Abstract
Objective
To examine the literature to understand the extent that music-associated head banging (MAHB), a common form of self-expression that involves rhythmically swinging one's head to music, is a risk factor for traumatic brain injury (TBI), to identify areas for further research, and to inform primary prevention strategies.
Data Sources
A comprehensive search of several databases from database inception to June 30, 2021, was designed and conducted by an experienced librarian with input from study investigators.
Study Selection
Study inclusion criteria encompassed all study designs evaluating TBI associated with MAHB. Two independent reviewers reviewed all titles, abstracts, and full texts.
Data Extraction
Data were extracted by 2 independent reviewers, and results were summarized descriptively.
Data Synthesis
Of 407 eligible studies, 13 met inclusion criteria. All included studies were case reports from multiple countries describing a case of moderate-severe TBI occurring as a direct consequence of MAHB. Of the individuals reported (n=13), they had 1 or more of the following: traumatic subdural hematoma (n=8), internal carotid artery dissection (n=2), basilar artery thrombosis (n=2), traumatic vertebral artery aneurism (n=1), or intracerebral hemorrhage (n=1). No studies were found involving mild TBI after MAHB.
Conclusions
This scoping review suggests that MAHB is a risk factor for moderate-severe TBI, although the incidence of mild TBI after MAHB remains unknown. Additional research is needed to understand the association of TBI after MAHB through the spectrum of injury severity, including the potential sequelae of multiple subconcussive injuries.
KEYWORDS: Brain injuries, traumatic; Music; Rehabilitation; Review
List of abbreviations: CT, computed tomography; MAHB, music-associated head banging; mTBI, mild traumatic brain injury; PRISMA, Preferred Reporting Items for Systematic Reviews and Meta-Analysis; TBI, traumatic brain injury
Up to 69 million individuals worldwide sustain a traumatic brain injury (TBI) every year, making TBI a leading cause of global morbidity and mortality.1,2 The leading causes of TBI worldwide are falls, motor vehicle collisions, and sports-related injuries.1,3
Regardless of etiology or injury severity, TBI can result in chronic neurobehavioral symptoms along with physical and cognitive impairment that can persist years after injury.1,3, 4, 5, 6 These impairments can lead to restricted societal participation, decreased driving, and lower levels of employment, all of which account for a high prevalence of disability after TBI.7, 8, 9, 10
TBI is defined as a disruption in the normal function of the brain due to a blunt or penetrating force, a nonimpact blast, or an inertial load.11,12 A common mechanism of TBI is a whiplash injury, which is characterized by acceleration and deceleration forces to the head and neck from either direct or indirect contact, with a motion related inertial load that can result in diffuse brain injury.13, 14, 15 There is evidence of blood flow changes and decreased gray matter density associated with whiplash injury,14,16 suggesting traumatic axonal injury in the setting of an inertial loading of vulnerable axons.13,14,17 Individuals who sustain a TBI associated with a whiplash injury can present with symptoms that include headache, neck pain, dizziness, and increased cognitive difficulties. Whiplash-associated TBI can also result in increased prevalence of disability; thus, preventing TBI associated with whiplash injury remains an important public health priority.18
While whiplash-associated TBI is most commonly associated with motor vehicle collisions and sports-related concussions,19 a potentially unrecognized risk factor for TBI may be in the sphere of nonoccupational high-intensity music, including concerts, discotheques (clubs), and personal music players.20 A common form of self-expression activity done throughout the world by both musicians and music listeners in these settings is referred to as music-associated head banging (MAHB), in which the listener swings ones head in a rhythmic—and often high-velocity fashion—as directed by the beat of the song, particularly to rock, punk, or heavy metal music. MAHB overall involves extremes in flexion and extension of the cervical spine and when combined with acceleration/deceleration motions, it has been reported to have a mechanism of injury similar to known whiplash-associated TBI associated most commonly with motor vehicle collisions or sports-related concussion.21 The authors found several case reports of MAHB leading to severe TBI with resulting severe morbidity, although there have been no systematic reports of the scope of MAHB as a potential risk factor for TBI.
The primary objective of this scoping review is to understand whether MAHB is a risk factor for TBI of any severity, as well as to understand the extent of this risk. Considering the popularity of concerts throughout the world and MAHB in general, identifying the extent that MAHB is a risk factor for TBI could serve to identify public health needs in this area and ultimately decrease the incidence and resulting morbidity of TBI.
