Abstract
While most children with coronavirus 2019 (COVID-19) experience mild illness, some are vulnerable to severe disease and develop long-term complications. Children with disabilities, those from lower-income homes, and those from racial and ethnic minority groups are more likely to be hospitalized and to have poor outcomes following an infection. For many of these same children, a wide range of social, economic, and environmental disadvantages have made it more difficult for them to access COVID-19 vaccines. Ensuring vaccine equity in children and decreasing health disparities promotes the common good and serves society as a whole. In this article, we discuss how the pandemic has exposed long-standing injustices in historically marginalized groups and provide a summary of the research describing the disparities associated with COVID-19 infection, severity, and vaccine uptake. Last, we outline several strategies for addressing some of the issues that can give rise to vaccine inequity in the pediatric population.
Keywords: SARS-CoV-2, COVID-19, pediatric, health disparities, vaccines
KEY POINTS.
Vaccination is key to mitigating the disproportionate impact of COVID-19.
Achieving high COVID-19 vaccine uptake has been a significant challenge.
Vaccine equity will not be realized until communities of color trust the vaccines and the institutions overseeing them.
INTRODUCTION
There has long been a disparity in life expectancy and health outcomes between people of color in the United States and the rest of the country [1]. A long history of unequal treatment, racism, discriminatory policies, and economic hardship has contributed to the known disparities [1–4]. However, coronavirus 2019 (COVID-19), the disease caused by the SARS-CoV-2 virus, has placed these health inequities in the spotlight. Although no one has been spared the direct or indirect harmful effects of the virus, it is clear that the burden of COVID-19 has not been distributed equally. Indeed, race and ethnicity have largely come to define the risk of SARS-CoV-2 infection, with Black, Indigenous, and People of Color (BIPOC) communities experiencing the highest rates of infection, hospitalization, and death [4]. Though children have not been the face of the pandemic, they have also been profoundly affected. Since the start of the pandemic, children have accounted for roughly 19% of COVID-19 cases, affecting nearly 13.1 million children in the United States [5]. Although most children with SARS-CoV-2 survive their illness, some can develop new physical, cognitive, or psychiatric impairments that can significantly affect their daily functioning [6–8].
Vaccines are the key to mitigating the disproportionate impact of COVID-19. However, achieving high uptake in children and BIPOC communities has been a significant challenge. To avoid perpetuating these disparities for future generations, we must address the structural and historical barriers that encourage unequal access to and uptake of vaccines. In this article, we describe the impact COVID-19 has had on children and examine the underlying causes of the existing health and vaccine inequities. We conclude with a sample of success stories and strategies that can be put into action to address the numerous issues that contribute to vaccine disparities in children.
PEDIATRIC COVID-19: A MICROCOSM OF WIDER HEALTH DISPARITIES
Disparities in children have largely followed trends in adults—meaning children of color, like their adult counterparts, have suffered the brunt of infections, hospitalizations, and deaths [9–14]. The Centers for Disease Control and Prevention (CDC) estimates that from March 1, 2020, through April 2, 2022, Black, Hispanic, American Indian, and Alaska Native (AIAN) children were twice as likely to be hospitalized compared to non-Hispanic White children [15]. Despite accounting for only 40% of the population, nearly 80% of pediatric deaths have occurred among Black, Hispanic, and AIAN children [16].
COVID-19 has not introduced new health disparities; rather, it has brought to light and exacerbated the inequalities that have always existed [17]. These disparities can be traced back to long-standing structural failings that have led to economic hardships, housing instability, food insecurity, and inadequate health care [4]. Having adequate and affordable health insurance, for example, is crucial to sustaining the health of children and adolescents, yet close to a third of the children in the country are uninsured or underinsured [18, 19]. In 2021, Hispanic and Black families were the most likely to lack health insurance coverage (30%, and 14%, respectively) [20]. Certain immigration policies may have only further exacerbated the problem by discouraging undocumented families from enrollment in government aid programs out of fear of deportation [21]. The absence of stable insurance coverage has a direct chilling effect on the uptake of vaccines and other therapeutics [22–25]. Thus, even though effective COVID-19 therapeutics and prophylactic agents are available for the pediatric population [26–29], many undocumented and underinsured families delay or entirely avoid treatment due to concerns about their migratory situation or anxiety about incurring devastating medical bills in the process [30–33].
Persistent poverty, exacerbated by the pandemic, was another factor that undoubtedly contributed to the observed COVID-19 disparities. Historically, the AIAN population has had one of the highest poverty rates (25%) in the nation [34], followed closely by the Black and Hispanic populations (20% and 17%, respectively) [35]. Children from immigrant households, who make up nearly a quarter of all children in the United States, have also consistently had rates of poverty above 20% [36]. During the pandemic, the number of persons living in poverty increased to 37 million, roughly 3 million higher than the year prior [35]. Children with undocumented-immigrant parents were particularly affected by the economic effects of the pandemic because their eligibility for anti-poverty programs was extremely limited [37]. These financial constraints not only made it difficult for families to manage expenses and access affordable housing, nutritious food, and childcare but they also hampered access to crucial SARS-CoV-2 testing and personal protective equipment [4].
