Abstract
Antopol Goldman lesion is a renal pelvis subepithelial hematoma or hemorrhage, a sporadic disease. Although the causes are not well established yet, multiple factors were linked. Radiology is the cornerstone for the diagnosis. However, it may be mistaken for renal tumors. Herein we present a case of a 17-year-old male who presented with recurrent flank pain and gross hematuria and was diagnosed with an Antopol Goldman lesion.
Keywords: Antopol goldman lesion, Hematuria, Case report
Introduction
Antopol Goldman lesion (AGL) is a sporadic disease [1]. It is described as a renal pelvis subepithelial hematoma or hemorrhage [1,2]. However, it may involve the renal calyces and proximal ureter [3,4]. Although several factors, such as excessive analgesic or anticoagulant medication use, diabetes mellitus, hypertension, hemophilia, etc., were linked to the development of this lesion, the definitive cause is not well established yet [1,5].
A universal presentation of AGL is hematuria associated with flank pain, which was noticed in most reported cases [1,2,6]. The lesion is unilateral and affects the elderly in most cases [2,6]. This clinical presentation and the associated radiological findings on imaging modalities may be mistaken for renal tumors. Therefore, diverting the management toward more invasive, unnecessary surgeries, since such lesions are now managed conservatively, highlights the importance of diagnosing such lesions [5–8].
Herein, we present a case of unilateral AGL in a young patient diagnosed based on clinical and radiological findings and resolved spontaneously with conservative management.
Case presentation
A 17-year-old male student presented to the emergency room (ER) complaining of recurrent right flank pain and hematuria. The pain was intermittent, progressive, awakened him up from sleep, associated with vomiting and generalized fatigue, and relieved by analgesia given in the ER. The hematuria was painless, all over the stream, with blood clots. The patient denied any history of analgesic use, anticoagulation use, trauma, abdominal pain, facial puffiness, leg swelling, and kidney stones. On physical examination, the patient was in distress due to pain. After administering analgesia, the patient had no facial or leg swelling, abdominal masses, or skin changes. Laboratory tests were ordered, including complete blood count, blood smear, liver function tests, kidney function tests, urine analysis, and culture. They came back standard apart from thrombocytosis. The patient has no family history of hematological disorders or malignancies.
In addition, genetic testing for bleeding disorders did not reveal any abnormalities. A contrasted computer Tomography tomography(CT) scan was ordered. It showed a hyperdense blood density lesion occupying the right lower renal calyx and extending to the renal pelvis—Fig. 1. In addition, no enhancement of the lesion was seen in Fig. 2. He was diagnosed with AGL depending on the findings of the CT scan. A follow-up magnetic resonance image (MRI) was ordered 2 weeks after the CT, showing an interval decrease in size, Fig. 3, without enhancement of the lesion (Fig. 4). The patient's symptoms have come to a full resolution 4 weeks after the MRI, and he is doing well.
Fig. 1.
A coronal non-enhanced CT image shows a hyperdense blood density lesion occupying the right lower renal calyx and extending to the renal pelvis.
Fig. 2.
Axial contrast-enhanced CT image shows no enhancement of the lesion.
Fig. 3.
A coronal T2 MRI showed an interval decrease in the lesion size.
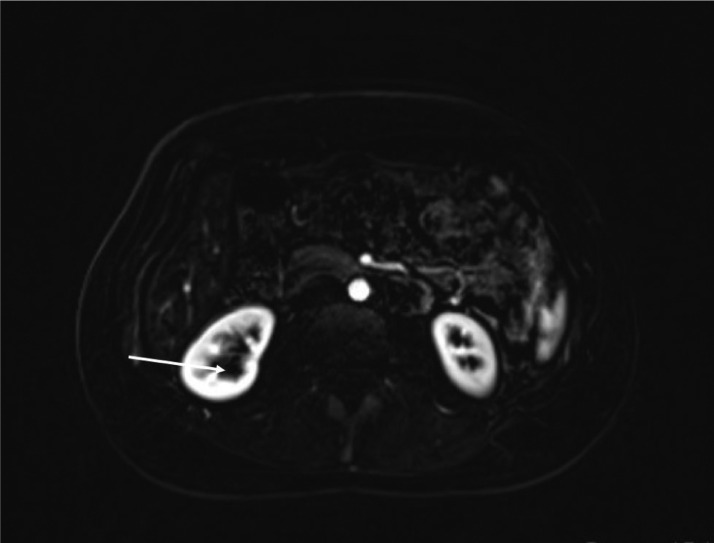
Fig. 4.
Axial contrast-enhanced MR fat sat image shows no enhancement of this lesion. No other enhancing lesions.
Discussion
With only around 50 cases being reported in the literature, AGL remains a rare condition [1]. Most of the time, it has been used to describe renal pelvic hematoma, despite that renal calyces and proximal ureter involvement may rarely happen [7,8]. In our case, the hematoma occupied the lower calyx and the renal pelvic. Most reported cases were unilateral, affecting the elderly without propensity toward gender or specific side [3,4]. However, the patient in our case was 17 years old, considered much younger than the age that AGL patients present in [4].
