Abstract
Background
In India, the socioeconomic shift in the past few decades has led to a sedentary lifestyle with poor dietary habits, leading to an increased incidence of overweight and obesity in children. Furthermore, obesity and anemia share some common links.
Objectives
In this study, we have prevalence of anemia and obesity in Indian schoolchildren.
Methods
The study was carried out on 1675 children and adolescent participants aged 6–18 years for the prevalence of obesity and anemia. Height, weight, waist and hip circumference were taken. Hemoglobin levels was measured for each participant.
Results
Males and females differed in height (p = 0.007), waist circumference (p = 0.019), waist-to-hip ratio (p < 0.001) and hemoglobin levels (p < 0.001). A total of 294 girls (44.4%) and 283 boys (29.7%) were anemic. There were significant differences between BMI within age groups for both boys (p < 0.001) and girls (p < 0.001). The highest percentage of anemia was observed in the 12–14 years age group in girls (54.2%) and 15–18 years-old boys (54.2%). Among the obese children, 28.2% were anemic, while 29.3% of overweight children were anemic (Pearson’s chi-squared = 7.68, p = 0.020).
Conclusion
This study sheds light on the prevalence of obesity and anemia in Indian schoolchildren and adolescents, while also suggesting an association between the two conditions. Nutritional counselling as well as lifestyle modification should be advocated in school curricula to make an early impact.
Keywords: Anemia, Obesity, Prevalence, Schoolchildren
1. Introduction
Anemia amongst children has been associated with impaired cognitive functions, developmental delays, behavioral and learning disturbances.1,2 It is commonly believed that the children who are undernourished suffer from anemia because of less intake of food and thereby low intake of iron in their diet which is essential for synthesis of hemoglobin.2 Developing countries are undergoing nutrition transition due to increased economic development and market globalization leading to rapid changes in lifestyle and dietary habits. Poor dietary habits combined with decreased physical activity have led to an increase in overweight and obesity among adults and children.3 Overweight and obese children are not only at risk for insulin resistance, hypertension, dyslipidemia and hyper-triglyceridemia, but also for micronutrient deficiency.4 Obesity and anemia due to iron deficiency are two of the most common nutritional disorders worldwide. Anemia has been associated with decreased exercise capacity, impaired cognitive function, developmental delays, and behavioral dist urbances.5,6 Obese children are at risk of increased morbidity starting already in childhood or adolescence.7 Despite their excessive dietary and caloric intake, obese children and adolescents may be at risk of ID (Iron deficiency) because they tend to consume unbalanced meals, particularly rich in carbohydrates and fat. Both obesity and ID are also more prevalent in all socioeconomic groups, who consume fast-foods that are low in essential nutrients and rich in fats, sugars and preservatives. In view of the above, the present study was carried out to ascertain the prevalence of anemia and obesity in school children, within the age group 6–18 years. The objectives of the study were – 1) To find out the prevalence of anaemia in children & adolescents, 2) Prevalence of overweight and obesity in children & adolescents, 3) To assess whether overweight children and adolescents are at increased risk of anemia.
2. Methodology
2.1. Ethical considerations and participant recruitment
All research carried out regarding this manuscript adheres to the guidelines of the Declaration of Helsinki involving human subjects and conducted after Ethical Committee approval.
The study was carried out in one of the leading public school of Udhampur city. All school children aged 6–18 yrs were included in the study after getting informed consent from their parents as well as from school staff.
2.2. Subjective parameters
1) Age was recorded from birthday by calendar to the nearest of year (<6 months and >6 months); 2) Standing height was recorded without shoes and with light clothes on a wall mounted measuring tape to the nearest of centimeters (<5 mm and >5 mm); 3) Weight was recorded without shoes and with light clothes on a Krups weighing machine; 4) BMI was calculated by the formula, BMI = Weight (kg)/{Height (m)}2; 5) Overweight & obesity were determined by body mass index (BMI) for age and gender as per WHO growth chart. BMI was taken as follows: between 5th to 85 above 85th percentile-Normal, between 85th to 97th percentile-Overweight, above 97th percentile – Obese.
