Abstract
Invasive fungal infections represent an increasing problem associated with high mortality. The present study was undertaken to identify leukocyte subsets that are activated by hyphal fragments in a whole-human-blood model, as well as to examine the involvement of CD14 and Toll-like receptors (TLRs) in activation of monocytes by hyphae. Incubation of whole human blood with hyphal fragments from Aspergillus fumigatus and Scedosporium prolificans for 6 h caused induction of mRNAs for tumor necrosis factor alpha (TNF-α), interleukin-1β (IL-1β), and IL-6 in T cells, B cells, and monocytes, but not in granulocytes, as analyzed by reverse transcription-PCR with mRNA isolated from very pure populations of these leukocyte subsets. In primary adherent human monocytes, induction of TNF-α by hyphal fragments was dependent on plasma. Heat treatment of plasma at 56°C for 30 min strongly reduced the ability of plasma to prime for activation. Pretreatment of human monocytes with different concentrations (1, 3, and 10 μg/ml) of monoclonal antibody (MAb) HTA125 (anti-TLR4) or MAb 18D11 (anti-CD14) for 30 min inhibited the release of TNF-α induced by hyphal fragments in a dose-dependent manner. Maximal inhibitions of 35 and 70% were obtained with 10 μg of HTA125 and 18D11 per ml, respectively. In contrast, pretreatment with MAb TL2.1 (anti-TLR2) did not affect signaling induced by hyphae. Pretreatment with the lipid A antagonist B975 blocked lipopolysaccharide signaling but did not inhibit TNF-α production induced by hyphal fragments. Our results suggest that T cells, B cells, and monocytes are involved in the innate immune response to invasive fungal pathogens and that serum components are relevant for activation of monocytes by hyphae. CD14 and TLR4 may be involved in signaling of Aspergillus hyphae in monocytes, but further studies to elucidate this issue are warranted.
Sepsis caused by fungal infections is a major and increasing problem that is responsible for high rates of morbidity and mortality (6, 19, 37). As the number of immunocompromised patients has increased, invasive aspergillosis has become the second most common opportunistic fungal infection (1, 11). The major host defense against invasive aspergillosis has been shown to be mediated by cells of the innate immune system. Macrophages in the lung ingest inhaled airborne Aspergillus conidia and thereby inhibit their intracellular germination (16, 31, 36). In addition, polymorphonuclear leukocytes, as well as monocytes, cause damage to escaping conidia and hyphae by secretion of oxidative metabolites and nonoxidative compounds, thereby preventing establishment of invasive infections (7, 16, 31).
The role of cytokines in the host response to Aspergillus has just recently begun to be elucidated (3, 4, 28–30). It was recently demonstrated that killed hyphal fragments and, to a lesser degree, conidia from Aspergillus fumigatus provoke an inflammatory response in whole human blood (A. Warris, J. E. Wang, P. E. Verweij, P. Gaustad, and T. G. Abrahamsen, unpublished data), as seen by release of the proinflammatory cytokines tumor necrosis factor alpha (TNF-α) and interleukin-6 (IL-6). The anti-inflammatory cytokine IL-10 was not significantly induced by any of the fungal structures. The chain of events that leads to activation of human leukocytes by fungal structures is still elusive.
The Toll protein in Drosophila was recently demonstrated as being involved in dorsoventral patterning in embryonic development (2), as well as mediating antifungal defense in the adult fly (15). Mammalian homologues of Toll, termed Toll-like receptors (TLRs), have been cloned (22), and TLRs are attributed key roles in the induction of immunity (20, 21). Today, only two of these receptors have any known ligands. TLR4 has been shown to mediate cell signaling by lipopolysaccharide (LPS) (27, 34), whereas TLR2 has been implicated in the response to diverse bacterial products (9, 17). Despite their role in antifungal defense in the fly, the involvement of TLRs in the host response to fungal pathogens in mammals has not previously been studied.
The present study examined the influence of blockade of CD14, TLR2, and TLR4 with specific monoclonal antibodies (MAbs) on activation of human monocytes by hyphal fragments. The requirement of plasma for cell activation by hyphae was also studied. Finally, we have identified the leukocyte subsets responsible for cytokine release in whole blood stimulated with hyphal fragments from A. fumigatus or Scedosporium prolificans.
MATERIALS AND METHODS
Reagents and antibodies.
