Abstract
Background
In a considerable subgroup of glioma patients treated with (chemo) radiation new lesions develop either representing tumor progression (TP) or treatment-related abnormalities (TRA). Quantitative diffusion imaging metrics such as the Apparent Diffusion Coefficient (ADC) and Fractional Anisotropy (FA) have been reported as potential metrics to noninvasively differentiate between these two phenomena. Variability in performance scores of these metrics and absence of a critical overview of the literature contribute to the lack of clinical implementation. This meta-analysis therefore critically reviewed the literature and meta-analyzed the performance scores.
Methods
Systematic searching was carried out in PubMed, EMBASE and The Cochrane Library. Using predefined criteria, papers were reviewed. Diagnostic accuracy values of suitable papers were meta-analyzed quantitatively.
Results
Of 1252 identified papers, 10 ADC papers, totaling 414 patients, and 4 FA papers, with 154 patients were eligible for meta-analysis. Mean ADC values of the patients in the TP/TRA groups were 1.13 × 10−3mm2/s (95% CI 0.912 × 10–3–1.32 × 10−3mm2/s) and 1.38 × 10−3mm2/s (95% CI 1.33 × 10–3–1.45 × 10−3mm2/s, respectively. Mean FA values of TP/TRA was 0.19 (95% CI 0.189–0.194) and 0.14 (95% CI 0.137–0.143) respectively. A significant mean difference between ADC and FA values in TP versus TRA was observed (p = 0.005).
Conclusions
Quantitative ADC and FA values could be useful for distinguishing TP from TRA on a meta-level. Further studies using serial imaging of individual patients are warranted to determine the role of diffusion imaging in glioma patients.
Keywords: Apparent diffusion coefficient, Fractional anisotropy, Glioblastoma, Tumor progression, Treatment-related abnormalities
Key points
ADC and FA values can differentiate between TP versus TRA.
ADC is reduced in TP due to reduced extracellular water diffusion
FA is hypothesized to be reduced in TRA due to necrosis
Lack of reporting according to FAIR principles lead to excluded papers
Background
In approximately 40% of high-grade glioma patients (WHO 3 + 4), the combination of chemotherapy and radiation provokes increased contrast agent uptake and apparent enlargement of residual tumor, or the appearance of new lesions mimicking glioma progression, which can also occur as radiation-induced injury in the treatment of low-grade glioma [1–3]. These phenomenon are called Treatment-Related Abnormalities (TRA), its pathophysiology is not known entirely, but it is likely to relate to endothelial cell injury as a consequence of treatment, leading to tissue inflammation and increased edema due to upregulation of VEGF. TRA are described in the literature as pseudoprogression and radio necrosis. It is a benign occurrence which regresses without additional treatment and is related to better outcomes [2]. On conventional magnetic resonance imaging (MRI), transient increases in post-contrast ring-enhancing lesions and increases in surrounding T2/FLAIR hyperintense regions similar to true tumor progression (TP) can be observed [4]. Although conventional MRI can serve to detect changes in the imaging follow-up of glioma, it is not sufficient by itself to distinguish TRA from TP. Therefore, this has become one of the major challenges in the radiological follow-up of glioma patients as only tissue biopsy or serial imaging can provide a conclusive diagnosis [5]. As conventional MRI protocols provide insufficient diagnostic accuracy to distinguish TRA from TP more sophisticated imaging protocols have been suggested. Such imaging protocols include the use of diffusion-weighted imaging (DWI), perfusion-weighted imaging (PWI) and diffusion tensor imaging (DTI). One of the DWI metrics concerns the apparent diffusion coefficient (ADC) of tissue [6]. Processes which degrade cellular integrity (e.g., necrosis) result in increased free water in the extracellular space, increasing ADC value, whereas increased cellularity with tumors reduces extracellular water, and is associated with a lower ADC value [7]. In the clinical setting the ADC value was found to be suitable to assess glioma response to therapy and to predict survival serially, with the same scanner and protocol [8]. In contrast, the DTI metric fractional anisotropy (FA) increases when water is more restricted in its diffusion directions [9]. A higher FA value indicates increased cellularity and reduced isotropy and has been shown to be able to assess glioma infiltration as well [10]. Additionally, various reports have been published with regard to the use of the ADC and/or FA values to distinguish TRA from TP [11, 12]. However, these studies reported different sensitivity/specificity-rates, positive predictive values and threshold-ratios and a clear overview of quantitative ADC or FA measures on a meta-level remains elusive. The present study reviews the evidence on DWI and DTI in the discernment of TRA from TP and assessed whether there is sufficient evidence on a meta-level to support the use of the ADC or FA values in the daily clinical setting. Finally, challenges and opportunities for future clinical studies are elucidated.
Materials and methods
Search strategy and inclusion criteria/exclusion criteria
The updated Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA 2020) guidelines [13] were followed during the conduction of this study. PubMed, EMBASE and The Cochrane Library were searched systematically to retrieve relevant literature published before January 2021. Cross-referencing was used to add relevant literature to the database. Searches were conducted between May 1, 2020 and January 1, 2021.
In order to be eligible for this review, studies needed to describe the use of the ADC or FA values to distinguish TRA from TP in post-treatment glioma patients. To be included (1) studies needed to provide statistics with regard to the ADC/FA values or these data could be retrieved by contacting the corresponding author; (2) ADC/FA data needed to be presented for the TRA and TP group separately; (3) grading of the included glioma needed to be presented following the World Health Organization (WHO) grading system; (4) demographics of the included patients needed to be presented for each group separately (e.g., sex, mean age) and (5) information on the MR imaging protocol, especially the used b-value needed to be reported as b-values, among others, impact the diffusion metrics [14]. Papers were excluded if they were letters, preprints, case reports, congress proceedings, narrative reviews or when based on animals or pediatric populations.
