Abstract
Background
Hand basal cell carcinoma is a rare and complex disorder. Due to the hand's anatomical features, managing hand BCC is challenging. Therefore, we have conducted this systematic review to investigate various clinical characteristics, investigations, and treatment options related to hand BCC. Furthermore, a meta-analysis was used to provide pooled recurrence rates.
Methods
We conducted this review per the International Prospective Register of Systematic Reviews (PROSPERO) guidelines. This study performed a systematic literature review in February 2022 using the following electronic databases: Cochrane, MEDLINE, and EMBASE. Key terms include hand basal cell carcinoma, basal cell carcinoma, management, outcome, and recurrence. We evaluated articles according to predefined quality criteria.
Results
The study included 9725 patients and 51 published articles. A total of 35 case reports, 2 case series, 1 prospective study, and the remaining retrospective studies were evaluated. An asymptomatic skin lesion was the main complaint. In 10 studies, Moh surgery was the most frequently used treatment method. In the seven studies included in the meta-analysis, the overall incidence rate of recurrence among the included patients was 1.49 cases per year.
Conclusion
The optimal extent of surgical treatment is still controversial, though an early biopsy can help identify lesions at an early stage. It is the first study to provide occurrence rates based on a meta-analysis. Developing treatment guidelines for BCC of the hand will be the focus of future research.
Keywords: Basal cell carcinoma, Prognosis, Survival, Meta-analysis, Nonmelanoma skin cancer, Hand surgery
Level of evidence: III, Risk/prognostic study
Introduction
Basal Cell Carcinoma (BCC) is the most common type of skin cancer, and its incidence is increasing worldwide.1 BCC is usually a slow-growing tumor that hardly ever metastasizes. However, it can lead to significant patient morbidity.2 It is well established that sun exposure is the leading risk factor for BCC.2 Although patients' cumulative exposure to ultraviolet light is a significant risk factor for BCC, exposure to ultraviolet light alone does not precisely predict the probability of developing BCC at a specific site.2 Other factors include lighter skin phototypes, smoking, the number of blistering sunburns, and immunosuppression.3,4 The dorsum of the hand is considered a frequently sun-exposed area; the occurrence of BCC in that area is relatively uncommon.5 One of the major causes of the rare occurrence of BCC in the dorsum of the hand is the paucity of sebaceous structures in that area.6 It is believed that BCC originates from pluripotential epithelial cells in the deep layers of the epidermis and hair follicles, and it tends to occur only in areas where both hair follicles and sebaceous glands are present.6,7 The incidence of hand skin cancer is estimated to be around 10–15% of all skin cancers.8 Of these, the incidence of hand BCC is approximately 11%.8 Moreover, when BCC occurs proximally to the upper extremity, it usually presents as classical BCC. On the other hand, acral BCC presents as erythematous skin plaques with scaling or exophytic tumors with the absence of the classical pearly appearance and telangiectasia. The diagnosis of a suspected BCC is made through either a shave biopsy or a punch biopsy.9 There are several histological types of BCC, including superficial and nodular, and types with high recurrence rates, such as micronodular, infiltrative, metatypical, and morpheaform patterns.10 Nodular BCC is the most commonly documented histological subtype on the dorsum of the hand.10 Treatment options for BCC of the hand vary; they include both surgical and nonsurgical treatment options. Nonsurgical options include topical immunomodulators (e.g., imiquimod), cryotherapy, radiation, photodynamic therapy, intralesional treatment (e.g., 5-fluorouracil), curettage, and electrodesiccation.9,11 Although the tumor management of the hand surgically requires special considerations, surgical excision is the favored treatment method for BCC. Reconstruction of the hand is challenging as the surgeon must consider protecting both the hand's function and appearance. Margins differ depending on the grade and the size of the lesion. The recommended margins for smaller or low-grade lesions are 4 mm, while larger, high-grade lesions require margins of at least 6 mm.9 Moreover, Moh surgery is thought to be beneficial in maximizing tissue preservation and lowering the recurrence rate.9 The literature lacks comprehensive systematic reviews and meta-analyses of the literature regarding the presentation, optimal management, and outcomes of hand BCC. To the authors' knowledge, this is the first systematic review that assesses a variety of clinical characteristics, investigations, and treatment options in the literature for hand BCC. We have additionally presented pooled recurrence rates based on a meta-analysis.
Methods & materials
Literature review
We designed this systematic review using Cochrane review methods and utilized preferred reporting items for systematic reviews and meta-analyses (PRISMA) guidelines.12,13
This study followed the International Prospective Register of Systematic Reviews (PROSPERO) statement (ID: CRD42022313017).12 The ethical approval was waived due to the type of study, and the review was carried out in compliance with the Helsinki Declaration. In February 2022, a systematic search was conducted in the following databases: MEDLINE, Cochrane, and EMBASE. The keywords used were the following: basal cell carcinoma, BCC, hand, nail, thumb, subungual, treatment, wide excision, local excision, amputation, conservative therapy, recurrence, and outcome. The search results included studies published without time frame limitations.
Study selection
Four reviewers evaluated the titles and abstracts of the gathered articles that were included, and the included studies were selected for a comprehensive review. If the title or abstract did not provide enough information about the article's content, the full text was examined. A fifth independent reviewer reviewed all articles selected by both groups. The inclusion criteria of the study review are as follows: (1) articles published from inception to February 2022; (2) conveyed a randomized controlled trial; prospective or retrospective cohort/comparative, case-control, case series, or case reports; (3) adult and pediatric patients; (4) patients with hand BCC (volar, dorsal, and nail unit); (5) those that reported outcomes of interest for the clinical questions proposed; and (6) all languages were included in the review. The studies that were eliminated for satisfying the exclusion criteria were as follows: (1) improper method (illustrated by a meta-analysis/systematic review, economic analysis, animal study, cadaver study, narrative review, or editorial); (2) conveyed no outcomes of interest; and (3) articles that did not include patients with hand BCC.
Screening and data extraction
Four independent reviewers screened full-text articles using the Rayyan search engine,14 and data were collected. Any disagreement was resolved by a fifth reviewer. General demographic data were gathered, such as authors' last names, country, study design, sample size, patients' age, sex, race, main presenting symptom, history of skin cancer, immune status, location of lesion, morphology, tumor invasion, treatment modality, follow-up timeframe, diagnosis, and recurrence/cure rates, which were further analyzed for meta-analysis. The level of evidence was assigned to each of the included articles, following the criteria described in the American Society of Plastic Surgeons' rating levels of evidence and grading recommendations.15
Bias assessment
We used the methodological index for the nonrandomized studies (MINORS) assessment tool. The instrument is a validated 12-item instrument designed to assess the quality of nonrandomized surgical studies.16 Two reviewers evaluated the risk of bias in all included studies using the MINORS criteria, and a third reviewer reviewed the assessments. The methodological quality and synthesis of case series and case reports were assessed using the methodological quality and synthesis of case series and case report assessment tool.17 A total of eight questions are divided into four main domains: selection, ascertainment, causality, and reporting. For both reviewers, the final answers were identical.
Statistical analysis
In the data analysis stage, the pooled estimates were calculated based on studies with at least 10 patients and available follow-up periods (years). The overall proportion of patients with BCC was computed according to the meta-analysis of single proportions. The incidence rate of recurrence was collected from each study, and a pooled outcome was estimated using person-time as time (years), the rate of recurrence as an event, and the total number of patients with BCC as the overall number. We calculated the overall incidence rate using log transformation and the inverse variance method, and continuity correction was applied for studies with zero events. Random-effects models were applied for all the analytical approaches. Heterogeneity assessment was carried out using the I2 test. To assess the sources of heterogeneity, we carried out a subgroup analysis based on the treatment modality and sensitivity analysis.
