If we ask a group of intelligent and educated individuals not familiar with the science or practice of radiation protection to review published information on health effects of exposures to low levels of radiation and share their findings, they are likely to come away with an understanding that is as clear as mud. This is unfortunate.
While the unfamiliar jargon, complex quantities and concepts, linguistic nuances, and inherent uncertainties provide a fertile ground for confusion, there is another contributing factor to this bewilderment, with potentially damaging long-term consequences: it is not unusual to find instances in scientific publications or conferences where the system of radiation protection or its scientific underpinnings are misrepresented or mischaracterised. The language used by some authors target the credibility and intentions of respected institutions and independent radiation protection commissions that for nearly a century have laid the foundation of radiation protection practice and are the regarded authoritative voices in this field. Eroding trust in those institutions, not only among young professionals entering the field but the public in general, can have devastating consequences.
To ‘immunise’ against such misinformation and misleading characterisations, objective overviews of the current state of science and demonstrations of how that science is used to inform radiation protection policy and decision making can equip radiation protection professionals with the information they need.
Recognising this need, the American Academy of Health Physics (AAHP) sponsored a full-day technical session on 17 July 2018 at the annual meeting of the Health Physics Society (HPS) in Cleveland, Ohio. This session was structured to describe the current state of science, from molecular biology to human epidemiology, as well as to explain how that science is translated to radiation protection policy and regulations for low levels of radiation. In addition, the expected role of radiation protection professionals was discussed at length. The feedback from conference attendees was positive and encouraging, indicating that the information presented filled a need.
To make this material available to the broader community, the Journal of Radiological Protection invited speakers of the AAHP session to submit manuscripts based on their presentations for peer review and inclusion in this special issue.
1. The big picture
In spite of decades of research and a large volume of data from molecular, cellular, and animal experiments as well as large epidemiologic investigations, uncertainty in potential health effects of exposure to low doses and low dose rates of radiation remain. It is important to provide some perspective, however. We do know a great deal about the interactions of ionising radiation with living tissue. At high radiation doses, we can predict with some certainty the expected acute health effects for individuals exposed, and predict their prognosis (figure 1). At moderate doses of radiation, we do not expect any acute clinical effects, but we can estimate with high assurance the expected increase in cancer