Abstract
Objectives
This study aims to compare the clinical results of patients rehabilitated with or without a rehabilitative knee brace (RKB) after anterior cruciate ligament (ACL) reconstruction.
Patients and methods
This retrospective, comparative study was conducted at between January 2013 and December 2017. A total of 119 patients (112 males, 7 females; mean age: 32.0±8.6 years; range, 18 to 45 years) with acute ACL ruptures treated with arthroscopic ACL reconstruction and rehabilitated with (n=56) or without RKB (n=63) participated in the study. The minimum follow-up time was 24 months. The ACL quality of life (QoL) questionnaire, Lysholm Knee Scoring Scale, and Tegner Activity Level Scale were used for the evaluation of the QoL, knee function, and activity level, respectively. The time to return to sports was recorded. The side-to-side difference in the anterior translation of the tibia was measured using a KT-1000 arthrometer.
Results
The mean follow-up time was 38.4±9.1 (range, 24 to 56) months. Baseline demographics and clinical characteristics were similar between groups. Regarding QoL, knee function, and activity level, no significant difference was observed between patients who used RKB and those who did not use it at the postoperative 12th month (p=0.95, p=0.56, p=0.98, respectively) and the latest follow-up (p=0.21, p=0.73, p=0.99, respectively). The mean time to return to sports (nearly 11 months for both groups) and side-to-side difference in the anterior tibial translation at the latest follow-up was also similar between groups (p=0.15 and p=0.15, respectively). There was no graft rupture during the follow-up in both groups. The complication rates were 7.9% and 7.1% for no brace and brace groups, respectively, without a statistically significant difference (p=0.87).
Conclusion
According to the results of this study, there was no significant difference between the rehabilitative brace and no brace groups in clinical outcomes after ACL reconstruction.
Keywords: Anterior cruciate ligament reconstruction; knee brace, rehabilitation.
Introduction
Knee injuries account for 60% of sports injuries.[1] Among these, the anterior cruciate ligament (ACL) is the most commonly injured structure.[2] Anterior cruciate ligament reconstruction (ACLR), followed by postoperative rehabilitation, is the mainstay treatment for ACL rupture, allowing patients to return to their former active lifestyle.[3] The prescription of knee braces after ACLR is a common procedure.[4] According to a survey among the American Orthopedic Society for Sports Medicine members, 85% of surgeons recommend braces after ACLR.[5]
The primary purposes of knee bracing are protecting the graft, preventing subsequent injury to the index or contralateral knee, and increasing joint proprioception and patient confidence.[6] To achieve these tasks, knee braces should limit the range of motion as desired, protect the knee from excessive varus and valgus forces, and prevent anterior tibial translation (ATT) and rotation.[7] However, there are also reported disadvantages of using knee braces, such as the increased risk of injury when the knee brace is worn improperly, muscle atrophy, a reduction of knee extension velocity, decreased perception of maximal performance, increased fatigability during exercise, and additional cost of knee braces.[6,8]
There are three main types of knee braces: prophylactic knee braces, rehabilitative knee braces (RKBs), and functional knee braces. Prophylactic knee braces are used to prevent knee injury or decrease the severity of knee injury. Rehabilitative knee braces are the subject of this study, and they are used in rehabilitation protocols to allow early controlled motion after ACLR. Functional knee braces are employed after a rehabilitation process when returning to sports or work.[9]
Although RKBs have been used in postoperative rehabilitation programs for many years, data in the literature regarding the use of RKBs after ACLR are conflicting.[5,10,11] This study compared the functional and clinical results of patients rehabilitated with or without RKBs after ACLR. We hypothesized that the use of an RKB during rehabilitation after ACLR has no impact on the functional and clinical outcomes.
Patients and Methods
This retrospective, comparative study was conducted at the Erzincan University Hospital between January 2013 and December 2017. The participants were selected from a consecutive series of 208 patients who underwent arthroscopic ACLR for acute (<6 months) ACL ruptures in our level 1 trauma center. Patients with acute isolated ACL ruptures, patients aged ≥18 years, patients without any other ligamentous, meniscal, and chondral injuries, patients operated with single bundle semitendinosus gracilis autograft and endobutton via an arthroscopic ACLR technique, patients rehabilitated with or without RKB, patients with RKB compliance equal or more than 90% (for the brace group), and patients with a minimum follow-up of 24 months after surgery were included in this study. Patients with an injury to surgery time more than six months that may adversely affect the results (n=12), patients with a previous injury/surgery on the knee (n=2), patients with neuromuscular, rheumatic, or metabolic diseases (n=2), patients with any other concomitant ligamentous, meniscal, and chondral injuries (n=22), patients with less than 90% compliance with RKB (n=15), and patients operated with a bone-patellar tendon-bone autograft (n=18) were excluded from the study. Eighteen patients were lost to follow-up and excluded. Thus, 119 patients (112 males, 7 females; mean age: 32.0±8.6 years; range, 18 to 45 years) were enrolled in this study. The patients were divided into two groups: the no brace group comprising 63 patients (mean age: 32.2±8.5 years) and the RKB group consisting of 56 patients (mean age: 31.7±8.8 years). No patient had a bilateral ACL injury.
