Summary
In the last decades, clinical neuroscience found a novel ally in neurotechnologies, devices able to record and stimulate electrical activity in the nervous system. These technologies improved the ability to diagnose and treat neural disorders. Neurotechnologies are concurrently enabling a deeper understanding of healthy and pathological dynamics of the nervous system through stimulation and recordings during brain implants. On the other hand, clinical neurosciences are not only driving neuroengineering toward the most relevant clinical issues, but are also shaping the neurotechnologies thanks to clinical advancements. For instance, understanding the etiology of a disease informs the location of a therapeutic stimulation, but also the way stimulation patterns should be designed to be more effective/naturalistic. Here, we describe cases of fruitful integration such as Deep Brain Stimulation and cortical interfaces to highlight how this symbiosis between clinical neuroscience and neurotechnology is closer to a novel integrated framework than to a simple interdisciplinary interaction.
Subject areas: Clinical neuroscience, Bioelectronics
Graphical abstract

Clinical neuroscience; Bioelectronics
Introduction
The history of clinical neuroscience unfolds across the millennia, with brain injuries and their treatment being notably the first topic treated in the Edwin Smith Papyrus describing surgical procedures used in the Ancient Egypt and dating approximately 1600 BC (Moore, 2011). In the following centuries, clinical neuroscience used a very broad range of tools to explore the dynamics of the nervous system and to fix its dysfunctions. New therapeutic and surgical approaches have been developed to address different types of neurological issues. Each in turn led to a better neuroscientific understanding of the human brain, which again fostered novel concepts for neuromodulation.
After the groundbreaking intuition of Luigi Galvani that electricity was the driving force of the nervous system (Piccolino, 1998), the scientific and technological progress achieved during the 19th and 20th centuries allowed the development of new electrical tools. In particular, electrodes for recording and stimulating the activity of the neurons could be used to probe and understand how the nervous system works (Table 1). These kinds of tools can be broadly referenced as neurotechnologies, and they started having a prominent role in clinical neuroscience. Among the pioneers we can cite the electroencephalographic recordings of Hans Berger (Haas, 2003) and the electroconvulsive therapies of Ugo Cerletti (1950).
Table 1.
Main types of electrodes for recording/stimulating central nervous system
| Type | Technical characteristics | Application |
|---|---|---|
| Deep-brain stimulation (DBS) leads | 1–2 mm thick probes with several ∼1 mm long electrodes. | Stimulation and recording from subcortical structures. |
| Microelectrodes recordings (MER) leads | Thin probes with a single recording contact in the μm scale. | MER are acquired intraoperatively at different depths. Compared to recordings done through DBS leads, MER allows a more localized characterization of activity. |
| Microelectrode arrays (MEAs) | Tens to hundreds of ∼1 mm long electrodes with diameters of some μm densely packed in rectangular arrays. | Cortical recordings and intracortical microstimulation (ICMS). ICMS differs from DBS in that ICMS delivers a targeted electrical stimulation through MEAs at the cortical level, whereas DBS lead stimulate larger volumes of subcortical structures. |
| Stereo-electroencephalography (SEEG) leads | Depth electrodes with ∼1 mm diameter and tens of contacts in the mm scale. | Stimulation and recording from cortical and subcortical structures. |
| Electrocorticography (ECoG) grids | 64 to 128 electrodes with a diameter of some mm and spaced apart ∼1 cm. | Recording from the cortical surface. |
Neurotechnologies have been developed in the past 40 years with the crucial help of clinical neuroscientists to restore sensory (House, 1976), motor (Micera et al., 2020) and recently cognitive functions (Roelfsema et al., 2018). Indeed, clinical neuroscience has always been and must be the key driver for the development of neurotechnology, but at the same time, neurotechnology can not only support clinical practice by leading to treatments, but also support clinical neuroscience by shedding light on how neural activity shapes our behavior (Figure 1).
Figure 1.
Interplay between clinical neuroscience and neurotechnology
Representative scheme of the positive feedback loop between neurotechnology and clinical neuroscience.
The field of functional neurosurgery is a prime example of this idea. Out of medical necessity (i.e., significant burden of disease without alternative therapeutic options), patients consensually undergo procedures that would be otherwise unthinkable in humans (e.g., open skull surgery). From a scientific perspective, this opens a unique window of opportunity to record directly from the brain, and to focally stimulate it by delivering weak electrical pulses. In their famous “final summary and discussion” about the brain’s responses to auditory and visual experience following electric stimulation of the cortex, Wilder Penfield and Phanor Perot wrote:
“…it is fair to say that, over the years, every accessible part of the cortical mantle of the two hemispheres has been subjected to stimulation at one time or another”. (Penfield and Perot, 1963)
In other words, the authors meant that since the foundation of the Montreal Neurological Institute in 1934 until the retirement of Wilder Penfield in 1960, his team had direct access to most if not all parts of the cortical mantle. They used this opportunity to probe responses of awake surgical patients (most often operated because of treatment refractory or drug-resistant epilepsy) after modulating small portions (∼1.5 mm2 in size) with 200–500 μs pulses delivered at 40–100 Hz with a stimulation amplitude of around 0.5 mA (Penfield and Perot, 1963).
Along a similar vein, modern-day neurosurgeons have been associated with the quote “No neuron is safe” (Ponce et al., 2018), indicating that one time or the other, each part of the brain could become, and has been, subject to electrical stimulation. Among the many insights that the Penfield team has brought us, one of the most salient ones is arguably the homunculus of the motor and sensory cortices. Famously described by Penfield and Rasmussen in 1950, these maps have refined our knowledge of human anatomy, with a reproducible pattern of somatotopic segregation of primary motor and sensory cortices that by size map to importance of sensorimotor functions (Penfield and Rasmussen, 1950). Because fingers and hands are needed to carry out fine motor skills, their regions on M1 and S1 are comparably large, with the trunk region – huge on the body – comparing to the same size of the one attributed to the ring-finger.
In the following sections of this review, we will follow the inspiration of these seminal works and we will illustrate the interplay between clinical neuroscience and neurotechnology focusing on two of the main neurotechnologies for the central nervous system (CNS): deep brain stimulation to subcortical structures and cortical brain machine interfaces.
Understanding and restoring motor control through deep brain stimulation
The use of deep brain stimulation (DBS) (Figures 2A and 2B) to mitigate the symptoms of motor disorders (Lozano et al., 2019) could be seen as both one of the most effective neurotechnologies developed to alleviate clinical symptoms, and as an invaluable method to explore the dynamics relating neural activity and behavior in the human brain. The first input was from clinical neurosurgery to neurotechnology: tests of electrical stimulation preceding surgical ablation led to the idea of a DBS therapy (Cooper et al., 1980). This therapy was initially grounded only on phenomenological observation of motor symptoms suppression (Montgomery, 2017) (although later refined on the ground of physiological studies) but later the neurotechnology provided clinical neuroscience with rich datasets on neural circuitry dysfunctions (Lozano et al., 2019). Clinical neuroscience integrated these functional studies with molecular and anatomical studies to advance the understanding of the pathological circuital dynamics underlying motor disorders, and this in turn allowed advancements in the neurotechnology such as adaptive DBS (aDBS) (Meidahl et al., 2017). This movement from clinical neuroscience to neurotechnologies and back and back again is highly representative of the symbiosis between the two fields (Figure 2C).
Figure 2.
Deep-brain stimulation and basal ganglia neuroscience
(A) Reconstruction of bilateral directional deep brain stimulation (DBS) electrodes (model Boston Scientific Cartesia) implanted to the subthalamic nucleus (orange), view from right posterior. The right electrode shows a stimulation volume (red) steering the current toward the target nucleus. Small white arrows surrounding the right electrode depict the magnitude and direction of the electric field generated by a 3mA anodal stimulation. Internal (green) and external (blue) pallidum and subthalamic nucleus (STN) defined by the DISTAL atlas (Ewert et al., 2018). The backdrop shows a section of the 100um postmortem brain template (Edlow et al., 2019).
(B) Schematic illustration of the volume of tissue activated by a DBS electrode in the STN (putative functional divisions are represented). Active contacts (displayed in white) generate electric fields of decaying intensity (high in red, medium in orange, low in yellow and threshold in dashed black). Eddy currents that diffuse from the target regions are represented as radial black arrows. From (Vissani et al., 2020).
(C) Positive feedback loop between DBS neurotechnologies (left) and associated advancements in the understanding of neural underpinnings of motor control and cognitive brain disorders (right). LFPs: local field potentials. Pink areas in the inset identifies basal ganglia.
Deep brain stimulation and mapping of subcortical structures
Pioneered already in 1948 by stimulating the caudate nucleus in a patient with Parkinson’s disease with the aim of alleviating psychiatric symptoms (Pool, 1954), the breakthrough of DBS came after the success of the Grenoble group to treat motor diseases in the 1990s (Benabid et al., 1991; Limousin et al., 1995). Non-surprisingly, DBS was used to probe and study the brain as a by-product of therapy soon thereafter.
Mirroring the work of Penfield in subcortical structures, for instance, the Montpellier group used DBS to the pallidum to map its homuncular structure in 19 patients with dystonia – a neurological disorder characterized by involuntary muscle contractions that cause abnormal movements or postures (Balint et al., 2018) - that affected different parts of the body (Vayssiere et al., 2004) elucidating the functional and clinical relevance of its somatotopic organization, previously described through neuronal recordings in non-human primates (DeLong et al., 1985). This way, a homunculus of the pallidum could be confirmed in the human brain.
Along similar lines, Krack et al. studied how stimulating subregions of the pallidum would lead to anti- and prodyskinetic effects (i.e., that increases or decreases involuntary muscle movements), among other symptoms (Krack et al., 1998). A crucial prerequisite for these types of analyses is to precisely reconstruct DBS electrode placements after surgery.
To learn something, we need to know exactly where we stimulated to associate location with observed effects. Also, although this factor is bluntly visible on the cortex (see next sections), it is not when stimulating in the deep regions of the brain.
Numerous methodological advances were necessary to achieve high precision in DBS electrode localizations. Imaging procedures have advanced both in terms of resolution, signal to noise ratio and their ability to visualize deep brain targets, as well as processing procedures (Ewert et al., 2019; Neudorfer et al., 2022). Magnetic resonance imaging data have been integrated with high resolution histology (Edlow et al., 2019) and structural connectivity data to provide detailed subcortical atlases (Ewert et al., 2018). Several toolboxes, such as Cicerone (Miocinovic et al., 2007), cranial vault (D’Haese et al., 2012) and Lead-DBS (Horn et al., 2019a; Horn and Kühn, 2015) now allow the scientists to estimate not only the location of the DBS probes but also to estimate the associated volume of tissue activated based on pre- and postmortem neuroimaging data.
To map the subcortex in similar ways as Wilder Penfield could, these developments were crucial, as well as making approaches openly available inform of open-source research software (Horn et al., 2019a, p. 2). Since ∼2015, this has made it possible for laboratories, world-wide, to map stimulation effects in the subcortex to observed behavioral and clinical effects – and by doing so learn and understand more about human brain function. Examples include mapping the sites for stimulation-induced panic (Elias et al., 2020), seizures (Boutet et al., 2019) or aggressiveness (Yan et al., 2019a) based on individual case-reports with DBS. In larger attempts, Irmen et al. investigated the effects of risk-taking behavior after stimulating different subregions of the subthalamic nucleus (STN) (Irmen et al., 2019) or the modulation of affect following the same procedure (Irmen et al., 2020). Mosley et al. studied effects on impulsivity following stimulations of specific subcortical tract connections in Parkinson’s disease (Mosley et al., 2020). In a prime example integrating systems-level with translational neuroscience research, Lofredi et al. used data from DBS patients to invasively validate the “stopping triangle” (Lofredi et al., 2020) – a network connecting inferior frontal gyrus, supplementary motor area and STN that had been described using functional imaging studies, before (Aron et al., 2007; Aron and Poldrack, 2006). Finally, in what may be the most detailed analysis of these types of studies to date, Neudorfer et al. mapped group-level data of DBS responses to the hypothalamic region to investigate functionality of specific hypothalamic nuclei in humans (Neudorfer et al., 2021). When including brain connectivity metrics, subcortical DBS research can close the circle to the Penfieldian cortical stimulation sites. Namely, in patients with essential tremor syndrome (a neurological condition characterized by rhythmic shaking of the patients’ body (Welton et al., 2021)), Al-Fatly et al. demonstrated that stimulating subzones of the thalamus that were most strongly connected to the hand region of Penfield’s homunculus in primary motor cortex would maximize the effect of suppressing hand tremor (Al-Fatly et al., 2019). Correspondingly, DBS electrodes strongly connected with homuncular head region led to maximal effect when treating head tremor. Examples like these illustrate how invasive access to human brains that undergo functional neurosurgery procedures can broaden our horizon about human brain function. Mapping stimulation sites in precise and comparable fashion is key to our understanding of the human brain. Brain connectivity data can integrate information learned from cortical with subcortical stimulation experiments. Altogether, advances in localization of functionally heterogeneous stimulation sites and their connectivity to distributed brain networks (within a framework referred to as Connectomic DBS (Horn and Fox, 2020)) allow to identify circuits, which, when modulated, affect specific symptoms (Horn et al., 2022). Connectomic DBS has been used extensively in recent years, starting from movement disorders (Ferreira and Akram, 2022; Horn and Fox, 2020). Connectivity studies enabled the prediction of DBS effects on PD across cohorts and surgeons (Horn et al., 2017b, 2019b), Tourette Syndrome (Johnson et al., 2020) and Essential Tremor (Al-Fatly et al., 2019). Of interest, the approach has also been extended to psychiatric disorders (Irmen et al., 2022) with applications to DBS target localization for obsessive-compulsive disorder (Baldermann et al., 2021; Li et al., 2020) and treatment-resistant depression (Riva-Posse et al., 2018; Zhu et al., 2021). These findings may inform the next generation of personalized therapies for neurological and psychiatric disorders while providing a plethora of new hypotheses to mechanistically test for basic neuroscience research (Hollunder et al., 2022).
Insights on subcortical functions from DBS-related recordings
The functional role of the basal ganglia and their subregions has been investigated by correlating the stimulation sites and resulting clinical effects, but also through the analysis of neural signals recorded in different locations from the DBS electrodes or microelectrodes recordings (MER) used during the implant for the localization of the optimal spot (Montgomery, 2017). This latter kind of recordings have some advantages compared to the analysis of recordings from DBS electrodes. First, it allows a more extensive mapping of the activity because recordings are performed at different depths and along three to five directions (“tracks”) (Bjerknes et al., 2018). Second, it allows a more localized characterization of activity thanks to the ability of recording action potentials, whose identification is hindered in DBS electrodes (van Wijk et al., 2020). Thanks to this, MER performed during awake DBS surgery are not only used for online target localization (in many diseases such as Parkinson, dystonia (Valsky et al., 2020), essential tremor (Pedrosa et al., 2018) and Tourette syndrome (Vissani et al., 2019)), but also to shed light on the functional structure of the STN. Studies range from the somatotopic body map within the nucleus (Romanelli et al., 2004) to phenomena as diverse as the synchronization between basal and cortical activity (Lipski et al., 2017), and the role of subthalamic neural populations in speech (Lipski et al., 2018) or decision making, as we will see below. Local field potentials (LFPs) provide complementary information to multi-unit recordings, as they provide a network-wide integrated view and information about the network input rather than the network output (Buzsáki et al., 2012), hence also the LFP acquired from microelectrodes have been used for both target localization (Telkes et al., 2016) and functional characterization (Telkes et al., 2018). On the other hand, there are a limited number of tasks that can be performed during a DBS surgery, and it is therefore necessary to make use of LFPs recorded from DBS electrodes after surgery to have a complete picture. LFPs have been acquired from macroelectrodes during surgery over decades. Spectral analysis of STN LFPs can help in the localization of optimal DBS target during the implant (Horn et al., 2017a; Milosevic et al., 2020). Recently, clinicians world-wide are beginning to make use of LFP recorded from STN from aDBS sensing devices to clarify the role of STN in movements. For instance, beta bursts in DBS-recorded STN LFP have been associated with peak velocity (Torrecillos et al., 2018) and the realization of the different phases of movement execution (Vissani et al., 2021) in reaching movements, and a frequency shift in the beta band toward higher frequencies has been associated with onset of gait (Canessa et al., 2020; Tinkhauser et al., 2019). Of course, further investigation is necessary to assess whether these mechanisms subserve movement control also in subjects without movement disorders. Following a similar pattern, directional DBS electrodes have been introduced to optimize clinical outcome of stimulation (Pollo et al., 2014), but are currently used “in reading mode”, not only to help finding the optimal stimulation site (Nguyen et al., 2020), but also to characterize basal ganglia activity (Telkes et al., 2020) and functional segregation (Aman et al., 2020) to a finer degree than previously achieved.
Other key applications for LFPs recorded from DBS electrodes can be seen in identifying motor symptom markers to control the stimulation. In the past decade, the paradigm shifted from continuous DBS (active the whole time) to an adaptive DBS (aDBS) capable of activating or modulating the stimulation depending on patient’s biomarkers. In particular, the onset of specific motor symptoms detected from the local field potential recorded from the DBS electrodes have been used (Little et al., 2013; Priori et al., 2013), but different solutions are also possible (see (Lozano et al., 2019; Vissani et al., 2020) for a review). The search for motor symptom biomarkers could in principle lead to a clarification of the dynamics associated with different motor dysfunctions, but so far the only commonly accepted marker subthalamic beta power (Arlotti et al., 2018; Little and Brown, 2014; Rosa et al., 2015) or the duration of beta bursts (Tinkhauser et al., 2017). Although use of these markers is becoming popular, a single marker will not be able to represent the broad spectrum of Parkinson’s symptoms, i.e., this concept has obvious limitations. We believe that more advanced approaches that take in multiple factors or apply machine learning concepts will be necessary going forward (Ewert et al., 2018; Little and Brown, 2020; Merk et al., 2022). One of them could be the use of information theory to dissect the role of beta band in motor control, taking into account both frequency (rather than power) modulations (Canessa et al., 2020) and investigating the possibility of sub-band functional ranges (Vissani et al., 2021). Similar investigations are undergoing for other motor disorders as Tourette syndrome (Marceglia et al., 2017).
Although DBS has proven to be an incredible tool to dissect the anatomical and physiological basis of natural and pathological motor control, much is still uncharted on its circuit underpinnings. In fact, a detailed mechanistic circuit-level understanding of most movement disorders is still lacking together with a definitive explanation for the astounding effects of functional neurosurgical therapies. In this regard, basal ganglia invasive studies on motor control can also be performed on animal models where a broader set of techniques can be used to investigate neural circuits and their activity. Rodent models provide the ability to access neuronal circuits in health and disease in a cell-type specific manner through genetics and viral vectors (Kim et al., 2017; Kravitz et al., 2010), whereas non-human primates have been useful to study the functional architecture of the basal ganglia (Shink et al., 1996) and both the dysfunction associated to Parkinson’s disease and the effects of DBS (Vitek and Johnson, 2019). We believe that intense crosstalk between basic/clinical neuroscience and neuroengineering will enable the next major advancements and help fill these gaps to build an integrated understanding of the motor system and its disorders.
Deep brain stimulation beyond motor control: Mood and decision-making disorders
The previous section was dedicated to clinical studies on the effects of DBS that contributed to our understanding of neural circuits underlying motor dynamics and the associated pathologies, whereas here we will review selected contributions in the field of mood and cognition. Also in this case animal studies can be performed to investigate other functions of the basal ganglia, as mood control (e.g., (Bostan and Strick, 2018)) or decision making (e.g., (Hikosaka et al., 2018; Thura and Cisek, 2017) in primates or rodents (Cenci et al., 2015)), but in this case the complexity of human behavior renders specific investigations on humans, as those provided by clinical DBS studies, even more necessary.
