Abstract
Purpose of Review
The purpose of this review is to highlight the radiographic assessments of utility in the evaluation of a pediatric patient with patellofemoral instability to facilitate a thorough work-up. Understanding of these measures is useful in understanding evolving research in this field, providing accurate patient risk assessment, and appropriately directing surgical decision-making.
Recent Findings
Recent literature has broadened the radiographic characterization of the pediatric patellar instability and its anatomic risk factors. Knee MRI can inform the assessment of skeletal maturity and novel axial alignment measurements may enhance our identification of patients at increased risk of recurrent instability. Additional improvements have been made in the objective measurement and classification of trochlear dysplasia.
Summary
Knee MRI-based skeletal age assessments may obviate the need for hand bone age assessments in growing children with patellofemoral instability. Novel objective measures exist in the evaluation of pediatric patellar instability both in the assessment of axial alignment and trochlear dysplasia. Future work should focus on how these measures can aid in guiding surgical decision-making.
Keywords: Pediatric patellofemoral instability, Radiographic evaluation in pediatrics, Axial alignment, Coronal alignment, Trochlear dysplasia, Pediatric knee morphology
Introduction
Lateral patellar dislocation (LPD) or recurrent patellofemoral instability (PFI) is a common condition affecting pediatric patients. The estimated annual incidence across all populations ranges from 2.29 to 77.4 per 100,000 person-years, but has been shown to be as high as 100 to 150 per 100,000 among late adolescent female cohorts [1–10]. Recent work suggests that the incidence may be slowly rising, resulting in increased rates of surgical intervention for stabilization [11–13]. The vast majority of primary instability events are known to occur as the result of sport participation [1, 4, 14, 15]; however, a variety of contact and non-contact mechanisms of injury have been described.
Numerous anatomic, demographic, and radiographic factors have been identified demonstrating increased risk of recurrent patellar instability [14–17]. Radiographic assessments including the presence of open regional physes, trochlear dysplasia, patella alta, and axial malalignment assessments (e.g., tibial tubercle-trochlear groove, or TT-TG, distance) are among the strongest and most consistent across studies of these risk factors. Recurrent ipsilateral patellar dislocation occurs in 15% to 54% of pediatric patients following primary dislocation [1, 7, 15, 16, 18–21], while contralateral dislocation is estimated to occur in 10–11% of pediatric patients [1, 7, 18]. Recurrence peaks during adolescence with most episodes occurring within 5 years of the first dislocation [15, 18]. Prior work has found that two-thirds of patients with both open regional physes of the knee and trochlear dysplasia at the time of their first dislocation sustained recurrent episodes of instability, carrying a 3-fold increased risk of recurrent instability events as compared to skeletally mature patients without dysplasia [15]. As such, the radiographic assessment of these patients plays a critical role in the counseling of patients and their families regarding recurrence and in directing surgical decision-making.
This article will provide a review of radiographic measures relevant to the evaluation of pediatric patients with PFI. The purpose is to equip the orthopedic clinician with an up-to-date and detailed review of a “complete” radiographic assessment for patients with patellar instability. While all of the described assessments are not necessary at every phase of clinical care, we feel that a global understanding will enable providers to better tailor their patient counseling and treatment plans. We will highlight measures and classifications to objectively describe and categorize skeletal age, axial and coronal deformity, and trochlear dysplasia, focusing on those that have been described or evaluated in pediatric cohorts and those that have been cited frequently in the orthopedic literature to help guide surgical intervention decisions. While surgical interventions will be mentioned as they relate to these measures, detailed discussion of these procedures, their indications, and their outcomes are beyond the intended scope of this review.
Skeletal Age Assessments
Skeletal age, or “bone age”, assessments provide significant value in the management of many orthopedic conditions. In the setting of PFI, they are critical both in the counseling of patients and families regarding the risk of recurrence, but also in determining the indications for and safety of various procedural interventions which may or may not be appropriate for patients with considerable remaining growth. The Greulisch and Pyle (G&P) atlas [22] estimates of bone age using left hand radiographs and remains the most widely utilized tool for estimating skeletal maturation. Patients with considerable growth remaining are contraindicated for some surgical interventions (e.g., tibial tubercle osteotomy) due to the risk of physeal arrest and may require physeal-respecting technical modifications to other orthopedic interventions for patellar instability. However, open physes also allow for the utilization of growth guidance techniques to address coronal limb deformities which can play a major role in PFI. The G&P method can help to estimate remaining years of growth and the anticipated timing of knee physeal closure. This, however, has the obvious limitation in that it requires imaging outside of the anatomic region undergoing evaluation (i.e., the knee) and is therefore not routinely or immediately available for review for all patients being evaluated for PFI. As such, efforts have been made to develop novel systems for bone age evaluation using knee magnetic resonance imaging (MRI), which is often obtained in the work-up of a patient with PFI.
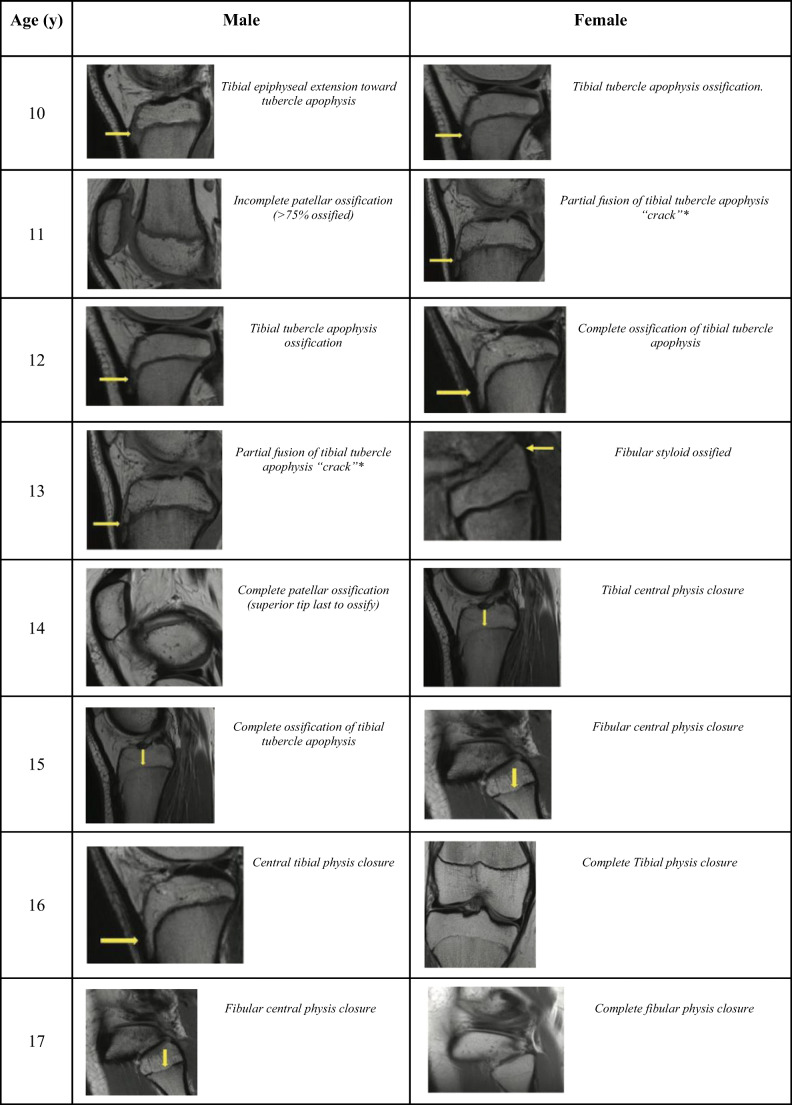
To avoid the need for additional imaging, bone age systems based on MRI imaging of the knee have been developed. The initial system developed by Pennock et al. [23] identified a series of stepwise changes that occur as the skeleton matures and found excellent correlation with chronological age (r = 0.978, p ≤ 0.001), outperforming the Greulisch and Pyle (G&P) derived bone age (r = 0.865, p ≤ 0.001). Intra- and interrater reliability using knee MRI for bone age assessment were also excellent, similar to that of the G&P atlas. Meza et al. [24••] subsequently developed a “shorthand” knee MRI bone age assessment (Fig. 1). This work also demonstrated a strong correlation with G&P-derived bone age and had good to excellent interrater reliability. Key skeletal maturity timepoints include (1) complete ossification of the tibial apophysis typically occurring at 12 in females and 15 in males, and (2) the start of physeal closure about the knee occurring first centrally about the tibia most commonly at 14 in females and 16 in males. Clinically, this indicates that patients with complete ossification of the tibial apophysis are 1–2 years away from the beginning of physeal closure and may be at lower risk for major growth disturbances from surgical interventions occurring near the physis. Further work is necessary to validate these findings in other cohorts, but both of these studies offer a reliable and reproducible means of skeletal age assessment that obviate the need for additional hand radiographs.
Fig. 1.
