OBJECTIVES:
Tracheostomy is commonly performed in critically ill patients requiring prolonged mechanical ventilation (MV). We evaluated the outcomes of tracheostomy in patients who received greater than or equal to 1 week MV and were followed for 1 year.
DESIGN:
In this secondary analysis of a prospective observational study, we compared outcomes in tracheostomy versus nontracheostomy patients. Outcomes post ICU included Functional Independence Measure (FIM) subscales, 6-Minute Walk Test (6MWT), Short Form 36 (SF36), Medical Research Council (MRC) Scale, pulmonary function tests (PFTs), Impact of Event Scale (IES), Beck Depression Inventory-II (BDI-II), and vital status and disposition.
SETTING:
Nine University affiliated ICUs in Canada.
PATIENTS:
Medical/surgical patients requiring MV for 7 or more days who were enrolled in the Towards RECOVER Study.
MEASUREMENTS AND MAIN RESULTS:
Of 398 ICU survivors, 193 (48.5%) received tracheostomy, on median ICU day 14 (interquartile range [IQR], 8–0 d). Patients with tracheostomy were older, had similar severity of illness, had longer MV duration and ICU and hospital stays, and had higher risk of ICU readmission (odds ratio [OR], 1.9; 95% CI, 1.0–3.2) and hospital mortality (OR, 2.6; 95% CI, 1.1–6.1), but not 1-year mortality (hazard ratio, 1.41; 95% CI, 0.88–1.2). Over 1 year, tracheostomy patients had lower FIM-Total (7.7 points; 95% CI, 2.2–13.2); SF36, IES, and BDI-II were similar. From 3 months, tracheostomy patients had 12% lower 6MWT (p = 0.0008) and lower MRC score (3.4 points; p = 0.006). Most PFTs were 5–8% lower in the tracheostomy group. Tracheostomy patients had similar specialist visits (rate ratio, 0.63; 95% CI, 0.28–2.4) and hospital readmissions (OR, 0.82; 95% CI, 0.54–1.3) but were less likely to be at home at hospital discharge and 1 year.
CONCLUSIONS:
Patients who received tracheostomy had more ICU and hospital care and higher hospital mortality compared with patients who did not receive a tracheostomy. In 1 year follow-up, tracheostomy patients required a higher daily burden of care, expressed by FIM.
Keywords: critical illness, disposition, mechanical ventilation, outcomes, tracheostomy
KEY POINTS
Question: We evaluated the outcomes of tracheostomy in patients who received ≥1 week mechanical ventilation and were followed for 1 year.
Findings: Patients who received tracheostomy had more ICU and hospital care and higher hospital mortality compared with patients who did not receive a tracheostomy. In 1 year follow-up, tracheostomy patients required a higher daily burden of care, expressed by Functional Independence Measure (FIM).
Meanings: Information regarding discharge disposition, independent living, and psychological health is vital when patients and family members make decisions about ongoing ICU support, including tracheostomy.
Tracheostomy to facilitate prolonged mechanical ventilation (MV) in critically ill patients may be justified by the potential for improved comfort, reduced sedative needs, reduced duration of MV, and reduced laryngeal trauma (1). However, these conclusions are based on small, heterogeneous trials. Tracheostomy in this setting has implications regarding quality of life, discharge disposition, and costs (1–4); however few studies have evaluated quality of life, functional status, and psychologic outcomes in patients who undergo tracheostomy in the ICU. These patient-centered data are integral to decision-making regarding tracheostomy procedures in the ICU.
The Towards RECOVER Study enrolled medical/surgical patients requiring MV for 7 or more days and demonstrated that the FIM at day 7 after ICU discharge, which was predicted by age and ICU length of stay (LOS), determined the recovery trajectory to 1 year after ICU discharge, and was an independent risk factor for post-ICU mortality (5). Overall, 193 patients (48.5%) had a tracheostomy inserted in the ICU, providing an opportunity to describe long-term outcomes in this population, and contrast them with patients who did not receive a tracheostomy.
The objectives of this secondary analysis of the RECOVER study were to compare the following variables between tracheostomy and nontracheostomy patients: 1) survival at 1 week and 3, 6, and 12 months after ICU discharge; 2) disposition at hospital discharge, ICU readmission, need for specialty visit; and 3) FIM at 1 week, 3, 6, and 12 months after ICU discharge, 6-Minute Walk Test (6MWT), Short Form 36 (SF36), Medical Research Council (MRC) score, Impact of Event Scale (IES), Beck Depression Inventory-II (BDI-II), and pulmonary function tests (PFTs). We hypothesized that patients who received a tracheostomy in the ICU had worse physical and psychologic outcomes than patients who did not receive a tracheostomy.