Retrieved papers were assessed in three rounds by two researchers independently (an MD-PhD student with 2 years of research experience and a fourth-year resident in radiology/nuclear medicine holding a PhD in neuro-imaging with over 7 years of expertise in experimental imaging of the brain). The first round comprised screening on title and abstract; the second round comprised full-text analysis to assess whether the papers met any inclusion criteria and/or exclusion criteria. In the third round, information was extracted from the included papers.
Data extracted from each study were (a) first author and year of publication, (b) number of patients included in the TRA and TP groups, (c) mean age of the included participants (per group), (d) sex of the included participants (per group), (e) WHO grade of the glioma, (f) ADC/FA metrics (e.g., mean values, standard deviation, median values, quartiles, ranges), (g) sensitivity/specificity rates and (h) MR imaging protocol (e.g., b-values). Researchers met periodically to discuss their findings, cross-check data and resolve discrepancies.
Meta-analysis
Meta-analysis of the yielded quantitative data was carried out using Review Manager (RevMan) (IOS Version 5.3. Copenhagen: The Nordic Cochrane Centre, The Cochrane Collaboration, 2014) and OpenMetaAnalyst (IOS Version 12.11.14. MetaAnalyst, Tufts Medical Center). A random-effects model was used to compute mean differences in ADC and FA values across studies. Additionally, to assess sensitivity and specificity of the ADC value to distinguish TRA from TP, a diagnostic test accuracy review using a single test approach was conducted. Furthermore, pooled sensitivity/specificity ratio for the included studies were assessed. Heterogeneity was assessed by use of the I2 statistic; I2 ranges from 0% (i.e., no heterogeneity) to 100% (i.e., the highest heterogeneity). To calculate I2 in order to assess its impact on the analysis, first the Chi2-value and degrees of freedom were calculated. Moreover, the estimated standard deviation of the distribution of true effect size (Tau2) was calculated to assign weights to the studies for the random-effects model. The test for overall effect using the Z-test was also calculated to examine whether the pooled estimate of effect is statistically significant. To evaluate the risk of bias and applicability of primary diagnostic accuracy studies, the QUADAS-2 checklist was used. To determine publication bias, the Egger’s regression test was used.
Results
A total of 820 unique studies were identified by systematic searching; four papers were retrieved through cross-referencing. The papers (n = 824) were systematically screened on title and abstract. Based on title and abstract, 662 papers were deemed irrelevant and therefore excluded. The 162 remaining papers were included for full-text analysis. In 52 papers, the primary goal of the study was to assess the infiltration of the glioma in the surrounding brain parenchyma, whereas in 43 papers, response prediction to bevacizumab was the primary outcome. Twenty-six studies focused on the use of diffusion metrics in survival analysis. In thirteen papers, the authors focused on the use of tractography. Seven papers provided insufficient data to be included. Five reviews were excluded; one paper concerned a study on brain metastases and one paper focused on implementing artificial intelligence to discriminate TP from TRA. Ten papers using ADC measurements were included in the meta-analysis [11, 12, 15–22]. Four papers using FA measurements were included for analysis [12, 16, 23, 24]. The WHO classification used to differentiate between tumor grade differs between papers depending on the date of publication. Both WHO 2007 criteria and WHO 2016 criteria have been reported. The differentiation in definite diagnosis between TRA and TP was made using either histopathologic findings after a second look operation [12] or by using the Response Assessment in Neuro-Oncology (RANO) criteria, based on radiological and clinical follow-up over time (i.e., newly appearing enhancing lesion outside of the radiation field or clinical confirmation of disease progression [25]). For the PRISMA flowchart, please see Fig. 1. As assessed by the QUADAS-2 tool, the risk of bias was considered low in all included studies (Fig. 2a, b).
Fig. 1.
PRISMA 2020 Flow Diagram
Fig. 2.
a Barplot of risk of bias and applicability concerns across all ADC studies assessed by QUADAS2. b Barplot of risk of bias and applicability concerns across all FA studies assessed by QUADAS2
Meta-analysis on the use of apparent diffusion coefficient
In total, 413 patients (252 males; 161 females) with an estimated mean age of 50.7 ± 1.3 years were included in this meta-analysis. All studies provided information with regard to the WHO grade of the glioma with the exception of the study of Zakhari et al. [21]. Seven patients suffered from a glioma WHO Grade 2, 101 from a glioma WHO Grade 3 and 288 from a glioma WHO grade 4. In all studies the diffusion tensor imaging related parameter, the b-values, concerned b = 0 s/mm2 and b = 1000 s/mm2. Only the study of Chu et al. (2013) also investigated an additional b-value of 3000 s/mm2 [22] (Table 1). ADC values were determined in different ways based on regions of interest (ROI) of enhancing lesions. In some papers, the ROI were manually drawn, some were manually placed circular ROI and Kazda et al. did not report how the region of interest was selected. On a meta-level, the mean ADC value of the patients in the TP group showed to be 1.13 × 10−3mm2/s with a 95%-confidence interval (95% CI) of 0.912 × 10–3–1.32 × 10−3mm2/s (I2 = 99%; p < 0.001). In the TRA group, on the other hand, the mean ADC value showed to be 1.38 × 10−3mm2/s with a 95% CI of 1.33 × 10–3–1.452 × 10−3mm2/s (I2 = 87%; p < 0.001). Meta-analysis showed that there was a mean difference of − 0.24 × 10−3mm2/s between the mean ADC metrics in TP and TRA. This indicated that there was a significant mean difference between ADC values in TP versus TRA (p = 0.005). However, a highly significant heterogeneity of the included studies was observed with an I2 of 87% (p < 0.0001) (Fig. 3). Figure 4 provides an overview of the sensitivity/specificity ratios of the included studies; only the paper of Zeng et al. (2007) provided insufficient data to be included in this part of the meta-analysis [15]. Pooled sensitivity showed to be 85% (95% CI 78.5–89.8%); pooled specificity showed to be 81% (95% CI 72.3–86.6%). Egger’s regression test showed no significant publication bias (p = 0.700).