Results
Characteristics of the included studies
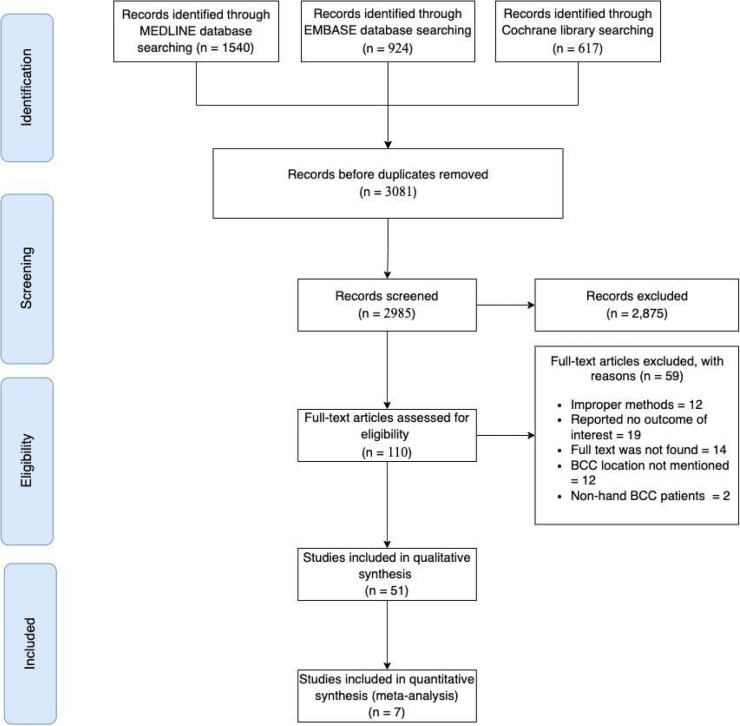
A total of 3081 articles were found in this systematic review, including 924 articles from EMBASE, 1540 articles from MEDLINE, and 617 articles from the Cochrane library. The number of articles for review remained at 2985 after removing duplicates. Initially, we were able to retrieve 110 full-text publications. However, after applying the previously defined inclusion and exclusion criteria, 51 studies were included in the qualitative synthesis published between 2006 and 2020 (Fig. 1). The following reasons prompted the exclusion of 59 articles: improper methods (systematic review, review article, and letter to editor), n = 12, no outcome of interest (n = 19), the full text could not be located (n = 14), the specific location of BCC was not stated (n = 12), included non-hand BCC patients (n = 2). Thirty-five studies were case reports,18, 19, 20, 21, 22, 23, 24, 25, 26, 27, 28, 29, 30, 31, 32, 33, 34, 35, 36, 37, 38, 39, 40, 41, 42, 43, 44, 45, 46, 47, 48, 49, 50, 51, 52 2 studies were case series,53,54 1 study was a prospective cohort analysis,55 and the remaining studies were retrospective cohort studies. Two studies were published in Australia,27,40 6 studies were published in Asia,22,23,27,32,47,49 17 studies were published in Europe,8,19,25,34,35,38.39.41.43.45.53.56, 57, 58, 59, 60, 61 and the remaining studies were published in North America. A total of 9725 patients were included (760 patients had BCC). More details about the characteristics of studies and patients are provided in Table 1.
Fig. 1.
The PRISMA flowchart for systematic review. The process of selecting the included studies.
Table 1.
Characteristics of the included studies and the recruited patients.
| Author | Design | Country | BCC/N | M/F* | Mean Age | Race | Level of evidence |
|---|---|---|---|---|---|---|---|
| Abeldaño et al. 2006 53 | CS | USA | 01-Mar | 0/1 | 64 | NA | Level IV |
| Bean et al. 198463 | R | USA | 16/70 | NA /NA | NA | White | level II |
| Chakrabarti et al. 199361 | R | UK | 4/275 | 2/2 | 68 | NA | level II |
| Clifford et al. 195564 | R | USA | May-62 | NA/NA | NA | NA | Level II |
| Coulombe et al. 201818 | CR | Canada | 01-Jan | 0/1 | NA | NA | Level II |
| Dika et al. 201343 | CR | Italy | 01-Jan | 0/1 | 73 | NA | level V |
| Engel et al. 200819 | CR | Germany | 01-Jan | 1/0 | 58 | NA | level V |
| Enna et al. 197844 | CR | USA | 01-Jan | 1/0 | 87 | white | Level V |
| Fischbach et al. 198062 | R | USA | 241/315 | NA/NA | NA | NA | level V |
| Forman et al. 200720 | CR | USA | 01-Jan | 1/0 | 70 | White | level II |
| Fournier et al. 202055 | P | Canada | 73/100 | 53/47 | NA | White | Level V |
| Galeano et al. 200245 | CR | Italy | 01-Jan | 1/0 | 81 | NA | Level I |
| Grine et al. 199721 | CR | USA | 01-Jan | 1/0 | 62 | White | level V |
| Guana et al. 199446 | CR | USA | 01-Jan | 1/0 | 74 | white | Level V |
| Higuchi et al. 198847 | CR | Japan | 01-Jan | 1/0 | 84 | white | level V |
| Hoffman et al. 197348 | CR | USA | 01-Jan | 0/1 | 65 | NA | level V |
| Kendall et al. 196965 | R | USA | Aug-73 | 8/0 | 70 | na | Level II |
| Kim et al. 200022 | CR | Korea | 01-Jan | 0/1 | 51 | Korean | Level V |
| Kim et al. 200923 | CR | Korea | 01-Jan | 0/1 | 63 | NA | Level V |
| Lam et al. 201924 | CR | USA | 01-Jan | 0/1 | 71 | NA | level V |
| Lateo et al. 200525 | CR | UK | 01-Jan | 0/1 | 73 | white | level V |
| Loh et al. 201566 | R | USA | 14/6654 | NA /NA | NA | White | level V |
| Loh et al. 20166 | R | USA | 14/176 | 12-Feb | 65.1 | White | Level II |
| Lopez-Sanchez et al. 201926 | CR | Australia | 01-Jan | 0/1 | 60 | Caucasian | Level II |
| Machida et al. 201127 | CR | Japan | 01-Jan | 0/1 | 76 | NA | level V |
| Maciburko et al. 20128 | R | UK, Australia | 61/407 | NA/NA | 71.8 | NA | level V |
| Martinelli et al. 200628 | CR | USA | 18/18 | NA/NA | NA | NA | level II |
| Mikhail et al. 198529 | CR | USA | 02-Feb | 1/0 | 36 | NA | Level V |
| Okuyama et al. 200649 | CR | Japan | 01-Jan | 0/1 | 90 | white | Level V |
| Oriba et al. 199730 | CR | USA | 01-Jan | 0/1 | 85 | NA | level V |
| Özkan et al. 201754 | CS | Turkey | 03-Jul | 3/0 | 56 | NA | Level V |
| Pollo et al. 201931 | CR | Brazil | 01-Jan | 0/1 | 70 | NA | level V |
| Rallis et al. 201032 | CR | India | 01-Jan | 0/1 | 63 | NA | Level IV |
| Riml et al. 201356 | R | Austria | NA/524 | NA/NA | 74.7 | NA | level V |
| Robins et al. 198133 | CR | USA | 02-May | 01-Jan | NA | NA | Level V |
| Rudolph et al. 198750 | CR | USA | 01-Jan | 0/1 | 59 | white | level II |
| Salomão et al. 199951 | CR | Brazil | 01-Jan | 0/1 | 49 | fair skinned | Level V |
| Sarfati et al. 200834 | CR | French | 01-Jan | 1/0 | 64 | NA | level V |
| Serrano-Ortega et al. 200235 | CR | Spain | 01-Jan | 1/0 | 63 | white | level V |
| Shimizu et al. 201336 | CR | USA | 01-Jan | 0/1 | 68 | NA | Level V |
| Tavares et al. 201837 | CR | Brazil | 01-Jan | 0/1 | 58 | NA | level V |
| Tehrani et al. 200938 | CR | UK | 01-Jan | 0/1 | 50 | NA | level V |
| Torrelo et al. 201439 | CR | Spain | 02-Feb | 2/0 | 5.65 | NA | Level V |
| Tripoli et al. 201758 | R | Italy | 98/629 | 388/241 | NA | NA | Level V |
| Tripoli et al. 202059 | R | Italy | 149/354 | 211/143 | 69.5 | NA | Level II |
| van Zuuren et al. 200060 | R | Netherlands | 11-Nov | 09-Feb | 63.3 | White | Level II |
| Vandeweyer et al. 200357 | R | Belgium | 07-Jul | 06-Jan | 71.2 | NA | level II |
| Watson et al. 201940 | CR | Australia | 01-Jan | 1/0 | 52 | white | level V |
| West et al. 199052 | CR | USA | 01-Jan | 1/0 | 70 | white | level V |
| Yousif et al. 201341 | CR | UK | 01-Jan | 1/0 | 45 | NA | Level V |
| Zhu et al. 201442 | CR | USA | 01-Jan | 1/0 | 43 | Caucasian | level V |
Gender distribution was based on the total number of patients with BCC; CR: case report; CS: case series; R: retrospective cohort; P: prospective cohort; M: male; F: female.
