Abstract
Background
Haemorrhoidectomy is often complicated by significant post-operative pain, to which spasm of the internal anal sphincter is thought to be a contributing factor. This study appraises the evidence behind interventions aimed at lowering sphincter spasm to relieve post-haemorrhoidectomy pain.
Methods
A Preferred Reporting Items for Systematic Reviews and Meta-analyses compliant systematic review was conducted. Medline, EMBASE, and CENTRAL databases were systematically searched. All RCTs which compared interventions targeting the internal anal sphincter to relieve pain post excisional haemorrhoidectomy were included. The primary outcome measure was pain on the visual analogue scale.
Results
Of the initial 10,221 search results, 39 articles were included in a qualitative synthesis, and 33 studies were included in a meta-analysis. Topical glyceryl trinitrate (GTN) reduced pain on day 7 (7 studies, 485 participants), with a mean difference and 95% confidence interval (MD, 95% CI) of −1.34 (−2.31; −0.37), I2 = 91%. Diltiazem reduced pain on day 3 on the VAS, and the MD was −2.75 (−398; −1.51) shown in five studies (n = 227). Botulinum toxin reduced pain on day 7, in four studies with 178 participants, MD −1.43 (−2.50; −0.35) I2 = 62%. The addition of Lateral Internal Sphincterotomy to haemorrhoidectomy reduced pain on day 2 in three studies with 275 participants, MD of −2.13 (−3.49; −0.77) I2 = 92%. The results were limited by high heterogeneity and risk of bias.
Conclusion
Evidence suggests that lateral sphincterotomy, administration of botulinum toxin and the application of topical diltiazem or GTN can reduce post-operative pain after haemorrhoidectomy. Lateral sphincterotomy should not be routinely used due to the risk of incontinence.
Supplementary Information
The online version contains supplementary material available at 10.1007/s00268-022-06807-3.
Introduction
Haemorrhoids are common and can significantly affect quality of life [1]. Excisional haemorrhoidectomy remains the most effective procedure with the lowest recurrence for prolapsing haemorrhoids [2]. In the past 2 decades, considerable research aimed to improve post-operative pain after haemorrhoidectomy [3, 4]. After excisional haemorrhoidectomy, patients develop linear wounds that extend up to the anorectal ring at the site of the vascular pedicle [5]. The appearance of these wounds is similar to that of a fissure-in-ano, where hypertonia of the internal anal sphincter has been associated with anal fissure [6, 7]. It is believed that spasm of hypertonia of the internal sphincter is responsible for the discomfort after haemorrhoidectomy, especially during defecation. Mechanisms contributing to pain and hypertonia include incarceration of the smooth muscle fibres and mucosa at the transfixed vascular pedicle, and epithelial loss of the canal [2, 5].
Current research suggests the use of multimodal pain relief protocols after ambulatory anorectal surgery can reduce pain and opiate usage [4, 8]. Such protocols include opiate sparing protocols as well as adjunctive treatments [8]. In particular, specific to haemorrhoidectomy, targeting sphincter spasm has been proposed to reduce post-operative pain [9]. It is hypothesised that spasm of the internal anal sphincter contributes to significant pain after haemorrhoidectomy. Numerous interventions trialled have investigated this hypothesis from utilising anal stretch to lateral sphincterotomy and pharmacological treatments [10–12].
This systematic review and meta-analysis summarises and appraises evidence behind methods of pain relief focusing on the reduction of sphincter spasm as a mechanism of pain. The Grading of Recommendations Assessment Developments (GRADE) approach is used to appraise the certainty of evidence [13]. The results of this review can be used to develop clinical recommendations and provide future research direction.
Methods
A systematic review and meta-analysis was conducted according the preferred reporting of systematic reviews and meta-analyses (PRISMA) guidelines [14]. The study was registered with PROSPERO-registration: CRD42021288125. The original registration was subsequently changed to restrict studies targeting sphincter spasm only.
Data sources
A comprehensive literature search was carried out from inception until January 2022, using relevant medical subject headings and keywords. The search terms incorporated the following themes: 1. pain relief/sphincter spasm/analgesia, and 2. haemorrhoidectomy/haemorrhoids. Results were restricted to the English language. Medline, Embase and CENTRAL were searched to identify randomised clinical trials comparing techniques to reduce sphincter spasm to improve post-haemorrhoidectomy pain. The references of the identified trials were also searched to find additional trials for inclusion. Only full-texts available in English were selected for inclusion, and this did not impact on the number of final included texts. The full search strategy is documented in Online Appendix 1, and the protocol is outlined in Online Appendix 2.
Eligibility criteria
Inclusion criteria
All RCTs that investigated treatments aimed at reducing pain by the mechanism of reducing sphincter spasm after haemorrhoidectomy were included. Examples included, but were not limited to topical medical therapy or procedural interventions or techniques such as botulinum toxin administration or sphincterotomy.
Exclusion criteria
Studies that did not compare an intervention aiming to reduce sphincter spasm were excluded. Studies that compared different techniques of haemorrhoidectomy were excluded, and studies that were non-randomised or did not involve haemorrhoidectomy were excluded.
Selection process
A multi-stage study selection process was conducted, starting with title and abstract screening followed by full-text review of eligible studies. Two independent reviewers (J.J and H.U) screened the search results against the inclusion and exclusion criteria at all stages. If there were disagreements, consensus was reached by discussion with the senior author.
Data collection process
Data were independently extracted according to a predefined form in Microsoft Excel (Redmond, Washington, USA) by two authors (H.U., P.B.), followed by validation of all extracted data by the first author. Data in a graphical format were transformed into a numerical format using WebPlotDigitizer v4.5 (Ankit Rohatgi, Pacifica, California, USA). Data were accessed from the published manuscript, and further data were not obtained from study investigators.
Data items
Study and participants characteristics were extracted according to a predefined form. The primary outcome of interest was pain measured on a 0–10 cm visual analogue scale (VAS) across the most frequently reported post-operative days. Time points with sufficient measurements taken were pooled in a meta-analysis. If pain was measured using a categorical method this was synthesised using a risk ratio as appropriate. The secondary outcomes included incidence of headache, incontinence, and measurements of wound healing.
Meta-analysis
The results were synthesised using a meta-analysis if outcomes measured were deemed similar and combinable. Continuous outcomes were synthesised using mean difference (MD) along with 95% confidence intervals. If the mean and standard deviation (SD) for continuous outcomes were unavailable, these were estimated using median, range, or inter-quartile range using the methods of Wan and Luo et al. [15] Categorical outcomes were synthesised using Risk Ratio, with the risk of outcome in having the intervention versus without the intervention. Meta-analysis was conducted using the package ‘meta’ in R [16, 17]. A random effects meta-analysis was conducted as the default method, using the Mantel Haenszel method for pooling, with the results displayed as a forest plot. Continuity correction was given as 0.5 for all zero cell frequencies in categorical outcomes. Heterogeneity was measured using the I-squared statistic. Publication bias was evaluated using a funnel plot if there were ten or more studies. A sensitivity analysis was conducted on type of excisional procedure, based on open or closed haemorrhoidectomy.
