Abstract
Purpose:
Transgender and gender nonconforming (TGNC) individuals have difficulty accessing mental health professionals (MHPs) prepared to deliver culturally informed care. This study aims to (1) explore the training experiences that had been available to MHPs who are actively providing care to TGNC individuals, (2) define which opportunities had been most beneficial in TGNC career development, and (3) determine the reasons MHPs sought training when it was absent in graduate curricula.
Methods:
A voluntary cross-sectional electronic survey was distributed through professional Listservs and public referral lists to interdisciplinary MHPs, who self-identified as having experience in providing care to TGNC individuals.
Results:
Two hundred eighty-one (n=281) counselors, marriage/family therapists, social workers, psychologists, psychiatrists, or psychiatric nurse practitioners responded to the survey. The two most common motivators for seeking training in gender-affirming care were filling a need in the community (68.8%) and having met a TGNC person in a clinical setting, who requested care (67.2%). Only 20.0% of our sample were exposed to relevant content in a graduate course, and 25.2% during clinical training. The most commonly available training opportunities were professional conferences (76.4%) and mentorship (41.2%). Respondents were most likely to recommend that others in their field be trained through structured clinical experience.
Conclusion:
This study identifies key strategies for graduate and post-graduate educators to better prepare MHPs to serve TGNC individuals. Wider availability of structured clinical experiences, didactic content delivered during graduate school or at professional conferences, and direct clinical mentorship will increase access to welcome and prepared mental health care providers for the TGNC population.
Keywords: education, gender dysphoria, graduate, mental health, training, transgender
Introduction
Transgender and gender nonconforming (TGNC) individuals face significant stress, abuse, harassment, rejection, discrimination, and violence.1,2–6 As a result of this,7 TGNC individuals are disproportionately affected by poor mental health,8–10 depression,3–5,9,11 anxiety,11 post-traumatic stress disorder,9 substance use disorders,1 and suicidal ideation/attempts.1–5,9 While many TGNC individuals and communities have developed resiliency strategies and peer support systems that can be protective,12,13 professional mental health services may still be required to address mental health needs.
The disproportionate burden of mental illness is not matched by proportional access to appropriate mental health care.14,15 There are frequently financial, insurance-related, and/or logistical barriers,14–19 including in the United States where insurance coverage is inconsistent. Even when financial or logistical barriers are not present, stigma and fear of refusal of services or of discriminatory experiences may prevent individuals from seeking care.18,20 Despite three consecutive studies, each about two decades apart, demonstrating progressively less trans-negative attitudes in mental health professionals (MHPs),21–23 and evidence that there is less transphobia in MHPs compared to the general population,23–26 and to other health professionals,22 instances of transphobia in mental health care persist.2,6,16,27 Previous bad experiences with MHPs have led many TGNC individuals to avoid seeking mental health care even when they are suffering,15,18,27 which can have devastating implications.
Some TGNC individuals continue to seek out mental health care despite fear because this care may be required to access medical or surgical interventions. MHPs are still sometimes placed in “gatekeeper” positions: a letter from an MHP asserting that a person meets the criteria for gender dysphoria and that any mental health conditions they have is “reasonably well controlled” may still be required to initiate treatment.28 Hormones and surgical interventions have overwhelmingly been shown to improve well-being in TGNC individuals,29 and accessing these services is often the reason that TGNC individuals risk contact with a medical system in which they previously had negative experiences.6 The gatekeeper role of MHPs may also interfere with mental health treatment; some TGNC individuals have described not feeling safe to be fully transparent about mental health symptoms if this information could be used to deny access to the care, which might alleviate some of their distress.30
Once TGNC individuals overcome the significant barriers to accessing professional mental health care, many MHPs who would willingly provide this care are ill prepared to do so.23,31,32 Qualitative studies of TGNC experiences in professional mental health care have described instances of the client needing to educate their MHP on terminology or issues relevant to the broader TGNC experience to explain the context of their symptoms.27,33–36 Also, even though many TGNC individuals will seek mental health care for the same reasons that cisgender individuals do (such as stress, relationship issues, depression, or anxiety),18,27,33 many have described bothersome instances of their MHP focusing too much on gender when that was not their goal for psychotherapy.30,36 Others who wanted to explore gender identity described avoidance of the subject by MHPs who felt unprepared to address gender concerns.36 MHPs who are prepared to deliver appropriate affirmative care describe feeling unable to meet the volume of the demand due to the limited size of the workforce of experienced affirmative providers.37
Recent work demonstrates that counselors describe rare didactic or supervised clinical exposure in training to the care of TGNC individuals.31 All research exploring curricula combines content about lesbian, gay, bisexual (LGB), and TGNC mental health, despite work showing that many health professionals are significantly less comfortable treating TGNC individuals than cis-gender LGB individuals.38 Therefore, it is unknown what amount of time is dedicated specifically to TGNC mental health. There are no studies clarifying which teaching methods or training opportunities best inspire individuals to serve TGNC individuals, and studies on the outcomes of training curricula/programs examine only short-term knowledge or attitude changes.39–44
Given that TGNC individuals are becoming an increasingly large proportion of the population,45 and because initiation of medical or surgical transition sometimes still requires ongoing mental health care, providing targeted training to MHPs is critical to improve access to competent gender-affirming mental health care. This study aims to (1) explore the training experiences that had been available to MHPs who are actively providing care to TGNC individuals, (2) define which opportunities had been most beneficial in TGNC career development, and (3) determine the reasons that MHPs sought additional training when it was absent in graduate curricula. This information could help illuminate the highest-yield training methods for inclusion in limited curricular schedules.
