Abstract
The elimination of cervical cancer has been a priority of the World Health Organization since 2018. The number of these cancers induced by the human papillomavirus (HPV) could be drastically reduced through vaccination and regularly screening by Pap tests. Guidelines for cervical cancer screening apply to all women, including those who have sexual relations with women (WSW), as HPV can be transmitted during sex between two women. As far as we know, our study is the first that compare the Pap test rate between WSW and other women in France. We developed an 18-item questionnaire available on the internet for 15 days and finally analyzed the responses of 2032 women. Based on their responses about their self-definition of their sexual orientation and their sexual behavior, we classified them into three groups of women: exclusive WSW, mixed WSW, and non-WSW. For each question, we tested the statistical differences in responses between these three groups. Our study shows in a large sample representative of the French population that exclusive WSW undergo Pap tests significantly less often than either mixed WSW or non-WSW. Among the exclusive WSW, 28.9 % had never had a Pap test, compared with 9 % of the mixed WSW and 3.1 % of non-WSW (p < 0,001). The responses to our questionnaire contribute to an understanding of this disparity and thus help to envision solutions for better care of all women, regardless of their sexual orientation; this point is crucial for prevention of cervical cancer.
Keywords: WSW, Pap test, Cervical cancer, HPV, Gynecology
1. Introduction
Cervical cancer is a virus-induced cancer: the persistence of infection by high-risk human papillomaviruses (HPVs) induces first precancerous and then cancerous lesions in the cervix. Cervical cancer is one of the diseases against which we have effective weapons: vaccination against HPV for primary prevention and the Papanicolaou (Pap) test for secondary prevention. Despite these two weapons, the number of cases per year worldwide is expected to increase from 511,000 in 2018 to 700,000 in 2030 (World Health Organization, 2020). In the face of these and other alarming observations, the World Health Organization (WHO) declared the worldwide elimination of cervical cancer to be a public health priority in 2018 (Sauvaget and Weiderpass, 2019).
Until 2019, France conducted individual screening for cervical cancer. A Pap test was recommended every 3 years for women aged 25 to 65 years old. During the period of these guidelines, the incidence of cervical cancer incidence decreased drastically in France; the number of new cases fell from 3990 new cases in 1990 to 2920 cases in 2018, and mortality rate also fell markedly to 1117 deaths in 2018 (Hamers and Woronoff, 2019). Nonetheless this diminution began to slow down in 2005. Cervical cancer is one of the only cancers with a prognosis that is worsening in France (Barré et al., 2016); its 5-year survival rate is dropping. National uptake of the Pap test in France is inadequate. The Weekly Epidemiologic Bulletin (Bulletin Épidémiologique Hebdomadaire, BEH) estimates it at 58.7 % although it had previously been expected to reach 80 % (Hamers and Jezeweski-Serra, 2019). In comparison, in the UK, where 3197 cases of cancer and 854 deaths from cervical cancer were recorded in 2018 (Cancer Research UK, 2021), the organized screening of women aged 25–64 years has achieved an uptake of the Pap test over 72 % (National Health Service, 2020), with a downward trend over the last decade (National Health Service, 2021). As a reminder, organized screening is part of a screening campaign offered systematically to the entire population concerned, as opposed to individualized screening at the physician's initiative. It can be hypothesized that for an equal population size, organized screening has resulted in more cancers being detected and deaths avoided in the UK than in France.
In France, the reliance until 2019 on individual and not organized screening, except in several regions conducting pilot studies, created several disparities. This opportunistic screening produces geographical, social, and economic disparities affecting women in vulnerable situations including those from sexual minorities, such as women who have sexual relations with women (WSW) (Barré et al., 2016). Belonging, to a sexual minority is in itself a health determinant. A body of literature shows that being exposed to minority stress and experiencing situations of discrimination leads to more risky behaviors (Meyer, 2003, Lick et al., 2013). Although the French literature on the health of WSW is extremely sparse (Chetcuti et al., 2013), foreign publications report that these women are in poorer health than their non-WSW counterparts. For example, they consume more tobacco, alcohol, and anxiolytics, and they utilize health care less often (Gonzales and Henning-Smith, 2017). WSW also have several risk factors for cervical cancer (Cochran et al., 2001). At the same time, they seem to have a lower perception of their risk of cervical cancer and more reluctance to be screened (McNair, 2009)(Tracy et al., 2010), although we have known since the end of the 1990 s that HPV can be transmitted between two women (Marrazzo et al., 1998). Results of a recent study from the USA looking at cervical cancer screening in WSW suggests that WSW may have fewer Pap tests than other women (Agénor et al., 2017).
