Abstract
Introduction:
Current guidelines for the restoration of endodontically treated anterior teeth (ETT) are based on laboratory results and insufficient clinical findings. This retrospective cohort study aimed to compare the survival rates of ETT with unrestorable fracture restored with direct resin composite (DRC) or full coverage crown (FCC), and identify predisposing factors.
Methods and Materials:
Dental records and radiographs of ETT restored with DRC or FCC were collected from the dental charts of patients who received endodontic treatments and attended recall(s) from 2007 to 2019. Clinical/radiographic data and incidence of unrestorable fracture were recorded. Survival rates of ETT with unrestorable fracture treated with DRC and FCC were analyzed using Kaplan-Meier survival analysis and log-rank test, whereas predisposing factors were identified using Cox proportional-hazard model. Moreover, the survival rates of maxillary ETT with different sites of remaining cervical tooth structure were analyzed.
Results:
A total of 263 ETT with 157 DRC and 106 FCC were recruited. At an average recall period of 38 months, the survival rate of ETT restored with FCC was significantly higher (99.1%) than DRC (90.4%) (P<0.05). The predisposing factors of ETT with FCC were not identified; however, the identified predisposing factors of ETT with DRC were: (i) considered less than three walls of remaining cervical tooth structure, (ii) the ratio between root dentin thickness and root canal width at the cervical region was less than 1:1:1, (iii) loss of posterior-teeth support, and (iv) parafunctional habits. Maxillary ETT with complete or palatal structure had a significantly higher survival rate than those without the palatal structure (P<0.05).
Conclusion:
Based on the findings of the current cohort study, the survival rate of ETT with unrestorable fracture restored with FCC was significantly higher than DRC. However, ETT without predisposing factors were not susceptible to fracture and could be successfully restored with DRC.
Key Words: Composite Resins, Dental Crown, Endodontically Treated Teeth, Survival Rate, Tooth Fracture
Introduction
Unrestorable fracture is a common failure in endodontically treated teeth (ETT) [1]. ETT are susceptible to fracture due to extensive loss of tooth structure from dental caries, coronal fracture or pre-existing large restorations [2]. Direct resin composite (DRC) or full-coverage crown (FCC) is placed as a coronal restoration that reinforces ETT to withstand occlusal forces and protect from fracture [3, 4].
From a recent systematic review, anterior ETT with minimal to moderate loss of tooth structure could be conservatively restored with DRC to achieve an acceptable resistance to fracture; FCC would be required only if a significant loss of tooth structure is present [5]. The location of remaining cervical tooth structure is important for resistance to fracture [6]. For instance, the fracture strength of anterior ETT with partial loss of cervical structure and existing palatal wall is considered comparable with ETT having sound cervical structure [6].
Current clinical evidence about the effect of different coronal restorations on the survival from fracture of anterior ETT is scarce. From the recent clinical studies [7, 8], the benefit of FCC over DRC in prevention of tooth fracture is controversial. In addition, the reported clinical outcomes were combined from the data of anterior and posterior teeth. However, the risk of fracture in the anterior and posterior teeth are not the same and should be separately investigated. Only a retrospective study by Sorensen and Martinoff in 1984 [9] reported the separated data of anterior and posterior ETT. The survival rate from fracture of anterior ETT restored with DRC was higher than 90% and not significantly different from those restored with FCC.
Predisposing factors to unrestorable fracture have been reported in clinical studies of posterior ETT, i.e. remaining tooth structure, loss of adjacent tooth, or non-cuspal coverage restoration [10, 11]. From a clinical study in anterior ETT restored with glass-fiber posts and crowns [12], the survival rate of ETT with 3-4 remaining coronal walls tended to be higher, but was not significantly different from those with 1-2 remaining coronal walls. No other clinical study in anterior ETT has identified predisposing factors or directly compared between ETT with DRC and FCC restorations.
Current guidelines for restoration of anterior ETT are primarily based on laboratory results and insufficient clinical data. Therefore, this retrospective cohort study aimed to compare the survival rates from unrestorable fracture of anterior ETT restored with DRC and FCC. In addition, any predisposing factors to unrestorable fracture were identified.
Materials and Methods
The study protocol was approved by the institutional ethic committee (MU-DT/PY-IRB 2018/014.2302). Dental records and radiographs of anterior ETT were collected from dental charts of the patients who received endodontic treatments and attended recalls during the period of 2007–2019 at the Endodontic Postgraduate Clinic, Faculty of Dentistry, Mahidol University, Bangkok, Thailand.
