Case
A man in his 60 s presented to the emergency department with fever, weakness and lower extremity pain. The patient had an 11-year history of mantle cell lymphoma and was undergoing treatment with ibrutinib.
He was found to be febrile to 38.4 °C, hypotensive, and tachycardic with a large dark brown thin plaque on the right lower leg with a violaceous, reticulated border and overlying bullae (Fig. 1 A-B). The remainder of his exam was remarkable for tender, edematous, erythematous papules and nodules diffusely. White blood cell count was 3100 cells per microliter in comparison to 9600 the day prior. Serum creatinine had increased from 2.3 mg/dl to 5.0 mg/dl and lactate level was elevated (5 mmol/L). Blood cultures were obtained and a punch biopsy of skin was performed for histologic examination and cultures.
Fig. 1.
A - B: Patient’s leg showing thin dark brown plaque with darkly violaceous to erythematous border surrounding dusky appearing bullae with surrounding violaceous indurated papules.
Immediate diagnostic and therapeutic considerations focused on infectious etiologies. Differential diagnosis included cutaneous vasculitis, autoimmune bullous disease, neutrophilic conditions including bullous Sweet’s Syndrome, or a reaction to chemotherapy such as ibrutinib induced skin toxicity.
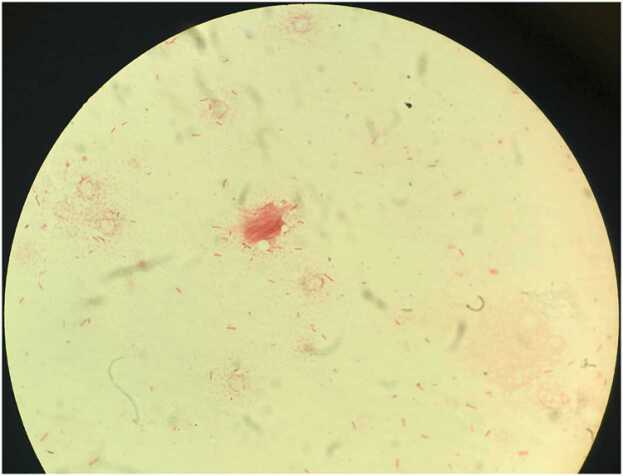
A smear from a touch prep of the punch biopsy revealed Gram negative rods (Fig. 2). Histopathology demonstrated thrombosis and organisms within and surrounding the deep dermal vessels with overlying subepidermal bullae and epidermal necrosis consistent with ecthyma gangrenosum. Gram stain of the tissue revealed Gram negative rods in the vessel walls (Fig. 3) and cultures grew Pseudomonas aeruginosa.
Fig. 2.
Gram stain of a smear of punch biopsy of skin showing Gram negative rods.
Fig. 3.
Histopathologic examination of a medium sized vessel shows numerous Gram negative bacteria (Gram Stain, original magnification 40x).
Pseudomonas aeruginosa is a Gramnegative bacillus with several skin and soft tissue manifestations. Infection can develop in areas exposed to moisture with or without skin disruption such as “hot tub folliculitis”, nail infections, external ear infections, and Pseudomonas hot-foot syndrome; and carry a good prognosis [1], [2], [3]. In contrast, ecthyma gangrenosum, infection of burns, and other skin or systemic infections in immunocompromised individuals can be life-threatening [2]. Ecthyma gangrenosum results from bacterial invasion into the media and adventitia of vessels. The presence of retiform purpura is a sign of medium vessel involvement. P. aeruginosa is one cause of ecthyma gangrenosum although other bacterial, viral, and fungal pathogens can present with similar morphologies and tissue culture is necessary [4]. When ecthyma gangrenosum is suspected and Gramnegative rods are isolated, antipseudomonal antimicrobial therapy should be initiated.
He remained critically ill despite treatment with cefepime, levofloxacin and meropenem. He subsequently developed acute respiratory failure and the family elected to withdraw life support. This case illustrates the urgency in establishing a diagnosis of ecthyma gangrenosum.
CRediT authorship contribution statement
Chae A. Sutherland: Writing – original draft, Visualization. Tyler L. Quest: Conceptualization, Writing – review & editing. Karolyn A. Wanat: Conceptualization, Writing – review & editing, Supervision.
Ethical approval
N/A
Consent
Written informed consent was obtained from the patient for use of images for publication.
Funding
None.
Conflict of interest
None.
Author contribution
Please specify the contribution of eachauthor to the paper, e.g. study design, data collections, dataanalysis, writing, others, who have contributedin other ways should be listed as contributors.
Footnotes
The authors have no declarations of interest. This manuscript is original work and is not under consideration for publication elsewhere. All authors meet the criteria for authorship and authors will sign a statement attesting authorship, disclose all potential conflicts of interest, and release the copyright should the manuscript be accepted for publication.
All authors had access to the data and contributed to writing this case.
References
- 1.Silvestre J.F., Betlloch M.I. Cutaneous manifestations due to pseudomonas infection. Int J Dermatol. 1999;38(6):419–431. doi: 10.1046/j.1365-4362.1999.00606.x. [DOI] [PubMed] [Google Scholar]
- 2.Fiorillo L., Zucker M., Sawyer D., Lin A.N. The pseudomonas hot-foot syndrome. N Eng J Med. 2001;345(5):335–338. doi: 10.1056/nejm200108023450504. [DOI] [PubMed] [Google Scholar]
- 3.Gucluer H., Ergun T., Demircay Z. Ecthyma gangrenosum. Int J Dermatol. 1999;38(4):299–302. doi: 10.1046/j.1365-4362.1999.00691.x. [DOI] [PubMed] [Google Scholar]
- 4.Reich H.L., Williams Fadeyi D., Naik N.S., Honig P.J., Yan A.C. Nonpseudomonal ecthyma gangrenosum. J Am Acad Dermatol. 2004;50(5):114–117. doi: 10.1016/j.jaad.2003.09.019. [DOI] [PubMed] [Google Scholar]