rates for a population exposed as described by Boice et al [1]. At low doses, however, where the probability of adverse health effects is less than 1%, it is not possible to predict cancer rates in populations with any degree of accuracy. Nor is it possible to determine if health effects in a given individual are radiogenic because we have not yet identified any biomarkers that are specific to radiation. In others words, we cannot clinically distinguish a radiogenic cancer from one that resulted from other causes, either at high doses or at low doses.
Figure 1.
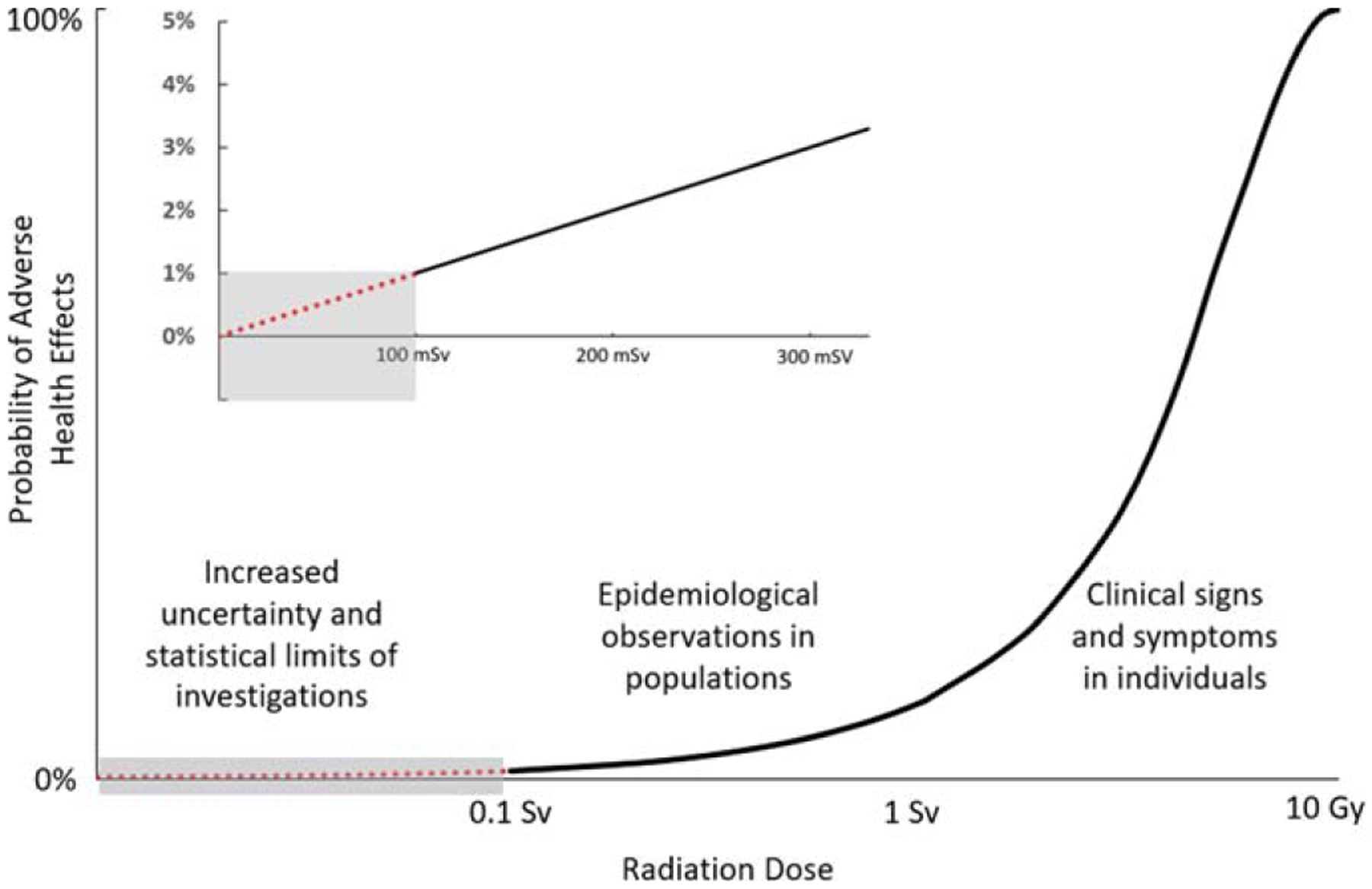
Relationship of radiation doses and effects. Adapted and revised from United Nations Environment Programme (UNEP) booklet, Radiation Effects and Sources http://wedocs.unep.org/handle/20.500.11822/7790. The grey area represents the low dose region where routine occupational, environmental and diagnostic medical exposures occur.
With the exception of a radiological accident, all routine occupational, environmental, and diagnostic medical exposures are in this low dose region (the grey box in figure 1). This is good news because the probability of adverse health effects from these exposures is correspondingly very low. However, we cannot be certain quantitatively how low that possibility is - it is the difference between very low, extremely low, or potentially zero risk. These limitations fuel the ongoing debate.
2. What it means to be stochastic
While we have learned a great deal about the process of carcinogenesis, and there remains a great deal more to learn, it is widely accepted that this complex process is stochastic, meaning there exists an element of chance. The excess risk of cancer from radiation exposures down to about 100 mSv is documented. A myriad of complex molecular and biochemical changes have been reported at lower doses as reviewed by Azzam [2]. The lowest dose at which biological effects are detected with confidence appears to be a matter of technology. Single cell analyses, which are now possible, have suggested that radiation responses observed in whole cell cultures are not indicative of identical patterns in all cells. While it is not yet possible to predict how these molecular and cellular changes may ultimately affect the probability of cancer in an individual, we continue to identify mechanisms and pathways through which the stochastic nature of carcinogenesis is expressed. As described by Shuryak [3], mathematical and biological response models, based on our current knowledge of radiobiology, carcinogenesis and epidemiology, can help improve estimates of radiation health effects and develop testable hypotheses.
It is vital to separate two very different applications of our knowledge as well as our uncertainty in low dose health effects. One application (risk assessment) seeks to project and estimate health effects following low level exposures. While large uncertainties exist, it should be acknowledged that these uncertainties have an upper bound as evident from well-documented epidemiological studies. The upper bound of this uncertainty still presents a low probability of occurrence (figure 1).