Risk of bias
The risk of bias was assessed by two study authors (J.J., P.B.) using the Cochrane Risk of bias 2.0 tool with the following outcome domains: Risk of bias from the randomisation process, deviations from intended interventions, missing outcome data, measurement of the outcome, and selection of the reported result [18].
Certainty of evidence
The certainty of evidence was assessed using the Grading of Recommendations Assessment Development and Evaluation (GRADE) approach [13]. Factors assessed include the risk of bias, precision of effect estimates, consistency of individual study results, directness of evidence, and publication or reporting biases. The GRADEpro software was used to deliver the final certainty of evidence rating [19]. Interpretation of GRADE certainty of evidence is outlined in Online Appendix 1.
Results
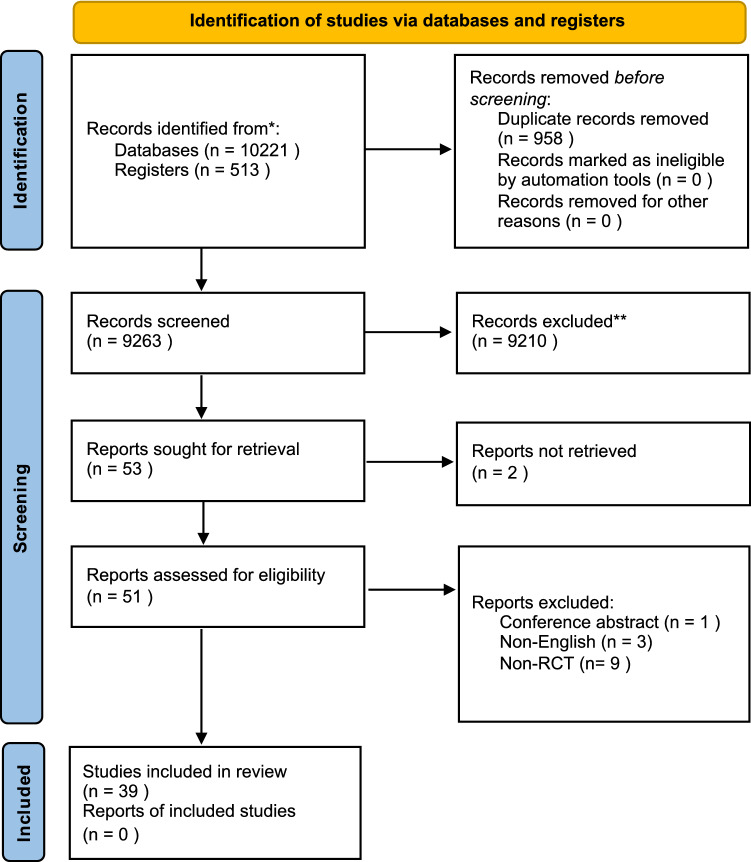
Of 10,224 initial search results, 704 were reviewed as abstracts, and 51 full-texts were reviewed for consideration. Following review of full-texts, 12 articles were excluded, leaving 39 articles included in a qualitative synthesis. A total of 33 studies with combinable outcomes were included in a quantitative synthesis. The PRISMA flow diagram is displayed in Fig. 1. The characteristics of included studies are displayed in Table 1. Figure 2 shows the forest plots for pain measured on the VAS for Glyceryl Trinitrate (GTN) and diltiazem. The remainder of figures for each meta-analysis is supplied in Online Appendix 1.
Fig. 1.
PRISMA diagram of included studies
Table 1.
Characteristics of included studies
| Study name | Year | Country | Journal | Total participants | Total per cent female | Mean age (SD) | Follow-up period (days) | Dose/duration/description of intervention | Haemorrhoidectomy technique | Prophylactic antibiotics on induction | Post-operative antibiotics | Adjunct pain relief | Local anaesthesia infiltration |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| GTN versus Placebo | |||||||||||||
| Asif | 2020 | Pakistan | Pakistan Journal of Medical and Health Sciences | 110 | 38 | 35 (12) | 14 | 0.2% GTN versus placebo for TDS 12 days | Open | n.r | n.r | n.r | n.r |
| Di Vita | 2004 | Italy | Annali Italiani di chirurgia | 30 | 43 | 38 (19) | 14 | 0.2% GTN TDS versus placebo | Open | n.r | Metronidazole 400 mg PO TDS for 1 week | Lactulose | n.r |
| Franceshilli | 2013 | Italy | International Journal of Colorectal disease | 203 | 38 | 49 (11) | 42 | 0.4% GTN TDS versus placebo for 6 weeks | Ligasure | 1 g Cefazolin and 500 mg metronidazole | Not mentioned | Ketorolac and laxatives | 0.75% Naropine 20mls |
| Hwang | 2013 | Korea | Diseases of the Colon & Rectum | 102 | 64 | 42 (11) | 21 | 0.2% GTN TDS versus placebo 14 days | Open with suture ligation | 2 g Cefazolin | 2 g Cefazolin for 4 days | Amfenac and laxatives | n.r |
| Karanlik | 2009 | Turkey | Diseases of the Colon & Rectum | 60 | 48 | 36 (11) | 42 | 0.2% GTN versus placebo | Closed with ligation | n.r | n.r | Paracetamol, naproxen, metamizole, laxatives | n.r |
| Khan | 2013 | Pakistan | International Journal of Surgery | 125 | 49 | 43 (9) | 42 | 0.2% GTN versus lidocaine versus 0.2% GTN + lidocaine TDS for 6 weeks | Open | n.r | n.r | Paracetamol, codeine sitz baths | n.r |
| Lashari | 2020 | Pakistan | Pakistan Journal of Medical and Health Sciences | 124 | 34 | 36 (11) | 21 | 0.2% GTN versus placebo TDS for 14 days | n.r | n.r | n.r | n.r | n.r |
| Mari | 2013 | Italy | Diseases of the Colon & Rectum | 41 | 32 | 49 (9) | 14 | 0.4% GTN ointment versus lidocaine gel for 14 days | Stapled Haemorrhoidopexy | n.r | n.r | Ketorolac and laxatives | n.r |
| Patti | 2005 | Italy | Chirurgia Italiana | 30 | 43 | 35 (17) | 14 | 0.2% GTN ointment | Open | n.r | Metronidazole 500 mg PO TDS 7 days | Diclofenac, laxatives | n.r |
| Soltany | 2009 | Iran | Surgery Journal Medwell Journals | 44 | 100 | 35 (13) | 28 | 0.2% GTN BD versus placebo | Open | n.r | n.r | Ibuprofen 400 mg TDS | n.r |
| Tan | 2006 | Singapore | British Journal of Surgery | 82 | 26 | 43 (11) | 42 | 0.2% GTN (Rectogesic) versus placebo | Open diathermy | n.r | n.r | Paracetamol, diclofenac, sitz baths | 0.25% Bupivicaine |
| Vahabi | 2019 | Iran | The Surgery Journal | 40 | n.r | n.r | 2 | 0.2% GTN versus placebo | Open | n.r | n.r | Laxatives | n.r |
| Wasvary | 2001 | USA | Diseases of the Colon & Rectum | 39 | 49 | 52 (n.r.) | 7 | 0.2% NTG ointment for 7 days versus placebo | Closed | n.r | n.r | Hydrocodone, paracetamol, NSAIDs, and laxative | No local anaesthesia |
| DILTIAZEM versus Placebo | |||||||||||||
| Abidi | 2021 | Pakistan | Journal Ayub Medical College | 80 | 34 | 39 (8) | 3 | 2% diltiazem gel TDS versus placebo | Open | n.r | Antibiotics | Oral analgesics, sitz baths | n.r |
| Amoli | 2011 | Iran | Colorectal Disease | 33 | 18 | 53 (16) | 7 | 2% diltiazem ointment versus Vaseline | Open with diathermy | n.r | Not mentioned | Paracetamol, codeine, pethidine and laxatives | n.r |
| Rodriguez-Wong | 2019 | Mexico | Revista de Gastroenterologia de Mexico | 52 | 48 | 48 (n.r.) | 42 | 2% diltiazem gel versus placebo | Closed with suture | n.r | Not mentioned | Ketorolac, laxatives and sitz baths | n.r |
