Abstract
Study design
Meta-analysis.
Objective
To compare the clinical and radiological outcomes in patients with Adolescent Idiopathic scoliosis (AIS) treated by selective thoracic fusion (STF) with lowest instrumented vertebra (LIV) at touched vertebra (TV) vs stable vertebra (SV).
Methods
The databases PubMed, Embase and Google Scholar were searched until November 2020.Studies which had Lenke type 1 curves and Lenke type 2 curves in adolescent population treated by STF and which reported pre- and post-operative curve characteristics including correction percentage and complications were included. Studies which did not report the LIV selection, curve correction percentages and whose full text could not be acquired were excluded.
Results
Eight studies were included for analysis of which seven were found to be retrospective studies (level III evidence) and one was prospective study (level II evidence) each. Overall proportional meta-analysis found no significant difference in correction rate, total srs-22 scores, and complication rates.
Conclusion
The evaluation of SV group and TV group as LIV for selective thoracic fusions in AIS reveals a comparable outcome in terms of curve correction, patient satisfaction scores and complication rates. The TV can be chosen safely as the LIV especially in type A and B Lenke 1&2 curves, as it saves more motion segments when compared to SV.
Keywords: adolescent idiopathic scoliosis, Lenke 1 & 2 curves, Selective thoracic fusion, Stable vertebra, Touched vertebra
Introduction
Adolescent idiopathic scoliosis (AIS) curves are commonly classified according to the Lenke classification system. 1 Selective thoracic fusion (STF) is one of the surgical modalities to treat the Lenke type 1 and 2 curves. STF includes the fusion of the main thoracic curve ,and saves the motion segments of the lumbar spine.2‐4 Choosing a lower instrumented vertebra (LIV) too proximal may lead to decompensation and progression of unfused curves, whereas choosing a LIV too distal leads to reduced motion segments .Striking a perfect balance between saving the motion segments and preventing the curve decompensation is vital for superior post-operative outcomes.5,6 Majority of the surgeons believe fusion till stable vertebra (SV) is a safe option and is associated with good post-operative outcomes, but few recent studies have propagated that curves can be adequately treated by LIV proximal to SV. 7 Studies done by Lenke et al. showed that selecting the last touched vertebra (TV) as LIV in type 1 and type 2 curves led to good post-operative outcomes. Few other studies done by Cao et al. 8 and Matsumoto et al. 9 put forward the theory that TV can be a safe option to choose LIV in treating Lenke type 1 and type 2 curves. However, there is a lack of consensus in the literature with regards to selection of LIV while performing a STF.
The aim of this meta-analysis is to collect the existing scientific evidence from the literature and to compare the outcomes such as curve correction and clinical outcomes between the two groups which were divided based on LIV selection (TV vs SV). We have tried to incorporate all the available literature from the past two decades and have followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses guidelines to help improve the reporting quality of our study.
Methods
Literature Search
The search included extensive electronic and manual literature using PubMed, EMBASE and Google Scholar by two independent reviewers. The literature on target were the articles which reported the outcomes of selective thoracic fusion in AIS for Lenke curves 1 and 2 published from 2000 to 2020.Articles published in a language other than English were not included. Medical subject heading (MeSH) words used for search were ‘scoliosis’ and ‘Scoliosis/surgery’ and non-MeSH words used were ‘selective thoracic fusion’, ‘adding on phenomenon’, ‘Lenke type 1 curve’, ‘Lenke type 2 curve’, ‘touched vertebra’ and ‘lowest instrumented vertebra’. The manual search was done by cross-checking the references of the included citations. Unpublished data was excluded. Duplicates were eliminated by using Zotero’s de-duplication function followed by manual elimination after merging all the references.
Study Selection
The studies having the following criteria were included in the analysis (1) Lenke type 1 curves and Lenke type 2 curves in adolescent population, (2) selective thoracic fusion of the curves, (3) studies with curves less than 70 degrees, (4) retrospective and prospective case studies, (5) studies mentioning LIV, pre- and post-operative curve characteristics including correction percentages and complications.
Studies which did not report the LIV selection, curve correction percentages, follow-up less than 24 months, studies with osteotomy more than Schwab grade 3 10 and whose full text could not be acquired were excluded. Case reports were also excluded.