Differences in susceptibility may have also led to the increased rate of severe infections. Many of these same uninsured, impoverished, or minority children are also more likely to have undiagnosed chronic diseases [38], or conditions that have been associated with progression to severe COVID-19 (eg, diabetes, hypertension, obesity, and chronic lung disease) [2, 39–43]. Although difficult to quantify, the stress of dealing with poverty and racial discrimination can also take its toll on the body. This has been demonstrated to be the case for several other medical conditions [44–46] and may have also contributed to the elevated risk of severe COVID-19 in the pediatric population.
There is also evidence to suggest that BIPOC children were exposed to the virus at a higher rate than the general population. Many minorities live in multigenerational homes, crowded conditions, and densely populated urban areas, making social distancing difficult [4]. Black and Hispanic parents are also disproportionately represented in essential work settings (eg, healthcare facilities, farms, factories, food production and processing, grocery stores, and public transportation) that do not typically permit remote work and increase the risk of exposure to the virus [4, 47–49]. On reservations, employment is highly concentrated in the casino (55%) and administrative sectors (34%), which are also frontline and public-facing positions that increase the risk of infection [50]. Thus, limited access to diagnostics, personal protective equipment, as well as increased exposure to the virus undoubtedly contributed to the unmitigated transmission in underserved and low-income communities.
PEDIATRIC COVID-19 VACCINES
COVID-19 vaccines were first introduced in December 2020 and have been available to adolescents 12 years of age and above since May 2021 and to children 6 months and older since June 2022 [51–53]. These vaccines have been shown to be effective at preventing hospitalization and severe disease [27, 54–57]. A successful immunization program depends not only on the availability of safe and effective vaccines but also on high vaccine uptake in relevant communities. Yet, since their introduction, there has been low uptake of the COVID-19 vaccines in the pediatric population and significant disparities in coverage. As of May 2022, only half of the children 12–17 years of age have completed the 2-dose series, while only 28% who are 5–11 years of age have done so [58]. Among the states that have reported pediatric COVID-19 vaccine data disaggregated by race/ethnicity, most found Black and Hispanic children to have had the lowest overall uptake [59]. Failing to achieve high uptake of COVID-19 vaccines in these vulnerable and underserved subpopulations will only lead to persistent community transmission and amplify the pandemic’s detrimental social and economic effects.
DRIVERS OF COVID-19 VACCINE INEQUITY AND STRATEGIES GOING FORWARD
Providing equitable access to vaccines and decreasing health disparities in the pediatric population is a public health priority. Historically, however, there have been significant disparities in vaccination coverage rates. According to the National Immunization Surveys, between 2009 and 2018, the proportion of infants who have completed the 7-vaccine series has been consistently lower for infants who are uninsured or publicly insured, who live below poverty, and who are Black or Hispanic [60]. A similar disparity in vaccine uptake along racial/ethnic lines was seen during the 2009 H1N1 influenza pandemic, which, much like COVID-19, required high coverage of a novel vaccine to reduce viral transmission. These long-standing immunization coverage gaps resonate with what we have observed during the COVID-19 pandemic. However, vaccine equity can be achieved through programs and policies that are sensitive to the needs of these subgroups of the population and address the barriers that have historically contributed to disparities in uptake.
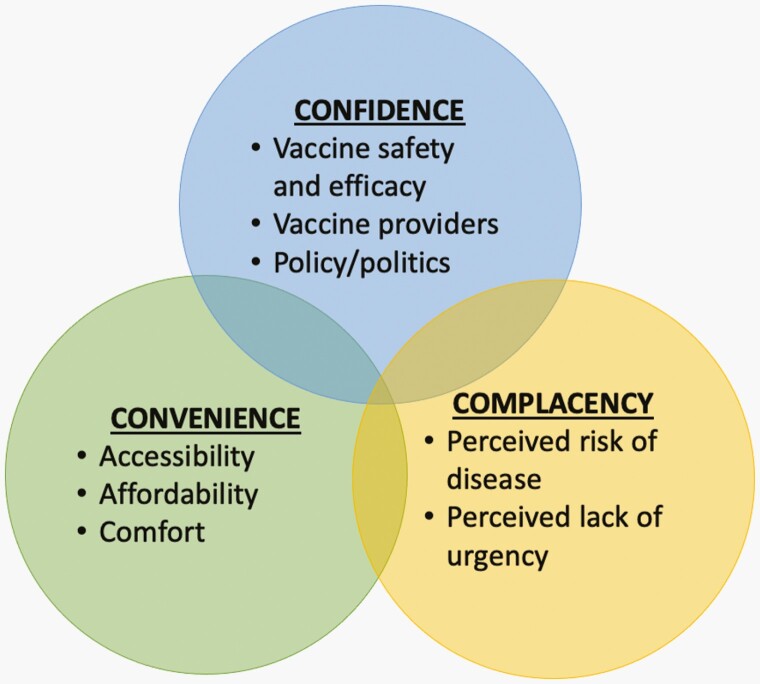
The decision-making process that results in an individual accepting a vaccine can be influenced by several factors. An intuitive conceptual model for understanding the determinants of vaccine uptake is the “3 C’s model,” which identifies complacency, convenience, and confidence as key contributors (Figure 1) [61]. In this model, hesitancy can result from a lack of confidence, or trust, in either the vaccine (ie, safety and efficacy), the vaccine providers (ie, health systems, clinicians, and investigators), or the public health officials mandating their use. Complacency can also influence the choice to get vaccinated and occurs when the individual perceives the risks of a given vaccine-preventable illness as low and thus considers immunization a non-essential or non-urgent task. Last, how convenient it is to get a vaccine can also affect uptake and is tied to its affordability and accessibility. In the subsequent section, we explore how these factors have contributed to the disparities in COVID-19 vaccine uptake and provide a sample of strategies that have strong evidence of support and can be used going forward to address these challenges (Table 1).
