Abstract
Background
Motherhood involves a process of adaptation and the perception of social support influences mental health, breastfeeding or newborn care among others. The COVID-19 pandemic has generated a distancing from family, friends and health professionals.
Methods
Quantitative, descriptive, cross-sectional study. The present study aims to describe and analyze the social support and mental health of mothers during this period.
Methods
The sample were 179 women with children older than 6 months. The questionnaires used were the DUKE-UNC-11 and GHQ-12. Data analysis was carried out with Spearman's Rho and Mann Whitney U test.
Results
75.8% of the sample perceived normal social support during the pandemic. Within the dimensions of social support, women reported perceiving satisfactory confidential support, while affective support was perceived as low. Correlational analysis reported a significant relationship between mental health, confidential support and affective support. Group comparison noted greater confidential support in primiparous.
Conclusions
The sample is sensitive to changes originated by COVID-19 constraints influencing perceived social support and mental health. Affective and confidential support as well as the involvement of health professionals and the environment are fundamental for mental health during the first year of maternity.
Relevance to clinical practice
Mothers' mental health is sensitive and vulnerable to social changes, in this case, those that occurred as a consequence of the COVID-19 outbreak.
Keywords: COVID-19, Maternity, Mental health and social support
Introduction
Studies demonstrate the existence of a link between levels of social support and health outcomes, both in terms of mental and physical health (Muñoz-Bermejo et al., 2020), with the link being particularly strong for women (Gaino et al., 2019; Szkody and McKinney, 2020). Taking the specific case of pregnant women, social support is not only linked to better mental health in general (Li et al., 2017; Peter et al., 2017) but also specifically connected to lower levels of stress, anxiety, and depression (Rodríguez Leis and Flores Gallegos, 2018). In addition, good social support has been shown to have positive effects during labor (Zamani et al., 2019), and in the postpartum period (Tani and Castagna, 2017; Vaezi et al., 2019; Webster et al., 2011), as well as helping reduce women's risk of developing postnatal depression generally (Contreras-García et al., 2017) and throughout the period of breastfeeding (Maleki-Saghooni et al., 2020). Indeed, Tani & Castagna (Tani and Castagna, 2017) were able to prove the positive influence of social support during labor, as well as showing it to be a protective factor against depression (Tani and Castagna, 2017). In the same vein, Li et al. (Li et al., 2017) showed that women who reported high levels of social support were less likely to develop depression. With respect to breastfeeding, it has been shown that good social support during this period leads to longer breastfeeding times and more exclusive breastfeeding (McFadden et al., 2017) and, in addition, access to advice within the community before and after the baby's birth can also encourage breastfeeding (Kummer et al., 2020; Sehhatie et al., 2020).
Studies considering the psychological impact of the COVID-19 pandemic on the population as a whole tend to show the outbreak caused increased levels of emotional distress and social upheaval, and this affected women in particular (Parrado-Gonzalez and León-Jaruego, 2020). It is also widely accepted that the pandemic had significant repercussions for reproductive and perinatal care in the sense that maternity and infant health services had to change and develop new working protocols to reduce infection risk (Liang and Acharya, 2020; Valdés-Bango et al., 2020) and avoid the adverse effects of contracting the disease. Research at the European level, for example, revealed significant reductions in the support given to expectant mothers and their families. In general, there have been reductions in the number of antenatal consultations, with some of these being replaced by telephone appointments, meaning that foetal heart rates are monitored less often leading to higher levels of maternal anxiety; limiting the number of people who can accompany expectant mothers and the involvement of her partner during labor; and reductions in the use of epidural anesthesia due to staffing considerations (Kotlar et al., 2021).
The consequences of these changes can be seen in a reported increase in symptoms of anxiety and depression among pregnant women compared to pre-pandemic levels. Major concerns seem to be related to changes in antenatal care, the presence (or otherwise) of their birth partner in hospital, early discharge, disconnection from their extended support network during the postnatal period, work commitments, and caring for other children (DeYoung and Pregnancy, 2021; Lebel et al., 2020). Other variables related to the COVID-19 lockdowns described by pregnant women as impacting on their mental health include feelings of loneliness, fear of infection, stress, as well as the development of obsessions, compulsions, phobias, and insomnia (Khoury et al., 2021; Romero-Gonzalez et al., 2021). The pandemic has also affected the mental health of postnatal mothers, with evidence indicating a growth in the prevalence of postnatal depression, and post-traumatic stress disorder reported during the COVID-19 lockdowns (Ostacoli et al., 2020). Of particular relevance here, is a study from Italy that explored depression among mothers with children under the age of one year old and discovered a significant relationship between depressive symptoms and factors such as fear of infection (of the mother or her child), fear of close contact with the coronavirus infection, and financial worries concerning loss of income (Spinola et al., 2020).
The COVID-19 pandemic has also had an effect on rates of breastfeeding. The first studies to look at breastfeeding and COVID-19 infection identified significant risks (Stumpfe et al., 2020) to the extent that women testing positive for the infection have been advised to feed their babies on formula rather than to breastfeed (Coxon et al., 2020; Jing et al., 2020). At the same time, mothers deciding to breastfeed have suffered from reduced levels of social support during the pandemic, including a reduction in the availability of professional advice about breastfeeding, as well as lower levels of support from family, friends, and postnatal support organisations (Ceulemans et al., 2020). In addition, the lack of personal interactions and the difficulty of accessing mother and baby services during the pandemic has reduced women's’ ability to get help for breastfeeding (Snyder and Worlton, 2021). Furthermore, during the pandemic, breastfeeding mothers were given erroneous information with regard to the infection and breastfeeding (Brown and Shenker, 2021).