Hemoglobin was measured by colorimeter using drabkin dilution method. Anemia was diagnosed and classified according to severity following the WHO guidelines.8
2.3. Statistical analysis
Data was analysed by SPSS software ver 22. P-value <0.05 was considered statistically significant.
3. Results
A total of 1675 participants were surveyed, among which 60.5% were males and 39.5% were females (Table 1). The difference in age between males and females (median age 10 years for both) was non-significant (p = 0.70). However, they differed in height (median [IQR] boys 140 [125–158], girls 138 [122–153], p = 0.007), waist circumference (median [IQR] boys 59 [52–68], girls 58 [51–65], p = 0.019), waist-to-hip ratio (median [IQR] boys 0.87 [0.83–0.90], girls 0.85 [0.81–0.89], p < 0.001) and hemoglobin levels (median [IQR] boys 12.8 [11.5–13.7], girls 11.9 [11.0–12.8], p < 0.001). A total of 294 girls (44.4%) and 283 boys (29.7%) were anemic (Tables 2 and 3). There were significant differences between BMI within age groups for both boys (median [IQR] for 6–11 years: 22.77 [20.16–23.79], 12–14 years: 27.11 [27.06–27.19], 15–18 years: 29.75 [28.38–30.83], p < 0.001) and girls (median [IQR] for 6–11 years: 23.38 [21.89–24.87], 12–14 years: 29.28 [27.39–30.98], 15–18 years: 30.11 [29.32–30.49], p < 0.001) (Tables 4 and 5, Fig. 1). The highest percentage of anemia was observed in the 12–14 years age group in girls (54.2%) and 15–18 year-old boys (54.2%). Also, 4.4% of boys and 4.9% of girls were found to be obese, whereas 8.4% boys and 9.2% girls were overweight. Among the obese children, 28.2% were anemic, while 29.3% of overweight children were anemic (Pearson’s chi-squared = 7.68, p = 0.020) (Table 6, Fig. 2). A total of 30.9% schoolchildren were anemic in the normal weight group.
Table 1.
Anthropometric and blood parameters of school children.
| Parameters | Boys (1014) Median (IQR) |
Girls (661) Median (IQR) |
p-value |
|---|---|---|---|
| Age (yrs) | 10 (7–13) | 10 (7–13) | 0.697 |
| Weight (kg) | 33 (24–45) | 33 (23–45) | 0.239 |
| Height (cm) | 140 (125–158) | 140 (122–153) | 0.007* |
| BMI (kg/m2) | 16.22 (14.48–18.77) | 16.42 (14.41–19.11) | 0.314 |
| Waist (cm) | 59 (52–68) | 58 (51–65) | 0.019* |
| Hip (cm) | 69 (60–80) | 70 (59–80) | 0.777 |
| Waist-Hip ratio | 0.87 (0.83–0.9) | 0.85 (0.81–0.89) | <0.001* |
| Hb (g/dl) | 12.8 (11.5–13.7) | 11.9 (11–12.8) | <0.001* |
Statistically significant at p < 0.05 by Wilcoxon rank sum test.
The difference between height, waist, waist-hip ratio & hemoglobin of boys and girls were found to be statistically significant (p < 0.05).
Table 2.
Anemia in schoolgirls.
| Age (yrs) | Girls (N = 661) | Girls (N = 294) | |||
|---|---|---|---|---|---|
|
|
|
||||
| Anemia present No (%) | Anemia absent No (%) | Mild Anemia No (%) | Moderate Anemia No (%) | Severe Anemia No (%) | |
| 6–11 | 168 (40.3%) | 248 (59.6%) | 62 (14.9%) | 106 (25.4%) | 0 |
| 12–14 | 89 (54.2%) | 75 (45.8%) | 64 (39.0%) | 25 (15.2%) | 0 |
| 15–18 | 37 (45.7%) | 44 (54.3%) | 23 (29.1%) | 12 (15.1%) | 2 (2.5%) |
There is no statistical significant difference in the Hb level of different age group among school girls.
