Abstract
Background
The detection of the first cases of transfusion-transmitted West Nile virus in 2002 posed a new challenge for transfusion safety. Institutions like the World Health Organization have stated that blood transfusion centers need to know the epidemiology of the different emerging infectious agents and their impact on blood transfusion. The aim of the study is to review the published cases of arbovirus transmission through transfusion of blood or blood components and to analyze their main clinical and epidemiological characteristics.
Material and methods
Systematic literature searches were conducted in MEDLINE, Embase and Scopus. Pairs of review authors selected a variety of scientific publications reporting cases of transfusion-transmitted arboviruses. Main clinical and epidemiological characteristics were reviewed of the cases described. The study protocol was registered in PROSPERO CRD42021270355.
Results
A total of 74 cases of transfusion-transmitted infections were identified from 10 arboviruses: West Nile virus (n = 42), dengue virus (n = 18), Zika virus (n = 3), yellow fever vaccine virus (n = 3), tick-borne encephalitis virus (n = 2), Japanese encephalitis virus (n = 2), Powassan virus (n = 1), St. Louis encephalitis virus (n = 1), Ross River virus (n = 1) and Colorado tick fever virus (n = 1). The blood component most commonly involved was red blood cells (N = 35, 47.3%; 95% confidence interval [CI] 35.9% to 58.7%). In 54.1% (N = 40; 95% CI: 42.7%-65.47%) of the cases, the recipient was immunosuppressed. Transmission resulted in death in 18.9% (N = 14; 95% CI: 10.0%-27.8%) of the recipients. In addition, 18 additional arboviruses were identified with a potential threat to transfusion safety.
Discussion
In the last 20 years, the number of published cases of transfusion-transmitted arboviruses increased notably, implicating new arboviruses. In addition, a significant number of arboviruses that may pose a threat to transfusion safety were detected. In the coming years, it is expected that transmission of arboviruses will continue to expand globally. It is therefore essential that all responsible agencies prepare for this potential threat to transfusion safety.
Author summary
The transfusion of blood and blood components entails some risks and potential complications, chief among them the transmission of infectious agents. Organizations like the American Association of Blood Banks have warned of the risks posed by emerging and re-emerging viruses for transfusion safety and have classified transmission of several arboviruses as a high or very high risk to the transfusion of blood and blood components. Following recommendations by the World Health Organization (WHO), this study aims to enable safe blood transfusion services, by making available the latest updated information of transfusion-transmitted arboviruses and comprehensive knowledge of the current epidemiology of reported cases.
Research revealed case reports of transfusion transmission of 10 arboviruses, with West Nile virus and dengue virus as the most prevalent. Main clinical characteristics of reported cases were collected, including the type of blood component transfused and the state of immunosuppression of the recipient. Research also revealed 18 additional arboviruses with potential risk of transmission through other direct transmission routes. This systematic review provides an updated overview of the clinical characteristics of reported cases of transfusion-transmitted arboviruses. It is the most complete record published to date that assesses the risk posed by arboviruses to blood transfusion.
Background
Throughout history, transfusion safety has been threatened by the emergence of various infectious agents [1]. Currently, health service consumers expect a total absence of transfusion-related transmission of infectious diseases. However, the 2002 notification of the first cases of West Nile virus transmission through transfusion of blood components, highlighted the threat posed to transfusion safety by emerging and re-emerging infectious agents [2,3].
Among the emerging viruses, arboviruses are especially relevant due to their known or theoretical potential for transmission through blood transfusion. These viruses are transmitted by arthropods, mainly mosquitoes (genera Culex spp. and Aedes spp.) and ticks (particularly the genus Ixodes) but also flies, dragonflies, and lice. In humans, they can cause clinical presentations ranging from asymptomatic infections or mild flu-like symptoms, to severe, potentially fatal hemorrhagic and neurological syndromes. Their epidemiology is highly variable and unpredictable and may manifest as isolated and localized cases; seasonal waves; or widespread, epidemic outbreaks. Originally from tropical regions, arboviruses have now spread widely, producing numerous epidemic outbreaks over the past 20 years and constituting a major public health problem all over the planet. Arboviruses are classified into different taxonomic families: Flaviviridae, Bunyaviridae, Togaviridae, Rhabdoviridae, Reoviridae, and Asfarviridae. The most important arboviruses that cause disease in humans belong to the families Flaviviridae, Togaviridae and Bunyaviridae [4].
Threats to transfusion safety arising from new infectious agents have traditionally been addressed through the development of methods to screen blood donors, and this also holds true for arboviruses. Screening methods used include serological and non-serological antigen rapid testing techniques as well as nucleic acid (PCR) tests. These tests may be used routinely or according to the epidemiological profile of the areas or countries in question. However, they may not be sufficient to fully guarantee transfusion safety in the case of donors with a very low viral load and/or who are in the window period after infection [5].
In recent years, various international organizations have created tools to assess the transfusion risk posed by these newly emerging and re-emerging infectious agents. In 2009, the AABB Transfusion-Transmitted Diseases Committee, in collaboration with members of the Food and Drug Administration (FDA), the Centers for Disease Control and Prevention (CDC), and other agencies, developed guidance to identify infectious agents that could pose a real or potential risk to transfusion safety. In this process, 68 infectious agents, including arboviruses, were classified according to their epidemiological profile and the public’s awareness and perception of them. Of the arboviruses in this classification, dengue virus was assigned in the highest risk category, while chikungunya and St. Louis encephalitis viruses were included in the second-highest risk category [6]. In 2011, fact sheets were developed for miscellaneous arboviruses, including for yellow fever virus and yellow fever vaccine virus [7]. Various infectious agents were also classified in 2011 by the European Center for Disease Prevention and Control (ECDC) based on the epidemiological and environmental characteristics of these viruses in Europe. The agents given the highest priority include a number of arboviruses: West Nile virus, dengue virus, chikungunya virus and tick-borne encephalitis virus [8]. In Asia, the WHO also published the Asia Pacific Strategy for Emerging Diseases and Public Health Emergencies (APSED III) in 2017 with the aim of detecting and addressing the different emerging infectious diseases in the region [9].
With the development of these risk assessment tools, major global public health entities have expressed the need for comprehensive knowledge of the epidemiological characteristics of the various emerging transfusion-transmitted infections and to evaluate their potential impact on donor selection criteria and the supply of blood and blood products [10].
The main objective of this study is, therefore, to review the published cases of arbovirus transmission through the transfusion of blood or blood components throughout the history of transfusion and to study their main clinical and epidemiological characteristics. For the research question in PICOT format, please see (S1 Table). The secondary objective is to, additionally, identify arboviruses that can be a threat to transfusion safety through other non-vector, non blood transfusion related direct routes of transmission such as: organ and/or hematopoietic stem cell transplantation, mother-to-child transmission, direct blood contact or by their prevalence in blood donors.
Materials and methods
Design
This systematic literature review was designed and conducted in accordance with the Cochrane Handbook of Systematic Reviews of Interventions and reported in line with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) Statement [11]. For the PRISMA checklist, please see the (S1 PRISMA Checklist). The protocol for this systematic review was published and registered in PROSPERO (www.crd.york.ac.uk/prospero, CRD42021270355).
First, a global descriptive analysis was completed including all cases of transfusion-transmitted arboviruses. Consequently, a brief study was conducted of the main clinical and epidemiological characteristics of reported cases of arboviral transfusion transmission. After a general analysis that included all cases, we specifically analyzed the arboviruses with the most reported cases of transmission through blood transfusion or blood components: West Nile virus and dengue virus. Finally, a descriptive analysis was performed of arboviruses that can be considered a potential threat to transfusion safety, based on published reports of any non-vector, non-blood related direct route of transmission or because of their prevalence in blood donors, regardless of reported evidence of transfusion transmission.
Source of data collection
Systematic literature searches were conducted in MEDLINE, Embase, Scopus using the server of University Miguel Hernández server.
Search strategy
The complete search strategy is described in more detail in the study protocol and (S1 Text). Initially, the authors have performed searches with free text terms in all three bibliographic databases using the term "transfusion" in combination with the name of the arboviruses being reviewed. In MEDLINE, Medical Subject Headings (MeSH) such as “Blood Transfusion”[Mesh] OR “Transfusion Reaction”[Mesh] also served as search terms. In Embase the Entree thesaurus was used to search articles based on the following terms: “blood transfusion”/exp.
As a second search strategy, free text searches were performed in MEDLINE using the terms: “transplantation”, “vertical transmission”, “blood donors”, while in Embase a free text search was conducted by entering the following terms in the Entree Thesaurus: “transplantation”/exp OR transplantation, “vertical transmission”/exp OR “vertical transmission” AND “blood donor”/exp OR “blood donor”. In Scopus, we ran searches only using free text terms in the fields for title, abstract, and key words. Bibliographies of all included records to identify other potentially relevant publications were also hand-searched.
The authors included records published from the year of inception of each bibliographic database (start date—we did not apply any specific limits to the start date) to 10 November 2021 (end date). The records were entered into the Mendeley Desktop reference manager (Elsevier).
Study selection
In answer to the primary objective, selected publications were those in any language describing cases of transfusion-transmitted arboviruses transmitted through transfusion of blood or blood components. A wide variety of scientific studies (original articles, reviews, brief reports, case reports, letters to the editor, conference papers and others) were included reporting cases of arboviruses transmitted through transfusion of blood or blood components. Publications that collected cases of transmission in non-humans were excluded, as were publications that did not detail the specific type of arbovirus transmitted through the transfusion of blood or blood components.
Search records were independently evaluated by two review authors for inclusion in the publication overview. Any discrepancies were resolved by consensus. Inter-observer agreement was measured by determining the kappa index.
The bibliographic reference manager Mendeley Desktop was used to create folders containing records for each virus, eliminating duplicates. Titles and abstracts were screened to pre-select records in any language that included general information on the possible transmission of arboviruses through the transfusion of blood or blood components. Consequently, full texts of all potentially relevant records were reviewed independently by two researchers. Records included, were those that reported cases of transfusion transmission of blood or blood components in humans over the entire period under study.
To answer to the secondary objective, publications in any language were first selected, describing cases stemming from direct non-vector or transfusion related routes of arbovirus transmission (e.g.: organ and/or hematopoietic stem cell transplantation, mother-to-child transmission, direct blood contact) or reports of prevalence of these arboviruses in blood donors. Consequently, a wide variety of records (original articles, reviews, brief reports, case reports, letters to the editor, conference papers and others) were included to accommodate this review. Lastly, for each encountered route of transmission and each arbovirus found prevalent in blood donors, one publication was selected for the produced publication overview, representing the routes of transmission or evidence of prevalence in screened blood donors. Representative publications were selected based on the following criteria: most recent date of publication, most cited publication, or publication in a journal with the highest impact factor. This evaluation was independently done by two review authors. Final selection for inclusion in the publication overview was determined by consensus. Inter-observer agreement was measured by determining the kappa index.