| Rodriguez-Wong | 2016 | Mexico | Revista de Gastroenterologia de Mexico | 34 | 44 | 46 (n.r.) | 3 | 2% diltiazem gel TDS versus placebo | Closed | n.r | Not mentioned | Ketorolac and sitz baths | n.r |
| Silverman | 2005 | USA | Diseases of the Colon & Rectum | 18 | 61 | 45 (11) | 7 | 2% diltiazem versus Vaseline TDS | Closed | n.r | n.r | Hydrocodone and laxatives | n.r |
| Suchdev | 2014 | Pakistan | Pakistan Journal of Surgery | 80 | 18 | 39 (15) | 3 | 2% diltiazem TDS versus placebo | Open | n.r | Metronidazole 400 mg TDS 3 days | Diclofenac, stool softener and sitz baths | n.r |
| Sugimoto | 2013 | Japan | World Journal of Surgery | 62 | 58 | 63 (14) | 14 | 2% diltiazem gel TDS versus methylcellulose gel | Harmonic Scalpel, Closed with suture | n.r | n.r | Loxoprofen 60 mg TDS | n.r |
| Botulinum Toxin versus Placebo | |||||||||||||
| Alvandipour et al | 2021 | Iran | Journal of Research in Medical Sciences | 67 | 36 | n.r | 14 | Botox 40 IU intersphincteric bilateral | Open | None | None | Intravenous apotel and morphine PRN | n.r |
| Davies | 2003 | England | Diseases of the Colon & Rectum | 49 | 41 | 56 (12) | 7 | Botox 20 IU internal anal sphincter bilateral | Open with suture ligation | n.r | n.r | Codeine and paracetamol with laxatives | 0.25% Bupivicaine 20mls |
| Patti | 2005 | Italy | Diseases of the Colon & Rectum | 30 | 50 | 38 (16) | 7 | Botox 20 IU internal anal sphincter | Open-single suture fixation | Metronidazole on induction | Metronidazole 500 mg TDS 1 week | Nimesulide 100 mg | n.r |
| Singh | 2008 | England | Colorectal Disease | 32 | 25 | 53 (10) | 14 | Dysport 150 IU intersphincteric bilateral | Open with diathermy | n.r | Metronidazole 5 days | Paracetamol, NSAID, codeine | 0.5% Bupivicaine 20 ml |
| Sirikurnpiboon | 2020 | Thailand | Journal of the Anus, Rectum and Colon | 82 | 46 | 42 (13) | 180 | Botox 30 IU intersphincteric space | Closed | n.r | Metronidazole for 1 week | Paracetamol, diclofenac, norfloxacin | n.r |
| Lateral internal sphincterotomy versus none | |||||||||||||
| Butt | 2018 | Pakistan | Pakistan Journal of Medical and Health Sciences | 60 | 33 | 46 (8) | 14 | Sphincterotomy to left side open wound 1 cm to the dentate line | Open | Ceftriaxone 1 g metronidazole 500 mg × 3 doses | n.r | n.r | n.r |
| Chauhan | 2009 | India | Journal of Postgraduate Medicine | 102 | 31 | 48 (9) | 14 | Sphincterotomy to dentate line | Open | n.r | n.r | Tramadol and sitz baths | n.r |
| Das | 2013 | Malaysia | International Journal of Collaborative Research on Internal Medicine & Public Health | 50 | 24 | 90 | Sphincterotomy through haemorrhoidectomy wound up to 1 cm upwards of dentate line | Open | 2 g Cephalosporin and metronidazole × 3 doses | Total of 3 doses perioperatively | Laxatives and sitz baths | ||
| Galizia | 2000 | Italy | European Journal of Surgery | 42 | 48 | 41 (5) | n.r | Sphincterotomy up to dentate line | Open | n.r | n.r | n.r | n.r |
| Hosseini | 2007 | Iran | Archives of Iranian Medicine | 120 | 44 (14) | 14 | Cutting one third of the internal sphincter by cauterisation | n.r | n.r | n.r | n.r | Under local anaesthesia | |
| Kanellos | 2005 | Greece | World Journal of Surgery | 78 | 50 | 51 (13) | 7 | LIS up to the dentate line | Open | n.r | n.r | n.r | n.r |
| Khubchandani | 2002 | USA | Diseases of the Colon & Rectum | 42 | 48 | 52 (11) | n.r | Sphincterotomy not further specified | Closed | n.r | n.r | Paracetamol and oxycodone | n.r |
| Lu | 2013 | China | World Journal of Gastroenterology | 192 | 49 | 48 (n.r.) | n.r | Lower edge of the internal sphincter was divided and cut off at the interscalene in the 3 or 9 o’clock position | Open | 2 g Cephalosporin | n.r | n.r | n.r |
| Mathai | 1996 | Singapore | British Journal of Surgery | 33 | 45 | 40 (9) | 180 | Internal sphincterotomy in haemorrhoidectomy wound up to dentate line | Open | n.r | n.r | Ketoprofen and laxatives | n.r |
| Sushel | 2015 | Pakistan | J Liaquat Uni Med Health Sci | 116 | 34 | 42 (10) | 10 | Internal sphincter divided up to the dentate line through one of the haemorrhoidectomy wounds | Open | n.r | n.r | Sitz baths | n.r |
| Raza | 2013 | Pakistan | Journal of Rawalpindi Medical College | 108 | 36 | 43 (n.r.) | 28 | Sphincterotomy not further specified | Open | n.r | n.r | n.r | n.r |
| Vijayaraghavalu | 2021 | India | Cureus | 200 | 40 | 42 (11) | 720 | 1 cm lateral incision 3 o’clock | Open with suture fixation | n.r | Metronidazole for 5 days | Topical magnesium sulphate, sitz baths | n.r |
| Other | |||||||||||||
| Ho | 1998 | Singapore | British Journal of Surgery | 160 | 53 | 50 (12) | 70 | trimebutine 120 mg and Ruscogenins 10 mg (Proctolog) versus no intervention | Open diathermy | n.r | n.r | Ketoprofen, laxatives, sitz baths | n.r |
| Perrotti | 2010 | Italy | Canadian Journal of Surgery | 270 | 42 | 49 (13) | 14 | 0.3% nifedipine + 1.5% lidocaine ointment versus 1.5% lidocaine ointment | Open | n.r | n.r | n.r | n.r |
n.r. not reported, GTN glyceryl trinitrate, NTG nitroglycerin, LIS lateral internal sphincterotomy
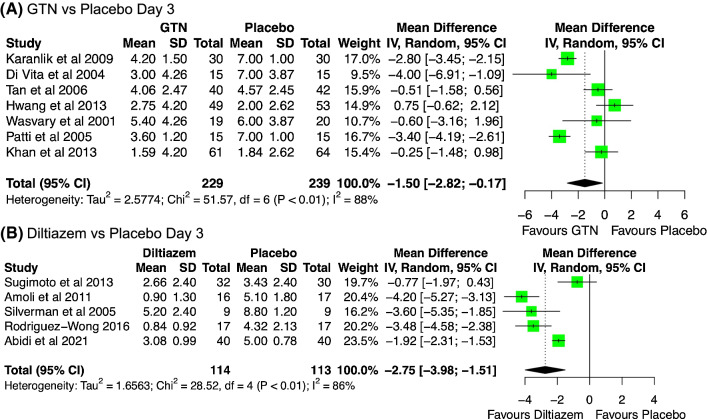
Fig. 2.