Table 3.
Anemia in schoolboys.
| Age (yrs) | Boys (N = 1014) | Boys (N = 283) | |||
|---|---|---|---|---|---|
|
|
|
||||
| Anemia present No (%) | Anemia absent No (%) | Mild Anemia No (%) | Moderate Anemia No (%) | Severe Anemia No (%) | |
| 6–11 | 160 (27.4%) | 424 (72.6%) | 58 (9.2%) | 101 (16.0%) | 1 (0.1%) |
| 12–14 | 34 (12.7%) | 232 (87.2%) | 28 (10.5%) | 6 (2.2%) | 0 |
| 15–18 | 89 (54.2%) | 75 (45.7%) | 64 (39.0%) | 25 (15.2%) | 0 |
There is statistical significant in the Hb levels of different age group among school boys.
Table 4.
Descriptive statistics of overweight and obese schoolgirls.
| Age (yrs) | Girls | |||
|---|---|---|---|---|
|
| ||||
| Obese No (%) |
Overweight No (%) |
Normal No (%) |
Underweight No (%) |
|
| 6–11 | 26 (6.2%) | 32 (7.6%) | 276 (66.1%) | 83 (1.9%) |
| 12–14 | 4 (2.4%) | 22 (13.3%) | 119 (72.1%) | 20 (12.1%) |
| 15–18 | 3 (3.7%) | 7 (8.8%) | 59 (74.6%) | 10 (12.6%) |
| Total | 33 (4.9%) | 61 (9.2%) | 454 (68.6%) | 113 (17.0%) |
Table 5.
Descriptive statistics of overweight and obese schoolboys.
| Age (yrs) | Boys | |||
|---|---|---|---|---|
|
| ||||
| Obese No (%) |
Overweight No (%) |
Normal No (%) |
Underweight No (%) |
|
| 6–11 | 37 (5.8%) | 56 (8.8%) | 361 (57.2%) | 177 (28.05%) |
| 12–14 | 5 (1.8%) | 21 (7.8%) | 196 (73.6%) | 44 (16.5%) |
| 15–18 | 3 (2.5%) | 9 (7.6%) | 86 (73.5%) | 19 (16.3%) |
| Total | 45 (4.4%) | 86 (8.4%) | 643 (63.4%) | 240 (23.6%) |
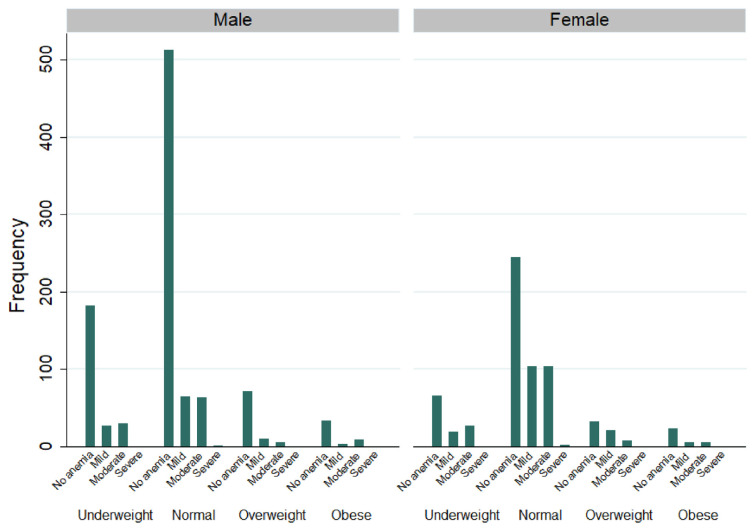
Fig. 1.
Anemia frequency in different weight groups.
Table 6.
