Abstract
TRK inhibition can lead to on-target neurologic adverse events. Two cases illustrate the development of neuropathic arthropathy as a side effect of entrectinib. After starting entrectinib, both patients developed foot pain, swelling, and sensory changes with magnetic resonance imaging revealing marrow edema. Providers should have a low threshold to investigate foot pain or gait abnormalities thoroughly with magnetic resonance imaging and referral to specialists to aid in the diagnosis of neuropathic arthropathy, with consideration to transition to an alternative agent.
Keywords: Entrectinib, NTRK, Neuropathic Charcot arthropathy, Case report
Introduction
NTRK genes encode for TRKs, specifically TRKA, TRKB, and TRKC. These transmembrane proteins bind neutrophins and affect the differentiation and survival of sensory neurons. Pathogenic NTRK fusions, found in approximately 0.26% of all cancers, lead to neoplastic changes that can be treated with tyrosine kinase inhibitors, such as larotrectinib and entrectinib, to block abnormal TRK constitutive activation.1 Entrectinib also has activity in the treatment of ROS1-fused NSCLC.
Case Presentation
Case 1
Patient 1 is a 56-year-old man with polycystic kidney disease diagnosed with having metastatic GOPC-ROS1–rearranged NSCLC 3.5 years ago and initially received crizotinib. He switched to entrectinib due to worsening renal function.
After switching to entrectinib, he developed perineal numbness and dysgeusia. This was followed by painful ankle swelling after 9 months—without fevers or joint erythema—necessitating a controlled ankle motion boot. Weight-bearing and ankle range of motion exacerbated the symptoms. Results of magnetic resonance imaging (MRI) (Fig. 1) revealed diffuse bone marrow edema in the right ankle and hindfoot bones, joint effusion, subchondral fluid collections within the calcaneus, and soft tissue swelling consistent with either infection or neuropathic arthropathy. Subsequent radiograph results revealed pes planus and hindfoot valgus. Clinically, he developed severe planovalgus deformities of both ankles with loss of ankle mobility.
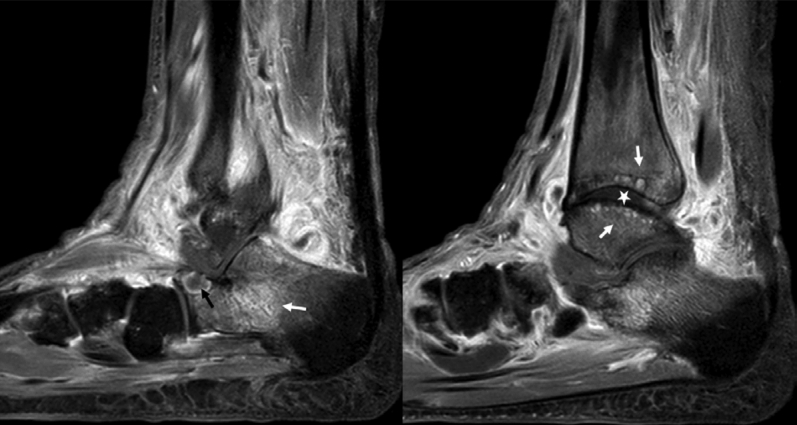
Figure 1.
Sagittal view magnetic resonance images of the right foot (T1-weighted, fat-suppressed without contrast) of patient 1 revealing diffuse bone marrow edema in the ankle and hindfoot bones (white arrows), subchondral fluid collections in the body of the calcaneus (black arrow), and a joint effusion (star).
The patient received two courses of antibiotics, which temporarily aided his symptoms. After evaluation by sports medicine and orthopedics, he was recommended to use bilateral dynamic carbon fiber ankle foot orthoses due to his ankle deformity and dysfunction likely caused by Charcot neuropathy. He was also found to have severe tricompartmental knee arthritis and effusions. He transitioned from entrectinib to crizotinib 21 months after starting.
