Abstract
Previous research has shown that job loss, financial strain, and/or loss of housing (JFH) in midlife elevate suicide risk. In this study based on the 2017–2019 National Violent Death Reporting System, we examined other suicide precipitants and contributors of decedents whose suicide was in part precipitated by JFH and the circumstances under which they died. First, we examined all adult decedents (N = 94,454; 74,042 males [78.4%] and 20,412 females [21.6%]) and then focused on decedents age 45–64 (N = 34,208; 25,640 males [75%] and 8568 females [25.0%]). The 45–64 age group had the highest rate of JFH (22.0% for males and 15.1% for females) as a suicide precipitant. The results of generalized linear models for all adult suicide decedents of both sexes showed that the 45–64 age group (IRR = 2.02, 95% CI = 1.89–2.16), compared to 65+ age group, and relationship problems, mental disorders, and alcohol problems were associated with significantly higher risk of JFH-precipitated suicide. In male decedents age 45–64, JFH was positively associated with depressed mood (IRR = 1.95, 95% CI = 1.85–2.06), alcohol problems (IRR = 1.14, 95% CI = 1.07–1.21), and number of crises (IRR = 1.48, 95% CI = 1.43–1.53). In female decedents age 45–64, JFH was positively associated with relationship problems (IRR = 1.19, 95% CI = 1.05–1.35), legal problems (IRR = 1.27, 95% CI = 1.06–1.54), depressed mood (IRR = 1.78, 95% CI = 1.59–1.99), and number of crises (IRR = 1.58, 95% CI = 1.48–1.68). In both sexes, the risk of JFH was also positively associated with a college education. In female decedents, JFH risk was higher among divorced or never-married individuals. Coroner/medical examiner and law enforcement agency reports show that some experienced depression and started misusing alcohol and/or other substances following a job loss, but others had these problems throughout life, which caused/contributed to JFH. These findings show the significance of suicide prevention approaches at both systemic (generous unemployment insurance, housing subsidies) and individual (treatment of depression and alcohol/substance misuse problems and social support/connection) levels.
Keywords: Suicide, Job loss, Financial stress, Housing instability, Depression, Alcohol misuse
Highlights
-
•
16.2% of male and 13.0% of female suicide decedents age 18+ in 2017–2019 had job/finance/housing problems (JFH).
-
•
Among decedents age 45–64, 22.0% of male and 15.1% of female had JFH.
-
•
JFH was positively associated with number of crises, depressed mood, and relationship and alcohol problems in both sexes.
-
•
Suicide prevention approaches are needed at both systemic and individual levels.
1. Introduction
Research shows that increased rates of job loss, financial distress/poverty, and housing loss during economic recessions were associated with increases in suicide attempts and suicide among working-age adults, particularly middle-aged White males in the U.S. (Haw et al., 2015; Houle & Light, 2017; Kerr et al., 2017; Milner et al., 2014; Ilgun et al., 2021). Regardless of macroeconomic context, job loss and unemployment, financial strain (e.g., debts/bankruptcy), and/or foreclosure of housing or eviction due to unaffordability elevate suicide risk among affected individuals as these events may set off or exacerbate existing depression, other mental health, and alcohol and/or other substance use problems (Blakely et al., 2003; Elbogen et al., 2020; Frasquilho et al., 2016; Kaplan et al., 2016). Suicide risk is further heightened when job loss/unemployment is coupled with other stressful life events and poor social support (Milner et al., 2013; Pompili et al., 2014; Stack, 2021).
Understandably, the impact of job loss is harder on middle-aged or late-middle-aged individuals given a significant negative relationship between age and reemployment status and speed of reemployment (Wanberg et al., 2016). Job loss for many individuals in this age group may also trigger a sense of loss of status, perceived control, and self-esteem, and engender shame, grief, and despair, leading to severe psychological distress, relationship problems, family disruptions and divorce, physical health problems (especially cardiovascular diseases), and/or suicide and premature nonsuicide mortality (Anaf et al., 2013; Brand, 2015; Doiron & Mendolia, 2012; Gallo et al., 2006; Mulia et al., 2014; Nie et al., 2020; Roelfs et al., 2011).
Systematic reviews of studies also found that stress from home foreclosure or eviction, by itself or following a job loss, negatively affected/worsened both physical and mental health, increased adverse/violent behavior, and decreased access to healthcare (Downing, 2016; Tsai, 2015). A study of suicide decedents, 2005–2010, reported that foreclosure-related suicides increased more than 250% during the study period and most suicides occurred before the actual housing loss, suggesting that there is a window of opportunity to prevent suicide during often-protracted foreclosure/eviction procedures (Fowler et al., 2015). A study that examined the association between foreclosures and race-by-sex specific suicide rates, 2005–2010, also found that the relationship was particularly strong for White males (Houle & Light, 2017).
Case and Deaton (2015, 2020) showed that rising rates of alcohol and drug poisonings and suicide, which they referred to as “deaths of despair,” during the late 1990 through mid-2010's were responsible for a marked increase in the morbidity and mortality of middle-aged (45–54) non-Hispanic Whites of both sexes. They also showed that increased morbidity and mortality was especially salient among middle-aged Whites without a college degree and proposed progressively worsening labor market opportunities at the time of this cohort's entry as the primary probable cause (Case & Deaton, 2017, 2020). Unemployment rates for all age groups decreased steadily since 2010 till 2020 (when the COVID-19 started) (U.S. Bureau of Labor Statistics, 2022). Suicide rates for both male and female working-age people generally increased between 2000 and 2017 and then decreased in 2018 and 2019. However, suicide rates for males age 45–64 remained the second highest after the 75+ age group, and those for females age 45–64 remained the highest among females over the past two decades (Garnett et al., 2022, pp. 1–8).
Although many previous studies investigated the associations between job/financial/housing problems and suicide, our review showed that most tended to focus on a single issue (e.g., unemployment, eviction), suicide rates, and a limited number of moderators or mediators (e.g., mental health, alcohol problems). Economic effects from job loss cannot be separated from financial and housing problems and other suicide precipitants and contributors. The present study, based on the 2017–2019 National Violent Death Reporting System (NVDRS), aimed to examine other suicide precipitants and contributors of decedents whose suicide was in part precipitated by job/financial/housing problems (JFH hereafter) and the circumstances under which they died.
We first compared all adult suicide decedents with and without JFH with respect to demographic characteristics, other suicide precipitating factors, mental illness, and alcohol and other substance use problems. Based on significant sex differences in suicide rates, we conducted separate analyses for males and females. Second, given the high suicide rates for the 45–64 age group and the disproportionate impact of JFH on them, we also conducted separate analyses for this age group to compare differences in characteristics between those with and without JFH. Based on previous study findings, we posited the following hypotheses: (H1) male decedents in all age groups with JFH as a suicide precipitant would have higher rates of relationship problems, mental disorder, and alcohol and substance use problems than those without; and (H2) among decedents aged 45–64, male decedents with than without JFH would also have higher rates of physical health problems. We did not pose any hypothesis for female decedents who had JFH as a suicide precipitant, as little research has been done on these women; however, per Case & Deaton (2015, 2020), we expected similar pattern for both sexes. We also expected that compared to non-Hispanic Whites, racial/ethnic minority groups would have lower odds of having had JFH as a suicide precipitant. The study findings will provide more insight into multiple stressful life events of decedents whose suicide was in part JFH-precipitated.
2. Material and methods
2.1. Data source
NVDRS is the only state-based violent death reporting system in the US that provides information and context on when, where, and how violent deaths occur and who is affected (National Center for Injury Prevention and Control [NCIPC], 2021). NVDRS links data from death certificates and reports from coroners/medical examiners (CME) and law enforcement (LE) agencies on cases of violent deaths: suicides, homicides, deaths from legal intervention (i.e., victim killed by LE acting in the line of duty), deaths of undetermined intent, and unintentional firearm deaths. CME/LE reports are from the injury/death scene, ongoing investigations, or family/friend accounts, and often serve as the basis of the circumstances of death as well as NVDRS variables that were “calculated” (coded “Yes” when endorsed by the CME and/or LE reports vs. “No/not available/unknown”). When available, crime lab and toxicology reports included in CME reports are also abstracted and entered in NVDRS.