Data extraction and analysis
All data of cases of transfusion-transmitted arboviruses were extracted from the selected publications and directly entered into a Microsoft Excel database by a single review author. Data quality control was consequently done by a second review author. If a publication included more than one case of transfusion transmission, each case was recorded and entered separately in the database. Basic epidemiological and clinical data of the reported cases of transfusion transmission were then analyzed: type of blood component implicated, immunosuppression and clinical presentation in the recipient, fatality of the outcome following transmission as well as the plausibility of the respective transmission route. From the selected publications, study authors conclusions on transfusion transmission and mortality, attributable to the arboviral infection, were recorded. Determinants of potential alternative routes of transmission were additionally collected such as: exposure to the vector, prolonged hospital stay, additional patients infected by the same contaminated donated product or whether the authors themselves ruled out other potential explanations for the patient’s infection.
Results were expressed as proportion with a 95% confidence interval (95% CI). The proportion was calculated as the number of the reported parameter under study divided by the total number of reported cases of transfusion transmission (Example: number of cases of transfusion-transmitted arboviruses related with the transfusion of red blood cells / total number of cases of transfusion-transmitted arboviruses x 100). The 95% CIs were for proportions (p±Zα/2√(p(1-p)/n)).
Quality assessment
Due to the mainly descriptive objective of this study and the type of publications included (case reports, letters to the editor), no standard quality control tool, such as ROBINS-I or STROBE checklist, was applied for assessing risk of bias in non-randomized studies.
Results
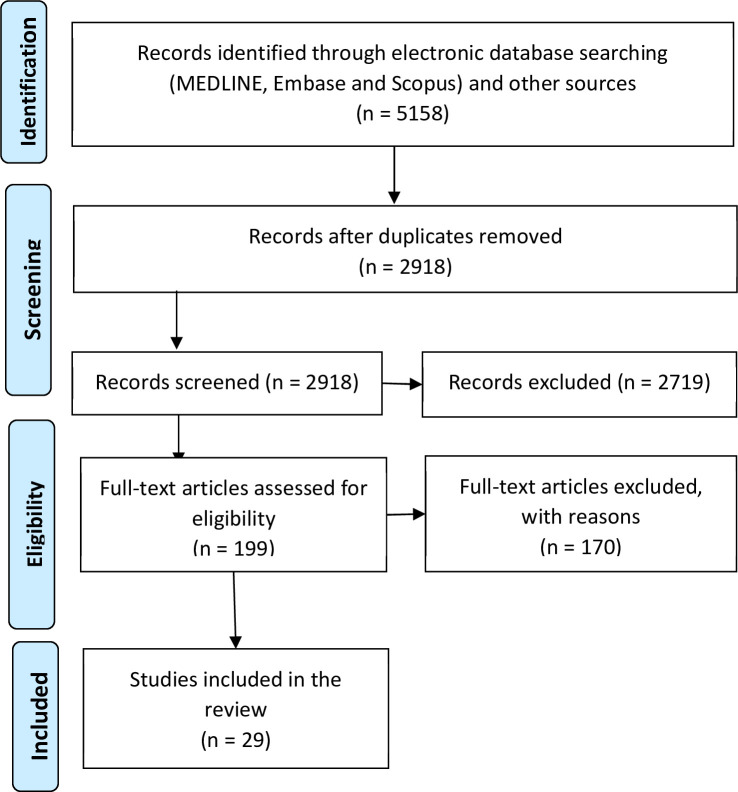
The search strategy yielded a total of 5158 records. After eliminating duplicates, the authors screened the title and abstract of 2918 records and retrieved the full text of 199. The authors selected any records that suggest human transmission of arboviruses through blood transfusion or studies that display information that could facilitate the identification of other publications that report cases of transfusional transmission of arboviruses. Finally, 29 studies reporting cases of human transmission of arboviruses through transfusion of blood or blood components were included. Fig 1 presents the PRISMA flow chart, describing the selection process for including published studies of transfusion-transmitted arboviruses.
Fig 1. PRISMA flow chart on selection of included studies covered by the literature review.
Of the 29 records included, 11 studies described transfusion-transmitted West Nile virus; 9, dengue virus; 2, Zika virus; 1 Japanese encephalitis virus; 1, St. Louis encephalitis virus; 1, tick-borne encephalitis virus; 1, Powassan virus; 1, yellow fever virus; 1, Colorado tick fever virus; and 1, Ross River fever virus. Interobserver concordance was very high (κ = 0.97). For the PRISMA flow chart assessing each specific arbovirus, please see the (S1 Flow Chart).
For the PRISMA flow chart with the process of selecting records describing non-vector and non-transfusion related direct routes of transmission of arboviruses and publications reporting the prevalence of arboviruses in blood donors, please see (S2 Flow Chart). A total of 32 records were selected for the publication overview with an interobserver K value of 0.84.
Analysis of results
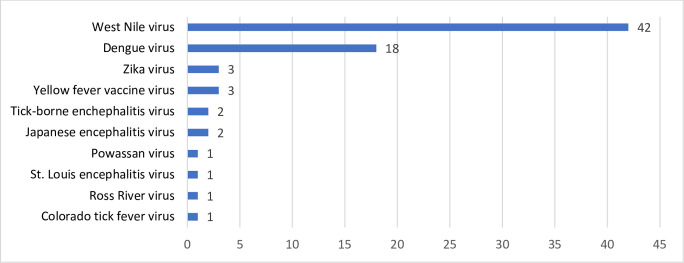
Included studies described 74 cases of suspected transfusion transmission of 10 arboviruses. Most cases involved transfusion transmission of West Nile virus (N = 42, 56.8%; 95% CI: 45.5–68.0%) and dengue virus (N = 18, 24.3%; 95% CI: 14.5–34.1%). Remaining cases described transfusion transmission of Zika virus, yellow Fever vaccine virus, tick-borne encephalitis virus, Japanese encephalitis virus, Powassan virus, St. Louis encephalitis virus, Ross River virus and Colorado tick fever virus (Fig 2).
Fig 2. Reported transfusion-transmitted arbovirus cases.
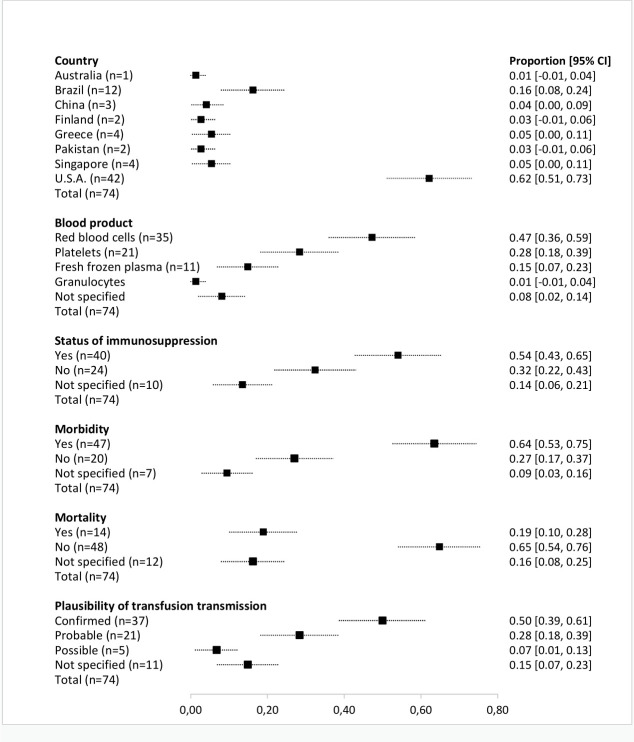
The USA was the country with the most reported cases of transfusion transmission (N = 42, 62%.2%, 95% CI: 51.1–73,2%). The main type of blood component implicated was red blood cells (N = 35, 47.3%; 95% CI: 35.9–58.7%).
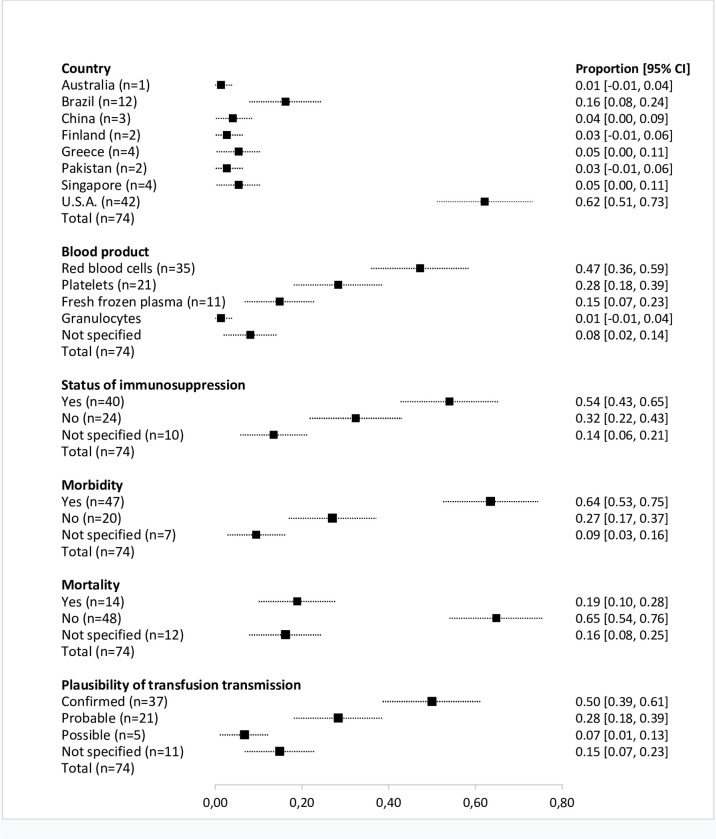
Over half of the reported transfusion-transmitted arbovirus cases, selected for the overview, were described in recipients classified as immunocompromised (N = 40, 54.1%; 95% CI: 42.7–65.5%). Arboviral morbidity and mortality was reported in 63.5% (N = 47; 95% CI: 52.5–74.5%) and 18.9% (N = 14; 95% CI: 10.0–27.8%) of cases described, respectively. Recipient mortality was mostly reported for the West Nile virus (N = 13; 92.9%; 95% CI: 79.4–100%) and 78.6% (N = 13; 95% CI: 57.1–100%). of fatal cases the recipient was classified as immunocompromised. Plausibility of transfusion-transmission was confirmed by the authors of the selected records in 50.0% (N = 37; 95% CI: 38.6–61.4%) of cases. For the main clinical and epidemiological characteristics of selected cases, see Fig 3.