The state of emergency provoked by the COVID-19 pandemic, particularly in terms of the social isolation, has resulted in fragmentation of the family, social networks, and indeed professional networks, including among healthcare workers. This has caused huge, unprecedented changes that have had an important impact on the experience of motherhood (Molgora and Accordini, 2020) particularly in the context of mental health (Parrado-Gonzalez and León-Jaruego, 2020), as well as in connection with the low levels of social support encountered during this period of upheaval (Zhou et al., 2021). In this way, the objective of the current study is to describe the perceived level of social support reported by mothers with children under one year old during the COVID-19 pandemic and to study the relationship between this and their self-perceived state of mental health.
Methods
Study design
A descriptive, transversal, observational study completed using an online questionnaire.
Sample
Participants were recruited to the study using snowball sampling. The inclusion criteria were that participants had children under one year of age at the time the state of emergency was declared on 15th March 2020 or that they had given birth during the 2021 year. Those who became mothers outside this time period, with children under six months at the time of the study, were excluded.
Procedure
Data collection was completed using a Google Forms digital questionnaire and took place between 1st July 2021 to 12th November 2021. Midwives in various roles in Primary or Specialist Care were contacted through the XX Official College of Nursing Professionals to be our first point of contact and begin disseminating information about the study to other health care professionals. We also enlisted the help of various breastfeeding associations and, in addition, used a variety of social media platforms to increase the visibility of the study. The questionnaire was accompanied by an introductory letter to explain the aims of the study and give instructions on how to complete the questionnaire. Informed consent was obtained for all participants after appropriate assurances were given concerning the voluntary nature of the questionnaire, anonymity, confidentiality, and data protection. Furthermore, participants were given a contact email address in the case that they had any questions or required further clarification on any aspect of the study.
Instruments
The online questionnaire had three sections. The first comprised questions about socio-demographics, the second contained questions about participants’ perceptions concerning their level of social support, and the third was aimed at assessing participants’ self-perceived mental health status.
To measure perceptions of social support, the Duke-UNC-11 Functional Social Support Questionnaire (FSSQ) was used. This tool has been validated for use with the Spanish population (Bellón Saameño et al., 1996) and when self-administered or administered by an interviewer has reliability of 0.92 and 0.80 respectively. Factor analysis shows the existence of two dimensions of social support: confidant support (having people to talk to) and affective support (receiving care, love, and empathy). The questionnaire is deemed suitable for populations containing individuals of 15 years of age or above and comprises 11 items. Answers are scored on a Likert scale graded from 1 (much less than I would like) to 5 (as much as I like). The scores should vary between 11 and 55 points with a cut-off score of ≤32 indicating a perceived low level of social support with scores >32 considered normal. For the individual dimensions, this cut-off, is ≤15 for affective support and ≤18 for confidant support (Rodríguez y Flores, 2018).
Self-perceived general health was measured using the General Health Questionnaire-12 (GHQ-12) which comprises 12 items (Goldberg, 1988), and has been validated for use with the Spanish population (Muñoz Rodríguez, 1993; Lobo and Muñoz, 1996; Sánchez-López M del and Dresch, 2008). Answers are scored on a Likert scale graded from 0 to 3 and the total score is obtained from adding those of individual items. Higher scores indicate a greater self-perceived risk of poor mental health.
Statistical analysis
The coding and analysis of data were completed using the capture and analysis software program SPSS v.26. Descriptive analysis involved taking the medians of frequency, position, and dispersion as appropriate to the variable type (qualitative or quantitative). The Lilliefors corrected Kolmogorov-Smirnov test confirmed that the distributions of qualitative variables were non-normal thus these were analysed using non-parametric tests. Spearman's rho was calculated to assess the relationships between quantitative variables and the analysis of independent samples was completed using the Mann Whitney U test. In order to determine the psychometric indicators for our measurement instruments, we calculated the coefficients of reliability (Cronbach's Alpha)
Ethical considerations
All data used in this study was collected and analysed anonymously. Confidentiality was ensured as required under EU regulation 2016/679, of 27th April, concerning the General Protection of Personal Data and according to the Organic Law 3/2018 for the Protection of Personal Data and the guarantee of digital rights. In order to complete this study, an application (code number XX) was made to the XX Ethics Committee. Our application received a favourable review and was approved.
Results
The study sample comprised 178 women with a median age of 35.07±9.47. The majority of the sample population (73%) were aged between 30 and 40 years old, 12% were younger than 30 years old, and 14% were older than 40 years.
Table 1 shows the socio-demographic profile of the sample. It can be seen that 96.1% of women in our sample lived with a partner and 57.3% were primiparous at the time of the study. The majority of participants (77%) reported having higher education of some sort (beyond secondary school). Data gathered concerning the type of delivery and infant nutrition in the first six months of life showed that 77% of mothers had given birth vaginally, and 64% had chosen to breast feed exclusively. When asked about their return to employment, while 19.1% of our participants reported not having returned to the workplace at all, most participants (50.6%) had returned to work when their baby was between four and twelve months of age. The questionnaire also included several questions specifically designed for the current study concerning the formal support received by participants from professionals involved in their care during pregnancy and in the postpartum period. Only 11.8% of participants reported getting professional help up to 6 months after delivery.
Table 1.