As far as we know, our study is the first study aimed at determining whether WSW have fewer Pap tests than other women in France. The secondary objective is to understand the determinants of this lower uptake.
2. Material and methods
2.1. Study design
The participants in our study were cisgender Frenchwomen whom we recruited to complete an internet questionnaire distributed by social networks, LGBT associations, and the investigator's network of acquaintances. We used snowball sampling, a method often used to study populations to whom it is normally difficult to gain access (Sadler et al., 2010, Meyer and Wilson, 2009).
The 18-item questionnaire was completed anonymously. It was hosted on the Nantes University Hospital Center's Sphinx site to protect the data. It was available for 15 days (from February 3–18, 2020) and enabled us to collect information from 3074 women. We hoped to recruit 150–300 WSW, who account for 5 %–10 % of the female population in France (L’Institut français d’opinion publique (IFOP), 2017, Bajos Nathalie, 2008).
The questionnaire responses were included in this study only if participants responded to all questions (except for one question, for which 6 answers were missing).
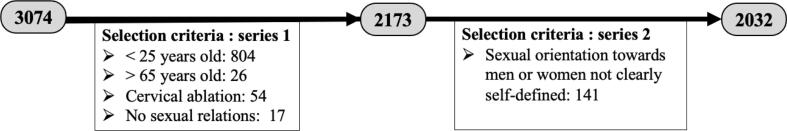
We considered only the women aged from 25 to 65 years, the age group for whom the Pap test is recommended. Women who had undergone cervical ablation were excluded because they are subject to a different screening regimen than the general population. Women who had never had sexual relations with either a man or woman were also excluded, as it is not recommended to use a speculum to examine them. Finally, among the 3074 women who completed the questionnaire, 2173 were included in the analysis after application of these criteria (Fig. 1).
Fig. 1.
Selection criteria used before analysis and number of individuals to whom they applied. Left: total number of women who completed the questionnaire. Right: total number of women included in this analysis after the application of 2 series of filters.
2.2. Measures
Our objective was to compare Pap test uptake between the WSW and the other women. We combined two criteria related to sexual behavior and self-definition to reliably define the WSW status reliably (Diamant et al., 1999); using only one of these two criteria can lead to more discordances as two studies have reported (Sell, 1997)(Shively et al., 1983). One question (n° 5) asked them if they considered themselves to be WSW. Another (n° 6) asked them if they had sex only with women, only with men, with more women than men, or with more men than women. Accordingly, based on their responses on these two dimensions, we classified them into three groups.
Thus, we called the group that both considered themselves WSW and had sex only with women exclusive WSW (n = 166) (Table 1). The group that considered themselves WSW and reported having sex with women and with men were called mixed WSW (n = 444). Finally, we labeled the women who responded both that they did not consider themselves WSW and that they had sex only with men non-WSW (n = 1422).
Table 1.
Distribution of respondents according to their questionnaire answers.
| WSW No | WSW Yes | Groups of women | |
|---|---|---|---|
| Relations with more men than women | 129δ | 220 | Mixed WSW 444 (20 %) |
| Relations with more women than men | 3δ | 224 | |
| Relations only with women | 4δ | 166 | Exclusive WSW166 (8 %) |
| Relations only with men | 1422 | 5δ | Non-WSW |
| 1422 (65 %) |
δWomen not included.
Table 2.
Comparison of the distribution of socioprofessional categories of the respondents compared with the general population.
| Study sample |
INSEE 2019 | p value | ||
|---|---|---|---|---|
| Number | % | % | ||
| Farmer (owner) | 4 | 0.2 | 0.8 | 0.22 |
| Tradesperson, shopkeeper, business owner | 69 | 3.4 | 3.9 | |
| Manager and self-employed professional + Intermediate professional** | 777 + nr | 38.2 + nr | 16.8 + 28.3 | |
| Office, sales, and service staff | 869 | 42.8 | 41.7 | |
| Blue-collar workers | 20 | 1 | 8.1 | |
| Not determined ** | Not reported | Not reported | 0.4 | |
| Retiree * | 28 | 1 | Not reported | |
| Student * | 167 | 8 | Not reported | |
| No occupation * | 98 | 5 | Not reported | |
* Category specific to our study;
** Category specific to INSEE;
nr = not reported́.
