Abstract
Objective
Knee osteoarthritis (OA) can substantially limit function, which can be assessed both objectively and subjectively. We examined whether objective performance tests are associated with self-reported function.
Methods
We analyzed baseline data from the Osteoarthritis Registry of Biomarker and Imaging Trajectories (ORBIT) of participants ≥40 years old with symptomatic and radiographic knee OA. Subjects completed the Knee Injury and Osteoarthritis Outcome Score (KOOS) Pain and Activities of Daily Living (ADL) scales and other assessments of pain and comorbidity. Subjects performed the timed single leg balance test (SLB), 30-s sit-to-stand (30s STS), Timed-Up-and-Go (TUG), and 40-m fast paced walk (40 m Walk). We used Pearson correlation coefficients to examine associations between performance and KOOS subscales. We adjusted for potential confounders using partial correlations.
Results
We enrolled 101 subjects (mean age 63.7 (standard deviation (SD) 10.1), mean BMI 30.0 (SD 5.6), and 63% female). The mean (SD) values for the performance tests were: SLB 20.1 (18.9) seconds, 30s STS 11.7 (4.6) stands, TUG 9.4 (2.3) seconds, and 40 m Walk 27.6 (6.5) seconds. Correlations between performance tests and self-report measures did not exceed 0.39, with the absolute value of correlations between KOOS ADL and performance measures ranging from 0.24 to 0.39. Adjusted partial correlations were largely similar to the crude correlations.
Conclusions
Self-reported function in persons with knee OA had weak to modest correlations with objective function. Objective performance tests capture elements of physical function that self-report data do not and point to the potential value of including objective measures of functional status in OA trials.
1. Introduction
Osteoarthritis (OA) is the most common joint disorder in the United States (US) affecting more than 32 million US adults [1,2]. Symptomatic knee OA accounts for approximately one third of OA ambulatory visits [3]. Pain predominates the lived experience of people with knee OA, limiting valued physical activities [3]. Consequently, the key outcome domains in studies of knee OA include pain and physical function.
Most investigations of the natural history and treatment outcomes of OA use self-report measures to assess pain and physical functional status [4], with objective physical performance measures evaluated less frequently. Self-report measures do not require face-to-face contact between subjects and the research team, but they may not accurately reflect the subject's true capability. Objective measures have been associated with several clinically important outcomes in persons with OA including falls, incident diabetes, and total knee replacement [[5], [6], [7], [8]]. Several studies have examined associations between self-report measures of pain and function and objective performance tests in adults with knee OA. Most of these studies were performed in persons with OA who underwent joint replacement [[9], [10], [11], [12]], with more limited research among persons with knee OA who are treated nonoperatively [13].
The goal of this study was to examine the associations of self-reported pain and function measures with objective physical performance measures in men and women with knee OA.
2. Methods
The Osteoarthritis Registry of Biomarkers and Imaging Trajectories (ORBIT) is a prospective cohort study of adults with a diagnosis of knee OA recruited from the practices of sixteen orthopedic surgeons and rheumatologists at the Brigham and Women's Hospital Orthopedic and Arthritis Center. We used the Partners Research Patient Data Repository (RPDR) to identify potentially eligible subjects by diagnosis codes. The initial screening consisted of a review of both medical records and an assessment of a standing bilateral radiograph taken within 2 years of the screen date. Eligible subjects were at least 40 years of age, English-speaking, community-dwelling, had radiographic evidence of OA in one knee defined by Kellgren-Lawrence (KL) grade 2 or 3,14 and reported at least mild knee pain in the prior four weeks. Exclusion criteria included pregnancy, dementia or other psychological condition precluding safe participation, claiming worker's compensation for knee pain, clinical contraindication for MRI, inflammatory joint disease (gout/pseudogout allowed), prior or planned total knee replacement, and KL grade of 4 in either knee on a standing bilateral radiograph. Subjects who met all inclusion criteria and did not meet any exclusion criteria were considered eligible and approached to participate. Interested subjects were scheduled for an in-person study visit, consisting of a battery of questionnaires, imaging (magnetic resonance imaging (MRI) of both knees and a standing bilateral radiograph), the collection of blood and urine samples, and performance tests.