Descriptive statistics: socio-demographic variables.
| Socio-demographic variables | % | N = 178 | |
|---|---|---|---|
| Family structure | Two parents/ partners with children | 96.1 | 171 |
| Single parent with children | 0.6 | 1 | |
| Parent with or without second parent or partner and other family members | 3.4 | 6 | |
|
Number of deliveries |
Primiparous | 57.3 | 102 |
| Multiparous | 42.7 | 76 | |
|
Educational level |
First stage of Secondary Education | 10.1 | 18 |
| Second stage of Secondary Education | 12.9 | 23 | |
| Higher Education | 77.0 | 137 | |
| Infant nutrition in the first 6 months | Breastfeeding | 64.0 | 114 |
| Artificial Lactation/ Mixed feeding (AL/MF) | 36.0 | 64 | |
|
Infant nutrition after the first 6 months |
Baby Led Weaning (BLW) | 18.0 | 32 |
| Mashes or purees | 32.0 | 57 | |
| Baby Led Introduction to solids (BLISS) | 50.0 | 89 | |
| Type of delivery | Vaginal | 77.0 | 137 |
| Abdominal | 23.0 | 41 | |
| Return to the workplace | Not returned | 19.1 | 34 |
| When baby was less than 6 weeks | 3.9 | 7 | |
| When baby was less than 4 months | 12.9 | 23 | |
| When baby was less than 12 months | 50.6 | 90 | |
| Formal support: antenatal care | Yes | 55.6 | 99 |
| No | 44.4 | 79 | |
| Formal support: 6 weeks post delivery | Yes | 60.1 | 107 |
| No | 39.9 | 71 | |
| Formal support: 6 months after delivery | Yes | 11.8 | 21 |
| No | 88.2 | 157 | |
The descriptive statistics for social support and general health variables are shown on Table 2 . Results for the total sample and various sub-groups (type of delivery and feeding in the first six months) have been separated out. The mean total score for the DUKE UNC-11 questionnaire for the whole sample was 37.84±9.47 while for the GHQ-12 this value was 16.06±6.89. The Mann Whitney U test demonstrates the existence of a statistically significant relationship between type of delivery and perceived levels of confidant support (p<.05) with primiparous women gaining higher scores for this form of support than multiparous women.
Table 2.
Descriptive statistics of the variables social support and general health for the total sample and mean difference between groups (type of delivery and feeding up to 6 months).
| Questionnaire | Sample | Min-Max | M±SD | Me | IQR | Asym | Kurtosis | α | p |
|---|---|---|---|---|---|---|---|---|---|
|
Confidant Support. DUKE-UNC-11 |
Total sample | 7–35 | 23.97±6.37 | 24 | 28 | −0.34 | −0.60 | .837 | – |
| Primiparous | 9–35 | 24.81±6.24 | 25 | 26 | −0.50 | −0.36 | .811 | .033* | |
| Multiparous | 7–35 | 22.84±6.41 | 22 | 28 | −0.13 | −0.68 | .841 | ||
| Breastfeeding | 7–35 | 24.22±6.52 | 25 | 28 | −0.53 | −0.46 | .839 | .327 | |
| AL/MF | 12–35 | 23.53±6.11 | 23 | 23 | .05 | −0.71 | .803 | ||
|
Affective Support. DUKE-UNC-11 |
Total sample | 4–20 | 13.86±3.87 | 14 | 16 | −0.60 | −0.37 | .795 | – |
| Primiparous | 4–20 | 13.98±3.93 | 15 | 16 | −0.73 | −0.93 | .801 | .552 | |
| Multiparous | 5–20 | 13.71±3.80 | 14 | 15 | −0.42 | −0.68 | .787 | ||
| Breastfeeding | 4–20 | 14.03±3.81 | 14 | 16 | −0.68 | −0.21 | .779 | .447 | |
| AL/MF | 5–20 | 13.58±3.99 | 14.5 | 15 | −0.47 | −0.53 | .799 | ||
|
Total. DUKE-UNC-11 |
Total sample | 14–55 | 37.84±9.47 | 39 | 41 | −0.44 | −0.44 | .880 | – |
| Primiparous | 14–55 | 38.79±9.27 | 40 | 41 | −0.62 | .46 | .869 | .112 | |
| Multiparous | 15–54 | 36.55±9.63 | 37 | 39 | −0.22 | −0.82 | .893 | ||
| Breastfeeding | 14–54 | 38.25±9.63 | 40.5 | 40 | −0.64 | −0.28 | .888 | .271 | |
| AL/MF | 17–55 | 37.11±9.19 | 37 | 38 | −0.07 | −0.53 | .865 | ||
| GHQ-12 | Total sample | 2–35 | 16.06±6.89 | 15 | 33 | .67 | .19 | .888 | – |
| Primiparous | 2–35 | 15.70±7.25 | 14 | 33 | .76 | .22 | .900 | .232 | |
| Multiparous | 4–34 | 16.54±6.38 | 16 | 30 | .57 | .26 | .868 | ||
| Breastfeeding | 4–35 | 15.65±7.32 | 14 | 31 | .83 | .24 | .906 | .096 | |
| AL/MF | 2–33 | 16.78±6.01 | 16 | 31 | .31 | .27 | .840 |
Note: Min-Max: Minimum-Maximun. M±SD: Mean ± Standard Deviation. Me: Median. Asym: Asymmetry. IQR: interquartile rango. DUKE-UNC-11: Social Support Questionnaire Duke. GHQ-12: General Health Questionnaire. p: U the Mann-Whitney test.
p < .05. AL/MF: Artificial Lactation/ Mixed Feeding α: Cronbach's Alpha.