Methods
To gather information from gender-affirming care providers, the study team developed an online, anonymous, cross-sectional survey. Face validity of the survey was established by a panel of experts, which included physicians who are involved with TGNC care as both primary care providers and psychiatrists. Face validity has been established as an important feature of surveys.46 The survey was distributed to health care professionals with experience in providing care to TGNC individuals through email, professional contacts (colleagues of the investigators at other institutions), and one or two emails sent out through Listservs (such as the list serve for the World Professional Association of Transgender Health [WPATH] and an LGBT Mental Health professional Listserv), and single emails were sent to publicly available lists of gender-affirming care providers; SurveyMonkey™ was used to create the survey and gather responses. We chose emailing the survey not only because of cost-effectiveness and quick response turnaround47 but also because of the potential for a wider geographic reach; the survey was not restricted to US-based professionals, and the link was kept active for 5 months (3 months after the last invitation email was sent). In the email invitation, participants were encouraged to forward the survey to interdisciplinary colleagues with gender-affirming care experience. The study was reviewed by the University of Cincinnati Institutional Review Board and was considered nonhuman subject research.
To participate, respondents needed to have self-described experience in providing care to TGNC individuals. There were no minimum criteria for length or volume of their experience and no requirement that the individual meets knowledge standards in gender-affirming care; this was intentional so as to include a range of professionals actively providing care, including trainees with clinical experience, recent graduates, those new to gender-affirming care, and those with a lower volume of TGNC clients, but who are nevertheless offering these services outside of settings that emphasize this care. Physicians, nurse practitioners, and physician assistants were included if they described their specialty as “psychiatry” and described providing psychopharmacology services and/or psychotherapy; those choosing other specialties were not included. Master's level social workers and individuals writing in comments that they have a doctorate in a field other than psychology were included only if they provided “psychotherapy or mental health diagnosis/assessment.” Because some respondents chose multiple overlapping job descriptions related to inconsistent titles/licensing across states lines, interprofessional colleagues of the authors were consulted when recategorization or clarification was warranted. The results described in this study are limited to the responses of MHP respondents; results from advance practice nurses, physician assistants, and physicians of all specialties have previously been described.48 Individuals who did not respond to the complete set of questions central to our objectives were excluded from the final analysis.
The survey instrument collected information on respondents' (1) professional credentials and, when applicable, specialty; (2) the services they personally provide from a list of interdisciplinary team services; (3) geographic location (country and, when in United States, state); (4) practice setting/type; (5) years and volume of experience working with TGNC individuals; (6) motivations for seeking training in gender-affirming care; (7) previous access to training opportunities in gender-affirming care; and (8) recommendations for training others with their credentials to care for TGNC individuals.
We used Grubb's procedure to identify any outliers before dichotomization of variables.49 No outliers were found. Little's MCAR test was used to check whether our data were missing at random.50 Results from this test revealed that data were missing completely at random (p=0.320). Survey data were analyzed using descriptive analyses (e.g., frequencies and proportions), and were performed using Microsoft Excel™. All analyses were two tailed in nature and the level of significance was set at p<0.05.
Results
Respondent characteristics
Of the 473 interdisciplinary respondents to the survey, 281 (59.4%) were MHPs (psychiatric social workers, counselors, marriage/family therapists, psychologists, psychiatrists, or psychiatric nurse practitioners). Thirty-nine individuals provided incomplete survey responses, 10 of whom failed to provide full demographic information and 29 of whom did not provide answers to the questions key to the objectives; these 29 were excluded from the final analysis, yielding 250 respondents. Approximately one-third (n=78, 31.3%) of respondents indicated that at least half of their panel identified as TGNC, and more than a third (n=89, 35.7%) reported that they had been providing care for TGNC individuals for a decade or more (see Table 1 for more respondent characteristics).
