Abstract
Purpose
To characterize nail and enthesis abnormalities using high frequency ultrasound (HFUS) in patients with psoriasis (PSO), psoriatic arthritis (PSA) with PSO, and PSA sine PSO.
Material and Methods
Patients with PSO, PSA with PSO, and PSA sine PSO were evaluated and compared in a cross-sectional single centre study. Nail and enthesis abnormalities were evaluated by HFUS using high frequency probes (27 MHz). After a descriptive assessment, Brown University Nail Enthesis Scale (BUNES) and Madrid Sonography Enthesitis Index (MASEI) were used to assess nail and enthesis, respectively.
Results
Fifty-nine patients were enrolled (19 PSO, 22 PSA with PSO, 18 PSA sine PSO). In patients with PSO and in those with PSA and PSO, HFUS evaluation identified the following nail alterations characterised by thickened matrix, inhomogeneous echogenicity of the nail bed, and increased blood flow by power Doppler. In 38.9% patients with PSA sine PSO, a subclinical nail involvement was described. No difference was observed comparing BUNES values in three groups. In PSA patients with PSO and in those with PSA sine PSO, HFUS assessment of entheses mainly showed a hypoechoic aspect and thickness of the tendon, focal cortical erosion, and ossification. A subclinical enthesis involvement in 47.4% patients with PSO was observed. No difference was reported comparing MASEI values in three groups.
Conclusion
Qualitative and quantitative abnormalities of nail and enthesis were demonstrated by HFUS in patients with PSO, PSA with PSO, and PSA sine PSO, suggesting a practical additional tool to be used in clinical settings. Furthermore, HFUS highlighted a subclinical nail involvement in patients with PSA sine PSO and enthesis subclinical alterations in patients with PSO.
Keywords: Psoriasis, Psoriatic arthritis, Musculoskeletal ultrasonography, High frequency ultrasound
Introduction
In last years, the concept of psoriatic disease has been developed thanks to a better understanding of molecular pathogenetic mechanisms leading to psoriasis (PSO) and associated musculoskeletal manifestations [1]. PSO is a common chronic skin inflammatory condition associated with quality-of-life impairment and disability [2, 3]. The disease presents cutaneous manifestation as erythematous and scaling plaques with prototypical distribution in plaque-type PSO, but also rarer and severe variants, such as pustular and erythrodermic PSO and special localization such as nails, genitals, skin folds, and palmo-plantar areas [4, 5]. Independently from the cutaneous phenotypical variability, a percentage of patients with PSO may develop psoriatic arthritis (PSA), variously characterized by the involvement of peripheral joints, entheses, synovial sheaths of tendons, and axial skeleton [6]. PSA may also be observed in patients without PSO but with a family history positive for PSO in first or second-degree relatives, defined as PSA sine PSO [6]. In this context, the involvement of nails is one of the hallmarks and diagnostic clues of PSO, esteemed to be present in up to 70% of patients affected by PSO [7]. It may involve all the nail components and may predict the evolution from cutaneous to musculoskeletal involvement [8]. Furthermore, the involvement of synovio-entheseal complex and the enthesis-related inflammation may be considered as an early event in PSA and its diagnostic usefulness has been pointed out [9]. Thus, as described in other rheumatic diseases [10–12], the role of imaging features is increasingly suggested in identifying those clinically silent abnormalities which may predict the development of PSA in PSO patients and may help to early diagnosis of the disease for a timely treatment [13–15]. On these bases, musculoskeletal ultrasonography with the use of high frequency probes (HFUS) and power Doppler (PD) may be suggested in determining subclinical inflammation of the area under ultrasound examination [16–18].
In this study, we aimed at performing a qualitative and quantitative characterization of nail and enthesis abnormalities using HFUS in patients with PSO, PSA with PSO, and PSA sine PSO.
Patients and methods
Clinical features
In this cross-sectional single centre study, patients were selected among those consecutively admitted to the Dermatologic and/or Rheumatologic Clinics of University of L’Aquila at San Salvatore Hospital, L’Aquila, Italy, from June to December 2021. All patients were assessed if fulfilled widely available criteria for PSO or PSA classification criteria [19, 20].