Fig 3. Main clinical and epidemiological characteristics of reported cases of transfusion-transmitted arboviruses.
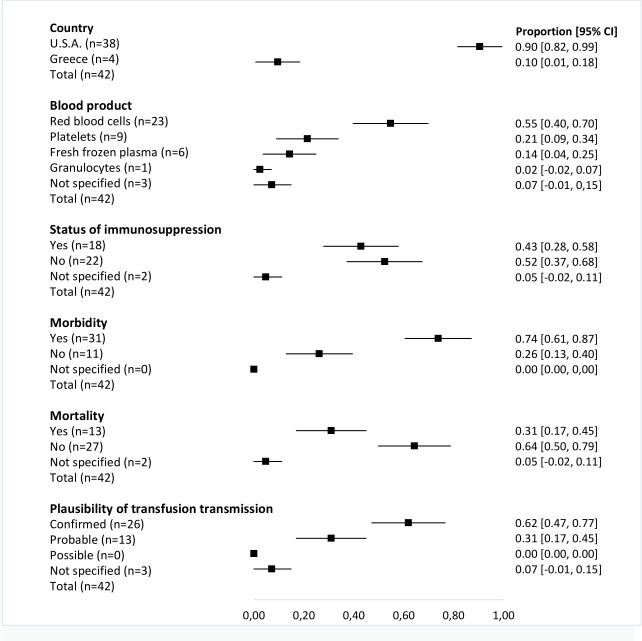
Regarding West Nile virus, 90.5% (N = 38; 95% CI: 81.6–99.4%) of reported cases were diagnosed in the USA, and the main type of blood component implicated was red blood cells 54.8% (N = 23; 95% CI: 39.7–69.8%). Symptoms as a result of transmission were reported in 73.8% (N = 31; 95% CI: 60.5–87.1%) of recipients and in 31.0% (N = 13; 95% CI: 17.0–44.9%) death was reported as the ultimate outcome of transmission. Fig 4 shows the main reported clinical and epidemiological characteristics of cases of West Nile virus transfusion transmission.
Fig 4. Main reported clinical and epidemiological characteristics of transfusion-transmitted West Nile virus.
Of the reported transfusion transmitted cases related to dengue virus, 50% (N = 9; 95% CI: 26.9–73.1%) originated from Brazil. Transfusion of red blood cells was the main route of transmission described (N = 8, 44.4%; 95% CI: 21.5–67.4%). Symptoms were reported for 61.1% (N = 11; 95% CI: 38.6–83.6%) of recipients. None of the selected cases of transfusion transmission of dengue virus were reported as fatal. In 38.9% (N = 7; 95% CI: 16.4–61.4%) of cases, the serotype involved was DENV-4. Fig 5 presents the main reported clinical and epidemiological characteristics of cases of transfusion transmission of dengue virus.
Fig 5. Main reported clinical and epidemiological characteristics of transfusion-transmitted dengue virus.
Tables 1, 2 and 3 provide an overview of the main the main characteristics of reported cases of transfusion-transmitted arboviruses apart from dengue and West Nile virus.
Table 1. Transfusion-transmitted arboviruses cases.
| Virus | Publication | Type of publication | Country | Year | Blood product | Recipient | IC | Morbidity | Mortality | Diagnostic method | Alternative explanation | Other non-vector, non-blood transfusion related transmission | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Exposure to Vector | Prolonged hospital stay | Other infected recipients | Non-vector vias rejected | Plausibility | Additional data | ||||||||||||
| Colorado tick fever virus | Randall 1975 [12] | Case report | U.S.A. | 1975 | Not specified (WB?) | Colon carcinoma | Yes | Yes | No | Clinical Not specified |
No | − | − | − | − | − | Vertical transmission[13] |
| Japanese encephalitis virus | Cheng 2018 [14] | Original article | China | 2017 | RBC | Double lung transplantation | Yes | Yes | Yes | RT-PCR Sanger sequencing Phylogenetic analysis |
N.P. | Yes | Yes | Yes | Confirmed | Same donor No data available about PL recipient |
Screening in blood donors[15] Vertical transmission[12] |
| Platelets | Acute myeloid leukemia | Yes | No | No | Serology IgM | − | − | Yes | − | ||||||||
| Ross River virus | Hoad 2015 [16] | Case reports | Australia | 2014 | RBC | Myelodysplastic syndrome | Yes | No | No | Serology IgM RT-PCR |
N.P. | − | No | − | − | − | Screening in blood donors[17] Vertical transmission[12] |
| St. Louis encephalitis virus | Venkat 2017 [18] | Original article | U.S.A. | 2015 | RBC | Kidney transplant | Yes | Yes | − | Serology IgM+ PRNT |
N.P. | Yes | No | Yes | Possible | No data available about PL recipient. | Screening in blood donors[19] |
| Powassan virus | Taylor 2020 [20] | Original article | U.S.A. | 2018 | RBC | Kidney transplant | Yes | Yes | No | Serology IgM+ PRNT RT-PCR |
No | Yes | No * | Yes | Probable | − | − |
| Tick-borne encephalitis virus | Wahlberg 1989 [21] | Original article | Finland | 1959–1987 | Not specified | Not specified | − | Yes | No | Not specified | N.P. | − | − | − | − | − | Blood contact[22] S.O.T. transmission[23] Screening in blood donors[24] |
| Not specified | Not specified | − | Yes | No | Not specified | N.P. | − | − | − | − | |||||||
| Yellow fever vaccine virus | Lederman 2010 [25] | Original article | U.S.A. | 2009 | Platelets (irradiated) | Wilm’s tumor (relapsed), QMT | Yes | No | No | Serology IgM+ PRNT |
− | − | − | − | − | 2 exposed recipients without evidence of transmission | Screening in blood donors[26] Vertical transmission[12] |
| Platelets | Kidney/liver transplantation, DM | Yes | No | No | − | − | − | − | − | ||||||||
| FFP (2 units) | CKF, TBC, psoriasis (infliximab) | Yes | No | No | − | − | − | − | − | ||||||||
| Zika virus | Barjas-Castro 2016 [27] | Case report | Brazil | 2015 | Platelets (Pool) | Liver transplantation | Yes | No | No | Virus isolation RT-PCR Phylogenetic analysis |
No | No | No * | − | Probable | Blood contact[29] Screening in blood donors[30] Vertical transmission[31] |
|
| Motta 2016 [28] | Letter to the editor | Brazil | 2016 | Platelets (apheresis) | Primary myelofibrosis | Yes | No | No | Serology IgG/IgM+ PRNT RT-PCR Molecular sequencing Phylogenetic analysis |
− | − | Yes | − | Confirmed | Same donor | ||
| Platelets (apheresis) | Acute myeloid leukemia—BMT | Yes | No | No | No | Yes | Yes | − | |||||||||
BMT: bone marrow transplantation, CKD: chronic kidney disease, CTX: chemotherapy, DM: diabetes mellitus, FFP Fresh frozen plasma, NP: not probable, PL: plasma, PRNT Plaque reduction neutralization test, TBC Tuberculosis, RBC red blood cells, IC: Immunocompromised, RT-PCR Reverse transcription polymerase chain reaction, SOT: Solid organ transplantation, ZIKV: Zika virus, RNA: Ribonucleic Acid
− Data not available
* PL not transfused was positive
Table 2. Transfusion-transmitted dengue virus cases.
| Publication | Type of publication | Country | Year | Blood product | Recipient | IC. | Morbidity | Mortality | Diagnostic method | Serotype | Alternative explanation | Plausibility | Additional data | Other non-vector, non-blood transfusion related transmission | |||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Exposure to Vector | Prolonged hospital stay | Other infected recipients | Non-vector vias rejected | ||||||||||||||
| Chuang 2008 [32] | Original article | China | 2002 | RBC | Bronchiectasis, vitamin B12 deficiency anaemia | No | Yes | No | Serology IgM+ HI RT-PCR |
1 | − | − | − | − | Confirmed | ||
| Tambyah 2008 [33] | Letter to the editor | Singapore | 2007 | RBC | DM, ischemic heart disease | Yes | Yes | No | Serology IgG/IgM PCR Sequencing |
2 | − | − | Yes | − | − | Same donor | Blood contact (needle-stick related transmissión) [41] HSCT transmission [42] Screening in blood donors [43] S.O.T. transmission [44] Vertical transmission [45] |
| Platelets | Hepatocellular carcinoma | Yes | No | No | − | − | Yes | − | − | ||||||||
| FFP | DM, hypertension, ischemic heart disease, CRI. | Yes | Yes | No | N.P. | Yes | Yes | − | − | ||||||||
| Boon Oh 2015 [34] | Case report | Singapore | Not specified, 2014? | RBC | Gastrointestinal bleeding. | No | Yes | No | Serology IgG/IgM RT-PCR Sanger sequencing |
2 | No | Yes | No * | − | Confirmed | ||
| Levi 2015 [35] | Original article | Brazil | 2014 | Platelets (apheresis) | Aplastic anemia and neutropenic colitis. | Yes | Yes | No | Serology IgG/IgM RT-PCR |
1 | N.P. | Yes | No | − | Confirmed | ||
| Sabino 2015 [36] | Original article | Brazil | 2012 | Platelets | Not specified | − | − | − | Serology IgG/IgM NAT |
4 | − | − | − | − | Probable | Different donors | |
| FFP | Not specified | − | − | − | − | − | − | − | Probable | ||||||||
| RBC | Not specified | − | − | − | − | − | − | − | Probable | ||||||||
| RBC | Not specified | − | − | − | − | − | − | − | Probable | ||||||||
| Platelets | Not specified | − | − | − | − | − | − | − | Probable | ||||||||
| FFP (2 units) | Not specified | − | − | − | − | − | − | − | Possible | ||||||||
| Alves 2016 [37] | Conference abstract | Brazil | Not specified, 2015–2016? | Platelets | Lymphoblastic lymphoma—autologus H.S.C.T. | Yes | Yes | − | Serology IgM RT-PCR Sequencing NS1 Phylogenetic analysis |
− | N.P. | Yes | − | − | Confirmed | ||
| Karim 2016 [38] | Original article | Pakistan | 2015 | Platelets | Coronary artery bypass grafting | No | Yes | − | Serology IgM RT-PCR |
− | N.P. | Yes | Yes | Yes | Possible | Same donor RBC recipient was not tested for dengue virus |
|
| FFP | Coronary artery bypass surgery | No | Yes | − | N.P. | No | Yes | Yes | Possible | ||||||||
| Matos 2016 [39] | Original article | U.S.A. | 2010 | RBC | Lung cancer, coronary heart disease | Yes | Yes | No | Serology IgM/IgG RT-PCR |
4 | − | − | − | − | Probable | Different donors | |
| 2011 | RBC | Pancreatic cancer, DM, dementia. | Yes | Yes | No | Serology IgM | − | − | − | − | − | Possible | |||||
| Santos 2020 [40] | Case report | Brazil | 2019 | RBC | Sickle cell disease on chronic transfusion therapy | Yes | Yes | No | RT-PCR In house sequencing Phylogenetic analysis |
2 | − | − | − | − | Confirmed | ||
CKD: chronic kidney disease, DM: diabetes mellitus, FFP: fresh frozen plasma, HI: hemagglutination inhibition assay, HSCT: hematopoietic stem cell transplantation, IC: immunocompromised, PL: plasma, NAT: nucleic acid testing, NP: not probable, RBC: red blood cells, RT-PCR: reverse transcription polymerase chain reaction, SOT: solid organ transplantation.