Table 1.
Characteristics of Survey Respondents
| n | Total responses | % | |
|---|---|---|---|
| Job descriptiona | |||
| Counselorb | 51 | 250 | 20.4 |
| Marriage/Family Therapistb | 23 | 9.2 | |
| Social Workerb | 63 | 25.2 | |
| Psychology (PhD) | 55 | 22.0 | |
| Psychology (PsyD) | 25 | 10.0 | |
| Other doctorate-level psychotherapist (PhD or EdD) | 10 | 4.0 | |
| Psychiatrist | 21 | 8.4 | |
| Psychiatric nurse practitioner | 2 | 0.8 | |
| Years in practice | |||
| Still in training | 7 | 249 | 2.8 |
| 0–4.9 Years | 53 | 21.3 | |
| 5–9.9 Years | 50 | 20.1 | |
| 10–19.9 Years | 63 | 25.3 | |
| 20 Years or more | 76 | 30.5 | |
| Years providing care to TGNC individuals | |||
| 0–4.9 Years | 98 | 249 | 39.4 |
| 5–9.9 Years | 62 | 24.9 | |
| 10 Years or more | 89 | 35.7 | |
| Estimated percentage of client panel that identifies as TGNC | |||
| <5% | 64 | 249 | 25.7 |
| 5–24.9% | 70 | 28.1 | |
| 25–49.9% | 37 | 14.9 | |
| 50% or more | 78 | 31.3 | |
When multiple job descriptions/degrees were chosen, the highest level degree was used for categorization.
Master's level.
TGNC, transgender and gender nonconforming.
The majority (n=243, 97.2%) of the providers worked within the United States, with distribution across 42 of the 50 states and within the District of Columbia; all major geographic census regions were represented. Most respondents (n=153, 62.2%) worked in urban settings, while a significant minority (n=18, 7.3%) worked in rural areas. Most (n=167, 66.8%) described working in a private outpatient mental health practices, with others describing working in academic settings (n=28, 11.2%), outpatient community mental health (n=27, 10.8%), primary care offices (n=25, 10.0%), or an interdisciplinary program/office dedicated to serving LGB, and transgender individuals (n=20, 8.0%). Over 80% of respondents served individuals 19–59 years old, with less serving those who were above or below these age ranges (Table 2). Self-pay or private insurance was most likely to be accepted by the respondents. Some respondents also wrote in additional payment methods: 9 (3.7%) described out-of-network payment structures, 8 (3.3%) described offering a sliding scale, and 34 (14.0%) described that their services were free to eligible individuals who did not have insurance (e.g., veterans, students, and residents).
Table 2.
Settings in Which Respondents Work
| n | Total responses | % | |
|---|---|---|---|
| In which settings do you currently work?a | |||
| Urban | 153 | 246 | 62.2 |
| Suburban | 58 | 23.6 | |
| Town | 26 | 10.6 | |
| Rural | 18 | 7.3 | |
| In which types of practices do you work?a | |||
| Outpatient private mental health practice | 167 | 250 | 66.8 |
| Academic setting (university-affiliated hospital or office) | 28 | 11.2 | |
| Outpatient community mental health center | 27 | 10.8 | |
| Outpatient primary care office | 25 | 10.0 | |
| Interdisciplinary LGBT office/program | 20 | 8.0 | |
| Active military or veteran-serving government-run hospital/outpatient office | 19 | 7.6 | |
| Other outpatient specialty office or services (excluding mental health) | 16 | 6.4 | |
| Inpatient mental health setting | 7 | 2.8 | |
| Inpatient medical setting | 7 | 2.8 | |
| Inpatient consultation | 6 | 2.4 | |
| Outpatient women's health center | 6 | 2.4 | |
| Surgical setting (outpatient consults with inpatient procedures) | 4 | 1.6 | |
| Outpatient university student health office | 2 | 0.8 | |
| Other | 18 | 7.2 | |
| Which types of insurance does your office accept?b | |||
| Self-pay | 172 | 243 | 70.8 |
| Private insurance | 130 | 53.5 | |
| State-sponsored public insurance | 91 | 37.4 | |
| Medicare | 72 | 29.6 | |
| Uninsured | 63 | 25.9 | |
| I do not know | 11 | 4.5 | |
| What age groups do you provide care for?a | |||
| 18 Years of age or younger | 141 | 249 | 56.6 |
| 19–25 Years of age | 206 | 82.7 | |
| 26–59 Years of age | 217 | 87.1 | |
| 60 Years of age and older | 150 | 60.2 | |
Choose all that apply.
