Abstract
The management of (peri)pancreatic collections has undergone a paradigm shift from open surgical drainage to minimally invasive endoscopic, percutaneous, or surgical interventions. Minimally invasive interventions are associated with less morbidity and mortality compared to open necrosectomy. The (peri)pancreatic collections are currently treated with a “step-up approach” of an initial drainage procedure followed, if necessary, by a more invasive debridement. The step-up approach for management of (peri)pancreatic collections is mainly of two types, namely, surgical and endoscopic. Surgical step up includes initial image-guided percutaneous catheter drainage followed, if necessary, by minimally invasive video-assisted retroperitoneal debridement. Endoscopic step-up approach includes endoscopic transluminal drainage followed, if necessary by direct endoscopic necrosectomy. The development of endoscopic ultrasound and lumen apposing metal stents (LAMSs) has revolutionized the endoscopic management of (peri)pancreatic collections. Compared to surgical step-up approach, endoscopic step-up treatment approach has been reported to be associated with less new-onset organ failure, pancreatic fistula, enterocutaneous fistula, or perforation of visceral organ and shorter hospital/intensive care unit stay. This review will mainly focus on indications, techniques, timing, and recent advances related to endoscopic step-up approach in management of symptomatic(peri)pancreatic collections.
Acute pancreatitis (AP) is an important cause of hospitalization worldwide with its recent global incidence reported to be 34 cases per 100,000 persons annually [1]. It is a complex disorder due to associated local and systemic inflammation and variable clinical course depending upon the disease severity. As per the revised Atlanta classification (2012), severity of AP is graded as mild, moderate, and severe depending upon the presence or absence of local/systemic complications and organ failure [2]. AP is also classified morphologically as either interstitial pancreatitis or necrotizing pancreatitis depending upon the appearances of pancreas on contrast-enhanced cross-sectional imaging like computed tomography or magnetic resonance imaging [3].
(Peri)pancreatic collections are a common local complication of AP, and a clear distinction should be made between collections associated with interstitial edematous pancreatitis and those arising from acute necrotizing pancreatitis (ANP) for planning appropriate management strategy. (Peri)pancreatic collections arising from interstitial edematous pancreatitis are termed as acute peripancreatic fluid collections within 4 weeks of disease onset and as pseudocysts if they persist beyond 4 weeks with a well-defined wall. The collections forming after an attack of acute interstitial edematous pancreatitis usually resolve with time without any intervention in majority of patients. Similarly, (peri)pancreatic collections arising in the setting of ANP are termed as acute necrotic collections within 4 weeks of disease onset, and walled off necrosis (WON) is the term used for an encapsulated necrotic collection that has an enclosing wall of granulation tissue that usually develops after 4 weeks from the onset of ANP.
Because of associated higher morbidity and mortality, management of (peri)pancreatic collections requires tailored and multidisciplinary team approach. Infection is a sinister event in the history of (peri)pancreatic collections as it is associated with a dramatic increase in the morbidity and mortality. Confirmed infected (peri)pancreatic collections is almost always an indication for invasive intervention as less than 5% of patients will improve on antibiotics alone [4]. Sterile necrosis can be managed conservatively irrespective of size unless there are persistent abdominal pain, nausea, vomiting, and failure to thrive or associated complications, including gastrointestinal luminal obstruction, biliary obstruction, recurrent acute pancreatitis, fistulas, or persistent systemic inflammatory response syndrome [5]. Traditionally, open necrosectomy with surgical debridement and postoperative lavage was the preferred treatment for infected necrosis [6]. However, surgical insult has been shown to increase the morbidity and mortality in AP resulting in poor outcomes. Therefore, the interventions for infected (peri)pancreatic collections have shifted from open surgery to minimally invasive interventions including endoscopic, laparoscopic, and video-assisted retroperitoneal debridement, which are associated with less morbidity and mortality. The management of infected pancreatic necrosis underwent a paradigm shift after the PANTER trial was published in 2010. Van Santvoort et al demonstrated that minimally invasive surgical approach is associated with reduced morbidity and cost in patients of infected WON as compared to open necrosectomy [7]. This approach was termed as a step-up approach, indicating a gradual increase from a less invasive to a more invasive procedure if needed.
The development of endoscopic ultrasound (EUS) and lumen apposing metal stents (LAMSs) has revolutionized the endoscopic management of (peri)pancreatic collections. The availability of better endoscopic accessories has expanded the role of endoscopy in the management of (peri)pancreatic collections [8]. The (peri)pancreatic collections which earlier could only be drained surgically are now being increasingly drained endoscopically via the transgastric or transduodenal route with better outcomes. The development of direct endoscopic necrosectomy (DEN) has further improved the outcomes of endoscopic approach for treatment of pancreatic necrosis [5,9]. Similar to the percutaneous step-up approach for treatment of pancreatic necrosis, an endoscopic step approach of less invasive drainage only approach followed by more aggressive approach of DEN in nonresponders has been recommended for the management of patients with symptomatic (peri)pancreatic collections [10,11]. This review will focus on indications, techniques, timing, and recent advances related to endoscopic step-up approach in management of symptomatic (peri)pancreatic collections.
STEP-UP APPROACH
Step-up approach for management of necrotizing pancreatitis is mainly of 2 types. Surgical step up includes image-guided percutaneous catheter drainage followed, if necessary, by minimally invasive video-assisted retroperitoneal debridement or laparoscopic necrosectomy. Endoscopic step-up approach includes endoscopic transluminal drainage (ETD) followed, if necessary, by DEN in non- or partial responders and surgery or open necrosectomy in the event of persistent collections or complications.
ENDOTHERAPY VERSUS SURGERY IN PANCREATIC NECROSIS
Endoscopic step-up approach is speculated to be associated with better outcomes because of lack of use of general anesthesia as well as surgical exploration resulting in reduction of surgical stress and surgery-associated complications such as pancreatic fistulas. Three randomized controlled trials (RCTs) have compared endotherapy and minimally invasive surgery for treatment of infected necrotizing pancreatitis and confirmed this hypothesis of better outcomes with endoscopic step-up treatment approach. The PENGUIN trial published in 2012 was the first RCT on this topic where Bakker et al directly compared endoscopic necrosectomy and surgical necrosectomy in 20 patients [12]. Primary end point was measurement of serum interleukin-6 levels as marker of postprocedure proinflammatory response. Secondary clinical end points included a predefined composite end point of major complications (new-onset multiple organ failure, intra-abdominal bleeding, enterocutaneous fistula, or pancreatic fistula) or death [12]. Endoscopic necrosectomy had lower levels of postprocedure interleukin-6 (P = .004), and the composite clinical end point occurred less often after endoscopic necrosectomy (20% vs 80%; risk difference 0.60, 95% CI 0.16–0.80, P = .03) compared to the surgical approach. This was followed by the TENSION trial conducted by the Dutch Pancreatitis Group [13]. This RCT reported comparable outcomes in terms of mortality and major complications between both groups. However, length of hospital stay, incidence of pancreatic fistulas, and persistent cardiovascular organ failure were significantly lower in endoscopy group. Recent RCT by Bang et al randomized 66 patients to groups that received minimally invasive surgery (laparoscopic or video-assisted retroperitoneal debridement, depending on location of collection, n = 32) or an endoscopic step-up approach (transluminal drainage with or without necrosectomy, n = 34) [14]. They reported significantly reduced major complications, lowered costs, and increased quality of life with endoscopic step up. Mortality was comparable in both groups. However, inclusion of pancreatic fistula in primary composite outcome, which was seen in 28.1% patients in surgery group, could be the reason for the statistically significant difference of the main outcome in this trial.
Despite some intertrial methodological differences, 2 recent meta-analyses of these 3 RCTs reported lower frequency of new onset organ failure, pancreatic fistula, enterocutaneous fistula, or perforation of visceral organ and shorter hospital/intensive care unit (ICU) stay with endoscopic intervention [15,16]. Apart from meta-analysis of only RCTs, Khan et al in a meta-analysis involving 641 patients (2 RCTs and 4 observational studies) with infected or symptomatic WON reported lower mortality with endotherapy [17]. Another recent meta-analysis by Tang et al involving 10 studies and 401 patients reported comparable efficacy of both endoscopy and surgical interventions in ANP with lower postoperative mortality, intestinal cutaneous fistula, gastrointestinal perforation, and pancreatic fistula in endoscopy group [18].
Therefore, available evidence suggests that endoscopic step-up approach should be preferred intervention for infected (peri)pancreatic collections with encapsulation whenever feasible in skilled hands. Minimally invasive surgical approach should be preferred when collections are not accessible endoscopically or when endotherapy is unavailable or unsuccessful.