We used 2017–2019 NVDRS data because the number of participating states increased from 27 in 2017 to 37 in 2017 and to 43 states, the District of Columbia, and Puerto Rico in 2019, although not all states provided complete data for all three years (NCIPC, 2020). Our preliminary analysis showed that some important results vary depending on the number of participating states. Our preliminary analysis also showed that a small proportion of suicide cases during the study period are missing CME or LE reports. The authors of this study were granted access to de-identified NVDRS data, 2017–2019, by the Centers for Disease Control and Prevention's NVDRS-Restricted Access Data (RAD) review committee. In this study, we first focused on suicide decedents aged 18 and older (N = 94,454; 74,042 males [78.4%] and 20,412 females [21.6%], after excluding 3 decedents with missing data on sex). Then, we focused on the 45–64 age group (N = 34,208; 25,640 males [75%] and 8568 females [25.0%]). This study based on decedents was exempt from the authors' institutional review board's review.
2.2. Measures
Demographic variables: Data on age at the time of death, sex, race/ethnicity, marital status, level of education, and military service status were from the death certificates and CME/LE reports. We also included census region (Northeast, Midwest, South, West, Puerto Rico and US territories) of decedents’ residence to examine possible geographic differences. In this study, decedents were categorized into 18–24, 25–44, 45–64, and 65+ age groups to examine age group differences, and the 65+ age group was used as the reference category in multivariable models for all decedents because this age group was least likely to have job/financial/housing problems.
JFH as suicide precipitants: Job problems refer to job loss (fired or laid off) and/or difficulties finding/keeping a job or difficulties with demotion or serious conflict/stress at work. Financial problems refer to financial difficulties, e.g., bankruptcy, overwhelming debts, or foreclosure of a home or business. Eviction or loss of housing refers to a recent eviction or other loss of the victim's housing, or the threat of it. Although the NVDRS coded job problems, financial problems, and eviction or loss of housing separately, we combined them into a single category in this study given that these problems tend to occur in step with one another (i.e., job loss leading to financial problems and finally, loss of housing).
Other suicide precipitants: These included physical health problems, relationship problems, suicide/death of family/friend, and criminal/civil legal problems in NVDRS. Physical health problems were recorded “Yes” only if any diagnosed or perceived physical health problem (e.g., terminal disease, debilitating condition, chronic pain) was relevant to the death (e.g., “despondent over recent diagnosis of cancer” or “complained that he could not live with the pain associated with a condition” even if the condition may not have been diagnosed or existed). Relationship problems refer to conflict with an intimate partner and/or other family members, arguments, other family stressors, caregiver burden, or abuse by a caregiver. Suicides or other deaths of family/friends were coded “Yes” if the decedent was distraught over or reacting to a suicide of a friend or family member or to an anniversary of the suicide. Criminal legal problems refer to conducts (including driving under the influence) with negative legal or law enforcement consequences (e.g., about to enter jail, facing a court date, on the run from law enforcement). Civil legal problems refer to a divorce, custody dispute, civil lawsuit, or legal problems.
Depressed mood at the time of injury: This refers to “sad, despondent, down, blue, low, and/or unhappy” mood without the need to have a clinical diagnosis or any indication that the depression directly contributed to the death.
Mental disorder, alcohol, and other substance use problems: In NVDRS, mental health and substance misuse problems were recorded “Yes” without the need for any indication that they directly contributed to the death and included the following: (1) any diagnosed mental health problem (disorders and syndromes listed in DSM-5 [American Psychiatric Association, 2013]) at the time of death; (2) alcohol problem/addiction; and (3) other substance misuse/addiction (e.g., prescription drug misuse, chronic/abusive/problematic marijuana use, any use of other illicit drugs or inhalants).
Number of crises refers to “current/acute event within two weeks of death” that the decedent faced with respect to physical health, and relationship, and other life stressors as well as mental health and substance misuse/addiction discussed above.
History of suicide attempt: This refers to any previous suicide attempt before the fatal incident, regardless of the severity and injury status. We included suicidal intent disclosure for descriptive purposes only, and it refers to: (a) disclosure of suicidal thoughts or intent to die by suicide to another person via verbal, written, or electronic communications within a month before suicide (i.e., not at the moment of the suicide), whether explicitly (e.g., “I plan to go to my cabin with my gun and never come back”) or indirectly (e.g., “I know how to put a permanent end to this pain”), or (b) a separate suicide attempt within a month of the suicide.
Suicide means: We provide data on suicide means for descriptive purposes only. Means were identified from the International Classification of Diseases, 10th Revision (ICD-10), codes for intentional self-harm (X60-X84) for underlying cause of death in death certificates and/or from the underlying cause descriptions in CME reports. They included the following: firearms; hanging/suffocation; poisoning due to any type of alcohol/drug/medicine/chemical overdose or with gas (e.g., carbon monoxide, nitrogen); laceration/sharp instruments; blunt objects; jumping from heights; contact with moving objects (train/other vehicles); drowning; and other (fire, hypothermia, electrocution, starvation, dehydration, not adhering to or refusing medical care, or undetermined causes). We classified them into four categories in this study: firearms, hanging/suffocation, poisoning, and all other means.
2.3. Analysis
First, we used cross-tabulations with Pearson's χ2 tests to describe the rates of JFH and other suicide precipitants and contributors by age group, separately for males and females. Second, again separately for males and females, we used cross-tabulations with Pearson's χ2 tests to compare demographic characteristics and other suicide precipitants and contributors between decedents who had JFH and decedents who did not, first for all age groups and second for the 45–64 age group. Third, to test study hypotheses (correlates of JFH), we fit four generalized linear models (GLMs) for a Poisson distribution with a log link for: (1) all males; (2) all females; (3) males aged 45–64; and (4) females aged 45–64. All statistical analyses were performed using Stata/MP 17. As a preliminary diagnostic, we used variance inflation factor (VIF), using a cut-off of 2.50 (Allison, 2012), from linear regression models to assess multicollinearity among covariates. VIF diagnostics indicated that multicollinearity was not a concern. GLM results are reported as incidence rate ratios (IRRs) with 95% confidence intervals (CIs). Significance was set at p < .05. Finally, to better understand the circumstances of deaths among those who had JFH, we reviewed a 5% (N = 350; 285 males and 65 females) random sample of CME/LE reports pertaining to decedents age 45–64 who had JFH. All 350 cases had CME and/or LE reports for review. (Among all 14,678 JFH cases, 2% were missing CME reports and nearly 14% were missing LE reports; however, no single case was missing both CME and LE reports.) Because direct quotes from CME/LE reports are not allowed in NVDRS, we compiled similar and dissimilar circumstances and developed composite case scenarios from similar circumstances.
3. Results
3.1. Percentages with JFH and other suicide precipitants and contributors
Table 1 shows that in both male and female decedents, JFH as a suicide precipitant was highest in the 45–64 age group (22.0% for males and 15.1% for females), followed by the 25–44, 18–24, and 65+ age groups. In males with JFH, job problems were most common, followed by financial problems, in the under-65 age group, whereas financial problems were most common, followed by housing problems, in the 65+ age group. In females with JFH, job problems were most common in the 18–24 and 25–44 age groups, whereas financial problems were most common in the 45–64 and 65+ age groups. Additional analyses showed that in both sexes, a significant proportion of those who had job problems also had financial and housing problems (refer to Table 1 footnotes).
Table 1.