Clinical characteristics
The mean patient's age was 62.8 years old (a range between 1.16 to 90 years old). Two studies were reported in the pediatric age groups in 1.16 and 5.56 years old. The main presenting complaint in ten of the articles was an asymptomatic skin lesion, 3 were mass-like, 3 were nail deformities, 4 were nonhealing ulcers, 14 were ulcerated lesions, and 15 did not mention anything. In terms of race, 20 of the articles were Caucasians, and only 1 study reported an Asian patient.22
The clinical characteristics are listed in Table 2. Nail involvement was reported in 41 studies, of which the nails were involved among the patients in 16 studies (39%).20, 21, 22,28,31,33,35,36,38,42,43,45,46,48, 49, 50 Hand laterality was reported in 37 studies,6,18, 19, 20, 21, 22, 23, 24, 25, 26, 27, 28, 29, 30, 31, 32, 33, 34, 35, 36, 37,39, 40, 41, 42, 43, 44, 45, 46, 47, 48, 49, 50, 51, 52, 53,60 and the lesions were approximately equally distributed (33 and 31 lesions in the right and left hands, respectively). Metastasis was positive in a case report,23 and bone involvement was positive in another case report.40 In-situ lesions were reported in 4 studies,22,30,32,39 and invasive lesions in 8 articles.20,23,24,29,38,40,41,51 Treatment modalities included Moh surgery in 10 studies,6,19, 20, 21,24,30,33,36,43 curettage and cryosurgery in 1 study,55 amputation in 4 studies,35,40,45,48 and surgical excision in the remaining studies.
Table 2.
Clinical characteristics of patients.
| Author | Location | Morphology | Nail involvement | Diagnosis |
|---|---|---|---|---|
| Abeldaño et al. 200653 | palm | erythematous ulcerated lesion with distinct borders, | No | BCC Unspecified |
| Bean et al. 198463 | dorsum (7) - thumb (1) - fingers (2) - wrist (3) - web (1) | NA | NA | NA |
| Chakrabarti et al. 199361 | Fingers and dorsum of the hand | NA | No | NA |
| Clifford et al. 1955 64 | dorsum of hand | NA | No | NA |
| Coulombe et al. 201818 | Palms and lateral fingers | erythematous and edematous, and some were crusted | NA | BCC (Gorlin syndrome) |
| Dika et al. 201343 | The proximal nail fold of the right IV and V fingers | An ulcerated lesion | Yes | Perinugual basal cell carcinoma (BCC) |
| Engel et al. 200819 | Thumb | Erosive and erythematous | No | BCC Unspecified |
| Enna et al. 197844 | dorsal aspect of the middle phalanx of the ring finger | diffusely erythematous | No | variant basal cell carcinoma with an adenomatoid pattern |
| Fischbach et al. 198062 | NA | NA | NA | NA |
| Forman et al. 200720 | Thumb Nail | Eroded plaque | Yes | Nodular BCC |
| Fournier et al. 202055 | Hand | NA | NA | Superficial |
| Galeano et al. 200245 | dorsal and medial surface of left-hand thumb just distal to MP joint | small flat ulcerated lesion | painful exophytic mass on the dorsal and medial surface of his left thumb just distal to the MP joint, which had infiltrated the first commissura | Bowenoid BCC |
| Grine et al. 199721 | Posterior nailfold of the thumb | Ill-defined erythematous scaly lesion | Yes | Nodular BCC |
| Guana et al. 199446 | The dorsal distal phalanx of the right thumb involving the proximal and lateral nail fold | Scaly, erythematous nodule with a central ulceration | Yes | Nodulo-ulcerative BCC with minor sclerosing component |
| Higuchi et al. 198847 | The lateral surface of the proximal phalanx of the ring finger | A sharply circumscribed ulcer with a dusky red, partially blackish, irregular surface | No | BCC |
| Hoffman et al. 197348 | The ulnar side of the thumb | ulceration with surrounding induration and redness and exposure of the distal phalanx | Yes | BCC |
| Kendall et al. 196965 | dorsum of hand | NA | No | NA |
| Kim et al. 200022 | The right fifth fingernail | Linear longitudinal Melanonychia on fingernail | Yes | Superficial BCC |
| Kim et al. 200923 | Fourth finger | Erythematous plaque | No | Infiltrative |
| Lam et al. 201924 | Palm | Well-demarcated, erythematous, ulcerated plaque | No | Collusion tumor BCC and SCC in situ |
| Lateo et al. 200525 | Palm | Erythematous, minimally raised, smooth plaque | No | BCC with eccrine-type ductal differentiation. |
| Loh et al. 201566 | Dorsum | NA | No | 8 BCC unspecified- 4 nodular- 1 ulcerative- 1 infiltrative |
| Loh et al. 20166 | Dorsum | NA | NA | Nodular BCC |
| Lopez-Sanchez et al. 201926 | Palm | A well-defined pink plaque | No | Nodular |
| Machida et al. 201127 | Palm | slightly elevated, skin-colored plaque with a keratotic, crusted center | No | Superficial |
| Maciburko et al. 20128 | Dorsum | Erythematous plaque | NA | Nodular |
| Martinelli et al. 200628 | Nadorsumil unit | Ulcerative lesion | Yes | unspecified bcc |
| Mikhail et al. 198529 | Lateral nail fold to the radial aspect of fifth finger | Erythematous, crusted, tender papule | No | Unspecified |
| Okuyama et al. 200649 | The ulnar side of the proximal nail bed of the thumb | a well-defined ulcer, pigmented spots and crusty debris over the nail | Yes | BCC |