Quality Assessment
Two reviewers independently assessed the quality of the included studies using NIH quality assessment tool 11 and is enumerated in Table 1 below. The tool assesses each study based on nine pre-defined criteria including adequate description of research question, study population, research question, outcome measures, statistical analysis and results, consecutiveness of cases and comparability of subjects. Each study was given a score out of nine. Studies with score less than 6 of 9 were excluded from the analysis. Any dispute between the reviewers was settled after discussion with the senior researcher (PK).
Table 1.
Quality Assessment of Each Study using NIH Quality Assessment Tool.
| Research Question | Study Population | Cases Consecutive? | Subjects Comparable? | Intervention Clearly Described? | Outcome Measures Clearly Defined, Valid, Reliable, | Length of Follow-Up Adequate? | Statistical Analyses | Results Well-Described? | |
|---|---|---|---|---|---|---|---|---|---|
| Qin X et al. 2018 (China) | 1 | 1 | 0 | 0 | 1 | 1 | 1 | 1 | 1 |
| Masayuki Ishikawa et al. 2017 (japan) | 1 | 1 | 1 | 0 | 1 | 1 | 1 | 1 | 1 |
| Shen M et al. 2018 (China) | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 |
| Yang C et al. 2016(China) | 1 | 1 | 0 | 0 | 1 | 1 | 1 | 1 | 1 |
| Oksanen H et al. 2018 (Finland) | 1 | 1 | 1 | 0 | 1 | 1 | 1 | 1 | 1 |
| Munakata R et al et al. 2020(Japan) | 0 | 1 | 1 | 0 | 1 | 1 | 1 | 1 | 1 |
| Sakai Y et al. 2020 (Japan) | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 |
| Bai J et al. 2017 (China) | 1 | 1 | 1 | 0 | 1 | 1 | 1 | 1 | 1 |
Data Extraction
The data was extracted from the retrieved articles by two authors (SI, KA). The data extracted included the study characteristics, outcome variables and demographic data. The study characteristics included the name of the author, title, study design, information on LIV, journal and year of publication, level of evidence and quality of study. The extracted demographic data included the number of patients, mean age and number of males and females. Curve characteristics such as pre- and post-operative Cobbs angle, correction percentages, SRS-22 score with its components and complications constituted the measured outcome variables. Once the data was extracted, the studies were classified into two groups for analysis – (1) with LIV at stable vertebra (SV) and (2) with LIV at touched vertebra (TV). In the case of data being incomplete or unclear, the corresponding author of the study was contacted for complete data sheet.
Statistical Analysis
Descriptive analysis using means, standard deviation (SD) and ranges (minimum, maximum) of the pooled data across the included studies were performed. Meta-analysis was performed using the Metafor package in R statistical software v4.0.0 (R Core Team, Vienna, 2020). Analysis was performed using a random effects model using the DerSemonian Laird method. Forest plots were generated to draw comparisons between the two groups (SV and TV). Weighted mean difference (WMD) and relative risk (RR) were used for analysing continuous and categorical or binary data, respectively. A P-value of less than .05 was considered significant, whereas any overlap within the 95% CI or P-value more than .05 was considered insignificant.
Results
The PRISMA flowchart of study selection is shown in Figure 1. A total of 468 articles were acquired after excluding duplicated articles from various databases. After initial screening, 34 articles were yielded for full-text analysis based on the pre-decided inclusion and exclusion criteria. Further, 26 articles were excluded because of incomplete data, lack of clarity on LIV selection, and studies dealing with sagittal LIV. Subsequently, 8 studies were evaluated for final analysis.
Figure 1.
PRISMA flowchart showing the selection of studies for the meta-analysis.
Study Characteristics
Of the 8 included studies, 7 were found to be retrospective studies (level III evidence),12‐18 whereas 1 was prospective study (level II evidence) 19 . No RCTs were found in the literature. Of the 8 studies, 2 studies were found to focus their results on comparison of outcomes between the touched vertebra group (TV) and stable vertebra group (SV). Among the remaining 6 studies, three evaluated the outcomes of deformity correction with TV group and SV group each. All the studies were found to have a quality score of 6 or above out of 9 and were subsequently included in analysis (Table 1).
