Abstract
Objective
To investigate the effect of cervical stabilization exercises on cervical position error in patients with axial spondyloarthritis (axSpA).
Materials and methods
Thirty-nine patients with axSpA were randomly allocated to two groups as exercise group (n = 20, 11 males) and control group (n = 19, 12 males). The exercise group performed a progressive home-based cervical stabilization exercise program, while the control group did not receive any exercise intervention. To control exercise adherence and progression, text messages and video instructions were delivered via a freeware and cross-platform messaging service on a weekly basis. All patients were evaluated regarding physical characteristics, disease activity (Bath Ankylosing Spondylitis Disease Activity Index), functional status (Bath Ankylosing Spondylitis Functional Index), and spinal mobility (Bath Ankylosing Spondylitis Metrology Index). Cervical position error was evaluated in flexion, extension, rotation, and lateral flexion directions. All evaluations were performed at baseline and after 6 weeks.
Results
Baseline physical and disease-related characteristics were similar between the groups (p > 0.05). After 6 weeks, significant improvements were observed in cervical position error in all directions in the exercise group (p < 0.05), whereas no improvements were detected in the control group (p > 0.05).
Conclusion
A 6-week home-based cervical stabilization exercise program seems to be beneficial for improving impaired cervical proprioception in patients with axSpA.
Keywords: Spondyloarthritis, Exercise, Proprioception, Neck, Functional status
Abstract
Ziel
Ziel der Arbeit war es, die Wirkung von Übungen zur Stabilisierung der Halswirbelsäule auf deren zervikaler Positionsfehler bei Patienten mit axialer Spondyloarthritis (axSpA) zu untersuchen.
Material und Methoden
Dazu wurden 39 Patienten mit axSpA randomisiert in 2 Gruppen eingeteilt, eine Übungsgruppe (n = 20, 11 m.) und eine Kontrollgruppe (n = 19, 12 m.). Die Übungsgruppe führte ein stufenweise aufbauendes Heimprogramm zur Halswirbelsäulenstabilisierung durch, während die Kontrollgruppe keine Übungsintervention erhielt. Um die Einhaltung der Übungen und ihren Fortschritt zu kontrollieren, wurden wöchentlich Textnachrichten und Videoanleitungen über einen freien und plattformübergreifenden Messagerdienst gesendet. Sämtliche Patienten wurden hinsichtlich körperlicher Merkmale, Krankheitsaktivität (Bath Ankylosing Spondylitis Disease Activity Index), funktionellem Status (Bath Ankylosing Spondylitis Functional Index), und Wirbelsäulenbeweglichkeit (Bath Ankylosing Spondylitis Metrology Index) untersucht. Zervikale Positionsfehler der Halswirbelsäule wurden in Flexion, Extension, Rotation und Lateralflexion beurteilt. Alle Untersuchungen wurden zu Anfang der Studie und nach 6 Wochen durchgeführt.
Ergebnisse
Die körperlichen und krankheitsbezogenen Merkmale zu Anfang waren zwischen den beiden Gruppen ähnlich (p > 0,05). Nach 6 Wochen wurden in der Übungsgruppe signifikante Verbesserungen der zervikalen Positionsfehler der Halswirbelsäule in allen Richtungen festgestellt (p < 0,05), während in der Kontrollgruppe keine Verbesserungen zu beobachten waren (p > 0,05).
Schlussfolgerung
Ein 6‑wöchiges häusliches Übungsprogramm zur Stabilisierung der Halswirbelsäule scheint vorteilhaft zu sein, um die beeinträchtigte zervikale Propriozeption bei Patienten mit axSpA zu verbessern.
Schlüsselwörter: Spondyloarthritis, Bewegungsübungen, Propriozeption, Hals, Funktioneller Status
Introduction
Axial spondyloarthritis (axSpA) is a chronic inflammatory disease which is classified into two subtypes according to radiographic findings as radiographic axSpA (ankylosing spondylitis) and non-radiographic axSpA [1]. Spinal involvement is a dominant feature of the disease, and the sacroiliac joints along with lumbar and cervical regions are frequently involved. It is well known that functional status, muscle functions, quality of life, and emotional status may be diminished in patients with axSpA [2–4]. Recently, our group showed deterioration in the sense of cervical joint position in patients with axSpA [5].