Three groups of patients were assessed: (i) patients affected by PSO but without any musculoskeletal involvement (PSO group); (ii) patients affected by PSA and evident skin involvement by PSO (PSA with PSO group); (iii) patients affected by PSA but without any skin involvement by PSO (PSA sine PSO group). Voluntary adult patients (> 18 years) with a minimum disease duration of 12 months were considered in this study. Patients were excluded if treated with ongoing systemic immunomodulating therapies for PSO and/or PSA, insufficient wash-out period from previous systemic immunomodulating therapies, and/or other medical conditions potentially influencing nail and enthesis conditions. An adequate wash-out period from systemic immunomodulating therapies was codified as the discontinuation for a time of at least 3 half-lives of the administered drug.
Experienced dermatologists and rheumatologists performed the clinical evaluation. The Psoriasis Area and Severity Index (PASI) [21] was used to measure severity and extension of PSO and the specific Nail Area and Severity Index (NAPSI) for nail involvement [22]. Tender and swollen joint counts, and Leed Enthesitis Index (LEI) were used to evaluate the features of PSA [23].
Ethical approval was obtained from the Internal Review Board of the University of L’Aquila (protocol number Internal Review Board University of L’Aquila 01/2022). Moreover, patients signed an informed consent allowing the use of clinical records for scientific purposes.
HFUS features
HFUS was carried out at the Radiology Department of the University of L’Aquila using high frequency probes (27 MHz), available on US machines (Esaote my Lab X8), having available a software implementation improving the quality of ultrasound imaging with Color Doppler. The imaging parameters for Doppler ultrasound examinations were set to increase the detection of low-velocity, low-volume flows within the inside of the nail bed and tendon enthesis. The PD specifications have been standardized through a frequency ranging from 10.0 to 12.5 MHz and pulse repetition frequencies ranging from 0.9 to 1.0 kHz; color gain was set avoiding excessive color noise (color vs. echo priority ranging from 40 to 60% and color persistence adjusted to high values).
Ultrasound assessment of nail abnormalities was performed evaluating hands in all subgroups of patients. All ten nails of the hands were imaged. Longitudinal scan identified nail plate, composed by two hyperechoic lines representing the dorsal and ventral areas with a virtual anechoic space between them; nail bed a hypoechoic band between the superior hyperechoic nail plate and the inferior hyperechoic distal phalanx; nail matrix visualized as an isoechoic region under the proximal nailfold at the proximal portion of the nail bed. Brown University Nail Enthesis Scale (BUNES) was used to evaluate different nail structures and PD activity [24]. Morphologic normal findings were indicated with a score of 0 for each area scanned (nail plate, matrix, and bed). Nail plate changes (focal hyperechoic areas of the ventral plate/irregular border of ventral and dorsal plate), abnormal or thickened nail beds (2.0–3.0 mm) and/or matrix were scored as 1. Nail bed and matrix PD findings were assessed by 0 = no signal, 1 = confluent signal in < 25% of the area, 2 = confluent signal in > 25% and < 50%, 3 = confluent signal > 50%. A mean score of BUNES morphometry of 1.5 and a mean score of BUNES PD of 3 were used as threshold to identify a pathologic nail involvement. In addition, an ultrasound evaluation of enthesis abnormalities was provided in all subgroups of patients. Madrid Sonography Enthesitis Index (MASEI) score was used to assess entheses, exploring six sites bilaterally: proximal plantar fascia, distal Achilles tendon, distal and proximal patellar tendon insertion, distal quadriceps tendon and distal brachial triceps tendon [25]. The evaluation of the tendon thickness was based on the subjective measurement of the assessor. Each tendon was scanned in both the longitudinal and transverse planes. The HFUS evaluation was performed for each enthesis about the following features: calcifications, bursae, erosions, thickness, and structure of tendon (cortical bone profile, intratendon and paratendon echogenicity) and PD signal in bursa or enthesis. Each item was scored as 1 point, except for calcification (0 = absent, 1 = small calcification or ossification with an irregularity of enthesis cortical bone profile; 2 = clear presence of enthesophytes; 3 = large calcifications or ossifications) erosion, and PD signal (0 or 3 whether they are present or not) [25]. As reported in available literature [26], a cut-off of 4.5 of MASEI was used to codify a pathologic enthesis involvement.
Statistical analysis
Mean BUNES and MASEI scores derived by HFUS assessment of nail and enthesis abnormalities were compared among patients with PSO, PSA with PSO, and PSA sine PSO by using the one-way analysis of variance (ANOVA) test. Two-sided P values < 0.05 were considered as being statistically significant.