2.1. Self-report measures
We ascertained self-reported knee pain with the KOOS Pain scale, and we assessed self-reported functional status with the KOOS ADL scale (0–100, 100 best) [[15], [16], [17]]. For pain-related analyses, we either used KOOS Pain from the self-reported most bothersome knee or the higher of the two KOOS Pain scores for subjects who stated that their two knees bothered them similarly. We assessed depressive symptoms using the five-item Mental Health Index (MHI-5, a measure of anxiety and depressive symptoms) scored as a sum of 5 responses (two reversed in scoring) and transposed the sum to a 0–100 scale, with 100 best [18]. We also included the Neuropathic Pain Scale (NPS), which is comprised of 10 pain descriptor items, each rated 0–10, totaling 0–100 with 100 most severe [19,20]. To assess the degree of pain catastrophizing, including patients’ negative or exaggerated attitudes toward pain, we used the 13-item Pain Catastrophizing Scale (PCS) [[21], [22], [23], [24]]. Finally, we included an adapted widespread pain index (WPI; sum of 23 possible musculoskeletal pain locations) that assessed pain during the past week.
2.2. Objective performance measures
The single leg balance test (SLB) included two timed trials of balancing on each leg for as long as possible with an upper bound of 60 s per trial [25]. The average of the two tests in each leg were calculated and the analysis used either the average from the more bothersome knee or the lower (worse) value if the subject reported that both knees were equally bothersome. The 30-s sit-to-stand (30s STS) test required participants to complete a full weight transfer from sitting to standing to sitting as many times as possible in 30 s [[25], [26], [27], [28]]. The Timed-Up-and-Go (TUG) captured the time it took for participants to rise from sitting, walk 3 m at their regular pace, return to their seat and sit down. The timed 40-m fast paced walk (40 m Walk) recorded the amount of time it took for participants to walk four consecutive straight segments of 10 m at their fastest walking pace [25,28,29].
2.3. Statistical analysis
We present descriptive demographic and baseline clinical data on the cohort of 101 participants. Given evidence that females, on average, have lower gait speed, strength, and balance, we also examine baseline data and correlation analyses separately for males and females [30,31]. Categorical variables are summarized as percentages and continuous variables as means with standard deviations (SD). We assessed gender differences using chi-square and Fisher's exact tests for categorical variables and t-tests for continuous variables.
We used Pearson correlation coefficients to examine linear associations between each of the performance tests and the self-report measures of pain and functional status. We depicted the relationships between KOOS ADL and the performance measures graphically using box plots, with scores on the performance tests categorized in quartiles. We used partial correlations to adjust the correlations between performance tests and self-reported knee pain and function for MHI-5, NPS, WPI, and PCS. All statistical analyses were performed with the use of SAS software, Version 9.4 (Cary, NC, USA), and a two-sided p value of ≤0.05 was considered to indicate statistical significance.
3. Results
We assessed 101 participants with mean age 63.7 (SD 10.1) and mean body mass index (BMI) of 30.0 (SD 5.6). Participants were predominantly female (63%) and white (86%), and 72 participants (71%) had at least one knee with KL-3 radiographic severity (Table 1). We observed few differences between male and female participants. Males had a significantly higher level of education, with 89% reporting having obtained a post high school degree compared with 62% of females (P = 0.02, Table 1).