Table 1.
Overview of the included ADC studies and demographics of the included patients
| Author | Total (n) | Mean age (SD/range) | Sex (M/F) | WHO grade (n) | b-values (s/mm2) | TP | Mean ADC value (SD) | 95% CI | PsP | Mean ADC (SD); | 95%-CI | TP | FP | FN | TN | Sensitivity/ Specificity (%/%) |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| (n; lesions) | Enhancing lesion (× 10–3 mm2/s) | (n; lesions) | ||||||||||||||
| Enhancing lesion (× 10–3 mm–2/s) | ||||||||||||||||
| Zeng et al. [15] | 55 | 43.67 (11.9) years | 30/25 | 3 (36) | b0/1000 | 32 | 1.20 (0.80) | 0.92–1.48 | 23 | 1.39 (0.90) | 1.02–1.76 | NR | NR | NR | NR | NR |
| 4 (19) | ||||||||||||||||
| Xu et al. [16] | 35 | 45.2 (21–65) years | 19/16 | 2 (4) | b0/1000 | 20 | 1.23 (0.20) | 1.14–1.32 | 15 | 1.54 (0.17) | 1.45–1.63 | 17 | 2 | 3 | 13 | 85/87 |
| 3 (14) | ||||||||||||||||
| 4 (17) | ||||||||||||||||
| Lee et al. [17] | 22 | 48.5 (15.8) | 14-Aug | 3 (3) | b0/1000 | 10 | 1.22 (0.39) | 0.98–1.45 | 12 | 1.35 (0.17) | 1.24–1.45 | 8 | 2 | 2 | 10 | 80/83 |
| 4 (19) | ||||||||||||||||
| Chu et al. [22] | 30 | 50.8 (25–72) | 16/14 | 4 (30) | b0/1000/ | 15 | 1.27 (0.10) | 1.07–1.46 | 15 | 1.33 (0.06) | 1.30–1.36 | 14 | 1 | 0 | 15 | 100/94 |
| 3000 | ||||||||||||||||
| 12 unmethylated; | ||||||||||||||||
| 18 methylated | ||||||||||||||||
| Song et al. (2013) | 20 | 57.1 (8.3); 44.4 (15.1) | 10-Oct | 4 (20) | b0/1000 | 10 | 1.27 (0.2) | 1.18–1.44 | 10 | 1.44 (0.18) | 1.36–1.52 | 9 | 1 | 1 | 9 | 90/90 |
| 7 unmethylated; 13 methylated | ||||||||||||||||
| Prager et al. [19] | 68 | 54.9 (22.6–79.4) years | 51/17 | 3 (13) | b0/1000 | 58 | 1.38 (0.13) | 1.35–1.41 | 10 | 1.59 (0.19) | 1.47–1.71 | 41 | 2 | 3 | 5 | 93/71 |
| 4 (55) | ||||||||||||||||
| 19 unmethylated; 12 methylated | ||||||||||||||||
| Kazda et al. [20] | 39 | 51 (29–66) | 28-Nov | 4 (39) | b0/1000 | 29 | 0.61 (0.04) | 0.59–0.63 | 10 | 1.33 (0.4) | 1.08–1.58 | 28 | 1 | 0 | 10 | 100/91 |
| Zakhari et al. [21] | 17 | 55.9 (10.3) years | 13-Apr | HGG | b0/1000 | 9 | 1.10 (0.21) | 0.96–1.24 | 8 | 1.06 (0.27) | 0.87–1.25 | 7 | 3 | 2 | 5 | 78/63 |
| Yang et al. [11] | 91 | 48.7 (14.2)(9–77) years | 53/38 | 3 (29) | b0/1000 | 51 | 0.80 (0.08) | 0.78–0.82 | 40 | 1.3 (0.05) | 1.28–1.32 | 40 | 7 | 11 | 33 | 78/83 |
| 4 (62) | ||||||||||||||||
| 22 IDHm; 69 IDHwt | ||||||||||||||||
| Park et al. [12] | 36 | 52.3 (13.7)(n = 25) 57.1 (14.8)(n = 11) | 18/18 | 2 (3) | b0/1000 | 25 | 1.28 (0.14) | 1.23–1.33 | 11 | 1.47 (0.21) | 1.35–1.59 | 21 | 4 | 4 | 7 | 84/64 |
| 3 (6) | ||||||||||||||||
| 4 (27) |
Fig. 3.
Forest plot of included studies on ADC metrics
Fig. 4.