Forest plot of pain on the VAS for (A) GTN vs placebo on day 3, and (B) Diltiazem vs placebo on day 3
Topical glyceryl trinitrate (GTN)
Thirteen RCTs compared GTN against placebo [20–32]. Intervention groups were randomised to the application of topical GTN (0.2–0.4%) applied peri-anally to the haemorrhoidectomy wound two to three times daily.
Post-operative day 1
Nine studies with 549 participants reported pain measured on day 1 post-operation using the 0–10 VAS. Topical GTN significantly reduced post-operative pain compared to placebo. [MD: −1.03, 95% CI (−2.03, −0.023), p = 0.045]. Heterogeneity was significant, I2 = 91%. (Fig. 1, Online Appendix 1).
Post-operative day 2
Seven studies reported results on post-operative day 2. Topical GTN significantly reduced pain compared to placebo [MD: −2.06, 95% CI (−3.44; −0.67), p = 0.036], with significant heterogeneity, I2 = 90%. (Fig. 2, Online Appendix 1).
Post-operative day 3
Similarly for post-operation day 3, a significant difference was observed across seven studies and 468 participants [MD: −1.50, 95% CI (−2.82; −0.17), p = 0.027]. There was significant heterogeneity I2 = 88%. (Fig. 3, Online Appendix 1).
Post-operative day 7
Seven studies with 485 participants showed that pain was significantly reduced on day 7 post-operation, [MD: −1.34, 95% CI (−2.31; −0.37), p = 0.012] I2 = 91%. (Fig. 4, Online Appendix 1).
Wound healing at 3 weeks
Wound healing at 3 weeks was reported in three studies with 252 participants [23, 24, 30]. The relative risk (RR) was 1.73, 95% CI (1.26; 2.36) p = 0.01, I2 = 0%, suggesting that participants were 73% more likely to have wounds fully epithelialized at 3 weeks. Among the studies, a total of 47% of participants had fully epithelialized wounds at 3 weeks. (Fig. 5, Online Appendix 1).
Incidence of headache
Headache was reported in 10 studies and results of nine studies were synthesised in a meta-analysis involving 679 participants. A random effects model indicated GTN use was associated with a sixfold increase in the incidence of headache [RR = 6.11, 95% CI (2.11–17.70) p = 0.004], with low heterogeneity I2 = 15%. (Fig. 6, Online Appendix 1).
Analgesic use
Two studies did not report pain on standardised scale, but rather reported analgesic use [26, 29]. Analgesic use was not able to be compared between studies, as studies reported different types and modes of analgesia given. Only one study reported pain on defecation [21]. Among trials involving GTN, there were no studies of anal manometry.
Diltiazem
Seven studies evaluated the effect of topical diltiazem against placebo [33–39]. Intervention groups were randomised to the application of 2% topical diltiazem to the haemorrhoidectomy wound two to three times daily.
Post-operative day 1
Five studies with 227 participants show pain on the VAS was significantly reduced on post-operation day 1, [MD: −2.41, 95% CI (−3.71; −1.09) p < 0.001] with high heterogeneity, I2 = 84%. (Fig. 7, Online Appendix 1).
Post-operative day 2
Similarly, for day 2, pain reduction was significant [MD: −2.94, 95% CI (−4.36; −1.51) p <0.001], I2 = 89%. This was analysed in four studies with 209 participants. (Fig. 8, Online Appendix 1).
Post-operative day 3
Pain on day 3 was also significantly reduced on the VAS, [MD: −2.75, 95% CI (−3.98; −1.51) p < 0.001], I2 = 86%, shown in five studies 227 participants. (Fig. 9, Online Appendix 1).
Post-operative day 7
Pain on day 7 was measured in three studies and 113 participants [MD: −2.01, 95% CI (−3.92; −0.1) p = 0.038, I2 = 93%]. (Fig. 10, Online Appendix 1).
Other outcomes
The primary outcome was pain on the VAS for six of the seven studies. One study reported the primary outcome as time to complete wound healing, defined by complete epithelisation of the wound [36]. One study presented results of pain on defecation [39]. Analgesia amount was presented by five studies, however the method of measuring analgesia taken were heterogenous, thus was unable to be synthesised [33–35, 37, 39]. Anal manometry was not reported in any study comparing diltiazem.
Botulinum toxin
Five studies compared the administration of botulinum toxin against placebo [40–44]. Participants in the intervention groups had botulinum toxin injected at the site of the internal anal sphincter intraoperatively.
Post-operative day 1
Pain measured with the VAS on day 1 in five studies with 260 participants show pain was significantly reduced, [MD: −.47, 95% CI (−2.04; −0.91) p <0.001], with low heterogeneity, I2 = 0%. (Fig. 11, Online Appendix 1).
Post-operative day 2
Pain on day 2 from five studies with 227 participants show a significant reduction in pain, [MD: −2.75, (−3.98; −1.51) p < 0.001], with high heterogeneity, I2 = 86%. (Fig. 12, Online Appendix 1).
Post-operative day 7
Pain on day 7 was reported in four studies with 178 participants. A significant reduction was found with moderate heterogeneity [MD: −1.43, 95% CI (−2.50; −0.35), p = 0.009], I2 = 62%. (Fig. 13, Online Appendix 1).
Other outcomes
Anal manometry was assessed in two studies [42, 43]. Both studies reported the botulinum toxin group had significantly lower mean resting pressures compared to the control groups at week 6. Singh et al. reported there were no significant differences in mean resting pressures by week 12 [43]. Results of resting anal pressures are summarised in Table 1, Online Appendix 1.
Only two studies reported pain at day 14 [40, 43]. Pain on defecation was reported in three studies. Analgesia use was presented in two studies, Alvandipour and Sirikunbpoon.
Lateral internal sphincterotomy (LIS)
A total of 12 studies compared routine haemorrhoidectomy with lateral internal sphincterotomy (LIS) against haemorrhoidectomy without LIS [45–56].