Because women whose answers did not allow us to classify them in one of these three groups were not included in the study (n = 141) (Fig. 1), the sample size of this analysis fell from 2173 to 2032 women.
Accordingly, we used these three groups — exclusive WSW, mixed WSW and non-WSW — as the independent variable with three modalities to explain the following 10 dependent variables: one related to the rate of pap test uptake (Supplementary Data, questionnaire, question 16), 7 related to knowledge and beliefs about the Pap test (Supplementary Data, questionnaire, questions 9–15), 2 related to the “reluctance” (Supplementary Data, questionnaire, questions 17 and 18). Note that question 18, “Why are you reluctant to have a pap test?”, was a multiple-choice question, the women could choose one or more answers and add free text if they wished. This question was only asked of women who had answered “yes” to the previous question: Are you reluctant to have a Pap test? (Question 17)”.
We received approval for this study from the Nantes Group for Ethics in Health (GNEDS).
2.3. Statistical analysis
A Chi-2 test was performed for each question to test the independence between the responses and the 3 groups of women considered. In the case of small numbers, we used Fisher’s exact test instead. The tests were considered significant when p < 0.05. The statistical analyses were performed with R software, version 3.6.
A multivariate analysis was performed to take into account specific confounding factors when they existed (residential zone and work in a medical setting) in the statistical analyses of the variable to be explained.
Supplementary Table 1 reports the numbers and percentages of the categorical variables characterizing the responders. We compared them with INSEE data, using a Chi-2 test.
3. Results
3.1. Population characteristics
We compared the participants' socioprofessional categories to those of the general population of women in France by using INSEE data from 2019 (Institut National Statistique et des Études Économiques (INSEE), 2019). Our sample is comparable to the general French population in terms of socioprofessional category. Women workers were nonetheless underrepresented in our study (1 % vs 8 % according to INSEE) (Table 2).
Next, we compared our three groups for four factors: age, socioprofessional category, place of residence, and work in a medical setting. The three groups were similar in age and socioprofessional category (Supplementary Table 1). They differed for work in a medical setting and in place of residence. That is, the highest proportion of women working in this setting was found in the non-WSW (45.8 %) group, compared with the exclusive WSW (27.1 %) and mixed WSW (29.5 %) groups. To overcome this bias, we created two subgroups defined by their work in a medical setting (yes/no) but otherwise similar for age and socioprofessional category (Supplementary Tables 2 and 3).
3.2. Rate of Pap test uptake
The group of exclusive WSW had significantly fewer Pap tests than both the mixed WSW and the non-WSW (p < 0.001): 28.9 % of the exclusive WSW had never had a Pap test, compared with 9 % of the mixed WSW and 3.1 % of non-WSW. Only 55.4 % of the exclusive WSW reported they were up to date in their Pap tests, versus 76.8 % of the mixed WSW and 90 % of the non-WSW (Table 3).
Table 3.
Performance of a PAP test.
| Exclusive WSW (N = 166) | Mixed WSW (N = 444) | Non-WSW (N = 1422) | Total (N = 2032) | p value | |
|---|---|---|---|---|---|
| Your last Pap test dates from: | < 0.001 | ||||
| I've never had one | 48 (28.9 %) | 40 (9.0 %) | 44 (3.1 %) | 132 (6.5 %) | |
| 3 years or less | 92 (55.4 %) | 341 (76.8 %) | 1280 (90.0 %) | 1713 (84.3 %) | |
| 4–6 years | 10 (6.0 %) | 42 (9.5 %) | 74 (5.2 %) | 126 (6.2 %) | |
| More than 6 years | 16 (9.6 %) | 21 (4.7 %) | 24 (1.7 %) | 61 (3.0 %) | |
The same gradient was found among women not working in a medical setting. Among the exclusive WSW, 56.2 % were up to date in their Pap test, 76 % of the mixed WSW, and 89.4 % of the non-WSW (p < 0.001).
Trends were similar for women working in medical settings; exclusive WSW were significantly (p < 0.001) less often up to date in their Pap tests (53.3 %) than those in the other groups: 78.6 % for the mixed WSW and 90.8 % for the non-WSW.
A multivariate analysis adjusted for work in a medical setting showed that the up-to-date Pap test remained significantly associated with sexual behavior (p < 0.001) (Supplementary Table 4 and Supplementary Fig. 1). A similar multivariate analysis adjusted for residential zone also showed that up-to-date Pap tests remained significantly associated with sexual behavior regardless of zone (p < 0.001) (Supplementary Table 5 and Supplementary Fig. 2).