ENDOSCOPIC ULTRASOUND-GUIDED TRANSMURAL DRAINAGE VERSUS CONVENTIONAL TRANSMURAL DRAINAGE
Conventional transmural drainage of (peri)pancreatic collections involved visualization of bulge in gastric or duodenal wall due to extrinsic compression from collections and subsequent blind puncture with a cautery enhanced needle knife. However, visualized bulge is noticed in only 40%–50% of collections, which is a major limitation of this technique. EUS-guided transmural drainage (EUS-TD) enables drainage of collections irrespective of bulge in real time and also potentially avoiding intervening blood vessels. Two prospective RCTs reported superiority of EUS-TD over conventional transmural drainage of (peri)pancreatic collections, and therefore, EUS-guided transmural drainage is the preferred endoscopic technique for drainage of (peri)pancreatic collections [19,20].
FLUOROSCOPIC VERSUS NONFLUOROSCOPIC ENDOSCOPIC TRANSMURAL DRAINAGE
The guidance of fluoroscopic images during EUS-guided transmural drainage of (peri)pancreatic collections provides additional help for accurate localization of stent and endoscopic accessories. Fluoroscopy also aids in timely recognition of complications such as free intraperitoneal or retroperitoneal gas which can occur in situations of stent misdeployment. However, option to complete procedure in the absence of fluoroscopy provides an opportunity for emergent drainage of (peri)pancreatic collections in critically ill patients as it can be performed at the bedside. Rana et al reported that transmural drainage of nonbulging WON using plastic stents and nasocystic drains can be safely and effectively achieved nonfluoroscopically using EUS guidance only [21]. Recently, Braden et al demonstrated similar outcomes using fully covered self-expandable metal stents (FCSEMSs) without fluoroscopy for drainage of WON [22]. Consiglieri et al also reported similar clinical as well as technical success of EUS-guided transmural drainage of (peri)pancreatic collections with and without fluoroscopic guidance [23].
TECHNIQUE OF ENDOSCOPIC STEP-UP DRAINAGE
The endoscopic step-up treatment approach consists of an initial EUS-guided transluminal drainage followed, if necessary, by DEN. The initial drainage can be accomplished with either multiple plastic stents or metal stents. The insertion of plastic stents is a multistep procedure that involves puncture and entry into WON cavity under EUS guidance from gastroduodenal lumen followed by dilatation of transmural tract and subsequent placement of plastic stents. After securing the guide wire in the WON cavity, the transmural tract is dilated using noncautery methods using bougie dilators or cautery enhanced accessory like a needle knife or a cystotome. Over-the-wire coaxial cautery device (cystotome) helps in controlled dilatation and is a preferred accessory for dilatation of the transmural tract. Thereafter, the transmural tract is further dilated using dilating balloons, and the size of dilating balloon used depends upon the location of the transmural tract as well as whether multiple plastic stents or fully covered self-expanding metal stent (SEMS) is to be placed. If plastic stents are to be placed, we usually dilate up to 10 mm in esophagus, 15–18 mm in the stomach, and 10–12 mm in the duodenum [8]. In case a fully covered SEMS is being placed, the transmural tract is dilated to ensure smooth passage of the stent delivery system, and we usually dilate up to 6 mm. Cautery enhanced LAMSs like Hot Spaxus (Taewoong Medical Co., Gimpo, Korea) and Hot Axios (Boston Scientific, Marlborough, MA) stent systems enable quicker delivery of LAMS without the need for guide wire placement and further dilatation of fistula [8].
Majority of patients with WON can be managed with endoscopic drainage, and use of large-diameter LAMS has further improved the efficacy of endoscopic drainage [10,11]. However, drainage alone may not be sufficient in patients with significant necrotic debris (> 40%), and these patients may require additional interventions like DEN [8]. Therapeutic endoscope with a large working channel along with water jet and carbon dioxide insufflation is preferred for DEN as it allows irrigation during necrosectomy as well as easy insertion of various endoscopic accessories for removal of necrotic debris along with decreased risk of air embolism as well as perforation. The standard endoscopic accessories like dormia, snare, baskets, grasping forceps, and extraction balloons are used for DEN.
STENTS IN TRANSMURAL DRAINAGE
Traditionally, multiple plastic stents with double pigtail design were mainstay of therapy for endoscopic management of WON (Fig 1). However, despite showing high efficacy for drainage of pseudocysts (85.1%–90.8%), treatment success is significantly lower for drainage of WON (69.5%–81.8%). This can be attributed to the small lumen diameter of plastic stent, and therefore, multiple plastic stents have been advocated for drainage of necrotic collections [24]. Although efficacious, multiple plastic stent insertion is time-consuming and cumbersome with repeated need of balloon dilatation of fistulous tract for each session of endoscopic necrosectomy, and this is associated with increased risk of intraperitoneal leak/perforation and bleeding complications [25]. To overcome these limitations of plastic stents, FCSEMSs (biliary or esophageal) have been used for the drainage of WON as the wider diameter of these stents permits better drainage of solid debris [[26], [27], [28]]. However, their tubular design and lack of lumen apposing properties resulted in high risk of migration, fluid leakage, and injury of the duodenal/gastric wall or of the retroperitoneum, resulting in bleeding and/or perforation.
Fig 1.
EUS-guided transmural drainage with multiple plastic stents. (A) EUS: WON with predominantly liquid content. (B) Transmural tract dilatation with balloon. (C) Placement of multiple plastic stents by placing multiple guide wires in WON. (D) Multiple plastic stents placed in WON.
The development of specially designed LAMS has revolutionized the endoscopic management of WON. LAMSs have wider diameter, shorter length, and biflanged design that result in more effective drainage of solid necrotic debris and reduced chances of migration and facilitate easy DEN (Fig 2) [29]. As mentioned earlier, cautery enhanced LAMSs like Hot Spaxus and Hot Axios stent systems enable quicker delivery of LAMS without the need for guide wire and further dilatation of fistula [29,30].
Fig 2.
EUS-guided transmural drainage with cautery enhanced LAMS. (A) Puncture of WON with cautery enhanced LAMS. (B) Deployment of LAMS. Guide wire negotiated into WON cavity through the deployed LAMS for dilatation of deployed LAMS. (C) Balloon dilatation of the deployed LAMS. (D) DEN being performed through the deployed LAMS.
COMPARISON OF VARIOUS TYPES OF STENTS:
Metal vs Plastic Stents
Multiple comparative studies on management of (peri)pancreatic collections with plastic and metal stents have reported conflicting results. An RCT comparing both modalities reported no significant difference in the treatment outcomes including the total number of procedures performed, treatment success, and readmissions for patients of WON [31]. Rana et al reported similar findings in a retrospective analysis conducted at our center [24]. Contrary to these results, Bapaye et al in their retrospective study compared outcomes of transmural drainage of WON using multiple plastic stents and biflanged metal stents and reported that metal stents appear to be superior to multiple plastic stents in terms of clinical success, number of DEN sessions, adverse events, need for salvage surgery, and duration of hospital stay [32].
Multiple recent meta-analyses comparing metal stents with plastic stents have also reported conflicting results [[33], [34], [35], [36]]. Recent meta-analysis which included only those studies which directly compared both techniques for PFC drainage to reduce bias reported comparable technical and clinical success [37]. However, on subgroup analysis in patients with WON, adverse events associated with LAMS were less as compared to drainage with plastic stents. Lack of large prospective RCTs and nonuniform reporting among different studies are major drawbacks for conducting such analysis on this topic. A large multicenter trial by Chen et al reported that despite being more expensive, the higher efficacy of LAMS makes it a more cost-effective option for management of WON as compared to multiple plastic stents [38].
LAMS vs FCSEMS
Siddiqui et al analyzed comparative outcomes of EUS-guided drainage of WON using traditional FCSEMS (n = 121) and LAMS (n = 86) [39]. They reported superiority of LAMS over FCSEMS in terms of lesser number of procedures for WON resolution (2.2 vs 3), reduced need for endoscopic reintervention following stent occlusion (3.5% vs 21.5%), and lower stent migration rate (0% vs 5.8%). Technical and clinical success was comparable in both the groups with higher chances of early adverse events predominantly bleeding at stent site in LAMS group. A recent case control study compared efficacy and safety of LAMS and biliary FCSEMS for drainage of (peri)pancreatic collections [40]. The authors reported higher use of coaxial double pigtail plastic stents (DPSs) and nasocystic tube irrigation (33% vs 100%, and 13% vs 58%, respectively; P < .0001), increased procedure time (P = 0.0001), and more adverse events (4% vs 18%, P = 0.04) with FCSEMS use. They reported similar technical success but higher clinical success with use of LAMS (96% vs 82%, P = .055). A recent comparative study with retrospective design and small sample size reported that despite comparable technical success, LAMS is superior in terms of clinical success (95.7% vs 66.7% with FCSEMS), lower adverse events, and lesser procedure time as compared to FCSEMS and multiple plastic stents in patients undergoing drainage of WON [41].