Descriptive statistics of anemia in overweight and obese schoolchildren.
| Age (yrs) | Obese No (%) |
Overweight No (%) |
Normal No (%) |
Underweight No (%) |
|---|---|---|---|---|
| No anemia | 56 (71.7%) | 104 (70.7%) | 758 (69.1%) | 250 (70.8%) |
| Mild | 8 (10.2%) | 31 (21.0%) | 169 (15.4%) | 46 (13.0%) |
| Moderate | 14 (17.9%) | 12 (8.1%) | 167 (15.2%) | 57 (16.1%) |
| Severe | 0 | 0 | 3 (0.3%) | 0 |
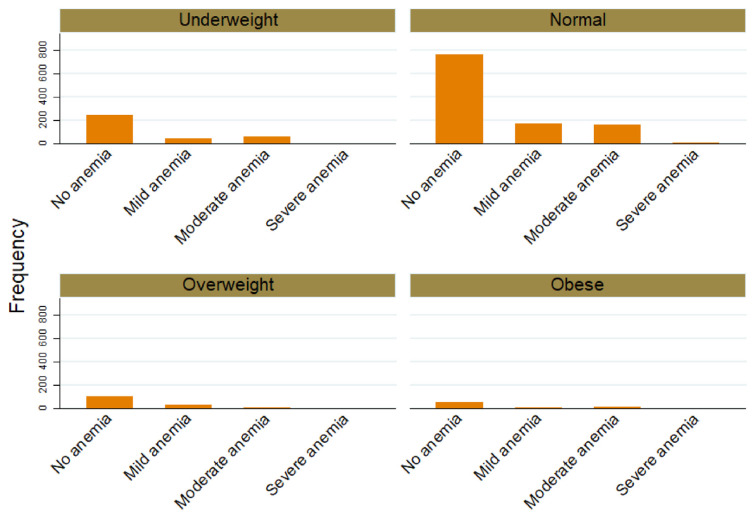
Fig. 2.
Frequency of different grades of anemia in normal and underweight children.
4. Discussion
Anemia remains a burning issue in the Indian population. However, the increased incidence of obesity has turned it into a twofold crisis. In this article, we have discussed the prevalence of both anemia and obesity in Indian schoolchildren and adolescents as well as their association. A number of studies9–15 have previously commented on the prevalence of anemia in Indian population. Varghese and Stein16 had analysed the fourth round of the National Family Health Survey (NFHS-4) data of 145,653 children (6–59 months of age) and 655,156 women across 36 states and 640 districts in India but found no significant clustering of overweight and anemia. The prevalence of anemia in children aged 5–9 years and 10–19 years, according to the NFHS-4, were in the range 81–95% and 49–90%, respectively.14 The anemia prevalence of 6–59-month-old children saw a drop of 13.5% since NFHS-3.11 A study15 among Santal Adivasi children in Birbhum district of West Bengal revealed that 73.3% suffered from moderate to severe anemia, lagging behind the national average of 58.5%. Our study shows the prevalence of anemia to be 54.2% which is lesser than the national average which could be attributed to the fact that our subjects were children from middle income groups. On the other hand, the prevalence of overweight among school going population of 5–18 years of age in Delhi were 0.1% and 2.7%, 0.6% and that of obesity were 6.5%, and 6.8% and 15.3% in low-income, middle-income and high-income groups, respectively.17 A similar study in Chandigarh which sampled data from 1030 school going children in the age group 10–14 years, the prevalence of overweight and obesity were 9.9% and 14.0%, respectively.18 In another study,19 children aged 6–15 years had 7.5% prevalence of obesity; also, it was 3.0% and 5.3% for boys and girls, respectively. Our study shows a prevalence of 4.4% among boys and 4.9% among girls. This population surveyed were children from middle income group, hence we do not see very high prevalence of obesity in our group as compared to studies which have surveyed high income group children. However, there is a dearth of studies reporting the association between obesity and anemia in Indian schoolgoing children. Siyaram et al.20 reported a 28% anemia in children, albeit a low sample size (n = 71). Obesity and obesity-related disorders affect iron homeostasis. Anemia, especially iron deficiency anemia is observed in obese subjects. Also, obesity is a hyper-inflammatory state, high levels of ferritin are expected. Indeed, hyper-ferritinemia and high transferrin saturation is seen in patients of metabolic syndrome, known as the “dysmetabolic iron overload syndrome”.21 In India, iron-deficiency anemia is the most common cause of nutritional anemia. In a recent Indian study, the prevalence of anemia was 53.2%, out of which 45.1% were anemic males and 54.6% anemic females.22 In this study, we found the prevalence of anemia to be higher in females than males, while obesity was observed to