In recent years, research efforts were focused on identifying the boundaries of associative/limbic areas within the STN (Jahanshahi et al., 2015; Mosher et al., 2021). Once again this research has been boosted by a clinical drive, i.e., the need to avoid the collateral effects of DBS associated with the stimulation of functional areas not directly affected by the addressed motor disorder (Montgomery, 2014). Indeed, non-motor outcomes in DBS of PD patients have depended on stimulation localization (Heiden et al., 2017; Mosley et al., 2018; Petry-Schmelzer et al., 2019). DBS clinical studies have not only set the question but have also provided the practical tools to answer it. The hypothesis that ventral STN might be dedicated to cognitive functions and dorsal STN to motor functions (Jahanshahi et al., 2015) stems from the observation that prefrontal cortical areas project to the former, whereas motor and premotor cortices project to the latter (Haynes and Haber, 2013). This observation has been corroborated by the effects on DBS outcome of the location of the target stimulation in the dorsoventral/occipitorostral axis of the STN (Greenhouse et al., 2013; Scherrer et al., 2020; van Wouwe et al., 2017, 2020).
The spectral analysis of LFP recorded from DBS electrodes during cognitive tasks highlighted that the functional activity of the STN in cognitive tasks involves mainly frequency below the beta band usually associated with movement control (see above). Incongruent trials in stroop and flanker tasks (in which selective attention and executive and inhibition control are required (Voelcker-Rehage et al., 2016)) have been associated with beta (12–30 Hz) desynchronization and theta (4–8 Hz) synchronization increase (Brittain et al., 2012; Zavala et al., 2013). In high conflict decisions (Cavanagh et al., 2011) delta-theta (2–5 Hz) frequencies were increased during high conflict trials. Theta band activity was found to be more synchronized in patients with impulsive compulsive behaviors (ICB) both at rest (Rodriguez-Oroz et al., 2011) and during decision making tasks (Mazzoni et al., 2018). In particular, theta power was stronger in the presence of highly conflicting decisions (Rosa et al., 2013). Theta band was found to increase further when the conflict was an ethical one (Fumagalli et al., 2011) rather than a perceptive or cognitive one. However, conflict might not represent the whole story as low frequency LFP in STN have been attributed to subjective value in both non impulsive (Zénon et al., 2016) and impulsive subjects (Mazzoni et al., 2018). In agreement with these results, STN-prefrontal cortex coherence has been found to be particularly strong in the theta band (Herz et al., 2017; Horn et al., 2017a; Rodriguez-Oroz et al., 2011) and that this coherence associates with behavior (Herz et al., 2016).
The involvement of STN in (conflictual) decision making has been investigated also with MER studies (Zaghloul et al., 2012) MER studies observed ICB-related changes at the level of single neurons in STN but not in the pallidum (Rossi et al., 2017) further confirming the relevance of the former in the decision making circuit, and a complementary role corroborated by complementary LFP studies (Eisinger et al., 2021). MER studies can also help understand the link between ICB and dopamine agonists (DA): in DA off condition the activity of STN neurons displayed less beta activity in ICB rather than non-ICB patients (Micheli et al., 2021), suggesting that DA exerts an overcompensation leading an abnormal disinhibition of behavioral impulses.
The results reported above, although not yet combined in an integrated model of the contribution of basal ganglia to decision making, testify the key relevance of the clinical stimulation and recordings for our understanding of the matter. In turn, these advancements will be a critical asset to develop novel stimulation therapies addressing ICB, as current DBS therapies are sub-optimal in this respect (Santin et al., 2021). We have focused on impulse control as an example of an associative function, also because of its relevance as a non-motor symptom in PD, but DBS recordings of basal ganglia activity have also been used to characterize emotion or non-exclusively-motor processes as language, both associated with DBS side effects (see (Eisinger et al., 2018) for a review). Moreover, DBS is currently used to directly address psychiatric disorders such as obsessive-compulsive disorders (Tastevin et al., 2019), with clinical results helping in the identification of the circuitry underlying the pathology (Karas et al., 2019; Voon et al., 2017). Also of note, a recent study integrated lesional, transcranial magnetic stimulation and deep brain stimulation studies to identify the distributed brain network underlying depression (Siddiqi et al., 2021).
To conclude, we have to mention that novel “open recording” DBS devices might allow long-term recordings of LFP from implanted patients, with the prospective of shedding light on the mechanisms of plastic reorganization of neural circuitry. These are hypothesized to underlie the effects of DBS on the timescales of weeks and months, that are particularly relevant for psychiatric/cognitive disorders (Ashkan et al., 2017).
Understanding and restoring motor control through cortical brain machine interfaces
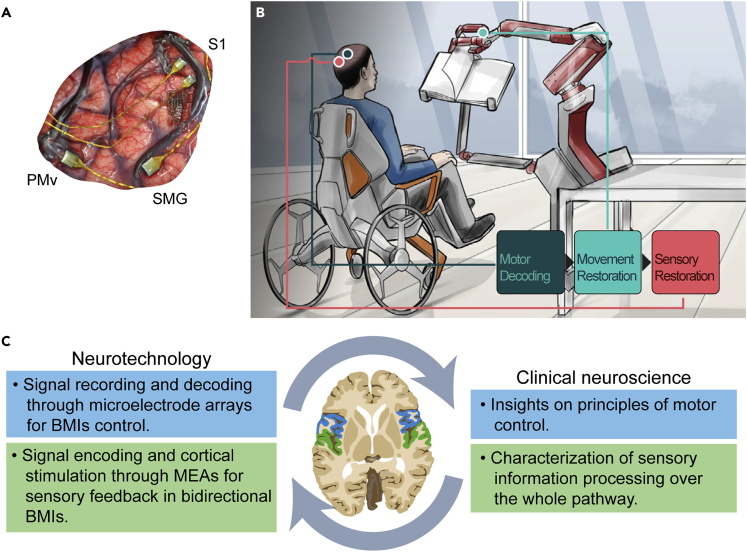
Brain-machine interfaces use cortical neuronal signals to control an artificial device (Nicolelis, 2003). Deeply rooted in our knowledge of the motor system, they have become an effective solution to restore function of the upper limb in sundry neurological disorders. As mentioned in the Introduction, it was in the 30s that Penfield and colleagues started to map the cortical surface through neurosurgical exploration and microstimulation, identifying body maps in primary motor cortex (Penfield and Boldrey, 1937). Later, single unit recordings in this brain region revealed how ensembles of neurons jointly represent movement direction (Georgopoulos et al., 1982). Thus, readings from this area could be employed to direct an artificial effector (Georgopoulos and Carpenter, 2015). On these theoretical premises and thanks to new recording technologies, the first BMIs were implemented, recording cortical neurons and using their firing to control an actuator (Carmena et al., 2003; Taylor et al., 2002; Velliste et al., 2008) (Figures 3A and 3B). Beyond fulfillment of unmet medical needs, their astounding development has provided invaluable insights on the principles of motor control. They have contributed to a new vision of how cortical neurons support action and its refinement and have spotlighted the importance of feedback signals to the motor cortex. Provided insights, together with new basic neuroscience discoveries, have led to development of more dexterous and long-term stable BMIs. Overall, (1) clinical neuroscience studies identified motor control areas that could be used to control artificial movements and this led to the development of BMI, (2) decoding of data acquired from BMIs led to novel insights into population coding of movement intention, (3) clinical studies integrated these findings with studies on the relevance of feedback and fostered the development of bidirectional BMIs (Figure 3C).
Figure 3.
Brain-machine interfaces and neuroscience of sensorimotor functions
(A) 96-channels microelectrode arrays (MEAs) implanted into ventral premotor cortex (PMv), and supramarginal gyrus (SMG), and two 48-channel stimulating arrays implanted into primary somatosensory cortex (S1). Reproduced with permission from (Armenta Salas et al., 2018).
(B) Schematic representation of bidirectional brain-machine interface (BMI) allowing user to voluntarily control external devices, such as a robotic arm. Sensors embedded in the actuator can provide sensory information to the subjects by stimulating their cortex. From (Shokur et al., 2021).
(C) Clinical applications of MEAs for BMIs (left) and associated advancements in the understanding of motor control and sensory processing (right) inside the positive feedback loop. Green: somatosensory cortices; blue: motor cortices.
In this section, dedicated to cortical BMIs, we will go back and forth between clinical neuroscience and neuroengineering through examples of bidirectional crosstalk, highlighting the potential of the latter to drive major advancements for both disciplines. In the following, we fill focus on upper limb motor control, but cortical BMIs have been used also for the study of gait (e.g., (Dietz, 2003; McCrimmon et al., 2018)).
Movement encoding and control with native and prosthetic effectors
The challenge of operating an effector lies in the need to concurrently control different movement dimensions, using a subset of neurons from one brain region. Advanced neuroprosthetic devices entail many degrees of freedom (DoF), akin to the primate upper limb, increasing control complexity. Understanding the principles of neuronal encoding of native arm movements in different cortical areas is thus fundamental to guide neurotechnological development.
During upper limb movement, motor cortical neurons have been reported to represent different variables, e.g., movement direction of the hand, joint angles and velocities, torques (Ethier et al., 2012; Georgopoulos et al., 1988; Georgopoulos and Carpenter, 2015; Hepp-Reymond et al., 1999; Kalaska et al., 1989; Kurtzer et al., 2005; Morrow et al., 2007; Scott and Kalaska, 1997; Sergio et al., 2005). At the single neuron level, these variables might be encoded in a segregated or mixed manner, i.e., with neurons solely representing one of them or jointly encoding many. Analogous reasoning can be applied to the neuronal encoding of different movements, like reaching and grasping. Paralleling native arm movement and BMI control of an actuator, researchers have shown that each neuron contributes to the control of different movement parameters concerning the proximal and distal limb, like arm-end velocity and gripping force (Carmena et al., 2003; Wessberg et al., 2000). These first results pointed toward a mixed coding model of movements and kinematic variables. Mixed and relatively shallow selectivity supports, in fact, high-dimensional encoding of behavioral variables, facilitating optimal readout from downstream, decoding brain regions, as well as BMIs (Fusi et al., 2016; Rigotti et al., 2013). Taking advantage of this feature of cortical circuitry and, particularly, mixed encoding of movement of proximal and distal limb segments, researchers enabled a tetraplegic patient to control a robotic arm with a ten-DoF hand (three-dimensional translation and orientation and four hand shape dimensions), using a small motor cortical neuronal population (Wodlinger et al., 2015). Single neuron tuning within this population often spanned many of these artificial ten dimensions. This consolidated further the idea that mixed tuning and the ensuing high dimensionality are key to motor cortical computation. Recently, high-density recordings in the motor cortex of non-human primates have estimated this dimensionality to be around 102 and, in line with this finding, researchers have shown successful offline decoding of complex hand movements with up to 30 DoF from the activity of cortical neuronal ensembles, paving the way for development of high-complexity BMIs (Okorokova et al., 2020).
To the end of enabling restoration of arm movements in patients, there is not only the need to control the prosthetic actuator but also the requirement to do so stably in different conditions and for long timeframes. From a neuroscientific standpoint, how stable movement control of the native arm is achieved by brain circuits is an active area of investigation.
The encoding properties of cortical circuits have been found to not only be high-dimensional, as described above, but also to vary in different contexts like fast and slow executions of the same movement or on changes in initial conditions, casting doubt on the meaning of single-neuron responses (Churchland and Shenoy, 2007; Ethier et al., 2012; Fetz, 1992; Hepp-Reymond et al., 1999; Kalaska et al., 1989; Kurtzer et al., 2005; Morrow et al., 2007; Scott, 2008; Scott and Kalaska, 1997; Sergio et al., 2005) but see (Jensen et al., 2021). In neuroengineering context, single-neuron tuning heterogeneity is paired with the problem of recording instability because of movement of the electrode array and inflammation around it, making long-term stable BMIs very hard to develop. In the past fifteen years, caveats of the representational view of motor cortical activity, together with new technologies for neuronal recordings and statistical methods to make sense of them, have prompted the development of a subsuming theory. This suggests that motor cortex function consists in the generation of coordinated neuronal population dynamics driving downstream circuits for action (Churchland et al., 2012; Gallego et al., 2017; Kao and Hennequin, 2019; Russo et al., 2018; Shenoy et al., 2013; Vyas et al., 2020). Despite the high dimensionality of recordings from motor cortex, few (in the order of 10) linear combinations of recorded neurons (from here on latent factors) are sufficient to capture most variance during upper limb motor tasks, resulting in a low-dimensional manifold were most activity patterns lie (Gallego et al., 2018). Latent factors have been correlated with specific actions or with general movement, during execution of different tasks (Churchland et al., 2012; Gallego et al., 2018; Russo et al., 2018), but see (Suresh et al., 2020). Modeling single trial neuronal activity with a dynamical systems framework improved online BMI performance, highlighting the evolution of neuronal population activity according to the rules of a dynamical system (Kao et al., 2015). Furthermore, recent work shows that, opposite to single or multi-unit recordings, extracted latent factors can be aligned across months and then be used as input features for long-term stable movement decoding, suggesting their time-invariant correlation with movement (Gallego et al., 2020). In line with this, another research group, developed a different strategy of manifold alignment based on stable recording electrodes, enabling robust control of a computer cursor by motor cortical neuronal activity in the face of severe recording instabilities (Degenhart et al., 2020).
Learning to move bodies and machines
Motor learning consists in the acquisition of new skills through modification of neuronal activity patterns. Pivotal lesion and functional imaging studies have revealed potential plasticity of adult motor cortical circuits (Dayan and Cohen, 2011; Sanes and Donoghue, 2000). Using the precision of animal models, single-neuron dynamics, cortical regions, corticocortical pathways and subcortical circuits have been implicated in skill learning (Barnes et al., 2005; Dhawale et al., 2021; Huber et al., 2012; Kawai et al., 2015; Komiyama et al., 2010; Makino et al., 2017; Masamizu et al., 2014; Miyachi et al., 1997; Peters et al., 2014,2017; Rioult-Pedotti et al., 1998; Veuthey et al., 2020; Wang et al., 2011; Xu et al., 2009; Yin, 2010). Nonetheless, given the massive convergence from neurons to muscles and inevitable experimental undersampling, it is very hard to map how these adaptive changes in brain dynamics contribute to learning. BMIs offer an incredible entry point to tackle this problem because of their known, controllable mapping between neuronal activity and effector movement. Subjects using BMIs rapidly improve their performance, with parallel changes in the relationship between movement and neuronal activity (Carmena et al., 2003; Collinger et al., 2013; Taylor et al., 2002; Wodlinger et al., 2015). As subjects switch from natural to artificial motor control with a fixed decoder, neurons remap their tuning to proficiently guide the actuator: Error detection drives changes in neuronal tuning and modulation depth to enhance BMI control (Carmena et al., 2003; Ganguly et al., 2011; Jarosiewicz et al., 2008; Lebedev et al., 2005; Zacksenhouse et al., 2007). Dynamic changes in neuronal tuning during natural skill learning have, in fact, been reported using longitudinal imaging of the same cortical neurons across days in rodents (Huber et al., 2012; Komiyama et al., 2010; Peters et al., 2014,2017). Over the course of learning a BMI task, a small motor cortical population stabilizes. After an increase in variability, day-to-day correlation in neuronal tuning properties progressively increases and plateaus suggesting the formation of a motor memory (Ganguly and Carmena, 2009). The establishment of stable activity patterns has similarly been observed recording the activity of excitatory layer 2/3 cortical neurons as rodents learned a lever pressing task (Peters et al., 2014) and during learning in other species (Katlowitz et al., 2018), suggesting the generality of stabilization as a neuronal learning mechanism.
At the population level, intrinsic circuit properties constrain the ability of cortical circuits to generate new activity patterns (Golub et al., 2018; Sadtler et al., 2014). By manipulating the neuron to movement transform through a BMI, researchers have shown that subjects easily learn to generate activity patterns within the low-dimensional manifold where activity naturally lies but need days to produce “new” patterns outside of this space (Oby et al., 2019). Interestingly, during learning neuronal covariance increases and progressively aligns with the behavior relevant subspace (Athalye et al., 2017). Such population level changes can be recapitulated by selectively reinforcing cortical activity patterns through optogenetic stimulation of midbrain dopaminergic neurons (Athalye et al., 2018), hinting at the importance of basal ganglia circuits in neuroprosthetic learning. In fact, the striatum, input nucleus in the basal ganglia, is needed by cortical neurons to learn arbitrary activity patterns (Koralek et al., 2012; Neely et al., 2018), as well as natural patterns leading to action (Miyachi et al., 1997).
When executing and learning natural actions, specific ensembles of neurons interact and adapt (Arber and Costa, 2018). Such functional specificity seems to be present at all hierarchical levels within the nervous system, but it becomes more and more difficult to identify going up from spinal cord to cortex. The difficulty of identifying these neuronal ensembles solely based on their topographical location has hindered our ability to study how neuronal circuits refine their activity patterns and behavior. Plasticity could occur exclusively at the level of these action-specific ensembles or result from a general modulation of different neuronal populations. Interestingly, BMI systems allow the assignment of a control role to only a subset of recorded neurons (“direct” neurons), mimicking physiologically action-specific ensembles. By doing so, as the subject learns to operate the BMI, it is possible to discern differential changes in the activity of neurons directly involved in moving the actuator and remaining, “indirect”, neurons (Ganguly et al., 2011; Koralek et al., 2012, 2013; So et al., 2012). Once proficient performance is achieved, direct neurons display stronger tuning and they are more redundant in encoding of behavior-related information compared to indirect neurons (Ganguly et al., 2011; Koralek et al., 2013; So et al., 2012). On the other hand, indirect cells significantly decrease their modulation depth across learning, independently of their anatomical distance from direct neurons. Interestingly, they display changes in their tuning of a magnitude similar to those observed in direct neurons, suggesting the existence of both selective and general plasticity mechanisms (Ganguly et al., 2011). Various candidates such as neuromodulators, cortico-basal ganglia-thalamocortical loops, cerebello-thalamocortical loops are being implicated in general and specific refinement of neuronal activity during natural action learning. Nonetheless, further study is needed to understand their differential contributions and verify if the same principles apply during neuroprosthetic skill acquisition.
Many questions are still unanswered concerning neuronal tuning, low-dimensional dynamics, learning in motor circuits. Nonetheless, learned principles have prompted major advances in neurotechnological development, leading to further discoveries on the relationship between brain and behavior. As we go forward, more effective, clinically viable and durable BMIs will be implemented, allowing extensive longitudinal study of the relationship between neurons and movement, falsification of existing theoretical models of motor function and generation of new hypotheses on brain circuits for action.
Artificial somatosensory feedback to improve action and understand sensation
The attempt to develop ever improving BMIs has also improved our understanding of the somatosensory cortex and its functional role in motor control. These findings have resulted in the development of brain-machine-brain interfaces, in which the prostheses have a bidirectional connection with the cortex, for reading motor intentions and eliciting controlled sensations (Bensmaia et al., 2020; Flesher et al., 2021; Pandarinath and Bensmaia, 2022; Shokur et al., 2021). We will discuss these aspects in the next paragraph, together with a glance at the possible future developments. Then, we will also see that such BMIs are unique opportunities for unveiling the importance of sensory feedback for motor control (Schroeder and Chestek, 2016). Here again, the positive feedback loop between neuroscience and neuroengineering emerges as a source of powerful scientific development.
