Abstract
Background
Meningioma is the most common primary CNS tumour. Most meningiomas are benign, and most patients are 65 years or older. Surgery is usually the primary treatment option. Most prior studies on early surgical outcomes in older patients with meningioma are small, and there is a lack of larger population-based studies to guide clinical decision-making. We aimed to explore the risks for perioperative mortality and morbidity in older patients with meningioma and to investigate changes in surgical incidence over time.
Methods
In this retrospective population-based study on patients in Sweden, 65 years or older with surgery 1999–2017 for meningioma, we used data from the Swedish Brain Tumour Registry. We analysed factors contributing to perioperative mortality and morbidity and used official demographic data to calculate yearly incidence of surgical procedures for meningioma.
Results
The final study cohort included 1676 patients with a 3.1% perioperative mortality and a 37.6% perioperative morbidity. In multivariate analysis, higher age showed a statistically significant association with higher perioperative mortality, whereas larger tumour size and having preoperative symptoms were associated with higher perioperative morbidity. A numerical increased rate of surgical interventions after 2012 was observed, without evidence of worsening short-term surgical outcomes.
Conclusions
Higher mortality with increased age and higher morbidity risk in larger and/or symptomatic tumours imply a possible benefit from considering surgery in selected older patients with a growing meningioma before the development of tumour-related symptoms. This study further underlines the need for a standardized method of reporting and classifying complications from neurosurgery.
Supplementary Information
The online version contains supplementary material available at 10.1007/s00701-022-05336-1.
Keywords: Meningioma, Surgical complications, Elderly, Neurosurgical complications, Perioperative complications
Introduction
Meningioma is the most common primary CNS tumour diagnosis, representing approximately 40% of all primary CNS tumours [19, 22]. With a median age at diagnosis of 66 years, most patients with a meningioma are 65 years or older, and there is a reported approximate 2.3:1 female predominance [19, 22]. The majority of meningiomas are benign, with a good prognosis. Ostrom et al. reports 10-year survival rates of 83.7% in benign meningiomas but with a worse prognosis with higher age and with malignant meningioma [22].
Although observation is the recommended therapeutic strategy for incidental, asymptomatic suspected meningiomas, surgery remains the primary treatment option for patients in good clinical condition and with rapidly growing or symptomatic tumours [13].
Prior studies on early surgical outcomes in older patients with meningioma have, with a few exceptions, been small, single-institution studies which are prone to selection bias, thus making the generalizability of the results questionable [1, 4, 12, 14, 24].
This warrants the need for larger, population-based studies to get results applicable to the clinical decision-making regarding older patients with meningioma.
In this study, we used real-world data from a national quality registry to investigate the pattern of surgical procedures for meningioma in older patients over time and in relation to demographic changes and explore risks for complications during the perioperative period.
Methods
Study design
We used data from the Swedish Brain Tumour Registry (SBTR) to perform a retrospective population- and registry-based study including all patients in Sweden who, according to the SBTR, had surgery for meningioma of any type at an age of 65 years or older between the years 1999 and 2017.
The Swedish Brain Tumour Registry
The SBTR is a nationwide registry that collected data on patients with brain tumours from 1999 to the end of 2017 when the registry was closed. All patients in Sweden with surgery for a primary brain tumour were included. The SBTR has, historically, had a near complete coverage in three of the six Swedish geographical healthcare regions [3]. In addition, a fourth region has retrospectively completed their data to reach an almost complete coverage and is, thus, included as a fourth high-coverage region in this study [25]. These four healthcare regions cover approximately 60% of the Swedish population, covering both urban and rural areas [29].
Study cohort
For the present study, all patients from the four SBTR high-coverage regions with a reported diagnosis of meningioma, a surgical date between 1999 and 2017 and age at surgery of 65 years or older were included. Diagnosis was determined from the reported SNOMED morphology code. All meningioma codes in the SBTR (code 953X/X) were included. Meningeal sarcomatosis (code 9539/3) was not included as it represents a primary sarcoma of the central nervous system [21]. The SNOMED coding table is available as Supplementary material (Section A).
The age of 65 years or older was chosen as this is a commonly used cut-off age for defining an older patient population [6, 12, 15, 24, 26].
Variables
Basic patient characteristics were collected or calculated from available data in the SBTR. Age was defined as age at date of surgery. Preoperative symptoms were available as three different variables: preoperative seizures, focal deficits and symptoms of increased intracranial pressure. During the initial study period (1999–2005), only focal deficits were registered. As a result, reporting and analyses using preoperative symptoms included only patients who underwent surgery from 2006 to 2017.
WHO/ECOG performance status (WHO-PS) was available as a preoperative variable and used in this study as a surrogate marker for being frail [20]. Being frail was defined as WHO-PS 3 or 4 (corresponding to a Karnofsky performance status of 40 or lower), whereas patients with WHO-PS of 2 were categorized as intermediate and those with WHO-PS 0 or 1 as fit.
Tumour size was reported between 2006 and 2015, defined in the SBTR as the largest diameter divided into three groups: < 4 cm, 4–6 cm or > 6 cm.
Tumour site has been reported in different ways throughout the years. From 2006 and onwards, it was possible to report multifocality (yes/no) as well as laterality, bilateral, posterior cranial fossa, skull base and central location (by multiple choice). For the present study, we combined these variables to form three groups: multifocal tumour, skull base (posterior fossa, skull base or central location) and supratentorial.
