Abstract
The development and delivery of religiously integrated health interventions is increasing, however lack of nomenclature to specify the religious components presents barriers to replication, implementation, and evidence synthesis. We describe the development of the “Religious Health Interventions in Behavioural Sciences (RHIBS)” Taxonomy, the first scientific classification of religious intervention components to be used globally by chaplains, healthcare providers, and researchers interested in the scientific study of religion, spirituality, and health. We developed a taxonomy of empirically used religious intervention components in health, sought international cross-disciplinary consensus for definitions and tested its usability. Study 1: systematic review of intervention studies to identify religious components tested within healthcare; development of taxonomy nomenclature, definitions, and categories. Study 2: Delphi exercise with 19 international, cross-disciplinary experts from a variety of religions. Study 3: “think aloud” study and usability testing with 10 end-users. Study 1: 12,337 papers identified from search, 167 intervention studies included, plus an additional 74 from hand-searching 14 systematic reviews. A taxonomy of 191 religious components, grouped into 27 categories resulted. Study 2: two Delphi rounds resulted in international and cross-disciplinary consensus of a revised taxonomy of 81 religious components grouped into 23 categories. Study 3: usability testing by participants (range of disciplines, geography, and religions) led to a final taxonomy comprising 82 religious components grouped into 22 categories and supported by online training. The “RHIBS Taxonomy,” is the first multidisciplinary, global shared language within religion, spirituality, and health, ushering in a new era for religious interventions to be precisely defined, developed, and tested; shaping the evidence-base for future healthcare research/practice.
Keywords: Religious components, Interventions, Synthesis, Taxonomy
The Religious Health Interventions in Behavioural Sciences Taxonomy is ushering in a new multi-faith, cross-disciplinary, international language to revolutionise the scientific evaluation of religiously integrated healthcare interventions.
Implications.
Practice: Chaplains, healthcare professionals that are developing and delivering spiritual care plans could use the RHIBS Taxonomy to inform which religious practices they promote or facilitate engagement with to improve patients’ health outcomes.
Policy: Once interventions have been developed using the RHIBS Taxonomy and shown to be effective these can confidently be incorporated into healthcare policy.
Research: Future research should adopt the RHIBS Taxonomy when developing religiously integrated healthcare interventions. Incorporating these clearly defined intervention components will enhance rigorous reporting, enable better replication, and support implementation of religiously integrated healthcare interventions in practice.
INTRODUCTION
A growing evidence-base continues to demonstrate that engagement with religion and spirituality can affect health [1]. Equally, there is a growing number of healthcare interventions incorporating religious components, but some of these religious components are not well-defined or explained. Poorly defined interventions pose several challenges for researchers in replicating, implementing, and synthesizing research [2–4].
A solution is to develop a standardized classification system, creating a shared language among researchers, and practitioners within the field. This will facilitate compliance to international standards of CONSORT [5] and TIDIER [6] that expects individual components of complex behavioral interventions to be specified and clearly defined. Similar taxonomy development within the field of behavioral science/medicine has had great success [4].
Within the field of religion, spirituality, and health early attempts at taxonomy development have highlighted the need for a comprehensive taxonomy of religious healthcare interventions. A broad taxonomy which comprised of four dimensions: “affective,” “behavioral,” “cognitive,” and “other” [7] was developed out of a series of meta-analyses exploring the impact of religion and spirituality on physical, mental, and social health in cancer [8–10]. While this taxonomy was theoretically and scientifically informed using observational evidence, it did not classify individual, intervention components used within treatment.
A taxonomy for spirituality orientated counseling and psychotherapy identified five relationships that describe how spirituality and psychology interact within therapy providing a framework to determine effectiveness [11]. While this theorized the intersectionality of spirituality and psychology, the taxonomy, again did not detail or define the individual spiritual components within therapy.
A taxonomy of chaplaincy activities and interventions for spiritual care, comprising of 100 labeled, and defined items that chaplains use to develop and deliver spiritual care plans [12]. However, this did not include all the practices, from the empirical literature, used by a wider variety of health disciplines, and religions.
The RHIBS Taxonomy project was designed to meet these gaps (isolate, organize, label, and define single empirically tested religious practices) to develop a taxonomy of empirically used religious intervention components across multiple disciplines and religions. Its intended use is for health researchers, healthcare practitioners, chaplain, and faith leaders of all faith and backgrounds. It follows established taxonomy development methods from behavioral sciences, embracing an iterative process across three studies [4, 13, 14].
STUDY 1 OBJECTIVE
To develop an empirically driven taxonomy of religious components used within healthcare interventions.
STUDY 1 METHOD
A systematic search in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidance [15] of existing systematic reviews, and intervention studies exploring religious healthcare interventions was conducted. The study protocol was added to OSF (https://osf.io/ckg8s/).
Data sources
We searched electronic databases from January 1998 to January 2019; Allied and Complimentary Medicine Database (AMED), Atla Religion Database (ATLA RDB), Cumulative Index to Nursing and Allied Health Literature (CINAHL), MEDLINE, PsychINFO Database, and the following clinical trials registers: www.clinicaltrials.gov, www.isrctn.com.
To identify additional religious components already used in practice we hand-searched textbooks recommended by international experts teaching/training spiritual care to healthcare students/staff. We also conducted a brain storming exercise within the team.
Search strategy
MeSH terms/subject headings thesaurus terms, or text word search terms for each database were combined in search strings using Boolean operators (and/or). This was done using the PIST (Population, Intervention, and Study Type) acronym:
Population: health need for example, mental health, physical health, health behaviors.
Intervention: (a) Religion for example, faith, church-based, holistic, religiously integrated and (b) Intervention descriptors for example, therapy, treatment program
Study Type: for example, systematic review, literature review, meta-review, randomized controlled trial, feasibility study, evaluation.
The full search strategy is available on request (see Table 1 for eligibility criteria).
Table 1.
Eligibility criteria for systematic search
| Inclusion criteria | Exclusion criteria | |
|---|---|---|
| Population | The context of the study must be to help those with a health need | Those studies that explored religious practices but these were unrelated to a health need |
| Intervention | Religiously integrated interventions where the definition of the religious component aligned with the following definition: A multidimensional construct that includes beliefs, behaviors, rituals, and ceremonies that may be held or practiced in private or public settings, but are in some way derived from established traditions that developed over time within a community. This can also include practices that are part of an organized system of beliefs designed (a) to facilitate closeness to the transcendent, and (b) to foster an understanding of one’s relationship and responsibility to others in living together in a community | Healthcare interventions without a religious component, such interventions may be secular, spiritual but not religious, purely humanistic, existential, and/or compassion orientated |
| Study Type | Intervention studies, randomized controlled trials (RCTs) or pre–post designs, feasibility quasi-experimental studies or research protocols Systematic review of the above |
Observational studies describing associations between a health and religiosity (i.e., cross sectional, case control, cohort) commentaries, theses, and dissertations Qualitative studies |
Eligibility criteria
Studies were limited to those published in English.
Study screening and selection
Following electronic searches, retrieved records were uploaded to endnote. RP and DL double screened 10% of initial papers to pilot the inclusion/exclusion criteria. After this, RP screened the remaining titles, abstracts, and full texts to identify potentially eligible papers. Interventions that originated in a religious tradition (e.g., Yoga, mindfulness) but were conducted without reference to the religion, or a higher power did not meet our inclusion criteria or definition of a religious health intervention; and so were excluded. Disagreements were resolved through consensus.
Data extraction and quality assessment
The following data were extracted: details of the healthcare intervention (i.e., mode of delivery, who delivered the intervention, context of the intervention, dose of the intervention, health condition targeted, religious components, and any definition thereof, religious affiliation).
The intervention description quality was assessed, and determined by applying the TIDIER checklist [6] and allocated a traffic light coding with red indicating little description, amber indicating components are mentioned but not fully defined and green indicating full description of intervention components that would facilitate replication.
Data extraction and quality assessment were completed by RP and reviewed by DL.