Methods
To comprehensively search the literature and synthesize the evidence on this topic, a scoping review was conducted according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses for Scoping Reviews Statement.22 The protocol for this scoping review has not been published.
Data sources and search strategy
A search of several literature databases from database inception to June 30, 2021, limited to English language and excluding animal studies, was designed and conducted by an experienced librarian with input from study investigators. The same strategy was rerun from database inception to September 2, 2021, to include non-English language articles. The databases included Ovid MEDLINE (1946+) and Epub Ahead of Print, In-Process & Other Non-Indexed Citations and Daily, Ovid Embase (1974+), Ovid Cochrane Central Register of Controlled Trials (1991+), Ovid Cochrane Database of Systematic Reviews (2005+), Ovid APA PsycInfo (1967+), and Web of Science, and Scopus (1788+). Because we found no synonyms for head banging and adding terms that might indicate music such as rock, metal, or band would only restrict the search and potentially miss articles, we performed the most comprehensive search by using only variations of the term head banging. We reviewed all retrieved articles and then screened for those related to MAHB. The complete search strategy showing all search terms, date ranges, and limits for each database is available in online supplemental appendix S1.
Study selection
Study inclusion criteria included all age groups and encompassed the following study designs: (1) randomized trials, (2) observational studies, (3) case series, (4) case studies, and/or (5) conference abstracts studying TBI associated with MAHB. Published studies examining all severity of TBI resulting from MAHB were included. We included studies resulting from any traumatic cervical related sequelae such as cerebral artery dissection as well in our search, given the same mechanism of injury. Exclusion criteria included (1) TBI due to other etiology, (2) head banging in contexts other than along to music, (3) other non-TBI due to MAHB, and (4) MAHB not reporting TBI as a sequela. We included all languages in our search and excluded animal studies.
Two independent reviewers screened each title and abstract identified by the search strategy. Any disagreements between authors resulted in inclusion for full-text review. Two independent reviewers subsequently screened each full text of all studies included after title and abstract review. If inclusion criteria were not clear from screening of abstract and titles, the article was included for full-text review. Interrater reliability of full-text review for final inclusion for data extraction was assessed. Interrater agreement between 2 independent reviewers was 90.5% (κ=80.0%; 95% CI, 54.2%-100%), indicating substantial agreement. Disagreements were resolved by mutual consensus between 4 coauthors. The references of the included articles were also used to screen for other potentially relevant articles.
Data extraction
Data were extracted by 2 independent reviewers separately, with discrepancies in data extraction resolved by mutual consensus. Abstracted data included authorship, publication year, study design, sample size, patient demographics, mechanism of injury, severity of injury, time between injury and symptom onset, time between injury and presentation to physician, treatment plan, surgical intervention if applicable, and details regarding outcome.
Because of the heterogeneity in studies defining TBI severity, the authors used the Mayo classification system to uniformly classify TBI severity (supplemental appendix S2).23 This classification system uses all positive evidence in study details to diagnose TBI events more accurately than single indicator systems (eg, length of posttraumatic amnesia, initial Glasgow Coma Score, length of loss of consciousness).24
Results
Study selection and characteristics
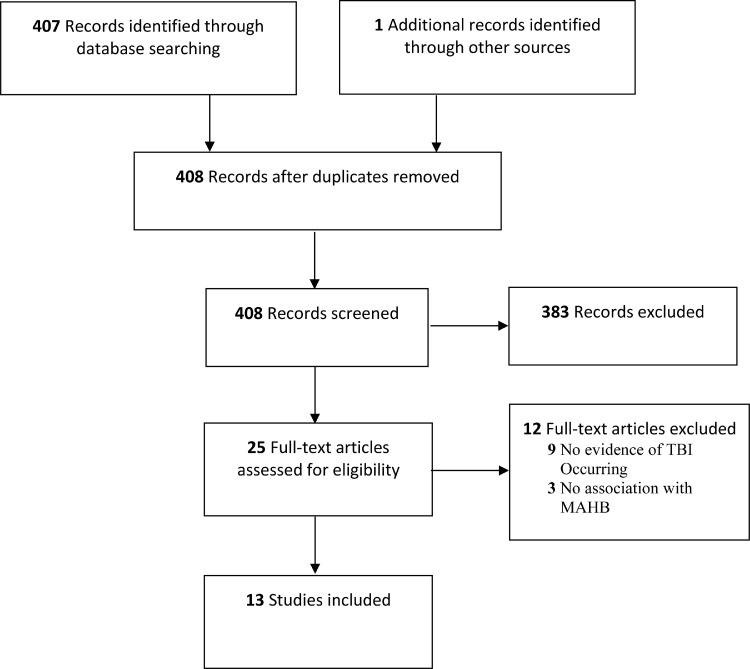
Of the 408 abstracts identified, 25 were selected for full-text review, and of those, 13 met inclusion criteria as noted in fig 1. There were no epidemiologic or population-based studies found. All 13 studies were case studies (table 1).25, 26, 27, 28, 29, 30, 31, 32, 33, 34, 35, 36, 37 The mean ± SD age was 22.8±10.5 years, with a range of 11-50 years. Sex distribution leaned heavily male (77%). The most common place of occurrence was at rock concerts (54%). These 13 cases were reported in England (3),30,31,37 Germany (2),34,36 India (2),32,35 Canada (1),25 Belgium (1),26 Sweden (1),27 Italy (1),29 Japan (1),33 and the United States (1).28 The time interval from MAHB to presentation was variable, including within 24 hours (5),28, 29, 30, 31,35 a few days (4),32,33,36,37 a few weeks (2),27,34 and up to 3 months (1).26 One case did not report a time interval.25
Fig 1.