METHODS
Towards RECOVER was a multicenter prospective cohort study conducted between February 2007 and March 2014 in collaboration with the Canadian Critical Care Trials Group and involving nine university-affiliated ICUs in Toronto (four sites), Hamilton, Ottawa, Montreal, Sherbrooke, and Vancouver (5).
We obtained written informed consent from the substitute decision-maker when the patient met study criteria, and this consent extended to the 7-day in-hospital follow-up. At 3-month follow-up, when the patient had capacity, we obtained a first person written informed consent to proceed with the 1-year follow-up. The study was approved by the Research Ethics Boards at each participating hospital (University Health Network REB no. 06-0157-AE, April 7, 2006; Mount Sinai Hospital REB no. 07-0287-E, Dec 12, 2007; Sunnybrook Health Sciences Center REB no. 356-2007, December 10, 2007; St. Michaels Hospital REB no. 08-080, September 11, 2008; St. Joseph’s Hamilton REB no. 09-3151, March 31, 2009; Ottawa Health Science Network REB no. 2009686-01H, December 14, 2009; Maisonneuve Rosemont REB no. 2012-465, May 11, 2011; Centre intégré universitaire de santé et de services sociaux de l’Estrie—Centre hospitalier universitaire de Sherbrooke REB no. 10-184, February 1, 2011; University of British Columbia—Saint Paul’s REB no. H10-00606, September 27, 2010). The procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional or regional) and with the Helsinki Declaration of 1975.
Eligible patients were 16 years old or older with dependence on MV in ICU for 7 days or more. Detailed patient inclusion and exclusion criteria and study methods may be found in the original publication (5). In total, 534 patients were enrolled, 398 survived to ICU discharge, seven of 398 died within 7 days, and 391 were included in the 1-year cohort.
Patient Population: Baseline Characteristics and ICU Course
As per the original publication, patients were stratified into four disability risk groups: Group 1—young short LOS (age < 42 yr, < 2 wk in ICU); Group 2—mid age variable LOS (≥ 42 yr, < 2 wk in ICU and ≤ 45 yr, ≥ 2 wk in ICU); Group 3—older long LOS (46–66 yr, ≥ 2 wk in ICU); and Group 4—oldest long LOS; (> 66 yr, ≥ 2 wk in ICU) (1). Within each disability risk group, we compared demographics, severity of chronic and acute illness, and reason for ICU admission between tracheostomy and nontracheostomy patients. For tracheostomy patients, we describe the indication; data on technique (percutaneous or surgical) and on decannulation timing were not collected. Severity of illness was defined by the Acute Physiology and Chronic Health Evaluation (APACHE) II score calculated within the first 24 hours after ICU admission (day 0), Multiple Organ Dysfunction Score (MODS) determined daily from day 0 to day 7 and then twice per week for the duration of the ICU stay, and Elixhauser and Charlson scores.
Outcomes
Short-term outcomes included durations of MV and ICU and hospital stay, receipt of renal replacement therapy (RRT) and steroids, and hospital mortality. Long-term functional outcomes measured at 3, 6, and 12 months post ICU discharge included the following: 1) FIM total, motor, and cognitive subscales, where higher scores represent more independence (6); 2) 6MWT with continuous oximetry (7); 3) MRC score, where higher scores represent greater strength (8); 4) health-related quality of life (Medical Outcome SF-36) mental summary score (MCS) and physical summary score (PCS) (9), where higher scores represent better quality of life; 5) IES (10), where higher scores represent more distress; 6) BDI-II (11), where higher scores represent higher severity of depression; and 7) pulmonary function tests (PFTs). IES and BDI are self-administered questionnaires of posttraumatic stress disorder and depressive symptoms respectively. Health utilization outcomes included ICU and hospital readmission and the number of specialty visits; the many different specialists seen precluded detailed analysis of each specialty. Finally, we measured disposition (home, other hospital, rehabilitation center) at hospital discharge and at 1 year and survival 1 year after ICU discharge.
Statistical Analysis
We summarized baseline characteristics in eight groups formed by the cross-tabulation of RECOVER disability risk group and the receipt of tracheostomy using means and sds or counts and percentages.