We divided the tumours according to WHO tumour grade into two groups (grade 1 and grades 2–3) using the SNOMED morphology codes (coding is available as Supplementary material, Section A).
Type of surgical intervention was reported as either biopsy, resection or radical resection in 1999–2015 with the addition of near radical resection from 2016. Simpson grading (1–5) was available from 2009 [28]. We used the Simpson grade when available and “type of surgical intervention” when Simpson grade was missing. For calculations, the combined information was dichotomized into radical resection (representing Simpson grades 1–3) and partial resection or biopsy (representing Simpson grades 4–5).
SBTR variables used for this study with years of availability and details on variable characteristics are presented as Supplementary material (Section B). Further details on data entry is available as Supplementary material (Section C).
Results were divided into the two surgical periods 1999–2008 and 2009–2017 for the purpose of baseline comparisons over time.
Outcome variables
Date of death was included in the registry from official sources at the Swedish Tax Agency (Skatteverket). Death within the first 30 days of surgery was defined as death attributed to surgery (perioperative mortality).
Perioperative complications were recorded (as yes/no) from the start of the SBTR in 1999 using three variables (local infection, local hematoma and thromboembolism) with the addition of new seizures, new or worsened focal deficits and reoperation (due to side effects) from 2006. For the purpose of the present study, a combined variable (perioperative morbidity) was created representing any type of perioperative complication. The combined variable is reported from 2006 and onwards due to the changes in variables. According to registry instructions, all complications registered occurred within the first 30 days after surgery.
Statistics
We presented age at surgery as median and interquartile range with variance between surgical periods analysed using Mann–Whitney U test. Categorical data variables were summarized using descriptive statistics. When possible, p values were calculated using Pearson’s χ2 test. The analysis of incidence rates of surgical procedures per year in relation to the age-specific population used logistic regression with Performed surgery (yes/no) as the dependent variable and year of surgery as the only independent variable. Demography data were collected from official sources at Statistics Sweden (Statistiska centralbyrån) [29].
Crude risk estimates with odds ratios (OR), confidence intervals (CI) and p values for perioperative morbidity and perioperative mortality were calculated using univariate logistic regression.
To calculate adjusted ORs and their corresponding CI for these outcomes, we used logistic regression with the following predefined independent variables (entered simultaneously): age, sex, WHO-PS frailty groups, preoperative symptoms present, tumour site, tumour size, type of surgical intervention (dichotomized Simpson grading) and tumour type.
Due to the different uses of variables in various periods, only data from years 2009–2015 were used for univariate and multivariate analyses (with the exception of “age groups and perioperative mortality” where the entire time span was used for univariate logistic regression).
IBM SPSS Statistics for Windows, version 25.0, Armonk, NY, USA, was used for all statistical calculations. Microsoft Excel 2016 was used for initial sorting, calculating legal sex, date of birth and for calculating time from surgery to date of death.
Statistical significance level was set to p < 0.05, and all CIs are at the 95% confidence level.
Results
Study cohort
We included 1676 patients to the final study cohort after initial sorting. Exclusion and data selection from the initial 17,731 records received from the SBTR are depicted in Fig. 1. The study population characteristics are reported in Table 1. Visual distribution of age by sex is available as Supplementary material (Section D).
Fig. 1.
Study flowchart. Data selection and reasons for exclusion. £, as described in the Methods sections; #, date of surgery superseded by official date of death
Table 1.
Baseline characteristics
| Surgical period | |||||
|---|---|---|---|---|---|
| Variable | Total | 1999–2008 | 2009–2017 | p value | |
| Total number of patients | N | 1676 | 715 | 961 | |
| Age | Median (IQR) | 72 (68–76) | 72 (68–77) | 72 (68–76) | 0.291 |
| Age groups | N (%) | ||||
| 65–69 | 592 (35.3) | 250 (35.0) | 342 (35.6) | 0.180 | |
| 70–74 | 508 (30.3) | 209 (29.2) | 299 (31.1) | ||
| 75–79 | 374 (22.3) | 177 (24.8) | 197 (20.5) | ||
| 80 + | 202 (12.1) | 79 (11.0) | 123 (12.8) | ||
| Sex | Female | 1137 (67.8) | 499 (69.8) | 638 (66.4) | 0.140 |
| Male | 539 (32.2) | 216 (30.2) | 323 (33.6) | ||