Suicide precipitating/contributing factors among adult decedents, 2017–2019, by sex and age group (%).
| N(%) | Male |
||||
|---|---|---|---|---|---|
| All N = 74,042 (100%) |
18–24 N = 8388 (11.3%) |
25–44 N = 25,158 (34.0%) |
45–64 N = 25,640 (34.6%) |
65+ N = 14,856 (20.1%) |
|
| Job/financial/housing problem | 16.2 | 11.6 | 16.3 | 22.0 | 8.8 |
| Problem type (among those who had the problem) | |||||
| Job problema | 57.1 | 67.4 | 64.1 | 57.6 | 25.9 |
| Financial problem | 49.9 | 37.1 | 45.0 | 52.6 | 62.7 |
| Eviction/loss of home | 20.5 | 16.2 | 18.0 | 20.7 | 31.2 |
| Physical health problem | 19.8 | 3.1 | 6.6 | 20.2 | 50.7 |
| Relationship problem | 32.3 | 38.5 | 42.8 | 30.7 | 14.0 |
| Criminal/civil legal problem | 10.9 | 9.5 | 14.9 | 11.5 | 3.7 |
| Death/suicide of family/friend | 7.6 | 6.3 | 6.3 | 7.9 | 10.0 |
| Depressive mood | 30.5 | 29.4 | 28.6 | 31.8 | 32.2 |
| Mental disorder | 39.9 | 39.9 | 41.9 | 42.1 | 32.7 |
| Alcohol problem/addiction | 17.9 | 11.2 | 20.8 | 22.7 | 8.7 |
| Other substance use problem | 15.4 | 19.2 | 23.9 | 13.2 | 2.8 |
| Female | |||||
| All N = 20,412 (100%) |
18–24 N = 1859 (9.1%) |
25–44 N = 6924 (33.9%) |
45–64 N = 8568 (42.0%) |
65+ N = 3061 (15.0%) |
|
| Job/financial/housing problem | 13.0 | 8.9 | 13.4 | 15.1 | 8.6 |
| Problem type (among those who had the problem) | |||||
| Job problemb | 45.9 | 47.6 | 54.4 | 45.5 | 16.8 |
| Financial problem | 52.3 | 43.4 | 48.2 | 54.2 | 63.4 |
| Eviction/loss of home | 25.9 | 28.3 | 21.2 | 26.6 | 37.4 |
| Physical health problem | 19.4 | 4.8 | 10.4 | 22.1 | 41.0 |
| Relationship problem | 32.3 | 42.6 | 42.9 | 28.2 | 13.5 |
| Criminal/civil legal problem | 6.2 | 5.2 | 9.4 | 5.4 | 1.7 |
| Death/suicide of family/friend | 9.8 | 7.5 | 7.9 | 10.7 | 12.9 |
| Depressive mood | 31.7 | 31.6 | 30.2 | 32.7 | 32.6 |
| Mental disorder | 59.8 | 55.4 | 59.8 | 63.2 | 53.0 |
| Alcohol problem/addiction | 15.4 | 9.6 | 18.3 | 17.5 | 6.6 |
| Other substance use problem | 17.9 | 18.9 | 26.1 | 15.0 | 5.5 |
Note: All age group differences were significant at p < .01 (calculated with Pearson's χ2 tests).
Of male decedents with job problems, 32.2% also had financial problems, and 8.3% had housing problems.
Of female decedents with job problems, 28.8% also had financial problems, and 9.5% had housing problems.
Of other suicide precipitants, in both sexes, relationship problems were the most common in the under-65 age groups, but physical health problems were the most common suicide precipitant in the 65+ age group. Table 1 also shows that 39.9% of males and 59.8% of females in all age groups had mental disorders; 17.9% of males and 15.4% of females had alcohol problems; and 15.4% of males and 17.9% of females had other substance use problems.
3.1.1. Demographic and clinical characteristics of all adult suicide decedents with and without JFH
Table 2 shows that compared to those without JFH, both male and female decedents with JFH included higher proportions of non-Hispanic Whites, those with a college degree, and those in the Midwest and West. Male decedents with JFH included higher proportions of those who were married or divorced/separated, and female decedents with JFH included a higher proportion of those who were divorced/separated. In both sexes, decedents with JFH also included higher proportions of those had relationship and legal problems, suicide/death of family/friend, mental disorders, and alcohol/other substance use problems, and disclosed suicidal intent. Male decedents with JFH also included a higher proportion of those who previously attempted suicide attempt. Of suicide means, 53.1% of males with JFH died by firearms and 31.9% by hanging/suffocation; and 32.5% of females with JFH died by firearms, 31.3% by hanging/suffocation, and 28.7%% by poisoning.
Table 2.
Demographic and clinical characteristics of all suicide decedents by job/financial/housing problem (JFH) status.
| N (%) | Male |
Female |
||||
|---|---|---|---|---|---|---|
| No JFH 62,015 (83.8) |
Yes JFH 12,027 (16.2) |
p | No JFH 17,767 (87.0) |
Yes JFH 2651 (13.0) |
p | |
| Age group (%) | <.001 | <.001 | ||||
| 18-24 | 12.0 | 8.1 | 9.5 | 6.3 | ||
| 25-44 | 33.9 | 34.2 | 33.8 | 34.8 | ||
| 45-64 | 32.3 | 46.8 | 40.9 | 49.0 | ||
| 65+ | 21.8 | 10.9 | 15.8 | 9.9 | ||
| Race/ethnicity (%) | <.001 | .106 | ||||
| Non-Hispanic White | 80.3 | 84.1 | 80.9 | 82.7 | ||
| Black/African American | 6.7 | 5.2 | 6.0 | 5.8 | ||
| Hispanic | 8.0 | 6.3 | 6.7 | 5.7 | ||
| Asian/Pacific Islander | 2.5 | 2.7 | 3.8 | 3.7 | ||
| Other | 2.5 | 1.7 | 2.6 | 2.1 | ||
| Education (%) | <.001 | <.001 | ||||
| =< High school | 57.4 | 50.9 | 45.1 | 39.3 | ||
| Some college/associate degree | 23.4 | 24.5 | 29.5 | 29.7 | ||
| Bachelor's degree or higher | 16.9 | 22.3 | 23.2 | 28.9 | ||
| Unknown | 2.3 | 2.3 | 2.2 | 2.1 | ||
| Marital status (%) | <.001 | <.001 | ||||
| Married | 31.0 | 33.1 | 31.6 | 27.9 | ||
| Divorced/separated | 22.6 | 26.9 | 28.4 | 36.4 | ||
| Widowed | 5.8 | 2.6 | 8.0 | 5.8 | ||
| Never married | 39.5 | 36.3 | 31.0 | 29.2 | ||
| Missing | 1.1 | 1.1 | 1.0 | 0.7 | ||
| Military service (%) | 20.8 | 15.9 | <.001 | 2.9 | 3.1 | .421 |
| Region of residence | <.001 | <.001 | ||||
| Northeast | 16.6 | 14.9 | 17.8 | 15.2 | ||
| Midwest | 27.9 | 30.5 | 25.7 | 27.6 | ||
| South | 28.0 | 23.5 | 28.2 | 23.0 | ||
| West | 26.2 | 30.4 | 27.5 | 33.8 | ||
| Puerto Rico & territories | 1.2 | 0.8 | 0.8 | 0.4 | ||
| Other suicide precipitating factors (%) | ||||||
| Physical health problema | 20.0 | 18.4 | .002 | 19.3 | 20.4 | .147 |
| Relationship problemb | 30.1 | 43.8 | <.001 | 30.3 | 45.8 | <.001 |
| Criminal or civil legal problem | 9.9 | 15.8 | <.001 | 5.1 | 13.2 | <.001 |
| Suicide/death of family/friend or traumatic anniversary | 7.1 | 10.0 | <.001 | 9.3 | 12.7 | <.001 |
| Depressed mood at the time of injury (%) | 26.9 | 49.3 | <.001 | 29.1 | 49.1 | <.001 |
| Any recent mental health disorderc (%) | 38.7 | 46.0 | <.001 | 59.0 | 65.6 | <.001 |
| Types of disorder (among all decedents) (%) | ||||||
| Depressive disorder/dysthymia | 28.0 | 36.5 | <.001 | 45.0 | 53.3 | <.001 |
| Bipolar disorder | 5.3 | 5.8 | .012 | 11.8 | 11.2 | .426 |
| Anxiety disorder | 6.9 | 10.5 | <.001 | 14.3 | 19.5 | <.001 |
| Post-traumatic stress disorder | 2.5 | 2.1 | .008 | 2.5 | 3.1 | .068 |
| Schizophrenia | 2.8 | 1.6 | <.001 | 3.1 | 1.7 | <.001 |
| Alcohol problem/addiction (%) | 16.2 | 26.6 | <.001 | 14.5 | 22.0 | <.001 |
| Other substance use problemd (%) | 14.8 | 18.4 | <.001 | 17.4 | 21.2 | <.001 |
| Number of crisese, M (SD) | 0.29 (0.56) | 0.65 (0.91) | <.001 | 0.24 (0.52) | 0.67 (0.93) | <.001 |
| History of suicide attempt (%) | 14.3 | 16.1 | <.001 | 30.2 | 32.0 | .054 |
| Disclosed suicidal intent within last month (%) | 20.8 | 24.6 | 21.2 | 26.4 | <.001 | |
| Suicide means | <.001 | <.001 | ||||
| Firearms | 55.0 | 53.1 | 29.6 | 32.5 | ||
| Hanging/suffocation | 27.8 | 31.9 | 28.1 | 31.3 | ||
| Poisoning | 9.0 | 8.7 | 32.6 | 28.7 | ||
| Other | 8.2 | 6.3 | 9.7 | 7.5 | ||
Note: P-values are calculated based on Pearson's χb tests for all categorical variables and t-tests for the number of crises (t = −57.75 for male and t = −34.35 for female).