The second application (dose management) is in the realm of protecting against possible health effects of radiation in various exposure situations. It is unreasonable to assume that risk of cancer from low doses of radiation suddenly dives to zero at doses below 100 mSv [4]. The focus of the remainder of this special issue is on how the science and knowledge of health effects from low dose radiation (and the uncertainties therein) are used to inform radiation protection policy and practices and make radiation protection decisions that are defensible and based on both the strongest science and accepted ethical principles.
3. What it means for radiation protection
As discussed above, it is important to distinguish effort to predict health effects of low level radiation for individuals (risk assessment) from effort to establish a system of radiation protection to protect the health and safety of all individuals (dose management). The development of new recommendations by the National Council on Radiation Protection and Measurements (NCRP) for occupational, public, medical, emergency worker, and environmental protection categories is described by Cool [5]. Ethical values, stakeholder engagement, and safety culture are specifically addressed as important components for implementing the system of protection.
How the science and the recommendations of the national [6] and international [7] advisory bodies are used to implement radiation protection policy by three federal agencies in the United States are described by:
Al-Nabulsi and Favret for the US Department of Energy [8],
Pawel and Boyd for the US Environmental Protection Agency [9], and
Jones for the US Nuclear Regulatory Commission [10].
These authors provide an overview of the approach and methodology employed by regulating agencies to consider recommendations by advisory bodies and stakeholder input, among other factors, to develop, document, and implement radiation protection policy for the nation.
In 2017, the US General Accountability Office (GAO) conducted an independent evaluation of how federal agencies in the United States develop and apply radiation protection requirements and guidance for workers and the public. The GAO also examined the extent to which these federal agencies fund and coordinate research on the health effects of low dose radiation. Neumann et al describe the findings of this report and the GAO recommendations regarding the need for a coordinated research effort [11].
What is striking in all this information is the laborious, deliberative, and painstaking methodology to arrive at the radiation protection practices we have today to protect workers, patients, and the public (including sensitive subpopulations) in all exposure situations including emergency circumstances. This effort is not visible to many, and it often goes unappreciated.
There is a tendency among some radiation professionals to think that radiation is singularly targeted for more stringent protection criteria. In his paper, Irwin compares radiological protection to approaches employed to protect against potential chemical carcinogens, and concludes that controls on radiation exposure do not appear to be more stringent than restrictions on exposure to chemical carcinogens [12].
Our role as radiation protection professionals is both clear and challenging. We are ethically obligated to practice the profession within the established guidelines set forth by advisory bodies and regulating authorities. This ethical obligation is similar in this respect to the medical profession. While there are established mechanisms for radiation professionals to have input to the process, providing advice that may be contrary to the guidelines and recommendations from regulatory authorities and respected scientific bodies can erode public confidence in the system of radiological protection which has been so successful over the past 100 years. And it can harm the credibility of our profession [13].
Our role is also challenging because we are often on the frontlines of communication with stakeholders, and need to be able to explain the rationale and basis of our radiation protection practices. The system of radiation protection is robust, but it does not lend itself to easy communication messages. This is particularly challenging for us because the subject of ‘radiation’ is alarming and generates immediate negative emotions for many people.
4. The road ahead
It is advisable to preface any discussion of health effects from exposures to low levels of radiation with an acknowledgement of the upper probability bounds of health effects under consideration and to provide the larger context (figure 1). The uncertainties in the dose response relationships have been acknowledged since the first ICRP publication [14]. While there is undisputed need for more biological and epidemiological studies [15, 16], some level of uncertainty in probability of health effects (primarily cancer) at low doses will always exist.
A major challenge in our profession is in effectively communicating this risk and its uncertainties to stakeholders. The AAHP sponsored a second full-day session at the annual HPS meeting in Orlando, Florida, on 9 July 2019. The aim of that technical session was to discuss risk communication challenges and approaches and examine how we can improve our public communication practices using research-based risk communication strategies.
While we concentrate our efforts in reaching out to the public, providing radiation protection practitioners periodic and frequent updates on the state of science and the principle underpinnings of the system of radiation protection they practice is also important. The potential benefits of such effort are twofold: (1) radiation protection professionals will become resistant to misinformation with which they are increasingly bombarded, and (2) they are better equipped to communicate with their stakeholders. We have a robust system of radiation protection in which we can take pride. A robust approach to public communication and a clear and concise messaging strategy can further strengthen this system.