| Preoperative symptoms | N (% of valid per variable) | ||||
| Any symptoms present | 1023 (87.1) $ | 188 (88.3) # | 835 (86.9) | 0.588 | |
| Focal deficit | 721 (66.8) $ | 128 (63.7) # | 593 (67.5) | 0.295 | |
| Seizures | 249 (23.3) $ | 47 (24.5) # | 202 (23.0) | 0.662 | |
| Symptoms of intracranial pressure | 443 (41.4) $ | 66 (34.4) # | 377 (42.9) | 0.029 | |
| WHO/ECOG performance status | N (% of valid) | N = 1644 | N = 708 | N = 936 | |
| 0 | 630 (38.3) | 332 (46.9) | 298 (31.8) | < 0.001 | |
| 1 | 517 (31.4) | 189 (26.7) | 328 (35.0) | ||
| 2 | 281 (17.1) | 124 (17.5) | 157 (16.8) | ||
| 3 | 187 (11.4) | 49 (6.9) | 138 (14.7) | ||
| 4 | 29 (1.8) | 14 (2.0) | 15 (1.6) | ||
| By frailty group | Fit (0–1) | 1147 (69.8) | 521 (73.6) | 626 (66.9) | < 0.001 |
| Intermediate (2) | 281 (17.1) | 124 (17.5) | 157 (16.8) | ||
| Frail (3–4) | 216 (13.1) | 63 (8.9) | 153 (16.3) | ||
| Tumour size | N (% of valid) | N = 736 € | N = 149 # | N = 587 £ | |
| < 4 cm | 360 (48.9) € | 63 (42.3) # | 297 (50.6) £ | 0.192 | |
| 4–6 cm | 278 (37.8) € | 64 (43.0) # | 214 (36.5) £ | ||
| > 6 cm | 98 (13.3) € | 22 (14.8) # | 76 (12.9) £ | ||
| Tumour site | N (% of valid) | N = 1535 $ | N = 577 # | N = 958 | < 0.001 |
| Supratentorial | 1148 (74.8) $ | 442 (76.6) # | 706 (73.7) | ||
| Skull base | 266 (17.3) $ | 112 (19.4) # | 154 (16.1) | ||
| Multifocal | 121 (7.9) $ | 23 (4.0) # | 98 (10.2) | ||
| Tumour grade | N (%) | ||||
| WHO grade 1 | 1502 (89.6) | 669 (93.6) | 833 (86.7) | < 0.001 | |
| WHO grade 2–3 | 174 (10.4) | 46 (6.4) | 128 (13.3) | ||
| Type of surgical intervention | N (% of valid) | ||||
| Radical resection (Simpson 1–3) | 1420 (84.9) | 608 (85.5) | 812 (84.5) | 0.565 | |
| Partial res./biopsy (Simpson 4–5) | 252 (15.1) | 103 (14.5) | 149 (15.5) | ||
N, numbers; IQR, interquartile range. Years: $, 2006–2017; €, 2006–2015; #, 2006–2008; £, 2009–2015
The overall female/male ratio was approximately 2:1 (68%, n = 1137 female, and 32%, n = 539 male).
Most patients (87.1%, n = 1023) had one or more preoperative symptom/-s. From the 1000 patients with specified preoperative symptoms 63.5% (n = 635) had one, 32.3% (n = 323) had two, and 4.2% (n = 42) had three.
The differences in patient and tumour characteristics between the surgical periods proved statistically significant concerning WHO-PS (including frailty groups), tumour site, tumour grade and for having preoperative symptoms of increased intracranial pressure. Notably 10.2% (n = 98) had a multifocal tumour in the later period, compared to 4.0% (n = 23) in the earlier.
Perioperative mortality
The overall 30-day mortality was 3.1% (n = 52) as depicted in Table 2, with no statistically significant difference between the surgical periods.
Table 2.
Perioperative outcomes
| Surgical period | |||||
|---|---|---|---|---|---|
| Variable | Total | 1999–2008 | 2009–2017 | p value | |
| Perioperative mortality | N (%) | 52 (3.1) | 24 (3.4) | 28 (2.9) | 0.605 |
| Perioperative morbidity | N (% of valid per variable) | ||||
| Any complication | 441 (37.6) $ | 76 (35.7) # | 365 (38.0) | 0.530 | |
| Local infection | 111 (9.5) $ | 17 (8.0) # | 94 (9.8) | 0.417 | |
| Local hematoma | 193 (16.4) $ | 25 (11.7) # | 168 (17.5) | 0.041 | |
| Thromboembolism | 51 (4.4) $ | 7 (3.3) # | 44 (4.6) | 0.416 | |
| New seizures | 96 (8.2) $ | 13 (6.3) # | 83 (8.6) | 0.278 | |
| New focal deficit | 241 (20.7) $ | 44 (21.6) # | 197 (20.5) | 0.732 | |
| Reoperation | 70 (6.0) $ | 14 (6.8) # | 56 (5.8) | 0.583 | |
| Cause for reoperation | N (% of reoperations) | ||||
| Reoperation and local infection | 14 (20.0) $ | 4 (17.9) # | 10 (17.9) | 0.144 | |
| Reoperation and local hematoma | 32 (45.7) $ | 3 (21.4) # | 29 (51.8) | ||
| Reoperation, local infection and hematoma | 14 (20.0) $ | 3 (21.4) # | 11 (19.6) | ||
N, numbers; IQR, interquartile range. Years: $, 2006–2017; #, 2006–2008
Among patients who died within 30 days of surgery during the years with consistent reporting of complications (2006–2017), perioperative complications were simultaneously registered in 66.7% (n = 22). Worsened neurological function was the most common simultaneous complication with 81.8% (n = 18), followed by local hematoma with 59.1% (n = 13), reoperation due to side effects with 31.8% (n = 7), perioperative local infection with 27.3% (n = 6), new or worsened seizures with 27.3% (n = 6) and thromboembolism with 9.1% (n = 2).
Unadjusted and adjusted ORs for perioperative mortality are summarized in Table 3. While being frail (determined by WHO-PS), having a larger than 6 cm tumour and higher age showed statistically significant results in the univariate logistic regression, only higher age remained with a statistically significant influence to the outcome perioperative mortality in multivariate analysis. Hosmer and Lemeshow test for goodness of fit shows support for our adjusted model (p = 0.458).