Including any terminal/other illness, debilitating condition, chronic/acute pain, or other physical/functional issue (perceived, or diagnosed) that were relevant to suicide.
Problems with intimate partner and/or other family/relatives, other family stressors, caregiver burden, arguments, or abuse by a caregiver.
Including those disorders and syndromes listed in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) with the exception of alcohol and other substance dependence.
Including illicit drug use, even if addiction or abuse is not specifically mentioned. The exception to this is marijuana use. For marijuana, the use must be noted as chronic, abusive, or problematic.
Total number of precipitating or contributing factors that posed a crisis within 2 weeks of death.
3.1.2. Demographic and clinical characteristics of suicide decedents aged 45–64 with and without JFH
Table 3 shows that demographic differences between decedents in the 45–64 age group with and without JFH mirrored the differences shown when all adult decedents were compared. However, with respect to other suicide precipitating factors, a higher proportion of male decedents aged 45–64 with than without JFH had physical health problems. Also, both male and female decedents in this age group with JFH did not differ on their suicide attempt history from their counterparts who did not have JFH. The overall rates of poisoning use as suicide means among female decedents in this age group (33.3% with JFH and 37.7% without JFH) were higher than the rates among all female decedents.
Table 3.
Demographic and clinical characteristics of suicide decedents aged 45–64 by job/financial/housing problem (JFH) status.
| N (%) | Male |
Female |
||||
|---|---|---|---|---|---|---|
| No JFH 20,007 (78.0) |
Yes JFH 5633 (22.0) |
p | No JFH 7270 (84.9) |
Yes JFH 1298 (15.1) |
p | |
| Race/ethnicity (%) | <.001 | .460 | ||||
| Non-Hispanic White | 85.7 | 89.4 | 86.5 | 87.7 | ||
| Black/African American | 4.7 | 3.0 | 4.2 | 3.6 | ||
| Hispanic | 6.1 | 4.3 | 4.9 | 4.0 | ||
| Asian/Pacific Islander | 1.9 | 2.3 | 2.8 | 3.2 | ||
| Other | 1.6 | 1.0 | 1.6 | 1.5 | ||
| Education (%) | <.001 | .005 | ||||
| =< High school | 55.3 | 48.0 | 43.9 | 39.6 | ||
| Some college/associate degree | 21.9 | 23.1 | 28.0 | 28.2 | ||
| Bachelor's degree or higher | 20.0 | 26.2 | 25.6 | 29.9 | ||
| Unknown | 2.8 | 2.7 | 2.5 | 2.3 | ||
| Marital status (%) | <.001 | <.001 | ||||
| Married | 38.0 | 39.7 | 39.4 | 31.8 | ||
| Divorced/separated | 34.9 | 35.3 | 37.5 | 44.0 | ||
| Widowed | 3.4 | 2.2 | 6.8 | 6.2 | ||
| Never married | 22.2 | 21.3 | 15.1 | 17.3 | ||
| Missing | 1.5 | 1.5 | 1.1 | 0.7 | ||
| Military service (%) | 16.2 | 14.8 | .010 | 2.7 | 2.4 | .637 |
| Region of residence | <.001 | <.001 | ||||
| Northeast | 19.0 | 17.6 | 18.8 | 16.1 | ||
| Midwest | 27.9 | 30.5 | 25.7 | 26.9 | ||
| South | 27.5 | 22.6 | 29.1 | 24.2 | ||
| West | 24.2 | 28.5 | 25.6 | 32.6 | ||
| Puerto Rico & territories | 1.4 | 0.8 | 0.8 | 0.2 | ||
| Other suicide precipitating factors (%) | ||||||
| Physical health problem | 19.7 | 22.1 | <.001 | 21.8 | 24.0 | .088 |
| Relationship problem | 28.6 | 38.2 | <.001 | 26.2 | 39.1 | <.001 |
| Criminal or civil legal problem | 10.5 | 15.1 | <.001 | 4.4 | 11.1 | <.001 |
| Suicide/death of family/friend or traumatic anniversary | 7.3 | 10.0 | <.001 | 10.3 | 12.7 | .011 |
| Depressed mood at the time of injury (%) | 26.6 | 50.0 | <.001 | 29.7 | 49.4 | <.001 |
| Any recent mental health disorder (%) | 41.0 | 46.3 | <.001 | 62.6 | 66.9 | .003 |
| Types of disorder (among all decedents) (%) | ||||||
| Depressive disorder/dysthymia | 30.6 | 38.2 | <.001 | 48.5 | 55.5 | <.001 |
| Bipolar disorder | 5.5 | 5.3 | .485 | 12.6 | 10.3 | .017 |
| Anxiety disorder | 7.9 | 10.9 | <.001 | 15.2 | 19.0 | <.001 |
| Post-traumatic stress disorder | 2.0 | 1.4 | .002 | 2.4 | 2.7 | .593 |
| Schizophrenia | 2.6 | 1.2 | <.001 | 3.4 | 1.6 | .001 |
| Alcohol problem/addiction (%) | 21.1 | 28.3 | <.001 | 16.7 | 22.3 | <.001 |
| Other substance use problem (%) | 13.1 | 13.5 | .436 | 15.4 | 16.3 | .405 |
| Number of crises, M (SD) | 0.27 (0.56) | 0.65 (0.92) | <.001 | 0.22 (0.50) | 0.62 (0.90) | <.001 |
| History of suicide attempt (%) | 14.4 | 14.5 | .798 | 30.7 | 30.0 | .624 |
| Disclosed suicidal intent within last month (%) | 19.4 | 22.5 | <.001 | 19.2 | 24.4 | <.001 |
| Suicide means | <.001 | <.001 | ||||
| Firearms | 52.4 | 52.9 | 30.5 | 33.4 | ||
| Hanging/suffocation | 26.6 | 29.9 | 22.1 | 25.6 | ||
| Poisoning | 12.0 | 10.7 | 37.7 | 33.3 | ||
| Other | 9.0 | 6.5 | 9.7 | 7.7 | ||
Note: P-values are calculated based on Pearson's χ2 tests for all categorical variables and t-tests for the number of crises (t = −37.78 for male and t = −23.14 for female).
3.2. Correlates of JFH in all age groups: Results from multivariable models
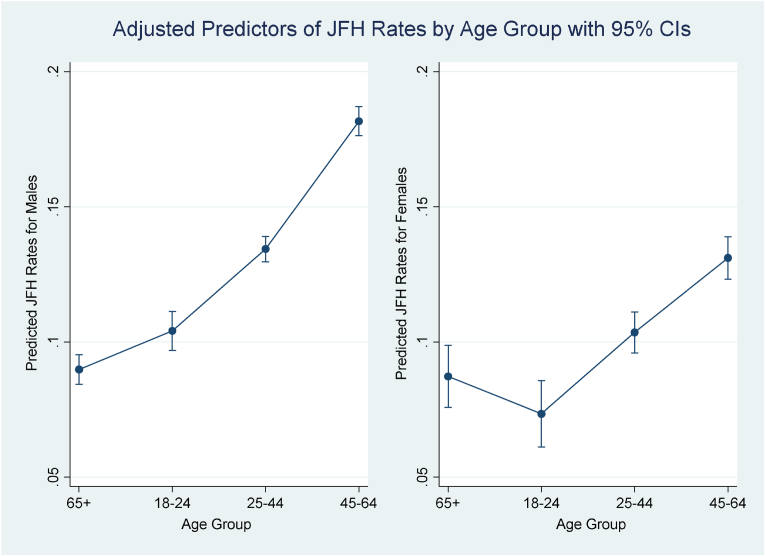
The first and second columns in Table 4 shows that in both sexes, JFH risks were higher in the 25–44 (IRR = 1.50, 95% CI = 1.39–1.61 for males; IRR = 1.19, 95% CI = 1.01–1.39 for females) and 45–64 (IRR = 2.02, 95% CI = 1.89–2.16 for males; IRR = 1.50, 95% CI = 1.30–1.73 for females) age groups, compared to the 65+ age group. See Fig. 1 for age group differences in the predicted mean JFH rates adjusted by other suicide precipitants, contributors, and demographic factors.