The implementation of bidirectional BMIs is grounded on the neurophysiological basis of the sense of touch. Tactile and proprioceptive information are transduced by various mechanoreceptors and conveyed to the somatosensory cortex, where they are processed (Delhaye et al., 2018; Mountcastle, 2011). Subsequent elaborations result in the brain learning to tailor motor outputs to the constant incoming flow of sensory information and the physical properties of the external world (Johansson and Flanagan, 2009; Mathis et al., 2017; Wolpert et al., 2011). The first step toward the implementation of bidirectional BMIs is the ability to elicit controlled sensation from a prosthetic device. Intracortical microstimulation (ICMS) in somatosensory cortex allows us to elicit controllable sensations thanks to its potential time, amplitude and frequency modulation (Armenta Salas et al., 2018; Callier et al., 2019; Collinger et al., 2018; Flesher et al., 2016; Hughes et al., 2021a). Studies in non-human primates from the beginning of 2010s provided the first concrete demonstrations of the feasibility of a bidirectional BMI based on S1 microstimulation (J. A. Berg et al., 2013; O’Doherty et al., 2012, 2011; Tabot et al., 2013). In humans, sensations associated with palm and finger pressure can be elicited with ICMS, according to somatotopic rules (Flesher et al., 2016). Promisingly, not only these sensations were reported to remain similar if replicated long after the implantation (Callier et al., 2015; Fifer et al., 2022; Hughes et al., 2021b), but also they seem to be effective in subjects suffering from long-standing loss of sensory inputs (Makin and Bensmaia, 2017). Percept intensity can be modulated using high or low frequencies, depending on the somatosensory cortex stimulation sites (Callier et al., 2019; Hughes et al., 2021a). Continuous high frequency stimulation causes a rapid decrease in perceived sensations, highlighting the dynamical nature of cortical sensory processing and suggesting that intermittent pacing strategies may be more effective to restore the sense of touch and natural motor control (Hughes et al., 2022). In fact, recent studies on non-human primates, investigating cortical representations of object contact and texture have shown that neuronal population dynamics are more responsive to initiation and termination of touch, rather than its maintenance and that texture representation involves high dimensional encoding (190,195). Tailoring ICMS based on these findings will extend our ability to elicit controlled sensations, like vibrations (Christie et al., 2022), needed for everyday tasks like object manipulation and identification (Osborn et al., 2021) and will ultimately allow development of more principled and effective prostheses, as happened for the peripheral nervous system (George et al., 2019; Raspopovic et al., 2014).
Flesher and colleagues have harnessed the potential of ICMS to improve control of a prosthetic 7-DoFs arm, equipped with pressure sensors, by a tetraplegic patient (Flesher et al., 2021). The researchers implanted the stimulator in area 1, a cutaneous region of sensory cortex already investigated in previous studies (Flesher et al., 2016), as well as recording electrodes in motor cortex. The reproduction of a sensorimotor feedback loop through coherent activity in S1 allowed to obtain a more effective prosthesis, cutting down the total grasping time and improving dexterity. This seminal work constituted the first implementation of a bidirectional BMI (Flesher et al., 2021). From a neuroscientific standpoint, a bidirectional prosthesis is a unique discovery tool, because the feedback loop between movements and evoked sensations is available to the experimenter (O’Doherty et al., 2012; Schroeder and Chestek, 2016). Indeed, bidirectional BMIs enable to investigate the functionality of the sensory cortex, besides the perceived effects of its stimulation: in practice, amplitude-modulated ICMS cut down the learning time of the grasp and move task, proving that it constitutes intuitive feedback for sensorimotor coordination. Most importantly, the experiment showed that the peripheral information of transient subtasks (i.e., object grasping and releasing) is fundamental for motor control. Indeed, grasp and release were the phases in which the subject performance was significantly enhanced. The example above demonstrates that naturalistic sensation can help in the control of a prosthetic actuator as predicted by the view of the motor system as a very complex feedback controller (Todorov, 2004). Nonetheless, extending this notion, artificial feedback physically distinct from the actuator also improved the performance of a tetraplegic subject controlling a computer cursor (Deo et al., 2021). In particular, the patient was receiving haptic feedback at the back of the neck, highlighting the capability of the sensorimotor system to learn arbitrary associations between motor cortical activity patterns and sensations.
Up to now, all mentioned studies investigated the sense of touch and its utility to restore motor control. Nonetheless, one main driver of skilled action is our ability to perceive our body without the need for visual feedback or contact: proprioception. Loss of proprioception can have devastating consequences in the clinical realm (Cole, 2016), thus, its restoration holds incredible potential to improve usability in BMIs. Involved mechanisms are relatively well understood from a molecular and circuit perspective at the periphery (Wu et al., 2021), but how cerebellar and cortical systems make use of this information is not fully understood. Artificial S1 stimulation to achieve a sense of bodily pose has received less focus, but has also shown promising results (Tomlinson and Miller, 2016). A tetraplegic subject reported repeatable cutaneous and proprioceptive sensations, still respecting somatotopy despite chronic loss of spinal input (Armenta Salas et al., 2018). Reiterating on the ability of cortical circuits to learn the “meaning” of arbitrary stimulation patterns, an experimental work in non-human primates used ICMS to convey information in S1 about the position of the hand of the subject relative to an occluded target and showed optimal performance even in absence of other feedback modalities, highlighting cortical learning capacity (Dadarlat et al., 2015). Most recently, experimental work in rodents and newly developed analytical approaches have revealed that action – more than posture or trajectory - is relevant to explain neuronal encoding of proprioception in sensory areas of the cortex and brainstem (Sandbrink et al., 2020). In fact, the strong intertwining of action and sensation even at the neuronal level, is of extreme relevance, as suggested by pioneering bidirectional BMIs implemented in non-human primates (Suminski et al., 2010). In particular, Suminski et al. trained non-human primates to perform a reaching task, using a cursor controlled by motor cortical activity. During task execution, the arm of the subject was passively displaced with a robotic exoskeleton to provide feedback additional to vision. When hand position was controlled to strictly replicate cursor motion, the reaching task was performed faster and straighter. Thus, the authors demonstrated that the consistent proprioceptive feedback enhanced kinematic performance. Most importantly, proprioceptive feedback also induced an increase in movement-related information in M1 neurons. The presence of feedback induced activity in otherwise silent neurons just before cursor movement and reduced the average dimensionality of recorded spiking activity. This suggests that better performance was obtained thanks to a better state estimate and more effective decoding of intended movement from M1 population activity. Interestingly, in a similar study, the presence of coherent visual and proprioceptive feedback, without voluntary movement, evoked M1 firing very similar to that generated during overt action (Suminski et al., 2009). These findings highlight the driving role of feedback for motor cortical circuits and give clinicians the chance to calibrate M1 BMIs in subjects who are not able to physically perform calibration movements.
To summarize, not only bidirectional BMIs are confirming the central role of sensory signals for motor control, but also, they are revealing the importance of functional relationships within different cortical areas and the incredible learning properties of the sensorimotor cortex. As researchers started venturing in the meanders of the brain, the vision of the motor system as an intricate feedback controller has been gaining increasing value (Kalidindi et al., 2021; Todorov, 2004). Based on this view, we foresee incredible advancements in the development of bidirectional BMI, which will reveal, in return, yet unknown properties of cortical circuits.
Although we focused on cortical and subcortical neural interfaces, peripheral neural interfaces are potentially also part of the clinical neuroscience-neurotechnology positive feedback loop. Neurotechnology based on peripheral neural interfaces was able to restore sensory feedback in amputees (Mazzoni et al., 2020; Oddo et al., 2016; Raspopovic et al., 2014; Shokur et al., 2021). The search for the optimal code delivering useful feedback through the peripheral neural interfaces (Valle et al., 2018) was able to give insights about the code with which the human nervous system encodes tactile sensory information (Graczyk et al., 2016). A biomimetic stimulation may improve the naturalness of the sensory feedback, increase the embodiment of the artificial limb, and improve the performance on object manipulation tasks (George et al., 2019; Saal and Bensmaia, 2015; Valle et al., 2018). The analysis of anatomy and function of peripheral nerves can in turn drive the design of the peripheral neural interfaces (Romeni et al., 2020).
Cortical BMIs beyond motor control
Brain machine interfaces for surgical treatment of epilepsy
About 30–40% of the patients with focal epilepsy suffer from drug-resistant epilepsy (Rugg-Gunn et al., 2020). For those, there is the need to intervene surgically. The surgery is done by resecting the parts of the brain responsible for the initiation of the epileptic seizure (i.e., the epileptogenic zones) (Cossu et al., 2005). Pre-operative evaluation is done to precisely locate the epileptogenic zones. The presurgical evaluation is performed mainly with non-invasive methods such as scalp electroencephalography (EEG), magnetoencephalography (MEG), magnetic resonant imaging (MRI), and positron emission tomography (PET), but intracranial recordings may be needed if the non-invasive investigations do not allow to precisely locate the epileptogenic zones (Baumgartner et al., 2019). Tailored resections based on a careful presurgical evaluation may lead to achieving a good balance between surgical resection and quality of life following the surgery (Freri et al., 2017; Sonoda et al., 2022). Intracranial recordings can also provide biomarkers to predict the surgical outcome for focal epilepsy, thus guiding the clinicians in the decision on whether to perform the surgery (Klimes et al., 2022). The intracranial recordings can be done using two different techniques (or a combination of both): electrocorticography (ECoG) and stereo-electroencephalography (SEEG) (Figure 4A).
Figure 4.
Intracortical neural interfaces, neurosurgery and cognitive neuroscience
(A) Subdural grid versus depth electrode placement in previously operated brain tumor patients. (left) electrocorticographic (ECoG) grid. (right) Stereo-electroencephalographic (SEEG) electrodes. Reproduced with permission from (Sweet et al., 2013).
(B) Intraoperative functional mapping done by analyzing the ECoG signal while the patient executes cognitive tasks during awake surgery. From (Erez et al., 2021).
(C) Clinical applications of SEEG and ECoG (left) and associated advancements in the understanding of cognitive brain functions (right) inside the positive feedback loop. Red: temporal lobes.
ECoG was developed in the 1950s by Penfield and Jasper at the Montreal Neurological Institute (Penfield and Perot, 1963). It consists of grids (or stripes) of electrodes placed under the dura mater, after craniotomy. Modern ECoG setups consist of square grids of 64–128 platinum electrodes with about 1 cm of intercontact distance (Asano et al., 2005). The placement of the ECoG grids is guided by the results of scalp EEG, MRI, and/or PET. SEEG was developed in the 1960s by Talairach and Blancaud at Sainte-Anne Hospital, Paris (Talairach and Française, 1974). It is generally performed using 8–15 depth electrodes with a 0.8 mm diameter and 5 to 18 2 mm long contacts spaced by 1.5 mm (Bartolomei et al., 2017). The SEEG implantation is done stereotactically and thus craniotomy is not necessary. The absence of craniotomy drastically reduces the complications associated with SEEG implantation, which are significantly less than those of ECoG (Iida and Otsubo, 2017). Compared to ECoG grids, SEEG depth electrodes sample a larger volume of gray matter (Anderson et al., 2021), but ECoG could be preferred if the non-invasive analysis failed at locating a precise surgical intervention area (Englot, 2018). In a 2019 review, Yan et al. reported that SEEG was associated with 61.0% seizure freedom, 4.8% morbidity, and 0.2% mortality, whereas ECoG was associated with 56.4% seizure freedom, 15.5% morbidity, and 0.4% mortality (Yan et al., 2019b). Thus, SEEG depth electrodes make a better and safer alternative to subdural ECoG electrodes for the presurgical evaluation done on subjects suffering from drug-resistant epilepsy. However, epidural grid electrodes have recently been shown to decrease the possibility of post-operative complications while maintaining a quality of the signal comparable to that of subdural ECoG (Park et al., 2022).
Intracranial recordings are not exclusively used for pre-operative evaluation but can also guide the clinicians during the surgery. This is the case for brain tumor surgery. Epileptic activity often arises in patients with gliomas (Ghinda et al., 2021; Saito et al., 2018), thus some patients with brain tumors undergo intraoperative ECoG monitoring, typically during awake craniotomy (Goldstein and Feyissa, 2018; Yao et al., 2018). The presence of high-frequency oscillations in the ECoG signal seems to be a spatial marker of the epileptogenic zones in brain tumor-related epilepsy (Feyissa et al., 2018; Peng et al., 2021; Quitadamo et al., 2018; Sun et al., 2022; van Klink et al., 2021; Zhang et al., 2021), even though there is some disagreement between researchers (Robertson et al., 2019; Zhu et al., 2022). Apart from epileptogenic zone identification, intracranial recordings are also used to functionally map cortical regions before or during surgery. Functional mapping is essential to optimize resection boundaries while not affecting functional sites (Vakani and Nair, 2019). Intraoperative functional mapping of the brain during awake surgery is usually performed using direct electrical stimulation (DES). DES temporarily disturbs behavior or cognition, thus allowing the identification of cortical areas essential for a function (Boyer et al., 2021). ECoG signal processing has been proposed as a valid alternative to DES to avoid the risks associated with cortical stimulation. Functional mapping can be done by analyzing the ECoG signal while the patient executes tasks during awake surgery (Erez et al., 2021) (Figure 4B). As an example, changes in the somatosensory evoked potentials can inform the clinicians and thus improve the outcome of brain tumor surgery (Simon et al., 2021). ECoG during awake craniotomy has also been shown to be a suitable option for the surveillance of the patients’ consciousness during the surgery (Lange et al., 2019).
One other key application of SEEG electrodes is the non-surgical treatment of drug-resistant epilepsy through radiofrequency thermocoagulation. In radiofrequency thermocoagulation, SEEG contacts are connected to a radiofrequency lesion generator which delivers a continuous current through SEEG electrodes near the epileptogenic zone (Mirandola et al., 2017). The parameters of the stimulation are defined to increase the tissue temperature and induce a lesion around the selected contacts (Cossu et al., 2017).
Overall, the intracortical recordings give a unique opportunity to acquire data with unmatched temporal and spatial resolutions and without the common limitations associated with non-invasive recordings (He et al., 2019). For this reason, clinicians and scientists are focusing increasingly their attention on these invasive recordings to develop new treatments for focal epilepsy. For example, researchers used SEEG delivered stimulation to investigate the semiology of temporal lobe epilepsy (Mariani et al., 2021), study uncommon forms of epilepsy such as musicogenic epilepsy (Pelliccia et al., 2019), or predict seizure onset (Wang et al., 2022), type (Sanz-García et al., 2022), duration (Liu et al., 2022), and termination (Salami et al., 2022). Results from these studies pave the way to closed-loop treatment strategies that could minimize the clinical impact of seizures. We observe here that the interplay between clinical neuroscience and neuroengineering led to the same path we already discussed above for DBS and cortical BMIs for movement control: from clinical surgical procedures to novel neurotechnologies to clinical neuroscience understanding of pathological dynamics to closed loop neurotechnologies (Figure 4C).
Cortical brain machine interfaces for cognitive disorders
The intrinsic characteristics of intracortical recordings give the researchers the unparalleled opportunity to unravel the complex brain mechanisms associated with human behavior and cognition (Parvizi and Kastner, 2018). Moreover, the knowledge acquired using intracortical recordings can help clinicians plan the surgical resection in order to not worsen the cognitive abilities of the patients after the surgery. The present section will present some prototypical examples of how intracortical recordings can help scientists in the study of cognitive functions.
A common element between all cognitive functions is the cooperation between several brain regions needed to accomplish them. A typical example is constituted by arithmetic processing. Intracranial recordings revealed cooperation between the intraparietal sulcus, the superior parietal lobe, and the posterior inferior temporal gyrus (Das and Menon, 2022). The latter may have a role in the early identification of the problem difficulty (Pinheiro-Chagas et al., 2018), regardless of input format (digits or number words) (Baek et al., 2018). Depth electrodes allow direct access to deep brain zones such as the hippocampus and the amygdala. SEEG studies revealed the activation of the hippocampus for speech segmentation (Ramos-Escobar et al., 2022), recent and remote autobiographical events recollection (Norman et al., 2021), and working memory processing (Li et al., 2022). Notably, in a 2022 study, Castelhano et al. identified three hippocampal-centered task-related networks for visual attention, memory, and face recognition or object-based search (Castelhano et al., 2022). The functional role of the amygdala was investigated using both SEEG recordings and SEEG delivered stimulation. Amygdala electrical stimulation was reported to alter the emotional perception of images (Bujarski et al., 2021), whereas Manssuer et al. identified a network constituted by the amygdala, hippocampus, and the orbitofrontal cortex for reward and loss coding, using a monetary incentive delay task during SEEG recording (used to study the neural correlates of incentive receipt anticipation (Helfinstein et al., 2013)) (Manssuer et al., 2022). The orbitofrontal cortex has a role also in decision making (Saez et al., 2018), and emotional processing (Weisholtz et al., 2022). The latter function is carried out by the anterior insula as well (Frot et al., 2022).
Intracranial recordings have provided unique understandings of the spatiotemporal dynamics of speech production and perception. This is because high-frequency activity (from 50 Hz up to 300 Hz) is important in encoding speech-related information, as shown by many intracortical studies (Flinker et al., 2015; Korzeniewska et al., 2011; Magrassi et al., 2015; Murphy et al., 2022; Riès et al., 2017). For example, in 2020, Artoni et al. found that high gamma band activity (150–300 Hz) recorded using SEEG electrodes showed a significant difference during the presentation of noun phrases or verb phrases (Artoni et al., 2020). Because of the intrinsic limitations of other non-invasive recording methods, it would be impossible to record such high frequencies without directly accessing the brain. Another way of studying the brain networks related to speech is the use of cortico-cortical evoked potentials (CCEPs). CCEPs are an invasive method to estimate effective connectivity (Matsumoto and Kunieda, 2019). They consist of the direct electrical stimulation (usually 1 Hz pulses) of cortical structures followed by the detection of evoked potentials at distant channels. CCEPs are an indicator of the presence of a direct corticocortical or cortico-subcortico-cortical anatomical pathway (Matsumoto et al., 2004). CCEPs had been used to map cortical networks responsible for speech processing (Jahangiri et al., 2021; Sonoda et al., 2022). The knowledge of speech production and perception acquired using intracranial recordings can in turn be leveraged to develop speech prostheses (Anumanchipalli et al., 2019; Luo et al., 2022).
The default mode network (DMN) is a large-scale brain network comprising the angular gyrus, the medial prefrontal cortex, and the posterior cingulate cortex and plays a critical role in behavior, internally directed cognition (Fox et al., 2018), and mentalizing about self and others (Tan et al., 2022). Non-invasive methods are not able to fully capture the network dynamics of the DMN because of their intrinsic limitations, thus intracortical recordings are critical for its investigation (Das et al., 2022). The DMN is composed of many subnetworks, one of which is the posteromedial cortex (PMC). Intracortical recordings and direct electrical stimulation of the PMC have shown that it has a pivotal role in spontaneous thought and goal-driven internally oriented processes (Daitch and Parvizi, 2018), and more broadly in the sense of self (Parvizi et al., 2021).
Other brain networks such as the frontoparietal network and the salience network support other aspects of human cognition and behavior (Corbetta and Shulman, 2002; Uddin, 2015). But how are these large-scale networks interacting? Intracranial electrodes have been used to answer this question. Some works investigated the directionality of information flow within and between networks (Das and Menon, 2020). Other trials studied the timing of activation or de-activation of different networks during task-related processing (Kucyi et al., 2020; Raccah et al., 2018) or task switching (Mitsuhashi et al., 2022). Finally, there has been an attempt to map the connections between these networks using CCEPs (Shine et al., 2017).
