 10.1002/ptr.890. [DOI] [PubMed] [Google Scholar]
- 44.Qing Z.-X., Yang P., Tang Q., Cheng P., Liu Y., Zheng Y., Liu Y.-S., Zeng J.-G. Isoquinoline Alkaloids and Their Antiviral, Antibacterial, and Antifungal Activities and Structure-Activity Relationship. Current Organic Chemistry. 2017;21:1920–1934. doi: 10.2174/1385272821666170207114214. [DOI] [Google Scholar]
- 45.Wang R., Deng X., Gao Q., Wu X., Han L., Gao X., Zhao S., Chen W., Zhou R., Li Z., et al. Sophora Alopecuroides L.: An Ethnopharmacological, Phytochemical, and Pharmacological Review. J. Ethnopharmacol. 2020;248:112172. doi: 10.1016/j.jep.2019.112172. [DOI] [PubMed] [Google Scholar]
- 46.Kochanowska-Karamyan A.J., Hamann M.T. Marine Indole Alkaloids: Potential New Drug Leads for the Control of Depression and Anxiety. Chem. Rev. 2010;110:4489–4497. doi: 10.1021/cr900211p. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Amirkia V., Heinrich M. Alkaloids as Drug Leads—A Predictive Structural and Biodiversity-Based Analysis. Phytochem. Lett. 2014;10:48–53. doi: 10.1016/j.phytol.2014.06.015. [DOI] [Google Scholar]
- 48.Dobi A., Gasque P., Guiraud P., Selambarom J. Irinotecan (CPT-11) Canonical Anti-Cancer Drug Can Also Modulate Antiviral and Pro-Inflammatory Responses of Primary Human Synovial Fibroblasts. Cells. 2021;10:1431. doi: 10.3390/cells10061431. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Omar F., Tareq A.M., Alqahtani A.M., Dhama K., Sayeed M.A., Emran T.B., Simal-Gandara J. Plant-Based Indole Alkaloids: A Comprehensive Overview from a Pharmacological Perspective. Molecules. 2021;26:2297. doi: 10.3390/molecules26082297. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Krishnan N., Devadasan V., Raman P. Plant-Derived Alkaloids as Anti-Viral Agents. Int. J. Res. Pharm. Sci. 2020;11:6174–6182. doi: 10.26452/ijrps.v11i4.3291. [DOI] [Google Scholar]
- 51.Ti H., Zhuang Z., Yu Q., Wang S. Progress of Plant Medicine Derived Extracts and Alkaloids on Modulating Viral Infections and Inflammation. Drug Des. Develop. Ther. 2021;15:1385–1408. doi: 10.2147/DDDT.S299120. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Abookleesh F.L., Al-Anzi B.S., Ullah A. Potential Antiviral Action of Alkaloids. Molecules. 2022;27:903. doi: 10.3390/molecules27030903. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Troost B., Mulder L.M., Diosa-Toro M., van de Pol D., Rodenhuis-Zybert I.A., Smit J.M. Tomatidine, a Natural Steroidal Alkaloid Shows Antiviral Activity towards Chikungunya Virus In Vitro. Sci. Rep. 2020;10:6364. doi: 10.1038/s41598-020-63397-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Troost-Kind B., van Hemert M.J., van de Pol D., van der Ende-Metselaar H., Merits A., Borggrewe M., Rodenhuis-Zybert I.A., Smit J.M. Tomatidine Reduces Chikungunya Virus Progeny Release by Controlling Viral Protein Expression. PLoS Negl. Trop. Dis. 2021;15:e0009916. doi: 10.1371/journal.pntd.0009916. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Plazas E., Avila M.M.C., Muñoz D.R., Cuca S.L.E. Natural Isoquinoline Alkaloids: Pharmacological Features and Multi-Target Potential for Complex Diseases. Pharmacol. Res. 2022;177:106126. doi: 10.1016/j.phrs.2022.106126. [DOI] [PubMed] [Google Scholar]
- 56.Rosales P.F., Bordin G.S., Gower A.E., Moura S. Indole Alkaloids: 2012 until Now, Highlighting the New Chemical Structures and Biological Activities. Fitoterapia. 2020;143:104558. doi: 10.1016/j.fitote.2020.104558. [DOI] [PubMed] [Google Scholar]