Therefore, available evidence supports use of LAMS for effective drainage of WON and ease of DEN, if required. However, high cost of LAMS, need to replace it with plastic stents in patients with disconnected pancreatic duct syndrome, and clogging by necrotic material necessitating repeated procedures are important limitations of LAMS [8]. However, all patients of (peri)pancreatic collections do not need LAMS; majority of patients with WON can be treated with multiple plastic stents, and patients with large size WON with more necrotic debris only required metal stents or DEN [10].
SIZE OF LAMS
The basis of inserting LAMS for drainage of WON is to provide a wider drainage route that enables easy and spontaneous drainage of solid necrotic debris. Therefore, it is logical that a large diameter LAMS will provide a better egress route for solid necrotic output from WON cavity along with better and easy access for DEN with a therapeutic endoscope with larger diameter of accessory channel. However, larger diameter LAMS may also increase the risk of adverse events like bleeding due to higher area of surface contact increasing the chances of vessel erosion. An international multicenter case matched study by Parsa et al retrospectively evaluated efficacy and safety of 15 mm and 20 mm LAMS (AXIOS; Boston Scientific, Marlborough, MA) [42]. They reported comparable clinical success (92.2% vs 91.7%, odds ratio 0.92; P = .91), overall adverse events (21.6% vs 15.2%; P = .72), and bleeding events (4.9% vs 3.4%; P = .54) between the 20-mm and 15-mm LAMS groups, respectively. The number of DEN sessions were significantly lower with 20-mm LAMS (mean 1.3 vs 2.1; P < .001) despite having larger WON collections (transverse axis 118.2 vs 101.9 mm, P = .003; anteroposterior axis 95.9 vs 80.1 mm, P = .01). Therefore, more complex and large WON may potentially benefit from placement of a 20-mm LAMS. However, this study was retrospective and limited by heterogeneity in both recruitment and follow-up of patients. Therefore, large prospective RCTs are needed to conclusively answer whether a larger stent is always better in terms of safety and efficacy.
COAXIAL DPS IN LAMS
In recent years, use of coaxial DPS in LAMS has been suggested to minimize risk of bleeding complication reported with LAMS use for drainage of (peri)pancreatic collections. Theoretically, this technique might help by preventing direct contact of mucosa and surrounding blood vessels following collapse of (peri)pancreatic collection cavity and thus minimizing risk of vessel erosion and subsequent bleeding [43]. However, high-quality evidence to support its use is lacking, and retrospective studies with small sizes have reported conflicting results. Whereas Puga et al reported significantly higher rate of adverse events (42.9% vs 10.0%; P = .04) with bleeding being the most common adverse event using LAMS alone as compared to LAMS plus coaxial DPS for drainage of (peri)pancreatic collections, Ali et al described no benefit of this approach [44,45]. A recent meta-analysis comparing LAMS with multiple plastic stents for WON drainage also reported no benefit of this approach [46]. Co-axial DPS has also been hypothesized to reduce the risk of infection by reducing the frequency of food reflux in cavity. Aburajab et al reported a trend toward higher infection with LAMS, and placing a DPS across the LAMS minimized this risk [47].
TIMING OF ENDOTHERAPY
As revised Atlanta classification gave cutoff of 4 weeks for (peri)pancreatic collections to get walled off, international consensus recommends to wait for at least 4 weeks to attempt endoscopic drainage/debridement of collection. The concept of “wall” is important as it allows accurate demarcation of necrotic from viable tissue and allows time for liquefaction, and endotherapy in the absence of wall is associated with risk of pneumoperitoneum or pneumoretroperitoneum and consequent infective complications [48,49]. However, the cutoff period of 4 weeks is arbitrary, and necrotic collections may get walled off completely or partially in < 4 weeks of onset of illness [50,51]. Moreover, the timing of endoscopic intervention was adopted from poor outcomes of surgery in early phase. There is considerable disagreement regarding timing of intervention in early infected necrosis (IN) as shown in a survey conducted among 118 international pancreatologists with only 45% preferring immediate intervention [52]. Recent evidence suggests that early intervention is possible and should be reserved for patients with clinical deterioration despite maximum support. The role of ETD in early phase of necrotizing pancreatitis was evaluated first by Trikudanathan et al and subsequently in other comparative studies [9,[53], [54], [55], [56]]. These studies have reported that ETD is technically feasible in the early phase of illness of (peri)pancreatic collections with satisfactory efficacy and acceptable complication rates. However, evidence to support early intervention is still limited and mainly retrospective. Endoscopic intervention in early phase is technically challenging because of increased proportion of solid debris as compared to well-formed relatively liquefied WON in delayed phase. Rana et al reported that early endoscopic intervention, though feasible and effective, is associated with more frequent need of DEN, higher mortality, and need for rescue surgery as compared to delayed group [9]. Therefore, early intervention should be attempted only by skilled endoscopists with surgical and interventional radiology backup in selected group of patients with strong indication and who have endoscopically accessible collections with partial or complete encapsulation, and if possible, only in the third or fourth week of illness. Percutaneous step-up approach should be preferred when these prerequisites are not met and drainage is strongly indicated in early phase. Recently, the POINTER trial comparing immediate catheter drainage within 24 hours after randomization once infected necrosis was diagnosed with drainage that was postponed until the stage of walled-off necrosis was published [57]. It reported nonsuperiority of immediate drainage over postponed drainage with regard to complications with lesser requirement of invasive interventions in delayed drainage group. However, this study had some important limitations including the early arm having relatively “milder” disease [median (IQR) time to intervene was 24 (IQR 20–30) days] and fully or largely encapsulated collections in 60% patients with organ failure only in 24% patients. Thus, the current evidence suggests that there is a role for early ETD in select critically ill patients with infected (peri)pancreatic collections and organ failure who are completely refractory to antibiotics in centers with expertise in pancreatic endotherapy and radiological as well as surgical backup. Rana et al retrospectively compared ETD in early phase of illness with conventional PCD in symptomatic pancreatic necrosis and reported shorter duration for resolution, infrequent need of salvage surgery, and significantly lesser chances of external pancreatic fistula with endotherapy [56].
TIMING OF DEN
Direct endoscopic necrosectomy (DEN) refers to debridement of necrotic tissue via the transmural tract/stent. The optimal timing to perform DEN is still matter of debate. A multicenter survey among experts performing this procedure reported that 86.4% (19/22) of respondents would prefer step-up DEN [58]. Several studies have reported that 20%–90% of patients with WON improve following drainage with plastic or metallic stent alone [10,11,59]. Also, maturation of transmural tract following stent placement minimizes chances of stent dislodgement during delayed DEN. However, some experts recommend DEN at the time of stent deployment for better outcomes in terms of lesser endoscopic sessions which translate into lesser health care cost and reduced risk of endoscopy-related complications. Yan et al retrospectively analyzed 271 patients of WON with 69 patients undergoing immediate DEN in comparison to step-up DEN in 202 patients [60]. There was no difference in technical and clinical success as well overall adverse events in both groups. However, number of endoscopic sessions needed for resolution of WON was significantly lower in immediate DEN group. Stent dislodgement associated with DEN is usually managed with repositioning of stent in same setting without any further complication in reported studies. With the advent of LAMS and technological advances in its deployment, large prospective RCTs are needed to standardize the criteria for early or delayed DEN for better outcomes in management of symptomatic or infected WON. Most experts recommend an interval of 2–3 days between stent placement and DEN, depending upon clinical condition of patient, size of cavity, amount of solid debris, and degree of adhesion to the adjacent wall [61].
FACTORS PREDICTING OUTCOMES OF EUS-TD AND NEED FOR STEP UP
Patient with WON usually require multiple sessions of endoscopic reintervention which increase hospitalization cost/stay and associated complications. Therefore, factors predicting outcomes can obviate need of repeat procedures and thus reduce morbidity. Rana et al first reported that the size of the collection and the amount of the solid debris have a significant impact on the number of endoscopic procedures required for successful outcome in patients with WON. This study used only plastic stents, and > 40% debris was associated with need for endoscopic or surgical necrosectomy [62]. Later, Guo et al in their retrospective analysis using mostly plastic stents (71.8%) reported that solid debris content (≤ 30% or > 30%) was significantly associated with prognosis (endoscopic necrosectomy and hospitalization cost) [63]. Interestingly, their analysis reported metal stent and female sex to be associated with higher chances of necrosectomy and prolonged hospitalization. Recently, a study using only LAMS for EUS-TD reported that ≥ 30% solid necrosis, size of PFCs ≥ 10 cm, or paracolic extension is more likely to require step-up therapy and should be considered for early endoscopic reintervention [64]. However, Seicean et al using LAMS demonstrated that performance of 3 or more necrosectomies was significantly associated with more than 50% pancreatic necrosis but not with WON size or location [65]. Therefore, threshold for solid necrotic material to predict DEN is variable across studies because of different institutional practices, and there is a need to develop uniform objective method to quantify necrotic content in WON to accurately predict outcomes [66].