Conclusions
Contemporary science is mostly about interdisciplinarity ("Mind meld", 2015), in an attempt to make established scientific fields able to evolve and cope with novel challenges. However, as illustrated, the interaction between clinical neuroscience and neurotechnologies goes deeper than a simple interdisciplinary collaboration and can in perspective become a framework on its own. This process is far from being over and far from being an easy one: for neurotechnology to become a branch of clinical neuroscience both disciplines must change, starting from education paths and science organization, with the establishment of novel graduate and undergraduate programs as well as integrated research centers. However, the promise lies in a dramatic increase of our ability to understand and treat the dysfunctions of the human nervous system. For instance, a foreseeable key challenge will be to understand the long-term dynamics between nervous system and neurotechnologies (e.g., some of the improvements seen in movement disorders only weeks after the implant (Ashkan et al., 2017), the displacement of sensory perception weeks after the implant of neuroprosthetic devices (Petrini et al., 2019)). A better understanding of these dynamics will pave the way to improve neurotechnologies and to shed light on learning, plasticity and circuits in our brain.
Acknowledgments
A.C. was supported by the Italian Ministry of University and Research (MUR) through PRIN-2017 'INSPECT' (Project 2017JPMW4F). A.F. was supported by a Biozentrum PhD Fellowship. A.H. was supported by the German Research Foundation (Deutsche Forschungsgemeinschaft, 424778381 – TRR 295), Deutsches Zentrum für Luft- und Raumfahrt (DynaSti grant within the EU Joint ProgramNeurodegenerative Disease Research, JPND), the National Institutes of Health (2R01 MH113929) as well as the New Venture Fund (FFOR Seed Grant). A.M. was supported by a grant from New York University School of Medicine and The Marlene and Paolo Fresco Institute for Parkinson’s and Movement Disorders and PREVIEW project from Bando Salute Regione Toscana 2018. S.M. was supported by the Bertarelli Foundation, PRIN-2017 INSPECT 2017JPMW4F from the Italian Ministry of University and Research (MUR), and PERSONA project from Bando Salute Regione Toscana 2018.
Author contributions
Conceptualization, A.M and S.M.; Writing – Original Draft, A.C., A.F., M.B., A.H., and A.M.; Writing – Review & Editing, all authors; Visualization, A.C.; Supervision, A.M. and S.M.; Project Administration, J.C, A.M., and S.M.; Funding Acquisition, A.M. and S.M.
Declaration of interests
S.M. holds shares in the companies IUVO, GTX, and SensArs Neurotechnologies, which are all developing neurotechnologies to restore sensorimotor functions of people with disabilities. All other authors declare no competing interests.
References
- Al-Fatly B., Ewert S., Kübler D., Kroneberg D., Horn A., Kühn A.A. Connectivity profile of thalamic deep brain stimulation to effectively treat essential tremor. Brain. 2019;142:3086–3098. doi: 10.1093/brain/awz236. [DOI] [PubMed] [Google Scholar]
- Aman J.E., Johnson L.A., Sanabria D.E., Wang J., Patriat R., Hill M., Marshall E., MacKinnon C.D., Cooper S.E., Schrock L.E., et al. Directional deep brain stimulation leads reveal spatially distinct oscillatory activity in the globus pallidus internus of Parkinson’s disease patients. Neurobiol. Dis. 2020;139:104819. doi: 10.1016/j.nbd.2020.104819. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Anderson D.N., Charlebois C.M., Smith E.H., Arain A.M., Davis T.S., Rolston J.D. Probabilistic comparison of gray and white matter coverage between depth and surface intracranial electrodes in epilepsy. Sci. Rep. 2021;11:24155. doi: 10.1038/s41598-021-03414-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Anumanchipalli G.K., Chartier J., Chang E.F. Speech synthesis from neural decoding of spoken sentences. Nature. 2019;568:493–498. doi: 10.1038/s41586-019-1119-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Arber S., Costa R.M. Connecting neuronal circuits for movement. Science. 2018;360:1403–1404. doi: 10.1126/science.aat5994. [DOI] [PubMed] [Google Scholar]
- Arlotti M., Marceglia S., Foffani G., Volkmann J., Lozano A.M., Moro E., Cogiamanian F., Prenassi M., Bocci T., Cortese F., et al. Eight-hours adaptive deep brain stimulation in patients with Parkinson disease. Neurology. 2018;90:e971–e976. doi: 10.1212/WNL.0000000000005121. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Armenta Salas M., Bashford L., Kellis S., Jafari M., Jo H., Kramer D., Shanfield K., Pejsa K., Lee B., Liu C.Y., Andersen R.A. Proprioceptive and cutaneous sensations in humans elicited by intracortical microstimulation. Elife. 2018;7:e32904. doi: 10.7554/eLife.32904. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Aron A.R., Behrens T.E., Smith S., Frank M.J., Poldrack R.A. Triangulating a cognitive control network using diffusion-weighted magnetic resonance imaging (MRI) and functional MRI. J. Neurosci. 2007;27:3743–3752. doi: 10.1523/JNEUROSCI.0519-07.2007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Aron A.R., Poldrack R.A. Cortical and subcortical contributions to stop signal response inhibition: role of the subthalamic nucleus. J. Neurosci. 2006;26:2424–2433. doi: 10.1523/JNEUROSCI.4682-05.2006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Artoni F., d’Orio P., Catricalà E., Conca F., Bottoni F., Pelliccia V., Sartori I., Russo G.L., Cappa S.F., Micera S., Moro A. High gamma response tracks different syntactic structures in homophonous phrases. Sci. Rep. 2020;10:7537. doi: 10.1038/s41598-020-64375-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Asano E., Juhász C., Shah A., Muzik O., Chugani D.C., Shah J., Sood S., Chugani H.T. Origin and propagation of epileptic spasms delineated on electrocorticography. Epilepsia. 2005;46:1086–1097. doi: 10.1111/j.1528-1167.2005.05205.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ashkan K., Rogers P., Bergman H., Ughratdar I. Insights into the mechanisms of deep brain stimulation. Nat. Rev. Neurol. 2017;13:548–554. doi: 10.1038/nrneurol.2017.105. [DOI] [PubMed] [Google Scholar]
- Athalye V.R., Santos F.J., Carmena J.M., Costa R.M. Evidence for a neural law of effect. Science. 2018;359:1024–1029. doi: 10.1126/science.aao6058. [DOI] [PubMed] [Google Scholar]
- Athalye V.R., Ganguly K., Costa R.M., Carmena J.M. Emergence of coordinated neural dynamics underlies neuroprosthetic learning and skillful control. Neuron. 2017;93:955–970.e5. doi: 10.1016/j.neuron.2017.01.016. [DOI] [PubMed] [Google Scholar]
- Baek S., Daitch A.L., Pinheiro-Chagas P., Parvizi J. Neuronal population responses in the human ventral temporal and lateral parietal cortex during arithmetic processing with digits and number words. J. Cogn. Neurosci. 2018;30:1315–1322. doi: 10.1162/jocn_a_01296. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Baldermann J.C., Schüller T., Kohl S., Voon V., Li N., Hollunder B., Figee M., Haber S.N., Sheth S.A., Mosley P.E., et al. Connectomic deep brain stimulation for obsessive-compulsive disorder. Biol. Psychiatry. 2021;90:678–688. doi: 10.1016/j.biopsych.2021.07.010. [DOI] [PubMed] [Google Scholar]
- Balint B., Mencacci N.E., Valente E.M., Pisani A., Rothwell J., Jankovic J., Vidailhet M., Bhatia K.P. Dystonia. Nat. Rev. Dis. Primers. 2018;4:25. doi: 10.1038/s41572-018-0023-6. [DOI] [PubMed] [Google Scholar]
- Barnes T.D., Kubota Y., Hu D., Jin D.Z., Graybiel A.M. Activity of striatal neurons reflects dynamic encoding and recoding of procedural memories. Nature. 2005;437:1158–1161. doi: 10.1038/nature04053. [DOI] [PubMed] [Google Scholar]
- Bartolomei F., Lagarde S., Wendling F., McGonigal A., Jirsa V., Guye M., Bénar C. Defining epileptogenic networks: contribution of SEEG and signal analysis. Epilepsia. 2017;58:1131–1147. doi: 10.1111/epi.13791. [DOI] [PubMed] [Google Scholar]
- Baumgartner C., Koren J.P., Britto-Arias M., Zoche L., Pirker S. Presurgical epilepsy evaluation and epilepsy surgery. F1000Research. 2019;8 doi: 10.12688/f1000research.17714.1. F1000 Faculty Rev-1818. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Benabid A.L., Pollak P., Gervason C., Hoffmann D., Gao D.M., Hommel M., Perret J.E., de Rougemont J. Long-term suppression of tremor by chronic stimulation of the ventral intermediate thalamic nucleus. Lancet. 1991;337:403–406. doi: 10.1016/0140-6736(91)91175-t. [DOI] [PubMed] [Google Scholar]
- Bensmaia S.J., Tyler D.J., Micera S. Restoration of sensory information via bionic hands. Nat. Biomed. Eng. 2020 doi: 10.1038/s41551-020-00630-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Berg J.A., Dammann J.F., Tenore F.V., Tabot G.A., Boback J.L., Manfredi L.R., Peterson M.L., Katyal K.D., Johannes M.S., Makhlin A., et al. Behavioral demonstration of a somatosensory neuroprosthesis. IEEE Trans. Neural Syst. Rehabil. Eng. 2013;21:500–507. doi: 10.1109/TNSRE.2013.2244616. [DOI] [PubMed] [Google Scholar]
- Bjerknes S., Toft M., Konglund A.E., Pham U., Waage T.R., Pedersen L., Skjelland M., Haraldsen I., Andersson S., Dietrichs E., Skogseid I.M. Multiple microelectrode recordings in STN-DBS surgery for Parkinson’s disease: a randomized study: microelectrode recordings in STN-DBS surgery. Mov. Disord. Clin. Pract. 2018;5:296–305. doi: 10.1002/mdc3.12621. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bostan A.C., Strick P.L. The basal ganglia and the cerebellum: nodes in an integrated network. Nat. Rev. Neurosci. 2018;19:338–350. doi: 10.1038/s41583-018-0002-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Boutet A., Jain M., Elias G.J.B., Gramer R., Germann J., Davidson B., Coblentz A., Giacobbe P., Kucharczyk W., Wennberg R.A., et al. Network basis of seizures induced by deep brain stimulation: literature review and connectivity analysis. World Neurosurg. 2019;132:314–320. doi: 10.1016/j.wneu.2019.08.094. [DOI] [PubMed] [Google Scholar]
- Boyer A., Ramdani S., Duffau H., Dali M., Vincent M.A., Mandonnet E., Guiraud D., Bonnetblanc F. Electrophysiological mapping during brain tumor surgery: recording cortical potentials evoked locally, subcortically and remotely by electrical stimulation to assess the brain connectivity on-line. Brain Topogr. 2021;34:221–233. doi: 10.1007/s10548-020-00814-0. [DOI] [PubMed] [Google Scholar]
- Brittain J.-S., Watkins K.E., Joundi R.A., Ray N.J., Holland P., Green A.L., Aziz T.Z., Jenkinson N. A role for the subthalamic nucleus in response inhibition during conflict. J. Neurosci. 2012;32:13396–13401. doi: 10.1523/JNEUROSCI.2259-12.2012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bujarski K.A., Song Y., Xie T., Leeds Z., Kolankiewicz S.I., Wozniak G.H., Guillory S., Aronson J.P., Chang L., Jobst B.C. Modulation of emotion perception via amygdala stimulation in humans. Front. Neurosci. 2021;15:795318. doi: 10.3389/fnins.2021.795318. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Buzsáki G., Anastassiou C.A., Koch C. The origin of extracellular fields and currents — EEG, ECoG, LFP and spikes. Nat. Rev. Neurosci. 2012;13:407–420. doi: 10.1038/nrn3241. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Callier T., Schluter E.W., Tabot G.A., Miller L.E., Tenore F.V., Bensmaia S.J. Long-term stability of sensitivity to intracortical microstimulation of somatosensory cortex. J. Neural. Eng. 2015;12:056010. doi: 10.1088/1741-2560/12/5/056010. [DOI] [PubMed] [Google Scholar]
- Callier T., Suresh A.K., Bensmaia S.J. Neural coding of contact events in somatosensory cortex. Cereb. Cortex. 2019;29:4613–4627. doi: 10.1093/cercor/bhy337. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Canessa A., Palmisano C., Isaias I.U., Mazzoni A. Gait-related frequency modulation of beta oscillatory activity in the subthalamic nucleus of parkinsonian patients. Brain Stimul. 2020;13:1743–1752. doi: 10.1016/j.brs.2020.09.006. [DOI] [PubMed] [Google Scholar]
- Carmena J.M., Lebedev M.A., Crist R.E., O’Doherty J.E., Santucci D.M., Dimitrov D.F., Patil P.G., Henriquez C.S., Nicolelis M.A.L., Segev I. Learning to control a brain–machine interface for reaching and grasping by primates. PLoS Biol. 2003;1:e42. doi: 10.1371/journal.pbio.0000042. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Castelhano J., Duarte I., Bernardino I., Pelle F., Francione S., Sales F., Castelo-Branco M. Intracranial recordings in humans reveal specific hippocampal spectral and dorsal vs. ventral connectivity signatures during visual, attention and memory tasks. Sci. Rep. 2022;12:3488. doi: 10.1038/s41598-022-07225-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cavanagh J.F., Wiecki T.V., Cohen M.X., Figueroa C.M., Samanta J., Sherman S.J., Frank M.J. Subthalamic nucleus stimulation reverses mediofrontal influence over decision threshold. Nat. Neurosci. 2011;14:1462–1467. doi: 10.1038/nn.2925. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cenci M.A., Francardo V., O’Sullivan S.S., Lindgren H.S. Rodent models of impulsive–compulsive behaviors in Parkinson’s disease: how far have we reached? Neurobiol. Dis. 2015;82:561–573. doi: 10.1016/j.nbd.2015.08.026. [DOI] [PubMed] [Google Scholar]
- Cerletti U. Old andnewinformationaboutelectroshock. Am. J. Psychiatry. 1950;107:87–94. doi: 10.1176/ajp.107.2.87. [DOI] [PubMed] [Google Scholar]
- Christie B., Osborn L.E., McMullen D.P., Pawar A.S., Thomas T.M., Bensmaia S.J., Celnik P.A., Fifer M.S., Tenore F.V. Perceived timing of cutaneous vibration and intracortical microstimulation of human somatosensory cortex. Brain Stimul. 2022;15:881–888. doi: 10.1016/j.brs.2022.05.015. [DOI] [PubMed] [Google Scholar]
- Churchland M.M., Cunningham J.P., Kaufman M.T., Foster J.D., Nuyujukian P., Ryu S.I., Shenoy K.V. Neural population dynamics during reaching. Nature. 2012;487:51–56. doi: 10.1038/nature11129. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Churchland M.M., Shenoy K.V. Temporal complexity and heterogeneity of single-neuron activity in premotor and motor cortex. J. Neurophysiol. 2007;97:4235–4257. doi: 10.1152/jn.00095.2007. [DOI] [PubMed] [Google Scholar]
- Cole J. First edition. Oxford University Press; 2016. Losing Touch: A Man without His Body. [Google Scholar]
- Collinger J.L., Gaunt R.A., Schwartz A.B. Progress towards restoring upper limb movement and sensation through intracortical brain-computer interfaces. Curr. Opin. Biomed. Eng. 2018;8:84–92. doi: 10.1016/j.cobme.2018.11.005. [DOI] [Google Scholar]
- Collinger J.L., Wodlinger B., Downey J.E., Wang W., Tyler-Kabara E.C., Weber D.J., McMorland A.J., Velliste M., Boninger M.L., Schwartz A.B. High-performance neuroprosthetic control by an individual with tetraplegia. Lancet. 2013;381:557–564. doi: 10.1016/S0140-6736(12)61816-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cooper I.S., Upton A.R., Amin I. Reversibility of chronic neurologic deficits. Some effects of electrical stimulation of the thalamus and internal capsule in man. Appl. Neurophysiol. 1980;43:244–258. doi: 10.1159/000102263. [DOI] [PubMed] [Google Scholar]
- Corbetta M., Shulman G.L. Control of goal-directed and stimulus-driven attention in the brain. Nat. Rev. Neurosci. 2002;3:201–215. doi: 10.1038/nrn755. [DOI] [PubMed] [Google Scholar]
- Cossu M., Cardinale F., Casaceli G., Castana L., Consales A., D’Orio P., Lo Russo G. Stereo-EEG–guided radiofrequency thermocoagulations. Epilepsia. 2017;58:66–72. doi: 10.1111/epi.13687. [DOI] [PubMed] [Google Scholar]
- Cossu M., Cardinale F., Castana L., Citterio A., Francione S., Tassi L., Benabid A.L., Lo Russo G. Stereoelectroencephalography in the presurgical evaluation of focal epilepsy: a retrospective analysis of 215 procedures. Neurosurgery. 2005;57:706–718. discussion706–718. [PubMed] [Google Scholar]
- Dadarlat M.C., O’Doherty J.E., Sabes P.N. A learning-based approach to artificial sensory feedback leads to optimal integration. Nat. Neurosci. 2015;18:138–144. doi: 10.1038/nn.3883. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Daitch A.L., Parvizi J. Spatial and temporal heterogeneity of neural responses in human posteromedial cortex. Proc. Natl. Acad. Sci. USA. 2018;115:4785–4790. doi: 10.1073/pnas.1721714115. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Das A., de los Angeles C., Menon V. Electrophysiological foundations of the human default-mode network revealed by intracranial-EEG recordings during resting-state and cognition. Neuroimage. 2022;250:118927. doi: 10.1016/j.neuroimage.2022.118927. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Das A., Menon V. Causal dynamics and information flow in parietal-temporal-hippocampal circuits during mental arithmetic revealed by high-temporal resolution human intracranial EEG. Cortex. 2022;147:24–40. doi: 10.1016/j.cortex.2021.11.012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Das A., Menon V. Spatiotemporal integrity and spontaneous nonlinear dynamic properties of the salience network revealed by human intracranial electrophysiology: a multicohort replication. Cereb. Cortex. 2020;30:5309–5321. doi: 10.1093/cercor/bhaa111. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Dayan E., Cohen L.G. Neuroplasticity subserving motor skill learning. Neuron. 2011;72:443–454. doi: 10.1016/j.neuron.2011.10.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Degenhart A.D., Bishop W.E., Oby E.R., Tyler-Kabara E.C., Chase S.M., Batista A.P., Yu B.M. Stabilization of a brain–computer interface via the alignment of low-dimensional spaces of neural activity. Nat. Biomed. Eng. 2020;4:672–685. doi: 10.1038/s41551-020-0542-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Delhaye B.P., Long K.H., Bensmaia S.J. Neural basis of touch and proprioception in primate cortex. Compr. Physiol. 2018;8:1575–1602. doi: 10.1002/cphy.c170033. [DOI] [PMC free article] [PubMed] [Google Scholar]