Demographic Data
The analysis included a total of 539 patients with 309 and 230 patients in TV and SV groups, respectively. There was a female preponderance with 440 female patients (192 in SV and 248 in TV group) and 99 male patients (38 in SV and 61 in TV group). The mean age at surgery was 15.3 ± 1.2 in the TV group and 14.4 ± 1.1 in SV group (P = .09). Mean preoperative Cobbs angle for Main thoracic curve in TV and SV groups was 52.5 ± 1.5 and 52.5 ± 4.0, respectively (P = .36). All the mean values described are in effect the pooled means and standard deviations of all the included studies in one group. All the studies mentioned the Lenke curve in their studies to be either 1 or 2. Majority of studies in the analysis used rod rotation with insitu bending as the curve correction manoeuvre, however, one study by Oksanen et al. 19 used Ponte osteotomy in addition to the above manoeuvres (Table 2).
Table 2.
Demographic Details of the Involved Studies.
| Demographic Details of Included Studies | ||||||||
|---|---|---|---|---|---|---|---|---|
| Studies with LIV at Stable Vertebra | ||||||||
| STUDY | Oxford Score | Level of Evidence | Mean Age | Number of Patients | Males | Females | Lenke Type | Follow up(Months) |
| Qin et al 1, 2018 (China) | 7 | III | 14.62 | 24 | 5 | 19 | 1A&2A | 42.1 |
| Qin et al 2, 2018 (China) | 7 | III | 15.33 | 37 | 5 | 32 | 1A&2A | 42.1 |
| Ishikawa M et al, 2017 (Japan) | 8 | III | 15.1 | 21 | 1 | 20 | 1C,2C | 37 |
| Shen M et al 2, 2018 (China) | 9 | III | 14.8 | 29 | 5 | 24 | 1A | 24 |
| Yang C et al 1, 2016 (China) | 7 | III | 14.3 | 16 | 4 | 12 | 1&2 | 24 |
| Yang C et al 2, 2016 (China) | 7 | III | 14.8 | 82 | 17 | 65 | 1&2 | 24 |
| Oksanen H et al 2, 2018 (Finland) | 8 | II | 12 | 21 | 1 | 20 | 1&2 | 26 |
| Studies with LIV at Touched vertebra | ||||||||
| Oksanen H et al 1,2018(Finland) | 8 | II | 15.8 | 84 | 23 | 61 | 1&2 | 25 |
| Munakata R et al 2020(Japan) | 7 | III | 14.4 | 45 | 1 | 44 | 1A | 43.2 |
| Sakai Y et al 12 020(Japan) | 9 | III | 16.3 | 10 | 2 | 8 | 1 | 24 |
| Sakai Y et al 22 020(Japan) | 9 | III | 17.4 | 24 | 5 | 19 | 1 | 24 |
| Bai J et al 1, 2017 (China) | 8 | III | 14.51 | 16 | 4 | 12 | 1A&2A | 36 |
| Bai J et al 2, 2017 (China) | 8 | III | 15.33 | 104 | 20 | 84 | 1A&2A | 36 |
| Shen M et al 1 ,2018(China) | 9 | III | 13.6 | 26 | 6 | 20 | 1A | 24 |
Correction Rate
All the studies were included in the primary analysis of correction rate for the main thoracic curve between the two groups (SV and TV). No significant difference was found in the correction percentage between the two groups (MD–70.1; 95% CI–65.15,75.21 vs MD–71.2; 95% CI–66.44, 76.14) (Figure 2). Significant heterogeneity was detected for the outcome (P < .001).
Figure 2.
Proportional meta-analysis comparing the curve correction rates between the two groups.
Post-Operative Functional Outcomes (SRS-22 Scores)
Functional outcomes in terms of SRS scores were reported in 5 out of 8 studies. A primary analysis was done between the two groups for all the domains of srs-22 scores viz function, pain, image, mental health and satisfaction. Both the groups were also compared for the total srs scores. No significant difference was found between the two groups for function (MD–3.9; 95% CI–3.59, 4.36, I2 = 87.7% vs MD–4.3; 95% CI–4.08, 4.67, I2 = 96.7%), pain (MD–4.1; 95% CI–4.04, 4.81, I2 = 0% vs MD–4.3; 95% CI–4.32, 4.43, I2 = 36.4%), self-image (MD–3.0; 95% CI–2.16, 3.93, I2 = 98.8% vs MD–4.0; 95% CI–3.76, 4.25, I2 = 94.7%), mental health (MD–3.9; 95% CI–3.71, 4.10, I2 = 71.3% vs MD–4.1; 95% CI–4.07, 4.29, I2 = 36.1%), and satisfaction (MD–3.8; 95% CI–3.54, 4.12, I2 = 78.4% vs MD–4.1; 95% CI–4.03, 4.26, I2 = 47.6%). There was no significant difference when the total srs scores were compared between the two groups (MD–3.7; 95% CI–3.46, 4.05, I2 = 89.4% vs MD–4.1; 95% CI–4.09, 4.26, I2 = 93.4%).
