Abstract
Patient engagement (PE) is a well-known strategy introduced and implemented by pharmaceutical and medical device companies for patient compliance and adherence to treatment protocols during clinical trials and care processes. This can affect a wider range of outcomes such as the quality of treatment decisions and quality of care outcomes. Few studies have paid attention to it. The involvement of patient is one of the crucial stakeholders of health care in their treatment that makes controversial opinions about the potential outcomes of their engagement in various aspects of healthcare. This scoping review was conducted in 2022 to collect the results of PE. The search was performed in the MEDLINE and Web of Sciences databases. The selected documents were categorized and reported by the direct content analysis method. Out of 3974 published documents, 17 articles were selected. Findings are categorized into 4 groups: (1) Health outcome, (2) patient compliance, (3) self-efficiency, and (4) return on investment. PE can improve both treatment outcomes and consequently patient satisfaction and health, as well as the productivity of the service provider. However, increasing self-care and patient adherence are among the positive effects of this engagement on the patient, and return on investment is still a challenge for PE.
Keywords: patient engagement, involvement, participation, impact, patient-centered outcomes, stakeholder engagement
Introduction
Healthcare industry players, mostly treatment and solution providers, address patient engagement (PE) as an imperative strategy. Access to information has increased with the advancement of technology so patients are more aware of their care conditions and options than ever before (1). PE in health care has turned into a worldwide priority because evidence shows that it improves patient adherence and compliance with clinical protocols (2). According to healthcare quality concepts patient centeredness, patient education, and empowerment are recognized as key component in improving the quality and delivery of health services (3). So, PE can be considered a quality driver in addition to the initial purposes by concept developers.
Patients are defined as one of the crucial stakeholders of health care and decision-making, and this shows the need for involving them in the treatment process (4). It is an ideal healthcare situation in which patients are well informed and motivated to be involved in their own medical care, and it is a means of ensuring that patients are provided the right care appropriate to the individual characteristics, needs, preferences, and conditions of the patients (5).
In addition to the patient, other stakeholders also influence this engagement. In Marzban et al. study, a model for PE leadership was presented by considering and combining all stakeholders: data and technology partners, providers and delivery roles, healthcare organizations, patients/families, and payor organizations. An appropriate interaction between these stakeholders and their capacity is effective in shaping PE (6).
Over the past 2 decades, the use of patient experiences in assessing the quality of care from a patient perspective has received more attention, which shows that it is not only possible to involve patients in delivery or redesign of health care, but such engagement can lead to a reduction in the number of hospitalizations, improved effectiveness, efficiency, quality of health services, quality of life, and responsiveness (7). It increase patient awareness and health literacy, so patients satisfaction are improved(8). Engagement in health improves patients’ behaviors and improves health outcomes (5, 6). Also, PE can affect the costs and other aspects (7). Engaged patients can improve health outcomes and transform health care. Patients have several expectations of the health system in regard to value, responsibility, transparency, choice, and engagement (9).
Despite the mentioned advantages, some studies showed different results. Findings of a study on patient-reported outcome measures showed that giving feedback to patients did not have a clinically significant effect on patient empowerment or satisfaction (10). In low-income settings, patients and providers are less supportive of PE in long-term chronic care because their financial and emotional problems outweigh their illness (11).
Many documents provide helpful guidelines for conducting PE and quality assessments (12–14). Evaluation studies focus mainly on qualitative methods and are only occasionally linked to specific results or outcomes (15–18). Then, due to the growing importance of PE and the gap in studies on the effects and outcomes of Engaging, in this study, we seek to identify the impact of PE by conducting a scoping review. Our scoping review implies a knowledge synthesis that addresses how PE impacts quality in healthcare aiming to highlight key concepts, types of evidence, and gaps in this research field.
Methods
This scoping review was conducted from January to September 2021 to identify the PE impact. We conducted the review through Arksey and O’Malley's original framework. This method helps to identify key characters and factors that are crucial in decision making. Mapping the topic and highlighting the gaps in existing knowledge will be possible by this method (19).
There are 6 steps in this framework including the following: (1) identification of research questions, (2) identification of related studies, (3) study selection, (4) data extraction, (5) summary and synthesis, and (6) optional consultation with experts (due to the optionality of this step, it was not done in this research) (20, 21).
Our research question was “What is the effect or consequence of PE?”. The question is designed to cover a large body of literature to avoid missing valuable documents.
Databases searched were MEDLINE (PubMed) and Web of Sciences. We used the following search MeSH terms “patient engagement” and/or “patient participation” and/or “patient involvement” and “impact or consequence or outcome” The search terms were kept broad to encompass all possibilities for relevant studies. The search was conducted in title and abstract. The search yielded 1992 results. A total of 9 studies were included in our review.
The selection criteria are (1) English language, (2) open access, (3) did address the study's question (what is the effect or consequence of PE?), (4) articles that have been published between 2010 and August 2021, and (5) All types of research including qualitative, quantitative, mixed methods, and review. Table 1 shows the search strategy in the database.
Table 1.
