Abstract
Primary hyperparathyroidism (PHPT) is a common condition associated with significant morbidity and mortality. Recently Endocrine multidisciplinary team (MDT) has greatly influenced the care of such patient and has helped in improving the outcome and reducing the complications related with surgery. We conducted a review of prospectively collected data of all consecutive parathyroidectomies carried out in our district general hospital between October 2016 and Jan 2020 by a single surgeon. The collected data include patient’s characteristics, laboratory results, radiological findings and operative outcomes. There were 53 parathyroidectomies performed during this period for PHPT. Mean age of patients was 75 years. Our results demonstrated a reduction in post-operative PTH in 46 patients (92%). We have identified no cases of vocal cord palsy, significant neck haemorrhage or mortality. 6 patients had temporary hypocalcaemia and 2 patients had hungry bone syndrome. Patient selection and evaluation for parathyroidectomies under endocrine MDT has greatly influenced the outcome for our patients. We had low complication rate and surgery was done at a more convenient location for selected patients. We benefit from dedicated monthly parathyroid clinic and weekly endocrine multidisciplinary team meetings to assist with patient selection and optimisation. A team effort helps in reducing complications and improving outcomes. We feel that surgery can be provided safely and successfully in a district general hospital in rural settings.
Keywords: Primary hyperparathyroidism, Parathyroidectomy, Hyperparathyroidism
Introduction
Primary hyperparathyroidism (PHPT) is affecting about 250 per million populations per year with significant associated morbidity and mortality [1]. Parathyroidectomy is a hugely rewarding operation as it provides a cure for the majority of cases of PHPT by removing the offending parathyroid adenoma.
This disease more commonly occurs above the age of 50 years. PHPT prevalence steadily increases with age. Older individuals tend to develop much more target organ related complications of the disease such as osteoporosis, nephrocalcinosis and cognitive dysfunction. The cumulative adverse hormonal effect from elevated PTH levels on bones and kidneys increases with the duration of PHPT [2]. Increased healthcare burden and the related financial loss are the significant consequences of such complications. Removal of parathyroid adenoma or hyperplastic glands provides a cure for this condition and therefore American guideline suggest surgery even in asymptomatic patients of < 50 years of age.
Most people of the rural area prefer surgery to be performed close to their home and travelling to a long distance is a huge burden (mainly socio-economic) on them and their family members. We feel that parathyroidectomy can be performed safely and successfully in a district general hospital with a dedicated team [3]. Recently Endocrine MDT has influenced the care of such patient significantly at each step viz. patient selection, clinical, biochemical and radiological evaluation, postoperative complication management as well as long term follow-up. We share our experience from a single surgeon operated list in a district general hospital in rural England. Our patients come from a majority rural, elderly population and patients were carefully selected by endocrine MDT.
Materials and Methods
Study Design and Study Cohort
Audit and review of the parathyroid surgery was planned after the introduction of endocrine MDT in the management of parathyroid disease in our centre. Permission was obtained from the audit department of our Hospital to conduct audit and evaluate the outcomes of parathyroidectomies. We now have completed two cycles of the audit and collected all data prospectively. In our hospital, all parathyroid surgery performed during this period was done by a single ENT surgeon (FT). Data captured included patient demographics, pre- and post-operative vocal cord assessment, pre- and post-operative biochemical results {Calcium, Vit. D, renal function & parathyroid hormone (PTH)} and histological results including weight and volume of the excised glands (Table 1).
Table 1.