MAb TL2.1 was generated as previously described (9). MAb HTA125 was a kind gift from Kensuke Miyake (Saga Medical School, Saga, Japan) (32). A MAb against CD14 (18D11) and a negative control antibody (immunoglobulin G1 [IgG1]) were purchased from Diatec AS (Oslo, Norway). B975 is a synthetic analogue of Rhodobacter capsulatus lipid A, provided by D. P. Rossignol and W. J. Christ (Eisai Research Institute, Andover, Mass.) (26).
Isolation of killed hyphal fragments
The A. fumigatus and S. prolificans strains used in this study were obtained from clinical isolates of invasive aspergillosis and scedosporiosis, respectively. The strains were grown on Sabouraud glucose agar supplemented with penicillin-streptomycin for 4 to 7 days at 35°C. Abundant conidia were elaborated under these conditions. Conidia were harvested by gently scraping the surfaces of the slants and suspending them in phosphate-buffered saline (PBS). To suspend the very hydrophobic conidia of A. fumigatus, 0.05% Tween 80 was added to the PBS. To remove hyphae and debris, the conidial suspension was filtered through eight layers of cheesecloth. Hyphal fragments were developed from these conidia as previously described (Warris et al., unpublished). In brief, conidia from both A. fumigatus and S. prolificans were added to 5 ml of yeast nitrogen base (Difco Laboratories, Detroit, Mich.) in a final concentration of 106 conidia per ml. After 18 h of incubation at 37°C, the tubes were centrifuged (2,800 × g for 10 min) in order to spin down the pellet. The pellet, containing almost exclusively mycelia, was washed twice in Hanks balanced saline solution without Ca2+ and Mg2+ (HBSS w/o). The mycelia were resuspended in ethanol-PBS (70%) and stored in a refrigerator for 24 h. The sterilized hyphae were centrifuged and resuspended vigorously in PBS containing 10 mg of RNase A (from bovine pancreas; Sigma-Aldrich, St. Louis, Mo.) per ml and incubated for 30 min at 37°C to remove intracellular RNA. Finally, the hyphal fragments were washed three times with HBSS w/o, and aliquots of 1.5 ml containing hyphal fragments from, initially, 5 × 106 conidia were stored at −80°C. The lack of viability after ethanol treatment was always confirmed by culture in Sabouraud glucose broth. Microscopically, the morphology of the killed hyphal fragments seemed intact.
Whole-blood experiments.
The whole-blood model used in this study has recently been established and characterized (38). Venous blood from healthy volunteers was anticoagulated with heparin (30 IU per ml of blood). Blood was incubated in Monovette syringes (Sarstedt, Germany) in the absence or presence of hyphal fragments from A. fumigatus or S. prolificans or of LPS (Escherichia coli O26:B7; Difco Laboratories). At indicated time points, leukocyte subsets or plasma was isolated.
Primary adherent monocytes.
Peripheral blood mononuclear cells (PBMCs) were isolated from heparinized human blood (30 IU per ml of blood) (24). PBMCs (3 × 106 to 4 × 106 per ml) were seeded at 200 μl per well in 96-well dishes (Costar). Monocytes were allowed to adhere for 90 min in 5% CO2 at 37°C before being washed three times in HBSS. For blockade of receptors, monocytes were incubated at room temperature with various doses of MAbs HTA125 (anti-TLR4), TL2.1 (anti-TLR2), and 18D11 (anti-CD14); IgG1 control antibody; or the B975 lipid A antagonist in RPMI medium under serum-free conditions. The monocytes were subsequently added to a mixture of 5% autologous plasma and hyphal fragments (15 μl of hyphal suspension grown from 3.3 × 106 conidia) or LPS. Supernatants were collected after 8 h and stored at −20°C.
Fractionation of leukocytes.
CD14+ cells were isolated from whole blood as previously described (33). In brief, Dynabeads M450 CD14 (Dynal, Oslo, Norway) were used to isolate a pure population of leukocytes expressing the CD14 receptor (monocytes, macrophages, and a subset of granulocytes). Fifty microliters of Dynabeads (4 × 108 beads per ml) was used per 400 μl of blood. The beads and blood were incubated with gentle rotation for 5 min at 4°C and subsequently placed on a magnet (MPC 6; Dynal) for 3 min. After being washed twice in cold PBS, the cells were lysed by addition of 300 μl of lysis-and-binding buffer (Dynal). The lysates were used directly for mRNA isolation or frozen at −20°C.
Pure populations of T cells (CD2+), granulocytes (CD15+), and B cells (CD19 positive) were isolated in a similar manner from 400, 800, and 100 μl of blood, respectively, in accordance with protocols provided by the manufacturer (Dynal).