Figure 1.
Conceptual model for understanding the determinants of vaccine uptake.
Table 1.
Key Factors Contributing to Vaccine Inequities and Targeted Strategies to Increase Immunization
| Contributors to Inequity | Strategies |
|---|---|
| Confidence and vaccine research | • Invest in strategies to build trust in communities of color through increased transparency and accountability in vaccine research • Build networks of vaccine clinical trial sites in underserved communities • Improve diversity among pediatric investigators and clinicians • Partner with trusted voices in communities to disseminate vaccine messages and recommendations |
| Complacency and misinformation | • Ensure that messaging of risks and benefits of vaccines is evidence-based and sustains awareness of the seriousness of the disease • Engage community-based organizations and leaders to implement vaccine advocacy campaigns • Develop messaging strategies that are culturally relevant and incorporate communities’ beliefs and values • Address misinformation on social media with clear and brief corrections reinforcing with illustrations |
| Convenience and access | • Utilize community sites for vaccine clinics and mobile vaccine units with after work and weekend hours • Establish school-based immunization programs • Leverage partnerships with local government, health providers and community organizations to establish a vaccine-distribution network |
Trust and Equity in Vaccine Research
Vaccine hesitancy, largely centered around trust and confidence, has significantly contributed to COVID-19 vaccine disparities. In a recent study, investigators found that for both Black and Hispanics, confidence in the vaccine’s safety and effectiveness is the best predictor of expected uptake [62]. Additional factors that fuel mistrust and drive vaccine hesitancy include a lack of trust in institutions and pharmaceutical companies and inadequate representation of racial and ethnic groups in the vaccine development process [63, 64]. Building trust will require considerable investments in communities of color, increased transparency, and accountability across the spectrum, from vaccine development to its dissemination [65, 66].
If families within underrepresented racial/ethnic subgroups of the population are to believe in and accept the vaccines, studies that adequately represent children of racial and ethnic minority groups are an important first step. However, reaching the desired level of diversity in vaccine research is easier said than done. Systemic racism, decades of abuse, and a long history of unconsented research on people of color have engendered a deep-seated suspicion in clinical research and make it difficult for people of color to participate in vaccine trials [67]. The US Food and Drug Administration (FDA) has recently outlined a comprehensive plan to encourage clinical trial sponsors to pursue diversity more deliberately, which is a good starting point [68]. Going forward, investing in a network of clinical trial sites in underserved communities and diversifying the pool of investigators and support staff will be critical to bridging the gap between investigators and BIPOC participants.
Combating Misinformation and Disinformation
Another major hurdle in implementing widespread COVID-19 vaccination is misinformation and disinformation. The anti-vaccine movement is not a new phenomenon. However, there has been an acceleration in the spread of vaccine myths and disinformation in recent years, which has been amplified through social media [69–71]. Every day, individuals are flooded with information that might be confusing, contradictory, and sometimes intentionally deceptive [72, 73]. Though the intensity of the anti-vaccine movement has grown, studies have shown that its influence is not unsurmountable. During the smallpox eradication campaign, the robust anti-vaccine campaigns were overcome in large part due to public awareness of the severity of the disease [74]. Several approaches have been proposed for recognizing and addressing health-related misinformation [75]. Evidence suggests that when it comes to refuting misinformation on social media, simple and concise corrections coupled with visual representations tend to be the most effective [76]. Messaging emphasizing the significance of COVID-19 has also proven helpful and will likely be even more important after the incidence of COVID-19 declines and media interest fades. After the H1N1 influenza virus transitioned from a pandemic status to a “regular” seasonal infection, complacency, or reduced perception of illness severity, became one of the leading causes of vaccine hesitancy [77]. Thus, equity in COVID-19 immunization will not be successful unless there is a strategic and evidence-based communication plan. Messaging of the risks and benefits of the vaccines must not only be strongly grounded in evidence but also should be concise, and framed in a way that is easy to understand, culturally and linguistically relevant, and sensitive to the needs of the intended audience.
Who conveys information about the risks and benefits of vaccines is as essential as the content of the message itself. Studies have shown that a strong recommendation from a trustworthy source, like a pediatrician, can heavily influence a parent’s motivation to immunize their children [78, 79]. The recommendation to vaccinate is particularly potent when provided by a culturally concordant healthcare provider [80] or by a trusted messenger in the community, such as a faith leader [81]. Numerous studies have shown that a high degree of community support for vaccination has the capacity to shift parental attitudes around vaccinations [82, 83]. These studies further highlight the importance of continued efforts to diversify the pediatric workforce and how valuable it can be to engage community-based organizations to boost vaccine confidence and uptake.