Taxonomy development
A list of religious components was compiled from extracted data and inductively grouped into general categories describing several individual religious components to create a hierarchical structure. Each single category and general category was defined according to the research report and met the following criteria:
-
•
be in its simplest defined form,
-
•
not overlap with other practices in the taxonomy,
-
•
be well enough defined that it is obvious for an individual to engage with.
STUDY 1 RESULTS
The systematic search identified 167 intervention studies, and an additional 74 intervention studies from hand-searching systematic reviews (Fig. 1).
Fig 1.
Systematic review flow diagram: the PRISMA flow diagram for the systematic review detailing the database searches, the number of abstracts screened, and the full texts retrieved.
From these 178 individual religious practices were identified. An additional 13 practices were identified from textbooks and brainstorming. These 191 religious practices were sorted into 27 general categories (version available on request). Each individual practice and general category were labeled and defined. The taxonomy comprised 5 descriptors:
-
(1)
A general category of the religious component designated by a number (1–27).
-
(2)
An individual component designated by a letter (a–n).
-
(3)
The potential ways in which the intervention was delivered (i.e., self-delivered, chaplain, healthcare professional).
-
(4)
The context in which the religious component was delivered (e.g., individually, in a group).
-
(5)
The religious affiliation that the component was used within (e.g., Christianity, Islam, Hinduism).
An example of a religious component, within the first draft of the taxonomy is shown in Table 2. The draft taxonomy resulting from study 1 was then used in study 2.
Table 2.
An example of a religious component, within the first draft of the RHIBS Taxonomy
STUDY 2 OBJECTIVE
To conduct an expert, international Delphi exercise to attain consensus on the taxonomy and inform further development.
STUDY 2 METHODS
Design
An online international consensus study was conducting using the Delphi method to provide evaluation of the RHIBS Taxonomy. The Delphi method is the most appropriate methodology used within health research for developing consensual guidance on best practice [16]. It is especially helpful in situations where face-to-face discussions are impractical [17]. It is characterized by four methodological features: (a) a group of experts, forming a review panel, who individually provide feedback; (b) anonymity to avoid social pressure and conformity to a dominant view; (c) an iterative process, comprising several rounds (typically 2–3 but this can increase if necessary to achieve consensus); and
(d) the design of subsequent rounds is informed by a summary of the group response of the previous round [17–19]. The method is most appropriate when the research aim benefits from subjective judgments of experts to create a collective intelligence within an area where there is limited consensus [19, 20]. As there is currently no shared language within the field of religion, spirituality, and health, the Delphi method to establish the first shared language was used.
Setting
To reduce participant and researcher burden, the Delphi study was conducted using JISC online surveys [21], which shows a status bar indicating completion progress and the option to save current progress and return later.
Participants
Participants were internationally recognized experts within the field of religion, spirituality, and health, either through their research activities or through their clinical or professional practice (e.g., clinicians, academics, chaplains, religious leaders). Participants’ expertise was determined by their publications, citations, and keynote addresses. Additionally, the John Templeton Foundation also provided a list of experts known to them. We also purposely recruited experts to represent as all major world religions. Participants had to commit to all rounds of the Delphi exercise.
Recruitment
Recruitment commenced in January 2020. Experts were recruited purposefully to ensure the panel comprised a range of disciplines, roles, faiths, and geographic locations. Experts were contacted through research networks, advertisements on the project website and personal contact. Participants were recruited mainly via email or personal invitation during academic conferences.
Procedure
After enrollment, a notification email, 2 weeks before the Delphi exercise, was sent to participants so they could schedule in the exercise. Participants were emailed a personal link which contained the Delphi exercise, a copy of the prototype version of taxonomy, and draft instructions for its intended use. They were sent a copy of the full taxonomy and instructions so they could also provide feedback on how helpful the instructions for use are and whether the taxonomy is usable in its current format. Turnaround time was one month, with reminders sent two weeks after commencement of the Delphi study, and one week before it closed.
Delphi exercise round 1
Participants were provided with the study definition of religion, and what constitutes a religious component (see inclusion criteria). Participants were informed that the taxonomy was not an exhaustive list of religious practices, rather a contained list identified from our systematic search of the empirical evidence-base, in the context of healthcare.
The Delphi exercise comprised two key activities; the first was answering the following five questions about each of the individual 191 religious components identified from the systematic search:
-
-
Do you agree with the definition given to this religious component?
-
-
Is this definition clear?
-
-
Is this definition describing a single practice?
-
-
Can this practice be used in a healthcare intervention?
-
-
Is the definition sufficient to instruct you how to practice the component?
The second activity was related to the 27 general categories the 191 individual religious components had been grouped into they were asked the following questions about each general category grouping:
-
-
Do you agree with this definition?
-
-
Do you agree with all the practices placed in this general category?
The response format for each question was a four-point Likert scale (1 “Completely agree,” 2 “Partially agree,” 3 “Partially disagree,” and 4 “Completely disagree.”). Using a four-point Likert scale meant participants were not able to give a neutral decision, this is appropriate for participants, who are experts in a subject [22]. Additionally, participants could provide additional comments or justifications for their decisions in the case of uncertainty [23].
Participants were asked for suggestions for including any religious components they thought were missing together with the appropriate evidence.
Implication of coronavirus pandemic on study procedures
The second round of the Delphi study was due in March 2020, but due to the coronavirus pandemic, 10 participants dropped out to return to clinical duties, so to prevent the loss of participants the Delphi study was paused for three months (until June 2020) and panelists were notified.
Delphi exercise round 2 (final round)
Participants were emailed the agreement results from the first round, together with a thematic summary of their comments and additional responses. Details of how these were applied to the new version of the taxonomy, alongside the new version were circulated. Participants were asked to state whether they agreed or disagreed to the new, revised components, and categories. Given the overall consensus from the first Delphi round was 85% (see results), a second round was not necessary. However given the comprehensive and insightful feedback we made revisions nonetheless and conducted a second round to ensure our changes were acceptable and did not raise major concerns. Such practice has been done previously where consensus was defined as “I can live with it,” a technique defined by Haggerty et al. [24] which allows for variation in the details but provides panelists an opportunity to modify definitions of components and categories or indicate they were adequate. This consensus method has been used previously [25, 26].
Honorariums
Upon task completion, participants were given an honorarium in the form of shopping vouchers.
Data analysis
The criteria for consensus were determined a priori, in line with Delphi study recommendations. We sought to achieve moderate agreement of >50% per question. This threshold was based on Landis and Koch [27] where
<0, no agreement; 0–0.20, slight agreement; 0.21–0.40, fair agreement; 0.41–0.60, moderate agreement; 0.61–0.80, substantial agreement; 0.81–1.0, almost perfect agreement which is appropriate for nominal and categorical data [28].
Equal weighting was given to each of the questions asked and to the open feedback for enhancing definitions and labels.
STUDY 2 RESULTS
Participant characteristics
Seventy-two experts were invited to participate, 25 did not respond, 18 declined as they were unable to commit to the tasks and 29 agreed to participate. We purposefully attempted to recruit one or two experts that would be representative of the major world religions. However, 10 withdrew due to competing priorities of the coronavirus pandemic (40% response rate). Of the 19 remaining, 13 were male and six were female, age ranged from 37 to 73 years. Most were Christian protestant (n = 10) and catholic (n = 4), two were Unitarian Universalist and one was Jewish (Orthodox), one Hindu and one had no religious affiliation. Geographically most of the panel were from the USA (n = 12), the remaining were from UK (n = 2), Ireland (n = 1), Netherlands (n = 1), Germany (n = 1), Australia (n = 1), and India (n = 1).
Most participants worked within an academic setting (n = 10), the remaining a combined academic and clinical setting (n = 4), and clinical setting alone (n = 4). Seventeen participants had research or professional doctorates, and two participants had a masters degrees.
Four participants were practicing psychiatrists, two were practicing clinical psychologists, two were chaplains and one was a medical physician. All of the participants had used a range of religious practices either clinically or within their research activities, with over half having designed and tested their own religiously integrated healthcare interventions.
Seventeen of the 19 participants completed the second Delphi round.
Delphi round 1
The percentage of participants who agreed with the general category or individual component was calculated for each question. On the basis of these scores the modal percentages achieved for the combined responses of agreement were over 80% (63%–74% for “completely agree” and 15%–22% for “partially agree”) for the individual components and 89% for the general categories.