- 57.O’Connor S.E., Maresh J.J. Chemistry and Biology of Monoterpene Indole Alkaloid Biosynthesis. Nat. Prod. Rep. 2006;23:532. doi: 10.1039/b512615k. [DOI] [PubMed] [Google Scholar]
- 58.Mohammed A.E., Abdul-Hameed Z.H., Alotaibi M.O., Bawakid N.O., Sobahi T.R., Abdel-Lateff A., Alarif W.M. Chemical Diversity and Bioactivities of Monoterpene Indole Alkaloids (MIAs) from Six Apocynaceae Genera. Molecules. 2021;26:488. doi: 10.3390/molecules26020488. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Li X., Tang Z., Wen L., Jiang C., Feng Q. Matrine: A Review of Its Pharmacology, Pharmacokinetics, Toxicity, Clinical Application and Preparation Researches. J. Ethnopharmacol. 2021;269:113682. doi: 10.1016/j.jep.2020.113682. [DOI] [PubMed] [Google Scholar]
- 60.Zhou H., Li J., Sun F., Wang F., Li M., Dong Y., Fan H., Hu D. A Review on Recent Advances in Aloperine Research: Pharmacological Activities and Underlying Biological Mechanisms. Front. Pharmacol. 2020;11:538137. doi: 10.3389/fphar.2020.538137. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Hou Q., He W.-J., Wu Y.-S., Hao H.-J., Xie X.-Y., Fu X.-B. Berberine: A Traditional Natural Product with Novel Biological Activities. Altern. Ther. Health Med. 2020;26:20–27. [PubMed] [Google Scholar]
- 62.Och A., Podgórski R., Nowak R. Biological Activity of Berberine—A Summary Update. Toxins. 2020;12:713. doi: 10.3390/toxins12110713. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Warowicka A., Nawrot R., Goździcka-Józefiak A. Antiviral Activity of Berberine. Arch. Virol. 2020;165:1935–1945. doi: 10.1007/s00705-020-04706-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Varghese F.S., Kaukinen P., Gläsker S., Bespalov M., Hanski L., Wennerberg K., Kümmerer B.M., Ahola T. Discovery of Berberine, Abamectin and Ivermectin as Antivirals against Chikungunya and Other Alphaviruses. Antivir. Res. 2016;126:117–124. doi: 10.1016/j.antiviral.2015.12.012. [DOI] [PubMed] [Google Scholar]
- 65.Varghese F., van Woudenbergh E., Overheul G., Eleveld M., Kurver L., van Heerbeek N., van Laarhoven A., Miesen P., den Hartog G., de Jonge M., et al. Berberine and Obatoclax Inhibit SARS-CoV-2 Replication in Primary Human Nasal Epithelial Cells In Vitro. Viruses. 2021;13:282. doi: 10.3390/v13020282. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Bodiwala H.S., Sabde S., Mitra D., Bhutani K.K., Singh I.P. Synthesis of 9-Substituted Derivatives of Berberine as Anti-HIV Agents. Eur. J. Med. Chem. 2011;46:1045–1049. doi: 10.1016/j.ejmech.2011.01.016. [DOI] [PubMed] [Google Scholar]
- 67.Lv X.-Q., Zou L.-L., Tan J.-L., Li H., Li J.-R., Liu N.-N., Dong B., Song D.-Q., Peng Z.-G. Aloperine Inhibits Hepatitis C Virus Entry into Cells by Disturbing Internalisation from Endocytosis to the Membrane Fusion Process. Eur. J. Pharmacol. 2020;883:173323. doi: 10.1016/j.ejphar.2020.173323. [DOI] [PubMed] [Google Scholar]