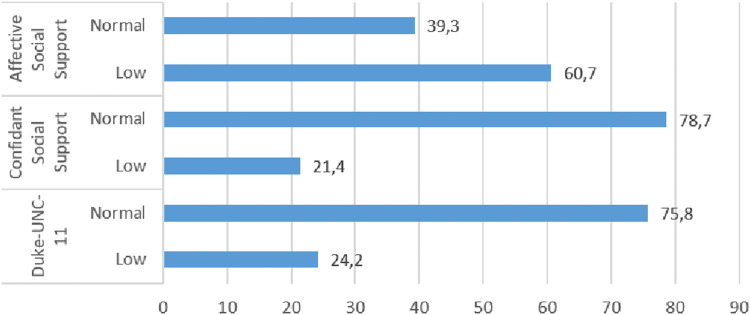
As can be seen in Fig. 1 , 75.8% of participants scored within the normal range in terms of social support compared to 24.2% who scored in the low range for this variable. Considering the separate dimensions of confidant support (having people to talk to) and affective support (receiving care, love, sympathy), here median scores were 23.97 and 13.87 respectively. In the case of confidant support, 78.7% of participants scored in the normal range, however, for affective support this percentage was lower (60.7%).
Fig. 1.
Functional Social Support Questionnaire (FSSQ) Duke-UNC-11.
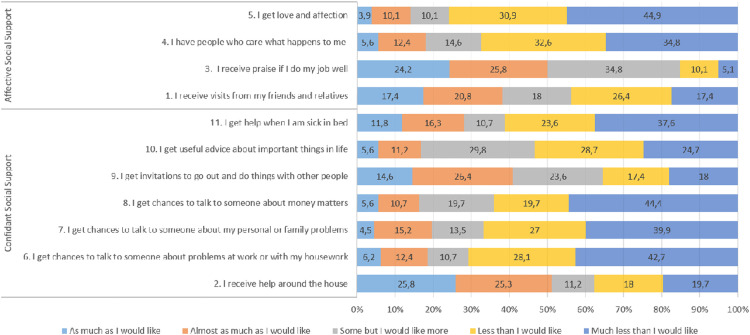
Fig. 2 shows the scores obtained for each of the items of the Duke-UNC-11 Functional Social Support Questionnaire (FSSQ). The results demonstrate that participants tended to score highly in the confidant support dimension to give high median scores for all items. However, two items stand out from the general trend: item 2 “I receive help around the house” and item 9 “I get invitations to go out and do things with other people” which showed much higher proportions of low scores. Similarly, in the affective support dimension, median scores are high for all items except item 3 “I receive praise if I do my job well” for which the median score is low, and the most common score was 3.
Fig. 2.
Items Functional Social Support Questionnaire (FSSQ) Duke-UNC-11.
Results for the items on the GHQ-12 are shown in Fig. 3 . Intermediate scores dominate here apart from in items 10 and 11 where the lowest score is the most frequent response. These items correspond to the questions, respectively: “Have you lost confidence in yourself?” and “Have you thought that you are a person worthless person?”.
Fig. 3.
Items General Health Questionnaire (GHQ 12).
The correlations between the study's key variables are shown in Table 3 and these confirm that social support is significantly related to general health. It was found that confidant support and affective support both have an inversely proportional relationship with self-perceived risk of poor mental health and these relationships are statistically significant: in the case of each dimension, rho values were, respectively −0.420 (p<.01) and −0.338 (p<.01). The higher the perceived degree of social support, the lower the self-perceived risk of poor mental health and vice versa.
Table 3.
Spearman inter-scale correlations between Duke-UNC-11 and GHQ-12.
|
DUKE-UNC-11 |
|||||
|---|---|---|---|---|---|
| Confidant Support | Affective Support | Total | |||
| DUKE-UNC-11 | Confidant Support | Spearman's Rho | 1 | ||
| Sig. (bilateral) | |||||
| Affective Support | Spearman's Rho | .671⁎⁎ | 1 | ||
| Sig. (bilateral) | .000 | ||||
| Total | Spearman's Rho | .954⁎⁎ | .856⁎⁎ | 1 | |
| Sig. (bilateral) | .000 | .000 | |||
| GHQ-12 | Total | Spearman's Rho | −0.467⁎⁎ | −0.408⁎⁎ | −0.482⁎⁎ |
| Sig. (bilateral) | .000 | .000 | .000 | ||
p <0.01.
Discussion
This study took a sample of women who became mothers during the COVID-19 pandemic and considered relationships between several socio-demographic variables as well as those of social support and self-perceived general health. Among the socio-demographic variables studied, infant nutrition stands out with 64% (N = 114) of mothers reporting exclusive breastfeeding in the first six months. Comparing this result to other studies concerning breastfeeding rates in Spain before the COVID-19 pandemic, the rates found in this work are high. For example, in a cohort of women in Gipuzkoa (Basque Country), Oribe et al. (Oribe et al., 2015) found that only 15.4% of mothers in their study had breastfed exclusively for the first six months while Rodríguez-Pérez et al. (Rodríguez-Pérez et al., 2017) researching breastfeeding rates among women in Vigo (Galicia) reported rates of 50.28%. Finally, a more recent study by Ramiro González et al. (2018) which used a corpus of women living in the Community of Madrid, found that only 25.4% were breastfeeding at 6 months. That our study shows high rates of breastfeeding during the period of the pandemic suggests that difficulties in accessing professional help with lactation described by authors such as Ceulemans et al. (Ceulemans et al., 2020) and Brown & Shenker (Brown and Shenker, 2021) do not appear to have had an impact in our investigation. In agreement with these authors, we believe that the COVID-19 lockdown may have had a positive effect on infant nutrition by facilitating situations that favor breastfeeding such as spending more time with the baby, experiencing fewer interruptions, and having greater protection from unwanted opinions. A further explanation for our results may lie in the fact that mothers vaccinated against SARS CoV 2 virus pass antibodies to their infants via their milk (Golan et al., 2021; Lechosa-Muñiz et al., 2021), providing an additional motivation for mothers to breastfeed in the first place and to continue breastfeeding for longer. However, more research is required to explore this hypothesis. Indeed, our results also show our sample comprised a high proportion of mothers living with partners (96.1%), and it has been shown that mothers with conjugal support tend to breastfeed for longer (Vieira E de et al., 2018) and this factor alone may account for the high rates of breastfeeding found in our study.