Summary of feedback and revisions made to taxonomy
Granularity
The simplest definition of some components were considered over-granulized resulting in a loss of meaning. Therefore, several items were combined and either grouped into a new general category or added as an example of a component rather than considered an individual component. For example, in version 1 of the taxonomy, the general category: “Religious Arts and Literature” contained subcategories of religious painting, religious drawing, religious coloring, creating a religious blueprint, creating prayer cards. In version 2 these became examples for the subcategory: “Creative Religiosity.”
Appropriateness to healthcare
Some components were considered by some as inappropriate for a healthcare setting (e.g., deliverance, exorcism). in light of this we added cautionary notes to the taxonomy around the need for appropriate training or ordination for some practices. Within the taxonomy there is also a category where the usual expectation of practices are conducted only by ordained faith leaders.
Religious representation
The term “The Divine” was not considered inclusive of all religions, we replaced this with “A Transcendent/Higher Power.” Several participants made reference to a Christian bias of the components. However, this reflects the evidence-base, that to date the majority of religiously integrated healthcare interventions are from a Christian context. Where other religious examples exist these were included.
Missing components
Some participants thought religious practices (e.g., sweat lodges, whirling dervish), and religious events (e.g., quinceañera, Bat Mitzvah) were missing; however these were only added if they were practices or rituals that were used in a health intervention context (see inclusion criteria).
Following these changes, an adjusted taxonomy of 81 religious components grouped into 23 general categories was created (full version available on request), this went forward to Delphi round 2. In addition we added an extra column within the RHIBS Taxonomy table, this was to exemplify how the individual subcategory could be used in a healthcare intervention.
Delphi round 2
The percentage of participants who agreed with the category or component was calculated for each component and category. On the basis of these scores the modal percentages achieved were over 90%. This version was then used for phase 3.
STUDY 3 OBJECTIVES
-
1
To test the usability of the taxonomy in real time.
-
2
To investigate the reliability of the taxonomy when coding intervention descriptions.
STUDY 3 METHODS
Design
A hybrid “think aloud” research design. Think aloud combined with semi-structured interviews produces complimentary data when exploring usability. Real-time data are generated from the think aloud activity and deeper exploration of cognitions, thought processes, emotions, and solutions from retrospective interviewing [29].
“Think aloud” activity to test the usability of the taxonomy in real time
A think aloud is an introspective approach to assess usability (the ease of use/interaction, without prior training) of a new system or resource [30]. This approach has been used widely across health research settings [31, 32]. Think aloud elicits an individual’s process of reasoning to gain an understanding of the conscious processes that occur whilst completing a cognitive task and/or activity [33]. Participants are asked to verbalize their thinking through self-talk, enabling insights into internal narratives and decision making processes. This is conducted with a researcher present and the activity is recorded.
Retrospective semi-structured interviews to explore how the taxonomy can be enhanced for users
Retrospective interviewing provides an opportunity to elaborate on problems and explore user-centered solutions [34] this takes place immediately after the think aloud activity.
Inter-rater reliability exercise to investigate the reliability of taxonomy coding by users
An inter-rater reliability exercise where participants, independently, code an intervention description to explore the similarly of coding between participants. Participants were provided with the published intervention description of a religiously integrated health intervention for repeated negative thinking. They were then asked to code the religious subcomponent and general category. Participants were given the descriptions of each of the sessions that were delivered as part of the intervention, and they were asked to highlight and code the part of the text they thought described the religious component of the intervention using the descriptors from the RHIBS Taxonomy.
Setting
Due to restrictions of the coronavirus pandemic the think aloud study and retrospective interviews were conducted remotely using Zoom.
Participants
We purposively recruited participants from varying disciplines (academics, religious leaders, healthcare professionals, and end-users), religious faiths and geographical locations. To be included participants had to have a knowledge of or experience in religion, spirituality, and health for example, from clinical practice, research, pastoral care, or chaplaincy. Participants also had to be available to commit the time to participate in both activities.
Recruitment
Recruitment commenced in November 2020. All participants, who had expressed interest via our website or networking events, were emailed a participant pack. This contained a participant information sheet, consent form (to be emailed back to researcher), the RHIBS Taxonomy with instructions on use for the think aloud and inter-rater reliability activities, plus a zoom link.
Materials
Both activities were to code intervention descriptions using the RHIBS Taxonomy. In line with previous studies [35, 36] and to ensure that the coding was an objective test of the taxonomy, we selected intervention descriptions that had not been used to build the initial RHIBS Taxonomy. We identified three intervention descriptions published after the systematic search date.
Think aloud and retrospective semi-structured interview
These activities were audio-recorded using software embedded within zoom.
The concurrent think aloud used a standardized protocol [31], involving instructions and a warm-up activity. Participants were then asked to identify religious components from two intervention descriptions. During the think aloud the researcher used the following prompts based on McDonald et al. [29]:
-
-
If there is a pause for longer than 10 s—keep talking [reminder probe]
-
-
What are you thinking now? [exploration probe]
-
-
Are you stuck with something? [help probe]
-
-
Why did you go to that page first? [explanation, clarification probe]
At all other times the researcher was quiet. Once the exercise was completed, a semi-structured interview was conducted. The topic guide was based on guidance written by McDonald et al. [29] to provide participants with an opportunity to elaborate on their thought processes, describe their experiences, and offer suggestions for improvement (Table 3).
Table 3.
Topic guide based on guidance outlines by McDonald et al. [29]
| What are your thoughts about the taxonomy now that you have completed the activity? |
| What was the most easy/challenging when using the taxonomy to complete the activity? |
| How easy was it to use the taxonomy? |
| How intuitive was it to apply the taxonomy? |
| How applicable would you consider the taxonomy to your own work? |
| Tell us your thoughts around any improvements you would recommend to improving the usefulness of the taxonomy |
| How could the instructions on how to use the taxonomy have been clearer? |
| Was there anything you didn’t understand? |
| Do you have any final thoughts or comments? |
Inter-rater reliability task
Before the zoom call ended the researcher briefly discussed the inter-rater reliability task, during this time participants were provided with an opportunity to ask questions about it. Participants were reminded that they had one week to complete the activity, and then return it via email.
Honorariums
Upon task completion, participants were given an honorarium in the form of shopping vouchers.
Data analysis
Concurrent think aloud and retrospective interview
All interviews (concurrent think aloud and retrospective semi-structured) were transcribed verbatim. Transcripts were read and re-read, codes were created, and data were analyzed deductively, using thematic analysis [37]. Memos were made to note where the participants described usability issues, or appeared to struggle interpreting the intervention description. Qualitative data from concurrent think aloud transcripts, retrospective semi-structured interviews and memos were triangulated and presented together. To ensure rigor, RP had discussions with DL to peer review the data interpretation and check the credibility of emerging themes.
Inter-rater reliability
To calculate inter-rater reliability among coders, we divided the sum of agreed identified components, by the combined total of agreements and disagreements [38]. This step was repeated for each session that was within the intervention description at both general category level and subcategory level. This analysis was chosen as we were not calculating agreement to a standard or correct answer, but investigating the level of similarity reached between coders.
STUDY 3 RESULTS
Concurrent think aloud (CTA) and retrospective semi-structured interviews (RSSI).
Participant characteristics
Fifteen participants were invited to participate and 10 accepted (response rate of 67%). Seven were female; three were male, ages ranged from 28 to 57 years. The majority were of a Christian religious background (n = 5), three identified as Muslim, one identified as Jewish (Orthodox), and one as humanistic. Seven participants were registered/licensed practitioners (Psychology, nursing, emergency medicine, dietetics), and the remaining were a community officer, chaplain, and ordained clergy. All participants had experience in addressing religion/spirituality in the clinical practice or conducting research in religion/spirituality and health.
Participants took an average of 36 min (16–62 min) to code intervention description 1, and an average of 5 min (2–10 min) to code intervention description 2 within the CTA activity. All participants completed this and the RSSI, but one participant dropped out of exercise two (inter-rater reliability coding), and so only nine participants completed exercise two.