Knowledge and beliefs about the Pap test.
The exclusive WSW group considered gynecologic care significantly less important than their overall medical care (21.7 % among exclusive WSW vs 5 % in non-WSW, p < 0.001) (question 8, Supplementary Table 6). At the same time, significantly more women in the exclusive WSW group did not answer the question about the purpose of the Pap test correctly (p < 0.001) (Question 9, Supplementary Table 7). Similarly, knowledge of the risk factors for cervical cancer tended (p = 0.055) to be poorer in the mixed and exclusive WSW groups (32.4 % to 33.1 %) than among non-WSW (38.1 %) (Question 13, Supplementary Table 8).
As for the recommendations for the Pap test (questions 10–12), the exclusive WSW answered these 3 questions significantly (p < 0.001) more inaccurately than the other groups. We found the same trend when we analyzed these answers by professional experience, medical setting or not. The non-WSW always knew more about these issues than the other groups (Supplementary Tables 10 and 11).
Among the exclusive WSW, 16.9 % considered a Pap test for WSW less useful than for other women, compared with 2 % of the non-WSW (p < 0.001) (Question 14, Supplementary Table 12). Question 20 asked about the risk of cervical cancer in WSW, and 27.7 % of the exclusive WSW thought they were at less risk than other women, versus 7.8 % of the non-WSW (p < 0.001) (Question 15, Supplementary Table 12).
3.3. Reluctance
The exclusive WSW were significantly more reluctant to undergo a Pap test than women in the other groups (p < 0.001): 58.2 % were reluctant versus 37.4 % of the mixed WSW and 19.9 % of the non-WSW (Table 4).
Table 4.
Reluctance to undergo a Pap test.
| Exclusive WSW (N = 166) | Mixed WSW (N = 444) | Non-WSW (N = 1422) | Total (N = 2032) | p value | |
|---|---|---|---|---|---|
| Are you reluctant to have a Pap test? | < 0.001 | ||||
| NA | 1 | 0 | 2 | 3 | |
| No | 69 (41.8 %) | 278 (62.6 %) | 1137 (80.1 %) | 1484 (73.1 %) | |
| Yes | 96 (58.2 %) | 166 (37.4 %) | 283 (19.9 %) | 545 (26.9 %) | |
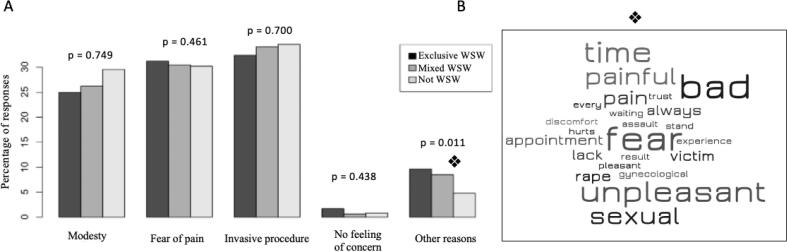
We asked a supplementary question (n° 18) to understand the reasons for this reluctance; these results are presented in Fig. 2. The answers of the three groups did not differ for the three proposed items, “Modesty”, Fear of pain” and “Invasive procedure”, the first cited by at least 25 % of responders and the other by at least 30 %, regardless of group. In contrast, the exclusive WSW and mixed WSW groups responded significantly more to the open response (p = 0.011). The word cloud associated with the answers of the 136 responders shows that the main words used by the responders are redundant with the previous closed questions (Fear, Unpleasant, Bad, Painful, Pain). We note among the answers some new words as “Time” and less frequently “Victim” and “Rape” (3 responders).
Fig. 2.
Reasons for reluctance to have a Pap test: Legend: A. Barplot representing the percentage of answers per group (Exclusive WSW/Mixed WSW/Not WSW) for the different possible responses of question 18. B Wordcloud for the responses (136 responders) to the “other reasons” open question. Words that appear at least twice in the answers are represented.