A study by Feligreras-Alcalá et al. (Feligreras-Alcalá et al., 2020) examined perceived levels of social support in Spain before the COVID-19 pandemic using the same questionnaire as the present work. Comparing the results of this study with our own, we see a reduction in total score from 47.50 to 37.84 demonstrating that perceptions of social support in general were lowered during the pandemic. This may have been due to the restrictions imposed across Spain aimed at controlling the spread of the infection such as social isolation, and limitations on travel. To appreciate the full extent of the impact of these measures we must also take into account the fact that being female and being in a situation that increases vulnerability are both risk factors for depression. Added to this, the findings of other work show that the pandemic also saw increased levels of social upheaval and anxiety, both of which affected women disproportionately (Parrado-Gonzalez and León-Jaruego, 2020). Furthermore, in our work, questions relating to help around the home, being invited to go out, or receiving praise for good work are those which received among the lowest scores demonstrating that there are specific areas of women's experience of motherhood that require greater attention.
The GHQ-12 median score for our sample was 16.06 where scores equal to or above 16 are associated with low self-perceived general health (García-Viniegras, 1999), which is indicative of a high risk of mental health problems among participants in this study. The median score found in the present study is also elevated compared to that found in other similar work. For instance, using a Dutch version of the GHQ-12, Van Bussel et al. (Van Bussel et al., 2006) evaluated self-perceived mental health in a group of at different times during the postpartum period and obtained values of 12.09 and 11.16 at, respectively, four and six months after giving birth. In contrast, our findings concerning the median scores obtained for each item on the GHQ-12 do coincide with those of other authors, for example, as in our investigation, Gómez-Salgado et al. (Gómez-Salgado et al., 2020) reported the lowest scores for items related to self-confidence and self-esteem. It is well known that the pandemic had a significant mental health impact on mothers with children between 0 and 12 months, specifically, causing increased anxiety and stress, and feelings of loneliness and isolation (Ollivier et al., 2021). Our study tends to confirm the poor mental health outcomes of lockdown and the social isolation caused by the COVID-19 outbreak, however, more research into this phenomenon is required to deepen our understanding.
Comparisons between sample subgroups showed that being a first-time mother was related to higher levels of confidant support, that is, these mothers reported having more people in their immediate environment who were able to provide them with information, advice, and guidance. In a phenomenological study of psycho-adaptive changes experienced by first-time mothers Korukcu (Korukcu, 2020) noted how these women adapted their values, personalities, time management, and their social lives in response to motherhood. Thus, it would seem that becoming a mother for the first time incentivises women to search for support and suggests there is perhaps more awareness that such mothers require this support. Our analysis didn't show any differences between a mother's choice of infant nutrition before six months and their reported levels of social support or self-perceived mental health. However, other studies do show the existence of a significant relationship between mothers choosing to breastfeed and their level of social support with high levels tending to increase the length of time breastfeeding continues and its exclusivity (McFadden et al., 2017).
Correlation analysis revealed a statistically significant linear, inverse relationship between confidant support levels and mental health. This suggests that during the postpartum period, women who can count on the support of others to talk about their issues, enjoy better mental health than those who cannot. A similarly significant inverse relationship was also found between affective support and mental health, that is, self-perceived mental health among participants in this study was significantly better for those women living in an environment of empathy and trust. These results agree with findings reported in other recent studies that show an important relationship between mental health and social support during the postpartum period. In this regard, the findings of Li et al. (Li et al., 2017) demonstrate that women scoring highly for social support in the fourth week after giving birth are significantly less likely to suffer from postnatal depression than low scorers. Webster et al. (Webster et al., 2011) also studied the impact of social support on postnatal depression and found a similar, strong correlation between the two variables. In their investigation, they noted that women with low levels of social support had more depressive symptoms and the highest propensity to develop postnatal depression; this was especially true for women with little support from other family members or a partner.
Several limitations placed on the scope of this work have resulted in potential weaknesses. One of these is that, due to the exclusion of mothers with children under six months at the time of the investigation, there were very few mothers of babies this age in the study. Thus, results cannot be generalised to this population. The same consideration has also limited the assessment of social support received by mothers in the first stages of breastfeeding. The interpretation of the findings presented here should take into account all these limitations.
Conclusion
The present study describes the relationship between social support (confidant and affective) and mental health in women who had children during the pandemic. Taken together, our findings indicate that the mental health of mothers is sensitive to and vulnerable to social changes, in this case, those that occurred as a result of the COVID-19 outbreak. Healthcare professionals need to be aware of this situation, both in terms of acknowledging the degree of influence social restrictions can have on maternal mental health and indeed how such restrictions can cause health problems in this population. In this way, these professionals should take steps to prevent psychological trauma and its complications. Likewise, health authorities need to improve existing protocols and put in place new ones where necessary, that properly address the needs of women in the months after they have given birth. The pandemic has highlighted pre-existing deficits in the support women can expect in the postpartum months and it is important they receive more rounded and extended care that is not limited only to the first six weeks after giving birth.