Addressing Barriers to Vaccine Access
Decades of prejudice and disparate allocation of resources in certain communities have led to barriers that can make it more difficult for parents with limited resources to get their children immunized despite being willing to do so. Underprivileged parents, for example, may be unable to take time off from work to get their children immunized or may not have reliable access to the technology needed to navigate the appointment systems. Transportation insecurity is also a major barrier prevalent among those living below the poverty threshold or in rural settings [84, 85]. To reach children who might not otherwise have access to COVID-19 vaccines, it will be crucial to set up vaccine clinics in spaces where families regularly visit (eg, community spaces, local pharmacies, libraries, and community health facilities), at different times of day, including on weekends [86].
Several other strategies can be utilized to address some of these challenges. For example, school-based immunization programs, while not without challenges [87], have been a successful strategy for supplementing the medical home and raising vaccination rates [88]. Schools address various practical concerns and, given their reach, can be leveraged to address the issue of equity. Mobile vaccine units can also be used to immunize children who have limited access to pediatricians and that lack reliable transportation. This may be particularly effective at reaching children living in hard-to-reach rural communities, those not yet enrolled in school, or those who are homebound due to disabilities.
THE SUCCESSFUL IMMUNIZATION PROGRAM IN TRIBAL COMMUNITIES
Although there are many barriers to immunization that need to be overcome, they are not insurmountable. The success of the COVID-19 vaccination program among the AIAN community, whose uptake of other vaccines has historically been low [89], is cause for optimism. According to the CDC’s vaccine administration data, as of April 15, 2022, 72% of AIAN had received a COVID-19 vaccine [58]. In comparison, during the same period, only 48% of non-Hispanic Black and 53% of non-Hispanic White Americans had been immunized [58].
The high rates of COVID-19 infections, hospitalizations, and fatalities in AIAN communities certainly contributed, at least in part, to the increased demand for vaccination [90]. However, AIAN communities also led the way on several advocacy campaigns that undoubtedly boosted vaccine confidence. For example, because of the long history of mistrust in government-backed activities, tribal leaders were proactive about including their communities in the vaccine trials and addressed the concerns of distrust early on through effective messaging strategies [91]. They enlisted the help of trusted community members as vaccine advocates and engaged in messaging campaigns that incorporated the AIAN communities’ cultural values [92]. Much of their messaging focused on the importance of vaccines to protect their community, including the most vulnerable elders, rather than the individual [93]. Others incentivized immunization by requiring proof of immunization to participate in important cultural traditions, like sacred ceremonies [90]. Some tribes employed financial incentives to boost vaccination rates. For example, one tribe gave $2000 to any member who could provide immunization documentation [90]. The AIAN communities’ success in distributing the vaccine was equally impactful as their vaccine confidence campaigns. Tribal leaders engaged their community early on to assess potential barriers and facilitators to vaccine delivery and were able to effectively organize a multifaceted vaccine-distribution network that integrated local government, health providers (Indian Health Services), and community partners (eg, community centers, mobile clinics, casinos, schools) [90–93].
CONCLUSIONS
In sum, although the virus has unquestionably had far-reaching ramifications on all levels of our society, the greatest burden has been borne by the vulnerable and underrepresented communities. A disproportionate uptake of COVID-19 vaccinations may further fuel this trend. Adopting a health equity-centered approach to vaccine research, communication, and dissemination will be critical to addressing vaccine disparities and ensuring that the health benefits of the COVID-19 immunization program extend to all.
Notes
Financial Support. This work was supported, in part, by grants from the Robert Wood Johnson Foundation (to ERU) and the National Institutes of Health (NIH) K23AI159518 (to CRO) and K08AI151253 (to ERU). Contents are solely the responsibility of the authors and do not necessarily reflect the views of the Foundation or the NIH. No honorarium, grant, or other forms of payment was given to anyone to produce the manuscript.
Supplement sponsorship. This supplement was sponsored through a grant provided by Sanofi Pasteur.
Potential conflicts of interest. KAF is an employee of Merck Sharp & Dohme Corp., a subsidiary of Merck & Co., Inc., Kenilworth, NJ, USA, and may own stock or stock options in Merck & Co., Inc., Kenilworth, NJ, USA. The other authors have no conflicts of interest relevant to this article to disclose.
All authors have submitted the ICMJE Form for Potential Conflicts of Interest. Conflicts that the editors consider relevant to the content of the manuscript have been disclosed.
Contributor Information
Carlos R Oliveira, Department of Pediatrics, Section of Infectious Diseases and Global Health, Yale University School of Medicine, New Haven, CT, USA; Department of Biostatistics, Section of Health Informatics, Yale University School of Public Health, New Haven, CT, USA.
Kristen A Feemster, Vaccine Education Center, The Children’s Hospital of Philadelphia, Philadelphia, PA, USA; Department of Pediatrics, Division of Infectious Disease, University of Pennsylvania Perelman School of Medicine, Philadelphia, PA, USA.
Erlinda R Ulloa, Department of Pediatrics, University of California Irvine School of Medicine, Irvine, CA 92697, USA; Division of Infectious Diseases, Children’s Health of Orange County, Orange, CA 92868, USA.