Preferred reporting items for systematic review and meta-analyses flow chart for the study selection process.
Table 1.
Study characteristics
| Study | Study Design | N | Age | Sex | Diagnosis | Severity of TBI* | Time Between Injury and 1. Symptom Onset and 2. Presentation to Physician | Treatment Course | Outcome |
|---|---|---|---|---|---|---|---|---|---|
| De Carvalho et al25 | CS | 1 | 22 | Female | Subdural hematoma | Definite | 1. Not reported; 2. Not reported | 2-burr-hole craniotomy | Survived |
| De Cauwer et al26 | CS | 1 | 15 | Male | Subdural hematoma | Definite | 1. Within 24 h; 2. 3 mo | Surgical drainage; reintervention 40 d later because of rebleed | Uneventful recovery |
| Edvardsson et al27 | CS | 1 | 20 | Male | Basilar artery thrombosis | NA | 1. Not reported; 3 wk | Intra-arterial fibrinolytic agent administration | Locked-in state |
| Egnor et al28 | CS | 1 | 15 | Male | Traumatic true aneurysm of vertebral artery leading to a hemorrhagic infarction | Definite | 1. Immediately; 2. 2 h, 4 wk, 6 wk | Excision of aneurysm | Full recovery after 1 y |
| Gilberti et al29 | CS | 1 | 16 | Male | Subdural hematoma, internal carotid artery dissection leading to a cerebral ischemic infarction | Definite | 1. Within 24 h; 2. Within 24 h | Conservative nonsurgical treatment | Full recovery after 90 d |
| Jackson et al30 | CS | 1 | 15 | Male | Internal carotid artery dissection leading to both cerebral ischemic and hemorrhagic infarctions | Definite | 1. Within 24 h; 2. 14 h | Dexamethasone and mannitol | Died |
| Mackenzie et al31 | CS | 1 | 20 | Male | Subdural hematoma | Definite | 1. Within 24 h; 2. Within 24 h | Died before treatment | Died |
| Neyaz et al32 | CS | 1 | 29 | Male | Subdural hematoma | Definite | 1. Immediately; 2. 3 d | Conservative nonsurgical treatment | Full recovery after 1 wk |
| Nitta et al33 | CS | 1 | 24 | Female | Subdural hematoma | Definite | 1. Not reported; 2. 3 d | Conservative nonsurgical treatment | Full recovery after 8 mo |
| Pirayesh Islamian et al34 | CS | 1 | 50 | Male | Subdural hematoma | Definite | 1. 2 wk; 2. 4 wk | Burr hole evacuation; subdural drainage for 6 d post operation | Full recovery after 2 mo |
| Rajasekharan et al35 | CS | 1 | 35 | Female | Basilar artery thrombosis leading to a brainstem ischemic infarction | NA | 1. Within 24 hours; 2. Within 24 hours | Anticerebral edema measures; antiplatelet agents | Locked-in state |
| Scheel et al36 | CS | 1 | 24 | Male | Subdural hematoma | Definite | 1. Not reported; 2. 2 d | Surgical evacuation | Survived |
| Torrey et al37 | CS | 1 | 11 | Male | Colloid cyst rupture leading to an intracerebral hematoma | Definite | 1. Immediately; 2. 4 d, 17 d, and 18 d | General practitioner prescribed aspirin for headache; general practitioner prescribed ampicillin for sinus; mother gave aspirin for headache | Died |
| Abbreviation: CS, case study; NA, not applicable. | |||||||||
TBI was classified by the Mayo classification system (insert reference).