Post-operative day 2
Pain was analysed at day 2 in three studies with 275 participants. The addition of LIS to haemorrhoidectomy reduced pain on the VAS, [MD: −2.13, 95% CI (−3.49; −0.77), p = 0.0021]. Heterogeneity was significant at I2 = 92%. Insufficient information was available to analyse pain on the VAS at other time points. (Fig. 14, Online Appendix 1).
Other measurements of pain
Pain was measured categorically in five studies [49, 50, 52, 54]. The severity of pain was categorised as mild pain, moderate pain and severe pain, with some studies defining ‘severe pain’ as pain > 6 on the 1–10 scoring system. Five studies with 614 patients show patients who had LIS in addition to haemorrhoidectomy were half as likely to have ‘severe pain’ at day 7–10 post-operation [RR: 0.47, 95% CI (0.32; 0.69) p = 0.009]. There was no significant heterogeneity I2 = 0%. (Fig. 15, Online Appendix 1).
Incontinence
Nine studies reported incontinence, defined as any incidence of new gas, liquid or solid faecal incontinence measured at a median follow-up of 4 weeks. Those who underwent lateral sphincterotomy were more than twice as likely to have any symptom of faecal or flatus incontinence in the early post-operative period [RR: 2.26, 95% CI (1.42; 3.58) p = 0.0035]. (Fig. 16, Online Appendix 1).
Other outcomes
Anal manometry was measured in three studies, of which two reported a significant decrease in mean resting pressures in the LIS group [48, 49]. The summary of anal manometry results are reported in Table 1, Online Appendix 1. Two studies reported wound healing at different time points.
Sensitivity analysis
Sensitivity analysis based on type of haemorrhoid excision resulted in a reduction in number of studies when comparing open and closed haemorrhoidectomy separately. This resulted in a widened confidence interval for outcome analyses. Diltiazem versus placebo for open haemorrhoidectomy showed a larger effect in favour of diltiazem, compared to closed haemorrhoidectomy; however, this was based on two studies. The results of the sensitivity analysis are displayed in Table 2, Online Appendix 1.
Other interventions
Ho et al. study investigated the effect of the “Proctolog” (trimebutine 120 mg and Ruscogenins 10 mg) suppository to reduce anal spasm, and found resting pressures were reduced, however had no effect on pain [57]. Perrotti et al. investigated the addition of nifedipine to lidocaine after haemorrhoidectomy, which did not show a conclusive improvement in pain [58].
Risk of bias
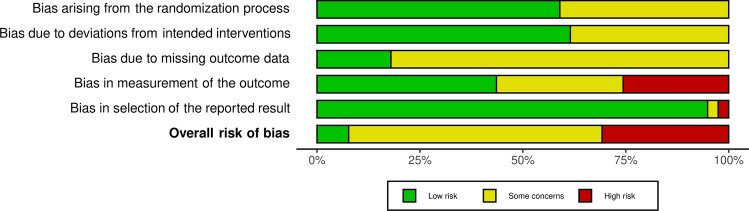
The risk of bias was assessed using ROB 2.0. The majority of studies had ‘some concerns’ and 30.7% of studies had a ‘high’ risk of bias. The main source of bias related to the measurement of the outcome, where outcome assessors were aware of the intervention, and their knowledge of it may have influenced the outcome. Another source of bias arises from domain 3, bias due to missing outcome data. Although the majority of studies analysed results in a modified intention to treat analysis, 79.5% of studies did not relay any information regarding missing outcome data. The risk of bias summary is shown in Fig. 3. Risk of bias for individual studies is displayed in Fig. 17, Online Appendix 1.
Fig. 3.
Risk of bias summary chart according to ROB 2.0
GRADE certainty of evidence
The GRADE certainty evidence for the reduction in pain for was generally ‘low’ for pain outcomes for all interventions, due to serious bias and inconsistency. The certainty of evidence for adverse event outcomes of headache and incontinence was high, due to a large effect being observed. An overall summary of findings is displayed in Table 2, and the GRADE appraisal tables for each outcome is displayed in Figs. 18–21, Online Appendix 1.
Table 2.
GRADE summary of findings table
| Outcome | Number of RCTs | Number of Patients (Intervention vs Control) | Risk of Bias | Other considerations | Pooled effect estimate | Certainty |
|---|---|---|---|---|---|---|
| GTN versus placebo | ||||||
| Day 1 (VAS) | 9 | 270 versus 279 | Serious | Very serious inconsistency | MD 1.03 cm lower (2.03 lower to 0.02 lower) | ⊕◯◯◯ Very low |
| Day 3 (VAS) | 7 | 229 versus 239 | Serious | None | MD 1.5 cm lower (2.82 lower to 0.17 lower) | ⊕⊕◯◯ Low |
| Day 7 (VAS) | 7 | 243 versus 242 | Serious | None | MD 1.34 cm lower (2.31 lower to 0.37 lower) | ⊕⊕◯◯ Low |
| Wound healing | 3 | 125 versus 127 | Very Serious | None | 247 more per 1000 (from 88 to 460 more) | ⊕⊕◯◯ Low |
| Headache | 10 | 334 versus 337 | Not Serious | Very strong association | 76 more per 1000 (from 16 to 248 more) | ⊕⊕⊕⊕ High |
| Diltiazem versus placebo | ||||||
| Day 1 (VAS) | 5 | 112 versus 115 | Serious | Serious inconsistency | MD 2.4 cm lower (3.71 lower to 1.1 lower) | ⊕⊕◯◯ Low |
| Day 3 (VAS) | 5 | 114 versus 113 | Serious | Serious inconsistency | MD 2.75 cm lower (3.98 lower to 1.51 lower) | ⊕⊕◯◯ Low |
| Day 7 (VAS) | 3 | 57 versus 56 | Serious | Serious inconsistency | MD 2.01 cm lower (3.92 lower to 0.11 lower) | ⊕⊕◯◯ Low |
| Botulinum toxin versus placebo | ||||||
| Day 1 (VAS) | 5 | 127 versus 133 | Serious | None | MD 1.27 cm lower (2.04 lower to 0.91 lower) | ⊕⊕⊕◯ Moderate |
| Day 2 (VAS) | 5 | 127 versus 133 | Serious | Serious inconsistency | MD 1.98 cm lower (3.25 lower to 0.7 lower) | ⊕⊕◯◯ Low |
| Day 7 (VAS) | 4 | 88 versus 90 | Serious | Serious inconsistency | MD 1.43 cm lower (2.5 lower to 0.35 lower) | ⊕⊕◯◯ Low |
| Lateral internal sphincterotomy versus none | ||||||
| Day 2 (VAS) | 3 | 139 versus 136 | Very serious | None | MD 2.13 cm lower (3.49 lower to 0.77 lower) | ⊕◯◯◯ Very low |
| Incontinence | 9 | 447 versus 441 | Serious | Strong association | 43 more per 1000 (from 14 to 88 more) | ⊕⊕⊕⊕ High |
| Severe pain | 5 | 249 versus 249 | Very Serious | Strong association | 170 fewer per 1000 (from 218 to 100 fewer) | ⊕⊕⊕◯ Moderate |
GTN glyceryl trinitrate, VAS visual analogue scale, MD mean difference
Discussion
The results of this meta-analysis show a significant benefit in pain reduction across multiple time points after haemorrhoidectomy. Several measures are effective in reducing pain, and these include the topical treatments GTN and diltiazem, as well as procedures such as botulinum toxin injection and lateral internal sphincterotomy. The magnitude of reduction of pain levels on the VAS was clinically meaningful and statistically significant despite the studies having small sample size. The certainty of evidence is low when appraised using the GRADE approach due to a moderate or high risk of bias especially in the domain of outcome assessment. A low certainty of evidence indicates that confidence in the effect is limited and the true effect may be substantially different from the estimated effect.