Reproducible regional physeal changes of the knee visualized on sagittal intermediate-weighted non-fat saturated images in males and females aged 10 to 17 years old. *Crack represents incomplete fusion and should cross entire apophysis. Figure adapted from Meza et al. [24••]
Coronal Limb Alignment
Coronal limb alignment is a critical component in the evaluation of pediatric patients with patellofemoral instability. Genu valgum, which can be physiologic in many pre-adolescents, contributes to an increased functional Q-angle and results in a laterally directed vector imposed by the extensor mechanism on the patella during knee motion thereby increasing the risk of lateral patellar dislocation events. Correction of genu valgum alone can improve patellofemoral tracking and effectively reduce the risk of patellar instability events [25–29]. While clinical evaluation of limb alignment on examination provides initial screening, subtle deformities can be missed or hidden due to body habitus or ligamentous laxity. The standing orthoroentgenogram [30], a composite, often weight-bearing, lower extremity radiographic image, compliments the clinical limb alignment assessment, allowing a more precise determination of the anatomic and mechanical axes of the lower extremity [25, 27, 31–34].
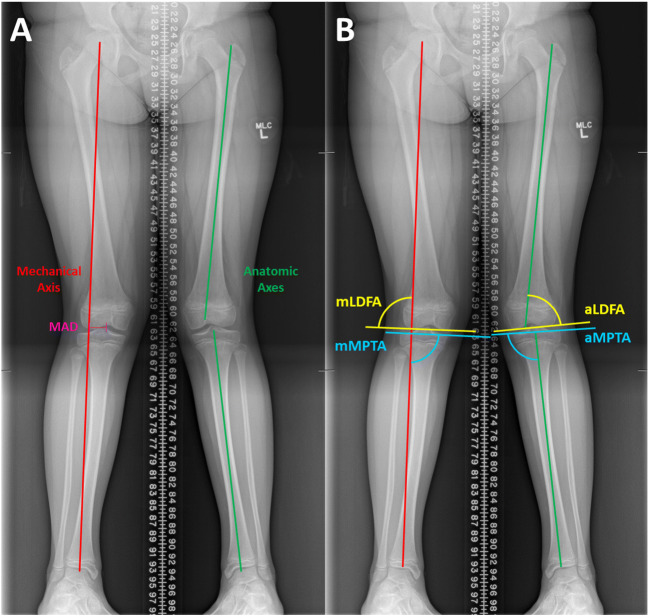
Limb alignment assessment on orthoroentgenogram begins with determination of the limb mechanical axis (drawn from the center of the femoral head to the center of the ankle joint) and the degree or zone of mechanical axis deviation (MAD), which is classified into zones (1–3, Fig. 2a), with Zone 0 being in the intercondylar notch, zone 1 being in the inner half of the hemijoint, zone 2 in the outer half of the hemijoint, and zone 3 outside of the weightbearing zone. If significant coronal deformity is present, evaluation should next consider what local deformities are contributing to the overall malalignment. Assessment of the anatomic and mechanical lateral distal femoral angle (mLDFA) and medial proximal tibial angle (MPTA) help identify whether the distal femur, proximal tibia, or a combination of the two is most contributing to the patient’s coronal plane malalignment (Fig. 2b) [29, 31, 33]. While normative values have been established for all of these angles in adolescent and adult patients, previous work [33] has shown that children under 7 years of age should use separate standards as normal given that physiologic changes in coronal limb alignment occur during growth in this age group that can correct without intervention. In addition to characterizing the severity of a patient’s coronal plane deformity at presentation, these angles are also utilized in follow-up to monitor the angular deformity correction following surgical intervention or with growth.
Fig. 2.
Measures for assessment of coronal plane angular deformity using standing alignment film. a Illustrates the mechanical axis, mechanical axis deviation (MAD), and anatomic axes of the femur and tibia. b Illustrates angles of interest relative to the mechanical and anatomical axes: lateral distal femoral angle (LDFA) and medial proximal tibial angle (MPTA)
Excessive genu valgum with MAD can serve as an indication for surgical intervention in PFI patients, as soft tissue procedures alone (e.g., MPFL) may be at greater risk of failure [29••]. Correction can be achieved via “guided growth,” using hemiepiphysiodesis for skeletally immature patients, and opening- or closing-wedge osteotomy for the skeletally mature [27, 29, 31, 35, 36]. The anatomic location of these interventions is based on the primary source of the underlying coronal deformity (tibia, femur, or both).
Lower Extremity Version Assessments
Excessive femoral anteversion and external tibial torsion impact rotational limb alignment, resulting in internal rotation of the distal femoral trochlea and external rotation of the distal attachment of the extensor mechanism. Together, these rotational abnormalities have been referred to as “miserable malalignment” and may increase the risk of patellar instability in addition to causing patellofemoral pain [37–40]. This is due to the maladaptive forces on the knee leading to greater tension on the MPFL and increased lateral patellofemoral tracking resulting in asymmetric tracking of the patella, subluxation or dislocation [41–43].
Evaluation of the rotation profile begins on clinical exam with evaluation of the thigh-foot axis (tibial version) and hip rotation (femoral version). When a pathologic degree of version is suspected, cross-sectional imaging can be used to more precisely quantify the rotational profile, which has traditionally utilized osseous data from computed tomography (CT) scanning [41–44]. Notably, MRI may also be used and may be a more desirable approach in adolescents due to the decreased levels of radiation exposure compared to CT scanning. A variety of measurement techniques have been described using different key axial slices of the femur and tibia [40, 45–47]; however, regardless of technique, the normal version of the femur is approximately 22° in children (range 0–65) as compared to roughly 15° (range 10–20) in adults [48–51]. In children, the average version of the tibia is 20° (range 0–45) [52].
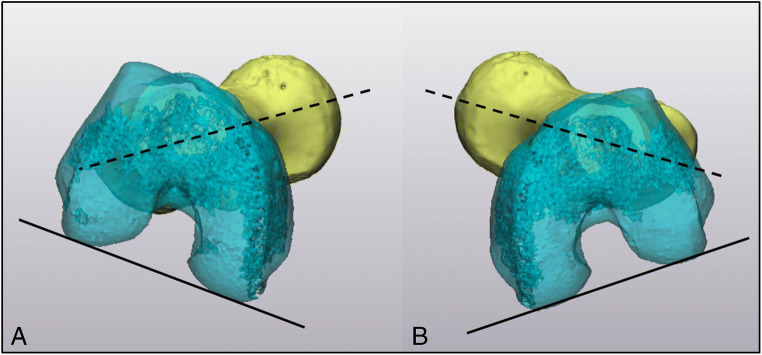
It is important to consider these imaging results in the context of the patient, as many young children have physiologic degrees of femoral anteversion and/or tibial torsion that tends to spontaneously resolve [41, 42]. Additionally, some ligamentously lax patients with significant femoral anteversion are still capable of “normal” mobility and may not require surgical intervention [43•]. While many cases of pediatric femoral anteversion and/or tibial torsion may not require surgical intervention, those pediatric patients dealing with symptomatic PFI in the setting of significant rotation deformity may be considered candidates from femoral or tibial derotational osteotomies [40, 41, 43]. However, it is important to continue to monitor coronal plane alignment post-operatively, as rotational osteotomies have been shown to impact coronal alignment [41, 43] (Fig. 3).
Fig. 3.
CT version study with 3D reconstruction of the right (a) and left (b) legs in a patient with patellar instability and femoral anteversion. Versional assessment is determined by finding the angle made by the femoral neck (dashed line) and the posterior condylar axis of the femur (solid line). In this patient, femoral anteversion was 36 degrees in the right femur and 35 degrees in the left femur
Patellar Height
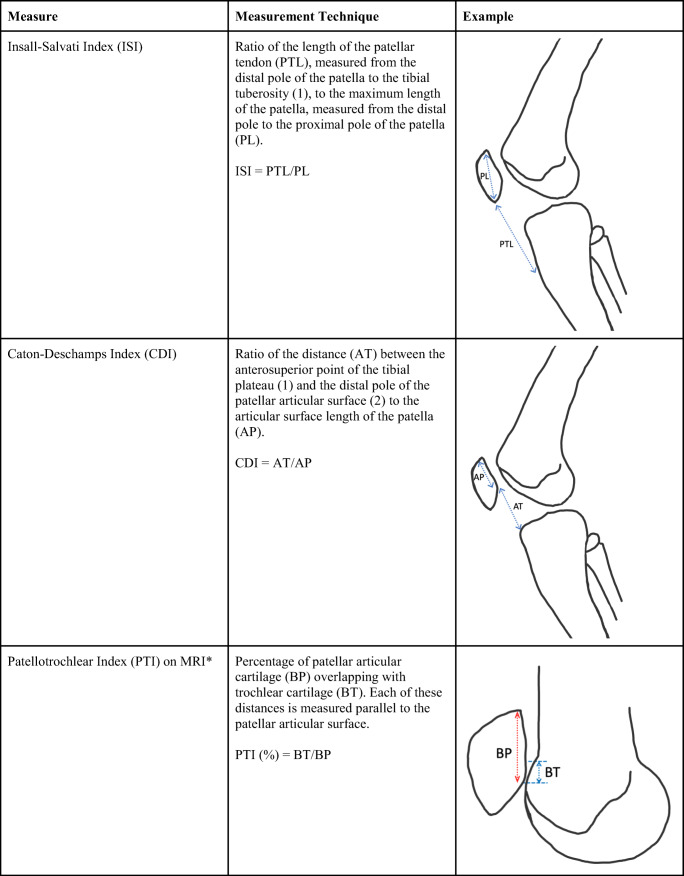
Patella alta is a well-established risk factor for PFI as this results in late engagement of the bony stability of the patellofemoral articulation during knee flexion [14, 16, 17]. Several methods have been described to quantify patellar height on radiograph including the Caton-Deschamps Index [53], the Insall-Salvati index (ISI) [54, 55], the Koshino index (KI) [56], and the Blackburne-Peel (BP) ratio [57] (Fig. 4). Some of these, however, have limited utility in the pediatric population due to complex measurement technique or measurement reliability impacted by ossification changes occurring during growth. Thévenin-Lemoine et al. found the Caton Deschamps index (CDI) to be both simple and reliable, representing the preferred measure of patellar height on radiographs in children and adolescents [58]. Their study findings also indicated that patellar height appears to decrease with age, reaching adult normative values by 12 years old.