Radiological concordance and histology including Gland weight & volume (n = 49)
| Radiology | |
|---|---|
| Ultrasound—Positive, n (%) | 36(73.4%) |
| Sestamibi—Positive, n (%) | 45(91%) |
| Concordance for USS + Sestamibi—Positive, n (%) | 36(100%) |
| Histology | |
| Adenoma—n (%) | 36 (74%) |
| Gland weight, g (range)a | 1.454 (0.500–1.336) |
| Gland volume, mm3 (range)a | 2713 (866–2513) |
Only patients who underwent initial surgery for PHPT were included. Patients presenting with PHPT symptoms (e.g. bones, stones, psychic moan and abdominal groan) were initially referred to the endocrinology team at our centre. Work-up includes blood tests, ultrasound scan (USS) of the neck and kidney, sestamibi/SPECT scan to locate the adenoma and DEXA (Dual energy x-ray absorptiometry) scan to check the bone mineral density (BMD). Patients are discussed in weekly endocrine multidisciplinary meeting (MDT) that includes consultant endocrinologists, biochemists and ENT surgeon. Cases of familial hypocalciuric hypercalciurea (FHH) were looked for by checking 24 h urinary calcium level (usually < 100 mg/24 h) or urinary calcium creatinine ratio (UCCR < 0.015) in all patients. We did genetic study {Calcium sensing receptor (CaSR) gene on 3q} in one younger patient. We didn’t find any case of FHH or MEN (multiple endocrine neoplasia) syndrome in our database.
Those patients who wished to proceed with parathyroid surgery are medically optimised for it by the endocrinology team, for example, control of very high calcium level with hydration and medication i.e. cinaclcet (calcinomimetic) or by prescribing supplementary vitamin D if needed (e.g. vit. D < 70 ng/ml) in order to prevent complications such as hungry bone syndrome (HBS).
The patient is also seen by an ENT surgeon in a dedicated monthly parathyroid ENT clinic and consented for surgery. All patients have a pre assessment for fitness for anaesthesia by a dedicated senior nurse practitioner or in some cases by senior anaesthetist and optimised medically.
Parathyroid surgery is performed on an elective admission basis. A blood sample is taken for parathyroid hormone and serum calcium just prior to the induction of anaesthesia and intra-operative parathyroid hormone level (IOPTH) is also checked. Post-operative calcium is repeated 6 and 12 h post-procedure to monitor hypocalcaemia. Operation is done with minimal incision access techniques. Patients are followed up in an ENT clinic in 6–8 week for vocal cord function assessment. Thereafter patients are followed up by an endocrine team member for annual calcium level check. Follow-up period varied between 1 month and 3 years (Median follow-up ~ 18 months).
Statistical Analysis
Microsoft Excel was used for calculation of mean, Inter quartile range and standard deviation. SPSS (SPSS Inc., Chicago, IL) was used for statistical analysis and Paired t test was used for comparison of laboratory variables such as parathyroid hormone (PTH), adjusted calcium and vitamin D levels pre- and post- surgery. Statistical significance was attributed where p < 0.05.The D’Agostino and Pearson test was used to assess data for normality, and subsequent parametric or non-parametric tests were used as appropriate on GraphPad Prism (version 6, GraphPad Software, LaJolla, USA). Unless otherwise specified, data is given as mean (interquartile range).
Results
Between October 2016 and Jan 2020, there were 53 parathyroid operations on 50 patients performed for PHPT in our district general hospital. One patient had bilateral targeted parathyroid adenoma and one had ipsilateral two glands targeted removal. One patient had revision surgery. We have not included one patient in the study whose histology came back as parathyroid carcinoma. We had 3 cases of giant parathyroid adenoma (> 3 cm) Fig. 1.
Fig. 1.

Giant parathyroid adenoma
Patient Characteristics, Biochemistry Tests and Localising Studies –
There were 34 (68%) female and 16 (32%) male patients. Median age was 75 (63–80) years. 14 patients (30%) were aged 80 years or over. Only 4 patients (8%) were younger than 50 years of age.
In 36 (72%) patients USS were positive (localised) and in 14 (28%) patients were negative. In 46 (92%) patients sestamibi scan were positive (Table 1) and in 2 (4%) patients were negative. Two of the sestamibi scans were reported as indeterminate with faint tracer uptake.