This meta-analysis reported lateral internal sphincterotomy to be effective in reducing pain. Sphincterotomy remains the most effective treatment for chronic anal fissure; however, anal incontinence remains a risk as a recent meta-analysis showed incontinence rates estimated at 6% across all randomised controlled trials [6]. Alternative, safer options include botulinum toxin administration as well as topical therapies. Botulinum toxin has been shown to be an effective agent in both lowering sphincter pressures and reducing pain. It is administered as a single dose and it is safe and its effect is reversible; however, its routine use is limited by high cost.
Chemical sphincterotomy with topical agents is an alternative strategy, which avoids the irreversibility of a lateral sphincterotomy and the effects on incontinence. Both topical agents GTN and diltiazem are potent vasodilators and trigger smooth muscle relaxation [59]. Increased anal spasm following haemorrhoidectomy is thought to account for the increase in mean resting pressures (MRP) of the sphincter [7]. MRPs were only measured in 10% of included studies, all of which are studies involving botulinum toxin administration or lateral internal sphincterotomy. There were no studies which tested manometry on patients who were given topical therapy; therefore, the effect on sphincter spasm with topical agents remains unclear in the post-haemorrhoidectomy setting. An alternative mechanism of topical therapies is a hypothesised effect of increasing anodermal blood flow to improve healing. Only three studies report wound healing after GTN administration, which found a RR of 1.73 (1.26; 2.36) for wounds that had fully epithelialized at 3 weeks compared to placebo; however, these results are limited by measurement bias where study assesors were unblinded.
The results of this meta-analysis are limited by the high degree of heterogeneity. The variation in study methods and co-interventions may cause significant heterogeneity in the meta-analysis. The studies use different analgesic drugs perioperatively which may affect the pain score on day one post-operation. Furthermore, most studies did not discharge patients using a standardised pain management regime. The inconsistent use of adjunctive techniques across studies such as oral metronidazole may affect post-operative pain [60]. Pain levels are perceived differently depending on the population involved and also depending on how the scores are ascertained; whether scores were self-recorded by participant or ascertained by an assessor may contribute to bias and heterogeneity. Other limitations include the in-ability to pool analgesia data in a meta-analysis due to different types of analgesia used, and variation in frequency of measurement in VAS scores, which result in insufficient data for certain days to be analysed.
In conclusion, this meta-analysis reports a range of interventions targeting a reduction in sphincter spasm to be effective in reducing pain after haemorrhoidectomy. Procedural treatments such as sphincterotomy and botulinum toxin administration are effective for reducing pain; however, sphincterotomy carries a twofold risk of early incontinence compared to haemorrhoidectomy alone. Botulinum toxin is an effective option; however, its routine use may not be cost-effective for pain relief alone. Pharmacologic reduction of sphincter tone could be a viable option, as it is safe and effective with few drawbacks. GTN is effective; however, there is a risk of headache. Diltiazem could be a promising treatment option, due to the absence of adverse effects. More well-designed randomised trials are required to investigate the effect of diltiazem post-haemorrhoidectomy.
Supplementary Information
Below is the link to the electronic supplementary material.
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions. Dr Jin was supported by a Health Research Council of New Zealand Clinical Research Training Fellowship under Grand Number: 22/056
Declarations
Conflict of interest
The author’s declared that they have no conflict of interest.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Change history
1/29/2023
Missing Open Access funding information has been added in the Funding Note
References
- 1.Jin J, Xia W, Connolly A, Hill A. Symptom-based scoring for haemorrhoidal disease: a systematic review. Colorectal Dis. 2020;22(11):1518–1527. doi: 10.1111/codi.15253. [DOI] [PubMed] [Google Scholar]
- 2.Jin J, Bhat S, Lee K-T, Xia W, Hill A. Interventional treatments for prolapsing haemorrhoids: network meta-analysis. BJS Open. 2021;5(5):zrab091. doi: 10.1093/bjsopen/zrab091. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Sammour T, Barazanchi AW, Hill AG. Evidence-based management of pain after excisional haemorrhoidectomy surgery: a PROSPECT review update. World J Surg. 2017;41(2):603–614. doi: 10.1007/s00268-016-3737-1. [DOI] [PubMed] [Google Scholar]
- 4.Sammour T (2022) Pain after hemorrhoidectomy. LWW [DOI] [PubMed]
- 5.Ganio E, Altomare D, Gabrielli F, Milito G, Canuti S. Prospective randomized multicentre trial comparing stapled with open haemorrhoidectomy. Br J Surg. 2001;88(5):669–674. doi: 10.1046/j.0007-1323.2001.01772.x. [DOI] [PubMed] [Google Scholar]
- 6.Jin JZ, Bhat S, Park B, Hardy M-O, Unasa H, Mauiliu-Wallis M et al (2022) A systematic review and network meta-analysis comparing treatments for anal fissure. Surgery 172(1):41–52 [DOI] [PubMed]
- 7.Alper D, Ram E, Stein GY, Dreznik Z. Resting anal pressure following hemorrhoidectomy and lateral sphincterotomy. Dis Colon Rectum. 2005;48(11):2080–2084. doi: 10.1007/s10350-005-0165-y. [DOI] [PubMed] [Google Scholar]
- 8.Ivatury SJ, Swarup A, Wilson MZ, Wilson LR. Prospective evaluation of a standardized opioid reduction protocol after anorectal surgery. J Surg Res. 2020;256:564–569. doi: 10.1016/j.jss.2020.07.028. [DOI] [PubMed] [Google Scholar]
- 9.Xia W, Sammour T, Hill A. Pursuit of the painless haemorrhoidectomy: current and future research directions. ANZ J Surg. 2020;90(5):656–657. doi: 10.1111/ans.15582. [DOI] [PubMed] [Google Scholar]
- 10.Goligher JC, Graham NG, De Dombal FT, Giles GR, Clark CG. The value of stretching of anal sphincters in the relief of pain after haemorrhoidectomy. Br J Surg. 1969;56(5):390. [PubMed] [Google Scholar]
- 11.Emile SH, Youssef M, Elfeki H, Thabet W, El-Hamed TM, Farid M. Literature review of the role of lateral internal sphincterotomy (LIS) when combined with excisional hemorrhoidectomy. Int J Colorectal Dis. 2016;31(7):1261–1272. doi: 10.1007/s00384-016-2603-9. [DOI] [PubMed] [Google Scholar]
- 12.Asfar SK, Juma TH, Ala-Edeen T. Hemorrhoidectomy and sphincterotomy. Dis Colon Rectum. 1988;31(3):181–185. doi: 10.1007/BF02552543. [DOI] [PubMed] [Google Scholar]
- 13.Group GW Grading quality of evidence and strength of recommendations. BMJ. 2004;328(7454):1490. doi: 10.1136/bmj.328.7454.1490. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Int J Surg. 2021;88:105906. doi: 10.1016/j.ijsu.2021.105906. [DOI] [PubMed] [Google Scholar]
- 15.Luo D, Wan X, Liu J, Tong T. Optimally estimating the sample mean from the sample size, median, mid-range, and/or mid-quartile range. Stat Methods Med Res. 2018;27(6):1785–1805. doi: 10.1177/0962280216669183. [DOI] [PubMed] [Google Scholar]
- 16.Team RC (2013) R: A language and environment for statistical computing
- 17.Schwarzer G. meta: an R package for meta-analysis. R News. 2007;7(3):40–45. [Google Scholar]
- 18.Sterne JA, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I, et al. (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. Bmj: 366 [DOI] [PubMed]
- 19.GRADEpro G (2016) GRADEpro guideline development tool [software]. McMaster University, 2015 (developed by Evidence Prime, Inc.)