- 68.Dang Z., Zhu L., Lai W., Bogerd H., Lee K.-H., Huang L., Chen C.-H. Aloperine and Its Derivatives as a New Class of HIV-1 Entry Inhibitors. ACS Med. Chem. Lett. 2016;7:240–244. doi: 10.1021/acsmedchemlett.5b00339. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Sang X., Wang R., Han Y., Zhang C., Shen H., Yang Z., Xiong Y., Liu H., Liu S., Li R., et al. T Cell-Associated Immunoregulation and Antiviral Effect of Oxymatrine in Hydrodynamic Injection HBV Mouse Model. Acta Pharm. Sin. B. 2017;7:311–318. doi: 10.1016/j.apsb.2017.02.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Cecil C.E., Davis J.M., Cech N.B., Laster S.M. Inhibition of H1N1 Influenza A Virus Growth and Induction of Inflammatory Mediators by the Isoquinoline Alkaloid Berberine and Extracts of Goldenseal (Hydrastis Canadensis) Int. Immunopharmacol. 2011;11:1706–1714. doi: 10.1016/j.intimp.2011.06.002. [DOI] [PubMed] [Google Scholar]
- 71.Shin H.-B., Choi M.-S., Yi C.-M., Lee J., Kim N.-J., Inn K.-S. Inhibition of Respiratory Syncytial Virus Replication and Virus-Induced P38 Kinase Activity by Berberine. Int. Immunopharmacol. 2015;27:65–68. doi: 10.1016/j.intimp.2015.04.045. [DOI] [PubMed] [Google Scholar]
- 72.Varghese F.S., Thaa B., Amrun S.N., Simarmata D., Rausalu K., Nyman T.A., Merits A., McInerney G.M., Ng L.F.P., Ahola T. The Antiviral Alkaloid Berberine Reduces Chikungunya Virus-Induced Mitogen-Activated Protein Kinase Signaling. J. Virol. 2016;90:9743–9757. doi: 10.1128/JVI.01382-16. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Yang M.-W., Chen F., Zhu D.-J., Li J.-Z., Zhu J.-L., Zeng W., Qu S.-L., Zhang Y. [Clinical efficacy of Matrine and Sodium Chloride Injection in treatment of 40 cases of COVID-19] Zhongguo Zhong Yao Za Zhi. 2020;45:2221–2231. doi: 10.19540/j.cnki.cjcmm.20200323.501. [DOI] [PubMed] [Google Scholar]
- 74.Dong Y., Xi H., Yu Y., Wang Q., Jiang K., Li L. Effects of Oxymatrine on the Serum Levels of T Helper Cell 1 and 2 Cytokines and the Expression of the S Gene in Hepatitis B Virus S Gene Transgenic Mice: A Study on the Anti-Hepatitis B Virus Mechanism of Oxymatrine. J. Gastroenterol. Hepatol. 2002;17:1299–1306. doi: 10.1046/j.1440-1746.2002.02885.x. [DOI] [PubMed] [Google Scholar]
- 75.Dai J.-P., Wang Q.-W., Su Y., Gu L.-M., Deng H.-X., Chen X.-X., Li W.-Z., Li K.-S. Oxymatrine Inhibits Influenza A Virus Replication and Inflammation via TLR4, P38 MAPK and NF-ΚB Pathways. Int. J. Mol. Sci. 2018;19:965. doi: 10.3390/ijms19040965. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Chin L.W., Cheng Y.-W., Lin S.-S., Lai Y.-Y., Lin L.-Y., Chou M.-Y., Chou M.-C., Yang C.-C. Anti-Herpes Simplex Virus Effects of Berberine from Coptidis Rhizoma, a Major Component of a Chinese Herbal Medicine, Ching-Wei-San. Arch. Virol. 2010;155:1933–1941. doi: 10.1007/s00705-010-0779-9. [DOI] [PubMed] [Google Scholar]
- 77.Luganini A., Mercorelli B., Messa L., Palù G., Gribaudo G., Loregian A. The Isoquinoline Alkaloid Berberine Inhibits Human Cytomegalovirus Replication by Interfering with the Viral Immediate Early-2 (IE2) Protein Transactivating Activity. Antivir. Res. 2019;164:52–60. doi: 10.1016/j.antiviral.2019.02.006. [DOI] [PubMed] [Google Scholar]
- 78.Chen X.S., Wang G.J., Cai X., Yu H.Y., Hu Y.P. Inhibition of Hepatitis B Virus by Oxymatrine In Vivo. World J. Gastroenterol. 2001;7:49–52. doi: 10.3748/wjg.v7.i1.49. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Kausar S., Said Khan F., Ishaq Mujeeb Ur Rehman M., Akram M., Riaz M., Rasool G., Hamid Khan A., Saleem I., Shamim S., Malik A. A Review: Mechanism of Action of Antiviral Drugs. Int. J. Immunopathol. Pharmacol. 2021;35:20587384211002621. doi: 10.1177/20587384211002621. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Conant M.A. Immunomodulatory Therapy in the Management of Viral Infections in Patients with HIV Infection. J. Am. Acad. Dermatol. 2000;43:S27–S30. doi: 10.1067/mjd.2000.107810. [DOI] [PubMed] [Google Scholar]