| Oriba et al. 199730 | Dorsal aspect of second digit | Crescent-shaped, eczematous, and pink plaque | No | Nodular |
| Özkan et al. 201754 | Phalanges | Rash and swelling | No | NA |
| Pollo et al. 201931 | Nail | Friable lesion with periungual erythema and onychodystrophy | Yes | infiltrative |
| Rallis et al. 201032 | Second interdigital space | Fleshy | No | Ulcerated |
| Riml et al. 201356 | NA | NA | NA | Nodular BCC |
| Robins et al. 198133 | 1 nail unit- 1 palm | Scaly erosion | Yes | NA |
| Rudolph et al. 198750 | thumb nail | The affected nail is slightly ridged, wide brown streak extending along the entire length of the nail. | Yes | BCC |
| Salomão et al. 199951 | In the palm of the right hand, next to the proximal phalanx of the second digit | A crusty ulcerated lesion | No | BCC Unspecified |
| Sarfati et al. 200834 | Dorsum of Thumb | Irregular periungual ulceration | No | Ulcerated BCC |
| Serrano-Ortega et al. 200235 | The proximal nailfold of the middle finger of the right hand | a painless ulceration with well-defined edges and a necrotic base | Yes | BCC Unspecified |
| Shimizu et al. 201336 | right 5th digit & left thumb | A plaque extended from the distal interphalangeal joint to the fingertip (right), & a pink papule was noted beneath the nail plate(left) | Yes | Superficial BCC (right) & superficial and nodular BCC (left) |
| Tavares et al. 201837 | Periungual region of the left thumb | granulomatous and friable ulcer with infiltrated margins | No | Basosquamous cell carcinoma |
| Tehrani et al. 200938 | Base of thumbnail | NA | Yes | BCC |
| Torrelo et al. 201439 | Dorsum of hand, second finger | Papules | No | Nodular, syndromic |
| Tripoli et al. 201758 | Dorsum | Ulcerated lesion | NA | Superficial |
| Tripoli et al. 202059 | Dorsum | Ulcerated lesion | NA | Unspecified |
| van Zuuren et al. 200060 | Dorsum | NA | No | Nodular BCC |
| Vandeweyer et al. 200357 | Dorsum of the hand | ulcerated | No | infiltrative BCC with free margins |
| Watson et al. 2019 40 | Hand | A locally invasive ulcerated lesion of the right upper limb | No | Nodular |
| West et al. 199052 | The dorsum surface of the proximal phalanx of the index finger | An ulcer with a clean, granular base and a raised erythematous border | NA | Sclerosing BCC |
| Yousif et al. 201341 | Dorsoradial aspect of ring finger | Ulcerative, raised with a rolled edge | No | Nodular |
| Zhu et al. 201442 | dorsal aspect of both hands (transversed joint) & distal tip of the left small finger | large ulcerated | Yes | BCC multilobular |
Results of the meta-analysis
In the meta-analysis, seven studies were included. A total of 2051 patients were included, of whom 652 patients had BCC with an overall pooled proportion of 32.24% (95%CI, 14.37% to 57.44%, Fig. 2). There was a significant heterogeneity among studies (I2 = 98.7%, p < 0.0001).
Fig. 2.
A forest plot shows the rate of BCC among the included patients.
The incidence of recurrence
The overall incidence rate of recurrence among the included patients was 1.49 cases per year (95%CI, 0.58 to 3.82, Fig. 2). The heterogeneity among studies was significant (I2 = 83.2%, p < 0.0001). However, studies which recruited patients who underwent surgical excision showed no significant heterogeneity in the incidence rate of recurrence (incidence = 1.48 case-years, 95%CI, 0.86 to 2.55, I2 = 0%, p = 0.56). Additionally, subgroup differences were significant based on the treatment provided (Chi2= 35.66, p < 0.0001). Heterogeneity analysis for other treatment modalities was not conducted because these treatment approaches were performed in a single study (Fig. 3).
Fig. 3.
A forest plot shows the incidence rate of BCC recurrence among patients treated by four modalities.
To further investigate the sources of heterogeneity, we implemented an influence analysis (sensitivity analysis) by omitting each included study at once. The study of Fischbach et al. had the largest influence effect size.62 Following the exclusion of such a study, the overall heterogeneity dropped to 1.2%, and the overall incidence rate was 1.28 cases per year (95%CI, 0.76 to 2.14, Fig. 4). The exclusion of other studies did not influence the heterogeneity analysis.
Fig. 4.
A forest plot shows the results of the influence analysis.
Quality assessment and risk of bias
The authors evaluated the case reports and case series included in the study. Bias was evaluated separately and concurrently by two reviewers. We used a methodological quality assessment tool based on 8 components that are divided into 4 domains: selection, ascertainment, causation, and reporting (Table 3).60 The findings of both reviewers were the same, regardless of whether the material seemed biased. MINORs were at least 52,84% in all retrospective and prospective studies considered. There was 1 comparative study, and it ranked a total score of 24. Eleven noncomparative studies had an average score of 8.45 (range 12–4). The results are summarized in Tables 4 and 5.
Table 3.
Qualitative assessment of the included studies.