Summary receiver operator characteristics plot of sensitivity and 1-specificity ratios of the included studies
Meta-analysis on the use of fractional anisotropy
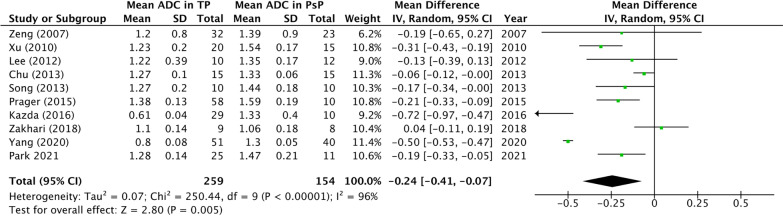
Four studies totaling 154 patients (85 males; 69 females; estimated mean age of 51.8 ± 4.6 years) were included in this analysis. Razek et al. [24] did not report mean age or WHO grade for individual patients, only that they included WHO 3 and WHO 4 gliomas. Studies that reported the individual participants’ characteristics showed that seven patients had WHO 2 gliomas, twenty had WHO 3 and 85 patients suffered from WHO 4 grade glioma. In total the studies found 90 TP and 64 TRA. In all studies, the b-values used were b = 0 s/mm2 and b = 1000 s/mm2. More information on baseline populations can be found in Table 2. All FA values are based on ROI in and around the contrast-enhancing lesion, in three studies they were manually drawn, Wang et al. used semi-automated segmentation. Mean FA value for TP was 0.19 (95% CI 0.189–0.194), while mean FA value for TRA was 0.14 (95% CI 0.137–0.143). The mean difference of FA values between TP and TRA groups was found to be 0.05 and showed to be significantly different (p = 0.002) (Fig. 5). Pooled sensitivity and pooled specificity showed to be 75.2% (95% CI 53.3–89.1%) and 77.6% (95% CI 60.5–90.4%), respectively (Fig. 6). Egger’s regression test again showed no significant publication bias (p = 0.200).
Table 2.
Overview of the included FA studies and demographics of the included patients
| Author | Total (n) | Mean age (SD/range) | Sex (M/F) | WHO grade (n) | b-values (s/mm2) | TP | Mean FA value (SD) | 95% CI | TRA | Mean FA value (SD) | 95%-CI | TP | FP | FN | TN | Sensitivity/ Specificity (%/%) |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| (n; lesions) | (n; lesions) | |||||||||||||||
| Enhancing lesion | Enhancing lesion | |||||||||||||||
| Xu et al. (2010) | 35 | 45.2 (21–65) | 19/16 | 2 (4) | b0/1000 | 20 | 0.24 (0.05) | 0.218–0.262 | 15 | 0.14 (0.03) | 0.125–0.155 | 17 | 2 | 3 | 13 | 85/87 |
| 3 (14) | ||||||||||||||||
| 4 (17) | ||||||||||||||||
| Wang et al. (2016) | 41 | 55.71 (11.83) | 27/14 | 4 (41) | b0/1000 | 21 | 0.14 (0.04) | 0.123–0.157 | 20 | 0.11 (0.03) | 0.0969–0.123 | 15 | 5 | 6 | 15 | 71/75 |
| Razek et al | 42 | NR | 13-Nov | 3 (NR) | b0/1000 | 24 | 0.20 (0.04) | 0.184–0.216 | 18 | 0.15 (0.03) | 0.136–0.164 | 20 | 4 | 4 | 14 | 83/78 |
| 4 (NR) | ||||||||||||||||
| Park et al. (2021) | 36 | 52.3 (13.7)(n = 25) 57.1 (14.8)(n = 11) | 18/18 | 2 (3) | b0/1000 | 25 | 0.19 (0.05) | 0.18–0.22 | 11 | 0.16 (0.03) | 0.142–0.178 | 16 | 3 | 9 | 8 | 64/73 |
| 3 (6) | ||||||||||||||||
| 4 (27) |
Fig. 5.
Forest plot of included studies on FA metrics
Fig. 6.
Summary receiver operator characteristics plot of sensitivity and 1-specificity ratios of the included studies
Discussion
Although of paramount importance in the follow-up and management of glioma patients, to date it is proven difficult to accurately differentiate between the TP and TRA. Because the outcome between TRA and TP is vitally different, early accurate differentiation of the two could help prevent re-intervention in TRA patients while also providing grounds for treatment in the TP patient group. This meta-analysis shows that, on a group level, the ADC and, to a lesser extent, FA values can be used to distinguish TP from TRA in post-treatment glioma patients (p = 0.005) with pooled sensitivities and specificities of 85% and 81%, and 75% and 78% for ADC and FA values, respectively. The estimated mean ADC and FA values of the patients in the TP group and in the TRA group were consistent with the theory that TP is the result of increased tumor cell proliferation, which causes a reduction in extracellular water diffusion, resulting in a lower ADC value [26, 27]. It has been hypothesized that decreased cellularity due to necrosis as a result of treatment damage (TRA) results in a lower FA value with more extracellular volume, whereas the FA value would increase due to an increased cellularity in TP when growing along existing white matter tracts [28]. The mechanisms driving TRA, however, remain partially elusive. It is believed that due to the (micro)vascular damage after radiation therapy, capillary leakage occurs, resulting in the production of cytotoxic and vasogenic edema [29]. In addition, oligodendroglial injury also plays an important role in the development of TRA [30]. Thereby, it is believed that TRA is reflected by relatively increased ADC value of the tissue [19], with a relative decrease of FA [9]. These hypotheses are corroborated by current findings.
The presented ADC data available for meta-analysis was limited when compared to the abundance of literature dealing with DWI in the follow-up of glioma. This is due to the use of different statistical measures and different outcomes in different papers. Research into different measures of the ADC value, like 5th percentile or relative ADC value could provide new information for the development of ADC maps [10, 27, 31]. However, the use of different measures might slow down further developments and future research due to limited availability of comparable data for meta-analysis. This would be disadvantageous as the ADC maps have also shown promising results with regard to identifying infiltrative patterns of glioma growth [32], predicting O6-methylguanine-DNA methyl-transferase (MGMT) methylation status [33] and predicting treatment outcomes and survival [33–35]. In addition, in patients who underwent laser interstitial thermal therapy for glioblastoma, the ADC value of the direct postoperative MRI scan (< 24 h) in the peritumoral region showed to be correlated with regions of later tumor recurrence [36].