Complications
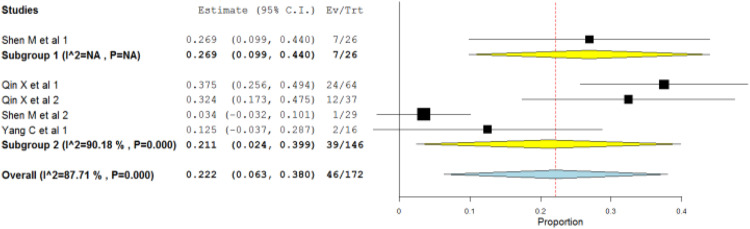
The complications reported in the included studies were mainly adding on phenomenon and sagittal or coronal imbalance. No neurological complications were reported in any of the studies. The number of cases with adding on phenomenon or sagittal and coronal imbalance are shown in Table 3. There was no significant difference between the two groups with respect to relative risk of complications (RR = .269; 95% CI-.09,0.44 vs RR = .21; 95% CI-.02,0.39) (Figure 3).
Table 3.
Cases with Adding-on Phenomenon and Imbalance in the Analysis.
| Adding on | Coronal Imbalance | Sagittal Imbalance | |
|---|---|---|---|
| Qin et al | 37/64 | 8 off 37 | 4 off 37 |
| Shen M et al. 2 | 1 | — | — |
| Yang C et al. 1 | 2 | — | — |
Figure 3.
Proportional meta-analysis comparing the complications between the two groups.
Discussion
The standard treatment of progressive AIS curves is by surgical fusion of the curve. The most important factor influencing the post-operative outcomes in AIS curve corrections are the fusion levels.20,21 Incorrect selection of fusion levels , especially incorrect selection of LIV may cause either under correction of the curve or may involve more motion segments thereby reducing mobility and overall functional outcomes.20,22 The treatment has evolved over few decades and the current focus is on preserving as many motion segments as possible while obtaining optimum correction of the deformity. This led to the concept of selective fusion of curves, especially in Lenke type 1& 2 curves. The concept of selective thoracic fusion was first popularised by King et al. where the study group fused the major curve and hoped for the spontaneous correction of other curves. 22 The study group noticed that the lumbar curves did correct spontaneously when only the thoracic curves were fused. 22 As the selective thoracic fusion started gaining popularity, there was a debate among the surgeons with respect to choosing the LIV. King et al. advocated that choosing the LIV at the stable or neutral vertebra led to spontaneous correction of lumbar curve and modest correction of the thoracic deformity. 22 Subsequently, studies were done by Cao et al. and Matsumoto et al. in which TV was used as the LIV and the study groups reported good clinical results.8,9 The authors in the current article compared the curve correction percentage between the two groups based on LIV (TV and SV) and found no significant difference in the curve correction rates between the two groups. It must be noted that all the studies involved in the analysis had Lenke curve modifier ‘A’, with exception of only one study by Ishikawa et al. 18 Further, due to differences between sample size and length of follow-up period, some interpretations may be limited. The curve correction does not serve the purpose if the correction does not translate into better functional outcomes. Five of the eight studies reported the improvement of functional status in terms of srs scores. When sub group analysis was done, there was no significant difference between the two groups for all the domains of srs-22 scores. The total srs scores were compared between the two groups and there was no significant difference between the two groups. The data for pain modality was homogenous, whereas the data for other modalities was heterogenous. Boniello J et al. did a study to compare the functional outcomes of selective vs non-selective fusion in Lenke 1 curves and compared the SRS scores between the two groups. The study group came out with conclusions that selective thoracic fusions have good functional outcomes which are similar to non-selective fusions and selective fusions can be done in curves even with lumbar ‘C’ modifier. 23 Though most of the studies included in our analysis had either lumbar ‘A’ or ‘B’ modifier, the good functional outcomes which were statistically similar in both the groups indicate that selective fusions which are stopped short at TV can give similar functional results to those fusions stopped at SV.