After a thorough evaluation of all our findings, we suggest there needs to be greater awareness of, and higher visibility given to the impact of social support in the first year of motherhood. This is a time when new mothers are adapting to their new role and the demands of the new-born, and this is a significant challenge both personally and to their other relationships which requires active support from those around them. The current model for mother and baby health care support is based solely on clinical needs, particularly physical recuperation, and gives little importance to the experience of motherhood. From the new mother's point of view there is a lack of support structures, both socially and in terms of education, that would empower and sustain them through this period of life, and which could improve their mental health and enable them to better adapt to their new situation.
Author contributions
Alonso Titos, T: Conceptualization and Formal Analysis. Arias-Ramos, N: Data curation, Writing-Original draft preparation. Valle-Barrio, V: Methodology and Validation. Marqués-Sánchez, P : Supervision. García-Fernández, R: Investigation and Visualization. Liébana-Presa, C: Writing- Reviewing and Editing.
Ethical approval
Ethical approval was obtained from the León University Ethics Committee (code number ETICA-ULE-050–2021). Our application received a favourable review and was approved on January 10, 2022.
Funding sources
This work has not received any type of funding.
Declaration of Competing Interest
There are no conflict of interests.
Acknowledgements
The authors would like to thank the mothers of the infants born during COVID-19 who agreed to take part in this study.
References
- Bellón Saameño J.A., Delgado Sánchez A., Luna del Castillo J., de D., Lardelli Claret P. Validez y fiabilidad del cuestionario de apoyo social funcional Duke-UNC-11. Aten. Primaria. 1996;18(4):153–163. https://www.elsevier.es/es-revista-atencion-primaria-27-articulo-validez-fiabilidad-del-cuestionario-apoyo-14325 Available from. [PubMed] [Google Scholar]
- Brown A., Shenker N. Experiences of breastfeeding during COVID-19: lessons for future practical and emotional support. Matern Child Nutr [Internet]. 2021;17. Available from: https://doi.org/10.1111/mcn.13088 [DOI] [PMC free article] [PubMed]
- Ceulemans M., Verbakel J.Y., Van Calsteren K, Eerdekens A., Allegaert K., Foulon V. SARS-CoV-2 Infections and Impact of the COVID-19 Pandemic in Pregnancy and Breastfeeding: results from an Observational Study in Primary Care in Belgium. Int. J. Environ. Res. Public Health. 2020;17:6766. doi: 10.3390/ijerph17186766. www.mdpi.com/journal/ijerph Available from. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Contreras-García Y., Sobarzo Rodríguez P., Manríquez-Vidal C. Characterization of perceived social support during postpartum and the presence of maternal depression. Revista Cubana de Obstetricia y Ginecología [Internet] 2017;43(1) http://scielo.sld.cuhttp//scielo.sld.cu Available from. [Google Scholar]
- Coxon K., Turienzo C.F., Kweekel L., Goodarzi B., Brigante L., Simon A., et al. The impact of the coronavirus (COVID-19) pandemic on maternity care in Europe. Midwifery. 2020;88 doi: 10.1016/j.midw.2020.102779. Sep. [DOI] [PMC free article] [PubMed] [Google Scholar]
- DeYoung S.E., Mangum M. Pregnancy, birthing, and postpartum experiences during COVID-19 in the United States. Front. Sociol. 2021;6 doi: 10.3389/fsoc.2021.611212. www.frontiersin.org Available from. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Feligreras-Alcalá D., Frías-Osuna A., Del-Pino-Casado R. Personal and family resources related to depressive and anxiety symptoms in women during Puerperium. Int. J. Environ. Res. Public Health. 2020;17 doi: 10.3390/ijerph17145230. www.mdpi.com/journal/ijerph Available from. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gómez-Salgado J., Andrés-Villas M., Domínguez-Salas S., Díaz-Milanés D., Ruiz-Frutos C. Related health factors of psychological distress during the COVID-19 pandemic in Spain. Int. J. Environ. Res. 2020;17(11):3947. doi: 10.3390/ijerph17113947. Jun 2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gaino L.V., de A.L.Y., de O.J.L., Nievas A.F., Saint-Arnault D., de S.J. O papel do apoio social no adoecimento psíquico de mulheres. Rev. Lat. Am. Enfermagem. 2019:27. doi: 10.1590/1518-8345.2877.3157. [DOI] [PMC free article] [PubMed] [Google Scholar]
- García-Viniegras C.R. Manual para la utilización del cuestionario de Salud General de Goldberg. Adaptación cubana. Rev. Cubana Med. Gen. Integr. 1999;15(1):88–97. [Google Scholar]
- Golan Y., Prahl M., Cassidy A.G., Gay C., Wu A.H.B., Jigmeddagva U., et al. COVID-19 mRNA vaccination in lactation: assessment of adverse events and vaccine related antibodies in mother-infant dyads. Front. Immunol. 2021;12 doi: 10.3389/fimmu.2021.777103. Nov 3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Goldberg D. A user's guide to the General Health Questionnaire. NFER-NELSON; 1988. 129 p.