REFERENCES
- 1.National Academies of Sciences, Engineering, and Medicine. https://www.ncbi.nlm.nih.gov/books/NBK425848/ Communities in Action: Pathways to Health Equity. [PubMed]
- 2.Centers for Disease Control and Prevention. https://www.cdc.gov/coronavirus/2019-ncov/covid-data/covid-net/purpose-methods.html Coronavirus Disease 2019 (COVID-19)-Associated Hospitalization Surveillance Network (COVID-NET).
- 3.Centers for Disease Control and Prevention. https://www.cdc.gov/nchs/data/vsrr/VSRR015-508.pdf Provisional Life Expectancy Estimates for 2020.
- 4.Centers for Disease Control and Prevention. https://www.cdc.gov/healthequity/racism-disparities/impact-of-racism.html Impact of Racism on our Nation’s Health.
- 5.American Academy of Pediatrics. https://www.aap.org/en/pages/2019-novel-coronavirus-covid-19-infections/children-and-covid-19-state-level-data-report/ Children and COVID-19: State-Level Data Report.
- 6. Buonsenso D, Munblit D, De Rose C, et al. Preliminary evidence on long COVID in children. Acta Paediatr 2021; 110:2208–11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Ashkenazi-Hoffnung L, Shmueli E, Ehrlich S, et al. Long COVID in Children: observations from a designated pediatric clinic. Pediatr Infect Dis J 2021; 40:e509–11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8. Fashina TP, Elijah P, Oliveira C.. Characteristics of post-acute sequelae of Covid-19 (PASC) in pediatrics. J Investig Med 2022; 70:977–1202. [Google Scholar]
- 9. Cooper DM, Zulu MZ, Jankeel A, et al. SARS-CoV-2 Acquisition and immune pathogenesis among school-aged learners in four diverse schools. medRxiv 2021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10. Leidman E, Duca LM, Omura JD, et al. COVID-19 Trends Among Persons Aged 0-24 Years - United States, March 1-December 12, 2020. MMWR Morb Mortal Wkly Rep 2021; 70:88–94. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Bailey LC, Razzaghi H, Burrows EK, et al. Assessment of 135794 pediatric patients tested for severe Acute Respiratory Syndrome Coronavirus 2 across the United States. JAMA Pediatr 2021; 175:176–84. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. Goyal MK, Simpson JN, Boyle MD, et al. Racial and/or ethnic and socioeconomic disparities of SARS-CoV-2 infection among children. Pediatrics. 2020; 146:e2020009951. [DOI] [PubMed] [Google Scholar]
- 13. Peaper DR, Murdzek C, Oliveira CR, Murray TS.. Severe acute respiratory syndrome coronavirus 2 testing in children in a large regional US health system during the coronavirus disease 2019 pandemic. Pediatr Infect Dis J 2021; 40:175–81. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14. Wang L, Berger NA, Kaelber DC, Davis PB, Volkow ND, Xu R.. COVID infection rates, clinical outcomes, and racial/ethnic and gender disparities before and after Omicron emerged in the US. medRxiv 2022. [Google Scholar]
- 15.Centers for Disease Control and Prevention. https://www.cdc.gov/coronavirus/2019-ncov/community/health-equity/racial-ethnic-disparities/disparities-hospitalization.html Disparities in COVID-19-Associated Hospitalizations.
- 16. Bixler D, Miller AD, Mattison CP, et al. SARS-CoV-2-associated deaths among persons aged <21 years—United States, February 12–July 31, 2020. MMWR Morb Mortal Wkly Rep 2020; 69:1324–9. [DOI] [PubMed] [Google Scholar]
- 17. Zirinsky E, Paintsil E, Oliveira CR.. The clinical epidemiology of coronavirus disease 2019 in children and adolescents mirrors the widening gap in healthcare disparities. Curr Opin Pediatr 2021; 33:281–5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Centers for Disease Control and Prevention. https://www.cdc.gov/nchs/fastats/health-insurance.htm Health Insurance Coverage.