The FA value is a scalar value between 0 and 1.0 and thereby is a more consistent metric between participants. Next to differentiating TP from TRA, the FA value has also been reported to be able to detect isocitrate dehydrogenase (IDH) status in oligodendroglial tumors to assess the prognosis and treatment options noninvasively and with an accuracy of about 80% [37]. Another possibility of FA value is to assess infiltration of tumor cells and predict sites of recurrence of glioma by analyzing peritumoral edema or by using distance-informed Track-weighted imaging [38, 39]. This shows promise for detecting invasion and aid in determining the clinical radiation target volume.
Additionally, there have been studies which add other metrics to the imaging diagnostics pipeline (multimodality MRI) in order to make the differentiation between recurrence and treatment-induced change more reliable. Perfusion magnetic resonance imaging (dynamic contrast enhancement, dynamic susceptibility contrast and arterial spin labeling) and magnetic resonance spectroscopy have been reported to be able to accurately distinguish between tumor tissue and radiation induced TRA [2, 20, 40]. PET-MR can be used to monitor treatment response in glioma and to detect recurrence [2]. It is important to note that all diagnostics have their own strengths and boundaries. Knowledge of the properties of these advanced imaging techniques can facilitate the synthesis of more evidence-based assessment of the tissue and help lead to accurate diagnosis of the problem at hand.
Limitations and challenges for implementation of ADC and FA analysis in individual patients
A limitation of this review concerns the fact that the review was not registered in an international database of prospectively registered systematic reviews.
As shown in the present meta-analysis, the ADC and FA values can be used to distinguish TP and TRA in research settings on a group level. A prominent and characteristic limitation of DWI/DTI is the lack of validated diagnostic criteria on an individual level. This partly explains the different sensitivity and specificity values between research populations and further research is warranted in order to be able to specify and validate individual diagnostic criteria and improve the scope of use for DWI/DTI metrics.
Another general limitation for diffusion metrics is that the interpretation of values without context is highly ambiguous and the ADC/FA values are influenced by other factors such as clinical data (e.g., age, atrophy, other white matter defects), measurement purpose (i.e., detect IDH status or discriminate TRA from TP) as well as scanner type and protocol) which all can lead to significant intra-individual differences in ADC/FA values. Significant differences in ADC values can occur on an individual level depending on the scanner and scanning protocol used, thereby not only reflecting a difference between TP and TRA but also a difference on group level inflicted by scanner type. This is inherent to current standards for reporting diffusion weights with only b-values, rather than reporting the duration of, and time between, the pulsed magnetic field gradients encoding motion [41]. In order to tackle this shortcoming, we suggest standardizing acquisition or reporting these additional timings according to the FAIR-principles. Longitudinal single center studies using the same DWI protocol to follow, e.g., treatment response, do not experience this issue as long as they use their institutional reference values. Apart from only reporting b-values rather than DWI gradient timing, the low b-value used in current research (b0) does not take into consideration signal present from blood flow or perfusion which has not yet been attenuated. b-values above approximately 100 s/mm2 have been shown to attenuate these signals, and only signal from diffusing water remains[41]. Future studies might consider calculating DWI metrics using b-values of 100 s/mm2 as the lower value in order to avoid perfusion and blood flow effects to assess possible differences in diagnostic outcome and reliability.
It should also be taken into consideration that, despite the general recommendation that the radiological follow-up of glioma should be performed by experienced radiologists using with a multiparametric MRI protocol containing up-to-date sequences. Using FA parameters in the follow-up of glioma implies that all MRI scanners have access to this modality. This is, however, not always the case, as the value of the DTI sequences is still being investigated. Diffusion-weighted imaging, on the other hand, is available as a standard sequence and therefore widely available for the follow-up of glioma. Therefore, it is recommended to focus future research on harmonization of imaging protocols and diffusion metrics in order to create more interchangeable ADC values. This will allow for more reliable diagnoses based on diffusion metrics.
The different means of tissue mapping (ROI/manual segmentation) are another variable thwarting normalization of the process. Advanced analysis is warranted in order to determine the best course of action for tissue mapping. Furthermore, the co-occurrence of TP and necrotic changes [42, 43] impact the diffusion values which further complicates usage and standardized application in the daily clinical setting. It is also important to note that Xu et al. and Park et al. included WHO 2 glioma patients, which are defined as low-grade gliomas and could respond differently to treatment and possibly influence imaging results, as this paper focuses on high-grade gliomas.
Additionally, the quality of the majority of the papers on this subject was insufficient as most authors did not report standard metrics (e.g., mean, standard deviation, 95% CI) though instead reported values which produced significant results in relatively small datasets. Future research should focus on the publication of study data following the FAIR principles (i.e., findable, accessible, interoperable, re-usable). The FAIR principles underline the importance of the capacity of computational systems to find, access, interoperate, and reuse data with none or minimal human intervention as the data which has to be dealt with shows an increase in volume and complexity and is created significantly faster than before [44].
Finally, the clinical implementation of the reported results of this meta-analysis will be hampered by inter-subject variability of the ADC/FA maps. Therefore, an externally validated prediction model with diagnostic criteria on an individual level is necessary and cannot be derived from group analyses. This could be achieved by using a uniform method of normalization on a prospective cohort, for example by obtaining the ADC value from the same region in a standardized atlas, using a normalized scanning protocol with a standardized method of tissue mapping.