Isolation of mRNA.
Isolation of mRNA was carried out as previously described (33), with oligo(dT)25-coated Dynabeads (Dynal). Briefly, 30 μl of prewashed oligo(dT)25 (5 mg/ml)-coated Dynabeads and lysates from CD2+, CD14+, CD15+, or CD19+ cells were rotated for 5 min at room temperature. After a thorough washing, the mixture of beads and mRNA was resuspended in 20 μl of diethyl pyrocarbonate-treated distilled water and used directly in reverse transcription-PCR (RT-PCR) or frozen at −20°C.
RT-PCR.
Semiquantitative analyses of cytokine mRNA expression were performed by RT-PCR according to a previously described protocol (33). Briefly, RT and PCR were performed in a PCR Cycler (GeneAmp 9600; Perkin-Elmer Cetus Corp., Norwalk, Conn.). Synthesis of cDNA was performed by RT directly on the mRNA attached to the oligo(dT)25 beads by using a GeneAmp RNA PCR kit (Perkin-Elmer). Subsequently, the cDNA pool was analyzed by PCR for cDNA specific for TNF-α, IL-6, IL-10, and β-actin with specific primers as previously described (33).
Plasma cytokine analysis.
At the indicated times, plasma was removed from the blood by centrifugation at 7,000 × g for 2 min and stored at −20°C for later analyses by enzyme immunoassay (EIA) specific for TNF-α according to protocols provided by the manufacturer (CLB, Amsterdam, The Netherlands). The detection limit was 1 pg/ml.
Statistical evaluation.
Data are presented as means ± standard errors. Student's t test or analysis of variance with Tukey's post hoc assessment was used to evaluate the statistical significance of the results. Differences with P values of <0.05 were considered significant.
RESULTS
Cytokine mRNAs in leukocyte subsets.
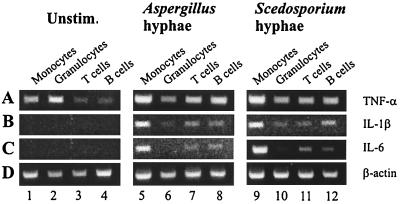
Figure 1 shows accumulation of mRNAs for TNF-α (A), IL-1β (B), IL-6 (C), and β-actin (D) in pure populations of leukocyte subsets isolated after stimulation of whole human blood with hyphal fragments from A. fumigatus or S. prolificans, as detected by RT-PCR. Figure 1A shows that TNF-α mRNA was detected in all leukocyte subsets in unstimulated blood (lanes 1 to 4). Stimulation with hyphal fragments from A. fumigatus or S. prolificans caused enhanced levels of TNF-α mRNA in monocytes (lanes 5 and 9), T cells (lanes 7 and 11), and B cells (lanes 8 and 12), but not in granulocytes (lanes 6 and 10). Neither IL-1β mRNA (Fig. 1B) nor IL-6 mRNA (Fig. 1C) was detected in leukocytes isolated from unstimulated blood (lanes 1 to 4). In contrast, in blood treated with hyphae from A. fumigatus or S. prolificans, IL-1β mRNA was strongly induced in monocytes (lanes 5 and 9). Low levels of IL-1β were also detected in granulocytes (lanes 6 and 10), T cells (lanes 7 and 11), and B cells (lanes 8 and 12). Figure 1C shows that, similar to TNF-α, IL-6 mRNA was induced in monocytes (lanes 5 and 9), T cells (lanes 7 and 11), and B cells (lanes 8 and 12), but not in granulocytes (lanes 6 and 10).
FIG. 1.
Expression of mRNAs for TNF-α, IL-1β, IL-6, and β-actin in various leukocyte populations 6 h after incubation of whole blood in the absence (lanes 1 to 4) or presence of hyphal fragments isolated from A. fumigatus (lanes 5 to 8) or S. prolificans (lanes 9 to 12). Monocytes (CD14+), granulocytes (CD15+), T cells (CD2+), and B cells (CD19+) were isolated by immunomagnetic separation. mRNA from these cells was isolated by oligo(dT)25-coated magnetic beads, reverse transcribed, and analyzed for transcripts encoding TNF-α (A [443 bp]), IL-1β (B [802 bp]), IL-6 (C [628 bp]), and β-actin (D [660 bp]) by PCR. Unstim., unstimulated.
Dependency on plasma for stimulation of human monocytes by hyphal fragments.