Cervical joint position accuracy is important to maintain optimal head and neck position which is crucial for most activities of daily living. A sense of joint position along with a sense of movement and sense of force are the components of proprioception, which represents the awareness of the body in the space [6]. Sense of joint position is provided by receptors in tendons, ligaments, joint capsules, and joint surfaces [7].
In inflammatory arthritis, chronic inflammation might damage joint surfaces which contribute to the sense of joint position. On the other hand, proprioceptive acuity is also affected by muscle activity [8]. Knoop et al. reported that muscle weakness along with damage in the mechanoreceptors contributes to a decreased sense of position in patients with arthritis [9]. Thus, improving muscle function may help to enhance proprioceptive function.
Jull et al. showed that conventional proprioceptive and craniocervical flexion exercises improved cervical joint position sense in patients with neck pain [10]. Later, they reported that craniocervical exercises improve proprioception by activating the deep flexor muscles and restoring the coordination between deep and superficial neck muscles [11]. Similarly, cervical stabilization exercises primarily aim to activate deep cervical muscles. Thus, utilizing these exercises may help to improve proprioception sense. Moreover, Lee et al. showed that performing cervical stabilization exercises leads to improvement in the accuracy of joint position sense in healthy participants [12]. However, to the best of our knowledge, there are no previous studies investigating the effects of cervical stabilization exercises on proprioception in patients with axSpA. Therefore, in the present pilot study, we aimed to investigate the effects of cervical stabilization exercises on cervical joint position error in patients with axSpA.
Methods
This was a prospective study performed between September and December 2019 in Izmir Katip Celebi University, Ataturk Research and Training Hospital. The study was approved by the Izmir Katip Celebi University Ethical Committee with approval number of 325/2019. The study was registered in ClinicalTrials.gov (NCT04483648).
Patients
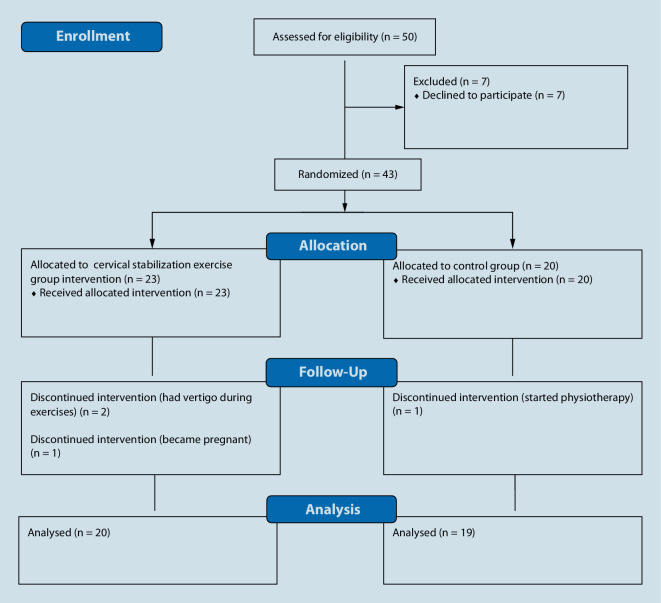
Fifty patients with axSpA according to the Assessment of Spondyloarthritis International Society (ASAS) criteria were invited to join the study [1]. Seven patients declined to participate. Patients who had neck trauma history, complete spinal ankylosis, orthopedic disability, cervical spinal surgery, and/or vestibular system problems were excluded. The flowchart of the study is given in Fig. 1. All patients gave informed consent prior to participation in the study.
Fig. 1.
Flowchart of the study
Procedures
Every participant completed a structured form containing demographic data (age, sex, height, weight), disease activity (Bath Ankylosing Spondylitis Disease Activity Index) [13], and functional status (Bath Ankylosing Spondylitis Functional Index) [14]. Spinal mobility (Bath Ankylosing Spondylitis Metrology Index) [15] was assessed by a rheumatologist and the cervical joint position error (JPE) was evaluated by a physiotherapist. Patients were then randomly allocated to two groups as exercise and control using opaque envelopes. The patients in the exercise group performed a 6-week progressive home-based cervical stabilization exercise program along with their regular treatment, while the patients in the control group maintained their regular treatment only. Cervical JPE was reassessed after 6 weeks.