Conclusion
The current meta-analysis showed that ADC and FA metrics can accurately distinguish TP and TRA in groups of patients. For further clinical implementation, harmonization of imaging protocols and reading procedures is required. In addition, well-validated criteria that can be used in individual patients, based on clinical studies, preferably in large, prospective cohorts with FAIR publication of study data, are warranted for this field to further develop.
Abbreviations
- ADC
Apparent diffusion coefficient
- DTI
Diffusion tensor imaging
- DWI
Diffusion-weighted imaging
- FA
Fractional anisotropy
- FAIR
Findable, accessible, interoperable, reusable
- IDH
Isocitrate dehydrogenase
- MGMT
O6-methylguanine-DNA methyltransferase
- PRISMA
Preferred reporting items for systematic reviews and meta-analyses
- PWI
Perfusion-weighted imaging
- RANO
Response Assessment in Neuro-Oncology
- ROI
Region of interest
- TP
Tumor progression
- TRA
Treatment-related abnormalities
- VEGF
Vascular endothelial growth factor
- WHO
World Health Organization
Author contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by the first and last author. The first draft of the manuscript was written by the first author and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Funding
Part of this work was funded by INTERREG Europe (Project NR. 203020/2020P18).
Availability of data and materials
The datasets generated during and/or analyzed during the current study are available from the corresponding author at reasonable request.
Declarations
Ethical approval and consent to participate
Ethical approval was waived.
Consent for publication
All authors read and approved the final manuscript and gave consent for publication.
Competing interests
The authors declare that they have no competing interests.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Abbasi AW, Westerlaan HE, Holtman GA, Aden KM, van Laar PJ, van der Hoorn A. Incidence of tumour progression and pseudoprogression in high-grade gliomas: a systematic review and meta-analysis. Clin Neuroradiol. 2018;28(3):401–411. doi: 10.1007/s00062-017-0584-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Strauss SB, Meng A, Ebani EJ, Chiang GC. Imaging glioblastoma posttreatment: progression, pseudoprogression, pseudoresponse, radiation necrosis. Neuroimaging Clin N Am. 2021;31(1):103–120. doi: 10.1016/j.nic.2020.09.010. [DOI] [PubMed] [Google Scholar]
- 3.Lu VM, Welby JP, Laack NN, Mahajan A, Daniels DJ. Pseudoprogression after radiation therapies for low grade glioma in children and adults: a systematic review and meta-analysis. Radiother Oncol. 2020;142:36–42. doi: 10.1016/j.radonc.2019.07.013. [DOI] [PubMed] [Google Scholar]
- 4.Ryken TC, Aygun N, Morris J, Schweizer M, Nair R, Spracklen C, et al. The role of imaging in the management of progressive glioblastoma: a systematic review and evidence-based clinical practice guideline. J Neurooncol. 2014;118(3):435–460. doi: 10.1007/s11060-013-1330-0. [DOI] [PubMed] [Google Scholar]
- 5.Thust SC, van den Bent MJ, Smits M (2018) Pseudoprogression of brain tumors. J Magn Reson Imaging 48:571–589 [DOI] [PMC free article] [PubMed]
- 6.Mardor Y, Roth Y, Ocherashvilli A, Spiegelmann R, Tichler T, Daniels D, et al. Pretreatment prediction of brain tumors' response to radiation therapy using high b-value diffusion-weighted MRI. Neoplasia. 2004;6(2):136–142. doi: 10.1593/neo.03349. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Sugahara T, Korogi Y, Kochi M, Ikushima I, Shigematu Y, Hirai T, et al. Usefulness of diffusion-weighted MRI with echo-planar technique in the evaluation of cellularity in gliomas. J Magn Reson Imaging. 1999;9(1):53–60. doi: 10.1002/(SICI)1522-2586(199901)9:1<53::AID-JMRI7>3.0.CO;2-2. [DOI] [PubMed] [Google Scholar]
- 8.Mangraviti A, Legnani FG. Diffusion magnetic resonance imaging phenotypes predict overall survival benefit from bevacizumab or surgery in recurrent glioblastoma with large tumor burden COMMENT. Neurosurgery. 2020;87(5):938. doi: 10.1093/neuros/nyaa135. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Olsen KI, Schroeder P, Corby R, Vucic I, Bardo DM. Advanced magnetic resonance imaging techniques to evaluate CNS glioma. Expert Rev Neurother. 2005;5(6 Suppl):S3–11. doi: 10.1586/14737175.5.6.S3. [DOI] [PubMed] [Google Scholar]
- 10.Bette S, Huber T, Gempt J, Boeckh-Behrens T, Wiestler B, Kehl V, et al. Local fractional anisotropy is reduced in areas with tumor recurrence in glioblastoma. Radiology. 2017;283(2):499–507. doi: 10.1148/radiol.2016152832. [DOI] [PubMed] [Google Scholar]
- 11.Yang YL, Yang YJ, Wu XL, Pan Y, Zhou D, Zhang HD, et al. Adding DSC PWI and DWI to BT-RADS can help identify postoperative recurrence in patients with high-grade gliomas. J Neurooncol. 2020;146(2):363–371. doi: 10.1007/s11060-019-03387-6. [DOI] [PubMed] [Google Scholar]
- 12.Park YW, Ahn SS, Kim EH, Kang SG, Chang JH, Kim SH, et al. Differentiation of recurrent diffuse glioma from treatment-induced change using amide proton transfer imaging: incremental value to diffusion and perfusion parameters. Neuroradiology. 2021;63(3):363–372. doi: 10.1007/s00234-020-02542-5. [DOI] [PubMed] [Google Scholar]