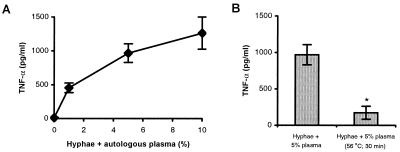
Figure 2A shows that hyphal fragments were unable to induce TNF-α release from primary adherent human monocytes in the absence of plasma. Stimulation of monocytes by hyphal fragments (A. fumigatus) in the presence of autologous plasma (1, 5, and 10%) resulted in induction of TNF-α production in a plasma dose-dependent manner. Heat treatment of plasma at 56°C for 30 min to inactivate complement strongly reduced TNF-α production (Fig. 2B).
FIG. 2.
Dependency on plasma for stimulation of TNF-α release by human monocytes (four donors) by hyphal fragments from A. fumigatus. (A) Human monocytes isolated from whole blood were spiked with autologous plasma (0, 1, 5, or 10%) and cultured for 8 h in the absence or presence of hyphal fragments. (B) Monocytes were stimulated with hyphal fragments in the presence of 5% untreated plasma or 5% plasma that had been heat treated at 56°C for 30 min. Supernatants were subsequently analyzed for TNF-α by EIA. Data are means ± standard errors of four experiments. ∗, significantly lower (P < 0.05) than values obtained with untreated plasma, as calculated by Student's t test.
Blockade of signaling events.
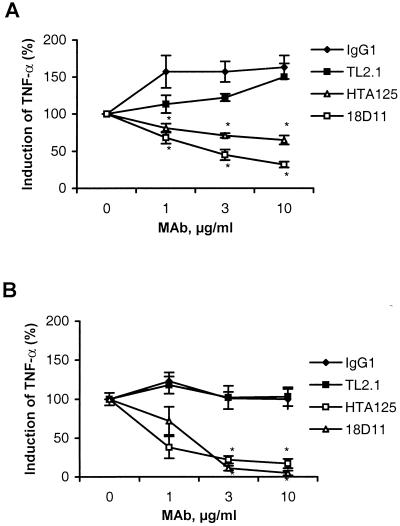
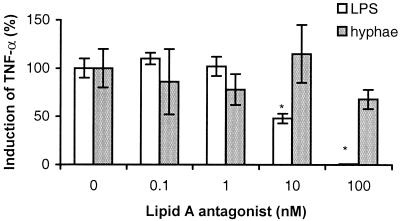
Pretreatment of human monocytes with MAb HTA125 (anti-TLR4) or 18D11 (anti-CD14) inhibited the production of TNF-α induced by Aspergillus hyphae in a dose-dependent manner (Fig. 3A). Maximal inhibition levels of 35 and 70% were obtained with 10 μg of HTA125 or 18D11 per ml, respectively. Pretreatment with TL2.1 or an isotype control (IgG1) antibody did not inhibit the release of TNF-α induced by hyphal fragments. In comparison, HTA125 and 18D11 at 10 μg/ml inhibited LPS-induced TNF-α by 85 and 95%, respectively (Fig. 3B), whereas this stimulation was not influenced by TL2.1 or the control antibody. Figure 4 shows that pretreatment of human monocytes with a synthetic analogue of Rhodobacter capsulatus (B975) (26) inhibited LPS-induced release of TNF-α in a dose-dependent manner. At 100 nM B975, the TNF-α release induced by LPS was completely blocked. In contrast, B975 did not influence the TNF-α release induced by hyphal fragments.
FIG. 3.
Influence of blockade of CD14, TLR4, and TLR2 on primary adherent monocytes by MAbs on stimulation of TNF-α production by Aspergillus hyphae (A) and LPS (B). Human monocytes were pretreated with different concentrations (1, 3, or 10 μg/ml) of 18D11 (anti-CD14), HTA125 (anti-TLR4), TL2.1 (anti-TLR2), or an IgG1 control antibody for 30 min at room temperature under serum-free conditions. Hyphal fragments and 5% plasma (or LPS [10 ng/ml]) were subsequently added, followed by incubation for 8 h. Supernatants were analyzed for TNF-α by EIA. Results are means ± standard errors of six to nine experiments. ∗, significantly lower (P < 0.05) than values obtained with control antibodies, as calculated by analysis of variance.
FIG. 4.