Results
Clinical features of evaluated patients
In this study, 59 patients (17 males/42 females) were included, belonging to the three groups, 19 affected by PSO, 22 by PSA with PSO, and 18 by PSA sine PSO. On clinical dermatologic evaluation, PASI and NAPSI characterized patients affected by PSO and those by PSA with PSO. The most common clinical PSO variant was plaque-type PSO which was present in 94.7% and 81.6% in patients affected by PSO and in those by PSA with PSO, respectively. Nail PSO was present in 68.4% and 81.8% in patients with PSO and in those affected by PSA with PSO, respectively. The clinical rheumatologic evaluation showed that patients with PSA with PSO and PSA sine PSO were characterised by an increased number of tender and swollen joints, as well as by LEI. Clinical findings of evaluated patients are reported in Table 1.
Table 1.
Descriptive features of assessed patients
| PSO | PSA with PSO | PSA sine PSO | |
|---|---|---|---|
| Patients | 19 | 22 | 18 |
| Demographic features | |||
| Age, years | 50.2 ± 14.3 | 56.5 ± 11.4 | 56.2 ± 1.5 |
| Male Sex | 47.4% | 22.7% | 16.7% |
| BMI | 26.9 ± 6.8 | 27.7 ± 5.5 | 25.6 ± 3.2 |
| Dermatologic assessment | |||
| PASI | 7.9 ± 6.2 | 3.4 ± 4.8 | 0.0 |
| Plaque type PSO | 94.7% | 81.6% | 0.0% |
| Inverse/genital PSO | 31.6% | 4.5% | 0.0% |
| Palmo-plantar PSO | 5.3% | 18.2% | 0.0% |
| Guttate PSO | 31.6% | 9.1% | 0.0% |
| Nail PSO | 68.4% | 81.8% | 0.0% |
| NAPSI | 15.3 ± 12.3 | 23.2 ± 16.6 | 0.0 |
| Rheumatologic assessment | |||
| Tender joints | 2.0 ± 3.9 | 9.0 ± 7.0 | 9.5 ± 7.1 |
| Swollen Joints | 0.0 | 0.4 ± 0.1 | 0.7 ± 0.5 |
| LEI | 0.0 | 1.5 ± 0.6 | 1.4 ± 0.8 |
| Ultrasound evaluation | |||
| BUNES nail morphometry | 1.5 ± 0.4 | 1.6 ± 0.6 | 1.3 ± 0.5 |
| BUNES nail PD | 1.9 ± 1.9 | 2.5 ± 2.1 | 2.4 ± 2.1 |
| MASEI | 4.6 ± 3.7 | 6.5 ± 3.6 | 4.9 ± 2.9 |
Continuous variables are expressed ad mean and standard deviation, dichotomic variables are expressed as percentage
PSO psoriasis, PSA psoriatic arthritis, BMI body mass index, PASI Psoriasis Area and Severity Index, NAPSI Nail Area and Severity Index (NAPSI), LEI Leed Enthesitis Index, MASEI Madrid Sonography Enthesitis Index, BUNES Brown University Nail Enthesis Scale, PD power doppler
HFUS nail evaluation
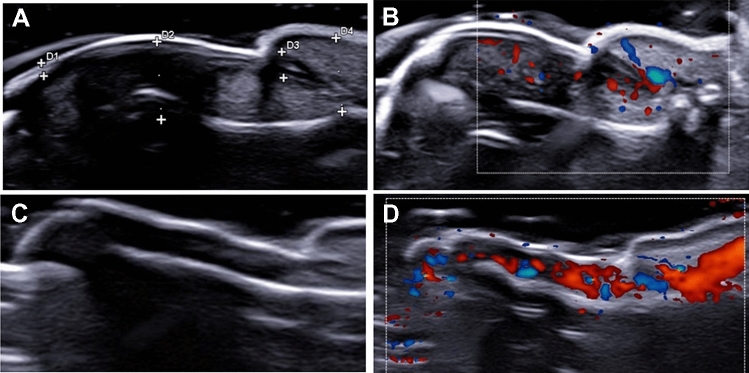
Descriptively, HFUS evaluation identified different morphological and vascular nail findings in the three groups. In patients with PSO, the structure of nail was mainly preserved but an increased blood flow, identified by PD, was found as elongated, dilated, and tortuous blood vessels because of an active inflammatory process. Assessing the nails in patients with PSA with PSO, HFUS evaluation showed some structural changes. Thickened matrix, inhomogeneous echogenicity nail bed, enlarged nail enthesis, increased blood flow, loss of ventral and dorsal plate definition, were observed in this group of patients. These findings are shown in Fig. 1. The assessment of patients with PSA sine PSO showed a less marked evidence of vascular and echogenicity changes in the evaluated nails by HFUS. However, 38.9% of patients with PSO sine PSA were codified as having a subclinical involvement of nails, characterised by the presence of nail hyperechoic areas and thickened beds associated with PD findings in nail bed and matrix. The nail ultrasound abnormalities were also scored by BUNES. No significant difference was reported comparing the three groups of patients based on the mean values of BUNES morphometry (p = 0.201) and BUNES PD (p = 0.391).