Given the small number of patients, low tracheostomy rate (2/23), and nearly uniform good outcomes of group 1 (5), we restricted our analysis of outcomes to patients in groups 2, 3, and 4, which were the highest risk groups. All analyses of outcomes in patients with versus without a tracheostomy were adjusted for RECOVER group and are reported with 95% CIs. We compared durations (ICU stay, hospital stay, MV) using linear regression on log-duration, reported as a ratio of mean duration (RoM). We compared binary outcomes using logistic regression, reported as odds ratios (ORs). Analyses of functional outcomes used a linear mixed effects model with random intercepts for site and for patients nested within site, and factors for time and tracheostomy group, after ruling out an interaction between time and tracheostomy. Results are presented as mean differences (MDs). For specialty visits, we used Poisson regression with each patient’s follow-up time as an offset; results are presented as rate ratios. Disposition—a multicategory variable—was analyzed using a log linear model. Survival between 1 week and 12 months after ICU discharge was analyzed using a Cox regression model to account for censoring due to loss to follow-up, with and without adjustment for RECOVER group. Survival over the time period is shown in a Kaplan-Meier plot.
In a sensitivity analysis, we compared baseline demographics and outcomes in tracheostomy versus nontracheostomy patients in all 463 ICU admissions (Groups 1, 2, 3, and 4), regardless of ICU survivorship (Electronic Supplementary Material—ESM, http://links.lww.com/CCX/B74).
For statistical analysis, R 4.1.1 (2021) was used (R Core Team [2021]. R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria, https://www.R-project.org/).
RESULTS
Baseline demographics of 398 ICU survivors are shown in Supplemental Digital Content - Table 1 (http://links.lww.com/CCX/B74); 193 patients (48.5%) underwent tacheostomy insertion in the ICU. The four RECOVER groups were characterized by different age (by study design), a similar sex distribution, and nonsignificantly different admission diagnoses (Supplemental Digital Content - Table 1, http://links.lww.com/CCX/B74).
APACHE II score, MODS on day 7 of MV, and Elixhauser and Charlson scores did not differ between tracheostomy and nontracheostomy patients (Supplemental Digital Content - Table 2, http://links.lww.com/CCX/B74). In all groups, acute respiratory failure was the most common reason for ICU admission. In groups 2, 3, and 4, tracheostomy was performed in 34%, 57%, and 67% of patients, respectively (Supplemental Digital Content - Table 1, http://links.lww.com/CCX/B74), with a median interval from intubation to tracheostomy insertion of 15, 13, and 13 days, respectively (Supplemental Digital Content - Table 3, http://links.lww.com/CCX/B74). The primary reason for tracheostomy was prolonged MV, whereas extubation failure, muscle weakness, and upper airway obstruction were less frequent (Supplemental Digital Content - Table 1, http://links.lww.com/CCX/B74). Patient flow is shown in Supplemental Digital Content - Figure 1 (http://links.lww.com/CCX/B74).
Outcomes in ICU and Hospital
The duration of MV was significantly longer in tracheostomy patients (Supplemental Digital Content - Table 3, http://links.lww.com/CCX/B74) (RoM, 1.9; 95% CI, 1.7–2.1). ICU and hospital LOS were significantly longer in tracheostomy patients (RoM 1.8 for both). FIM on day 7 after ICU discharge was lower in the tracheostomy group, indicating worse functional status, but the difference was not statistically significant (MD, –5.7; 95% CI –11.9 to +0.5; p = 0.07). Corticosteroid administration and use of RRT were similar.
Hospital mortality was higher in the tracheostomy group (OR, 2.6; 95% CI, 1.1–6.1; p = 0.03). Without adjustment for RECOVER group, tracheostomy was associated with worse 1-year survival (hazard ratio [HR], 1.62; 95% CI, 1.0–2.5) (Fig. 1). The adjusted effect was nonsignificant (HR, 1.41; 95% CI, 0.88–1.2).
Figure 1.
Kaplan-Meier curves showing cumulative post-ICU mortality by tracheostomy in RECOVER groups 2–4. Numbers at risk for the tracheostomy and nontracheostomy groups are shown beneath the figure. The unadjusted hazard ratio comparing those with and without tracheostomy is 1.6 (95% CI, 1.0–2.5; p = 0.04). After adjusting for RECOVER group, the hazard ratio comparing those with and without tracheostomy is 1.4 (95% CI, 0.9–2.2; p = 0.15).
Healthcare Utilization
Over 1 year of follow-up, ICU readmission was more common in tracheostomy patients (p = 0.04), but hospital readmissions were similar (p = 0.38) (Table 1). Tracheostomy patients were less likely to be discharged home from hospital (p = 0.01), but there was no significant difference in overall disposition at 1 year (p = 0.11). Outpatient specialty visits were similar (p = 0.37) (Table 1; and Supplemental Digital Content - Table 4, http://links.lww.com/CCX/B74).