Choose all that apply, only for those who practice within the United States.
Motivations for seeking training
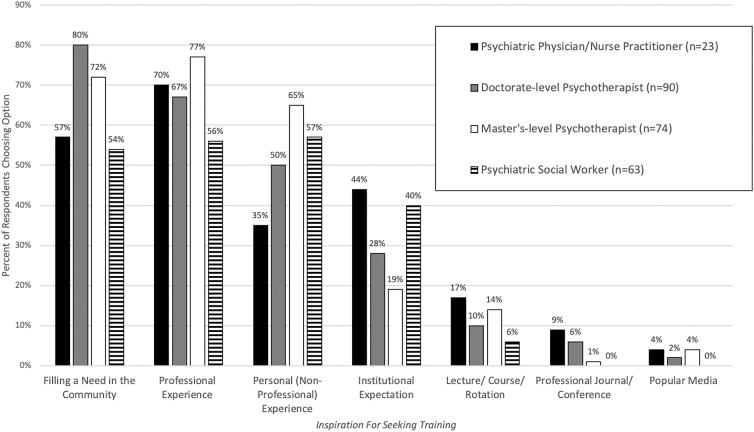
The two most common motivators for providers having sought training in gender-affirming care were filling a need in the community (n=172, 68.8%) and/or seeking to learn more after having met a transgender person in a clinical setting who requested this care (n=168, 67.2%) (Figs. 1 and 2). Slightly more than half (n=137, 54.8%) indicated that personally knowing (or being) a person with TGNC experience motivated them to seek training in gender-affirming care. Only a small portion (n=27, 10.8%) reported having been inspired to seek out this training due to a lecture, course, or rotation, while they were in graduate school or during training, and only 3.2% (n=8) were motivated to expand their set by a presentation at a professional conference or an article in a professional journal. Several psychiatrists cited information/education provided through the Association of Gay and Lesbian Psychiatrists as an influential source in the comments section.
FIG. 1.
Reasons MHPs sought training in affirmative care (choose all that apply). MHP, mental health professional.
FIG. 2.
Reasons MHPs sought training in affirmative care (choose all that apply) by training background.
Training opportunities
Seventeen individuals (6.8%) described being exclusively self-taught without access to any other opportunities, while many more (n=202, 80.8%) indicated being in part (or initially) self-taught, but that they had been able to supplement self-study with other opportunities (Table 3); nine wrote in the comments that they now teach/train others. The opportunities most commonly available were professional conferences (n=191, 76.4%) and mentorship (n=103, 41.2%). In fact, while most (n=208, 83.2%) had access to conferences and/or mentorship, a third (n=86, 34.4%) described having had access to both conferences and mentorship. Among the conferences that MHPs specifically named in comments, the Philadelphia Trans Wellness Conference (PTWC) and the WPATH Global Education Initiative (GEI) courses were the most commonly named (PTWC was mentioned three times and GEI 13 times). Only one in five (n=50, 20.0%) respondents described access to gender-affirmative care training within a graduate course, but one in four (n=63, 25.2%) described training during internship, residency, or fellowship (responses were combined in an effort to bridge differences in terminology for clinical training across professions). In addition, several respondents (n=8) wrote in the comments that they had learned about gender-affirming care from the experiences of their clients, friends/family, or their own experiences as a TGNC individual. See Figure 3 for those opportunities available to different groups of MHPs.
Table 3.
Training Opportunities Available to Respondents
| Opportunity | Respondents reporting exposure to this opportunity (choose all that apply) |
Respondents choice for which was the most helpful opportunity they had exposure to (choose one only) |
||
|---|---|---|---|---|
| n | Percent of total respondents reporting having been able to access this opportunity | n | Percent of those who reported exposure to this opportunity that chose it as the single most helpful opportunity for their career development | |
| Self-study of literature or guidelines (along with other opportunities)a | 202 | 80.8 | 51 | 25.2 |
| Professional conference | 191 | 76.4 | 79 | 41.4 |
| Mentorship | 103 | 41.2 | 40 | 38.8 |
| On-site training provided by employer | 72 | 28.8 | 25 | 34.7 |
| Training during internship | 51 | 20.4 | 22 | 43.1 |
| Graduate course | 50 | 20.0 | 6 | 12.0 |
| Training during fellowship | 16 | 6.4 | 4 | 25 |
| Training during residency | 14 | 5.6 | 1 | 7.1 |
| Undergraduate course | 6 | 2.4 | 1 | 16.7 |
Seventeen individuals were exclusively self-taught and are not included in this table.