Table 1.
Distribution of cohort demographics and baseline measures (n = 101).
| Characteristics | All |
Female |
Male |
P-value |
|---|---|---|---|---|
| (N = 101) |
(N = 64) |
(N = 37) |
||
| N (%) or Mean (SD) | N (%) or Mean (SD) | N (%) or Mean (SD) | ||
| Demographics | ||||
| Age, years | 63.7 (10.1) | 62.6 (10.0) | 65.6 (10.1) | 0.15 |
| Body Mass Index | 30.0 (5.6) | 30.5 (6.1) | 29.1 (4.7) | 0.20 |
| Race (subjects) | 97 | 61 | 36 | 0.34 |
| White | 83 (85.6) | 50 (82.0) | 33 (91.7) | |
| Black | 8 (8.3) | 7 (11.5) | 1 (2.8) | |
| Asian | 4 (4.1) | 2 (3.3) | 2 (5.6) | |
| Other | 2 (2.1) | 2 (3.3) | 0 (0.0) | |
| Hispanic or Latino ethnicity (subjects) | 93 | 62 | 31 | 0.29 |
| No | 85 (91.4) | 57 (91.9) | 28 (90.3) | |
| Yes | 8 (8.6) | 5 (8.1) | 3 (9.7) | |
| Highest Level of Education (subjects) | 99 | 63 | 36 | 0.02 |
| High School | 8 (8.1) | 8 (12.7) | 0 (0.0) | |
| Some College | 20 (20.2) | 16 (25.4) | 4 (11.1) | |
| Associate Degree | 6 (6.1) | 3 (4.8) | 3 (8.3) | |
| Bachelor's Degree or Beyond | 65 (65.7) | 36 (57.1) | 29 (80.6) | |
| KL Grade - Left Knee (subjects) | 101 | 64 | 37 | 0.98 |
| 0 | 0 (0.0) | 0 (0.0) | 0 (0.0) | |
| 1 | 21 (20.8) | 13 (20.3) | 8 (21.6) | |
| 2 | 34 (33.7) | 22 (34.4) | 12 (32.4) | |
| 3 | 46 (45.5) | 29 (45.3) | 17 (46.0) | |
| KL Grade - Right Knee (subjects) | 101 | 64 | 37 | 0.02 |
| 0 | 1 (1.0) | 1 (1.6) | 0 (0.0) | |
| 1 | 5 (5.0) | 2 (3.1) | 3 (8.1) | |
| 2 | 35 (34.7) | 28 (43.8) | 7 (18.9) | |
| 3 | 60 (59.4) | 33 (51.6) | 27 (73.0) | |
| Duration of Pain in More Bothersome Knee (subjects) | 100 | 64 | 36 | 0.11 |
| 0–1 years | 9 (9.0) | 5 (7.8) | 4 (11.1) | |
| 1–2 years | 28 (28.0) | 22 (34.4) | 6 (16.7) | |
| 3–5 years | 24 (24.0) | 17 (26.6) | 7 (19.4) | |
| >5 years | 39 (39.0) | 20 (31.3) | 19 (52.8) | |
| Problem Performing Usual Activities (subjects) | 100 | 64 | 36 | 0.33 |
| No Problem | 26 (26.0) | 17 (26.6) | 9 (25.0) | |
| Some Problems | 46 (46.0) | 32 (50.0) | 14 (38.9) | |
| Moderate Problems | 26 (26.0) | 13 (20.3) | 13 (36.1) | |
| Severe Problems | 2 (2.0) | 2 (3.1) | 0 (0.0) | |
| Measures of Pain, Physical and Mental Health | ||||
| KOOS Pain (in Most Bothersome Knee) | 101 | 64 | 37 | 0.11 |
| Mean score (SD) | 55.8 (17.0) | 54.0 (18.0) | 58.8 (14.7) | |
| KOOS Function (subjects) | 100 | 63 | 37 | 0.53 |
| 66.6 (17.0) | 65.6 (17.1) | 68.3 (16.9) | ||
| Timed Single Leg Balance (subjects) | 99 | 64 | 35 | 0.51 |
| Most Bothersome Knee | 20.1 (18.9) | 20.1 (18.0) | 20.0 (20.8) | |
| 30-Second Sit to Stand (subjects) | 101 | 64 | 37 | 0.06 |
| (mean # stands (SD)) | 11.7 (4.6) | 10.9 (3.6) | 13.1 (5.8) | |
| Timed Up and Go (subjects) | 98 | 62 | 36 | 0.36 |
| Mean seconds (SD) | 9.4 (2.3) | 9.5 (2.2) | 9.2 (2.6) | |
| 40 Meter Walk (subjects) | 99 | 63 | 36 | 0.02 |
| Mean seconds (SD) | 27.6 (6.5) | 28.6 (6.4) | 25.7 (6.4) | |
| MHI-5 (subjects) | 100 | 64 | 36 | 0.54 |
| Mean score (SD) | 73.0 (19.7) | 72.6 (19.9) | 73.7 (19.6) | |
| Neuropathic Pain Scale (subjects) | 100 | 64 | 36 | 0.05 |
| Mean (SD) | 32.3 (16.6) | 34.5 (17.9) | 28.2 (13.2) | |
| Widespread Pain Index (subjects) | 101 | 64 | 37 | 0.14 |
| Mean # Painful Areas (SD) | 6.6 (4.0) | 7.0 (4.2) | 5.8 (3.5) | |
| Pain Catastrophizing Scale (subjects) | 101 | 64 | 37 | 0.22 |
| Mean score (SD) | 9.5 (11.6) | 11.1 (13.3) | 6.7 (7.3) | |
KL = Kellgren-Lawrence osteoarthritis grade, 0 = absence of osteoarthritic changes, 1 = doubtful, possible, 2 = minimal, 3 = moderate [14]; KOOS = Knee Injury and Osteoarthritis Outcome Score, 100 = best [[15], [16], [17]]; MHI = Mental Health Index Score, 100 = best [18]; Neuropathic Pain Scale, 100 = most severe [19,20].