Qualitative findings
Three themes were developed from the dataset and are described below, with an example of the coding process illustrated in Fig. 2.
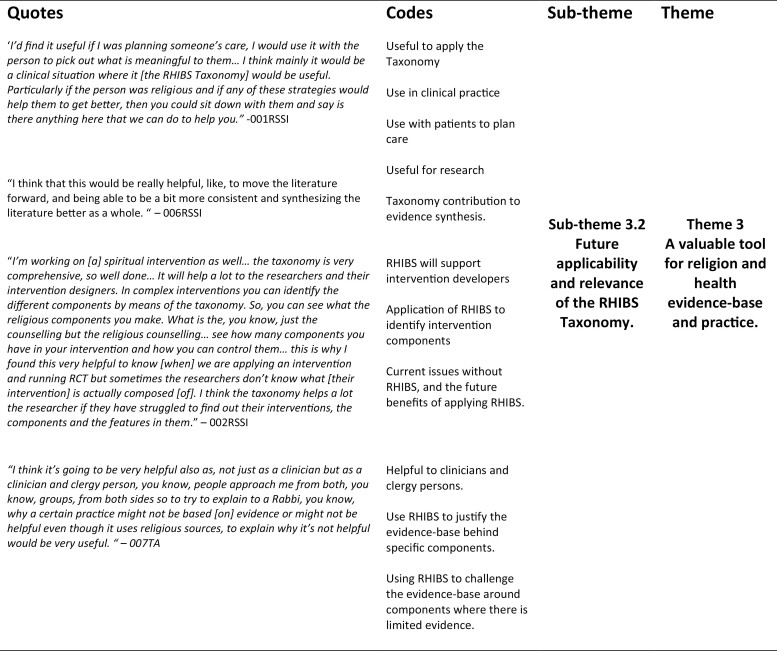
Figure 2.
Detailed coding tree for subtheme 3.2. The coding tree depicts quotes and codes that form the subtheme: Future applicability and relevance of the RHIBS Taxonomy.
Theme 1: Strategies and assumptions whilst using the RHIBS Taxonomy
This theme captures how participants applied the RHIBS Taxonomy when completing a coding exercise. There were three key subthemes that contributed to this theme, the first describes strategies participants used to complete the coding exercise, the second describes problems encountered when coding, and the third emphasizes the importance of familiarity with the RHIBS Taxonomy.
Subtheme 1.1. Strategies used by participants to code intervention descriptions
Coding an intervention description using any taxonomy for many was an activity not previously done, therefore the participants were novice usability testers. During the CTA activity participants reported using a range of different ways to identify religious components within the intervention descriptions and then find them in the RHIBS Taxonomy. Many participants appeared to search for keywords or “buzz words” that they knew had religious/spiritual connotations and then would look to see if there was something related to this in the RHIBS Taxonomy.
“… ‘they’re introduced to the concept of mantra…’ [mantra] to me is a word… [that] triggers spirituality in religion to me… So here I would look for something on meditation, stillness… let me scroll to 6 [General category for meditation in the RHIBS Taxonomy]. Let’s go up to the top. ‘Meditation, mindfulness meditation,’ ‘non-judgemental awareness, present experience.’ Okay, I’m gonna scroll down to 2, movement, meditation, I’m gonna pass that [RHIBS Taxonomy sub-component ‘Movement Meditation’] because just by looking at the name we’re not talking about movement. ‘Concentrated meditation using a stimulus, structured concentration toward meditation [RHIBS Taxonomy sub-component and definition]’… so I see the word ‘mantra’ [in the examples column] in C… So I’d really focus on that C.”—003CTA.
It also appeared that participants would code using the RHIBS Taxonomy, even when they saw certain words within the intervention description that triggered thoughts about religion and spirituality, even if the component was not religious/spiritual from the intervention description.
“It [Intervention session] ‘introduces discussions of core beliefs’. So I suppose the use of the word core belief would bring in religion for some people, so that would be…it [Religious counselling] would be appropriate in there.”—009CTA
Participants also appeared to use and rely on the examples column within the RHIBS Taxonomy to code intervention components.
“I don’t know enough about mantras, if it’s then A or B, no it’s not B, so C, so maybe C because the example [a column in the RHIBS Taxonomy] says mantra so 6C.”—005CTA
Additionally participants relied on their own clinical or pastoral experiences to interpret what would occur in the intervention, then decided what to code. For example in the following quote you can see a participant is thinking as a religious leader about what would be happening in the session. However this could lead to presumption or overthinking.
“Then how they are challenged and shaped by trauma’, I guess we’re still in eight [Religious counselling]… I feel like I’m assuming that this person [Intervention facilitator] has some kind of religious or spiritual kilt… I’m almost trying to visualise in my head what’s going on, okay, you’re in the room with this person and in my head I’m trying to create a picture and again because of my experience being a faith leader, I’m connecting it [intervention session] with, you know, patients or scenarios and over-thinking [the coding process].”—008TA
Subtheme 1.2. Problems encountered during the coding exercise
Participants flagged issues with both the RHIBS Taxonomy and the intervention description itself which made the coding exercise difficult for them. Problems related to the intervention description were lack of clarity within the description which prevented them from identifying components to map to the RHIBS Taxonomy.
“If we are going to apply the taxonomy here to the intervention we’re doing a lot of the coding with assumptions, how this is written [Intervention description] it doesn’t have clarity.”—004CTA
“[When discussing session 7 around forgiveness] I’m trying not to read into what I would want this protocol to say but I guess if I were writing such a protocol I would say often what helps people forgive themselves and others is to base one’s framework on an external framework… but I’m struggling here….”—007CTA
Two participants discussed how they would use all of the columns to determine whether the RHIBS component could be coded. In particular when information around who is delivering the component and in which context did not match the intervention description, participants felt they should not be coding that particular component. This was noted as a misunderstanding around how the taxonomy should be used.
“In my mind if I don’t see the thing I’m looking for [RHIBS component can be delivered in a group setting (with who column)] that negates from the previous things that I’ve checked off [general category, sub-category, example, facilitated by].”—003CTA
Participants also note how the example column in particular could make you change your mind about whether or not to code a component. This was because participants were perceiving the examples column to exemplify all of the ways the religious component could be used in a healthcare intervention.
“In here [RHIBS Taxonomy] ‘concentrated meditation using your stimulus to direct your concentration towards doing meditation’ [definition of concentrated meditation in RHIBS Taxonomy]. So I think this can but the example [column in RHIBS Taxonomy] as ‘a mantra or a candle flame’… that doesn’t fit [the intervention description as the meditation is not using a mantra or candle flame]”—002CTA
Subtheme 1.3. Familiarity and practice makes a confident coder
All of the participants stated the RHIBS Taxonomy was an “overwhelming size” (discussed in a later subtheme). In particular the number of religious components categorized initially overwhelmed participants but as they begun coding and went through the intervention descriptions coding became easier and participants expressed feeling confident in their ability to use the RHIBS Taxonomy.
“The first session you’re just a little bit confused which category this will go, but I think the explanation under the categories is very clear. So, at the second or the third attempt of doing this it became easier to find the categories and you can code more appropriately into the categories.”—002RSSI
“I’m noticing that… having a much more in-depth, like, knowledge of, the whole [RHIBS Taxonomy] would be helpful in this taxonomy applying practice. Just because I’ll see one, I’ll be oh, that’s it. But then, keep reading… keep looking at the other ones. And it’s like, oh, D, religious meaning making. Like, there it is…that one fits better.”—006RSSI
When reflecting on their experiences of coding the first and second intervention descriptions, all were in agreement, the second activity was quicker because it was shorter and they were more familiar with using the RHIBS Taxonomy and doing a coding exercise.
“I found the second activity easier, probably ‘cos it’s shorter… it took me a while to get into the first activity… I could see clearly what I thought were the indicators of some sort of spiritual or religious connection… but it took me a while, a bit of a slow process because I’m not familiar with the document [RHIBS Taxonomy].”—001RSSI
Theme 2: Improving the RHIBS Taxonomy to promote better engagement
All participants were comfortable critiquing the RHIBS Taxonomy and providing recommendations to improve engagement with the RHIBS Taxonomy. Two subthemes were developed which centered on shortening the taxonomy and how to demonstrate instructions for use.