Results of electromyography and nerve conduction studies 4 months after stopping entrectinib were consistent with severe sensorimotor polyneuropathy. Results of sensory nerve conduction studies of the lower extremities (sural and superficial peroneal nerves) and motor conduction studies of the peroneal nerves were nonreactive, and there was no abnormal electrical activity suggestive of a myopathic process.
The patient is planned for bilateral knee replacements and right subtalar arthrodesis due to rapid progression of ankle arthritis.
Case 2
Patient 2 is a 48-year-old woman with no medical history diagnosed with having metastatic ROS1+ NSCLC by fluorescence in situ hybridization 2.5 years ago.
She noticed bilateral lower extremity edema 4 months after starting first-line entrectinib, changes in sensation in her feet after 9 months, and worsened carpal tunnel in bilateral wrists and tongue numbness. By 14 months, she developed pain in both feet, worsened with standing and walking. Her gait became antalgic and unsteady due to pain and diminished sensation in the right greater than the left foot. Strength in knee extension, knee flexion, ankle dorsiflexion, and ankle plantarflexion was maintained. She exhibited tenderness to palpation of the metatarsals and midfoot bones with no laxity or instability of ankle ligaments.
Radiograph results of both feet revealed soft tissue swelling without fractures or deformities. Furthermore, MRI results of bilateral feet (Fig. 2) revealed marrow edema within the fourth metatarsal, fifth metatarsal, and cuboid on the right, and on the left within the fourth metatarsal, fifth metatarsal, and midfoot suggestive of an acute stress reaction.
Figure 2.
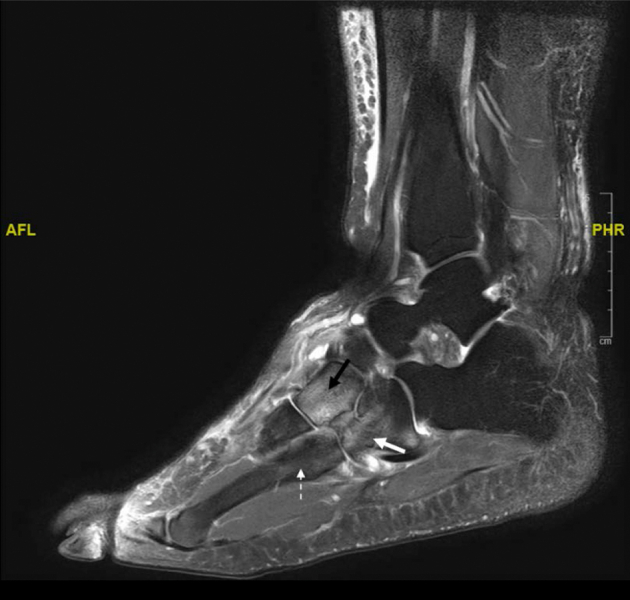
Sagittal view magnetic resonance image of the left foot (T1-weighted, fat-suppressed without contrast) of patient 2 revealing nonspecific marrow edema within the cuboid (white arrow), lateral cuneiform (black arrow), and fourth proximal metatarsal shaft (dotted arrow).
Owing to concern for neuropathic arthropathy, the patient tapered off entrectinib 15 months after starting. She was seen by physical medicine and rehabilitation with concern for neuropathic arthropathy and was prescribed a right controlled ankle motion pneumatic boot to offload the foot and ankle when walking. The patient noticed substantial improvement in her pain a month after and was transitioned to crizotinib.