Fig. 4.
Measurement techniques for sagittal alignment ratios of ISI, CDI, and PTI. *PTI measured on the midline sagittal section MRI through the patella with the thickest articular cartilage and maximal length of the patella
While all of the aforementioned techniques were first described using lateral radiographs as a basis for measurement, MRI-based comparisons have been made with evidence indicating acceptable correlation between radiographs and 3-dimensional imaging (CT and/or MRI) for both ISI and CDI in largely adult cohorts [59–61]. In skeletally immature patients, ISI has demonstrated comparable radiograph and MRI measurements [60•], but no study has evaluated radiograph- and MRI-derived CDI measures exclusively in this age group. Subtle differences between these modalities are likely the result of the discrepancy between articular cartilage geometry and subchondral osseous structures seen on radiograph which is accentuated in the skeletally-immature patient.
The patellotrochlear index (PTI) is another patellar height assessment described by Biedert et al. that uses sagittal MRI to evaluate the overlap of articular surfaces on the patella and trochlea [62], which authors argue is the important anatomic factor of patellar height in PFI. Benefits of this measure include the evaluation of true patellotrochlear articular congruence, immunity from changes posed by osseous variations or previous surgeries, high reliability, and measurement in full extension limiting variation imposed by knee flexion angles required by other measures [59, 62–64]. Despite these purported benefits, there is limited evidence validating this measure as a PFI risk factor in skeletally immature patients or a measure to specifically guide surgical decision-making. Therefore, based on the available evidence, the preferred method of measuring patellar height in pediatric patients is uncertain, but limited evidence suggests that CDI is the preferred method on radiographs, while ISI may be more appropriate with MRI. The PTI also shows promise as its measure is uniquely relevant to the anatomic basis of PFI.
Treatment options described for the PFI patient with excessive patella alta include distalizing tibial tubercle osteotomy in skeletally mature patients [65] or patellar tendon advancement/imbrication in those who are skeletally immature [66–68]. While clinically significant cutoffs exist for patella alta, indications for and necessity of correction remains unclear, particularly when other surgical interventions are already being implemented [69, 70].
Axial Alignment Assessments
The axial alignment of the extensor mechanism refers to the relative translational position of the patella, patellar tendon, trochlea, and tibial tubercle on axial imaging in addition to the rotational relationship of the distal femoral and proximal tibia. A more lateral distal attachment of the patellar tendon increases the lateral forces imposed on the patella and extensor mechanism during knee flexion [71]. Lateralization of the tibial tubercle relative to the distal femoral trochlea is quantified using the tibial tubercle-trochlear groove (TT-TG) distance which is one of the most frequently cited modifiable risk factors for recurrent PFI [17, 18, 72–78]. Normative data in adults suggests that TT-TG distances below 15 mm are considered normal while values over 20 mm may indicate surgical correction in symptomatic patients [78]. However, like many radiographic measures, values in adult populations are not directly applicable to pediatric patients. Dickens et al. validated TT-TG using MRI in skeletally immature patients showing that this measure gradually increased with age reaching adult-based normative values by approximately 15 years of age [79]. The mean TT-TG of in pediatric patients (9 months to 15 years old) with and without instability was 8.5 mm and 12.1 mm, respectively. A percentile-based growth curve was generated for TT-TG distance in the skeletally immature patient [79].
Although CT is the gold standard for visualizing bony structures, such as TT-TG, MRI is becoming the preferred comprehensive advanced imaging modality of choice in the imaging work-up of these patients as it also provides information regarding cartilaginous trochlear morphology, integrity of the regional ligaments, and tendons without the use of ionizing radiation. However, the measured TT-TG distance may differ between CT and MRI due to the use of different anatomic landmarks. While the initial published paper found no significant difference in TT-TG distances between CT and MRI with excellent interrater and intrarater [72]. More recent work has demonstrated differences with CT measuring approximately 2 mm greater than MRI. This difference increased with greater TT-TG measures (i.e., over 20 mm). Similarly, new studies focusing on the skeletally immature population have also shown that CT produced relatively greater measurements when compared to MRI, with a mean difference of 4 mm and 2 mm using bony and cartilaginous landmarks, respectively [80].
Two newer measures have been described exploring the concept of containment of the extensor mechanism by the trochlear groove. Mistovich et al. examined the axial width of the patellar tendon beyond the lateral trochlear ridge (PT-LTR) and compared this to the TT-TG in addition to numerous other axial alignment measures in pediatric patients with and without patellar instability [81•]. The authors found the PT-LTR distance to be reliable and discriminative for patellofemoral instability in addition to showing similar sensitivity but higher specificity for this condition than TT-TG. Building on this patellofemoral containment logic, Weltsch et al. explored the tibial tubercle to lateral trochlear ridge (TT-LTR) distance and found that the localization of the tibial tubercle outside of the lateral trochlear ridge was the only axial MRI measure predictive of recurrent patellar instability in their multivariate logistic regression analysis [82••]. While neither study has examined the surgical implications of these measures, their findings together suggest that our understanding of the axial alignment in pediatric patient with PFI extends beyond just the TT-TG distance, with localization of the tibial tubercle outside of the lateral trochlear ridge being more important than any one threshold TT-TG value.
Pathologic axial malalignment is both a risk factor for recurrent instability, and for failure of surgical stabilization with soft tissue reconstruction (i.e., MPFL) alone [83]. Therefore, in the setting of elevated axial alignment measures, consideration may be made for realignment procedures. In skeletally mature patients, this can be done with tibial tubercle medialization or anteromedialization [84, 85] to better centralize the extensor mechanism within the trochlear groove during knee motion. Due to the proximity to the proximal tibial growth plate and the risk of physeal arrest, this procedure is contraindicated in skeletally immature patients in whom deferred surgical treatment or soft tissue transfers (e.g., Roux-Goldwaithe) may be considered [86–88].
Trochlear Dysplasia
Trochlear dysplasia, defined as flattening or even convexity of the femoral trochlear groove, has been identified as a significant risk factor for recurrent patellar instability [14, 15, 37, 89–91]. Distal femur morphology including the trochlear groove is established early in life, with dysplasia likely having both congenital and developmental factors resulting from aberrant forces applied to the patellofemoral joint during growth due to lateral tracking and/or recurrent instability [92, 93]. A dysplastic trochlea decreases the bony stability of the patellofemoral joint resulting in reduced restraint to lateral translation of the patella with increased stress placed upon the MPFL (Fig. 5).
Fig. 5.