| Domain For Evaluating the Methodological Quality of Case Reports and Case Series | ||||||||
|---|---|---|---|---|---|---|---|---|
| Selection | Ascertainment |
Causality |
Reporting |
|||||
| Leading Explanatory Questions |
||||||||
| Reference | Q. 1 | Q. 2 | Q. 3 | Q. 4 | Q. 5 | Q. 6 | Q. 7 | Q. 8 |
| Mikhail, 198529 | YES | YES | NO | YES | NO | NO | YES | NO |
| Rallis, 2010 32 | YES | YES | YES | YES | NO | NO | YES | YES |
| Oriba, 1997 30 | YES | YES | YES | YES | NO | NO | NO | YES |
| Torrelo, 201439 | YES | YES | NO | YES | NO | NO | NO | NO |
| Yousif, 201341 | YES | YES | YES | NO | NO | NO | YES | YES |
| Tehrani, 200938 | YES | YES | YES | NO | NO | NO | YES | YES |
| Kim, 200923 | YES | YES | NO | YES | NO | NO | NO | NO |
| Sarfati, 200834 | YES | YES | YES | YES | NO | NO | NO | NO |
| Engel, 200819 | YES | YES | NO | NO | NO | NO | NO | NO |
| Kim, 200022 | YES | YES | NO | YES | NO | NO | NO | NO |
| Forman, 200720 | YES | YES | YES | NO | NO | NO | NO | YES |
| Grine, 199721 | YES | YES | YES | YES | NO | NO | NO | YES |
| Watson, 201940 | YES | YES | YES | NO | NO | NO | NO | NO |
| Lam, 201924 | YES | YES | NO | YES | NO | NO | NO | YES |
| Lateo, 200525 | YES | YES | NO | YES | NO | NO | NO | NO |
| Lopez-Sanchez, . 201926 | YES | YES | YES | YES | NO | NO | YES | YES |
| Machida, 201127 | YES | YES | YES | YES | NO | NO | YES | YES |
| Pollo, 201931 | YES | YES | YES | NO | NO | NO | YES | YES |
| Tavares, 201837 | YES | YES | YES | YES | NO | NO | NO | YES |
| Shimizu, 201336 | YES | YES | YES | YES | NO | NO | NO | YES |
| ORTEGA, 200235 | YES | YES | NO | YES | NO | NO | NO | NO |
| Coulombe, 201818 | YES | YES | NO | YES | NO | NO | NO | NO |
| Zhu, 201442 | YES | YES | YES | NO | NO | NO | YES | YES |
| Higuchi, 198847 | YES | YES | YES | YES | NO | NO | YES | YES |
| Enna, 197844 | YES | YES | YES | YES | NO | NO | NO | YES |
| Okuyama, 200649 | YES | YES | NO | YES | NO | NO | NO | YES |
| Hoffman, 1973 48 | YES | YES | YES | YES | NO | NO | NO | YES |
| Rudolph, 198750 | YES | YES | YES | YES | NO | NO | NO | YES |
| Galeano, 200245 | YES | YES | YES | YES | NO | NO | YES | YES |
| Guana, 199446 | YES | YES | YES | YES | NO | NO | NO | YES |
| West, 199052 | YES | YES | YES | YES | NO | NO | NO | YES |
| Dika, 201343 | YES | YES | YES | YES | NO | NO | NO | YES |
| Salomão, 199951 | YES | YES | YES | YES | NO | NO | YES | YES |
| Martinelli, 200628 | YES | YES | YES | YES | NO | NO | NO | YES |
| Robins, 198133 | YES | YES | YES | YES | NO | NO | NO | YES |
| Ozkan, 201754 | YES | YES | YES | YES | NO | NO | YES | YES |
| Abeldano, 200653 | YES | YES | YES | YES | NO | NO | NO | YES |
| Zuuren, 200060 | YES | YES | YES | YES | NO | NO | YES | YES |
| Maciburko, 20128 | YES | YES | YES | YES | NO | NO | YES | YES |
Selection: [question 1]. Does the patient(s) represent(s) the whole experience of the investigator (center) or is the selection method unclear to the extent that other patients with similar presentations may not have been reported?.
Ascertainment: [question 2]. Was the exposure adequately ascertained? [question 3]. Was the outcome adequately ascertained?.
Causality: [question 4]. Were other alternative causes that may explain the observation ruled out? [question 5]. Was there a challenge/rechallenge phenomenon? [question 6]. Was there a dose-response effect? [question 7]. Was follow-up long enough for outcomes to occur?.
Reporting: [8] Is the case(s) described with sufficient details to allow other investigators to replicate the research or to allow practitioners to make inferences related to their own practice?.
Table 4.
MINORS assessment tool for nonrandomized comparative studies (n = 1).
| Item | Fournier, 2020 55 |
|---|---|
| A clearly stated aim | 2 |
| Inclusion of consecutive patients | 2 |
| Prospective collection of data | 2 |
| Endpoints appropriate to the aim of the study | 2 |
| Unbiased assessment of the study endpoint | 2 |
| Follow-up period appropriate to the aim of the study | 2 |
| Loss to follow-up less than 5% | 2 |
| Prospective calculation of the study size | 2 |
| An adequate control group | 2 |
| Contemporary groups | 2 |
| Baseline equivalence of groups | 2 |
| Adequate statistical analyses | 2 |
| Total score | 24 |
Table 5.
MINORS assessment tool for nonrandomized noncomparative studies (n = 11).
| Item | Tripoli, 2017 58 | Loh, 2016 6 | CHAKRABARTI, 1993 61 | Loh, 2015 66 | Riml, 201,356 | Bean, 198,464 | Fischbach, 1980 62 | Clifford, 1955 64 | Kendall, 1969 65 | Tripoli, 2020 59 | Vandeweyer, 2016 57 |
|---|---|---|---|---|---|---|---|---|---|---|---|
| A clearly stated aim | 2 | 2 | 2 | 2 | 2 | 2 | 2 | 2 | 0 | 2 | 0 |
| Inclusion of consecutive patients | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 2 | 0 |
| Prospective collection of data | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| Endpoints appropriate to the aim of the study | 2 | 2 | 2 | 2 | 2 | 2 | 2 | 2 | 2 | 2 | 2 |
| Unbiased assessment of the study endpoint | 2 | 2 | 2 | 2 | 2 | 2 | 2 | 2 | 2 | 2 | 0 |
| Follow-up period appropriate to the aim of the study | 2 | 2 | 0 | 2 | 2 | 2 | 2 | 0 | 0 | 2 | 2 |
| Loss to follow-up less than 5% | 1 | 2 | 0 | 2 | 2 | 2 | 2 | 0 | 0 | 2 | 2 |
| Prospective calculation of the study size | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| Total score | 9 | 10 | 6 | 10 | 10 | 10 | 10 | 6 | 4 | 12 | 6 |
Discussion
Skin malignancies are considered the most common primary malignancies of the hand.9 Although basal cell carcinoma accounts for 80% of all cutaneous malignancies, squamous cell carcinoma occurs more frequently on the hand when compared to basal cell carcinoma.9
Furthermore, the dorsum of the hand is considered a frequently sun-exposed area. However, hand BCC occurrences are relatively uncommon when compared to the head and neck.6 This is mainly attributed to the deficiency of pilosebaceous glands in that area.21 Moreover, Zuuren et al. argue that the dorsum of the hand is considered a rare site of BCC occurrence when compared to other body sites.60 When taking skin surface into account, BCC of the dorsum of the hand tends to have roughly the same frequency as other body sites—excluding the face and neck, where BCC is most common.60 To the best of the authors' knowledge, this is the first systematic review that examines a variety of clinical characteristics, investigations, and treatment options available in the literature for hand BCC. Furthermore, we have presented pooled recurrence rates based on a meta-analysis. The overall rate of hand BCC recurrence was 1.49 cases per year. However, after excluding cases treated with radiotherapy as a single modality, which accounts for the highest recurrence rate among the included studies,62 the overall incidence rate will be 1.28 cases per year, with