Four senior surgeons performed surgery following the same surgical technique (arthroscopic single-bundle ACLR with semitendinosus and gracilis autograft using endobutton fixation for the femur, as well as bioabsorbable screw and staple fixation for the tibia).
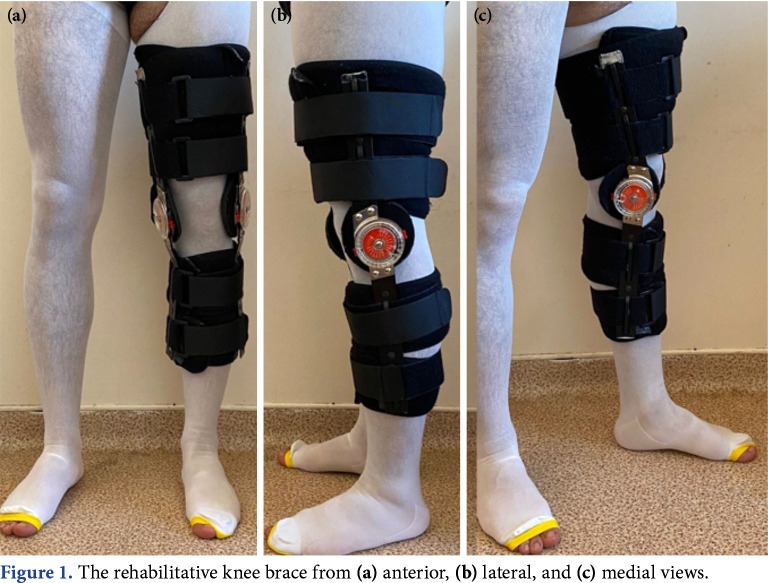
The RKB in this study was a commonly used off-the-shelf ACL rehabilitation brace (SLS311, Soles Inc., Istanbul, Türkiye), which consists of two pairs of sidebars (upper and lower knee) connected by a pair of adjustable hinges and four fastening velcro straps covered with soft cotton pads and can be adjusted to provide a better fit if required (Figure 1). Patients in the brace group were advised to wear the RKB for 24 h during all physical activities, rehabilitation exercises, and sleep. A self-reported question was used at the end of the third month to measure the compliance with RKB with a 100-mm VAS response format that asked the patients to rate how often they wore their brace. A score of 0 indicated that the patient never wore RKB, whereas a score of 100 indicated that the patient wore RKB all the time and that the compliance with RKB was 100%.[12]
Figure 1. The rehabilitative knee brace from (a) anterior, (b) lateral, and (c) medial views.
The decision to use an RKB was not based on injury or patient characteristics but at the surgeon’s discretion. Two of our surgeons routinely used an RKB after ACLR, while the other two did not agree with the potential benefits of the RKB use. This disagreement was the starting point of our study. Nonetheless, the retrospective design of the study also prevented the potential patient selection bias regarding brace use.
All patients underwent the same rehabilitation protocol, which was a standardized physical therapy based on closed kinetic chain exercises and functional strengthening that ref lects the current literature and guidelines for ACLR rehabilitation.[13-17] Early weight-bearing and full range of motion (ROM) training were encouraged. Closed kinetic chain exercises were started in the first postoperative week. There was no limit for ROM exercises; thus, patients progressed as tolerated. Twice-daily quadriceps and hamstring contraction exercises were recommended, and no neuromuscular stimulation was used. The latest phase of the rehabilitation process was progressive strengthening exercises. Jogging was permitted after one month, running after three months, and contact sports after nine months. In the brace group, patients wore the RKB locked in full extension for three weeks after surgery. The RKB was unlocked twice each day for the physical therapy sessions. Between the end of the 3rd and 12th weeks, the RKB was adjusted to allow a ROM from full extension to 10° short of the maximum flexion achieved during the physical therapy. After the 12th week, the RKB was removed, and no braces were recommended after this point. Similarly, for patients without the brace, knee flexion was not allowed until the end of the third week, except two times each day during the physical therapy. From the 3rd to 12th week, the ROM slowly progressed to the maximum achievable flexion and extension. Magnetic resonance imaging and Doppler ultrasonography were utilized if needed for any clinical doubt of graft rupture or deep venous thrombosis. All patients were evaluated with magnetic resonance imaging at the 12th month and the latest follow-up.