THE TIMING OF STENT REMOVAL
The timing for stent removal is variable depending upon stent type. Plastic stents can remain in place until the collection resolves as evidenced by cross-sectional imaging studies and potentially indefinitely in patients with associated disconnected pancreatic duct syndrome to prevent recurrence of PFCs [67,68]. The European Society of Gastrointestinal Endoscopy (ESGE) recommends retrieval of LAMS within 4 weeks to avoid stent-related adverse effects [69]. Ahmad et al analyzed 40 consecutive cases with PFCs (21 of them with WON) with none developing any LAMS-related bleeding using 15 mm × 10 mm LAMS (Hot Axios, Boston Scientific, Marlborough, MA) along with pig tail stent placed coaxially and suggested a protocol of early stent removal if WON resolves on repeat imaging done at 3 weeks [70]. Bang et al also suggested similar timeline for repeat imaging to identify patients suitable for early stent removal in their RCT [71]. Ahmad et al also analyzed data from 21 studies evaluating LAMS-related bleeding and reported early bleeding (< 3 weeks from procedure) to be more common than delayed bleeding (> 3 weeks from procedure), with most of early bleeding occurring in first week of procedure [70]. The authors suggested that better procedure technique, choosing the site of stent placement carefully to avoid nearby vessels, and proper preprocedure screening (to detect any pseudoaneurysm) could prevent this serious adverse event. Another recent study concluded that presence or absence of coaxial plastic stents through LAMS did not have any impact on the incidence of pseudoaneurysms [72]. This study also concluded that although the choice of initial cystenterostomy stents did not impact the incidence of pseudoaneurysms, LAMS was associated with an earlier onset of pseudoaneurysms. The authors thus emphasized the need for earlier cross-sectional imaging in patients who were treated with LAMS.
ADJUNCTIVE THERAPIES
Several approaches have been evaluated to increase the outcomes following ETD and subsequent DEN.
Nasocystic Catheter Irrigation
A nasocystic catheter is used to provide continuous irrigation and drainage of the cystic cavity to prevent or treat infections. It requires placing NCT adjacent to plastic stent or through a deployed metal stent. In studies on WON, placement of the NCT to irrigate the necrotic cavity with saline has been shown to reduce the rate of stent occlusion, potentially shortening the time required for resolution and ultimately resulting in higher short-term success rates [11,73]. Although evidence is limited, experts recommend nasocystic catheter irrigation in large complicated WON with thick necrotic debris and concomitant sepsis [74].
Hydrogen Peroxide Irrigation
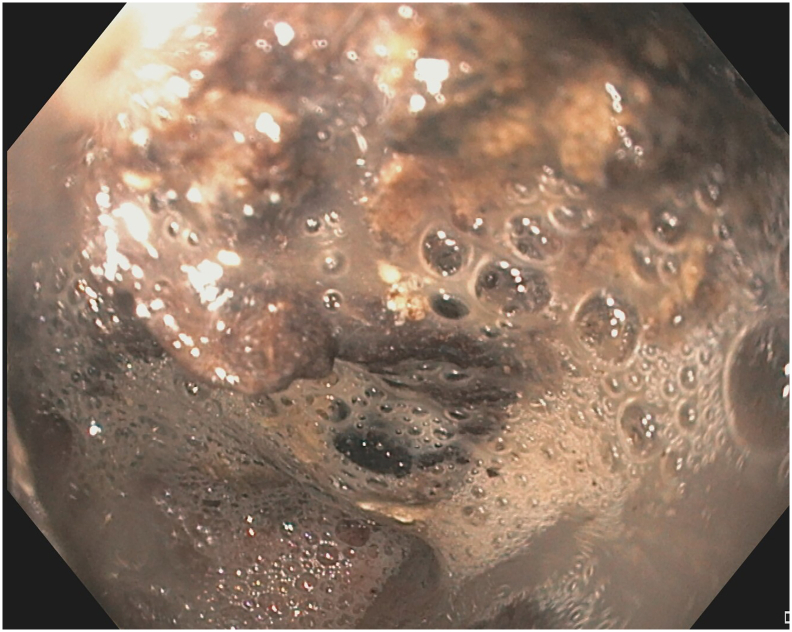
Hydrogen peroxide (H2O2) rapidly dissociates into oxygen and water when in contact with organic tissues, producing soft foam that aids in debridement of necrotic tissue (Fig 3). Also, it promotes wound healing by stimulating granulation and fibrosis. Lack of RCTs on its efficacy precludes any recommendations on optimum dose and indications for H2O2-assisted DEN. Recent multicenter comparative study and a meta-analysis have reported high clinical and technical success rates with H2O2-assisted DEN with comparable adverse events to standard necrosectomy [75,76]. The median H2O2 concentration used was 3% (range 0.1%–3%), with dilution and volume ranging from 1:1 to 10:1 and 20 mL to 1 L, respectively.
Fig 3.
Hydrogen peroxide assisted DEN.
Single and Multiple Transluminal Gateway Multiple Drainage
The traditional single transluminal gateway technique (SGT) involves placing single or multiple transmural stents with or without subsequent DEN for effective drainage of necrotic collection. However, this method is usually insufficient in management of multiple or multiloculated complicated WON. Novel innovations like multiple transluminal gateway technique (MTGT) or single transluminal gateway trancystic multiple drainage had reported good outcomes in such cases. MTGT requires creating multiple transmural fistulas between necrotic cavity and gastrointestinal lumen for better drainage of necrotic collections. This technique was first described by Varadarajulu et al in 2011 [77]. The authors reported treatment success in 11/12 (91.7%) patients treated with MTGT (creating 2–3 transmural fistulas) in comparison to 25/48 (52.1%) patients who underwent SGT. Also, need for endoscopic necrosectomy and surgery was lesser in MTGT technique. A case series of 6 patients demonstrated single-step MTGT by placing 2 LAMS with cautery enhanced tip [78]. They reported 100% technical success with mean of 2 DEN sessions. However, 2 patients had bleeding, one of whom required surgery. Therefore, more data are needed to validate efficacy and safety of this technique using multiple LAMS.
Mukai et al in 2014 described single transluminal gateway trancystic multiple drainage technique which involved additional access to extensive necrotic areas through single transmural fistula. The authors reported treatment success in all 5 patients [79]. Recently, Jagielski et al described this technique in 21 patients [80]. The authors reported therapeutic success in 20 patients and long-term success of this technique in 19 patients with median time to follow-up of 22 months. Complications were seen in 7/21 patients with bleeding as the predominant complication (managed conservatively with blood transfusions).
Dual Modality Drainage
Dual modality drainage (DMD) refers to combined transluminal and percutaneous drainage for effective management of large WON particularly with extension to paracolic gutters (Fig 4). This procedure was developed with intention to reduce rate of pancreatocutaneous fistula and need for surgery. During this procedure, placement of percutaneous drains is followed by endoscopic transmural drainage to ensure internal drainage. A comparative analysis of 49 patients undergoing DMD with 46 patients with percutaneous drainage reported shorter hospital stay and lesser number of endoscopic retrograde cholangiopancreatographies and computed tomographic scans [81]. Also, time to drain removal was shorter in DMD group. Ross et al reported 0% rate of pancreatocutaneous fistula in 103 patients of symptomatic or infected WON who completed treatment (out of 113 enrolled patients) with DMD as compared to previously reported rate of 20% with percutaneous drainage alone [82]. Also, none of the studied patients required additional surgical necrosectomy.
Fig 4.

Dual-modality drainage for WON with multiple plastic stents and large bore percutaneous catheter. (A) X-ray. (B) Computed tomography.
Role of Discontinuation of Proton Pump Inhibitors
Two retrospective studies have evaluated the role of discontinuation of proton pump inhibitor (PPI) post transmural drainage of WON. One study with large sample size reported significant difference in the required number of DEN to achieve clinical success in the PPI versus non-PPI group (4.6 vs 3.2, respectively; P < .01) [83]. Interestingly, stent occlusion occurred significantly more in the non-PPI group (9.5% vs 20.1%. P = .012). Although evidence is limited to recommend against use of PPI post drainage, its judicious use is recommended, and they should be stopped when there is no strong indication to continue their use.