TABLE 1.
Healthcare Utilization for Tracheostomy and Nontracheostomy Patients in the Three RECOVER Groups
| Group 2 | Group 3 | Group 4 | p for Tracheostomy | ||||
|---|---|---|---|---|---|---|---|
| Variables | No Tracheostomy, N = 91 | Tracheostomy, N = 47 | No Tracheostomy, N = 62 | Tracheostomy, N = 82 | No Tracheostomy, N = 31 | Tracheostomy, N = 62 | |
| Disposition at hospital discharge, n (%) | 0.01 | ||||||
| Dead | 2 (2) | 4 (9) | 4 (6) | 9 (11) | 2 (6) | 11 (18) | |
| Home | 45 (49) | 12 (26) | 17 (27) | 26 (32) | 9 (29) | 6 (10) | |
| Other hospital | 17 (19) | 16 (34) | 24 (39) | 20 (24) | 10 (32) | 24 (39) | |
| Rehabilitation | 27 (30) | 15 (32) | 17 (27) | 27 (33) | 10 (32) | 21 (34) | |
| Disposition at 1 yr, n (%) | 0.11 | ||||||
| Dead | 12 (13) | 9 (19) | 12 (19) | 15 (18) | 7 (23) | 25 (40) | |
| Home | 56 (62) | 21 (45) | 32 (52) | 39 (48) | 16 (52) | 18 (29) | |
| Other | 5 (5) | 8 (17) | 10 (16) | 8 (10) | 3 (10) | 9 (15) | |
| Unknown | 18 (20) | 9 (19) | 8 (13) | 20 (24) | 5 (16) | 10 (16) | |
| ICU readmission within index hospitalization, n (%) | 8 (9) | 7 (15) | 8 (13) | 18 (22) | 7 (23) | 20 (32) | 0.04 |
| Hospital readmission within 1 yr, n (%) | 44 (48) | 17 (36) | 26 (42) | 33 (40) | 11 (35) | 23 (37) | 0.38 |
| Any outpatient specialist visit within 1 yr, n (rate per 100 person-years) | 346 (401) | 112 (261) | 172 (304) | 251 (337) | 93 (350) | 123 (271) | 0.37 |
Data are presented as n (%) or n (rate per 100 person years). Group 2—mid age variable length of stay (LOS) (≥ 42 yr, < 2 wk in ICU and ≤ 45 yr, ≥ 2 wk in ICU); Group 3—older long LOS (46–66 yr, ≥ 2 wk in ICU); Group 4—oldest long LOS; (> 66 yr, ≥ 2 wk in ICU).
Functional and Neuropsychologic Outcomes
In linear mixed effects models adjusting for RECOVER group, tracheostomy patients had, on average across all time points, lower FIM Motor Subscale (by 7.8 points, 95% CI, 3.8–11.9; p = 0.0002) and FIM Total Scores (by 9.4 points 95% CI, 4.3–14.5; p = 0.0004) (Fig. 2). The mean FIM cognitive subscale was similar (lower in tracheostomy patients by 1.4 point; 95% CI 0.2 higher to 3.0 lower).
Figure 2.
Mean Functional Independence Measure (FIM) in RECOVER groups 2–4. From left to right: FIM Cognitive Subscale, FIM Motor Subscale, and FIM Total Score. In linear mixed effects models adjusting for RECOVER group, tracheostomy patients had on average, across all time points, lower FIM Motor Subscale (by 6.5 points, 95% CI, 2.3–10.8; p = 0.003) and FIM Total Scores (by 7.7 points 95% CI, 2.2–13.2; p = 0.006) than nontracheostomy patients.
Over months 3–12, mean SF36-PCS (1 point lower in tracheostomy group), MCS (0.8 points lower in tracheostomy group), BDI (1.1 points higher in tracheostomy group), and IES (3.6 points higher in tracheostomy group) were not significantly different. However, MRC (3.4 points lower; 95% CI, 1.0–5.8) and percent predicted 6MWT (12% lower; 95% CI, 5–19%) were significantly lower in tracheostomy patients (Fig. 3).
Figure 3.