Measurement techniques for axial alignment assessments including TT-TG, PT-LTR, and LTR-TT are described and presented with representative drawings
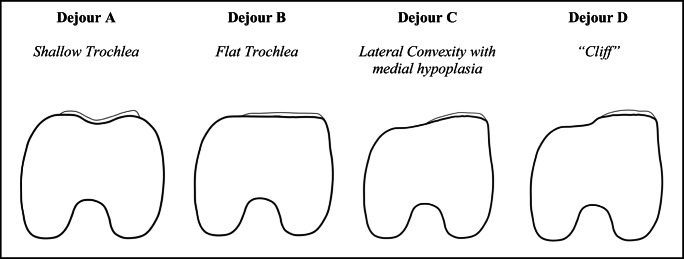
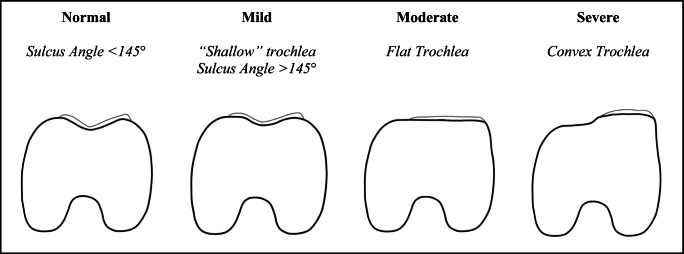
Traditionally, trochlear dysplasia assessments in the literature have been largely based on the classification system described by Dejour et al. [37]. This system, which uses a true lateral radiograph of the knee, categorizes patients into four types (A through D) based on the presence of radiographic findings. The hallmark finding of a Dejour A trochlea is the crossing sign which indicates a shallow trochlear groove (sulcus angle > 145°). Dejour B trochleae have both the crossing sign and a supratrochlear spur which correlates with a flat or convex trochlea. Dejour C findings include a crossing sign and a double contour sign manifested by asymmetry of the trochlear facets while Dejour D having all of these radiographic changes. Given the limitations and reproducibility of true lateral radiographs, some have described MRI adaptations of this classification by evaluating the contour of the proximal trochlea [94••]. However, despite this system being widely utilized clinically and within the literature, there has been controversy regarding its utility as it is notably sensitive to the quality of radiographs, has low intra- and interrater reliability, and does not provide distinct guidance for surgical decision-making [89, 94, 95]. More recently, the MRI-based Oswestry-Bristol classification (OBC) was developed in part to address some of these limitations and provide a more reliable system for categorizing the severity of trochlear dysplasia [96•]. The OBC grades dysplasia as normal, mild, moderate, or severe (corresponding to a normal, shallow, flat, or convex proximal trochlea, respectively). Though early in its use and not yet validated in skeletally immature patients, this system has demonstrated greater reliability than the Dejour classification [97, 98]. The Dejour and Oswestry-Bristol classifications and their characteristic findings are depicted in Figs. 6 and 7, respectively.
Fig. 6.
The Dejour classification of trochlear dysplasia is described along with representative figures depicting expected findings on axial MRI (MRI Dejour [94•]) at the proximal-most aspect of the trochlear cartilage for each subtype are presented
Fig. 7.
The Oswestry-Bristol classification of trochlear dysplasia is described and presented along with representative axial MRI findings at the proximal-most aspect of the trochlear cartilage
In addition to categorical classification systems like Dejour and OBC, a number of quantitative measures of trochlear morphology have also been described including the sulcus angle (SA), lateral trochlear inclination (LTI) angle [99, 100], trochlear depth index (TDI) [101], and medial condyle trochlear offset (MCTO) [94••]. While sulcus angle was one of the earliest objective measures of dysplasia prescribed on merchant radiographs of the knee, its reliability is impacted by knee flexion angle, age of the patient, and precise selection of location along the groove for measurements [92, 93, 102, 103]. Sulcus angle has been adapted to measure trochlear morphology on axial CT and MRI images using bone and cartilage landmarks, but variability exists in the literature regarding the location of measurement on axial imaging (proximal-most visible trochlear cartilage, full articular cartilage across both trochlear facets, or at the level of measurement of the posterior condylar axis) [104, 105]. Additional work has further demonstrated the limitations of bony assessments of trochlear morphology in the pediatric population [106, 107]. In skeletally immature patients (7–16 years old), Stephanovich et al. found that pediatric-modified LTI, TDI, and MCTO measures demonstrated better reliability and improved detection of patients with patellar instability when compared to radiographic or MRI-based Dejour classification. LTI, TDI, and MCTO critical cutoffs of 17°, 3 mm, and 1 mm, respectively, were identified [94••]. Further work is needed to determine the clinical implications of these more objective assessments, but their diagnostic power, reliability, and accuracy may facilitate enhanced understanding of trochlear dysplasia in the pediatric patient. Objective trochlear dysplasia measures are compared in Fig. 8.
Fig. 8.
Objective trochlear measurements to identify and characterize trochlear dysplasia on axial MRI of the knee are presented. Measurement techniques for SA, LTI, TDI, and MCTO are described with representative drawings
Currently, trochleoplasty is the only described surgical procedure that directly addresses the dysplastic trochlea. A variety of techniques for trochleoplasty have been described [108–110], but the general principles of the procedure are to increase the concavity and lateralize the trochlear groove to both enhance patellofemoral bony stability during knee flexion and reduce axial malalignment. Controversy exists [111–116] regarding the indications for use of trochleoplasty and the preferred surgical approach for patients with recurrent PFI and severe trochlear dysplasia when alternative interventions to address complex instability (namely tibial tubercle osteotomy) are available. While a growing body of evidence has demonstrated highly successful patellofemoral stabilization using trochleoplasty in pediatric [117–119] and adult [120, 121] patients with severe trochlear dysplasia, improved evidence is needed to clarify the indications for this procedure in patients with PFI as considerable variation in the rate of reported complications exists in the published literature [122, 123].
Conclusions
Due to the complex anatomic considerations impacting patellofemoral instability and the changes that can occur during skeletal maturity, providers caring for this condition should be aware of the numerous tools and measures that exist to appropriately evaluate skeletal maturity, coronal alignment, lower extremity limb version, patellar height, axial extensor mechanism alignment, and trochlear morphology in the pediatric PFI patient. This study provides an in-depth review of the most up-to-date literature regarding the evolution of imaging assessments most relevant to children and adolescents.
While all of these assessments described are not necessary to evaluate at every stage of clinical care, familiarity with each enables providers to comprehensively evaluate, counsel, and treat this unique patient population. The authors’ preferred approach to the radiographic assessment of pediatric patients with patellar instability is as follows:
Skeletal age assessment with knee MRI can be safely and reliably utilized in lieu of hand radiographs in risk counseling and surgical decision-making.
Clinically apparent valgus should be explored radiographically with standing alignment imaging. Treatment implications of this study depend on the severity of MAD, other concomitant risk factors, and remaining growth.
Clinically significant version abnormalities can be further assessed with rotational MRI or CT studies; however, the indications for versional correction remain controversial.
Patellar height is assessed with radiographs and knee MRI using CDI. Values > 1.3 are considered abnormal and correction is considered if surgery has been indicated.
Axial alignment is assessed on Knee MRI using TT-TG, PT-LTR, and LTR-TT measures. Abnormal TT-TG is used primarily to indicate surgical correction; however, the other measures may influence decision-making in otherwise borderline cases.
Trochlear morphology is assessed both subjectively and objectively for the diagnosis and characterization of trochlear dysplasia, but at this time their impact on surgical decision-making in pediatric patients is not clear and varies by provider. The measures and classifications described in this review are actively being utilized in ongoing research to further our understanding of the femoral trochlea and the appropriate indications for correction in this patient population.
Author Contribution
This manuscript has not been published previously. All authors made significant contributions to multiple aspects of the study as described in the ICMJE authorship criteria recommendations, detailed here:
• Kevin J. Orellana: substantial contributions to data acquisition, data interpretation, manuscript drafting, critical revision, and final approval of the version to be published.
• Morgan G. Batley: substantial contributions to data acquisition, data interpretation, manuscript drafting, critical revision, and final approval of the version to be published.
• J. Todd R. Lawrence: substantial contributions to concept and design, data interpretation, critical revision, and final approval of the version to be published.
• Jie C. Nguyen: substantial contributions to concept and design, data interpretation, critical revision, and final approval of the version to be published.
• Brendan A. Williams: substantial contributions to conception and design, data acquisition, data interpretation, manuscript drafting, critical revision, and final approval of the version to be published.