4. Discussion
This study, conducted in France among 2032 women, shows that WSW are significantly less often up to date in their Pap test than non-WSW, that is, the women who have sexual relations only with men (55.4 % vs 90.0 %). This finding did not change regardless of whether women worked or had worked in a medical setting. A cross-sectional study of a sample of 269 WSW in New York by Kerker et al., published in 2006, also found this large difference; 66 % of the WSW were up to date, somewhat higher than in our study, versus 88 % of the non-WSW (Kerker et al., 2006). A more recent study published in 2017 by Agénor et al. analyzed a sample of 11,300 US women (Agénor et al., 2017). The authors showed a significant difference in Pap test uptake in the preceding 3 years between the women we defined as non-WSW and as exclusive WSW (90.5 % vs 46.6 %). The exclusive WSW in our study reported that they had never had a Pap test more often than those also sexually active with men (mixed WSW): 28.9 % versus 9.0 %, respectively. These figures were also found in a study published in 2000 by Bailey et al., in which 42 % of the exclusive WSW had never had a Pap test versus 12 % of mixed WSW (Bailey et al., 2000). Thus, the fact that a woman had sexual relations with a man appears to influence her cervical cancer screening behavior.
Various reasons might explain this difference in rates between WSW and other women. We are going to try to analyze some of them in the light of our results. The most evident reason is the higher rate of reluctance about Pap tests expressed by WSW: 58.2 % of exclusive WSW, 37.4 % of mixed WSW, and 19.9 % of non-WSW.
The finding that of gap in expressed reluctance between the three groups was also found among women working in medical settings suggests that awareness of health issues does not really have an effect on the higher rate of reluctance about Pap tests. The responses to question 18 indicate that the main reasons for this reluctance (modesty, fear of pain, invasive procedure) are the same in the 3 groups of women, regardless of their sexual orientation (Supplementary Fig. 2). At the same time, we note that the WSWs responded significantly more frequently in free text. These results highlight two points. First, WSWs seem to have taken more advantage of this opportunity to express their reticence, emphasizing the issue of their invisibility in the health field (Daley, 1998). Second, pain seems to be a cause for reluctance shared by all women. Although little studied in the literature, this point appears to be a crucial one to investigate to improve women's adherence to screening. An exhaustive consideration of patient reluctance requires taking other elements into account as well. For example, many studies show that WSW internalize biases such as internalized homophobia and fear of discrimination when they reveal their sexual orientation (Hirsch et al., 2016, Bjorkman and Malterud, 2009). The minority stress model, developed by several authors (Meyer, 2003, Lick et al., 2013), is a further explanation of reluctance to undergo a Pap test and contributes to health disparities in general.
Women's knowledge of this test appears globally poor; they seem to be unaware of its utility and value, of the risk factors for cervical cancer, and of the guidelines for this preventive test. Our study showed that WSW had significantly less knowledge about the Pap test than the non-WSW, regardless of whether they worked in medical or non-medical settings. It may be explained in part by their lack of attention to their gynecologic care. That is, around four times as many exclusive WSW than the non-WSW in our study reported thinking that their gynecologic care is unimportant. This could be due to their lower rate of use of such gynecologic care as contraception and pregnancy-related care compared to that of other women.
Moreover, the WSW in our study misperceived their risk of developing cervical cancer and their need for screening by Pap tests. The results of the study by Bailey et al. were similar: 22 % of the women defining themselves as lesbians thought they needed Pap tests less than other women (Bailey et al., 2000). This belief was associated with their screening practices.
Healthcare professionals in general and physicians in particular have an essential role in providing information and thus in preventing cervical cancer. Several studies have already described erroneous recommendations to women that they did not need Pap tests (Marrazzo et al., 2001). These inaccurate recommendations are probably due, at least in part, to a heteronormative professional training that mentioned sexual minorities very little if at all, although WSW may account for up to 10 % of French women. Physicians' lack of awareness on this topic is unfortunate as disclosing sexual orientation to providers was positively associated with cervical cancer screening (Greene et al., 2018). Understanding that sexual orientation is a real health determinant can encourage doctors to pay more attention to it.
WSW need to receive the same screening by Pap tests as other women. The transmission of HPV between women has been established for several years (Marrazzo et al., 1998, Marrazzo et al., 2001). Case reports have described high-grade cervical HPV lesions in WSW who have never had sexual relations with men (Anderson et al., 2014). Moreover, their partners might previously have had sexual relations with men. WSW also have several risk factors for developing cervical cancer: they smoke more (Boehmer et al., 2012), they are at higher risk of STIs such as Chlamydiae (Singh et al., 2011), their age at first sexual relations is earlier than among women who have sexual relations only with men (16.8 vs 18.5 years) (Lhomond and Saurel-Cubizolles, 2003), and mixed WSW have more different lifetime partners than non-WSW (Fethers et al., 2000, Oswalt and Wyatt, 2013).