Table 3.
Perioperative mortality
| Variable | Crude OR (CI) | p value | Adjusted OR (CI) | p value |
|---|---|---|---|---|
| Age at surgery | 1.134 (1.048–1.226) | 0.002 | 1.135 (1.026–1.255) | 0.014 |
| Sex (f/m) | 1.086 (0.422–2.793) | 0.865 | 1.528 (0.487–4.790) | 0.467 |
| WHO performance status | 0.003 # | 0.318 # | ||
| 0–1 vs 2 | 3.172 (0.839–12.001) | 0.089 | 1.649 (0.360–7.554) | 0.520 |
| 0–1 vs 3–4 | 7.146 (2.291–22.289) | < 0.001 | 2.843 (0.734–11.016) | 0.131 |
| Preoperative symptoms (no vs yes) | ||||
| Symptoms present | 2.753 (0.363–20.869) | 0.327 | 1.076 (0.122–9.493) | 0.948 |
| Focal deficit | 0.942 (0.353–2.515) | 0.905 | ||
| Seizures | 1.895 (0.733–4.898) | 0.187 | ||
| Symptoms of intracranial pressure | 0.764 (0.298–2.116) | 0.644 | ||
| Tumour site | 0.445 # | 0.079 # | ||
| Supratentorial vs skull base | 1.974 (0.682–5.717) | 0.210 | 3.912 (1.039–14.728) | 0.044 |
| Supratentorial vs multifocal | 1.437 (0.314–6.573) | 0.640 | 4.098 (0.721–23.291) | 0.112 |
| Tumour size | 0.017 # | 0.298 # | ||
| < 4 cm vs 4–6 cm | 2.113 (0.589–7.581) | 0.251 | 1.464 (0.354–6.057) | 0.599 |
| < 4 cm vs > 6 cm | 6.279 (1.725–22.848) | 0.005 | 3.191 (0.700–14.542) | 0.134 |
| Type of surgery | ||||
| Radical vs non-radical/biopsy | 2.649 (0.985–7.127) | 0.054 | 3.185 (0.971–10.446) | 0.056 |
| Tumour type | ||||
| WHO grade 1 vs 2–3 | 2.306 (0.812–6.551) | 0.117 | 1.280 (0.308–5.326) | 0.734 |
Odds ratio and 95% confidence interval for perioperative morbidity; #, variable p value
Table 4 shows the association of age (in 5-year groups) with perioperative mortality, showing statistically significant higher risk of perioperative mortality in the two oldest age groups (Pearson’s χ2 test: p < 0.001).
Table 4.
Age groups and perioperative mortality
| Perioperative mortality | ||||
|---|---|---|---|---|
| Age at surgery | No, n (%) | Yes, n (%) | Crude OR (CI) | p value |
| 65–69 | 585 (98.8) | 7 (1.2) | ||
| 70–74 | 496 (97.6) | 12 (2.4) | 2.022 (0.790–5.175) | 0.142 |
| 75–79 | 359 (96.0) | 15 (4.0) | 3.492 (1.410–8.646) | 0.007 |
| > 80 | 184 (91.1) | 18 (8.9) | 8.175 (3.362–19.881) | < 0.001 |
Numbers and percentage for each age group. Unadjusted OR and 95% CI for perioperative mortality from logistic regression with age 65–69 as index. Variable p value < 0.001
Perioperative morbidity
Perioperative morbidity is presented in Table 2. In total, 37.6% (n = 441) suffered from perioperative morbidity of any kind. There were no statistically significant differences in overall perioperative morbidity between the surgical periods, nor regarding any of the available types of complications, except for local hematoma. Complications per patient showed no statistically significant changes between the surgical periods (p = 0.811), and in total 19.7% (n = 231) had one, 10.2% (n = 119) had two, and 7.6% (n = 89) had three or more listed complications.
The summary of OR for perioperative morbidity is depicted in Table 5. Univariate analysis showed being frail (determined by WHO-PS), having preoperative symptoms, having a larger tumour or the tumour being WHO grades 2–3, as statistically significantly correlated to a higher risk of suffering from perioperative morbidity. In the multivariate analysis, however, only larger tumour size and having preoperative symptoms made an independent statistically significant contribution to the outcome. Hosmer and Lemeshow test for goodness of fit indicates support for the adjusted model (p = 0.277).
Table 5.