Adding-on phenomenon(AO) is one of the common complications after STF in AIS curves, which often leads to poor clinical outcomes.8,24 This was first reported by Suk et al. where they found that after STF, the lumbar curve corrected spontaneously in the immediate post-operative period. However, there was an extension of main thoracic curve into spontaneously corrected lumbar curve in the follow-up period. 25 The selection of LIV highly correlated with AO and the incidence increased as the LIV selection moved proximally. 26 The other reasons for AO suggested were over correction of main thoracic curve. 27 Anticipation of AO phenomenon was one of the main arguments by the surgeons group who chose distal LIV(SV) in preference to proximal LIV(TV).Wang et al. studied 10 different factors that may be responsible for AO and found LIV selection and immaturity as the only factors which highly correlated with AO. 27 The authors in this study found that 46 patients(26.7%) out of 172 patients developed AO during follow-up. When the incidence of AO was compared between the two groups, there was no significant difference between the two groups. It is worth noting that studies in TV group did not report of AO except for one study. 14 Tan et al. proposed another hypothesis for the development of AO that this phenomenon may likely be generated due to the residual uncorrected and unsupported rotational deformities of main thoracic curves despite the instrumentation extended to the stable vertebra. 28 There were no incidences of transient or permanent neurological deficits in any of the patients in the entire study. There are reports of coronal and sagittal decompensation after STF in AIS.29,30 However, our study had a total of 12 cases which showed decompensation among all the patients. The overall complications were not significant between the two study groups. The main goal of STF is maintenance of a balanced spine, spontaneous correction of compensatory curves, and saving more mobile lumbar segments. 31 All these goals can be achieved by choosing either SV or TV as the LIV. As the TV allows for the saving of more motion segments, TV can safely be chosen as LIV with similar satisfaction and complication rates to SV as LIV.
A few limitations of this study are noteworthy. All the studies included in the analysis except one are retrospective studies which amount to level III evidence in the literature. Randomised control studies with two arms (SV, TV) would have been ideal to be analysed for this study, but paucity of such evidence in the literature made the authors choose the available evidence for the analysis. Homogeneity of the involved studies in this meta-analysis was questionable in terms of surgical techniques, outcome measures and countries where the studies were done. Though AO phenomenon is the major determinant of choosing the distal fusion levels, our study had only few studies which had AO phenomenon as major outcome. More studies concentrated on this complication are warranted for better understanding of the distal fusion level. Majority of the literature involved in this review is recent which indicates that a lot of research is being done in the recent times on these topics of ambiguity and this review provides a decent evidence on choosing the distal fusion levels while considering STF for AIS curves.
Conclusions
The current review with evaluation of SV group and TV group as LIV for selective thoracic fusions in AIS reveals a comparable outcome in terms of curve correction, patient satisfaction scores and complication rates. The TV can be safely chosen as the LIV especially in type A and B Lenke 1&2 curves. This saves more lumbar motion segments when compared to SV. Further analysis with good quality RCTs involving both the groups can establish a definite consensus among the surgeons in choosing LIV.
Appendix.
Abbreviations
- LIV
lowest instrumented vertebra
- TV
touched vertebra
- SV
stable vertebra
- AIS
adolescent idiopathic scoliosis
- STF
selective thoracic fusion
- NIH
National Institute of Health
- SD
standard difference
- WMD
weighted mean difference
- RR
relative risk
- CI
confidence interval
- PRSIMA
preferred reporting items for systematic reviews and meta-analyses
- AO
adding-on phenomenon
Footnotes
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding: The author(s) received no financial support for the research, authorship, and/or publication of this article.