Search Strategy.
| Database | Search | Result |
|---|---|---|
| PubMed | Search query: ((((((((patient engagement[MeSH Terms])) OR (patient participation[MeSH Terms])) OR (patient involvement[MeSH Terms])) AND (outcome[Title/Abstract]) AND ((ffrft[Filter]) AND (2010/1/1:2022/7/19[pdat]) AND (english[Filter]))) AND (((((patient engagement[MeSH Terms])) OR (patient participation[MeSH Terms])) OR (patient involvement[MeSH Terms])) AND (outcome[Title/Abstract]) AND ((ffrft[Filter]) AND (2010/1/1:2022/7/19[pdat]) AND (english[Filter])))) OR (((((patient engagement[MeSH Terms])) OR (patient participation[MeSH Terms])) OR (patient involvement[MeSH Terms])) AND (IMPACT[Title/Abstract]) AND ((ffrft[Filter]) AND (2010/1/1:2022/7/19[pdat]) AND (english[Filter])))) OR (((((patient engagement[MeSH Terms])) OR (patient participation[MeSH Terms])) OR (patient involvement[MeSH Terms])) AND (consequence[Title/Abstract]) AND ((ffrft[Filter]) AND (2010/1/1:2022/7/19[pdat]) AND (english[Filter])))) OR (((((patient engagement[MeSH Terms])) OR (patient participation[MeSH Terms])) OR (patient involvement[MeSH Terms])) AND (consequence[Title/Abstract]) AND ((ffrft[Filter]) AND (2010/1/1:2022/7/19[pdat]) AND (english[Filter]))) | 3019 |
| Web of Sciences | (((TI = (patient engagement)) OR TI = (patient participation)) OR TI = (patient involvement)) AND TI = (outcome) (((TI = (patient engagement)) OR TI = (patient participation)) OR TI = (patient involvement)) AND TI = (impact) (((TI = (patient engagement)) OR TI = (patient participation)) OR TI = (patient involvement)) AND TI = (consequence) #1 OR #2 OR #3 and Open Access and English (Languages) | 955 |
The screening of titles and abstracts and the selection of articles from retrieved potentially relevant full manuscripts were conducted by 2 independent reviewers (MN and SM) using the selection criteria described above. Disagreements were resolved through discussion by all authors. All selected papers were transferred to Endnote software where their title and abstract were screened by the reviewer (MN) based on the selection criteria.
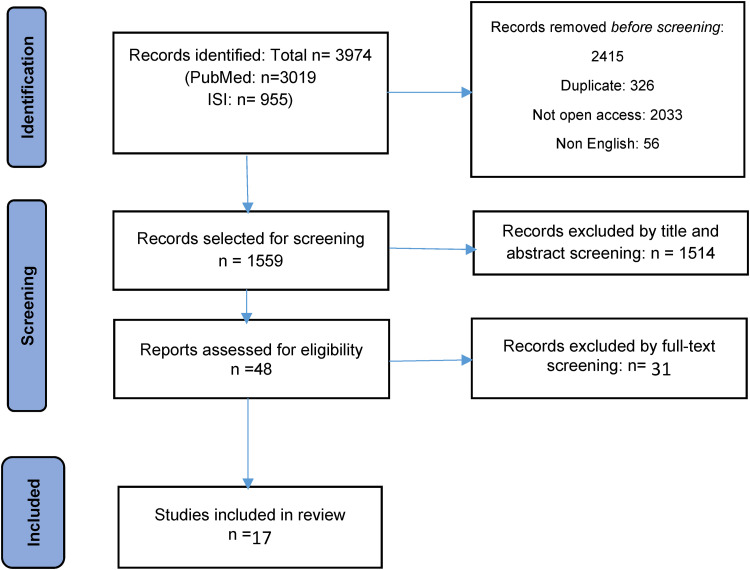
From all 3974 published documents, only 48 studies satisfied our study criteria. The full texts of articles regarded as potentially eligible for consideration were extracted and screened for further analysis based on the predefined inclusion and exclusion criteria. After all text review 17 articles were selected for this study . While writing this paper, we looked at the references used by the 17 selected articles when required. The screening process and search results are shown in Figure 1.
Figure 1.
Flowchart of the study selection process.
Data Extraction and Analysis
In the fourth step, data related to the effect or consequence of PE was extracted and tabulated based on the type of effect.Content analysis was performed to classify key themes in the selecting documents . This method starts with a predefined coding framework, but then allows new code to be used as the analysis progresses (22).
Initial codes were developed by a reviewer (SM) through regular discussion with the second reviewer (MN). If there was a disagreement about the coding, it was done in consultation with the third reviewer (EA) and by a majority decision. The content analysis of the texts was performed using MAXQDA20.
Summary and Synthesis
Finally, we summarized and reported the findings. The selection of documents was categorized according to the consequent, effect, and impact of PE (Table 2).
Table 2.
Summary of Selected Articles.
