Abstract
Syphilitic infection is usually observed in young patients, and the first stage of the disease (primary syphilis) is characterized by painless cutaneous and lymph node lesions. Herein, we describe a 71-year-old Japanese man with primary syphilis that presented as unilateral inguinal lymphadenopathy without skin lesions. Originally, an incarcerated hernia was clinically suspected. The lymph node pathologically showed suppurative lymphadenitis with vague granulomas; immunohistochemistry was highly suggestive of a syphilitic infection. Primary syphilis was confirmed by positive serological tests. Syphilitic infection should be included in the clinicopathological differential diagnoses for patients with inguinal lymphadenopathy, even in elderly patients without skin lesions.
Keywords: Syphilis, Lymphadenopathy, Lymphadenitis, Pathology, Differential diagnosis, Inguinal hernia
Introduction
In Japan, the number of patients with syphilis is continuing to increase, with the highest number of patients with syphilitic infections (7983 cases, 0.006% of the national population) reported in 2021 [1]. Syphilitic infection is most commonly observed in individuals with high levels of sexual activity; individuals between 20 and 50 years old comprised 78% of the total number of infected patients in Japan in 2021 [1]. Although the percentage of elderly people in Japan who contract syphilis is low, the number of infected people who are ≥ 60 years old has been increasing in Japan, accounting for 7.4% (men, 5.6%; women, 1.8%) of all individuals with syphilis infections in 2021 [1].
Diagnosing a syphilitic infection, at any age, during the early stage of the infection (primary syphilis) is necessary to stop the spread of the infection. Primary syphilis is clinically characterized by one or more skin ulcers (chancres) at the site of the infection and is associated with regional lymphadenopathy. Syphilitic lymphadenopathy is usually seen in inguinal lymph nodes and is infrequently observed in the cervical and axillary lymph nodes [2]; syphilitic skin and lymph node lesions are usually painless [3,4]. Herein, we report a case of primary syphilis with atypical clinical manifestations; the pathological diagnosis of a swollen inguinal lymph node contributed to the definitive diagnosis.
Case report
A 71-year-old Japanese man, with a medical history of hypertension and surgical treatment of left (age, 61 years) and right (age, 70 years) inguinal hernias, experienced swelling and pain in the region of his left inguinal incision. He visited a local hospital 6 days after symptom onset. An incarcerated hernia was suspected, and the patient was referred to a surgeon at our hospital the next day. His vital signs were unremarkable and he was afebrile. A physical examination revealed tenderness and swelling in the left inguinal region, where elastic, hard masses were palpable. Blood tests showed leukocytosis (8350/µL; normal range, 3500-8000/µL) and an elevated C-reactive protein level (10.19 mg/dL; normal, <0.16 mg/dL). Abdominal to pelvic computed tomography revealed a left inguinal hernia and confirmed 5-6 swollen left inguinal lymph nodes (Fig. 1), with maximum sizes of 1-4 cm. The soft tissue surrounding the swollen lymph nodes showed increased computed tomography density, but swollen lymph nodes were not found in other areas, including in the right inguinal region (Fig. 1). Therefore, infectious lymphadenitis of the left inguinal lymph node was suspected. The patient was referred to a plastic surgeon on the same day. Mucosal or cutaneous lesions were not found on the penis, scrotum, or the left lower limb, making metastatic carcinoma unlikely. The swollen lymph nodes were biopsied for bacteriological testing and pathological diagnosis. Upon biopsy, the swollen lymph nodes were fragile and discharged pus. Thus, the lymph nodes were partially resected. Bacterial examination of the pus failed to reveal the presence of microorganisms.