- 81.Alijotas-Reig J., Esteve-Valverde E., Belizna C., Selva-O’Callaghan A., Pardos-Gea J., Quintana A., Mekinian A., Anunciacion-Llunell A., Miró-Mur F. Immunomodulatory Therapy for the Management of Severe COVID-19. Beyond the Anti-Viral Therapy: A Comprehensive Review. Autoimmun. Rev. 2020;19:102569. doi: 10.1016/j.autrev.2020.102569. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 82.Chow A., Her Z., Ong E.K.S., Chen J., Dimatatac F., Kwek D.J.C., Barkham T., Yang H., Rénia L., Leo Y.-S., et al. Persistent Arthralgia Induced by Chikungunya Virus Infection Is Associated with Interleukin-6 and Granulocyte Macrophage Colony-Stimulating Factor. J. Infect. Dis. 2011;203:149–157. doi: 10.1093/infdis/jiq042. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Wolf S., Taylor A., Zaid A., Freitas J., Herrero L.J., Rao S., Suhrbier A., Forwood M.R., Bucala R., Mahalingam S. Inhibition of Interleukin-1β Signaling by Anakinra Demonstrates a Critical Role of Bone Loss in Experimental Arthritogenic Alphavirus Infections. Arthritis Rheumatol. 2019;71:1185–1190. doi: 10.1002/art.40856. [DOI] [PubMed] [Google Scholar]
- 84.Kuo C.-L., Chi C.-W., Liu T.-Y. The Anti-Inflammatory Potential of Berberine In Vitro and In Vivo. Cancer Lett. 2004;203:127–137. doi: 10.1016/j.canlet.2003.09.002. [DOI] [PubMed] [Google Scholar]
- 85.Lin J.-P., Yang J.-S., Wu C.-C., Lin S.-S., Hsieh W.-T., Lin M.-L., Yu F.-S., Yu C.-S., Chen G.-W., Chang Y.-H., et al. Berberine Induced Down-Regulation of Matrix Metalloproteinase-1, -2 and -9 in Human Gastric Cancer Cells (SNU-5) In Vitro. In Vivo. 2008;9:223–230. [PubMed] [Google Scholar]
- 86.Li L., Wang X., Sharvan R., Gao J., Qu S. Berberine Could Inhibit Thyroid Carcinoma Cells by Inducing Mitochondrial Apoptosis, G0/G1 Cell Cycle Arrest and Suppressing Migration via PI3K-AKT and MAPK Signaling Pathways. Biomed. Pharmacother. 2017;95:1225–1231. doi: 10.1016/j.biopha.2017.09.010. [DOI] [PubMed] [Google Scholar]
- 87.Jabbarzadeh Kaboli P., Leong M.P.-Y., Ismail P., Ling K.-H. Antitumor Effects of Berberine against EGFR, ERK1/2, P38 and AKT in MDA-MB231 and MCF-7 Breast Cancer Cells Using Molecular Modelling and In Vitro Study. Pharmacol. Rep. 2019;71:13–23. doi: 10.1016/j.pharep.2018.07.005. [DOI] [PubMed] [Google Scholar]
- 88.Wu J.-M., Chen Y., Chen J.-C., Lin T.-Y., Tseng S.-H. Tetrandrine Induces Apoptosis and Growth Suppression of Colon Cancer Cells in Mice. Cancer Lett. 2010;287:187–195. doi: 10.1016/j.canlet.2009.06.009. [DOI] [PubMed] [Google Scholar]
- 89.Kim J.Y., Lee S.G., Chung J.-Y., Kim Y.-J., Park J.-E., Koh H., Han M.S., Park Y.C., Yoo Y.H., Kim J.-M. Ellipticine Induces Apoptosis in Human Endometrial Cancer Cells: The Potential Involvement of Reactive Oxygen Species and Mitogen-Activated Protein Kinases. Toxicology. 2011;289:91–102. doi: 10.1016/j.tox.2011.07.014. [DOI] [PubMed] [Google Scholar]
- 90.Guo S., Gao C., Xiao W., Zhang J., Qu Y., Li J., Ye F. Matrine Protects Cardiomyocytes from Ischemia/Reperfusion Injury by Regulating HSP70 Expression Via Activation of the JAK2/STAT3 Pathway. Shock. 2018;50:664–670. doi: 10.1097/SHK.0000000000001108. [DOI] [PubMed] [Google Scholar]