Subtheme 2.1. A shorter version of the RHIBS Taxonomy would be better
The large size of the RHIBS Taxonomy was considered overwhelming by all. Reading and seeing the document in one go poses a heavy cognitive load for first-time users, participants felt that reducing the size was important to avoid putting novice users off.
“It’s a complex tool because what we’re addressing is a complex task, but is there a way that we can make the taxonomy look less complex, because that in itself is often a bit like ‘oh I don’t wanna use it, it’s complex.’ The tool is actually to help you… so it can’t be dirt simple, but at the same time if it looks unwieldy already [it’s off-putting].”—008RSSI
“It’s really interesting for me to have the right column in the taxonomy [references] but I think it’s really preferable when you’re on the work floor… I would make like a supplemental version with the right column, a more short version with the other column available [general category, sub-category, examples of the category].”—005RSSI
Subtheme 2.2. “You won’t be there when people will be using this for real” therefore “instructions manual is not enough”
Prior to the coding exercise, participants were provided with written instructions for use and an example of how to code using the RHIBS Taxonomy. All the participants went through this, but all noted it was more valuable to have RP with them when they attempted coding with the RHIBS Taxonomy for the first time.
“Working through those two exercises or those activities… once you tune in and you feel a bit more enlightened about it [the RHIBS Taxonomy content], you can see where it fits [how the components in the intervention description fit with the categories in the RHIBS Taxonomy]. It was good you were there saying ‘have you thought of this?’ and giving some prompts to direct, I think that’s helpful… but you won’t be there when people will be using this for real!”—009RSSI
Although participants found the instructions for use clear and straightforward, there were suggestions for improvement, particularly having an interactive instruction manual through various formats to help different types of learners.
“Without a video tutorial [pause] and without someone who has used it in the past to explain it to me, I think I would make a mess of it. I don’t think I would be an effective user… I do have a learning disability… in a broader sense… people are different types of learners, they’re kinaesthetic learners, they’re audio, right?… And so, without that… walking-through process I have a hard time just reading a flat document, and having it make sense to me, I have to see it in action.”—003RSI
Theme 3: A valuable tool for the field of religion, spirituality, and health
This theme captures the perceived contribution the RHIBS Taxonomy would make to the field of religion, spirituality, and health. Sentiments of gratitude were expressed to the research team for developing the RHIBS Taxonomy, and the evidence-base and scientific underpinning of its development was considered significant strength.
“I’m very impressed by all the work you’ve put into this and I know how incredibly difficult it is so yeah, so congratulations on the work.”—005RSSI
Subtheme 3.1 The RHIBS Taxonomy is a “one-stop shop” that people can refer to
Participants said it was helpful to have one taxonomy, with all the evidence of empirically tested religious components, in a useable format. This was particularly helpful for those less familiar with the academic literature.
“Having a taxonomy and having all of this new data like that’s out there, but it finally being combined into something useable is super-cool… because then we as religious providers or chaplains can actually create some evidence-based programming… when I started in chaplaincy 12 years ago there was nothing that was written out… I’m not a writer, I’m a talker… I’m not a researcher… so having something that’s there that we can actually use, that’s evidence-based, and is super-cool.”—010 RSSI
“What I thought was really helpful because I completely…and this is the researcher talking, is that it’s really, really helpful to have everything put down [on paper]… it’s difficult to get an intervention into categories because everything always overlaps, and you kind of have to decide this will be the structure, and it never really falls into place, because everything is always connected. But still just seeing a version put down that people are free to not give one code to an intervention but give several codes… is helpful.”—005RSSI
Subtheme 3.2. Future applicability and relevance of the RHIBS Taxonomy
All participants discussed ways the RHIBS Taxonomy would be useful to them or applicable in the future. As some participants were healthcare professionals they expressed how the RHIBS Taxonomy could be applied in clinical settings.
“I’d find it useful if I was planning someone’s care, I would use it with the person to pick out what is meaningful to them… I think mainly it would be a clinical situation where it [the RHIBS Taxonomy] would be useful. Particularly if the person was religious and if any of these strategies would help them to get better, then you could sit down with them and say is there anything here that we can do to help you.”—001RSSI
For chaplains, the RHIBS Taxonomy could be useful to show managers and senior staff what had been delivered as part of chaplaincy care plans.
“To tell my boss or my manager what I’ve done and why that’s important… it will be very helpful to be able to code okay, this is what I’ve done. I’ve done it so many times, this is the effect of such an intervention… Making sure that… the money is well spent on me as a chaplain, it will be really helpful, [and also for being clear what] chaplains are doing what kind of interventions and for whom… [it would] probably [be] helpful for chaplains themselves and especially it’s interesting for the researchers.”—005RSSI
The RHIBS Taxonomy was commended and recognized to be a valuable tool for future research of religion and health. Participants interested in developing religiously integrated healthcare interventions thought RHIBS Taxonomy would be of great significance to their future work.
“I’m working on [a] spiritual intervention as well… the taxonomy is very comprehensive, so well done… It will help a lot to the researchers and intervention designers. In complex interventions you can identify the different components by means of the taxonomy. So, you can see what the religious components you make. What is the, you know, just the counselling but the religious counselling… see how many components you have in your intervention and how you can control them… this is why I found this very helpful to know [when] we are applying an intervention and running RCT [Randomised Controlled Trial] but sometimes the researchers don’t know what [their intervention] is actually composed [of]. I think the taxonomy helps a lot the researcher if they have struggled to find out their interventions, the components and the features in them.”—002RSSI
The RHIBS Taxonomy was also seen to be a relevant tool for addressing the replicability crisis that exists in religion, spiritualty, and health research.
“I think when complete it will be an amazing tool, and because the study of religion and spirituality and health is such a relatively newer field, I think it will help with that replicability and so people will take the science seriously… I think that will really get the train moving to have something that we can all agree upon, we can all use and really get the science talking to each other. So, I think that’s huge.”—002RSSI
All participants found the RHIBS Taxonomy to be a comprehensive tool, and final thoughts related to its usability and relevance centered on the need for getting people to use it so that it could further developed and enhance the scientific study of religion spirituality and health.
“It looks comprehensive, it looks well developed… I think [now] it’s a process of refinement and the more you get people to engage with it and use it, I think the more you get people to engage with it and use it and get feedback, I think the more you’ll be able to enhance it and develop it… But it’s certainly comprehensive in terms of how it’s approaching spirituality and those other concepts.”—009RSSI
Inter-rater reliability
Inter-rater reliability (IRR) was highest at the general category level, but lowest at subcategory level. At general category level there was a mean IRR of 73.3% (range 44.4%–100%). At subcategory level mean was 32.0% (range 8%–44.4%) (Table 4).
Table 4.