Fig. 1.
HFUS nail evaluation. PATIENT 1: A structural nail changes characterized by inhomogeneous echogenicity nail bed (d1), enlarged nail enthesis (d2), thickened matrix (d4) and plate (d3) with overall increased blood flow (B); PATIENT 2: C normal nail morphology without and with an increased Doppler signal (D)
HFUS enthesis evaluation
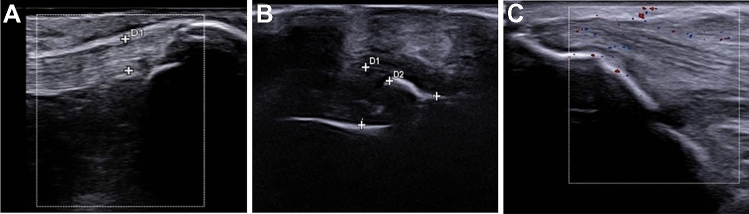
HFUS evaluation of entheses showed overlapping alterations in patients with PSA with PSO and in those with PSA sine PSO. In these groups, modifications of the structure of the entheses have been identified as a hypoechoic aspect and thickness of the tendon, focal cortical erosion, and enthesis ossification. No significant difference was noticed assessing the two sides of each scanned tendon. However, an increase of vascularity was rarely reported by PD assessment. These findings are shown in Fig. 2. In 52.6% of patients with PSO, a normal enthesis insertion with normal fibrillar pattern and bone profile was observed. Whereas in 47.4% of these patients with PSO without a clinically relevant musculoskeletal involvement, some alterations of entheses were reported by HFUS. Altered echogenicity of tendon structure, irregularity of enthesis cortical bone profile, and enthesophytes were observed despite normal values of LEI, which were retrieved in these patients. MASEI was also employed to score the enthesis abnormalities and no significant difference was reported comparing the three groups of patients (p = 0.166).
Fig. 2.
HFUS enthesis evaluation. A Thickened distal rotuleus tendon (d1: 4.5 mm) with irregular cortical profile without significant increase in the vascular pattern; B Thickened Achilles tendon (d1: 5.6 mm) with large calcification (d2; MASEI score = 3); C Normal fibrillar pattern of triceps tendon without significant Doppler signal
Discussion
In our single centre cross-sectional study, the potentiality of HFUS was explored in evaluating nail and enthesis abnormalities in patients with PSO, PSA with PSO, and PSA sine PSO. HFUS may be considered as the next frontier in ultrasound evaluation. It may have many clinical applications increasing diagnostic potentiality and evaluating the efficacy of administered therapies. In addition, the relevance of this noninvasive imaging tool may highlight the possibility to reduce the need of invasive investigations. By using HFUS, we provided a qualitative and quantitative characterization of nail and enthesis abnormalities in patients with PSO, PSA with PSO, and PSA sine PSO.
In patients affected by PSO and in those by PSA with PSO, HFUS evaluation identified some nail alterations characterised by thickened matrix, inhomogeneous echogenicity of nail bed, and increased blood flow by PD assessment. In fact, ultrasonography may provide valuable information regarding the morphostructural changes and PD in nails in patients with PSO and PSA [27]. This technique may identify nail alterations in patients with PSO and PSA, with or without a relevant clinical involvement, when compared with healthy control [28–30]. Therefore, ultrasonography may allow the clinicians to assess the presence of nail changes offering the possibility to score the severity of the inflammatory lesions, thus suggesting its clinical usability as diagnostic and prognostic tool [31, 32]. In addition, in our patients with PSA sine PSO, a subclinical nail involvement was also observed overlapping with what reported in PSA with PSO and in those with PSO considering the values of BUNES. These data could suggest a nail subclinical involvement in some patients with PSA sine PSO, which could predict the occurrence of skin involvement. It has been reported that rheumatological manifestations may precede the clinical presence of cutaneous involvement in 20% of patients with PSA sine PSO [33]. Furthermore, this subclinical nail involvement could reinforce the concept of psoriatic disease continuum, ranging from skin involvement to the musculoskeletal manifestations [34]. According to the nail-entheseal pathogenesis proposed in psoriatic disease [1, 9, 35], the nail lesions are frequently associated with the presence of enthesis involvement suggesting the relevance of their evaluation in managing these patients [36–38].