| Authors | References | Year | Article title | Methods | Findings | Aim |
|---|---|---|---|---|---|---|
| Arvanitis, M | (23) | 2020 | Development of the influence, motivation, and patient activation in diabetes (IMPACT-D (TM)) measure | Literature review, expert opinion, and qualitative interviews and focus groups | The effect and motivation of patient stimulation in diabetes care (TM) leads to better physical health and less severity of depressive and anxiety symptoms. | We sought to create a new research and clinical instrument-the Influence and Motivation for Patient ACTivation in Diabetes care (IMPACT-D (TM))—to measure the degree to which patients with type 2 diabetes (T2DM) value health and believe they can influence it |
| Gremyr, I | (24) | 2018 | Exploring the phase for highest impact on radicality: a cross-sectional study of patient involvement in quality improvement in Swedish healthcare | Exploratory cross-sectional survey | Involving patients in improvement projects can increase the quality of care and help identify completely new ways of providing care. The effect of patient involvement on perceived radicality depends on the stage of patient involvement. The greatest effect on being radical was observed in the stages of recording and action experiences, in the stage of moderate impact evaluation and the least effect was observed in the stage of identification and prioritization. | Thus, the purpose of this study was to identify the phase of an improvement cycle in which patient involvement had the highest impact on radicality of improvement |
| Gillani, SMR | (12) | 2017 | A randomised controlled trial in diabetes demonstrating the positive impact of a patient activation strategy on diabetes processes and HbA(1c): the WICKED project | Cluster randomised | By providing structural information directly to diabetic people, they become active in their care, as shown by the results of a study on care and the results of glycemic control. | We developed a structured information booklet to promote patient activation and report the 1-year outcomes of a randomised controlled trial assessing its impact on diabetes care processes and on glycaemic control |
| Vidyanti, I | (3) | 2015 | Low-income minority patient engagement with automated telephonic depression assessment and impact on health outcomes | Mixed-method analyses (including regression analyses and coding of interviews) | The biggest barrier to patient engagement is timing. The level of patient involvement varies in terms of baseline depression and has no significant effect on health outcomes and care satisfaction at 6, 12, and 18 months. However, from the results of the preliminary clinical trials, the intervention group (depression care) is more satisfied than the 2 control groups. Therefore, technology is more likely to influence satisfaction with depression care outcomes through provider participation than patient engagement. | We investigated dimensions of low-income minority patient engagement in the context of diabetes depression care management with automated telephone assessment (ATA) calls as a facilitator |
| Aung, E | (13) | 2015 | Joint influence of patient-assessed chronic illness care and patient activation on glycaemic control in type 2 diabetes | Population-based prospective cohort study | When Patient Assessment of Chronic Illness Care (PACIC) was low, a positive correlation was observed between patient activation and glycemic control. | To examine the association of the Patient Assessment of Chronic Illness Care (PACIC) with glycaemic control and the modulating effect of patient activation on this association |
| Kim, JY | (14) | 2016 | The Influence of Wireless Self-Monitoring Program on the Relationship Between Patient Activation and Health Behaviors, Medication Adherence, and Blood Pressure Levels in Hypertensive Patients: A Substudy of a Randomized Controlled Trial | Randomized controlled trial | Participating in a wireless self-monitoring program motivates people to take more control of their health management. Patient activation reduces smoking and controls blood pressure. This relationship was more observed in the reduction of smoking, alcohol consumption and systolic and diastolic blood pressure in 6 months among the participants, but no difference was observed in terms of drug adherence. | To study the influence of wireless self-monitoring program and patient activation measures on health behaviors, medication adherence, and blood pressure levels as well as control of blood pressure in hypertensive patients |
| Mc Namara, KP | (23) | 2014 | Patient engagement strategies used for hypertension and their influence on self-management attributes | A survey of patients with treated hypertension was undertaken in 27 community pharmacies. | Engaging the patient in self-monitoring or documenting blood pressure readings was associated with an increased likelihood of reaching the target blood pressure. | The aim of this study is to establish the prevalence of use of key strategies and to determine their independent relationship with patient self-management attributes. |
| Woehrle, H | (16) | 2018 | Effect of a patient engagement tool on positive airway pressure adherence: analysis of a German healthcare provider database | Data from a German healthcare provider (ResMed Healthcare Germany) were retrospectively analyzed. | Adding a PE tool may help improve adherence to treatment and reduce mask leakage. | This study investigated the addition of a real-time feedback patient engagement tool on positive airway pressure (PAP) adherence when added to a proactive telemedicine strategy |