Baseline demographics and clinical characteristics of the patients, including age, sex, side, body mass index (BMI), type of sport during injury, follow-up duration, injury to surgery time, and graft diameter, were recorded. Clinical outcome measures were the ACL quality of life (ACL-QoL) questionnaire, Lysholm knee scoring scale, Tegner Activity Level Scale (which were assessed preoperatively, 12 months postoperatively, and at the latest follow-up), the side-to-side difference in ATT (between operated and contralateral knee, which was evaluated at the latest follow-up), and the mean time to return to sports. A KT-1000 arthrometer (Medmetric Corp., San Diego, USA) was used to measure ATT. This measurement was performed at a standard force of 134 N.[18]
The Lysholm scale is a patient-reported outcome measure that consists of eight items: pain (25 points), instability (25 points), locking (15 points), swelling (10 points), limping (5 points), stair climbing (10 points), squatting (5 points), and the need for support (5 points). The total score may range between 0 and 100, with higher scores indicating better outcomes.[19]
The Tegner scale is used to provide a standardized method to grade work and sports activities on a scale of 0 to 10. Zero indicates disability due to knee problems, while 10 indicates a national or international level player.[20]
The ACL-QoL questionnaire provides a selfadministered, disease-specific, subjective, healthrelated QoL outcome score, and it is developed and validated for ACL deficiency.[21] It consists of five parts (symptoms and physical complaints, work-related concerns, recreational activities and sports participation, lifestyle, as well as social and emotional aspects) and 31 questions. Each question has a 100-mm VAS response format. Higher scores indicate better outcomes.
Statistical analysis
Statistical analysis was performed using IBM SPSS version 25.0 software (IBM Corp., Armonk, NY, USA). Numerical variables were expressed as means and standard deviations, while categorical variables were expressed as frequencies and percentages. Means were compared using the Student’s t-test following the Shapiro-Wilk normality test. Repeated measures analysis of variance (ANOVA) was used to compare scores obtained at the baseline, the 12th month, and the latest follow-up. Tukey’s (for equal variances) and Games-Howell’s (for non-equal variances) post hoc analyses were used for multiple comparisons of significant results. The Bonferroni correction method was used in the adjustment for multiple comparisons. The chi-square test was used to test differences between observed frequencies. A p-value of <0.05 was considered statistically significant.
Results
The patients’ baseline demographics and clinical characteristics were similar between groups and are represented in Table 1. There mean follow-up duration of the patients in the no brace group was 36.9±8.7 months, whereas it was 40.2±9.4 months in the RKB group. Most patients in both groups were males (nearly 94%) who sustained ACL injury to the right knee (almost 61%) during recreational football matches (about 86%). There were no professional players in this study, and less than 30% of patients in each group had a competitive level of sports participation. The level of sports participation was similar between groups (p=0.22). In terms of QoL (ACL-QoL), knee function (Lysholm score), activity level (Tegner score; preoperatively, at the first year, and the latest follow-up), mean time to return to sports, and sideto-side difference of ATT (at the latest follow-up), no differences were observed between patients with and without RKB (Table 2). Intragroup comparisons of ACL-QoL, Lysholm, and Tegner scores at different time intervals are demonstrated in Table 3. There were statistically significant differences between the preoperative, first year, and latest follow-ups’ scores (Tegner, Lysholm, and ACL-QoL) of both groups (p <0.05), except for the differences in both groups’ Tegner scores between the first year and the latest follow-up. Thus, knee function, activity level, and QoL significantly improved until 12 months after ACLR. After 12 months, this improvement continued, albeit slightly, in knee function and QoL. The increase in activity level after the 12th month was not statistically significant (no brace group, p=0.53; brace group, p=0.63).
Table 1. Baseline demographics and clinical characteristics.
| No brace group (n=63) | Brace group (n=56) | p | |||||
| n | % | Mean±SD | n | % | Mean±SD | ||
| Mean age (year) | 32.2±8.5 | 31.7±8.8 | 0.78* | ||||
| Mean follow-up (month) | 36.9±8.7 | 40.2±9.4 | 0.06* | ||||
| Mean injury to surgery time (month) | 4.3±1.4 | 3.8±1.3 | 0.08* | ||||
| BMI (kg/m2) | 22.1±3.2 | 22.3±2.8 | 0.80* | ||||
| Sex | 0.32** | ||||||
| Male | 59 | 93.7 | 53 | 94.6 | |||
| Female | 4 | 6.3 | 3 | 5.4 | |||
| Side | 0.89** | ||||||
| Right | 39 | 61.9 | 34 | 60.7 | |||
| Left | 24 | 38.1 | 22 | 39.3 | |||
| Sports during ACL injury | 0.70** | ||||||
| Football | 55 | 87.3 | 48 | 85.6 | |||
| Basketball | 4 | 6.3 | 3 | 5.4 | |||
| Ski | 3 | 4.8 | 2 | 3.6 | |||
| Other | 1 | 1.6 | 3 | 5.4 | |||
| Participation in sports | 0.22** | ||||||
| Recreational | 51 | 81 | 40 | 71.4 | |||
| Competitive | 12 | 19 | 16 | 28.6 | |||
| Graft diameter (mm) | 0.97** | ||||||
| 8 | 41 | 65 | 36 | 64.3 | |||
| 9 | 19 | 30.2 | 18 | 32.1 | |||
| 10 | 2 | 3.2 | 1 | 1.8 | |||
| 11 | 1 | 1.6 | 1 | 1.8 | |||
| SD: Standart deviation; BMI: Body mass index; ACL: Anterior cruciate ligament; * Student’s t-test; ** Chi-square test. | |||||||
Table 2. Intergroup comparison of clinical outcomes.