almost all patients managed surgically. A systematic review published in 2009 investigated the clearance rate of BCC after 5 years of follow-up and found a 99% clearance rate with Mohs micrographic surgery, 91–95% with wide local excision, and radiotherapy associated with a lower clearance rate of 90%. In spite of its higher recurrence rate than surgical excision, radiotherapy still provides better cosmetic outcomes. It must be considered as one of the first nonsurgical choices in patients who cannot survive surgeries.67 A recent RCT compared the combination of curettage and cryosurgery versus curettage and electrodesiccation in managing sBCC. At 12 months of follow-up, only one patient experienced a recurrence in the cryosurgery group. Both techniques had good scar results by the end of the study. Nonetheless, the short follow-up period might not reflect reality, and more studies are needed to investigate the combination of different modalities.55 However, involvement of the nail unit is much more frequent on the fingernails than on toes.28 In these studies, 34 out of 2051 patients experienced fingernail involvement with variable morphological features including ulcerative, longitudinal plaque, or onychodystrophy.20, 21, 22,28,31,33,35,36,38,42,43,45,46,48, 49, 50 Many of the reported studies found initial difficulties in obtaining the correct diagnosis of BCC due to the wide variety of lesions and malignancies that can arise from the hand with similar morphological features, including glomus tumor,29 melanoma,50 and actinic keratosis.20 These findings highlight the importance of performing biopsies in cases with uncertain diagnoses or failure of treatments to detect misdiagnosis. Almost all patients with nail involvement were managed surgically by MSS (43%), simple excision (31%), or amputation (19%). None of the patients experienced recurrence except for a single case reported ten months post-operation. The author suggested a minimal clearance margin of 0.5 mm to be responsible for the recurrence rather than the failure of the modality.38 Mohs micrographic surgery has shown superiority in the clearance rate and the advantages in preserving the adjacent soft tissue with high accuracy. Therefore, the integrity of sophisticated hand function is preserved. The need for soft-tissue coverage post-excision is variable according to the lesion size and site. Several studies reported the successful usage of FTSG with optimum function restoration and good cosmetic outcomes.20,32,41,46 In a single case report, a local flap was used successfully, but two months later, a recurrence occurred and ended with amputation of the thumb.38 However, in most cases, where Mohs micrographic surgery has been used, they found no indication for autologous reconstruction and managed the case by dressing and healing subsequently by secondary intention.21,29,28,33
To our knowledge, this systematic review and meta-analysis are the first to investigate the current management options and outcomes of BCC in the hand. The strengths of this systematic review and meta-analysis are that it is noncommercial, has strict inclusion and exclusion criteria, and was reported in line with the PRISMA criteria with no deviations from the protocol. The methodological quality and synthesis of all the studies were assessed for bias, and all had MINORS above 70%. This study analyzed the most recent hand BCC studies at the time of writing, providing the most comprehensive data pool available. Nonetheless, our study has several limitations. First, most of our results were based on case reports, which comprised most of the studies included in this systematic review, with the weakest evidence level. Second, most of the studies included in this study were from North America and Europe; hence, the results may not be generalizable. Third, not all studies included in this systematic review are recent, mainly due to the paucity of published articles discussing this topic. Finally, a long-term follow-up period is needed to measure the accurate prognosis, and not all studies had a sufficient follow-up period. Due to heterogeneity and a lack of data from several studies, prospective randomized studies are needed to shed light on the recurrence rate, management of hand BCC, and health advances. In conclusion, the treatment options for BCC of the hand vary depending on the presentation. Moh surgery was the preferred treatment option for hand BCC with no reported recurrences, whereas radiotherapy alone had the highest recurrence rate and inferior cosmetic results. The overall incidence rate of recurrence among the included patients was 1.28 case years (95%CI, 0.76 to 2.14). Collaboration between different medical practitioners is required to manage hand BCC. In the future, research should focus on developing an appropriate set of criteria for treating BCCs of the hands, especially regarding the recurrence rates of various treatments and the long-term complications of such treatments.
Statements and declarations
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Declaration of Competing Interests
The authors have no relevant financial or nonfinancial interests to disclose.
Acknowledgments
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was waived due to the nature of the study.
Acknowledgement
This work was supported by the College of Medicine Research Center, Deanship of Scientific Research, King Saud University Medical City, King Saud University, Riyadh, Saudi Arabia.
Contributor Information
Hatan Mortada, Email: Hatanmortada@gmail.com.
Rema Aldihan, Email: Reema.aldihan@gmail.com.
Nawaf Alhindi, Email: Nalhindi0010@stu.kau.edu.sa.
Rakan Abu alqam, Email: rakanalqam97@gmail.com.
Muna Faisal Alnaim, Email: Monafalnaim@gmail.com.
Abdullah E. Kattan, Email: kattan@me.com.
References
- 1.Fania L., Didona D., Morese R., et al. Basal cell carcinoma: from pathophysiology to novel therapeutic approaches. Biomedicines. 2020;8(11):449. doi: 10.3390/biomedicines8110449. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Ceilley R.I., Del Rosso J.Q. Current modalities and new advances in the treatment of basal cell carcinoma. Int J Dermatol. 2006;45(5):489–498. doi: 10.1111/j.1365-4632.2006.02673.x. [DOI] [PubMed] [Google Scholar]
- 3.Hoban P.R., Ramachandran S., Strange R.C. Environment, phenotype and genetics: risk factors associated with BCC of the skin. Expert Rev Anticancer Ther. 2002;2(5):570–579. doi: 10.1586/14737140.2.5.570. [DOI] [PubMed] [Google Scholar]
- 4.Garg S., Carroll R.P., Walker R.G., Ramsay H.M., Harden P.N. Skin cancer surveillance in renal transplant recipients: re-evaluation of U.K. practice and comparison with Australian experience. Br J Dermatol. 2009;160(1):177–179. doi: 10.1111/j.1365-2133.2008.08837.x. [DOI] [PubMed] [Google Scholar]