- 20.Asif K, Maaz Ul H, Rehman PM, Rasheed T, Zahid L. Compare the efficacy of 0.2% topical glyceryl trinitrate (GTN) versus placebo in prevention of wound infection in patients undergoing Milligan-Morgan hemorrhoidectomy. Pak J Med Health Sci. 2020;14(2):581–583. [Google Scholar]
- 21.Di Vita G, Patti R, Arcara M, Petrone R, Davi V, Leo P. A painless treatment for patients undergoing Milligan-Morgan haemorrhoidectomy. Ann Ital Chir. 2004;75(4):471–474. [PubMed] [Google Scholar]
- 22.Franceschilli L, D'Ugo S, de Luca E, Cadeddu F, Milito G, di Lorenzo N, et al. Role of 0.4% glyceryl trinitrate ointment after haemorrhoidectomy: results of a prospective randomised study. Int J Colorectal Dis. 2013;28(3):365–369. doi: 10.1007/s00384-012-1544-1. [DOI] [PubMed] [Google Scholar]
- 23.Hwang DY, Yoon SG, Kim HS, Lee JK, Kim KY. Effect of 0.2% glyceryl trinitrate ointment on wound healing after a hemorrhoidectomy: results of a randomized, prospective, double-blind, placebo-controlled trial. Dis Colon Rectum. 2003;46(7):950–954. doi: 10.1007/s10350-004-6692-0. [DOI] [PubMed] [Google Scholar]
- 24.Karanlik H, Akturk R, Camlica H, Asoglu O. The effect of glyceryl trinitrate ointment on posthemorrhoidectomy pain and wound healing: results of a randomized, double-blind, placebo-controlled study. Dis Colon Rectum. 2009;52(2):280–285. doi: 10.1007/DCR.0b013e31819c98a7. [DOI] [PubMed] [Google Scholar]
- 25.Khan KI, Waqas A, Akmal M, Mahmood S, Iqbal A. Efficacy of combination of 0.2% GTN and lignocaine ointments in wound healing and pain relief after Milligan Morgan hemorrhoidectomy–a comparison with lignocaine and 0.2% GTN ointments separately. Int J Surg. 2014;12(4):329–333. doi: 10.1016/j.ijsu.2014.01.013. [DOI] [PubMed] [Google Scholar]
- 26.Lashari AALI, Bozdar AG, Bhellar ZH, Baker A, Shar ZALI, Narejo GALI. Determine the effectiveness of 0.2% topical glyceryl trinitrate in preventing postoperative wound infection after hemorrhoidectomy. Pak J Med Health Sci. 2020;14(4):1327–1329. [Google Scholar]
- 27.Mari FS, Nigri G, Dall'Oglio A, Cosenza UM, Milillo A, Terrenato I, et al. Topical glyceryl trinitrate ointment for pain related to anal hypertonia after stapled hemorrhoidopexy: a randomized controlled trial. Dis Colon Rectum. 2013;56(6):768–773. doi: 10.1097/DCR.0b013e31828b282c. [DOI] [PubMed] [Google Scholar]
- 28.Patti R, Arcara M, Padronaggio D, Bonventre S, Angileri M, Salerno R, et al. Efficacy of topical use of 0.2% glyceryl trinitrate in reducing post-haemorrhoidectomy pain and improving wound healing. Chir Ital. 2005;57(1):77–85. [PubMed] [Google Scholar]
- 29.Soltany S, Toussy JA, Foruzesh FM. The effect of 0.2% glyceryl trinitrate ointment on pain and wound healing after hemorrhoidectomy. Surg J. 2009;4(1):8–12. [Google Scholar]
- 30.Tan KY, Sng KK, Tay KH, Lai JH, Eu KW. Randomized clinical trial of 0.2% glyceryl trinitrate ointment for wound healing and pain reduction after open diathermy haemorrhoidectomy. Br J Surg. 2006;93(12):1464–1468. doi: 10.1002/bjs.5483. [DOI] [PubMed] [Google Scholar]
- 31.Vahabi S, Beiranvand S, Karimi A, Moradkhani M. Comparative study of 0.2% glyceryl trinitrate ointment for pain reduction after hemorrhoidectomy surgery. Surgery. 2019;5(4):e1926-e6. doi: 10.1055/s-0039-3400532. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Wasvary HJ, Hain J, Mosed-Vogel M, Bendick P, Barkel DC, Klein SN. Randomized, prospective, double-blind, placebo-controlled trial of effect of nitroglycerin ointment on pain after hemorrhoidectomy. Dis Colon Rectum. 2001;44(8):1069–1073. doi: 10.1007/BF02234622. [DOI] [PubMed] [Google Scholar]
- 33.Abidi SS, Bakhtiar N, Kerawala AA, Awan S. Topical diltiazem ointment for post-hemorrhoidectomy pain. J Ayub Med Coll Abbottabad. 2021;33(1):125–128. [PubMed] [Google Scholar]
- 34.Amoli HA, Notash AY, Shahandashti FJ, Kenari AY, Ashraf H. A randomized, prospective, double-blind, placebo-controlled trial of the effect of topical diltiazem on posthaemorrhoidectomy pain. Colorectal Dis. 2011;13(3):328–332. doi: 10.1111/j.1463-1318.2009.02138.x. [DOI] [PubMed] [Google Scholar]
- 35.Rodriguez-Wong U, Ocharan-Hernandez ME, Toscano-Garibay J. Topical diltiazem for pain after closed hemorrhoidectomy. Rev Gastroenterol Mex. 2016;81(2):74–79. doi: 10.1016/j.rgmx.2016.02.001. [DOI] [PubMed] [Google Scholar]
- 36.Rodriguez-Wong U, Rodriguez-Medina U, Medina-Murillo GR. Randomized clinical trial with topical diltiazem for post-hemorrhoidectomy wound healing. Rev Gastroenterol Mex. 2019;84(1):119–122. doi: 10.1016/j.rgmx.2018.10.001. [DOI] [PubMed] [Google Scholar]
- 37.Silverman R, Bendick PJ, Wasvary HJ. A randomized, prospective, double-blind, placebo-controlled trial of the effect of a calcium channel blocker ointment on pain after hemorrhoidectomy. Dis Colon Rectum. 2005;48(10):1913–1916. doi: 10.1007/s10350-005-0135-4. [DOI] [PubMed] [Google Scholar]
- 38.Suchdev S, Ghayassuddin M, Younus SM, Mirani AJ, Ghias N, Qazi A, et al. Calcium channel blockers for pain relief after haemorrhoidectomy; a randomized controlled trial from Karachi Pakistan. Pak J Surg. 2014;30(2):187–192. [Google Scholar]
- 39.Sugimoto T, Tsunoda A, Kano N, Kashiwagura Y, Hirose K, Sasaki T. A randomized, prospective, double-blind, placebo-controlled trial of the effect of diltiazem gel on pain after hemorrhoidectomy. World J Surg. 2013;37(10):2454–2457. doi: 10.1007/s00268-013-2124-4. [DOI] [PubMed] [Google Scholar]