| Dukhanin V | (15) | 2018 | Metrics and Evaluation Tools for Patient Engagement in Healthcare Organization- and System-Level Decision-Making: A Systematic Review | Systematic review | Forty-four outcome metrics were grouped into 3 domains (internal, external, and aggregate outcomes) that included 6 subdomains: impact on engagement participants, impact on services provided by the healthcare organization, impact on the organization itself, influence on the broader public, influence on population health, and engagement cost-effectiveness. d when systems or organizations evaluate cost-effectiveness, they should include the time and resource costs accruing to P2C2 participants | Define a taxonomy of possible P2C2 engagement metrics and compare existing evaluation tools against this taxonomy |
| Higgins, MA | (25) | 2016 | Unraveling the meaning of patient engagement: A concept analysis | Literature review, concept analysis | Four defining attributes of actively patient engagement in care include personalization, access, commitment and therapeutic alliance | This study seeks to define the concept by identifying patient engagement in the context of its use |
| Newman, B | (26) | 2021 | Do patient engagement interventions work for all patients? A systematic review and realist synthesis of interventions to enhance patient safety | Systematic review, Meta-analysis | Collaborative strategy development, a user-friendly design, proactive messaging and agency sponsorship were identified as mechanisms to improve engagement about safety at the point of direct care | This review identifies the strategies used to engage patients in safety during direct care, explores who is engaged and determines the mechanisms that impact effectiveness. |
| Anjana, E | (23) | 2018 | Patient Engagement In Health Care Safety: An Overview Of Mixed-Quality Evidence | Systematic review | Supporting patient engagement in medication and chronic disease self-management, adverse event reporting, and medical record accuracy has a positive effect on safety efforts | This research aims to develop guidelines to enhance patient partnership within safety efforts |
| Barello, S | (3) | 2012 | Patient Engagement as an Emerging Challenge for Healthcare Services: Mapping the Literature | Bibliometric and qualitative content analyses | Patient engagement has been identified as a key factor to improve health services delivery and quality | This study was conducted with the aim of the impact of patient engagement on the quality of health care |
| Bombard, Y | (16) | 2018 | Engaging patients to improve quality of care: a systematic review | Systematic review, Meta-analysis | Identify strategies for optimal patient engagement to improve quality of health care such as: techniques to enhance (1) design, (2) recruitment, (3) involvement, (4) creating a receptive context, and (5) leadership actions. | The aim of this research was to identify factors and strategies that make patient engagement possible and lead to improving the health services quality. |
| Schwappach, B | (27) | 2010 | Engaging Patients as Vigilant Partners in Safety | Systematic review | The involvement of patients in safety may be successful if initiatives are based on patients’ perspectives, promote complex behavioral change, and if their implementation is accompanied by serious efforts for cultural and normative change in health care institutions that place patients and their safety at the center of health care. | This study was conducted with the aim of investigating the evidence of patients’ attitudes toward engagement in error prevention and the effectiveness of efforts to increase patient participation |
| Hibbard, J | (2) | 2003 | Engaging health care consumers to improve the quality of care | Conceptual framework and review of the literature | Engaging patients in collaborative care, shared decision-making with their providers, and chronic disease self-management have improved health outcomes and lead to increases functioning, reduces pain, and decreases costs. | The purpose of this study To examine the evidence available on the contribution of consumers to care quality through the coproducer and evaluator roles |
| Liang, L | (28) | 2018 | Patient engagement in hospital health service planning and improvement: a scoping review Implementing family-integrated care in the NICU: engaging veteran parents in program design and delivery | Scoping review | Asking patients to provide insight into problems rather than solutions and deploying provider champions may enhance patient influence on hospital services. | The purpose of this study was to evaluate PE in hospital health service improvement. |
Ethical considerations such as the risk of bias assessment during document selection, data extraction, and data analysis were observed at all stages.
Results
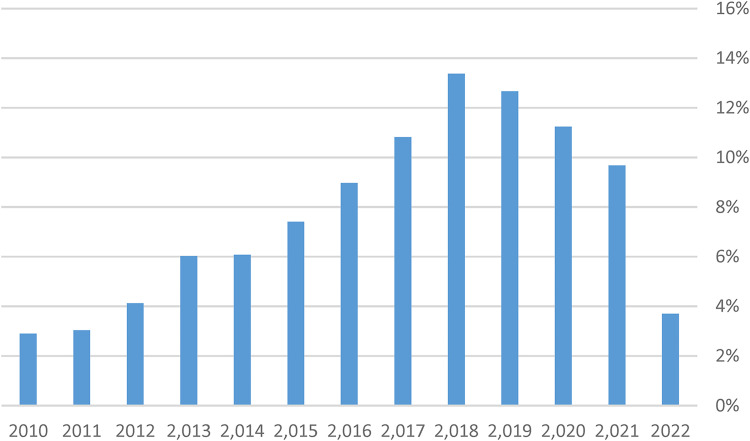
Our search revealed a total of 3974 published documents. After screening the titles and abstracts, only 48 documents remained. After all the authors reviewed the included full-text articles, only 17 articles were selected for this study. Figure 2 shows that studies related to PE have been on the rise over the past 10 years, however, still studies on this topic are few. The most studies had published between 2019 and 2022.
Figure 2.
Patient engagement (PE) consequences study by publication year.
Based on Table 3, findings are categorized into 4 groups: (1) Health outcome/effectiveness: improving the quality of care (16, 3 23, 24, 26–28), the likelihood of achieving treatment results (30), patient satisfaction, and reducing depression and anxiety (25, 31), (2) patient compliance: improving patient adherence to treatment process (32), (3) self-efficiency: increasing patient responsibility and motivates people can take more control of their health management (2, 12–14, 23, 33), and (4) return on investment: cost-effectiveness determined by time and resources, and timing is the biggest barrier to PE so it is more likely care outcomes improve through provider engagement rather than PE(2, 15).
Table 3.
Classification of Consequences of Patient Engagement (PE).