The exact etiology of AGL is not clear until now. Nevertheless, a strong correlation with various factors was established throughout reported cases over time [1]. These factors include diabetes mellitus, hypertension, non-steroidal anti-inflammatory drugs, anticoagulants, hemophilia, amyloidosis, trauma, congenital malformations, and others (1,3). Furthermore, as in our case, hematuria and flank pain are considered characteristics of patients with AGL, as they are found in most cases with minor differences in their character [2,6]. Meanwhile, spontaneous bleeding from other places, such as the nose or oral mucosa, is not commonly encountered in patients [4]. However, episodes of epistaxis were present in our case several years prior to the onset of hematuria.
As it was challenging to distinguish AGL from renal and collecting system tumors based on imaging techniques, histopathological examination after nephrectomy was the diagnostic modality at the beginning [3,4]. Due to this, many unnecessary nephrectomies were done for patients with AGL [1,6]. However, as reported cases increased, clinical presentation and radiological findings such as Computer Tomography (CT) scan and Ultrasound (US) became the mainstay of diagnosis [1], [2], [3]. Imaging modalities may demonstrate a filling defect, mural thickening, and luminal narrowing of the renal pelvis and proximal ureters, which may be misdiagnosed as a tumor. However, hydronephrosis is rarely found [4,5].
It is of high importance to mention that CT, specifically the non-enhanced phase, is considered the best to diagnose such lesion and superior to the US. It shows the hyperdense hemorrhagic component on pre-contrast images, and shows non-enhancement of the lesion on contrast enhanced images [3,5].
AGL can be easily mistaken with other serious pathologies, but it was managed with partial or complete nephrectomies in most cases [4,6]. Fortunately, the first AGL to be treated conservatively was reported in 2008 [8]. Nowadays, conservative management, watchful waiting alongside withdrawing and controlling offending factors such as diabetes mellitus, hypertension, hemophilia, amyloidosis, anticoagulants reversal, and others are becoming the mainstay of management [1–3]. Arterial embolization was reported to be used when the lesion is refractory to conservative measures [8].
Conclusion
AGL is a rare condition with yet no clear etiology. Patients primarily present with flank pain and hematuria. AGL used to be misdiagnosed with malignancy causing many unnecessary nephrectomies. However, clinical presentation and imaging techniques are the mainstays of diagnosis, and it is managed conservatively.
Patient consent
Written informed consent for the publication of this case report was obtained from the patient.
Footnotes
Competing Interests: There is no conflict of interest to declare.
References
- 1.Swati S., Arun C., Anupam C., Udupa CBK, Kanthilata P., Vishwapriya M.G. Lésion d'Antopol-Goldman (Antopol-Goldman lesion): spontaneous renal pelvic subepithelial hematoma. Indian J Pathol Microbiol. 2022;65(1):173–175. doi: 10.4103/ijpm.ijpm_111_21. [DOI] [PubMed] [Google Scholar]
- 2.Sahin T.K., Aladag E., Setterzade E., Guven G.S., Haznedaroglu I.C., Aksu S. Spontaneous subepithelial hemorrhage of renal pelvis and ureter (Antopol-Goldman lesion) in hemophilia A patient with an inhibitor: case report and review of the literature. Medicine. 2020;99(26):e20851. doi: 10.1097/MD.0000000000020851. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Seker K.G., Şam E., Özdemir O., Yigitbasi I., Evren I., Güner E., et al. A rare case mimicking collecting system tumor: Antopol-Goldman lesion. Bull Urooncol. 2018;17:150–152. [Google Scholar]
- 4.Zelaya R., Byerly D., Zarka A. Spontaneous suburothelial hemorrhage associated with forniceal rupture and retroperitoneal hemorrhage. Cureus. 2022;14(4):e23728. doi: 10.7759/cureus.23728. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Fonseca E., Torres R., Scoppetta L., Nomura C.H. Spontaneous subepithelial hemorrhage: the Antopol-Goldman lesion. Einstein (Sao Paulo, Brazil) 2021;19:eAI5829. doi: 10.31744/einstein_journal/2021AI5829. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Eccher A., Brunelli M., Gobbo S., Ghimenton C., Grosso G., Iannucci A., et al. Subepithelial pelvic hematoma (Antopol–Goldman lesion) simulating renal neoplasm: report of a case and review of the literature. Int J Surg Pathol. 2009;17(3):264–267. doi: 10.1177/1066896908330482. [DOI] [PubMed] [Google Scholar]
- 7.Jeevanandham B, Dhanapal V, Ramachandran R, Vaishnavi R. Induction chemotherapy causing pseudolesion in the kidney Antopol-Goldman lesion: a radiological diagnosis and follow up with review of literature. Int J Sci Res. 2018;7(3):6–7. [Google Scholar]
- 8.Altay B., Barışık C.C., Erkurt B., Kiremit M.C. Subepithelial pelvic hematoma of the kidney (Antopol-Goldman Lesion) Turk J Urol. 2015;41(1):48–50. doi: 10.5152/tud.2014.48208. [DOI] [PMC free article] [PubMed] [Google Scholar]