Inclusion and exclusion criteria
Anterior ETT with DRC or FCC coronal restorations were included according to the inclusion and exclusion criteria. The inclusion criteria of ETT were (1) having mature root; (2) restored with single-unit coronal restorations, DRC or FCC; (3) having occluding pair; and (4) at least one-year recall period.
The exclusion criteria of ETT were (1) teeth with preoperative root resorption, crack, or fracture; (2) restored with direct or indirect veneers; (3) had supporting alveolar bone loss more than half of root length; (4) history of post removal before retreatment; (5) with procedural error(s) during endodontic and/or restorative treatment (such as root perforation); and (6) ongoing orthodontic treatment.
Endodontic and restorative procedures
Endodontic treatment was carried out under rubber dam isolation. Conservative access and working length determination were performed. Root canals were prepared using the crown-down technique using hand and/or rotary Ni-Ti files, and irrigated with 2.5% sodium hypochlorite and 17% EDTA. All root canals were medicated with calcium hydroxide paste for one to four weeks. The root canals were obturated with gutta-percha and root canal sealer [zinc oxide eugenol or epoxy resin sealer (AH-Plus, Dentsply-Maillefer, Tulsa, OK, USA)], using lateral or warm vertical compaction, up to 1-2 mm level below the cemento-enamel junction (CEJ). The teeth were planned for coronal restorations, DRC or FCC.
DRC restorations were placed as a permanent restoration, except in the cases that intermediate restorations were required prior to FCC. The access cavities were lined with non-eugenol, zinc-oxide based material (Caviton, GC corp., Tokyo, Japan) and/or GIC lining (Vitrebond, 3M ESPE, St. Paul, MN, USA; or Fuji VII, GC corp., Tokyo, Japan) at 1-2 mm thick. The cavities were bonded with a resin-based adhesive [etch and rinse adhesive, Adper Single Bond 2 (3M ESPE, St. Paul, USA); or self-etch adhesive, Clearfil SE Bond (Kuraray, Osaka, Japan)] according to the manufacturers’ instructions. Micro-hybrid or nano-hybrid resin composite [Z350 XT (3M ESPE, St Paul, USA), or Estelite Sigma (Tokuyama Dental Corp., Tokyo, Japan)] was filled into the cavities using the incremental technique in 2-mm thick and light cured for 20 sec in each layer.
FCC restorations with a placement of intra-radicular post was planned. Post spaces were prepared using electrical heat carriers (System B, SybronEndo, Orange, CA, USA) or Peeso-reamer drills (Dentsply, Maillefer, Tulsa, OK, USA). Cast metal posts or prefabricated fiber posts [D.T. Light-Post (BISCO Inc., Schaumburg, IL, USA)] were prepared and cemented into the canals with a resin-based material [Rely-X U200 (3M ESPE, USA) or MultiCore Flow (Ivoclar Vivadent AG, Amherst, NY, USA)]. All-ceramic crowns (Empress E. Max, Ivoclar Vivadent AG, Schaan, Liechtenstein) or porcelain-fused-to-metal crowns were fabricated and cemented on the prepared teeth.
Predisposing factors and incidence of fracture
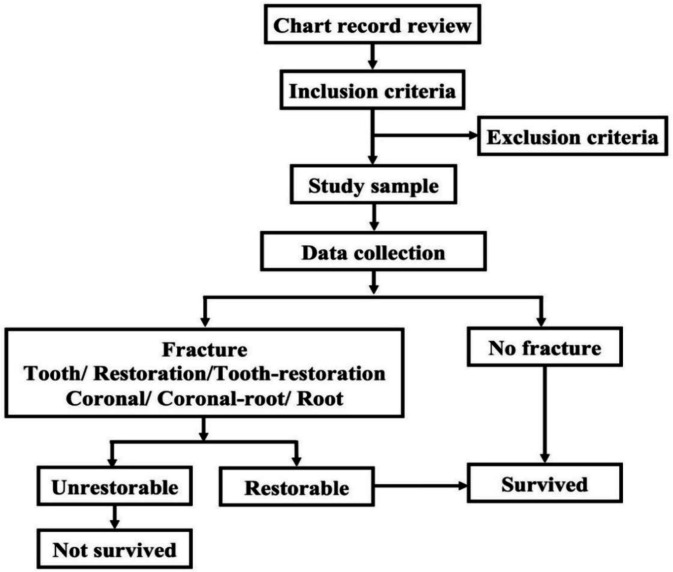
An overview of the methodology is present in Figure 1. The information were collected from dental records and radiographs. The age, gender, and recall periods were noted. The details of preoperative, intraoperative, and postoperative factors were identified as follows: (1) tooth type (incisor, canine) and location (maxillary, mandible); (2) type of coronal restorations (DRC, FCC); (3) surface(s) of restoration for DRC, or core build-up for FCC; (4) incidence of tooth/root fracture (yes, no); (5) fracture site (coronal, coronal-root, or root); (6) posterior support, with at least one pair of occluding teeth (none, 1, or 2); (7) adjacent teeth (none, 1, or 2); (8) type of post (none, cast metal, or prefabricated fiber post); (9) relationship between post length and alveolar bone level (below, above, or at the level); (10) wall(s) of remaining cervical tooth structure; (11) cervical root dentin thickness (mesial and distal sites) at 2 mm below the CEJ, calculated into a ratio to the root canal width (< 1:1:1 or ≥ 1:1:1); and (12) parafunctional habits, such as bruxism or clenching (yes, no).