| Consequences | Type | Example |
|---|---|---|
| Health outcome/effectiveness | Improving the quality of care | Involving patients in improvement projects can increase the quality of care and help identify completely new ways of providing care. The effect of patient involvement on perceived radiculitis depends on the stage of patient involvement. The greatest effect on being radical was observed in the stages of recording and action experiences, in the stage of moderate impact evaluation and the least effect was observed in the stage of identification and prioritization (24). Supporting patient engagement in medication and chronic disease adverse event reporting, and medical record accuracy has a positive effect on safety efforts (29). |
| Achieving treatment results | Engaging the patient in self-monitoring or documenting blood pressure readings was associated with an increased likelihood of reaching the target blood pressure (26). | |
| Patient satisfaction | From the results of the preliminary clinical trials, the intervention group (depression care) is more satisfied than the 2 control groups. Therefore, technology is more likely to influence satisfaction with depression care outcomes through provider participation than patient engagement (3). | |
| Reduce depression and anxiety | The effect and motivation of patient simulation in diabetes care (TM) leads to better physical health and less severity of depressive and anxiety symptoms (23). | |
| Patient compliance | Improving patient adherence to the treatment process | Adding a PE tool may help improve adherence to treatment and reduce mask leakage and positive airway pressure adherence (16). |
| Self-efficiency | Increasing patient responsibility | When Patient Assessment of Chronic Illness Care (PACIC) was low, a positive correlation was observed between patient activation and glycemic control (13). |
| Better self-control | By providing structural information directly to diabetic people, they become active in their care, as shown by the results of a study on care and the results of glycemic control. (12) | |
| Participating in a wireless self-monitoring program motivates people to take more control of their health management. Patient activation reduces smoking and controls blood pressure. This relationship was more observed in the reduction of smoking, alcohol consumption, and systolic and diastolic blood pressure in 6 months among the participants, but no difference was observed in terms of drug adherence. (14) | ||
| Return on investment | Time and resources | The biggest barrier to PE is timing.(3) |
| When systems or organizations evaluate cost-effectiveness, they should include the time and resource costs accruing to PE.(15) |
Discussion
This review showed that studies related to PE have been on the rise over the past 10 years. According to Bhati et al. (34), patients engaged in 3 primary care research studies found the experience to be positive and felt good that they had contributed to the research. In addition the last pandemic, it is thought to cause the US hospitals to face between $53 billion and $122 billion in missed revenue in 2021. It is reported that currently 897 hospitals are at risk of closing and many are being forced to reduce staffing (34). Studies show that patients with the lowest activation have the most expensive costs and vice versa. When examining the causal factors that contribute to the association between PE and costs, highly engaged patients are more likely to perform health-improving behaviors that correlate with better outcomes and lower long-term costs. Results of a study showed that highly engaged patients can have a better control on high-density lipoproteins cholesterol, and triglycerides and are less likely to smoke or be obese. They are more likely to get pap smears and mammograms, have their depression better controlled and have fewer emergency visits and hospitalizations (35). Furthermore, PE can be very beneficial in 4 different ways:
Health Outcome/Effectiveness
Improving the quality of care, the likelihood of achieving treatment results, patient satisfaction, and reducing depression and anxiety: PE can improve the quality of care by informing patients and providers and enhancing governance and service delivery (16). Geramita's study showed that 11% of participants with the highest engagement levels have significant improvements in anxiety (17).
There are several strategies for patient and family engagement to reduce anxiety and depression. The results of a review study showed that the most common strategies were patient education and self-management support. Individual care planning shared decision-making, and family or peer support were also common strategies (18).
An engaged patient is more likely to take their medications as prescribed by their doctors, resulting in fewer complications, minimizing unnecessary visits, and emergency admissions in the hospital. There is a high chance that these patients engage more in preventative behaviors such as immunizations, mammograms, regular health checkups, healthy eating, or STI/STD screenings (36).
Patient Compliance
Improving patient adherence to the treatment process: To improve the quality of healthcare, patients must adhere to treatment recommendations. In addition to a threat to health and the effectiveness of treatment, patient noncompliance can also have a significant economic burden. misunderstanding, forgetting, or ignoring care recommendations can put more than 40% of patients at significant risk. Engaging between physician and patient when choosing a treatment option can maximize patient commitment and adherence. This interaction reduces the risks of noncompliance by increasing patient satisfaction and improve health outcomes (20). In Danielson's study, the core components for adherence to treatment in patients were identified; motivation, cohesion, commitment, and empowerment. (21).
Self-Efficacy
Increasing patient responsibility and motivating people to take more control of their health management. Patient self-efficacy is defined as the confidence and ability to take the necessary steps to achieve their goals. Self-efficacy provides a roadmap for using the power of patients to engage in their care (37). The results of Hoffman study showed that oncology nurses can use perceived self-efficacy to improve patients’ quality of life (38). Patients with multiple diseases and with low self-efficacy have a lower quality of life. Awareness of the level of self-efficacy among patients with multiple diseases may help identify patients who need more support. Supporting self-management in patients with chronic diseases is one of the important features of good care (39).
Return on Investment
Return on investment is one of the methods of evaluating alternative solutions. This method tries to quantify the financial benefits and costs of the solutions (40). That is determined by time and resources, and selected documents showed time is the biggest barrier to PE, so it is more likely care outcomes improve through provider engagement rather than PE. PE efforts should focus on supporting and encouraging health workers to ensure patients’ experience is based on interaction with them (41). Although patients, service providers, and sponsors are increasingly considering PE, sponsors are often reluctant to engage with patients because of uncertainty about return on investment (42). The Return on Investment (ROI) is also a well-recognized and trusted method of evaluation. The main benefit of PE for the healthcare team is increased productivity (43). In order to check the progress, it is essential to be aware of every investment's returns in different campaigns and advertisements that focus on PE. Measuring the return of investment is complicated, however, there are certain parameters that can assist us and make the process easier. Important parameters that can help us understand the ROI might be the number of outpatient visits, number of visitors to online portals, an increased messages database, and an increased number of patient admissions. ROI is the most important factor in successfully managing a business and healthcare is no exception. In this perspective, assessing the working techniques and continuously improving them is essential (29). Le et al., in their review, found that the impacts of PE can be better determined using a coherent set of measures versus single indicators (7).