- DeLong M.R., Crutcher M.D., Georgopoulos A.P. Primate globus pallidus and subthalamic nucleus: functional organization. J. Neurophysiol. 1985;53:530–543. doi: 10.1152/jn.1985.53.2.530. [DOI] [PubMed] [Google Scholar]
- Deo D.R., Rezaii P., Hochberg L.R., M Okamura A., Shenoy K.V., Henderson J.M. Effects of peripheral haptic feedback on intracortical brain-computer interface control and associated sensory responses in motor cortex. IEEE Trans. Haptics. 2021;14:762–775. doi: 10.1109/TOH.2021.3072615. [DOI] [PMC free article] [PubMed] [Google Scholar]
- D’Haese P.-F., Pallavaram S., Li R., Remple M.S., Kao C., Neimat J.S., Konrad P.E., Dawant B.M. CranialVault and its CRAVE tools: a clinical computer assistance system for deep brain stimulation (DBS) therapy. Med. Image Anal. 2012;16:744–753. doi: 10.1016/j.media.2010.07.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Dhawale A.K., Wolff S.B.E., Ko R., Ölveczky B.P. The basal ganglia control the detailed kinematics of learned motor skills. Nat. Neurosci. 2021;24:1256–1269. doi: 10.1038/s41593-021-00889-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Dietz V. Spinal cord pattern generators for locomotion. Clin. Neurophysiol. 2003;114:1379–1389. doi: 10.1016/s1388-2457(03)00120-2. [DOI] [PubMed] [Google Scholar]
- Edlow B.L., Mareyam A., Horn A., Polimeni J.R., Witzel T., Tisdall M.D., Augustinack J.C., Stockmann J.P., Diamond B.R., Stevens A., et al. 7 Tesla MRI of the ex vivo human brain at 100 micron resolution. Sci. Data. 2019;6:244. doi: 10.1038/s41597-019-0254-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Eisinger R.S., Cagle J.N., Alcantara J.D., Opri E., Cernera S., Le A., Torres Ponce E.M., Lanese J., Nelson B., Lopes J., et al. Distinct roles of the human subthalamic nucleus and dorsal pallidum in Parkinson’s disease impulsivity. Biol. Psychiatry. 2021;91:370–379. doi: 10.1016/j.biopsych.2021.03.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Eisinger R.S., Urdaneta M.E., Foote K.D., Okun M.S., Gunduz A. Non-motor characterization of the basal ganglia: evidence from human and non-human primate electrophysiology. Front. Neurosci. 2018;12:385. doi: 10.3389/fnins.2018.00385. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Elias G.J.B., Giacobbe P., Boutet A., Germann J., Beyn M.E., Gramer R.M., Pancholi A., Joel S.E., Lozano A.M. Probing the circuitry of panic with deep brain stimulation: connectomic analysis and review of the literature. Brain Stimul. 2020;13:10–14. doi: 10.1016/j.brs.2019.09.010. [DOI] [PubMed] [Google Scholar]
- Englot D.J. A modern epilepsy surgery treatment algorithm: incorporating traditional and emerging technologies. Epilepsy Behav. 2018;80:68–74. doi: 10.1016/j.yebeh.2017.12.041. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Erez Y., Assem M., Coelho P., Romero-Garcia R., Owen M., McDonald A., Woodberry E., Morris R.C., Price S.J., Suckling J., et al. Intraoperative mapping of executive function using electrocorticography for patients with low-grade gliomas. Acta Neurochir. 2021;163:1299–1309. doi: 10.1007/s00701-020-04646-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ethier C., Oby E.R., Bauman M.J., Miller L.E. Restoration of grasp following paralysis through brain-controlled stimulation of muscles. Nature. 2012;485:368–371. doi: 10.1038/nature10987. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ewert S., Horn A., Finkel F., Li N., Kühn A.A., Herrington T.M. Optimization and comparative evaluation of nonlinear deformation algorithms for atlas-based segmentation of DBS target nuclei. Neuroimage. 2019;184:586–598. doi: 10.1016/j.neuroimage.2018.09.061. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ewert S., Plettig P., Li N., Chakravarty M.M., Collins D.L., Herrington T.M., Kühn A.A., Horn A. Toward defining deep brain stimulation targets in MNI space: a subcortical atlas based on multimodal MRI, histology and structural connectivity. Neuroimage. 2018;170:271–282. doi: 10.1016/j.neuroimage.2017.05.015. [DOI] [PubMed] [Google Scholar]
- Ferreira F., Akram H. In: Connectomic Deep Brain Stimulation. Horn A., editor. Academic Press; 2022. Chapter 19 - connectomic DBS in Parkinson’s disease, essential tremor and dystonia; pp. 405–431. [DOI] [Google Scholar]
- Fetz E.E. Are movement parameters recognizably coded in the activity of single neurons? Behav. Brain Sci. 1992;15:679–690. doi: 10.1017/S0140525X00072599. [DOI] [Google Scholar]
- Feyissa A.M., Worrell G.A., Tatum W.O., Mahato D., Brinkmann B.H., Rosenfeld S.S., ReFaey K., Bechtle P.S., Quinones-Hinojosa A. High-frequency oscillations in awake patients undergoing brain tumor-related epilepsy surgery. Neurology. 2018;90:e1119–e1125. doi: 10.1212/WNL.0000000000005216. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Fifer M.S., McMullen D.P., Osborn L.E., Thomas T.M., Christie B., Nickl R.W., Candrea D.N., Pohlmeyer E.A., Thompson M.C., Anaya M.A., et al. Intracortical somatosensory stimulation to elicit fingertip sensations in an individual with spinal cord injury. Neurology. 2022;98:e679–e687. doi: 10.1212/WNL.0000000000013173. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Flesher S.N., Collinger J.L., Foldes S.T., Weiss J.M., Downey J.E., Tyler-Kabara E.C., Bensmaia S.J., Schwartz A.B., Boninger M.L., Gaunt R.A. Intracortical microstimulation of human somatosensory cortex. Sci. Transl. Med. 2016;8:361ra141. doi: 10.1126/scitranslmed.aaf8083. [DOI] [PubMed] [Google Scholar]
- Flesher S.N., Downey J.E., Weiss J.M., Hughes C.L., Herrera A.J., Tyler-Kabara E.C., Boninger M.L., Collinger J.L., Gaunt R.A. A brain-computer interface that evokes tactile sensations improves robotic arm control. Science. 2021;372:831–836. doi: 10.1126/science.abd0380. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Flinker A., Korzeniewska A., Shestyuk A.Y., Franaszczuk P.J., Dronkers N.F., Knight R.T., Crone N.E. Redefining the role of Broca’s area in speech. Proc. Natl. Acad. Sci. USA. 2015;112:2871–2875. doi: 10.1073/pnas.1414491112. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Fox K.C.R., Foster B.L., Kucyi A., Daitch A.L., Parvizi J. Intracranial electrophysiology of the human default network. Trends Cogn. Sci. 2018;22:307–324. doi: 10.1016/j.tics.2018.02.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Freri E., Matricardi S., Gozzo F., Cossu M., Granata T., Tassi L. Perisylvian, including insular, childhood epilepsy: presurgical workup and surgical outcome. Epilepsia. 2017;58:1360–1369. doi: 10.1111/epi.13816. [DOI] [PubMed] [Google Scholar]
- Frot M., Mauguière F., Garcia-Larrea L. Insular dichotomy in the implicit detection of emotions in human faces. Cereb. Cortex. 2022:bhab477. doi: 10.1093/cercor/bhab477. [DOI] [PubMed] [Google Scholar]
- Fumagalli M., Giannicola G., Rosa M., Marceglia S., Lucchiari C., Mrakic-Sposta S., Servello D., Pacchetti C., Porta M., Sassi M., et al. Conflict-dependent dynamic of subthalamic nucleus oscillations during moral decisions. Soc. Neurosci. 2011;6:243–256. doi: 10.1080/17470919.2010.515148. [DOI] [PubMed] [Google Scholar]
- Fusi S., Miller E.K., Rigotti M. Why neurons mix: high dimensionality for higher cognition. Curr. Opin. Neurobiol. 2016;37:66–74. doi: 10.1016/j.conb.2016.01.010. [DOI] [PubMed] [Google Scholar]
- Gallego J.A., Perich M.G., Chowdhury R.H., Solla S.A., Miller L.E. Long-term stability of cortical population dynamics underlying consistent behavior. Nat. Neurosci. 2020;23:260–270. doi: 10.1038/s41593-019-0555-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gallego J.A., Perich M.G., Miller L.E., Solla S.A. Neural manifolds for the control of movement. Neuron. 2017;94:978–984. doi: 10.1016/j.neuron.2017.05.025. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gallego J.A., Perich M.G., Naufel S.N., Ethier C., Solla S.A., Miller L.E. Cortical population activity within a preserved neural manifold underlies multiple motor behaviors. Nat. Commun. 2018;9:4233–4313. doi: 10.1038/s41467-018-06560-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ganguly K., Carmena J.M. Emergence of a stable cortical map for neuroprosthetic control. PLoS Biol. 2009;7:e1000153. doi: 10.1371/journal.pbio.1000153. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ganguly K., Dimitrov D.F., Wallis J.D., Carmena J.M. Reversible large-scale modification of cortical networks during neuroprosthetic control. Nat. Neurosci. 2011;14:662–667. doi: 10.1038/nn.2797. [DOI] [PMC free article] [PubMed] [Google Scholar]
- George J.A., Kluger D.T., Davis T.S., Wendelken S.M., Okorokova E.V., He Q., Duncan C.C., Hutchinson D.T., Thumser Z.C., Beckler D.T., et al. Biomimetic sensory feedback through peripheral nerve stimulation improves dexterous use of a bionic hand. Sci. Robot. 2019;4:eaax2352. doi: 10.1126/scirobotics.aax2352. [DOI] [PubMed] [Google Scholar]
- Georgopoulos A.P., Carpenter A.F. Coding of movements in the motor cortex. Curr. Opin. Neurobiol. 2015;33:34–39. doi: 10.1016/j.conb.2015.01.012. [DOI] [PubMed] [Google Scholar]
- Georgopoulos A.P., Kalaska J.F., Caminiti R., Massey J.T. On the relations between the direction of two-dimensional arm movements and cell discharge in primate motor cortex. J. Neurosci. 1982;2:1527–1537. doi: 10.1523/JNEUROSCI.02-11-01527.1982. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Georgopoulos A.P., Kettner R.E., Schwartz A.B. Primate motor cortex and free arm movements to visual targets in three-dimensional space. II. Coding of the direction of movement by a neuronal population. J. Neurosci. 1988;8:2928–2937. doi: 10.1523/JNEUROSCI.08-08-02928.1988. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ghinda D.C., Lambert B., Lu J., Jiang N., Tsai E., Sachs A., Wu J.-S., Northoff G. Scale-Free analysis of intraoperative ECoG during awake craniotomy for glioma. Front. Oncol. 2021;10:625474. doi: 10.3389/fonc.2020.625474. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Goldstein E.D., Feyissa A.M. Brain tumor related-epilepsy. Neurol. Neurochir. Pol. 2018;52:436–447. doi: 10.1016/j.pjnns.2018.06.001. [DOI] [PubMed] [Google Scholar]
- Golub M.D., Sadtler P.T., Oby E.R., Quick K.M., Ryu S.I., Tyler-Kabara E.C., Batista A.P., Chase S.M., Yu B.M. Learning by neural reassociation. Nat. Neurosci. 2018;21:607–616. doi: 10.1038/s41593-018-0095-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Graczyk E.L., Schiefer M.A., Saal H.P., Delhaye B.P., Bensmaia S.J., Tyler D.J. The neural basis of perceived intensity in natural and artificial touch. Sci. Transl. Med. 2016;8:362ra142. doi: 10.1126/scitranslmed.aaf5187. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Greenhouse I., Gould S., Houser M., Aron A.R. Stimulation of contacts in ventral but not dorsal subthalamic nucleus normalizes response switching in Parkinson’s disease. Neuropsychologia. 2013;51:1302–1309. doi: 10.1016/j.neuropsychologia.2013.03.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Haas L.F. Hans Berger (1873-1941), Richard Caton (1842-1926), and electroencephalography. J. Neurol. Neurosurg. Psychiatry. 2003;74:9. doi: 10.1136/jnnp.74.1.9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Haynes W.I.A., Haber S.N. The organization of prefrontal-subthalamic inputs in primates provides an anatomical substrate for both functional specificity and integration: implications for basal ganglia models and deep brain stimulation. J. Neurosci. 2013;33:4804–4814. doi: 10.1523/JNEUROSCI.4674-12.2013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- He B., Astolfi L., Valdes-Sosa P.A., Marinazzo D., Palva S.O., Benar C.G., Michel C.M., Koenig T. Electrophysiological brain connectivity: theory and implementation. IEEE Trans. Biomed. Eng. 2019;66:2115–2137. doi: 10.1109/TBME.2019.2913928. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Heiden P., Heinz A., Romanczuk-Seiferth N. Pathological gambling in Parkinson’s disease: what are the risk factors and what is the role of impulsivity? Eur. J. Neurosci. 2017;45:67–72. doi: 10.1111/ejn.13396. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Helfinstein S.M., Kirwan M.L., Benson B.E., Hardin M.G., Pine D.S., Ernst M., Fox N.A. Validation of a child-friendly version of the monetary incentive delay task. Soc. Cogn. Affect. Neurosci. 2013;8:720–726. doi: 10.1093/scan/nss057. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hepp-Reymond M., Kirkpatrick-Tanner M., Gabernet L., Qi H.-X., Weber B. Context-dependent force coding in motor and premotor cortical areas. Exp. Brain Res. 1999;128:123–133. doi: 10.1007/s002210050827. [DOI] [PubMed] [Google Scholar]
- Herz D.M., Tan H., Brittain J.-S., Fischer P., Cheeran B., Green A.L., FitzGerald J., Aziz T.Z., Ashkan K., Little S., et al. Distinct mechanisms mediate speed-accuracy adjustments in cortico-subthalamic networks. Elife. 2017;6:e21481. doi: 10.7554/eLife.21481. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Herz D.M., Zavala B.A., Bogacz R., Brown P. Neural correlates of decision thresholds in the human subthalamic nucleus. Curr. Biol. 2016;26:916–920. doi: 10.1016/j.cub.2016.01.051. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hikosaka O., Ghazizadeh A., Griggs W., Amita H. Parallel basal ganglia circuits for decision making. J. Neural. Transm. 2018;125:515–529. doi: 10.1007/s00702-017-1691-1. [DOI] [PubMed] [Google Scholar]
- Hollunder B., Rajamani N., Siddiqi S.H., Finke C., Kühn A.A., Mayberg H.S., Fox M.D., Neudorfer C., Horn A. Toward personalized medicine in connectomic deep brain stimulation. Prog. Neurobiol. 2022;210:102211. doi: 10.1016/j.pneurobio.2021.102211. [DOI] [PubMed] [Google Scholar]
- Horn A., Al-Fatly B., Neumann W.-J., Neudorfer C. In: Connectomic Deep Brain Stimulation. Horn A., editor. Academic Press; 2022. Chapter 1 - connectomic DBS: an introduction; pp. 3–23. [DOI] [Google Scholar]
- Horn A., Fox M.D. Opportunities of connectomic neuromodulation. Neuroimage. 2020;221:117180. doi: 10.1016/j.neuroimage.2020.117180. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Horn A., Kühn A.A. Lead-DBS: a toolbox for deep brain stimulation electrode localizations and visualizations. Neuroimage. 2015;107:127–135. doi: 10.1016/j.neuroimage.2014.12.002. [DOI] [PubMed] [Google Scholar]
- Horn A., Li N., Dembek T.A., Kappel A., Boulay C., Ewert S., Tietze A., Husch A., Perera T., Neumann W.-J., et al. Lead-DBS v2: towards a comprehensive pipeline for deep brain stimulation imaging. Neuroimage. 2019;184:293–316. doi: 10.1016/j.neuroimage.2018.08.068. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Horn A., Neumann W.-J., Degen K., Schneider G.-H., Kühn A.A. Toward an electrophysiological “sweet spot” for deep brain stimulation in the subthalamic nucleus. Hum. Brain Mapp. 2017;38:3377–3390. doi: 10.1002/hbm.23594. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Horn A., Reich M., Vorwerk J., Li N., Wenzel G., Fang Q., Schmitz-Hübsch T., Nickl R., Kupsch A., Volkmann J., et al. Connectivity Predicts deep brain stimulation outcome in Parkinson disease: DBS outcome in PD. Ann. Neurol. 2017;82:67–78. doi: 10.1002/ana.24974. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Horn A., Wenzel G., Irmen F., Huebl J., Li N., Neumann W.-J., Krause P., Bohner G., Scheel M., Kühn A.A. Deep brain stimulation induced normalization of the human functional connectome in Parkinson’s disease. Brain. 2019;142:3129–3143. doi: 10.1093/brain/awz239. [DOI] [PubMed] [Google Scholar]
- House W.F. Cochlear implants. Ann. Otol. Rhinol. Laryngol. 1976;85:3. doi: 10.1177/00034894760850S303. [DOI] [PubMed] [Google Scholar]
- Huber D., Gutnisky D.A., Peron S., O’Connor D.H., Wiegert J.S., Tian L., Oertner T.G., Looger L.L., Svoboda K. Multiple dynamic representations in the motor cortex during sensorimotor learning. Nature. 2012;484:473–478. doi: 10.1038/nature11039. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hughes C.L., Flesher S.N., Gaunt R.A. Effects of stimulus pulse rate on somatosensory adaptation in the human cortex. Brain Stimul. 2022;15:987–995. doi: 10.1016/j.brs.2022.05.021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hughes C.L., Flesher S.N., Weiss J.M., Boninger M., Collinger J.L., Gaunt R.A. Perception of microstimulation frequency in human somatosensory cortex. Elife. 2021;10:e65128. doi: 10.7554/eLife.65128. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hughes C.L., Flesher S.N., Weiss J.M., Downey J.E., Boninger M., Collinger J.L., Gaunt R.A. Neural stimulation and recording performance in human sensorimotor cortex over 1500 days. J. Neural. Eng. 2021;18:045012. doi: 10.1088/1741-2552/ac18ad. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Iida K., Otsubo H. Stereoelectroencephalography: indication and efficacy. Neurol. Med.Chir. 2017;57:375–385. doi: 10.2176/nmc.ra.2017-0008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Irmen F., Horn A., Meder D., Neumann W.-J., Plettig P., Schneider G.-H., Siebner H.R., Kühn A.A. Sensorimotor subthalamic stimulation restores risk-reward trade-off in Parkinson’s disease. Mov. Disord. 2019;34:366–376. doi: 10.1002/mds.27576. [DOI] [PubMed] [Google Scholar]
- Irmen F., Horn A., Mosley P., Perry A., Petry-Schmelzer J.N., Dafsari H.S., Barbe M., Visser-Vandewalle V., Schneider G.-H., Li N., et al. Left prefrontal connectivity links subthalamic stimulation with depressive symptoms. Ann. Neurol. 2020;87:962–975. doi: 10.1002/ana.25734. [DOI] [PubMed] [Google Scholar]
- Irmen F., Krack P., Kühn A.A. Connectomic Deep Brain Stimulation. Elsevier; 2022. Investigating cognitive neuroscience concepts using connectomic DBS; pp. 483–504. [DOI] [Google Scholar]
- Jahangiri F.R., Chima G.S., Pearson M., Jackson J., Siddiqui A.A. Mapping of the language cortex. Cureus. 2021;13:e14960. doi: 10.7759/cureus.14960. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jahanshahi M., Obeso I., Rothwell J.C., Obeso J.A. A fronto–striato–subthalamic–pallidal network for goal-directed and habitual inhibition. Nat. Rev. Neurosci. 2015;16:719–732. doi: 10.1038/nrn4038. [DOI] [PubMed] [Google Scholar]