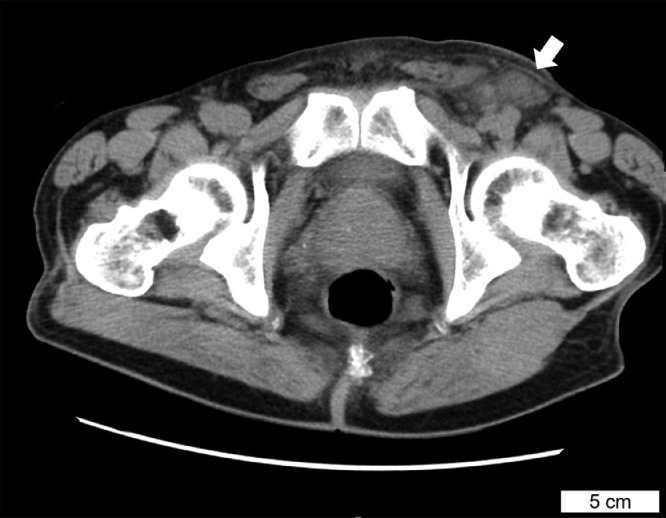
Fig. 1.
Computed tomography image of the left inguinal lymphadenopathy in a patient with primary syphilis. The left inguinal lymphadenopathy is indicated by the arrow. The soft tissue surrounding the swollen lymph nodes shows an increased density. A scale bar length is shown in the image.
The main histological finding in the resected lymph node was the presence of an abscess and suppurative lymphadenitis. The lymphoid follicles were inconspicuous, and multifocal abscesses were noted in the central portion of the lymph node (Fig. 2A, B). The lymph node capsule was inconspicuous and might have been replaced by suppurative inflammation or suppurative exudate (Fig. 2A, C). Dense fibrosis was not observed in the peripheral region of the lymph node. Many histiocytes had infiltrated the lymph node and several vague granulomas were suggested (Fig. 2D). The suppurative granulomas might have been present because of the dense histiocytic infiltrates around some abscesses. A few multinucleated histiocytes (Fig. 2B, inset) were observed in one abscess. The lymph node cortex consisted mainly of lymphocytes and plasma cells associated with proliferating vessels, suggestive of marked interfollicular hyperplasia (Fig. 2E). Plasma cells were located around the vessels (Fig. 2E), but did not show a sheet-like arrangement. Neutrophils were present in many vessels, suggesting endoarteritis (Fig. 2F) and phlebitis. Suppurative (granulomatous) lymphadenitis was observed in the lymph node.
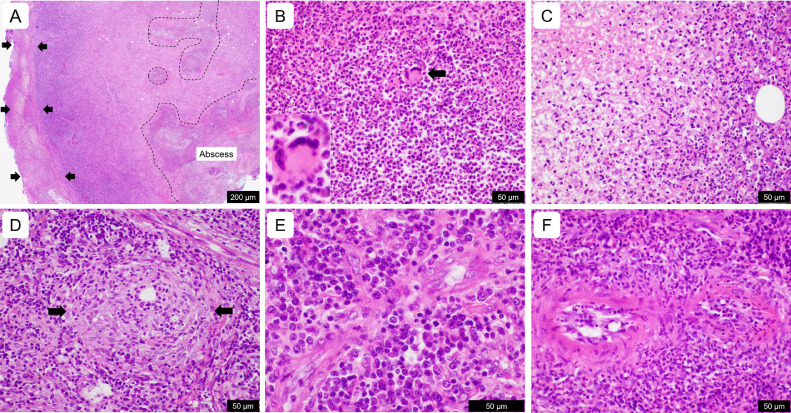
Fig. 2.
Microscopic findings of left inguinal lymphadenopathy in a patient with primary syphilis. Histologically, the left inguinal lymph node shows multifocal abscesses (A, areas inside the dotted lines; B, high magnification) in the central portion of the lymph node and purulent exudate (A, area indicated by arrows; C, high magnification) in the periphery. Lymphoid follicles and lymph node capsules are not evident. A multinucleated giant cell (B [arrow] and inset) is present in the abscess as is a vague granuloma (D, indicated by arrows). Perivascular localization of plasma cells is seen (E). Neutrophils are evident in the vessels, suggesting endarteritis and/or obliterative arteritis (F). (A-F) Hematoxylin and eosin staining. The lengths of the scale bars are shown.