Influence of a synthetic analog of Rhodobacter capsulatus lipid A (B975) on TNF-α release from primary adherent human monocytes induced by Aspergillus hyphae or LPS (10 ng/ml). Monocytes were pretreated with various doses of B975 (0, 0.1, 1, 10, or 100 nM) for 30 min prior to addition of Aspergillus hyphae or LPS (10 ng/ml). After 8 h of stimulation, supernatants were isolated and analyzed for TNF-α by EIA. Results are means ± standard deviations of triplicate samples in one typical experiment performed three times. ∗, significantly lower (P < 0.05) than values obtained in the absence of B975, as calculated by analysis of variance.
DISCUSSION
This is the first study of the involvement of TLRs in the host response to filamentous fungal pathogens. The partial inhibition of hypha-induced activation observed with antibodies against TLR4 and CD14 suggests that several receptors may be involved, of which TLR4 and CD14 are two candidates. A receptor complex consisting of TLR4, CD14, and MD-2 mediates LPS signaling (27, 34). This may suggest that hyphae stimulate cells through mechanisms partly similar to those of LPS. Compared with control antibody, a weak inhibition was also obtained with TL2.1 (anti-TLR2), and we cannot rule out a role for TLR2 in hyphal signaling. Another interpretation of these results is that different TLRs are actually involved. The weak and partial inhibition of monocyte activation by anti-TLR2 and anti-TLR4 antibodies may be attributed to cross-reactivities with yet uncharacterized TLRs. The immunostimulatory molecule(s) in the hyphal fragments that interacts with pathogen recognition receptors on monocytes is not known. The hyphal cell wall consists of β-glucan and galactomannan, which have immunogenic properties (12). An undefined “endotoxin” derived from A. fumigatus mycelia that is toxic in animal models of aspergillosis has also been described (5). The latter study supports the contention that hyphae may activate LPS signaling pathways. However, the failure of a lipid A antagonist to interfere with hyphal stimulation demonstrates that hyphae activate cells differently from LPS. More studies are clearly warranted to elucidate the involvement of CD14 and TLRs in recognition and signaling of hyphae in vitro and in vivo, as well as the roles of these receptors during invasive fungal infections.
We observed an absolute requirement of serum for activation of human monocytes by hyphae. Plasma contains secreted pathogen recognition receptors such as LPS-binding protein (LBP), soluble CD14 (sCD14), and mannan-binding lectin (reviewed in reference 20). Mannan-binding lectin opsonizes mannan for presentation to signaling receptors (8, 10). Binding of microbial ligand to mannan-binding lectin results in an amplified cascade of complement activation (8), and Aspergillus hyphae have indeed been demonstrated to activate complement via both the alternative and classical pathways in human serum (13, 14). A role for mannan-binding lectin in the innate response to fungal infections, however, has not yet been demonstrated (20). In support of the contention that activation of leukocytes is mediated by complement, inactivation of complement by heat treatment strongly attenuated activation in the present study. Hence, studies of complement receptor involvement in activation of monocytes by hyphae are warranted. Inactivation of complement by heat treatment did not result in complete loss of leukocyte activation, which suggests that other factors in the plasma, such as LBP and sCD14, also may be involved in cellular activation by hyphae. Alternatively, the residual activation obtained by heat-treated plasma may also be due to cross-linking of Fc receptors by natural antibodies to hyphae. Further studies are clearly needed to dissect the basis for the serum requirements observed in the present study.
This is the first report on the induction by hyphae of mRNAs for TNF-α, IL-1β, and IL-6 in leukocytes. The ability of hyphae to induce cytokine release has been previously observed by us and others (35; Warris et al., unpublished). That cytokine mRNAs were increased in T cells, B cells, and monocytes in blood stimulated with hyphal fragments suggests that these leukocyte subsets contribute to the cytokine production during invasive fungal infection. This notion is supported by the fact that a similar pattern was seen with hyphal fragments isolated from two different fungal pathogens. Furthermore, the fact that hyphal fragments induce cytokine production in several leukocyte subsets supports the contention that cytokines play important roles in the host's defense against fungal pathogens (3, 4, 28–30). The failure of hyphal fragments to induce cytokine mRNA production in granulocytes is somewhat surprising. Polymorphonuclear leukocytes, as well as circulating monocytes, are thought to represent the major host defense against invasive fungal infections, by secretion of microbicidal compounds (7, 16, 31). However, hyphal structures are too large to be phagocytosed and thus have to be attacked extracellularly. This calls upon other cell types, such as B cells and T cells. Whether NK cells may also play a role in this respect is not known. The cytokine pattern induced by hyphae in the present study is partly different from what has been previously reported with bacterial components, in which only T cells and monocytes were activated (39). A role for lymphocytes in innate immune responses has gained new support due to the recent discovery that members of the TLR family are expressed on mammalian T cells (18, 23) and B cells (25).