The mean (SD) baseline values of the self-report KOOS Pain and KOOS ADL scales were 55.8 (17.0) and 66.6 (17.0), respectively. Mean baseline values of the performance tests included: SLB (average of the two trials on the most bothersome knee) 20.1 (18.9) seconds, 30s STS 11.7 (4.6) stands, TUG 9.4 (2.3) seconds, and 40 m Walk 27.6 (6.5) seconds (Table 1). Males completed the 40 m walk more quickly than females (28.6 (6.4) vs. 26.7 (6.4) seconds, P = 0.02).
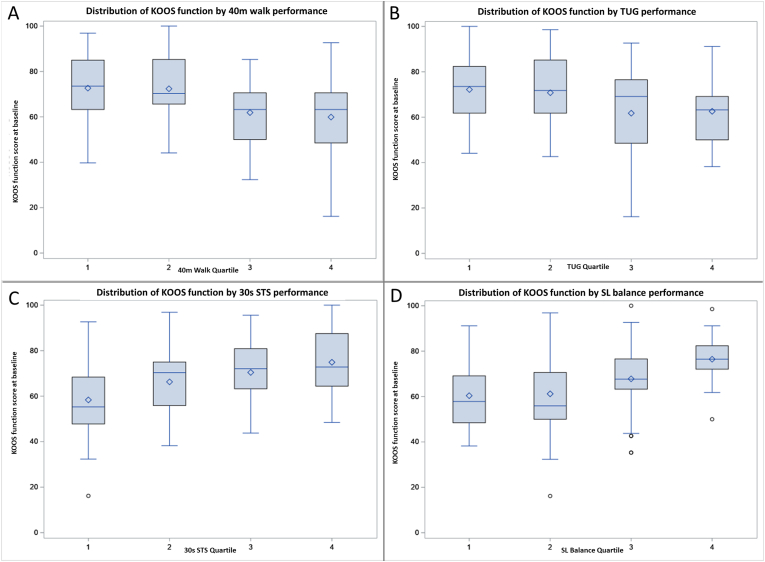
The correlations between performance tests and KOOS Pain, KOOS ADL, PCS, NPS, WPI and MHI-5 are shown in Table 2. Higher (better) scores on KOOS ADL were associated with longer duration on single leg balance (r = 0.39) and greater number of repetitions of sit-to-stand (r = 0.37). Similarly, higher (better) scores on KOOS ADL were associated with faster times on the timed up and go (r = −0.24) and on the 40-m walk (r = −0.30). When these correlation analyses were stratified by gender, the results were similar. The Box Plots in Fig. 1 depict visually the associations between KOOS ADL and the four performance tests. Partial correlations between KOOS ADL score and the performance tests, adjusted for MHI-5, NPS, WPI and PCS, were largely similar to the crude correlations (Table 2).
Table 2.
Correlations (crude and adjusted) associations among self-report and performance measures.
| Timed Single Leg Balancea | 30-Second Sit to Stand | Timed Up and Go | 40 Meter Walk | |
|---|---|---|---|---|
| Pearson Correlation Coefficients for Associations Between Performance Tests and Self-report Measures of Pain, Function and Chronic Pain Features | ||||
| KOOS Pain | 0.31 | 0.29 | −0.14 | −0.34 |
| KOOS ADL | 0.39 | 0.37 | −0.24 | −0.30 |
| Mental Health Index | 0.13 | 0.06 | −0.04 | −0.08 |
| Neuropathic Pain Scale | 0.03 | −0.16 | 0.07 | 0.24 |
| Widespread Pain | −0.23 | −0.21 | 0.00 | 0.17 |
| Pain Catastrophizing | −0.20 | −0.27 | 0.23 | 0.34 |
| Partial Correlations Adjusting for Mental Health, Neuropathic Pain, Widespread Pain and Pain Catastrophizing | ||||
| KOOS Pain | 0.22 | 0.24 | −0.12 | −0.21 |
| KOOS ADL | 0.33 | 0.34 | −0.23 | −0.10 |
The timed single leg (SL) balance values were an average of two trials on the self-reported most bothersome knee. If both knees were reported to be equally bothersome, the knee with the worst (shortest) performance on the SL balance was chosen.
Fig. 1.
Box plots demonstrating association of performance measures with KOOS ADL score.
Box plots indicating relationship between quartiles of performance test and KOOS functional score. KOOS ADL ranges from 0 worst to 100 best. In the 40 m walk (1A) and TUG (1B), the 4th quartile represents those who performed the worst on the test. For the 30s STS (1C) and SL balance (1D), the 4th quartile represents the best performance.