Endoscopic Vacuum-Assisted Therapy
There are few case reports of successful use of endoscopic vacuum-assisted therapy and Endo-SPONGE (B. Braun, Melsungen, Germany) in management of infected WON subsequent to EUS-TMD and DEN [[84], [85], [86]]. The mechanism hypothesized is that vacuum therapy promotes healing through enhanced formation of granulation tissue, increasing vascularity and decreasing stasis, and its combination with Endo-SPONGE, which absorbs inflammatory fluids as well as results in formation of granulation tissue, is hypothesized to lead to faster resolution. However, data are still very limited, and large prospective data from RCTs are needed to recommend its routine use in clinical practice.
Powered Endoscopic Debridement (PED) System for DEN
Lack of dedicated endoscopic accessories for DEN has been a major limitation for effective endoscopic necrosectomy. Standard endoscopic accessories like dormie, basket, and snares cannot effectively remove large necrotic material. The PED device (EndoRotor PED System; Interscope, Inc, Northbridge, MA) is a novel device for DEN that removes necrotic material by simultaneous cutting and suction using negative pressure. A prospective, single-arm, multicenter trial in 30 patients with symptomatic WON concluded that patients undergoing DEN with EndoRotor system required fewer sessions of DEN when compared with studies using conventional instruments [87]. Importantly, none of these patients developed postnecrosectomy bleeding, a dreaded complication of DEN. Small sample size and lack of comparator arm were important limitations of this study, and a large sample prospective comparative study is required to determine its safety and efficacy compared to other endoscopic accessories used for DEN.
Fluid Collections Associated With Disconnected Pancreatic Duct
Disconnected pancreatic duct (DPD) complicates the clinical course of patients as the disconnected viable part of the pancreas continues to secrete pancreatic juice secretions that do not drain into the duodenum, resulting in recurrent (peri)pancreatic collections [68]. Therefore, it is advocated to prevent the closure of iatrogenic transmural internal fistula created at the time of ETD of (peri)pancreatic collections by leaving transmural plastic stents in situ permanently [68,88,89]. This strategy of leaving transmural plastic stents in situ for an indefinite period has been shown to be safe as well as effective in preventing recurrence of (peri)pancreatic collections in patients with WON and DPD successfully treated with multiple plastic stents. However, strategy of leaving transmural plastic stents in patients of WON and DPD successfully treated with LAMS has been questioned by few studies including an RCT [[90], [91], [92]]. On the other hand, few studies have supported the practice of replacing LAMS with long-term plastic stents in patients with DPD as this strategy has been shown to reduce the risk of recurrence of (peri)pancreatic collections [[93], [94], [95]]. Despite the discordant results, all these studies have demonstrated that some patients with DPD develop recurrence of (peri)pancreatic collections, and the current challenge is to identify these patients at the time of removal of LAMS so that these patients can be offered long-term plastic stents.
In conclusion, advancements in pancreatic endotherapy have revolutionized the management of local complications of acute pancreatitis. The development of EUS as well as LAMS has expanded the indications of pancreatic endotherapy from bulging pseudocysts to all types of (peri)pancreatic collections including necrotic collections with significant solid necrotic debris. The development of DEN has further improved the outcomes of endoscopic approach for treatment of pancreatic necrosis. The current management approach of (peri)pancreatic collections is a step-up approach of initial drainage followed, if necessary, by debridement. The endoscopic step approach consists of initial ETD followed by endoscopic necrosectomy if drainage alone does not result in clinical improvement. Endoscopic step-up approach is associated with better outcomes compared to surgical step-up approach because of lack of use of general anesthesia as well as surgical exploration resulting in reduction of surgical stress and surgery-associated complications such as pancreatic fistulas. The development of better endoscopic accessories for DEN is going to further improve the results of endoscopic step-up treatment approach. However, AP is a heterogeneous disease, and therefore, a single treatment strategy cannot be advocated for all the patients. The drainage route and treatment strategy depend upon on the location of (peri)pancreatic collections, extent of disease, and expertise in the various techniques and therefore are multidisciplinary decisions involving pancreatologists, surgeons, and interventional radiologists.
Author Contribution
-
1.
Vaneet Jearth: collection and interpretation of data, drafting of manuscript
-
2.
Surinder Singh Rana: collection and interpretation of data, drafting as well as critical evaluation of manuscript for intellectual content
Funding Source
None.
Ethics Approval
Not required; this is a review article.
Conflict of Interest
None.
References
- 1.Xiao A.Y., Tan M.L., Wu L.M., et al. Global incidence and mortality of pancreatic diseases: a systematic review, meta-analysis, and meta-regression of population-based cohort studies. Lancet Gastroenterol Hepatol. 2016;1:45–55. doi: 10.1016/S2468-1253(16)30004-8. [DOI] [PubMed] [Google Scholar]
- 2.Banks P.A., Bollen T.L., Dervenis C., et al. Classification of acute pancreatitis—2012: revision of the Atlanta classification and definitions by international consensus. Gut. 2013;62:102. doi: 10.1136/gutjnl-2012-302779. [DOI] [PubMed] [Google Scholar]
- 3.Boxhoorn L., Voermans R.P., Bouwense S.A., et al. Acute pancreatitis. Lancet. 2020;396:726–734. doi: 10.1016/S0140-6736(20)31310-6. [DOI] [PubMed] [Google Scholar]
- 4.Werge M., Novovic S., Schmidt P.N., et al. Infection increases mortality in necrotizing pancreatitis: a systematic review and meta-analysis. Pancreatology. 2016;16:698–707. doi: 10.1016/j.pan.2016.07.004. [DOI] [PubMed] [Google Scholar]
- 5.Baron T.H., DiMaio C.J., Wang A.Y., et al. American Gastroenterological Association clinical practice update: management of pancreatic necrosis. Gastroenterology. 2020;158:67–75.e1. doi: 10.1053/j.gastro.2019.07.064. [DOI] [PubMed] [Google Scholar]
- 6.Connor S., Neoptolemos J.P. Surgery for pancreatic necrosis: “whom, when and what”. World J Gastroenterol. 2004;10:1697–1698. doi: 10.3748/wjg.v10.i12.1697. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.van Santvoort H.C., Besselink M.G., Bakker O.J., et al. A step-up approach or open necrosectomy for necrotizing pancreatitis. N Engl J Med. 2010;362:1491–1502. doi: 10.1056/NEJMoa0908821. [DOI] [PubMed] [Google Scholar]
- 8.Rana S.S. An overview of walled-off pancreatic necrosis for clinicians. Expert Rev Gastroenterol Hepatol. 2019;13:331–343. doi: 10.1080/17474124.2019.1574568. [DOI] [PubMed] [Google Scholar]
- 9.Rana S.S., Sharma R., Kishore K., et al. Safety and efficacy of early (< 4 weeks of illness) endoscopic transmural drainage of post-acute pancreatic necrosis predominantly located in the body of the pancreas. J Gastrointest Surg. 2021;25:2328–2335. doi: 10.1007/s11605-021-04945-y. [DOI] [PubMed] [Google Scholar]
- 10.Rana S.S., Sharma V., Sharma R., et al. Endoscopic ultrasound guided transmural drainage of walled off pancreatic necrosis using a “step-up” approach: a single centre experience. Pancreatology. 2017;17:203–208. doi: 10.1016/j.pan.2017.02.007. [DOI] [PubMed] [Google Scholar]
- 11.Lakhtakia S., Basha J., Talukdar R., et al. Endoscopic “step-up approach” using a dedicated biflanged metal stent reduces the need for direct necrosectomy in walled-off necrosis (with videos) Gastrointest Endosc. 2017;85:1243–1252. doi: 10.1016/j.gie.2016.10.037. [DOI] [PubMed] [Google Scholar]