Footnotes
Disclaimer
The findings, conclusions, or statements in this manuscript are those of the authors and do not necessarily represent the official positions of the Centers for Disease Control and Prevention, the American Academy of Health Physics, Vanderbilt University School of Medicine, or the National Council on Radiation Protection and Measurements.
References
- [1].Boice JD, Held K and Shore R 2019. Radiation epidemiology and low dose health effects following low-LET radiation J. Radiol. Prot 39 S14. [DOI] [PubMed] [Google Scholar]
- [2].Azzam EI. What does radiation biology tell us about potential health effects at low dose and low dose rates. J. Radiol. Prot. 2019;39:S28. doi: 10.1088/1361-6498/ab2b09. [DOI] [PubMed] [Google Scholar]
- [3].Shuryak I. Enhancing low dose risk assessment using mechanistic mathematical models of radiation effects. J. Radiol. Prot. 2019;39:S1. doi: 10.1088/1361-6498/ab3101. [DOI] [PubMed] [Google Scholar]
- [4].Wakeford R 2005. The risk to health from exposure to low levels of ionising radiation Ann. ICRP 35 v–ii [DOI] [PubMed] [Google Scholar]
- [5].Cool D. Translating science into recommendations: The development of NCRP Report 180. J. Radiol. Prot. 2019;39:S57. doi: 10.1088/1361-6498/ab1b98. [DOI] [PubMed] [Google Scholar]
- [6].National Council on Radiation Protection and Measurements, Management of Exposure to Ionizing Radiation: Radiation Protection Guidance for the United States 2018. NCRP Report No. 180 (Bethesda, MD: National Council on Radiation Protection and Measurements; ) [Google Scholar]
- [7].International Commission on Radiological Protection 2007. The recommendations of the International Commission on Radiological Protection, ICRP publication 103 Ann. ICRP vol 37 (Oxford: Elsevier Science Ltd; ) [DOI] [PubMed] [Google Scholar]
- [8].Al-Nabulsi I and Favret D 2019. Low-dose radiation research and radiation protection policy implementation at the Department of Energy J. Radiol. Prot 39 S65. [DOI] [PubMed] [Google Scholar]
- [9].Pawel D and Boyd M 2019. Studies of radiation health effects inform EPA actions J. Radiol. Prot 39 S40. [DOI] [PMC free article] [PubMed] [Google Scholar]
- [10].Jones CG. The US nuclear regulatory commission radiation protection policy and opportunities for the future. J. Radiol. Prot. 2019;39:R51. doi: 10.1088/1361-6498/ab1d75. [DOI] [PubMed] [Google Scholar]
- [11].Neuman J, Cook J and Chan A 2019. Low-dose radiation: interagency collaboration on planning research could improve information on health effects J. Radiol. Prot Accepted ( 10.1088/1361-6498/ab1ada) [DOI] [PubMed] [Google Scholar]
- [12].Irwin W 2019. Radiological & toxicological risk assessment and the linear no-threshold perspective J. Radiol. Prot Accepted ( 10.1088/1361-6498/ab396d) [DOI] [PubMed] [Google Scholar]
- [13].Ansari A 2019. The role of radiation protection professionals in the landscape of low dose radiation J. Radiol. Prot Accepted ( 10.1088/1361-6498/ab15e6) [DOI] [PMC free article] [PubMed] [Google Scholar]
- [14].International Commission on Radiological Protection 1959. Recommendations of the international commission on radiological protection ICRP Publication 1 (New York: Pergamon; ) [DOI] [PubMed] [Google Scholar]
- [15].The United States Government Accountability Office 2017. Low-Dose Radiation: Interagency Collaboration on Planning Research Could Improve Information on Health Effects GAO-17–546 (Washington, DC: The United States Government Accountability Office; ) [Google Scholar]
- [16].Engineering and Medicine 2019. Gilbert W. Beebe Symposium on the Future of Low-Dose Radiation Research in the United States (Washington, DC: The National Academies of Sciences; ) (http://dels.nas.edu/Upcoming-Event/Gilbert-Beebe-Symposium/AUTO-5-92-64-H) (Accessed 12 August 2019) [Google Scholar]