KOOS = Knee Injury and Osteoarthritis Outcome Score, ADL = Activities of Daily Living, 40 m walk = 40 m fast-paced walk, 30s STS = 30 s sit to stand test, TUG = timed up and go, SL balance = single leg balance.
4. Discussion
In a cohort of participants with symptomatic knee OA and moderate (KL 2 or 3) radiographic involvement, we found that self-report pain and function measures had weak to moderate correlations with objective physical performance measures, with Pearson correlation coefficients ranging from 0.24 to 0.39 (Table 2). These data suggest that some elements of physical function that can be measured with objective performance tests (e.g., walking speed, balance, ability to transfer quickly from sit to stand) are not captured fully with self-report measures. These findings point to the potential value of including objective function measures in the assessment of functional status in persons with knee OA and in OA trials.
To our knowledge, few studies have reported the correlation between self-report of functional status and objective physical performance in non-surgical cohorts with knee OA. One study of subjects with primary OA reported moderate correlation between a 6-min walk test (6 MW) and KOOS Pain and ADL subscales (0.62 and 0.46, respectively; Table 3) [13]. While our study did not use the 6 MW, we used the same KOOS scoring rubric (100 = best), and found that the correlation between KOOS ADL and the 40 m walk (which took our subjects a mean of 27.6 s) was −0.30. The contrasting findings in these two studies of a brief (40-m walk) and longer (6-min walk) walking test suggest that self-reported functional limitation may be governed in part by endurance.
Table 3.
Previous studies examining correlations between self-report and performance measures.
| Author, Year & Country | Cohort | N | Self-report Measure(s) | Performance Measure(s) | Timepoint(s) | Correlation | ||
|---|---|---|---|---|---|---|---|---|
| Dayton, 2016e USA |
THAa due to OA | 23 | HOOSb Pain and ADL Subscales | TUG, SCTc, 6 MWd | 1mo preoperative & 1mo–6mo postoperative | HOOS Pain vs. TUG HOOS Pain vs. SCT HOOS Pain vs. 6 MW HOOS ADL vs. TUG HOOS ADL vs. SCT HOOS ADL vs. 6 MW |
Preop (0.04) (0.04) (0.49) (0.08) (0.08) (0.46) |
Postop (0.11) (0.01) (0.07) (0.32) (0.27) (0.34) |
| Stevens-Lapsley, 2011f USA |
Unilateral TKA due to OA | 39 | KOOS Pain and ADL Subscales | 6 MW | 6mo postoperative | KOOS Pain vs. 6 MW (−0.23) KOOS ADL vs. 6 MW (−0.18) |
||
| Graff, 20168 Australia |
Unilateral TKA | 24 | KOOS | TUG | 12–58mo postoperative | KOOS Pain vs. TUG (−0.68) KOOS ADL vs. TUG (−0.72) |
||
| Sivachidambaram, 20149 India |
Primary Knee OA | 251 | KOOS | 6 MW | Cross-sectional | KOOS Pain vs. 6 MW (0.63) KOOS ADL vs. 6 MW (0.46) |
||
Range of Motion, frontal (medio-lateral).
Total Hip Arthroplasty.
Hip Dysfunction and Osteoarthritis Outcome Score.
Stair Climbing Test.
6 Minute Walk Test.
Western Ontario and McMaster Universities Osteoarthritis Index.
Block Step-up.
The predictive validity of performance tests adds to their utility as baseline and outcome measures in clinical research. For example, the 30-s sit to stand test was useful in distinguishing older persons with and without sarcopenia in one study [32]. In a study of persons with lower extremity osteoarthritis, those with timed up and go > 13.5 s were twice as likely to report a fall in the prior year as those with timed up and go < 13.5 s (58% vs. 31%, p = 0.003) [5]. In a study of persons with hip OA, 44% of those with a TUG >14 s had a frequent near-falls, as compared with 15% of those with TUG <10 s [6]. Alenazi and colleagues found that lower gait speed was associated with incident diabetes mellitus in OAI participants [7]. Finally, Zeni and colleagues showed that persons with knee OA who had slower times on the TUG and a stair climbing test were more likely to undergo total knee replacement [8]. We note as well that walking speed may have a tangible influence on patient safety in circumstances such as crossing a street.