− Data not available
* PL not transfused was positive
Table 3. Transfusion-transmitted West Nile virus cases.
| Publication | Type of publication | Country | Year | Blood product | Recipient | IC. | Morbility | Mortality | Diagnostic method | Alternative explanation | Plausibility | Addtitional data |
Other non-vector, non-blood transfusion related transmission | |||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Exposure to Vector | vProlonged hospital stay | Other infected recipients | Non-vector vias rejected | |||||||||||||
| Pealer 2003 [46] | Original article | U.S.A. | 2002 | RBC | Post partum | No | Yes | No | Serology IgM RT-PCR | Possible | − | − | − | Confirmed | 16 implicated blood donors | S.O.T. transmission [57] Screening in blood donors [58] Vertical transmission [12] |
| Platelets | Liver transplantation | Yes | Yes | No | − | − | − | − | Confirmed | |||||||
| RBC | Post partum | No | Yes | No | − | − | − | − | Confirmed | |||||||
| Platelets (2 units) | Acute myeloid leukemya | Yes | Yes | No | − | − | − | − | Confirmed | |||||||
| RBC | Lung cancer | Yes | Yes | Yes | − | − | − | − | Confirmed | |||||||
| FFP | Breast cancer | Yes | Yes | No | − | − | Yes | − | Confirmed | |||||||
| Platelets | Acute myeloid leukemya—BMT | Yes | Yes | Yes | − | − | − | − | Confirmed | |||||||
| FFP | Aneurysm repair | No | No | No | − | − | Yes | − | Confirmed | |||||||
| RBC | Acute myeloid leukemya—HSCT | Yes | No | No | − | − | Yes | − | Confirmed | |||||||
| Platelets | Rhabdomyosarcoma | Yes | Yes | No | − | − | − | − | Confirmed | |||||||
| RBC | Pneumonia, septic shock | No | No | No | − | − | Yes | − | Confirmed | |||||||
| RBC | Coronary-artery bypass grafting | No | Yes | Yes | N.P. | Yes | − | − | Confirmed | |||||||
| Platelets | Aortic-valve replacement | No | No | No | − | − | Yes | − | Confirmed | |||||||
| Platelets | Coronary-artery bypass grafting | No | Yes | No | − | − | − | − | Confirmed | |||||||
| RBC | Acute myloid leukemya—BMT | Yes | No | Yes | − | − | − | − | Confirmed | |||||||
| Platelets | Congenital bone marrow failure—HSCT | Yes | Yes | No | − | − | − | − | Confirmed | |||||||
| FFP | Motor vehicle accident | No | No | No | − | − | − | − | Confirmed | |||||||
| RBC | Lumbar laminectomy | No | Yes | No | − | − | − | − | Confirmed | |||||||
| RBC | Femur-fracture repair | No | No | No | − | − | Yes | − | Confirmed | |||||||
| RBC | Motor vehicle accident | No | No | Yes | − | − | − | − | Confirmed | |||||||
| RBC | Kidney transplantation | Yes | Yes | Yes | − | − | − | − | Confirmed | |||||||
| RBC | Gastrointestinal bleeding | No | Yes | No | − | − | − | − | Confirmed | |||||||
| RBC | Aplastic anemia | Yes | Yes | Yes | − | − | − | − | Confirmed | |||||||
| Caglioti 2004 [47] | Case report | U.S.A. | 2004 | RBC | Above-knee amputation—DM | Yes | Yes | Yes | Serology IgM RT-PCR | Possible | No | No * | Yes | Probable | ||
| Kightlinger 2006 [48] | Case report | U.S.A. | 2006 | RBC | Kidney transplantation | Yes | Yes | No | Serology IgM | N.P. | Yes | Yes | Yes | Probable | Traceback case 1 RBC |
|
| FFP | Kidney transplantation, DM, spinal fracture | Yes | Yes | No | − | − | Yes | − | Probable | |||||||
| Montgomery 2006 [49] | Original article | U.S.A. | 2003 | RBC | Coronary artery bypass graft surgery | No | Yes | No | Serology IgM+ PRNT RT-PCR |
N.P. | Yes | No | Yes | Confirmed | Different donors MP-NAT nonreactive. |
|
| RBC | Myelodysplastic syndrome | Yes | Yes | Yes | − | − | No * | Yes | Probable | |||||||
| RBC | Motor vehicle accident | No | Yes | No | − | − | No * | Yes | Probable | |||||||
| RBC | Coronary bypass, aortic valve replacement | No | Yes | No | − | No | No * | Yes | Probable | |||||||
| RBC | Coronary artery bypass graft surgery | No | No | No | − | − | No * | Yes | Probable | |||||||
| Not specified | Coronary artery bypass graft surgery | No | Yes | No | − | − | − | Yes | Probable | |||||||
| Stanley 2009 [50] | Case report | U.S.A. | 2008 | FFP | Heart transplant | Yes | Yes | No | Serology IgG+ PRNT |
N.P. | − | Yes | Yes | Probable | Traceback case 1 FFP |
|
| RBC | Atrial fibrillation, anemia | No | No | No | − | − | Yes | − | Probable | |||||||
| Meny 2011 [51] | Letter to the editor | U.S.A. | 2010 | Granulocytes (apheresis) | B-lymphoblatic leukemia | Yes | Yes | Yes | Serology IgG/IgM NAT |
− | Yes | No | − | − | NAT results after transfusion | |
| Politis 2011 [52] | Conference abstract | Greece | 2010 | Not specified (RBC?) | Thalassaemia | No | Yes | − | Serology IgG/IgM PCR |
− | − | − | − | Confirmed | Different donors. One aditional inconclusive case |
|
| Not specified (RBC?) | Thalassaemia | No | Yes | − | − | − | − | − | Confirmed | |||||||
| Kelly 2013 [53] | Case report | U.S.A. | 2012 | Platelets (apheresis) | Non-Hodgkin’s lymphoma—HSCT | Yes | Yes | Yes | Serology IgM PRNT RT-PCR |
N.P. | Yes | No * | Yes | Probable | MP-NAT nonreactive. | |
| Pervanidou 2014 [54] | Original article | Greece | 2012 | Not specified | Not specified | − | Yes | No | Not specified | N.P. | − | Yes | − | − | Same donor | |
| Not specified | Not specified | − | No | No | Not specified | − | − | Yes | − | |||||||
| Groves 2017 [55] | Original article | U.S.A. | 2016 | FFP | Aortic valve replacement and coronary bypass surgery |
No | Yes | Yes | Serology IgG/IgM | N.P. | No | − | Yes | Probable | MP-NAT nonreactive No data available about RBC recipient. |
|
| Hayes 2018 [56] | Conference abstract | U.S.A. | 2017 | Platelets (apheresis) | Heart transplant | Yes | Yes | Yes | Serology IgG/IgM PCR |
− | No | No | Yes | Probable | ID-NAT negative | |
BMT: bone marrow transplantation, CKD: chronic kidney disease, DM: diabetes mellitus, FFP: fresh frozen plasma, HSCT: hematopoietic stem cell transplantation, MP: minipool, NAT: nucleic acid testing, NP: not probable, PL: plasma, PRNT: plaque reduction neutralization test, RBC: red blood cells, RT-PCR: reverse transcription polymerase chain reaction, SOT: solid organ transplantation
− Data not available
* PL not transfused was positive
Arboviruses with a potential threat to transfusion safety
In addition to the 10 arboviruses involved in reported cases of transfusion-transmitted infections, 18 additional arboviruses were identified with a potential threat to transfusion safety by means of organ and/or hematopoietic stem cell transplantation, mother-to-child transmission, direct blood contact and/or prevalence in blood donors. The characteristics of published cases on these arboviruses are listed in Table 4. Reference studies on these other arboviruses describing the risk of direct transmission, are depicted in Table 5.