In our cohort, HFUS assessment of entheses showed modifications of these structures mainly characterised by a hypoechoic aspect and thickness of the tendon, focal cortical erosion, and ossification. These features were mainly observed in patients affected by PSA with PSO and in those by PSA sine PSO. However, our preliminary data could also propose a subclinical enthesis involvement in patients with PSO overlapping with what observed in PSA with PSO and in PSA sine PSO as per results of MASEI. These results may provide further insights in this context by using HFUS suggesting that enthesis abnormalities may be highlighted in a substantial proportion of patients with PSO who are asymptomatic for musculoskeletal involvement [39–42]. Therefore, a more accurate assessment of a subclinical enthesis involvement, provided by HFUS, could possibly answer to the question if these imaging features could predict the risk of future clinically relevant musculoskeletal inflammation in these patients.
Taking together all these findings, HFUS may be added to an integrated and multidisciplinary approach of the psoriatic disease. The combination of clinical, both dermatological and rheumatological, assessment with HFUS may provide the ideal environment for a prompt assessment, immediate discussion, and an optimum management for each patient.
Although providing some insights of HFUS potentiality in patients with psoriatic disease, some limitations, mainly related to the single centre design and the relatively small sample size, should be considered in limiting the external validity of our data. Thus, subsequent confirmatory studies are needed to fully confirm these data and to evaluate their clinical relevance. The predictive role of these imaging abnormalities should be properly evaluated in specific designed longitudinal studies. Finally, an additional limitation of the present work could be that a single operator was involved in HFUS assessment, therefore the possible inter-observer variability of the ultrasonography findings should be entirely clarified in additional specific designed studies.
In conclusion, qualitative and quantitative abnormalities of nail and enthesis were demonstrated by HFUS in assessed patients with PSO, PSA with PSO, and PSA sine PSO, suggesting a practical and reliable tool to be used in clinical settings. Furthermore, HFUS highlighted a subclinical nail involvement in patients with PSA sine PSO and some enthesis subclinical alterations in patients with PSO. Although further studies are needed, our findings may offer the opportunity to better characterize the phases of the psoriatic disease by a multidisciplinary approach combining dermatological and rheumatological assessments with HFUS.
Funding
Open access funding provided by Università degli Studi dell’Aquila within the CRUI-CARE Agreement. This work has been supported by “Bando per il finanziamento dei progetti anno 2021 (RIA 2021)” from Department of Biotechnological and Applied Clinical Sciences, University of L’Aquila, L’Aquila, Italy.
Data availability
All the generated data are included in the body of the article.
Declarations
Conflict of interest
None declared.
Ethics approval
The local ethics committee approved the study (protocol number Internal Review Board University of L’Aquila 01/2022), which was performed according to Good Clinical Practice guidelines and Declaration of Helsinki.
Informed consent
Not applicable, all the data are de-identified.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Piero Ruscitti, Maria Esposito and Camilla Gianneramo have contributed equally to this work.
Paola Cipriani, Antonio Barile, and Maria Concetta Fargnoli have contributed equally to this work.