Associations between self-report and objective performance measures in persons with OA have been examined in several cohorts assessed just prior to or shortly following total joint replacement (TJR; Table 3) [[9], [10], [11], [12]]. These studies largely demonstrate weak to moderate correlations between self-reported function and objective performance tests. For example, one study that examined a total hip replacement (THR) cohort 1–6 months postoperatively reported weak correlations between the TUG and Hip Injury and Osteoarthritis Outcome Score (HOOS) Pain and ADL subscales (r = 0.11 and 0.32, respectively) [9]. In contrast, a study performed 12–58 months following total knee replacement reported stronger correlations between TUG performance and KOOS Pain and ADL scales (r = −0.68 and −0.72, respectively) [12]. These findings suggest that associations between self-report and objective performance measures may be stronger in persons with less pain, such as individuals fully recovered from joint replacement [33]. Our subjects had mean KOOS Pain score of 55.8, resembling scores observed prior to total knee replacement. Thus, our findings of weak associations between self-report function and observed performance align well with those of subjects assessed prior to total joint replacement (Table 3).
Adjustment for mental health, neuropathic pain, widespread pain, and pain catastrophizing had little effect on the correlations between self-report measures and each objective performance measure (Table 2). This finding suggests that these pain-related variables have little influence on the association of self-report function and observed performance.
Our study was conducted in a single center on subjects who were generally white and well educated. It would be useful to confirm these findings in less homogeneous samples.
These findings have implications for design of studies of persons with knee OA. The objective performance measures we employed require little time and equipment. For example, the TUG requires only a chair, 3 m of space, and typically less than 30 s to perform. While objective performance measures typically are administered in face-to-face visits, some measures like the TUG could potentially be conducted virtually. One study reported clinically acceptable test-retest reliability (ICC = 0.94) and excellent concurrent validity (ICC = 0.88) for a virtually-proctored TUG among healthy community-dwelling elders [34]. Further validation of virtually administered objective performance measures is an important research goal. Additional studies such as ours would permit a mapping of subjective and objective measures of physical functional status, which would be useful for interpreting studies based solely on subjective measures.
Performance tests may be especially useful as intermediary outcomes of studies that involve interventions to improve strength, balance, or neuromuscular function and studies that examine outcomes known to be associated with performance test findings such as falls and total knee replacement. Self-report measures have gaps that are filled by objective measures and vice versa. For example, the KOOS does not have an item that captures balance as explicitly as the single leg balance test and, conversely, the performance measures do not capture complex integrated activities such as difficultly with ‘heavy domestic duties (such as moving heavy boxes, scrubbing floors, etc) [17]. Even when domains are similar (e.g. the self-report KOOS ADL Scale of the KOOS includes getting on and off the toilet and rising from sitting, which involve of some the same muscle groups as the timed up and go and the 30 s sit to stand), the KOOS items ask about difficulty and do not assess speed of performing these activities.
Understanding both a patient's perception of their physical limitation and objective knee performance may be useful for clinical decision making. Treating a patient based solely on self-report functional status may miss deficits that are not appreciated from responses to questionnaires [33]. Other authors have suggested that comprehensive assessment of joint OA is best achieved by a combination of subjective and objective assessments [[9], [10], [11], [12]]. The current study offers further support for inclusion of both subjective and objective measures in assessing functional status in subjects with knee OA.
The authors appreciate the editorial assistance of Maame Opare-Addo and Lily Waddell.
Declaration of competing interest
The authors declared no conflicts of interest.
Acknowledgemnent
This research was funded by Biosplice
References
- 1.Felson D.T., Lawrence R.C., Dieppe P.A., Hirsch R., Helmick C.G., Jordan J.M., et al. Osteoarthritis: new insights. Part 1: the disease and its risk factors. Ann. Intern. Med. 2000;133:635–646. doi: 10.7326/0003-4819-133-8-200010170-00016. [DOI] [PubMed] [Google Scholar]
- 2.Prevention CfDCa . 2020. Osteoarthritis (OA)https://www.cdc.gov/arthritis/basics/osteoarthritis.htm2020 [Google Scholar]
- 3.Hochberg M, Cisternas M, Watkins-Castillo S, Osteoarthritis. United States Bone and Joint Initiative: the Burden of Musculoskeletal Diseases in the United States (BMUS), vol. fourth ed.. (Rosemont, IL.forthcoming).