FIG. 3.
Types of training opportunities available to types of MHPs (choose all that apply).
When asked to choose the most helpful of available opportunities, training during internship was most likely to be recommended, with 43.1% of those who had this opportunity describing this as the single most helpful method they had access to (22 of 51 respondents). Seventy-nine of the 191 (41.4%) of those who had attended a professional conference cited this training opportunity as the most helpful, and 40 who had mentorship (n=103, 38.8% of those who had engaged in this opportunity) identified this as the most helpful. Around 42.9% (n=27 of 63) of those who had training during clinical training (internship, residency, or fellowship) reported that this had been the most helpful of the opportunities they had (all 63 of these reported having had access to at least one other opportunity).
Training recommendations
When respondents were asked to recommend the top training method for future providers in their profession (whether or not they had personally experienced this training method), respondents were most likely to recommend clinical experience (e.g., a rotation or longitudinal exposure during training; n=65, 26.0%), followed by a professional conference (n=36, 14.4%) and mentorship (n=31, 12.4%) (Fig. 4). Twenty-nine individuals (11.6%) chose “other” and wrote in responses; 19 of these 29 wrote in some combination of the available options or “all of the above.” The difference between groups' recommendations for how to train others in their field is described in Figure 5.
FIG. 4.
Results of all MHP respondents: What would be the most effective way to train interested professionals/students within your field to provide affirmative care to TGNC individuals? (choose one). TGNC, transgender and gender nonconforming.
FIG. 5.
Results by training background: What would be the most effective way to train interested professionals/students within your field to provide affirmative care to TGNC individuals? (choose one). The 29 respondents who chose “other” are not included.
Discussion
TGNC individuals often have difficulties accessing professional mental health care that is prepared to meet their needs. A deficiency of gender-affirming content in the formal training of MHPs contributes to the insufficient size of the workforce to competently serve this population. Consistent with other work,31 only a minority of MHPs in our sample were exposed to relevant content in a graduate course (20.0%) or during clinical training (25.2%), although a majority (93.2%) of MHPs providing gender-related care report having successfully accessed some form of training during their career.
To date, the only other similar survey of MHPs' training experiences in gender-affirming care sampled a nontargeted group of 304 interdisciplinary Australian MHPs.51 In that survey, while the majority (64.5%) of MHPs reported that they had provided care for a TGNC adult during their career, only 25.3% reported any prior training in gender-affirming care.51 A distinct difference in our survey sample is that our sampling focused on those MHPs who self-identified as providing gender-affirming care, which likely explains the higher percentage reporting prior training (93.2% vs. 25.3%). No similar large-scale, interdisciplinary survey has been done to assess US-based MHPs' training experiences.
MHPs in our study most commonly gained knowledge and skills through a combination of self-study, conferences, and mentorship, but were most likely to recommend training others through clinical experiences, didactic content at conferences, and mentorship (which could be provided through supervised clinical experiences during training). Their recommendations for clinical exposure as a critical component to professional development and skill acquisition are consistent with recent work demonstrating MHPs had higher levels of knowledge, confidence, and comfort in working with TGNC individuals when training occurred through clinical work51 Other work has also shown that among medical students, clinical care opportunities are important features of training that can build upon didactic knowledge,52 and that a combination of didactic sessions, case discussion, and expert consultation is acceptable to practicing MHPs.53 These modalities could be combined into graduate training programs, similar to that discussed by Fisher et al.54
MHPs in this study were inspired to seek out additional training/information by a desire to fill an unmet need for this care in the community (68.8%), to augment their own professional skills/knowledge after a TGNC client requested their services (67.2%), or because they had a personal connection with someone who identifies as TGNC (54.8%). Previous work has demonstrated that personal contact with someone with TGNC experience is associated with higher self-described competence to provide affirmative care in MHPs.31 This suggests that educating students and trainees on the barriers TGNC individuals face in accessing services could serve to inspire the MHP to learn gender-affirming care principles and continue working with this population throughout their careers.