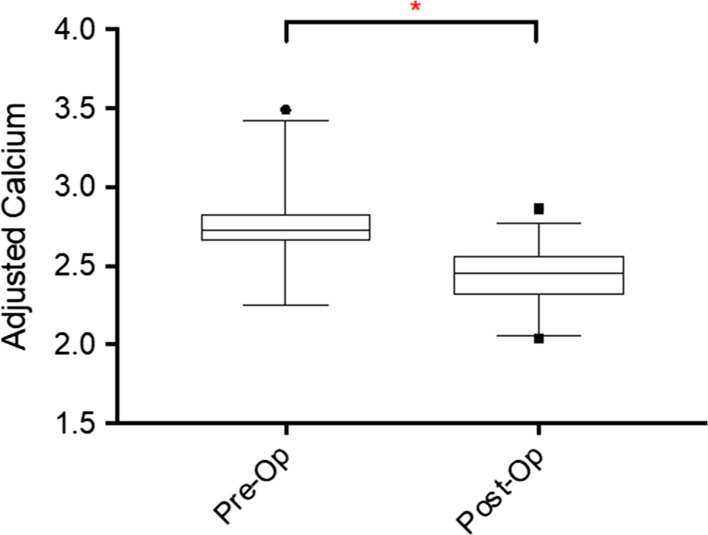
Our results demonstrated a reduction in post-operative PTH in 46 patients (92%). Furthermore as shown in Table 2, there was a significant reduction in mean PTH (mean pre-op level 21.10 (12.6–21.2) pmol/L, mean post-post op level 4.29 (1.90–4.85) pmol/L, p < 0.0001, see Fig. 2). There was a statistically significant reduction in mean adjusted calcium level after surgery, across the cohort (mean pre-op level 2.74 (2.68–2.82) mmol/L, mean post-post op level 2.40 (2.31–2.50) mmol/L, p < 0.0001, see Fig. 3).
Table 2.
Pre and post-op calcium and parathyroid hormone level
| Biochemical result | Total (n = 49) Mean (range)a | p value | |
|---|---|---|---|
| Pre-op | Post-op | ||
| Adj calcium, mmol/l, mean | 2.74 (2.68–2.82) | 2.4 (2.31–2.50) | P < 0.0001 |
| PTH, pmol/ml, mean | 21.1(12.6–21.2) | 4.29 (1.9–4.85) | P < 0.0001 |
aMean (interquartile range)
n—number; Adj Ca—adjusted calcium; PTH—parathyroid hormone
Fig. 2.
Comparison of pre and post-operative adjusted serum calcium level
Fig. 3.
Comparison of pre and post-operative serum parathyroid hormone level
Histology, BMD in DEXA Scan and Complication
Most cases were solitary adenoma. 2 cases were of two gland adenomas. Hyperplastic glands were found in 13 cases (26%). Mean adenoma weight was 1.454 (S.D ± 1.821) gm and mean adenoma volume (length x breadth x height) was 2713 (S.D ± 3522) mm3 (Table 1). There was a statistically significant, moderately strong correlation between pre-operative PTH level and adenoma volume (Spearman r = 0.32, n = 49, p = 0.029, see Fig. 4). However there was no correlation between pre op calcium and parathyroid hormone level and gland weight or between pre-op calcium level and gland volume.
Fig. 4.

Spearman correlation (r = 0.32, n = 49, p = 0.029)
To compare the potential effect of surgical intervention, we compared the BMD between interval studies. We had DEXA scan pre and post operatively within 12–24 months of surgery in 6 patients {Fig. 5i, ii}. 50% (n = 3) of patients demonstrated an improvement in both the hip and spine T-score on repeat DEXA imaging. 33% (n = 2) demonstrated no difference between serial imaging, whilst 1 patient developed minor deterioration in bone mineral density. Of note, this isolated patient demonstrating decline in BMD also experienced significant weight gain (13 Kg), of unknown aetiology, during the post-operative follow up period.