References
- 1.Scarpa R. Psoriatic Syndrome or Psoriatic Disease? J Rheumatol. 2020;47(6):941. doi: 10.3899/jrheum.200051. [DOI] [PubMed] [Google Scholar]
- 2.Parisi R, Symmons DP, Griffiths CE, Ashcroft DM. Identification and management of psoriasis and associated comorbidiTy (IMPACT) project team. Global epidemiology of psoriasis: a systematic review of incidence and prevalence. J Invest Dermatol. 2013;133(2):377–85. doi: 10.1038/jid.2012.339. [DOI] [PubMed] [Google Scholar]
- 3.Esposito M, Giunta A, Nanni RC, Criscuolo S, Manfreda V, Del Duca E, Bianchi L, Troisi A. Depressive symptoms and insecure attachment predict disability and quality of life in psoriasis independently from disease severity. Arch Dermatol Res. 2021;313(6):431–437. doi: 10.1007/s00403-020-02116-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Griffiths CEM, Armstrong AW, Gudjonsson JE, Barker JNWN. Psoriasis Lancet. 2021;397(10281):1301–1315. doi: 10.1016/S0140-6736(20)32549-6. [DOI] [PubMed] [Google Scholar]
- 5.Langley RG, Krueger GG, Griffiths CE. Psoriasis: epidemiology, clinical features, and quality of life. Ann Rheum Dis. 2005;64:18–23. doi: 10.1136/ard.2004.033217. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Van den Bosch F, Coates L. Clinical management of psoriatic arthritis. Lancet. 2018;391(10136):2285–2294. doi: 10.1016/S0140-6736(18)30949-8. [DOI] [PubMed] [Google Scholar]
- 7.Jiaravuthisan MM, Sasseville D, Vender RB, Murphy F, Muhn CY. Psoriasis of the nail: anatomy, pathology, clinical presentation, and a review of the literature on therapy. J Am Acad Dermatol. 2007;57(1):1–27. doi: 10.1016/j.jaad.2005.07.073. [DOI] [PubMed] [Google Scholar]
- 8.Langenbruch A, Radtke MA, Krensel M, Jacobi A, Reich K, Augustin M. Nail involvement as a predictor of concomitant psoriatic arthritis in patients with psoriasis. Br J Dermatol. 2014;171(5):1123–1128. doi: 10.1111/bjd.13272. [DOI] [PubMed] [Google Scholar]
- 9.McGonagle D, Lories RJ, Tan AL, Benjamin M. The concept of a "synovio-entheseal complex" and its implications for understanding joint inflammation and damage in psoriatic arthritis and beyond. Arthritis Rheum. 2007;56(8):2482–2491. doi: 10.1002/art.22758. [DOI] [PubMed] [Google Scholar]
- 10.Barile A, Arrigoni F, Bruno F, Guglielmi G, Zappia M, Reginelli A, Ruscitti P, Cipriani P, Giacomelli R, Brunese L, Masciocchi C. Computed tomography and MR imaging in rheumatoid arthritis. Radiol Clin North Am. 2017;55(5):997–1007. doi: 10.1016/j.rcl.2017.04.006. [DOI] [PubMed] [Google Scholar]
- 11.Acanfora C, Bruno F, Palumbo P, Arrigoni F, Natella R, Mazzei MA, Carotti M, Ruscitti P, Di Cesare E, Splendiani A, Giacomelli R, Masciocchi C, Barile A. Diagnostic and interventional radiology fundamentals of synovial pathology. Acta Biomed. 2020;91(8-S):107–115. doi: 10.23750/abm.v91i8-S.9993. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Bruno F, Palumbo P, Arrigoni F, Mariani S, Aringhieri G, Carotti M, Natella R, Zappia M, Cipriani P, Giacomelli R, Di Cesare E, Splendiani A, Masciocchi C, Barile A. Advanced diagnostic imaging and intervention in tendon diseases. Acta Biomed. 2020;91(8–S):98–106. doi: 10.23750/abm.v91i8-S.10007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Scher JU, Ogdie A, Merola JF, Ritchlin C. Preventing psoriatic arthritis: focusing on patients with psoriasis at increased risk of transition. Nat Rev Rheumatol. 2019;15(3):153–166. doi: 10.1038/s41584-019-0175-0. [DOI] [PubMed] [Google Scholar]