- 13.Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71. doi: 10.1136/bmj.n71. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Hagmann P, Jonasson L, Maeder P, Thiran JP, Wedeen VJ, Meuli R. Understanding diffusion MR imaging techniques: from scalar diffusion-weighted imaging to diffusion tensor imaging and beyond. Radiographics. 2006;26(Suppl 1):S205–S223. doi: 10.1148/rg.26si065510. [DOI] [PubMed] [Google Scholar]
- 15.Zeng QS, Li CF, Liu H, Zhen JH, Feng DC. Distinction between recurrent glioma and radiation injury using magnetic resonance spectroscopy in combination with diffusion-weighted imaging. Int J Radiat Oncol. 2007;68(1):151–158. doi: 10.1016/j.ijrobp.2006.12.001. [DOI] [PubMed] [Google Scholar]
- 16.Xu JL, Li YL, Lian JM, Dou SW, Yan FS, Wu H, et al. Distinction between postoperative recurrent glioma and radiation injury using MR diffusion tensor imaging. Neuroradiology. 2010;52(12):1193–1199. doi: 10.1007/s00234-010-0731-4. [DOI] [PubMed] [Google Scholar]
- 17.Lee WJ, Choi SH, Park CK, Yi KS, Kim TM, Lee SH, et al. Diffusion-weighted MR imaging for the differentiation of true progression from pseudoprogression following concomitant radiotherapy with temozolomide in patients with newly diagnosed high-grade gliomas. Acad Radiol. 2012;19(11):1353–1361. doi: 10.1016/j.acra.2012.06.011. [DOI] [PubMed] [Google Scholar]
- 18.Ma L, Song ZJ. Differentiation between low-grade and high-grade glioma using combined diffusion tensor imaging metrics. Clin Neurol Neurosurg. 2013;115(12):2489–2495. doi: 10.1016/j.clineuro.2013.10.003. [DOI] [PubMed] [Google Scholar]
- 19.Prager AJ, Martinez N, Beal K, Omuro A, Zhang Z, Young RJ. Diffusion and perfusion MRI to differentiate treatment-related changes including pseudoprogression from recurrent tumors in high-grade gliomas with histopathologic evidence. AJNR Am J Neuroradiol. 2015;36(5):877–885. doi: 10.3174/ajnr.A4218. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Kazda T, Bulik M, Pospisil P, Lakomy R, Smrcka M, Slampa P, et al. Advanced MRI increases the diagnostic accuracy of recurrent glioblastoma: single institution thresholds and validation of MR spectroscopy and diffusion weighted MR imaging. Neuroimage Clin. 2016;11:316–321. doi: 10.1016/j.nicl.2016.02.016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Zakhari N, Taccone MS, Torres C, Chakraborty S, Sinclair J, Woulfe J, et al. Diagnostic accuracy of centrally restricted diffusion in the differentiation of treatment-related necrosis from tumor recurrence in high-grade gliomas. AJNR Am J Neuroradiol. 2018;39(2):260–264. doi: 10.3174/ajnr.A5485. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Chu HH, Choi SH, Ryoo I, Kim SC, Yeom JA, Shin H, et al. Differentiation of true progression from pseudoprogression in glioblastoma treated with radiation therapy and concomitant temozolomide: comparison study of standard and high-b-value diffusion-weighted imaging. Radiology. 2013;269(3):831–840. doi: 10.1148/radiol.13122024. [DOI] [PubMed] [Google Scholar]
- 23.Wang S, Martinez-Lage M, Sakai Y, Chawla S, Kim SG, Alonso-Basanta M, et al. Differentiating tumor progression from pseudoprogression in patients with glioblastomas using diffusion tensor imaging and dynamic susceptibility contrast MRI. AJNR Am J Neuroradiol. 2016;37(1):28–36. doi: 10.3174/ajnr.A4474. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Razek A, El-Serougy L, Abdelsalam M, Gaballa G, Talaat M. Differentiation of residual/recurrent gliomas from postradiation necrosis with arterial spin labeling and diffusion tensor magnetic resonance imaging-derived metrics. Neuroradiology. 2018;60(2):169–177. doi: 10.1007/s00234-017-1955-3. [DOI] [PubMed] [Google Scholar]
- 25.Wen PY, Macdonald DR, Reardon DA, Cloughesy TF, Sorensen AG, Galanis E, et al. Updated response assessment criteria for high-grade gliomas: response assessment in neuro-oncology working group. J Clin Oncol. 2010;28(11):1963–1972. doi: 10.1200/JCO.2009.26.3541. [DOI] [PubMed] [Google Scholar]
- 26.Fudaba H, Shimomura T, Abe T, Matsuta H, Momii Y, Sugita K, et al. Comparison of multiple parameters obtained on 3T pulsed arterial spin-labeling, diffusion tensor imaging, and MRS and the Ki-67 labeling index in evaluating glioma grading. AJNR AJNR Am J Neuroradiol. 2014;35(11):2091–2098. doi: 10.3174/ajnr.A4018. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Agarwal A, Kumar S, Narang J, Schultz L, Mikkelsen T, Wang S, et al. Morphologic MRI features, diffusion tensor imaging and radiation dosimetric analysis to differentiate pseudo-progression from early tumor progression. J Neurooncol. 2013;112(3):413–420. doi: 10.1007/s11060-013-1070-1. [DOI] [PubMed] [Google Scholar]
- 28.Server A, Graff BA, Josefsen R, Orheim TE, Schellhorn T, Nordhøy W, et al. Analysis of diffusion tensor imaging metrics for gliomas grading at 3 T. Eur J Radiol. 2014;83(3):e156–e165. doi: 10.1016/j.ejrad.2013.12.023. [DOI] [PubMed] [Google Scholar]