| No brace group | Brace group | p | |
| Mean±SD | Mean±SD | ||
| Tegner activity level scale | |||
| Preoperative | 2.1±0.6 | 2.1±0.6 | 0.87* |
| First-year | 6.0±0.3 | 6.0±0.5 | 0.98* |
| Latest follow-up | 6.2±0.8 | 6.2±0.9 | 0.99* |
| Lysholm knee scoring scale | |||
| Preoperative | 58.2±11.7 | 56.8±10.6 | 0.50* |
| First-year | 87.3±5.9 | 86.8±5.3 | 0.56* |
| Latest follow-up | 89.7±4.3 | 89.4±4.7 | 0.73* |
| ACL-QoL questionnaire | |||
| Preoperative | 36.2±3.7 | 36.4±4.1 | 0.78* |
| First-year | 71.2±10.3 | 71.0±12.0 | 0.95* |
| Latest follow-up | 78.5±11.8 | 81.3±12.7 | 0.21* |
| ATT side-to-side difference (injured-uninjured) | 1.1±1.3 | 1.4±1.4 | 0.15* |
| Return to sports time | 10.8±2.2 | 11.4±2.3 | 0.15* |
| SD: Standard deviation; ACL: Anterior cruciate ligament; QoL: Quality of life; ATT: Anterior tibial translation; * Student's t-test. | |||
Table 3. Intragroup comparison of clinical outcomes.
| Tegner Score | ||||
| Preoperative | 1st year follow-up | Latest follow-up | ||
| Points±SD | Points±SD | Points±SD | p | |
| No brace group | 2.1±0.6a | 6.0±0.3b | 6.2±0.8b | <0.01* |
| Brace group | 2.1±0.6a | 6.0±0.5b | 6.2±0.9b | <0.01* |
| Lysholm score | ||||
| Preoperative | 1st year follow-up | Latest follow-up | ||
| Points±SD | Points±SD | Points±SD | p | |
| No brace group | 58.2±11.7a | 87.3±5.9b | 89.7±4.3c | <0.01* |
| Brace group | 56.8±10.6a | 86.8±5.3b | 89.4±4.7c | <0.01* |
| ACL-QoL score | ||||
| Preoperative | 1st year follow-up | Latest follow-up | ||
| Points±SD | Points±SD | Points±SD | p | |
| No brace group | 36.2±3.7a | 71.2±10.3b | 78.5±11.8c | <0.01* |
| Brace group | 36.4±4.1a | 71.0±12.0b | 81.3±12.7c | <0.01* |
| SD: Standard deviation; The superscripts a, b, c were used to indicate the difference between intragroup time intervals in post hoc analysis. In post hoc analysis, different letters were used if there was a statistically significant difference between time intervals (p<0.05), and the same letters were used if there was no difference (p>0.05). ACL-QoL: Anterior cruciate ligament quality of life; * Repeated measures ANOVA. | ||||
There were no graft ruptures or deep infections during the follow-up in both groups. There were four patients (two in the brace group and two in the no brace group) with deep venous thrombosis, which was resolved after anticoagulant treatment within six months. There were five patients (two in the brace group and three in the no brace group) with a superficial infection that was resolved after the administration of oral antibiotics. The complication rates were 7.9% and 7.1% for no brace and brace groups, respectively, without a statistically significant difference (p=0.87).