Declarations
Conflict of Interest
Kevin J. Orellana, Morgan G. Batley, Jie C. Nguyen, and Brendan A. Williams declare that they have no conflict of interest. J. Todd R. Lawrence is a board or committee member of the American Academy of Pediatrics and has received IP royalties from Sawbones/Pacific Research Laboratories.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Footnotes
This article is part of the Topical Collection on Pediatric Orthopedics
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Contributor Information
Kevin J. Orellana, Email: kevin.orellana01@utrgv.edu
Morgan G. Batley, Email: batleym@chop.edu
J. Todd R. Lawrence, Email: lawrencej@chop.edu
Jie C. Nguyen, Email: nguyenj6@chop.edu
Brendan A. Williams, Email: williamsba@chop.edu
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
- 1.Fithian DC, Paxton EW, Stone ML, Silva P, Davis DK, Elias DA, et al. Epidemiology and natural history of acute patellar dislocation. Am J Sports Med. 2004;32:1114–1121. doi: 10.1177/0363546503260788. [DOI] [PubMed] [Google Scholar]
- 2.Sanders TL, Pareek A, Hewett TE, Stuart MJ, Dahm DL, Krych AJ. Incidence of first-time lateral patellar dislocation: a 21-year population-based study. Sports Health. 2018;10:146–151. doi: 10.1177/1941738117725055. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Sillanpää P, Mattila VM, Iivonen T, Visuri T, Pihlajamäki H. Incidence and risk factors of acute traumatic primary patellar dislocation. Med Sci Sports Exerc. 2008;40:606–611. doi: 10.1249/MSS.0b013e318160740f. [DOI] [PubMed] [Google Scholar]
- 4.Nietosvaara Y, Aalto K, Kallio PE. Acute patellar dislocation in children: incidence and associated osteochondral fractures. J Pediatr Orthop. 1994;14:513–515. doi: 10.1097/01241398-199407000-00018. [DOI] [PubMed] [Google Scholar]
- 5.Buchner M, Baudendistel B, Sabo D, Schmitt H. Acute traumatic primary patellar dislocation: long-term results comparing conservative and surgical treatment. Clin J Sport Med. 2005;15:62–66. doi: 10.1097/01.jsm.0000157315.10756.14. [DOI] [PubMed] [Google Scholar]
- 6.Kiviluoto O, Pasila M, Santavirta S, Sundholm A, Hämäläinen M. Recurrences after conservative treatment of acute dislocation of the patella. Ital J Sport Traumatol. 1986;3:159–162. [Google Scholar]
- 7.Gravesen KS, Kallemose T, Blønd L, Troelsen A, Barfod KW. High incidence of acute and recurrent patellar dislocations: a retrospective nationwide epidemiological study involving 24.154 primary dislocations. Knee Surg Sports Traumatol Arthrosc. 2018;26:1204–1209. doi: 10.1007/s00167-017-4594-7. [DOI] [PubMed] [Google Scholar]
- 8.Atkin DM, Fithian DC, Marangi KS, Stone ML, Dobson BE, Mendelsohn C. Characteristics of patients with primary acute lateral patellar dislocation and their recovery within the first 6 months of injury. Am J Sports Med. 2000;28:472–479. doi: 10.1177/03635465000280040601. [DOI] [PubMed] [Google Scholar]
- 9.Hsiao M, Owens BD, Burks R, Sturdivant RX, Cameron KL. Incidence of acute traumatic patellar dislocation among active-duty United States military service members. Am J Sports Med. 2010;38:1997–2004. doi: 10.1177/0363546510371423. [DOI] [PubMed] [Google Scholar]
- 10.Waterman BR, Belmont PJ, Jr, Owens BD. Patellar dislocation in the United States: role of sex, age, race, and athletic participation. J Knee Surg. 2012;25:51–57. doi: 10.1055/s-0031-1286199. [DOI] [PubMed] [Google Scholar]
- 11.Poorman MJ, Talwar D, Sanjuan J, Baldwin KD, Sutliff N, Franklin CC. Increasing hospital admissions for patellar instability: a national database study from 2004 to 2017. Phys Sportsmed. 2020;48:215–221. doi: 10.1080/00913847.2019.1680088. [DOI] [PubMed] [Google Scholar]
- 12.Arshi A, Cohen JR, Wang JC, Hame SL, McAllister DR, Jones KJ. Operative management of patellar instability in the United States: an evaluation of national practice patterns, surgical trends, and complications. Orthop J Sports Med. 2016;4:2325967116662873. doi: 10.1177/2325967116662873. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.•.KH MF, Coene RP, Feldman L, Miller PE, Heyworth BE, Kramer DE, et al. Increased incidence of acute patellar dislocations and patellar instability surgical procedures across the United States in paediatric and adolescent patients. J Child Orthop. 2021;15:149–156. doi: 10.1302/1863-2548.15.200225. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Lewallen L, McIntosh A, Dahm D. First-time patellofemoral dislocation: risk factors for recurrent instability. J Knee Surg. 2015;28:303–309. doi: 10.1055/s-0034-1398373. [DOI] [PubMed] [Google Scholar]
- 15.Lewallen LW, McIntosh AL, Dahm DL. Predictors of recurrent instability after acute patellofemoral dislocation in pediatric and adolescent patients. Am J Sports Med. 2013;41:575–581. doi: 10.1177/0363546512472873. [DOI] [PubMed] [Google Scholar]
- 16.Jaquith BP, Parikh SN. Predictors of recurrent patellar instability in children and adolescents after first-time dislocation. J Pediatr Orthop. 2017;37:484–490. doi: 10.1097/BPO.0000000000000674. [DOI] [PubMed] [Google Scholar]
- 17.Christensen TC, Sanders TL, Pareek A, Mohan R, Dahm DL, Krych AJ. Risk factors and time to recurrent ipsilateral and contralateral patellar dislocations. Am J Sports Med. 2017;45:2105–2110. doi: 10.1177/0363546517704178. [DOI] [PubMed] [Google Scholar]
- 18.Sanders TL, Pareek A, Hewett TE, Stuart MJ, Dahm DL, Krych AJ. High rate of recurrent patellar dislocation in skeletally immature patients: a long-term population-based study. Knee Surg Sports Traumatol Arthrosc. 2018;26:1037–1043. doi: 10.1007/s00167-017-4505-y. [DOI] [PubMed] [Google Scholar]
- 19.Stefancin JJ, Parker RD. First-time traumatic patellar dislocation: a systematic review. Clin Orthop Relat Res. 2007;455:93–101. doi: 10.1097/BLO.0b013e31802eb40a. [DOI] [PubMed] [Google Scholar]
- 20.Mäenpää H, Lehto MU, Patellar dislocation. The long-term results of nonoperative management in 100 patients. Am J Sports Med. 1997;25:213–217. doi: 10.1177/036354659702500213. [DOI] [PubMed] [Google Scholar]
- 21.Zhang K, Jiang H, Li J, Fu W. Comparison between surgical and nonsurgical treatment for primary patellar dislocations in adolescents: a systematic review and meta-analysis of comparative studies. Orthop J Sports Med. 2020;8:2325967120946446. doi: 10.1177/2325967120946446. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Greulich WW, Pyle SI. Radiographic atlas of skeletal development of the hand and wrist. Stanford University Press; 1959. [Google Scholar]
- 23.Pennock AT, Bomar JD. Bone age assessment utilizing knee MRI. Orthop J Sports Med. 2017;5:2325967117S00428. doi: 10.1177/2325967117S00428. [DOI] [Google Scholar]
- 24.••.Meza BC, LaValva SM, Aoyama JT, DeFrancesco CJ, Striano BM, Carey JL, et al. A novel shorthand approach to knee bone age using MRI: a validation and reliability study. Orthop J Sports Med. 2021;9:23259671211021582. doi: 10.1177/23259671211021582. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Navali AM, Bahari LAS, Nazari B. A comparative assessment of alternatives to the full-leg radiograph for determining knee joint alignment. Sports Med Arthrosc Rehabil Ther Technol. 2012;4:40. doi: 10.1186/1758-2555-4-40. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Teitge R. Osteotomy in the treatment of patellofemoral instability. Tech Knee Surg. 2006;5:2–18. doi: 10.1097/00132588-200603000-00003. [DOI] [Google Scholar]
- 27.•.Wilson PL, Black SR, Ellis HB, Podeszwa DA. Distal femoral valgus and recurrent traumatic patellar instability: is an isolated varus producing distal femoral osteotomy a treatment option? J Pediatr Orthop. 2018;38:e162–e167. doi: 10.1097/BPO.0000000000001128. [DOI] [PubMed] [Google Scholar]
- 28.Frings J, Krause M, Akoto R, Wohlmuth P, Frosch K-H. Combined distal femoral osteotomy (DFO) in genu valgum leads to reliable patellar stabilization and an improvement in knee function. Knee Surg Sports Traumatol Arthrosc. 2018;26:3572–3581. doi: 10.1007/s00167-018-5000-9. [DOI] [PubMed] [Google Scholar]
- 29.••.Lin KM, Fabricant PD. CORR synthesis: can guided growth for angular deformity correction be applied to management of pediatric patellofemoral instability? Clin Orthop Relat Res. 2020;478:2231–2238. doi: 10.1097/CORR.0000000000001311. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Sabharwal S, Kumar A. Methods for assessing leg length discrepancy. Clin Orthop Relat Res. 2008;466:2910–2922. doi: 10.1007/s11999-008-0524-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Palmer RC, Podeszwa DA, Wilson PL, Ellis HB. Coronal and transverse malalignment in pediatric patellofemoral instability. J Clin Med Res. 2021;10. 10.3390/jcm10143035. [DOI] [PMC free article] [PubMed]