Our data suggest that T cells, B cells, and monocytes are involved in the innate host response to invasive fungal infections and that serum components are relevant for activation of monocytes by hyphae. CD14 and TLR4 may be involved in signaling of Aspergillus hyphae in monocytes, but further studies are warranted to elucidate this issue.
ACKNOWLEDGMENTS
We are indebted to Kensuku Miyake (Saga Medical School, Saga, Japan) for providing us with HTA125 MAb and William J. Christ and Daniel P. Rossignol (Eisai Resarch Institute, Andover, Mass.) for giving us the synthetic analogue of Rhodobacter capsulatus lipid A (B975).
This work was supported by the Norwegian Research Council.
REFERENCES
- 1.Beck-Sague C M, Jarvis W R. Secular trends in the epidemiology of nosocomial fungal infections in the United States, 1980–1990. National Nosocomial Infections Surveillance. Syst J Infect Dis. 1993;167:1247–1251. doi: 10.1093/infdis/167.5.1247. [DOI] [PubMed] [Google Scholar]
- 2.Belvin P M, Anderson K V. A conserved signaling pathway: the Drosophila Toll-dorsal pathway. Annu Rev Cell Dev Biol. 1996;12:393–416. doi: 10.1146/annurev.cellbio.12.1.393. [DOI] [PubMed] [Google Scholar]
- 3.Cenci E, Menacci A, Fe d'Ostiani C, Montagnoli C, Bacci A, Del Sero G, Perito S, Bistoni F, Romani L. Cytokine and T-helper-dependent immunity in murine aspergillosis. Res Immunol. 1998;149:445–453. doi: 10.1016/s0923-2494(98)80768-2. [DOI] [PubMed] [Google Scholar]
- 4.Cenci E, Menacci A, Fe d'Ostiani C, Del Sero G, Mosci P, Montagnoli C, Bacci A, Romani L. Cytokine and T-helper-dependent lung mucosal immunity in mice with invasive pulmonary aspergillosis. J Infect Dis. 1998;178:1750–1760. doi: 10.1086/314493. [DOI] [PubMed] [Google Scholar]
- 5.Chaudhary B, Singh B. Role of endotoxin of Aspergillus fumigatus in its pathogenicity. Mykosen. 1983;26:430–434. [PubMed] [Google Scholar]
- 6.Denning D W. Invasive aspergillosis. Clin Infect Dis. 1998;26:781–805. doi: 10.1086/513943. [DOI] [PubMed] [Google Scholar]
- 7.Diamond R, Krzesicki R, Epstein B, Jao W. Damage to hyphal forms of fungi by human leukocytes in vitro. Am J Pathol. 1978;91:313–328. [PMC free article] [PubMed] [Google Scholar]
- 8.Epstein J, Eichbaum Q, Sheriff S, Ezekowitz R A. The collectins in innate immunity. Curr Opin Immunol. 1996;8:29–35. doi: 10.1016/s0952-7915(96)80101-4. [DOI] [PubMed] [Google Scholar]
- 9.Flo T H, Halaas Ø, Lien E, Ryan L, Teti G, Golenbock D T, Sundan A, Espevik T. Human toll-like receptor 2 mediates monocyte activation by Listeria monocytogenes, but not group B streptococci or lipopolysaccharide. J Immunol. 2000;164:2064–2069. doi: 10.4049/jimmunol.164.4.2064. [DOI] [PubMed] [Google Scholar]
- 10.Fraser I P, Koziel H, Ezekowitz R A. The serum mannose-binding protein and the macrophage mannose receptor are pattern recognition molecules that link innate and adaptive immunity. Semin Immunol. 1998;10:363–372. doi: 10.1006/smim.1998.0141. [DOI] [PubMed] [Google Scholar]
- 11.Groll A H, Shah P M, Mentzel C, Schneider M, Just-Nuebling G, Huebner K. Trends in the postmortem epidemiology of invasive fungal infections at a university hospital. J Infect. 1996;33:23–32. doi: 10.1016/s0163-4453(96)92700-0. [DOI] [PubMed] [Google Scholar]
- 12.Hearn V M, Sietsma J H. Chemical and immunological analysis of the Aspergillus fumigatus cell wall. Microbiology. 1994;140:789–795. doi: 10.1099/00221287-140-4-789. [DOI] [PubMed] [Google Scholar]