Health care is experiencing patients that have expectations for value, transparency, choice, and engagement (9). However, PE studies are still limited (35) and, meaningfully engaging patients has often proven to be difficult (9). Patient advisors have provided the clinical research team with insight into objective issues that can cause a patient's reluctance to participate in a clinical trial. Among other factors, they mention time, expense, and prior beliefs and attitudes about clinical trials. Patients may fear that they might not be seen as persons but rather as research subjects and sometimes they don't understand what clinical research means (44). In addition, for rare diseases because of the low number of patients available for collaboration researchers struggle to gain the insights they need to understand these uncommon illnesses (45). It is recommended to encourage patient partners to actively participate in discussions regarding the protocol, including them in decisions made, and ask and evaluate each individual's true understanding of the topics that are being discussed. It is important to ensure that their perspective is at the forefront (46). Healthcare organizations are under pressure to control costs while maintaining the quality of care especially as they assume more financial risk for population health management. Effective PE solutions, such as telehealth or remote patient monitoring would improve patient outcomes. As a result, it will decrease readmission, emergency department utilization, and overall usage of the health system which in the turn would reduce total costs of care (47). Beyond the revenue and patient satisfaction increases that a health system can obtain from using inpatient telemedicine is the opportunity to reduce staffing costs (48). One barrier for providers regarding the implementation of various types of healthcare technologies (not limited to e-visits) in the United States is the reported lack of return on investment in the literature. As computerized provider order entry and electronic medical records systems are potentially related to e-visit technologies, the reported lack of return on investment for these technologies may serve as a barrier to the adoption of e-visit technologies (29). Healthcare quality is considered a health system that continuously seeks to make improvements in 6 areas or dimensions of quality, as follows: safety, effectively, patient-centered, timely, efficiency, equitable (49).
PE aims to strengthen and support patients’ abilities and self-care responsibilities and then collaborate with their healthcare providers to improve their health and achieve the maximum values of healthcare services (50).
PE helps healthcare professionals to collaborate with patients to work together to improve health outcomes. Recent studies indicated that improving PE could bring a positive influence on the healthcare quality of care. However, the relationship might be deeply influenced by an individual's psychological, and physical or social characteristics (51).
Limitations of Study
Some weaknesses of the present research are denoted here. First, Studies about PE impacting on quality of care were limited. PE is a relatively new concept and lack of prior research studies on the topic is noted. Second, we have only included papers written in English language and conducted the search in 2 databases. Third, more investigations are necessary to discover the magnitude in which PE can impact the quality of health care services.
Conclusions
PE and impact on healthcare is relatively a new concept and only a few studies have assessed the outcomes and impacts of various PE interventions. This might be due to heterogeneous strategies that engage patients mostly through clinical research rather than routine healthcare services or might be related to a gap in the evidence. Further research is required to improve the knowledge on how PE can advance the quality of care in the health industry. Our findings suggest that PE might be beneficial to patients and service providers alike. Patients can be apprehensive about participating in clinical trials, but it is imperative to have the patient's perspective when designing, and implementing trials to ensure that their perspective is at the forefront (52).
Acknowledgements
The author(s) also extend their gratitude and appreciation to the esteemed reviewers who provided constructive and valuable suggestions for improving the quality of this article.
Author Biographies
Sima Marzban, PhD of health service management, president and CEO at Key Patient Insights, Chapel Hill, North Carolina. Keypatientinsights.com. simam1349@gmail.com
Marziye Najafi, PhD Student in Health Services Management, Department of Health Economics and Management, School of Public Health, Tehran University of Medical Sciences, Tehran, Iran. Department of Health Management, School of Public Health, Karaj University of Medical Sciences, Karaj, Iran. Marziyenajafi@yahoo.com
Arjola Agolli, Post-Doctoral Fellow, Department of Family and Community Medicine, Pennsylvania State University, Pennsylvania. Division of Clinical and Translational Research, Larkin Community Hospital, Florida, USA. aagolli@penstatehealth.psu.edu
Ensieh Ashrafi, PhD Student in Health Services Management, Department of Health Economics and Management, School of Public Health, Tehran University of Medical Sciences, Tehran, Iran. En_ashrafi@yahoo.com
Footnotes
Author’s Contribution: SM and MN conceptualized this scoping review. MN and EA searched across databases and selected relevant articles or documents for this scoping review. SM, MN, and EA reviewed the articles. MN and AA wrote the manuscript. All authors read and approved the final manuscript.
Declaration of Conflicting Interests: The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding: The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval and Consent to Participate: Not applicable.
Consent for Publication: Not applicable.
Availability of Data and Materials: All data generated or analyzed during this study are included in this manuscript.