Discussion
The most significant finding of this study is the similar clinical outcomes in those with and without RKBs in terms of functional scores, health quality scores, and objective KT measurements at the postoperative first year and the latest follow-up visits. Thus, our null hypothesis can be accepted, suggesting that the use of RKBs after ACLR is not necessary. Similar to our study, in studies with follow-ups ranging from two to five years, the Lysholm score, Tegner score, and side-to-side difference in ATT were similar between the brace and no brace groups.[22] In the literature, the Lysholm score ranges between 87 and 99 for the brace group and between 90 and 95 for the no brace group; the Tegner score ranges between 5 and 6.5 for the brace group and between 5 and 6.3 for the no brace group; the side-to-side difference in ATT ranges between 0.6 and 2.9 mm for the brace group and between 0.5 and 2.6 mm for the no brace group during the follow-up.[23] The meta-analysis of Yang et al.[24] demonstrated that knee bracing does not improve the clinical outcomes (function and stability) after ACLR. Pooled data of this meta-analysis showed that the international knee documentation committee score, Lysholm and Tegner scores, side-to-side difference, single-leg hop test, and VAS scores were similar between the brace and no brace groups. They also speculated that the brace might have disadvantages, such as a negative influence on the knee outcome and an additional cost. Similarly, the systematic review of Wright et al.[25] concluded that postoperative bracing was not necessary after ACLR. In another systematic review by Wright and Fetzer,[26] no evidence was found to suggest that pain, ROM, graft stability, and subsequent injury risk were affected by brace use. Masini and Owens[27] stated that a brace prescription was not required for successful long-term outcomes and return to sports in their review. In his review, Rodríguez-Merchán[28] claimed that postoperative bracing after ACLR did not help the pain, function, rehabilitation, and stability. In their review, Pezzullo and Fadale[29] pointed out that the use of braces to lower the risk of reinjury was not supported in the literature, except in skiing, but braces may help increase the athlete’s confidence when returning to sports. A review by Smith et al.[8] indicated that brace use did not improve long-term patient outcomes following ACLR but reduced ACL injury rates while skiing and concluded that a brace designed to apply forces to the knee similar to the native ACL should be pursued. In their systematic review, Lowe et al.[6] reported that the effectiveness of bracing after ACLR remains controversial. Our results were consistent with the literature. We attribute this indifference to the high stability of the modern arthroscopic ACLR and fixation techniques and the advantage of early rehabilitation protocol.
To the best of our knowledge, there is only one study in the literature reporting ACL-QoL findings on a knee brace. In this study, Birmingham et al.[12] reported similar ACL-QoL results between groups before the operation (35.8 for brace group and 36.3 for sleeve group), at the 12th month (68.7 for brace group and 69.2 for sleeve group), and the 24th month (76.1 for brace group and 77.6 for sleeve group). Our results were similar to this study. As mentioned above, owing to modern techniques that developed over the years in both operative and rehabilitative periods, the ACLR treatment yields better outcomes. Thus, due to the consistent results in the recent studies, authors do not strongly recommend the routine use of RKB after ACLR. However, there are still limited studies in the literature regarding the use of RKB after ACLR, and future studies are needed on this issue to reach a higher level of evidence.
In contrast to these studies that do not strongly recommend the routine use of RKB after ACLR, DeVita et al.[30] found that, with the advantage of the power and moment adaptations that develop in the lower extremity joints after the use of a brace, bracing can reduce the load on the graft while walking and thus cause indirect protection on the graft. Melegati et al.[31] showed that locking the brace in full extension in the first week after ACLR was more effective in achieving full extension than allowing a ROM of 0 to 90°. A similar study by Risberg et al.[32] reported that -5° hyperextension bracing was more successful in achieving full extension without a loss than 0° extension bracing. Masini and Owens[27] pointed out that postoperative bracing may only be indicated for at-risk patients to avoid compromising surgical results under two circumstances: postoperative extension loss and painful effusion. Mcdevitt et al.[16] consider that bracing after ACLR may positively normalize the knee joint kinematics and minimize the translational, rotational, and valgus forces across the joint, which would protect the graft. Increased patient confidence due to enhanced sensorimotor feedback after the use of a brace during high-level activities was also reported in the literature.[12,16] Skiers are found to have fewer recurrent injuries after ACLR with the help of a brace.[33] Some authors have speculated that brace use might benefit ACLR by improving functional performance, preventing quadriceps inhibition, reducing anteroposterior laxity, and allowing protected motion by preventing excessive loading.[34] Lu et al.[35] stated that bracing after ACLR may help achieve better bilateral kinetic symmetry during gait.
The ideal time to return to play after ACLR is still controversial, and for most surgeons, the time after ACLR is the only criterion.[36] Petersen and Zantop[37] recommended at least six to eight months to return to play. However, Van Grinsven et al.[14] suggested the following criteria to return to sports: full ROM, more than 85% quadriceps and hamstring strength and single-leg hop distance compared to the contralateral leg, less than 15% deficit in hamstring/ quadriceps strength ratio, no pain or swelling, and a stable knee during sports activities. Our criteria for returning to sports were similar to this, except for muscle strength testing. Our patients achieved these goals relatively late, which may have protected them from early graft ruptures. The complication rate of ACLR has been reported to be up to 25%.[38-40] Our complication rates were similar between groups (around 8%), comparable with data in the literature.