- 13.Kozel T R, Wilson M A, Farrell T P, Levitz S M. Activation of C3 and binding to Aspergillus fumigatus conidia and hyphae. Infect Immun. 1989;57:3412–3417. doi: 10.1128/iai.57.11.3412-3417.1989. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Kozel T R. Activation of the complement system by pathogenic fungi. Clin Microbiol Rev. 1996;9:34–46. doi: 10.1128/cmr.9.1.34. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Lemaitre B, Nicolas E, Michaut L, Reichhart J M, Hoffmann J A. The dorsoventral regulatory gene cassette spatzle/Toll/cactus controls the potent antifungal response in Drosophila adults. Cell. 1996;86:973–983. doi: 10.1016/s0092-8674(00)80172-5. [DOI] [PubMed] [Google Scholar]
- 16.Levitz S M, Selsted M E, Ganz T, Lehrer R I, Diamond R D. In vitro killing of spores and hyphae of Aspergillus fumigatus and Rhizopus oryzae by rabbit neutrophil cationic peptides and bronchoalveolar macrophages. J Infect Dis. 1986;154:483–489. doi: 10.1093/infdis/154.3.483. [DOI] [PubMed] [Google Scholar]
- 17.Lien E, Sellati T J, Yoshimura A, Flo T H, Rawadi G, Finberg R W, Carroll J D, Espevik T, Ingalls R R, Radolf J D, Golenbock D T. Toll-like receptor 2 functions as a pattern recognition receptor for diverse bacterial products. J Biol Chem. 1999;274:33419–33425. doi: 10.1074/jbc.274.47.33419. [DOI] [PubMed] [Google Scholar]
- 18.Matsuguchi T, Takagi K, Musikacharoen T, Yoshikai Y. Gene expressions of lipopolysaccharide receptors, toll-like receptors 2 and 4, are differently regulated in mouse T lymphocytes. Blood. 2000;95:1378–1385. [PubMed] [Google Scholar]
- 19.Medoff G, Kobayashi G S. Systemic fungal infections: an overview. Hosp Pract. 1991;26:41–52. doi: 10.1080/21548331.1991.11704143. [DOI] [PubMed] [Google Scholar]
- 20.Metzhitov R, Janeway C A., Jr Innate immunity. N Engl J Med. 2000;343:338–344. doi: 10.1056/NEJM200008033430506. [DOI] [PubMed] [Google Scholar]
- 21.Metzhitov R, Janeway C A., Jr Innate immunity: impact on the adaptive immune response. Curr Opin Immunol. 1997;9:4–9. doi: 10.1016/s0952-7915(97)80152-5. [DOI] [PubMed] [Google Scholar]
- 22.Metzhitov R, Preston-Hurlburt P, Janeway C A., Jr A human homologue of the Drosophila Toll protein signals activation of adaptive immunity. Nature. 1997;388:394–397. doi: 10.1038/41131. [DOI] [PubMed] [Google Scholar]
- 23.Mokuno Y, Matsuguchi T, Takano M, Nishimura H, Washizu J, Ogawa T, Takeuchi O, Akira S, Nimura Y, Yoshikai Y. Expression of toll-like receptor 2 on γδ T cells bearing invariant Vγ6/Vδ1 induced by Escherichia coli infection in mice. J Immunol. 2000;165:931–940. doi: 10.4049/jimmunol.165.2.931. [DOI] [PubMed] [Google Scholar]
- 24.Mosmann T. Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. J Immunol Methods. 1983;65:55–63. doi: 10.1016/0022-1759(83)90303-4. [DOI] [PubMed] [Google Scholar]
- 25.Ogata H, Su I, Miyake K, Nagai Y, Akashi S, Mecklenbrauker I, Rajewsky K, Kinoto M, Tarakhovsky A. The toll-like receptor protein RP105 regulates lipopolysaccharide signaling in B cells. J Exp Med. 2000;192:23–29. doi: 10.1084/jem.192.1.23. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Perera P-Y, Qureshi N, Christ W J, Stütz P, Vogel S N. Lipopolysaccharide and its analog antagonists display differential serum factor dependencies for induction of cytokine genes in murine macrophages. Infect Immun. 1998;66:2562–2569. doi: 10.1128/iai.66.6.2562-2569.1998. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Poltorak A, He X, Smirnova I, Liu M Y, Huffel C V, Du X, Birdwell D, Alejos E, Silva M, Galanos C, Freudenberg M, Ricciardi-Castagnoli P, Layton B, Beutler B. Defective LPS signaling in C3H/HeJ and C57BL/10ScCr mice: mutations in Tlr4 gene. Science. 1998;282:2085–2088. doi: 10.1126/science.282.5396.2085. [DOI] [PubMed] [Google Scholar]