ORCID iD: Marziye Najafi https://orcid.org/0000-0002-5445-2235
References
- 1.Manafo E, Petermann L, Mason-Lai P, et al. Patient engagement in Canada: a scoping review of the ‘how’ and ‘what’ of patient engagement in health research. Health Res Policy Sys. 2018;16(1):5. doi: 10.1186/s12961-018-0282-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Liang L, Cako A, Urquhart R, et al. Patient engagement in hospital health service planning and improvement: a scoping review. BMJ. Open. 2018;8(1):e018263. doi: 10.1136/bmjopen-2017-018263. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Barello S, Graffigna G, Vegni E. Patient engagement as an emerging challenge for healthcare services: mapping the literature. Nurs Res Pract. 2012;2012:905934. doi: 10.1155/2012/905934. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Gallivan J, Kovacs Burns K, Bellows M, et al. The many faces of patient engagement. J Particip Med. 2012;4:e32. [Google Scholar]
- 5.Street RL, Jr, Millay B. Analyzing patient participation in medical encounters. Health Commun. 2001;13(1):61‐73. [DOI] [PubMed] [Google Scholar]
- 6.Nelson DE, Kreps GL, Hesse BW, et al. The health information national trends survey (HINTS): development, design, and dissemination. J Health Commun. 2004;9(5):443‐60. [DOI] [PubMed] [Google Scholar]
- 7.Forbat L, Cayless S, Knighting K, et al. Engaging patients in health care: an empirical study of the role of engagement on attitudes and action. Patient EducCouns. 2009;74(1):84‐90. [DOI] [PubMed] [Google Scholar]
- 8.Coulter A. Patient engagement—what works? J Ambul Care Manage. 2012;35(2):80‐9. doi: 10.1097/JAC.0b013e318249e0fd. [DOI] [PubMed] [Google Scholar]
- 9.Abdelhak M. Patient engagement: opportunities and challenges for nursing and health care professionals. Stud Health Technol Inform. 2016;225:707‐9. [PubMed] [Google Scholar]
- 10.Ackermans L, Hageman MG, Bos AH, et al. Feedback to patients about patient-reported outcomes does not improve empowerment or satisfaction. Clin Orthop Relat Res. 2018;476(4):716‐22. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Abrahams N, Gilson L, Levitt NS, et al. Factors that influence patient empowerment in inpatient chronic care: early thoughts on a diabetes care intervention in South Africa. BMC Endocr Disord. 2019;19(1):133. doi: 10.1186/s12902-019-0465-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Gillani SMR, Nevill A, Singh BM. A randomised controlled trial in diabetes demonstrating the positive impact of a patient activation strategy on diabetes processes and HbA(1c): the WICKED project. British Journal of Diabetes. 2017;17(2):58‐63. [Google Scholar]
- 13.Aung E, Donald M, Williams GM, et al. Joint influence of patient-assessed chronic illness care and patient activation on glycaemic control in type 2 diabetes. Int J Qual Health Care. 2015;27(2):117‐24. [DOI] [PubMed] [Google Scholar]
- 14.Kim JY, Wineinger NE, Steinhubl SR. The influence of wireless self-monitoring program on the relationship between patient activation and health behaviors, medication adherence, and blood pressure levels in hypertensive patients: a substudy of a randomized controlled trial. J Med Internet Res. 2016;18(6):e116. doi: 10.2196/jmir.5429. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Dukhanin V, Topazian R, DeCamp M. Metrics and evaluation tools for patient engagement in healthcare organization- and system-level decision-making: a systematic review. Int J Health Policy Manag. 2018;7(10):889‐903. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Bombard Y, Baker GR, Orlando E, et al. Engaging patients to improve quality of care: a systematic review. Implement Sci. 2018;13(1):98. doi: 10.1186/s13012-018-0784-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Geramita EM, HerbeckBelnap B, Abebe KZ, et al. The association between increased levels of patient engagement with an internet support group and improved mental health outcomes at 6-month follow-up: post-hoc analyses from a randomized controlled trial. J Med Internet Res. 2018;20(7):e10402. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Menear M, Dugas M, Careau E, et al. Strategies for engaging patients and families in collaborative care programs for depression and anxiety disorders: a systematic review. J Affect Disord. 2020;263:528‐39. doi: 10.1016/j.jad.2019.11.008. [DOI] [PubMed] [Google Scholar]
- 19.Peters M, Godfrey C, Khalil H, McInerney P, Parker D, Soares CB. Guidance for conducting systematic scoping reviews. Int J Evid Based Healthc. 2015;13(3):141‐6. doi: 10.1097/XEB.0000000000000050. [DOI] [PubMed] [Google Scholar]
- 20.Martin LR, Williams SL, Haskard KB, et al. The challenge of patient adherence. TherClin Risk Manag. 2005;1(3):189‐99. [PMC free article] [PubMed] [Google Scholar]
- 21.Danielson E, Melin-Johansson C, Modanloo M. Adherence to treatment in patients with chronic diseases: from alertness to persistence. Int J Community Based Nursing & Midwifery. 2019;7(4):248‐57. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Hsieh H-F, Shannon SE. Three approaches to qualitative content analysis. Qual Health Res. 2005;15(9):1277‐88. doi: 10.1177/1049732305276687. [DOI] [PubMed] [Google Scholar]
- 23.Sharma AE, Rivadeneira NA, Barr-Walker J, Stern RJ, Johnson AK, Sarkar U. Patient engagement in health care safety: an overview of mixed-quality evidence. Health Aff (Millwood). 2018;37(11):1813‐20. doi: 10.1377/hlthaff.2018.0716. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Gremyr I, Elg M, Smith F, et al. Exploring the phase for highest impact on radicality: a cross-sectional study of patient involvement in quality improvement in Swedish healthcare. BMJ Open. 2018;8(11). [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Vidyanti I, Wu B, Wu SY. Low-income minority patient engagement with automated telephonic depression assessment and impact on health outcomes. Qual Life Res. 2015;24(5):1119‐29. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Newman B, Joseph K, Chauhan A, et al. Do patient engagement interventions work for all patients? A systematic review and realist synthesis of interventions to enhance patient safety. Health Expect. 2021;24(6):1905‐23. doi: 10.1111/hex.13343. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Schwappach DL. Review: engaging patients as vigilant partners in safety: a systematic review. Med Care Res Rev. 2010;67(2):119‐48. doi: 10.1177/1077558709342254. [DOI] [PubMed] [Google Scholar]