- 5.Betti R., Bruscagin C., Inselvini E., Crosti C. Basal cell carcinomas of covered and unusual sites of the body. Int J Dermatol. 1997;36(7):503–505. doi: 10.1046/j.1365-4362.1997.00139.x. [DOI] [PubMed] [Google Scholar]
- 6.Loh T.Y., Rubin A.G., Brian Jiang S.I. Basal cell carcinoma of the dorsal hand: an update and comprehensive review of the literature. Dermatol Surgery. 2016;42(4):464–470. doi: 10.1097/DSS.0000000000000695. [DOI] [PubMed] [Google Scholar]
- 7.Silapunt S., Peterson S.R., Goldberg L.H., Friedman P.M., Alam M. Basal cell carcinoma on the vermilion lip: a study of 18 cases. J Am Acad Dermatol. 2004;50(3):384–387. doi: 10.1016/j.jaad.2003.08.027. [DOI] [PubMed] [Google Scholar]
- 8.Maciburko S.J., Townley W.A., Hollowood K., Giele H.P. Skin cancers of the hand: a series of 541 malignancies. Plast Reconstr Surg. 2012;129(6):1329–1336. doi: 10.1097/PRS.0b013e31824ecc58. [DOI] [PubMed] [Google Scholar]
- 9.Ilyas E.N., Leinberry C.F., Ilyas A.M. Skin cancers of the hand and upper extremity. J Hand Surg [Am] 2012;37(1):171–178. doi: 10.1016/j.jhsa.2011.10.042. [DOI] [PubMed] [Google Scholar]
- 10.Piro G.F., Collier D.U. Basal cell carcinoma of the palm. J Am Acad Dermatol. 1995;33(5 Pt 1):823–824. doi: 10.1016/0190-9622(95)91839-6. [DOI] [PubMed] [Google Scholar]
- 11.Leibovitch I., Huilgol S.C., Selva D., Richards S., Paver R. Basal cell carcinoma treated with Mohs surgery in Australia II. Outcome at 5-year follow-up. J Am Acad Dermatol. 2005;53(3):452–457. doi: 10.1016/j.jaad.2005.04.087. [DOI] [PubMed] [Google Scholar]
- 12.Moher D., Liberati A., Tetzlaff J., Altman D.G., PRISMA Group Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6(7) doi: 10.1371/journal.pmed.1000097. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Higgins, J.P.T., & Green, S. (2011). eds. Cochrane Handbook for Systematic Reviews of Interventions Version 5.1. 0. The Cochrane Collaboration
- 14.Ouzzani M., Hammady H., Fedorowicz Z., Elmagarmid A. Rayyan-a web and mobile app for systematic reviews. Syst Revi. 2016;5(1):210. doi: 10.1186/s13643-016-0384-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Sullivan D., Chung K.C., Eaves F.F., 3rd, Rohrich R.J. The level of evidence pyramid: indicating levels of evidence in Plastic and Reconstructive Surgery articles. Plast Reconstr Surg. 2011;128(1):311–314. doi: 10.1097/PRS.0b013e3182195826. [DOI] [PubMed] [Google Scholar]
- 16.Slim K., Nini E., Forestier D., Kwiatkowski F., Panis Y., Chipponi J. Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg. 2003;73(9):712–716. doi: 10.1046/j.1445-2197.2003.02748.x. [DOI] [PubMed] [Google Scholar]
- 17.Murad M.H., Sultan S., Haffar S., Bazerbachi F. Methodological quality and synthesis of case series and case reports. BMJ Evid-Based Med. 2018;23(2):60–63. doi: 10.1136/bmjebm-2017-110853. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Coulombe C., Gagnon L.P., Larouche V., Dionne M.C. Infantile-onset palmo-plantar basal cell carcinomas and pits in Gorlin syndrome. JAAD Case Reports. 2018;4(7):662–664. doi: 10.1016/j.jdcr.2018.06.017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Engel E., Ulrich H., Vasold R., et al. Azo pigments and a basal cell carcinoma at the thumb. Dermatology. 2008;216(1):76–80. doi: 10.1159/000109363. [DOI] [PubMed] [Google Scholar]
- 20.Forman S.B., Ferringer T.C., Garrett A.B. Basal cell carcinoma of the nail unit. J Am Acad Dermatol. 2007;56(5):811–814. doi: 10.1016/j.jaad.2006.12.027. [DOI] [PubMed] [Google Scholar]
- 21.Grine R.C., Parlette H.L., 3rd, Wilson B.B. Nail unit basal cell carcinoma: a case report and literature review. J Am Acad Dermatol. 1997;37(5 Pt 1):790–793. doi: 10.1016/s0190-9622(97)70120-8. [DOI] [PubMed] [Google Scholar]
- 22.Kim H.J., Kim Y.S., Suhr K.B., Yoon T.Y., Lee J.H., Park J.K. Basal cell carcinoma of the nail bed in a Korean woman. Int J Dermatol. 2000;39(5):397–398. doi: 10.1046/j.1365-4362.2000.00869-1.x. [DOI] [PubMed] [Google Scholar]
- 23.Kim H.S., Min J.A., Kim H.O., Park Y.M. Basal cell carcinoma of the finger resembling a pyogenic granuloma. J Dermatol. 2009;36(3):174–175. doi: 10.1111/j.1346-8138.2009.00620.x. [DOI] [PubMed] [Google Scholar]
- 24.Lam C., Fuller C., Flamm A., Billingsley E.M. Collision tumor of basal and squamous cell carcinoma of the palm. J Clin Aesthetic Dermatol. 2019;12(4):28–30. [PMC free article] [PubMed] [Google Scholar]
- 25.Lateo S., Charlton F.G., Ormond P. A palmar injury that failed to heal. Diagnosis: basal cell carcinoma of the palm. Clin Exp Dermatol. 2006;31(5):731–732. doi: 10.1111/j.1365-2230.2006.02173.x. [DOI] [PubMed] [Google Scholar]
- 26.López-Sánchez C., Ferguson P., Collgros H. Basal cell carcinoma of the palm: an unusual presentation of a common tumour. Australas J Dermatol. 2020;61(1):69–70. doi: 10.1111/ajd.13129. [DOI] [PubMed] [Google Scholar]
- 27.Machida M., Ansai S., Hida Y., Kubo Y., Arase S., Kuramoto K. Basal cell carcinoma arising on the palm. J Dermatol. 2011;38(1):94–96. doi: 10.1111/j.1346-8138.2010.00997.x. [DOI] [PubMed] [Google Scholar]
- 28.Martinelli P.T., Cohen P.R., Schulze K.E., Dorsey K.E., Nelson B.R. Periungual basal cell carcinoma: case report and literature review. Dermatol Surg. 2006;32(2):320–323. doi: 10.1111/j.1524-4725.2006.32062.x. [DOI] [PubMed] [Google Scholar]
- 29.Mikhail G.R. Subungual basal cell carcinoma. J Dermatol Surg Oncol. 1985;11(12):1222–1223. doi: 10.1111/j.1524-4725.1985.tb03101.x. [DOI] [PubMed] [Google Scholar]
- 30.Oriba H.A., Tauscheck A., Snow S.N. Basal-cell carcinoma of the finger: a case report and review of the literature. J Hand Surg [Am] 1997;22(6):1103–1106. doi: 10.1016/S0363-5023(97)80058-5. [DOI] [PubMed] [Google Scholar]
- 31.Pollo T., Rabay F., de Lima E., Gonçalves F., Mandelbaum S.H. Subungual basal cell carcinoma: a rare nail tumor with a challenging diagnosis. Skin Appendage Disorders. 2019;5(4):251–253. doi: 10.1159/000496707. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Rallis E., Nasiopoulou A., Arvanitis A. Interdigital basal cell carcinoma of the hand: a rare site. Ind J Dermatol, Venereol Leprol. 2010;76(5):593. doi: 10.4103/0378-6323.69099. [DOI] [PubMed] [Google Scholar]
- 33.Robins P., Rabinovitz H.S., Rigel D. Basal-cell carcinomas on covered or unusual sites of the body. J Dermatol Surg Oncol. 1981;7(10):803–806. doi: 10.1111/j.1524-4725.1981.tb00170.x. [DOI] [PubMed] [Google Scholar]
- 34.Sarfati B., Lazar C.C., Goubin I., Zwillinger N., Lorenceau B. Vol. 55. Elsevier Masson; 2010. Épithélioma basocellulaire des doigts: une localisation rare à ne pas ignorer; pp. 74–77. (Annales De Chirurgie Plastique Esthetique). [DOI] [PubMed] [Google Scholar]
- 35.Serrano-Ortega S., Fernández-Angel I., Dulanto-Campos E., Rodríguez-Archilla A., Linares-Solano J. Basal cell carcinoma arising in professional radiodermatitis of the nail. Br J Dermatol. 2002;147(3):628–629. doi: 10.1046/j.1365-2133.2002.500815.x. [DOI] [PubMed] [Google Scholar]