A limitation of this study is the inability to measure a response rate; because the invitation was sent out through professional Listservs with unknown total membership and participants were invited to share the survey with colleagues, it is unknown to how many people the survey was sent. Since this survey represents a convenience sample, there may be overrepresentation of some groups based on the geographic and specialty networks of the study team. Because participation was voluntary and electronically distributed, there may have been selection bias in who decided to contribute responses. Finally, because there was no way to confirm the knowledge, practices, competence, attitudes, or biases of the participants, there may have been respondent bias. Because of some of these limitations, the practice patterns and training experiences described by this sample cannot be used to define the larger MHP workforce.
The results of this study provide the perspective of experienced gender-affirming care MHPs on how best to prepare trainees or other professionals to develop their skill sets; this could better prepare graduate and post-graduate educators to incorporate didactic content and clinical experiences relevant to the care of TGNC individuals into curricula. Based on the assessments of motivators and training recommendations, MHP training experiences that involve clinical encounters with TGNC persons, mentorship, and opportunities for self-directed learning are best suited for increasing competency in gender-affirming care.
Future work should clarify the ideal timing for training experiences within various MHP training programs. In addition, further exploration of which experiences reduce transphobia in MHPs would be crucial so that these trainings/experiences can be integrated early into training before clinical interactions begin; we know the prior education is correlated with lower transphobia and data suggest that even a 40-min webinar can reduce short-term transphobia scores,39 but getting more detail about which educational modalities can accomplish this is critical. A survey of volume and content related to TGNC in different graduate curricula could also be enlightening and could augment self-report of curricular experiences. Recruiting and better preparing MHPs to join the gender-affirming care workforce will increase access to essential mental health services and promote wellbeing in TGNC individuals.
Conclusion
Most MHPs did not learn to provide gender-affirming care during their own graduate-level training. Those who had access to training during an internship experience were most likely to cite that experience as the single most helpful experience for their career development. More professional structured clinical learning experiences for trainees, training during a graduate school course, and content shared within a professional conference were recommended methods. Because filling a need in the community and professional contact with TGNC individuals were common motivators for seeking additional training, exposure to these opportunities early in training could serve to motivate students early in their careers to serve this population when they have completed their training.
Abbreviations Used
- GEI
Global Education Initiative
- LGB
lesbian, gay, bisexual
- MHP
mental health professional
- PTWC
Philadelphia Trans Wellness Conference
- TGNC
Transgender and gender nonconforming
- WPATH
World Professional Association of Transgender Health
Author Disclosure Statement
No competing financial interests exist.
Funding Information
No funding was received for this article.
Cite this article as: Stryker SD, Pallerla H, Yockey RA, Bedard-Thomas J, Pickle S (2022) Training mental health professionals in gender-affirming care: a survey of experienced clinicians, Transgender Health 7:1, 68–77, DOI: 10.1089/trgh.2020.0123.
References
- 1. Xavier JM, Bobbin M, Singer B, Budd E. A needs assessment of transgendered people of color living in Washington, DC. Int J Transgenderism. 2005;8:31–47. [Google Scholar]
- 2. Grant JM, Mottet LA, Tanis J, et al. Injustice at Every Turn: A Report of the National Transgender Discimination Survey. Washington, DC: National Center for Transgender Equality and National Gay and Lesbian Task Force, 2010. [Google Scholar]
- 3. Nuttbrock L, Hwahng S, Bockting W, et al. Psychiatric impact of gender-related abuse across the life course of male-to-female transgender persons. J Sex Res. 2010;47:12–23. [DOI] [PubMed] [Google Scholar]
- 4. Valentine SE, Shipherd JC. A systematic review of social stress and mental health among transgender and gender non-conforming people in the United States. Clin Psychol Rev. 2018;66:24–38. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Su D, Irwin JA, Fisher C, et al. Mental Health Disparities Within the LGBT Population: a Comparison Between Transgender and Nontransgender Individuals. Transgender Health. 2016;1:12–20. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. James SE, Herman JL, Rankin S, et al. The Report of the 2015 U.S. Transgender Survey. Washington, DC: National Center for Transgender Equality, 2016. [Google Scholar]