- 29.Fike JR, Cann CE. Contrast medium accumulation and washout in canine brain tumors and irradiated normal brain: a CT study of kinetics. Radiology. 1984;151(1):115–120. doi: 10.1148/radiology.151.1.6701300. [DOI] [PubMed] [Google Scholar]
- 30.Brandsma D, Stalpers L, Taal W, Sminia P, van den Bent MJ. Clinical features, mechanisms, and management of pseudoprogression in malignant gliomas. Lancet Oncol. 2008;9(5):453–461. doi: 10.1016/S1470-2045(08)70125-6. [DOI] [PubMed] [Google Scholar]
- 31.Reimer C, Deike K, Graf M, Reimer P, Wiestler B, Floca RO, et al. Differentiation of pseudoprogression and real progression in glioblastoma using ADC parametric response maps. PLoS One. 2017;12(4):e0174620. doi: 10.1371/journal.pone.0174620. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Lutz K, Wiestler B, Graf M, Baumer P, Floca R, Schlemmer HP, et al. Infiltrative patterns of glioblastoma: identification of tumor progress using apparent diffusion coefficient histograms. J Magn Reson Imaging. 2014;39(5):1096–1103. doi: 10.1002/jmri.24258. [DOI] [PubMed] [Google Scholar]
- 33.Pope WB, Lai A, Mehta R, Kim HJ, Qiao J, Young JR, et al. Apparent diffusion coefficient histogram analysis stratifies progression-free survival in newly diagnosed bevacizumab-treated glioblastoma. AJNR Am J Neuroradiol. 2011;32(5):882–889. doi: 10.3174/ajnr.A2385. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Buemi F, Guzzardi G, Del Sette B, Sponghini AP, Matheoud R, Soligo E, et al. Apparent diffusion coefficient and tumor volume measurements help stratify progression-free survival of bevacizumab-treated patients with recurrent glioblastoma multiforme. Neuroradiol J. 2019;32(4):241–249. doi: 10.1177/1971400919847184. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Elson A, Bovi J, Siker M, Schultz C, Paulson E. Evaluation of absolute and normalized apparent diffusion coefficient (ADC) values within the post-operative T2/FLAIR volume as adverse prognostic indicators in glioblastoma. J Neurooncol. 2015;122(3):549–558. doi: 10.1007/s11060-015-1743-z. [DOI] [PubMed] [Google Scholar]
- 36.Mahammedi A, Bachir S, Escott EJ, Barnett GH, Mohammadi AM, Larvie M. Prediction of recurrent glioblastoma after laser interstitial thermal therapy: the role of diffusion imaging. Neurooncol Adv. 2019;1(1):vdz021. doi: 10.1093/noajnl/vdz021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Xiong J, Tan WL, Pan JW, Wang Y, Yin B, Zhang J, et al. Detecting isocitrate dehydrogenase gene mutations in oligodendroglial tumors using diffusion tensor imaging metrics and their correlations with proliferation and microvascular density. J Magn Reson Imaging. 2016;43(1):45–54. doi: 10.1002/jmri.24958. [DOI] [PubMed] [Google Scholar]
- 38.Metz MC, Molina-Romero M, Lipkova J, Gempt J, Liesche-Starnecker F, Eichinger P, et al. Predicting glioblastoma recurrence from preoperative MR scans using fractional-anisotropy maps with free-water suppression. Cancers. 2020;12(3):728. doi: 10.3390/cancers12030728. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Bell C, Pannek K, Fay M, Thomas P, Bourgeat P, Salvado O, et al. Distance informed track-weighted imaging (diTWI): a framework for sensitising streamline information to neuropathology. Neuroimage. 2014;86:60–66. doi: 10.1016/j.neuroimage.2013.07.077. [DOI] [PubMed] [Google Scholar]
- 40.Heiss WD, Raab P, Lanfermann H. Multimodality assessment of brain tumors and tumor recurrence. J Nucl Med. 2011;52(10):1585–1600. doi: 10.2967/jnumed.110.084210. [DOI] [PubMed] [Google Scholar]
- 41.Scheenen TW, Rosenkrantz AB, Haider MA, Fütterer JJ. Multiparametric magnetic resonance imaging in prostate cancer management: current status and future perspectives. Invest Radiol. 2015;50(9):594–600. doi: 10.1097/RLI.0000000000000163. [DOI] [PubMed] [Google Scholar]
- 42.Ellingson BM, Chung C, Pope WB, Boxerman JL, Kaufmann TJ. Pseudoprogression, radionecrosis, inflammation or true tumor progression? Challenges associated with glioblastoma response assessment in an evolving therapeutic landscape. J Neurooncol. 2017;134(3):495–504. doi: 10.1007/s11060-017-2375-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Wang S, Martinez-Lage M, Sakai Y, Chawla S, Kim SG, Alonso-Basanta M, et al. Differentiating tumor progression from pseudoprogression in patients with glioblastomas using diffusion tensor imaging and dynamic susceptibility contrast MRI. AJNR AJNR Am J Neuroradiol. 2016;37(1):28–36. doi: 10.3174/ajnr.A4474. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Wilkinson MD, Dumontier M, Jan Aalbersberg I, Appleton G, Axton M, Baak A, et al. Addendum: the FAIR Guiding Principles for scientific data management and stewardship. Sci Data. 2019;6(1):6. doi: 10.1038/s41597-019-0009-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The datasets generated during and/or analyzed during the current study are available from the corresponding author at reasonable request.