Outcome measures
Cervical joint position error
The neutral head position method, which shows high reliability and accuracy, was used to evaluate cervical JPE [16]. The patients were seated upright with a straight head position on a standard chair with a back support at 100 cm from the measurement wall. A piece of 1‑mm-squared graphical drawing paper (width 100 cm, height 100 cm) was placed on the wall. Then a plastic helmet with a laser pointer inserted at the top was placed on the head of the patient [5]. The method was also recently employed by our group to determine the status of cervical JPE in patients with axSpA [5]. A soft opaque fabric eye mask was placed over their eyes, and they were asked to memorize their neutral head position. The patients were then instructed to move their head into flexion, extension, right and left lateral flexion, and right and left rotation. Initially, a reference point was determined for each direction and each movement was repeated three times. Ten seconds of rest were provided between attempts for the same direction and 1 min rest was allowed between different directions. The absolute JPE was calculated using the formula angle = tan − 1 (error distance/90 cm) for each trial, and the average of three measurements was used in the analysis for each direction for each participant. All JPE assessments were performed by the same investigator.
Interventions
Cervical stabilization exercises
The patients in the cervical stabilization exercise group performed progressive home-based cervical stabilization exercises three times a week for 6 weeks. The unilateral/bilateral upper and lower extremity movements with/without an external loads were performed in four different positions: lying in supine, lying in prone, in quadrupedal, and in standing. Chin-tuck position was maintained during each movement. The exercise program was progressed by increasing isometric contraction times of the chin-tuck exercises and the repetitions of the movements (Table 1; Fig. 2). Each week, a short video message including exercises along with the instructions was delivered to patients via a freeware and cross-platform messaging service (WhatsApp messenger; Meta, Menlo Park, CA, USA) in order to control exercise adherence and to inform about exercise progression. An exercise session lasted approximately 20 min.
Table 1.
Progression of the cervical stabilization exercises
| Week | Movements | Chin-tuck time | Repeats (for each position) |
|---|---|---|---|
| 1–2 | Maintaining chin-tuck position in supine, prone, quadrupedal, and standing positions | 10 s | 10 times |
| 3 | Maintaining chin-tuck position plus unilateral and bilateral upper and reciprocal lower extremity movements in supine, prone, quadrupedal, and standing positions | 5 s | 5 times |
| 4 | Maintaining chin-tuck position plus unilateral and bilateral upper extremity with an external load of 500 ml full water bottle and reciprocal lower extremity movements in supine, prone, quadrupedal, and standing positions | 5 s | 12 times |
| 5 | Maintaining chin-tuck position plus unilateral and bilateral upper extremity with an external load of 500 ml full water bottle and reciprocal lower extremity movements in supine, prone, quadrupedal, and standing positions | 10 s | 12 times |
| 6 | Maintaining chin-tuck position plus unilateral and bilateral upper extremity with an external load of 500 ml full water bottle and reciprocal lower extremity movements in supine, prone, quadrupedal, and standing positions | 15 s | 12 times |
Fig. 2.
Cervical stabilization exercise samples (red arrows to this direction)
Statistical analysis
Statistical Package for the Social Sciences software (SPSS) version 18.0 (IBM®, Armonk, NY, USA) was used for statistical analyses. The normality of the data was investigated using the Shapiro–Wilk test and histograms. Non-parametric analyses were used due to the heterogeneity of the data. Thus, continuous variables were expressed as median (interquartile range) and categorical variables were presented as percentages. Mann–Whitney U test and chi-square tests were used to compare the groups. Wilcoxon signed-rank test was used to compare in-group changes. A p-value of < 0.05 was accepted as the statistical significance level.