Table 4.
Correlates of job/financial/housing problems as a suicide precipitant by sex: Results from generalized linear modeling.
| All decedents |
Decedents aged 45-64 |
|||
|---|---|---|---|---|
| Male |
Female |
Male |
Female |
|
| IRR (95% CI) | IRR (95% CI) | IRR (95% CI) | IRR (95% CI) | |
| Age group: vs. 65+ | ||||
| 18-24 | 1.16 (1.05–1.28)** | 0.84 (0.67–1.05) | ||
| 25-44 | 1.50 (1.39–1.61)*** | 1.19 (1.01–1.39)* | ||
| 45-64 | 2.02 (1.89–2.16)*** | 1.50 (1.30–1.73)*** | ||
| Physical health problem | 0.93 (0.89–0.98)** | 1.01 (0.91–1.11) | 0.98 (0.91–1.04) | 1.03 (0.90–1.17) |
| Relationship problem | 1.14 (1.10–1.19)*** | 1.25 (1.14–1.36)*** | 1.05 (0.99–1.11) | 1.19 (1.05–1.35)** |
| Criminal or civil legal problem | 0.99 (0.94–1.05) | 1.34 (1.18–1.51)*** | 0.96 (0.89–1.04) | 1.27 (1.06–1.54)* |
| Suicide/death of family/friend or traumatic anniversary | 1.09 (1.03–1.16)** | 1.05 (0.93–1.18) | 1.04 ((0.95–1.14) | 0.92 (0.77–1.09) |
| Depressed mood at the time of injury | 1.96 (1.89–2.03)*** | 1.76 (1.63–1.91)*** | 1.95 (1.85–2.06)*** | 1.78 (1.59–1.99)*** |
| Any recent mental health disorder | 1.06 (1.02–1.10)** | 1.11 (1.02–1.21)* | 1.03 (0.98–1.09) | 1.07 (0.95–1.21) |
| Alcohol problem/addiction | 1.20 (1.15–1.25)*** | 1.14 (1.03–1.25)* | 1.14 (1.07–1.21)*** | 1.11 (0.96–1.27) |
| Other substance use problem | 1.05 (1.00–1.10)ǂ | 1.01 (0.92–1.12) | 0.96 (0.89–1.04) | 0.90 (0.77–1.05) |
| Number of crises | 1.46 (1.43–1.49)*** | 1.55 (1.48–1.61)*** | 1.48 (1.43–1.53)*** | 1.58 (1.48–1.68)*** |
| History of suicide attempt | 0.94 (0.89–0.99)* | 0.93 (0.85–1.01) | 0.91 (0.85–0.99)* | 0.88 (0.77–0.99)* |
| Race/ethnicity: vs. Non-Hispanic White | ||||
| Black/African American | 0.94 (0.86–1.02) | 1.17 (0.99–1.38) | 0.81 (0.70–0.95)** | 1.02 (0.76–1.37) |
| Hispanic | 0.81 (0.75–0.88)*** | 0.88 (0.74–1.04) | 0.79 (0.68–0.90)** | 0.87 (0.65–1.15) |
| Asian/Pacific Islander | 1.10 (0.98–1.22) | 1.11 (0.90–1.36) | 1.14 (0.96–1.36) | 1.22 (0.90–1.67) |
| Other | 0.72 (0.62–0.82)*** | 0.81 (0.62–1.06) | 0.65 (0.49–0.85)** | 0.98 (0.63–1.53) |
| Education: vs. =< High school | ||||
| Some college/associate degree | 1.10 (1.06–1.15)*** | 1.09 (0.99–1.20) | 1.12 (1.04–1.19)** | 1.05 (0.92–1.20) |
| Bachelor's degree or higher | 1.32 (1.26–1.39)*** | 1.29 (1.17–1.42)*** | 1.29 (1.21–1.38)*** | 1.17 (1.02–1.34)* |
| Unknown | 1.13 (0.99–1.28) | 1.15 (0.87–1.52) | 1.12 (0.94–1.34) | 1.02 (0.69–1.49) |
| Marital status: vs. Married | ||||
| Divorced/separated | 1.02 (0.97–1.07) | 1.31 (1.19–1.45)*** | 1.00 (0.94–1.06) | 1.42 (1.25–1.61)*** |
| Widowed | 0.65 (0.58–0.74)*** | 1.02 (0.85–1.23) | 0.69 (0.57–0.83)*** | 1.22 (0.95–1.56) |
| Never married | 1.02 (0.97–1.07) | 1.25 (1.12–1.40)*** | 1.05 (0.98–1.13) | 1.51 (1.28–1.78)*** |
| Missing | 1.16 (0.96–1.39) | 0.93 (0.58–1.51) | 1.21 (0.95–1.54) | 0.87 (0.44–1.73) |
| Military service (%) | 0.90 (0.85–0.94)** | 0.94 (0.76–1.18) | 0.92 (0.86–0.99)* | 0.83 (0.58–1.18) |
| Region of residence: vs. Northeast | ||||
| Midwest | 1.14 (1.08–1.21)*** | 1.15 (1.02–1.30)* | 1.10 (1.02–1.19)* | 1.15 (0.97–1.37) |
| South | 1.00 (0.94–1.06) | 0.97 (0.85–1.10) | 0.94 (0.87–1.02) | 1.02 (0.85–1.21) |
| West | 1.17 (1.11–1.24)*** | 1.22 (1.08–1.38)** | 1.10 (1.01–1.19)* | 1.27 (1.08–1.51)** |
| Puerto Rico & territories | 0.90 (0.72–1.12) | 0.58 (0.30–1.14) | 0.78 (0.57–1.08) | 0.40 (0.13–1.29) |
| N | 74,042 | 20,412 | 25,640 | 8568 |
ǂp = 0.05; *p < .05; **p < .01; ***p < .001.
Fig. 1.
Age group differences in the predicted JFH rates adjusted by other suicide precipitants, contributors, and demographic factors.
In both sexes, JFH was positively associated with relationship problems (IRR = 1.14, 95% CI = 1.10–1.19 for males; IRR = 1.25, 95% CI = 1.14–1.36 for females), depressed mood, mental disorder, alcohol problems (IRR = 1.20, 95% CI = 1.15–1.25 for males; IRR = 1.14, 95% CI = 1.03–1.25 for females), and the number of crises (IRR = 1.46, 95% CI = 1.43–1.49 for males; IRR = 1.55, 95% CI = 1.48–1.61 for females). In males, JFH was also positively associated with suicide/death of family/friend (IRR = 1.09, 95% CI = 1.03–1.16), but negatively associated with physical health problems and suicide attempt history. JFH was marginally significantly associated with other substance use problems in all age groups of males. In females, JFH was positively associated with legal problems (IRR = 1.34, 95% CI = 1.18–1.51). These findings partially support H1.
The third and fourth columns of Table 4 show that in both male and female decedents age 45–64, JFH was positively associated with depressed mood (IRR = 1.95, 95% CI = 1.85–2.06 for males; IRR = 1.78, 95% CI = 1.59–1.99 for females) and the number of crises (IRR = 1.48, 95% CI = 1.43–1.53 for males; IRR = 1.58, 95% CI = 1.48–1.68 for females), but negatively associated with history of suicide attempt. In males age 45–64, JFH was also positively associated with alcohol problems (IRR = 1.14, 95% CI = 1.07–1.21). In females age 45–64, JFH was also positively associated with relationship (IRR = 1.19, 95% CI = 1.05–1.35) and legal (IRR = 1.27, 95% CI = 1.06–1.54) problems. These findings partially support H2.
Among demographic factors pertaining to males of all age groups, JFH risks were lower in Hispanics and those of “Other” racial/ethnic groups than in non-Hispanic Whites, widowed than married individuals, and those with than without military service. Among females of all age groups, JFH risks were higher in divorced/separated or never married than married decedents. In both sexes, JFH risk were higher for those with college education compared to those with high school or less education and in the Midwest and West regions compared to the Northeast region. Among the 45–64 age group, JFH risks were higher among those with college education and in the Midwest region in both sexes. JFH risks were lower in Blacks, Hispanics, and/or “other” racial/ethnic groups only among males, whereas they were higher among divorced/separated or never-married women.