- Jing Y., Run-Qian L., Hao-Ran W., Hao-Ran C., Ya-Bin L., Yang G., et al. Potential influence of COVID-19/ACE2 on the female reproductive system. Mol. Hum. Reprod. 2020;26(6):367–373. doi: 10.1093/molehr/gaaa030. Jun 1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Khoury J.E., Atkinson L., Bennett T., Jack S.M., Gonzalez A. COVID-19 and mental health during pregnancy: the importance of cognitive appraisal and social support. J. Affect. Disord. 2021;282:1161–1169. doi: 10.1016/j.jad.2021.01.027. Mar 1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Korukcu O. Psycho-adaptive changes and psychological growth after childbirth in primiparous women. Perspect. Psychiatr. Care. 2020;56(1):213–221. doi: 10.1111/ppc.12413. Jan 21. [DOI] [PubMed] [Google Scholar]
- Kotlar B., Gerson E., Petrillo S., Langer A., Tiemeier H. The impact of the COVID-19 pandemic on maternal and perinatal health: a scoping review. Reproductive Health. BioMed Central Ltd. 2021;18 doi: 10.1186/s12978-021-01070-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kummer L., Duke N., Davis L., Borowsky I. Association of social and community factors with u.s. breastfeeding outcomes. Breastfeed. Med. 2020;15(10):646–654. doi: 10.1089/bfm.2020.0083. Oct 1. [DOI] [PubMed] [Google Scholar]
- Lebel C., MacKinnon A., Bagshawe M., Tomfohr-Madsen L., Giesbrecht G. Elevated depression and anxiety symptoms among pregnant individuals during the COVID-19 pandemic. J. Affect. Disord. 2020;277:5–13. doi: 10.1016/j.jad.2020.07.126. Dec 1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lechosa-Muñiz C., Paz-Zulueta M., Mendez-Legaza J.M., Irure-Ventura J., González R.C., Montes J.C., et al. Induction of sars-cov-2-specific igg and iga in serum and milk with different sars-cov-2 vaccines in breastfeeding women: a cross-sectional study in northern spain. Int. J. Environ. Res. 2021;18(16) doi: 10.3390/ijerph18168831. Aug 2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Li Y., Long Z., Cao D., Cao F. Social support and depression across the perinatal period: a longitudinal study. J. Clin. Nurs. 2017;26(17–18):2776–2783. doi: 10.1111/jocn.13817. Sep 1. [DOI] [PubMed] [Google Scholar]
- Liang H., Acharya G. Novel corona virus disease (COVID-19) in pregnancy: what clinical recommendations to follow? Acta Obstet. Gynecol. Scand. 2020;99(4):439–442. doi: 10.1111/aogs.13836. Apr 1. [DOI] [PubMed] [Google Scholar]
- Lobo A., Muñoz P. Cuestionario de salud general GHQ (General Heath Questionnaire). Guía Para El Usuario De Las Distintas Versiones En Lengua Española Validadas. Masson. Barcelona. Masson. Masson; 1996.
- Maleki-Saghooni N., Amel Barez M., Karimi F.Z. Investigation of the relationship between social support and breastfeeding self-efficacy in primiparous breastfeeding mothers. J. Matern. Fetal Neonatal Med. 2020;33(18):3097–3102. doi: 10.1080/14767058.2019.1568986. Sep 16. [DOI] [PubMed] [Google Scholar]
- McFadden A., Gavine A., Renfrew M.J., Wade A., Buchanan P., Taylor J.L., et al. Support for healthy breastfeeding mothers with healthy term babies. Cochrane Database Syst. Rev. 2017;2 doi: 10.1002/14651858.CD001141.pub5. John Wiley and Sons Ltd. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Molgora S., Accordini M. Motherhood in the time of coronavirus: the impact of the pandemic emergency on expectant and postpartum women's psychological well-being. Front. Psychol. 2020;11 doi: 10.3389/fpsyg.2020.567155. Oct 26. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Muñoz Rodríguez P.E. Estudio de validación predictiva del General Health Questionnaire (GHQ) en población general urbana (expediente 93/0905) Anales del Fondo de Investigación Sanitaria. 1993 [Google Scholar]
- Muñoz-Bermejo L., Adsuar J.C., Postigo-Mota S., Casado-Verdejo I., de Melo-Tavares C.M., Garcia-Gordillo M.Á., et al. Relationship of perceived social support with mental health in older caregivers. Int. J. Environ. Res. 2020;17(11) doi: 10.3390/ijerph17113886. Jun 1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ollivier R., Aston D.M., Price D.S., Sim D.M., Benoit D.B., Joy D.P., et al. Mental health & parental concerns during COVID-19: the experiences of new mothers amidst social isolation. Midwifery. 2021:94. doi: 10.1016/j.midw.2020.102902. Mar 1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Oribe M., Lertxundi A., Basterrechea M., Begiristain H., Santa Marina L., Villar M., et al. Prevalencia y factores asociados con la duración de la lactancia materna exclusiva durante los 6 primeros meses en la cohorte INMA de Guipúzcoa. Gac. Sanit. 2015;29(1):4–9. doi: 10.1016/j.gaceta.2014.08.002. Jan. [DOI] [PubMed] [Google Scholar]
- Ostacoli L., Cosma S., Bevilacqua F., Berchialla P., Bovetti M., Carosso A.R., et al. Psychosocial factors associated with postpartum psychological distress during the Covid-19 pandemic: a cross-sectional study. BMC Pregnancy Childbirth. 2020;20(1) doi: 10.1186/s12884-020-03399-5. Dec 1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Parrado-Gonzalez A., León-Jaruego J.C. COVID-19: factores asociados al malestar emocional y morbilidad psíquica en población española. Rev. Esp Salud Publica. 2020:94. Jul 8. [PMC free article] [PubMed] [Google Scholar]