Bacterial, fungal, and mycobacterial infections were considered, with syphilitic infection and cat scratch disease included in the differential diagnoses. Gram, periodic acid-Schiff, and Ziehl-Neelsen stains failed to confirm the presence of microorganisms; however, some spiral microorganisms were suggested by Warthin-Starry staining. Immunohistochemically, numerous spiral microorganisms, positive for anti-Treponema pallidum polyclonal antibodies (1:800; Abcam, Cambridge, UK), were confirmed. The microorganisms were mainly present around or in the walls of the proliferating vessels (Fig. 3A-C) and were scattered throughout the suppurative areas. Negative results were found in the sections stained with anti-bacille Calmette-Guerin polyclonal antibodies (1:1000; DAKO, Glostrup, Denmark), anti-mycobacterial tuberculosis polyclonal antibodies (1:800; Abcam), and antibodies reactive to Bartonella henselae proteins (1:50; lone H2A10, Biocare Medical, Pacheco, CA). Therefore, syphilitic lymphadenitis was strongly suggested.
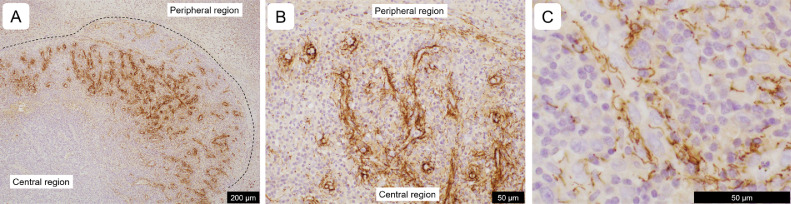
Fig. 3.
Immunohistochemical findings of left inguinal lymphadenopathy in a patient with primary syphilis. Immunohistochemistry with anti-Treponema pallidum antibodies (A-C) shows that positive-staining microorganisms are present, particularly in the lymph node cortex that also shows vascular proliferation. Spiral microorganisms are present in the wall and around the proliferating vessels (B, higher magnification of A; C, highest magnification). The lengths of the scale bars are shown.
After the pathological diagnosis, the patient met with a dermatologist, approximately 2 weeks after symptom onset. The medical interview revealed that the patient had engaged in sexual intercourse with a woman at a brothel approximately 2 weeks before symptom onset. His physical examination had not shown any skin lesions, and he had not noticed cutaneous itching or lesions following the presumed day of infection. Serological tests for rapid plasma regain (RPR, 75 RU; normal, 0-0.9 RU) and the T pallidum hemagglutination assay (32; normal, <1.0) were both positive; anti-human immunodeficiency virus antibodies were not detected. Therefore, the patient was diagnosed with primary syphilis.
The patient was treated with oral amoxicillin (1.5 g/d) for 4 weeks, resulting in his RPR titer decreasing to 34 RU. An additional 2 weeks of antibiotic therapy resulted in successful treatment, as indicated by a further 4-fold reduction in RPR titer (to 6.9 RU). During this time, the left inguinal lymph nodes became non-palpable.
The patient provided written consent for the publication of this report.
Discussion
In the present case, a pathological diagnosis was important because primary syphilis was difficult to include in the clinical differential diagnosis. The difficulty arose because the patient showed atypical clinical manifestations of primary syphilis, such as its presence in an elderly patient and causing painful lymphadenopathy without chancres. Such patient descriptions were not found in a PubMed search of patients with primary syphilis. Even if clinicians suspect infectious lymphadenopathy, T pallidum cannot be detected using typical bacterial tests. Thus, suspicion of syphilitic infection is clinically and pathologically needed when patients present with inguinal lymphadenopathy [5]. In such cases, a correct diagnosis requires a clinicopathological evaluation of the 4 main causes of inguinal lymphadenopathy: infection (eg, syphilis, lymphogranuloma venereum, chancroid, cat scratch disease, tuberculosis), cancer, autoimmune disorder, and sarcoidosis [5].