Perioperative morbidity
| Variable | Crude OR (CI) | p value | Adjusted OR (CI) | p value |
|---|---|---|---|---|
| Age at surgery | 1.011 (0.983–1.039) | 0.458 | 0.998 (0.965–1.033) | 0.916 |
| Sex (f/m) | 1.112 (0.812–1.522) | 0.509 | 1.025 (0.700–1.503) | 0.898 |
| WHO performance status | 0.046 # | 0.136 # | ||
| 0–1 vs 2 | 0.884 (0.578–1.351) | 0.569 | 0.766 (0.465–1.261) | 0.295 |
| 0–1 vs 3–4 | 1.615 (1.064–2.453) | 0.024 | 1.413 (0.859–2.324) | 0.173 |
| Preoperative symptoms (no vs yes) | ||||
| Symptoms present | 1.823 (1.123–2.960) | 0.015 | 2.030 (1.128–3.654) | 0.018 |
| Focal deficit | 1.522 (1.074–2.157) | 0.018 | ||
| Seizures | 1.445 (1.008–2.072) | 0.045 | ||
| Symptoms of intracranial pressure | 0.928 (0.671–1.283) | 0.650 | ||
| Tumour site | 0.184 # | 0.254 # | ||
| Supratentorial vs skull base | 0.829 (0.543–1.266) | 0.385 | 0.805 (0.483–1.340) | 0.404 |
| Supratentorial vs multifocal | 1.488 (0.881–2.514) | 0.137 | 1.505 (0.810–2.794) | 0.196 |
| Tumour size | < 0.001 # | 0.006 # | ||
| < 4 cm vs 4–6 cm | 1.747 (1.207–2.529) | 0.003 | 1.647 (1.100–2.466) | 0.015 |
| < 4 cm vs > 6 cm | 2.586 (1.545–4.328) | < 0.001 | 2.274 (1.294–3.997) | 0.004 |
| Type of surgery | ||||
| Radical vs non-radical/biopsy | 1.204 (0.797–1.820) | 0.378 | 1.350 (0.832–2.191) | 0.224 |
| Tumour type | ||||
| WHO grade 1 vs 2–3 | 1.725 (1.126–2.643) | 0.012 | 1.447 (0.876–2.391) | 0.149 |
Odds ratio and 95% confidence interval for perioperative morbidity; #, variable p value
Incidence rates of surgical procedures over time
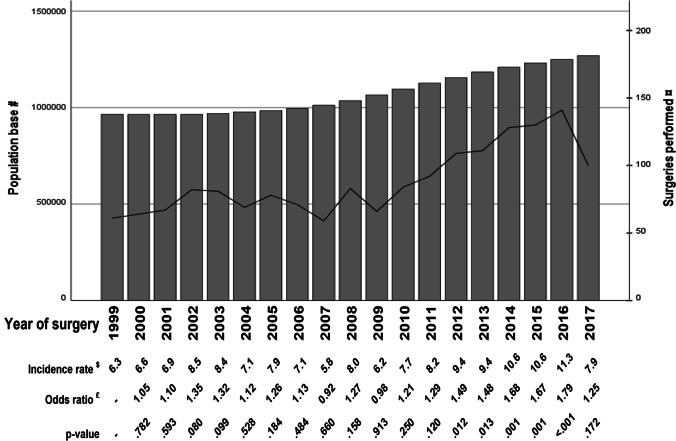
The comparison of number of surgeries performed each year and the population (older than 65 years) of each year is reported in Fig. 2. The overall logistic regression of number of surgeries performed on this age group over time proved statistically significant (p < 0.001). The increased incidence of years 2012 to 2016 was statistically significantly different from the index year 1999.
Fig. 2.
Population base and number of surgeries by year of surgery. N of persons age 65 years or older living in the studied healthcare regions and number of surgeries performed, incidence rate, OR for having surgery and corresponding p value by year of surgery. #, N of persons age 65 years or older (bars); ¤, N of surgeries performed (line); $, incidence rate of surgery per 100,000 for each year; £, OR for having surgery from univariate logistic regression with 1999 as index year. p value for the regression < 0.001
Discussion
In this retrospective population-based registry study on patients in Sweden, 65 years or older, we showed that higher age is a major prognostic factor for perioperative mortality after meningioma surgery. In addition, larger tumour size and having preoperative symptoms were associated with increased risk for perioperative complications. These findings of risk factors for perioperative mortality and perioperative morbidity imply that it could be beneficial to consider surgery in older patients with a growing meningioma before the development of tumour-related symptoms.
Our evaluation of incidence rates of surgical procedures over time showed a relatively stable curve until 2012, with a trend towards an increased rate of surgical interventions afterwards, without evidence of worsening short-term surgical outcomes.
Perioperative mortality
We observed a higher perioperative mortality by age which is in accordance to prior studies [1, 4, 14, 30]. The perioperative mortality rates in prior smaller cohorts which are prone to selection bias vary greatly, from 0% in some recent cohorts[17, 23] to more than 20% in some historical cohorts [10, 18]. However, our perioperative mortality rates and the finding of higher perioperative mortality with increasing age correspond well with other large cohorts as the studies by Grossman et al. (3.2% inpatient mortality, 65 years and older), Bateman et al. (4% inpatient mortality, 70 years and older) and Albert et al. (1.4% 30-day mortality in age 61–70; 2.4% in age 71–80; 6.9% in age > 80) [1, 4, 14]. In comparison to cohorts with younger patient populations, Corell et al., with data from the SBTR but with all ages included, showed a 1.5% 30-day mortality, and the younger cohorts in the study by Albert et al. had 0.7% 30-day mortality in ages 18–60, clearly demonstrating the increased perioperative mortality by age [1, 9]. High age being an independent risk factor for this outcome in multivariate analysis has been previously shown in several studies [4, 14, 30].
Perioperative morbidity
When looking at perioperative morbidity or perioperative complications, the published studies vary greatly in terms of the occurrence of complications, as summarized in two literature reviews [12, 24]. Eksi et al. calculated the mean occurrence of postsurgical complications to 37.1% with data from 23 studies on older patients with meningioma which is in accordance to our findings with 37.6% overall perioperative morbidity [12]. Poon et al. chose not to meta-analyse complication data because of the wide range of reported complication rates (2.7–29.8% in five studies) and the heterogeneity of eligible studies [24].