Fig. 6.

18F Fluorocholine PET in patient where USS localisation was negative
We have identified no cases of vocal cord palsy, significant neck haemorrhage requiring aspiration/drainage or mortality. 6 patients had temporary hypocalcaemia (5 were above 65 years and one patient was of 48 years age). We had two patients (4%) presented post-operatively with HBS requiring hospital admission and calcium gluconate infusion under endocrine supervision. One of them has continued to take cinacalcet despite having a clear advice to stop it following surgery. One patient was 82 years of age, pre-operative vitamin D was 61 ng/ml (normal range 30–100 ng/ml) and adjusted calcium was 2.78 mmol/l (normal range 2.20–2.60 mmol/l). Adenoma size was 20 × 10 × 10mm, with a weight of 1.673 g. He was advised to take vit. D supplements pre-operatively but was not compliant. One patient had vocal cord granuloma. One patient developed post-operative chest infection.
Discussion
Recently the collaboration between endocrinologists and ENT/endocrine surgeon has improved and a new partnership is evolving. Thyroid and parathyroid surgery in the UK is mostly undertaken up by head and neck surgeons. Endocrine MDT provides a pivoting role and is crucial for best patient outcome (Table 3).
Table 3.
Role of endocrine MDT in patient selection and outcome of parathyroid surgery
| 1. Evaluation of General physician referral and selection of patient for surgery |
| 2. Discussion of patient’s biochemistry and localisation scan in the MDT |
| 3. Pre-operative optimisation of medical and endocrine condition ± referral for genetic evaluation |
| 4. Support of endocrinology team in the management of hungry bone syndrome post-operatively |
| 5. Long term follow-up for patients with hyperplasia as there is chance of recurrence of hypercalcaemia |
| 6. Preparation of local database for the future teaching, training and research purposes |
Age is an important risk factor for surgical patients as morbidity and mortality has a linear relationship with increasing age [4]. The average age of patients undergoing parathyroidectomy in our centre was 75 years. However, proper patient selection by experienced team under endocrine MDT, pre-operative anaesthetic evaluation and dedicated post-operative care have significant role in reducing complications and postoperative morbidity. This was appreciated by the GRIFT, UK (Get it right first time) team review at our centre in July 2019. We used American guidelines [5] for patient selection as no UK guideline was available until May 2019 (NICE, UK guideline NG132).
In our centre, we operate an average of 17–18 cases of parathyroidectomy per annum and our database demonstrate a cure rate of 92% with no cases of recurrent laryngeal nerve injury, significant haemorrhage or mortality. The literature search has shown acceptable surgical cure rates by experienced surgeon to be around 85–97% (www.parathyroid.com). They have also reported less than 1% chance of recurrent laryngeal nerve injury or permanent hypoparathyroidism and essentially no mortality [6].
Although 80–85% of PHPT is caused by solitary adenoma, location of offending gland can be highly variable specifically for the inferior parathyroid gland as we know that it develops from 3rd branchial pouch and descends along the thymus in thymopharyngeal duct. To have targeted surgery it is important to localise it accurately pre-operatively. Different radiological modalities have been used to localise the gland and each has its own merits and limitations. Findings of a meta-analysis of preoperative localization techniques [7] and brief literature search are outlined in Table 4. We used the combination of USS and sestamibi/SPECT to improve overall accuracy in our centre. Recently PET scan with methionine [8] and choline [9] tracer is being used with better sensitivity and localisation in difficult cases (Fig. 5).
Table 4.