Discussion
Neuropathic or Charcot arthropathy occurs secondary to progressive denervation leading to joint destruction, most often in patients with diabetes, particularly affecting the feet and ankles. The pathophysiology is a combination of neuropathy and angiopathy. Neuropathy allows microtrauma and cumulative stress to occur, whereas angiopathy from changes in the blood vessel smooth muscle innervation leads to arteriovenous shunting and enrichment of monocytes and osteoclasts causing local osteopenia and bony destruction. The diagnosis is both clinical and radiological. MRI can detect marrow edema and microfractures. Demineralization and fragmentation of the bones can lead to sclerotic changes, fusion, dislocation, and deformity.2
On-target adverse events, many specific to NTRK inhibition, are well documented. The European Medicines Agency compiled a safety analysis of 504 patients treated with entrectinib. Neurologic adverse events included dysgeusia, weight gain, peripheral neuropathy, cognitive changes, ataxia, syncope, and seizures. Furthermore, 6.2% of patients experienced fractures.3
TRK inactivation leading to neurologic dysfunction and subsequent fractures is mechanistically plausible. Congenital insensitivity to pain with anhidrosis is a rare autosomal recessive sensory autonomic neuropathy defined by alterations in NTRK1 and characterized by lack of pain sensation and anhidrosis, with resultant episodic fevers, repeated painless fractures, Charcot arthropathy, and osteomyelitis. In a case series of patients with congenital insensitivity to pain with anhidrosis, one boy developed multiple lower extremity fractures and Charcot arthropathy of the left ankle by age 5 years whereas another developed bilateral Charcot arthropathy and osteonecrosis of the ankles by age 3 years.4
In this case series, neither patient exhibited preexisting neuropathy or conditions predisposing to neuropathy including diabetes. Patient 1 was found to have severe sensorimotor polyneuropathy on electromyography and nerve conduction studies with MRI changes consistent with neuropathic arthropathy with improvement in symptoms using ankle foot orthoses and stopping entrectinib. Patient 2 was found to have bony edema concerning for early Charcot arthropathy with improvement after transitioning off entrectinib and bracing.
Conclusions
Neuropathic arthropathy may be an underrecognized complication of NTRK tyrosine kinase inhibitor therapy. Described are two cases of progressive lower extremity pain found to have neuropathic arthropathy, which improved after appropriate foot bracing and entrectinib cessation. Physicians should recognize these symptoms and refer to the appropriate specialties for aid in management.
CRediT Authorship Contribution Statement
Nicholas P. Giustini: Conceptualization, Data curation, Writing—original draft.
Hanna Oh: Writing—review and editing, Visualization.
Keith D. Eaton: Conceptualization, Methodology, Investigation, Writing—review and editing, Supervision.
Acknowledgments
The authors of this manuscript obtained written or verbal consent from the patients described in this case series to have their anonymized information published in the medical literature.
Footnotes
Disclosure: The authors declare no conflict of interest.
Cite this article as: Giustini NP, Oh H, Eaton KD, et al. Development of neuropathic arthropathy with entrectinib: case report. JTO Clin Res Rep. 2022;3:100419
References
- 1.Amatu A., Sartore-Bianchi A., Bencardino K., Pizzutilo E.G., Tosi F., Siena S. Tropomyosin receptor kinase (TRK) biology and the role of NTRK gene fusions in cancer. Ann Oncol. 2019;30 doi: 10.1093/annonc/mdz383. viii5–viii15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Trieb K. The Charcot foot. Bone Joint J. 2016;98-B:1155–1159. doi: 10.1302/0301-620X.98B9.37038. [DOI] [PubMed] [Google Scholar]
- 3.Delgado J., Pean E., Melchiorri D., et al. The European Medicines Agency Review of entrectinib for the treatment of adult or paediatric patients with solid tumours who have a neurotrophic tyrosine receptor kinase gene fusions and adult patients with non-small-cell lung cancer harbouring ROS1 rearrangements. ESMO Open. 2021;6 doi: 10.1016/j.esmoop.2021.100087. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Lv F., Xu X-Jie, Song Y.W., et al. Recurrent and novel mutations in the NTRK1 gene lead to rare congenital insensitivity to pain with anhidrosis in two Chinese patients. Clin Chim Acta. 2017;468:39–45. doi: 10.1016/j.cca.2017.02.007. [DOI] [PubMed] [Google Scholar]