Presenting the inter-rater reliability at general and subcategory level
| Intervention description | Identified general categories | IRR at general category level (n = 9) (%) | Identified subcategories | Inter-rater reliability a subcategory level (%) |
|---|---|---|---|---|
| Session 1 | Using religious text within interventions (Category 11) | 89 | 11A (Reading religious text) 11C (Using religious themes within religious texts in intervention sessions). |
44.4 |
| Meditation (Category 6) | 89 | 6A (Mindfulness Meditation); 6D Transcendental Meditation 6E Religious/Spiritual Meditation | 15 | |
| Positive religious coping (Category 17) | 67 | 17A (Surrendering to the Transcendent/Higher power); 17B (Journaling); 17C (Cognitive reframing using religious/spiritual viewpoint); 17D (Religious meaning-making) | 8 | |
| Session 2 | Using religious text within interventions (Category 11) | 100 | 11A (Reading religious text) 11C (Using religious themes within religious texts in intervention sessions). |
44.4 |
| Meditation (Category 6) | 78 | 6A (Mindfulness Meditation); 6E (Religious/Spiritual Meditation) | 39 | |
| Positive religious coping (Category 17) | 44.4 | 17A (Surrendering to the Transcendent/Higher power); 17C (Cognitive reframing using religious/spiritual viewpoint) | 22.2 | |
| Session 3 | Using religious text within interventions (Category 11) | 100 | 111A (Reading religious text) 11C (Using religious themes within religious texts in intervention sessions) |
39 |
| Meditation (Category 6) | 66.7 | 6A (Mindfulness Meditation); 6E (Religious/Spiritual Meditation) | 28 | |
| Positive religious coping (Category 17) | 56 | 17A (Surrendering to the Transcendent/Higher power); 17C (Cognitive reframing using religious/spiritual viewpoint) | 28 | |
| Session 4 | Using religious text within interventions (Category 11) | 89.0 | 11A (Reading religious text) 11C (Using religious themes within religious texts in intervention sessions). |
44.4 |
| Meditation (Category 6) | 66.7 | 6A (Mindfulness Meditation); 6E (Religious/Spiritual Meditation) | 33.3 | |
| Positive religious coping (Category 17) | 33.3 | 17B (Journaling) | 33.3 |
Changes to the taxonomy following study 3:
Whilst the aim of the usability study was not to amend items within the taxonomy, participants provided feedback on the taxonomy and items of their own accord. Where appropriate we did take some of these suggestions to modify the taxonomy. An additional individual component was added and additional Islamic examples provided by participants with supporting references were added. Participants demonstrated uncertainty around whether they could code more than one component, so in response to this we added links between the components to show where two or more components may be used together. The final version of the RHIBS Taxonomy comprises 82 individual components categorized into 22 general categories and is available as electronic Supplementary Material 1 but the final list is presented in Table 5.
Table 5.
A full list of the religious components included in the RHIBS Taxonomy
| General category of the religious component | Religious component |
|---|---|
| 1.Intercessory prayer | A.Distant Intercessory Prayer |
| B.Proximal Intercessory Prayer | |
| C.Intercessory Prayer using religious items and rituals. | |
| D.Requesting Intercessory Prayer | |
| 2.Personal prayer | A.Private Prayer |
| B.Contemplative Prayer | |
| C.Engaging with items perceived/representative of religion during private prayer | |
| D.Reading pre-written prayers | |
| 3.Religious arts and literature | A.Creative Religiosity |
| B.Reading religiously inspired text | |
| C.Discussing religiously inspired text | |
| 4.Religious media | A.Religious Media |
| 5.Meditation | A.Mindfulness meditation |
| B.Movement Meditation | |
| C.Concentrated Meditation | |
| D.Religious/spiritual meditation | |
| 6.Involving the religious leader | A.Delivering a health focused religious service |
| B.Involvement of the religious leader within a healthcare intervention | |
| C.Establish a new religious ruling to change health behavior | |
| 7.Religious counseling | A.Discussing patient’s perception of a Transcendent/Higher Power |
| B.Discussing the health benefits of Religion/spirituality | |
| C.Addressing theological misinterpretations | |
| D.Addressing religious/spiritual struggles related to a Transcendent/Higher Power | |
| E.Addressing internal/intrapsychic religious/spiritual struggle | |
| F.Addressing interpersonal/communal religious/spiritual struggles | |
| G.Addressing demonic oppression | |
| H.Addressing guilt and shame | |
| I.Addressing religious fatalism | |
| J.Addressing religious meanings of mortality | |
| K.Receiving spiritual guidance | |
| L.Mapping religious development | |
| 8.Imaginative activities | A.Role play of religiously motivated virtues |
| B.Revisioning/reconstructing personal constructions of a Transcendent/Higher Power | |
| 9.Religious music | A.Listening to religious music with lyrics |
| B.Listening to instrumental religious music (without lyrics) | |
| C.Singing/chanting religious songs | |
| D.Engaging in physical activity to religious music | |
| 10.Using religious texts within interventions | A.Reading religious text |
| B.Listening to religious text | |
| C.Using religious themes within religious texts in intervention sessions | |
| D.Reciting passages from religious texts | |
| 11.Religiously motivated character development | A.Self-Esteem |
| B.Religious Humility | |
| C.Love | |
| D.Compassion/Empathy | |
| E.Honesty | |
| F.Equanimity | |
| G.Morality | |
| H.Patience | |
| I.Kindness | |
| J.Wisdom | |
| K.Faith | |
| L.Religious Hope | |
| M.Religious gratitude | |
| N.Worship | |
| 12.Religiously motivated forgiveness | A.Decisional forgiveness of self |
| B.Decisional forgiveness of others | |
| C.Confession | |
| D.Repentance | |
| 13.Pilgrimage | A.Pilgrimage |
| 14.Retreats | A.Retreats |
| 15.Religious social support | A.Congregational support |
| B.Religious Leader Support | |
| C.Testimonials | |
| 16.Religious coping | A.Surrendering to the Transcendent/Higher power |
| B.Journaling | |
| C.Cognitive reframing using religious/spiritual viewpoint | |
| D.Religious meaning-making | |
| E.Reflecting on characteristics of a Transcendent/Higher Power | |
| 17.Abstinence/prohibition | A.Dietary restrictions |
| B.Abstinence from stimulants | |
| C.Abstinence from alcohol | |
| D.Abstinence from narcotics | |
| E.Fasting | |
| 18.Communal gatherings | A.Attending religious services |
| B.Religious Dancing | |
| 19.Expression of commitment | A.Expression of Commitment |
| 20.Conducting a religious/spiritual assessment | A.Conducting a religious/spiritual case history/assessment |
| 21.Religious rituals | A.Rituals around the time of death |
| B. Religious rituals to address “evil” | |
| 22.Religious experience | A.Sensing the Transcendent/Higher Power |
| B.Religious harmony |
DISCUSSION
Summary of results
The RHIBS Taxonomy is an extensive nomenclature organizing and defining empirically tested religious practices used in health interventions. We have established a shared language that can be used internationally across multiple disciplines and religions. The development has been an iterative process with the initial taxonomy of 191 individual practices organized into 27 categories, arising from a systematic review of 241 intervention studies; to 81 individual practices into 23 categories following the Delphi study where international consensus was agreed at 85%. Following usability testing, which resulted in 73% IRR at general category level, and 32% at individual practice level, the final taxonomy comprised 82 individual practices that are labeled, defined, and organized into 22 categories.
Difficulties experienced in use included the vastness of the taxonomy—particularly when unfamiliar with it, overreliance on specific aspects that is, those that were most obviously religious or spiritual. Suggestions for improvement included an interactive version and a shortened “at a glance” list. The need for the taxonomy and the benefits of having it were expressed by all participants therefore it was important appropriate support is created to enable use and uptake.
Consistency with other literature
The RHIBS Taxonomy is distinct from existing behavioral taxonomies [4, 35] due to its focus on religiosity rather than more general spirituality [11], and on integrated healthcare interventions in particular, with no restriction condition or disease state of patients, or discipline of healthcare professional [12].
The defining feature of the RHIBS Taxonomy in relation to existing taxonomies is that it breaks down religious components used in healthcare interventions, to their simplest form. There are components within the RHIBS Taxonomy that map onto other categorizations within the chaplaincy taxonomy [12]. For example the chaplaincy taxonomy references specific and general religious practices as “interventions” conducted by chaplains that is, providing a religious item, prayer, performing a religious rite or ritual, providing spiritual/religious resources [12]. The RHIBS Taxonomy can be used in conjunction with this, but takes it further to provide more detailed description of individual components and reference to the evidence-base of these used within, and applied, to a wider variety of healthcare contexts.
Our inter-rater reliability scores did not reach an established threshold of 80% agreement between coders on 95% of the codes [38], but considering this is the first time coding of religious components in health interventions has taken place, that few healthcare professionals are familiar with, some further refinement is to be expected and this is described under “implications.”
Strengths and limitations
There is currently no agreed upon methodology for taxonomy development, however we have built the RHIBS Taxonomy drawing on tried and tested methods of successfully developed taxonomies from the discipline of behavioral science [4, 13, 14] but while this is a strength, our work is not without limitations.