Results
In total, 39 patients with axSpA completed the study (exercise group: n = 20, 11 males; control group: n = 19, 12 males). Fifteen (75%) and 16 patients (84%) were using anti-tumor necrosis factor (TNF) agents in the exercise group and in the control group, respectively. No changes in patients’ medication were performed during the study. Thirteen (65%) and 14 patients (74%) were radiographic axSpA in the exercise group and in the control group (p = 0.557), respectively. Ten patients had cervical syndesmophytes in the exercise group, and 5 patients has syndesmophytes in the control group (p = 0.049). The demographic, physical, and disease-related characteristics were comparable between groups (Table 2). No patients reported adverse effects related to the exercise program.
Table 2.
Physical and disease-related characteristics
| Exercise group (n = 20) | Control group (n = 19) | P-value | |
|---|---|---|---|
| Median (IQR 25/75) | Median (IQR 25/75) | ||
| Physical characteristics | |||
| Age (years) | 40.5 (36.0/52.5) | 44.0 (39.0/49.5) | 0.496a |
| Height (cm) | 168.5 (160.0/176.5) | 175.0 (168.5/178.5) | 0.214a |
| Weight (kg) | 78.5 (67.0/91.5) | 84.0 (70.0/90.0) | 0.687a |
| Body mass index (kg/m2) | 27.5 (24.5/30.2) | 26.8 (23.6/29.3) | 0.569a |
| Male sex (n, %) | 11 (55%) | 12 (63%) | 0.605b |
| Disease-related characteristics | |||
| Time since onset of symptoms (years) | 14.5 (9.0/20) | 11 (7.0/14.0) | 0.403a |
| Time since diagnosis (years) | 9.0 (4.0/11.5) | 6.0 (3.0/7.0) | 0.113a |
| BASDAI (score) | 2.0 (1.0/3.3) | 1.8 (1.3/2.5) | 0.687a |
| BASMI tragus–wall distance (score) | 2.0 (1.0/3.2) | 2.0 (1.0/3.2) | 0.945a |
| BASMI cervical rotation (score) | 2.0 (1.6/3.1) | 2.0 (1.4/3.2) | 0.708a |
| BASMI total (score) | 2.9 (1.7/4.1) | 2.3 (1.8/3.1) | 0.127a |
| BASFI (score) | 1.8 (0.6/2.9) | 1.2 (1.0/2.2) | 0.496a |
| Cervical proprioception error | |||
| Flexion (o) | 4.9 (2.2/7.0) | 6.3 (3.5/7.3) | 0.444a |
| Extension (o) | 4.5 (3.3/6.4) | 5.5 (4.5/7.3) | 0.247a |
| Right Rotation (o) | 5.2 (3.0/8.9) | 6.4 (4.3/9.0) | 0.513a |
| Left Rotation (o) | 4.3 (2.5/5.0) | 5.4 (3.5/7.9) | 0.084a |
| Right Lateral Flexion (o) | 4.9 (3.3/6.8) | 5.9 (3.6/8.4) | 0.531a |
| Left Lateral Flexion (o) | 4.3 (2.1/6.7) | 3.8 (2.4/5.6) | 0.857a |
IQR 25/75 Interquartile range 25/75, BASDAI Bath Ankylosing Spondylitis Disease Activity Index, BASMI Bath Ankylosing Spondylitis Metrology Index, BASFI Bath Ankylosing Spondylitis Functional Index
aMann–Whitney U test
bChi-square test
Cervical JPE was similar between groups for all directions at baseline (p > 0.05, Table 3). Cervical JPE was significantly improved after 6 weeks in the exercise group for all directions (p < 0.05, Table 3), while no improvements were observed in the control group (p > 0.05, Table 3). Although cervical stabilization exercises resulted higher net changes in JPE measurements in comparison to control patients, those differences did not reach statistical significance (Table 4, p > 0.05).
Table 3.