Regarding cohort studies investigating the perioperative morbidity after surgery for meningioma in older patients, Bateman et al. showed 53.2% adverse outcomes in patients aged 70 years or older [4], and Grossman et al. had a total complication rate of 17.5% in patients 65 years or older [14]. These differences in outcomes highlight the need for an internationally agreed convention for defining and grading complications after meningioma surgery to enable benchmarking and valuable comparisons among different cohorts. The proposed scoring system by Clavien and Dindo is one such possibility [7, 16].
Incidence rates of surgical procedures over time
Our evaluation of incidence of surgical interventions showed a relatively stable curve over time, with the later years 2012–2016 deviating from the expected increase caused by the increase of the age-specific population. This observation along with the absence of an increased perioperative mortality or increased perioperative morbidity over time could indicate that minor changes in indications for meningioma surgery might have occurred or that an increased overall meningioma incidence might be the reason for the transient increase in surgical procedures.
Nilsson et al. reported no evidence for increased incidence of meningioma in Sweden during partially overlapping years but rather a slight decrease in the older patient group, perhaps owing to a higher chance of early incidental discovery [19]. Speculatively, this could indicate that our slightly increased incidence of surgery might have an underlying larger increase in true incidence of performed surgery, considering the potential decrease in the incidence of meningioma in older patients.
In our cohort, there were no statistically significant differences over time regarding major preoperative symptoms, but multifocal tumours and frail patients were more common in the later surgical period. These findings imply that there might be an underlying drift in the Swedish Neurosurgical Society towards suggesting surgery for patients older than 65 years of age, with more complex meningiomas than earlier. If this is the case, this shift regarding the indication for meningioma surgery has been managed without the cost of worse short-term outcomes.
Strengths and limitations
The major strengths of this study were the population coverage and the large number of included patients. There are few population-based multicentre studies focusing on the perioperative outcome of older meningioma patients. With 1676 patients aged 65 and above, this is one of very few studies presenting results from more than 1000 patients [1, 4, 12, 14, 24]. The large number of patients has allowed us to perform regression analyses making our findings more robust compared to smaller studies. In addition, the access to official demographic data for the covered parts of the country has made it possible to evaluate the changes in surgical incidence over time in relation to the increase of the age-specific population. The SBTR recorded patients that had undergone surgery, meaning that we do not have data to compare these changes with changes in the total numbers of patients with meningioma.
Our study has several limitations that deserve discussion. First, the outcome variables regarding perioperative morbidity were recorded without grading of severity or information on permanence. In addition, the time where each complication occurred during the perioperative period could not be determined nor the outcome of each complication. Of note, all the variables on complications were retrospectively derived from hospital records, a method that has known issues in comparison with patient reported outcome measures [11]. In the same manner, the preoperative symptom variables are dichotomous and have no grading of severity of symptoms. We can, however, assume that the symptoms must have had a high degree of impact on the patients to be recorded. Furthermore, we lack potentially relevant information (e.g. concurrent medication, comorbidities or peritumoural oedema) to assess commonly used meningioma grading scores and to provide a more comprehensive frailty assessment other than WHO-PS [2, 5, 8, 27].
An additional limitation is the differences in recorded variables throughout the years that the SBTR covers. As an example, even though records of type of surgery were available for the entire timeframe of the registry (divided in 3 or 4 levels), Simpson grading was only available from 2009. These changes in variables, including the late use of Simpson grading, limit the available years of consistent reporting and thus the number of patients available for multivariate analysis.
Conclusion
Despite the caveats, this study presented results on the short-term outcome after surgery from one of the largest cohorts of older patients with meningioma. Higher age seems to be an independent risk factor in dying within 30 days of meningioma surgery, whereas tumour size and having preoperative symptoms from meningioma were associated with higher risk for perioperative complications. The latter findings imply that it could be beneficial to consider surgery in older patients with a growing meningioma before the development of tumour-related symptoms.
This study further underlines the need for a more standardized method of reporting and classifying complications from neurosurgery.
Supplementary information
Below is the link to the electronic supplementary material.
Acknowledgements
The authors express their gratitude to the SBTR staff at Cancercentrum Norr, for their kind assistance with the data extraction and explanations of registration routines and to all the individuals reporting data to the registry, making this research possible.
Abbreviations
- CI
Confidence intervals
- ECOG
Eastern Cooperative Oncology Group
- OR
Odds ratios
- SBTR
Swedish Brain Tumour Registry
- SNOMED
Systematized Nomenclature of Medicine
- WHO
World Health Organization
- WHO-PS
WHO/ECOG performance status
Author contribution
David Löfgren and Magnus Olivecrona contributed with conception and design of the study and acquisition of data. All authors contributed in analysis and interpretation of data and drafting and revising and final manuscript approval.
Funding
Open access funding provided by Örebro University. David Löfgren has obtained funding from the Research Committee of Region Örebro County (OLL-591961 and OLL-869421). All authors have received funding through the agreement concerning research and education of doctors (ALF) from Region Örebro County.
Data availability
The datasets generated during and/or analysed during the current study are not publicly available due to their sensitive personal nature but are available from the corresponding author on reasonable request.
Declarations
Ethics approval
This study was approved by the Regional Ethical Review Board, Uppsala, Sweden (Diary number 2016/014). All procedures performed were in accordance with the approval and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Consent to participate
In accordance with Swedish legislation and regulations regarding patient consent for participation in a national quality registry, before undergoing surgery, patients were given written information about SBTR including the choice to opt out from registration in SBTR or for their data to be removed from the registry at any time.