be higher in males. In obesity, there are profound changes in energy metabolism in various organs, including liver and adipose tissue, and they are closely and distinctly related to iron homeostasis. The NHANES population study showed that low transferrin and low serum ferritin were twice as high in overweight adolescents compared to normal weight adolescents.23 Conversely, in lean adolescents, higher serum ferritin and transferrin correlated with higher BMI quartiles.24 In adults, too, iron deficiency is associated with severe obesity. However, there was generally a higher haemoglobin concentration and ferritin concentration compared to normal weight subjects.25 In a cross-sectional study involving 256 adult Iranian women showed that only 13.4% of the obese women had iron deficiency anemia.26 Hence, the decrease of serum iron and transferrin saturation in adolescents may be attributed to the obesity-related inflammation.21 Moreover, BMI can be a non-invasive screening tool to identify the adolescents who are prone to anemia.27 Further, the treatment of iron-deficiency anemia has been shown to induce weight loss and the improvement of several metabolic parameters.28 Iron status improvement was observed in weight reduction surgeries.29,30 The assessment of iron status is recommended during follow-up after bariatric surgery.
The etiology of anemia in children in India is multifactorial, and includes hemoglobinopathies and anemia, malnutrition. The prevalence of pathological hemoglobinopathies is 1.2 per 1000 live births.31 A few major causes of anemia in children include thalassemia syndromes (trait, intermedia and major) and sickle cell disease which are very common in India and can co-exist with iron deficiency. In present times, automated CBC counters do help in early diagnosis of haemoglobinopathies based on Mentzer’s index. Intestinal parasitic infections are also a common cause of anaemia in children. In our study, Hb for screening was estimated by cyanmeth haemoglobin method, hence RBC indices were not present for referring patients for High pressure liquid chromatography for diagnosis of haemoglobinopathies. Furthermore, children were from middle income families, hence malnutrition as a cause of anemia could be ruled out. As the study primarily was conducted as a medical check-up for school children, all children with anemia, identified in our study, were referred to paediatrician for medical treatment.
5. Conclusion
We have reported the prevalence of obesity and anemia in Indian schoolchildren and adolescents, which suggests an association between the two conditions. The obesity epidemic has caught up to the Indian population due to a seismic shift in the socioeconomic status and sedentary lifestyle. Despite the increase in calorie consumption, obese children are still nutritionally challenged. To combat this, we can employ certain measures, such as education on balanced diet, less consumption of high calorie fast foods, and banning of the same from school canteens, distribution of diet sheets, encouraging physical exercise and making physical education and sports mandatory in the school curriculum, and creating awareness in children early on.
Acknowledgements
None.
Footnotes
Author contributions
Concept and Design: 1A; Data Acquisition: 1A; Data analysis and interpretation: 1A, 2A, 3A; Manuscript drafting: 3A; Critical revision of the manuscript: 1A, 2A; Statistical analysis: 1A, 2A, 3A; Supervision: 1A.
Funding
None.
Conflict of interest
The authors declare no potential conflicts of interest.