Review of the imaging modality for diagnosis and localisation
| Modality | Feature/mechanism | Localisation | Comments |
|---|---|---|---|
| USS [7] | Homogenous hypoechoic mass | Sensitivity—76.1% PPV—93% | Multinodular goitre can effect accuracy |
| Tc99m-Sestamibi/SPECT [7] (Single photon emission computed tomography) | Oxyphil cells with abundant mitochondria absorbs sestamibi | Sensitivity—78.9% PPV—90.7% Accuracy—86% | False positive—Thyroid nodule, lymph node. Gives 3D picture; Ectopic adenomas |
| ultrasound + MIBI/SPECT | Concordance—50/60% Sensitivity—97.3% PPV—93.5% | Accuracy for single gland disease—91%. [10] | Reduced accuracy for multiple gland hyperplasia |
| 4D CT scan [7] | Multiphase CT scan with I.V. Iodinated contrast | Sensitivity—89.4% Specificity—89% PPV—93.5% | Increased anatomical details e.g. ectopic glands |
| PET CT 11C Methionine [8] | Tracer is involved in synthesis of the precursor of PTH | Sensitivity—83%, Detection—96.2% | Better spatial resolution |
| 18F Fluorocholine PET [9] | Tracer has better uptake utilising choline kinase pathway | Sensitivity—95% PPV—97% Detection—91% | smaller lesions are better identified (See Fig. 6) |
Fig. 5.

(i) T-score of BMD at spine in DEXA scan (ii) T-score of BMD at hip in DEXA scan
Although intraoperative frozen section (FS) was previously used as a method for identifying an adenoma in our centre, we nowadays use intraoperative parathormone (IOPTH) level by taking the blood from peripheral veins. The advent of IOPTH assays has superseded FS and it minimises failure rate [11]. It is readily available and doesn’t require trained histopathologists. IOPTH monitoring has been reported to predict 97.5% of parathyroidectomies in patients with single gland disease. [12] Reduction of intraoperative PTH by at least 50% post-excision in 10 min were considered acceptable (Miami criteria)13. Our turnover time from laboratory was about 30 min.
The average weight of adenoma excised in our patient cohort was 1.45 g (interquartile range: 0.5–1.3). Volume of adenoma was correlated as published in previous studies [14]. Large and cystic adenoma can tear and can lead to spill over and seeding of the cells in nearby tissue (Parathyromatosis). There can also be an increased risk of injury to recurrent laryngeal nerve.
We had two cases of Hungry bone syndrome. HBS is a serious condition post-parathyroidectomy characterised by rapid, profound and prolonged hypocalcaemia associated with hypophosphatatemia and hypomagnesaemia [15, 16]. Risk factors have been suggested to predict this condition such as older age, weight/volume of resected parathyroid glands, radiological evidence of bone disease, and vitamin D deficiency [17].
There are a few recent systematic reviews and meta-analysis on the overall health benefit of surgery [10, 18] and it suggests moderate health benefits of parathyroidectomy in elderly people with PHPT [19]. There are papers also showing improvements in bone mineral density [17–21]. To demonstrate skeletal cure and improvement in BMD in our cohort, nowadays we do DEXA scan 12–18 months postoperatively. Our preliminary results in few of the patients are encouraging and are comparable to previous studies [22]. Higher powered studies in this area with prolong follow-up of our patients are required to further support the current data and assist in establishing optimal timeframe for post-operative imaging, as early imaging (less than 12 months post-surgery) may not demonstrate significant improvement [23].
Conclusion
Patient selection and evaluation for parathyroidectomies under endocrine MDT has greatly influenced the outcome for our patients. We report a cure rate of 92% with no significant morbidity (viz. laryngeal nerve palsy, haemorrhage) or mortality from parathyroidectomies performed in our district general hospital by a single surgeon. The lower complication rate is attributed to team work between ENT surgeons, endocrinologist, radiologists, pathologist and biochemist in selecting the most appropriate candidates for surgery. We benefit from dedicated monthly parathyroid clinic and weekly endocrine multidisciplinary team meetings to assist with patient selection and optimisation. With our experience we feel that parathyroid surgery can be provided to elderly population nearer to their home under the supervision of endocrine MDT with dedicated team.
Summary
PHPT prevalence and its related complications steadily increase with advancing age.