Figure 1.
An overview of the methodology in this retrospective cohort study
Restorative surface(s) of resin composite or core build-up were noted in mesial (M), distal (D), palatal (Pa), labial (La), and incisal (I) sufaces, which were further categorized into two groups as 1-3 or 4-5 restorative surfaces.
Remaining cervical tooth structure was identified according to the residual walls at the cervical area in M, D, Pa, and La. The cervical tooth structures were further categorized into two groups: 0-2 and 3-4 walls. For the maxillary anterior ETT, the cervical tooth structures were subcategorized, according to the remaining wall of cervical tooth structure, into the four subgroups- (1) ‘complete’, all four walls existed; (2) ‘none’, all walls were absent; (3) ‘partial with Pa’, other wall(s) were missing but the palatal wall remained; and (4) ‘partial without Pa’, the palatal wall was missing but the other wall(s) remained.
A ratio of root dentin and root canal width at the cervical region (2 mm below the CEJ) was estimated. Root dentin thicknesses (M and D) and root canal width (C) were measured from the post-operative radiographs. M:C:D ratio was calculated and classified into two groups, < 1:1:1 and ≥ 1:1:1.
Incidence of fracture was noted into restorable and unrestorable. The definition of restorable fracture was the fracture that can be repaired or replaced with a new restoration. The definition of unrestorable fracture was the fracture with an extensive destruction of tooth structure leading to tooth extraction. The survival rate from unrestorable fracture was calculated into percentage.
Statistical analysis
Statistical analysis was performed using SPSS version 22 for MAC (SPSS Inc., Chicago, IL, USA) with a significant level set at P<0.05. Survival rates from unrestorable fracture of anterior ETT with DRC and FCC was analyzed using the Kaplan-Meier survival analysis and the log-rank test. Predisposing factors to unrestorable fracture with P≤0.25 were identified from the univariate analysis and further analyzed using the Cox proportional-hazard multivariate model.
In the subgroup analysis, the log-rank test was used to compare the survival rates between ETT with DRC and their significant risk factors, and ETT with FCC. In addition, the Cox proportional-hazard model was used to evaluate the effect of remaining wall of cervical tooth structure on the survival rates of maxillary anterior ETT.
Results
Overall, 263 anterior ETT in 155 females (58.9%) and 108 males (41.1%) between 11–79 (56±15.5) years old were included. Tooth locations were 204 maxillary teeth (77.6%), and 59 mandibular teeth (22.4%). Tooth types were 185 incisors (70.3%), and 78 canines (29.7%). Coronal restorations were 157 DRC (59.7%) and 106 FCC (40.3%). ETT with FCC were treated with cast metal posts (45 teeth), prefabricated fiber posts (58 teeth), or no post (3 teeth). All posts in ETT with FCC restorations were placed below the alveolar crestal bone level. No post was placed in ETT with DRC restorations.
Survival rates from unrestorable fracture
Recall periods ranged from 12 to 144 months, with a mean of 38±21.4 months. The overall survival rates of anterior ETT were 93.9%, which 16 cases (15 DRC and one FCC) were extracted because of unrestorable fracture. The survival rates of ETT with DRC and FCC were 90.4% and 99.1% respectively. The survival rates of anterior ETT were analyzed using the log-rank test (Table 1), and ETT with FCC showed the significantly higher survival rate than ETT with DRC (P<0.01).
Table 1.