- 40.Alvandipour M, Tavallaei M, Rezaei F, Khodabakhsh H. Postoperative outcomes of intrasphincteric botox injection during hemorrhoidectomy: a double-blind clinical trial. J Res Med Sci. 2021;26(1):53. doi: 10.4103/jrms.JRMS_612_18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Davies J, Duffy D, Boyt N, Aghahoseini A, Alexander D, Leveson S. Botulinum toxin (botox) reduces pain after hemorrhoidectomy: results of a double-blind, randomized study. Dis Colon Rectum. 2003;46(8):1097–1102. doi: 10.1007/s10350-004-7286-6. [DOI] [PubMed] [Google Scholar]
- 42.Patti R, Almasio PL, Arcara M, Sammartano S, Romano P, Fede C, et al. Botulinum toxin versus topical glyceryl trinitrate ointment for pain control in patients undergoing hemorrhoidectomy: a randomized trial. Dis Colon Rectum. 2006;49(11):1741–1748. doi: 10.1007/s10350-006-0677-0. [DOI] [PubMed] [Google Scholar]
- 43.Singh B, Box B, Lindsey I, George B, Mortensen N, Cunningham C. Botulinum toxin reduces anal spasm but has no effect on pain after haemorrhoidectomy. Colorectal Dis. 2009;11(2):203–207. doi: 10.1111/j.1463-1318.2008.01549.x. [DOI] [PubMed] [Google Scholar]
- 44.Sirikurnpiboon S, Jivapaisarnpong P. Botulinum toxin injection for analgesic effect after hemorrhoidectomy: a randomized control trial. J Anus Rectum Colon. 2020;4(4):186–192. doi: 10.23922/jarc.2020-027. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Butt AS, Dogar MA, Sadiq I. Comparison of outcomes, with and without lateral internal sphincterotomy, in patients undergoing open Haemorrhoidectomy. Pak J Med Health Sci. 2018;12(4):1471–1474. [Google Scholar]
- 46.Chauhan A, Tiwari S, Mishra V, Bhatia P. Comparison of internal sphincterotomy with topical diltiazem for post-hemorrhoidectomy pain relief: a prospective randomized trial. J Postgrad Med. 2009;55(1):22–26. doi: 10.4103/0022-3859.48436. [DOI] [PubMed] [Google Scholar]
- 47.Das D, Choudhury U, Lim Z. Effectiveness of internal sphincterotomy in reducing post open hemorrhoidectomy pain: a randomized comparative clinical study. Int J Collab Res Intern Med Public Health. 2013;5(6):0. [Google Scholar]
- 48.Galizia G, Lieto E, Castellano P, Pelosio L, Imperatore V, Pigantelli C. Lateral internal sphincterotomy together with haemorrhoidectomy for treatment of haemorrhoids: a randomised prospective study. Eur J Surg. 2000;166(3):223–228. doi: 10.1080/110241500750009320. [DOI] [PubMed] [Google Scholar]
- 49.Hosseini SV, Sharifi K, Ahmadfard A, Mosallaei M, Pourahmad S, Bolandparvaz S. Role of internal sphincterotomy in the treatment of hemorrhoids: a randomized clinical trial. Arch Iran Med. 2007;10(4):504–508. [PubMed] [Google Scholar]
- 50.Kanellos I, Zacharakis E, Christoforidis E, Angelopoulos S, Kanellos D, Pramateftakis MG, et al. Usefulness of lateral internal sphincterotomy in reducing postoperative pain after open hemorrhoidectomy. World J Surg. 2005;29(4):464–468. doi: 10.1007/s00268-004-7432-2. [DOI] [PubMed] [Google Scholar]
- 51.Khubchandani IT. Internal sphincterotomy with hemorrhoidectomy does not relieve pain: a prospective, randomized study. Dis Colon Rectum. 2002;45(11):1452–1457. doi: 10.1007/s10350-004-6450-3. [DOI] [PubMed] [Google Scholar]
- 52.Lu M, Shi G-Y, Wang G-Q, Wu Y, Liu Y, Wen H. Milligan-Morgan hemorrhoidectomy with anal cushion suspension and partial internal sphincter resection for circumferential mixed hemorrhoids. World J Gastroenterol: WJG. 2013;19(30):5011. doi: 10.3748/wjg.v19.i30.5011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Mathai V, Ong BC, Ho YH. Randomized controlled trial of lateral internal sphincterotomy with haemorrhoidectomy. Br J Surg. 1996;83(3):380–382. doi: 10.1002/bjs.1800830327. [DOI] [PubMed] [Google Scholar]
- 54.Raza MW. Haemorrhoidectomy with and without lateral internal sphinterotomy. J Rawalpindi Med Coll. 2013;17(2):189–191. [Google Scholar]
- 55.Sushel C, Dalwani AG, Memon KN, Shaikh NA, Otho S, Syed BM. Haemorrhoidectomy with internal sphincterotomy: a useful method to relieve post operative pain? J Liaquat Univ Med Health Sci. 2015;14(2):73–77. [Google Scholar]
- 56.Vijayaraghavalu S, Prasad RG, Rajkumar S. The role of lateral internal sphincterotomy in haemorrhoidectomy: a study in a tertiary care center. Cureus. 2021;13(6):e15630. doi: 10.7759/cureus.15630. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Ho YH, Seow-Choen F, Low JY, Tan M, Leong AP. Randomized controlled trial of trimebutine (anal sphincter relaxant) for pain after haemorrhoidectomy. Br J Surg. 1997;84(3):377–379. [PubMed] [Google Scholar]
- 58.Perrotti P, Dominici P, Grossi E, Cerutti R, Antropoli C. Topical nifedipine with lidocaine ointment versus active control for pain after hemorrhoidectomy: results of a multicentre, prospective, randomized, double-blind study. Can J Surg. 2010;53(1):17–24. [PMC free article] [PubMed] [Google Scholar]
- 59.Jin JZ, Hardy M-O, Unasa H, Mauiliu-Wallis M, Weston M, Connolly A et al (2022) A systematic review and meta-analysis of the efficacy of topical sphincterotomy treatments for anal fissure. Int J Colorectal Dis 37(1):1–15 [DOI] [PubMed]
- 60.Xia W, Barazanchi AW, MacFater WS, MacCormick AD, Svirskis D, Sammour T, Hill AG (2022) Topical versus oral metronidazole after excisional hemorrhoidectomy: A double-blind randomized controlled trial. Dis Colon Rectum 65(11):1362–1372 [DOI] [PubMed]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.