- 12.Bakker O.J., van Santvoort H.C., van Brunschot S., et al. Endoscopic transgastric vs surgical necrosectomy for infected necrotizing pancreatitis: a randomized trial. JAMA. 2012;307:1053–1061. doi: 10.1001/jama.2012.276. [DOI] [PubMed] [Google Scholar]
- 13.van Brunschot S., van Grinsven J., van Santvoort H.C., et al. Endoscopic or surgical step-up approach for infected necrotising pancreatitis: a multicentre randomised trial. Lancet. 2018;391:51–58. doi: 10.1016/S0140-6736(17)32404-2. [DOI] [PubMed] [Google Scholar]
- 14.Bang J.Y., Arnoletti J.P., Holt B.A., et al. An endoscopic transluminal approach, compared with minimally invasive surgery, reduces complications and costs for patients with necrotizing pancreatitis. Gastroenterology. 2019;156:1027–1040.e3. doi: 10.1053/j.gastro.2018.11.031. [DOI] [PubMed] [Google Scholar]
- 15.Bang J.Y., Wilcox C.M., Arnoletti J.P., et al. Superiority of endoscopic interventions over minimally invasive surgery for infected necrotizing pancreatitis: meta-analysis of randomized trials. Dig Endosc. 2020;32:298–308. doi: 10.1111/den.13470. [DOI] [PubMed] [Google Scholar]
- 16.Haney C.M., Kowalewski K.F., Schmidt M.W., et al. Endoscopic versus surgical treatment for infected necrotizing pancreatitis: a systematic review and meta-analysis of randomized controlled trials. Surg Endosc. 2020;34:2429–2444. doi: 10.1007/s00464-020-07469-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Khan M.A., Kahaleh M., Khan Z., et al. Time for a changing of guard: from minimally invasive surgery to endoscopic drainage for management of pancreatic walled-off necrosis. J Clin Gastroenterol. 2019;53:81–88. doi: 10.1097/MCG.0000000000001141. [DOI] [PubMed] [Google Scholar]
- 18.Tang P., Zha Q., Zhou L., et al. Effectiveness of digestive endoscopy and surgery in the treatment of necrotizing pancreatitis: a meta-analysis and systematic review. Gland Surg. 2021;10:2754–2765. doi: 10.21037/gs-21-516. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Varadarajulu S., Christein J.D., Tamhane A., et al. Prospective randomized trial comparing EUS and EGD for transmural drainage of pancreatic pseudocysts (with videos) Gastrointest Endosc. 2008;68:1102–1111. doi: 10.1016/j.gie.2008.04.028. [DOI] [PubMed] [Google Scholar]
- 20.Park D.H., Lee S.S., Moon S.H., et al. Endoscopic ultrasound-guided versus conventional transmural drainage for pancreatic pseudocysts: a prospective randomized trial. Endoscopy. 2009;41:842–848. doi: 10.1055/s-0029-1215133. [DOI] [PubMed] [Google Scholar]
- 21.Rana S.S., Bhasin D.K., Rao C., et al. Non-fluoroscopic endoscopic ultrasound-guided transmural drainage of symptomatic non-bulging walled-off pancreatic necrosis. Dig Endosc. 2013;25:47–52. doi: 10.1111/j.1443-1661.2012.01318.x. [DOI] [PubMed] [Google Scholar]
- 22.Braden B., Koutsoumpas A., Silva M.A., et al. Endoscopic ultrasound-guided drainage of pancreatic walled-off necrosis using self-expanding metal stents without fluoroscopy. World J Gastrointest Endosc. 2018;10:93–98. doi: 10.4253/wjge.v10.i5.93. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Consiglieri C.F., Gornals J.B., Busquets J., et al. Fluoroscopy-assisted vs fluoroless endoscopic ultrasound-guided transmural drainage of pancreatic fluid collections: a comparative study. Gastroenterol Hepatol. 2018;41:12–21. doi: 10.1016/j.gastrohep.2017.07.008. [DOI] [PubMed] [Google Scholar]
- 24.Rana S.S., Sharma R., Dhalaria L., et al. Efficacy and safety of plastic versus lumen-apposing metal stents for transmural drainage of walled-off necrosis: a retrospective single-center study. Ann Gastroenterol. 2020;33:426–432. doi: 10.20524/aog.2020.0499. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Rana S.S., Shah J., Kang M., et al. Complications of endoscopic ultrasound-guided transmural drainage of pancreatic fluid collections and their management. Ann Gastroenterol. 2019;32:441–450. doi: 10.20524/aog.2019.0404. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Talreja J.P., Shami V.M., Ku J., et al. Transenteric drainage of pancreatic-fluid collections with fully covered self-expanding metallic stents (with video) Gastrointest Endosc. 2008;68:1199–1203. doi: 10.1016/j.gie.2008.06.015. [DOI] [PubMed] [Google Scholar]
- 27.Penn D.E., Draganov P.V., Wagh M.S., et al. Prospective evaluation of the use of fully covered self-expanding metal stents for EUS-guided transmural drainage of pancreatic pseudocysts. Gastrointest Endosc. 2012;76:679–684. doi: 10.1016/j.gie.2012.04.457. [DOI] [PubMed] [Google Scholar]
- 28.Sarkaria S., Sethi A., Rondon C., et al. Pancreatic necrosectomy using covered esophageal stents: a novel approach. J Clin Gastroenterol. 2014;48:145–152. doi: 10.1097/MCG.0b013e3182972219. [DOI] [PubMed] [Google Scholar]
- 29.Sharaiha R.Z., Tyberg A., Khashab M.A., et al. Endoscopic therapy with lumen-apposing metal stents is safe and effective for patients with pancreatic walled-off necrosis. Clin Gastroenterol Hepatol. 2016;14:1797–1803. doi: 10.1016/j.cgh.2016.05.011. [DOI] [PubMed] [Google Scholar]
- 30.Bhenswala P., Lakhana M., Gress F.G., et al. Novel uses of lumen-apposing metal stents: a review of the literature. J Clin Gastroenterol. 2021;55:641–651. doi: 10.1097/MCG.0000000000001566. [DOI] [PubMed] [Google Scholar]
- 31.Bang J.Y., Navaneethan U., Hasan M.K., et al. Non-superiority of lumen-apposing metal stents over plastic stents for drainage of walled-off necrosis in a randomised trial. Gut. 2019;68:1200–1209. doi: 10.1136/gutjnl-2017-315335. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Bapaye A., Dubale N.A., Sheth K.A., et al. Endoscopic ultrasonography-guided transmural drainage of walled-off pancreatic necrosis: comparison between a specially designed fully covered bi-flanged metal stent and multiple plastic stents. Dig Endosc. 2017;29:104–110. doi: 10.1111/den.12704. [DOI] [PubMed] [Google Scholar]
- 33.Panwar R., Singh P.M. Efficacy and safety of metallic stents in comparison to plastic stents for endoscopic drainage of peripancreatic fluid collections: a meta-analysis and trial sequential analysis. Clin J Gastroenterol. 2017;10:403–414. doi: 10.1007/s12328-017-0763-y. [DOI] [PubMed] [Google Scholar]
- 34.Yoon S.B., Lee I.S., Choi M.G. Metal versus plastic stents for drainage of pancreatic fluid collection: a meta-analysis. United Eur Gastroenterol J. 2018;6:729–738. doi: 10.1177/2050640618761702. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Bang J.Y., Hawes R., Bartolucci A., et al. Efficacy of metal and plastic stents for transmural drainage of pancreatic fluid collections: a systematic review. Dig Endosc. 2015;27:486–498. doi: 10.1111/den.12418. [DOI] [PubMed] [Google Scholar]
- 36.Hammad T., Khan M.A., Alastal Y., et al. Efficacy and safety of lumen-apposing metal stents in management of pancreatic fluid collections: are they better than plastic stents? A systematic review and meta-analysis. Dig Dis Sci. 2018;63:289–301. doi: 10.1007/s10620-017-4851-0. [DOI] [PubMed] [Google Scholar]
- 37.Guzmán-Calderón E., Chacaltana A., Díaz R., et al. Head-to-head comparison between endoscopic ultrasound guided lumen apposing metal stent and plastic stents for the treatment of pancreatic fluid collections: a systematic review and meta-analysis. J Hepatobiliary Pancreat Sci. 2022;29:198–211. doi: 10.1002/jhbp.1008. [DOI] [PubMed] [Google Scholar]
- 38.Chen Y.I., Barkun A.N., Adam V., et al. Cost-effectiveness analysis comparing lumen-apposing metal stents with plastic stents in the management of pancreatic walled-off necrosis. Gastrointest Endosc. 2018;88:267–276.e1. doi: 10.1016/j.gie.2018.03.021. [DOI] [PubMed] [Google Scholar]
- 39.Siddiqui A.A., Kowalski T.E., Loren D.E., et al. Fully covered self-expanding metal stents versus lumen-apposing fully covered self-expanding metal stent versus plastic stents for endoscopic drainage of pancreatic walled-off necrosis: clinical outcomes and success. Gastrointest Endosc. 2017;85:758–765. doi: 10.1016/j.gie.2016.08.014. [DOI] [PubMed] [Google Scholar]