Table 4. Arboviruses that could pose a threat to transfusion safety due to direct non-vector related transmission mechanisms.
| Source of threat to transfusion safety | Arboviruses |
|---|---|
| Transmission through organ—and/or hematopoietic stem cell transplantation | Dengue virus, eastern equine encephalitis virus, heartland virus, Jamestown Canyon virus, tick-borne encephalitis virus, and West Nile virus |
| Mother-to-child transmission | Colorado tick fever virus, Japanese encephalitis virus, Ross River virus, yellow fever virus, Zika virus, dengue virus, West Nile virus, chikungunya virus, Crimean-Congo hemorrhagic virus, La Crosse virus, O’nyong’nyong virus, Rift Valley fever virus, Sindbis virus, Venezuelan equine encephalitis virus and Western equine encephalitis virus. |
| Prevalence in blood donors | Japanese encephalitis virus, Ross River virus, St. Louis encephalitis virus, tick-borne encephalitis virus, yellow fever virus, Zika virus, dengue virus, West Nile virus, Barmah Forest Virus, chikungunya virus, Crimean-Congo hemorrhagic virus, eastern equine encephalitis virus, Heartland virus, Jamestown Canyon virus, Mayaro virus, Murray Valley encephalitis virus, O’nyong’nyong virus, Rift Valley fever virus, Huaiyangshan banyangvirus (Severe fever with thrombocytopenia syndrome Virus), Sindbis virus, Tahyna virus, Toscana virus, and Piry vesiculovirus. |
| Other direct routes of transmission | Blood contact: tick-borne encephalitis virus, dengue virus, chikungunya virus, Crimean-Congo haemorrhagic virus, La Crosse virus, Zika virus |
Table 5. Reference studies on arboviruses that could be a threat to transfusion safety.
| Virus | Publication | Type of publication | Threat to transfusion safety–Direct transmission (non-vector related transmission) |
|---|---|---|---|
| Barmah Forest Virus | Faddy 2014 [59] | Short communication | Screening in blood donors: 5.791 samples screened in 2011 by ELISA IgM: 68 positives (1,17%). |
| Chikungunya virus | Parola 2006 [60] | Original article | Blood contact: A 60-year-old female nurse developed symptom 3 days after contact with a patient with dengue. Interview and examination did not show recent travel abroad, mosquito bite, accidental skin puncture during blood sampling, skin lesion, or eczema. She noted direct contact with patient blood during hemostasis. |
| Simmons 2016 [61] | Original article | Screening in blood donors: 3.007 samples screened by NAT: 56 (1.86%) were confirmed positive. | |
| Villamil-Gómez 2015 [62] | Original article | Vertical transmission: From September 2014 to February 2015, 7 pregnant women with serological and reverse transcription-polymerase chain reaction-positive test for CHIK delivered 8 infants with CHIK. | |
| Couderc 2012 [63] | Original article | Other: 4 infected corneas from apparently uninfected donors. | |
| Crimean-Congo haemorrhagic virus | Tsergouli 2019[64] | Original article | Blood contact: Between 1953–2016: 158 cases of nosocomial transmission (2 needle-stick injury or abrasion). |
| Charlier 2017 [12] | Original article | Vertical transmission: Transmission documented: miscarriages, stillbirths with maternal death and 1 case of documented fatal neonatal infection. | |
| Barabás 2018 [65] | Conference abstract | Screening in blood donors: Screening of 1885 blood donors with an IFA in-house method, 10 were positive (0.53%). | |
| Eastern equine encephalitis virus | Leiby 2014 [66] | Conference abstract | Screening in blood donors: 1.314 samples have been screened by PRNT: 2 (0.15%) were confirmed positive. |
| Pouch 2019 [67] | Original article | Solid organ transplantation: In 2017, 3 solid organ (heart, liver and lung) transplant recipients from a common donor developed encephalitis by Eastern equine encephalitis virus (EEEV). | |
| Heartland virus | Hevey 2019 [68] | Case report | Solid organ transplantation: Heartland virus infection in a heart transplant recipient from the Heartland (U.S.A.). |
| Lindsey 2019 [69] | Orginal article | Screening in blood donors: Of the 487 blood donors tested, 12 were positives, and 7 of those were confirmed for Heartland virus neutralizing antibodies by PRNT. | |
| Jamestown Canyong virus | Askar 2019 [70] | Case report | Solid organ transplantation: Jamestown Canyon virus encephalitis in a heart transplant patient. |
| Mayo 2001 [71] | Letter to the Editor | Screening in blood donors: Of the 1,086 sera collected from blood donors in 1990, 164 (15%) were positive by IFA. | |
| La Crosse virus | R. Bowen 2013 [72] | Conference abstract | Blood contact: During the 2011 outbreak in China it was discovered that the virus was able to be transmitted person to person through blood contact, indicating the possibility this virus could be transmitted through a tainted blood product. |
| Charlier 2017 [12] | Original article | Vertical transmission: Transmission documented: 1 asymptomatic mother-to-child transmission documented serologically in cord serum, after a maternal infection. | |
| Mayaro virus | Romeiro 2020 [73] | Original article | Screening in blood donors: 5608 blood donor samples were tested. IgM and IgG antibodies to MAYV were detected in 36 and 11 samples, respectively. |
| Murray valley encephalitis virus | Williams 2013 [74] | Original article | Screening in blood donors: 592 samples from blood donors from the Murray Valley region, 6 positives for IgG antibodies (1%; 95% CI: 0.2–1.8%) |
| O’nyong’nyong virus | Clements 2019 [75] | Original article | Screening in blood donors: 24 of 552 CHIKV IgG-positive samples (4.4%) were tested for their ability to neutralize CHIKV and other related alphaviruses. 23 of the samples showed higher titers against ONNV than CHIKV. |
| Charlier 2017 [12] | Original article | Vertical transmission: Transmission uncertain; 2 miscarriages reported. | |
| Rift Valley fever virus | Azhar 2010 [76] | Original article | Screening in blood donors: 2 of 1260 (0.16%) blood donors were RVFV IgG positive. |
| Charlier 2017 [12] | Original article | Vertical transmission: Transmission documented; increased risk of miscarriage. Two symptomatic cases of mother-to-child transmission. | |
| SFTS Virus | Zeng 2015 [77] | Original article | Screening in blood donors: 14,764 donor samples were tested for anti-SFTSV IgG antibodies, 86 of which were repeat-reactive and defined as seropositive. |
| Sindbis virus | Jöst 2011 [78] | Letter to the Editor | Screening in blood donors: 389 investigated blood donor samples were tested for SINV-specific-IgG antibodies, 4 were positive. |
| Charlier 2017 [12] | Original article | Vertical transmission: Transmission uncertain; two stillbirths reported. | |
| Tahyna virus | Sonnleitner 2014 [79] | Original article | Screening in blood donors: IgG antibodies were determined in sera of 1630 blood donors. 10 (0.6%) reacted positive by TAHV IFA, 5 of which (0.3%) were confirmed by neutralization test. |
| Toscana virus | Brisbarre 2011 [80] | Letter to the Editor | Screening in blood donors: 84 (11.5%) of 729 plasma samples were positive for IgG. 24 (3.3%) were positive for IgM, and 5 (0.7%) were positive for IgG and IgM. |
| Venezuelan equine encephalitis virus | Charlier 2017 [12] | Original article | Vertical transmission: virus documented in the brains of ten aborted fetuses; developmental brain lesions in infants borne by infected mothers. |
| Vesiculovirus Piry | Tavares-Neto 1990 [81] | Original article | Screening in blood donors: frequency of neutralizing antibodies 8% (13/162). |
| Western equine encephalitis virus | Charlier 2017 [12] | Original article | Vertical transmission: three cases with severe encephalitis. |
IFA: indirect fluorescent antibody, NAT: nucleic acid testing, PRNT: plaque reduction neutralization test, SFTS Virus: Severe fever with thrombocytopenia syndrome virus (Huaiyangshan banyangvirus).
Discussion
Until the year 2000, transfusion transmission of arboviruses was almost anecdotal, with only one isolated case of transmission of Colorado tick fever virus and two cases of tick-borne encephalitis virus. However, after the West Nile virus outbreak in the USA in 2002, the number of cases increased considerably [46]. Since then, more than 70 cases of arbovirus transmission have been published, including several cases of emerging arboviruses: Japanese encephalitis virus, Ross River virus, St. Louis encephalitis virus, Powassan virus, and Zika virus [13,15,17,19,26,27].
This study confirms the possibility that arboviruses can be transmitted through transfusion of blood and blood components. A total of 74 reported cases of suspected transfusion-transmitted infections from 10 arboviruses were identified. Infections were reported to be symptomatic in 63.5% and fatal in 18.9% of the reported cases. This transmission route therefore poses a considerable threat to transfusion safety, reportedly causing significant morbidity and mortality and an increased health spending. As more than 50% of affected patients were classified as immunocompromised, transmission of arboviruses through blood or blood components can additionally be considered a threat to a particularly vulnerable section of the population. Analysis of reported cases revealed that transfusion transmission occurred through various blood products. It is observed that transmission through platelet transfusion was found to be higher in cases of dengue virus transmission, compared to other arboviral transmission cases, including the West Nile virus cases. This finding could be related to signs of tropism of the dengue virus against platelets or at least some of their components, such as glycoprotein Ib (CD42b) [82].
In addition to the published cases of transfusion transmission of arboviruses, our review identified 18 additional arboviruses with potential threat to transfusion safety through solid organ transplantation, mother-to-child transmission, blood contact or prevalence in blood donors. The results of this review further confirm identification of arboviruses with a high-risk of future transfusion transmission, as they were reported to be involved in direct non-vector related transmission and prevalent among blood donors. These are: Chikungunya virus, Crimean-Congo haemorrhagic virus, Eastern equine encephalitis virus, Heartland virus and Jamestown Canyong virus.
Based on the results of this review, the reported rapid growth of arboviral cases in recent years can also be confirmed and seems to correspond to the expanding endemicity of arboviruses globally. According to literature, the increased frequency of outbreaks can be explained by multiple environmental and anthropogenic factors, including increased travel and trade, population growth, changing land use patterns, and the urbanization of rural areas [83].
These facts come on top of a growing list of emerging infectious diseases. It is estimated that from 1940 to 2004, 5.3 new viruses were discovered each year, of which at least two-thirds were zoonoses [84]. In consonance with their emerging nature, there is very little knowledge on some of these new arboviruses, such as the SFTS virus, which has already caused multiple deaths in South Korea [85].
To improve transfusion safety, blood banks have taken a number of measures. One common measure is the exclusion of donors presenting symptoms. This is a measure with limited effectiveness given the high rate of asymptomatic infections. Another measure taken is the cancellation of blood donations in affected regions, which is at times difficult to apply, if the epidemic outbreak is extensive and no contingency plans are in place to guarantee the supply of blood and blood components from other geographical regions. So far, the most useful measure is the application of nucleic acid testing (NAT) in donor screening. One example illustrating this success comes from the significant reduction in transmission of West Nile virus in the USA, after the implementation of NAT screening in 2003. However, NAT tests are not infallible: for instance, one case of West Nile virus transmission was reported in a donor with very low viremia who had undergone NAT screening, using a simple sample [56]. Another compromising aspect is the expense: the implementation of NAT testing for West Nile virus in the USA, had an estimated cost of USD 483,000–1,300,000 per quality-adjusted life year (QALY), clearly exceeding the widely accepted threshold of USD 50,000–100,000 per QALY [3,86]. Furthermore, implementing NAT tests requires human and logistical resources that are not available in all settings. As an alternative, techniques for the inactivation of pathogens such as methylene blue and visible light, could also be applied where available, as these methods were proven effective against several arboviruses [87,88]. In general, and despite limitations, the best probable strategy is probably to screen using NAT techniques and apply pathogen inactivation techniques to as many blood components as resources allow.