- 28.Rex J H, Bennett J E, Gallin J I, Malech H L, DeCarlo E S, Melnick D A. In vivo interferon-gamma therapy augments the in vitro ability of chronic granulomatous disease neutrophils to damage Aspergillus hyphae. J Infect Dis. 1991;163:849–852. doi: 10.1093/infdis/163.4.849. [DOI] [PubMed] [Google Scholar]
- 29.Roilides E, Uhlig K, Venzon D, Pizzo P A, Walsh T J. Enhancement of oxidative response and damage caused by human neutrophils to Aspergillus fumigatus hyphae by granulocyte colony-stimulating factor and gamma interferon. Infect Immun. 1993;61:1185–1193. doi: 10.1128/iai.61.4.1185-1193.1993. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Roilides E, Dimitriadou A, Kadiltsoglou I, Sein T, Karpouzas J, Pizzo P A, Walsh T J. IL-10 exerts suppressive and enhancing effects on antifungal activity of mononuclear phagocytes against Aspergillus fumigatus. J Immunol. 1997;158:322–329. [PubMed] [Google Scholar]
- 31.Schaffner A, Douglas H, Braude A I. Selective protection against conidia by mononuclear and against mycelia by polymorphonuclear phagocytes in resistance to Aspergillus: observations on these two lines of defense in vivo and in vitro with human and mouse phagocytes. J Clin Investig. 1982;69:617–631. doi: 10.1172/JCI110489. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Shimazu R, Akashi S, Ogata H, Nagai Y, Fukudome K, Miyake K, Kimoto M. MD-2, a molecule that confers lipopolysaccharide responsiveness on toll-like receptor 4. J Exp Med. 1999;189:1777–1782. doi: 10.1084/jem.189.11.1777. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Solberg R, Scholz T, Videm V, Okkenhaug C, Aasen A O. Heparin coating reduces cell activation and mediator release in an in vitro venovenous bypass model for liver transplantation. Transplant Int. 1998;11:252–258. doi: 10.1007/s001470050137. [DOI] [PubMed] [Google Scholar]
- 34.Takeuchi O, Hoshino K, Kawai T, Sanjo H, Takada H, Ogawa T, Takeda K, Akira S. Differential roles of TLR2 and TLR4 in recognition of gram-negative and gram-positive bacterial cell wall components. Immunity. 1999;11:443–451. doi: 10.1016/s1074-7613(00)80119-3. [DOI] [PubMed] [Google Scholar]
- 35.Taramelli D, Malabarba M G, Sala G, Basilico N, Cocuzza G. Production of cytokines by alveolar and peritoneal macrophages stimulated by Aspergillus fumigatus conidia or hyphae. J Med Vet Mycol. 1996;34:49–56. [PubMed] [Google Scholar]
- 36.Waldorph A R, Levitz S M, Diamond R D. In vivo bronchoalveolar macrophage defense against Rhizopus oryzae and Aspergillus fumigatus. J Infect Dis. 1984;120:752–760. doi: 10.1093/infdis/150.5.752. [DOI] [PubMed] [Google Scholar]
- 37.Walsh T J. Invasive aspergillosis in patients with neoplastic diseases. Semin Respir Infect. 1990;5:111–122. [PubMed] [Google Scholar]
- 38.Wang J E, Solberg R, Okkenhaug C, Jørgensen P F, Krohn C D, Aasen A O. Cytokine modulation in experimental endotoxemia: characterization of an ex vivo whole blood model. Eur Surg Res. 2000;32:65–73. doi: 10.1159/000008743. [DOI] [PubMed] [Google Scholar]
- 39.Wang J E, Jørgensen P F, Almlöf M, Thiemermann C, Foster S J, Aasen A O, Solberg R. Peptidoglycan and lipoteichoic acid from Staphylococcus aureus induce tumor necrosis factor alpha, interleukin 6 (IL-6), and IL-10 production in both T cells and monocytes in a human whole blood model. Infect Immun. 2000;68:3965–3970. doi: 10.1128/iai.68.7.3965-3970.2000. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Wright S D, Ramos R A, Tobias P S, Ulevitch R J, Mathieson J C. CD14, a receptor for complexes of lipopolysaccharide (LPS) and LPS binding protein. Science. 1990;249:1431–1433. doi: 10.1126/science.1698311. [DOI] [PubMed] [Google Scholar]