Similar to the development of previous taxonomies [13, 36], we first conducted a systematic search of the empirical literature. We used gold standard methods to do this, following the PRISMA guidelines [15]; our search strategy was transparent, well-defined, and comprehensive. However no search strategy can be guaranteed as completely exhaustive, and so some potentially relevant articles may not have been picked up by our search terms, within the databases we used. Our search was also limited to publications written in English, it is possible that non-English literature could have explored other healthcare interventions conducted within other religions. Our search would not have captured this and so our RHIBS Taxonomy needs to be considered in light of this. PRISMA guidance recommends that two reviewers should complete screening and study selection to reduce the risk of studies being missed. We only had one reviewer to screen and extract data, however, given this was an experienced reviewer, this is considered acceptable within the tight schedule of the project [39]. Additionally 10% of the sample screened and 10% of the data extraction was verified through a second reviewer.
In conducting our Delphi study we exceeded the minimum recommended sample size of 10–18 panel members representative of at least three disciplines [40]. We had 19 international experts from 5 disciplines and 6 different faith backgrounds. It is important to acknowledge, this phase of the research was interrupted by the coronavirus pandemic and though we attempted to minimize the impact of this we were not able to capture experts from all religious backgrounds or maintain all participants through subsequent rounds. Nonetheless our drop-out rate between rounds was only 10%, lower than the 20%–30% drop-out rate that is considered acceptable [41].
In line with good Delphi practice guidance set out by CREDES [19] we set clear a priori criterion for how consensus will be determined and how to define it, this protocol was made available prior to study commencement. Additionally, despite achieving consensus at the end of the first round, the research team made adjustments based on expert feedback, and still conducted a second round to ensure the taxonomy reflects shared input from various disciplines, nationalities, and religions which go beyond the core research team. The Delphi panel all collectively highlighted a Christian bias in the taxonomy, as our search was based on English language only literature.
Our usability testing had a strong research design with data collected concurrently and retrospectively [34]. We had a good sample size of 10 participants, 5 participants is considered sufficient to uncover 80% of usability problems and issues [30]. We reached data saturation with several key usability issues identified. One limitation of our usability study was that the corresponding author who created the RHIBS Taxonomy conducted the think aloud study and RSSI. This may have introduced interview bias, and may have meant participants were reluctant to criticize it. To address this probing questions were asked and peer review was conducted throughout.
Implication of findings
The RHIBS Taxonomy can now be used as a tool to identify religious components within healthcare interventions and to inform the design of new interventions to be tested. This can be done with confidence that these techniques have been trialed previously and their definitions have been agreed upon by a multidisciplinary, multifaith panel of international experts.
The RHIBS Taxonomy is already being applied to develop healthcare interventions in a variety of healthcare conditions (breast cancer, obesity, emotional eating, long COVID) across a range of contexts and populations. It is also being used to conduct evidence syntheses [42].
We expect to see the RHIBS Taxonomy evolve over time through collaborations, discussions, and user feedback. The usability study identified important support parameters that need to be addressed which includes opportunities for familiarization, “at a glance” and interactive versions. We have developed an online training module, with demonstrations, peer support, and opportunities for colleagues to provide comments and feedback. This can be accessed directly through this link [43] or our website [44].
Through ongoing application of the RHIBS Taxonomy, clear specification of religious components in healthcare interventions will enable better replication and testing, consequently building a stronger evidence-base around the benefits and harms of incorporating religious practices into health. Collective use and adoption of this shared language will enable efforts and funding to be prioritized in the most promising areas. The format of describing religious components in healthcare using the RHIBS Taxonomy to define the component, its mode of delivery, context, and investigate its association with changes in health related outcomes makes great strides into developing a more rigorous evidence-base for religious healthcare interventions in behavioral science.
When considered in light of existing taxonomies of similar stature in the scientific study of behavioral science, for example the Behaviour Change Techniques (BCT) Taxonomy [4], the contribution of RHIBS to the widening the evidence-base and scientific study of religion and health promises huge potential.
The RHIBS Taxonomy now needs to be tested across different contexts, different religions, different populations, and health conditions and refined further. We welcome and encourage colleagues to contact us so we can integrate their work into future versions of the taxonomy.
CONCLUSION
We developed a taxonomy of empirically used religious practices in healthcare. This aligns with rigourous reporting guidelines outlined by CONSORT and TIDIER. The RHIBS Taxonomy achieved international cross-disciplinary consensus for its definitions and groupings. We tested its usability and it is a usable product, which we will continue to develop and improve training for use. The RHIBS Taxonomy and its uptake presents a pivotal paradigm shift to enhance the development, reporting, and evidence synthesis of religious components within religiously integrated healthcare interventions. It is recommended for wide adaptation in healthcare.
Supplementary Material
Acknowledgments
This project was made possible through the support of a grant from the John Templeton Foundation. The opinions expressed in this publication are those of the authors and do not necessarily reflect the views of John Templeton Foundation. Finally, we would like to thank all of the participants who participated in studies 2 and 3. In particular we would like to thank our Delphi panelists (Professor Arndt Bussing, Dr Avdesh Sharma, Dr Bernice Mathisen, Professor Christopher Cook, Professor Crystal Park, Professor David Rosmarin, Professor Fiona Timmons, Professor John Peteet, Professor John Salsman, Professor Jon Webb, Dr Keith Edwards, Professor Loren Touissant, Dr Mark Newitt, Professor Melissa Bopp, Professor Peter Verhagen, Associate Professor Paul Perrin, and Associate Professor Tracy Balboni) for their time and commitment to the Delphi exercise.
Contributor Information
Riya Patel, Centre for Intelligent Healthcare, Coventry University, Coventry, UK.
Jonathan Jong, Centre for Peace, Trust and Social Relations, Coventry University, Coventry, UK.
Everett L Worthington, Department of Psychology, Virginia Commonwealth University, Richmond, VA, USA.
Deborah Lycett, Centre for Intelligent Healthcare, Coventry University, Coventry, UK.
Funding
This project was funded by the John Templeton Foundation grant number #61188.
Compliance with Ethical Standards
Ethical Approval: We confirm that all procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent: We confirm that informed consent was obtained from all individual participants included in the study.
Conflict of Interest: We confirm that Riya Patel, Jonathan Jong, Everett L. Worthington and Deborah Lycett declare that they have no conflicts of interest.
Welfare of Animals: We confirm that this article does not contain any studies with animals performed by any of the authors.
Transparency Related Statements: (i) This study was registered after the study began. The study is registered at https://osf.io/ckg8s/. (ii) The analysis plan was not formally pre-registered. (iii) Deidentified data from this study are not available in a public archive. Deidentified data from this study will be made available (as allowable according to institutional IRB standards) by emailing the corresponding author. (iv) There is not analytic code associated with this study. (v) Some of the materials used to conduct the study are presented in a public archive: https://osf.io/ckg8s/.