Syphilitic lymphadenopathy is usually painless; however, our patient showed painful lymphadenopathy, leading to the clinical diagnosis of an inguinal hernia. A previous study showed that painful inguinal lymphadenopathy was seen in 7 of 9 cases of primary syphilis (78%) and 2 of 11 cases of secondary syphilis (18%) [2]. Thus, painful inguinal lymphadenopathy appears to be typical in patients with primary syphilis. In addition, an incarcerated or strangulated hernia was clinically suspected in 6 of 9 patients (67%) with primary and secondary syphilis who demonstrated painful inguinal lymphadenopathy [2]. Thus, physicians should include syphilitic infection in the differential diagnosis of incarcerated or strangulated hernias.
The specific histological findings of lymphadenopathy in patients with primary syphilis have not yet been reported. Hartsock et al. reported detailed histological findings of syphilitic lymphadenopathy in 1970 [2]. They evaluated 21 lymph nodes from 20 cases of primary (n = 9) and secondary syphilis (n = 11); 17 of the 21 lymph nodes were inguinal (primary syphilis, n = 9; secondary syphilis, n = 8). They concluded that the histological findings of syphilitic lymphadenopathy were variable and not pathognomonic. However, the 4 main histological findings of syphilitic lymphadenopathy in 14 inguinal lymph nodes were summarized as follows: (1) chronic inflammation and extensive fibrosis of the lymph node capsule and pericapsular tissues; (2) sheets of plasma cells in the interfollicular, capsular, and pericapsular areas; (3) vascular changes, such as phlebitis and endarteritis; and (4) follicular hyperplasia [2]. In addition, they also documented the minor histological findings of syphilitic lymphadenopathy: variable numbers of polymorphonuclear leukocytes present between the follicles and in lymph node sinuses, abscesses (n = 5, 25%), and granulomas (n = 6, 30%) [2]; 2 cases were misdiagnosed as sarcoidosis. The authors reported the histological finding of lymphadenopathy in both primary and secondary syphilis, but they did not demonstrate histological differences between the lymph nodes in cases of primary vs secondary syphilis. Moreover, whether abscesses tend to occur more frequently in patients with primary rather than secondary syphilis is unknown. Farhi et al. reported that the histological findings in 12 cases of syphilitic lymphadenopathy in patients with secondary syphilis included capsular fibrosis (92%, 11 of 12 cases), follicular/interfollicular hyperplasia (100%, all cases), vascular proliferation (100%), perivascular cuffing by plasma cells (100%), obliterative endarteritis (58%, 7 of 12 cases), and granulomas or giant cells (8%, 1 of 12 cases) [6]. The same authors also reported that neutrophils were occasionally seen in all lymph nodes; the distribution of abscesses was not described [6]. Other reports that analyzed the histology of multiple cases of syphilitic lymphadenopathy are rare in the PubMed database. Two previous reports [2,6] suggest that lymph node histology findings in both primary and secondary syphilis cases appear to overlap. In fact, the lymph node histology in our case contained many of the secondary syphilis lymphadenopathy histological findings reported by Farhi et al. [6], such as interfollicular hyperplasia, vascular proliferation, perivascular cuffing by plasma cells, obliterative endarteritis, and the presence of granulomas or giant cells. Abscesses and the absence of capsular fibrosis might be more common in primary than in secondary syphilis, as suggested by our case and 2 previously cited reports [2,6]; this hypothesis will need to be evaluated in a larger number of cases of primary syphilitic lymphadenopathy.
The pathological differential diagnoses for syphilitic lymphadenopathy are diverse; they include suppurative granulomatous and granulomatous lymphadenitis, such as bacterial lymphadenitis (eg, lymphogranuloma venereum [7], cat scratch disease, sarcoidosis [2], and tuberculosis). Including the differential diagnosis of syphilitic lymphadenopathy may be appropriate if the multiple histological findings reported by Hartsock et al. [2] and Farhi et al. [6] are observed. The detection of T pallidum is necessary for the pathological diagnosis of syphilis. In our case, immunohistochemistry, using anti-T pallidum antibodies, was more useful than Warthin-Starry staining; numerous microorganisms were detected via immunohistochemistry, whereas microorganisms were difficult to detect using Warthin-Starry staining. Immunohistochemical evaluations may be recommended based on our experience and that of others, wherein Warthin-Starry staining was shown to have a lower sensitivity than immunohistochemistry for detecting T pallidum [8].