Functional and neuropsychologic outcomes in RECOVER groups 2–4. Adjusted for RECOVER groups, from 3 mo onwards, those who had a tracheostomy had a 10% lower percent predicted 6-min walk test with continuous oximetry (6MWT) distance (p = 0.004) and a lower Medical Research Council (MRC) score (2.6 points; p = 0.04). The tracheostomy patients exhibited only small decrements in SF36-PCS (1 point; p = 0.45), SF-36-MCS (0.7 points; p = 0.67), IES (1.2 points; p = 0.66) and BDI (0.8 points; p = 0.51) with adjustment for RECOVER groups. BDI = Beck Depression Inventory-II, IES = Impact of Event Scale, PCS and MCS = Physical and Mental Component Summary scores of the Health Related Quality of Life (Medical Outcome Study Short Form-36 Questionnaire, SF-36).
Pulmonary Function Tests
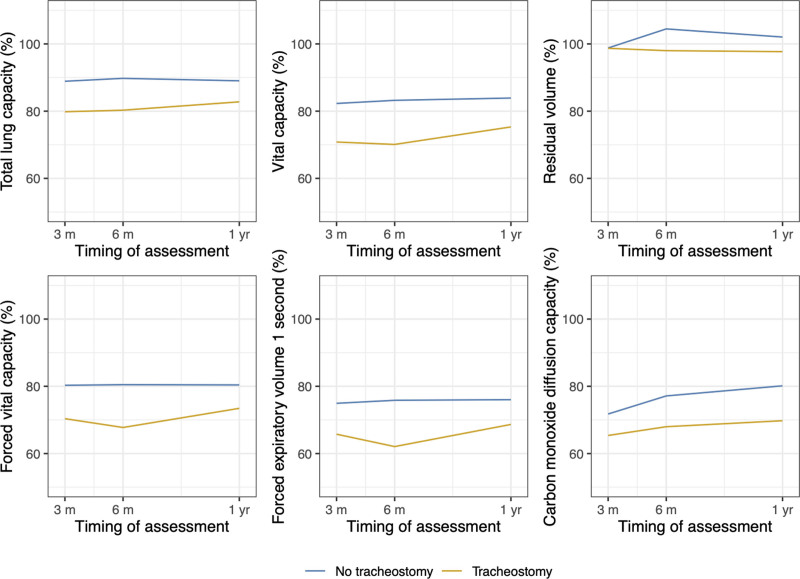
Tracheostomy patients had worse PFTs (except for residual volume) from 3 to 12 months post ICU discharge (Fig. 4), with significantly lower percent predicted values for total lung capacity (6.4%; 95% CI, 1.6–11.2%), vital capacity (8.0%; 95% CI, 2.2–13.9%), forced vital capacity (7.6%; 95% CI, 2.2–13.0%), forced expiratory volume 1 second (7.9%; 95% CI, 2.4–13.4%), and carbon monoxide lung diffusion (5.1%; 95% CI, 0–10.5%).
Figure 4.
Pulmonary function tests in RECOVER groups 2–4 (%). Mean percent predicted values on pulmonary function tests in RECOVER groups 2–4 were significantly reduced in tracheostomy patients compared with nontracheostomy patients by an amount that did not vary appreciably with time since ICU discharge for: total lung capacity (6.4%; 95% CI, 1.6–11.2%), vital capacity (8.3%; 95% CI, 2.5–14.1%), forced vital capacity (7.6%; 95% CI, 2.3–13.0%), forced expiratory volume 1 s (7.9%; 95% CI, 2.4–13.4%), and percent carbon monoxide lung diffusion (7.5%; 95% CI, 1.7–13.4%). Percent residual volume was also lower (4.6%; 95% CI, –4.5% to 13.6%) in tracheostomy patients, but the CIs were wide.
Tracheostomy Outcomes in the Entire RECOVER Cohort
Considering all patients in RECOVER (n = 463, Groups 1, 2, 3, and 4, regardless of ICU survivorship) tracheostomy versus nontracheostomy patients were older, had higher MODS on day 1, and had lower FIM on day 7 (Supplemental Digital Content - Table 2, http://links.lww.com/CCX/B74). Tracheostomy patients had significantly longer MV days and ICU and hospital stays. MV days and ICU stay and hospital stay were twice as long in tracheostomy patients. Although ICU mortality was similar, hospital mortality was significantly higher in tracheostomy patients (10.7% vs 4.2%; p = 0.012). Orders for limitations of care were similar but were instituted significantly later in tracheostomy patients. For example, a no cardiopulmonary resuscitation (CPR) order was placed on median MV day 31 for tracheostomy patients versus day 12 for nontracheostomy patients (p < 0.001).
Tracheostomy patients had more ICU readmissions during the index hospital admission (20.5% vs 11.7%; p = 0.014). Tracheostomy patients were less likely to be discharged home (p < 0.001) and less likely to be at home at 1 year (p = 0.029).