Changes in cervical joint position errors in the groups
| Before | After | p-valuea | |
|---|---|---|---|
| Median (IQR 25/75) | Median (IQR 25/75) | ||
| Exercise group (n = 20) | |||
| Flexion (o) | 4.9 (2.2/7.0) | 2.8 (1.7/3.8) | 0.033* |
| Extension (o) | 4.5 (3.3/6.4) | 3.1 (1.8/4.8) | 0.040* |
| Right rotation (o) | 5.2 (3.0/8.9) | 3.7 (1.9/4.7) | 0.006* |
| Left rotation (o) | 4.3 (2.5/5.0) | 2.8 (2.2/3.3) | 0.017* |
| Right lateral flexion (o) | 4.9 (3.3/6.8) | 2.3 (1.8/3.7) | 0.009* |
| Left lateral flexion (o) | 4.3 (2.1/6.7) | 2.0 (1.5/3.4) | 0.010* |
| Control group (n = 19) | |||
| Flexion (o) | 6.3 (3.5/7.3) | 5.2 (3.8/7.0) | 0.856 |
| Extension (o) | 5.5 (4.5/7.3) | 4.1 (3.3/8.2) | 0.809 |
| Right rotation (o) | 6.4 (4.3/9.0) | 5.5 (3.0/8.5) | 0.472 |
| Left rotation (o) | 5.4 (3.5/7.9) | 5.0 (3.5/7.2) | 0.778 |
| Right lateral flexion (o) | 5.9 (3.6/8.4) | 4.3 (2.7/7.7) | 0.717 |
| Left lateral flexion (o) | 3.8 (2.4/5.6) | 4.9 (2.9/5.7) | 0.904 |
IQR 25/75 Interquartile range 25/75
aWilcoxon signed-rank test
*p < 0.05
Table 4.
Comparison of the net changes in the cervical joint position errors between groups
| Direction | Exercise group | Control group | p-valuea |
|---|---|---|---|
| (n = 20) | (n = 19) | ||
| Median (IQR 25/75) | Median (IQR 25/75) | ||
| ∆ Flexion (o) | −1.5 (−4.8/0.8) | 0.3 (−1.6/2.5) | 0.079 |
| ∆ Extension (o) | −1.9 (−3.5/0.9) | 0.3 (−2.4/2.7) | 0.177 |
| ∆ Right rotation (o) | −2.5 (−5.2/−0.6) | −0.4 (−2.3/1.0) | 0.081 |
| ∆ Left rotation (o) | −2.0 (−3.3/−0.7) | 0.7 (−3.7/2.7) | 0.133 |
| ∆ Right lateral flexion (o) | −1.0 (−2.6/−0.1) | 0.2 (−1.9/1.4) | 0.164 |
| ∆ Left lateral flexion (o) | −1.9 (−4.9/−0.3) | −0.2 (−2.7/2.8) | 0.109 |
IQR 25/75 Interquartile range 25/75, ∆ difference
aMann–Whitney U test
Discussion
The results of the present pilot study showed for the first time that performing a home-based cervical stabilization exercise program three times a week is beneficial for improving cervical position error compared to usual care in patients with axSpA.
The cervical spine is a commonly affected region in axSpA. Our group recently showed that patients with axSpA have higher cervical joint position error compared to healthy controls [5]. The cervical region contains a high density of mechanoreceptors [17], where most are located in the deep cervical muscles and their attachments. Thus, a static chin-tuck exercise was mainly used as the cervical stabilization exercise in various body positions in the present study and combined with dynamic extremity movements. Sustaining chin-tuck exercises activates deep cervical muscles and allows patients to be aware of their cervical positions at a certain time which might lead to improvements in proprioception. In addition, cervical stabilization exercises might lead to improvements in muscle functions such as strength and endurance, which may also improve the cervical joint position error.
The positive effects of exercise on cervical proprioception have been reported previously [10, 18]. However, there is no established standardized exercise protocol for proprioceptive rehabilitation of the cervical region. Previous studies used eye/head coordination exercises, gaze stability exercises, head relocation exercises, eye-follow exercises, and craniocervical flexion training. Craniocervical training as described by Jull et al. targets the deep flexor muscles that control cervical lordosis flattening during exercises [10]. The chin-tuck exercises in the present study also flatten the cervical lordosis, similar to exercises in the study of Jull et al. [10]. It seems that positioning the neck in a flattened cervical position may lead to improvements in proprioception sense by activating deep cervical flexor muscles. Repeated contractions during cervical stabilization exercises may also enhance the spindle function, which contributes to cervical proprioception. In addition, Lee et al. showed improvements in the cervical position error following cervical stabilization exercises in healthy subjects [12].