In addition, blood transfusion centers should develop robust hemovigilance systems with the ability to trace blood products from infected donors, so that these can be destroyed prior to use or, in case these have already been transfused, the physician responsible for clinical management of the recipient, can be informed in a timely fashion.
The risk of transfusion-transmitted arbovirus infections is of particular concern in low-income countries, usually in endemic areas or areas where extensive epidemic outbreaks occur. Particularly since blood bank systems are usually not based on voluntary donations, but rather on replacement donations. In addition, testing for infectious agents is not optimal, due to technical and resource constraints or a lack of qualified personnel, often relying on rapid diagnostic tests, known to have a poor sensitivity [89,90].
One limitation of this systematic review is the inherent difficulty of confirming the transmission of the arbovirus through the transfusion of blood components. Unequivocally concluding that an infection was transmitted through transfusion would require demonstrating that the infectious agent was found in samples from the donor or in residual blood components from the donation, that the recipient was not infected before receiving the transfusion, and that the virus was not transmitted through the bite of a vector. This is especially complicated in endemic areas, where the population is exposed to vector bites (mainly mosquitoes), with the possible exception of patients admitted to specific units such as: units specialized in transplantation and intensive care units. However, even in these “mosquito free” units, patients could have been infected before hospital admission. Phylogenetic analysis may be relevant to exclude the transfusion hypothesis, but if the donor and recipient reside in the same geographic area, the same genetic sequence may not be enough to confirm this exclusion [91]. Therefore, definitively classifying a case as transfusion transmission is often unfeasible.
Similarly, a significant number of transfusion-transmitted arbovirus infections are likely to go undetected. If, despite the transmission, the recipient does not present symptoms, or if the transmission occurs in a geographical region during an epidemic outbreak, where transmission through the vector cannot be ruled out, transfusion transmission may go unnoticed.
Another limitation of the study is that conclusions of authors of the reviewed records on the plausibility of transfusion transmission and mortality as a consequence of the arboviral infection, were copied with limited information available to confirm these independently. In addition, each author may have applied different criteria in establishing the plausibility of arboviral transmission through the transfusion of blood or blood components and mortality as a possible outcome.
In conclusion, this review updated, characterized and classified cases of arbovirus transmission through transfusion. In addition, a significant number of arboviruses were identified with a potential threat to future transfusion safety. In recent years a global increase was seen in the number of epidemic outbreaks of various arboviruses. In the coming years, it is expected that this number will continue to increase. For this reason, it is important that each system or organization responsible for transfusion safety has adequate surveillance systems, contingency plans, and protocols in place to guarantee transfusion safety. The different regulatory agencies, public health bodies, medical communities, and the medical industry should collaborate closely and coordinate efforts to provide a rapid and effective response to any threat to transfusion safety.
Supporting information
(DOCX)
(DOCX)
(DOCX)
(DOCX)
(DOCX)
Acknowledgments
The authors wish to express their thanks to Meggan Harris for her assistance in editing this manuscript, and Professor Gregorio Gonzalez-Alcaide of the Department of Documentation of the University of Valencia, for reviewing the systematic review protocol.
Data Availability
All relevant data are within the manuscript and its Supporting Information files.
Funding Statement
The authors received no specific funding for this work.
References
- 1.Perkins HA, Busch MP. Transfusion-associated infections: 50 years of relentless challenges and remarkable progress. Transfusion. 2010;50(10):2080–2099. doi: 10.1111/j.1537-2995.2010.02851.x [DOI] [PubMed] [Google Scholar]
- 2.Stramer SL, Dodd RY. AABB Transfusion-Transmitted Diseases Emerging Infectious Diseases Subgroup. Transfusion-transmitted emerging infectious diseases: 30 years of challenges and progress. Transfusion. 2013;53(10 Pt 2):2375–2383. doi: 10.1111/trf.12371 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Petersen LR, Busch MP. Transfusion-transmitted arboviruses. Vox Sang. 2010;98(4):495–503. doi: 10.1111/j.1423-0410.2009.01286.x [DOI] [PubMed] [Google Scholar]
- 4.Go YY, Balasuriya UB, Lee CK. Zoonotic encephalitides caused by arboviruses: transmission and epidemiology of alphaviruses and flaviviruses. Clin Exp Vaccine Res. 2014;3(1):58–77. doi: 10.7774/cevr.2014.3.1.58 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Giménez-Richarte Á, de Salazar MO, Arbona C, Giménez-Richarte MP, Collado M, Fernández PL, et al. Prevalence of Chikungunya, Dengue and Zika viruses in blood donors: a systematic literature review and meta-analysis Blood Transfus. 2022;20(4):267–280. doi: 10.2450/2021.0106-21 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Stramer SL, Hollinger FB, Katz LM, Kleinman S, Metzel PS, Gregory KR, et al. Emerging infectious disease agents and their potential threat to transfusion safety. Transfusion. 2009;49(Suppl 2):1S–29S. doi: 10.1111/j.1537-2995.2009.02279.x [DOI] [PubMed] [Google Scholar]
- 7.American Association of Blood Banks. Fact Sheets Created or Updated Post Publication Of The TRANSFUSION August 2009 Supplement. 2020 Available from http://www.aabb.org/tm/eid/Pages/eidpostpub.aspx.
- 8.European Centro for Disease Prevention and Control. Assessing the risk of communicable diseases transmissible through substances of human origin. 2011. Available from https://www.ecdc.europa.eu/sites/default/files/media/en/publications/Publications/diseases-communicable-by-substances-of-human-origin-SoHo.pdf.
- 9.World Health Organization. Asia Pacific Strategy for Emerging Diseases and Public Health Emergencies (APSED III). 2017. Available from https://iris.wpro.who.int/bitstream/handle/10665.1/13654/9789290618171-eng.pdf.
- 10.World Health Organization. Blood donor selection: guidelines on assessing donor suitability for blood donation. 2012. Available from https://www.who.int/bloodsafety/publications/guide_selection_assessing_suitability.pdf. [PubMed]
- 11.Higgins JPT, Green S. Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 [updated March 2011]. The Cochrane Collaboration, 2011. Available from www.cochrane-handbook.org.
- 12.Centers for Disease Control and Prevention (CDC). Transmission of Colorado tick fever virus by blood transfusion–Montana. MMWR Morb Mortal Wkly Rep. 1975;24(50):422–427. [Google Scholar]
- 13.Charlier C, Beaudoin MC, Couderc T, Lortholary O, Lecuit M. Arboviruses and pregnancy: maternal, fetal, and neonatal effects. Lancet Child Adolesc Health. 2017;1(2):134–146. doi: 10.1016/S2352-4642(17)30021-4 [DOI] [PubMed] [Google Scholar]
- 14.Cheng VCC, Sridhar S, Wong SC, Wong SCY, Chan JFW, Yip CCY et al. Japanese Encephalitis Virus Transmitted Via Blood Transfusion, Hong Kong, China. Emerg Infect Dis. 2018;24(1):49–57. doi: 10.3201/eid2401.171297 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Sayama Y, Suksakhone C, Keokhamphoui C, Kongphaly D, Mazda T, Hoshi Y, et al. Prevalence of mosquito-borne viral infection (dengue fever, Japanese encephalitis, and Chikungunya fever) among blood donors in Lao PDR. Vox Sang. 2013;105(SUPPL.2):98–99 [Google Scholar]
- 16.Hoad VC, Speers DJ, Keller AJ, Dowse GK, Seed CR, Lindsay MD, et al. First reported case of transfusion-transmitted Ross River virus infection. Med J Aust. 2015;202(5):267–270. doi: 10.5694/mja14.01522 [DOI] [PubMed] [Google Scholar]
- 17.Faddy H, Dunford M, Seed C, Olds A, Harley D, Dean M, et al. An evidence-based evaluation of the risk posed by ross river virus to the safety of the australian blood supply. Vox Sang. 2012;103(SUPPL. 1):184–185. [Google Scholar]
- 18.Venkat H, Adams L, Sunenshine R, Krow-Lucal E, Levy C, Kafenbaum T, et al. St. Louis encephalitis virus possibly transmitted through blood transfusion-Arizona, 2015. Transfusion. 2017;57(12):2987–2994. doi: 10.1111/trf.14314 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Spinsanti L, Re V, Aguilar J, Contigiani M. An indirect immunofluorescence assay to detect antibodies against St. Louis Encephalitis virus. Rev Inst Med Trop Sao Paulo. 2001;43(6):339–340. doi: 10.1590/s0036-46652001000600008 [DOI] [PubMed] [Google Scholar]
- 20.Taylor L, Stevens T, Destrampe EM, Brown JA, McGavic J, Gould CV, et al. Powassan virus infection likely acquired through blood transfusion presenting as encephalitis in a kidney transplant recipient [published online ahead of print, 2020 Jun 15]. Clin Infect Dis. 2020;ciaa738. doi: 10.1093/cid/ciaa738 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Wahlberg P, Saikku P, Brummer-Korvenkontio M. Tick-borne viral encephalitis in Finland. The clinical features of Kumlinge disease during 1959–1987. J Intern Med. 1989;225(3):173–177. doi: 10.1111/j.1365-2796.1989.tb00059.x [DOI] [PubMed] [Google Scholar]