Results by type of injury
All TBIs of case studies were defined as definite TBI. Of these, the most common mechanism was subdural hematoma. Other mechanisms included internal carotid artery dissection, basilar artery thrombosis, traumatic true aneurysm, and intracerebral hematoma.
TBI from subdural hematoma
Eight case studies involving TBI after MAHB were caused from subdural hematomas, the most prevalent etiology in the current literature.25,26,29,31, 32, 33, 34,36 Gilberti et al29 presented a 16-year-old boy with sudden-onset global diffuse headache from an internal carotid artery dissection with subsequent temporal and parietal lobe infarctions and a subdural hematoma from a presumed definite TBI after head banging at a rock concert the night prior. The patient had a full recovery after 90 days. Nitta et al33 presented a 24-year-old woman with partial seizures affecting the right upper and lower limbs from a left-sided subdural hematoma 3 days after head banging at a punk rock concert. She previously had an acute left-sided subdural hematoma as a newborn after an accidental fall from a baby buggy. The patient had a full recovery after 8 months. Mackenzie et al31 presented a 20-year-old man with severe occipital headache and seizures after head banging to rock music the night prior. An extensive subdural hematoma was found, with midline shift and cerebellar tonsillar herniation leading to the death of the patient. Neyaz et al32 presented a 29-year-old male radiology resident with symptoms of headaches and uneasiness that developed while head banging at a rock show 3 days previously, without any drug or alcohol consumption, leading to the discovery of a small left-sided subdural hematoma. The patient fully recovered after 1 week. De Cauwer et al26 presented a 15-year-old boy with a 3-month history of chronic headaches and new sudden-onset severe frontal headache with associated photophobia after head banging to music at a party. A head computed tomography (CT) revealed a chronic right-sided frontoparietal subdural hematoma with a resultant midline shift to the left. The patient had an uneventful recovery. Scheel et al36 presented a 24-year-old “hard rock enthusiast” with severe left-sided headaches 2 days after intense head banging at a rock concert. A head CT showed a left-sided subdural hemorrhage and a left temporal pole arachnoid cyst. The patient was discharged from an acute care hospital. Pirayesh Islamian et al34 presented a 50-year-old man with a 2-week constant worsening global headache, starting after head banging at a Motörhead concert almost a month previously. He denied substance abuse. A head CT revealed a right-sided chronic subdural hematoma with midline shift. The patient had a full recovery after 2 months. De Carvalho et al25 presented a 22-year-old woman with persistent severe headaches with an associated increase of “head whipping” maneuvers within the last 4 years because of changes in the style of a popular dance performed on her university dance team. She did not consume alcohol or smoke. A head CT showed a right-sided chronic subdural hematoma in the frontal lobe, and she subsequently underwent evacuation. The patient was discharged from an acute care hospital.
TBI from internal carotid artery dissection
Two case studies involving TBI after MAHB were caused from internal carotid artery dissections.29,30 Jackson et al30 presented a 15-year-old boy with right hemiparesis, facial weakness, and either right homonymous hemianopia or right-sided inattention deficit after head banging at a rock concert the previous evening. He consumed 3 pints of beer during the rock concert. The postmortem autopsy showed evidence of a dissecting aneurysm of the left internal carotid artery, presumably caused by the extreme flexion-extension motions of head banging. The dissection occurred at the bony prominences of the C1 and C2 vertebral levels, where the shearing stresses caused a tear of the internal carotid artery. He had a definite TBI from a left internal carotid artery dissection, which led to large cerebral ischemic infarctions, an occipital hemorrhagic infarction, cerebral edema, and uncal herniation. He subsequently died 1 week after admission to an acute care hospital. In the case study by Gilberti et al29 with the subdural hematoma, the sudden-onset global diffuse headache was caused from an internal carotid artery dissection with subsequent subdural hematoma. One-month follow-up imaging also revealed right-sided temporal and parietal lobe infarctions.