References
- 1. Pollitt E. The developmental and probabilistic nature of the functional consequences of iron-deficiency anemia in children. J Nutr. 2001 Feb;131(2S-2):669S–675S. doi: 10.1093/jn/131.2.669S. [DOI] [PubMed] [Google Scholar]
- 2. Halterman JS, Kaczorowski JM, Aligne CA, Auinger P, Szilagyi PG. Iron deficiency and cognitive achievement among school-aged children and adolescents in the United States. Pediatrics. 2001 Jun;107(6):1381–1386. doi: 10.1542/peds.107.6.1381. [DOI] [PubMed] [Google Scholar]
- 3.World Health Organization. Diet, nutrition and prevention of chronic diseases, WHO technical report series. Geneva: Report of a joint WHO/FAO expert consultation; 2003. [Google Scholar]
- 4. Li YP, Yang KG, Zhai FY, et al. Disease risks of childhood obesity in China. Biomed Environ Sci. 2005;18:401–410. [PubMed] [Google Scholar]
- 5. Bhatia D, Seshadri S. Growth performance in anemia and following iron supplementation. Indian Pediatr. 1993;30:195–200. [PubMed] [Google Scholar]
- 6. Saloojee H, Pettifor JM. Iron deficiency and impaired child development. Br Med J. 2001;15:1377–1378. doi: 10.1136/bmj.323.7326.1377. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Barlow ES, Dietz WH. The Maternal and Child Health Bureau, Health Resources and Services Administration and the Department of Health and Human Services. Obesity evaluation and treatment: expert committee recommendations. Pediatrics. 1998;102:E29. doi: 10.1542/peds.102.3.e29. [DOI] [PubMed] [Google Scholar]
- 8.World Health Organization. Haemoglobin concentrations for the diagnosis of anaemia and assessment of severity. Available at: https://www.who.int/vmnis/indicators/haemoglobin.pdf.
- 9. Patel A, Prakash AA, Das PK, Gupta S, Pusdekar YV, Hibberd PL. Maternal anemia and underweight as determinants of pregnancy outcomes: cohort study in eastern rural Maharashtra, India. BMJ Open. 2018 Aug 8;8(8):e021623. doi: 10.1136/bmjopen-2018-021623. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Pathania A, Haldar P, Kant S, Gupta SK, Pandav CS, Bachani D.Prevalence of anemia among elderly persons residing in old age homes in national capital territory, Delhi, India Indian J Publ Health 2019. Oct–Dec634288–292. 10.4103/ijph.IJPH_412_18 [DOI] [PubMed] [Google Scholar]
- 11. Bharati S, Pal M, Bharati P. Prevalence of anaemia among 6-to 59-month-old children in India: the latest picture through the NFHS-4. J Biosoc Sci. 2020 Jan;52(1):97–107. doi: 10.1017/S0021932019000294. . Epub 2019 May 20. [DOI] [PubMed] [Google Scholar]
- 12. Hussain S, Habib A, Najmi AK. Anemia prevalence and its impact on health-related quality of life in Indian diabetic kidney disease patients: evidence from a cross-sectional study. J Evid Base Med. 2019 Nov;12(4):243–252. doi: 10.1111/jebm.12367. [DOI] [PubMed] [Google Scholar]
- 13. Kant S, Kumar R, Malhotra S, Kaur R, Haldar P. Prevalence and determinants of anemia among adult males in a rural area of Haryana, India. J Epidemiol Glob Health. 2019 Jun;9(2):128–134. doi: 10.2991/jegh.k.190513.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14. Kapil U, Kapil R, Gupta A. Prevention and control of anemia amongst children and adolescents: theory and practice in India. Indian J Pediatr. 2019 Jun;86(6):523–531. doi: 10.1007/s12098-019-02932-5. . Epub 2019 May 11. [DOI] [PubMed] [Google Scholar]
- 15. Stiller CK, Golembiewski SKE, Golembiewski M, Mondal S, Biesalski HK, Scherbaum V. Prevalence of undernutrition and anemia among santal Adivasi children, Birbhum district, West Bengal, India. Int J Environ Res Publ Health. 2020 Jan 3;17(1):342. doi: 10.3390/ijerph17010342. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16. Varghese JS, Stein AD. Malnutrition among women and children in India: limited evidence of clustering of underweight, anemia, overweight, and stunting within individuals and households at both state and district levels. Am J Clin Nutr. 2019 Apr 1;109(4):1207–1215. doi: 10.1093/ajcn/nqy374. [DOI] [PubMed] [Google Scholar]