- Jarosiewicz B., Chase S.M., Fraser G.W., Velliste M., Kass R.E., Schwartz A.B. Functional network reorganization during learning in a brain-computer interface paradigm. Proc. Natl. Acad. Sci. USA. 2008;105:19486–19491. doi: 10.1073/pnas.0808113105. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jensen K.T., Harpaz N.K., Dhawale A.K., Wolff S.B.E., Ölveczky B.P. Long-term stability of single neuron activity in the motor system (preprint) Neuroscience. 2021 doi: 10.1101/2021.10.27.465945. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Johansson R.S., Flanagan J.R. Coding and use of tactile signals from the fingertips in object manipulation tasks. Nat. Rev. Neurosci. 2009;10:345–359. doi: 10.1038/nrn2621. [DOI] [PubMed] [Google Scholar]
- Johnson K.A., Duffley G., Anderson D.N., Ostrem J.L., Welter M.-L., Baldermann J.C., Kuhn J., Huys D., Visser-Vandewalle V., Foltynie T., et al. Structural connectivity predicts clinical outcomes of deep brain stimulation for Tourette syndrome. Brain. 2020;143:2607–2623. doi: 10.1093/brain/awaa188. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kalaska J.F., Cohen D.A., Hyde M.L., Prud’Homme M. A comparison of movement direction-related versus load direction-related activity in primate motor cortex, using a two-dimensional reaching task. J. Neurosci. 1989;9:2080–2102. doi: 10.1523/JNEUROSCI.09-06-02080.1989. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kalidindi H.T., Cross K.P., Lillicrap T.P., Omrani M., Falotico E., Sabes P.N., Scott S.H. Rotational dynamics in motor cortex are consistent with a feedback controller. Elife. 2021;10:e67256. doi: 10.7554/eLife.67256. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kao J.C., Nuyujukian P., Ryu S.I., Churchland M.M., Cunningham J.P., Shenoy K.V. Single-trial dynamics of motor cortex and their applications to brain-machine interfaces. Nat. Commun. 2015;6:7759. doi: 10.1038/ncomms8759. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kao T.-C., Hennequin G. Neuroscience out of control: control-theoretic perspectives on neural circuit dynamics. Curr. Opin. Neurobiol. 2019;58:122–129. doi: 10.1016/j.conb.2019.09.001. [DOI] [PubMed] [Google Scholar]
- Karas P.J., Lee S., Jimenez-Shahed J., Goodman W.K., Viswanathan A., Sheth S.A. Deep brain stimulation for obsessive compulsive disorder: evolution of surgical stimulation target parallels changing model of dysfunctional brain circuits. Front. Neurosci. 2019;12:998. doi: 10.3389/fnins.2018.00998. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Katlowitz K.A., Picardo M.A., Long M.A. Stable sequential activity underlying the maintenance of a precisely executed skilled behavior. Neuron. 2018;98:1133–1140.e3. doi: 10.1016/j.neuron.2018.05.017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kawai R., Markman T., Poddar R., Ko R., Fantana A.L., Dhawale A.K., Kampff A.R., Ölveczky B.P. Motor cortex is required for learning but not for executing a motor skill. Neuron. 2015;86:800–812. doi: 10.1016/j.neuron.2015.03.024. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kim J., Kim Y., Nakajima R., Shin A., Jeong M., Park A.H., Jeong Y., Jo S., Yang S., Park H., et al. Inhibitory basal ganglia inputs induce excitatory motor signals in the thalamus. Neuron. 2017;95:1181–1196.e8. doi: 10.1016/j.neuron.2017.08.028. [DOI] [PubMed] [Google Scholar]
- Klimes P., Peter-Derex L., Hall J., Dubeau F., Frauscher B. Spatio-temporal spike dynamics predict surgical outcome in adult focal epilepsy. Clin. Neurophysiol. 2022;134:88–99. doi: 10.1016/j.clinph.2021.10.023. [DOI] [PubMed] [Google Scholar]
- Komiyama T., Sato T.R., O’Connor D.H., Zhang Y.-X., Huber D., Hooks B.M., Gabitto M., Svoboda K. Learning-related fine-scale specificity imaged in motor cortex circuits of behaving mice. Nature. 2010;464:1182–1186. doi: 10.1038/nature08897. [DOI] [PubMed] [Google Scholar]
- Koralek A.C., Costa R.M., Carmena J.M. Temporally precise cell-specific coherence develops in corticostriatal networks during learning. Neuron. 2013;79:865–872. doi: 10.1016/j.neuron.2013.06.047. [DOI] [PubMed] [Google Scholar]
- Koralek A.C., Jin X., Long J.D., II, Costa R.M., Carmena J.M. Corticostriatal plasticity is necessary for learning intentional neuroprosthetic skills. Nature. 2012;483:331–335. doi: 10.1038/nature10845. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Korzeniewska A., Franaszczuk P.J., Crainiceanu C.M., Kuś R., Crone N.E. Dynamics of large-scale cortical interactions at high gamma frequencies during word production: event related causality (ERC) analysis of human electrocorticography (ECoG) Neuroimage. 2011;56:2218–2237. doi: 10.1016/j.neuroimage.2011.03.030. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Krack P., Pollak P., Limousin P., Hoffmann D., Benazzouz A., Le Bas J.F., Koudsie A., Benabid A.L. Opposite motor effects of pallidal stimulation in Parkinson's disease. Ann. Neurol. 1998;43:180–192. doi: 10.1002/ana.410430208. [DOI] [PubMed] [Google Scholar]
- Kravitz A.V., Freeze B.S., Parker P.R.L., Kay K., Thwin M.T., Deisseroth K., Kreitzer A.C. Regulation of parkinsonian motor behaviours by optogenetic control of basal ganglia circuitry. Nature. 2010;466:622–626. doi: 10.1038/nature09159. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kucyi A., Daitch A., Raccah O., Zhao B., Zhang C., Esterman M., Zeineh M., Halpern C.H., Zhang K., Zhang J., Parvizi J. Electrophysiological dynamics of antagonistic brain networks reflect attentional fluctuations. Nat. Commun. 2020;11:325. doi: 10.1038/s41467-019-14166-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kurtzer I., Herter T.M., Scott S.H. Random change in cortical load representation suggests distinct control of posture and movement. Nat. Neurosci. 2005;8:498–504. doi: 10.1038/nn1420. [DOI] [PubMed] [Google Scholar]
- Lange N., Schleifer S., Berndt M., Jörger A.K., Wagner A., Krieg S.M., Jordan D., Bretschneider M., Ryang Y.-M., Meyer B., Gempt J. Permutation entropy in intraoperative ECoG of brain tumour patients in awake tumour surgery- a robust parameter to separate consciousness from unconsciousness. Sci. Rep. 2019;9:16482. doi: 10.1038/s41598-019-52949-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lebedev M.A., Carmena J.M., O’Doherty J.E., Zacksenhouse M., Henriquez C.S., Principe J.C., Nicolelis M.A.L. Cortical ensemble adaptation to represent velocity of an artificial actuator controlled by a brain-machine interface. J. Neurosci. 2005;25:4681–4693. doi: 10.1523/JNEUROSCI.4088-04.2005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Li J., Cao D., Dimakopoulos V., Shi W., Yu S., Fan L., Stieglitz L., Imbach L., Sarnthein J., Jiang T. Anterior–posterior hippocampal dynamics support working memory processing. J. Neurosci. 2022;42:443–453. doi: 10.1523/JNEUROSCI.1287-21.2021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Li N., Baldermann J.C., Kibleur A., Treu S., Akram H., Elias G.J.B., Boutet A., Lozano A.M., Al-Fatly B., Strange B., et al. A unified connectomic target for deep brain stimulation in obsessive-compulsive disorder. Nat. Commun. 2020;11:3364. doi: 10.1038/s41467-020-16734-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Limousin P., Pollak P., Benazzouz A., Hoffmann D., Le Bas J.F., Broussolle E., Perret J.E., Benabid A.L. Effect of parkinsonian signs and symptoms of bilateral subthalamic nucleus stimulation. Lancet. 1995;345:91–95. doi: 10.1016/s0140-6736(95)90062-4. [DOI] [PubMed] [Google Scholar]
- Lipski W.J., Alhourani A., Pirnia T., Jones P.W., Dastolfo-Hromack C., Helou L.B., Crammond D.J., Shaiman S., Dickey M.W., Holt L.L., et al. Subthalamic nucleus neurons differentially encode early and late aspects of speech production. J. Neurosci. 2018;38:5620–5631. doi: 10.1523/JNEUROSCI.3480-17.2018. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lipski W.J., Wozny T.A., Alhourani A., Kondylis E.D., Turner R.S., Crammond D.J., Richardson R.M. Dynamics of human subthalamic neuron phase-locking to motor and sensory cortical oscillations during movement. J. Neurophysiol. 2017;118:1472–1487. doi: 10.1152/jn.00964.2016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Little S., Brown P. Debugging adaptive deep brain stimulation for Parkinson’s disease. Mov. Disord. 2020;35:555–561. doi: 10.1002/mds.27996. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Little S., Brown P. The functional role of beta oscillations in Parkinson’s disease. Parkinsonism Relat. Disord. 2014;20:S44–S48. doi: 10.1016/S1353-8020(13)70013-0. [DOI] [PubMed] [Google Scholar]
- Little S., Pogosyan A., Neal S., Zavala B., Zrinzo L., Hariz M., Foltynie T., Limousin P., Ashkan K., FitzGerald J., et al. Adaptive deep brain stimulation in advanced Parkinson disease. Ann. Neurol. 2013;74:449–457. doi: 10.1002/ana.23951. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Liu Y., Razavi Hesabi Z., Cook M., Kuhlmann L. Epileptic seizure onset predicts its duration. Eur. J. Neurol. 2022;29:375–381. doi: 10.1111/ene.15166. [DOI] [PubMed] [Google Scholar]
- Lofredi R., Auernig G.C., Irmen F., Nieweler J., Neumann W.-J., Horn A., Schneider G.-H., Kühn A.A. Subthalamic stimulation impairs stopping of ongoing movements. Brain. 2020;144:44–52. doi: 10.1093/brain/awaa341. [DOI] [PubMed] [Google Scholar]
- Lozano A.M., Lipsman N., Bergman H., Brown P., Chabardes S., Chang J.W., Matthews K., McIntyre C.C., Schlaepfer T.E., Schulder M., et al. Deep brain stimulation: current challenges and future directions. Nat. Rev. Neurol. 2019;15:148–160. doi: 10.1038/s41582-018-0128-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Luo S., Rabbani Q., Crone N.E. Brain-computer interface: applications to speech decoding and synthesis to augment communication. Neurotherapeutics. 2022;19:263–273. doi: 10.1007/s13311-022-01190-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Magrassi L., Aromataris G., Cabrini A., Annovazzi-Lodi V., Moro A. Sound representation in higher language areas during language generation. Proc. Natl. Acad. Sci. USA. 2015;112:1868–1873. doi: 10.1073/pnas.1418162112. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Makin T.R., Bensmaia S.J. Stability of sensory topographies in adult cortex. Trends Cogn. Sci. 2017;21:195–204. doi: 10.1016/j.tics.2017.01.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Makino H., Ren C., Liu H., Kim A.N., Kondapaneni N., Liu X., Kuzum D., Komiyama T. Transformation of cortex-wide emergent properties during motor learning. Neuron. 2017;94:880–890.e8. doi: 10.1016/j.neuron.2017.04.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Manssuer L., Qiong D., Wei L., Yang R., Zhang C., Zhao Y., Sun B., Zhan S., Voon V. Integrated amygdala, orbitofrontal and hippocampal contributions to reward and loss coding revealed with human intracranial EEG. J. Neurosci. 2022;42:2756–2771. doi: 10.1523/JNEUROSCI.1717-21.2022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Marceglia S., Rosa M., Servello D., Porta M., Barbieri S., Moro E., Priori A. Adaptive deep brain stimulation (aDBS) for tourette syndrome. Brain Sci. 2017;8:4. doi: 10.3390/brainsci8010004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mariani V., Balestrini S., Gozzo F., Pelliccia V., Mai R., Francione S., Sartori I., Cardinale F., Tassi L. Intracerebral electrical stimulations of the temporal lobe: a stereoelectroencephalography study. Eur. J. Neurosci. 2021;54:5368–5383. doi: 10.1111/ejn.15377. [DOI] [PubMed] [Google Scholar]
- Masamizu Y., Tanaka Y.R., Tanaka Y.H., Hira R., Ohkubo F., Kitamura K., Isomura Y., Okada T., Matsuzaki M. Two distinct layer-specific dynamics of cortical ensembles during learning of a motor task. Nat. Neurosci. 2014;17:987–994. doi: 10.1038/nn.3739. [DOI] [PubMed] [Google Scholar]
- Mathis M.W., Mathis A., Uchida N. Somatosensory cortex plays an essential role in forelimb motor adaptation in mice. Neuron. 2017;93:1493–1503.e6. doi: 10.1016/j.neuron.2017.02.049. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Matsumoto R., Kunieda T. In: Invasive Studies of the Human Epileptic Brain - Principles and Practice. Lhatoo S., Kahane P., Lüders H., editors. Oxford University Press; 2019. Cortico-cortical evoked potentials mapping; pp. 431–452. [Google Scholar]
- Matsumoto R., Nair D.R., LaPresto E., Najm I., Bingaman W., Shibasaki H., Lüders H.O. Functional connectivity in the human language system: a cortico-cortical evoked potential study. Brain. 2004;127:2316–2330. doi: 10.1093/brain/awh246. [DOI] [PubMed] [Google Scholar]
- Mazzoni A., Oddo C.M., Valle G., Camboni D., Strauss I., Barbaro M., Barabino G., Puddu R., Carboni C., Bisoni L., et al. Morphological neural computation restores discrimination of naturalistic textures in trans-radial amputees. Sci. Rep. 2020;10:527. doi: 10.1038/s41598-020-57454-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mazzoni A., Rosa M., Carpaneto J., Romito L.M., Priori A., Micera S. Subthalamic neural activity patterns anticipate economic risk decisions in gambling. eNeuro. 2018;5 doi: 10.1523/ENEURO.0366-17.2017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McCrimmon C.M., Wang P.T., Heydari P., Nguyen A., Shaw S.J., Gong H., Chui L.A., Liu C.Y., Nenadic Z., Do A.H. Electrocorticographic encoding of human gait in the leg primary motor cortex. Cereb. Cortex. 2018;28:2752–2762. doi: 10.1093/cercor/bhx155. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Meidahl A.C., Tinkhauser G., Herz D.M., Cagnan H., Debarros J., Brown P. Adaptive deep brain stimulation for movement disorders: the long road to clinical therapy: adaptive DBS review. Mov. Disord. 2017;32:810–819. doi: 10.1002/mds.27022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Merk T., Peterson V., Lipski W.J., Blankertz B., Turner R.S., Li N., Horn A., Richardson R.M., Neumann W.-J. Electrocorticography is superior to subthalamic local field potentials for movement decoding in Parkinson’s disease. Elife. 2022;11:e75126. doi: 10.7554/eLife.75126. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Micera S., Caleo M., Chisari C., Hummel F.C., Pedrocchi A. Advanced neurotechnologies for the restoration of motor function. Neuron. 2020;105:604–620. doi: 10.1016/j.neuron.2020.01.039. [DOI] [PubMed] [Google Scholar]
- Micheli F., Vissani M., Pecchioli G., Terenzi F., Ramat S., Mazzoni A. Impulsivity markers in parkinsonian subthalamic single-unit activity. Mov. Disord. 2021;36:1435–1440. doi: 10.1002/mds.28497. [DOI] [PubMed] [Google Scholar]
- Milosevic L., Scherer M., Cebi I., Guggenberger R., Machetanz K., Naros G., Weiss D., Gharabaghi A. Online mapping with the deep brain stimulation lead: a novel targeting tool in Parkinson’s disease. Mov. Disord. 2020;35:1574–1586. doi: 10.1002/mds.28093. [DOI] [PubMed] [Google Scholar]
- Miocinovic S., Noecker A.M., Maks C.B., Butson C.R., McIntyre C.C. Cicerone: stereotactic neurophysiological recording and deep brain stimulation electrode placement software system. Acta Neurochir. Suppl. 2007;97:561–567. doi: 10.1007/978-3-211-33081-4_65. [DOI] [PubMed] [Google Scholar]
- Mirandola L., Mai R.F., Francione S., Pelliccia V., Gozzo F., Sartori I., Nobili L., Cardinale F., Cossu M., Meletti S., Tassi L. Stereo-EEG: diagnostic and therapeutic tool for periventricular nodular heterotopia epilepsies. Epilepsia. 2017;58:1962–1971. doi: 10.1111/epi.13895. [DOI] [PubMed] [Google Scholar]
- Mitsuhashi T., Sonoda M., Firestone E., Sakakura K., Jeong J.-W., Luat A.F., Sood S., Asano E. Temporally and functionally distinct large-scale brain network dynamics supporting task switching. Neuroimage. 2022;254:119126. doi: 10.1016/j.neuroimage.2022.119126. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Miyachi S., Hikosaka O., Miyashita K., Kárádi Z., Rand M.K. Differential roles of monkey striatum in learning of sequential hand movement. Exp. Brain Res. 1997;115:1–5. doi: 10.1007/PL00005669. [DOI] [PubMed] [Google Scholar]
- Montgomery E.B. Second edition. Oxford University Press; 2017. Deep Brain Stimulation Programming: Mechanisms, Principles, and Practice. [Google Scholar]
- Montgomery E.B., Jr. Oxford University Press; 2014. Intraoperative Neurophysiological Monitoring for Deep Brain Stimulation: Principles, Practice and Cases. [DOI] [Google Scholar]
- Moore W. The Edwin Smith papyrus. BMJ. 2011;342:d1598. doi: 10.1136/bmj.d1598. [DOI] [Google Scholar]
- Morrow M.M., Jordan L.R., Miller L.E. Direct comparison of the task-dependent discharge of M1 in hand space and muscle space. J. Neurophysiol. 2007;97:1786–1798. doi: 10.1152/jn.00150.2006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mosher C.P., Mamelak A.N., Malekmohammadi M., Pouratian N., Rutishauser U. Distinct roles of dorsal and ventral subthalamic neurons in action selection and cancellation. Neuron. 2021;109:869–881.e6. doi: 10.1016/j.neuron.2020.12.025. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mosley P.E., Paliwal S., Robinson K., Coyne T., Silburn P., Tittgemeyer M., Stephan K.E., Perry A., Breakspear M. The structural connectivity of subthalamic deep brain stimulation correlates with impulsivity in Parkinson’s. Brain. 2020;143:2235–2254. doi: 10.1093/brain/awaa148. [DOI] [PubMed] [Google Scholar]
- Mosley P.E., Smith D., Coyne T., Silburn P., Breakspear M., Perry A. The site of stimulation moderates neuropsychiatric symptoms after subthalamic deep brain stimulation for Parkinson’s disease. Neuroimage. Clin. 2018;18:996–1006. doi: 10.1016/j.nicl.2018.03.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mountcastle V.B. Comprehensive Physiology. John Wiley & Sons, Ltd; 2011. Central nervous mechanisms in mechanoreceptive sensibility; pp. 789–878. [DOI] [Google Scholar]
- Murphy E., Woolnough O., Rollo P.S., Roccaforte Z.J., Segaert K., Hagoort P., Tandon N. Minimal phrase composition revealed by intracranial recordings. J. Neurosci. 2022;42:3216–3227. doi: 10.1523/JNEUROSCI.1575-21.2022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Nature editorial Mind meld. Nature. 2015;525:289–290. doi: 10.1038/525289b. [DOI] [PubMed] [Google Scholar]