- 32.Unal M, Ercan S, Budeyri A, Toprak U, Şalkaci A. Anatomical axis validation of lower extremity for different deformities: A radiological study. SAGE Open Med. 2020;8:2050312120923822. doi: 10.1177/2050312120923822. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Sabharwal S, Zhao C, Edgar M. Lower limb alignment in children: reference values based on a full-length standing radiograph. J Pediatr Orthop. 2008;28:740–746. doi: 10.1097/BPO.0b013e318186eb79. [DOI] [PubMed] [Google Scholar]
- 34.Schmale GA, Bayomy AF, O’Brien AO, Bompadre V. The reliability of full-length lower limb radiographic alignment measurements in skeletally immature youth. J Child Orthop. 2019;13:67–72. doi: 10.1302/1863-2548.13.180087. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Inan M, Chan G, Bowen JR. Correction of angular deformities of the knee by percutaneous hemiepiphysiodesis. Clin Orthop Relat Res. 2007;456:164–169. doi: 10.1097/01.blo.0000246560.65714.c8. [DOI] [PubMed] [Google Scholar]
- 36.Kearney SP, Mosca VS. Selective hemiepiphyseodesis for patellar instability with associated genu valgum. J Orthop. 2015;12:17–22. doi: 10.1016/j.jor.2015.01.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Dejour H, Walch G, Nove-Josserand L, Guier C. Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc. 1994;2:19–26. doi: 10.1007/BF01552649. [DOI] [PubMed] [Google Scholar]
- 38.Lee TQ, Anzel SH, Bennett KA, Pang D, Kim WC. The influence of fixed rotational deformities of the femur on the patellofemoral contact pressures in human cadaver knees. Clin Orthop Relat Res. 1994:69–74. Available: https://www.ncbi.nlm.nih.gov/pubmed/8168325. [PubMed]
- 39.Dejour D, Le Coultre B. Osteotomies in patello-femoral instabilities. Sports Med Arthrosc. 2018;26:8–15. doi: 10.1097/JSA.0000000000000183. [DOI] [PubMed] [Google Scholar]
- 40.Bruce WD, Stevens PM. Surgical correction of miserable malalignment syndrome. J Pediatr Orthop. 2004;24:392–396. doi: 10.1097/00004694-200407000-00009. [DOI] [PubMed] [Google Scholar]
- 41.Nelitz M. Femoral derotational osteotomies. Curr Rev Musculoskelet Med. 2018;11:272–279. doi: 10.1007/s12178-018-9483-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Parikh S, Noyes FR. Patellofemoral disorders: role of computed tomography and magnetic resonance imaging in defining abnormal rotational lower limb alignment. Sports Health. 2011;3:158–169. doi: 10.1177/1941738111399372. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.•.Stiebel M, Paley D. Derotational osteotomies of the femur and tibia for recurrent patellar instability. Oper Tech Sports Med. 2019;27:150691. doi: 10.1016/j.otsm.2019.150691. [DOI] [Google Scholar]
- 44.Mahboubi S, Horstmann H. Femoral torsion: CT measurement. Radiology. 1986;160:843–844. doi: 10.1148/radiology.160.3.3737928. [DOI] [PubMed] [Google Scholar]
- 45.Imhoff FB, Beitzel K, Zakko P, Obopilwe E, Voss A, Scheiderer B, et al. Derotational osteotomy of the distal femur for the treatment of patellofemoral instability simultaneously leads to the correction of frontal alignment: a laboratory cadaveric study. Orthop J Sports Med. 2018;6:2325967118775664. doi: 10.1177/2325967118775664. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Liodakis E, Doxastaki I, Chu K, Krettek C, Gaulke R, Citak M, et al. Reliability of the assessment of lower limb torsion using computed tomography: analysis of five different techniques. Skelet Radiol. 2012;41:305–311. doi: 10.1007/s00256-011-1185-4. [DOI] [PubMed] [Google Scholar]
- 47.Nelitz M, Lippacher S, Reichel H, Dornacher D. Evaluation of trochlear dysplasia using MRI: correlation between the classification system of Dejour and objective parameters of trochlear dysplasia. Knee Surg Sports Traumatol Arthrosc. 2014;22:120–127. doi: 10.1007/s00167-012-2321-y. [DOI] [PubMed] [Google Scholar]
- 48.Tomczak RJ, Guenther KP, Rieber A, Mergo P, Ros PR, Brambs HJ. MR imaging measurement of the femoral antetorsional angle as a new technique: comparison with CT in children and adults. Am J Roentgenol. 1997;168:791–794. doi: 10.2214/ajr.168.3.9057536. [DOI] [PubMed] [Google Scholar]
- 49.Tönnis D, Heinecke A. Acetabular and femoral anteversion: relationship with osteoarthritis of the hip. J Bone Joint Surg Am. 1999;81:1747–1770. doi: 10.2106/00004623-199912000-00014. [DOI] [PubMed] [Google Scholar]
- 50.Maruyama M, Feinberg JR, Capello WN, D’Antonio JA. The Frank Stinchfield Award: morphologic features of the acetabulum and femur: anteversion angle and implant positioning. Clin Orthop Relat Res. 2001:52–65. Available: https://www.ncbi.nlm.nih.gov/pubmed/11764371. [PubMed]
- 51.Hartel MJ, Petersik A, Schmidt A, Kendoff D, Nüchtern J, Rueger JM, et al. Determination of femoral neck angle and torsion angle utilizing a novel three-dimensional modeling and analytical technology based on CT datasets. PLoS One. 2016;11:e0149480. doi: 10.1371/journal.pone.0149480. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Fabry G, Cheng LX, Molenaers G. Normal and abnormal torsional development in children. Clin Orthop Relat Res. 1994:22–6. Available: https://www.ncbi.nlm.nih.gov/pubmed/8168306. [PubMed]
- 53.Caton J, Deschamps G, Chambat P, Lerat JL, Dejour H. Patella infera. Apropos of 128 cases. Rev Chir Orthop Reparatrice Appar Mot. 1982;68:317–325. [PubMed] [Google Scholar]
- 54.Insall J, Salvati E. Patella position in the normal knee joint. Radiology. 1971;101:101–104. doi: 10.1148/101.1.101. [DOI] [PubMed] [Google Scholar]
- 55.Grelsamer RP, Meadows S. The modified Insall-Salvati ratio for assessment of patellar height. Clin Orthop Relat Res. 1992:170–6. Available: https://www.ncbi.nlm.nih.gov/pubmed/1516309. [PubMed]
- 56.Koshino T, Sugimoto K. New measurement of patellar height in the knees of children using the epiphyseal line midpoint. J Pediatr Orthop. 1989;9:216–218. [PubMed] [Google Scholar]
- 57.Blackburne JS, Peel TE. A new method of measuring patellar height. J Bone Joint Surg Br. 1977;59:241–242. doi: 10.1302/0301-620X.59B2.873986. [DOI] [PubMed] [Google Scholar]
- 58.Thévenin-Lemoine C, Ferrand M, Courvoisier A, Damsin J-P, Ducou le Pointe H, Vialle R. Is the Caton-Deschamps index a valuable ratio to investigate patellar height in children? J Bone Joint Surg Am. 2011;93:e35. doi: 10.2106/JBJS.J.00759. [DOI] [PubMed] [Google Scholar]
- 59.Verhulst FV, van Sambeeck JDP, Olthuis GS, van der Ree J, Koëter S. Patellar height measurements: Insall-Salvati ratio is most reliable method. Knee Surg Sports Traumatol Arthrosc. 2020;28:869–875. doi: 10.1007/s00167-019-05531-1. [DOI] [PubMed] [Google Scholar]
- 60.•.Kurowecki D, Shergill R, Cunningham KM, Peterson DC, Takrouri HSR, Habib NO, et al. A comparison of sagittal MRI and lateral radiography in determining the Insall-Salvati ratio and diagnosing patella alta in the pediatric knee. Pediatr Radiol. 2021. 10.1007/s00247-021-05207-4. Found that there were not statistically significant differences between mean ISI values on MRI as compared to traditional radiographs. These findings provide evidence in favor of using ISI to measure patellar height on sagittal MRIs. [DOI] [PubMed]
- 61.Paul RW, Brutico JM, Wright ML, Erickson BJ, Tjoumakaris FP, Freedman KB, et al. Strong agreement between magnetic resonance imaging and radiographs for Caton–Deschamps index in patients with patellofemoral instability. Sports Med Arthrosc Rehabil Ther Technol. 2021;3:e1621–e1628. doi: 10.1016/j.asmr.2021.07.017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Biedert RM, Albrecht S. The patellotrochlear index: a new index for assessing patellar height. Knee Surg Sports Traumatol Arthrosc. 2006;14:707–712. doi: 10.1007/s00167-005-0015-4. [DOI] [PubMed] [Google Scholar]
- 63.•.van Duijvenbode DC, van Dam MJJ, de Beer L, Stavenuiter MHJ, Hofstee DJ, van Dijke CF, et al. The reliability of the patellotrochlear index on magnetic resonance imaging for measuring patellofemoral height. Knee. 2021;32:56–63. doi: 10.1016/j.knee.2021.07.009. [DOI] [PubMed] [Google Scholar]
- 64.Barnett AJ, Prentice M, Mandalia V, Wakeley CJ, Eldridge JDJ. The patellotrochlear index: a more clinically relevant measurement of patella height? Orthopaedic Proceedings. The British Editorial Society of Bone & Joint Surgery; 2011. pp. 1–1. Available: https://online.boneandjoint.org.uk/doi/abs/10.1302/0301-620X.93BSUPP_I.0930001.