- 36.Shimizu I., Cohen P.R., Macfarlane D.F. Surgical treatment of basal cell carcinoma of the nail unit. Int J Dermatol. 2013;52(8):996–998. doi: 10.1111/ijd.12039. [DOI] [PubMed] [Google Scholar]
- 37.Tavares L.L., Costa J., Delcourt N.C., Rodrigues N. Periungual basal cell carcinoma. An Bras Dermatol. 2018;93(1):114–115. doi: 10.1590/abd1806-4841.20186515. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Tehrani H., Iqbal A. Basal cell carcinoma of the thumb. J Hand Surgery, Eur Volume. 2009;34(5):699–700. doi: 10.1177/1753193409104943. [DOI] [PubMed] [Google Scholar]
- 39.Torrelo A., Vicente A., Navarro L., et al. Early-onset acral basal cell carcinomas in Gorlin syndrome. Br J Dermatol. 2014;171(5):1227–1229. doi: 10.1111/bjd.13118. [DOI] [PubMed] [Google Scholar]
- 40.Watson M., Wichmann M., Ganguly T. Cutaneous basal cell carcinoma requiring limb amputation. ANZ J Surg. 2019;89(12):E560–E561. doi: 10.1111/ans.14971. [DOI] [PubMed] [Google Scholar]
- 41.Yousif S., Reid L., Kirkpatrick J. A case of basal cell carcinoma on the dorsum of a finger. J Hand Surg, Eur Vol. 2013;38(3):328–329. doi: 10.1177/1753193412471020. [DOI] [PubMed] [Google Scholar]
- 42.Zhu G.A., Chen A., Chang A.L. Oral smoothened inhibitor for advanced basal cell carcinoma of the hand: a case report. Hand (New York, N.Y.) 2014;9(1):127–128. doi: 10.1007/s11552-013-9555-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Dika E., Patrizi A., Fanti P.A., et al. Two synchronous periungual BCC treated with Mohs surgery. Nail polish related? Cutaneous Ocular Toxicol. 2013;32(2):161–163. doi: 10.3109/15569527.2012.708956. [DOI] [PubMed] [Google Scholar]
- 44.Enna C.D. Adenoid basal cell epithelioma involving a finger. Hand. 1978;10(3):309–311. doi: 10.1016/s0072-968x(78)80057-6. [DOI] [PubMed] [Google Scholar]
- 45.Galeano M., Lentini M., Stagno D'Alcontres F., Colonna M. Bowenoid basal cell carcinoma of the thumb: a case report and review of the literature. Hand Surg. 2002;7(2):295–298. doi: 10.1142/s0218810402001060. [DOI] [PubMed] [Google Scholar]
- 46.Guana A.L., Kolbusz R., Goldberg L.H. Basal cell carcinoma on the nailfold of the right thumb. Int J Dermatol. 1994;33(3):204–205. doi: 10.1111/j.1365-4362.1994.tb04985.x. [DOI] [PubMed] [Google Scholar]
- 47.Higuchi M., Mori O., Hachisuka H. Basal cell epithelioma involving a finger. Kurume Med J. 1988;35(4):225–227. doi: 10.2739/kurumemedj.35.225. [DOI] [PubMed] [Google Scholar]
- 48.Hoffman S. Basal cell carcinoma of the nail bed. Arch Dermatol. 1973;108(6):828. [PubMed] [Google Scholar]
- 49.Okuyama R., Watanabe H., Aiba S., Tagami H. Subungual basal cell carcinoma in an elderly Japanese woman. Acta Derm Venereol. 2006;86(3):261. doi: 10.2340/00015555-0038. [DOI] [PubMed] [Google Scholar]
- 50.Rudolph R.I. Subungual basal cell carcinoma presenting as longitudinal melanonychia. J Am Acad Dermatol. 1987;16(1 Pt 2):229–233. doi: 10.1016/s0190-9622(87)80069-5. [DOI] [PubMed] [Google Scholar]
- 51.Salomão P., Kopke L.F., MacHado-Pinto J. Palmar basal cell carcinoma: case report and literature review. Dermatol Surg. 1999;25(11):908–910. doi: 10.1046/j.1524-4725.1999.99047.x. [DOI] [PubMed] [Google Scholar]
- 52.West J.R., Berman B. Basal cell carcinoma presenting as a chronic finger ulcer. J Am Acad Dermatol. 1990;23(2 Pt 1):318–319. doi: 10.1016/s0190-9622(08)81243-1. [DOI] [PubMed] [Google Scholar]
- 53.Abeldaño A.M., Tiscornia J., Cendeño L.P., Brea P., Chouela E.N. Basal cell carcinoma in palm and sole. Skinmed. 2006;5(1):40–42. doi: 10.1111/j.1540-9740.2006.04057.x. [DOI] [PubMed] [Google Scholar]
- 54.Özkan A. Reverse dorsal metacarpal flaps for reconstruction of proximal phalanx defects following skin tumor excision: a case series. Eur J Plastic Surg. 2017;40(4):337–342. [Google Scholar]
- 55.Fournier S., Laroche A., Leblanc M., et al. Prospective clinical trial comparing curettage and cryosurgery to curettage and electrodesiccation in the management of minimally invasive basal and squamous cell carcinomas. J Cutan Med Surg. 2020;24(6):596–600. doi: 10.1177/1203475420943258. [DOI] [PubMed] [Google Scholar]
- 56.Riml S., Larcher L., Kompatscher P. Complete excision of nonmelanotic skin cancer: a matter of surgical experience. Ann Plast Surg. 2013;70(1):66–69. doi: 10.1097/SAP.0b013e3182223d7b. [DOI] [PubMed] [Google Scholar]
- 57.Vandeweyer E., Herszkowicz A. Basal cell carcinoma of the dorsum of the hand. Acta Chir Belg. 2003;103(3):300–303. doi: 10.1080/00015458.2003.11679428. [DOI] [PubMed] [Google Scholar]
- 58.Tripoli M., Cordova A., Moschella F. Characteristics, management techniques, and outcomes of the most common soft-tissue hand tumors: a literature review and our experience. Ann Plast Surg. 2017;79(6):558–565. doi: 10.1097/SAP.0000000000001148. [DOI] [PubMed] [Google Scholar]
- 59.Tripoli M., Franza M., Cordova A. An overview and our approach in the treatment of malignant cutaneous tumours of the hand. Acta Chir Plast. 2020;62(1–2):4–9. [PubMed] [Google Scholar]
- 60.van Zuuren E.J., Bastiaens M.T., Posma A.N., Bouwes Bavinck J.N. Basal cell carcinoma on the dorsum of the hand: report of 11 cases. J Eur Acad Dermatol Venereol. 2000;14(4):307–310. doi: 10.1046/j.1468-3083.2000.00106.x. [DOI] [PubMed] [Google Scholar]
- 61.Chakrabarti I., Watson J.D., Dorrance H. Skin tumours of the hand. A 10-year review. J Hand Surg (Edinburgh, Scotland) 1993;18(4):484–486. doi: 10.1016/0266-7681(93)90153-7. [DOI] [PubMed] [Google Scholar]
- 62.Fischbach A.J., Sause W.T., Plenk H.P. Radiation therapy for skin cancer. West J Med. 1980;133(5):379–382. [PMC free article] [PubMed] [Google Scholar]
- 63.Bean D.J., Rees R.S., O'Leary J.P., Lynch J.B. Carcinoma of the hand: a 20-year experience. South Med J. 1984;77(8):998–1000. doi: 10.1097/00007611-198408000-00016. [DOI] [PubMed] [Google Scholar]
- 64.CLIFFORD R.H., KELLY A.P., Jr Primary malignant tumors of the hand. Plastic Reconstruct Surg. 1955;15(3):227–232. doi: 10.1097/00006534-195503000-00007. [DOI] [PubMed] [Google Scholar]
- 65.Kendall T.E., Robinson D.W., Masters F.W. Primary malignant tumors of the hand. Plast Reconstr Surg. 1969;44(1):37–40. doi: 10.1097/00006534-196907000-00005. [DOI] [PubMed] [Google Scholar]
- 66.Clinical characteristics of basal cell carcinomas of the dorsal hand: a 7-year, single institution retrospective review. J Am Acad Dermatol. 2015;72(5):AB182. doi: 10.1016/j.jaad.2015.02.743. [DOI] [Google Scholar]
- 67.Thomson J., Hogan S., Leonardi-Bee J., Williams H.C., Bath-Hextall F.J. Interventions for basal cell carcinoma: abridged Cochrane systematic review and GRADE assessments. Br J Dermatol. 2021;185(3):499–511. doi: 10.1111/bjd.19809. [DOI] [PubMed] [Google Scholar]