- 22.Laboratory safety for arboviruses and certain other viruses of vertebrates. The Subcommittee on Arbovirus Laboratory Safety of the American Committee on Arthropod-Borne Viruses. Am J Trop Med Hyg. 1980;29(6):1359–1381. doi: 10.4269/ajtmh.1980.29.1359 [DOI] [PubMed] [Google Scholar]
- 23.Lipowski D, Popiel M, Perlejewski K, Nakamura S, Bukowska-Osko I, Rzadkiewicz E, et al. A Cluster of Fatal Tick-borne Encephalitis Virus Infection in Organ Transplant Setting. J Infect Dis. 2017;215(6):896–901. doi: 10.1093/infdis/jix040 [DOI] [PubMed] [Google Scholar]
- 24.Marvik Å, Tveten Y, Pedersen AB, Stiasny K, Andreassen ÅK, Grude N. Low prevalence of tick-borne encephalitis virus antibodies in Norwegian blood donors [published online ahead of print, 2020 Sep 14]. Infect Dis (Lond). 2020;1–8. doi: 10.1080/23744235.2020.1819561 [DOI] [PubMed] [Google Scholar]
- 25.Centers for Disease Control and Prevention (CDC). Transfusion-Related Transmission of Yellow Fever Vaccine Virus—California, 2009. MMWR Morb Mortal Wkly Rep. 2010;59(2):34–37. [PubMed] [Google Scholar]
- 26.Ergünay K, Saygan MB, Aydoğan S, Litzba N, Niedrig M, Pınar A, et al. Orta/Kuzey Anadolu Bölgesi kan donörlerinde Dengue virusu ve sarı humma virusu seropozitifliğinin araştırılması [Investigation of dengue virus and yellow fever virus seropositivities in blood donors from Central/Northern Anatolia, Turkey]. Mikrobiyol Bul. 2010;44(3):415–424. [PubMed] [Google Scholar]
- 27.Barjas-Castro ML, Angerami RN, Cunha MS, Suzuki A, Nogueira JS, Rocco IM, et al. Probable transfusion-transmitted Zika virus in Brazil. Transfusion. 2016;56(7):1684–1688. doi: 10.1111/trf.13681 [DOI] [PubMed] [Google Scholar]
- 28.Motta IJ, Spencer BR, Cordeiro da Silva SG, Arruda MB, Dobbin JA, Gonzaga YB, et al. Evidence for Transmission of Zika Virus by Platelet Transfusion. N Engl J Med. 2016;375(11):1101–1103. doi: 10.1056/NEJMc1607262 [DOI] [PubMed] [Google Scholar]
- 29.Hills SL, Morrison A, Stuck S, Sandhu K, Mason KL, Stanek D, et al. Case Series of Laboratory-Associated Zika Virus Disease, United States, 2016–2019. Emerg Infect Dis. 2021;27(5):1296–1300. doi: 10.3201/eid2705.203602 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Beau F, Lastère S, Mallet HP, Mauguin S, Broult J, Laperche S. Impact on blood safety of the last arboviruses outbreaks in French Polynesia (2012–18). Transfus Clin Biol 2020;27:4–9. doi: 10.1016/j.tracli.2019.12.001 [DOI] [PubMed] [Google Scholar]
- 31.Marbán-Castro E, Goncé A, Fumadó V, Romero-Acevedo L, Bardají A. Zika virus infection in pregnant women and their children: A review. Eur J Obstet Gynecol Reprod Biol. 2021;265:162–168. doi: 10.1016/j.ejogrb.2021.07.012 [DOI] [PubMed] [Google Scholar]
- 32.Chuang V, Wong TY, Leung YH, Ma E, Law YL, Tsang O, et al. Review of dengue fever cases in Hong Kong during 1998 to 2005. Hong Kong Med J. 2008;14(3):170–177. [PubMed] [Google Scholar]
- 33.Tambyah PA, Koay ES, Poon ML, Lin RV, Ong BK. Transfusion-Transmitted Dengue Infection Study Group. Dengue hemorrhagic fever transmitted by blood transfusion. N Engl J Med. 2008;359(14):1526–1527. doi: 10.1056/NEJMc0708673 [DOI] [PubMed] [Google Scholar]
- 34.Oh HB, Muthu V, Daruwalla ZJ, Lee SY, Koay ES, Tambyah PA. Bitten by a bug or a bag? Transfusion-transmitted dengue: a rare complication in the bleeding surgical patient. Transfusion. 2015;55(7):1655–1661. doi: 10.1111/trf.13054 [DOI] [PubMed] [Google Scholar]
- 35.Levi JE, Nishiya A, Félix AC, Salles NA, Sampaio LR, Hangai F, et al. Real-time symptomatic case of transfusion-transmitted dengue. Transfusion. 2015;55(5):961–964. doi: 10.1111/trf.12944 [DOI] [PubMed] [Google Scholar]
- 36.Sabino EC, Loureiro P, Lopes ME, Capuani L, McClure C, Chowdhury D, et al. Transfusion-Transmitted Dengue and Associated Clinical Symptoms During the 2012 Epidemic in Brazil. J Infect Dis. 2016;213(5):694–702. doi: 10.1093/infdis/jiv326 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Alves M, Infante V, Zenatti C, Vieira G, Silva I, Kayano S, et al. Blood-borne dengue virus: A case report of severe dengue in a hematopoietic stem cell recipient. Open Forum Infect. Dis. 2016;3(Supp1). [Google Scholar]
- 38.Karim F, Nasir N, Moiz B. Transfusion transmitted dengue: One donor infects two patients. Transfus Apher Sci. 2017;56(2):151–153. doi: 10.1016/j.transci.2016.10.013 [DOI] [PubMed] [Google Scholar]
- 39.Matos D, Tomashek KM, Perez-Padilla J, Muñoz-Jordán J, Hunsperger E, Horiuchi K, et al. Probable and possible transfusion-transmitted dengue associated with NS1 antigen-negative but RNA confirmed-positive red blood cells. Transfusion. 2016;56(1):215–222. doi: 10.1111/trf.13288 [DOI] [PubMed] [Google Scholar]
- 40.Santos FLS, Slavov SN, Bezerra RS, Santos EV, Silva-Pinto AC, Morais ALL, et al. Vaso-occlusive crisis in a sickle cell patient after transfusion-transmitted dengue infection. Transfusion. 2020;60(9):2139–2143. doi: 10.1111/trf.15968 [DOI] [PubMed] [Google Scholar]
- 41.De Wazières B, Gil H, Vuitton DA, Dupond JL. Nosocomial transmission of dengue from a needlestick injury. Lancet. 1998;351(9101):498. doi: 10.1016/S0140-6736(05)78686-4 [DOI] [PubMed] [Google Scholar]
- 42.Yadav A, Rastogi N, Upasana K, Arora S, Thakkar D, Yadav SP. Dengue virus transmission from donor to recipient during haploidentical stem cell transplantation. IDCases. 2021;25:e01220. doi: 10.1016/j.idcr.2021.e01220 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Ashshi AM. The prevalence of dengue virus serotypes in asymptomatic blood donors reveals the emergence of serotype 4 in Saudi Arabia. Virol J 2017;14:107. doi: 10.1186/s12985-017-0768-7 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Shaji Mathew J, Menon VP, Menon VP, Mallick S, Sivasankara Pillai Thankamony Amma B, et al. Dengue virus transmission from live donor liver graft. Am J Transplant. 2019;19(6):1838–1846. doi: 10.1111/ajt.15270 [DOI] [PubMed] [Google Scholar]
- 45.Evans-Gilbert T. Vertically transmitted Chikungunya, Zika and dengue virus infections: The pathogenesis from mother to fetus and the implications of co-infections and vaccine development. Int J Pediatr Adolesc Med. 2020;7(3):107–111. doi: 10.1016/j.ijpam.2019.05.004 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Pealer LN, Marfin AA, Petersen LR, Lanciotti RS, Page PL, Stramer SL, et al. Transmission of West Nile virus through blood transfusion in the United States in 2002. N Engl J Med. 2003;349(13):1236–1245. doi: 10.1056/NEJMoa030969 [DOI] [PubMed] [Google Scholar]
- 47.Centers for Disease Control and Prevention (CDC). Transfusion-associated transmission of West Nile virus—Arizona, 2004. MMWR Morb Mortal Wkly Rep. 2004;53(36):842–844. [PubMed] [Google Scholar]
- 48.Centers for Disease Control and Prevention (CDC). West Nile virus transmission through blood transfusion—South Dakota, 2006. MMWR Morb Mortal Wkly Rep. 2007;56(4):76–79. [PubMed] [Google Scholar]
- 49.Montgomery SP, Brown JA, Kuehnert M, Smith TL, Crall N, Lanciotti RS, et al. Transfusion-associated transmission of West Nile virus, United States 2003 through 2005. Transfusion. 2006;46(12):2038–2046. doi: 10.1111/j.1537-2995.2006.01030.x [DOI] [PubMed] [Google Scholar]
- 50.Centers for Disease Control and Prevention (CDC). West Nile virus transmission via Organ Transplantation and Blood Transfusion—Louisiana, 2008. MMWR Morb Mortal Wkly Rep. 2009;58(45):1263–1267. [PubMed] [Google Scholar]
- 51.Meny GM, Santos-Zabala L, Szallasi A, Stramer SL. West Nile virus infection transmitted by granulocyte transfusion. Blood. 2011;117(21):5778–5779. doi: 10.1182/blood-2011-02-335901 [DOI] [PubMed] [Google Scholar]
- 52.Politis C, Pappa A, Hassapopoulou H, Pantelidou D, Perifanis V, Teli A, et al. Transfusion transmitted west Nile virus (WNV) infection in thalassaemic patients in Greece. Vox Sanguinis. 2011;101(Supp.1):236. [Google Scholar]
- 53.Centers for Disease Control and Prevention (CDC). Fatal West Nile Virus Infection After Probable Transfusion-Associated Transmission—Colorado, 2012. MMWR Morb Mortal Wkly Rep. 2013;62(31):622–624. [PMC free article] [PubMed] [Google Scholar]
- 54.Pervanidou D, Detsis M, Danis K, Mellou K, Papanikolaou E, Terzaki I, et al. West Nile virus outbreak in humans, Greece, 2012: third consecutive year of local transmission [published correction appears in Euro Surveill. 2014;19(14):pii/20766]. Euro Surveill. 2014;19(13):20758. doi: 10.2807/1560-7917.es2014.19.13.20758 [DOI] [PubMed] [Google Scholar]
- 55.Groves JA, Shafi H, Nomura JH, Herron RM, Baez D, Dodd RY, et al. A probable case of West Nile virus transfusion transmission. Transfusion. 2017;57(3pt2):850–856. doi: 10.1111/trf.14018 [DOI] [PubMed] [Google Scholar]
- 56.Hayes C, Stephens L, Fridey JL, Snyder RE, Groves JA, Stramer SL, et al. Probable transfusion transmission of West Nile virus from an apheresis platelet that screened non-reactive by individual donor-nucleic acid testing. Transfusion. 2020;60(2):424–429. doi: 10.1111/trf.15568 [DOI] [PubMed] [Google Scholar]