- 19. Yu J, Perrin JM, Hagerman T, Houtrow AJ.. Underinsurance among children in the United States. Pediatrics 2022; 149:e2021050353. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Cohen RA, Cha AE, Terlizzi EP, Martinez ME.. Health insurance coverage: Early release of estimates from the National Health Interview Survey, 2021. National Center for Health Statistics; 2022. [Google Scholar]
- 21. Vilar-Compte M, Gaitan-Rossi P, Felix-Beltran L, Bustamante AV.. Pre-COVID-19 social determinants of health among Mexican migrants in Los Angeles and New York City and their increased vulnerability to unfavorable health outcomes during the COVID-19 pandemic. J Immigr Minor Health 2022; 24:65–77. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22. Zhou RA, Baicker K, Taubman S, Finkelstein AN.. The uninsured do not use the emergency department more-they use other care less. Health Aff (Millwood) 2017; 36:2115–22. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23. Shone LP, Szilagyi PG.. The State Children’s Health Insurance Program. Curr Opin Pediatr 2005; 17:764–72. [DOI] [PubMed] [Google Scholar]
- 24. Lindley MC, Shen AK, Orenstein WA, Rodewald LE, Birkhead GS.. Financing the delivery of vaccines to children and adolescents: challenges to the current system. Pediatrics 2009; 124(Suppl 5):S548–57. [DOI] [PubMed] [Google Scholar]
- 25. Hill HA, Yankey D, Elam-Evans LD, Singleton JA, Pingali SC, Santibanez TA.. Vaccination coverage by age 24 months among children born in 2016 and 2017 - National Immunization Survey-Child, United States, 2017-2019. MMWR Morb Mortal Wkly Rep 2020; 69:1505–11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26. Wolf J, Abzug MJ, Anosike BI, et al. Updated guidance on use and prioritization of monoclonal antibody therapy for treatment of COVID-19 in adolescents. J Pediatric Infect Dis Soc 2022; 11:117–85. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. Oliveira CR, Niccolai LM, Sheikha H, et al. Assessment of clinical effectiveness of BNT162b2 COVID-19 vaccine in US adolescents. JAMA Netw Open 2022; 5:e220935. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28. Chiotos K, Hayes M, Kimberlin DW, et al. Multicenter interim guidance on use of antivirals for children with coronavirus disease 2019/severe acute respiratory syndrome coronavirus 2. J Pediatric Infect Dis Soc 2021; 10:34–48. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29. Wolf J, Abzug MJ, Wattier RL, et al. Initial guidance on use of monoclonal antibody therapy for treatment of coronavirus disease 2019 in children and adolescents. J Pediatric Infect Dis Soc 2021; 10:629–34. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30. Gaffney A, Himmelstein DU, Woolhandler S.. COVID-19 and US health financing: perils and possibilities. Int J Health Serv 2020; 50:396–407. [DOI] [PubMed] [Google Scholar]
- 31. Hawkins D. Social Determinants of COVID-19 in Massachusetts, United States: an ecological study. J Prev Med Public Health 2020; 53:220–7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32. Yehia BR, Winegar A, Fogel R, et al. Association of race with mortality among patients hospitalized with coronavirus disease 2019 (COVID-19) at 92 US hospitals. JAMA Netw Open 2020; 3:e2018039. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.https://news.gallup.com/poll/309224/avoidcare-likely-covid-due-cost.aspx In U.S., 14% with likely COVID-19 to avoid care due to cost.
- 34.United States Census Bureau. https://www.census.gov/library/publications/2019/demo/p60-266.html Income and Poverty in the United States: 2018.
- 35.United States Census Bureau. https://www.census.gov/newsroom/press-releases/2021/income-poverty-health-insurance-coverage.html Income, Poverty and Health Insurance Coverage in the United States: 2020.
- 36. National Academies of Sciences E, Medicine. A Roadmap to Reducing Child Poverty. Washington, DC: The National Academies Press; 2019. [PubMed] [Google Scholar]
- 37. Page KR, Venkataramani M, Beyrer C, Polk S.. Undocumented U.S. immigrants and Covid-19. N Engl J Med 2020; 382:e62. [DOI] [PubMed] [Google Scholar]
- 38. Kim EJ, Kim T, Conigliaro J, Liebschutz JM, Paasche-Orlow MK, Hanchate AD.. Racial and ethnic disparities in diagnosis of chronic medical conditions in the USA. J Gen Intern Med 2018; 33:1116–23. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39. U.S. Department of Health and Human Services. Asthma and American Indians/Alaska Natives. https://minorityhealth.hhs.gov/omh/browse.aspx?lvl=4&lvlid=30#:~:text=In%202018%2C%20278%2C000%20American%20Indian,more%20likely%20to%20have%20asthma.
- 40.Centers for Disease Control and Prevention. https://www.cdc.gov/obesity/data/childhood.html Childhood Obesity Facts.
- 41.Centers for Disease Control and Prevention. https://www.cdc.gov/vitalsigns/childhood-asthma/index.html Asthma in Children.
- 42. Bullock A, Sheff K, Moore K, Manson S.. Obesity and overweight in American Indian and Alaska Native Children, 2006–2015. Am J Public Health 2017, 107(9):1502–1507. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43. Fernandes DM, Oliveira CR, Guerguis S, et al. Severe acute respiratory syndrome coronavirus 2 clinical syndromes and predictors of disease severity in hospitalized children and youth. J Pediatr 2021; 230:23–31 e10. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44. Cuevas AG, Reitzel LR, Adams CE, et al. Discrimination, affect, and cancer risk factors among African Americans. Am J Health Behav 2014; 38:31–41. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45. Paradies Y, Ben J, Denson N, et al. Racism as a determinant of health: a systematic review and meta-analysis. PLoS One 2015; 10:e0138511. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46. Forde AT, Sims M, Muntner P, et al. Discrimination and hypertension risk among African Americans in the Jackson Heart Study. Hypertension 2020; 76:715–23. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.U.S. Bureau of Labor Statistics. https://www.bls.gov/news.release/flex2.t01.htm Workers who could work at home, did work at home, and were paid for work at home, by selected characteristics, averages for the period 2017-2018.
- 48.University of California San Francisco. https://www.ucsf.edu/news/2020/05/417356/initial-results-mission-district-covid-19-testing-announced Initial Results of Mission District COVID-19 Testing Announced.
- 49. Webb Hooper M, Napoles AM, Perez-Stable EJ.. COVID-19 and racial/ethnic disparities. JAMA 2020; 323:2466–7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.U.S. Bureau of Labor Statistics. https://www.bls.gov/opub/mlr/2019/article/american-indians-and-alaska-natives-in-the-u-s-labor-force.htm American Indians and Alaska Natives in the U.S. labor force.