The cut-off value for the RKB compliance was set at 90%. We believe that there were three reasons for the high compliance rate of this study. First, the two surgeons who recommended knee braces personally trained the patients, admonished them, and gave strict instructions before the surgery about using the knee brace. The second reason is that the use of the brace is easy and comfortable. Only a few patients complained about discomfort and slippage. Third, patients may not be telling the truth about brace compliance, which there is no way to control. In addition, we believe that it can be misleading to provide the results of a study with a patient compliance rate of 50 to 60%.
The main strength of the study is that it is one of the few studies reporting the outcomes of a rehabilitative brace (instead of commonly used prophylactic or functional braces) with a no-brace control group. Additionally, our results were highlighted with a brief literature review focusing on the advantages and disadvantages of brace use, thus contributing to the readers’ interpretation of our results. Groups were homogeneous according to baseline demographics and clinical characteristics, particularly participation in sports and graft diameter. Furthermore, the relatively large number of patients and approximately three-year follow-up are among the positive features of this study. The main limitations of this study are the retrospective setting and allocation of patients into groups based on surgeons’ discretion rather than a blinded protocol. Although the same surgical technique was used in all cases, four different surgeons performed the surgeries, which may have caused a standardization problem. This was a retrospective study, and randomized controlled trials are more valuable to determine a more accurate difference between treatment methods.
In conclusion, prescription of knee braces after ACLR during the rehabilitation period is unnecessary since knee brace use does not affect the clinical outcomes.
Footnotes
Ethics Committee Approval: The study protocol was approved by the Erzincan University Faculty of Medicine Ethics Committee (33216249-903.99-E.14483). The study was conducted in accordance with the principles of the Declaration of Helsinki.
Conflict of Interest: The authors declared no conflicts of interest with respect to the authorship and/or publication of this article.
Author Contributions: All authors contributed equally to the article.
Financial Disclosure: The authors received no financial support for the research and/or authorship of this article.
Patient Consent for Publication: A written informed consent was obtained from each patient.<br><br><b>Data Sharing Statement:</b><br> The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
- 1.Rishiraj N, Taunton JE, Lloyd-Smith R, Woollard R, Regan W, Clement DB. The potential role of prophylactic/ functional knee bracing in preventing knee ligament injury. Sports Med. 2009;39:937–960. doi: 10.2165/11317790-000000000-00000. [DOI] [PubMed] [Google Scholar]
- 2.Buyukkuscu MO, Misir A, Cetinkaya E, Ezici A, Ozcafer R, Gursu SS. The interposition of soft tissue between the cortical button and femoral lateral cortex significantly increases button migration but does not negatively affect knee stability and clinical outcome. Knee. 2020;27:891–898. doi: 10.1016/j.knee.2020.02.021. [DOI] [PubMed] [Google Scholar]
- 3.Campbell JD. The evolution and current treatment trends with anterior cruciate, posterior cruciate, and medial collateral ligament injuries. Am J Knee Surg. 1998;11:128–135. [PubMed] [Google Scholar]
- 4.Decoster LC, Vailas JC, Swartz WG. Functional ACL bracing. A survey of current opinion and practice. Am J Orthop (Belle Mead NJ) 1995;24:838–843. [PubMed] [Google Scholar]
- 5.Delay BS, Smolinski RJ, Wind WM, Bowman DS. Current practices and opinions in ACL reconstruction and rehabilitation: Results of a survey of the American Orthopaedic Society for Sports Medicine. Am J Knee Surg. 2001;14:85–91. [PubMed] [Google Scholar]
- 6.Lowe WR, Warth RJ, Davis EP, Bailey L. Functional bracing after anterior cruciate ligament reconstruction: A systematic review. J Am Acad Orthop Surg. 2017;25:239–249. doi: 10.5435/JAAOS-D-15-00710. [DOI] [PubMed] [Google Scholar]
- 7.Cawley PW, France EP, Paulos LE. Comparison of rehabilitative knee braces. A biomechanical investigation. Am J Sports Med. 1989;17:141–146. doi: 10.1177/036354658901700201. [DOI] [PubMed] [Google Scholar]