- 14.Zabotti A, De Lucia O, Sakellariou G, Batticciotto A, Cincinelli G, Giovannini I, Idolazzi L, Maioli G, Tinazzi I, Aletaha D, De Vita S, Marchesoni A, Smolen J, Iagnocco A, McGonagle D, Caporali R. Predictors, risk factors, and incidence rates of psoriatic arthritis development in psoriasis patients: a systematic literature review and meta-analysis. Rheumatol Ther. 2021;8(4):1519–1534. doi: 10.1007/s40744-021-00378-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Caso F, Navarini L, Ruscitti P, Chimenti MS, Girolimetto N, Del Puente A, Giacomelli R, Scarpa R, Costa L. Targeted synthetic pharmacotherapy for psoriatic arthritis: state of the art. Expert Opin Pharmacother. 2020;21(7):785–796. doi: 10.1080/14656566.2020.1726317. [DOI] [PubMed] [Google Scholar]
- 16.Mlosek RK, Migda B, Migda M. High-frequency ultrasound in the 21st century. J Ultrason. 2021;20(83):e233–e241. doi: 10.15557/JoU.2020.0042. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Migda MS, Migda M, Słapa R, Mlosek RK, Migda B. The use of high-frequency ultrasonography in the assessment of selected female reproductive structures: the vulva, vagina and cervix. J Ultrason. 2019;19(79):261–268. doi: 10.15557/JoU.2019.0039. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Skrzypek E, Mlosek RK. High frequency ultrasound assessment of labial glands simulating small nodules or granulomas after lip augmentation. J Ultrason. 2021;20(83):e261–e267. doi: 10.15557/JoU.2020.0046. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Taylor W, Gladman D, Helliwell P, Marchesoni A, Mease P, Mielants H, CASPAR Study Group Classification criteria for psoriatic arthritis: development of new criteria from a large international study. Arthritis Rheum. 2006;54(8):2665–73. doi: 10.1002/art.21972. [DOI] [PubMed] [Google Scholar]
- 20.Raychaudhuri SK, Maverakis E, Raychaudhuri SP. Diagnosis and classification of psoriasis. Autoimmun Rev. 2014;13(4–5):490–5. doi: 10.1016/j.autrev.2014.01.008. [DOI] [PubMed] [Google Scholar]
- 21.Fredriksson T, Pettersson U. Severe psoriasis–oral therapy with a new retinoid. Dermatologica. 1978;157(4):238–244. doi: 10.1159/000250839. [DOI] [PubMed] [Google Scholar]
- 22.Rich P, Scher RK. Nail Psoriasis Severity Index: a useful tool for evaluation of nail psoriasis. J Am Acad Dermatol. 2003;49(2):206–212. doi: 10.1067/s0190-9622(03)00910-1. [DOI] [PubMed] [Google Scholar]
- 23.Healy PJ, Helliwell PS. Measuring clinical enthesitis in psoriatic arthritis: assessment of existing measures and development of an instrument specific to psoriatic arthritis. Arthritis Rheum. 2008;59(5):686–691. doi: 10.1002/art.23568. [DOI] [PubMed] [Google Scholar]
- 24.Cunha JS, Qureshi AA, Reginato AM. nail enthesis ultrasound in psoriasis and psoriatic arthritis: a report from the 2016 GRAPPA annual meeting. J Rheumatol. 2017;44(5):688–690. doi: 10.3899/jrheum.170146. [DOI] [PubMed] [Google Scholar]
- 25.de Miguel E, Cobo T, Muñoz-Fernández S, Naredo E, Usón J, Acebes JC, Andréu JL, Martín-Mola E. Validity of enthesis ultrasound assessment in spondyloarthropathy. Ann Rheum Dis. 2009;68(2):169–174. doi: 10.1136/ard.2007.084251. [DOI] [PubMed] [Google Scholar]
- 26.Ozkan F, Cetin GY, Bakan B, Kalender AM, Yuksel M, Ekerbicer HC, Sayarlioglu M. Sonographic evaluation of subclinical entheseal involvement in patients with Behçet disease. AJR Am J Roentgenol. 2012;199(6):W723–W729. doi: 10.2214/AJR.12.8576. [DOI] [PubMed] [Google Scholar]
- 27.Marina ME, Solomon C, Bolboaca SD, Bocsa C, Mihu CM, Tătaru AD. High-frequency sonography in the evaluation of nail psoriasis. Med Ultrason. 2016;18(3):312–317. doi: 10.11152/mu.2013.2066.183.hgh. [DOI] [PubMed] [Google Scholar]
- 28.Naredo E, Janta I, Baniandrés-Rodríguez O, Valor L, Hinojosa M, Bello N, Serrano B, Garrido J. To what extend is nail ultrasound discriminative between psoriasis, psoriatic arthritis and healthy subjects? Rheumatol Int. 2019;39(4):697–705. doi: 10.1007/s00296-018-4222-y. [DOI] [PubMed] [Google Scholar]
- 29.Sandobal C, Carbó E, Iribas J, Roverano S, Paira S. Ultrasound nail imaging on patients with psoriasis and psoriatic arthritis compared with rheumatoid arthritis and control subjects. J Clin Rheumatol. 2014;20(1):21–24. doi: 10.1097/RHU.0000000000000054. [DOI] [PubMed] [Google Scholar]