DISCUSSION
In this population of ICU survivors greater than or equal to 42 years old and mechanically ventilated greater than or equal to 1 week, patients who received a tracheostomy had longer durations of MV, ICU and hospital LOS, more ICU readmissions, and higher hospital mortality. In follow-up, patients who received a tracheostomy had worse pulmonary function and 6MWT. Although they had a higher daily burden of care, expressed by the total FIM score, the clinically meaningful difference in FIM is not known in this population, in contrast to patients with stroke (12). Survival at 1 year was similar; however, patients with tracheostomy were less likely to be at home.
Our results do not prove a causal relationship between tracheostomy and worse outcomes; rather, it is far more likely that the need for tracheostomy after prolonged MV and a long ICU stay is a marker of a more complex course during and following critical illness. Nevertheless, information regarding discharge disposition, independent living, and psychologic health is vital when patients and family members make decisions about ongoing ICU support, including tracheostomy.
Decisions about tracheostomy in patients anticipated to require prolonged MV are motivated by ease of weaning, patient comfort, reduced sedation needs, oral hygiene, and reduced laryngeal trauma (13, 14). However, published data do not support more rapid liberation from MV or reductions in ventilator-associated pneumonia or ICU or hospital LOS. Conversely, insertion of a tracheostomy may be associated with procedural risks, long-term consequences including psychologic and physical distress (15), impaired quality of life (16, 17), and implications for discharge disposition (13), particularly in older patients (18). In the absence of guidelines, as well as financial and disposition motivations for early tracheostomy in some countries, there exists tremendous variability in timing and patient selection (19, 20, 21).
Studies evaluating the timing of tracheostomy show that early tracheostomy has no advantages, and delaying tracheostomy insertion is associated with fewer procedures (4, 22). Observational studies showing that tracheostomy versus no tracheostomy is associated with more rapid weaning from MV and lower hospital mortality are limited by selection bias and immortal time bias (23, 24). Further, tracheostomy does not improve long-term survival and is associated with worse outcomes after ICU discharge, particularly in older adults (25). In a study of 270 patients greater than 70 years old who received an elective tracheostomy in one of two University of Toronto ICUs, we found that 54% survived to hospital discharge; however, only 6% were discharged home, all were frail (median clinical frailty scale 7), and most were tube-fed (70%), unable to speak (56%), and nonambulatory (68%) (26). Similar to our results, Morris et al (27) reported that patients who received a tracheostomy were four times more likely to be readmitted or die in the first year post index hospitalization. Mehta et al (20) also reported poor outcomes of 8,343 nonsurgical patients who received a tracheostomy for acute respiratory failure, with high risk of mortality at 1 year and hospital readmission, especially in older patients. In a study of trauma survivors, ICU LOS greater than or equal to 5 days and tracheostomy were significantly associated with limitations in return to usual major activities at 12 months (28).
In our cohort, longer durations of MV and LOS, higher hospital mortality, and worse PFTs in patients who received tracheostomy likely reflect their greater severity of illness and postintensive care syndrome, rather than being causally related to the tracheostomy procedure. Nonetheless, having a tracheostomy was associated with worse functional status and higher daily burden of care, and a lower likelihood of being at home at 1 year. The Large observational study to UNderstand the Global impact of Severe Acute respiratory FailurE population may be similar to the RECOVER study population (21): 309 of 2,377 patients (13%) underwent tracheostomy during the ICU stay, at a median delay of 14 days after the onset of acute respiratory distress syndrome. In the subsample matched by propensity score, ICU and hospital stay were longer in patients with a tracheostomy. Although tracheostomy appeared to prolong short term survival (i.e., lower 28-d mortality), it did not improve 60-day or 90-day mortality, suggesting that tracheostomy may delay death. Similarly, we found that tracheostomy insertion led to delayed decisions regarding foregoing CPR and reintubation, by approximately 2 weeks. Whether this delay was related to clinicians (29) or family members deferring goals of care discussions or wishing to observe clinical progression for a longer period of time is not clear. In patients for whom long-term limitations in functional status would not be acceptable, our data would support not performing tracheostomy.