ORCID iDs
Syed Ifthekar https://orcid.org/0000-0002-3546-5962
Kaustubh Ahuja https://orcid.org/0000-0003-1344-9889
P V. Sudhakar https://orcid.org/0000-0002-5976-561X
Samarth Mittal https://orcid.org/0000-0003-3528-0949
Pankaj Kandwal https://orcid.org/0000-0002-8801-6909
Nikhil Goyal https://orcid.org/0000-0002-0387-4358
References
- 1.Lenke LG, Betz RR, Clements D, et al. Curve prevalence of a new classification of operative adolescent idiopathic scoliosis: does classification correlate with treatment? Spine. 2002;27(6):604‐611. [DOI] [PubMed] [Google Scholar]
- 2.Dobbs MB, Lenke LG, Kim YJ, Kamath G, Peelle MW, Bridwell KH. Selective posterior thoracic fusions for adolescent idiopathic scoliosis: comparison of hooks versus pedicle screws. Spine. 2006;31(20):2400‐2404. [DOI] [PubMed] [Google Scholar]
- 3.Lenke LG, Betz RR, Harms J, et al. Adolescent idiopathic scoliosis: A new classification to determine extent of spinal arthrodesis. J Bone Joint Surg Am. 2001;83(8):1169‐1181. [PubMed] [Google Scholar]
- 4.Lehman RA, Lenke LG, Keeler KA, et al. Operative treatment of adolescent idiopathic scoliosis with posterior pedicle screw-only constructs: minimum three-year follow-up of one hundred fourteen cases. Spine (Phila Pa 1976). 2008;33(14):1598‐1604. [DOI] [PubMed] [Google Scholar]
- 5.Sanchez-Raya J, Bago J. The effect of the lower instrumented vertebra (LIV) on pain and quality of life in patients surgically treated for an idiopathic scoliosis. Scoliosis. 2012;7(Suppl 1):P16. [Google Scholar]
- 6.Lee MC, Õunpuu S, Solomito M, Smith BG, Thomson JD. Loss in spinal motion from inclusion of a single midlumbar level in posterior spinal fusion for adolescent idiopathic scoliosis. Spine. 2013;38(22):E1405-|E1410. [DOI] [PubMed] [Google Scholar]
- 7.Erickson MA, Baulesh DM. Lowest instrumented vertebra selection in AIS. J Pediatr Orthop. 2011;31(1 Suppl):S69-76. [DOI] [PubMed] [Google Scholar]
- 8.Cao K, Watanabe K, Kawakami N, et al. Selection of lower instrumented vertebra in treating Lenke type 2A adolescent idiopathic scoliosis. Spine. 2014;39(4):E253-E261. [DOI] [PubMed] [Google Scholar]
- 9.Matsumoto M, Watanabe K, Kawakami N, et al. Postoperative shoulder imbalance in Lenke Type 1A adolescent idiopathic scoliosis and related factors. BMC Musculoskelet Disord. 2014;15:366. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Schwab F, Blondel B, Chay E, et al. The comprehensive anatomical spinal osteotomy classification. Neurosurgery. 2014;74(1):112‐120. [DOI] [PubMed] [Google Scholar]
- 11.Study quality assessment tools | NHLBI, NIH [Internet]. https://www.nhlbi.nih.gov/health-topics/study-quality-assessment-tools
- 12.Qin X, Sun W, Xu L, Liu Z, Qiu Y, Zhu Z. Selecting the last “substantially” touching vertebra as lowest instrumented vertebra in lenke type 1A curve: Radiographic outcomes with a minimum of 2-year follow-up. Spine. 2016;41(12):E742‐E750. [DOI] [PubMed] [Google Scholar]
- 13.Munakata R, Koseki M, Oba H, Ikegami S, Uehara M, Kuraishi S, et al. Selecting the C7-LIV line vertebra as the upper instrumented vertebra for adolescent idiopathic scoliosis lenke type 1A curves: Multicenter and a minimum 2-year follow-up study. Spine. 2020;45(17):1239‐1245. [DOI] [PubMed] [Google Scholar]
- 14.Shen M, Li N, Luo M, Xu G, Wang W, Wang L. Comparison of SV and LSTV as the lowest instrumented vertebra in Lenke 1A adolescent idiopathic scoliosis: SV decreasing the distal adding-on phenomenon. Int J Clin Exp Med. 2018;11(9): 9520–9527. [Google Scholar]
- 15.Bai J, Chen K, Wei Q, et al. Selecting the LSTV as the lower instrumented vertebra in the treatment of lenke types 1A and 2A adolescent idiopathic Scoliosis: A minimal 3-year follow-up. Spine. 2018;43(7):E390‐E398. [DOI] [PubMed] [Google Scholar]