- 8.Smith SD, Laprade RF, Jansson KS, Arøen A, Wijdicks CA. Functional bracing of ACL injuries: Current state and future directions. Knee Surg Sports Traumatol Arthrosc. 2014;22:1131–1141. doi: 10.1007/s00167-013-2514-z. [DOI] [PubMed] [Google Scholar]
- 9.Stephens DL. The effects of functional knee braces on speed in collegiate basketball players. J Orthop Sports Phys Ther. 1995;22:259–262. doi: 10.2519/jospt.1995.22.6.259. [DOI] [PubMed] [Google Scholar]
- 10.Wu GK, Ng GY, Mak AF. Effects of knee bracing on the functional performance of patients with anterior cruciate ligament reconstruction. Arch Phys Med Rehabil. 2001;82:282–285. doi: 10.1053/apmr.2001.19020. [DOI] [PubMed] [Google Scholar]
- 11.Kocher MS, Sterett WI, Briggs KK, Zurakowski D, Steadman JR. Effect of functional bracing on subsequent knee injury in ACL-deficient professional skiers. J Knee Surg. 2003;16:87–92. [PubMed] [Google Scholar]
- 12.Birmingham TB, Bryant DM, Giffin JR, Litchfield RB, Kramer JF, Donner A, et al. A randomized controlled trial comparing the effectiveness of functional knee brace and neoprene sleeve use after anterior cruciate ligament reconstruction. Am J Sports Med. 2008;36:648–655. doi: 10.1177/0363546507311601. [DOI] [PubMed] [Google Scholar]
- 13.Shelbourne KD, Klootwyk TE, Decarlo MS. Update on accelerated rehabilitation after anterior cruciate ligament reconstruction. J Orthop Sports Phys Ther. 1992;15:303–308. doi: 10.2519/jospt.1992.15.6.303. [DOI] [PubMed] [Google Scholar]
- 14.van Grinsven S, van Cingel RE, Holla CJ, van Loon CJ. Evidence-based rehabilitation following anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc. 2010;18:1128–1144. doi: 10.1007/s00167-009-1027-2. [DOI] [PubMed] [Google Scholar]
- 15.Kruse LM, Gray B, Wright RW. Rehabilitation after anterior cruciate ligament reconstruction: A systematic review. J Bone Joint Surg [Am] 2012;94:1737–1748. doi: 10.2106/JBJS.K.01246. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.McDevitt ER, Taylor DC, Miller MD, Gerber JP, Ziemke G, Hinkin D, et al. Functional bracing after anterior cruciate ligament reconstruction: A prospective, randomized, multicenter study. Am J Sports Med. 2004;32:1887–1892. doi: 10.1177/0363546504265998. [DOI] [PubMed] [Google Scholar]
- 17.Wright RW, Preston E, Fleming BC, Amendola A, Andrish JT, Bergfeld JA, et al. A systematic review of anterior cruciate ligament reconstruction rehabilitation: Part II: Open versus closed kinetic chain exercises, neuromuscular electrical stimulation, accelerated rehabilitation, and miscellaneous topics. J Knee Surg. 2008;21:225–234. doi: 10.1055/s-0030-1247823. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Arneja S, Leith J. Review article: Validity of the KT-1000 knee ligament arthrometer. J Orthop Surg (Hong Kong) 2009;17:77–79. doi: 10.1177/230949900901700117. [DOI] [PubMed] [Google Scholar]
- 19.Celik D, Coşkunsu D, Kiliçoğlu O. Translation and cultural adaptation of the Turkish Lysholm knee scale: Ease of use, validity, and reliability. Clin Orthop Relat Res. 2013;471:2602–2610. doi: 10.1007/s11999-013-3046-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Briggs KK, Lysholm J, Tegner Y, Rodkey WG, Kocher MS, Steadman JR. The reliability, validity, and responsiveness of the Lysholm score and Tegner activity scale for anterior cruciate ligament injuries of the knee: 25 years later. Am J Sports Med. 2009;37:890–897. doi: 10.1177/0363546508330143. [DOI] [PubMed] [Google Scholar]
- 21.Kinikli GI, Celik D, Yuksel I, Atay OA. Turkish version of the anterior cruciate ligament quality of life questionnaire. Knee Surg Sports Traumatol Arthrosc. 2015;23:2367–2375. doi: 10.1007/s00167-014-3404-8. [DOI] [PubMed] [Google Scholar]
- 22.Mayr HO, Stüeken P, Münch EO, Wolter M, Bernstein A, Suedkamp NP, et al. Brace or no-brace after ACL graft. Four-year results of a prospective clinical trial. Knee Surg Sports Traumatol Arthrosc. 2014;22:1156–1162. doi: 10.1007/s00167-013-2564-2. [DOI] [PubMed] [Google Scholar]
- 23.Harilainen A, Sandelin J. Post-operative use of knee brace in bone-tendon-bone patellar tendon anterior cruciate ligament reconstruction: 5-year follow-up results of a randomized prospective study. Scand J Med Sci Sports. 2006;16:14–18. doi: 10.1111/j.1600-0838.2004.00435.x. [DOI] [PubMed] [Google Scholar]