Improvements in the cervical position error were observed in all directions following the cervical stabilization exercise program in the present study. On the other hand, the control group, who received their usual care, did not show any significant improvements in the study period. However, when the changes were compared between groups, even though the cervical stabilization exercise group obtained better results, no statistical significance was detected between groups. This may be related to the relatively small sample size of the study, or the 6‑week exercise period may not be adequate to establish a possible difference.
The effect of the exercises on cervical proprioception was investigated for the first time in the present study. The exercise program was delivered via a messaging service (WhatsApp messenger; Meta, Menlo Park, CA, USA) throughout the study. Patients received their exercises as short video instructions on a weekly basis, and they performed their exercises at home. In addition, they were regularly controlled via the same messaging platform weekly. Obtaining promising results from a such home exercise program is especially important for current conditions with the world facing the COVID-19 pandemic. In this regard, performing regular exercise programs with minimum physical contact may be a good example of telerehabilitation for these kinds of emergencies.
Previous studies have ensured the correct position during cervical exercises using a biofeedback unit (Stabilizer Pressure Biofeedback Unit; Chattanooga Group Inc., Hixson, TN, USA). However, as we used cervical stabilization exercises as a home-exercise program, we could not benefit from this tool.
Proprioception was evaluated in terms of one aspect only (position sense) in the present study; however, the effect of a stabilization exercise program on other parameters of proprioception such as kinesthesia may be different. Also, the effects of cervical stabilization exercises on other parameters such as balance, physical functions, and activities of daily living yet to be discovered and should be addressed in future studies. In addition, different cervical stabilization exercise programs with various loadings, durations, or times should be investigated to determine the optimal program. The lack of longer follow-up is another limitation of the present study. Moreover, the small sample size of the present pilot study may not allow us to draw firm conclusions. Future studies with more participants are needed to confirm the results.
According to the results of the present study, a 6-week home-based cervical stabilization exercise program is beneficial for improving cervical proprioception in patients with axSpA. Patients should be encouraged to exercise on a regular basis and home-based exercise programs with regular follow-ups may be used in cases where physical contact should be avoided.
Declarations
Conflict of interest
H.E. Oz, G. Duran, D. Bayraktar, M. Kara, D. Solmaz, and S. Akar declare that they have no competing interests.
All procedures performed in studies involving human participants or on human tissue were in accordance with the ethical standards of the institutional and/or national research committee and with the 1975 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study. Additional informed consent was obtained from all individual participants from whom identifying information is included in this article. Clinical trial registration: ClinicalTrials.gov (NCT04483648).
Footnotes

Scan QR code & read article online
References
- 1.Rudwaleit M, van der Heijde D, Landewé R, Listing J, Akkoc N, Brandt J, et al. The development of Assessment of SpondyloArthritis international Society classification criteria for axial spondyloarthritis (part II): validation and final selection. Ann Rheum Dis. 2009;68:777–783. doi: 10.1136/ard.2009.108233. [DOI] [PubMed] [Google Scholar]