TBI from basilar artery thrombosis
Two case studies involving TBI after MAHB were caused from basilar artery thrombosis.27,35 Edvardsson et al27 presented a 20-year-old professional musician who self-proclaimed participation in “intensive head banging,” who subsequently presented with a 3-week duration of neck pain, headache, and vertigo. The patient denied substance abuse. After an episode of intermittent loss of consciousness and several equivocal tests, cerebral digital subtraction angiography showed basilar artery thrombosis without evident dissection. Rajasekharan et al35 presented a 35-year-old woman with vomiting, urinary incontinence, altered sensorium, and tetraplegia, beginning the day after participating in a religious ritual dance known as devi thullal. This traditional dance involved fierce head banging for consecutive hours. A brain magnetic resonance imaging revealed an acute infarction of the ventral pons, with a subsequent brain magnetic resonance angiogram exposing basilar artery thrombosis. Both patients survived but remained in locked-in states.27,35
TBI from traumatic true aneurysm of the vertebral artery
One case study involving TBI after MAHB was caused from a traumatic true aneurysm of the cervical vertebral artery.28 Egnor et al28 presented a 15-year-old male drummer with new-onset vertigo, nausea, vomiting, difficulty with left arm and leg coordination, and slowed speech after fiercely banging his head and neck while performing in a neighborhood rock band. He had a definite TBI with a cerebellar hemorrhagic infarction with subsequent discovery of a traumatic true aneurysm of the cervical vertebral artery, which was found and treated with emergent neurosurgical excision of the aneurysm. The patient had a full recovery after 1 year.
TBI from intracerebral hematoma
One case study involving TBI after MAHB was caused from intracerebral hematoma.37 Torrey et al37 presented an 11-year-old boy with a severe headache, nausea, and persistent vomiting, who had participated in head banging to heavy metal music at a disco party. The patient died after 18 days of failed treatments for sinus headache before arriving at the hospital. On postmortem autopsy, it was revealed that a colloid cyst ruptured while head banging, leading to an intracerebral hematoma, a definite TBI.
Discussion
Each of these 13 case studies presented a patient who experienced a definite TBI (consistent with moderate-severe TBI) while head banging to music.25, 26, 27, 28, 29, 30, 31, 32, 33, 34, 35, 36, 37 Although no direct trauma at the time of the event was reported in any of these cases, a traumatic force as a direct result of extremes in motion was attributed to the concurrent pathophysiological changes and clinical findings. Hypothesized pathophysiology of these injuries included dramatic motion leading to sheer forces, further resulting in possible thrombus formation, which subsequently caused ischemia or infarction in some cases.27,28,35 The most common clinical presentation observed was a subdural hematoma. Subdural hematomas are typically caused by a tearing of the bridging veins resulting in rupture and bleeding into the subdural space.38 In each of the 8 cases studies, MAHB was thought to cause severe strain on the bridging veins leading to tears and subsequent hemorrhage.31
In this scoping review, no studies were found reporting MAHB causing mild TBI (mTBI). Patton et al21 performed an observational study to identify the most popular head banging technique and the predicted risk of mTBI from head banging. After observing that the up-down style of head banging was the most popular among musicians, they began a biomechanical analysis under the assumption that angular displacement of the head on the C7-T1 axis of rotation followed a sinusoidal motion pattern in a sagittal plane. Using this assumption, they constructed head injury criterion and neck injury criterion levels. They then asked a focus group of 10 musicians to tap the tempo of 11 popular heavy metal songs to calculate the perceived average tempo of each song. Applying the head injury criterion and neck injury criterion, cervical range of motion >45°, when related to the rising tempo, was found to increase the risk of sustaining an mTBI. When that 146-beats/min tempo was combined with a neck range of motion >75°, the individual was predicted to sustain an mTBI.
Overall, the evidence was very limited, with only 13 individual case studies reporting TBI after MAHB. When considering the popularity of hard rock and heavy metal music around the world, it is unclear whether MAHB is more common than reflected in our scoping review because of milder symptoms or spontaneously resolving concussive symptoms that are unreported.31 These injuries may simply go unreported by rock music enthusiasts; mTBI makes up the majority of TBI cases.24 A single occurrence of these mild, self-resolving mTBI may be self-limiting, but compounded by numerous occurrences, these injuries could do further damage than is currently reported. In addition, there is increasing evidence of a cumulative effect associated with repeated brain injuries, including repetitive subconcussive TBI, which can result in an increased risk of long-term sequelae.39,40 Given the repetitive nature of MAHB, it is possible that MAHB may be associated with a similar risk.21 Further research is needed to understand this risk.