- 51. Woodworth KR, Moulia D, Collins JP, et al. The Advisory Committee on Immunization Practices’ interim recommendation for use of Pfizer-BioNTech COVID-19 vaccine in children aged 5-11 years - United States, November 2021. MMWR Morb Mortal Wkly Rep 2021; 70:1579–83. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52. Wallace M, Woodworth KR, Gargano JW, et al. The advisory committee on immunization practices’ interim recommendation for use of Pfizer-BioNTech COVID-19 vaccine in adolescents aged 12-15 years—United States, May 2021. MMWR Morb Mortal Wkly Rep 2021; 70:749–52. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53. Fleming-Dutra KE, Wallace M, Moulia DL, et al. Interim recommendations of the advisory committee on immunization practices for use of Moderna and Pfizer-BioNTech COVID-19 vaccines in children aged 6 months-5 years—United States, June 2022. MMWR Morb Mortal Wkly Rep 2022; 71:859–68. [DOI] [PubMed] [Google Scholar]
- 54. Olson SM, Newhams MM, Halasa NB, et al. Effectiveness of BNT162b2 vaccine against critical Covid-19 in adolescents. N Engl J Med 2022; 386:713–23. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55. Zambrano LD, Newhams MM, Olson SM, et al. Effectiveness of BNT162b2 (Pfizer-BioNTech) mRNA vaccination against multisystem inflammatory syndrome in children among persons aged 12–18 years—United States, July–December 2021. MMWR Morb Mortal Wkly Rep 2022; 71:52–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56. Fowlkes AL, Yoon SK, Lutrick K, et al. Effectiveness of 2-dose BNT162b2 (Pfizer BioNTech) mRNA vaccine in preventing SARS-CoV-2 infection among children aged 5-11 years and adolescents aged 12–15 years - PROTECT Cohort, July 2021–February 2022. MMWR Morb Mortal Wkly Rep 2022; 71:422–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57. Price AM, Olson SM, Newhams MM, et al. BNT162b2 protection against the Omicron variant in children and adolescents. N Engl J Med 2022; 386:1899–909. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.https://covid.cdc.gov/covid-data-tracker Centers for Disease Control and Prevention. COVID Data Tracker.
- 59.https://www.kff.org/coronavirus-covid-19/issue-brief/latest-data-on-covid-19-vaccinations-by-race-ethnicity/ Latest Data on COVID-19 Vaccinations by Race/Ethnicity.
- 60. Kulkarni AA, Desai RP, Alcala HE, Balkrishnan R.. Persistent disparities in immunization rates for the seven-vaccine series among infants 19-35 months in the United States. Health Equity 2021, 5(1):135–139. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61. MacDonald NE, Hesitancy SWGV.. Vaccine hesitancy: definition, scope and determinants. Vaccine 2015; 33:4161–4. [DOI] [PubMed] [Google Scholar]
- 62.https://www.covidcollaborative.us COVID Collaborative Survey: Coronavirus Vaccination Hesitancy in the Black and Latinx Communities.
- 63. Jamison AM, Quinn SC, Freimuth VS.. “You don’t trust a government vaccine”: Narratives of institutional trust and influenza vaccination among African American and white adults. Soc Sci Med 2019; 221:87–94. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64. Jimenez ME, Rivera-Nunez Z, Crabtree BF, et al. Black and Latinx community perspectives on COVID-19 mitigation behaviors, testing, and vaccines. JAMA Netw Open 2021; 4:e2117074. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65. Lee TH, McGlynn EA, Safran DG.. A framework for increasing trust between patients and the organizations that care for them. JAMA 2019; 321:539–40. [DOI] [PubMed] [Google Scholar]
- 66. Avni-Singer LR, Yakely A, Sheth SS, Shapiro ED, Niccolai LM, Oliveira CR.. Assessing sociodemographic differences in human papillomavirus vaccine impact studies in the United States: a systematic review using narrative synthesis. Public Health 2020; 178:137–50. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67. Thompson HS, Manning M, Mitchell J, et al. Factors associated with racial/ethnic group-based medical mistrust and perspectives on COVID-19 vaccine trial participation and vaccine uptake in the US. JAMA Netw Open 2021; 4:e2111629. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68. FDA. Diversity plans to improve enrollment of participants from underrepresented racial and ethnic populations in clinical trials guidance for industry. 2022. https://www.federalregister.gov/documents/2022/04/14/2022-07978/diversity-plans-to-improve-enrollment-of-participants-from-underrepresented-racial-and-ethnic
- 69. Hotez P. COVID vaccines: time to confront anti-vax aggression. Nature 2021; 592:661. [DOI] [PubMed] [Google Scholar]
- 70. Chou WS, Oh A, Klein WMP.. Addressing health-related misinformation on social media. JAMA 2018; 320:2417–8. [DOI] [PubMed] [Google Scholar]
- 71. Merchant RM, Asch DA.. Protecting the value of medical science in the age of social media and “Fake News”. JAMA 2018; 320:2415–6. [DOI] [PubMed] [Google Scholar]
- 72. Tollefson J. The race to curb the spread of COVID vaccine disinformation. Nature 2021. doi: 10.1038/d41586-021-00997-x [DOI] [PubMed] [Google Scholar]