Survival rates and statistical analysis of anterior ETT according to the variables (n=263)
| Factors | Number of teeth ( n ) | Survival (%) | Not survival (%) | P -value |
|---|---|---|---|---|
| Gender | ||||
| Female | 155 | 147 (94.8) | 8 (5.2) | 0.59 |
| Male | 108 | 100 (92.6) | 8 (7.4) | |
| Tooth type | ||||
| Incisor | 185 | 176 (95.1) | 9 (4.9) | 0.13 |
| Canine | 78 | 71 (91) | 7 (9) | |
| Location | ||||
| Maxillary | 204 | 191 (93.6) | 13 (6.4) | 0.45 |
| Mandible | 59 | 56 (94.9) | 3 (5.1) | |
| Restoration | ||||
| Composite | 157 | 142 (90.4) | 15 (9.6) | <0.01* |
| Crown | 106 | 105 (99.1) | 1 (0.9) | |
* A significant difference from the log-rank test (P<0.05)
Kaplan-Meier survival analysis and the cumulative survival rates (%) at the time intervals of anterior ETT with DRC and FCC are presented in Figure 2. The cumulative survival rates of ETT with DRC decreased from 98.7% at 12 months to 80.6 % at 72 months. Only one ETT with FCC had unrestorable fracture at 60 months. The cumulative survival rates of ETT with FCC at 12–48 months were 100% and then decreased to 93.33% at 60–72 months.
Figure 2.
Kaplan‐Meier survival analysis from unrestorable fracture of anterior ETT with resin composite and crown restorations, and the cumulative survival rates at the time intervals
Predisposing factors to unrestorable fracture
Only a single incident of unrestorable fracture in ETT with FCC made statistical analysis of any predisposing factors was not possible. In ETT with DRC, the predisposing factors were analyzed (Table 2); the significant factors in unrestorable fracture were identified as follows: (1) remaining less than three walls of cervical tooth structure; (2) the ratio between root dentin thickness and root canal width at the cervical region <1:1:1; (3) loss of posterior-teeth support; and (4) parafunctional habits (P<0.05).
Table 2.
Univariate and multivariate analysis of anterior ETT restored with resin composite (n=157)
| Factors | Teeth ( n ) | Survival (%) | Univariate Analysis | Multivariate analysis | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| HR (95% CI) | P -value | Adjusted HR (95%CI) | P -value | |||||||
| Gender | ||||||||||
| Female | 96 | 88 (91.7) | 1 | 0.44 | NA | NA | ||||
| Male | 61 | 54 (88.5) | 1.49 (0.54, 4.15) | |||||||
| Tooth type | ||||||||||
| Incisor | 109 | 101 (92.7) | 0.44 (0.16, 1.22) | 0.12* | 1.784 (0.273, 11.679) | 0.55 | ||||
| Canine | 48 | 41 (85.4) | 1 | 1 | ||||||
| Location | ||||||||||
| Maxillary | 126 | 113 (89.7) | 2.20 (0.49, 9.79) | 0.30 | NA | NA | ||||
| Mandible | 31 | 29 (93.5) | 1 | |||||||
| Restorative surfaces | ||||||||||
| 1–3 | 130 | 121 (93.1) | 1 | <0.01* | 1 | 0.44 | ||||
| 4–5 | 27 | 21 (77.8) | 4.76 (1.68,13.52) | 1.780 (0.407, 7.782) | ||||||
| Remaining cervical tooth structure (walls) | ||||||||||
| 0–2 | 61 | 50 (82) | 3.69 (1.18, 11.62) | 0.03* | 8.947 (1.429, 56.012) | 0.02* | ||||
| 3–4 | 96 | 92 (95.8) | 1 | 1 | ||||||
| Posterior teeth support (side) | ||||||||||
| None | 13 | 7 (53.8) | 20.43 (5.72, 72.92) | <0.01* | 9.053 (1.680, 48.772) | 0.02* | ||||
| 1 | 32 | 27 (84.4) | 4.08 (1.09, 15.23) | <0.01* | 0.609 (0.095, 3.921) | 0.61 | ||||
| 2 | 112 | 108 (96.4) | 1 | 1 | ||||||
| Adjacent teeth (n) | ||||||||||
| None and 1 | 34 | 27 (79.4) | 5.03 (1.81, 13.99) | <0.01* | 3.487 (0.671, 18.111) | 0.14 | ||||
| 2 | 123 | 115 (93.5) | 1 | 1 | ||||||
| Cervical root dentin thickness (ratio) | ||||||||||
| < 1:1:1 | 98 | 86 (87.8) | 2.87 (0.81, 10.21) | 0.10* | 12.979 (1.549, 108.734) | 0.02* | ||||
| ≥ 1:1:1 | 59 | 56 (94.9) | 1 | 1 | ||||||
| Parafunctional habit | ||||||||||
| Yes | 25 | 20 (80) | 2.76 (0.83, 9.19) | 0.10* | 19.366 (2.250, 166.708) | <0.01* | ||||
| No | 105 | 99 (94.3) | 1 | 1 | ||||||
* A significant difference was indicated by the log-rank test (P<0.05) in the comparison of survival rates among the potential risk factors.