In conclusion, we described a case involving a 71-year-old Japanese man with primary syphilis who presented with painful left inguinal lymphadenopathy. Initially, an incarcerated hernia was clinically suspected. In this case, the pathological diagnosis was important as his syphilitic infection was not clinically suspected due to its atypical presentation: occurring in an elderly patient, the absence of chancres, and the presence of painful lymphadenopathy. Of note, the literature suggests that painful lymphadenopathy is typical of primary syphilis. Syphilitic infection should be included in the clinical and histological differential diagnoses of inguinal lymphadenopathy, and an immunohistochemical evaluation of the presence of T pallidum supports the diagnosis.
Patient consent
Written informed consent was obtained from the patient for publication of this case report.
Acknowledgments
We thank Keiko Mizuno, Masahiko Ohara, Kaori Yasuoka, Yukari Wada, and Hiroyuki Tsutsui for preparing the histological and immunohistochemical specimens. We thank Editage (www.editage.jp) for the English language editing.
Footnotes
Competing Interests: The authors declare that there is no conflict of interest in the present case report.
Supplementary material associated with this article can be found, in the online version, at doi:10.1016/j.radcr.2022.10.045.
Appendix. Supplementary materials
References
- 1.Notification trends among syphilis cases in Japan, summary of syphilis notifications in Japan as at 6 April 2022, Department of Bacteriology I, National Institute of Infectious Diseases [homepage on the Internet]. Available at: https://www.niid.go.jp/niid/images/epi/syphilis/2022q1/syphilis2022q1.pdf. Accessed August 3, 2022.
- 2.Hartsock RJ, Halling LW, King FM. Luetic lymphadenitis: a clinical and histologic study of 20 cases. Am J Clin Pathol. 1970;53:304–314. doi: 10.1093/ajcp/53.3.304. [DOI] [PubMed] [Google Scholar]
- 3.Ghanem KG, Ram S, Rice PA. The modern epidemic of syphilis. N Engl J Med. 2020;382:845–854. doi: 10.1056/NEJMra1901593. [DOI] [PubMed] [Google Scholar]
- 4.Singh AE, Romanowski B. Syphilis: review with emphasis on clinical, epidemiologic, and some biologic features. Clin Microbiol Rev. 1999;12:187–209. doi: 10.1128/CMR.12.2.187. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Charles RC, Sertic M, Neilan AM, Sohani AR. Case 11-2021: a 39-year-old woman with fever, flank pain, and Inguinal lymphadenopathy. N Engl J Med. 2021;384:1448–1456. doi: 10.1056/NEJMcpc2100273. [DOI] [PubMed] [Google Scholar]
- 6.Farhi DC, Wells SJ, Siegel RJ. Syphilitic lymphadenopathy. Histology and human immunodeficiency virus status. Am J Clin Pathol. 1999;112:330–334. doi: 10.1093/ajcp/112.3.330. [DOI] [PubMed] [Google Scholar]
- 7.Hadfield TL, Lamy Y, Wear DJ. Demonstration of Chlamydia trachomatis in inguinal lymphadenitis of lymphogranuloma venereum: a light microscopy, electron microscopy and polymerase chain reaction study. Mod Pathol. 1995;8:924–929. [PubMed] [Google Scholar]
- 8.Martín-Ezquerra G, Fernandez-Casado A, Barco D, Jucglà A, Juanpere-Rodero N, Manresa JM, et al. Treponema pallidum distribution patterns in mucocutaneous lesions of primary and secondary syphilis: an immunohistochemical and ultrastructural study. Hum Pathol. 2009;40:624–630. doi: 10.1016/j.humpath.2008.10.017. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.