- 65.Leite CBG, Santos TP, Giglio PN, Pécora JR, Camanho GL, Gobbi RG. Tibial tubercle osteotomy with distalization is a safe and effective procedure for patients with patella alta and patellar instability. Orthop J Sports Med. 2021;9:2325967120975101. doi: 10.1177/2325967120975101. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Patel RM, Gombosh M, Polster J, Andrish J. Patellar Tendon imbrication is a safe and efficacious technique to shorten the patellar tendon in patients with patella alta. Orthop J Sports Med. 2020;8:2325967120959318. doi: 10.1177/2325967120959318. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Yalcin S, Patel RM, Andrish J, Farrow LD. Patellar tendon imbrication. Video J Sports Med. 2021;1:26350254211006699. doi: 10.1177/26350254211006699. [DOI] [Google Scholar]
- 68.Kakazu R, Luczak SB, Grimm NL, Fitzsimmons KP, Andrish JT, Farrow LD, et al. Patellar tendon imbrication for patella alta. Arthrosc Tech. 2022;11:e7–e12. doi: 10.1016/j.eats.2021.08.029. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Fabricant PD, Ladenhauf HN, Salvati EA, Green DW. Medial patellofemoral ligament (MPFL) reconstruction improves radiographic measures of patella alta in children. Knee. 2014;21:1180–1184. doi: 10.1016/j.knee.2014.07.023. [DOI] [PubMed] [Google Scholar]
- 70.Lykissas MG, Li T, Eismann EA, Parikh SN. Does medial patellofemoral ligament reconstruction decrease patellar height? A preliminary report. J Pediatr Orthop. 2014;34:78–85. doi: 10.1097/BPO.0b013e3182a12102. [DOI] [PubMed] [Google Scholar]
- 71.Elias JJ, Soehnlen NT, Guseila LM, Cosgarea AJ. Dynamic tracking influenced by anatomy in patellar instability. Knee. 2016;23:450–455. doi: 10.1016/j.knee.2016.01.021. [DOI] [PubMed] [Google Scholar]
- 72.Schoettle PB, Zanetti M, Seifert B, Pfirrmann CWA, Fucentese SF, Romero J. The tibial tuberosity-trochlear groove distance; a comparative study between CT and MRI scanning. Knee. 2006;13:26–31. doi: 10.1016/j.knee.2005.06.003. [DOI] [PubMed] [Google Scholar]
- 73.Heidenreich MJ, Sanders TL, Hevesi M, Johnson NR, Wu IT, Camp CL, et al. Individualizing the tibial tubercle to trochlear groove distance to patient specific anatomy improves sensitivity for recurrent instability. Knee Surg Sports Traumatol Arthrosc. 2018;26:2858–2864. doi: 10.1007/s00167-017-4752-y. [DOI] [PubMed] [Google Scholar]
- 74.Hevesi M, Heidenreich MJ, Camp CL, Hewett TE, Stuart MJ, Dahm DL, et al. The recurrent instability of the patella score: a statistically based model for prediction of long-term recurrence risk after first-time Dislocation. Arthroscopy. 2019;35:537–543. doi: 10.1016/j.arthro.2018.09.017. [DOI] [PubMed] [Google Scholar]
- 75.Yeoh CSN, Lam KY. Tibial tubercle to trochlear groove distance and index in children with one-time versus recurrent patellar dislocation: a magnetic resonance imaging study. J Orthop Surg. 2016;24:253–257. doi: 10.1177/1602400226. [DOI] [PubMed] [Google Scholar]
- 76.Zhang G-Y, Ding H-Y, Li E-M, Zheng L, Bai Z-W, Shi H, et al. Incidence of second-time lateral patellar dislocation is associated with anatomic factors, age and injury patterns of medial patellofemoral ligament in first-time lateral patellar dislocation: a prospective magnetic resonance imaging study with 5-year follow-up. Knee Surg Sports Traumatol Arthrosc. 2019;27:197–205. doi: 10.1007/s00167-018-5062-8. [DOI] [PubMed] [Google Scholar]
- 77.Goutallier D, Bernageau J, Lecudonnec B. The measurement of the tibial tuberosity. [Patella groove distanced technique and results (author’s transl)]. Rev Chir Orthop Reparatrice Appar Mot. 1978;64:423–8 Available: https://www.ncbi.nlm.nih.gov/pubmed/152950. [PubMed]
- 78.Balcarek P, Jung K, Frosch K-H, Stürmer KM. Value of the tibial tuberosity-trochlear groove distance in patellar instability in the young athlete. Am J Sports Med. 2011;39:1756–1761. doi: 10.1177/0363546511404883. [DOI] [PubMed] [Google Scholar]
- 79.Dickens AJ, Morrell NT, Doering A, Tandberg D, Treme G. Tibial tubercle-trochlear groove distance: defining normal in a pediatric population. J Bone Joint Surg Am. 2014;96:318–324. doi: 10.2106/JBJS.M.00688. [DOI] [PubMed] [Google Scholar]
- 80.Dai Z-Z, Sha L, Zhang Z-M, Liang Z-P, Li H, Li H. Comparing the tibial tuberosity–trochlear groove distance between ct and mri in skeletally immature patients with and without patellar instability. Orthop J Sports Med. 2021;9:2325967120973665. doi: 10.1177/2325967120973665. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.•.Mistovich RJ, Urwin JW, Fabricant PD, Lawrence JTR. Patellar tendon-lateral trochlear ridge distance: a novel measurement of patellofemoral instability. Am J Sports Med. 2018;46:3400–3406. doi: 10.1177/0363546518809982. [DOI] [PubMed] [Google Scholar]
- 82.••.Weltsch D, Chan CT, Mistovich RJ, Urwin JW, Gajewski CR, Fabricant PD, et al. Predicting risk of recurrent patellofemoral instability with measurements of extensor mechanism containment. Am J Sports Med. 2021;49:706–712. doi: 10.1177/0363546520987007. [DOI] [PubMed] [Google Scholar]
- 83.Kita K, Tanaka Y, Toritsuka Y, Amano H, Uchida R, Takao R, et al. Factors affecting the outcomes of double-bundle medial patellofemoral ligament reconstruction for recurrent patellar dislocations evaluated by multivariate analysis. Am J Sports Med. 2015;43:2988–2996. doi: 10.1177/0363546515606102. [DOI] [PubMed] [Google Scholar]
- 84.Fulkerson JP. Anteromedialization of the tibial tuberosity for patellofemoral malalignment. Clin Orthop Relat Res 1983; 176–181. Available: https://www.ncbi.nlm.nih.gov/pubmed/6861394. [PubMed]
- 85.Ferrari MB, Sanchez G, Kennedy NI, Sanchez A, Schantz K, Provencher MT. Osteotomy of the tibial tubercle for anteromedialization. Arthrosc Tech. 2017;6:e1341–e1346. doi: 10.1016/j.eats.2017.05.012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 86.Trivellas M, Arshi A, Beck JJ. Roux-Goldthwait and medial patellofemoral ligament reconstruction for patella realignment in the skeletally immature patient. Arthrosc Tech. 2019;8:e1479–e1483. doi: 10.1016/j.eats.2019.07.027. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87.Felli L, Capello AG, Lovisolo S, Chiarlone F, Alessio-Mazzola M. Goldthwait technique for patellar instability: surgery of the past or here to stay procedure? A systematic review of the literature. Musculoskelet Surg. 2019;103:107–113. doi: 10.1007/s12306-018-0566-4. [DOI] [PubMed] [Google Scholar]
- 88.Longo UG, Rizzello G, Ciuffreda M, Loppini M, Baldari A, Maffulli N, et al. Elmslie-Trillat, Maquet, Fulkerson, Roux Goldthwait, and other distal realignment procedures for the management of patellar dislocation: systematic review and quantitative synthesis of the literature. Arthroscopy. 2016;32:929–943. doi: 10.1016/j.arthro.2015.10.019. [DOI] [PubMed] [Google Scholar]
- 89.Kazley JM, Banerjee S. Classifications in Brief: The Dejour classification of trochlear dysplasia. Clin Orthop Relat Res. 2019;477:2380–2386. doi: 10.1097/CORR.0000000000000886. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Askenberger M, Janarv P-M, Finnbogason T, Arendt EA. Morphology and anatomic patellar instability risk factors in first-time traumatic lateral patellar dislocations: a prospective magnetic resonance imaging study in skeletally immature children. Am J Sports Med. 2017;45:50–58. doi: 10.1177/0363546516663498. [DOI] [PubMed] [Google Scholar]
- 91.Steensen RN, Bentley JC, Trinh TQ, Backes JR, Wiltfong RE. The prevalence and combined prevalences of anatomic factors associated with recurrent patellar dislocation: a magnetic resonance imaging study. Am J Sports Med. 2015;43:921–927. doi: 10.1177/0363546514563904. [DOI] [PubMed] [Google Scholar]
- 92.Glard Y, Jouve J-L, Garron E, Adalian P, Tardieu C, Bollini G. Anatomic study of femoral patellar groove in fetus. J Pediatr Orthop. 2005;25:305–308. doi: 10.1097/01.bpo.0000161099.46339.eb. [DOI] [PubMed] [Google Scholar]