- 40.Garcia Garcia de Paredes A., Gonzalez Martin J.A., Foruny Olcina J.R., et al. Lumen-apposing metal stents versus biliary fully-covered metal stents for EUS-guided drainage of pancreatic fluid collections: a case control study: meeting presentations: European Society of Gastrointestinal Endoscopy ESGE Days 2018. Endosc Int Open. 2020;8:E6–e12. doi: 10.1055/a-1031-9295. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Kayal A., Taghizadeh N., Ishikawa T., et al. Endosonography-guided transmural drainage of pancreatic fluid collections: comparative outcomes by stent type. Surg Endosc. 2021;35:2698–2708. doi: 10.1007/s00464-020-07699-x. [DOI] [PubMed] [Google Scholar]
- 42.Parsa N., Nieto J.M., Powers P., et al. Endoscopic ultrasound-guided drainage of pancreatic walled-off necrosis using 20-mm versus 15-mm lumen-apposing metal stents: an international, multicenter, case-matched study. Endoscopy. 2020;52:211–219. doi: 10.1055/a-1096-3299. [DOI] [PubMed] [Google Scholar]
- 43.Aslam S., Ansari Z., Alani M., et al. Coaxial double-pigtail stent placement: a simple solution to decrease bleeding risk associated with lumen-apposing metal stent? Cureus. 2021;13 doi: 10.7759/cureus.15981. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Ali S.E., Benrajab K., Mardini H., et al. Anchoring lumen-apposing metal stent with coaxial plastic stent for endoscopic ultrasound-guided drainage of pancreatic fluid collections: any benefit? Ann Gastroenterol. 2019;32:620–625. doi: 10.20524/aog.2019.0414. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Puga M., Consiglieri C.F., Busquets J., et al. Safety of lumen-apposing stent with or without coaxial plastic stent for endoscopic ultrasound-guided drainage of pancreatic fluid collections: a retrospective study. Endoscopy. 2018;50:1022–1026. doi: 10.1055/a-0582-9127. [DOI] [PubMed] [Google Scholar]
- 46.Chandrasekhara V., Barthet M., Devière J., et al. Safety and efficacy of lumen-apposing metal stents versus plastic stents to treat walled-off pancreatic necrosis: systematic review and meta-analysis. Endosc Int Open. 2020;8:E1639–e1653. doi: 10.1055/a-1243-0092. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Aburajab M., Smith Z., Khan A., et al. Safety and efficacy of lumen-apposing metal stents with and without simultaneous double-pigtail plastic stents for draining pancreatic pseudocyst. Gastrointest Endosc. 2018;87:1248–1255. doi: 10.1016/j.gie.2017.11.033. [DOI] [PubMed] [Google Scholar]
- 48.Varadarajulu S., Rana S.S., Bhasin D.K. Endoscopic therapy for pancreatic duct leaks and disruptions. Gastrointest Endosc Clin N Am. 2013;23:863–892. doi: 10.1016/j.giec.2013.06.008. [DOI] [PubMed] [Google Scholar]
- 49.Sharma V., Rana S.S., Bhasin D.K. Endoscopic ultrasound guided interventional procedures. World J Gastrointest Endosc. 2015;7:628–642. doi: 10.4253/wjge.v7.i6.628. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Rana S.S., Gupta R. Endoscopic transluminal drainage in the early phase of acute necrotising pancreatitis. Am J Gastroenterol. 2019;114:688–689. doi: 10.1038/s41395-018-0405-0. [DOI] [PubMed] [Google Scholar]
- 51.Rana S.S., Sharma R.K., Gupta P., et al. Natural course of asymptomatic walled off pancreatic necrosis. Dig Liver Dis. 2019;51:730–734. doi: 10.1016/j.dld.2018.10.010. [DOI] [PubMed] [Google Scholar]
- 52.van Grinsven J., van Brunschot S., Bakker O.J., et al. Diagnostic strategy and timing of intervention in infected necrotizing pancreatitis: an international expert survey and case vignette study. HPB (Oxford) 2016;18:49–56. doi: 10.1016/j.hpb.2015.07.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Trikudanathan G., Tawfik P., Amateau S.K., et al. Early (< 4 weeks) versus standard (≥ 4 weeks) endoscopically centered step-up interventions for necrotizing pancreatitis. Am J Gastroenterol. 2018;113:1550–1558. doi: 10.1038/s41395-018-0232-3. [DOI] [PubMed] [Google Scholar]
- 54.Oblizajek N., Takahashi N., Agayeva S., et al. Outcomes of early endoscopic intervention for pancreatic necrotic collections: a matched case-control study. Gastrointest Endosc. 2020;91:1303–1309. doi: 10.1016/j.gie.2020.01.017. [DOI] [PubMed] [Google Scholar]
- 55.Chantarojanasiri T., Yamamoto N., Nakai Y., et al. Comparison of early and delayed EUS-guided drainage of pancreatic fluid collection. Endosc Int Open. 2018;6:E1398–e1405. doi: 10.1055/a-0751-2698. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Rana S.S., Verma S., Kang M., et al. Comparison of endoscopic versus percutaneous drainage of symptomatic pancreatic necrosis in the early (< 4 weeks) phase of illness. Endosc Ultrasound. 2020;9:402–409. doi: 10.4103/eus.eus_65_20. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Boxhoorn L., van Dijk S.M., van Grinsven J., et al. Immediate versus postponed intervention for infected necrotizing pancreatitis. N Engl J Med. 2021;385:1372–1381. doi: 10.1056/NEJMoa2100826. [DOI] [PubMed] [Google Scholar]
- 58.Guo J., Saftoiu A., Vilmann P., et al. A multi-institutional consensus on how to perform endoscopic ultrasound-guided peri-pancreatic fluid collection drainage and endoscopic necrosectomy. Endosc Ultrasound. 2017;6:285–291. doi: 10.4103/eus.eus_85_17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Nemoto Y., Attam R., Arain M.A., et al. Interventions for walled off necrosis using an algorithm based endoscopic step-up approach: outcomes in a large cohort of patients. Pancreatology. 2017;17:663–668. doi: 10.1016/j.pan.2017.07.195. [DOI] [PubMed] [Google Scholar]
- 60.Yan L., Dargan A., Nieto J., et al. Direct endoscopic necrosectomy at the time of transmural stent placement results in earlier resolution of complex walled-off pancreatic necrosis: results from a large multicenter United States trial. Endosc Ultrasound. 2019;8:172–179. doi: 10.4103/eus.eus_108_17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Pinto S., Bellizzi S., Badas R., et al. Direct endoscopic necrosectomy: timing and technique. Medicina (Kaunas) 2021;57 doi: 10.3390/medicina57121305. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Rana S.S., Bhasin D.K., Sharma R.K., et al. Do the morphological features of walled off pancreatic necrosis on endoscopic ultrasound determine the outcome of endoscopic transmural drainage? Endosc Ultrasound. 2014;3:118–122. doi: 10.4103/2303-9027.131039. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Guo J., Duan B., Sun S., et al. Multivariate analysis of the factors affecting the prognosis of walled-off pancreatic necrosis after endoscopic ultrasound-guided drainage. Surg Endosc. 2020;34:1177–1185. doi: 10.1007/s00464-019-06870-3. [DOI] [PubMed] [Google Scholar]
- 64.Chandrasekhara V., Elhanafi S., Storm A.C., et al. Predicting the need for step-up therapy after EUS-guided drainage of pancreatic fluid collections with lumen-apposing metal stents. Clin Gastroenterol Hepatol. 2021;19:2192–2198. doi: 10.1016/j.cgh.2021.05.005. [DOI] [PubMed] [Google Scholar]
- 65.Seicean A., Pojoga C., Mostean O., et al. What is the impact of the proportion of solid necrotic content on the number of necrosectomies during EUS-guided drainage using lumen-apposing metallic stents of pancreatic walled-off necrosis ? J Gastrointestin Liver Dis. 2020;29:623–628. doi: 10.15403/jgld-3128. [DOI] [PubMed] [Google Scholar]
- 66.Bush N., Rana S.S., Gupta R. Impact of solid necrotic content on the outcome of endoscopic ultrasound guided transmural drainage of walled off pancreatic necrosis. J Gastrointestin Liver Dis. 2021;30:408–409. doi: 10.15403/jgld-3777. [DOI] [PubMed] [Google Scholar]
- 67.Rana S.S., Shah J., Sharma R.K., et al. Clinical and morphological consequences of permanent indwelling transmural plastic stents in disconnected pancreatic duct syndrome. Endosc Ultrasound. 2020;9:130–137. doi: 10.4103/eus.eus_8_20. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Verma S., Rana S.S. Disconnected pancreatic duct syndrome: updated review on clinical implications and management. Pancreatology. 2020;20:1035–1044. doi: 10.1016/j.pan.2020.07.402. [DOI] [PubMed] [Google Scholar]