- 30.Aydin SZ, Castillo-Gallego C, Ash ZR, Marzo-Ortega H, Wakefield R, McGonagle D. Vascularity of nail bed by ultrasound to discriminate psoriasis, psoriatic arthritis and healthy controls. Clin Exp Rheumatol. 2017;35(5):872. [PubMed] [Google Scholar]
- 31.Krajewska-Włodarczyk M, Owczarczyk-Saczonek A. Usefulness of ultrasound examination in the assessment of the nail apparatus in psoriasis. Int J Environ Res Public Health. 2022;19(9):5611. doi: 10.3390/ijerph19095611.PMID:35565018;PMCID:PMC9105627. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Fassio A, Giovannini I, Idolazzi L, Zabotti A, Iagnocco A, Sakellariou G. Nail ultrasonography for psoriatic arthritis and psoriasis patients: a systematic literature review. Clin Rheumatol. 2020;39(5):1391–1404. doi: 10.1007/s10067-019-04748-2. [DOI] [PubMed] [Google Scholar]
- 33.Olivieri I, Padula A, D'Angelo S, Cutro MS. Psoriatic arthritis sine psoriasis. J Rheumatol Suppl. 2009;83:28–29. doi: 10.3899/jrheum.090218. [DOI] [PubMed] [Google Scholar]
- 34.Lubrano E, Scriffignano S, Perrotta FM. Psoriatic arthritis, psoriatic disease, or psoriatic syndrome? J Rheumatol. 2019;46(11):1428–1430. doi: 10.3899/jrheum.190054. [DOI] [PubMed] [Google Scholar]
- 35.McGonagle D, Aydin SZ, Tan AL. The synovio-entheseal complex and its role in tendon and capsular associated inflammation. J Rheumatol Suppl. 2012;89:11–14. doi: 10.3899/jrheum.120233. [DOI] [PubMed] [Google Scholar]
- 36.Acosta-Felquer ML, Ruta S, Rosa J, Marin J, Ferreyra-Garrot L, Galimberti ML, Galimberti R, Garcia-Monaco R, Soriano ER. Ultrasound entheseal abnormalities at the distal interphalangeal joints and clinical nail involvement in patients with psoriasis and psoriatic arthritis, supporting the nail-enthesitis theory. Semin Arthritis Rheum. 2017;47(3):338–342. doi: 10.1016/j.semarthrit.2017.05.002. [DOI] [PubMed] [Google Scholar]
- 37.Perrin C. Histological evaluation of the relationships between distal interphalangeal psoriatic arthritis and nail psoriasis: correlations with anatomical studies of the normal nail unit and the main radiological data concerning distal interphalangeal psoriatic arthritis. Am J Dermatopathol. 2020;42(12):911–915. doi: 10.1097/DAD.0000000000001786. [DOI] [PubMed] [Google Scholar]
- 38.Elliott A, Pendleton A, Wright G, Rooney M. The relationship between the nail and systemic enthesitis in psoriatic arthritis. Rheumatol Adv Pract. 2021;5(3):088. doi: 10.1093/rap/rkab088. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Offidani A, Cellini A, Valeri G, Giovagnoni A. Subclinical joint involvement in psoriasis: magnetic resonance imaging and X-ray findings. Acta Derm Venereol. 1998;78(6):463–465. doi: 10.1080/000155598442809. [DOI] [PubMed] [Google Scholar]
- 40.Simon D, Faustini F, Kleyer A, Haschka J, Englbrecht M, Kraus S, Hueber AJ, Kocijan R, Sticherling M, Schett G, Rech J. Analysis of periarticular bone changes in patients with cutaneous psoriasis without associated psoriatic arthritis. Ann Rheum Dis. 2016;75(4):660–666. doi: 10.1136/annrheumdis-2014-206347. [DOI] [PubMed] [Google Scholar]
- 41.Salaffi F, Carotti M, Beci G, Di Carlo M, Giovagnoni A. Radiographic scoring methods in rheumatoid arthritis and psoriatic arthritis. Radiol Med. 2019;124(11):1071–1086. doi: 10.1007/s11547-019-01001-3. [DOI] [PubMed] [Google Scholar]
- 42.Paparo F, Revelli M, Semprini A, Camellino D, Garlaschi A, Cimmino MA, Rollandi GA, Leone A. Seronegative spondyloarthropathies: what radiologists should know. Radiol Med. 2014;119(3):156–163. doi: 10.1007/s11547-013-0316-5. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
All the generated data are included in the body of the article.