The factors with P value≤0.25 were further analyzed using the multivariate model. HR, hazard ratio
Hazard ratios (HR) of the significant factors in anterior ETT with DRC were described. Firstly, ETT with 0-2 walls of cervical tooth structure were 8.95 times more likely to unrestorable fracture than those with 3-4 walls (HR: 8.95; 95%; confidence interval (CI): 1.43, 56.01; P=0.02). Secondly, ETT with no posterior-teeth support were lost at 9.05 times (HR: 9.05; 95%; CI: 1.68, 48.77; P=0.02), higher than those with the two-sided posterior-teeth support. Thirdly, ETT with the cervical root dentin thickness in the ratio <1:1:1 were lost at 12.98 times (HR: 12.98; 95%; CI: 1.55, 108.73; P=0.02), higher than those with the thickness in the ratio ≥1:1:1. Lastly, loss of anterior ETT in the patients who had a parafunctional habit were 19.37 times higher than those without the habit (HR: 19.37; 95%; CI: 2.25, 166.71; P<0.01).
ETT with DRC and significant predisposing factors
ETT with DRC and the significant predisposing factors were analyzed and compared with ETT with FCC. The comparative survival analysis are presented in Table 3. The survival rates of ETT with DRC and the significant predisposing factors were significantly lower than ETT with FCC (P<0.05). On the contrary, the survival rates of ETT with 3–4 walls of cervical tooth structure, two-sided posterior support, the ratio of root dentin thickness ≥1:1:1, and without parafunctional habits were not significantly different from ETT with FCC.
Table 3.
Survival analysis in anterior ETT with resin composite analyzed with the significant risk factors compared to ETT with crown restorations
| Restorations and risk factors | Not survival /Total (teeth) | Survival rate (%) | P -value |
|---|---|---|---|
| ETT with crown | 1/106 | 99.1 | |
| ETT with resin composite | |||
| Remaining cervical tooth structure (walls) | |||
| 0-2 vs crown | 11/61 | 82.0 | <0.01* |
| 3-4 vs crown | 4/96 | 95.8 | 0.15 |
| Posterior teeth support (side) | |||
| None vs crown | 6/13 | 53.8 | <0.01* |
| 1 vs crown | 5/32 | 84.4 | <0.01* |
| 2 vs crown | 4/112 | 96.4 | 0.20 |
| Cervi cal root dentin thickness (ratio) | |||
| <1:1:1 vs crown | 12/98 | 87.8 | <0.01* |
| ≥1:1:1 vs crown | 3/59 | 94.8 | 0.22 |
| Parafunctional habit | |||
| Yes vs crown | 5/25 | 80.0 | <0.01* |
| No vs crown | 6/105 | 94.3 | 0.05 |
* A significant difference from the log-rank test (P<0.05)
Effect of cervical tooth structure on survival rate of maxillary anterior ETT with DRC
From a total of 126 maxillary anterior ETT, 13 teeth (10.3%) were extracted from unrestorable fractures with an overall survival rate of 89.7%. ETT with the ‘complete’, ‘partial with Pa’, ‘partial without Pa’ and ‘no’ cervical tooth structure had the survival rates of 94.5%, 95.8%, 78.6%, and 44.4% respectively (Table 4).
Table 4.
Survival rates from unrestorable fracture of maxillary anterior ETT with the different sites of remaining cervical tooth structure
| Cervical tooth structure | Number of teeth | Survival [n (%)] | Hazard ratio (95%CI) | P -value | |
| Complete | 55 | 52 (94.5) | 1 | Reference | |
| Partial with Pa | 48 | 46 (95.8) | 0.69 (0.12, 4.17) | 0.69 | |
| Partial without Pa | 14 | 11 (78.6) | 6.21 (1.23, 31.48) | 0.03* | |
| None | 9 | 4 (44.4) | 16.78 (3.74, 75.21) | <0.01* | |
* A significant difference from Cox-regression analysis (P<0.05)
The survival rates between the ‘complete’ and ‘partial with Pa’ groups were not significantly different (P>0.05). In contrast, the survival rate of the ‘complete’ group was significantly higher than the ‘no’ and ‘partial without Pa’ groups (P<0.05). ETT with ‘no’ and ‘partial without Pa’ cervical tooth structures were 16.78 times (HR: 16.78; 95%; CI: 3.74, 75.21; P<0.01) and 6.21 times (HR: 6.21; 95%; CI: 1.23, 31.48; P=0.03) more likely to unrestorable fracture than those with the ‘complete’ cervical tooth structure, respectively.