- 17. Kaur S, Sachdev HP, Dwivedi SN, Lakshmy R, Kapil U. Prevalence of overweight and obesity amongst school children in Delhi, India. Asia Pac J Clin Nutr. 2008;17(4):592–596. [PubMed] [Google Scholar]
- 18. Singh DP, Arya A, Kondepudi KK, Bishnoi M, Boparai RK. Prevalence and associated factors of overweight/obesity among school going children in Chandigarh, India. Child Care Health Dev. 2020 Sep;46(5):571–575. doi: 10.1111/cch.12794. . Epub 2020 Jul 7. [DOI] [PubMed] [Google Scholar]
- 19. Cherian AT, Cherian SS, Subbiah S. Prevalence of obesity and overweight in urban school children in Kerala, India. Indian Pediatr. 2012 Jun;49(6):475–477. doi: 10.1007/s13312-012-0070-0. [DOI] [PubMed] [Google Scholar]
- 20. Siyaram D, Bhatia P, Dayal D, Bhalla AK, Marathe R. Hypoferremic state in overweight and obese children. Indian Pediatr. 2018 Jan 15;55(1):72–73. [PubMed] [Google Scholar]
- 21. Aigner E, Feldman A, Datz C. Obesity as an emerging risk factor for iron deficiency. Nutrients. 2014;6(9):3587–3600. doi: 10.3390/nu6093587. . Published 2014 Sep. 11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22. Kishore S, Singh M, Jain B, et al. A study to assess prevalence of anaemia among beneficiaries of Anaemia Mukt Bharat Campaign in Uttarakhand. J Fam Med Prim Care. 2020;9(3):1691–1694. doi: 10.4103/jfmpc.jfmpc_941_19. . Published 2020 Mar 26. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23. Nead KG, Halterman JS, Kaczorowski JM, Auinger P, Weitzman M. Overweight children and adolescents: a risk group for iron deficiency. Pediatrics. 2004;114:104–108. doi: 10.1542/peds.114.1.104. [DOI] [PubMed] [Google Scholar]
- 24. Aigner E, Hinz C, Steiner K, et al. Liver transaminase levels and metabolic risk in healthy teenagers. Eur J Clin Invest. 2010;40:155–163. doi: 10.1111/j.1365-2362.2009.02238.x. [DOI] [PubMed] [Google Scholar]
- 25. Cheng HL, Bryant C, Cook R, O’Connor H, Rooney K, Steinbeck K. The relationship between obesity and hypoferraemia in adults: a systematic review. Obes Rev. 2012;13:150–161. doi: 10.1111/j.1467-789X.2011.00938.x. [DOI] [PubMed] [Google Scholar]
- 26. Adib Rad H, Sefidgar SAA, Tamadoni A, et al. Obesity and iron-deficiency anemia in women of reproductive age in northern Iran. J Educ Health Promot. 2019;8(115) doi: 10.4103/jehp.jehp_371_18. . Published 2019 Jun 27. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. Pande S, Ranjan R, Kratasyuk VA. Is Body mass index a potential biomarker for anemia in obese adolescents? JNIM. 2019;15:1–2. doi: 10.1016/j.jnim.2018.11.001. [DOI] [Google Scholar]
- 28. Aktas G, Alcelik A, Yalcin A, et al. Treatment of iron deficiency anemia induces weight loss and improves metabolic parameters. Clin Ter. 2014;165:e87–e89. doi: 10.7471/CT.2014.1688. [DOI] [PubMed] [Google Scholar]
- 29. Anty R, Dahman M, Iannelli A, et al. Bariatric surgery can correct iron depletion in morbidly obese women: a link with chronic inflammation. Obes Surg. 2008;18:709–714. doi: 10.1007/s11695-007-9276-y. [DOI] [PubMed] [Google Scholar]
- 30. Ramalho R, Guimaraes C, Gil C, Neves C, Guimaraes JT, Delgado L. Morbid obesity and inflammation: a prospective study after adjustable gastric banding surgery. Obes Surg. 2009;19:915–920. doi: 10.1007/s11695-009-9848-0. [DOI] [PubMed] [Google Scholar]
- 31. Colah R, Italia K, Gorakshakar A. Burden of thalassemia in India: the road map for control. Pediat Hematol Oncol J. 2017;2(4):79–84. [Google Scholar]