- Neely R.M., Koralek A.C., Athalye V.R., Costa R.M., Carmena J.M. Volitional modulation of primary visual cortex activity requires the basal ganglia. Neuron. 2018;97:1356–1368.e4. doi: 10.1016/j.neuron.2018.01.051. [DOI] [PubMed] [Google Scholar]
- Neudorfer C., Elias G.J.B., Jakobs M., Boutet A., Germann J., Narang K., Loh A., Paff M., Horn A., Kucharczyk W., et al. Mapping autonomic, mood and cognitive effects of hypothalamic region deep brain stimulation. Brain. 2021;144:2837–2851. doi: 10.1093/brain/awab170. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Neudorfer C., Kroneberg D., Al-Fatly B., Goede L., Kübler D., Faust K., van Rienen U., Tietze A., Picht T., Herrington T.M., et al. Personalizing deep brain stimulation using advanced imaging sequences. Ann. Neurol. 2022;91:613–628. doi: 10.1002/ana.26326. [DOI] [PubMed] [Google Scholar]
- Nguyen T.A.K., Schüpbach M., Mercanzini A., Dransart A., Pollo C. Directional local field potentials in the subthalamic nucleus during deep brain implantation of Parkinson’s disease patients. Front. Hum. Neurosci. 2020;14:521282. doi: 10.3389/fnhum.2020.521282. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Nicolelis M.A.L. Brain–machine interfaces to restore motor function and probe neural circuits. Nat. Rev. Neurosci. 2003;4:417–422. doi: 10.1038/nrn1105. [DOI] [PubMed] [Google Scholar]
- Norman Y., Raccah O., Liu S., Parvizi J., Malach R. Hippocampal ripples and their coordinated dialogue with the default mode network during recent and remote recollection. Neuron. 2021;109:2767–2780.e5. doi: 10.1016/j.neuron.2021.06.020. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Oby E.R., Golub M.D., Hennig J.A., Degenhart A.D., Tyler-Kabara E.C., Yu B.M., Chase S.M., Batista A.P. New neural activity patterns emerge with long-term learning. Proc. Natl. Acad. Sci. USA. 2019;116:15210–15215. doi: 10.1073/pnas.1820296116. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Oddo C.M., Raspopovic S., Artoni F., Mazzoni A., Spigler G., Petrini F., Giambattistelli F., Vecchio F., Miraglia F., Zollo L., et al. Intraneural stimulation elicits discrimination of textural features by artificial fingertip in intact and amputee humans. Elife. 2016;5:e09148. doi: 10.7554/eLife.09148. [DOI] [PMC free article] [PubMed] [Google Scholar]
- O’Doherty J.E., Lebedev M.A., Ifft P.J., Zhuang K.Z., Shokur S., Bleuler H., Nicolelis M.A.L. Active tactile exploration using a brain–machine–brain interface. Nature. 2011;479:228–231. doi: 10.1038/nature10489. [DOI] [PMC free article] [PubMed] [Google Scholar]
- O’Doherty J.E., Lebedev M.A., Li Z., Nicolelis M.A.L. Virtual active touch using randomly patterned intracortical microstimulation. IEEE Trans. Neural Syst. Rehabil. Eng. 2012;20:85–93. doi: 10.1109/TNSRE.2011.2166807. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Okorokova E.V., Goodman J.M., Hatsopoulos N.G., Bensmaia S.J. Decoding hand kinematics from population responses in sensorimotor cortex during grasping. J. Neural. Eng. 2020;17:046035. doi: 10.1088/1741-2552/ab95ea. [DOI] [PubMed] [Google Scholar]
- Osborn L.E., Christie B.P., McMullen D.P., Nickl R.W., Thompson M.C., Pawar A.S., Thomas T.M., Alejandro Anaya M., Crone N.E., Wester B.A., et al. 2021 43rd Annual International Conference of the IEEE Engineering in Medicine & Biology Society (EMBC). Presented at the 2021 43rd Annual International Conference of the IEEE Engineering in Medicine & Biology Society (EMBC) IEEE; 2021. Intracortical microstimulation of somatosensory cortex enables object identification through perceived sensations; pp. 6259–6262. [DOI] [PubMed] [Google Scholar]
- Pandarinath C., Bensmaia S.J. The science and engineering behind sensitized brain-controlled bionic hands. Physiol. Rev. 2022;102:551–604. doi: 10.1152/physrev.00034.2020. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Park S.H., Jung I.H., Chang K.W., Oh M.K., Chang J.W., Kim S.H., Kang H.-C., Kim H.D., Chang W.S. Epidural grid, a new methodology of invasive intracranial EEG monitoring: a technical note and experience of a single center. Epilepsy Res. 2022;182:106912. doi: 10.1016/j.eplepsyres.2022.106912. [DOI] [PubMed] [Google Scholar]
- Parvizi J., Braga R.M., Kucyi A., Veit M.J., Pinheiro-Chagas P., Perry C., Sava-Segal C., Zeineh M., van Staalduinen E.K., Henderson J.M., Markert M. Altered sense of self during seizures in the posteromedial cortex. Proc. Natl. Acad. Sci. USA. 2021;118 doi: 10.1073/pnas.2100522118. e2100522118. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Parvizi J., Kastner S. Promises and limitations of human intracranial electroencephalography. Nat. Neurosci. 2018;21:474–483. doi: 10.1038/s41593-018-0108-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pedrosa D.J., Brown P., Cagnan H., Visser-Vandewalle V., Wirths J., Timmermann L., Brittain J.-S. A functional micro-electrode mapping of ventral thalamus in essential tremor. Brain. 2018;141:2644–2654. doi: 10.1093/brain/awy192. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pelliccia V., Villani F., Gozzo F., Gnatkovsky V., Cardinale F., Tassi L. Musicogenic epilepsy: a Stereo-electroencephalography study. Cortex. 2019;120:582–587. doi: 10.1016/j.cortex.2019.02.005. [DOI] [PubMed] [Google Scholar]
- Penfield W., Boldrey E. Somatic motor and sensory representation in the cerebral cortex of man as studied by electrical stimulation. Brain. 1937;60:389–443. doi: 10.1093/brain/60.4.389. [DOI] [Google Scholar]
- Penfield W., Perot P. The brain’s record of auditory and visual experience: a final summary and discussion. Brain. 1963;86:595–696. doi: 10.1093/brain/86.4.595. [DOI] [PubMed] [Google Scholar]
- Penfield W., Rasmussen T. The cerebral cortex of man: a clinical study of localization of function. J. Am. Med. Assoc. 1950;144:1412. doi: 10.1001/jama.1950.02920160086033. [DOI] [Google Scholar]
- Peng S.-J., Wong T.-T., Huang C.-C., Chang H., Hsieh K.L.-C., Tsai M.-L., Yang Y.-S., Chen C.-L. Quantitative analysis of intraoperative electrocorticography mirrors histopathology and seizure outcome after epileptic surgery in children. J. Formos. Med. Assoc. 2021;120:1500–1511. doi: 10.1016/j.jfma.2020.11.001. [DOI] [PubMed] [Google Scholar]
- Peters A.J., Chen S.X., Komiyama T. Emergence of reproducible spatiotemporal activity during motor learning. Nature. 2014;510:263–267. doi: 10.1038/nature13235. [DOI] [PubMed] [Google Scholar]
- Peters M.E., Ammar W., Bhagavatula C., Power R. Proceedings of the 55th Annual Meeting of the Association for Computational Linguistics (Volume 1: Long Papers) Association for Computational Linguistics; 2017. Semi-supervised sequence tagging with bidirectional language models; pp. 1756–1765. [DOI] [Google Scholar]
- Petrini F.M., Valle G., Strauss I., Granata G., Di Iorio R., D’Anna E., Čvančara P., Mueller M., Carpaneto J., Clemente F., et al. Six-month assessment of a hand prosthesis with intraneural tactile feedback: hand prosthesis. Ann. Neurol. 2019;85:137–154. doi: 10.1002/ana.25384. [DOI] [PubMed] [Google Scholar]
- Petry-Schmelzer J.N., Krause M., Dembek T.A., Horn A., Evans J., Ashkan K., Rizos A., Silverdale M., Schumacher W., Sack C., et al. Non-motor outcomes depend on location of neurostimulation in Parkinson’s disease. Brain. 2019;142:3592–3604. doi: 10.1093/brain/awz285. [DOI] [PubMed] [Google Scholar]
- Piccolino M. Animal electricity and the birth of electrophysiology: the legacy of Luigi Galvani. Brain Res. Bull. 1998;46:381–407. doi: 10.1016/S0361-9230(98)00026-4. [DOI] [PubMed] [Google Scholar]
- Pinheiro-Chagas P., Daitch A., Parvizi J., Dehaene S. Brain mechanisms of arithmetic: a crucial role for ventral temporal cortex. J. Cogn. Neurosci. 2018;30:1757–1772. doi: 10.1162/jocn_a_01319. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pollo C., Kaelin-Lang A., Oertel M.F., Stieglitz L., Taub E., Fuhr P., Lozano A.M., Raabe A., Schüpbach M. Directional deep brain stimulation: an intraoperative double-blind pilot study. Brain. 2014;137:2015–2026. doi: 10.1093/brain/awu102. [DOI] [PubMed] [Google Scholar]
- Ponce F.A., Foote K.D., Lozano A.M. Introduction. Deep brain stimulation in 2018. Neurosurg. Focus. 2018;45:E1. doi: 10.3171/2018.5.FOCUS18248. [DOI] [PubMed] [Google Scholar]
- Pool J.L. Psychosurgery in older people. J. Am. Geriatr. Soc. 1954;2:456–466. doi: 10.1111/j.1532-5415.1954.tb02138.x. [DOI] [PubMed] [Google Scholar]
- Priori A., Foffani G., Rossi L., Marceglia S. Adaptive deep brain stimulation (aDBS) controlled by local field potential oscillations. Exp. Neurol. 2013;245:77–86. doi: 10.1016/j.expneurol.2012.09.013. [DOI] [PubMed] [Google Scholar]
- Quitadamo L.R., Mai R., Gozzo F., Pelliccia V., Cardinale F., Seri S. Kurtosis-based detection of intracranial high-frequency oscillations for the identification of the seizure onset zone. Int. J. Neural Syst. 2018;28:1850001. doi: 10.1142/S0129065718500016. [DOI] [PubMed] [Google Scholar]
- Raccah O., Daitch A.L., Kucyi A., Parvizi J. Direct cortical recordings suggest temporal order of task-evoked responses in human dorsal attention and default networks. J. Neurosci. 2018;38:10305–10313. doi: 10.1523/JNEUROSCI.0079-18.2018. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ramos-Escobar N., Mercier M., Trébuchon-Fonséca A., Rodriguez-Fornells A., François C., Schön D. Hippocampal and auditory contributions to speech segmentation. Cortex. 2022;150:1–11. doi: 10.1016/j.cortex.2022.01.017. [DOI] [PubMed] [Google Scholar]
- Raspopovic S., Capogrosso M., Petrini F.M., Bonizzato M., Rigosa J., Di Pino G., Carpaneto J., Controzzi M., Boretius T., Fernandez E., et al. Restoring natural sensory feedback in real-time bidirectional hand prostheses. Sci. Transl. Med. 2014;6:222ra19. doi: 10.1126/scitranslmed.3006820. [DOI] [PubMed] [Google Scholar]
- Riès S.K., Dhillon R.K., Clarke A., King-Stephens D., Laxer K.D., Weber P.B., Kuperman R.A., Auguste K.I., Brunner P., Schalk G., et al. Spatiotemporal dynamics of word retrieval in speech production revealed by cortical high-frequency band activity. Proc. Natl. Acad. Sci. USA. 2017;114:E4530–E4538. doi: 10.1073/pnas.1620669114. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rigotti M., Barak O., Warden M.R., Wang X.-J., Daw N.D., Miller E.K., Fusi S. The importance of mixed selectivity in complex cognitive tasks. Nature. 2013;497:585–590. doi: 10.1038/nature12160. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rioult-Pedotti M.-S., Friedman D., Hess G., Donoghue J.P. Strengthening of horizontal cortical connections following skill learning. Nat. Neurosci. 1998;1:230–234. doi: 10.1038/678. [DOI] [PubMed] [Google Scholar]
- Riva-Posse P., Choi K.S., Holtzheimer P.E., Crowell A.L., Garlow S.J., Rajendra J.K., McIntyre C.C., Gross R.E., Mayberg H.S. A connectomic approach for subcallosal cingulate deep brain stimulation surgery: prospective targeting in treatment-resistant depression. Mol. Psychiatry. 2018;23:843–849. doi: 10.1038/mp.2017.59. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Robertson F.C., Ullrich N.J., Manley P.E., Al-Sayegh H., Ma C., Goumnerova L.C. The impact of intraoperative electrocorticography on seizure outcome after resection of pediatric brain tumors: a cohort study. Neurosurgery. 2019;85:375–383. doi: 10.1093/neuros/nyy342. [DOI] [PubMed] [Google Scholar]
- Rodriguez-Oroz M.C., López-Azcárate J., Garcia-Garcia D., Alegre M., Toledo J., Valencia M., Guridi J., Artieda J., Obeso J.A. Involvement of the subthalamic nucleus in impulse control disorders associated with Parkinson’s disease. Brain. 2011;134:36–49. doi: 10.1093/brain/awq301. [DOI] [PubMed] [Google Scholar]
- Roelfsema P.R., Denys D., Klink P.C. Mind reading and writing: the future of neurotechnology. Trends Cogn. Sci. 2018;22:598–610. doi: 10.1016/j.tics.2018.04.001. [DOI] [PubMed] [Google Scholar]
- Romanelli P., Heit G., Hill B.C., Kraus A., Hastie T., Brontë-Stewart H.M. Microelectrode recording revealing a somatotopic body map in the subthalamic nucleus in humans with Parkinson disease. J. Neurosurg. 2004;100:611–618. doi: 10.3171/jns.2004.100.4.0611. [DOI] [PubMed] [Google Scholar]
- Romeni S., Valle G., Mazzoni A., Micera S. Tutorial: a computational framework for the design and optimization of peripheral neural interfaces. Nat. Protoc. 2020;15:3129–3153. doi: 10.1038/s41596-020-0377-6. [DOI] [PubMed] [Google Scholar]
- Rosa M., Arlotti M., Ardolino G., Cogiamanian F., Marceglia S., Di Fonzo A., Cortese F., Rampini P.M., Priori A. Adaptive deep brain stimulation in a freely moving parkinsonian patient. Mov. Disord. 2015;30:1003–1005. doi: 10.1002/mds.26241. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rosa M., Fumagalli M., Giannicola G., Marceglia S., Lucchiari C., Servello D., Franzini A., Pacchetti C., Romito L., Albanese A., et al. Pathological gambling in Parkinson’s disease: subthalamic oscillations during economics decisions: STN Oscillations in Gambling. Mov. Disord. 2013;28:1644–1652. doi: 10.1002/mds.25427. [DOI] [PubMed] [Google Scholar]
- Rossi P.J., Shute J.B., Opri E., Molina R., Peden C., Castellanos O., Foote K.D., Gunduz A., Okun M.S. Impulsivity in Parkinson’s disease is associated with altered subthalamic but not globus pallidus internus activity. J. Neurol. Neurosurg. Psychiatry. 2017;88:968–970. doi: 10.1136/jnnp-2016-315325. [DOI] [PubMed] [Google Scholar]
- Rugg-Gunn F., Miserocchi A., McEvoy A. Epilepsy surgery. Pract. Neurol. 2020;20:4–14. doi: 10.1136/practneurol-2019-002192. [DOI] [PubMed] [Google Scholar]
- Russo A.A., Bittner S.R., Perkins S.M., Seely J.S., London B.M., Lara A.H., Miri A., Marshall N.J., Kohn A., Jessell T.M., et al. Motor cortex embeds muscle-like commands in an untangled population response. Neuron. 2018;97:953–966.e8. doi: 10.1016/j.neuron.2018.01.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Saal H.P., Bensmaia S.J. Biomimetic approaches to bionic touch through a peripheral nerve interface. Neuropsychologia. 2015;79:344–353. doi: 10.1016/j.neuropsychologia.2015.06.010. [DOI] [PubMed] [Google Scholar]
- Sadtler P.T., Quick K.M., Golub M.D., Chase S.M., Ryu S.I., Tyler-Kabara E.C., Yu B.M., Batista A.P. Neural constraints on learning. Nature. 2014;512:423–426. doi: 10.1038/nature13665. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Saez I., Lin J., Stolk A., Chang E., Parvizi J., Schalk G., Knight R.T., Hsu M. Encoding of multiple reward-related computations in transient and sustained high-frequency activity in human OFC. Curr. Biol. 2018;28:2889–2899.e3. doi: 10.1016/j.cub.2018.07.045. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Saito T., Tamura M., Chernov M.F., Ikuta S., Muragaki Y., Maruyama T. Neurophysiological monitoring and awake craniotomy for resection of intracranial gliomas. Prog. Neurol. Surg. 2018;30:117–158. doi: 10.1159/000464387. [DOI] [PubMed] [Google Scholar]
- Salami P., Borzello M., Kramer M.A., Westover M.B., Cash S.S. Quantifying seizure termination patterns reveals limited pathways to seizure end. Neurobiol. Dis. 2022;165:105645. doi: 10.1016/j.nbd.2022.105645. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sandbrink K.J., Mamidanna P., Michaelis C., Bethge M., Mathis M.W., Mathis A. Contrasting action and posture coding with hierarchical deep neural network models of proprioception (preprint) Neuroscience. 2020 doi: 10.1101/2020.05.06.081372. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sanes J.N., Donoghue J.P. Plasticity and primary motor cortex. Annu. Rev. Neurosci. 2000;23:393–415. doi: 10.1146/annurev.neuro.23.1.393. [DOI] [PubMed] [Google Scholar]
- Santin M.d.N., Voulleminot P., Vrillon A., Hainque E., Béreau M., Lagha-Boukbiza O., Wirth T., Montaut S., Bardinet E., Kyheng M., et al. Impact of subthalamic deep brain stimulation on impulse control disorders in Parkinson’s disease: a prospective study. Mov. Disord. 2021;36:750–757. doi: 10.1002/mds.28320. [DOI] [PubMed] [Google Scholar]
- Sanz-García A., Perez-Romero M., Ortega G.J. Spectral and network characterization of focal seizure types and phases. Comput. Methods Programs Biomed. 2022;217:106704. doi: 10.1016/j.cmpb.2022.106704. [DOI] [PubMed] [Google Scholar]
- Scherrer S., Smith A.H., Gowatsky J., Palmese C.A., Jimenez-Shahed J., Kopell B.H., Mayberg H.S., Figee M. Impulsivity and compulsivity after subthalamic deep brain stimulation for Parkinson’s disease. Front. Behav. Neurosci. 2020;14:47. doi: 10.3389/fnbeh.2020.00047. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Schroeder K.E., Chestek C.A. Intracortical brain-machine interfaces advance sensorimotor neuroscience. Front. Neurosci. 2016;10:291. doi: 10.3389/fnins.2016.00291. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Scott S.H. Inconvenient truths about neural processing in primary motor cortex. J. Physiol. 2008;586:1217–1224. doi: 10.1113/jphysiol.2007.146068. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Scott S.H., Kalaska J.F. Reaching movements with similar hand paths but different arm orientations. I. Activity of individual cells in motor cortex. J. Neurophysiol. 1997;77:826–852. doi: 10.1152/jn.1997.77.2.826. [DOI] [PubMed] [Google Scholar]
- Sergio L.E., Hamel-Pâquet C., Kalaska J.F. Motor cortex neural correlates of output kinematics and kinetics during isometric-force and arm-reaching tasks. J. Neurophysiol. 2005;94:2353–2378. doi: 10.1152/jn.00989.2004. [DOI] [PubMed] [Google Scholar]
- Shenoy K.V., Sahani M., Churchland M.M. Cortical control of arm movements: a dynamical systems perspective. Annu. Rev. Neurosci. 2013;36:337–359. doi: 10.1146/annurev-neuro-062111-150509. [DOI] [PubMed] [Google Scholar]