Discussion
The survival rates from unrestorable fracture of anterior ETT with FCC were significantly higher (99.1%) than those with DRC (90.4%). Other recent clinical studies combining data from the anterior and posterior teeth [7, 8] reported the similar survival rates, and ETT with FCC had the significantly higher survival rate than ETT with DRC. However, the prefabricated glass-fiber posts were placed in all ETT restored with DRC in the study by Skupien et al. [7]. In contrast, no post was inserted in the ETT with DRC in our study. The benefit of fiber-post placement on the survival of ETT has been controversial.
Sorensen and Martinoff in 1984 [9] reported the effect of coronal restorations on the survival rates of anterior and posterior ETT, separately. The survival rates of maxillary and mandibular anterior ETT with the full-coverage restorations were 87.5% and 97.5%, while for those with the direct restorations, the survival rates were 85.4% and 94.4%. Nevertheless, a statistically significant difference in the survival rates between ETT with FCC and DRC was not found in their study [9]. In contrast, our results showed the significant difference between ETT with the two types of coronal restorations. This might be explained by the marginal difference in the survival rates reported in the two studies.
Analysis of predisposing factors in ETT with FCC was not possible due to a single incident of unrestorable fracture. The analysis in ETT with DRC identified the four predisposing factors affecting the survival rate. The survival rate from unrestorable fracture of the ETT without these identified risk factors was much improved and comparable to the ETT with FCC.
The remaining cervical tooth structure less than three walls increased the risk of unrestorable fracture in ETT restored with DRC. The cervical tooth structure basically acts as a ‘ferrule’ to withstand occlusal force and reduce the chances of unrestorable fracture [13]. The survival rate of anterior ETT tends to be higher when the more cervical tooth structure remains.
Partial or complete loss of cervical tooth structure in ETT is frequently observed [6]. The sites of remaining cervical tooth structure directly affect the fracture resistance of ETT [6]. In our study, the effect of the remaining site was only analyzed in the maxillary anterior ETT. Unrestorable fractures in the mandibular anterior ETT were observed only in the two cases and insufficient for statistical analysis. The survival rate of maxillary ETT with the palatal cervical structure was comparable to those with the complete cervical structure. These results are in agreement with the results of fracture resistance from the in vitro studies [6, 14, 15]. In the maxillary anterior teeth, the cervical tooth structure at the palatal site protects the teeth against functional force and fatigue fracture by tension stress [16].
Loss of posterior-teeth support resulted in a significant decrease in the survival rate of anterior ETT. The patients with the loss of posterior teeth tended to increase function on the anterior teeth where the masticatory force is predominantly loaded and might be responsible for the higher incidence of fracture. From our results, the survival rate significantly improved in ETT with the two-sided posterior support that improves the distribution of masticatory force and decreases the stress on anterior teeth.
The survival rate of anterior ETT with cervical root dentin thickness in the ratio <1:1:1 was significantly lower than those with the ratio ≥1:1:1. Fracture resistance of ETT in vitro was significantly lower when the thickness ratio was lower than 1:1:1 [17]. When the lateral force is loaded on the anterior teeth, high stress is induced at the coronal one-third of root [18]. Anterior ETT with the reduced thickness of cervical root dentin are more susceptible to fracture [19]. Cervical root dentin must be preserved in the root canal and/or restorative treatment to resist functional forces and decrease chances of fracture [20].
Parafunctional habits, such as clenching, bruxism, and habitual eating, were detected as a significant risk factor in our study. Incidence of unrestorable fracture of anterior ETT in the patients with the parafunctional habit was higher than in those without the parafunction. Normal masticatory force in the anterior region was in a range between 71–142 N, while the force in the patients with bruxism highly increased to 569 N [21]. In addition, the clenching force is approximately 10 times greater than the maximum normal biting force [22]. Therefore, these parafunctional habits must be taken into a consideration when a coronal restoration for ETT is planned. Occlusal interference, in either centric or eccentric relation, should be carefully checked since it is a risk factor of teeth predisposed to crack or fracture [23].
Reattachment of tooth fragment is another option for restoration of anterior teeth fractured from traumatic injury [24]. This method shows a promising result with a low incidence of re-fracture and should be also considered when restoring anterior ETT.
For clinical recommendation, our results suggested that DRC could be successfully used as a permanent restoration in anterior ETT with the following conditions: 1) remained 3–4 walls of cervical tooth structure; 2) two-sided posterior support; 3) the ratio of cervical root dentin thickness ≥1:1:1; and 4) not having parafunctional habits. However, the long-term degradation of adhesion between resin composite and dentin might decrease the reinforcement effect [25] and increase the marginal leakage [26]. Therefore, the long-term stability of ETT restored with resin composite restoration should be further investigated. Furthermore, a randomized controlled trial should be conducted to confirm the results of this retrospective study.