- 91.Li W., Li Y., Zhao Y., Ren L. The Protective Effects of Aloperine against Ox-LDL-Induced Endothelial Dysfunction and Inflammation in HUVECs. Artif. Cells Nanomed. Biotechnol. 2020;48:107–115. doi: 10.1080/21691401.2019.1699816. [DOI] [PubMed] [Google Scholar]
- 92.Wang Z., Chen Z., Yang S., Wang Y., Huang Z., Gao J., Tu S., Rao Z. Berberine Ameliorates Collagen-Induced Arthritis in Rats Associated with Anti-Inflammatory and Anti-Angiogenic Effects. Inflammation. 2014;37:1789–1798. doi: 10.1007/s10753-014-9909-y. [DOI] [PubMed] [Google Scholar]
- 93.Wang X., He X., Zhang C.-F., Guo C.-R., Wang C.-Z., Yuan C.-S. Anti-Arthritic Effect of Berberine on Adjuvant-Induced Rheumatoid Arthritis in Rats. Biomed. Pharmacother. 2017;89:887–893. doi: 10.1016/j.biopha.2017.02.099. [DOI] [PubMed] [Google Scholar]
- 94.Dinesh P., Rasool M. Berberine Inhibits IL-21/IL-21R Mediated Inflammatory Proliferation of Fibroblast-like Synoviocytes through the Attenuation of PI3K/Akt Signaling Pathway and Ameliorates IL-21 Mediated Osteoclastogenesis. Cytokine. 2018;106:54–66. doi: 10.1016/j.cyto.2018.03.005. [DOI] [PubMed] [Google Scholar]
- 95.Ma A., Yang Y., Wang Q., Wang Y., Wen J., Zhang Y. Anti-Inflammatory Effects of Oxymatrine on Rheumatoid Arthritis in Rats via Regulating the Imbalance between Treg and Th17 Cells. Mol. Med. Rep. 2017;15:3615–3622. doi: 10.3892/mmr.2017.6484. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 96.Liang J., Chang B., Huang M., Huang W., Ma W., Liu Y., Tai W., Long Y., Lu Y. Oxymatrine Prevents Synovial Inflammation and Migration via Blocking NF-ΚB Activation in Rheumatoid Fibroblast-like Synoviocytes. Int. Immunopharmacol. 2018;55:105–111. doi: 10.1016/j.intimp.2017.12.006. [DOI] [PubMed] [Google Scholar]
- 97.Liu S.-C., Lee H.-P., Hung C.-Y., Tsai C.-H., Li T.-M., Tang C.-H. Berberine Attenuates CCN2-Induced IL-1β Expression and Prevents Cartilage Degradation in a Rat Model of Osteoarthritis. Toxicol. Appl. Pharmacol. 2015;289:20–29. doi: 10.1016/j.taap.2015.08.020. [DOI] [PubMed] [Google Scholar]
- 98.Yao R.-B., Zhao Z.-M., Zhao L.-J., Cai H. Sinomenine Inhibits the Inflammatory Responses of Human Fibroblast-like Synoviocytes via the TLR4/MyD88/NF-ΚB Signaling Pathway in Rheumatoid Arthritis. Pharmazie. 2017;72:355–360. doi: 10.1691/ph.2017.6946. [DOI] [PubMed] [Google Scholar]
- 99.Yi L., Lyn Y., Peng C., Zhu R., Bai S., Liu L., Wang P., Zhou H., Dong Y. Sinomenine Inhibits Fibroblast-like Synoviocyte Proliferation by Regulating A7nAChR Expression via ERK/Egr-1 Pathway. Int. Immunopharmacol. 2018;56:65–70. doi: 10.1016/j.intimp.2018.01.015. [DOI] [PubMed] [Google Scholar]
- 100.Whitehouse M.W., Fairlie D.P., Thong Y.H. Anti-Inflammatory Activity of the Isoquinoline Alkaloid, Tetrandrine, against Established Adjuvant Arthritis in Rats. Agents Actions. 1994;42:123–127. doi: 10.1007/BF01983477. [DOI] [PubMed] [Google Scholar]
- 101.Yin W., Wang T.-S., Yin F.-Z., Cai B.-C. Analgesic and Anti-Inflammatory Properties of Brucine and Brucine N-Oxide Extracted from Seeds of Strychnos Nux-Vomica. J. Ethnopharmacol. 2003;88:205–214. doi: 10.1016/S0378-8741(03)00224-1. [DOI] [PubMed] [Google Scholar]
- 102.Chen Q., Liu J., Zhuang Y., Bai L., Yuan Q., Zheng S., Liao K., Khan M.d.A., Wu Q., Luo C., et al. Identification of an IKKβ Inhibitor for Inhibition of Inflammation In Vivo and In Vitro. Pharmacol. Res. 2019;149:104440. doi: 10.1016/j.phrs.2019.104440. [DOI] [PubMed] [Google Scholar]