The strengths of our study are the multicenter prospective design, evaluation of the highest risk ICU survivors who required MV for greater than or equal to 1 week, and the long-term functional and quality of life follow-up. Limitations include the lack of data on tracheostomy technique (percutaneous or surgical), the impact on comfort, sedation needs, swallowing, phonation, and cosmesis, as well as decannulation rates and timing. Conclusions about 1 year disposition are weakened by disposition being unknown for almost 20% of patients. Furthermore, patient and family perspectives regarding tracheostomy are missing. The comparison of tracheostomy and nontracheostomy patients is almost certainly confounded by indication bias, given that tracheostomy is usually performed in patients who are clinically stable and predicted to need prolonged MV, as well as immortal time bias (patients who die early are less likely to receive tracheostomy) (21). We lack data regarding interventions and processes of care in the ICU, such as sedation, analgesia, delirium, and mobilization, which may contribute to patient outcomes. Our data may not be applicable to patients who receive tracheostomy for a neurologic disease.
CONCLUSIONS
In this secondary analysis of the highest risk patients enrolled in the Towards RECOVER study, all of whom were ventilated for greater than or equal to 1 week and survived to ICU discharge, tracheostomy was associated with worse long-term outcomes. Given that the use of tracheostomy in patients with acute respiratory failure had risen dramatically in the United States in the past 2 decades (20), it is vital to understand the patient-centered consequences of tracheostomy to inform shared decision-making regarding this procedure. Future studies should evaluate decannulation rates, particularly in elderly patients, as well as long-term consequences of tracheostomy in homogeneous populations on dysphagia, cosmesis, and the patient and family experience.
Supplementary Material
Footnotes
Supplemental digital content is available for this article. Direct URL citations appear in the printed text and are provided in the HTML and PDF versions of this article on the journal’s website (http://journals.lww.com/ccejournal).
The Towards RECOVER study was supported, in part, by Canadian Institutes of Health Research, Ontario Ministry of Health Innovation Fund; the University of Toronto—Department of Medicine Challenge Integration Fund; the John and Gail MacNaughton Family Fund; and the Jason Tham and Andrea Chan Family Fund, and the Don and Jane Luck Family Fund.
The authors have disclosed that they do not have any potential conflicts of interest.
Clinical trial registered with www.clinicaltrials.gov NCT 00896220.
REFERENCES
- 1.Siempos II, Ntaidou TK, Filippidis FT, et al. : Effect of early versus late or no tracheostomy on mortality and pneumonia of critically ill patients receiving mechanical ventilation: A systematic review and meta-analysis. Lancet Respir Med 2015; 3:150–158 [DOI] [PubMed] [Google Scholar]
- 2.Scales DC: What’s new with tracheostomy? Intensive Care Med 2013; 39:1005–1008 [DOI] [PubMed] [Google Scholar]
- 3.Trouillet JL, Luyt CE, Guiguet M, et al. : Early percutaneous tracheotomy versus prolonged intubation of mechanically ventilated patients after cardiac surgery: A randomized trial. Ann Intern Med 2011; 154:373–383 [DOI] [PubMed] [Google Scholar]
- 4.Young D, Harrison DA, Cuthbertson BH, et al. ; TracMan Collaborators: Effect of early vs late tracheostomy placement on survival in patients receiving mechanical ventilation: The TracMan randomized trial. JAMA 2013; 309:2121–2129 [DOI] [PubMed] [Google Scholar]
- 5.Herridge MS, Chu LM, Matte A, et al. ; RECOVER Program Investigators (Phase 1: TOWARDs RECOVER); Canadian Critical Care Trials Group: The RECOVER program: Disability risk groups and 1-year outcome after 7 or more days of mechanical ventilation. Am J Respir Crit Care Med 2016; 194:831–844 [DOI] [PubMed] [Google Scholar]
- 6.Koyama T, Matsumoto K, Okuno T, et al. : Relationships between independence level of single motor-FIM items and FIM-motor scores in patients with hemiplegia after stroke: An ordinal logistic modelling study. J Rehabil Med 2006; 38:280–286 [DOI] [PubMed] [Google Scholar]
- 7.Enright PL, Sherrill DL: Reference equations for the six-minute walk in healthy adults. Am J Respir Crit Care Med 1998; 158:1384–1387 [DOI] [PubMed] [Google Scholar]
- 8.Medical Research Council: Aids to the Examination of the Peripheral Nervous System. Memorandum No 45. London, United Kingdom, HMSO, 1976 [Google Scholar]
- 9.Ware JEJ, Kosinski M, Gandek B: SF-36 Health Survey: Manual and Interpretation Guide. Lincoln, RI, QuantityMetric Inc., 2002 [Google Scholar]