Parathyroidectomy is a hugely rewarding operation as it provides complete cure in most patients
Endocrine MDT comprising endocrinologists, biochemist, radiologist and ENT/endocrine surgeon provides a pivoting role for patient selection and is crucial for best patient outcome.
Parathyroidectomy can be safely and successfully performed in a district general hospital under endocrine MDT supervision.
Compliance with ethical standards
Conflict of interest
The authors declare that they have no conflict of interest.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Faiz Tanweer and Paul Zhaobo Liu have contributed equally to this work.
References
- 1.Shapey IM, Jaunoo SS, Hanson C, et al. Primary hyperthyroidism: how many cases are being miss? Ann R Coll Surg Engl. 2011;93(4):294–296. doi: 10.1308/003588411X13020175704352. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Oltmann SC, Rajaei MH, Sippel RS, Chen H, Schneider DF. Primary hyperparathyroidism across the ages: presentation and outcomes. J Surg Res. 2014;190(1):185–190. doi: 10.1016/j.jss.2014.04.010. [DOI] [PubMed] [Google Scholar]
- 3.Neychev VK, Ghanem M, Blackwood SL, et al. Parathyroid surgery can be safely performed in a community hospital by experienced parathyroid surgeons: a retrospective cohort study. Int J Surg. 2016;27:72–76. doi: 10.1016/j.ijsu.2015.11.026. [DOI] [PubMed] [Google Scholar]
- 4.Turrentine FE, Wang H, Simpson VB, Jones RS. Surgical risk factors, morbidity and mortality in elderly patients. J Am Coll Surg. 2006;203(6):865–877. doi: 10.1016/j.jamcollsurg.2006.08.026. [DOI] [PubMed] [Google Scholar]
- 5.Wilhelm SM, Wang TS, Ruan DT, et al. The American Association of Endocrine Surgeons Guidelines for Definitive Management of Primary Hyperparathyroidism. JAMA Surg. 2016;151(10):959–968. doi: 10.1001/jamasurg.2016.2310. [DOI] [PubMed] [Google Scholar]
- 6.Beyer TD, Solorzano CC, Starr F, et al. Parathyroidectomy outcomes according to operative approach. Am J Surg. 2007;193(3):368–372. doi: 10.1016/j.amjsurg.2006.09.023. [DOI] [PubMed] [Google Scholar]
- 7.Cheung K, Wang TS, Farrokhyar F, et al. A meta-analysis of preoperative localization techniques for patients with primary hyperparathyroidism. Ann SurgOncol. 2012;19:577–583. doi: 10.1245/s10434-011-1870-5. [DOI] [PubMed] [Google Scholar]
- 8.Noltes ME, Coester AM, van der Horst-Schrivers ANA, et al. Localization of parathyroid adenomas using 11C-methionine pet after prior inconclusive imaging. Langenbecks Arch Surg. 2017;402(7):1109–1117. doi: 10.1007/s00423-017-1549-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Broos WAM, van der Zant FM, Knol RJJ, Wondergem M. Choline PET/CT in parathyroid imaging: a systematic review. Nucl Med Commun. 2019;40(2):96–105. doi: 10.1097/MNM.0000000000000952. [DOI] [PubMed] [Google Scholar]
- 10.Cayo AK, Sippel RS, Schaefer S, Chen H. Utility of intraoperative PTH for primary hyperparathyroidism due to multigland disease. Ann Surg Oncol. 2009;16(12):3450–3454. doi: 10.1245/s10434-009-0699-7. [DOI] [PubMed] [Google Scholar]
- 11.Iacobone M, Scarpa M, Lumachi F, Favia G. Are frozen sections useful and cost-effective in the era of intraoperative qPTH assays? Surgery. 2005;138(6):1159–1164. doi: 10.1016/j.surg.2005.05.026. [DOI] [PubMed] [Google Scholar]