In addition to TBI, traumatic cervical injuries were also noted in the literature. While outside the scope of this review, it is important to consider cervical spinal cord injury as another possible risk factor after MAHB.41
Future directions
Future studies are necessary to further stratify TBI symptom severity, incidence of symptoms, and possible long-term sequelae of MAHB and to understand whether multiple subconcussive events associated with MAHB affects patient morbidity. Future retrospective cohort studies could also address the incidence of other non-TBI MAHB injuries, such as cervical injuries including whiplash, radiculopathy, vertebral fracture, and spinal cord injury. There is a scant amount of current research on this topic. While it is plausible that the incidence of TBI, and mTBI in particular, is higher than reported in the literature after MAHB, further research is needed to understand the public health implications. Potential considerations for future research include qualitative studies and survey methodology of concert goers to assess whether individuals describe symptoms of mild or moderate-severe TBI, observe others with these symptoms, and understand the relative frequency of co-occurring behaviors such as substance abuse or moshing.
Study limitations
This scoping review has its limitations. Our overall summary of the public health implications of MAHB was limited by very few case reports in the literature with an overall very small sample size (N=13). Our search included only studies where the mechanism of injury for TBI was MAHB, and mixed-etiology studies (such as general epidemiologic studies evaluating multiple etiology of TBI) were excluded, making it possible for occurrences of TBI by MAHB within such studies to be missed. For most public health problems, there is clear exposure data. While concerts and associated MAHB are generally a common phenomenon around the world, there is no objective data on the prevalence of concerts or the prevalence of engaging in dangerous behaviors, such as MAHB, at concerts, which makes it challenging to assess the incidence of MAHB. The “dose response” was unattainable from the case reports in that neither intensity of head banging nor duration of MAHB was described in any case reports, and this requires further research to understand. Additionally, a majority of the authors26,28,29,31,33,35, 36, 37 did not report concurrent risky behavior, such as drug or alcohol consumption, as potential confounding factors. Although we cannot be fully certain that MAHB was the cause, each case was described by medical professionals in a hospital setting who ultimately felt that the primary etiology of the injury was MAHB. Lastly, information regarding potential comorbidities that could predispose to injury was missing in all but 1 study.30
Conclusions
Despite how common MAHB is in popular culture, there are only a few isolated case reports of moderate-severe TBI reported in the literature. The discussed self-inflicted TBI are thought to be caused by the harsh repetitive rhythmic motions; however, there are still many unknowns when it comes to this cause of TBI. Additional research is needed to understand whether MAHB is associated with mTBI to guide clinical and preventative strategies further.
Footnotes
Presented as a poster to the International Society of Physical and Rehabilitation Medicine World Congress and Association of Academic Physiatrists, March, 3, 2020, Orlando, FL.
Disclosures: none
Supplementary material associated with this article can be found, in the online version, at doi:10.1016/j.arrct.2022.100192.
Appendix. Supplementary materials
References
- 1.Centers for Disease Control and Prevention. Surveillance report of traumatic brain injury-related emergency department visits, hospitalizations, and deaths—United States. Available at: https://www.cdc.gov/traumaticbraininjury/pdf/TBI-Surveillance-Report-FINAL_508.pdf. Accessed August 20, 2021.