- 28.Hibbard JH. Engaging health care consumers to improve the quality of care. Med Care. 2003;41(1 Suppl):I61‐70. doi: 10.1097/00005650-200301001-00007. [DOI] [PubMed] [Google Scholar]
- 29.https://imcdigital.life/blog/author/omkar/IMC-health.care.digital (2020). Quantifying Patient Engagement- How it Improves Your Return on Investment (R O I). https://imcdigital.life/blog/quantifying-patient-engagement-how-it-improves-your-return-on-investment-r-o-i/
- 30.Mc Namara KP, Versace VL, Marriott JL, et al. Patient engagement strategies used for hypertension and their influence on self-management attributes. Fam Pract. 2014;31(4):437‐44. [DOI] [PubMed] [Google Scholar]
- 31.Arvanitis M, Bailey SC, Wismer G, et al. Development of the influence, motivation, and patient activation in diabetes (IMPACT-D (TM)) measure. Diabetes Res Clin Pract. 2020;159:107965. doi: 10.1016/j.diabres.2019.107965. [DOI] [PubMed] [Google Scholar]
- 32.Woehrle H, Arzt M, Graml A, et al. Effect of a patient engagement tool on positive airway pressure adherence: analysis of a German healthcare provider database. Sleep Med. 2018;41:20‐6. [DOI] [PubMed] [Google Scholar]
- 33.Higgins T, Larson E, Schnall R. Unraveling the meaning of patient engagement: a concept analysis. Patient Educ Couns. 2017;100(1):30‐6. doi: 10.1016/j.pec.2016.09.002. [DOI] [PubMed] [Google Scholar]
- 34.Bhati DK, Fitzgerald M, Kendall C, et al. Patients’ engagement in primary care research: a case study in a Canadian context. Res Involv Engagem. 2020;6(1):65. doi: 10.1186/s40900-020-00238-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Murali NS, Deao CE. Patient engagement. Prim. Care. 2019:543. [DOI] [PubMed] [Google Scholar]
- 36.R1. Transform patient revenue performance. https://www.visitpay.com/blog-posts/improving-patient-engagement-despite-financial-challenges. Accessed on September 2021.
- 37.Kariuki Florence. The Complete Guide to Patient Engagement. https://www.healthrecoverysolutions.com/patient-engagement-guide. Accessed on September 2021.
- 38.Delfs J. Self-efficacy and patient engagement and empowerment: Imperative to improving health outcomes. The Foundation for Health Smart Consumers; 2011. [Google Scholar]
- 39.Hoffman AJ. Enhancing self-efficacy for optimized patient outcomes through the theory of symptom self-management. Cancer Nurs. 2013;36(1):E16‐26. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Peters M, Potter CM, Kelly L, Fitzpatrick R. Self-efficacy and health-related quality of life: a cross-sectional study of primary care patients with multi-morbidity. Health Qual Life Outcomes. 2019;17(1):37. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Walker JB, Fruin J. Active Patient Engagement Return on Investment (ROI). 2016, Available from: https://www.ecosofthealth.com/patient-engagement-return-on-investment-roi/.
- 42.Shiozaki L, Burgomaster K, Lemonde M. Improving patient engagement and satisfaction: lessons from a patient-driven care initiative in a community-based hospital. Healthcare Quarterly (Toronto, Ont). 2017;20(1):62‐6. [DOI] [PubMed] [Google Scholar]
- 43.EcoSoft Health. Significant ROI Can Be Achieved Using An Active Patient Engagement Technology. https://www.ecosofthealth.com/wp-content/uploads/Exec-Overview-Active-Patient-Engagement-Technology.pdf. Accessed on September 10, 2022.
- 44.Levitan B, Getz K, Eisenstein EL, et al. Assessing the financial value of patient engagement: a quantitative approach from CTTI’s patient groups and clinical trials project. Ther Innov Regul Sci. 2017;52(2):220‐9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Hale D, Marvel D, Wells J, PREP-IT Investigators. What’s important: patient engagement in research. The Journal of Bone and Joint Surgery. 2020;102(20):1836‐8. doi: 10.2106/JBJS.19.00625. [DOI] [PubMed] [Google Scholar]
- 46.Improving Patient and Worker Safety. Opportunities for Synergy, Collaboration and Innovation, 2012. https://www.jointcommission.org›tjc›resources. Accessed on November 2021.
- 47.Kariuki Florence. The Benefits of a Robust Patient Engagement Strategy. https://www.healthrecoverysolutions.com/patient-engagement-guide, Accessed on September 2021.
- 48.Whitten P, Buis L, Love B. Physician-Patient e-visit programs. Dis-Manage-Health-Outcomes. 2007;15:207‐14. 10.2165/00115677-200715040-00002. [DOI] [Google Scholar]
- 49.https://www.who.int/management/quality/assurance/QualityCare_B.Def.pdf
- 50.Hansen N, Kellgren M. Harnessing healthcare data. the value of healthcare data through a patient’s journey. https://www.medtronic.com/us-en/healthcare-professionals/services. Accessed January 2022.
- 51.Xu RH, Cheung AWL, Wong ELY. The relationship between patient engagement and health-related quality of life in patients: a cross-sectional study in general outpatient clinic in Hong Kong SAR, China. Patient Prefer Adherence. 2019;13:1451‐62. 10.2147/PPA.S216891. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Vat LE, Finlay T, Jan Schuitmaker-Warnaar T, et al. Evaluating the “return on patient engagement initiatives” in medicines research and development: a literature review. Health Expect. 2020;23(1):5‐18. doi: 10.1111/hex.12951. [DOI] [PMC free article] [PubMed] [Google Scholar]