- 10.Horowitz M, Wilner N, Alvarez W: Impact of event scale: A measure of subjective stress. Psychosom Med 1979; 41:209–218 [DOI] [PubMed] [Google Scholar]
- 11.Richter P, Werner J, Heerlein A, et al. : On the validity of the beck depression inventory. A review. Psychopathology 1998; 31:160–168 [DOI] [PubMed] [Google Scholar]
- 12.Beninato M, Gill-Body KM, Salles S, et al. : Determination of the minimal clinically important difference in the FIM instrument in patients with stroke. Arch Phys Med Rehabil 2006; 87:32–39 [DOI] [PubMed] [Google Scholar]
- 13.Jacob G, Jakab M, Ray J: Characteristics and outcomes of patients who underwent bedside surgical tracheostomy performed in the intensive care unit: A retrospective study. Can J Anaesth 2018; 65:327–328 [DOI] [PubMed] [Google Scholar]
- 14.Rumbak MJ, Newton M, Truncale T, et al. : A prospective, randomized, study comparing early percutaneous dilational tracheotomy to prolonged translaryngeal intubation (delayed tracheotomy) in critically ill medical patients. Crit Care Med 2004; 32:1689–1694 [DOI] [PubMed] [Google Scholar]
- 15.Sherlock ZV, Wilson JA, Exley C: Tracheostomy in the acute setting: Patient experience and information needs. J Crit Care 2009; 24:501–507 [DOI] [PubMed] [Google Scholar]
- 16.Vargas M, Sutherasan Y, Brunetti I, et al. : Mortality and long-term quality of life after percutaneous tracheotomy in intensive care unit: A prospective observational study. Minerva Anestesiol 2018; 84:1024–1031 [DOI] [PubMed] [Google Scholar]
- 17.Antonelli M, Michetti V, Di Palma A, et al. : Percutaneous translaryngeal versus surgical tracheostomy: A randomized trial with 1-yr double-blind follow-up. Crit Care Med 2005; 33:1015–1020 [DOI] [PubMed] [Google Scholar]
- 18.Mehta AB, Walkey AJ, Curran-Everett D, et al. : One-year outcomes following tracheostomy for acute respiratory failure. Crit Care Med 2019; 47:1572–1581 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Vargas M, Sutherasan Y, Antonelli M, et al. : Tracheostomy procedures in the intensive care unit: An international survey. Crit Care 2015; 19:291. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Mehta AB, Cooke CR, Wiener RS, et al. : Hospital variation in early tracheostomy in the United States: A population-based study. Crit Care Med 2016; 44:1506–1514 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Abe T, Madotto F, Pham T, et al. ; LUNG-SAFE Investigators and the ESICM Trials Group: Epidemiology and patterns of tracheostomy practice in patients with acute respiratory distress syndrome in ICUs across 50 countries. Crit Care 2018; 22:195. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Terragni PP, Antonelli M, Fumagalli R, et al. : Early vs late tracheotomy for prevention of pneumonia in mechanically ventilated adult ICU patients: A randomized controlled trial. JAMA 2010; 303:1483–1489 [DOI] [PubMed] [Google Scholar]
- 23.Lin WC, Chen CW, Wang JD, et al. : Is tracheostomy a better choice than translaryngeal intubation for critically ill patients requiring mechanical ventilation for more than 14 days? A comparison of short-term outcomes. BMC Anesthesiol 2015; 15:181. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Combes A, Luyt CE, Nieszkowska A, et al. : Is tracheostomy associated with better outcomes for patients requiring long-term mechanical ventilation? Crit Care Med 2007; 35:802–807 [DOI] [PubMed] [Google Scholar]
- 25.Engoren M, Arslanian-Engoren C, Fenn-Buderer N: Hospital and long-term outcome after tracheostomy for respiratory failure. Chest 2004; 125:220–227 [DOI] [PubMed] [Google Scholar]
- 26.Lee T, Li Tan Q, Sinuff T, et al. : Outcomes of prolonged mechanical ventilation and tracheostomy in critically ill elderly patients: A historical cohort study. Can J Anesth/J Can Anesth 2022; 69:1107–1116 [DOI] [PubMed] [Google Scholar]
- 27.Morris PE, Griffin L, Berry M, et al. : Receiving early mobility during an intensive care unit admission is a predictor of improved outcomes in acute respiratory failure. Am J Med Sci 2011; 341:373–377 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Davydow DS, Zatzick DF, Rivara FP, et al. : Predictors of posttraumatic stress disorder and return to usual major activity in traumatically injured intensive care unit survivors. Gen Hosp Psychiatry 2009; 31:428–435 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Kruser JM, Benjamin BT, Gordon EJ, et al. : Patient and family engagement during treatment decisions in an ICU: A discourse analysis of the electronic health record. Crit Care Med 2019; 47:784–791 [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.