- 7. Meyer IH. Minority stress and mental health in gay men. J Health Soc Behav. 1995;36:38–56. [PubMed] [Google Scholar]
- 8. Rider GN, Mcmorris BJ, Gower AL, et al. Health and care utilization of transgender and gender nonconforming youth: a population-based study. Pediatrics. 2018;141:e20171683. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Brown GR, Jones KT. Mental health and medical health disparities in 5135 transgender veterans receiving healthcare in the Veterans Health Administration: a case–control study. LGBT Health. 2016;3:122–131. [DOI] [PubMed] [Google Scholar]
- 10. Reisner SL, Poteat T, Keatley JA, et al. Global health burden and needs of transgender populations: a review. Lancet. 2016;388:412–436. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Bockting WO, Miner MH, Swinburne Romine RE, et al. Stigma, mental health, and resilience in an online sample of the US transgender population. Am J Public Health. 2013;103:943–951. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. Singh AA, Hays DG, Watson LS. Strength in the face of adversity: resilience strategies of transgender individuals. J Couns Dev. 2011;89:20–27. [Google Scholar]
- 13. Singh AA. Transgender youth of color and resilience: negotiating oppression and finding support. Sex Roles. 2013;68:690–702. [Google Scholar]
- 14. McCann E, Sharek D. Mental health needs of people who identify as transgender: a review of the literature. Arch Psychiatr Nurs. 2016;30:280–285. [DOI] [PubMed] [Google Scholar]
- 15. Simeonov D, Steele LS, Anderson S, Ross LE. Perceived satisfaction with mental health services in the lesbian, gay, bisexual, transgender, and transsexual communities in Ontario, Canada: an internet-based survey. Can J Community Ment Health. 2015;34:31–44. [Google Scholar]
- 16. Puckett JA, Cleary P, Rossman K, et al. Barriers to gender-affirming care for transgender and gender nonconforming individuals. Sex Res Soc Policy. 2018;15:48–59. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Noonan EJ, Sawning S, Combs R, et al. Engaging the transgender community to improve medical education and prioritize healthcare initiatives. Teach Learn Med. 2018;30:119–132. [DOI] [PubMed] [Google Scholar]
- 18. Shipherd JC, Green KE, Abramovitz S. Transgender clients: identifying and minimizing barriers to mental health treatment. J Gay Lesbian Ment Health. 2010;14:94–108. [Google Scholar]
- 19. White Hughto JM, Rose AJ, Pachankis JE, Reisner SL. Barriers to gender transition-related healthcare: identifying underserved transgender adults in Massachusetts. Transgender Health. 2017;2:107–118. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Applegarth G, Nuttall J. The lived experience of transgender people of talking therapies. Int J Transgenderism. 2016;17:66–75. [Google Scholar]
- 21. Green R, Stoller R, MacAndrew C. Attitudes toward sex transformation procedures. Arch Gen Psychiatry. 1966;15:178–182. [Google Scholar]
- 22. Franzini LR, Casinelli DL. Health professionals' factual knowledge and changing attitudes toward transsexuals. Soc Sci Med. 1986;22:535–539. [DOI] [PubMed] [Google Scholar]
- 23. Willoughby BLB, Hill DB, Gonzalez CA, et al. Who hates Gender outlaws? A multisite and multinational evaluation of the Genderism and Transphobia Scale. Int J Transgenderism. 2010;12:254–271. [Google Scholar]
- 24. Ali N, Fleisher W, Erickson J. Psychiatrists' and psychiatry residents' attitudes toward transgender people. Acad Psychiatry. 2016;40:268–273. [DOI] [PubMed] [Google Scholar]
- 25. Nisley EA. Counseling professionals' attitudes toward transgender people and responses to transgender clients. [PhD thesis]. Kalamazoo: Western Michigan University, 2010. [Google Scholar]
- 26. Brown S, Kucharska J, Marczak M. Mental health practitioners' attitudes towards transgender people: a systematic review of the literature. Int J Transgenderism. 2018;19:4–24. [Google Scholar]
- 27. McCullough R, Dispenza F, Parker LK, et al. The counseling experiences of transgender and gender nonconforming clients. J Couns Dev. 2017;95:423–434. [Google Scholar]
- 28. Coleman E, Bockting W, Botzer M, et al. Standards of care for the health of transsexual, transgender, and gender-nonconforming people, version 7. Int J Transgenderism. 2012;13:165–232. [Google Scholar]
- 29. Cornell University Public Policy Research Portal. What does the scholarly research say about the effect of gender transition on transgender well-being? https://whatweknow.inequality.cornell.edu/topics/lgbt-equality/what-does-the-scholarly-research-say-about-the-well-being-of-transgender-people Accessed June 13, 2020.