Conclusion
Based on this retrospective cohort study, with average recall period of 38 months, anterior ETT restored with FCC showed higher survival rate from unrestorable fracture happening than ETT with DRC. However, the cumulative survival rate of the ETT with DRC at 5 years was still higher than 80%. The significant predisposing factors in unrestorable fracture of ETT with DRC were 1) remaining less than three walls of cervical tooth structure, 2) the ratio of cervical root dentin thickness <1:1:1, 3) loss of posterior-teeth support, and 4) parafunctional habits. For maxillary anterior ETT with DRC, the presence of the palatal cervical tooth structure increased the survival rate.
Acknowledgment
This research is supported by a research grant from Faculty of Dentistry, Mahidol University, Thailand. The authors would like to thank Assist. Prof. Dr. Chulaluk Komoltri and Dr. Sittichoke Osiri for their assistances in statistical analysis.
Conflict of Interest:
‘None declared’.
References
- 1.Landys Boren D, Jonasson P, Kvist T. Long-term survival of endodontically treated teeth at a public dental specialist clinic. J Endod. 2015;41(2):176–81. doi: 10.1016/j.joen.2014.10.002. [DOI] [PubMed] [Google Scholar]
- 2.Dietschi D, Duc O, Krejci I, Sadan A. Biomechanical considerations for the restoration of endodontically treated teeth: a systematic review of the literature--Part 1 Composition and micro- and macrostructure alterations. Quintessence Int. 2007;38(9):733–43. [PubMed] [Google Scholar]
- 3.Aquilino SA, Caplan DJ. Relationship between crown placement and the survival of endodontically treated teeth. J Prosthet Dent. 2002;87(3):256–63. doi: 10.1067/mpr.2002.122014. [DOI] [PubMed] [Google Scholar]
- 4.Suksaphar W, Banomyong D, Jirathanyanatt T, Ngoenwiwatkul Y. Survival rates against fracture of endodontically treated posterior teeth restored with full-coverage crowns or resin composite restorations: a systematic review. Restor Dent Endod. 2017;42(3):157–67. doi: 10.5395/rde.2017.42.3.157. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Dietschi D, Duc O, Krejci I, Sadan A. Biomechanical considerations for the restoration of endodontically treated teeth: a systematic review of the literature, Part II (Evaluation of fatigue behavior, interfaces, and in vivo studies) Quintessence Int. 2008;39(2):117–29. [PubMed] [Google Scholar]
- 6.Ng CC, Dumbrigue HB, Al-Bayat MI, Griggs JA, Wakefield CW. Influence of remaining coronal tooth structure location on the fracture resistance of restored endodontically treated anterior teeth. J Prosthet Dent. 2006;95(4):290–6. doi: 10.1016/j.prosdent.2006.02.026. [DOI] [PubMed] [Google Scholar]
- 7.Skupien JA, Cenci MS, Opdam NJ, Kreulen CM, Huysmans MC, Pereira-Cenci T. Crown vs composite for post-retained restorations: A randomized clinical trial. J Dent. 2016;48:34–9. doi: 10.1016/j.jdent.2016.03.007. [DOI] [PubMed] [Google Scholar]
- 8.Fransson H, Dawson VS, Frisk F, Bjorndal L, Kvist T. Survival of Root-filled Teeth in the Swedish Adult Population. J Endod. 2016;42(2):216–20. doi: 10.1016/j.joen.2015.11.008. [DOI] [PubMed] [Google Scholar]
- 9.Sorensen JA, Martinoff JT. Intracoronal reinforcement and coronal coverage: a study of endodontically treated teeth. J Prosthet Dent. 1984;51(6):780–4. doi: 10.1016/0022-3913(84)90376-7. [DOI] [PubMed] [Google Scholar]
- 10.Jirathanyanatt T, Suksaphar W, Banomyong D, Ngoenwiwatkul Y. Endodontically treated posterior teeth restored with or without crown restorations: A 5-year retrospective study of survival rates from fracture. J Investig Clin Dent. 2019:e12426. doi: 10.1111/jicd.12426. [DOI] [PubMed] [Google Scholar]
- 11.Suksaphar W, Banomyong D, Jirathanyanatt T, Ngoenwiwatkul Y. Survival Rates from Fracture of Endodontically Treated Premolars Restored with Full-coverage Crowns or Direct Resin Composite Restorations: A Retrospective Study. J Endod. 2018;44(2):233–8. doi: 10.1016/j.joen.2017.09.013. [DOI] [PubMed] [Google Scholar]