Conflict of interest
David Löfgren and Magnus Olivecrona are members of the Swedish CNS Tumour Registry control group. Magnus Olivecrona is a previous member of the Swedish Brain Tumour Registry (SBTR) control group. Antonios Valachis reports no conflict of interest.
Footnotes
This article is part of the Topical Collection on Tumor – Meningioma
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Contributor Information
David Löfgren, Email: david.lofgren@regionorebrolan.se, Email: david.lofgren@oru.se.
Antonios Valachis, Email: antonios.valachis@oru.se.
Magnus Olivecrona, Email: magnus.olivecrona@oru.se.
References
- 1.Albert A, Lee A, Thomas TV, Vijayakumar S. Outcomes of benign meningioma in older patients in the United States. J Geriatr Oncol. 2020;11:709–717. doi: 10.1016/j.jgo.2019.10.017. [DOI] [PubMed] [Google Scholar]
- 2.Arienta C, Caroli M, Crotti F, Villani R. Treatment of intracranial meningiomas in patients over 70 years old. Acta Neurochir (Wien) 1990;107:47–55. doi: 10.1007/BF01402612. [DOI] [PubMed] [Google Scholar]
- 3.Asklund T, Malmstrom A, Bergqvist M, Bjor O, Henriksson R. Brain tumors in Sweden: data from a population-based registry 1999–2012. Acta Oncol. 2015;54:377–384. doi: 10.3109/0284186X.2014.975369. [DOI] [PubMed] [Google Scholar]
- 4.Bateman BT, Pile-Spellman J, Gutin PH, Berman MF (2005) Meningioma resection in the elderly: nationwide inpatient sample, 1998–2002. Neurosurgery 57:866–872; discussion 866–872. 10.1227/01.neu.0000179923.66729.87 [DOI] [PubMed]
- 5.Caroli M, Locatelli M, Prada F, Beretta F, Martinelli-Boneschi F, Campanella R, Arienta C. Surgery for intracranial meningiomas in the elderly: a clinical-radiological grading system as a predictor of outcome. J Neurosurg. 2005;102:290–294. doi: 10.3171/jns.2005.102.2.0290. [DOI] [PubMed] [Google Scholar]
- 6.Chen ZY, Zheng CH, Tang L, Su XY, Lu GH, Zhang CY, Xiao SW, Tan YF (2015) Intracranial meningioma surgery in the elderly (over 65 years): prognostic factors and outcome. Acta Neurochir (Wien) 157:1549–1557; discussion 1557. 10.1007/s00701-015-2502-9 [DOI] [PubMed]
- 7.Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, de Santibanes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M. The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg. 2009;250:187–196. doi: 10.1097/SLA.0b013e3181b13ca2. [DOI] [PubMed] [Google Scholar]
- 8.Cohen-Inbar O, Sviri GE, Soustiel JF, Zaaroor M (2011) The Geriatric Scoring System (GSS) in meningioma patients--validation. Acta Neurochir (Wien) 153:1501–1508; discussion 1508. 10.1007/s00701-011-1034-1 [DOI] [PubMed]
- 9.Corell A, Thurin E, Skoglund T, Farahmand D, Henriksson R, Rydenhag B, Gulati S, Bartek J, Jr, Jakola AS. Neurosurgical treatment and outcome patterns of meningioma in Sweden: a nationwide registry-based study. Acta Neurochir (Wien) 2019;161:333–341. doi: 10.1007/s00701-019-03799-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Djindjian M, Caron JP, Athayde AA, Fevrier MJ. Intracranial meningiomas in the elderly (over 70 years old). A retrospective study of 30 surgical cases. Acta Neurochir (Wien) 1988;90:121–123. doi: 10.1007/BF01560565. [DOI] [PubMed] [Google Scholar]
- 11.Drewes C, Sagberg LM, Jakola AS, Gulati S, Solheim O. Morbidity after intracranial tumor surgery: sensitivity and specificity of retrospective review of medical records compared with patient-reported outcomes at 30 days. J Neurosurg. 2015;123:972–977. doi: 10.3171/2014.12.JNS142206. [DOI] [PubMed] [Google Scholar]
- 12.Eksi MS, Canbolat C, Akbas A, Ozmen BB, Akpinar E, Usseli MI, Gungor A, Guduk M, Hacihanefioglu M, Ersen Danyeli A, Ozduman K, Pamir MN. Elderly patients with intracranial meningioma: surgical considerations in 228 patients with a comprehensive analysis of the literature. World Neurosurg. 2019;132:e350–e365. doi: 10.1016/j.wneu.2019.08.150. [DOI] [PubMed] [Google Scholar]
- 13.Goldbrunner R, Stavrinou P, Jenkinson MD, Sahm F, Mawrin C, Weber DC, Preusser M, Minniti G, Lund-Johansen M, Lefranc F, Houdart E, Sallabanda K, Le Rhun E, Nieuwenhuizen D, Tabatabai G, Soffietti R, Weller M. EANO guideline on the diagnosis and management of meningiomas. Neuro Oncol. 2021;23:1821–1834. doi: 10.1093/neuonc/noab150. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Grossman R, Mukherjee D, Chang DC, Bennett R, Brem H, Olivi A, Quinones-Hinojosa A. Preoperative Charlson comorbidity score predicts postoperative outcomes among older intracranial meningioma patients. World Neurosurg. 2011;75:279–285. doi: 10.1016/j.wneu.2010.09.003. [DOI] [PubMed] [Google Scholar]