- 2.Strand V, Singh JA. Patient burden of axial spondyloarthritis. J Clin Rheumatol. 2017;23:383–391. doi: 10.1097/RHU.0000000000000589. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Garrido-Cumbrera M, Delgado-Domínguez CJ, Gálvez-Ruiz D, Mur CB, Navarro-Compán V, Atlas Working Group The effect of axial spondyloarthritis on mental health: results from the atlas. J Rheumatol. 2019;46:1284–1289. doi: 10.3899/jrheum.180868. [DOI] [PubMed] [Google Scholar]
- 4.Valido A, Crespo CL, Pimentel-Santos FM. Muscle evaluation in axial spondyloarthritis-the evidence for sarcopenia. Front Med. 2019;6:219. doi: 10.3389/fmed.2019.00219. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Ozen T, Tonga E, Polat MG, Bayraktar D, Akar S. Cervical proprioception accuracy is impaired in patients with axial spondyloarthritis. Musculoskelet Sci Pract. 2021;51:102304. doi: 10.1016/j.msksp.2020.102304. [DOI] [PubMed] [Google Scholar]
- 6.Röijezon U, Clark NC, Treleaven J. Proprioception in musculoskeletal rehabilitation. Part 1: Basic science and principles of assessment and clinical interventions. Man Ther. 2015;20:368–377. doi: 10.1016/j.math.2015.01.008. [DOI] [PubMed] [Google Scholar]
- 7.Hogervorst T, Brand RA. Mechanoreceptors in joint function. J Bone Joint Surg Am. 1998;80:1365–1378. doi: 10.2106/00004623-199809000-00018. [DOI] [PubMed] [Google Scholar]
- 8.Proske U, Wise AK, Gregory JE. The role of muscle receptors in the detection of movements. Prog Neurobiol. 2000;60:85–96. doi: 10.1016/s0301-0082(99)00022-2.. [DOI] [PubMed] [Google Scholar]
- 9.Knoop J, Steultjens MP, van der Leeden M, van der Esch M, Thorstensson CA, Roorda LD, et al. Proprioception in knee osteoarthritis: a narrative review. Osteoarthritis Cartilage. 2011;19:381–388. doi: 10.1016/j.joca.2011.01.003. [DOI] [PubMed] [Google Scholar]
- 10.Jull G, Falla D, Treleaven J, Hodges P, Vicenzino B. Retraining cervical joint position sense: the effect of two exercise regimes. J Orthop Res. 2007;25:404–412. doi: 10.1002/jor.20220. [DOI] [PubMed] [Google Scholar]
- 11.Jull GA, Falla D, Vicenzino B, Hodges PW. The effect of therapeutic exercise on activation of the deep cervical flexor muscles in people with chronic neck pain. Man Ther. 2009;14:696–701. doi: 10.1016/j.math.2009.05.004. [DOI] [PubMed] [Google Scholar]
- 12.Lee MY, Kim SG, Lee HY. The effect of cervical stabilization exercise on active joint position sense: a randomized controlled trial. J Back Musculoskelet Rehabil. 2016;29:85–88. doi: 10.3233/BMR-150601. [DOI] [PubMed] [Google Scholar]
- 13.Akkoc Y, Karatepe AG, Akar S, Kirazli Y, Akkoc N. A Turkish version of the bath ankylosing spondylitis disease activity index: reliability and validity. Rheumatol Int. 2005;25(4):280–284. doi: 10.1007/s00296-003-0432-y. [DOI] [PubMed] [Google Scholar]
- 14.Ozer HT, Sarpel T, Gulek B, Alparslan ZN, Erken E. The Turkish version of the bath ankylosing spondylitis functional index: reliability and validity. Clin Rheumatol. 2005;24(2):123–128. doi: 10.1007/s10067-004-0984-6. [DOI] [PubMed] [Google Scholar]
- 15.Jenkinson TR, Mallorie PA, Whitelock HC, Kennedy LG, Garrett SL, Calin A. Defining spinal mobility in ankylosing spondylitis (AS). The Bath AS Metrology Index. J Rheumatol. 1994;21(9):1694–1698. [PubMed] [Google Scholar]
- 16.Revel M, Andre-Deshays C, Minguet M. Cervicocephalic kinesthetic sensibility in patients with cervical pain. Arch Phys Med Rehabil. 1991;72:288–291. [PubMed] [Google Scholar]
- 17.Boyd-Clark LC, Briggs CA, Galea MP. Muscle spindle distribution, morphology, and density in longus colli and multifidus muscles of the cervical spine. Spine. 1976;27:694–701. doi: 10.1097/00007632-200204010-00005. [DOI] [PubMed] [Google Scholar]
- 18.Humphreys BK, Irgens PM. The effect of a rehabilitation exercise program on head repositioning accuracy and reported levels of pain in chronic neck pain subjects. J Whiplash Rel Disord. 2002;1:99–112. [Google Scholar]