The lack of representation of WSW in screening campaigns is another important element to consider. Moreover, it could be interesting to target these campaigns even more specifically at women with additional vulnerabilities. Indeed, authors who have studied intersectionality theory have shown that access to screening is even more limited for certain subgroups of WSW (Greene et al., 2019). This type of study could be enriched in the future by addressing ethnicity and race for example.
This report is, to our knowledge, the first quantitative study in France to compare Pap test uptake between WSW and other women. Our use of social networks and the snowball method enabled us to obtain a large number of responses to our questionnaire (N = 3074) in 15 days. This method is used when seeking to include individuals with specific characteristics, such as a sexual minority, in a study. This large number of participants allowed us to recruit women in various occupational categories, representative of the general population, as shown by comparing them with the INSEE 2019 report. Women blue-collar workers are nonetheless underrepresented.
Other biases must be pointed out. First there is a selection bias. The distribution of a computerized questionnaire by social networks limited inclusion to women with internet access and belonging to social networks. These points explain why our population is globally young: 85 % of the women were aged between 25 and 45 years, with a high proportion of students. Moreover, we can suppose that women drawn to this topic were more likely to complete our questionnaire. We might therefore, despite our efforts, have selected women more interested in their health than most. Nonetheless, this means of questionnaire distribution seemed essential to us to be able to recruit the maximum number of participants.
Confounding biases must also be taken into account. The date of the last Pap test was self-reported, a method that tends to overestimate the real rate of cervical cancer screening by Pap tests among these women.
Overall, 827 women among 2032 participants worked in a medical setting, that is, 40 % of our sample. We might have supposed that women working in such an environment would have better knowledge about Pap tests and would be more up to date with this preventive care. Our questionnaire used the term “medical setting”, which actually covers a very heterogeneous population in terms of occupations and qualifications. A more precise term would have been desirable. Consequently, to avoid any confounding bias, we excluded these women from the analysis of some questions. We also performed a multivariate analysis adjusted for working in the medical setting to avoid this confounding bias. As a reminder, a smaller proportion of WSW than other women, regardless of whether they worked in a medical setting, were up to date with their Pap tests.
Another difficulty of conducting a study of WSW is the definition of WSW. This group is not homogeneous. Because every survey may use somewhat different criteria to define them, comparison between studies can be difficult.
There also appears to be a chronological association between sexual orientation and health care pathway that must be taken into account to avoid confounding biases (Meyer and Wilson, 2009). In a recent French study, for example, some respondents explained that they stopped having regular Pap tests once they started having sex only with women (Mitrochine, 2020). Nonetheless, our questionnaire did not ask about this data item.
5. Conclusion
Our study shows that French WSW suffer from a severe lack of cervical cancer screening by Pap tests. One reason for this is the lack of awareness among health professionals that patients' sexual orientation is a real health determinant. In addition, the reluctances of WSW to have a Pap test and their lesser knowledge than other women on this subject are important obstacles that need to be studied in greater depth in order to identify areas for improvement. The deployment of organized cervical cancer screening allows us to hope that national Pap test screening uptake will grow in France in the years to come. Nonetheless, to reach the WSW population better, these organized screening methods should be combined with campaigns targeting WSW and the results should be re-evaluated in a few years.
Declaration of Competing Interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Acknowledgments
The authors thank the translator, Ms CAHN Jo Ann.
Footnotes
Supplementary data to this article can be found online at https://doi.org/10.1016/j.pmedr.2022.101990.
Appendix A. Supplementary data
The following are the Supplementary data to this article:
Data availability
Data will be made available on request.
References
- Agénor M., Muzny C.A., Schick V., Austin E.L., Potter J. Sexual orientation and sexual health services utilization among women in the United States. Prev. Med. 2017;95:74–81. doi: 10.1016/j.ypmed.2016.11.023. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Anderson T.A., Schick V., Herbenick D., Dodge B., Fortenberry J.D. A study of human papillomavirus on vaginally inserted sex toys, before and after cleaning, among women who have sex with women and men. Sex. Transm. Infect. 2014;90:529–531. doi: 10.1136/sextrans-2014-051558. [DOI] [PubMed] [Google Scholar]
- Bailey J.V., Kavanagh J., Owen C. Lesbians and cervical screening. Br. J. Gen. Pract. 2000;50:481–482. [PMC free article] [PubMed] [Google Scholar]
- Bajos Nathalie, B.M., 2008. Enquête sur la sexualité en France : Pratiques, genre et santé, La Découverte. ed, Hors Collection Social.