- Peter P.J., de Mola C.L., de Matos M.B., Coelho F.M., Pinheiro K.A., da Silva R.A., et al. Association between perceived social support and anxiety in pregnant adolescents. Braz. J. Psychiatry. 2017;39(1):21–27. doi: 10.1590/1516-4446-2015-1806. Jan 1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rodríguez Leis P., Flores Gallegos R. Relación entre apoyo social, estrés, ansiedad y depresión durante el embarazo en una población mexicana. Ansiedad y Estrés. 2018;24(2–3):67–72. Jul. [Google Scholar]
- Rodríguez-Pérez M.J., Álvarez-Vázquez E., Medina-Pomares J., Velicia-Peñas C., Cal-Conde A., Goicoechea-Castaño A., et al. Prevalencia de lactanciamaterna en el Área Sanitaria de Vigo. Galicia. Rev esp salud Pública. 2017;91(9) [PubMed] [Google Scholar]
- Romero-Gonzalez B., Puertas-Gonzalez J.A., Mariño-Narvaez C., Peralta-Ramirez M.I. Variables del confinamiento por COVID-19 predictoras de sintomatología ansiosa y depresiva en mujeres embarazadas. Medicina Clínica. 2021;156(4):172–176. doi: 10.1016/j.medcli.2020.10.002. Feb. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sánchez-López M del P., Dresch V. El Cuestionario de Salud General de 12 ítems (GHQ-12): fiabilidad. validez externa y estructura factorial en la población española. 2008;20(4):839–843. 20(4),. Psicothema. [Google Scholar]
- Sehhatie F.S., Mirghafourvand M., Havizari S. Effect of prenatal counseling on exclusive breastfeeding frequency and infant weight gain in mothers with previous unsuccessful breastfeeding: a randomized controlled clinical trial. J. Maternal-Fetal Neonatal Med. 2020;33(21):3571–3578. doi: 10.1080/14767058.2019.1579191. Nov 1. [DOI] [PubMed] [Google Scholar]
- Snyder K., Worlton G. Social support during COVID-19: perspectives of breastfeeding mothers. Breastfeed. Med. 2021;16(1):39–45. doi: 10.1089/bfm.2020.0200. Jan 1. [DOI] [PubMed] [Google Scholar]
- Spinola O., Liotti M., Speranza A.M., Tambelli R. Effects of COVID-19 epidemic lockdown on postpartum depressive symptoms in a sample of Italian mothers. Front. Psychiatry. 2020;11 doi: 10.3389/fpsyt.2020.589916. Nov 17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Stumpfe F.M., Titzmann A., Schneider M.O., Stelzl P., Kehl S., Fasching P.A., et al. SARS-CoV-2 infection in pregnancy - a review of the current literature and possible impact on maternal and neonatal outcome. Geburtshilfe Frauenheilkd. 2020;80(4):380–390. doi: 10.1055/a-1134-5951. Apr 1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Szkody E., McKinney C. Appraisal and social support as moderators between stress and physical and psychological quality of life. Stress Health. 2020;36(5):586–595. doi: 10.1002/smi.2957. Dec 1. [DOI] [PubMed] [Google Scholar]
- Tani F., Castagna V. Maternal social support, quality of birth experience, and post-partum depression in primiparous women. J. Maternal-Fetal Neonatal Med. 2017;30(6):689–692. doi: 10.1080/14767058.2016.1182980. Mar 19. [DOI] [PubMed] [Google Scholar]
- Vaezi A., Soojoodi F., Banihashemi A.T., Nojomi M. The association between social support and postpartum depression in women: a cross sectional study. Women Birth. 2019;32(2):e238–e242. doi: 10.1016/j.wombi.2018.07.014. Apr 1. [DOI] [PubMed] [Google Scholar]
- Valdés-Bango M., Meler E., Cobo T., Hernández S., Caballero A., García F., et al. A clinical management protocol for COVID-19 infection in pregnant women. Clin. Invest. Ginecol. Obstet. 2020;47:118–127. doi: 10.1016/j.gine.2020.06.014. Elsevier Doyma. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Van Bussel J.C.H., Spitz B., Demyttenaere K. Women's mental health before, during, and after pregnancy: a population-based controlled cohort study. Birth. 2006;33(4):297–302. doi: 10.1111/j.1523-536X.2006.00122.x. Dec. [DOI] [PubMed] [Google Scholar]
- Vieira E de S., Caldeira N.T., Eugênio D.S., Di Lucca M.M., Silva I.A. Breastfeeding self-efficacy and postpartum depression: a cohort study. Rev. Lat. Am. Enfermagem. 2018;26 doi: 10.1590/1518-8345.2110.3035. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Webster J., Nicholas C., Velacott C., Cridland N., Fawcett L. Quality of life and depression following childbirth: impact of social support. Midwifery. 2011;27(5):745–749. doi: 10.1016/j.midw.2010.05.014. Oct. [DOI] [PubMed] [Google Scholar]
- Zamani P., Ziaie T., Lakeh N.M., Leili E.K. The correlation between perceived social support and childbirth experience in pregnant women. Midwifery. 2019;75:146–151. doi: 10.1016/j.midw.2019.05.002. Aug 1. [DOI] [PubMed] [Google Scholar]
- Zhou J., Havens K.L., Starnes C.P., Pickering T.A., Brito N.H., Hendrix C.L., et al. Changes in social support of pregnant and postnatal mothers during the COVID-19 pandemic. Midwifery. 2021:103. doi: 10.1016/j.midw.2021.103162. Dec 1. [DOI] [PMC free article] [PubMed] [Google Scholar]