- 93.Bollier M, Fulkerson JP. The role of trochlear dysplasia in patellofemoral instability. J Am Acad Orthop Surg. 2011;19:8–16. doi: 10.5435/00124635-201101000-00002. [DOI] [PubMed] [Google Scholar]
- 94.••.Stepanovich M, Bomar JD, Pennock AT. Are the current classifications and radiographic measurements for trochlear dysplasia appropriate in the skeletally immature patient? Orthop J Sports Med. 2016;4:2325967116669490. doi: 10.1177/2325967116669490. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 95.Koëter S, Bongers EMHF, de Rooij J, van Kampen A. Minimal rotation aberrations cause radiographic misdiagnosis of trochlear dysplasia. Knee Surg Sports Traumatol Arthrosc. 2006;14:713–717. doi: 10.1007/s00167-005-0031-4. [DOI] [PubMed] [Google Scholar]
- 96.•.Sharma N, Brown A, Bouras T, Kuiper JH, Eldridge J, Barnett A. The Oswestry-Bristol classification. Bone Joint J. 2020;102-B:102–107. doi: 10.1302/0301-620X.102B1.BJJ-2019-0366.R3. [DOI] [PubMed] [Google Scholar]
- 97.Sharma N, Rehmatullah N, Kuiper JH, Gallacher P, Barnett AJ. Clinical validation of the Oswestry-Bristol classification as part of a decision algorithm for trochlear dysplasia surgery. Bone Joint J. 2021;103-B:1586–1594. doi: 10.1302/0301-620X.103B10.BJJ-2020-1984.R1. [DOI] [PubMed] [Google Scholar]
- 98.Konrads C, Gonser C, Ahmad SS. Reliability of the Oswestry-Bristol classification for trochlear dysplasia: expanded characteristics. Bone Jt Open. 2020;1:355–358. doi: 10.1302/2633-1462.17.BJO-2020-0048.R1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 99.Carrillon Y, Abidi H, Dejour D, Fantino O, Moyen B, Tran-Minh VA. Patellar instability: assessment on MR images by measuring the lateral trochlear inclination-initial experience. Radiology. 2000;216:582–585. doi: 10.1148/radiology.216.2.r00au07582. [DOI] [PubMed] [Google Scholar]
- 100.Joseph SM, Cheng C, Solomito MJ, Pace JL. Lateral trochlear inclination angle: measurement via a 2-image technique to reliably characterize and quantify trochlear dysplasia. Orthop J Sports Med. 2020;8:2325967120958415. doi: 10.1177/2325967120958415. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 101.Pfirrmann CW, Zanetti M, Romero J, Hodler J. Femoral trochlear dysplasia: MR findings. Radiology. 2000;216:858–864. doi: 10.1148/radiology.216.3.r00se38858. [DOI] [PubMed] [Google Scholar]
- 102.Nietosvaara Y, Aalto K. The cartilaginous femoral sulcus in children with patellar dislocation: an ultrasonographic study. J Pediatr Orthop. 1997;17:50–53. doi: 10.1097/00004694-199701000-00012. [DOI] [PubMed] [Google Scholar]
- 103.Düppe K, Gustavsson N, Edmonds EW. Developmental morphology in childhood patellar instability: age-dependent differences on magnetic resonance imaging. J Pediatr Orthop. 2016;36:870–876. doi: 10.1097/BPO.0000000000000556. [DOI] [PubMed] [Google Scholar]
- 104.Trivellas M, Kelley B, West N, Jackson NJ, Beck JJ. Trochlear morphology development: study of normal pediatric knee MRIs. J Pediatr Orthop. 2021;41:77–82. doi: 10.1097/BPO.0000000000001697. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 105.Arendt EA, England K, Agel J, Tompkins MA. An analysis of knee anatomic imaging factors associated with primary lateral patellar dislocations. Knee Surg Sports Traumatol Arthrosc. 2017;25:3099–3107. doi: 10.1007/s00167-016-4117-y. [DOI] [PubMed] [Google Scholar]
- 106.Pagliazzi G, Ellermann JM, Carlson CS, Shea KG, Arendt EA. Trochlear development in children from 1 month to 10 years of age: a descriptive study utilizing analysis by magnetic resonance imaging. Orthop J Sports Med. 2021;9:23259671211028269. doi: 10.1177/23259671211028269. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 107.van Huyssteen AL, Hendrix MRG, Barnett AJ, Wakeley CJ, Eldridge JDJ. Cartilage-bone mismatch in the dysplastic trochlea. An MRI study. J Bone Joint Surg Br. 2006;88:688–691. doi: 10.1302/0301-620X.88B5.16866. [DOI] [PubMed] [Google Scholar]
- 108.Camathias C, Speth BM, Rutz E, Schlemmer T, Papp K, Vavken P, et al. Solitary trochleoplasty for treatment of recurrent patellar dislocation. JBJS Essent Surg Tech. 2018;8:e11. doi: 10.2106/JBJS.ST.17.00039. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 109.Dejour D, Saggin P. The sulcus deepening trochleoplasty-the Lyon’s procedure. Int Orthop. 2010;34:311–316. doi: 10.1007/s00264-009-0933-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 110.Vogel LA, Pace JL. Trochleoplasty, medial patellofemoral ligament reconstruction, and open lateral lengthening for patellar instability in the setting of high-grade trochlear dysplasia. Arthrosc Tech. 2019;8:e961–e967. doi: 10.1016/j.eats.2019.05.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 111.Fulkerson JP. Trochleoplasty has its place for select patients with complex patella instability. [cited 27 Feb 2021]. Available: https://www.healio.com/news/orthopedics/20190412/trochleoplasty-has-its-place-for-select-patients-with-complex-patella-instability.
- 112.Rush J, Diduch D. When is trochleoplasty a rational addition? Sports Med Arthrosc. 2019;27:161–168. doi: 10.1097/JSA.0000000000000254. [DOI] [PubMed] [Google Scholar]
- 113.Smith JM, Rush JK, Carstensen SE, Diduch DR. Trochleoplasty: indications and results. In: Dejour D, Zaffagnini S, Arendt EA, Sillanpää P, Dirisamer F, editors. Patellofemoral pain, instability, and arthritis: clinical presentation, imaging, and treatment. Berlin: Springer Berlin Heidelberg; 2020. pp. 303–312. [Google Scholar]
- 114.Blond L. Is there any indication for trochleoplasty? In: OrthopedicsToday [Internet]. [cited 27 Feb 2021]. Available: https://www.healio.com/news/orthopedics/20200408/is-there-any-indication-for-trochleoplasty.
- 115.Nolan JE 3rd, Schottel PC, Endres NK. Trochleoplasty: indications and technique. Curr Rev Musculoskelet Med. 2018. 10.1007/s12178-018-9478-z. [DOI] [PMC free article] [PubMed]
- 116.Levy BJ, Tanaka MJ, Fulkerson JP. Current concepts regarding patellofemoral trochlear dysplasia. Am J Sports Med. 2021;49:1642–1650. doi: 10.1177/0363546520958423. [DOI] [PubMed] [Google Scholar]
- 117.Camathias C, Studer K, Kiapour A, Rutz E, Vavken P. Trochleoplasty as a solitary treatment for recurrent patellar dislocation results in good clinical outcome in adolescents. Am J Sports Med. 2016;44:2855–2863. doi: 10.1177/0363546516652894. [DOI] [PubMed] [Google Scholar]
- 118.Nelitz M, Dreyhaupt J, Williams SRM. No growth disturbance after trochleoplasty for recurrent patellar dislocation in adolescents with open growth plates. Am J Sports Med. 2018;46:3209–3216. doi: 10.1177/0363546518794671. [DOI] [PubMed] [Google Scholar]
- 119.Pesenti S, Blondel B, Armaganian G, Parratte S, Bollini G, Launay F, et al. The lateral wedge augmentation trochleoplasty in a pediatric population: a 5-year follow-up study. J Pediatr Orthop B. 2017;26:458–464. doi: 10.1097/BPB.0000000000000395. [DOI] [PubMed] [Google Scholar]
- 120.Metcalfe AJ, Clark DA, Kemp MA, Eldridge JD. Trochleoplasty with a flexible osteochondral flap: results from an 11-year series of 214 cases. Bone Joint J. 2017;99-B:344–350. doi: 10.1302/0301-620X.99B3.37884. [DOI] [PubMed] [Google Scholar]
- 121.Rouanet T, Gougeon F, Fayard JM, Rémy F, Migaud H, Pasquier G. Sulcus deepening trochleoplasty for patellofemoral instability: a series of 34 cases after 15 years postoperative follow-up. Orthop Traumatol Surg Res. 2015;101:443–447. doi: 10.1016/j.otsr.2015.01.017. [DOI] [PubMed] [Google Scholar]
- 122.van Sambeeck JDP, van de Groes SAW, Verdonschot N, Hannink G. Trochleoplasty procedures show complication rates similar to other patellar-stabilizing procedures. Knee Surg Sports Traumatol Arthrosc. 2018;26:2841–2857. doi: 10.1007/s00167-017-4766-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 123.Leclerc J-T, Dartus J, Labreuche J, Martinot P, Galmiche R, Migaud H, et al. Complications and outcomes of trochleoplasty for patellofemoral instability: a systematic review and meta-analysis of 1000 trochleoplasties. Orthop Traumatol Surg Res. 2021;107:103035. doi: 10.1016/j.otsr.2021.103035. [DOI] [PubMed] [Google Scholar]