- 57.Winston DJ, Vikram HR, Rabe IB, Dhillon G, Mulligan D, Hong JC, et al. Donor-derived West Nile virus infection in solid organ transplant recipients: report of four additional cases and review of clinical, diagnostic, and therapeutic features. Transplantation. 2014;97(9):881–889. doi: 10.1097/TP.0000000000000024 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Busch MP, Caglioti S, Robertson EF, McAuley JD, Tobler LH, Kamel H, et al. Screening the blood supply for West Nile virus RNA by nucleic acid amplification testing. N Engl J Med. 2005;353(5):460–467. doi: 10.1056/NEJMoa044029 [DOI] [PubMed] [Google Scholar]
- 59.Faddy H, Dunford M, Seed C, Olds A, Harley D, Dean M, et al. Seroprevalence of Antibodies to Ross River and Barmah Forest Viruses: Possible Implications for Blood Transfusion Safety After Extreme Weather Events. Ecohealth. 2015;12(2):347–353. doi: 10.1007/s10393-014-1005-0 [DOI] [PubMed] [Google Scholar]
- 60.Parola P, de Lamballerie X, Jourdan J, Rovery C, Vaillant V, Minodier P, et al. Novel Chikungunya virus variant in travelers returning from Indian Ocean islands. Emerg Infect Dis. 2006;12(10):1493–1499. doi: 10.3201/eid1210.060610 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Simmons G, Brès V, Lu K, Liss NM, Brambilla DJ, Ryff KR, et al. High Incidence of Chikungunya Virus and Frequency of Viremic Blood Donations during Epidemic, Puerto Rico, USA, 2014. Emerging Infectious Diseases. 2016;22(7):1221–1228. doi: 10.3201/eid2207.160116 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Villamil-Gómez W, Alba-Silvera L, Menco-Ramos A, Gonzalez-Vergara A, Molinares-Palacios T, Barrios-Corrales M, et al. Congenital Chikungunya Virus Infection in Sincelejo, Colombia: A Case Series. J Trop Pediatr. 2015;61(5):386–392. doi: 10.1093/tropej/fmv051 [DOI] [PubMed] [Google Scholar]
- 63.Couderc T, Gangneux N, Chrétien F, Caro V, Le Luong T, Ducloux B, et al. Chikungunya virus infection of corneal grafts. J Infect Dis. 2012;206(6):851–859. doi: 10.1093/infdis/jis296 [DOI] [PubMed] [Google Scholar]
- 64.Tsergouli K, Karampatakis T, Haidich AB, Metallidis S, Papa A. Nosocomial infections caused by Crimean-Congo haemorrhagic fever virus. J Hosp Infect. 2020;105(1):43–52. doi: 10.1016/j.jhin.2019.12.001 [DOI] [PubMed] [Google Scholar]
- 65.Barabás E, Magyar N, Palyi B, Nagy A, Henczko J, Takacs M, et al. An emerging virus in a new geographic area–serological evidence of the Crimean-Congo haemorrhagic fever virus among hungarian blood donors. Vox Sanguinis. 2018;113(Suppl. 1):217. [Google Scholar]
- 66.Leiby DA, Hapip CA, Kenney JL, Mutebi J, Ahmed A, Stramer SL. Preliminary investigations of donor exposure to eastern equine encephalitis virus and implications for risk. Transfusion. 2014;54(Suppl. 2):214A. [Google Scholar]
- 67.Pouch SM, Katugaha SB, Shieh WJ, Annambhotla P, Walker WL, Basavaraju SV, et al. Transmission of Eastern Equine Encephalitis Virus From an Organ Donor to 3 Transplant Recipients. Clin Infect Dis. 2019;69(3):450–458. doi: 10.1093/cid/ciy923 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Hevey MA, O”Halloran JA, Jagger BW, Staples JE, Lambert AJ, Panella AJ, et al. Heartland virus infection in a heart transplant recipient from the Heartland. Transpl Infect Dis. 2019;21(4):e13098. doi: 10.1111/tid.13098 [DOI] [PubMed] [Google Scholar]
- 69.Lindsey NP, Menitove JE, Biggerstaff BJ, Turabelidze G, Parton P, Peck K, et al. Seroprevalence of Heartland Virus Antibodies in Blood Donors, Northwestern Missouri, USA. Emerg Infect Dis. 2019;25(2):358–360. doi: 10.3201/eid2502.181288 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Askar W, Menaria P, Thohan V, Brummitt CF. Jamestown Canyon virus encephalitis in a heart transplant patient. Transpl Infect Dis. 2020;22(1):e13210. doi: 10.1111/tid.13210 [DOI] [PubMed] [Google Scholar]
- 71.Mayo D, Karabatsos N, Scarano FJ, Brennan T, Buck D, Fiorentino T, et al. Jamestown Canyon virus: seroprevalence in Connecticut. Emerg Infect Dis. 2001;7(5):911–912. doi: 10.3201/eid0705.017529 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Keil D, Marschner S, Gosney EJ, Bowen R. Photochemical inactivation of la crosse virus (LCV) using the mirasol PRT system. Transfusion. 2013;53(Suppl. 2):217A. [Google Scholar]
- 73.Romeiro MF, Fumagalli MJ, Dos Anjos AB, Figueiredo LTM. Serological evidence of Mayaro virus infection in blood donors from São Carlos, São Paulo, Brazil. Trans R Soc Trop Med Hyg. 2020;114(9):686–689. doi: 10.1093/trstmh/traa016 [DOI] [PubMed] [Google Scholar]
- 74.Williams SA, Richards JS, Faddy HM, Leydon J, Moran R, Nicholson S, et al. Low seroprevalence of Murray Valley encephalitis and Kunjin viruses in an opportunistic serosurvey, Victoria 2011. Aust N Z J Public Health. 2013;37(5):427–433. doi: 10.1111/1753-6405.12113 [DOI] [PubMed] [Google Scholar]
- 75.Clements TL, Rossi CA, Irish AK, Kibuuka H, Eller LA, Robb ML, et al. Chikungunya and O’nyong-nyong Viruses in Uganda: Implications for Diagnostics. Open Forum Infect Dis. 2019;6(3):ofz001. doi: 10.1093/ofid/ofz001 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Azhar EI, Madani TA, Kao M, Jamjoom G. A seroepidemiological study of rift valley fever virus among slaughter houses’ workers in Saudi Arabia. Int. J. Med. Med. Sci. 2010;2(4):111–115. [Google Scholar]
- 77.Zeng P, Ma L, Gao Z, Wang J, Liu J, Huang X, et al. A study of seroprevalence and rates of asymptomatic viremia of severe fever with thrombocytopenia syndrome virus among Chinese blood donors. Transfusion. 2015;55(5):965–971. doi: 10.1111/trf.12953 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Jöst H, Bürck-Kammerer S, Hütter G, Lattwein E, Lederer S, Litzba N, et al. Medical importance of Sindbis virus in south-west Germany. J Clin Virol. 2011;52(3):278–279. doi: 10.1016/j.jcv.2011.08.002 [DOI] [PubMed] [Google Scholar]
- 79.Sonnleitner ST, Lundström J, Baumgartner R, Simeoni J, Schennach H, Zelger R, et al. Investigations on California serogroup orthobunyaviruses in the Tyrols: first description of Tahyna virus in the Alps. Vector Borne Zoonotic Dis. 2014;14(4):272–277. doi: 10.1089/vbz.2013.1360 [DOI] [PubMed] [Google Scholar]
- 80.Brisbarre N, Attoui H, Gallian P, Di Bonito P, Giorgi C, Cantaloube JF, et al. Seroprevalence of Toscana virus in blood donors, France, 2007. Emerg Infect Dis. 2011;17(5):941–943. doi: 10.3201/eid1705.101052 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Tavares-Neto J, Travassos DR, Amélia PA, Morais-Souza H, Vasconcelos P, Travassos da Rosa. Freqüência de anticorpos neutralizantes contra o vesiculovirus Piry, em doadores de sangue de Uberaba, Minas Gerais, Brasil. [Frequency of neutralizing antibodies to the vesiculovirus Piry, in blood donors of Uberaba, Minas Gerais, Brazil]. Rev Inst Med Trop Sao Paulo. 1990;32(3):211–214. [PubMed] [Google Scholar]
- 82.Attatippaholkun N, Kosaisawe N, U-Pratya Y, Supraditaporn P, Lorthongpanich C, Pattanapanyasat K, et al. Selective Tropism of Dengue Virus for Human Glycoprotein Ib [published correction appears in Sci Rep. 2018 Apr 12;8(1):6000]. Sci Rep. 2018;8(1):2688. doi: 10.1038/s41598-018-20914-z [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Petersen LR, Marfin AA. Shifting epidemiology of Flaviviridae. J Travel Med 2005; 12(Suppl. 1):S3–S11. doi: 10.2310/7060.2005.12052 [DOI] [PubMed] [Google Scholar]
- 84.Jones KE, Patel NG, Levy MA, Storeygard A, Balk D, Gittleman JL, et al. Global trends in emerging infectious diseases. Nature. 2008;451(7181):990–993. doi: 10.1038/nature06536 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85.Kim KH, Yi J, Kim G, Choi SJ, Jun KI, Kim NH, et al. Severe fever with thrombocytopenia syndrome, South Korea, 2012. Emerg Infect Dis 2013;19:1892–4. doi: 10.3201/eid1911.130792 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 86.Busch MP, Bloch EM, Kleinman S. Prevention of transfusion-transmitted infections. Blood. 2019;133(17):1854–1864. doi: 10.1182/blood-2018-11-833996 [DOI] [PubMed] [Google Scholar]
- 87.Fryk JJ, Marks DC, Hobson-Peters J, Prow NA, Watterson D, Hall RA, et al. Dengue and Chikungunya viruses in plasma are effectively inactivated after treatment with methylene blue and visible light. Transfusion. 2016; 56:2278–2285. doi: 10.1111/trf.13729 [DOI] [PubMed] [Google Scholar]
- 88.Papin JF, Floyd RA, Dittmer DP. Methylene blue photoinactivation abolishes West Nile virus infectivity in vivo. Antiviral Res. 2005; 68:84–87. doi: 10.1016/j.antiviral.2005.07.001 [DOI] [PubMed] [Google Scholar]
- 89.Laperche S. Francophone African Group for Research in Blood Transfusion. Multinational assessment of blood-borne virus testing and transfusion safety on the African continent. Transfusion. 2013;53(4):816–826. doi: 10.1111/j.1537-2995.2012.03797.x [DOI] [PubMed] [Google Scholar]
- 90.Prugger C, Laperche S, Murphy EL, Bloch EM, Kaidarova Z, Tafflet M, et al. Screening for transfusion transmissible infections using rapid diagnostic tests in Africa: a potential hazard to blood safety? Vox Sang. 2016;110(2):196–198. doi: 10.1111/vox.12327 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 91.Musso D, Gould E, Lanteri MC. Documentation of transfusion-transmitted arbovirus infections in endemic areas. Transfusion. 2016;56(12):3143–3144. doi: 10.1111/trf.13861 [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
(DOCX)
(DOCX)
(DOCX)
(DOCX)
(DOCX)
Data Availability Statement
All relevant data are within the manuscript and its Supporting Information files.