- 69.Arvanitakis M., Dumonceau J.M., Albert J., et al. Endoscopic management of acute necrotizing pancreatitis: European Society of Gastrointestinal Endoscopy (ESGE) evidence-based multidisciplinary guidelines. Endoscopy. 2018;50:524–546. doi: 10.1055/a-0588-5365. [DOI] [PubMed] [Google Scholar]
- 70.Ahmad W., Fehmi S.A., Savides T.J., et al. Protocol of early lumen apposing metal stent removal for pseudocysts and walled off necrosis avoids bleeding complications. Scand J Gastroenterol. 2020;55:242–247. doi: 10.1080/00365521.2019.1710246. [DOI] [PubMed] [Google Scholar]
- 71.Bang J.Y., Hasan M., Navaneethan U., et al. Lumen-apposing metal stents (LAMS) for pancreatic fluid collection (PFC) drainage: may not be business as usual. Gut. 2017;66:2054–2056. doi: 10.1136/gutjnl-2016-312812. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Abdallah M., Vantanasiri K., Young S., et al. Visceral artery pseudoaneurysms in necrotizing pancreatitis: risk of early bleeding with lumen-apposing metal stents. Gastrointest Endosc. 2022;95:1150–1157. doi: 10.1016/j.gie.2021.11.030. [DOI] [PubMed] [Google Scholar]
- 73.Siddiqui A.A., Dewitt J.M., Strongin A., et al. Outcomes of EUS-guided drainage of debris-containing pancreatic pseudocysts by using combined endoprosthesis and a nasocystic drain. Gastrointest Endosc. 2013;78:589–595. doi: 10.1016/j.gie.2013.03.1337. [DOI] [PubMed] [Google Scholar]
- 74.Boxhoorn L., Fockens P., Besselink M.G., et al. Endoscopic management of infected necrotizing pancreatitis: an evidence-based approach. Curr Treat Options Gastroenterol. 2018;16:333–344. doi: 10.1007/s11938-018-0189-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Messallam A.A., Adler D.G., Shah R.J., et al. Direct endoscopic necrosectomy with and without hydrogen peroxide for walled-off pancreatic necrosis: a multicenter comparative study. Am J Gastroenterol. 2021;116:700–709. doi: 10.14309/ajg.0000000000000987. [DOI] [PubMed] [Google Scholar]
- 76.Garg R., Gupta S., Singh A., et al. Hydrogen peroxide assisted endoscopic necrosectomy for walled-off pancreatic necrosis: a systematic review and meta-analysis. Pancreatology. 2021;21:1540–1547. doi: 10.1016/j.pan.2021.09.007. [DOI] [PubMed] [Google Scholar]
- 77.Varadarajulu S., Phadnis M.A., Christein J.D., et al. Multiple transluminal gateway technique for EUS-guided drainage of symptomatic walled-off pancreatic necrosis. Gastrointest Endosc. 2011;74:74–80. doi: 10.1016/j.gie.2011.03.1122. [DOI] [PubMed] [Google Scholar]
- 78.Binda C., Dabizzi E., Anderloni A., et al. Single-step endoscopic ultrasound-guided multiple gateway drainage of complex walled-off necrosis with lumen apposing metal stents. Eur J Gastroenterol Hepatol. 2020;32:1401–1404. doi: 10.1097/MEG.0000000000001793. [DOI] [PubMed] [Google Scholar]
- 79.Mukai S., Itoi T., Sofuni A., et al. Novel single transluminal gateway transcystic multiple drainages after EUS-guided drainage for complicated multilocular walled-off necrosis (with videos) Gastrointest Endosc. 2014;79:531–535. doi: 10.1016/j.gie.2013.10.004. [DOI] [PubMed] [Google Scholar]
- 80.Jagielski M., Smoczyński M., Adrych K. Single transluminal gateway transcystic multiple drainage for extensive walled-off pancreatic necrosis—a single-centre experience. Prz Gastroenterol. 2018;13:242–248. doi: 10.5114/pg.2018.78290. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Gluck M., Ross A., Irani S., et al. Dual modality drainage for symptomatic walled-off pancreatic necrosis reduces length of hospitalization, radiological procedures, and number of endoscopies compared to standard percutaneous drainage. J Gastrointest Surg. 2012;16:248–256. doi: 10.1007/s11605-011-1759-4. [discussion 256-7] [DOI] [PubMed] [Google Scholar]
- 82.Ross A.S., Irani S., Gan S.I., et al. Dual-modality drainage of infected and symptomatic walled-off pancreatic necrosis: long-term clinical outcomes. Gastrointest Endosc. 2014;79:929–935. doi: 10.1016/j.gie.2013.10.014. [DOI] [PubMed] [Google Scholar]
- 83.Powers P.C., Siddiqui A., Sharaiha R.Z., et al. Discontinuation of proton pump inhibitor use reduces the number of endoscopic procedures required for resolution of walled-off pancreatic necrosis. Endosc Ultrasound. 2019;8:194–198. doi: 10.4103/eus.eus_59_18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84.Loske G., Schorsch T., Gobrecht O., et al. Transgastric endoscopic vacuum therapy with a new open-pore film drainage device in a case of infective pancreatic necrosis. Endoscopy. 2016;48(Suppl. 1):E148–E149. doi: 10.1055/s-0042-106576. [DOI] [PubMed] [Google Scholar]
- 85.Wedemeyer J., Kubicka S., Lankisch T.O., et al. Transgastrically placed endoscopic vacuum-assisted closure system as an addition to transgastric necrosectomy in necrotizing pancreatitis (with video) Gastrointest Endosc. 2012;76:1238–1241. doi: 10.1016/j.gie.2012.08.014. [DOI] [PubMed] [Google Scholar]
- 86.Fähndrich M., Sandmann M. A new method for endoscopic drainage of pancreatic necrosis through a gastrostomy site using an endosponge. Endoscopy. 2014;46(Suppl. 1) doi: 10.1055/s-0034-1377554. [UCTN:E459] [DOI] [PubMed] [Google Scholar]
- 87.Stassen P.M.C., de Jonge P.J.F., Bruno M.J., et al. Safety and efficacy of a novel resection system for direct endoscopic necrosectomy of walled-off pancreas necrosis: a prospective, international, multicenter trial. Gastrointest Endosc. 2022;95:471–479. doi: 10.1016/j.gie.2021.09.025. [DOI] [PubMed] [Google Scholar]
- 88.Rana S.S., Bhasin D.K., Rao C., et al. Consequences of long term indwelling transmural stents in patients with walled off pancreatic necrosis & disconnected pancreatic duct syndrome. Pancreatology. 2013;13:486–490. doi: 10.1016/j.pan.2013.07.284. [DOI] [PubMed] [Google Scholar]
- 89.Téllez-Aviña F.I., Casasola-Sánchez L.E., Ramírez-Luna M., et al. Permanent indwelling transmural stents for endoscopic treatment of patients with disconnected pancreatic duct syndrome: long-term results. J Clin Gastroenterol. 2018;52:85–90. doi: 10.1097/MCG.0000000000000754. [DOI] [PubMed] [Google Scholar]
- 90.Basha J., Lakhtakia S., Nabi Z., et al. Impact of disconnected pancreatic duct on recurrence of fluid collections and new-onset diabetes: do we finally have an answer? Gut. 2021;70:447–449. doi: 10.1136/gutjnl-2020-321773. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 91.Dhir V., Adler D.G., Dalal A., et al. Early removal of biflanged metal stents in the management of pancreatic walled-off necrosis: a prospective study. Endoscopy. 2018;50:597–605. doi: 10.1055/s-0043-123575. [DOI] [PubMed] [Google Scholar]
- 92.Chavan R., Nabi Z., Lakhtakia S., et al. Impact of transmural plastic stent on recurrence of pancreatic fluid collection after metal stent removal in disconnected pancreatic duct: a randomized controlled trial. Endoscopy. 2022;54:861–868. doi: 10.1055/a-1747-3283. [DOI] [PubMed] [Google Scholar]
- 93.Pawa R., Dorrell R., Russell G., et al. Long-term transmural drainage of pancreatic fluid collections with double pigtail stents following lumen-apposing metal stent placement improves recurrence-free survival in disconnected pancreatic duct syndrome. Dig Endosc. 2022;34:1234–1241. doi: 10.1111/den.14266. [DOI] [PubMed] [Google Scholar]
- 94.Bang J.Y., Mel Wilcox C., Arnoletti J.P., et al. Importance of disconnected pancreatic duct syndrome in recurrence of pancreatic fluid collections initially drained using lumen-apposing metal stents. Clin Gastroenterol Hepatol. 2021;19:1275–1281.e2. doi: 10.1016/j.cgh.2020.07.022. [DOI] [PubMed] [Google Scholar]
- 95.Rana S.S., Gupta R. Disconnected pancreatic duct syndrome and lumen apposing metal stents. Clin Gastroenterol Hepatol. 2021;19:1505. doi: 10.1016/j.cgh.2020.08.056. [DOI] [PubMed] [Google Scholar]