- 16.Sakai Y, Takenaka S, Makino T, Yoshikawa H, Kaito T. Postoperative T1 tilt is a risk factor for postoperative distal adding-on in Lenke type 1 adolescent idiopathic scoliosis: A preliminary report. Medicine. 2020;99(21):e19983. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Yang C, Li Y, Yang M, et al. Adding-on Phenomenon After Surgery in Lenke Type 1, 2 Adolescent Idiopathic Scoliosis: Is it Predictable? Spine. 2016;41(8):698‐704. [DOI] [PubMed] [Google Scholar]
- 18.Ishikawa M, Cao K, Pang L, et al. Onset and remodeling of coronal imbalance after selective posterior thoracic fusion for Lenke 1C and 2C adolescent idiopathic scoliosis (a pilot study). Scoliosis. 2017;12(1):16. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Oksanen H, Lastikka M, Helenius L, Pajulo O, Helenius I. Posterior spinal fusion extended to stable vertebra provides similar outcome in juvenile idiopathic scoliosis patients compared with adolescents with fusion to the touched vertebra. Scand J Surg. 2019;108(1):83‐89. [DOI] [PubMed] [Google Scholar]
- 20.Suk S-I, Lee S-M, Chung E-R, Kim J-H, Kim W-J, Sohn H-M. Determination of distal fusion level with segmental pedicle screw fixation in single thoracic idiopathic scoliosis. Spine. 2003;28(5):484‐491. [DOI] [PubMed] [Google Scholar]
- 21.Suk S-I, Lee S-M, Chung E-R, Kim J-H, Kim S-S. Selective thoracic fusion with segmental pedicle screw fixation in the treatment of thoracic idiopathic scoliosis: more than 5-year follow-up. Spine (Phila Pa 1976). 2005;30(14):1602‐1609. [DOI] [PubMed] [Google Scholar]
- 22.King HA, Moe JH, Bradford DS, Winter RB. The selection of fusion levels in thoracic idiopathic scoliosis. J Bone Joint Surg Am. 1983;65(9):1302‐1313. [PubMed] [Google Scholar]
- 23.Boniello AJ, Hasan S, Yang S, Jalai CM, Worley N, Passias PG. Selective versus nonselective thoracic fusion in Lenke 1C curves: a meta-analysis of baseline characteristics and postoperative outcomes. J Neurosurg Spine. 2015;23(6):721‐730. [DOI] [PubMed] [Google Scholar]
- 24.Sponseller PD, Betz R, Newton PO, et al. Differences in curve behavior after fusion in adolescent idiopathic scoliosis patients with open triradiate cartilages. Spine. 2009;34(8):827‐831. [DOI] [PubMed] [Google Scholar]
- 25.Suk S-I, Lee S-M, Chung E-R, Kim J-H, Kim W-J, Sohn H-M. Determination of distal fusion level with segmental pedicle screw fixation in single thoracic idiopathic scoliosis. Spine. 2003;28(5):484‐491. [DOI] [PubMed] [Google Scholar]
- 26.Xu W, Chen C, Li Y, et al. Distal adding-on phenomenon in adolescent idiopathic scoliosis patients with thoracolumbar vertebra fusion. Medicine. 2017;96(38):e8099. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5617722/ [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Wang Y, Bünger CE, Zhang Y, Wu C, Li H, Hansen ES. Distal adding on in lenke 1A scoliosis: What causes it? how can it be prevented? Spine Deform. 2014;2(4):301‐307. [DOI] [PubMed] [Google Scholar]
- 28.Tan J-H, Hey HWD, Wong G, Wong H-K, Lau LL. Lumbar adding-on of the thoracic spine after selective fusion in adolescent idiopathic scoliosis lenke types 1 and 2 patients: A critical appraisal. Spine. 2021;46(3):E167‐E173. [DOI] [PubMed] [Google Scholar]
- 29.Gomez JA, Matsumoto H, Colacchio ND, et al. Risk factors for coronal decompensation after posterior spinal instrumentation and fusion in adolescent idiopathic scoliosis. Spine Deform. 2014;2(5):380‐385. [DOI] [PubMed] [Google Scholar]
- 30.Crawford CH, Lenke LG, Sucato DJ, et al. Selective thoracic fusion in Lenke 1C curves: Prevalence and criteria. Spine. 2013;38(16):1380‐1385. [DOI] [PubMed] [Google Scholar]
- 31.Lee CS, Hwang CJ, Lee D-H, Cho JH. Five major controversial issues about fusion level selection in corrective surgery for adolescent idiopathic scoliosis: a narrative review. Spine J. 2017;17(7):1033‐1044. [DOI] [PubMed] [Google Scholar]