- 2.Dewan MC, Rattani A, Gupta S, et al. Estimating the global incidence of traumatic brain injury. J Neurosurg. 2018 Apr 1 doi: 10.3171/2017.10.JNS17352. [Epub ahead of print] [DOI] [PubMed] [Google Scholar]
- 3.Centers for Disease Control and Prevention. Report to Congress on traumatic brain injury in the United States: epidemiology and rehabilitation. Available at: https://www.cdc.gov/traumaticbraininjury/pubs/congress_epi_rehab.html. Accessed August 20, 2021. [DOI] [PubMed]
- 4.Corrigan JD, Hammond FM. Traumatic brain injury as a chronic health condition. Arch Phys Med Rehabil. 2013;94:1199–1201. doi: 10.1016/j.apmr.2013.01.023. [DOI] [PubMed] [Google Scholar]
- 5.Hiploylee C, Dufort PA, Davis HS, et al. Longitudinal study of postconcussion syndrome: not everyone recovers. J Neurotrauma. 2017;34:1511–1523. doi: 10.1089/neu.2016.4677. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Wilson L, Stewart W, Dams-O'Connor K, et al. The chronic and evolving neurological consequences of traumatic brain injury. Lancet Neurol. 2017;16:813–825. doi: 10.1016/S1474-4422(17)30279-X. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Erler KS, Juengst SB, Smith DL, et al. examining driving and participation 5 years after traumatic brain injury. OTJR (Thorofare N J) 2018;38:143–150. doi: 10.1177/1539449218757739. [DOI] [PubMed] [Google Scholar]
- 8.Goverover Y, Genova H, Smith A, Chiaravalloti N, Lengenfelder J. Changes in activity participation following traumatic brain injury. Neuropsychol Rehabil. 2017;27:472–485. doi: 10.1080/09602011.2016.1168746. [DOI] [PubMed] [Google Scholar]
- 9.Grauwmeijer E, Heijenbrok-Kal MH, Haitsma IK, Ribbers GM. Employment outcome ten years after moderate to severe traumatic brain injury: a prospective cohort study. J Neurotrauma. 2017;34:2575–2581. doi: 10.1089/neu.2016.4846. [DOI] [PubMed] [Google Scholar]
- 10.Zaloshnja E, Miller T, Langlois JA, Selassie AW. Prevalence of long-term disability from traumatic brain injury in the civilian population of the United States, 2005. J Head Trauma Rehabil. 2008;23:394–400. doi: 10.1097/01.HTR.0000341435.52004.ac. [DOI] [PubMed] [Google Scholar]
- 11.Fehily B, Fitzgerald M. Repeated mild traumatic brain injury: potential mechanisms of damage. Cell Transplant. 2017;26:1131–1155. doi: 10.1177/0963689717714092. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Haydel MJ, Burns B. StatPearls. StatPearls Publishing; Treasure Island, FL: 2021. Blunt head trauma. [PubMed] [Google Scholar]
- 13.Jang SH. Diagnostic problems in diffuse axonal injury. Diagnostics (Basel) 2020;10:117. doi: 10.3390/diagnostics10020117. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Jang SH, Kwon YH. A review of traumatic axonal injury following whiplash injury as demonstrated by diffusion tensor tractography. Front Neurol. 2018;9:57. doi: 10.3389/fneur.2018.00057. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Krave U, Al-Olama M, Hansson HA. Rotational acceleration closed head flexion trauma generates more extensive diffuse brain injury than extension trauma. J Neurotrauma. 2011;28:57–70. doi: 10.1089/neu.2010.1431. [DOI] [PubMed] [Google Scholar]
- 16.Maas AI, Stocchetti N, Bullock R. Moderate and severe traumatic brain injury in adults. Lancet Neurol. 2008;7:728–741. doi: 10.1016/S1474-4422(08)70164-9. [DOI] [PubMed] [Google Scholar]
- 17.Povlishock JT. Traumatically induced axonal injury: pathogenesis and pathobiological implications. Brain Pathol. 1992;2:1–12. [PubMed] [Google Scholar]
- 18.Galasko CSB, Murray PA, Pitcher M. Prevalence and long-term disability following whiplash-associated disorder. Journal of Musculoskelet Pain. 2000;8:15–27. [Google Scholar]
- 19.Higgins JP, Elliott JM, Parrish TB. Brain Network Disruption in Whiplash. AJNR Am J Neuroradiol. 2020;41:994–1000. doi: 10.3174/ajnr.A6569. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Petrescu N. Loud music listening. Mcgill J Med. 2008;11:169–176. [PMC free article] [PubMed] [Google Scholar]
- 21.Patton D, McIntosh A. Head and neck injury risks in heavy metal: head bangers stuck between rock and a hard bass. BMJ. 2008;337:a2825. doi: 10.1136/bmj.a2825. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Tricco AC, Lillie E, Zarin W, et al. PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med. 2018;169:467–473. doi: 10.7326/M18-0850. [DOI] [PubMed] [Google Scholar]