REFERENCES
- 1. Koenig H. Religion, spirituality, and health: the research and clinical implications. ISRN Psychiatry. 2012;201:1–33. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Michie S, Fixsen D, Grimshaw JM, Eccles MP.. Specifying and reporting complex behaviour change interventions: the need for a scientific method. Implement Sci. 2009;40:1–6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. King M. The challenge of research into religion and spirituality (Keynote 1). J Study Spiritual. 2014;4(2):106–120. [Google Scholar]
- 4. Michie S, Richardson M, Johnston M, et al. The behavior change technique taxonomy (v1) of 93 hierarchically clustered techniques: building an international consensus for the reporting of behavior change interventions. Ann Behav Med. 2013;46(1):81–95. [DOI] [PubMed] [Google Scholar]
- 5. Boutron I, Moher D, Altman DG, et al. Extending the CONSORT statement to randomized trials of non-pharmacologic treatment: explanation and elaboration. Ann Intern Med. 2008;148(4):295–309. [DOI] [PubMed] [Google Scholar]
- 6. Hoffmann TC, Glasziou PP, Boutron I, et al. Better reporting of interventions: template for intervention description and replication (TIDieR) checklist and guide. BMJ. 2014;7(34):8–358. [DOI] [PubMed] [Google Scholar]
- 7. Salsman JM, Fitchett G, Merluzzi TV, Sherman AC, Park CL.. Religion, spirituality, and health outcomes in cancer: a case for a meta-analytic investigation. Cancer. 2015;121(375):37544–33759. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8. Sherman AC, Merluzzi TV, Pustejovsky JE, et al. A meta-analytic review of religious or spiritual involvement and social health among cancer patients. Cancer. 2015;121(21):3779–3788. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Jim HS, Pustejovsky JE, Park CL, et al. Religion, spirituality, and physical health in cancer patients: a meta-analysis. Cancer. 2015;121(21):3760–3768. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10. Salsman JM, Pustejovsky JE, Jim HS, et al. A meta-analytic approach to examining the correlation between religion/spirituality and mental health in cancer. Cancer. 2015;121(21):3769–3778. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Sperry L, Mansager E.. The relationship between psychology and spirituality: an initial taxonomy for spiritually oriented counseling and psychotherapy. J Individ Psychol. 2007;63(4):359–370. [Google Scholar]
- 12. Massey K, Barnes MJ, Villines D, et al. What do I do? Developing a taxonomy of chaplaincy activities and interventions for spiritual care in intensive care unit palliative care. BMC Palliat Care. 2015;14(1):1–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13. Taylor SJ, Pinnock H, Epiphaniou E, et al. A rapid synthesis of the evidence on interventions supporting self-management for people with long-term conditions: PRISMS–Practical systematic RevIew of Self-Management Support for long-term conditions. Health Serv Res. 2014;14(3):1–662. [PubMed] [Google Scholar]
- 14. Hartmann-Boyce J, Aveyard P, Koshiaris C, Jebb SA.. Development of tools to study personal weight control strategies: Ox FAB taxonomy. Obesity. 2016;24(2):314–320. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. Moher D, Liberati A, Tetzlaff J, Altman DG, Prisma G.. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;151(4):1–6. [PMC free article] [PubMed] [Google Scholar]
- 16. Nair R, Aggarwal R, Khanna D.. Methods of formal consensus in classification/diagnostic criteria and guideline development. Semin Arthritis Rheum. 2011;41(2):95–105. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Iqbal S, Pipon-Young L.. The Delphi method. Psychologist. 2009;22(7):598–601. [Google Scholar]
- 18. Hasson F, Keeney S.. Enhancing rigour in the Delphi technique research. Technol Forecast Soc Change. 2011;78(9):1695–1704. [Google Scholar]
- 19. Jünger S, Payne SA, Brine J, Radbruch L, Brearley SG.. Guidance on Conducting and REporting DElphi Studies (CREDES) in palliative care: recommendations based on a methodological systematic review. Palliat Med. 2017;31(8):684–706. [DOI] [PubMed] [Google Scholar]
- 20. Kezar A, Maxey D.. The Delphi technique: an untapped approach of participatory research. Int J Soc Res Methodol. 2016;19(2):143–160. [Google Scholar]
- 21. Holloway K. Doing the E-Delphi: using online survey tools. CIN: computers, informatics. Nursing. 2012;30(7):347–350. [DOI] [PubMed] [Google Scholar]
- 22. Johns R. One size doesn’t fit all: selecting response scales for attitude items. J Elect Public Opin Parties. 2005;15(2):237–264. [Google Scholar]
- 23. Chyung SY, Roberts K, Swanson I, Hankinson A.. Evidence-based survey design: the use of a midpoint on the Likert scale. Perform Improv. 2017;56(10):15–23. [Google Scholar]
- 24. Haggerty J, Burge F, Lévesque JF, et al. Operational definitions of attributes of primary health care: consensus among Canadian experts. Ann Fam Med. 2007;5(4):336–344. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25. van der Maaden T, van der Steen JT, de Vet HC, et al. Development of a practice guideline for optimal symptom relief for patients with pneumonia and dementia in nursing homes using a Delphi study. Int J Geriatr Psychiatry. 2015;30(5):487–496. [DOI] [PubMed] [Google Scholar]
- 26. Jünger S, Payne S, Brearley S, Ploenes V, Radbruch L.. Consensus building in palliative care: a Europe-wide Delphi study on common understandings and conceptual differences. J Pain Symptom Manag. 2012;44(2):192–205. [DOI] [PubMed] [Google Scholar]
- 27. Landis JR, Koch GG.. The measurement of observer agreement for categorical data. Biometrics. 1977;1:159–174. [PubMed] [Google Scholar]
- 28. Zapf A, Castell S, Morawietz L, Karch A.. Measuring inter-rater reliability for nominal data–which coefficients and confidence intervals are appropriate? BMC Med Res Methodol. 2016;16(1):1–10. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29. McDonald S, Zhao T, Edwards HM.. Look who’s talking: evaluating the utility of interventions during an interactive think-aloud. Interact Comput. 2016;28(3):387–403. [Google Scholar]
- 30. Benbunan-Fich R. Using protocol analysis to evaluate the usability of a commercial web site. Inf Manag. 2001;39(2):151–163. [Google Scholar]
- 31. Eccles DW, Arsal G.. The think aloud method: what is it and how do I use it? Qual Res Sport Exerc Health. 2017;9(4):514–531. [Google Scholar]
- 32. Ogden J, Roy-Stanley C.. How do children make food choices? Using a think-aloud method to explore the role of internal and external factors on eating behaviour. Appetite. 2020;1(104551):1–9. [DOI] [PubMed] [Google Scholar]
- 33. Fonteyn ME, Kuipers B, Grobe SJ.. A description of think aloud method and protocol analysis. Qual Health Res. 1993;3(4):430–441. [Google Scholar]
- 34. Perski O, Blandford A, Ubhi HK, West R, Michie S.. Smokers’ and drinkers’ choice of smartphone applications and expectations of engagement: a think aloud and interview study. BMC Med Inform Decis Mak. 2017;17(1):1–14. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35. Pearce G, Parke HL, Pinnock H, et al. The PRISMS taxonomy of self-management support: derivation of a novel taxonomy and initial testing of its utility. J Health Serv Res Policy. 2016;21(2):73–82. [DOI] [PubMed] [Google Scholar]
- 36. Michie S, Ashford S, Sniehotta FF, Dombrowski SU, Bishop A, French DP.. A refined taxonomy of behaviour change techniques to help people change their physical activity and healthy eating behaviours: the CALO-RE taxonomy. Psychol Health. 2011;26(11):1479–1498. [DOI] [PubMed] [Google Scholar]
- 37. Braun V, Clarke V.. Using thematic analysis in psychology. Qual Res Psychol. 2006;3(2):77–101. [Google Scholar]
- 38. Huberman AM, Miles MB.. Data management and analysis methods. In: Denzin NK, Lincoln YS, eds. Handbook of Qualitative Research. USA: Sage Publications, Inc; 1994:428–444 [Google Scholar]
- 39. Waffenschmidt S, Knelangen M, Sieben W, Bühn S, Pieper D.. Single screening versus conventional double screening for study selection in systematic reviews: a methodological systematic review. BMC Med Res Methodol. 2019;19(1):1–9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40. Santaguida P, Dolovich L, Oliver D, et al. Protocol for a Delphi consensus exercise to identify a core set of criteria for selecting health related outcome measures (HROM) to be used in primary health care. BMC Fam Pract. 2018;19(1):1–14. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41. Chalmer J, Armour M.. The Delphi technique. In: Liamputtong P, ed. Handbook of Research Methods in Health Social Sciences. Singapore: Springer; 2019:715–735. [Google Scholar]
- 42. Calteau E, Patel R, Lycett D.. Investigating religious/spiritual integrated interventions for adults with obesity eating disorders/or disordered eating—a systematic review protocol. 2021. Available at https://www.crd.york.ac.uk/prospero/display_record.php?RecordID=267706
- 43. RHIBS Taxonomy Team, RHIBS Taxonomy Website. 2022. Available at https://rhibs.coventry.ac.uk. Accessibility verified July 29, 2022.
- 44. RHIBS Taxonomy Team, RHIBS Taxonomy MOOC. 2022. Available at https://hopeprogramme.coventry.ac.uk/rhibs. Accessibility verified July 29, 2022.
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.