- Barré S., Massetti M., Leleu H., Catajar N., de Bels F. Caractérisation des femmes ne réalisant pas de dépistage du cancer du col de l’utérus par frottis cervico-utérin en France. Bull. Epidémiol. Hebdomadaire. 2016:39–47. [Google Scholar]
- Bjorkman M., Malterud K. Lesbian women’s experiences with health care: A qualitative study. Scand. J. Prim. Health Care. 2009:238–239. doi: 10.3109/02813430903226548. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Boehmer U., Miao X., Linkletter C., Clark M.A. Adult health behaviors over the life course by sexual orientation. Am. J. Public Health. 2012;102:292–300. doi: 10.2105/AJPH.2011.300334. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cancer Research UK, 2021. Cervical cancer incidence statistics | Cancer Research UK [WWW Document]. Cancer Research UK. URL https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/cervical-cancer/incidence#heading-Zero.
- Chetcuti N., Beltzer N., Methy N., Laborde C., Velter A., Bajos N., Group Preventive Care’s forgotten women: life course, sexuality, and sexual health among homosexually and bisexually active women in France. J. Sex Res. 2013;50:587–597. doi: 10.1080/00224499.2012.657264. [DOI] [PubMed] [Google Scholar]
- Cochran S.D., Bowen D., Gage S. Cancer-related risk indicators and preventive screening behaviors among lesbians and bisexual women. Am. J. Public Health. 2001;91(4):591–597. doi: 10.2105/ajph.91.4.591. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Daley A. Lesbian invisibility in health care services: heterosexual hegemony and strategies for change. Can. Soc. Work Rev. 1998;15:57–71. [Google Scholar]
- Diamant A.L., Schuster M.A., McGuigan K., Lever J. Lesbians’ sexual history with men: implications for taking a sexual history. Arch. Intern. Med. 1999;159:2730–2736. doi: 10.1001/archinte.159.22.2730. [DOI] [PubMed] [Google Scholar]
- Fethers K., Marks C., Mindel A., Estcourt C.S. Sexually transmitted infections and risk behaviours in women who have sex with women. Sex Transm. Inf. 2000:5. doi: 10.1136/sti.76.5.345. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gonzales G., Henning-Smith C. Health disparities by sexual orientation: results and implications from the behavioral risk factor surveillance system. J. Community Health. 2017;42:1163–1172. doi: 10.1007/s10900-017-0366-z. [DOI] [PubMed] [Google Scholar]
- Greene M.Z., Meghani S.H., Sommers M.S., Hughes T.L. Health care-related correlates of cervical cancer screening among sexual minority women: an integrative review. J. Midwifery Women’s Health. 2018;63:550–577. doi: 10.1111/jmwh.12872. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Greene M.Z., Hughes T.L., Hanlon A., Huang L., Sommers M.S., Meghani S.H. Predicting cervical cancer screening among sexual minority women using Classification and Regression Tree analysis. Prevent. Med. Rep. 2019;13:153–159. doi: 10.1016/j.pmedr.2018.11.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hamers F.F., Jezeweski-Serra D. Couverture du dépistage du cancer du col de l’utérus en France, 2012–2017. Bull. Epidémiol. Hebdomadaire. 2019:417–423. [Google Scholar]
- Hamers F.F., Woronoff A.-S. Cancer du col de l’utérus en France : Tendances de l’incidence et de la moralité jusqu’en 2018. Bull. Epidémiol. Hebdomadaire. 2019;22–23:7. [Google Scholar]
- Hirsch O., Löltgen K., Becker A. Lesbian womens’ access to healthcare, experiences with and expectations towards GPs in German primary care. BMC Fam. Pract. 2016;17:162. doi: 10.1186/s12875-016-0562-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kerker B.D., Mostashari F., Thorpe L. Health care access and utilization among women who have sex with women: sexual behavior and identity. J. Urban Health. 2006;83:970–979. doi: 10.1007/s11524-006-9096-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- L’Institut français d’opinion publique (IFOP), 2017. To Bi or not to Bi ? Enquête sur l’attirance sexuelle entre femmes.
- Lhomond, B., Saurel-Cubizolles, M.-J., 2003. Orientation sexuelle, violences contre les femmes et santé. Homosexualités au temps du sida pp. 107–130.