- 12.Signore A, Benedicenti S, Kaitsas V, Barone M, Angiero F, Ravera G. Long-term survival of endodontically treated, maxillary anterior teeth restored with either tapered or parallel-sided glass-fiber posts and full-ceramic crown coverage. J Dent. 2009;37(2):115–21. doi: 10.1016/j.jdent.2008.10.007. [DOI] [PubMed] [Google Scholar]
- 13.Juloski J, Radovic I, Goracci C, Vulicevic ZR, Ferrari M. Ferrule effect: a literature review. J Endod. 2012;38(1):11–9. doi: 10.1016/j.joen.2011.09.024. [DOI] [PubMed] [Google Scholar]
- 14.Dikbas I, Tanalp J, Ozel E, Koksal T, Ersoy M. Evaluation of the effect of different ferrule designs on the fracture resistance of endodontically treated maxillary central incisors incorporating fiber posts, composite cores and crown restorations. J Contemp Dent Pract. 2007;8(7):62–9. [PubMed] [Google Scholar]
- 15.Muangamphan P, Sattapan B, Kukiattrakoon B, Thammasitboon K. The effect of incomplete crown ferrules on fracture resistance and failure modes of endodontically treated maxillary incisors restored with quartz fiber post, composite core, and crowns. J Conserv Dent. 2015;18(3):187–91. doi: 10.4103/0972-0707.157239. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Torbjorner A, Fransson B. Biomechanical aspects of prosthetic treatment of structurally compromised teeth. Int J Prosthodont. 2004;17(2):135–41. [PubMed] [Google Scholar]
- 17.Wilcox LR, Roskelley C, Sutton T. The relationship of root canal enlargement to finger-spreader induced vertical root fracture. J Endod. 1997;23(8):533–4. doi: 10.1016/S0099-2399(97)80316-0. [DOI] [PubMed] [Google Scholar]
- 18.Assif D, Oren E, Marshak BL, Aviv I. Photoelastic analysis of stress transfer by endodontically treated teeth to the supporting structure using different restorative techniques. J Prosthet Dent. 1989;61(5):535–43. doi: 10.1016/0022-3913(89)90272-2. [DOI] [PubMed] [Google Scholar]
- 19.Sathorn C, Palamara JE, Palamara D, Messer HH. Effect of root canal size and external root surface morphology on fracture susceptibility and pattern: a finite element analysis. J Endod. 2005;31(4):288–92. doi: 10.1097/01.don.0000140579.17573.f7. [DOI] [PubMed] [Google Scholar]
- 20.Assif D, Gorfil C. Biomechanical considerations in restoring endodontically treated teeth. J Prosthet Dent. 1994;71(6):565–7. doi: 10.1016/0022-3913(94)90438-3. [DOI] [PubMed] [Google Scholar]
- 21.Anderson DJ. Measurement of stress in mastication I. J Dent Res. 1956;35(5):664–70. doi: 10.1177/00220345560350050201. [DOI] [PubMed] [Google Scholar]
- 22.Larson TD. Part one: The restoration of non-vital teeth: structural, biological, and micromechanical issues in maintaining tooth longevity. Northwest Dent. 2006;85(5):29–31. [PubMed] [Google Scholar]
- 23.de Toubes KMS, Maia LM, Goulart LC, Teixeira TF, Alves NRF, Seraidarian PI, Silveira FF. Optimization of Results for Cracked Teeth Using CAD-CAM System: A Case Series. Iran Endod J. 2020;15(1):57–63. doi: 10.22037/iej.v15i1.26731. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Mat Zainal MK, Abdullah D. Re-attachment of a Fractured Maxillary Central Incisor: A Case with Two Years Follow-up. Iran Endod J. 2021;16(2):131–6. doi: 10.22037/iej.v16i2.25939. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Hashimoto M, Ohno H, Kaga M, Endo K, Sano H, Oguchi H. In vivo degradation of resin-dentin bonds in humans over 1 to 3 years. J Dent Res. 2000;79(6):1385–91. doi: 10.1177/00220345000790060601. [DOI] [PubMed] [Google Scholar]
- 26.Banomyong D, Palamara JE, Messer HH, Burrow MF. Sealing ability of occlusal resin composite restoration using four restorative procedures. Eur J Oral Sci. 2008;116(6):571–8. doi: 10.1111/j.1600-0722.2008.00570.x. [DOI] [PubMed] [Google Scholar]