3.3. Circumstances of JFH-precipitated deaths in the 45–64 age group: CME/LE report narratives
CME/LE reports for males and females aged 45–64 with JFH showed that while some decedents had job-related stress and/or conflict at work, a large proportion appeared to be those who lost their job or were about to lose it. A majority of housing problems were related to going through foreclosure for nonpayment. The following cases show common circumstances of death:
Case 1
Had financial issues and a large amount of debt on his house since he was laid off from his job approximately 7–8 years ago and unable to find employment. He was having marital issues and felt he was a burden.
Case 2
Left a suicide note that stated that he loved his wife, but he had lost will to live as he lost his job, house, and dignity and asked her to take care of their children and that he was sorry. He had lost his job about two years ago and was having extreme financial difficulties, started drinking heavily, became depressed and reclusive, and had frequent arguments with his wife about drinking and money.
Case 3
Had suffered from pain and depression since his shoulder injury at work about a year ago. He and his wife had relationship problems and were also experiencing financial problems. He was concerned about losing his job over the shoulder injury. He had a prescription opioid misuse problem.
Case 4
Had been depressed since losing his job for showing up at work intoxicated four years prior and had accrued a large amount of debt since then. He was a daily drinker and had a restricted license due to DUI last year but he drove and got into an accident last night. He was afraid that he would go to jail this time. His relationship with wife and son was strained. There were numerous empty beer cans on the floor. The decedent left several suicide notes stating that he could no longer go on and how he was sorry for failing.
Case 5
Had a history of alcohol misuse and lost his job as a result a year before. His wife divorced him a few years ago, and his daughter did not allow him to see his grandchildren due to his alcohol problems. He had to be hospitalized for alcohol-poisoning last year but could not pay the hospital bills, his home was in foreclosure, and his car was repossessed for nonpayment. He left his foreclosure paper out to be found.
Case 6
Had been depressed since her son died by suicide a year ago and taking medications for her depression and sleeping pills. She had also lost her job, her unemployment insurance had run out, and she was about to be evicted from her apartment. Her daughter also claimed that the decedent had never gotten over her divorce. Toxicology was positive for ethanol.
Case 7
Had a history of depression. Was married but living with a daughter (no mention of whereabouts of spouse). She had sustained significant trauma and injuries in a car accident two years prior. She had to quit her job at a bank and was having financial problems. She felt sorry for her daughter for being a burden and recently made statements about wanting to go see the Lord.
4. Discussion
In this study, we examined adult suicide decedents who had JFH as a suicide precipitant. Consistent with previous study findings discussed earlier, we found that the rates of JFH were higher among middle-aged decedents, especially those aged 45–64, in both sexes. About one out of five male decedents and one out of six female decedents age 45–64 had JFH. This sex difference in JFH-precipitated suicides may reflect cultural expectations related to gender (Canetto, 2021; Canetto & Sakinofsky, 1998). Men, especially middle-aged men with family, have been expected to be the primary breadwinner, which may also explain the higher proportion of married individuals among male than female decedents with JFH.
CME/LE reports show that JFH was in large part due to a job loss and inability to reenter the labor force. Many had been out of work for some years, while others lost a job a short time before the fatal injury and still others were worried about an impending job loss. CME/LE reports also show that some experienced depression and started misusing alcohol and/or other substances following a job loss, but others had these problems preceding JFH, and that caused/contributed to JFH. Some also felt that they were a burden to their family, lending support for the interpersonal theory of suicide in which three main drivers of suicide are thwarted belongingness, perceived burdensomeness, and acquired capability (for lethal suicidal behaviors) (Joiner, 2005). Mental health or substance use treatment was rarely mentioned.
Multivariable models for all-age groups show that both male and female decedents with JFH had higher risks of having depressed mood, any mental disorder, and alcohol problems. In the 45–64 age group, both male and female decedents with JFH were almost twice likely to have had depressed mood, but they did not differ from those without JFH on mental disorders and JFH was associated with higher risk of alcohol misuse problems only in males. Alcohol problems, noted in 28.3% of males and 22.3% of females age 45–64 with JFH, could have serious negative effects on all aspects of life. Alcohol may also have led to impulsive suicidal acts in some decedents. Alcohol use itself is a strong suicide risk factor (Amiri & Behnezhad, 2020). The confluence of JFH and alcohol use problems no doubt set off or exacerbated other negative life events. It was not surprising that both male and female decedents with JFH were experiencing more crises (i.e., multiple life stressors) than those without JFH, given JFH's cascading negative effects on other life areas, including relationship and/or legal problems. These decedents likely perceived the weight of multiple negative life events to be too much to cope.
JFH were not associated with physical health problems in multivariable models for both sexes in the 45–64 age group, although descriptive analysis results show that a larger proportion of decedents in the 45–64 age group with than without JFH had physical health problems as a suicide precipitant. Previous studies showed that job loss and unemployment had deleterious effects on health and increased mortality (Gallo et al., 2006; Nie et al., 2020; Roelfs et al., 2011). The difference between these earlier study findings and our findings are likely due to the fact that our study included only suicide decedents and that physical health problems were noted only if they were a suicide precipitant. We could not examine actual extent of JFH's impact on physical health.
Similarities between sexes in terms of other suicide precipitating and contributing factors—relationship problems, depressed mood, mental disorder, alcohol problems—that were associated with JFH in all age groups are notable. Sex differences also existed in the associations between JFH and its correlates especially in the 45–64 age group. Relationship and legal problems were significant only in females, while, as mentioned, alcohol problems were significant only in males. The finding that divorced or never-married females were more likely to have had JFH suggests that single women had a tougher time when they also had JFH, but they did not have more alcohol or other substance use problems. Another notable finding was that in the 45–64 age group, Black and Hispanic males were less likely to have had JFH as a suicide precipitant than non-Hispanic White males, no such racial/ethnic differences were found in females. Suicide rates of Blacks and Hispanics in both sexes have always been lower those of Non-Hispanic Whites (Curtin & Hedegaard, 2019; Ramchand et al., 2021). The lower risk of JFH-precipitated suicides among middle-aged Black and Hispanic males may also be attributable to the fact that systemic oppression and cumulative effects from socioeconomic disadvantages throughout their lives led them to adjust to the misery and despair of adverse life events (Case & Deaton, 2020). More research is needed to examine why such racial/ethnic differences did not show among females.
Other significant findings are related to education and region of residence. In both sexes, especially in the 45–64 age group, those with a college degree, compared to those with high school or less education, were more likely to have had JFH. Research shows that education has substantial impacts on such labor market outcomes as employment and earnings and significantly increases re-employment rates of the unemployed (Card, 2011; Riddell & Song, 2011). Other studies that we discussed earlier (e.g., Case & Deaton, 2020) also showed more negative impact of labor market conditions on those with lower education. Our findings may simply reflect the fact that White males who tended to have higher education than their Black and Hispanic counterparts comprised a larger share of suicide decedents with than without JFH. It is also possible that those with college education had more to lose when they lost their job and were more selective in their search of the next job. Older people in general and those with psychosocial and physical health problems in particular, also face multiple barriers, including age discrimination, to remaining in the workforce and rejoining once they are separated from it (Ayalon et al., 2021; Derous & Decoster, 2017). The finding that the risks of JFH-precipitated suicide were higher in the Midwest and West compared to the Northeast needs further research. Although overall suicide rates are higher in the Midwest and West than in the Northeast and South (Centers for Disease Cont,rol and Prevention, 2022), it is not clear whether JFH-precipitated suicide risks reflect the overall higher suicide rate or they were affected by other economic or other systemic factors.