- 4.Wallis J.A., Taylor N.F., Bunzli S., Shields N. Experience of living with knee osteoarthritis: a systematic review of qualitative studies. BMJ Open. 2019;9 doi: 10.1136/bmjopen-2019-030060. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Zasadzka E., Borowicz A.M., Roszak M., Pawlaczyk M. Assessment of the risk of falling with the use of timed up and go test in the elderly with lower extremity osteoarthritis. Clin. Interv. Aging. 2015;10:1289–1298. doi: 10.2147/CIA.S86001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Arnold C.M., Faulkner R.A. The history of falls and the association of the timed up and go test to falls and near-falls in older adults with hip osteoarthritis. BMC Geriatr. 2007;7:17. doi: 10.1186/1471-2318-7-17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Alenazi A.M., Alqahtani B.A., Vennu V., Alshehri M.M., Alanazi A.D., Alrawaili S.M., et al. Gait speed as a predictor for diabetes incidence in people with or at risk of knee osteoarthritis: a longitudinal analysis from the osteoarthritis initiative. Int. J. Environ. Res. Publ. Health. 2021;18 doi: 10.3390/ijerph18094414. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Zeni J.A., Jr., Axe M.J., Snyder-Mackler L. Clinical predictors of elective total joint replacement in persons with end-stage knee osteoarthritis. BMC Muscoskel. Disord. 2010;11:86. doi: 10.1186/1471-2474-11-86. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Dayton M.R., Judd D.L., Hogan C.A., Stevens-Lapsley J.E. Performance-based versus self-reported outcomes using the hip disability and osteoarthritis outcome score after total hip arthroplasty. Am. J. Phys. Med. Rehabil. 2016;95:132–138. doi: 10.1097/PHM.0000000000000357. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Stevens-Lapsley J.E., Schenkman M.L., Dayton M.R. Comparison of self-reported knee injury and osteoarthritis outcome score to performance measures in patients after total knee arthroplasty. PMR. 2011;3:541–549. doi: 10.1016/j.pmrj.2011.03.002. [DOI] [PubMed] [Google Scholar]
- 11.Bolink S.A., Grimm B., Heyligers I.C. Patient-reported outcome measures versus inertial performance-based outcome measures: a prospective study in patients undergoing primary total knee arthroplasty. Knee. 2015;22:618–623. doi: 10.1016/j.knee.2015.04.002. [DOI] [PubMed] [Google Scholar]
- 12.Graff C., Hohmann E., Bryant A.L., Tetsworth K. Subjective and objective outcome measures after total knee replacement: is there a correlation? ANZ J. Surg. 2016;86:921–925. doi: 10.1111/ans.13708. [DOI] [PubMed] [Google Scholar]
- 13.Sivachidambaram K., Ateef M., Tahseen S. Correlation of self-reported questionnaire (KOOS) with some objective measures in primary OA knee patients. ISRN Rheumatol. 2014;2014:5. doi: 10.1155/2014/301485. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Kellgren J.H., Lawrence J.S. Radiological assessment of osteo-arthrosis. Ann. Rheum. Dis. 1957;16:494–502. doi: 10.1136/ard.16.4.494. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Roos E.M., Roos H.P., Lohmander L.S., Ekdahl C., Beynnon B.D. Knee injury and osteoarthritis outcome score (KOOS)--development of a self-administered outcome measure. J. Orthop. Sports Phys. Ther. 1998;28:88–96. doi: 10.2519/jospt.1998.28.2.88. [DOI] [PubMed] [Google Scholar]
- 16.Roos E.M., Lohmander L.S. The Knee injury and Osteoarthritis Outcome Score (KOOS): from joint injury to osteoarthritis. Health Qual. Life Outcome. 2003;1:64. doi: 10.1186/1477-7525-1-64. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Knee Injury and Osteoarthritis Outcome Score. 2012. http://www.koos.nu/index.html [Google Scholar]
- 18.Berwick D.M., Murphy J.M., Goldman P.A., Ware J.E., Jr., Barsky A.J., Weinstein M.C. Performance of a five-item mental health screening test. Med. Care. 1991;29:169–176. doi: 10.1097/00005650-199102000-00008. [DOI] [PubMed] [Google Scholar]
- 19.Galer B.S., Jensen M.P. Development and preliminary validation of a pain measure specific to neuropathic pain: the Neuropathic Pain Scale. Neurology. 1997;48:332–338. doi: 10.1212/wnl.48.2.332. [DOI] [PubMed] [Google Scholar]