- 15.Ikawa F, Kinoshita Y, Takeda M, Saito T, Yamaguchi S, Yamasaki F, Iida K, Sugiyama K, Arita K, Kurisu K. Review of current evidence regarding surgery in elderly patients with meningioma. Neurol Med Chir (Tokyo) 2017;57:521–533. doi: 10.2176/nmc.ra.2017-0011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Joubert C, Sellier A, Sahuc P, Beucler N, Desse N, Bernard C, Cungi PJ, Dagain A. Neurosurgery for intracranial meningioma in patients aged more than 80 years: benefits and rationale. Br J Neurosurg. 2021;35:470–475. doi: 10.1080/02688697.2021.1875397. [DOI] [PubMed] [Google Scholar]
- 17.Li Y, Lu D, Feng D, Cheng H, Huang Q, Zhao H, Chen P, Qin H, Cai Q. Management of incidental anterior skull base large and giant meningiomas in elderly patients. J Neurooncol. 2020;148:481–488. doi: 10.1007/s11060-020-03484-x. [DOI] [PubMed] [Google Scholar]
- 18.Mastronardi L, Ferrante L, Qasho R, Ferrari V, Tatarelli R, Fortuna A. Intracranial meningiomas in the 9th decade of life: a retrospective study of 17 surgical cases. Neurosurgery. 1995;36:270–274. doi: 10.1227/00006123-199502000-00005. [DOI] [PubMed] [Google Scholar]
- 19.Nilsson J, Jaras J, Henriksson R, Holgersson G, Bergstrom S, Estenberg J, Augustsson T, Bergqvist M. No evidence for increased brain tumour incidence in the Swedish National Cancer Register between years 1980–2012. Anticancer Res. 2019;39:791–796. doi: 10.21873/anticanres.13176. [DOI] [PubMed] [Google Scholar]
- 20.Oken MM, Creech RH, Tormey DC, Horton J, Davis TE, McFadden ET, Carbone PP. Toxicity and response criteria of the Eastern Cooperative Oncology Group. Am J Clin Oncol. 1982;5:649–655. doi: 10.1097/00000421-198212000-00014. [DOI] [PubMed] [Google Scholar]
- 21.Onofrio BM, Kernohan JW, Uihlein A. Primary meningeal sarcomatosis. A review of the literature and report of 12 cases. Cancer. 1962;15:1197–1208. doi: 10.1002/1097-0142(196211/12)15:6<1197::aid-cncr2820150617>3.0.co;2-1. [DOI] [PubMed] [Google Scholar]
- 22.Ostrom QT, Cioffi G, Waite K, Kruchko C, Barnholtz-Sloan JS. CBTRUS statistical report: primary brain and other central nervous system tumors diagnosed in the United States in 2014-2018. Neuro Oncol. 2021;23:iii1–iii105. doi: 10.1093/neuonc/noab200. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Poon MT, Fung LH, Pu JK, Leung GK. Outcome comparison between younger and older patients undergoing intracranial meningioma resections. J Neurooncol. 2013;114:219–227. doi: 10.1007/s11060-013-1173-8. [DOI] [PubMed] [Google Scholar]
- 24.Poon MT, Fung LH, Pu JK, Leung GK. Outcome of elderly patients undergoing intracranial meningioma resection–a systematic review and meta-analysis. Br J Neurosurg. 2014;28:303–309. doi: 10.3109/02688697.2013.841857. [DOI] [PubMed] [Google Scholar]
- 25.Regionalt cancercentrum norr (2018) [Nationellt kvalitetsregister för Hjärntumörer - Nationell rapport 1999–2017] (Swedish Brain Tumor Registry - National report 1999–2017). Onkologiskt centrum för norra sjukvårdsregionen,
- 26.Rockwood K, Song X, MacKnight C, Bergman H, Hogan DB, McDowell I, Mitnitski A. A global clinical measure of fitness and frailty in elderly people. CMAJ. 2005;173:489–495. doi: 10.1503/cmaj.050051. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Sacko O, Sesay M, Roux FE, Riem T, Grenier B, Liguoro D, Loiseau H (2007) Intracranial meningioma surgery in the ninth decade of life. Neurosurgery 61:950–954; discussion 955. 10.1227/01.neu.0000303190.80049.7d [DOI] [PubMed]
- 28.Simpson D. The recurrence of intracranial meningiomas after surgical treatment. J Neurol Neurosurg Psychiatry. 1957;20:22–39. doi: 10.1136/jnnp.20.1.22. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Statistics Sweden (2021) Population by region, marital status, age and sex. Year 1968 - 2020. https://www.scb.se. Accessed June 30 2021
- 30.Steinberger J, Bronheim RS, Vempati P, Oermann EK, Ladner TR, Lee NJ, Kothari P, Caridi JM, Shrivastava RK. Morbidity and mortality of meningioma resection increases in octogenarians. World Neurosurg. 2018;109:e16–e23. doi: 10.1016/j.wneu.2017.09.021. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
The datasets generated during and/or analysed during the current study are not publicly available due to their sensitive personal nature but are available from the corresponding author on reasonable request.