- 73. Cryst E,, DiResta R,, Meyersohn L,, et al. Memes, magnets and microchips: narrative dynamics around COVID-19 vaccines. Stanford Digital Repository. Stanford Digital Repository 2022. [Google Scholar]
- 74. Saint-Victor DS, Omer SB.. Vaccine refusal and the endgame: walking the last mile first. Philos Trans R Soc Lond B Biol Sci 2013; 368:20120148. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75. Desai AN, Ruidera D, Steinbrink JM, Granwehr B, Lee DH.. Misinformation and disinformation: the potential disadvantages of social media in infectious disease and how to combat them. Clin Infect Dis 2022; 74(Suppl_3):e34–9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76. Zhang Y, Guo B, Ding Y, et al. Investigation of the determinants for misinformation correction effectiveness on social media during COVID-19 pandemic. Inf Process Manag 2022; 59:102935. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77. Schmid P, Rauber D, Betsch C, Lidolt G, Denker ML.. Barriers of influenza vaccination intention and behavior - a systematic review of influenza vaccine hesitancy, 2005–2016. PLoS One 2017; 12:e0170550. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78. Ignacio M, Oesterle S, Mercado M, et al. Narratives from African American/Black, American Indian/Alaska Native, and Hispanic/Latinx community members in Arizona to enhance COVID-19 vaccine and vaccination uptake. J Behav Med 2022; 24:1–13. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79. Crawshaw AF, Farah Y, Deal A, et al. Defining the determinants of vaccine uptake and undervaccination in migrant populations in Europe to improve routine and COVID-19 vaccine uptake: a systematic review. Lancet Infect Dis 2022; 22:e254–66. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80. Alsan M, Stanford FC, Banerjee A, et al. Comparison of knowledge and information-seeking behavior after general COVID-19 public health messages and messages tailored for black and latinx communities: a randomized controlled trial. Ann Intern Med 2021; 174:484–92. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81. Privor-Dumm L, King T.. Community-based strategies to engage pastors can help address vaccine hesitancy and health disparities in black communities. J Health Commun 2020; 25:827–30. [DOI] [PubMed] [Google Scholar]
- 82. Schoeppe J, Cheadle A, Melton M, et al. The Immunity Community: A Community Engagement Strategy for Reducing Vaccine Hesitancy. Health Promot Pract 2017; 18:654–61. [DOI] [PubMed] [Google Scholar]
- 83. Rossen I, Hurlstone MJ, Lawrence C.. Going with the grain of cognition: applying insights from psychology to build support for childhood vaccination. Front Psychol 2016; 7:1483. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84. Wolfe MK, McDonald NC, Holmes GM.. Transportation barriers to health care in the United States: findings from the National Health Interview Survey, 1997–2017. Am J Public Health 2020; 110:815–22. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85. Samuels RC, Ward VL, Melvin P, Macht-Greenberg M, Wenren LM, Yi J, Massey G, Cox JE.. Missed appointments: factors contributing to high no-show rates in an urban pediatrics primary care clinic. Clin Pediatr (Phila) 2015, 54(10):976–982. [DOI] [PubMed] [Google Scholar]
- 86.CDC. https://www.cdc.gov/vaccines/covid-19/planning/children/equity.html Equity in Childhood COVID-19 Vaccination.
- 87. Torres AR, Johnson NP, Ellingson MK, Hansen CE, Oliveira CR, Niccolai LM, Sheth SS.. State laws permitting adolescent consent to human papillomavirus vaccination and rates of immunization. JAMA Pediatr 2022, 176(2):203–205. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 88. Lindley MC, Boyer-Chu L, Fishbein DB, et al. Working Group on the Role of Schools in delivery of adolescent V: the role of schools in strengthening delivery of new adolescent vaccinations. Pediatrics 2008; 121(Suppl 1):S46–54. [DOI] [PubMed] [Google Scholar]
- 89. Li C, Douglas M, Zahidi R, Josiah Willock R, Caplan L, Baltrus P, Gillis E, Mack D, Gaglioti A.. Racial and ethnic disparities in H1N1 vaccine uptake in Medicaid: lessons learned for a COVID-19 vaccine rollout. Prev Med Rep 2021, 24:101588. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90. Foxworth R, Redvers N, Moreno MA, Lopez-Carmen VA, Sanchez GR, Shultz JM.. Covid-19 vaccination in American Indians and Alaska natives—lessons from effective community responses. N Engl J Med 2021; 385:2403–6. [DOI] [PubMed] [Google Scholar]
- 91. Haroz EE, Kemp CG, O’Keefe VM, et al. Nurturing innovation at the roots: the success of COVID-19 vaccination in American Indian and Alaska native communities. Am J Public Health 2022; 112:383–7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 92.https://www.nga.org/wp-content/uploads/2021/08/Alaska_Covid_Case_Study_Aug2021.pdf A Case Study of Alaska’s State and Tribal Nation Partnerships for COVID-19 Vaccination.
- 93.https://www.healthaffairs.org/do/10.1377/forefront.20210723.390196 Native Americans and COVID-19 Vaccine Hesitancy: Pathways Toward Increasing Vaccination Rates For Native Communities.