- 11.Barczynski M, Konturek A, Cichon S, et al. parathyroid hormone assay improves outcomes of minimally invasive parathyroidectomy mainly in patients with a presumed solitary parathyroid adenoma and missing concordance of preoperative imaging. ClinEndocrinol (Oxf). 2007;66(6):878–85. doi: 10.1111/j.1365-2265.2007.02827.x. [DOI] [PubMed] [Google Scholar]
- 13.Irvin GL, 3rd, Solorzano CC, Carneiro DM. Quick intraoperative parathyroid hormone assay: surgical adjunct to allow limited parathyroidectomy, improve success rate, and predict outcome. World J Surg. 2004;28(12):1287–1292. doi: 10.1007/s00268-004-7708-6. [DOI] [PubMed] [Google Scholar]
- 14.Gatu A, Velicescu C, Grigorovici A, Danila R, Muntean V, Mogoş SJ, Mogoş V, Vulpoi C, Preda C, Branisteanu D. The volume of solitary parathyroid adenoma is related to preoperative PTH and 25OH-D3, but not to calcium levels. ActaEndocrinol (Buchar) 2017;13(4):441–446. doi: 10.4183/aeb.2017.441. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Cipriani C, Abraham A, Silva BC, et al. Skeletal changes after restoration of the euparathyroid state in patients with hypoparathyroidism and primary hyperparathyroidism. Endocrine. 2017;55(2):591–598. doi: 10.1007/s12020-016-1101-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Witteveen JE, van Thiel S, Romijn JA, Hamdy NA. Hungry bone syndrome: still a challenge in the post-operative management of primary hyperparathyroidsim: a systematic review of the literature. Eur J Endocrinol. 2013;168(3):R45–53. doi: 10.1530/EJE-12-0528. [DOI] [PubMed] [Google Scholar]
- 17.Brasier AR, Nussbaum SR. Hungry bone syndrome: clinical and biochemical predictors of its occurrence after parathyroid surgery. Am J Med. 1988;84:654–660. doi: 10.1016/0002-9343(88)90100-3. [DOI] [PubMed] [Google Scholar]
- 18.Singh Ospina N, Maraka S, Rodriguez-Gutierrez R, et al. Comparative efficacy of parathyroidectomy and active surveillance in patients with mild primary hyperparathyroidism: a systematic review and meta-analysis. Osteoporos Int. 2016;27(12):3395–3407. doi: 10.1007/s00198-016-3715-3. [DOI] [PubMed] [Google Scholar]
- 16.Irvin GL, III, Carneiro DM. “Limited” parathyroidectomy in geriatric patients. Ann Surg. 2001;233(5):612. doi: 10.1097/00000658-200105000-00003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Cheng SP, Lee JJ, Liu TP, Yang PS, et al. Quality of life after surgery or surveillance for asymptomatic primary hyperparathyroidism: a meta-analysis of randomized controlled trials. Medicine (Baltimore) 2015;94(23):e931. doi: 10.1097/MD.0000000000000931. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Rolighed L, Vestergaard P, Heickendorff L, et al. BMD improvements after operation for primary hyperparathyroidism. Langenbecks Arch Surg. 2013;398(1):113–120. doi: 10.1007/s00423-012-1026-5. [DOI] [PubMed] [Google Scholar]
- 22.Hansen S, Hauge EM, Rasmussen L, et al. Parathyroidectomy improves bone geometry and microarchitecture in female patients with primary hyperparathyroidism: a one-year prospective controlled study using high-resolution peripheral quantitative computed tomography. J Bone Miner Res. 2012;27(5):1150–1158. doi: 10.1002/jbmr.1540. [DOI] [PubMed] [Google Scholar]
- 23.Abdelhadi M, Nordenström J. Bone mineral recovery after parathyroidectomy in patients with primary and renal hyperparathyroidism. J Clin Endocrinol Metab. 1998;83(11):3845–3851. doi: 10.1210/jcem.83.11.5249. [DOI] [PubMed] [Google Scholar]