Overall, the findings show the significance of stable employment, financial assistance, and housing subsidies for suicide prevention, along with treatment of depression and other mental disorders and alcohol/substance use problems. Economic stability undergirds physical and mental well-being. A study found strong associations between welfare state generosity (for unemployment insurance, sickness benefits, and pensions) and life expectancy for the US and 17 other high-income countries, showing that the US mortality disadvantage is, in part, a welfare-state disadvantage (Beckfield & Bambra, 2017). Another study found that the impact of unemployment rates on suicide is offset by the presence of generous state unemployment benefit programs (Cylus et al., 2014). Recent studies have also shown significant associations between increased state minimum wage and decreased suicide rates in recent years, with the largest effects observed at higher unemployment levels (Gertner et al., 2019; Kaufman et al., 2020). Researchers have called for targeted suicide prevention interventions for unemployed people and those who are in the process of losing their homes (Fowler et al., 2015; Haw et al., 2015). However, these interventions should be at both systemic (e.g., generous unemployment and health insurance, housing assistance, low interest loans for small businesses; increased availability and affordability of treatment for mental health and substance use problems) and individual (e.g., mental health and substance use treatment to help improve coping skills for alleviating family conflicts and better manage other negative life events) levels.
The study has a few limitations due to NVDRS data constraints, including the uncertain validity of suicide contributing/precipitating factors in NVDRS and limited generalizability of the findings to NVDRS non-participating states. JFH and other suicide precipitating and contributing factors in NVDRS were based on reports from decedents' family/friends and other informants and/or suicide notes and could not be independently verified. Although 43 states, District of Columbia, and Puerto Rico participated in the 2017–2019 NVDRS, some states did not provide data on all three observation years and others provided only partial data limited to some counties. Furthermore, we suspect that the actual number of suicides was likely higher even in the states that fully participated. Studies have shown that suicides by drug overdose could have been misclassified as “accidental” drug overdose deaths as drug overdose deaths escalated over the past decades (Rockett et al., 2018, 2022). According to Rockett et al. (2020), such misclassifications are more likely for racial/ethnic minorities, particularly non-Hispanic Blacks, and for women. Future studies also need to examine “deaths of undetermined intent.” Finally, although CME/LE report narratives in NVDRS contain qualitative data on the circumstances of death, they are excerpts from actual reports, and thus, may have omitted some details. We did not conduct detailed analysis of these reports as they were beyond the present study's scope. Future studies are needed for in-depth analysis of CME/LE reports.
In conclusion, this study shows that a significant proportion of suicides in mid-life is precipitated by job loss and unemployment, financial problems, and/or housing loss. Middle-aged White males who had college education had higher risks of having these problems and also had depression and alcohol use problems. The latter problems preceded or followed JFH. Compared to married women, divorced or never-married middle-aged women also had higher risks of these problems along with relationship and legal problems, but they did not have higher rates of alcohol use problems. The findings indicate that prevention of suicide among middle-aged people with JFH require interventions at both social policy and individual levels.
Ethical statement
This study based on deceased individuals was exempt from the authors' Institutional Review Board's review.
Author statements
Namkee Choi, Bryan Choi: Conceptualization; Namkee Choi, C. Nathan Marti: Data curation; Namkee Choi: Formal analysis; Namkee Choi: Funding acquisition; Namkee Choi, Bryan Choi: Investigation; Namkee Choi, C. Nathan Marti: Methodology; Namkee Choi, Bryan Choi: Original draft; Namkee Choi, Bryan Choi, C. Nathan Marti: Review & editing.
Funding
The authors received support from the University of Texas at Austin's internal research fund.
Declaration of competing interest
None for any author.
Acknowledgments
The Centers for Disease Control and Prevention (CDC) administers the National Violent Death Reporting System (NVDRS) in conjunction with participating NVDRS states. CDC provided the NVDRS Restricted Access Data used in this study to the authors. Study findings and conclusions are those of the authors alone and do not necessarily represent the official position of CDC or of the participating NVDRS states.
Data availability
The authors do not have permission to share data.
References
- Allison P. 2012. Statistical horizons. When can you safely ignore multicollinearity?http://statisticalhorizons.com/multicollinearity [Google Scholar]
- American Psychiatric Association Diagnostic and statistical manual of mental disorders. 2013. 5th ed. [DOI]
- Amiri S., Behnezhad S. Alcohol use and risk of suicide: A systematic review and meta-analysis. Journal of Addictive Diseases. 2020;38(2):200–213. doi: 10.1080/10550887.2020.1736757. [DOI] [PubMed] [Google Scholar]
- Anaf J., Baum F., Newman L., Ziersch A., Jolley G. The interplay between structure and agency in shaping the mental health consequences of job loss. BMC Public Health. 2013;13:110. doi: 10.1186/1471-2458-13-110. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ayalon L., Perel-Levin S., Georgantzi N., Lima C.M. Participation of older persons with mental health conditions and psychosocial disabilities in the labor market. American Journal of Geriatric Psychiatry. 2021;29(10):1033–1037. doi: 10.1016/j.jagp.2021.06.014. [DOI] [PubMed] [Google Scholar]
- Beckfield J., Bambra C. Shorter lives in stingier states: Social policy shortcomings help explain the US mortality disadvantage. Social Science & Medicine. 2016;171:30–38. doi: 10.1016/j.socscimed.2016.10.017. [DOI] [PubMed] [Google Scholar]
- Blakely T.A., Collings S.C., Atkinson J. Unemployment and suicide. Evidence for a causal association? Journal of Epidemiology & Community Health. 2003;57(8):594–600. doi: 10.1136/jech.57.8.594. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Brand J.E. The far-reaching impact of job loss and unemployment. Annual Review of Sociology. 2015;41:359–375. doi: 10.1146/annurev-soc-071913-043237. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Canetto S.S. Language, culture, gender, and intersectionalities in suicide theory, research, and prevention: Challenges and changes. Suicide and Life-Threatening Behavior. 2021;51(6):1045–1054. doi: 10.1111/sltb.12758. [DOI] [PubMed] [Google Scholar]
- Canetto S.S., Sakinofsky I. The gender paradox in suicide. Suicide and Life-Threatening Behavior. 1998;28(1):1–23. [PubMed] [Google Scholar]
- Card D. Estimating the return to schooling: Progress on some persistent econometric problems. Econometrica. 2001;69(5):1127–1160. [Google Scholar]
- Case A., Deaton A. Rising morbidity and mortality in midlife among white non-Hispanic Americans in the 21st century. Proceedings of the National Academy of Sciences of the United States of America. 2015;112(49):15078–15083. doi: 10.1073/pnas.1518393112. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Case A., Deaton A. Mortality and morbidity in the 21st century. Brookings Papers on Economic Activity. 2017:397–476. doi: 10.1353/eca.2017.0005. 2017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Case A., Deaton A. Princeton University Press; Princeton, NJ: 2020. Deaths of despair and the future of capitalism. [Google Scholar]
- Centers for Disease Control and Prevention . 2022. Suicide mortality by state.https://www.cdc.gov/nchs/pressroom/sosmap/suicide-mortality/suicide.htm [Google Scholar]
- Curtin S.C., Hedegaard H. 2019. Suicide rates for females and males by race and ethnicity: United States, 1999 and 2017. NCHS health E-stat.https://www.cdc.gov/nchs/data/hestat/suicide/rates_1999_2017.pdf [Google Scholar]
- Cylus J., Glymour M.M., Avendano M. Do generous unemployment benefit programs reduce suicide rates? A state fixed-effect analysis covering 1968-2008. American Journal of Epidemiology. 2014;180(1):45–52. doi: 10.1093/aje/kwu106. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Derous E., Decoster J. Implicit age cues in resumes: Subtle effects on hiring discrimination. Frontiers in Psychology. 2017;8:1321. doi: 10.3389/fpsyg.2017.01321. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Doiron D., Mendolia S. The impact of job loss on family dissolution. Journal of Population Economics. 2012;25:367–398. doi: 10.1007/s00148-010-0353-5. [DOI] [Google Scholar]