- 103.Zhang D., Li X., Hu Y., Jiang H., Wu Y., Ding Y., Yu K., He H., Xu J., Sun L., et al. Tabersonine Attenuates Lipopolysaccharide-Induced Acute Lung Injury via Suppressing TRAF6 Ubiquitination. Biochem. Pharmacol. 2018;154:183–192. doi: 10.1016/j.bcp.2018.05.004. [DOI] [PubMed] [Google Scholar]
- 104.Huang M., Hu Y.-Y., Dong X.-Q., Xu Q.-P., Yu W.-H., Zhang Z.-Y. The Protective Role of Oxymatrine on Neuronal Cell Apoptosis in the Hemorrhagic Rat Brain. J. Ethnopharmacol. 2012;143:228–235. doi: 10.1016/j.jep.2012.06.028. [DOI] [PubMed] [Google Scholar]
- 105.Greten F.R., Grivennikov S.I. Inflammation and Cancer: Triggers, Mechanisms, and Consequences. Immunity. 2019;51:27–41. doi: 10.1016/j.immuni.2019.06.025. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 106.Pfeffer C., Singh A. Apoptosis: A Target for Anticancer Therapy. Int. J. Mol. Sci. 2018;19:448. doi: 10.3390/ijms19020448. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 107.Kishore R., Verma S.K. Roles of STATs Signaling in Cardiovascular Diseases. JAK-STAT. 2012;1:118–124. doi: 10.4161/jkst.20115. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 108.Weischenfeldt J., Porse B. Bone Marrow-Derived Macrophages (BMM): Isolation and Applications. Cold Spring Harb. Protoc. 2008;2008:pdb.prot5080. doi: 10.1101/pdb.prot5080. [DOI] [PubMed] [Google Scholar]
- 109.Nanus D.E., Badoume A., Wijesinghe S.N., Halsey A.M., Hurley P., Ahmed Z., Botchu R., Davis E.T., Lindsay M.A., Jones S.W. Synovial Tissue from Sites of Joint Pain in Knee Osteoarthritis Patients Exhibits a Differential Phenotype with Distinct Fibroblast Subsets. EBioMedicine. 2021;72:103618. doi: 10.1016/j.ebiom.2021.103618. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 110.Bartok B., Firestein G.S. Fibroblast-like Synoviocytes: Key Effector Cells in Rheumatoid Arthritis. Immunol. Rev. 2010;233:233–255. doi: 10.1111/j.0105-2896.2009.00859.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 111.Griffiths M.M., Cannon G.W., Corsi T., Reese V., Kunzler K. Collagen-Induced Arthristis in Rats. In: Cope A.P., editor. Arthritis Research. Volume 136. Humana Press; Totowa, NJ, USA: 2007. pp. 201–214. Methods in Molecular Medicine. [DOI] [PubMed] [Google Scholar]
- 112.Chillingworth N.L., Donaldson L.F. Characterisation of a Freund’s Complete Adjuvant-Induced Model of Chronic Arthritis in Mice. J. Neurosci. Methods. 2003;128:45–52. doi: 10.1016/S0165-0270(03)00147-X. [DOI] [PubMed] [Google Scholar]
- 113.Dang Z., Jung K., Zhu L., Lai W., Xie H., Lee K.-H., Huang L., Chen C.-H. Identification and Synthesis of Quinolizidines with Anti-Influenza A Virus Activity. ACS Med. Chem. Lett. 2014;5:942–946. doi: 10.1021/ml500236n. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 114.Kamarul Zaman M.A., Mohamad Azzeme A. Plant Toxins: Alkaloids and Their Toxicities. GSC Biol. Pharm. Sci. 2018;6:21–29. doi: 10.30574/gscbps.2019.6.2.0003. [DOI] [Google Scholar]
- 115.Ching K.-C., Ng L.F.P., Chai C.L.L. A Compendium of Small Molecule Direct-Acting and Host-Targeting Inhibitors as Therapies against Alphaviruses. J. Antimicrob. Chemother. 2017;72:2973–2989. doi: 10.1093/jac/dkx224. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
On demand–EPI research unit.