- Shine J.M., Kucyi A., Foster B.L., Bickel S., Wang D., Liu H., Poldrack R.A., Hsieh L.-T., Hsiang J.C., Parvizi J. Distinct patterns of temporal and directional connectivity among intrinsic networks in the human brain. J. Neurosci. 2017;37:9667–9674. doi: 10.1523/JNEUROSCI.1574-17.2017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Shink E., Bevan M.D., Bolam J.P., Smith Y. The subthalamic nucleus and the external pallidum: two tightly interconnected structures that control the output of the basal ganglia in the monkey. Neuroscience. 1996;73:335–357. doi: 10.1016/0306-4522(96)00022-X. [DOI] [PubMed] [Google Scholar]
- Shokur S., Mazzoni A., Schiavone G., Weber D.J., Micera S. A modular strategy for next-generation upper-limb sensory-motor neuroprostheses. Med. 2021;2:912–937. doi: 10.1016/j.medj.2021.05.002. [DOI] [PubMed] [Google Scholar]
- Siddiqi S.H., Schaper F.L.W.V.J., Horn A., Hsu J., Padmanabhan J.L., Brodtmann A., Cash R.F.H., Corbetta M., Choi K.S., Dougherty D.D., et al. Brain stimulation and brain lesions converge on common causal circuits in neuropsychiatric disease. Nat. Hum. Behav. 2021;5:1707–1716. doi: 10.1038/s41562-021-01161-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Simon M.V., Curry W.T., Jones P.S., Cahill D.P., Carter B.S., Rapalino O., Malik A.N., Nahed B.V. Intraoperative thalamocortical tract monitoring via direct cortical recordings during craniotomy. Clin. Neurophysiol. 2021;132:1416–1432. doi: 10.1016/j.clinph.2021.02.404. [DOI] [PubMed] [Google Scholar]
- So K., Koralek A.C., Ganguly K., Gastpar M.C., Carmena J.M. Assessing functional connectivity of neural ensembles using directed information. J. Neural. Eng. 2012;9:026004. doi: 10.1088/1741-2560/9/2/026004. [DOI] [PubMed] [Google Scholar]
- Sonoda M., Rothermel R., Carlson A., Jeong J.-W., Lee M.-H., Hayashi T., Luat A.F., Sood S., Asano E. Naming-related spectral responses predict neuropsychological outcome after epilepsy surgery. Brain. 2022;145:517–530. doi: 10.1093/brain/awab318. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Suminski A.J., Tkach D.C., Fagg A.H., Hatsopoulos N.G. Incorporating feedback from multiple sensory modalities enhances brain–machine interface control. J. Neurosci. 2010;30:16777–16787. doi: 10.1523/JNEUROSCI.3967-10.2010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Suminski A.J., Tkach D.C., Hatsopoulos N.G. Exploiting multiple sensory modalities in brain-machine interfaces. Neural Netw. 2009;22:1224–1234. doi: 10.1016/j.neunet.2009.05.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sun D., van Klink N.E.C., Bongaarts A., Zweiphenning W.E.J.M., van ’t Klooster M.A., Gebbink T.A., Snijders T.J., van Eijsden P., Robe P.A.J.T., Aronica E., Zijlmans M. High frequency oscillations associate with neuroinflammation in low-grade epilepsy associated tumors. Clin. Neurophysiol. 2022;133:165–174. doi: 10.1016/j.clinph.2021.08.025. [DOI] [PubMed] [Google Scholar]
- Suresh A.K., Goodman J.M., Okorokova E.V., Kaufman M., Hatsopoulos N.G., Bensmaia S.J. Neural population dynamics in motor cortex are different for reach and grasp. Elife. 2020;9:e58848. doi: 10.7554/eLife.58848. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sweet J.A., Hdeib A.M., Sloan A., Miller J.P. Depths and grids in brain tumors: implantation strategies, techniques, and complications. Epilepsia. 2013;54:66–71. doi: 10.1111/epi.12447. [DOI] [PubMed] [Google Scholar]
- Tabot G.A., Dammann J.F., Berg J.A., Tenore F.V., Boback J.L., Vogelstein R.J., Bensmaia S.J. Restoring the sense of touch with a prosthetic hand through a brain interface. Proc. Natl. Acad. Sci. USA. 2013;110:18279–18284. doi: 10.1073/pnas.1221113110. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Talairach J., Française S. de N.-C. de L. Masson; 1974. Approche nouvelle de la neurochirurgie de l’épilepsie: Méthodologie stéréotaxique et résultats thérapeutiques, Neurochirurgie: Supplément. [PubMed] [Google Scholar]
- Tan K.M., Daitch A.L., Pinheiro-Chagas P., Fox K.C.R., Parvizi J., Lieberman M.D. Electrocorticographic evidence of a common neurocognitive sequence for mentalizing about the self and others. Nat. Commun. 2022;13:1919. doi: 10.1038/s41467-022-29510-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tastevin M., Spatola G., Régis J., Lançon C., Richieri R. Deep brain stimulation in the treatment of obsessive-compulsive disorder: current perspectives. Neuropsychiatr. Dis. Treat. 2019;15:1259–1272. doi: 10.2147/NDT.S178207. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Taylor D.M., Tillery S.I.H., Schwartz A.B. Direct cortical control of 3D neuroprosthetic devices. Science. 2002;296:1829–1832. doi: 10.1126/science.1070291. [DOI] [PubMed] [Google Scholar]
- Telkes I., Jimenez-Shahed J., Viswanathan A., Abosch A., Ince N.F. Prediction of STN-DBS electrode implantation track in Parkinson’s disease by using local field potentials. Front. Neurosci. 2016;10:198. doi: 10.3389/fnins.2016.00198. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Telkes I., Sabourin S., Durphy J., Adam O., Sukul V., Raviv N., Staudt M.D., Pilitsis J.G. Functional use of directional local field potentials in the subthalamic nucleus deep brain stimulation. Front. Hum. Neurosci. 2020;14:145. doi: 10.3389/fnhum.2020.00145. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Telkes I., Viswanathan A., Jimenez-Shahed J., Abosch A., Ozturk M., Gupte A., Jankovic J., Ince N.F. Local field potentials of subthalamic nucleus contain electrophysiological footprints of motor subtypes of Parkinson’s disease. Proc. Natl. Acad. Sci. USA. 2018;115:E8567–E8576. doi: 10.1073/pnas.1810589115. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Thura D., Cisek P. The basal ganglia do not select reach targets but control the urgency of commitment. Neuron. 2017;95:1160–1170.e5. doi: 10.1016/j.neuron.2017.07.039. [DOI] [PubMed] [Google Scholar]
- Tinkhauser G., Pogosyan A., Little S., Beudel M., Herz D.M., Tan H., Brown P. The modulatory effect of adaptive deep brain stimulation on beta bursts in Parkinson’s disease. Brain. 2017;140:1053–1067. doi: 10.1093/brain/awx010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tinkhauser G., Shah S.A., Fischer P., Peterman K., Debove I., Nygyuen K., Nowacki A., Torrecillos F., Khawaldeh S., Tan H., et al. Electrophysiological differences between upper and lower limb movements in the human subthalamic nucleus. Clin. Neurophysiol. 2019;130:727–738. doi: 10.1016/j.clinph.2019.02.011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Todorov E. Optimality principles in sensorimotor control. Nat. Neurosci. 2004;7:907–915. doi: 10.1038/nn1309. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tomlinson T., Miller L.E. In: Progress in Motor Control: Theories and Translations. Laczko J., Latash M.L., editors. Springer International Publishing; 2016. Toward a proprioceptive neural interface that mimics natural cortical activity; pp. 367–388. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Torrecillos F., Tinkhauser G., Fischer P., Green A.L., Aziz T.Z., Foltynie T., Limousin P., Zrinzo L., Ashkan K., Brown P., Tan H. Modulation of beta bursts in the subthalamic nucleus predicts motor performance. J. Neurosci. 2018;38:8905–8917. doi: 10.1523/JNEUROSCI.1314-18.2018. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Uddin L.Q. Salience processing and insular cortical function and dysfunction. Nat. Rev. Neurosci. 2015;16:55–61. doi: 10.1038/nrn3857. [DOI] [PubMed] [Google Scholar]
- Vakani R., Nair D.R. In: Handbook of Clinical Neurology. Levin K.H., Chauvel P., editors. Elsevier; 2019. Chapter 20 - electrocorticography and functional mapping; pp. 313–327. [DOI] [PubMed] [Google Scholar]
- Valle G., Mazzoni A., Iberite F., D’Anna E., Strauss I., Granata G., Controzzi M., Clemente F., Rognini G., Cipriani C., et al. Biomimetic intraneural sensory feedback enhances sensation naturalness, tactile sensitivity, and manual dexterity in a bidirectional prosthesis. Neuron. 2018;100:37–45.e7. doi: 10.1016/j.neuron.2018.08.033. [DOI] [PubMed] [Google Scholar]
- Valsky D., Blackwell K.T., Tamir I., Eitan R., Bergman H., Israel Z. Real-time machine learning classification of pallidal borders during deep brain stimulation surgery. J. Neural. Eng. 2020;17:016021. doi: 10.1088/1741-2552/ab53ac. [DOI] [PubMed] [Google Scholar]
- van Klink N.E.C., Zweiphenning W.J.E.M., Ferrier C.H., Gosselaar P.H., Miller K.J., Aronica E., Braun K.P.J., Zijlmans M. Can we use intraoperative high-frequency oscillations to guide tumor-related epilepsy surgery? Epilepsia. 2021;62:997–1004. doi: 10.1111/epi.16845. [DOI] [PMC free article] [PubMed] [Google Scholar]
- van Wijk B.C.M., Alkemade A., Forstmann B.U. Functional segregation and integration within the human subthalamic nucleus from a micro- and meso-level perspective. Cortex. 2020;131:103–113. doi: 10.1016/j.cortex.2020.07.004. [DOI] [PubMed] [Google Scholar]
- van Wouwe N.C., Neimat J.S., van den Wildenberg W.P.M., Hughes S.B., Lopez A.M., Phibbs F.T., Schall J.D., Rodriguez W.J., Bradley E.B., Dawant B.M., Wylie S.A. Subthalamic nucleus subregion stimulation modulates inhibitory control. Cereb. Cortex Commun. 2020;1:tgaa083. doi: 10.1093/texcom/tgaa083. [DOI] [PMC free article] [PubMed] [Google Scholar]
- van Wouwe N.C., Pallavaram S., Phibbs F.T., Martinez-Ramirez D., Neimat J.S., Dawant B.M., D’Haese P.F., Kanoff K.E., van den Wildenberg W.P.M., Okun M.S., Wylie S.A. Focused stimulation of dorsal subthalamic nucleus improves reactive inhibitory control of action impulses. Neuropsychologia. 2017;99:37–47. doi: 10.1016/j.neuropsychologia.2017.02.016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Vayssiere N., van der Gaag N., Cif L., Hemm S., Verdier R., Frerebeau P., Coubes P. Deep brain stimulation for dystonia confirming a somatotopic organization in the globus pallidus internus. J. Neurosurg. 2004;101:181–188. doi: 10.3171/jns.2004.101.2.0181. [DOI] [PubMed] [Google Scholar]
- Velliste M., Perel S., Spalding M.C., Whitford A.S., Schwartz A.B. Cortical control of a prosthetic arm for self-feeding. Nature. 2008;453:1098–1101. doi: 10.1038/nature06996. [DOI] [PubMed] [Google Scholar]
- Veuthey T.L., Derosier K., Kondapavulur S., Ganguly K. Single-trial cross-area neural population dynamics during long-term skill learning. Nat. Commun. 2020;11:4057–4115. doi: 10.1038/s41467-020-17902-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Vissani M., Cordella R., Micera S., Eleopra R., Romito L.M., Mazzoni A. Spatio-temporal structure of single neuron subthalamic activity identifies DBS target for anesthetized Tourette syndrome patients. J. Neural. Eng. 2019;16:066011. doi: 10.1088/1741-2552/ab37b4. [DOI] [PubMed] [Google Scholar]
- Vissani M., Isaias I.U., Mazzoni A. Deep brain stimulation: a review of the open neural engineering challenges. J. Neural. Eng. 2020;17:051002. doi: 10.1088/1741-2552/abb581. [DOI] [PubMed] [Google Scholar]
- Vissani M., Palmisano C., Volkmann J., Pezzoli G., Micera S., Isaias I.U., Mazzoni A. Impaired reach-to-grasp kinematics in parkinsonian patients relates to dopamine-dependent, subthalamic beta bursts. NPJ Parkinsons Dis. 2021;7:53. doi: 10.1038/s41531-021-00187-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Vitek J.L., Johnson L.A. Understanding Parkinson’s disease and deep brain stimulation: role of monkey models. Proc. Natl. Acad. Sci. USA. 2019;116:26259–26265. doi: 10.1073/pnas.1902300116. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Voelcker-Rehage C., Niemann C., Hübner L., Godde B., Winneke A.H. In: Sport and Exercise Psychology Research. Raab M., Wylleman P., Seiler R., Elbe A.-M., Hatzigeorgiadis A., editors. Academic Press; 2016. Chapter 3 - benefits of physical activity and fitness for lifelong cognitive and motor development—brain and behavior; pp. 43–73. [DOI] [Google Scholar]
- Voon V., Droux F., Morris L., Chabardes S., Bougerol T., David O., Krack P., Polosan M. Decisional impulsivity and the associative-limbic subthalamic nucleus in obsessive-compulsive disorder: stimulation and connectivity. Brain. 2017;140:442–456. doi: 10.1093/brain/aww309. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Vyas S., Golub M.D., Sussillo D., Shenoy K.V. Computation through neural population dynamics. Annu. Rev. Neurosci. 2020;43:249–275. doi: 10.1146/annurev-neuro-092619-094115. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wang L., Conner J.M., Rickert J., Tuszynski M.H. Structural plasticity within highly specific neuronal populations identifies a unique parcellation of motor learning in the adult brain. Proc. Natl. Acad. Sci. USA. 2011;108:2545–2550. doi: 10.1073/pnas.1014335108. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wang X., Zhang G., Wang Y., Yang L., Liang Z., Cong F. One-dimensional convolutional neural networks combined with channel selection strategy for seizure prediction using long-term intracranial EEG. Int. J. Neural Syst. 2022;32:2150048. doi: 10.1142/S0129065721500489. [DOI] [PubMed] [Google Scholar]
- Weisholtz D.S., Kreiman G., Silbersweig D.A., Stern E., Cha B., Butler T. Localized task-invariant emotional valence encoding revealed by intracranial recordings. Soc. Cogn. Affect. Neurosci. 2022;17:549–558. doi: 10.1093/scan/nsab134. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Welton T., Cardoso F., Carr J.A., Chan L.-L., Deuschl G., Jankovic J., Tan E.-K. Essential tremor. Nat. Rev. Dis. Primers. 2021;7:83. doi: 10.1038/s41572-021-00314-w. [DOI] [PubMed] [Google Scholar]
- Wessberg J., Stambaugh C.R., Kralik J.D., Beck P.D., Laubach M., Chapin J.K., Kim J., Biggs S.J., Srinivasan M.A., Nicolelis M.A. Real-time prediction of hand trajectory by ensembles of cortical neurons in primates. Nature. 2000;408:361–365. doi: 10.1038/35042582. [DOI] [PubMed] [Google Scholar]
- Wodlinger B., Downey J.E., Tyler-Kabara E.C., Schwartz A.B., Boninger M.L., Collinger J.L. Ten-dimensional anthropomorphic arm control in a human brain-machine interface: difficulties, solutions, and limitations. J. Neural. Eng. 2015;12:016011. doi: 10.1088/1741-2560/12/1/016011. [DOI] [PubMed] [Google Scholar]
- Wolpert D.M., Diedrichsen J., Flanagan J.R. Principles of sensorimotor learning. Nat. Rev. Neurosci. 2011;12:739–751. doi: 10.1038/nrn3112. [DOI] [PubMed] [Google Scholar]
- Wu H., Petitpré C., Fontanet P., Sharma A., Bellardita C., Quadros R.M., Jannig P.R., Wang Y., Heimel J.A., Cheung K.K.Y., et al. Distinct subtypes of proprioceptive dorsal root ganglion neurons regulate adaptive proprioception in mice. Nat. Commun. 2021;12:1026. doi: 10.1038/s41467-021-21173-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Xu T., Yu X., Perlik A.J., Tobin W.F., Zweig J.A., Tennant K., Jones T., Zuo Y. Rapid formation and selective stabilization of synapses for enduring motor memories. Nature. 2009;462:915–919. doi: 10.1038/nature08389. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Yan H., Boutet A., Mithani K., Germann J., Elias G.J.B., Yau I., Go C., Kalia S.K., Lozano A.M., Fasano A., Ibrahim G.M. Aggressiveness after centromedian nucleus stimulation engages prefrontal thalamocortical circuitry. Brain Stimul. 2019;13:357–359. doi: 10.1016/j.brs.2019.10.023. [DOI] [PubMed] [Google Scholar]
- Yan H., Katz J.S., Anderson M., Mansouri A., Remick M., Ibrahim G.M., Abel T.J. Method of invasive monitoring in epilepsy surgery and seizure freedom and morbidity: a systematic review. Epilepsia. 2019;60:1960–1972. doi: 10.1111/epi.16315. [DOI] [PubMed] [Google Scholar]
- Yao P.-S., Zheng S.-F., Wang F., Kang D.-Z., Lin Y.-X. Surgery guided with intraoperative electrocorticography in patients with low-grade glioma and refractory seizures. J. Neurosurg. 2018;128:840–845. doi: 10.3171/2016.11.JNS161296. [DOI] [PubMed] [Google Scholar]
- Yin H.H. The sensorimotor striatum is necessary for serial order learning. J. Neurosci. 2010;30:14719–14723. doi: 10.1523/JNEUROSCI.3989-10.2010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zacksenhouse M., Lebedev M.A., Carmena J.M., O’Doherty J.E., Henriquez C., Nicolelis M.A.L. Cortical modulations increase in early sessions with brain-machine interface. PLoS One. 2007;2:e619. doi: 10.1371/journal.pone.0000619. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zaghloul K.A., Weidemann C.T., Lega B.C., Jaggi J.L., Baltuch G.H., Kahana M.J. Neuronal activity in the human subthalamic nucleus encodes decision conflict during action selection. J. Neurosci. 2012;32:2453–2460. doi: 10.1523/JNEUROSCI.5815-11.2012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zavala B., Brittain J.-S., Jenkinson N., Ashkan K., Foltynie T., Limousin P., Zrinzo L., Green A.L., Aziz T., Zaghloul K., Brown P. Subthalamic nucleus local field potential activity during the eriksen flanker task reveals a novel role for theta phase during conflict monitoring. J. Neurosci. 2013;33:14758–14766. doi: 10.1523/JNEUROSCI.1036-13.2013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zénon A., Duclos Y., Carron R., Witjas T., Baunez C., Régis J., Azulay J.-P., Brown P., Eusebio A. The human subthalamic nucleus encodes the subjective value of reward and the cost of effort during decision-making. Brain. 2016;139:1830–1843. doi: 10.1093/brain/aww075. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zhang Y., Lu Q., Monsoor T., Hussain S.A., Qiao J.X., Salamon N., Fallah A., Sim M.S., Asano E., Sankar R., et al. Refining epileptogenic high-frequency oscillations using deep learning: a reverse engineering approach. Brain Commun. 2021;4:fcab267. doi: 10.1093/braincomms/fcab267. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zhu Q., Liang Y., Fan Z., Liu Y., Zhou C., Zhang H., Li T., Zhou Y., Yang J., Wang L. The utility of intraoperative ECoG in tumor-related epilepsy: systematic review. Clin. Neurol. Neurosurg. 2022;212:107054. doi: 10.1016/j.clineuro.2021.107054. [DOI] [PubMed] [Google Scholar]
- Zhu Z., Hubbard E., Guo X., Barbosa D.A.N., Popal A.M., Cai C., Jiang H., Zheng Z., Lin J., Gao W., et al. A connectomic analysis of deep brain stimulation for treatment-resistant depression. Brain Stimul. 2021;14:1226–1233. doi: 10.1016/j.brs.2021.08.010. [DOI] [PubMed] [Google Scholar]