- Downing J. The health effects of the foreclosure crisis and unaffordable housing: A systematic review and explanation of evidence. Social Science & Medicine. 2016;162:88–96. doi: 10.1016/j.socscimed.2016.06.014. [DOI] [PubMed] [Google Scholar]
- Elbogen E.B., Lanier M., Montgomery A.E., Strickland S., Wagner H.R., Tsai J. Financial strain and suicide attempts in a nationally representative sample of US adults. American Journal of Epidemiology. 2020;189(11):1266–1274. doi: 10.1093/aje/kwaa146. [DOI] [PubMed] [Google Scholar]
- Fowler K.A., Gladden R.M., Vagi K.J., Barnes J., Frazier L. Increase in suicides associated with home eviction and foreclosure during the US housing crisis: Findings from 16 national violent death reporting system states, 2005-2010. American Journal of Public Health. 2015;105(2):311–316. doi: 10.2105/AJPH.2014.301945. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Frasquilho D., Matos M.G., Salonna F., Guerreiro D., Storti C.C., Gaspar T., Caldas-de-Almeida J.M. Mental health outcomes in times of economic recession: A systematic literature review. BMC Public Health. 2016;16:115. doi: 10.1186/s12889-016-2720-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gallo W.T., Teng H.M., Falba T.A., Kasl S.V., Krumholz H.M., Bradley E.H. The impact of late career job loss on myocardial infarction and stroke: A 10 year follow up using the health and retirement survey. Occupational and Environmental Medicine. 2006;63(10):683–687. doi: 10.1136/oem.2006.026823. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Garnett M.F., Curtin S.C., Stone D.M. Suicide mortality in the United States, 2000-2020. NCHS data brief. 2022;(433) [PubMed] [Google Scholar]
- Gertner A.K., Rotter J.S., Shafer P.R. Association between state minimum wages and suicide rates in the U.S. American Journal of Preventive Medicine. 2019;56(5):648–654. doi: 10.1016/j.amepre.2018.12.008. [DOI] [PubMed] [Google Scholar]
- Haw C., Hawton K., Gunnell D., Platt S. Economic recession and suicidal behaviour: Possible mechanisms and ameliorating factors. International Journal of Social Psychiatry. 2015;61(1):73–81. doi: 10.1177/0020764014536545. [DOI] [PubMed] [Google Scholar]
- Houle J.N., Light M.T. The harder they fall? Sex and race/ethnic specific suicide rates in the U.S. Foreclosure crisis. Social Science & Medicine. 2017;180:114–124. doi: 10.1016/j.socscimed.2017.03.033. [DOI] [PMC free article] [PubMed] [Google Scholar]
- İlgün G., Yetim B., Demirci Ş., Konca M. Individual and socio-demographic determinants of suicide: An examination on WHO countries. International Journal of Social Psychiatry. 2020;66(2):124–128. doi: 10.1177/0020764019888951. [DOI] [PubMed] [Google Scholar]
- Joiner T. Harvard University Press; Cambridge, MA, US: 2005. Why people die by suicide. [Google Scholar]
- Kaplan M.S., Huguet N., Caetano R., Giesbrecht N., Kerr W.C., McFarland B.H. Heavy alcohol use among suicide decedents relative to a nonsuicide comparison group: Gender-specific effects of economic contraction. Alcoholism: Clinical and Experimental Research. 2016;40(7):1501–1506. doi: 10.1111/acer.13100. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kaufman J.A., Salas-Hernández L.K., Komro K.A., Livingston M.D. Effects of increased minimum wages by unemployment rate on suicide in the USA. Journal of Epidemiology & Community Health. 2020;74(3):219–224. doi: 10.1136/jech-2019-212981. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kerr W.C., Kaplan M.S., Huguet N., Caetano R., Giesbrecht N., McFarland B.H. Economic recession, alcohol, and suicide rates: Comparative effects of poverty, foreclosure, and job loss. American Journal of Preventive Medicine. 2017;52(4):469–475. doi: 10.1016/j.amepre.2016.09.021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Milner A., Morrell S., LaMontagne A.D. Economically inactive, unemployed and employed suicides in Australia by age and sex over a 10-year period: What was the impact of the 2007 economic recession? International Journal of Epidemiology. 2014;43(5):1500–1507. doi: 10.1093/ije/dyu148. [DOI] [PubMed] [Google Scholar]
- Milner A., Page A., LaMontagne A.D. Long-term unemployment and suicide: A systematic review and meta-analysis. PLoS One. 2013;8(1) doi: 10.1371/journal.pone.0051333. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mulia N., Zemore S.E., Murphy R., Liu H., Catalano R. Economic loss and alcohol consumption and problems during the 2008 to 2009 U.S. recession. Alcoholism: Clinical and Experimental Research. 2014;38(4):1026–1034. doi: 10.1111/acer.12301. [DOI] [PMC free article] [PubMed] [Google Scholar]
- National Center for Injury Prevention and Control . 2021. National violent death reporting system data analysis guide. Mortality surveillance team, surveillance branch division of violence prevention. NVDRS document provided to the authors by the NVDRS Restrict Data Access Review Committee on April 2022. [Google Scholar]
- National Center for Injury Prevention and Control, Division of Violence Prevention Centers for Disease Control and Prevention . 2020. National violent death reporting system (NVDRS): Restricted access database (RAD) instructions for users. Updated October 2020. [Google Scholar]
- Nie J., Wang J., Aune D., Huang W., Xiao D., Wang Y., Chen X. Association between employment status and risk of all-cause and cause-specific mortality: A population-based prospective cohort study. Journal of Epidemiology & Community Health. 2020;74(5):428–436. doi: 10.1136/jech-2019-213179. [DOI] [PubMed] [Google Scholar]
- Pompili M., Innamorati M., Di Vittorio C., Baratta S., Masotti V., Badaracco A., Wong P., Lester D., Yip P., Girardi P., Amore M. Unemployment as a risk factor for completed suicide: A psychological autopsy study. Archives of Suicide Research. 2014;18(2):181–192. doi: 10.1080/13811118.2013.803449. [DOI] [PubMed] [Google Scholar]
- Ramchand R., Gordon J.A., Pearson J.L. Trends in suicide rates by race and ethnicity in the United States. JAMA Network Open. 2021;4(5) doi: 10.1001/jamanetworkopen.2021.11563. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Riddell W.C., Song X. The impact of education on unemployment incidence and re-employment success: Evidence from the U.S. Labour market. Labour Economics. 2011;18(4):453–463. doi: 10.1016/j.labeco.2011.01.003. [DOI] [Google Scholar]
- Rockett I., Caine E.D., Connery H.S., D'Onofrio G., Gunnell D.J., Miller T.R., Nolte K.B., Kaplan M.S., Kapusta N.D., Lilly C.L., Nelson L.S., Putnam S.L., Stack S., Värnik P., Webster L.R., Jia H. Discerning suicide in drug intoxication deaths: Paucity and primacy of suicide notes and psychiatric history. PLoS One. 2018;13(1) doi: 10.1371/journal.pone.0190200. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rockett I., Caine E.D., Connery H.S., Nolte K.B., Nestadt P.S., Nelson L.S., Jia H. Unrecognised self-injury mortality (SIM) trends among racial/ethnic minorities and women in the USA. Injury Prevention : Journal of the International Society for Child and Adolescent Injury Prevention. 2020;26(5):439–447. doi: 10.1136/injuryprev-2019-043371. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rockett I., Jia H., Ali B., Banerjee A., Connery H.S., Nolte K.B., Miller T., White F., DiGregorio B.D., Larkin G.L., Stack S., Kõlves K., McHugh R.K., Lulla V.O., Cossman J., De Leo D., Hendricks B., Nestadt P.S., Berry J.H., D'Onofrio G.…Caine E.D. Association of state social and environmental factors with rates of self-injury mortality and suicide in the United States. JAMA Network Open. 2022;5(2) doi: 10.1001/jamanetworkopen.2021.46591. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Roelfs D.J., Shor E., Davidson K.W., Schwartz J.E. Losing life and livelihood: A systematic review and meta-analysis of unemployment and all-cause mortality. Social Science & Medicine. 2011;72(6):840–854. doi: 10.1016/j.socscimed.2011.01.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Stack S. Contributing factors to suicide: Political, social, cultural and economic. Preventive Medicine. 2021;152(Pt 1) doi: 10.1016/j.ypmed.2021.106498. [DOI] [PubMed] [Google Scholar]
- Tsai A.C. Home foreclosure, health, and mental health: A systematic review of individual, aggregate, and contextual associations. PLoS One. 2015;10(4) doi: 10.1371/journal.pone.0123182. [DOI] [PMC free article] [PubMed] [Google Scholar]
- U.S. Bureau of Labor Statistics. (n.d.). Civilian unemployment rate. https://www.bls.gov/charts/employment-situation/civilian-unemployment-rate.htm.
- Wanberg C.R., Kanfer R., Hamann D.J., Zhang Z. Age and reemployment success after job loss: An integrative model and meta-analysis. Psychological Bulletin. 2016;142(4):400–426. doi: 10.1037/bul0000019. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The authors do not have permission to share data.