- 30. Carroll-Beight D, Larsson M. Exploring the needs, expectations, and realities of mental healthcare for transgender adults: a grounded theory study on experiences in Sweden. Transgender Health. 2018;3:88–104. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31. O'Hara C, Dispenza F, Brack G, Blood RAC. The preparedness of counselors in training to work with transgender clients: a mixed methods investigation. J LGBT Issues Couns. 2013;7:236–256. [Google Scholar]
- 32. Couture V. Counseling transgender college students: perceptions of college mental health clinicians' preparedness. Coll Stud J. 2017;51:463–472. [Google Scholar]
- 33. Benson KE. Seeking support: transgender client experiences with Mental Health Services. J Fem Fam Ther. 2013;25:17–40. [Google Scholar]
- 34. Baldwin A, Dodge B, Schick VR, et al. Transgender and genderqueer individuals' experiences with health care providers: what's working, what's not, and where do we go from here? J Health Care Poor Underserved. 2018;29:1300–1318. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35. Bess JA, Stabb SD. The experiences of transgendered persons in psychotherapy: voices and recommendations. J Ment Health Couns. 2009;31:264–282. [Google Scholar]
- 36. Mizock L, Lundquist C. Missteps in psychotherapy with transgender clients. Psychol Sex Orientat Gend Divers. 2016;3:148–155. [Google Scholar]
- 37. McIntyre J, Daley A, Rutherford K, Ross L. Systems-level barriers in accessing supportive mental health services for sexual and gender minorities: insights from the provider's perspective. Can J Community Ment Health. 2011;30:173–186. [Google Scholar]
- 38. Greene MZ, France K, Kreider EF, et al. Comparing medical, dental, and nursing students' preparedness to address lesbian, gay, bisexual, transgender, and queer health. PLoS One. 2018;13:71–81. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39. Mizock L, Hopwood R, Casey H, et al. The transgender awareness webinar: reducing transphobia among undergraduates and mental health providers. J Gay Lesbian Ment Health. 2017;21:292–315. [Google Scholar]
- 40. Lelutiu-Weinberger C, Pachankis JE. Acceptability and preliminary efficacy of a lesbian, gay, bisexual, and transgender-affirmative mental health practice training in a Highly Stigmatizing National Context. LGBT Health. 2017;4:360–370. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41. Pepping CA, Lyons A, Morris EMJ. Affirmative LGBT psychotherapy: outcomes of a therapist training protocol. Psychotherapy. 2018;55:52–62. [DOI] [PubMed] [Google Scholar]
- 42. Israel T, Willging CE, Ley D. Development and evaluation of training for rural LGBTQ mental health peer advocates. J Rural Ment Health. 2016;40:40–62. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43. Walch SE, Ngamake ST, Francisco J, et al. The attitudes toward transgendered individuals scale: psychometric properties. Arch Sex Behav. 2012;41:1283–1291. [DOI] [PubMed] [Google Scholar]
- 44. Bidell MP. Addressing disparities: the impact of a lesbian, gay, bisexual, and transgender graduate counselling course. Couns Psychother Res. 2013;13:300–307. [Google Scholar]
- 45. Zhang Q, Goodman M, Adams N, et al. Epidemiological considerations in transgender health: a systematic review with focus on higher quality data. Int J Transgender Health. 2020;21:125–137. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46. Nevo B. Face validity revisited. J Educ Meas. 1985;22:287–293. [Google Scholar]
- 47. Kent R, Brandal H. Improving email response in a permission marketing context. Int J Mark Res. 2003;45:1–13. [Google Scholar]
- 48. Stryker SD, Pallerla H, Pickle S. Considerations on medical training for gender-affirming care: motivations and perspectives. Int J Transgender Health. 2020;21:79–88. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49. Grubbs FE. Procedures for detecting outlying observations in samples. Technometrics. 1969;11:1–21. [Google Scholar]
- 50. Little RJA. A test of missing completely at random for multivariate data with missing values. J Am Stat Assoc. 1988;83:1198–1202. [Google Scholar]
- 51. Riggs DW. Australian mental health professionals' competencies for working with trans clients: a comparative study. Psychol Sex. 2016;7:225–238. [Google Scholar]
- 52. Park JA, Safer JD. Clinical exposure to transgender medicine improves students' preparedness above levels seen with didactic teaching alone: a Key Addition to the Boston University Model for Teaching Transgender Healthcare. Transgender Health. 2018;3:10–16. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53. Kauth MR, Shipherd JC, Lindsay JA, et al. Teleconsultation and training of VHA providers on transgender care: implementation of a Multisite Hub System. Telemed EHealth. 2015;21:1012–1018. [DOI] [PubMed] [Google Scholar]
- 54. Fisher WS, Hirschtritt ME, Haller E. Development and implementation of a residency area-of-distinction in lesbian, gay, bisexual, and transgender mental health. Acad Psychiatry. 2018;42:564–566. [DOI] [PMC free article] [PubMed] [Google Scholar]