- 23.Malec JF, Brown AW, Leibson CL, et al. The Mayo classification system for traumatic brain injury severity. J Neurotrauma. 2007;24:1417–1424. doi: 10.1089/neu.2006.0245. [DOI] [PubMed] [Google Scholar]
- 24.Leibson CL, Brown AW, Ransom JE, et al. Incidence of traumatic brain injury across the full disease spectrum: a population-based medical record review study. Epidemiology. 2011;22:836–844. doi: 10.1097/EDE.0b013e318231d535. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.De Carvalho D, Almenawer S, Lozej M, Noble H, Murty NK. Spontaneous chronic subdural hematoma in a 22-year-old healthy woman. World Neurosurg. 2013;80:654. doi: 10.1016/j.wneu.2012.11.065. [DOI] [PubMed] [Google Scholar]
- 26.De Cauwer H, Van Giel R, Mortelmans L, van den Hauwe L. An uncommon cause of headache after headbanging at a party. Eur J Emerg Med. 2009;16:212–213. doi: 10.1097/MEJ.0b013e32831016cc. [DOI] [PubMed] [Google Scholar]
- 27.Edvardsson B, Persson S. Head banging associated with basilar artery thrombosis. Neurol India. 2011;59:478–479. doi: 10.4103/0028-3886.82756. [DOI] [PubMed] [Google Scholar]
- 28.Egnor MR, Page LK, David C. Vertebral artery aneurysm–a unique hazard of head banging by heavy metal rockers. Case report. Pediatr Neurosurg. 1991;17:135–138. doi: 10.1159/000120583. [DOI] [PubMed] [Google Scholar]
- 29.Gilberti N, Gamba M, Gasparotti R, Padovani A, Magoni M. Head banging" causing subdural hemorrhage and internal carotid artery dissection. Neurol Sci. 2014;35:1833–1834. doi: 10.1007/s10072-014-1831-4. [DOI] [PubMed] [Google Scholar]
- 30.Jackson MA, Hughes RC, Ward SP, McInnes EG. "Headbanging" and carotid dissection. Br Med J (Clin Res Ed) 1983;287:1262. doi: 10.1136/bmj.287.6401.1262. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Mackenzie JM. "Headbanging" and fatal subdural haemorrhage. Lancet. 1991;338:1457–1458. doi: 10.1016/0140-6736(91)92757-s. [DOI] [PubMed] [Google Scholar]
- 32.Neyaz Z, Kandpal H, Sharma R, Kale S. Head banging' during rock show causing subdural hematoma. Neurol India. 2006;54:319–320. doi: 10.4103/0028-3886.27172. [DOI] [PubMed] [Google Scholar]
- 33.Nitta N, Jito J, Nozaki K. Recurrent subdural hematoma secondary to headbanging: a case report. Surg Neurol Int. 2015;6(Suppl 18):S448–S450. doi: 10.4103/2152-7806.166777. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Pirayesh Islamian A, Polemikos M, Krauss JK. Chronic subdural haematoma secondary to headbanging. Lancet. 2014;384:102. doi: 10.1016/S0140-6736(14)60923-5. [DOI] [PubMed] [Google Scholar]
- 35.Rajasekharan C, Renjith SW, Teena AM, Parvathy R. Basilar artery thrombosis due to head banging: hazard of a religious ritual. BMJ Case Rep. 2013;2013 doi: 10.1136/bcr-2013-009840. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Scheel M, Bauknecht HC. Teaching neuroimages: head banging without head trauma: subdural hemorrhage in association with arachnoid cysts. Neurology. 2011;76:e60. doi: 10.1212/WNL.0b013e318211c389. [DOI] [PubMed] [Google Scholar]
- 37.Torrey J. Sudden death in an 11-year-old boy due to rupture of a colloid cyst of the third ventricle following 'disco-dancing. Med Sci Law. 1983;23:114–116. doi: 10.1177/002580248302300211. [DOI] [PubMed] [Google Scholar]
- 38.Gennarelli TA, Thibault LE. Biomechanics of acute subdural hematoma. J Trauma. 1982;22:680–686. doi: 10.1097/00005373-198208000-00005. [DOI] [PubMed] [Google Scholar]
- 39.Walter AE, Scaramuzzo M, Bream T, Seidenberg P, Lynch S, Slobounov SM. Effect of subconcussive impacts on functional outcomes over a single collegiate football season. J Concussion. 2020;4 [Google Scholar]
- 40.Meconi A, Wortman RC, Wright DK, et al. Repeated mild traumatic brain injury can cause acute neurologic impairment without overt structural damage in juvenile rats. PLoS One. 2018;13 doi: 10.1371/journal.pone.0197187. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Fernando H, Baker JF. Spinal cord injury secondary to “head banging” at a punk rock concert. Cureus. 2020;12:e6707. doi: 10.7759/cureus.6707. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.