- Lick D.J., Durso L.E., Johnson K.L. Minority stress and physical health among sexual minorities. Perspect. Psychol. Sci. 2013;8:521–548. doi: 10.1177/1745691613497965. [DOI] [PubMed] [Google Scholar]
- Marrazzo J.M., Koutsky L.A., Stine K.L., Kuypers J.M., Grubert T.A., Galloway D.A., Kiviat N.B., Handsfield H.H. Genital human papillomavirus infection in women who have sex with women. J. Infect. Dis. 1998;178:1604–1609. doi: 10.1086/314494. [DOI] [PubMed] [Google Scholar]
- Marrazzo J.M., Koutsky L.A., Kiviat N.B., Kuypers J.M., Stine K. Papanicolaou test screening and prevalence of genital human papillomavirus among women who have sex with women. Am. J. Public Health. 2001;91:947–952. doi: 10.2105/ajph.91.6.947. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McNair R. Lesbian and bisexual women’s sexual health. Aust. Fam. Phys. 2009;38:388–393. [PubMed] [Google Scholar]
- Meyer I.H. Prejudice, social stress, and mental health in lesbian, gay, and bisexual populations. Concept. Issues Res. Evid. 2003;39 doi: 10.1037/0033-2909.129.5.674. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Meyer I.H., Wilson P.A. Sampling lesbian, gay, and bisexual populations. Journal of Counseling Psychology. 2009;56:23–31. doi: 10.1037/a0014587. [DOI] [Google Scholar]
- Mitrochine M. Bordeaux; UFR des sciences médicales: 2020. Facteurs lié à la réalisation du frottis cervico-utérin chez les femmes ayant des relations sexuelles avec des femmes en France (Thèse d’exercice) [Google Scholar]
- National Health Service, 2020. Cervical Screening Programme, England - 2019-20 [NS] [WWW Document]. NHS Digital. URL https://digital.nhs.uk/data-and-information/publications/statistical/cervical-screening-annual/england---2019-20.
- National Health Service, 2021. Cervical Screening Programme, England - 2020-21 [NS] [WWW Document]. NHS Digital. URL https://digital.nhs.uk/data-and-information/publications/statistical/cervical-screening-annual/england--2020-2021 (accessed 9.8.22).
- Oswalt S.B., Wyatt T.J. Sexual health behaviors and sexual orientation in a U.S. national sample of college students. Arch. Sex. Behav. 2013;42:1561–1572. doi: 10.1007/s10508-012-0066-9. [DOI] [PubMed] [Google Scholar]
- Sadler G.R., Lee H.-C., Seung-Hwan Lim R., Fullerton J. Recruiting hard-to-reach United States population sub-groups via adaptations of snowball sampling strategy. Nurs. Health Sci. 2010;12:369–374. doi: 10.1111/j.1442-2018.2010.00541.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sauvaget C., Weiderpass E. Eradication du cancer du col utérin : une priorité de santé publique. Bull. Epidémiol. Hebdomadaire. 2019:408–409. [Google Scholar]
- Sell R.L. Defining and measuring sexual orientation: a review. Arch. Sex. Behav. 1997;26:643–658. doi: 10.1023/a:1024528427013. [DOI] [PubMed] [Google Scholar]
- Shively M.G., Jones C., De Cecco J.P. Research on sexual orientation: definitions and methods. J. Homosex. 1983;9:127–136. doi: 10.1300/j082v09n02_08. [DOI] [PubMed] [Google Scholar]
- Singh D., Fine D.N., Marrazzo J.M. Chlamydia trachomatis infection among women reporting sexual activity with women screened in family planning clinics in the pacific northwest, 1997 to 2005. Am. J. Public Health. 2011;101:1284–1290. doi: 10.2105/AJPH.2009.169631. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Institut National Statistique et des Études Économiques (INSEE), 2019. Catégorie socioprofessionnelle selon le sexe et l’âge | Insee [WWW Document]. Insee.fr. URL https://www.insee.fr/fr/statistiques/2489546#tableau-figure1.
- Tracy J.K., Lydecker A.D., Ireland L. Barriers to cervical cancer screening among lesbians. J. Womens Health (Larchmt) 2010;19:229–237. doi: 10.1089/jwh.2009.1393. [DOI] [PMC free article] [PubMed] [Google Scholar]
- World Health Organization, 2020. A cervical cancer-free future: First-ever global commitment to eliminate a cancer [WWW Document]. URL https://www.who.int/news/item/17-11-2020-a-cervical-cancer-free-future-first-ever-global-commitment-to-eliminate-a-cancer.
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
Data will be made available on request.