- 20.Lape E.C., Selzer F., Davis A.M., Collins J.E., Losina E., Katz J.N. Psychometric properties of the Neuropathic Pain Scale (NPS) in a knee osteoarthritis population. Osteoarthritis Cartilage Open. 2020;2 doi: 10.1016/j.ocarto.2020.100027. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Wolfe F., Clauw D.J., Fitzcharles M.A., Goldenberg D.L., Häuser W., Katz R.S., et al. Fibromyalgia criteria and severity scales for clinical and epidemiological studies: a modification of the ACR Preliminary Diagnostic Criteria for Fibromyalgia. J. Rheumatol. 2011;38:1113–1122. doi: 10.3899/jrheum.100594. [DOI] [PubMed] [Google Scholar]
- 22.Wolfe F., Clauw D.J., Fitzcharles M.A., Goldenberg D.L., Katz R.S., Mease P., et al. The American College of Rheumatology preliminary diagnostic criteria for fibromyalgia and measurement of symptom severity. Arthritis Care Res. 2010;62:600–610. doi: 10.1002/acr.20140. [DOI] [PubMed] [Google Scholar]
- 23.Dave A.J., Selzer F., Losina E., Klara K.M., Collins J.E., Usiskin I., et al. Is there an association between whole-body pain with osteoarthritis-related knee pain, pain catastrophizing, and mental health? Clin. Orthop. Relat. Res. 2015;473:3894–3902. doi: 10.1007/s11999-015-4575-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Sullivan M.J.L., Bishop S.R., Pivik J. The pain catastrophizing scale: development and validation. Psychol. Assess. 1995;7:524–532. [Google Scholar]
- 25.Dobson F., Hinman R.S., Roos E.M., Abbott J.H., Stratford P., Davis A.M., et al. OARSI recommended performance-based tests to assess physical function in people diagnosed with hip or knee osteoarthritis. Osteoarthritis Cartilage. 2013;21:1042–1052. doi: 10.1016/j.joca.2013.05.002. [DOI] [PubMed] [Google Scholar]
- 26.Newcomer K.L., Krug H.E., Mahowald M.L. Validity and reliability of the timed-stands test for patients with rheumatoid arthritis and other chronic diseases. J. Rheumatol. 1993;20:21–27. [PubMed] [Google Scholar]
- 27.Jones C.J., Rikli R.E., Beam W.C. A 30-s chair-stand test as a measure of lower body strength in community-residing older adults. Res. Q. Exerc. Sport. 1999;70:113–119. doi: 10.1080/02701367.1999.10608028. [DOI] [PubMed] [Google Scholar]
- 28.Dunlop D.D., Semanik P., Song J., Sharma L., Nevitt M., Jackson R., et al. Moving to maintain function in knee osteoarthritis: evidence from the osteoarthritis initiative. Arch. Phys. Med. Rehabil. 2010;91:714–721. doi: 10.1016/j.apmr.2010.01.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Podsiadlo D., Richardson S. The timed "Up & Go": a test of basic functional mobility for frail elderly persons. J. Am. Geriatr. Soc. 1991;39:142–148. doi: 10.1111/j.1532-5415.1991.tb01616.x. [DOI] [PubMed] [Google Scholar]
- 30.Berger M.J., McKenzie C.A., Chess D.G., Goela A., Doherty T.J. Sex differences in quadriceps strength in OA. Int. J. Sports Med. 2012;33:926–933. doi: 10.1055/s-0032-1311587. [DOI] [PubMed] [Google Scholar]
- 31.Sialino L.D., Schaap L.A., van Oostrom S.H., Nooyens A.C.J., Picavet H.S.J., Twisk J.W.R., et al. Sex differences in physical performance by age, educational level, ethnic groups and birth cohort: the Longitudinal Aging Study Amsterdam. PLoS One. 2019;14 doi: 10.1371/journal.pone.0226342. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Sawada S., Ozaki H., Natsume T., Deng P., Yoshihara T., Nakagata T., et al. The 30-s chair stand test can be a useful tool for screening sarcopenia in elderly Japanese participants. BMC Muscoskel. Disord. 2021;22:639. doi: 10.1186/s12891-021-04524-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Mizner R.L., Petterson S.C., Clements K.E., Zeni J.A., Jr., Irrgang J.J., Snyder-Mackler L. Measuring functional improvement after total knee arthroplasty requires both performance-based and patient-report assessments: a longitudinal analysis of outcomes. J. Arthroplasty. 2010;26:728–737. doi: 10.1016/j.arth.2010.06.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.David Griswold K.R., Killa Carri, Maurer Michael, Landgraff Nancy, Learman Ken. Establishing the reliability and concurrent validity of physical performance tests using virtual reality equipment for community-dwelling healthy elders. Disabil. Rehabil. 2015;37:1097–1101. doi: 10.3109/09638288.2014.952451. [DOI] [PubMed] [Google Scholar]