- 24.Yang XG, Feng JT, He X, Wang F, Hu YC. The effect of knee bracing on the knee function and stability following anterior cruciate ligament reconstruction: A systematic review and meta-analysis of randomized controlled trials. Orthop Traumatol Surg Res. 2019;105:1107–1114. doi: 10.1016/j.otsr.2019.04.015. [DOI] [PubMed] [Google Scholar]
- 25.Wright RW, Preston E, Fleming BC, Amendola A, Andrish JT, Bergfeld JA, et al. A systematic review of anterior cruciate ligament reconstruction rehabilitation: Part I: Continuous passive motion, early weight bearing, postoperative bracing, and home-based rehabilitation. J Knee Surg. 2008;21:217–224. doi: 10.1055/s-0030-1247822. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Wright RW, Fetzer GB. Bracing after ACL reconstruction: A systematic review. Clin Orthop Relat Res. 2007;455:162–168. doi: 10.1097/BLO.0b013e31802c9360. [DOI] [PubMed] [Google Scholar]
- 27.Masini BD, Owens BD. Current recommendations for anterior cruciate ligament bracing: When to use. Phys Sportsmed. 2013;41:35–39. doi: 10.3810/psm.2013.02.1997. [DOI] [PubMed] [Google Scholar]
- 28.Rodríguez-Merchán EC. Knee bracing after anterior cruciate ligament reconstruction. e602-9Orthopedics. 2016;39 doi: 10.3928/01477447-20160513-04. [DOI] [PubMed] [Google Scholar]
- 29.Pezzullo DJ, Fadale P. Current controversies in rehabilitation after anterior cruciate ligament reconstruction. Sports Med Arthrosc Rev. 2010;18:43–47. doi: 10.1097/JSA.0b013e3181cdb5d3. [DOI] [PubMed] [Google Scholar]
- 30.DeVita P, Lassiter T Jr, Hortobagyi T, Torry M. Functional knee brace effects during walking in patients with anterior cruciate ligament reconstruction. Am J Sports Med. 1998;26:778–784. doi: 10.1177/03635465980260060701. [DOI] [PubMed] [Google Scholar]
- 31.Melegati G, Tornese D, Bandi M, Volpi P, Schonhuber H, Denti M. The role of the rehabilitation brace in restoring knee extension after anterior cruciate ligament reconstruction: A prospective controlled study. Knee Surg Sports Traumatol Arthrosc. 2003;11:322–326. doi: 10.1007/s00167-003-0386-3. [DOI] [PubMed] [Google Scholar]
- 32.Risberg MA, Holm I, Steen H, Eriksson J, Ekeland A. The effect of knee bracing after anterior cruciate ligament reconstruction. A prospective, randomized study with two years' follow-up. Am J Sports Med. 1999;27:76–83. doi: 10.1177/03635465990270012101. [DOI] [PubMed] [Google Scholar]
- 33.Sterett WI, Briggs KK, Farley T, Steadman JR. Effect of functional bracing on knee injury in skiers with anterior cruciate ligament reconstruction: A prospective cohort study. Am J Sports Med. 2006;34:1581–1585. doi: 10.1177/0363546506289883. [DOI] [PubMed] [Google Scholar]
- 34.Fleming BC, Renstrom PA, Beynnon BD, Engstrom B, Peura G. The influence of functional knee bracing on the anterior cruciate ligament strain biomechanics in weightbearing and nonweightbearing knees. Am J Sports Med. 2000;28:815–824. doi: 10.1177/03635465000280060901. [DOI] [PubMed] [Google Scholar]
- 35.Lu TW, Lin HC, Hsu HC. Influence of functional bracing on the kinetics of anterior cruciate ligament-injured knees during level walking. Clin Biomech (Bristol, Avon) 2006;21:517–524. doi: 10.1016/j.clinbiomech.2005.12.017. [DOI] [PubMed] [Google Scholar]
- 36.Barber-Westin SD, Noyes FR. Factors used to determine return to unrestricted sports activities after anterior cruciate ligament reconstruction. Arthroscopy. 2011;27:1697–1705. doi: 10.1016/j.arthro.2011.09.009. [DOI] [PubMed] [Google Scholar]
- 37.Petersen W, Zantop T. Return to play following ACL reconstruction: Survey among experienced arthroscopic surgeons (AGA instructors) Arch Orthop Trauma Surg. 2013;133:969–977. doi: 10.1007/s00402-013-1746-1. [DOI] [PubMed] [Google Scholar]
- 38.Eckenrode BJ, Carey JL, Sennett BJ, Zgonis MH. Prevention and management of post-operative complications following ACL reconstruction. Curr Rev Musculoskelet Med. 2017;10:315–321. doi: 10.1007/s12178-017-9427-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.van der List JP, DiFelice GS. Range of motion and complications following primary repair versus reconstruction of the anterior cruciate ligament. Knee. 2017;24:798–807. doi: 10.1016/j.knee.2017.04.007. [DOI] [PubMed] [Google Scholar]
- 40.Ma R, Sheth C, Fenkell B, Buyuk , AF The role of bracing in ACL injuries: The current evidentiary state of play. J Knee Surg. 2022;35:255–265. doi: 10.1055/s-0042-1742304. [DOI] [PubMed] [Google Scholar]